Abstract
Aim
In-hospital paediatric cardiopulmonary resuscitation (CPR) survival has been improving in high-income countries. This study aimed to analyse factors associated with survival and neurological outcome after paediatric CPR in a middle-income country.
Methods
This observational study of in-hospital cardiac arrest using Utstein-style registry included patients <18 years old submitted to CPR between 2015 and 2020, at a high-complexity hospital. Outcomes were survival and neurological status assessed using Paediatric Cerebral Performance Categories score at prearrest, discharge, and after 180 days.
Results
Of 323 patients who underwent CPR, 108 (33.4%) survived to discharge and 93 (28.8%) after 180 days. In multivariable analysis, lower survival at discharge was associated with liver disease (OR 0.060, CI 0.007–0.510, p = 0.010); vasoactive drug infusion before cardiac arrest (OR 0.145, CI 0.065–0.325, p < 0.001); shock as the immediate cause (OR 0.183, CI 0.069–0.486, p = 0.001); resuscitation > 30 min (OR 0.070, CI 0.014–0.344, p = 0.001); and bicarbonate administration during CPR (OR 0.318, CI 0.130–0.780, p = 0.01). The same factors remained associated with lower survival after 180 days. Neurological outcome was analysed in the 93 survivors after 180 days following CPR. Prearrest neurological dysfunction was observed in 31.4%, and neurological prognosis was favourable in 79.7% at discharge and similar after 180 days.
Conclusion
In-hospital paediatric cardiac arrest patients with complex chronic conditions had lower survival associated with liver disease, shock as cause of cardiac arrest, vasoactive drug infusion before cardiac arrest, bicarbonate administration during CPR, and prolonged resuscitation. Most survivors had favourable neurological outcome.
Keywords: Cardiac arrest, Cardiopulmonary resuscitation, In-hospital cardiac arrest, Pediatric, Prognostic factors, Neurological outcome
Introduction
Cardiac arrest is an infrequent event in the paediatric population compared to that in adults.1, 2 The estimated annual incidence in the United States is 292,000 cases in adults and 15,200 cases in children, posing a major challenge for conducting paediatric studies with robust data.2
The literature reports great variation in paediatric cardiac arrest outcomes due to different populations analysed, hospital and department characteristics, different outcomes, level of development between countries, and study periods.1, 3, 4, 5, 6, 7 However, there is a trend toward improved survival to discharge rate as high as 43% to 45%, in high-income countries.8, 9 In addition to survival, reports on neurological prognosis have gained increasing importance in paediatric resuscitation studies.1, 3, 9, 10, 11, 12, 13
An increased paediatric population with pre-existing chronic conditions has also been observed, reaching more than 50% of patients in paediatric intensive care.14, 15 Another subgroup of the paediatric population with increasing importance is patients with complex chronic conditions, defined as any condition expected to last at least 12 months, involving one major organ or with systemic involvement, requiring specialized follow-up, or involving hospitalization in a tertiary centre.16 This population has a high mortality rate and a greater need for intensive care and length of stay17; however, the factors associated with the prognosis of cardiac arrest in children with complex chronic conditions are unclear.
Most studies on in-hospital paediatric cardiac arrest involve large cardiopulmonary resuscitation (CPR) registries, multicentre studies, and single-centre studies with voluntary participation, with data especially concentrated in high-income countries.3, 4, 18, 19, 20, 21, 22, 23, 24, 25 The epidemiology of paediatric cardiac arrest was identified by the International Liaison Committee on Resuscitation as a priority area for larger studies.26
The primary objective of this study was to evaluate the factors associated with survival at discharge and after 180 days. The secondary objective was to analyse the neurological outcome.
Methods
Design, setting and patients
This observational study used data derived from the hospital cardiac arrest record that followed the Utstein style27 and had been filled out by the professionals responsible for patient care. The Paediatric Cerebral Performance Category (PCPC) score was used to assess neurological function through the analysis of medical records and interviews with professionals and family members. Neurological function was classified as favourable (Paediatric Cerebral Performance Category 1 or 2 or no change from baseline) or unfavourable (Paediatric Cerebral Performance Category ≥ 3). Only the index event was considered.
The data were collected during the period between January 1, 2015 and December 31, 2020 from a single center, which is a quaternary university public paediatric hospital with a rapid response team and a paediatric early warning system. Extracorporeal cardiopulmonary resuscitation is not offered during CPR. It is located in Sao Paulo, Brazil, in the biggest hospital complex of the country.
The study was approved by the local ethics and research committee, CAAE: 29237420.7.0000.0068. A presumed consent form was used due to the difficulty in obtaining a signature in extreme emergency situations.28, 29, 30
Participants
The study population included patients <18 years of age undergoing in-hospital cardiac arrest. The exclusion criteria were patients who did not receive CPR, out of hospital cardiac arrest, children with surgical cardiac diseases, trauma patients, and cardiac arrest in the delivery room. Trauma patients and patients with surgical heart diseases were treated in other sectors of the hospital complex.
Of the initial 447 patients, 323 were eligible, corresponding to the study population.
Independent variables
The data on the following variables were collected: sex, age, day of the week, period of the day and year when the cardiac arrest occurred, complex chronic conditions category, event location, interventions in place at time of cardiac arrest (mechanical ventilation, vasoactive drug infusion), immediate cause of cardiac arrest, duration of CPR attempt, initial cardiac rhythm, and drugs used during CPR (adrenaline, bicarbonate, and calcium). Paediatric Cerebral Performance Category score was evaluated in the periods prearrest, at discharge, and after 180 days. Dose, time, and interval of adrenaline administration; CPR quality parameters; and post-cardiac arrest care variables were not analysed.
Outcomes
Outcomes included survival and neurological status at hospital discharge and after 180 days. Neurological function was assessed using the Paediatric Cerebral Performance Category score prearrest, at discharge, and after 180 days.
Statistical analyses
Statistical analyses were conducted using IBM SPSS software version 24 and R software version 3.5. Outcomes were compared between groups using the Pearson’s chi-square test or Fisher’s exact test for categorical variables. Univariable and multivariable logistic regression analyses were performed to assess the effect of each one of the factors on survival to hospital discharge and survival at 180 days. All individual factors with statistical significance in the univariable analysis and p-value <0.10 were eligible for inclusion in the logistic regression model. Adjusted odds ratios (OR) and 95% confidence intervals (CI) were calculated for each model. P values less than 0.05 were considered significant.
Results
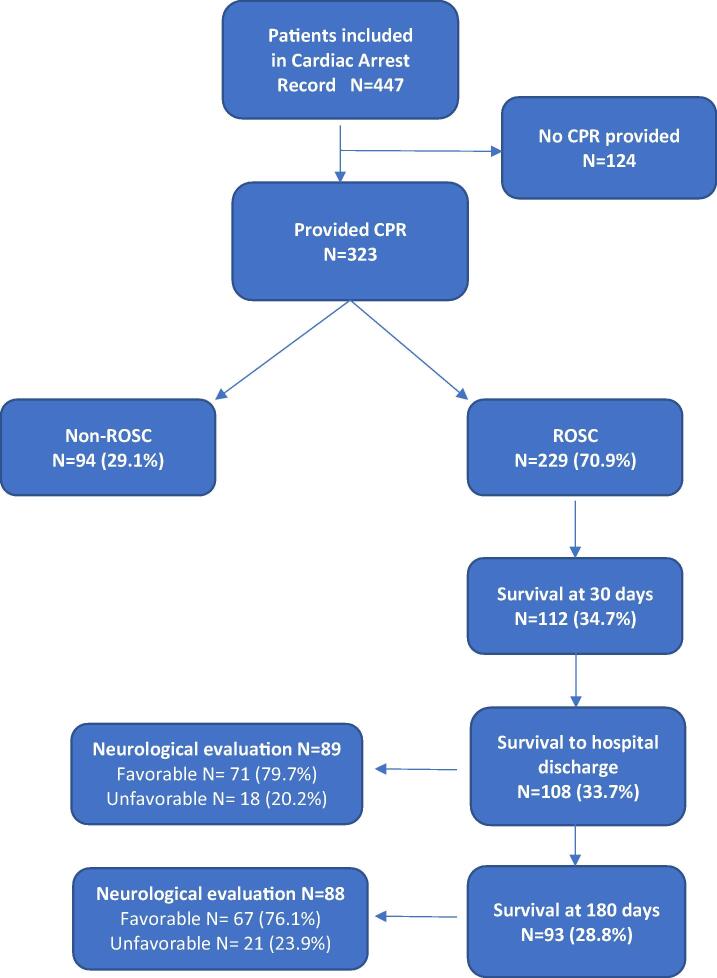
Of 323 patients who underwent CPR, 229 (70.9%) achieved return of spontaneous circulation (ROSC), 112 (34.7%) survived after 30 days, 109 (33.7%) to discharge, and 93 (28.8%) after 180 days (Fig. 1).
Fig. 1.
Patient inclusion flowchart and neurological outcome. CPR: cardiopulmonary resuscitation, ROSC: return of spontaneous circulation.
The characteristics of the study population are presented in Table 1. The following variables showed statistically significant differences: complex chronic conditions category, event location, day of the week and time of cardiac arrest, interventions prior to CPR (vasoactive drug infusion and mechanical ventilation), immediate cardiac arrest cause, CPR duration, and drugs given during CPR (adrenaline, bicarbonate, and calcium).
Table 1.
Characteristics of survivors versus non-survivors at hospital discharge.
| Total | Survival to hospital discharge |
|||
|---|---|---|---|---|
| Characteristics | n (%) | Survivors n (%) |
No survivors n (%) |
P-value |
| N = 323 | N = 109 | N = 214 | ||
| Year | ||||
| 2015 | 65 (20.1) | 24 (22.0) | 41 (19.2) | 0.19 |
| 2016 | 64 (19.8) | 21 (19.3) | 43 (20.1) | |
| 2017 | 59 (18.3) | 15 (13.8) | 44 (20.6) | |
| 2018 | 43 (13.3) | 10 (9.2) | 33 (15.4) | |
| 2019 | 47 (14.6) | 20 (18.3) | 27 (12.6) | |
| 2020 | 45 (13.9) | 19 (17.4) | 26 (12.1) | |
| Age group | ||||
| <1 month | 74 (22.9) | 19 (17.4) | 55 (25.7) | 0.06 |
| ≥1 month–1 year | 119 (36.8) | 50 (45.9) | 69 (32.2) | |
| ≥1–12 years | 107 (33.1) | 35 (32.1) | 72 (33.6) | |
| ≥12 years old | 23 (7.1) | 5 (4.6) | 18 (8.4) | |
| Sex | ||||
| Female | 164 (50.8) | 61 (56) | 103 (48.1) | 0.18 |
| Male | 159 (49.2) | 48 (44) | 111 (51.9) | |
| Complex chronic condition | ||||
| No | 12 (3.7) | 8 (7.3) | 4 (1.9) | 0.01 |
| Yes | 311 (96.3) | 101 (92.7) | 210 (98.1) | |
| Disease categories | ||||
| Prenatal condition or complications | 83 (25.7) | 26 (23.9) | 57 (26.6) | 0.002 |
| Hepatic | 77 (23.8) | 14 (12.8) | 63 (29.4) | |
| Genetic or metabolic | 59 (18.3) | 21 (19.3) | 38 (17.8) | |
| Oncohematologic or immunologic | 27 (8.4) | 10 (9.2) | 17 (7.9) | |
| Other | 65 (20.1) | 30 (27.5) | 35 (16.4) | |
| Event location | ||||
| PICU | 259 (80.2) | 77 (70.6) | 182 (85.0) | 0.005 |
| Emergency department | 29 (9.0) | 11 (10.1) | 18 (8.4) | |
| OR/Endoscopy/Diagnostic area | 25 (7.7) | 15 (13.8) | 10 (4.7) | |
| Wards | 10 (3.1) | 6 (5.5) | 4 (1.9) | |
| Period of the week | ||||
| Weekday | 237 (73.4) | 83 (76.1) | 154 (72.0) | 0.42 |
| Weekend | 86 (26.6) | 26 (23.9) | 60 (28.0) | |
| Period of the day | ||||
| Day (7 am–6:59 pm) | 184 (57.0) | 77 (70.6) | 107 (50.0) | <0.001 |
| Night (7 pm–6:59 am) | 139 (43.0) | 32 (29.4) | 107 (50.0) | |
| Witnessed | ||||
| No | 2 (0.6) | 1 (0.9) | 1 (0.5) | 0.62 |
| Yes | 321 (99.4) | 108 (99.1) | 213 (99.5) | |
| Previous interventions | ||||
| Mechanical ventilation | ||||
| No | 88 (27.2) | 43 (39.4) | 45 (21.0) | 0.002 |
| Yes | 232 (71.8) | 65 (59.6) | 167 (78.0) | |
| Unknown | 3 (0.9) | 1 (0.9) | 2 (0.9) | |
| Vasoactive drugs | ||||
| No | 168 (52.0) | 90 (82.6) | 78 (36.4) | <0.001 |
| Yes | 152 (47.1) | 18 (16.5) | 134 (62.6) | |
| Unknown | 3 (0.9) | 1 (0.9) | 2 (0.9) | |
| Immediate cause | ||||
| Respiratory | 153 (47.4) | 78 (71.6) | 75 (35.0) | <0.001 |
| Shock | 121 (37.5) | 10 (9.2) | 111 (51.9) | |
| Metabolic | 32 (9.9) | 9 (8.3) | 23 (10.7) | |
| Arrhythmia | 8 (2.5) | 5 (4.6) | 3 (1.4) | |
| Unknown | 9 (2.8) | 7 (6.4) | 2 (0.9) | |
| Rhythm | ||||
| Bradycardia | 181 (56.0) | 69 (63.3) | 112 (52.3) | 0.16 |
| PEA | 77 (23.8) | 24 (22.0) | 53 (24.8) | |
| Asystole | 49 (15.2) | 10 (9.2) | 39 (18.2) | |
| VT/VF | 10 (3.1) | 3 (2.8) | 7 (3.3) | |
| Unknown | 6 (1.9) | 3 (2.8) | 3 (1.4) | |
| CPR duration | ||||
| Up to 5 min | 130 (40.2) | 65 (59.6) | 65 (30.4) | <0.001 |
| >5–15 min | 87 (26.9) | 28 (25.7) | 59 (27.6) | |
| >15–30 min | 61 (18.9) | 12 (11) | 49 (22.9) | |
| >30 min | 42 (13.0) | 3 (2.8) | 39 (18.2) | |
| Unknown | 3 (0.9) | 1 (0.9) | 2 (0.9) | |
| Epinephrine | ||||
| No | 38 (11.8) | 25 (22.9) | 13 (6.1) | <0.001 |
| Yes | 285 (88.2) | 84 (77.1) | 201 (93.9) | |
| Bicarbonate | ||||
| No | 186 (57.6) | 89 (81.7) | 97 (45.3) | <0.001 |
| Yes | 137 (42.4) | 20 (18.3) | 117 (54.7) | |
| Calcium | ||||
| No | 226 (70.0) | 91 (83.5) | 135 (63.1) | <0.001 |
| Yes | 97 (30.0) | 18 (16.5) | 79 (36.9) | |
Subtitles PICU, paediatric intensive care unit; OR, operating room; PEA, pulseless electrical activity; VT, pulseless ventricular taquicardia; VF, ventricular fibrilation; CPR, cardiopulmonary resuscitation. Significant values in bold.
Patients <1 year old (59.7%) constituted the dominant population. Nearly the entire sample (96.3%) had a complex chronic conditions, the most frequent being prenatal conditions and complications (25.7%) and liver diseases (23.8%), followed by genetic-metabolic diseases (18.3%) and onco-hematologic and immunological diseases (8.4%).
The intensive care unit (ICU) was the location with the highest number of CPR occurrences (80.2%), followed by those in the emergency room (9%), operating room (7.7%), and wards (3.1%). CPR events were proportionally similar between weekdays and weekends, and 57% were during the daytime period.
Of the interventions in place prior to CPR, it is noteworthy that most patients (71.8%) were under mechanical ventilation and nearly half (47.1%) were on vasoactive drug support, reflecting the severity of the patient's condition. The primary immediate causes were respiratory (47.4%) and shock-related (37.5%), followed by metabolic (9.9%) and arrhythmias (2.5%).
Bradycardia, pulseless electrical activity, and asystole were the most frequent initial rhythms, and the presence of shockable rhythms was rare (3.1%). Short-duration CPR (up to 15 minutes) occurred in most events (67.1%), although the rate of prolonged CPR (>30 minutes) was not negligible (13.3%).
Adrenaline was used in the vast majority (88.2%) of patients. Bicarbonate and calcium, which are not routinely recommended by CPR guidelines, were used in 42.4% and 30% of patients, respectively.
Factors associated with survival to discharge
Table 2 presents the univariable analysis. The following factors were significantly associated with lower survival to discharge: age <1 month; liver disease; prenatal conditions and complications; occurrence at night;, interventions prior to CPR;, shock as the immediate cause; asystole as the initial rhythm; CPR duration >5 minutes; and use of adrenaline, bicarbonate, or calcium during CPR.
Table 2.
Regression analysis for characteristics associated with survival to hospital discharge.
| Characteristics | Univariate |
Multivariate |
||||
|---|---|---|---|---|---|---|
| OR | CI (95%) | P-value | OR | CI (95%) | P-value | |
| Age group | ||||||
| <1 month | 0.477 | [0.252; 0.901] | 0.02 | 0.954 | [0.349; 2.609] | 0.92 |
| ≥1 month–<1 year | 1.000 | – | – | 1.000 | – | – |
| ≥1 year–<12 years | 0.671 | [0.389; 1.155] | 0.15 | 0.997 | [0.421; 2.361] | 0.99 |
| ≥12 years old | 0.383 | [0.133; 1.102] | 0.07 | 0.341 | [0.068; 1.724] | 0.19 |
| Sex | ||||||
| Female | 1.000 | – | – | |||
| Male | 0.730 | [0.459; 1.161] | 0.18 | |||
| Complex chronic conditions | ||||||
| No | 1.000 | – | – | |||
| Yes | 0.240 | [0.071; 0.817] | 0.02 | |||
| Disease categories | ||||||
| Absent | 1.000 | – | – | 1.000 | – | – |
| Hepatic | 0.111 | [0.029; 0.421] | 0.001 | 0.060 | [0.007; 0.510] | 0.010 |
| Prenatal condition or complications | 0.228 | [0.063; 0.826] | 0.02 | 0.248 | [0.030; 2.036] | 0.19 |
| Other | 0.429 | [0.117; 1.566] | 0.20 | 0.119 | [0.015; 0.933] | 0.04 |
| Oncohematologic or immunologic | 0.294 | [0.070; 1.232] | 0.09 | 0.288 | [0.031; 2.632] | 0.27 |
| Genetic or metabolic | 0.276 | [0.074; 1.027] | 0.05 | 0.134 | [0.016; 1.190] | 0.06 |
| Event location | ||||||
| PICU | 1.000 | – | – | 1.000 | – | – |
| Wards | 3.545 | [0.973; 12.917] | 0.05 | 2.094 | [0.229; 19.134] | 0.51 |
| Emergency department | 1.444 | [0.652; 3.202] | 0.36 | 0.796 | [0.232; 2.737] | 0.71 |
| OR/Endoscopy/Diagnostic area | 3.545 | [1.525; 8.240] | 0.003 | 18.977 | [3.832; 93.976] | <0.001 |
| Period of the week | ||||||
| Weekday | 1.000 | – | – | |||
| Weekend | 0.804 | [0.472; 1.369] | 0.42 | |||
| Period of the day | ||||||
| Day (7 h–18 h59) | 1.000 | – | – | 1.000 | – | – |
| Night (7 pm–6.59am) | 0.416 | [0.254; 0.679] | <0.001 | 0.890 | [0.418; 1.894] | 0.76 |
| Previous interventions | ||||||
| Mechanical ventilation | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.407 | [0.245; 0.676] | 0.001 | 0.721 | [0.322; 1.610] | 0.42 |
| Vasoactive drugs | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.116 | [0.065; 0.207] | <0.001 | 0.145 | [0.065; 0.325] | <0.001 |
| Immediate cause | ||||||
| Respiratory | 1.000 | – | – | 1.000 | – | – |
| Shock/hypotension | 0.087 | [0.042; 0.178] | <0.001 | 0.183 | [0.069; 0.486] | 0.001 |
| Metabolic/Arrhythmia/Sudden/Unknown | 0.721 | [0.377; 1.379] | 0.32 | 1.739 | [0.632; 4.784] | 0.28 |
| Rhythm | ||||||
| Bradycardia | 1.000 | – | – | 1.000 | – | – |
| Assistolia | 0.416 | [0.195; 0.887] | 0.02 | 0.911 | [0.310; 2.682] | 0.86 |
| PEA | 0.735 | [0.417; 1.297] | 0.28 | 1.393 | [0.567; 3.422] | 0.47 |
| VT/VF | 0.696 | [0.174; 2.780] | 0.60 | 0.391 | [0.044; 3.474] | 0.39 |
| Unknown | 1.623 | [0.319; 8.269] | 0.56 | 0.781 | [0.051; 12.050] | 0.85 |
| CPR duration | ||||||
| Up to 5 min | 1.000 | – | – | 1.000 | – | – |
| >5–15 min | 0.475 | [0.269; 0.836] | 0.010 | 0.807 | [0.353; 1.845] | 0.61 |
| >15–30 min | 0.245 | [0.119; 0.503] | <0.001 | 0.317 | [0.106; 0.950] | 0.04 |
| >30 min | 0.077 | [0.023; 0.261] | <0.001 | 0.070 | [0.014; 0.344] | 0.001 |
| Epinephrine | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.217 | [0.106; 0.445] | <0.001 | 0.517 | [0.171; 1.561] | 0.24 |
| Bicarbonate | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.186 | [0.107; 0.324] | <0.001 | 0.318 | [0.130; 0.780] | 0.01 |
| Calcium | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.338 | [0.190; 0.602] | <0.001 | 1.022 | [0.403; 2.589] | 0.96 |
95% CI indicates 95% confidence interval; OR, odds ratio; PICU, paediatric intensive care unit; OR; operating room; PEA, pulseless electrical activity; VT, pulseless ventricular tachycardia; VF, ventricular fibrillation. Significant values in bold.
Multivariable analysis (Table 2) found lower survival to discharge to be significantly associated with pre-existing liver disease, vasoactive drug support before cardiac arrest, shock as the immediate cause, CPR prolonged duration, and use of bicarbonate during CPR.
Factors associated with survival after 180 days
Table 3 shows the factors associated with survival after 180 days found in univariable analysis. Male sex; liver disease; genetic and metabolic disease; prenatal conditions or complications; occurrence at night; interventions in place at time of event (mechanical ventilation and vasoactive drug infusion); shock as the immediate cause; asystole as initial rhythm; CPR duration >5 minutes; and use of adrenaline, bicarbonate, or calcium during CPR were significantly associated with lower survival after 180 days. Multivariable analysis identified following variables significantly associated with lower survival after 180 days: pre-existing liver disease, vasoactive drug support before cardiac arrest, shock as the immediate cause, CPR prolonged duration, and use of bicarbonate during CPR.
Table 3.
Regression analysis for characteristics associated with survival at 180 days.
| Characteristics | Univariate |
Multivariate |
||||
|---|---|---|---|---|---|---|
| OR | CI (95%) | P-value | OR | CI (95%) | P-value | |
| Age group | ||||||
| <1 month | 0.612 | [0.314; 1.192] | 0.14 | 1.603 | [0.574; 4.474] | 0.36 |
| ≥1 month–<1 year | 1.000 | – | – | 1.000 | – | – |
| ≥1 year–<12 years | 0.928 | [0.527; 1.633] | 0.79 | 1.588 | [0.669; 3.769] | 0.29 |
| ≥12 years old | 0.570 | [0.197; 1.652] | 0.30 | 0.651 | [0.135; 3.130] | 0.59 |
| Sex | ||||||
| Female | 1.000 | – | – | 1.000 | – | – |
| Male | 0.610 | [0.374; 0.995] | 0.04 | 0.554 | [0.280; 1.097] | 0.09 |
| Complex chronic conditions | ||||||
| No | 1.000 | – | – | – | – | – |
| Yes | 0.221 | [0.063; 0.775] | 0.01 | – | – | – |
| Disease categories | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Hepatic | 0.105 | [0.027; 0.417] | 0.001 | 0.070 | [0.007; 0.693] | 0.02 |
| Prenatal condition or complications | 0.178 | [0.047; 0.674] | 0.01 | 0.159 | [0.016; 1.534] | 0.11 |
| Other | 0.406 | [0.108; 1.526] | 0.18 | 0.122 | [0.013; 1.120] | 0.06 |
| Oncohematologic or immunologic | 0.336 | [0.078; 1.441] | 0.14 | 0.310 | [0.030; 3.220] | 0.32 |
| Genetic or metabolic | 0.251 | [0.065; 0.965] | 0.04 | 0.131 | [0.014; 1.266] | 0.07 |
| Event location | ||||||
| PICU | 1.000 | – | – | 1.000 | – | – |
| Wards | 4.669 | [1.276; 17.084] | 0.02 | 4.550 | [0.474; 43.628] | 0.18 |
| Emergency department | 1.902 | [0.852; 4.246] | 0.11 | 1.291 | [0.368; 4.530] | 0.69 |
| OR/Endoscopy/Diagnostic area | 3.962 | [1.711; 9.176] | 0.001 | 11.858 | [2.540; 55.349] | 0.002 |
| Period of the week | ||||||
| Weekday | 1.000 | – | – | |||
| Weekend | 0.920 | [0.531; 1.593] | 0.76 | |||
| Period of the day | ||||||
| Day (7 am − 6:59 pm) | 1.000 | – | – | 1.000 | – | – |
| Night (7 pm – 6:59 am) | 0.416 | [0.248; 0.699] | 0.001 | 0.762 | [0.355; 1.635] | 0.48 |
| Previous interventions | ||||||
| Mechanical ventilation | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.492 | [0.292; 0.831] | 0.008 | 1.037 | [0.464; 2.317] | 0.93 |
| Vasoactive drugs | ||||||
| No | 1.000 | – | – | |||
| Yes | 0.136 | [0.075; 0.249] | <0.001 | 0.192 | [0.085; 0.437] | <0.001 |
| Immediate cause | ||||||
| Respiratory | 1.000 | – | – | 1.000 | – | – |
| Shock/hypotension | 0.088 | [0.040; 0.194] | <0.001 | 0.163 | [0.057; 0.472] | 0.001 |
| Metabolic/Arrhythmia/Sudden/Unknown | 0.719 | [0.370; 1.397] | 0.33 | 1.271 | [0.470; 3.436] | 0.63 |
| Rhythm | ||||||
| Bradycardia | 1.000 | – | – | 1.000 | – | – |
| Assistolia | 0.394 | [0.173; 0.893] | 0.02 | 0.628 | [0.210; 1.879] | 0.40 |
| PEA | 0.756 | [0.419; 1.365] | 0.35 | 1.034 | [0.429; 2.491] | 0.94 |
| TV/FV | 0.864 | [0.216; 3.464] | 0.83 | 0.345 | [0.037; 3.250] | 0.35 |
| Unknown | 1.345 | [0.219; 8.267] | 0.74 | 0.787 | [0.031; 19.699] | 0.88 |
| CPR duration | ||||||
| Up to 5 min | 1.000 | – | – | 1.000 | – | – |
| >5–15 min | 0.523 | [0.291; 0.942] | 0.03 | 0.978 | [0.431; 2.217] | 0.95 |
| >15–30 min | 0.331 | [0.161; 0.682] | 0.003 | 0.513 | [0.167; 1.571] | 0.24 |
| >30 min | 0.068 | [0.016; 0.292] | <0.001 | 0.048 | [0.007; 0.340] | 0.002 |
| Epinephrine | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.229 | [0.113; 0.466] | <0.001 | 0.502 | [0.175; 1.445] | 0.20 |
| Bicarbonate | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.198 | [0.110; 0.355] | <0.001 | 0.347 | [0.138; 0.870] | 0.02 |
| Calcium | ||||||
| No | 1.000 | – | – | 1.000 | – | – |
| Yes | 0.372 | [0.203; 0.680] | 0.001 | 1.285 | [0.503; 3.280] | 0.60 |
95% CI indicates 95% confidence interval; OR, odds ratio; PICU, paediatric intensive care unit; OR, operating room; PEA, pulseless electrical activity; VT, pulseless ventricular tachycardia; VF, ventricular fibrillation. Significant values in bold.
Neurological outcome
Table 4 and Fig. 1 shows the neurological outcome in the 93 survivors after 180 days. Approximately-one-third already presented prearrest neurological dysfunction. Between the prearrest and discharge period, 20.2% of patients had an unfavourable prognosis. Neurological outcome was similar between discharge and after 180 days. Twenty-three patients with severe dysfunction prearrest (Paediatric Cerebral Performance Category 4) remained stable after 180 days. Neurological outcome was mostly favourable at discharge (79.7%) and after 180 days (76.1%).
Table 4.
Neurological outcome.
| PCPC | Pre-arrest N % |
Hospital Discharge N % |
180 days N % |
|||
|---|---|---|---|---|---|---|
| 1 | 56 | 60.2% | 31 | 33.3% | 30 | 32.3% |
| 2 | 7 | 7.5% | 15 | 16.1% | 11 | 11.8% |
| 3 | 5 | 5.4% | 5 | 5.4% | 8 | 8.6% |
| 4 | 23 | 24.7% | 41 | 44.1% | 41 | 44.1% |
| Unknown | 2 | 2.2% | 1 | 1.1% | 3 | 3.2% |
| Total | 93 | 100.0% | 93 | 100.0% | 93 | 100.0% |
PCPC, pediatric cerebral performance categories; N, number of patients.
Univariable and multivariable analysis was conducted to evaluate factors associated with good neurological prognosis was carried out in the 93 survivors after 180 days. In multivariable analysis, factors associated with favourable neurological prognosis age >1 year (OR: 23.894, 95%CI 2.735–208.735, p = 0.004) and non-administration of vasoactive drugs pre-CPR (OR: 4.518, 95%CI 1.116–18.291, p = 0.03) (Supplemental Table 1).
Discussion
This study analysed the association of a set of factors with paediatric CPR survival in patients with complex chronic conditions in a high-complexity hospital. Prior liver disease, vasoactive drug support before CA, shock as the immediate cause, prolonged CPR, and use of bicarbonate were significantly associated with lower survival both at discharge and after 180 days. Most patients had a favourable neurological prognosis at discharge and after 180 days.
This study is characterized by a robust sample of patients with complex chronic conditions (96.3%) in a middle-income country, where literature data are scarce. Patients with complex chronic conditions have a higher frequency of hospitalization,17 which is related with life expectancy currently increasing, likely as result of early diagnosis and technological advances, especially in cardiorespiratory support. This population should be highlighted in studies on in-hospital CPR from now on.
Paediatric in-hospital CPR outcomes greatly vary according to different services and between countries (Table 5). Inequality in cardiac arrest care, which depends on training, expertise, human resources, equipment, ICU beds, and multidisciplinary team along with the variability in human development indexes may explain the different outcomes.
Table 5.
Characterization of pediatric in-hospital CPR (adaptation of López-Herce, under authorization).
| Author | Country | Year | Study Type | N | Setting | ROSC (%) | Survival to discharge (%) | Good neurological survival (%) | 6 months or 1 year survival (%) |
|---|---|---|---|---|---|---|---|---|---|
| Slonin48 | USA | 1997 | Prospective | 205 | PICU | UNK | 13.7 | UNK | UNK |
| Suominen24 | Finland | 2000 | Retrospective | 118 | In-hospital | 62.7 | 19.5 | 12.7 | 17.8 |
| Reis3 | Brazil | 2002 | Prospective | 129 | In-hospital | 64 | 16.2 | 89.5 | 14.7 |
| Guay49 | Canada | 2004 | Retrospective | 203 | In-hospital | 73.8 | 40.8 | 23.4 | 26 |
| Rodriguez-Nuñes50 | Spain | 2006 | Prospective | 116 | PICU | 59.5 | 35.3 | 31 | 34.5 |
| Tibballs19 | Australia | 2006 | Prospective | 111 | In-hospital | 76 | 36 | UNK | 34 |
| Nadkarni1 | USA,Canada | 2006 | Prospective | 880 | In-hospital | 52 | 27 | 18 | UNK |
| de Mos51 | Canada | 2006 | Retrospective | 91 | PICU | 82 | 25 | 18 | UNK |
| Meaney38 | USA | 2006 | Prospective | 411 | PICU | 48.9 | 21.4 | 14 | UNK |
| Wu52 | China | 2009 | Retrospective | 316 | In-hospital | 72.2 | 20.9 | 15.5 | UNK |
| Olotu53 | Kenya | 2009 | Prospective | 114 | In-hospital | UNK | 22 | ND | UNK |
| Moreno54 | Argentina | 2010 | Prospective | 132 | PICU | 53 | 19.7 | 16.6 | UNK |
| Berens55 | USA | 2011 | Retrospective | 257 | In-hospital | 56.8 | 31.1 | 19.8 | UNK |
| Matos39 | USA | 2013 | Retrospective | 3419 | In-hospital | 63.7 | 27.9 | 19 | UNK |
| Girotra11 | USA | 2013 | Retrospective | 1031 | In-hospital | UNK | 34.8 | 61 | UNK |
| Zeng7 | China | 2013 | Prospective | 174 | In-hospital | 62.1 | 28.2 | 86 | 12.1 |
| López-Herce4 | Multinational | 2013 | Prospective | 502 | In-hospital | 69.5 | 39.2 | 34.8 | UNK |
| López-Herce40 | Spain | 2014 | Prospective | 200 | In-hospital | 74 | 41 | 77.9 | UNK |
| Straney42 | Australia, New Zealand | 2015 | Prospective | 677 | PICU | UNK | 63.7 | UNK | UNK |
| Rathore12 | India | 2016 | Prospective | 314 | In-hospital | 64.6 | 14 | 77 | 11.1 |
| Gupta46 | USA | 2017 | Retrospective | 154 | PICU | 100 | 66.6 | 94.3 | UNK |
| Andersen23 | USA | 2017 | Prospective | 182 | In-hospital | UNK | 53.8 | UNK | UNK |
| Sutton10 | USA | 2018 | Prospective | 164 | PICU | 90 | 47 | 75.7 | UNK |
| Edward-Jackson57 | Malawi | 2019 | Prospective | 135 | In-hospital | 6 | 0 | 0 | 0 |
| Mustafa58 | England | 2021 | Retrospective | 1528 | PICU | UNK | 61.9 | UNK | UNK |
| Hamzah59 | USA | 2021 | Retrospective | 20654 | In-hospital | UNK | 39.8 | UNK | UNK |
| Lee33 | China | 2022 | Retrospective | 233 | PICU | 74.8 | 25 | 21.9 | UNK |
| Shimoda-Sakano | Brazil | 2022 | Prospective | 323 | In-hospital | 70.9 | 33.7 | 79.7 | 28.8 |
CPR, cardiopulmonary resuscitation; N, number of patients; ROSC, return of spontaneous circulation; PICU, pediatric intensive care unit; UNK, unknown.
However, rates of survival to discharge (33.7%) and after 180 days (29.2%) as shown in this study are aligned with the literature from high-income countries (Table 5). Additionally, there was an overall improvement in survival when comparing a similar study previously conducted in the same hospital with the current data (ROSC from 64% to 70.9%; survival to discharge 16.3–33.7%; survival after 180 days 15.5–29.2%, respectively).3
In-hospital paediatric cardiac arrest typically occurs in patients with pre-existing diseases, who account for 71.0% to 90.9% of cases.20, 3, 4, 5, 31, 32, 33 In the present study, 96.3% of patients had complex chronic conditions, reinforcing the literature findings on the increased prevalence in this population.17 The prognosis of cardiac arrest appears to be influenced by the complex chronic conditions category, and thus further studies must address this issue.
Liver disease was the most frequent condition noted in the current study, having been associated with lower rates of survival to discharge and after 180 days. Previous studies in the same hospital have already reported liver disease as the most common condition.3, 34 These findings can be attributed to the fact that the hospital is a reference in liver transplantation and receive severely ill patients from all over the country. Delayed diagnosis and difficulty in accessing the hospital due to the continental size of Brazil may explain the greater severity.
Although comparison with other studies depends on institutional characteristics, data from children and adults also reported lower survival in cirrhotic patients35, 36 and unfavourable neurological prognosis.37
The administration of vasoactive drugs before cardiac arrest was associated with lower survival to hospital discharge and after 180 days along with poorer neurological prognosis. Other authors also have observed the same association with lower survival to hospital discharge12, 33, 38, as well as poorer neurological outcome.33 The use of vasoactive drug support may reflect patient condition and the association with lower survival rates may be a marker of severity rather than cause-and-effect relationship.
The main causes of cardiac arrest were respiratory (47.4%) and shock (37.5%), aligned to the literature.1, 3, 31, 39 Shock associated with lower survival to hospital discharge and after 180 days is confirmed by other studies.23, 40 The increasing number of children surviving with severe chronic diseases may explain the mortality due to shock.
The present study showed that the longer the CPR, the lower the survival rate at discharge and after 180 days, both in univariable and multivariable analysis. This influence of CPR duration on prognosis was also observed by other authors.3, 4, 9, 24, 31, 39, 41, 42 A multicentre registry reported a drop of 2.1% per minute in survival to discharge and of 1.2% per minute in favourable outcome in events which CPR duration was inferior to 15 min.39 However, it is possible to obtain a good prognosis, even in prolonged CPR. Studies including CPR duration greater than 30 minutes showed favourable neurological outcome in 60% to 89% of CPR events.9, 39 In addition, survival rates of 16.6% has been observed in patients undergoing CPR lasting longer than 35 min.39
CPR duration is a variable that is influenced by pre-cardiac arrest and intra-CPR events, and thus should be considered as an important prognostic factor. A child with chronic disease, who has shock and cardiac arrest in asystole, is expected to have longer CPR than a child who develops symptomatic bradycardia due to asphyxia and recover with ventilation, chest compression and one adrenaline dose.
The analysis of adrenaline's role in survival is complex and could not be explored in this study. Data on the time to the first dose, doses interval, and the number of doses are important in the analysis and were not collected in this study. In addition, other factors such as CPR duration and the initial rhythm of cardiac arrest should be considered. Holmberg et al. described in children receiving CPR for bradycardia with poor perfusion that adrenaline was associated with worse outcomes and this, at least partially, explains how complex it is to analyze the influence of adrenaline on survival.60
The use of bicarbonate during CPR was frequent and associated with lower survival to hospital discharge and after 180 days. In a meta-analysis, the use of bicarbonate during in-hospital paediatric cardiac arrest was also frequent (43.7–65.6%) and associated with lower survival to hospital discharge.43 Despite not being routinely recommended by paediatric resuscitation guidelines,44, 45 it is likely indicated in prolonged cardiac arrest in patients with high complexity or due to lower adherence to advanced life support recommendations.
Neurological outcome was favourable in 76.1% of survivors after 180 days and this result is confirmed by others studies.3, 4, 11, 31, 42, 46 Pre-cardiac arrest neurological dysfunction in complex chronic conditions carriers is expected and was present in about one-third (31.4%) of patients. Significant worsening of neurological function (20.2%) occurred between prearrest and discharge periods, but not between discharge and 180-day periods.
Patients with severe prearrest dysfunction (Paediatric Cerebral Performance Category 4) remained unchanged after 180 days. This group may not have had any Paediatric Cerebral Performance Category changes or this score is not sensitive enough to detect worsening brain function in patients with previous severe involvement. The International Liaison Committee on Resuscitation, through the Paediatric Core Outcome Set for Cardiac Arrest (P-COSCA) initiative, suggests the use of the Paediatric Cerebral Performance Category score, despite its limitations, for being validated and extensively used in paediatric CPR studies and for the possibility of being applied to children from birth to 18 years of age.47
Among the strengths of this study, some must be highlighted: the study included paediatric patients with complex chronic conditions, an increasingly important population; it was conducted in a middle-income country where epidemiological studies are scarce; it is a robust sample for a single centre; included Paediatric Cerebral Performance Category evaluation prearrest and post-cardiac arrest; and compared data from the current study with a previous one carried out in the same hospital.
Some of the limitations were those inherent to the performance of a study in a single centre, albeit the local validity remains, which may reflect the reality of tertiary and quaternary hospitals in middle-income countries. Although the recording of all CPR have been encouraged, it is not possible to guarantee that data regarding all eligible patients were recorded. Additionally, only the index event was considered, i.e., the first CPR performed in the hospital, and other cardiac arrest events may have negatively influenced survival and neurological outcome. Patients with trauma and surgical cardiac diseases have very specific characteristics and were not included, which may have influenced the comparison with other studies.
Conclusions
In-hospital paediatric cardiac arrest in patients with complex chronic conditions had lower survival to discharge and after 180 days associated with liver disease, shock as immediate cause of the arrest, vasoactive drug support before cardiac arrest, bicarbonate administration during CPR, and prolonged CPR attempt. Neurological outcome was favourable in most patients and similar in the evaluations performed at discharge and after 180 days.
Declaration of conflicts of interest
Authors have nothing to disclose with regard to commercial support.
Role of the funding source
The authors have not received any funding for undertaking this work.
Ethics and patient consent
These were not required for this study.
Collaborators
Tania M Shimoda-Sakano was responsible for data acquisition, analysed data, drafted the article and reviewed the manuscript.
Amelia G Reis was responsible for the conceptualization and designed the study, coordinated and supervised data collection, carried out the initial analyses and critically reviewed the manuscript.
Edison F Paiva supervised data collection, analysed the data, critically reviewed and helped to draft the manuscript.
Claudio Schvartsman revised the data and critically reviewed the manuscript.
All authors approved the final article as submitted, and agree to be accountable for all aspects of the work.
Contributors
Tania M Shimoda-Sakano was responsible for data acquisition, analyzed data, drafted the article and reviewed the manuscript.
Amelia G Reis was responsible for the conceptualization and designed the study, coordinated and supervised data collection, carried out the initial analyses and critically reviewed and the manuscript.
Paiva EF supervised data collection, analysed the data, critically reviewed and helped to draft the manuscript.
Schvartsman C revised the data and critically reviewed the manuscript.
All authors approved the final article as submitted, and agree to be accountable for all aspects of the work.
Footnotes
Supplementary material to this article can be found online at https://doi.org/10.1016/j.resplu.2022.100354.
Appendix A. Supplementary material
The following are the Supplementary material to this article:
References
- 1.Nadkarni V.M., Larkin G.L., Peberdy M.A., et al. First documented rhythm and clinical outcome from in-hospital cardiac arrest among children and adults. JAMA. 2006;295:50–57. doi: 10.1001/jama.295.1.50. [DOI] [PubMed] [Google Scholar]
- 2.Holmberg M.J., Ross C.E., Fitzmaurice G.M., et al. Annual Incidence of Adult and Pediatric In-Hospital Cardiac Arrest in the United States. Circ Cardiovasc Qual Outcomes. 2019;12:e005580. [PMC free article] [PubMed] [Google Scholar]
- 3.Reis A.G., Nadkarni V., Perondi M.B., Grisi S., Berg R.A. A prospective investigation into the epidemiology of in-hospital pediatric cardiopulmonary resuscitation using the international Utstein reporting style. Pediatrics. 2002;109:200–209. doi: 10.1542/peds.109.2.200. [DOI] [PubMed] [Google Scholar]
- 4.López-Herce J., Del Castillo J., Matamoros M., et al. Factors associated with mortality in pediatric in-hospital cardiac arrest: a prospective multicenter multinational observational study. Intensive Care Med. 2013;39:309–318. doi: 10.1007/s00134-012-2709-7. [DOI] [PubMed] [Google Scholar]
- 5.Del Castillo J., López-Herce J., Matamoros M., et al. Long-term evolution after in-hospital cardiac arrest in children: Prospective multicenter multinational study. Resuscitation. 2015;96:126–134. doi: 10.1016/j.resuscitation.2015.07.037. [DOI] [PubMed] [Google Scholar]
- 6.Alten J.A., Klugman D., Raymond T.T., et al. Epidemiology and Outcomes of Cardiac Arrest in Pediatric Cardiac ICUs. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc. 2017;18:935–943. doi: 10.1097/PCC.0000000000001273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Zeng J., Qian S., Zheng M., Wang Y., Zhou G., Wang H. The epidemiology and resuscitation effects of cardiopulmonary arrest among hospitalized children and adolescents in Beijing: an observational study. Resuscitation. 2013;84:1685–1690. doi: 10.1016/j.resuscitation.2013.08.007. [DOI] [PubMed] [Google Scholar]
- 8.Martinez P.A., Totapally B.R. The epidemiology and outcomes of pediatric in-hospital cardiopulmonary arrest in the United States during 1997 to 2012. Resuscitation. 2016;105:177–181. doi: 10.1016/j.resuscitation.2016.06.010. [DOI] [PubMed] [Google Scholar]
- 9.Berg R.A., Nadkarni V.M., Clark A.E., et al. Eunice Kennedy Shriver National Institute of Child Health and Human Development Collaborative Pediatric Critical Care Research Network. Incidence and Outcomes of Cardiopulmonary Resuscitation in PICUs. Crit Care Med. 2016;44:798–808. doi: 10.1097/CCM.0000000000001484. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Sutton R.M., Reeder R.W., Landis W., et al. Chest compression rates and pediatric in-hospital cardiac arrest survival outcomes. Resuscitation. 2018;130:159–166. doi: 10.1016/j.resuscitation.2018.07.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Girotra S., Spertus J.A., Li Y., et al. Survival trends in pediatric in-hospital cardiac arrests: an analysis from Get With the Guidelines-Resuscitation. Circ Cardiovasc Qual Outcomes. 2013;6:42–49. doi: 10.1161/CIRCOUTCOMES.112.967968. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Rathore V., Bansal A., Singhi S.C., Singhi P., Muralidharan J. Survival and neurological outcome following in-hospital paediatric cardiopulmonary resuscitation in North India. Paediatr Int Child Health. 2016;36:141–147. doi: 10.1179/2046905515Y.0000000016. [DOI] [PubMed] [Google Scholar]
- 13.Morgan R.W., Reeder R.W., Meert K.L., et al. Survival and Hemodynamics During Pediatric Cardiopulmonary Resuscitation for Bradycardia and Poor Perfusion Versus Pulseless Cardiac Arrest. Crit Care Med. 2020;48:881–889. doi: 10.1097/CCM.0000000000004308. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Junior C.J., Prata-Barbosa A., Lima-Setta F., et al. Brazilian Research in Intensive Care (BRICnet). Prevalence and functional status of children with complex chronic conditions in Brazilian PICUs during the COVID-19 pandemic. J Pediatr (Rio J) 2022;98:484–489. doi: 10.1016/j.jped.2021.12.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Arias López M.D.P., Fernández A.L., Fiquepron K., et al. Prevalence of Children With Complex Chronic Conditions in PICUs of Argentina: A Prospective Multicenter Study. Pediatr Crit Care Med. 2020;21:e143–e151. doi: 10.1097/PCC.0000000000002223. [DOI] [PubMed] [Google Scholar]
- 16.Feudtner C., Christakis D.A., Connell F.A. Pediatric deaths attributable to complex chronic conditions: a population-based study of Washington State, 1980–1997. Pediatrics. 2000;106:205–209. [PubMed] [Google Scholar]
- 17.Edwards J.D., Houtrow A.J., Vasilevskis E.E., et al. Chronic conditions among children admitted to U.S. pediatric intensive care units: their prevalence and impact on risk for mortality and prolonged length of stay*. Crit Care Med. 2012;40:2196–2203. doi: 10.1097/CCM.0b013e31824e68cf. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Shimoda-Sakano T.M., Schvartsman C., Reis A.G. Epidemiology of pediatric cardiopulmonary resuscitation. J Pediatr (Rio J) 2020;96:409–421. doi: 10.1016/j.jped.2019.08.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Tibballs J., Kinney S. A prospective study of outcome of in-patient paediatric cardiopulmonary arrest. Resuscitation. 2006;71:310–318. doi: 10.1016/j.resuscitation.2006.05.009. [DOI] [PubMed] [Google Scholar]
- 20.Meert K.L., Donaldson A., Nadkarni V., et al. Multicenter cohort study of in-hospital pediatric cardiac arrest. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc. 2009;10:544–553. doi: 10.1097/PCC.0b013e3181a7045c. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Del Castillo J., López-Herce J., Cañadas S., et al. Iberoamerican Pediatric Cardiac Arrest Study Network RIBEPCI. Cardiac arrest and resuscitation in the pediatric intensive care unit: a prospective multicenter multinational study. Resuscitation. 2014;85:1380–1386. doi: 10.1016/j.resuscitation.2014.06.024. [DOI] [PubMed] [Google Scholar]
- 22.Jayaram N., Spertus J.A., Nadkarni V., et al. Hospital variation in survival after pediatric in-hospital cardiac arrest. Circ Cardiovasc Qual Outcomes. 2014;7:517–523. doi: 10.1161/CIRCOUTCOMES.113.000691. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Andersen L.W., Vognsen M., Topjian A., et al. Pediatric In-Hospital Acute Respiratory Compromise: A Report From the American Heart Association’s Get With the Guidelines-Resuscitation Registry. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc. 2017;18:838–849. doi: 10.1097/PCC.0000000000001204. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Suominen P., Olkkola K.T., Voipio V., Korpela R., Palo R., Räsänen J. Utstein style reporting of in-hospital paediatric cardiopulmonary resuscitation. Resuscitation. 2000;45:17–25. doi: 10.1016/s0300-9572(00)00167-2. [DOI] [PubMed] [Google Scholar]
- 25.Ortmann L., Prodhan P., Gossett J., et al. for the American Heart Association’s Get With the Guidelines-Resuscitation Investigators. Outcomes after in-hospital cardiac arrest in children with cardiac disease: a report from Get With the Guidelines-Resuscitation. Circulation. 2011;124:2329–2337. doi: 10.1161/CIRCULATIONAHA.110.013466. [DOI] [PubMed] [Google Scholar]
- 26.Kleinman M.E., Perkins G.D., Bhanji F., et al. ILCOR Scientific Knowledge Gaps and Clinical Research Priorities for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care: A Consensus Statement. Resuscitation. 2018;127:132–146. doi: 10.1016/j.resuscitation.2018.03.021. [DOI] [PubMed] [Google Scholar]
- 27.Nolan J.P., Berg R.A., Andersen L.W., et al. Cardiac Arrest and Cardiopulmonary Resuscitation Outcome Reports: Update of the Utstein Resuscitation Registry Template for In-Hospital Cardiac Arrest: A Consensus Report From a Task Force of the International Liaison Committee on Resuscitation (American Heart Association, European Resuscitation Council, Australian and New Zealand Council on Resuscitation, Heart and Stroke Foundation of Canada, InterAmerican Heart Foundation, Resuscitation Council of Southern Africa, Resuscitation Council of Asia) Resuscitation. 2019 doi: 10.1161/CIR.0000000000000710. [DOI] [PubMed] [Google Scholar]
- 28.Raymond T.T., Carroll T.G., Sales G., Morris M.C. Effectiveness of the informed consent process for a pediatric resuscitation trial. Pediatrics. 2010;125:e866–e875. doi: 10.1542/peds.2009-2427. [DOI] [PubMed] [Google Scholar]
- 29.Committee on Pediatric Emergency Medicine and Committee on Bioethics Consent for emergency medical services for children and adolescents. Pediatrics. 2011;128:427–433. doi: 10.1542/peds.2011-1166. [DOI] [PubMed] [Google Scholar]
- 30.Eltorki M., Uleryk E., Freedman S.B. Waiver of informed consent in pediatric resuscitation research: a systematic review. Acad Emerg Med. 2013;20:822–834. doi: 10.1111/acem.12180. [DOI] [PubMed] [Google Scholar]
- 31.Meert K., Telford R., Holubkov R., et al. Paediatric in-hospital cardiac arrest: Factors associated with survival and neurobehavioural outcome one year later. Resuscitation. 2018;124:96–105. doi: 10.1016/j.resuscitation.2018.01.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Rodríguez-Núñez A., López-Herce J., del Castillo J., Bellón J.M. Iberian-American Paediatric Cardiac Arrest Study Network RIBEPCI. Shockable rhythms and defibrillation during in-hospital pediatric cardiac arrest. Resuscitation. 2014;85:387–391. doi: 10.1016/j.resuscitation.2013.11.015. [DOI] [PubMed] [Google Scholar]
- 33.Lee E.P., Chan O.W., Lin J.J., Hsia S.H., Wu H.P. Risk Factors and Neurologic Outcomes Associated With Resuscitation in the Pediatric Intensive Care Unit. Front Pediatr. 2022;10 doi: 10.3389/fped.2022.834746. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Perondi M.B.M., Reis A.G., Paiva E.F., Nadkarni V.M., Berg R.A. A comparison of high-dose and standard-dose epinephrine in children with cardiac arrest. N Engl J Med. 2004;350:1722–1730. doi: 10.1056/NEJMoa032440. [DOI] [PubMed] [Google Scholar]
- 35.Knudson J.D., Neish S.R., Cabrera A.G., et al. Prevalence and outcomes of pediatric in-hospital cardiopulmonary resuscitation in the United States: an analysis of the Kids' Inpatient Database*. Crit Care Med. 2012;40:2940–2944. doi: 10.1097/CCM.0b013e31825feb3f. [DOI] [PubMed] [Google Scholar]
- 36.Oud L. In-hospital cardiopulmonary resuscitation of patients with cirrhosis: A population-based analysis. PLoS One. 2019;14:e0222873. doi: 10.1371/journal.pone.0222873. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Levy P.D., Ye H., Compton S., Chan P.S., Larkin G.L., Welch R.D. American Heart Association National Registry of Cardiopulmonary Resuscitation Investigators. Factors associated with neurologically intact survival for patients with acute heart failure and in-hospital cardiac arrest. Circ Heart Fail. 2009;2:572–581. doi: 10.1161/CIRCHEARTFAILURE.108.828095. [DOI] [PubMed] [Google Scholar]
- 38.Meaney P.A., Nadkarni V.M., Cook E.F., et al. Higher survival rates among younger patients after pediatric intensive care unit cardiac arrests. Pediatrics. 2006;118:2424–2433. doi: 10.1542/peds.2006-1724. [DOI] [PubMed] [Google Scholar]
- 39.Matos R.I., Watson R.S., Nadkarni V.M., et al. Duration of cardiopulmonary resuscitation and illness category impact survival and neurologic outcomes for in-hospital pediatric cardiac arrests. Circulation. 2013;127:442–451. doi: 10.1161/CIRCULATIONAHA.112.125625. [DOI] [PubMed] [Google Scholar]
- 40.López-Herce J., del Castillo J., Cañadas S., Rodríguez-Núñez A., Carrillo A. Spanish Study Group of Cardiopulmonary Arrest in Children. In-hospital pediatric cardiac arrest in Spain. Rev Esp Cardiol (Engl Ed) 2014;67:189–195. doi: 10.1016/j.rec.2013.07.017. [DOI] [PubMed] [Google Scholar]
- 41.Rodríguez-Núñez A., López-Herce J., del Castillo J., Bellón J.M., Iberian-American Paediatric Cardiac Arrest Study Network RIBEPCI Shockable rhythms and defibrillation during in-hospital pediatric cardiac arrest. Resuscitation. 2014;85:387–391. doi: 10.1016/j.resuscitation.2013.11.015. [DOI] [PubMed] [Google Scholar]
- 42.Straney L.D., Schlapbach L.J., Yong G., et al. Trends in PICU Admission and Survival Rates in Children in Australia and New Zealand Following Cardiac Arrest. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc. 2015;16:613–620. doi: 10.1097/PCC.0000000000000425. [DOI] [PubMed] [Google Scholar]
- 43.Chang C.Y., Wu P.H., Hsiao C.T., Chang C.P., Chen Y.C., Wu K.H. Sodium bicarbonate administration during in-hospital pediatric cardiac arrest: A systematic review and meta-analysis. Resuscitation. 2021;162:188–197. doi: 10.1016/j.resuscitation.2021.02.035. [DOI] [PubMed] [Google Scholar]
- 44.Topjian A.A., Raymond T.T., Atkins D., et al. Part 4: Pediatric Basic and Advanced Life Support: 2020 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2020;142(16_suppl_2):S469–S523. doi: 10.1161/CIR.0000000000000901. [DOI] [PubMed] [Google Scholar]
- 45.Van de Voorde P., Turner N.M., Djakow J., et al. European Resuscitation Council Guidelines 2021: Paediatric Life Support. Resuscitation. 2021;161:327–387. doi: 10.1016/j.resuscitation.2021.02.015. [DOI] [PubMed] [Google Scholar]
- 46.Gupta P., Wilcox A., Noel T.R., et al. Characterizing cardiac arrest in children undergoing cardiac surgery: A single-center study. J Thorac Cardiovasc Surg fevereiro de. 2017;153:450–458.e1. doi: 10.1016/j.jtcvs.2016.10.013. [DOI] [PubMed] [Google Scholar]
- 47.Topjian A.A., Scholefield B.R., Pinto N.P., et al. P-COSCA (Pediatric Core Outcome Set for Cardiac Arrest) in Children: An Advisory Statement From the International Liaison Committee on Resuscitation. Resuscitation. 2021;162:351–364. doi: 10.1016/j.resuscitation.2021.01.023. [DOI] [PubMed] [Google Scholar]
- 48.Slonim A.D., Patel K.M., Ruttimann U.E., Pollack M.M. Cardiopulmonary resuscitation in pediatric intensive care units. Crit Care Med. 1997;25:1951–1955. doi: 10.1097/00003246-199712000-00008. [DOI] [PubMed] [Google Scholar]
- 49.Guay J., Lortie L. An evaluation of pediatric in-hospital advanced life support interventions using the pediatric Utstein guidelines: a review of 203 cardiorespiratory arrests. Can J Anaesth J Can Anesth. 2004;51:373–378. doi: 10.1007/BF03018242. [DOI] [PubMed] [Google Scholar]
- 50.Rodríguez-Núñez A., López-Herce J., García C., et al. Pediatric defibrillation after cardiac arrest: initial response and outcome. Crit Care Lond Engl. 2006;10:R113. doi: 10.1186/cc5005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.de Mos N., van Litsenburg R.R.L., McCrindle B., Bohn D.J., Parshuram C.S. Pediatric in-intensive-care-unit cardiac arrest: incidence, survival, and predictive factors. Crit Care Med. 2006;34:1209–1215. doi: 10.1097/01.CCM.0000208440.66756.C2. [DOI] [PubMed] [Google Scholar]
- 52.Wu E.-T., Li M.-J., Huang S.-C., et al. Survey of outcome of CPR in pediatric in-hospital cardiac arrest in a medical center in Taiwan. Resuscitation. 2009;80:443–448. doi: 10.1016/j.resuscitation.2009.01.006. [DOI] [PubMed] [Google Scholar]
- 53.Olotu A., Ndiritu M., Ismael M., et al. Characteristics and outcome of cardiopulmonary resuscitation in hospitalised African children. Resuscitation. 2009;80:69–72. doi: 10.1016/j.resuscitation.2008.09.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Moreno R.P., Vassallo J.C., Sáenz S.S., et al. Estudio colaborativo multicéntrico sobre reanimación cardiopulmonar en nueve unidades de cuidados intensivos pediátricos de la República Argentina: A multicentric study [Cardiopulmonary resuscitation in nine pediatric intensive care units of the Argentine Republic] Arch Argent Pediatr. 2010;108:216–225. doi: 10.1590/S0325-00752010000300007. [DOI] [PubMed] [Google Scholar]
- 55.Berens R.J., Cassidy L.D., Matchey J., et al. Probability of survival based on etiology of cardiopulmonary arrest in pediatric patients. Paediatr Anaesth. 2011;21:834–840. doi: 10.1111/j.1460-9592.2010.03479.x. [DOI] [PubMed] [Google Scholar]
- 57.Edwards-Jackson N., North K., Chiume M., et al. Outcomes of in-hospital paediatric cardiac arrest from a tertiary hospital in a low-income African country. Paediatr Int Child Health. 2019:1–5. doi: 10.1080/20469047.2019.1570443. [DOI] [PubMed] [Google Scholar]
- 58.Mustafa K., Buckley H., Feltbower R., Kumar R., Scholefield B.R. Epidemiology of Cardiopulmonary Resuscitation in Critically Ill Children Admitted to Pediatric Intensive Care Units Across England: A Multicenter Retrospective Cohort Study. J Am Heart Assoc. 2021;10:e018177. doi: 10.1161/JAHA.120.018177. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Hamzah M., Othman H.F., Almasri M., Al-Subu A., Lutfi R. Survival outcomes of in-hospital cardiac arrest in pediatric patients in the USA. Eur J Pediatr. 2021;180:2513–2520. doi: 10.1007/s00431-021-04082-3. [DOI] [PubMed] [Google Scholar]
- 60.Holmberg M.J., Ross C.E., Yankama T., Roberts J.S., Andersen L.W. Epinephrine in children receiving cardiopulmonary resuscitation for bradycardia with poor perfusion. Resuscitation. 2020;149:180–190. doi: 10.1016/j.resuscitation.2019.12.032. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.