Abstract
Stylalgia also referred to as Eagle’s or stylohyoid syndrome (first described by Watt Eagle) is a constellation of signs secondary to an elongated styloid process or due to mineralization of the stylohyoid or stylomandibular ligament or the posterior belly of the digastric muscle (Malik et al. in Iran J Otorhinolaryngol 30(6): 101, 2018). The Eagle’s syndrome includes symptoms ranging from stylalgia (i.e., pain in the tonsillar fossa, pharyngeal or hyoid region) to foreign-body sensation in the throat, cervicofacial pain, otalgia or even increased salivation or giddiness. Diagnosis is primarily based on symptomatology, physical examination and radiographic investigations and should not be missed. However, palpation of tonsillar fossa with radiological demonstration of the elongated styloid process confirms the diagnosis. Surgical treatment by tonsillo-styloidectomy produces satisfactory results in stylalgia. (Malik et al. in Iran J Otorhinolaryngol 30(6):101, 2018)
Keywords: Stylalgia, Styloidectomy, Eagle’s syndrome, Stylohyoid syndrome, Cervicofacial pain
Introduction
In 1937, Watt W. Eagle, an ENT surgeon at Duke University, described the first case defined as “stylalgia” secondary to elongated styloid process or calcification of the stylohyoid ligament or to mineralization of the stylohyoid ligament [1]. Eagle described it into two subtypes: the ‘‘classic syndrome’’ and the ‘‘stylocarotid artery syndrome.’’ And the length of a normal styloid process was found to be at 2.5–3 cms. [2–5].
Eagle's syndrome is a rare clinical condition, which often presents with recurrent pain in the oropharynx and cervicofacial region, foreign body sensation in the throat, dysphagia and referred otalgia due to an elongated styloid process or calcified stylohyoid ligament [3, 6]. One should have a high level of suspicion when neurological symptoms occur upon head rotation. Symptoms tend to be worsened on bimanual palpation of the styloid through the tonsillar bed [7]. The true incidence is about 0.16%, with a female to male predominance of 3:16. Bilateral involvement is quite common but does not always involve bilateral symptoms [2]. No significant difference is detectable between the right and left sides. More important than the elongation of the styloid process and the calcification of the stylohyoid ligament is the thickening or ossification of those structures [8].
The cause of stylohyoid calcification is not well understood, but it might be related to congenital factors such as persistence of a cartilaginous analog or an embryonic precursor to the styloid process. Other possible causes include previous trauma or an inflammatory process that produces a proliferation of granulation tissue and results in calcification or ossification. Calcification can lead to compression of the adjacent structures that are innervated by the glossopharyngeal, trigeminal and the chorda tympani nerve. There might also be impingement of the plexus of the carotid sheath that produces irritation of the sympathetic nerves [9].
Diagnosis is made both radiographically and by physical examination. Palpation of the styloid process in the tonsillar fossa is indicative of elongated styloid process; styloid process of normal length is not normally palpable. If highly suspicious for Eagle’s syndrome, confirmation can be made by radiographic studies. Most frequently, X-ray Towne’s view and lateral view of the skull and upper neck are used to determine whether the styloid process is elongated [10]. CT scan is very important to measure the length of styloid process [1]. (Figs. 1 and 2).
Fig. 1.
Panoramic radiography showing bilateral elongation of the styloid process
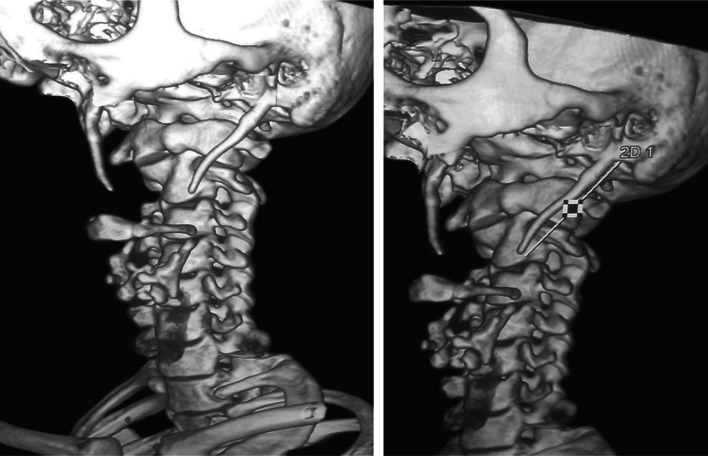
Fig. 2.
3D reconstructed CT images measuring the length of styloid process
Medical treatment includes analgesics, antidepressant and anticonvulsants. Partial/complete styloidectomy is the treatment of choice. Styloidectomy can be performed by an intraoral and extra oral approach. The intra oral approach may result in a restricted operative field, in the possibility of an incomplete control over many important vascular and nervous structures and in the risk of deep cervical infections. On the other hand, external surgical approach results in skin scars, longer hospitalization and risks of facial nerve injuries [11]. The choice of treatment usually depends on the experience & expertise of the surgeon.
Anatomy and Embryology [2]
The styloid process is usually a slender, elongated, cylindrical bony projection of the temporal bone, located between the internal and external carotid arteries and the internal jugular vein and anteromedial to the stylomastoid foramen [12]. Although typically straight, it is occasionally curved [13]. Three muscles (the styloglossus, stylopharyngeus and stylohyoid) are attached to the styloid process extending to the tongue, pharynx and hyoid bone, respectively [14] (Fig. 3).
Fig. 3.
Deep dissection of the right side of a female cadaver. st.m. sternocleidomastoid muscle, a.n accessory nerve, st.g. styloglossus muscle, st.p. styloid process, st.ph. stylopharyngeus muscle, f.a. facial artery, int.j.v. internal jugular vein, subm.gl submandibular gland, m mandible, m.m masseter muscle
The styloglossus and the stylohyoid muscles are innervated by the hypoglossal and facial nerves, respectively. The stylopharyngeus muscle is innervated by the glossopharyngeal nerve [15]. Two ligaments attach to the styloid process: the stylohyoid and stylomandibular ligaments. The stylohyoid ligament is attached to the tip of the styloid process and extends to the lesser cornu of the hyoid bone [16–18] (Fig. 4).
Fig. 4.

Special preparation of the human hyoid apparatus. The mandible was removed
Stylohyoid and stylomandibular ligaments help regulate the movements of the mandible, the hyoid bone, the tongue and the pharynx [19].
Many important anatomic structures are closely located to the styloid process and the stylohyoid ligament. Lateral to the styloid process one finds the facial and hypoglossal nerves, the occipital artery and the posterior belly of the digastric muscle. The facial nerve emerges from the stylomastoid foramen posteriorly and passes laterally through the parotid gland (Fig. 5). Medial to the styloid process (from posterior to anterior) the internal jugular vein (with the accessory, hypoglossal, vagus and glossopharyngeal nerves) and the internal carotid artery are seen (Fig. 6). The superior constrictor muscle and the pharyngobasilar fascia are situated medially to the tip of the styloid process and adjacent to the tonsillar fossa [20].
Fig. 5.

Deep parotid space anatomy. The facial nerve passes laterally through the parotid gland
Fig. 6.

Styloid process anatomy. From posterior to anterior are located the internal jugular vein (with the accessory, hypoglossal, vagus and glossopharyngeal nerves) and the internal carotid artery
Embryologically, the styloid process, stylohyoid ligament, lesser cornu of the hyoid bone and the superior portion of the hyoid body are derived from Reichert’s cartilage, which arises from the second pharyngeal arch. Reichert’s cartilage is divided into four distinct segments [21]. The proximal tympano-hyal part appears before birth and fuses with the petrous temporal bone to form the tympanic portion and stapes. The lower part of the styloid process and the upper part of the stylohyoid ligament stem from the stylo-hyal part, which appears after birth. These do not unite with the tympanic portion until after puberty and in some skulls never unite. The ossification of the stylo-hyal part and it’s fusion with the tympano-hyal part results in a long styloid process, while failed ossification results in a shortened styloid process. The cerato-hyal part usually deteriorates with its fibrous sheath forming the stylohyoid ligament and the hypo-hyal part forming the lesser cornu of the hyoid bone. The styloid process begins to ossify at the end of pregnancy and continues to undergo calcification over the first 8 years of life. The ossification time and degree of ossification vary greatly [2].
Epidemiological Facts [2]
The incidence of Eagle’s syndrome is very controversial [22]. Eagle estimated the incidence of an elongated styloid process in the general population to be 4%, of which only 4% display symptoms [23–25]. In another clinical study, Kaufman et al. [26] reported elongated styloid processes in 28% of their patients, while Woolery et al. [28] examined the largest number of radiographs (1,771 panoramic views) and estimated the incidence to be 18.2%, 93% of which exhibited bilateral elongation. Only a relatively small number of patients (8 out of 1,771) however, exhibited symptoms related to Eagle’s syndrome, most of which were unilateral [27]. Styloid process elongation, in most cases, appears bilaterally. However, in most of the symptomatic cases, the symptoms are unilateral, even in cases with bilateral elongation. Bilateral elongation is believed to occur frequently, although bilateral symptoms are quite rare styloid process elongation also appears to be slightly more common in women [28, 29]. Elongated styloid processes occur more frequently in older patients and result in the deposition of calcium salts into the ligaments and processes [30].
Direction and angulation of the elongated process may be responsible for the irritation of a number of anatomical structures traversing the parapharyngeal space [31]. Lateral deviation may cause its tip to impinge upon the external carotid artery, at its bifurcation into the maxillary and superficial temporal arteries. Posterior deviation may trap the last four cranial nerves, internal carotid artery and the internal jugular vein between the elongated styloid and the transverse process of the atlas. Medial deviation may impinge the tonsillar fossa [32]. Anterior angulation may result in mucosal irritation and pressure over vital structures in the tonsillar fossa [33] (Fig. 7).
Fig. 7.

Posterior view of the elongated process bilaterally (4 cm)
Discussion
Eagle’s syndrome is an aggregate of symptoms that includes recurrent throat pain, foreign body sensation, dysphagia and/or facial pain as a direct result of an elongated styloid process or calcified stylohyoid ligament [34]. Main symptoms of the syndrome include nonspecific neck pain, foreign body sensation in the pharynx, odynophagia, otalgia, pain in the temporomandibular joint and trismus [3], change in voice, and sensation of hypersalivation [47]. Painful palpation of the tonsillar fossa, together with suggestive clinical and radiological signs, corroborates the diagnosis of Eagle’s syndrome. In addition, pain relief achieved through infiltration of local anesthetics into the tonsillar fossa is suggestive of the disease [4, 35].
Steinmann [11] proposed four theories for the causation of variance in ossification and elongation of the styloid process:
The first theory is the theory of reactive hyperplasia which suggests that the styloid process reacts and proliferates causing elongation following pharyngeal trauma.
The second theory is the theory of reactive metaplasia which suggests that the stylohyoid ligament undergoes metaplasia and partial ossification which in turn results in abnormal ossification.
The theory of anatomic variance is the third theory which proposes that the ossification of the styloid process, and the stylohyoid ligament is a normal occurrence depicting an anatomical variation.
The fourth theory suggests that retained embryologic tissue from Reichert's cartilage is the causative factor for elongation [36].
Though all the four theories give feasible explanations for the styloid process elongation, a universal agreement has not been instituted [33, 38]. Styloid elongation, as described by Correll, is classified into 3 types [11]:
Type I—represents uninterrupted elongated styloid process,
Type II—represents a styloid process joined to the stylohyoid ligament by a single pseudo-articulation.
Type III—comprises of interrupted segments of the mineralized ligament, which has an appearance of multiple pseudo-articulations within the ligament.
Additionally Langlai [11] described 4 types of calcifications:
Type 1 is calcified outline.
Type 2 is partially calcified.
Type 3 is nodular complex.
Type 4 is complete calcification.
Radiological examination [39] can confirm the syndrome. Radiography can show the increased length of the styloid process. In addition, imaging should be ordered before surgery. Plain skull x-rays are sufficient to find elongated processes. Panorex view will allow better visualization of the styloid process, but posterior-anterior skull films will show any medial or lateral deviation of the tips. CT films of the skull may also be ordered, and they have been described as an adjunct to plain films [44]. If a carotid impingement is suspected, angiography of the neck may be useful to fully visualize the anatomic relationships [45]. Currently, computed tomography is considered to be the best examination for defining the length and angulation of the styloid process and also enables an evaluation of the anatomical relationships between the stylohyoid complex and adjacent structures [40–42]. According to some authors, panoramic or lateral radiographs are sufficient for diagnosing the disease [43].
At present, Eagle’s syndrome can be treated either pharmacologically or surgically. Conservative management includes Nonsteroidal Anti-Inflammatory Drugs (NSAIDS), drugs used to treat neuralgic pain like Gabapentin and tianeptine. In addition, 1 ml of triamcinolone 10 mg combined with 0.3% mepivacaine 3 mg injected once in the tosillar fossa can also be tried [46]. All of the above treatment provides temporary relief; hence, surgical management involving resection of elongated styloid process by intraoral or extraoral approach is the treatment of choice for Eagle’s syndrome. Surgical resection of styloid process is the most acceptable treatment option for Eagle’s syndrome. The surgical approaches include an external (transcervical) and an internal (intraoral). Severity of symptoms, degree of elongation and location of styloid process are considered as important factor in establishing the most suitable technique.
The advantages of intraoral approach observed are:
- The procedure can be done under local anesthesia, there is no blind dissection as dissection is limited to the tip of the process, inadvertent exposure of the fossa is limited, minimal bleeding, due to the elasticity of the tonsillar bed, healing is faster, the chances of neck space infection is low, shorter operative time and postoperative complication and pain is reduced, faster recovery (Figs. 8, 9, 10).An extraoral surgical approach:
Reduces the damage caused to the surrounding tissues and nerves that could occur during the intraoral route due to less anatomic exposure. Persistence of symptoms after adequate surgical excision is seen in 20% of cases, which is explained as glossopharyngeal nerve being entrapped in the fibrous tissue or the cut end of inadequately shortened styloid process irritating the overlying bed of the tonsillar fossa [11, 33].
Fig. 8.

X-ray Townes view
Fig. 9.

Elongated styloid process in tonsillar fossa
Fig. 10.

Styloid processes and tonsillar tissue after resection
Although both procedures are effective in removing an elongated styloid process, but both can have few complications. Intraoperative facial nerve monitoring during any approaches to the parapharyngeal space to guard against inadvertent excessive retraction of the facial nerve should be done [45]. No matter which approach is adopted excision of styloid processs from its complex anatomical location, in a precise & minimally invasive way is a challenging task.
Conclusion
Patients with Eagle’s syndrome generally have a history of chronic pain treated by several physicians. Appropriate knowledge of this disease is necessary for adequate treatment to be provided. The importance of diagnosing this uncommon and often unsuspected disease should be emphasized, given that correct clinical-surgical treatment is frequently delayed. The diagnosis of Eagle’s syndrome is clinical and radiographic, and the definitive treatment in cases of difficult-to-control pain is surgical.
Declarations
Conflict of interest
The authors have none conflicts to declare.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Saumya Taneja, Email: drsaumyataneja@gmail.com.
Shishir Dhar, Email: balboashishir@gmail.com.
References
- 1.Malik JN, et al. Stylalgia revisited: clinical profile and management. Iran J Otorhinolaryngol. 2018;30(6):101. [PMC free article] [PubMed] [Google Scholar]
- 2.Maria P, Sophia A, Konstantinos K, Giannoulis P. Eagle’s syndrome: a review of the literature. Clin Anat. 2009;22:545–558. doi: 10.1002/ca.20804. [DOI] [PubMed] [Google Scholar]
- 3.Eagle WW. Elongated styloid process: report of two cases. Arch Otolaryngol. 1937;25:584–587. doi: 10.1001/archotol.1937.00650010656008. [DOI] [PubMed] [Google Scholar]
- 4.Eagle WW. Elongated styloid process: further observations and a new syndrome. Arch Otolaryngol. 1948;47:630–640. doi: 10.1001/archotol.1948.00690030654006. [DOI] [PubMed] [Google Scholar]
- 5.Strauss M, Zohar Y, Laurian N. Elongated styloid process syndrome: a review. Laryngoscope. 1985;95(8):976–979. doi: 10.1288/00005537-198508000-00018. [DOI] [PubMed] [Google Scholar]
- 6.Eagle WW. Elongated styloid process; symptoms and treatment. AMA Arch Otolaryngol. 1958;67(2):172–176. doi: 10.1001/archotol.1958.00730010178007. [DOI] [PubMed] [Google Scholar]
- 7.Md. Arif HB, et al (2012) Tonsillo—styloidectomy for Eagle’s syndrome: review of 20 cases. Bangladesh J Otorhinolaryngol 18(2): 149-155
- 8.Rechtweg JS, Wax MK. Eagle’s syndrome: a review. Am J Otolaryngol. 1998;19:316–321. doi: 10.1016/S0196-0709(98)90005-9. [DOI] [PubMed] [Google Scholar]
- 9.Sudhir MN, Sarika SN (2020) Transoral transtonsillar styloidectomy: a minimally invasive technique for stylohyoid syndrome. Int J Head Neck Surg 11(2).
- 10.Naik SM, Naik SS. Tonsillo-styloidectomy for eagle’s syndrome: a review of 15 cases in KVG medical college sullia. Oman Med J. 2011;26(2):122–126. doi: 10.5001/omj.2011.30. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Maradesha PS, et al. Styloidectomy: our experience with intraoral approach. Int J Otorhinolaryngol Head Neck Surg. 2020;6(11):2106–2109. doi: 10.18203/issn.2454-5929.ijohns20204639. [DOI] [Google Scholar]
- 12.Perez Carro L, Nunez MP. Fracture of the styloid process of the temporal bone. A case report. Int Orthop. 1995;19:359–360. doi: 10.1007/BF00178349. [DOI] [PubMed] [Google Scholar]
- 13.Das S, Suhaimi FH, Othman F, Latiff AA. Anomalous styloid process and its clinical implications. Bratisl Lek Listy. 2008;109:31–33. [PubMed] [Google Scholar]
- 14.Camarda AJ, Deschamps C, Forest DI. Stylohyoid chain ossification: a discussion of etiology. Oral Surg Oral Med Oral Pathol. 1989;67:508–514. doi: 10.1016/0030-4220(89)90264-8. [DOI] [PubMed] [Google Scholar]
- 15.Palesy P, Murray GM, De Boever J, Klineberg I. The involvement of the styloid process in head and neck pain—a preliminary study. J Oral Rehabil. 2000;27:275–287. doi: 10.1046/j.1365-2842.2000.00515.x. [DOI] [PubMed] [Google Scholar]
- 16.Hollinshead WH. Textbook of anatomy. 2. New York: Harper and Row; 1969. pp. 772–839. [Google Scholar]
- 17.Gosh LM, Dubey SP. The syndrome of elongated styloid process. Auris Nasus Larynx. 1999;26:169–175. doi: 10.1016/s0385-8146(98)00079-0. [DOI] [PubMed] [Google Scholar]
- 18.Balbuena L, Jr, Hayes D, Ramirez SG, Johnson R. Eagle’s syndrome (elongated styloid process) South Med J. 1997;90:331–334. doi: 10.1097/00007611-199703000-00014. [DOI] [PubMed] [Google Scholar]
- 19.Beder E, Ozgursoy OB, Ozgursoy SK. Current diagnosis and transoral surgical treatment of Eagle’s syndrome. J Oral Maxillofac Surg. 2005;63:1742–1745. doi: 10.1016/j.joms.2005.08.017. [DOI] [PubMed] [Google Scholar]
- 20.Yavuz H, Caylakli F, Yildirim T, Ozluoglu LN. Angulation of the styloid process in Eagle’s syndrome. Eur Arch Otorhinolaryngol. 2008;265:1393–1396. doi: 10.1007/s00405-008-0686-9. [DOI] [PubMed] [Google Scholar]
- 21.Badhey A, Jategaonkar A, Anglin KAJ, Kadakia S, De Deyn PP, Ducic Y, et al. Eagle syndrome: a comprehensive review. Clin Neurol Neurosurg. 2017;159:34–38. doi: 10.1016/j.clineuro.2017.04.021. [DOI] [PubMed] [Google Scholar]
- 22.Rogers K, Chang H. Eagle’s syndrome: a case report. Columbia Dent Rev. 2007;11:12–14. [Google Scholar]
- 23.Fritz M. Elongated styloid process: cause of obscure throat symptoms. Arch Otolaryngol. 1940;31:911–918. doi: 10.1001/archotol.1940.00660010926002. [DOI] [Google Scholar]
- 24.Eagle WW. Symptomatic elongated styloid process: report of two cases of styloid process-carotid artery syndrome with operation. Arch Otolaryngol. 1949;49:490–503. doi: 10.1001/archotol.1949.03760110046003. [DOI] [PubMed] [Google Scholar]
- 25.Eagle WW. The symptoms, diagnosis and treatment of the elongated styloid process. Am Surg. 1962;28:1–5. [PubMed] [Google Scholar]
- 26.Kaufman SM, Elzay RP, Irish EF. Styloid process variation. Radiologic and clinical study. Arch Otolaryngol. 1970;91:460–463. doi: 10.1001/archotol.1970.00770040654013. [DOI] [PubMed] [Google Scholar]
- 27.Correll RW, Jensen JL, Taylor JB, Rhyne RR. Mineralization of the stylohyoid-stylomandibular ligament complex: a radiographic incidence study. Oral Surg Oral Med Oral Pathol. 1979;48:286–291. doi: 10.1016/0030-4220(79)90025-2. [DOI] [PubMed] [Google Scholar]
- 28.Woolery WA. The diagnostic challenge of styloid elongation (Eagle’s syndrome) J Am Osteopath Assoc. 1990;90:88–89. doi: 10.1515/jom-1990-900114. [DOI] [PubMed] [Google Scholar]
- 29.Liu SH, Wang Y, Zhang RH, Liu SY, Peng HH. Diagnosis and treatment of 23 cases with stylohyoid syndrome. Shanghai Kou Qiang Yi Xue. 2005;14:223–226. [PubMed] [Google Scholar]
- 30.Unlu Z, et al. Elongated styloid process and cervical spondylosis. Clin Med Case Rep. 2008;I:57–64. doi: 10.4137/ccrep.s792. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Walli AK, Thorawade VP, Parelkar K, Nagle S, Kulsange KL. Intraoral styloidectomy in Eagle’s syndrome-a risky and infrequently performed approach. J Clin Diagn Res. 2018;12(1):MD01–2. [Google Scholar]
- 32.Ghosh LM, Dubey SP. The syndrome of elongated styloid process. Auris Nasus Larynx. 1999;26:169–175. doi: 10.1016/S0385-8146(98)00079-0. [DOI] [PubMed] [Google Scholar]
- 33.Yavuz H, Caylakli F, Yildirim T, Ozluoglu LN. Angulation of the styloid process in Eagle’s syndrome. Eur Arch Otorhinolaryngol. 2008;265:1393–1396. doi: 10.1007/s00405-008-0686-9. [DOI] [PubMed] [Google Scholar]
- 34.Kapoor V, Jindal G, Garg S. Eagle’s syndrome: a new surgical technique for styloidectomy. J Maxillofac Oral Surg. 2015;14(Suppl 1):S360–S365. doi: 10.1007/s12663-013-0597-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Murtagh RD, Caracciolo JT, Fernandez G. CT findings associated with Eagle syndrome. AJNR Am J Neuroradiol. 2001;22(7):1401–1402. [PMC free article] [PubMed] [Google Scholar]
- 36.Badhey A, et al. Eagle syndrome: a comprehensive review. Clin Neurol Neurosurg. 2017;159:34–38. doi: 10.1016/j.clineuro.2017.04.021. [DOI] [PubMed] [Google Scholar]
- 37.Feldman VB. Eagle's syndrome: a case of symptomatic calcification of the stylohyoid ligaments. J Can Chiropr Assoc. 2003;47(1):21–27. [Google Scholar]
- 38.Steinmann EP. A new light on the pathogenesis of the styloid syndrome. Arch Otolaryngol. 1970;91(2):171–174. doi: 10.1001/archotol.1970.00770040241013. [DOI] [PubMed] [Google Scholar]
- 39.Gonçalves T, et al. Eagle’s syndrome. Int Arch Otorhinolaryngol. 2013;17(3):347–350. doi: 10.7162/S1809-977720130003000017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Fini G, et al. The long styloid process syndrome or Eagle’s syndrome. J Craniomaxillofac Surg. 2000;28:123–127. doi: 10.1054/jcms.2000.0128. [DOI] [PubMed] [Google Scholar]
- 41.Beder E, Ozgursoy OB, Ozgursoy SK, Anadolu Y. Three dimensional computed tomography and surgical treatment for Eagle’s syndrome. Ear Nose Throat J. 2006;85(7):443–445. doi: 10.1177/014556130608500715. [DOI] [PubMed] [Google Scholar]
- 42.Mendelsohn AH, Berke GS, Chhetri DK. Heterogeneity in the clinical presentation of Eagle’s syndrome. Otolaryngol Head Neck Surg. 2006;134:389–393. doi: 10.1016/j.otohns.2005.10.046. [DOI] [PubMed] [Google Scholar]
- 43.Prasad KC, Kamath MP, Reddy JM, Raju K, Agarwal S. Elongated styloid process (Eagle’s syndrome): a clinical study. J Oral Maxillofac Surg. 2002;60(2):171–175. doi: 10.1053/joms.2002.29814. [DOI] [PubMed] [Google Scholar]
- 44.Murtagh RD, Caracciolo JT, Fernandez G. CT findings associated with Eagle syndrome. AJNR Am J Neuroradiol. 2001;22(7):1401–2. [PMC free article] [PubMed] [Google Scholar]
- 45.Mendelsohn AH, Berke GS, Chhetri DK. Heterogeneity in the clinical presentation of Eagle’s syndrome. Otolaryngol Head Neck Surg. 2006;134:389–393. doi: 10.1016/j.otohns.2005.10.046. [DOI] [PubMed] [Google Scholar]
- 46.Wong ML, Rossi MD, Groff W, Castro S, Powell J. Physical therapy management of a patient with Eagle syndrome. Physiother Theory Pract. 2011;27(4):319–327. doi: 10.3109/09593985.2010.498036. [DOI] [PubMed] [Google Scholar]
- 47.Olszewski J, Miłoński J, Jałocha-Kaczka A. A rare case of late diagnosis of elongated styloid process syndrome. J Hear Sci. 2019;9(4):33–36. doi: 10.17430/1003481. [DOI] [Google Scholar]