Abstract
Posttraumatic subcutaneous emphysema, which can be benign and noninfectious, is associated with necrotizing fasciitis. Rarely, extensive emphysema occurs after a minor traumatic injury. A 23-year-old man came to our hospital with extensive emphysema, ranging from the left hand to the axilla, after a minor injury. Necrotizing fasciitis was suspected. Based on the blood and imaging tests, necrotizing fasciitis was not actively suspected. He was admitted and observed for one day, and he was discharged the following day. The mechanism by which air can enter through a small injury is unclear, but the one-way ball-valve mechanism is the most commonly proposed explanation. The nontraumatic causes of non-infectious subcutaneous emphysema include insect bites, skin biopsies, and the use of shock absorbers. Since it developed from a minor wound, other mechanisms, aside from the one-way ball-valve, were possibly involved. Based on the imaging results of this case, the air was predominantly distributed in the subcutaneous tissue along the neurovascular bundle. The relatively sparse tissue likely caused the extensive subcutaneous emphysema. While evaluating post-traumatic subcutaneous emphysema, benign and noninfectious cases should be differentiated to prevent unnecessary therapeutic intervention.
Keywords: Subcutaneous emphysema, Benign, Noninfectious, Traumatic injury, Necrotizing fasciitis
Subcutaneous emphysema; Benign; Noninfectious; Traumatic injury; Necrotizing fasciitis.
1. Introduction
Posttraumatic subcutaneous emphysema, which can be benign and noninfectious, has been associated with necrotizing fasciitis. While traumatic pneumothorax is the most common cause of posttraumatic subcutaneous emphysema, it can also occur from minor traumatic injuries. Multiple cases of benign necrotizing fasciitis that were managed surgically have been reported [1]. When evaluating patients with subcutaneous emphysema, a benign entity should be considered to prevent unnecessary therapeutic intervention. This study reports a case of extensive noninfectious subcutaneous emphysema, caused by a minor injury to the left palm, extending to the left axilla.
2. Case report
A healthy 23-year-old man struck his left palm on the corner of an oil-stained plastic box while reflexively reaching out to retrieve it (Figure 1). He immediately experienced numbness in the left shoulder and pain in the entire upper extremity. The next day, a radiograph showed subcutaneous gas, and he was referred to our hospital due to suspected necrotizing fasciitis.
Figure 1.
Photograph of the oil-stained plastic box that the patient got injured against.
There was a 7-mm crusted contusion on his left palm and swelling in the dorsum of the left hand without erythema or heat (Figure 2). The pain reached up to the wrist joint with no associated numbness, and the snowball crepitation reached up to the left axilla. The blood test showed a slightly elevated C-reactive protein, and the Laboratory Risk Indicator for Necrotizing Fasciitis (LRINEC) score was 0 points (Figure 3). Radiographs and contrast-enhanced computed tomography (CT) showed no fracture, pneumothorax, or soft tissue infection. Air was distributed along the neurovascular bundle in the deep skin layer from the left upper limb to the axilla (Figure 4(a-c), Figure 5(a-d), Figure 6). He was admitted on the same day for close monitoring and was diagnosed with benign subcutaneous emphysema rather than necrotizing fasciitis. He was discharged on the following day and fully recovered after one month.
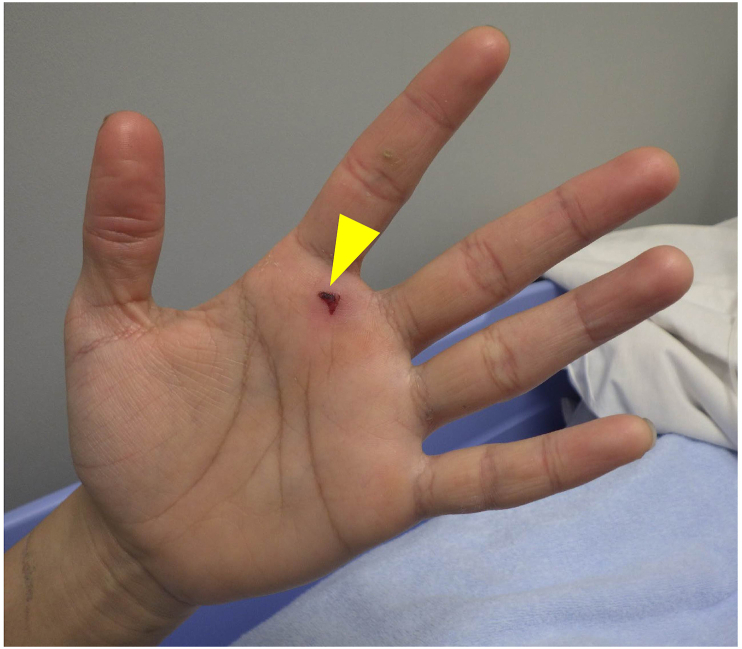
Figure 2.
Photograph of the left palm puncture site. There was a 7-mm crusted contusion on his left palm.
Figure 3.
Blood test results. White blood cell counts were not elevated, and the C-reactive protein (CRP) was mildly elevated. Laboratory Risk Indicator for Necrotizing Fasciitis (LRINEC) score∗ was 0 points.∗The LRINEC score is a robust score capable of detecting even clinically early cases of necrotizing fasciitis. Patients with a LRINEC score of ≥6 should be carefully evaluated for the presence of necrotizing fasciitis. Four points are given if the patient's CRP is ≥15 mg/dL, while 0 points are given if the patient's CRP <15 mg/dL. Two points are given if the patient's leukocyte count is >25×109/L, 1 point is given if the patient's leukocyte count is 15–25 ×109/L, and 0 points are given if the patient's leukocyte count is <15×109/L. Two points are given if the patient's hemoglobin is <11 g/dL. One point is given if the patient's hemoglobin is 11–13.5 g/dL, and 0 points are given if the patient's hemoglobin is 13.5 g/dL. Two points are given if the patient's sodium level is <135 mmol/L, while 0 points are given if the patient's sodium level is ≥135 mmol/L. Two points are given if the patient's creatinine level is >141 mmol/L, while 0 points are given if the patient's creatinine level is ≥141 mmol/L. Lastly, 1 point is given if the patient's glucose is >10 mmol/L, while 0 points are given if the patient's glucose is ≥10 mmol/L.
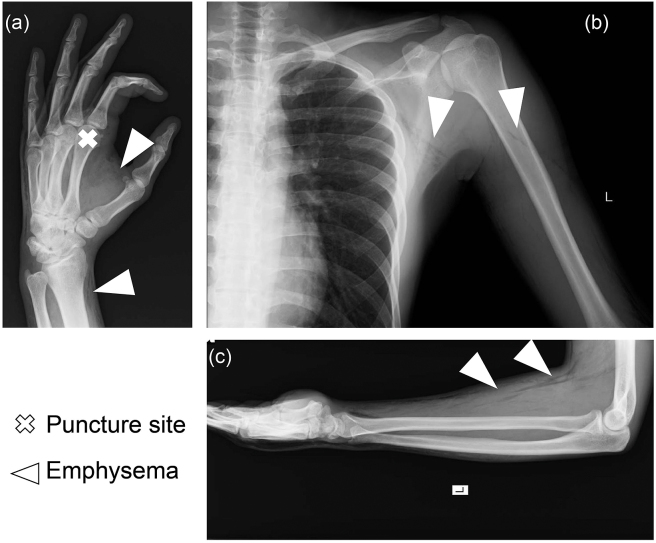
Figure 4.
Plain radiograph of the left palm (a), the left axilla (b), and the left forearm (c). Air was distributed from the left palm to the left axilla.
Figure 5.
The contrast-enhanced computed tomography image.(a) plain mediastinal window setting (b) pulmonary window setting (c) and (d) equilibrium phase mediastinal window setting Air distributed along the neurovascular bundle was seen deep in the skin from the left upper limb to the axilla.
Figure 6.
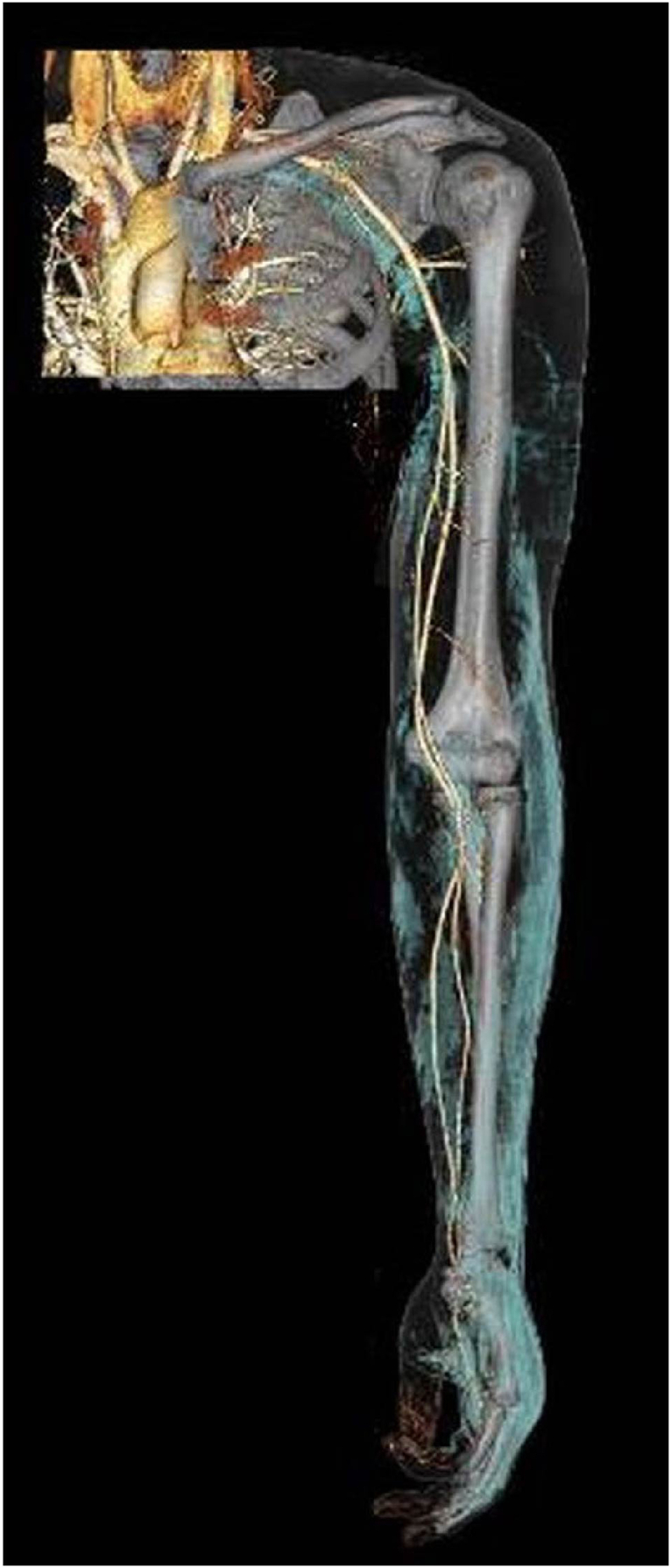
Reconstruction of the contrast-enhanced computed tomography image. Blue area is air. Air distribution was mainly in the subcutaneous area, with deeper distribution between the fascia and along the neurovascular bundle.
Written consent was obtained from the patient and patient's personal information was anonymized with great care. The patient provided informed consent for the publication of her case history.
3. Discussion
Posttraumatic subcutaneous emphysema, with a possibility of being noninfectious and benign, has been associated with necrotizing fasciitis according to many studies. Extensive benign subcutaneous emphysema rarely occurs due to minor trauma. In this case, the patient presented with a small contusion on the left palm and extensive subcutaneous emphysema, ranging from the fingertips to the axilla on the left side. However, there was no noted pneumothorax or rib fractures. No signs of infection at the wound site were found, and the patient had normal vital signs and a LRINEC score of 0 points. Therefore, necrotizing fasciitis was not a primary consideration [2].
We searched the PubMed database for "benign/noninfectious subcutaneous emphysema." Ten previous cases, excluding those involving insect bites, direct air inflow by high-pressure jets, and without trauma, were compared with the present case [3, 4, 5, 6, 7, 8, 9, 10, 11] (Table 1). The mean age was 43.18 ± 12.90, and no sex differences were noted. Most patients were right-handed, which could be accounted for the left-sided wounds observed in nine cases. Subcutaneous emphysema occurred within 20 min to one month following the injury. In most cases, it developed 9 h after the injury. However, some patients relied on their subjective judgment, while some only stated the interval between the injury and their arrival at the hospital. Thus, only vague evaluations were made. The subcutaneous emphysema was not limited to the wound's surrounding area, and it radiated to one to two proximal joints in most of the cases. The sizes of the wounds were not described in most cases.
Table 1.
Ten previous cases, excluding those involving insect bites, direct air inflow by high-pressure jets, and without trauma.
| year | author | age | sex | Feature of wound | Air distribution | Elapsed time | Reference |
|---|---|---|---|---|---|---|---|
| 1999 | van der Molen AB | 52 | M | a puncture wound in the first digital interspace | extending up to the elbow | ~9 h | [4] |
| 2005 | Lo SJ | 48 | F | a 5 mm transverse laceration on the left first dorsal webspace | the dorsum of the hand extending to the wrist joint | ~9 h | [5] |
| 2005 | Winshall JS | 59 | F | a small, clean wound over the left olecranon | the upper extremity extending from the wrist to the left hemithorax | ~4 days | [6] |
| 2007 | Fox A | 19 | M | the dorsum of his left hand | subcutaneous tissue | ∼1 month | [7] |
| 2007 | Fox A | 40 | F | a puncture wound in the first web space of her left hand | subcutaneous tissue | ~8 h | [7] |
| 2009 | Alvarez C | 30 | F | a laceration of the left forearm | from the biceps to the distal forearm | 3 h | [8] |
| 2013 | Aakash C | 46 | F | a 2-cm laceration in the left elbow | the forearm, around the elbow, and around the distal part of the humerus | ~24 h | [9] |
| 2014 | Smith MAC | 53 | M | 4 cm2 abrasion on his left elbow | from the left wrist to the left forearm | ~2 days | [10] |
| 2016 | Islam SMR | 49 | F | a trivial laceration to the right olecranon region | the right lower arm, whole forearm and dorsal aspect of the wrist | ~5・6 h | [11] |
| 2021 | Christen SM | 56 | M | a wood splinter injury in the left palm | the tip of the fingers and towards the forearm | ~20 min | [3] |
| 2021 | Kaede H | 23 | M | a 7mm-sized crusted contusion on his left palm | from the tip of the fingers to the left axilla | ~24 h |
The one-way ball-valve (check-valve) mechanism is the most frequently proposed mechanism for developing non-infectious subcutaneous emphysema after a minor trauma [2]. Samuel et al. reported a case of subcutaneous emphysema after a splinter wound of the left palm. The wood fragment reached the neurovascular bundle and became a check valve, possibly resulting in air distribution along the neurovascular bundle [3]. The reconstructed contrast-enhanced CT imaging results of this case showed air predominantly distributed in the subcutaneous tissues. Air distributed deep between the fascia and along the neurovascular bundle was also observed (Figure 6). Although measuring the depth was not feasible since the wound was already crusted at the time of the presentation, the deep, sparse tissue was accessible due to the absence of the tendon sheath. The nontraumatic causes of non-infectious subcutaneous emphysema include insect bites, skin biopsies, and the use of shock absorbers. Since the present case was caused by a minor wound, other mechanisms, aside from the one-way ball-valve mechanism, were likely involved. The one-way ball-valve mechanism alone is insufficient to explain the extensive subcutaneous emphysema.
4. Conclusion
Life-threatening necrotizing fasciitis should be suspected in patients with post-traumatic subcutaneous emphysema. However, non-infectious benign subcutaneous emphysema should also be identified to avoid unnecessary therapeutic intervention.
Declarations
Author contribution statement
Yes, all authors listed have significantly contributed to the investigation, development and writing of this article.
Funding statement
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Data availability statement
The authors do not have permission to share data.
Declaration of interest’s statement
The authors declare no competing interests.
Additional information
No additional information is available for this paper.
Acknowledgements
We would like to thank Editage (www.editage.com) for English language editing.
References
- 1.Onwochei V.E., Kelly M.E., Lyons R., Khan W., Barry K.M. Benign subcutaneous emphysema: a case report with bite. Int. J. Surg. Case Rep. 2015;9:89–91. doi: 10.1016/j.ijscr.2015.02.039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Wong C., Khin L. Clinical relevance of the LRINEC (laboratory Risk indicator for necrotizing fasciitis) score for assessment of early necrotizing fasciitis. Crit. Care Med. 2005;33:1677. doi: 10.1097/01.ccm.0000170199.43624.b8. [DOI] [PubMed] [Google Scholar]
- 3.Christen S.M., Gruenert J.G., Winsauer S. Benign subcutaneous emphysema: a rare and challenging entity a case report and review of the literature. Case Rep. Plast. Surg. Hand. Surg. 2021;8:153–157. doi: 10.1080/23320885.2021.1984922. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.van der Molen A.B., Birndorf M., Dzwierzynski W.W., Sanger J.R. Subcutaneous tissue emphysema of the hand secondary to noninfectious etiology: a report of two cases. J. Hand Surg. Am. 1999;24:638–641. doi: 10.1053/jhsu.1999.0638. [DOI] [PubMed] [Google Scholar]
- 5.Lo S.J., Hughes J., Armstrong A. Non-infective subcutaneous emphysema of the hand secondary to a minor webspace injury. J. Hand Surg. Br. 2005;30:482–483. doi: 10.1016/j.jhsb.2005.04.020. [DOI] [PubMed] [Google Scholar]
- 6.Winshall J.S., Weissman B.N. Images in clinical medicine. Benign subcutaneous emphysema of the upper extremity. N. Engl. J. Med. 2005;352:1357. doi: 10.1056/NEJMicm040914. [DOI] [PubMed] [Google Scholar]
- 7.Fox A., Sheick H., Ekwobi C., Ho-Asjoe M. Benign surgical emphysema of the hand and upper limb: gas is not always gangrene—a report of two cases. Emerg. Med. J. 2007;24:798–799. doi: 10.1136/emj.2007.046755. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Alvarez C., Julio A.M.D., Guy Stofman. Noninfectious subcutaneous emphysema of the upper extremity. Plast. Reconstr. Surg. 2009;123:154–155. doi: 10.1097/PRS.0b013e31819e5c2a. [DOI] [PubMed] [Google Scholar]
- 9.Aakash C., Brabender C., Mistovich R.J., Demeo P.J., Palmer B.A. An unusual cause for noninfectious subcutaneous emphysema of the upper extremity: a case report. JBJS Case Connect. 2013;3:e135. doi: 10.2106/JBJS.CC.M.00161. [DOI] [PubMed] [Google Scholar]
- 10.Smith M.A.C., Sivathasan N. A case of benign subcutaneous emphysema, BMJ Case Reports. BMJ Case Rep. 2014;2014 doi: 10.1136/bcr-2013-202261. bcr2013202261. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Islam S.M.R., Mamman K.G., Pande K.C. Benign subcutaneous emphysema of the upper limb: a case report. Malays. Orthop. J. 2016;10:39–41. doi: 10.5704/MOJ.1611.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The authors do not have permission to share data.