Abstract
Decades of research has recognized a solid role for Pim kinases in lymphoproliferative disorders. Often up-regulated following JAK/STAT and tyrosine kinase receptor signaling, Pim kinases regulate cell proliferation, survival, metabolism, cellular trafficking and signaling. Targeting Pim kinases represents an interesting approach since knock-down of Pim kinases leads to non-fatal phenotypes in vivo suggesting clinical inhibition of Pim may have less side effects. In addition, the ATP binding site offers unique characteristics that can be used for the development of small inhibitors targeting one or all Pim isoforms. This review takes a closer look at Pim kinase expression and involvement in hematopoietic cancers. Current and past clinical trials and in vitro characterization of Pim kinase inhibitors are examined and future directions are discussed. Current studies suggest that Pim kinase inhibition may be most valuable when accompanied by multi-drug targeting therapy.
Keywords: Pim1, Pim2, Pim3, Leukemia, Lymphoma, PIM, JAK, STAT, B-cell, T-cell
Introduction
Pim kinases (Provirus Integration site for Moloney leukemia virus) are a family of serine/threonine protein kinases with roles in cellular development, immunoregulation, and oncogenesis. Early studies of the original Pim kinase, Pim-1, led to the discovery of an oncogenic role for the Pim kinase family in lymphoma [1, 2]. Even though Pim-2 only shared 55% amino acid homology with Pim-1, it was considered a compensatory protein to Pim-1, as it shared a very similar kinase domain [3]. A third member of the family, Pim-3, was found to catalyze histone phosphorylation and autophosphorylation [4]. All three Pim proteins can phosphorylate serine and threonine amino acids [5]; and can activate similar cellular pathways. This has led researchers to believe that individual Pim kinases are compensatory, whereby the loss of one Pim kinase can be alleviated by the expression of another Pim kinase. There are several counterpoints to this theory, since individual Pim kinases have different expression patterns in cancer(s), distinct tissue locations, dissimilar regulation, and are encoded on different chromosomes [6]. Furthermore, Pim-1 and -2 have alternative isoforms that likely have unique functions. This suggests that while similar, individual Pim kinases may have distinct roles, which favor cellular distribution or various tumor microenvironments. This would explain why Pim-3 is highly over-expressed in some solid cancers, such as prostate and breast cancer, while Pim-1 and Pim-2 are generally over-expressed in hematopoietic cancers. The study of genetically modified mice deleted for Pim-1,-2, and-3 demonstrate that Pim kinases are not embryonically lethal, but exhibit reduced body sizes at birth and throughout life [7]; while mice that are knocked out for all three Pim kinases lack proper hematopoietic cell development and regulation [8]. Despite their expression in tumorigenic cells, Pim kinases are considered “weak” oncogenes since over-expression studies produce tumors at low frequency and after a long latency period. Pim kinases may have larger roles in tumor progression, rather than development; and have been proposed as broad drivers of chemotherapy resistance [9]. While an independent role in cancer initiation is weak, Pim kinases show especially strong synergistic roles in the presence of other oncogenes, such as c-Myc/n-Myc (C/N-MYC Proto-Oncogene), and Bcl-2 (BCL2 Apoptosis Regulator) and in the presence of various carcinogens to initiate cancer [10].
The over-expression of Pim kinases is largely specific to hematologic cancers compared to solid tumors, though exceptions do exist, particularly regarding Pim-3. Generally, Pim kinases are expressed at higher levels in hematopoietic cells compared to other tissue. Expression data obtained during normal human hematopoiesis shows Pim-1 and Pim-2 have similar distribution patterns, with stronger expression in CD4 and CD8 cells (Fig. 1A) (https://servers.binf.ku.dk/bloodspot/) [11, 12]. Indeed, Pim-1 protein is expressed during normal embryonic development in hematopoietic tissue especially the liver, spleen, and bone marrow, but is shut off in most adult tissues [13, 14]. Pim-3 differs significantly, whereby expression is higher in granulocyte monocyte progenitors (Fig. 1A). Data obtained from the Human Protein Atlas (http://www.proteinatlas.org) and publications, also confirms low, non-specific gene expression of Pim-3 in various adult tissue [15]. This contrasts with Pim-1 and Pim-2 with higher expression in cells of the bone marrow/lymphoid and in blood cells (Fig. 1B). In conjunction with their cellar distribution, Pim-1 transgenic mice are susceptible to lymphomas; and Pim kinases have roles in the differentiation, activation, and/or response of immune cells [16, 17]. Given the role of Pim kinases in tumorigenesis and their over-representation in immune cells, it should come as no surprise that Pim kinases often display robust expression in hematopoietic cancers.
Fig. 1.
Pim kinase expression during normal hematopoiesis. A Hierarchical differentiation trees for the expression of Pim-1, − 2, and − 3 during normal hematopoietic stem cell differentiation from the bone marrow (HSC-BM). Pim kinase expression levels are indicated by the legend, whereby the size and color of the nodes indicates general expression patterns. Data are derived from Normal human hematopoiesis (HemaExplorer) obtained from the BloodSpot Data base (https://servers.binf.ku.dk/bloodspot/) [11]. Definitions are as follows: CMP (Common myeloid progenitor cell), GMP (Granulocyte monocyte progenitors), MEP (Megakaryocyte-erythroid progenitor cell), NK cells (CD56+ natural killer cells), PM_BM (Promyelocyte from bone marrow), MY_BM (Myelocyte from bone marrow), PMN_BM (Polymorphonuclear cells from bone marrow), and PMN_PB (Polymorphonuclear cells from peripheral blood). B Pim-1, − 2, and − 3 expression patterns in blood samples. Graphs represent the normalized transcript expression values, denoted by average TPM (transcript per million). Data are derived from HPA (Human protein atlas) RNA-seq from the Human Protein Atlas database (https://www.proteinatlas.org/)
The role of Pim kinases in cancer
Pim kinases phosphorylate proteins involved in pro-survival and key T- and B-cell signaling pathways, which contribute to Pim kinase transforming properties in leukemias and lymphomas. In vivo evidence by way of gene insertion, knock-out, and transgenic mouse studies largely established Pim kinase involvement in initiating tumorigenesis independently of other oncogenes or tumor suppressor inactivation. Insertion of the Moloney-murine leukemia virus (M-MuLV), into either Pim gene locus leads to enhanced protein expression of Pim-1/− 2 that can lead to T- and B-cell lymphomas [1, 3, 18]. The use of Pim-1 and Pim-2 expressing lymphoid cells in transgenic mice also causes a low frequency of lymphomas after long latency periods; whereas Pim-3 expressing liver cells of transgenic mice produce carcinomas but only in the presence of carcinogens [18]. Pim-1 transgenic mice are also more susceptible to accumulating mutation(s) in response to genotoxic agents’ exposure, as evidenced by an increase in tumor development in Pim-1 transgenic mice exposed to carcinogens or ionizing radiation [19, 20]. These in vivo models demonstrated that Pim kinases are oncogenic; however, studies have also shown that when expressed cooperatively with other oncogenes, tumorigenesis is significantly enhanced. In particular, the Myc pathway (including c-Myc, N-Myc, and L-Myc) is strongly associated with Pim kinase-mediated transformation; and the two pathways act synergistically in tumorigenesis. Myc is often overexpressed at the gene/protein level or by translocation or rearrangement in a broad group of leukemias and lymphomas [21]. The cooperation between Pim and myc in the generation of leukemia/lymphoma is well documented: Pim-1/myc transgenic mice develop pre-B-cell leukemia at high frequency [16], c-Myc/N-Myc enhances Pim-1 development of T-cell lymphoma in utero [22], and Pim-2/c-Myc mice develop pre-B-cell, B-cell, and T-cell lymphomas [23]. A role for Myc in cooperating with Pim-3 in the develop of B- or T-cell lymphomas/leukemias has only been shown indirectly [24]. However, in Myc transgenic mice harboring Pim-1/− 2 deletion, Pim-3 was activated in tumor cells [25]. Several loci that enhance Myc/Pim kinase tumor development have already been identified, including Pal-1/Gfi-1 (Growth Factor Independent 1 Transcriptional Repressor), Bmi-1 (B Lymphoma Mo-MLV Insertion Region 1 Homolog), and Runx2 (RUNX Family Transcription Factor 2) [18, 26, 27].
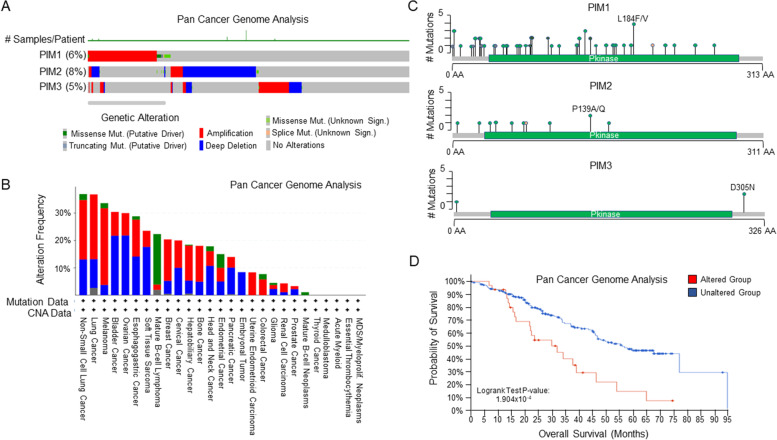
Pim kinases are constitutively active. They are largely overexpressed in cancer cells due to transcriptional activation and stabilization through positive feedback loops with upstream regulators, such as the JAK/STAT (Janus kinase/signal transducer and activator of transcription), PI3K/AKT (PI3-kinase/AKT serine/threonine kinase 1), and NF-κB (NF-Kappa-B transcription factor) signaling pathways. An examination of Pim kinase genomic alterations in cancer is largely lacking, even though mutations and gene modifications are prevalent. A Pan-cancer genomic analysis of Pim kinase mutations found numerous gene amplifications, deletions, missense mutations, and splice mutations in all 3 Pim kinases (Fig. 2A) [28–30]. Of note, this database did not include an analysis of non-solid tumor tissue; largely excluding leukemias and most lymphomas. Genetic alterations were found in 6, 8, and 5% of Pim1, Pim2, and Pim3, respectively, in the cancers examined. The most common alterations in the 3 kinases were gene amplifications and deep deletions (Fig. 2B). In contrast to other malignancies, mature B-cell lymphomas displayed a high rate (18.5%) of mutations, especially in Pim1 (Fig. 2C). The most common mutations were Pim1 missense mutations at L2F, L184F/N, and E135K. Data is still lacking on the biological significance of these mutations as it relates to Pim kinase activity and oncogenicity. However, due to their location in recurrent hotspots, most Pim1 mutations are hypothesized to be oncogenic. Examination of survival data suggests, but does not confirm, that alterations of the Pim genes decreases overall patient survival (Fig. 2D). These results will need to be confirmed in controlled, matched, and cancer specific patient samples.
Fig. 2.
Pan Cancer Analysis of Genetic Alterations in Pim kinases. A-D Results derived from the PanCancer Analysis of whole genomes (https://www.cbioportal.org/) for Pim-1, − 2, and − 3. Data encompasses whole genome sequencing from 2583 whole cancer genomes and matched normal tissue across 38 tumor types [28, 29]. A Oncoprint of genetic alterations in Pim kinases. Missense mutations (both putative drivers and unknown significance), splice and truncating mutations, amplification and deep deletions are shown. B The frequency of cancers harboring mutations, amplifications, and deep deletions in the Pim kinases are shown. C Mutations in Pim-1, − 2, and − 3 are demonstrated. Most mutations in Pim-1 are derived from samples with follicular lymphoma, nodal marginal zone lymphoma, and DLBCL. The position of the mutations in the Pim gene and the frequency of the mutation are shown. The most common mutation in each of the Pim genes is noted (Pim1: L184F/N, Pim2: P139A/Q), and Pim3: D305N). D Patient overall survival in individuals harboring Pim genetic alterations. Data represent 36 patients with alterations in Pim genes and 245 patients with unaltered Pim genes
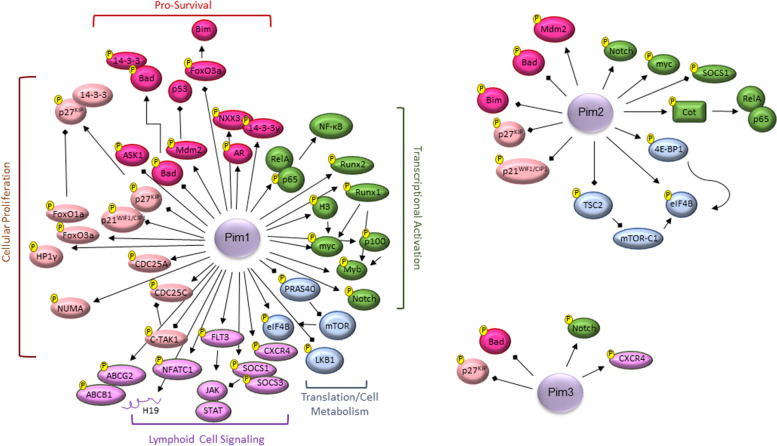
The pro-tumorigenic phenotype of Pim kinases is due to their phosphorylating specific serine/threonine motifs and increasing the activity of target proteins. These substrates have key roles in cell proliferation, cell survival, cap-dependent translation, metastasis, and tumorigenesis. The ability of Pim kinases to phosphorylate proteins involved in transmembrane drug efflux pumps, such as the ABC transporters (ATP-binding cassette transporters), increases their expression levels and leads to multi-drug resistance [31–33]. The multilateral effects of Pim kinases on translational components allow for increased microRNA (miRNA) function and polysome occupancy, allowing for miRNA targeting despite an enhanced need for protein synthesis in activated or transformed immune cells [34]. This effect was greater for JAK/STAT/Pim signaling than for the parallel, PI3K/AKT/mTOR (mammalian target of rapamycin) signaling pathway. Their role in regulating translation causes Pim kinases to directly affect the metabolic function of cells. Triple knock-out mice for all three Pim kinases demonstrate reduced growth, protein synthesis, and 5′-cap dependent translation [35]. While a detailed analysis of every target is beyond the scope of this review, a brief description of currently known targets is listed below (Table 1), not only to demonstrate the vast array of Pim kinase targets, but notably, to highlight the oncogenic and central role of Pim kinases in cancer (Fig. 3). While it may appear that Pim-3 does not have as large of a role in initiating and maintaining transformation of cells, this may be due to the lack of studies on Pim-3 phosphorylation targets, compared to the other Pim kinases.
Table 1.
Pim Kinase phosphorylation substrates
| Direct Phosphorylation Targets | Effect on Oncogenesis | Pim(s) | |
|---|---|---|---|
| Transcriptional Activation | p65/RelA [36] | NF-κB signaling pathway | Pim1 |
| Cot (MAP3K8/Mitogen-Activated Protein Kinase Kinase Kinase 8) [37] | NF-κB signaling pathway | Pim2 | |
| c-MyC (myc Proto-Oncogene Protein) [38] | c-Myc and NF-κB Signaling pathways | Pim-1 and 2 | |
| H3 (Histone H3) [39] | Enhance c-Myc transcriptional Activity | Pim-1 | |
| C-MyB and A-Myb (Myb Proto-Oncogene) [40] | Enhance transcriptional activities; Feedback: c-Myb can regulate c-Myc [41] | Pim-1 | |
| p100 (Nuclear Factor Kappa B Subunit 2) [42] | Up-regulates c-Myb; NF-κB signaling pathway | Pim-1 | |
| Runx1 and Runx2 (Acute Myeloid Leukemia Gene 1 and 2) [43] | (CBF) family of transcription factors; Required for Myc and Myb activity in leukemia [44] | Pim-1 | |
| Notch1 and Notch3 (Notch receptor 1 and 3) [45] | Transcriptional Activators (cleaved); activate c-Myc | Pim-1, −2, −3 | |
| Proliferation and Cell Cycle | p21CIP1/WAF1 (CDKN1A/cyclin Dependent Kinase Inhibitor 1A) [46, 47] | Cell Cycle Progression | Pim-1 and 2 |
| p27KIP1 (CDKN1B/cyclin Dependent Kinase Inhibitor 1B) [48] | Cell Cycle Progression | Pim-1, −2, −3 | |
| FoxO1a and FoxO3a (Forkhead box O1a and 3a) [49, 50] | Cell Cycle Progression | Pim-1 | |
| C-TAK1 (protein kinase Cdc25 C-associated kinase 1) [49] | Cell Cycle Regulator | Pim-1 | |
| CDC25A and CDC25C (Cell Division Cycle 25A and C) [50, 51] | Cell Cycle Progression | Pim-1 | |
| NuMA (Nuclear Mitotic Apparatus) [52] | Mitosis | Pim-1 | |
| HP1γ (heterochromatin-associated protein 1 gamma) [53] | Mitosis | Pim-1 | |
| Translation and Cell Metabolism | TSC2 (TSC Complex Subunit 2) [54] | Enhanced Protein Translation | Pim-2 |
| 4E-BP1 (Eukaryotic Translation Initiation Factor 4E Binding Protein 1) [55] | Enhanced Protein Translation; TSC2 target gene | Pim-2 | |
| PRAS40 (AKT1 Substrate 1) [56] | Increased mTOR activation of 4E-BP1 and p70S6K | Pim-1 | |
| eIF4B (Eukaryotic Translation Initiation Factor 4B) [57] | Translation Initiation | Pim-1 | |
| LKB1 (Serine/Threonine Kinase 11) [58] | Cell Metabolism and Energy Production | Pim-1 | |
| Apoptosis and Cellular Invasion | Bad (BCL2 Associated Agonist of Cell Death) [59] | Anti-apoptotic release of Bcl-XL | Pim-1, −2, −3 |
| Bim (BCL2 Like 11) [60] | Anti-apoptotic | Pim-2 | |
| ASK1 (Apoptosis signaling kinase 1) [61] | Anti-Apoptotic to stress and inflammation | Pim-1 | |
| MDM2 (MDM2 Proto-Oncogene) [62, 63] | p53 degradation and transactivation | Pim-1 and 2 | |
| AR (androgen receptor) [64] | Pro-migration and invasion [64, 65] | Pim-1 | |
| 14–3-3ζ [65] | AR co-activator | Pim-1 | |
| NKX3.1 (NK3 Homeobox 1) [66] | 14–3-3ζ functional partner | Pim-1 | |
| Lymphoid Signaling | NFATC1 (Nuclear Factor of Activated T Cells 1) [67] | T-cell signaling, bone formation, immunotherapy | Pim-1, −2, −3 |
| SOCS-1/3 (Suppressor of Cytokine Signaling 1/3) [68, 69] | T-cell Regulation; JAK/STAT Signaling | Pim-1 | |
| FLT3 (Fms Related Receptor Tyrosine Kinase 3) [70] | STAT5a/b regulation and cytokine-sensitive signaling pathways | Pim-1 | |
| CXCR4 (C-X-C Motif Chemokine Receptor 4) receptor [71, 72] | Cell trafficking through ligands, such as CXCL12 (C-X-C Motif Chemokine Ligand 12) | Pim-1 and − 3 | |
| H19 [73] | lncRNA involved in stem cell signature | Pim-1 | |
| ABCB1 and ABCG2 (BCRP) ATP Binding Cassette Subfamily G Member [31, 33] | Drug efflux; involved in drug resistance | Pim-1 |
Fig. 3.
Current Pim-1, − 2, and − 3 Phosphorylated Cellular Targets. Cellular Pim kinase substrates are grouped based on their effect on transcriptional activation (green), translation/cellular metabolism (blue), survival (dark pink), proliferation (light pink), and lymphoid signaling (purple)
As of 2020, the World Health Organization (WHO) reports the crude rate per 100,000 people worldwide of lymphoid cancers was 7.0, 6.1, 2.3, and 1.1 for non-Hodgkin’s lymphoma (NHL), leukemia, multiple myeloma (MM), and Hodgkin’s lymphoma (cHL), respectively. Novel therapeutics are needed to combat the rising incidence of lymphoid cancers. Gene expression profiling of hematological cancers, acute myeloid leukemia (AML), chronic myeloid leukemia (CML), acute lymphoblastic leukemia (ALL), chronic lymphocytic leukemia (CLL), and myelodysplastic syndromes (MDS), and their various subclasses, demonstrated high expression of Pim kinases across hematologic malignancies (Fig. 4A/B) [11, 12, 74, 75]. Pim-1 was highly expressed in complex AML, CLL, ALL, and MDS, while Pim-2 was especially prevalent in CML compared to other leukemias. Pim-3 showed higher expression in AML subclasses and c−/Pre-B-ALL. Given the strong role of Pim kinases in cancer progression, their over-expression in lymphoid cell lineage cancers, and their central role in several pro-tumorigenic pathways, Pim kinases represent an attractive therapeutic target. The following sections describe how Pim kinases are relevant in various lymphoid and myeloid cancers. These include, AML (acute myeloid leukemia), ALL (acute lymphocytic leukemia), and APL (acute promyelocytic leukemia); multiple myeloma (MM); lymphomas, that comprise non-Hodgkin’s lymphoma (NHL), Hodgkin’s lymphoma (cHL), and chronic lymphocytic leukemia (CLL); and chronic leukemias, that comprise, CLL, chronic myeloid leukemia (CML), adult T-cell leukemia (ATL), and myeloproliferative neoplasms (MPNs).
Fig. 4.
Microarray Expression of Pim kinases in AML, CML, ALL, CLL, and MDS. A-B Data are compiled from the BloodSpot Data base (https://servers.binf.ku.dk/bloodspot/) using expression data from the Microarray Innovations in Leukemia study (MILE) [11, 75]. Data are derived from four groups of leukemia: AML, CML, ALL, and CLL. The data are derived from 2095 patients, performed in various laboratories across the world. A Jitter strip chart demonstrating expression data of Pim-1, Pim-2, and Pim-3 across various subclasses of AML, CML, ALL, CLL, and MDS. B Hierarchical differentiation trees for the expression of Pim-1, − 2, and − 3 in AML, CML, ALL, CLL, and MDS. Pim kinase expression levels are indicated by the legend, whereby the size and color of the nodes indicates general expression patterns in various classes and subclasses of leukemia
Acute myeloid leukemia (AML)
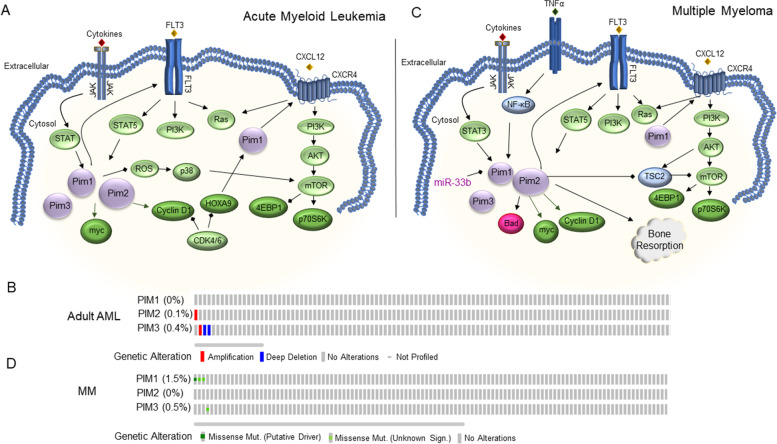
AML arises from the transformation of immature blast cells in the bone marrow through abnormal differentiation and genetic alterations, particularly in Fms-like tyrosine kinase 3 (FLT3), a driver mutation for AML. As much as 30% of AML patients have mutations in FLT3, with approximately 25% carrying constitutively activating internal tandem duplication mutations (FL3-ITD) [76]. FLT3 supports early hematopoietic and lymphoid cell proliferation. Expression of FLT3 or the presence of FLT3 mutations are linked to Pim kinases. While all three Pim kinases are over-expressed in AML patient samples, Pim-2 appears dominant (Fig. 5A). Genetic alterations in the Pim kinases, including mutations, are rare in AML patients. Whole exome sequencing verified a small percentage of adult AML patients harboring deep deletions and amplification of Pim-2 and Pim-3, but the clinical significance of this is unknown (Fig. 5B) [29, 77, 78]. Pim-1 expression regulates cellular homing and migration, an essential role that drives in vivo FLT3-ITD transformation of bone marrow cells [71]. This is in part due to Pim-1 increasing the expression and activation of CXCR4 (C-X-C Motif Chemokine Receptor 4) in AML blasts and hematopoietic cells in the bone marrow niche. CXCR4 drives mTOR signaling in AML. Even though Pim-2 is not sufficient to transform FLT3-ITD primary cells, Pim-2 has been shown to be necessary for the survival of immortalized, hematopoietic progenitor cells, that stably express FLT3-ITD [79]. In AML blasts derived from patient samples, the Pim-2 protein (and not Pim-1) was highly expressed compared to normal CD34+ cells [55]. Other studies have variable results and show high Pim-1 expression in AML patients, where Pim-1 and Pim-2 gene levels were higher in AML patient samples than those in complete remission. Furthermore, an association between high Pim-1 expression and higher risk groups and overall survival was reported [80, 81]. Pim-3 was also found to be over-expressed in the bone marrow derived samples from AML patients [82]. The difference in expression levels observed in different studies could be due to the lack of direct correlation between Pim-1 gene and protein levels, or to the fact that Pim-1 is not expressed in early, non-treated AML blasts, whereas Pim-1 is up-regulated in late stage, more aggressive cases. Indeed, microarray expression data demonstrates varying levels of Pim kinases in subclasses of AML [11, 75]. Pim-1 and Pim-3 expression were high in complex AML, whereas Pim-3 was also high in AML t(8;21) and AML inv.(16) compared to other AML subclasses (Fig. 4B). Additionally, Pim expression could correlate only with certain genetic mutations (ie. FLTD-ITD or FLTD-ITD), and therefore the percentage of AML patients in each data set harboring these mutations, which could explain varying levels of Pim kinases among studies. Indeed, wild-type FLT3 or expression of FLT3-ITD leads to increased Pim-1 expression [83]. STAT5 is downstream of FLT3 and JAK signaling, which are known to be potent inducers of Pim expression. Along with STAT5, the transcription factor, HOXA9 (homeobox A9), is up-regulated in AML and can also drive Pim-1 expression [84].
Fig. 5.
Pim Kinase Expression and Genetic Alterations in Acute Myeloid Leukemia (AML) and Multiple Myeloma (MM). A and C Model depicting Pim kinase regulation in AML (A) and MM (C). Pim kinases are depicted in purple, with relative expression depicted by the size of the node. B and D Oncoprints of genetic alterations in AML (B) and MM (D) for Pim kinases derived from the cBioPortal from Cancer Genomics [29]. For (B), the results published are from whole genome sequencing and/or whole exome sequencing generated by OHSU Beat AML Project and the TCGA AML Project [77, 78]. The Beat project encompassed 672 AML patients with 454 matched, normal samples, while the TCGA project included 200 adult de novo AML tumor/normal pairs. D Data are derived from the cBioPortal for Cancer Genomics. Data sourced to whole exosome sequencing of 203 paired MM and normal patient samples [85]
Acute promyelocytic leukemia (APL) is a type of AML characterized by an accumulation of immature granulocytes, promyelocytes, that harbor genetic translocations in the retinoic acid receptor alpha gene (RARα) that generates the PML/RARα gene, PRα. Mutated FLT3-ITD, along with PRα, is important in the pathogenesis and leukemogenesis of APL [86]. Pim-2 was found to cooperate with PRα to induce APL in mice, possibly by enhancing the likelihood of clonal events that lead to leukemia [87]. Accordingly, APL patient samples have high expression of Pim-2. Preclinical trials with Pim inhibitors have shown promising results. Treatment of newly diagnosed AML patients with K00135, an ATP-competitor of Pim kinases, leads to decreased cell viability in AML cells independent of FLT3-ITD, while the viability of normal, human cord blood cells was unchanged [88]. Treatment of the same patients with K00486, led to loss of Pim-1 regulated surface expression of CXCR4 without loss of cell viability [71]. AZD1208 and SGI-1776 also inhibit AML primary cells, xenograft AML tumors in animal models, and cell growth by down-regulating global RNA and protein synthesis [89–91]. These drugs inhibit Pim-mediated regulation of transcription and translation through c-Myc, 4E-BP1 (Eukaryotic Translation Initiation Factor 4E Binding Protein 1), and p70S6K (Ribosomal protein S6 kinase beta-1).
Acute lymphoblastic leukemia (ALL)
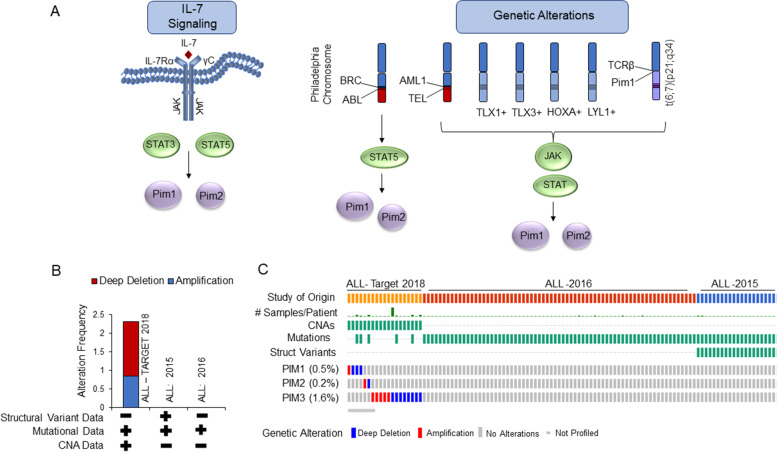
The most common type of ALL is precursor B-lymphoblastic leukemia (B-ALL) which accounts for 88% of childhood ALL, and 75% of adult ALL. A database analysis demonstrated high expression of Pim kinases in different subgroups of ALL patients, where Pim-1 expression was the highest in ALL patient samples (n = 350) when compared to AML, MM, and DLBCL samples [92]. Pim-3 is also elevated in ALL compared to other leukemias. Bone marrow mononuclear cells from B-ALL patients over-express Pim-1 and Pim2, whereas Pim-3 expression was unchanged compared to normal cells [93]. Pim-1 is also highly expressed in pediatric T-ALL patient samples, especially the early T-cell precursor, ETP-ALL subtype, suggesting Pim-1 is a driver of early T-ALL growth compared to more mature T-ALL disease [94]. Commutatively, these observations demonstrate that Pim kinases are active in ALL; and evidence strongly links Pim activation to genetic translocation or mutation/activation of the JAK/STAT and/or interleukin-7 (IL-7Rα) pathways (Fig. 6A). Most primary samples from T-ALL express IL-7Rα and respond to IL-7 [95, 96]. Pim-1 is activated downstream of the IL-7Rα, through STAT5, either through mutation or through IL-7 stimulation [97, 98]. A large percentage of ALL cases harbor genetic abnormalities in tyrosine kinases. The BCR/ABL-Ph + translocation (breakpoint cluster region/Proto-oncogene tyrosine-protein kinase ABL1), involving the Philadelphia chromosome (Ph+) translocation is the most common genetic translocation found in adult ALL cases, occurring in approximately 25% of cases. Though Pim-1 expression is not required for BCR/ABL-mediated transformation, it does benefit tumor cell survival. While the BCR/ABL is the most common genetic translocation in adult ALL, the TEL/AML1 (Transcription Factor ETV6/RUNX Family Transcription Factor 1) fusion is the most common in childhood ALL, occurring in approximately 22% of cases. Though rare, the BCR/ABL-Ph + translocation has also been reported in T-ALL. In addition to TEL/AM1, chromosome aberrations in chromosome 6 are found in B-ALL patients. In a small case study of TEL/AML1+ ALL childhood samples, 86% harbored additional chromosomal aberrations, including chromosome 6, where the Pim-1 gene (6p21–23) is located [99–101]. Though not confirmed it does suggest that genetic aberrations in the Pim-1 gene could contribute to leukemogenesis in B-ALL. Further supporting this, cells transformed by oncogenic tyrosine kinases (TEL/JAK2, TEL/TRKC (TEL/tyrosine kinase receptor C), TEL/ABL, BCR/ABL, FLT3-ITD, and H4/PDGFβR (D10S170/Platelet derived growth factor receptor beta)) all display elevated levels of Pim-1 and Pim-2 expression [102]. In addition, large genetic screens of ALL patients found a small percentage of genetic alterations in mostly pediatric ALL samples (Fig. 6B) [29, 30, 103, 104]. These consisted mostly of deep deletions in the Pim-3 gene, with gene amplifications in all 3 Pim kinases (Fig. 6C). The significance of these alterations, and whether they lead to enhanced Pim kinase activity, is currently unknown. T-cell acute lymphoblastic leukemia (T-ALL) comprises 12% of ALL in children and 25% in adults. Pim-1 is one of the critically deregulated oncogenes in T-ALL. Similar to B-ALL, genetic aberrations in Pim-1 gene locus have been found in T-ALL and T-LBL patients, t(6;7)(p21;q34), producing, TCRβ-PIM1 (T-cell receptor beta locus/PIM1), whereby the TCRβ enhancer was found juxtaposed to the 5’UTR (untranslated region) of the Pim-1 gene [105–108]. Although this genetic translocation is rare in T-ALL patients, TCRβ-PIM1+ T-ALL patients and T-ALL subgroups (HOXA, TLX, and LYL1+ (Lymphoblastic leukemia derived sequence 1)) that have JAK/STAT activating abnormalities (JAK1, JAK2, JAK3, IL7R, STAT5A/B, PTPN2 (protein tyrosine phosphatase non-receptor type 2), and/or NUP214-ABL1 (Nucleoporin Nup214-ABL1)) all lead to very high levels of Pim-1 gene expression [105, 108].
Fig. 6.
Cellular Signaling Pathways and Genetic Alterations Leading to Pim Kinase Expression in Acute Lymphoblastic Leukemia (ALL). A Model depicting the regulation of Pim kinase expression and activity in ALL. IL-7 signaling leads to enhanced Pim-1 and Pim-2 expression. Alternatively, common genetic alterations found in ALL patients leads to enhanced JAK/STAT activity and up-regulation of Pim kinases. B-C Cancer type summary (B) and OncoPrint (C) of genetic alterations from 3 cancer genomic studies on ALL. Data are derived from the cBioPortal for Cancer Genomics [29, 30]. The results published here (ALL, Target-2018) are in whole or part based upon data generated by the Therapeutically Applicable Research to Generate Effective Treatments (TARGET) https://ocg.cancer.gov/programs/target initiative, phs000464 (Acute Lymphoblastic Leukemia (ALL) Expansion Phase 2). The data used for this analysis are available at https://portal.gdc.cancer.gov/projects. Target-2018 are derived from pediatric ALL. ALL-2016 are derived from 69, primarily children and young adult, B-progenitor ALL patient samples [103]. ALL-2015 are derived from 85 ALL infants with MLL rearrangements [104]
Multiple myeloma (MM)
MM is characterized by over-proliferating plasma cells in the bone marrow. Pim-1, − 2, and − 3 are expressed in MM cell lines and in primary MM patients [109] (Fig. 5C). However, Pim-3 expression is not strongly associated with the occurrence of MM cells. Pim-2 is highly expressed in MM cells and Pim-2 knock-down studies demonstrate that Pim-2 is required for MM cell proliferation [54]. Pim-2 expression is up-regulated in MM cells through IL-6/JAK2/STAT3 and TNFα/NF-κB mediated pathways and inhibitors to either STAT3 (cucurbitacin I) or IKKα/β (I-Kappa-B Kinase)(parthenolide) decrease Pim-2 expression [110]. Mutations, including hot spot, putative driver mutations in Pim-1, have been found in MM patient samples (Fig. 5D) [29, 30, 85]. Pim-2 may also play an important role in osteolytic bone lesions often seen in MM patients. In fact, high expression of Pim-2 has been detected in osteoclasts and bone marrow stromal cells in the MM microenvironment [110]. This was associated with worsened osteoclastic functions and bone lesions in MM patients. In agreement with these observations, use of Pim kinase inhibitors provide some protective effect on bone disease in MM patients [109, 111, 112]. This was found to be at least partially due to Pim-2-mediated inhibition of osteoblastogenesis and Pim regulation of NFATC1 (Nuclear factor of activated T-cells 1) and cathepsin K.
Non-Hodgkin’s lymphoma (NHL), chronic lymphocytic leukemia (CLL), and Hodgkin’s lymphoma (cHL)
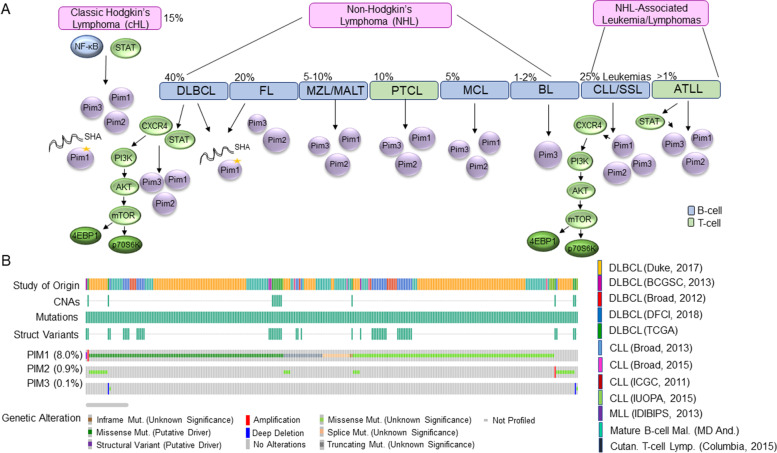
Non-Hodgkin’s lymphoma (NHL) encompasses a large array of leukemia/lymphomas, with over 60 subtypes recognized by the WHO. Nearly 85% of all NHLs are of B-cell origin. Aggressive NHLs include, diffuse large B-cell lymphomas (DLBCL) and its subtypes, Burkitt’s lymphoma (BL), peripheral T-cell lymphoma (PTCL), Mantle cell lymphoma (MCL), and transformed mucosa-associated lymphoid tissue (MALT) lymphoma and more indolent NHLs, including, chronic lymphocytic leukemia (CLL)/small lymphocytic lymphoma (SLL), follicular lymphoma (FL), cutaneous T-cell lymphoma (CTL), and nodal marginal zone lymphoma (NMZL). While an examination of Pim kinase expression, activity, and Pim kinase inhibitor therapy for all 60 NHL subtypes is beyond the scope of this review, there are key takeaways for NHLs. Most NHLs over-express Pim-1/Pim-2 – as an examination of patient samples from indolent and aggressive NHLs (MCL, DLBLC, FL, MZL-MALT, CLL, and NMZL) showed marked over-expression of Pim-2, and to a lesser degree, Pim-1, with Pim-3 levels similar to normal lymph node and tonsil tissues [113]. There are notable exceptions with BL patient samples displaying high levels of Pim-3 expression; and MCL expressing more Pim-1, while Pim-2 was only expressed in conjunction with Pim-1 [24, 63]. In addition, most NHLs are susceptible to Pim kinase inhibition either in mono or dual therapy; and the Pim-1 gene is susceptible to somatic hypermutation activity in some NHL subtypes (Fig. 7A).
Fig. 7.
Cellular Signaling and Genetic Alterations in Hodgkin’s and non-Hodgkin’s leukemia/lymphoma Leading to Enhanced Pim Kinase Activity. A Model depicting the regulation of Pim kinase expression and activity in various Hodgkin’s and non-Hodgkin’s lymphomas/leukemias. These include cHL (Classic Hodgkin’s Lymphoma), DLBCL (Diffuse Large B-cell Lymphoma), Follicular Lymphoma (FL), Marginal zone lymphoma (MZL), Mucosa-associated Lymphoid Tissue (MALT) lymphoma, Peripheral T-cell lymphoma (PTCL), Mantle Cell Lymphoma (MCL), Burkitt lymphoma (BL), Chronic lymphocytic leukemia (CLL), Small lymphocytic lymphoma (SLL), and Adult T-cell leukemia/lymphoma (ATLL). B OncoPrint of genetic alterations from 12 cancer genomic studies on various lymphomas and leukemias. Data was collected from cBioPortal for Cancer Genomics [29, 30]. These include whole genome sequencing from 4 chronic lymphocytic leukemia (CLL) studies: CLL from Broad-2013 [114], CLL tumors and normal samples from Broad-2015 [115], CLL, Monoclonal B-cell lymphocytosis (MBL), and 24 SLL from ICGC-11 [92], and CLL from IUOPA-2015 [93]. Whole genome sequencing from 5 diffuse large B-cell lymphoma (DLBCL) studies, including normal samples: DLBCL from Duke-17 [97], DLBCL from BCGSC-13 [95], DLBCL from Broad-12 [96], DLBCL from DFCI-18 [94], and DLBCL from TCGA [98]. Whole genome sequencing from cutaneous T-cell lymphomas from 25 Sezary syndrome and cutaneous T-cell lymphomas (CTCL) from Columbia-15 [99], mantle cell lymphoma (MCL) from IDIBIPS-13 [100], and mature B-cell malignancies from MD Anderson [101]
The most common subtype of NHL, DLBCL, compromises 30–40% of all NHL. DLBCL can occur from FLs and CLLs; and originates in germinal center B-cells. DLBCL patient samples express high levels of all Pim kinases, that correlate with active STAT3/STAT5/CXCR4. Survival and proliferation of these tumor cells rely upon activation of Pim as demonstrated by use of Pim inhibitors [113, 116]. There are two main molecular subtypes of DLBCL classified by their different source cells, stage of B-cell differentiation, and clinical outcomes: germinal center (GC-DLBCL) and activated B-cell-like DLBCL (ABC-DLBCL). Overall survival is lower in DLBCL patients expressing Pim-2, which appears to be restricted to the ABC subtype [113]. Pim-2 expression was found to be higher in the ABC-DLBCL subtype than the GC subtype; whereby Pim inhibition with ETP-39010 or Pim2 knock-down decreased BAD (Bcl2 associated antagonist of cell death), AKT, and 4E-BP1. There are numerous special subgroups of DLBCL. Primary mediastinal large B-cell lymphoma (PMLBCL) is a subgroup of DLBCL, while both nodular lymphocyte-predominant HL (NLPHL) and classic Hodgkin’s lymphoma (cHL) also arise from different differentiation stages in germinal center B-cells. A unique feature of these lymphomas, DLBCL, PMLBCL, NLPHL, and cHL, is the frequency of somatic hypermutation activity (SHA) that leads to genome instability. SHA is a common process of mutation of the immunoglobulin variable (IGV) region of B-cells undergoing antigen primed maturation. In contrast to most leukemias, the Pim kinases are subject to high rate of genetic alterations in lymphomas. Whole genome sequencing finds that almost 8% of DLBCLs, CLL, MLL, mature B-cell lymphomas, and cutaneous T-cell lymphomas carry Pim-1 genetic alterations (Fig. 7B) [29, 92–101, 114, 115]. These encompass, putative driver missense mutations, and amplifications, splice, missense, in frame, and truncating mutations of unknown significance. Pim-1 is one of four proto-oncogenes involved in DLBCL, PMLBCL, and FL SHA [102, 105, 106]. The 5’UTR of Pim-1, along with Pax-5 (Paired Box 5), RhoH/TFF (Ras homolog family member H/Trefoil Factor), and c-Myc, undergoes SHA with mutations occurring within coding exons leading to changes in amino acids and possibly Pim-1 activity. These genes, including Pim-1, are also highly susceptible to chromosomal translocations and double-strand DNA breaks [107]. SHA of the Pim-1 gene has also been shown for AIDS-related non-Hodgkin lymphomas (AIDS-NHLs) and HCV-positive B-cell NHL patients [108, 117]. In DLBCL, and particularly the subtype ABC-DLBCL, Pim-1 is one of the highest mutated genes [118]. The missense and frameshift mutations found in DLBCL due to SHA preserve Pim-1 functionality and tumor cells remain sensitive to PIM447 inhibition. These events were found to be only slightly correlated with negative disease prognosis. Even then, these phenotypes were mostly believed to arise from aberrant AID activity itself, and not Pim mutation [118]. In another subtype of NHL, primary central nervous system lymphoma (PCNSL), Pim-1 is one of the most highly mutated genes and over 77% of PCNSL harbored Pim1 mutations [119]. Pim-1 expression was high in PCNSL patients and correlated with MYD88 (Myeloid Differentiation Primary Response Protein MyD88) expression. High expression of either of these proteins led to a more unfavorable prognosis and lower overall survival. Therefore, Pim-1, along with other proto-oncogenes, may have a substantial role in the development of lymphomas and presents as an interesting therapeutic target. MCL is an NHL in which patients are characterized as having high levels of cyclin D1, with patients that go through patterns of continuous relapse following chemotherapy. MCL subtypes have shown especially high levels of Pim-1 and Pim-2 [120]. Preclinical use of the Pim inhibitor SGI-1776 resulted in decreased phosphorylation of translational targets (4E-BP1) associated with a lower expression of cyclin D1 and survival factor MCL1 (BCL2 family apoptosis regulator) leading to apoptosis of tumor cells [90].
T-cell lymphomas make up for less than 15% of all NHLs. These include lymphomas of the mature T-cells located in the periphery, such as primary peripheral T-cell lymphoma (PTCL) and adult T-cell leukemia/lymphoma (ATLL). In PTCL patient samples, Pim-1 and Pim-2 expression is elevated and correlates with STAT, NF-κB, and IL-2 (interleukin-2) compared to normal lymph nodes [121]. PTCL cells treated with the pan-Pim inhibitor, ETP-39010, lost viability due to apoptosis induction and an impaired DNA damage response. ATLL (adult T-cell leukemia/lymphoma) is a chronic leukemia/lymphoma deriving from mature T-cells infected with the human T-cell leukemia virus type-1 (HTLV-I). Leukemic patient cells from ATLL patients exhibit high expression of all Pim kinases with over-expression of Pim-2 and Pim-3 when compared to normal PBMCs (peripheral blood mononuclear cells) [122]. All three Pim kinases are regulated by the JAK/STAT pathway, particularly STAT3 and STAT5. Compared to normal PBMCs, ATLL cells are sensitive to Pim kinase inhibition (Smi-4a and AZD1208) and ex vivo ATLL tumor burden is decreased in mice treated with AZD1208 [122]. Since ATLL is caused by the HTLV-I virus, a role for Pim-1, − 2, and − 3 in inhibiting viral transactivation has also been seen, which may allow immune escape and sustainment of ATLL cells [123].
CLL is the most common chronic leukemia in adults. While CLL is not by definition an NHL, CLL patients can develop NHL through Richter’s syndrome. Studies have confirmed over-expression of Pim-1 and Pim-2 in CLL patients compared to normal lymphocytes [124, 125]. Pim-1/− 2 are especially elevated in B-CLL patients and correlated with worse prognosis in B-CLL (elevated in Binet stage C) and B-CLL subtype, while Pim-1/2 expression was lower in patients achieving complete remission [126–129]. Pim-3 did not correlate with any clinical characteristic. Like AML, CXCR4 phosphorylation, a hallmark of CLL cells, correlates with Pim-1 kinase expression [124]. CLL cells respond favorably to Pim kinase inhibitors– whereby K00135 and K00486 (two inhibitors which preferentially target Pim-1/− 2) and the pan-Pim inhibitor, A47, decreased CLL cell proliferation and apoptosis [124]. In addition, treatment with SGI-1776 inhibited ex vivo primary CLL patient samples by way of Mcl-1 mediated apoptosis and decreased RNA transcription [125]. Use of the Pim inhibitor, SEL24/MEN1703 (SEL24-B489), in ex vivo primary CLL patient samples led to similar effects that were not seen in normal B-cells [129]. Knock-down of individual Pim kinases in CLL cells demonstrated that Pim-1 regulates CXCR4 surface expression, while Pim-2 and Pim-3 are more important for CLL survival [124]. Therefore, the use of Pim kinase inhibitors leads to a loss in CLL chemotaxis due to less phosphorylation and expression of CXCR4 on the cells surface and loss of CXCR4 activation of mTOR [129].
The most common B-cell lymphoma outside of NHLs, are classic Hodgkin’s lymphoma (cHL). cHL is characterized by Reed-Sternberg cells, enlarged B-cells that express few B-cell specific genes. Aside from SHA of the Pim-1 gene that is also seen in DLBCL, cHL patient samples also express Pim kinases through normal transcriptional means. Patient samples from cHL have high expression of Pim-1,-2, and − 3 driven by NF-κB and STAT pathways and are sensitive to Pim kinase inhibition with the Pim/FLT3 inhibitor, SEL24/MEN1703 (SEL24-B489), or the dual Pim kinase combined with histone deacetylase inhibitor (suberoylanilide hydroxamic acid (SAHA) [130, 131]. Pim inhibition in cHL modulates expression of immunoregulatory molecules (PD-L1/2 and Gal-1) creating an immunosuppressive tumor microenvironment.
Myeloproliferative neoplasms (MPN)
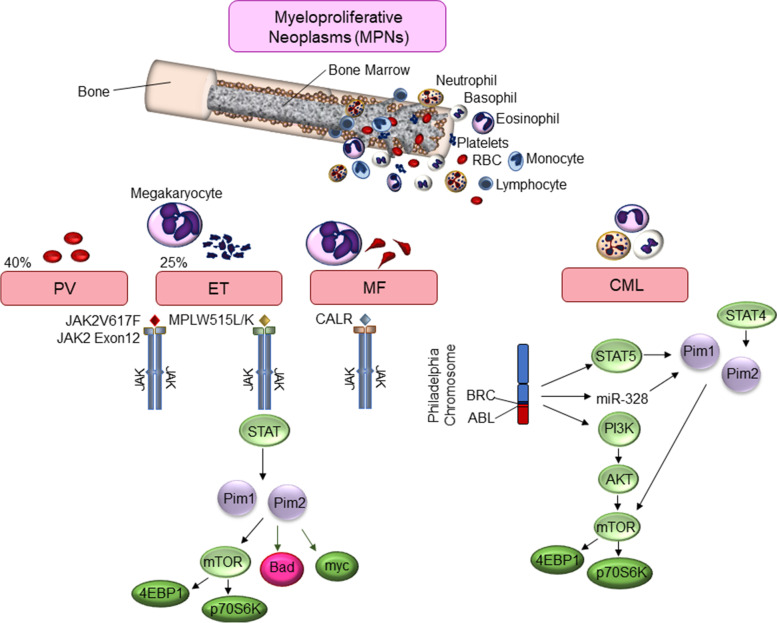
MPNs and CML comprise a class of chronic leukemias that arise from mature hematopoietic cells in the lymph nodes. MPNs are classified into Philadelphia chromosome-positive (Ph+) or -negative (Ph-) categories. Most MPNs are considered classical MPNs, without Ph- translocations and are divided into three main types, polycythemia vera (PV), myelofibrosis (MF), and essential thrombocythemia (ET). MPNs occur when bone marrow stem cells grow abnormally and over-produce leukocytes, such as red blood cells (PV), platelets (ET), granulocytes (CML), or neutrophils/eosinophils. MF is the deadliest MPN whereby scar tissue develops in the bone marrow, causing a disruption in normal leukocyte production, with enhanced megakaryocytes. MPNs are characterized not only by their cytology, but also the high level of JAK2 mutations. 95% of PVs and 50–60% of ETs and MFs harbor JAK2 mutations [132]. In addition, mutations in calreticulin (CALR) and MPL (thrombopoietin receptor), particularly the MPLW515L/K mutation, which signals through JAK2, are frequently seen. Pim-1/− 2 expression is dependent upon JAK2 signaling in MPN (Fig. 8) [133]. In PV patient samples carrying the constitutively active JAK2 mutation, V617F, Pim-1 is over-expressed due to an active JAK/STAT pathway compared to non-V617F PV patients samples [134]. Pim-1 is highly over-expressed in granulocytes, PBMCs, and bone marrow from MF patient samples [135]. Pim-1 cooperates with JAK or MPL mutants in the development of MF. Loss of Pim-1 gene expression or treatment with Pim inhibitors (TP-3654) in various in vivo MF models, involving JAK V617F or MPL515L, led to loss of MF development and decreased bone fibrosis. Furthermore, in vitro cell data demonstrated that V617F transformation in erythroleukemia cells was dependent upon downstream JAK signaling components, c-Myc, Pim-1, and Pim-2 [136].
Fig. 8.
Cellular Mechanisms for Increased Pim Kinase Activity in Myeloproliferative Neoplasms. Model depicting the regulation of Pim kinase expression in various myeloproliferative neoplasms (MPNs). These include Polycythemia Vera (PV) blood cancer, Essential Thrombocythemia (ET) blood cancer, Myelofibrosis (MF) blood cancer, and Chronic Myelogenous Leukemia (CML). These cancers arise from mature hematopoietic cells in the lymph nodes. Pim kinases are activated through various mechanism, including genetic alterations JAK/STAT pathway and BRC/ABL mutations leading to downstream activation of Pim kinases
CML results from hematopoietic stem cells of myeloid origin. As much as 90% of CML patients carry the Ph + translocation, which results in a shortened chromosome 22. Like ALL, this results in the oncogene tyrosine kinase gene, BCR-ABL. Pim-1 is up-regulated downstream of BCR-ABL through STAT5 induction and miR-328 mediated regulation of the Pim-1 3’UTR [137]. In CML patients Pim-1 is essential for BCR-ABL mediated in vivo transformation and leukemogenesis [138]; and simultaneous knockdown of Pim-1 and Pim-2 in cells transformed by BCR-ABL eliminated growth factor dependent growth [139]. These results suggest Pim kinase inhibition could also be an effective treatment against CML.
Targeting Pim kinases in leukemia and lymphoma
Pim kinases have a unique ATP binding mode, which unlike other kinases has a single hydrogen bond donor in the hinge region [140]. This structural difference has allowed the development of specific and selective inhibitors that target Pim kinases. First and second-class generations of Pim kinase inhibitors have been developed over the past decade (Table 2). Early Pim inhibitors, or 1st generation inhibitors, targeted solely Pim-1, without much efficacy against other isoforms. However, given the redundancy in some Pim kinase substrates it was soon realized that an inhibitor that blocked all three kinases was needed to block Pim signaling. Subsequently, inhibitors were developed that inhibited all three Pim kinases (pan-Pim kinase inhibitors, or 2nd class Pim inhibitors). These include most of the Pim kinase inhibitors used in clinical trials. SuperGen’s, SGI-1776, was the first, and only 1st generation Pim inhibitor to be used in human clinical trials. While showing limited efficacy in solid tumors and lymphomas, SGI-1776 caused adverse cardiac QTc prolongation events, leading SGI-1776 to be discontinued. The 2nd generation Pim inhibitor AZD1208, developed by AstraZeneca, entered Phase I human trials in 2012. Dose escalation studies were originally performed in advanced solid tumors and hematological malignancies. However, clinical results did not meet primary endpoints; and AZD1208 was associated with adverse events suggesting it would not be clinically useful [141]. More recently, two new 2nd class inhibitors, PIM447 (LGH447) and Uzansertib (INCB053914) have been developed. PIM447, developed by Novartis, shows greater pan-Pim inhibition than either AZD1208 or SGI-1776, enhancing the block against Pim-2 [142]. PIM447 was also effective at significantly lower doses and with low to moderate clearance. As of this review, PIM447 has been used in at least 5 clinical trials, with results from one limited study demonstrating positive results (discussed below for MM). Incyte Corporation developed Uzansertib as a 2nd class generation therapy with potent toxicity against all three Pim isoforms [143]. Uzansertib has been part of 3 Phase 1 clinical trials. While one study was terminated due to a lack of funding, another found possible efficacy as a monotherapy in advanced hematological malignancies (discussed below for AML) [144].
Table 2.
Current Pim inhibitors used in vitro, ex vivo, and in current or past clinical trials
| Drug Target | Development | Clinical Trials | Treatment Group | Therapy Type | |
|---|---|---|---|---|---|
| A47 | pan-PIM | Preclinical | – | – | – |
| Abemaciclib (Verzenio) | Pim1-CDK4/6 | Phase 1 | NCT03905889: Active (NR) | Metastatic Renal Cell Carcinoma | Dual therapy with Abemaciclib and Sunitinib |
| AZD1208 | pan-PIM |
Phase 1 Phase 1 |
NCT01588548: Completed NCT01489722: Terminated |
Adv Solid Tumors/Malignant Lymphoma Relapsed/Refractory AML |
Monotherapy Monotherapy |
| AZD1897 | pan-PIM | Preclinical | – | – | – |
| ETH-155008 | Pim3-CDK4/6 (FLT3) | Phase 1 | NCT04840784: Recruiting | R/R: B-NHL, CLL/SLL and AML | Monotherapy |
|
ETP-39010 ETP-45299 ETP-47551 |
pan-PIM | Preclinical | – | – | – |
| INCB053914 (Uzansertib) | pan-PIM |
Phase 1 Phase 1/2 Phase 1 |
NCT03688152: Completed NCT02587598: Ter/BD NCT04355039: WD/LF |
Relapsed/Refractory DLBCL Adv Solid Tumors Relapse/Refractory MM |
Dual therapy with INCB050465 Monotherapy and with cytarabine, azacitidine, and ruxolitinib Triple agent therapy with pomalidomide with dexamethasone |
| JP11646 | Pim2 | Preclinical | – | – | – |
| K00135 | Pim1/Pim2 | Preclinical | – | – | – |
| K00486 | Pim1/Pim2 | Preclinical | – | – | – |
| LGB321 | pan-PIM | Preclinical | – | – | – |
| PIM447 (LGH447) | pan-PIM |
Phase 1 Phase 1 Phase 1 Phase 1 Phase 1 |
NCT02370706: Completed NCT01456689: Completed NCT02078609: Completed NCT02144038: Completed NCT02160951: Completed |
Myelofibrosis Relapsed/Refractory MM AML or High Risk MDS Relapsed/Refractory MM Relapsed/Refractory MM (Japan) |
Triple agent therapy with Ruxolitinib and LEE011 Monotherapy Monotherapy or Dual therapy with midostaurin (AML only) Dual agent therapy with BYL719 Monotherapy |
| SEL24/MEN1703 (SEL24-B489) | PIM/FLT3 | Phase 1/2 | NCT03008187: Recruiting | AML | Dual Pim/FLT3 therapy |
| SGI-1776 | Pim1 |
Phase 1 Phase1 |
NCT01239108: Withdrawn NCT00848601: Terminated |
Relapsed/Refractory Leukemias Refractory Prostate and Refractory NHLs |
Monotherapy Monotherapy |
|
Smi-4a Smi-16a |
PIm1 Pim1/Pim2 |
Preclinical | – | – | – |
| TP-3654 | Pan-PIM | Phase 1/2 | NCT04176198: Recruiting | Intermediate/high-risk primary or secondary MF | Monotherapy |
At least three, Phase 1 clinical trials with Uzansertib have been conducted in advanced hematological malignancies, which included AML. Early data suggests Uzansertib was favorably tolerated, inhibited Pim activity, and had few adverse effects (that could be treated with reduced Uzansertib or additional therapy) [144]. This trial included advanced AML, high-risk MDS, MPN, MM, and lymphomas. The most common adverse effects were elevated alanine aminotransferase (ALT) and aspartate aminotransferase (AST) levels, which could be suggestive of liver or heart issues. Phase 1 clinical trials on AML patients using AZD1208 or PIM447 have also been performed. Monotherapy with AZD1208 was unable to clear disease and had adverse events, particularly related to gastrointestinal effects of nausea and diarrhea [141]. Febrile neutropenia and rash were also noted. While monotherapy with Pim inhibitors showed promise for treating AML, (particularly Uzansertib and PIM447) intrinsic resistance to Pim inhibition has made dual-therapeutic options a more attractive option. Addition of FLT3-ID inhibitors to AZD1208 is effective in enhancing apoptosis in primary AML blasts due to the positive feedback loop that exists between Pim-1 and FLT3 [70, 145]. Based on the fact that Pim loss leads to increases in ROS/p38/AKT/mTOR signaling (Fig. 3 and Table 3); dual targeting with a p38 inhibitor (SCIO-469), AKT inhibitors (MK2206 and AZD5363), mTOR inhibitors (AZD8055 and AZD2014), or PI3K inhibitors (GDC-0941) have all shown beneficial effects [146–150]. Dual chemotherapy of primary FLT3-ITD AML cells with topoisomerase inhibitors (daunorubicin, etoposide, and mitoxantrone) and AZD1208 also sensitizes cells because of accumulation of reactive oxygen species (ROS) and DNA double strand breaks [151, 152]. EC-70124, a multi-kinase drug targeting FLT3, JAK, SYK, and Pim kinases was also efficient at targeting AML cells [153]. Enhanced efficacy with dual pan-Pim kinase inhibitors and CDK4/6 (PD 0332991), JAK/STAT5 (ruxolitinib) inhibitors, or CXCR4 antagonists (BL-8040 and Plerixafor) that are in clinical trials, may also prove beneficial in treating refractory AML [154–159]. In fact, a Phase I human clinical trial has recently begun recruiting for the use of ETH-155008, a triple inhibitor to Pim-3, FLT3, and CDK4/6 in the treatment of relapsed/refractory AML, CLL/SLL, and B-cell NHL. ETH-155008 has shown promise in pre-clinical trials with AML cell lines and in vivo AML mouse models [160]. SEL24/MEN1703 is another dual-therapy drug showing promise in AML. SEL24/MEN1703 is a PIM/FLT3 inhibitor currently recruiting for Phase I/II clinical trials. Early results indicate SEL24/MEN1703 may be effective as a single use agent in AML. SEL24/MEN1703 had a manageable safety profile and complete remission was seen in several patients [161].
Table 3.
Pim kinase inhibitors used in preclinical and clinical (bold) trials for AML
| Acute Myeloid Leukemia | Target(s) | Type | Clinical Trials | |
|---|---|---|---|---|
| AZD1208 | pan-Pim | Single | AML | NCT01489722 |
| AZD1208 + Daunorubicin (etoposide, and mitoxantrone) | pan-Pim + Topoisomerase 2 | Dual-therapy | Preclinical | – |
| AZD1208 + SCIO-469 | pan-Pim + p38 | Dual-therapy | Preclinical | – |
| AZD1208 + MK2206 (AZD5363) | pan-Pim + AKT | Dual-therapy | Preclinical | – |
| AZD1208 + AZD2014 (AZD8055) | pan-Pim + mTOR | Dual-therapy | Preclinical | – |
| AZD1897 | pan-Pim | Single | Preclinical | – |
| EC-70124 | pan-kinase (Pim, FLT3, JAK, SYK) | Single | Preclinical | – |
| ETH-155008 |
Pim3 FLT3 CDK4/6 |
Triple inhibitor (FLT3, Pim-3 and CDK4/6) Monotherapy | AML | NCT04840784 |
| ETP-45299 + GDC-0941 | Pim1 + PI3K | Dual-therapy | Preclinical | – |
| K00135 | Pim1/Pim2 | Single | Preclinical | – |
| K00486 | Pim1/Pim2 | Single | Preclinical | – |
| PIM447 | pan-Pim | Single | AML | NCT02078609 |
| SEL24/MEN1703 |
PIM FLT3 |
Double inhibitor (FLT3, Pim) Monotherapy | AML | NCT03008187 |
| SGI-1776 | pan-Pim | Single | Yes | – |
| Uzansertib | Pan-Pim | Single | AML | NCT02587598 |
To date, there are currently no human clinical trials ongoing or recruiting for treatment of ALL with Pim inhibitors. However, extensive pre-clinical testing suggests this could be an interesting option to reduce ALL burden (Table 4). Inhibition of Pim kinases in Ph + ALL, including relapsed and refractory Ph + ALL, leads to robust reductions in colony formation, which are further enhanced with the addition of the Bcl-2 antagonist, sabutoclax [162]. This combination is also effective against leukemia burden in mice ejected with Ph + ALL cells. Treatment with Pim inhibitors (AZD1208 or TP-3654) in T-ALL or T-LBL patient derived xenograph mice models carrying the TCRβ-PIM1+ translocation or high Pim-1 expression levels caused tumor growth to be substantially inhibited [163]. Significant survival was further seen in these mouse models when dexamethasone, a glucocorticoid used in current ALL treatment, was given in parallel. T-ALL cells are also sensitive to Pim inhibitors (AZD1208 and LGB321) to varying degrees depending upon the level of Pim-1, JAK/STAT, IL-7, and/or the sensitivity to Notch gamma secretase inhibition [164, 165]. Combined Pim and tyrosine kinase inhibitor (ponatinib and dasatinib) therapy led to synergistic effects; with decreased tumor burden and prolonged survival in T-ALL engrafted mice [165]. Pim inhibitor therapy (Smi-4a) could also synergize with mitogen-activated protein kinase kinase 1/2 (MEK1/2) inhibitor (U0126) in reducing tumor burden in T-ALL and B-ALL engrafted mouse tumors [166, 167]. Interestingly, glucocorticoids that are given during the early, induction phase of T-ALL and T-LBL treatment, can induce IL-7Rα activity. This suggests that tumor cells surviving initial treatment may over-express Pim-1, given that IL-7 activity leads to JAK/STAT activation. Indeed, mouse xenograph models of T-ALL/T-LBL treated with a standard chemotherapy regimen (vincristine, dexamethasone and L-asparaginase) showed strong up-regulation of Pim-1 in residual leukemic blasts [168]. Increased survival was noted when PIM447 was added. This suggests that combination therapy, in which a Pim kinases inhibitor is added to ALL treatment, cannot only aid in reducing ALL leukemia cells, but also could be beneficial in reducing the MRD burden.
Table 4.
Pim kinase inhibitors used in preclinical and clinical (bold) trials for ALL
| Acute Lymphoblastic Leukemia | Target | Type | Clinical Trials |
|---|---|---|---|
| AZD1208 | pan-Pim | Single | Yes |
| AZD1208 + Ponatinib or Dasatinib | pan-Pim + TKI | Dual-therapy | – |
| AZD1208 + Ponatinib + Z-VAD-FMK | pan-Pim + TKI+ pan-caspase | Triple-therapy | – |
| AZD1208 + Sabutoclax | pan-Pim + BCL2 | Dual-therapy | – |
| AZD1208 + inLCK | pan-Pim + LCK | Dual-therapy | – |
| LGB321 | pan-Pim | Single | Preclinical |
| PIM447 | Pan-Pim | Single | Yes |
| Smi-4a | Pim1 | Single | Preclinical |
| Smi-4a + U0126 | pan-Pim + MEK1/2 | Dual | – |
| TP-3654 | Pan-Pim | Single | Preclinical |
| TP-3654 and dexamethasone | Pan-Pim and glucocorticoid therapy | Dual-therapy | – |
Several human clinical trials of Pim inhibitors to treat MM are underway (Table 5). MM patients were included in the clinical trials with Uzansertib that were discussed with the AML patients above. Phase I clinical trials with PIM447 in relapse/refractory MM are completed; however, results have not been officially published. In one trial of 79 patients with at least four previous treatments, the partial response rate (or better) was 8.9% with a clinical benefit rate of 25.3% [169]. PIM447 was well tolerated even with adverse events that comprised thrombocytopenia and anemia. A smaller study, comprised of 15 Japanese patients with relapsed or refractory MM, showed an overall response rate of 15.4% and a similar clinical benefit rate of 23.1%, with at least 2 patients achieving partial responses [170]. Thrombocytopenia, anemia, and leukopenia were also observed at high rates. These results are highly significant to MM therapy, considering these patients are often refractory to other therapies. As is the case with other leukemias, these studies suggest that Pim inhibitors can be used and are relatively well tolerated in MM patients but may require dual or multi-inhibitor combination therapies. In preclinical studies both Pim kinases inhibitors SGI-1776 and LGB321 inhibit MM cells in mouse xenograph models [54, 171]. LGB321 could combine with BKM12 (inPI3K), with subsequent loss of mTOR activity. The underlying mechanism was related to inhibition of Pim-2 phosphorylation of TSC2 and activation of mTOR activity in MM cells [54]. Additional studies showed that the Pim kinase inhibitor Smi-16a inhibits MM cell viability and demonstrated synergistic effect when combined with doxorubicin [172]. Dual and triple drugs that contain Pim kinase inhibitors, along with PI3K and/or mTOR inhibitors have also been effective in MM cells [172]. Based on these observations it is tempting to speculate that combination treatment used to treat AML patients could be effective for MM patients. The treatments developed to target FLT3, CXCR4, and the PI3K pathway could work in conjunction with Pim inhibitors in MM, given the similarity in oncogenic pathways found in both these cancers. Furthermore, Pim kinase inhibition also relieve symptoms of osteolytic bone lesions often seen in MM patients and in pre-clinical trials, treatment of MM cells with Smi-16a or PIM447 prevents MM tumor growth in mice and suppresses myeloma-induced bone destruction [109, 111]. Finally, targeting miRNAs that regulate Pim kinases may represent future solutions for the treatment of MM. The proteasomal inhibitor, MLN2238, has been used in clinical trials and has been found to positively regulate miR-33a expression [171]. miR-33a directly regulates Pim-1 and MM cells treated either with miR-33a or MLN2238 suffer reduced Pim-1 signaling and cell viability.
Table 5.
Pim kinase inhibitors used in preclinical and clinical (bold) trials for MM
| Multiple Myeloma | Target | Type | Clinical Trials | |
|---|---|---|---|---|
| IBL-202 | Pim/PI3K | Double inhibitor (PI3K, Pim) Monotherapy | Preclinical | – |
| IBL-301 | Pim/PI3K/mTOR | Triple inhibitor (PI3K, mTOR, Pim) Monotherapy | Preclinical | – |
| INCB053914 + pomalidomide + dexamethasone | pan-Pim + thalidomide analogue + corticosteroid | Triple-therapy | MM | NCT04355039 |
| JP11646 | Pim2 | Single | Preclinical | – |
| LGB321 | pan-Pim | Single | Preclinical | – |
| LGB321 + BKM120 | pan-Pim + PI3K | Dual-therapy | Preclinical | – |
| PIM447 | pan-Pim | Single | MM | NCT01456689 |
| MM | NCT02144038 | |||
| SGI-1776 | pan-Pim | Single | Yes | – |
| Smi-16a | Pim1/Pim2 | Single | Preclinical | – |
| Smi-16a + doxorubicin | Pim1/Pim2 + topoisomerase | Dual-therapy | – | – |
| Uzansertib | pan-Pim | Single | MM | NCT04355039 |
One of the first Pim kinases Phase I clinical trials included lymphoma patients (Table 6). As discussed above, Phase I clinical trials with SGI-1776 on relapsed/refractory NHL patients, showed proof of principle – that Pim kinase inhibition could be effective in treatment of lymphoma, but was terminated due to adverse cardiac events. Preclinical trials with SGI-1776 and Pim kinase inhibitors in MCL cells have also been successful, targeting transcription and translation in these cells [90, 173]. Preclinical and clinical data suggests that Pim kinase inhibition may facilitate to overcome the resistance associated with long-term chemotherapy. In fact, in Phase I trials of patients with recurrent NHL that has disseminated to the central nervous system (CNS), high Pim-2 expression was a marker for resistance to rituximab monotherapy [174]. In studies of MCL patients given high dose therapy, stem cell transplantation, and rituximab; Pim-1 expression also served as a predictive marker of poor outcome [120]. The CDK/Pim/FLT3 inhibitor, ETH-155008, is currently being assessed in refractory/relapsed B-cell, NHL patients as well as CLL and SLL patients. Clinical trials have also been conducted with DLBCL patients. Uzansertib has been used in Phase I clinical trials with relapsed/refractory DLBCL patient samples; however, results have not been reported. Incyte has actively recruited patients to test dual-therapy, Uzansertib with a PI3K inhibitor (Parsaclisib). This was based on preclinical data showing the effectiveness of Uzansertib along with Parsaclisib or JAK inhibitors (itacitinib or ruxolitinib), or cytarabine (a common chemotherapy reagent) in DLBCL xenografts [143]. While clinical trials have not been initiated for many of the NHLs and cHLs, preclinical data is very promising. As discussed above, preclinical xenograft models of ATL with AZD1208 led to reduced tumor burden, while in vitro treatment of PTCLs and cHLs with Pim inhibitors and/or led to reduced proliferation. LGB321 was also successful in reducing tumor burden in CLL xenografts. Similar to other conclusions, tumor burden was further reduced when the Pim kinase inhibitor was given as dual therapy with ibrutinib, an inhibitor of Bruton’s tyrosine kinase (BTK) [175]. Treatment with AZD1208 and ibrutinib was also successful in DLBCL cells [176].
Table 6.
Pim kinase inhibitors used in preclinical and clinical (bold) trials for cHL and NHL
| Pim Inhibitor | Target | Type | Clinical Trials | ||
|---|---|---|---|---|---|
| cHL | SEL24/MEN1703 | PIM/FLT3 | Double inhibitor (FLT3, Pim) Monotherapy | Yes | – |
| Pim Inhibitor + suberoylanilide hydroxamic acid (SAHA) or sodium butyrate (SB | Pim + Histone deacetylase inhibitors | Dual-therapy | Preclinical | – | |
| DLBCL | AZD1208 + ibrutinib | pan-Pim + BTK | Dual-therapy | Preclinical | – |
| ETH-155008 | Pim3-CDK4/6(FLT3) | Triple inhibitor (FLT3, Pim-3 and CDK4/6) Monotherapy | DLBCL | NCT04840784 | |
| Uzansertib | pan-Pim | Single | DLBCL | NCT03688152 | |
| Uzansertib + Parsaclisib | pan-Pim + PI3K | Dual-therapy | DLBCL | Incyte | |
| Uzansertib + Itacitinib (or ruxolitinib) | pan-Pim + JAK | Dual-therapy | Preclinical | – | |
| Uzansertib + cytarabine | pan-Pim + Chemotherapy | Dual-therapy | Preclinical | – | |
| PTCL | ETP-39010 | pan-Pim | Single | Preclinical | – |
| ETP-47551 | pan-Pim | Single | Preclinical | – | |
| MCL | SGI-1776 | PIM1 | Single | MCL | NCT01239108 |
| CLL/SLL | K00135 | Pim1/Pim2 | Single | Preclinical | – |
| K00486 | Pim1/Pim2 | Single | Preclinical | – | |
| A47 | pan-Pim | Single | Preclinical | – | |
| ETH-155008 | Pim3-CDK4/6 (FLT3) | Triple inhibitor (FLT3, Pim-3 and CDK4/6) Monotherapy | CLL/SLL | NCT04840784 | |
| SGI-1776 | PIM1 | Single | Yes | – | |
| SEL24/MEN1703 | PIM/FLT3 | Double inhibitor (FLT3, Pim) Monotherapy | Yes | – | |
| LGB321 | pan-Pim | Single | Preclinical | – | |
| LGB321 + ibrutinib | pan-Pim + BTK | Dual-therapy | Preclinical | – | |
| ATL | Smi-16a | Pim1/Pim2 | Single | Preclinical | – |
| AZD1208 | pan-Pim | Single | Yes | – |
JAK2 mutations, especially V617F, play a critical role in MPN pathogenesis and drug resistance; however, JAK2 inhibitor monotherapy is largely ineffective in achieving consistent remission in MPN patients carrying these mutations. Resistance to JAK2 inhibitors has been shown in MPN cells carrying JAK2 mutations and in CML patients harboring the BCR-ABL translocation [177]. Because tumor cells rely upon constitutive activation of STAT5, ERK-1/2 (Extracellular signal-regulated kinase 2), and AKT signaling pathways, targeting down-stream JAK2 targets, such as Pim kinases may have significant benefits in preventing JAK2 inhibitor resistance (Table 7). Indeed, the fact that JAK2 chemo resistant cells harboring the V617F mutation display high expression of Pim kinases, compared to sensitive cell lines, suggests a role of Pim kinases in drug resistance [178]. Pan-Pim kinase inhibitors, such as AZD1208, Uzansertib, and SGI-1447 have been shown to be effective in ex vivo MPN patient samples, when combined with JAK inhibitors (ruxolitinib, AZ960, TG101209, and SAR302503) [133, 178–181] (Fig. 6). Unlike other Pim inhibitors, preclinical models with single therapy, TP-3654 have shown efficacy, even over JAK2 inhibitors (ruxolitinib) in treating fibrosis MF in vivo models [135]. Furthermore, the combination of TP-3654 with ruxolitinib led to greater reductions in MPN cells and fibrosis. Preclinical data is also promising for the combination of PIM447, ruxolitinib, and the CDK4/6 inhibitor, LEE011, in JAK2 V617F and MPL515L in vivo MF models, with longer survival and no additive toxicity seen [182].
Table 7.
Pim kinase inhibitors used in preclinical and clinical (bold) trials for MPNs
| Pim Inhibitor | Target | Type | Clinical Trials | ||
|---|---|---|---|---|---|
| MPNs | AZD1208 | pan-Pim | Single | Yes | – |
| AZD1208 + Ruxolitinib | pan-Pim + JAK | Dual-therapy | Preclinical | – | |
| SGI-1776 | Pim1/Pim2 | Single | Yes | – | |
| INCB053914 + Ruxolitinib | pan-Pim + JAK | Dual-therapy | Preclinical | – | |
| PIM447 | pan-Pim | Single | MF | NCT02370706 | |
| PIM447 + Ruxolitinib + LEE011 | pan-Pim + JAK + CDK4/6 | Triple-therapy | Preclinical | – | |
| TP-3654 | pan-Pim | Single | MF | NCT04176198 | |
| TP-3654 + Ruxolitinib | pan-Pim + JAK | Dual-therapy | Preclinical | – | |
| Pim inhibitor (PIM447) + SAR302503 (TG101348) | pan-Pim + JAK | Dual-therapy | Preclinical | – | |
| Uzansertib | pan-Pim | Single | MF | NCT02587598 | |
| CML | Smi-4a | Pim1 | Single | Preclinical | – |
| AZD1208 | pan-Pim | Single | Yes | – | |
| AZD1208 + imatinib mesylate | pan-Pim + TKI | Dual-therapy | No | – | |
| SGI-1776 | Pim1 | Yes | – | ||
| SGI-1776 + imatinib mesylate | pan-Pim + TKI | Dual-therapy | No | – |
In BCR-ABL carrying CML cells Pim inhibitors influenced cell viability and proliferation by targeting GSK3-β (glycogen synthase kinase 3 beta), mTOR, translation, and MYC/Mcl-1 [183, 184]. Chemoresistance of cancer stem cells represent a significant challenge and CML stem cells are inherently resistant to imatinib mesylate, a standard therapy for CML. Part of this resistance is due to high levels of Pim-2, which phosphorylates and inactivates proapoptotic factor, BAD. While imatinib mesylate was effective in treating CML stem cells with high Pim-2 expression induced through STAT5; imatinib mesylate resistant cells continued to exist due to activation of Pim-2 through an alternative, STAT4 dependent pathway [185]. To overcome this block in imatinib mesylate CML therapy, mono Pim kinase inhibitor or dual therapy with imatinib mesylate has been used [183, 184]. Treatment with SGI-1447 or AZD1208, along with imatinib mesylate, has a suppressive effect on Ph + primitive, imatinib mesylate sensitive, leukemic progenitor cells and imatinib mesylate insensitive, CML stem cells from CML patients, respectively [183, 185]. This suggests (like other lymphoproliferative cancers) that effective inhibition of Pim kinase activity can be a very successful treatment option to reduce disease burden and/or overcome resistance to current therapies.
Conclusion
Clinical trials using first generation Pim inhibitors have failed to significantly reduce disease burden or alleviate chemoresistance in patients. In addition, higher doses of Pim inhibitors may have off-target effects and can lead to adverse effects, including cardiac events, gastrointestinal issues, febrile neutropenia, and rash, among others. Newer, highly specific Pim kinase inhibitors, such as PIM447, Uzansertib, and TP-3654 can overcome these problems, allowing Pim targeting at lower concentrations. Another option is to directly target Pim kinases through either monoclonal Pim antibody therapy or by indirectly targeting Pim kinase regulators. Pim-1 was found on the cell surface of some leukemic cells, that could be targeted, with loss of proliferation, by monoclonal Pim-1 (mPim-1) therapy [186]. In addition, in vivo prostate cancer models treated with mPim-1, led to tumor growth reductions [187]. These early, pre-clinical trials suggest mPim-1 therapy may work; however, whether redundancy with other Pim kinases would reduce in vivo efficacy remains to be seen. Previous studies in MM and CML suggest that Pim kinases are subject to 3’UTR mediated down-regulation by miRNAs through miR-33a and miR-328, respectively. Pim-1 and Pim-3 are both regulated by miR-33a [188, 189]; and in various tissues and cell lines, the 3’UTR of Pim-1 is also targeted for inhibition by miR-206 [190], miR-214 [122], miR-370 [191], miR-486-5p, [192] miR-328 [137, 193], miR-124 [194], miR-144 [195], miR-542-3p [196], miR-101-3p [197]. Pim-2 is targeted by miR-26-5p [198] and miR-135-3p [199], while Pim-3 can also be targeted by miR-506 [200]. Targeting miRNAs directly or indirectly, such as is the case with MLN2238 in MM, may be a future direction for therapy.
Effective strategies to treat leukemia/lymphoma will likely incorporate dual or combination therapy that includes a pan-Pim inhibitor. Numerous pre-clinical studies have demonstrated increased efficacy when Pim inhibitors are part of a dual therapy regimen along with JAK inhibitors. Pim kinases are elevated by common protein tyrosine kinase receptors that are deregulated in most lymphoproliferative disorders, therefore targeting Pim and the JAK/STAT pathway is a very interesting option. This would allow reduced Pim inhibitor dosing, while possibly preventing JAK inhibitor resistance. In addition, several JAK inhibitors are part of common chemotherapy regimens and have good safety profiles, including ruxolitinib for lymphoproliferative disorders and, tofacitinib, baricitinib, and upadacitinib, for rheumatoid arthritis that have already gained FDA approval. The dual Pim-CDK4/6 inhibitor, abemaciclib, and multi-inhibitors, Pim-3-CDK4/6-FLT3, ETH-155008, and PIM-FLT3, SEL24/MEN1703 show promise and are currently undergoing clinical trials. Another strategy is to pair pan-Pim inhibitors with inhibitors of the PI3K/AKT/mTOR pathway, for which Pim kinases show parallel functions. Clinical trials are already underway or completed for drugs like, AKT inhibitor, MK-2206, for CLL/SLL and relapse/refractory leukemias or lymphomas, while mTOR inhibitors sirolimus (rapamycin) and everolimus are being used in clinical trials. Dual therapy with Bcl-2 or Mcl-1 antagonists with pan-Pim inhibition may also prove useful, as evidenced by results from preclinical data in ALL with sabutoclax (in-Bcl-2). Future studies are still needed to delegate the specific roles of individual Pim isoforms, their downstream targets, and how Pims are regulated to refine therapeutic options more precisely. However, the sheer number of pre-clinical and clinical trials being conducted with Pim inhibitors demonstrates the clinical significance of targeting the Pim pathway in lymphoproliferative disorders and solid tumors.
Abbreviations
- 4E-BP1
Eukaryotic Translation Initiation Factor 4E Binding Protein 1
- ABC-DLBCL
Activated B-cell-like DLBCL
- ABCB1/2 (BCRP)
ATP Binding Cassette Subfamily G Member
- ABC transporters
ATP-binding cassette transporters
- AIDS-NHL
AIDS-related non-Hodgkin lymphoma
- AKT
AKT serine/threonine kinase 1
- ALL
Acute lymphoblastic leukemia
- ALT
Alanine aminotransferase
- AML
Acute myeloid leukemia
- APL
Acute promyelocytic leukemia
- AR
Androgen receptor
- ASK1
Apoptosis signaling kinase 1
- AST
Aspartate aminotransferase
- ATLL
Adult T-cell leukemia/lymphoma
- B-ALL
B-lymphoblastic leukemia ALL
- BAD
Bcl2 associated antagonist of cell death
- Bcl-2
BCL2 Apoptosis Regulator
- Bim
BCL2 Like 11
- Bmi-1
B Lymphoma Mo-MLV Insertion Region 1 Homolog
- BCR/ABL-Ph+
Breakpoint cluster region/Proto-oncogene tyrosine-protein kinase ABL1
- BL
Burkitt’s lymphoma
- C-MyB and A-Myb
Myb Proto-Oncogene
- C-Myc/N-Myc
C/N-MYC Proto-Oncogene
- C-TAK1
Protein kinase Cdc25 C-associated kinase 1
- CALR
Calreticulin
- CDC25A/C
Cell Division Cycle 25A and C
- cHL
Hodgkin’s lymphoma
- CLL
Chronic lymphocytic leukemia
- Cot
MAP3K8/Mitogen-Activated Protein Kinase Kinase Kinase 8
- CML
Chronic myeloid leukemia
- CNS
Central nervous system
- CTL
Cutaneous T-cell lymphoma
- CXCR4
C-X-C Motif Chemokine Receptor 4
- eIF4B
Eukaryotic Translation Initiation Factor 4B
- ERK-1/2
Extracellular signal-regulated kinase 2
- ET
Essential thrombocythemia
- ETP-ALL
Early T-cell precursor ALL
- FL
Follicular lymphoma
- FLT3
Fms-like tyrosine kinase 3
- FoxO1a and FoxO3a
Forkhead box O1a and 3a
- GC
Germinal center
- H3
Histone H3
- H4/PDGFβR
D10S170/Platelet derived growth factor receptor beta
- HOXA9
Homeobox A9
- HP1γ
Heterochromatin-associated protein 1 gamma
- HTLV-1
Human T-cell leukemia virus type-1
- IGV
Immunoglobulin variable
- IKKα/β
I-Kappa-B Kinase alpha/beta
- IL-2
Interleukin-2
- IL-7Rα
Interleukin-7
- ITD
Internal tandem duplication
- JAK
Janus kinase
- LKB1
Serine/Threonine Kinase 11
- LYL1
Lymphoblastic leukemia derived sequence 1
- M-MuLV
Moloney-murine leukemia virus
- mPim-1
Monoclonal Pim-1
- mTOR
Mammalian target of rapamycin
- MALT
Transformed mucosa-associated lymphoid tissue lymphoma
- MCL
Mantle cell lymphoma
- MCL1
BCL2 family apoptosis regulator
- MDM2
MDM2 Proto-Oncogene
- MDS
Myelodysplastic syndromes
- MEK1/2
Mitogen-activated protein kinase kinase ½
- MF
Myelofibrosis
- MM
Multiple myeloma
- MPL
Thrombopoietin receptor
- MYD88
Myeloid Differentiation Primary Response Protein MyD88
- NF-κB
NF-Kappa-B transcription factor
- NFATC1
Nuclear factor of activated T-cells 1
- NKX3.1
NK3 Homeobox 1
- NHL
Non-Hodgkin’s lymphoma
- NLPHL
Nodular lymphocyte-predominant HL
- NMZL
Nodal marginal zone lymphoma
- Notch-1/3
Notch receptor 1 and 3
- NuMA
Nuclear Mitotic Apparatus
- NUP214-ABL1
Nucleoporin Nup214-ABL1
- p21CIP1/WAF1
CDKN1A/cyclin Dependent Kinase Inhibitor 1A
- p27KIP1
CDKN1B/cyclin Dependent Kinase Inhibitor 1B
- p70S6K
Ribosomal protein S6 kinase beta-1
- p100
Nuclear Factor Kappa B Subunit 2
- Pal-1/Gfi-1
Growth Factor Independent 1 Transcriptional Repressor
- Pax-5
Paired Box 5
- PBMCs
Peripheral blood mononuclear cells
- PCNSL
Primary central nervous system lymphoma
- PI3K
PI3-kinase
- Pim
Provirus Integration site for Moloney leukemia virus
- PMLBCL
Primary mediastinal large B-cell lymphoma
- PRAS40
AKT1 Substrate 1
- PTCL
Peripheral T-cell lymphoma
- PTPN2
Protein tyrosine phosphatase non-receptor type 2
- PV
Polycythemia vera
- RARα
Retinoic acid receptor alpha
- RhoH
Ras homolog family member H
- Runx2
RUNX Family Transcription Factor 2
- SAHA
Suberoylanilide hydroxamic acid
- SHA
Somatic hypermutation activity
- SLL
Small lymphocytic lymphoma
- SOCS-1/3
Suppressor of Cytokine Signaling 1/3
- STAT
Signal transducer and activator of transcription
- TCRβ-PIM1
T-cell receptor beta locus/PIM1
- TEL/AML1
Transcription Factor ETV6/RUNX Family Transcription Factor 1
- TEL/TRKC
TEL/tyrosine kinase receptor C
- TFF
Trefoil Factor
- TSC2
TSC Complex Subunit 2
- UTR
Untranslated region
- WHO
World Health Organization
Authors’ contributions
MB wrote the manuscript and made figures. CN analyzed the manuscript. The author(s) read and approved the final manuscript.
Funding
This work was supported by grant R01CA201309 to Christophe Nicot.
Declarations
Ethics approval and consent to participate
Not Applicable.
Consent for publication
Not applicable.
Competing interests
Authors declare no financial conflict of interest. Dr. Nicot is an editorial board member of Molecular Cancer.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Cuypers HT, Selten G, Quint W, Zijlstra M, Maandag ER, Boelens W, van Wezenbeek P, Melief C, Berns A. Murine leukemia virus-induced T-cell lymphomagenesis: integration of proviruses in a distinct chromosomal region. Cell. 1984;37(1):141–150. doi: 10.1016/0092-8674(84)90309-X. [DOI] [PubMed] [Google Scholar]
- 2.Selten G, Cuypers HT, Boelens W, Robanus-Maandag E, Verbeek J, Domen J, van Beveren C, Berns A. The primary structure of the putative oncogene pim-1 shows extensive homology with protein kinases. Cell. 1986;46(4):603–611. doi: 10.1016/0092-8674(86)90886-X. [DOI] [PubMed] [Google Scholar]
- 3.van der Lugt NM, Domen J, Verhoeven E, Linders K, van der Gulden H, Allen J, Berns A. Proviral tagging in E mu-myc transgenic mice lacking the Pim-1 proto-oncogene leads to compensatory activation of Pim-2. EMBO J. 1995;14(11):2536–2544. doi: 10.1002/j.1460-2075.1995.tb07251.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Feldman JD, Vician L, Crispino M, Tocco G, Marcheselli VL, Bazan NG, Baudry M, Herschman HR. KID-1, a protein kinase induced by depolarization in brain. J Biol Chem. 1998;273(26):16535–16543. doi: 10.1074/jbc.273.26.16535. [DOI] [PubMed] [Google Scholar]
- 5.Hoover D, Friedmann M, Reeves R, Magnuson NS. Recombinant human pim-1 protein exhibits serine/threonine kinase activity. J Biol Chem. 1991;266(21):14018–14023. doi: 10.1016/S0021-9258(18)92804-8. [DOI] [PubMed] [Google Scholar]
- 6.Palaty CK, Clark-Lewis I, Leung D, Pelech SL. Phosphorylation site substrate specificity determinants for the Pim-1 protooncogene-encoded protein kinase. Biochem Cell Biol. 1997;75(2):153–162. doi: 10.1139/o97-026. [DOI] [PubMed] [Google Scholar]
- 7.Mikkers H, Nawijn M, Allen J, Brouwers C, Verhoeven E, Jonkers J, Berns A. Mice deficient for all PIM kinases display reduced body size and impaired responses to hematopoietic growth factors. Mol Cell Biol. 2004;24(13):6104–6115. doi: 10.1128/MCB.24.13.6104-6115.2004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.An N, Kraft AS, Kang Y. Abnormal hematopoietic phenotypes in Pim kinase triple knockout mice. J Hematol Oncol. 2013;6:12. doi: 10.1186/1756-8722-6-12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Toth RK, Warfel NA. Targeting PIM kinases to overcome therapeutic resistance in cancer. Mol Cancer Ther. 2021;20(1):3–10. doi: 10.1158/1535-7163.MCT-20-0535. [DOI] [PubMed] [Google Scholar]
- 10.Mondello P, Cuzzocrea S, Mian M. Pim kinases in hematological malignancies: where are we now and where are we going? J Hematol Oncol. 2014;7:95. doi: 10.1186/s13045-014-0095-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Bagger FO, Sasivarevic D, Sohi SH, Laursen LG, Pundhir S, Sonderby CK, Winther O, Rapin N, Porse BT. BloodSpot: a database of gene expression profiles and transcriptional programs for healthy and malignant haematopoiesis. Nucleic Acids Res. 2016;44(D1):D917–D924. doi: 10.1093/nar/gkv1101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Bagger FO, Kinalis S, Rapin N. BloodSpot: a database of healthy and malignant haematopoiesis updated with purified and single cell mRNA sequencing profiles. Nucleic Acids Res. 2019;47(D1):D881–D885. doi: 10.1093/nar/gky1076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Amson R, Sigaux F, Przedborski S, Flandrin G, Givol D, Telerman A. The human protooncogene product p33pim is expressed during fetal hematopoiesis and in diverse leukemias. Proc Natl Acad Sci U S A. 1989;86(22):8857–8861. doi: 10.1073/pnas.86.22.8857. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Eichmann A, Yuan L, Breant C, Alitalo K, Koskinen PJ. Developmental expression of pim kinases suggests functions also outside of the hematopoietic system. Oncogene. 2000;19(9):1215–1224. doi: 10.1038/sj.onc.1203355. [DOI] [PubMed] [Google Scholar]
- 15.Santio NM, Koskinen PJ. PIM kinases: from survival factors to regulators of cell motility. Int J Biochem Cell Biol. 2017;93:74–85. doi: 10.1016/j.biocel.2017.10.016. [DOI] [PubMed] [Google Scholar]
- 16.van Lohuizen M, Verbeek S, Krimpenfort P, Domen J, Saris C, Radaszkiewicz T, Berns A. Predisposition to lymphomagenesis in pim-1 transgenic mice: cooperation with c-myc and N-myc in murine leukemia virus-induced tumors. Cell. 1989;56(4):673–682. doi: 10.1016/0092-8674(89)90589-8. [DOI] [PubMed] [Google Scholar]
- 17.Liu Z, Han M, Ding K, Fu R. The role of Pim kinase in immunomodulation. Am J Cancer Res. 2020;10(12):4085–4097. [PMC free article] [PubMed] [Google Scholar]
- 18.Aguirre E, Renner O, Narlik-Grassow M, Blanco-Aparicio C. Genetic modeling of PIM proteins in cancer: proviral tagging and cooperation with oncogenes, tumor suppressor genes, and carcinogens. Front Oncol. 2014;4:109. doi: 10.3389/fonc.2014.00109. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Breuer M, Slebos R, Verbeek S, van Lohuizen M, Wientjens E, Berns A. Very high frequency of lymphoma induction by a chemical carcinogen in pim-1 transgenic mice. Nature. 1989;340(6228):61–63. doi: 10.1038/340061a0. [DOI] [PubMed] [Google Scholar]
- 20.van der Houven van Oordt CW, Schouten TG, van Krieken JH, van Dierendonck JH, van der Eb AJ, Breuer ML. X-ray-induced lymphomagenesis in E mu-pim-1 transgenic mice: an investigation of the co-operating molecular events. Carcinogenesis. 1998;19(5):847–853. doi: 10.1093/carcin/19.5.847. [DOI] [PubMed] [Google Scholar]
- 21.Delgado MD, Leon J. Myc roles in hematopoiesis and leukemia. Genes Cancer. 2010;1(6):605–616. doi: 10.1177/1947601910377495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Verbeek S, van Lohuizen M, van der Valk M, Domen J, Kraal G, Berns A. Mice bearing the E mu-myc and E mu-pim-1 transgenes develop pre-B-cell leukemia prenatally. Mol Cell Biol. 1991;11(2):1176–1179. doi: 10.1128/mcb.11.2.1176. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Allen JD, Verhoeven E, Domen J, van der Valk M, Berns A. Pim-2 transgene induces lymphoid tumors, exhibiting potent synergy with c-myc. Oncogene. 1997;15(10):1133–1141. doi: 10.1038/sj.onc.1201288. [DOI] [PubMed] [Google Scholar]
- 24.Forshell LP, Li Y, Forshell TZ, Rudelius M, Nilsson L, Keller U, Nilsson J. The direct Myc target Pim3 cooperates with other Pim kinases in supporting viability of Myc-induced B-cell lymphomas. Oncotarget. 2011;2(6):448–460. doi: 10.18632/oncotarget.283. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Mikkers H, Allen J, Knipscheer P, Romeijn L, Hart A, Vink E, Berns A. High-throughput retroviral tagging to identify components of specific signaling pathways in cancer. Nat Genet. 2002;32(1):153–159. doi: 10.1038/ng950. [DOI] [PubMed] [Google Scholar]
- 26.Scheijen B, Jonkers J, Acton D, Berns A. Characterization of pal-1, a common proviral insertion site in murine leukemia virus-induced lymphomas of c-myc and Pim-1 transgenic mice. J Virol. 1997;71(1):9–16. doi: 10.1128/jvi.71.1.9-16.1997. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Blyth K, Terry A, Mackay N, Vaillant F, Bell M, Cameron ER, Neil JC, Stewart M. Runx2: a novel oncogenic effector revealed by in vivo complementation and retroviral tagging. Oncogene. 2001;20(3):295–302. doi: 10.1038/sj.onc.1204090. [DOI] [PubMed] [Google Scholar]
- 28.Consortium ITP-CAoWG Pan-cancer analysis of whole genomes. Nature. 2020;578(7793):82–93. doi: 10.1038/s41586-020-1969-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Cerami E, Gao J, Dogrusoz U, Gross BE, Sumer SO, Aksoy BA, Jacobsen A, Byrne CJ, Heuer ML, Larsson E, et al. The cBio cancer genomics portal: an open platform for exploring multidimensional cancer genomics data. Cancer Discov. 2012;2(5):401–404. doi: 10.1158/2159-8290.CD-12-0095. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Gao J, Aksoy BA, Dogrusoz U, Dresdner G, Gross B, Sumer SO, Sun Y, Jacobsen A, Sinha R, Larsson E, et al. Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci Signal. 2013;6(269):pl1. doi: 10.1126/scisignal.2004088. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Xie Y, Xu K, Linn DE, Yang X, Guo Z, Shimelis H, Nakanishi T, Ross DD, Chen H, Fazli L, et al. The 44-kDa Pim-1 kinase phosphorylates BCRP/ABCG2 and thereby promotes its multimerization and drug-resistant activity in human prostate cancer cells. J Biol Chem. 2008;283(6):3349–3356. doi: 10.1074/jbc.M707773200. [DOI] [PubMed] [Google Scholar]
- 32.Natarajan K, Bhullar J, Shukla S, Burcu M, Chen ZS, Ambudkar SV, Baer MR. The Pim kinase inhibitor SGI-1776 decreases cell surface expression of P-glycoprotein (ABCB1) and breast cancer resistance protein (ABCG2) and drug transport by Pim-1-dependent and -independent mechanisms. Biochem Pharmacol. 2013;85(4):514–524. doi: 10.1016/j.bcp.2012.12.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Xie Y, Burcu M, Linn DE, Qiu Y, Baer MR. Pim-1 kinase protects P-glycoprotein from degradation and enables its glycosylation and cell surface expression. Mol Pharmacol. 2010;78(2):310–318. doi: 10.1124/mol.109.061713. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Olejniczak SH, La Rocca G, Radler MR, Egan SM, Xiang Q, Garippa R, Thompson CB. Coordinated regulation of cap-dependent translation and microRNA function by convergent signaling pathways. Mol Cell Biol. 2016;36(18):2360–2373. doi: 10.1128/MCB.01011-15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Beharry Z, Mahajan S, Zemskova M, Lin YW, Tholanikunnel BG, Xia Z, Smith CD, Kraft AS. The Pim protein kinases regulate energy metabolism and cell growth. Proc Natl Acad Sci U S A. 2011;108(2):528–533. doi: 10.1073/pnas.1013214108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Nihira K, Ando Y, Yamaguchi T, Kagami Y, Miki Y, Yoshida K. Pim-1 controls NF-kappaB signalling by stabilizing RelA/p65. Cell Death Differ. 2010;17(4):689–698. doi: 10.1038/cdd.2009.174. [DOI] [PubMed] [Google Scholar]
- 37.Hammerman PS, Fox CJ, Cinalli RM, Xu A, Wagner JD, Lindsten T, Thompson CB. Lymphocyte transformation by Pim-2 is dependent on nuclear factor-kappaB activation. Cancer Res. 2004;64(22):8341–8348. doi: 10.1158/0008-5472.CAN-04-2284. [DOI] [PubMed] [Google Scholar]
- 38.Zhang Y, Wang Z, Li X, Magnuson NS. Pim kinase-dependent inhibition of c-Myc degradation. Oncogene. 2008;27(35):4809–4819. doi: 10.1038/onc.2008.123. [DOI] [PubMed] [Google Scholar]
- 39.Zippo A, De Robertis A, Serafini R, Oliviero S. PIM1-dependent phosphorylation of histone H3 at serine 10 is required for MYC-dependent transcriptional activation and oncogenic transformation. Nat Cell Biol. 2007;9(8):932–944. doi: 10.1038/ncb1618. [DOI] [PubMed] [Google Scholar]
- 40.Winn LM, Lei W, Ness SA. Pim-1 phosphorylates the DNA binding domain of c-Myb. Cell Cycle. 2003;2(3):258–262. doi: 10.4161/cc.2.3.383. [DOI] [PubMed] [Google Scholar]
- 41.Cogswell JP, Cogswell PC, Kuehl WM, Cuddihy AM, Bender TM, Engelke U, Marcu KB, Ting JP. Mechanism of c-myc regulation by c-Myb in different cell lineages. Mol Cell Biol. 1993;13(5):2858–2869. doi: 10.1128/mcb.13.5.2858. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Leverson JD, Koskinen PJ, Orrico FC, Rainio EM, Jalkanen KJ, Dash AB, Eisenman RN, Ness SA. Pim-1 kinase and p100 cooperate to enhance c-Myb activity. Mol Cell. 1998;2(4):417–425. doi: 10.1016/S1097-2765(00)80141-0. [DOI] [PubMed] [Google Scholar]
- 43.Aho TL, Sandholm J, Peltola KJ, Ito Y, Koskinen PJ. Pim-1 kinase phosphorylates RUNX family transcription factors and enhances their activity. BMC Cell Biol. 2006;7:21. doi: 10.1186/1471-2121-7-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Choi A, Illendula A, Pulikkan JA, Roderick JE, Tesell J, Yu J, Hermance N, Zhu LJ, Castilla LH, Bushweller JH, et al. RUNX1 is required for oncogenic Myb and Myc enhancer activity in T-cell acute lymphoblastic leukemia. Blood. 2017;130(15):1722–1733. doi: 10.1182/blood-2017-03-775536. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Santio NM, Landor SK, Vahtera L, Yla-Pelto J, Paloniemi E, Imanishi SY, Corthals G, Varjosalo M, Manoharan GB, Uri A, et al. Phosphorylation of Notch1 by Pim kinases promotes oncogenic signaling in breast and prostate cancer cells. Oncotarget. 2016;7(28):43220–43238. doi: 10.18632/oncotarget.9215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Wang Z, Zhang Y, Gu JJ, Davitt C, Reeves R, Magnuson NS. Pim-2 phosphorylation of p21(Cip1/WAF1) enhances its stability and inhibits cell proliferation in HCT116 cells. Int J Biochem Cell Biol. 2010;42(6):1030–1038. doi: 10.1016/j.biocel.2010.03.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Zhang Y, Wang Z, Magnuson NS. Pim-1 kinase-dependent phosphorylation of p21Cip1/WAF1 regulates its stability and cellular localization in H1299 cells. Mol Cancer Res. 2007;5(9):909–922. doi: 10.1158/1541-7786.MCR-06-0388. [DOI] [PubMed] [Google Scholar]
- 48.Morishita D, Katayama R, Sekimizu K, Tsuruo T, Fujita N. Pim kinases promote cell cycle progression by phosphorylating and down-regulating p27Kip1 at the transcriptional and posttranscriptional levels. Cancer Res. 2008;68(13):5076–5085. doi: 10.1158/0008-5472.CAN-08-0634. [DOI] [PubMed] [Google Scholar]
- 49.Bachmann M, Hennemann H, Xing PX, Hoffmann I, Moroy T. The oncogenic serine/threonine kinase Pim-1 phosphorylates and inhibits the activity of Cdc25C-associated kinase 1 (C-TAK1): a novel role for Pim-1 at the G2/M cell cycle checkpoint. J Biol Chem. 2004;279(46):48319–48328. doi: 10.1074/jbc.M404440200. [DOI] [PubMed] [Google Scholar]
- 50.Bachmann M, Kosan C, Xing PX, Montenarh M, Hoffmann I, Moroy T. The oncogenic serine/threonine kinase Pim-1 directly phosphorylates and activates the G2/M specific phosphatase Cdc25C. Int J Biochem Cell Biol. 2006;38(3):430–443. doi: 10.1016/j.biocel.2005.10.010. [DOI] [PubMed] [Google Scholar]
- 51.Mochizuki T, Kitanaka C, Noguchi K, Muramatsu T, Asai A, Kuchino Y. Physical and functional interactions between Pim-1 kinase and Cdc25A phosphatase. Implications for the Pim-1-mediated activation of the c-Myc signaling pathway. J Biol Chem. 1999;274(26):18659–18666. doi: 10.1074/jbc.274.26.18659. [DOI] [PubMed] [Google Scholar]
- 52.Bhattacharya N, Wang Z, Davitt C, McKenzie IF, Xing PX, Magnuson NS. Pim-1 associates with protein complexes necessary for mitosis. Chromosoma. 2002;111(2):80–95. doi: 10.1007/s00412-002-0192-6. [DOI] [PubMed] [Google Scholar]
- 53.Koike N, Maita H, Taira T, Ariga H, Iguchi-Ariga SM. Identification of heterochromatin protein 1 (HP1) as a phosphorylation target by Pim-1 kinase and the effect of phosphorylation on the transcriptional repression function of HP1(1) FEBS Lett. 2000;467(1):17–21. doi: 10.1016/S0014-5793(00)01105-4. [DOI] [PubMed] [Google Scholar]
- 54.Lu J, Zavorotinskaya T, Dai Y, Niu XH, Castillo J, Sim J, Yu J, Wang Y, Langowski JL, Holash J, et al. Pim2 is required for maintaining multiple myeloma cell growth through modulating TSC2 phosphorylation. Blood. 2013;122(9):1610–1620. doi: 10.1182/blood-2013-01-481457. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Tamburini J, Green AS, Bardet V, Chapuis N, Park S, Willems L, Uzunov M, Ifrah N, Dreyfus F, Lacombe C, et al. Protein synthesis is resistant to rapamycin and constitutes a promising therapeutic target in acute myeloid leukemia. Blood. 2009;114(8):1618–1627. doi: 10.1182/blood-2008-10-184515. [DOI] [PubMed] [Google Scholar]
- 56.Zhang F, Beharry ZM, Harris TE, Lilly MB, Smith CD, Mahajan S, Kraft AS. PIM1 protein kinase regulates PRAS40 phosphorylation and mTOR activity in FDCP1 cells. Cancer Biol Ther. 2009;8(9):846–853. doi: 10.4161/cbt.8.9.8210. [DOI] [PubMed] [Google Scholar]
- 57.Yang J, Wang J, Chen K, Guo G, Xi R, Rothman PB, Whitten D, Zhang L, Huang S, Chen JL. eIF4B phosphorylation by pim kinases plays a critical role in cellular transformation by Abl oncogenes. Cancer Res. 2013;73(15):4898–4908. doi: 10.1158/0008-5472.CAN-12-4277. [DOI] [PubMed] [Google Scholar]
- 58.Mung KL, Eccleshall WB, Santio NM, Rivero-Muller A, Koskinen PJ. PIM kinases inhibit AMPK activation and promote tumorigenicity by phosphorylating LKB1. Cell Commun Signal. 2021;19(1):68. doi: 10.1186/s12964-021-00749-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Macdonald A, Campbell DG, Toth R, McLauchlan H, Hastie CJ, Arthur JS. Pim kinases phosphorylate multiple sites on Bad and promote 14-3-3 binding and dissociation from Bcl-XL. BMC Cell Biol. 2006;7:1. doi: 10.1186/1471-2121-7-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Xu Y, Xing Y, Xu Y, Huang C, Bao H, Hong K, Cheng X. Pim-2 protects H9c2 cardiomyocytes from hypoxia/reoxygenation-induced apoptosis via downregulation of Bim expression. Environ Toxicol Pharmacol. 2016;48:94–102. doi: 10.1016/j.etap.2016.10.011. [DOI] [PubMed] [Google Scholar]
- 61.Gu JJ, Wang Z, Reeves R, Magnuson NS. PIM1 phosphorylates and negatively regulates ASK1-mediated apoptosis. Oncogene. 2009;28(48):4261–4271. doi: 10.1038/onc.2009.276. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Ionov Y, Le X, Tunquist BJ, Sweetenham J, Sachs T, Ryder J, Johnson T, Lilly MB, Kraft AS. Pim-1 protein kinase is nuclear in Burkitt's lymphoma: nuclear localization is necessary for its biologic effects. Anticancer Res. 2003;23(1A):167–178. [PubMed] [Google Scholar]
- 63.Hogan C, Hutchison C, Marcar L, Milne D, Saville M, Goodlad J, Kernohan N, Meek D. Elevated levels of oncogenic protein kinase Pim-1 induce the p53 pathway in cultured cells and correlate with increased Mdm2 in mantle cell lymphoma. J Biol Chem. 2008;283(26):18012–18023. doi: 10.1074/jbc.M709695200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Ha S, Iqbal NJ, Mita P, Ruoff R, Gerald WL, Lepor H, Taneja SS, Lee P, Melamed J, Garabedian MJ, et al. Phosphorylation of the androgen receptor by PIM1 in hormone refractory prostate cancer. Oncogene. 2013;32(34):3992–4000. doi: 10.1038/onc.2012.412. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Ruff SE, Vasilyev N, Nudler E, Logan SK, Garabedian MJ. PIM1 phosphorylation of the androgen receptor and 14-3-3 zeta regulates gene transcription in prostate cancer. Commun Biol. 2021;4(1):1221. doi: 10.1038/s42003-021-02723-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Padmanabhan A, Gosc EB, Bieberich CJ. Stabilization of the prostate-specific tumor suppressor NKX3.1 by the oncogenic protein kinase Pim-1 in prostate cancer cells. J Cell Biochem. 2013;114(5):1050–1057. doi: 10.1002/jcb.24444. [DOI] [PubMed] [Google Scholar]
- 67.Eerola SK, Santio NM, Rinne S, Kouvonen P, Corthals GL, Scaravilli M, Scala G, Serra A, Greco D, Ruusuvuori P, et al. Phosphorylation of NFATC1 at PIM1 target sites is essential for its ability to promote prostate cancer cell migration and invasion. Cell Commun Signal. 2019;17(1):148. doi: 10.1186/s12964-019-0463-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Chen XP, Losman JA, Cowan S, Donahue E, Fay S, Vuong BQ, Nawijn MC, Capece D, Cohan VL, Rothman P. Pim serine/threonine kinases regulate the stability of Socs-1 protein. Proc Natl Acad Sci U S A. 2002;99(4):2175–2180. doi: 10.1073/pnas.042035699. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Peltola KJ, Paukku K, Aho TL, Ruuska M, Silvennoinen O, Koskinen PJ. Pim-1 kinase inhibits STAT5-dependent transcription via its interactions with SOCS1 and SOCS3. Blood. 2004;103(10):3744–3750. doi: 10.1182/blood-2003-09-3126. [DOI] [PubMed] [Google Scholar]
- 70.Natarajan K, Xie Y, Burcu M, Linn DE, Qiu Y, Baer MR. Pim-1 kinase phosphorylates and stabilizes 130 kDa FLT3 and promotes aberrant STAT5 signaling in acute myeloid leukemia with FLT3 internal tandem duplication. PLoS One. 2013;8(9):e74653. doi: 10.1371/journal.pone.0074653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Grundler R, Brault L, Gasser C, Bullock AN, Dechow T, Woetzel S, Pogacic V, Villa A, Ehret S, Berridge G, et al. Dissection of PIM serine/threonine kinases in FLT3-ITD-induced leukemogenesis reveals PIM1 as regulator of CXCL12-CXCR4-mediated homing and migration. J Exp Med. 2009;206(9):1957–1970. doi: 10.1084/jem.20082074. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Santio NM, Eerola SK, Paatero I, Yli-Kauhaluoma J, Anizon F, Moreau P, Tuomela J, Harkonen P, Koskinen PJ. Pim kinases promote migration and metastatic growth of prostate cancer xenografts. PLoS One. 2015;10(6):e0130340. doi: 10.1371/journal.pone.0130340. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Singh N, Padi SKR, Bearss JJ, Pandey R, Okumura K, Beltran H, Song JH, Kraft AS, Olive V. PIM protein kinases regulate the level of the long noncoding RNA H19 to control stem cell gene transcription and modulate tumor growth. Mol Oncol. 2020;14(5):974–990. doi: 10.1002/1878-0261.12662. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Haferlach T, Kohlmann A, Wieczorek L, Basso G, Kronnie GT, Bene MC, De Vos J, Hernandez JM, Hofmann WK, Mills KI, et al. Clinical utility of microarray-based gene expression profiling in the diagnosis and subclassification of leukemia: report from the International Microarray Innovations in Leukemia Study Group. J Clin Oncol. 2010;28(15):2529–2537. doi: 10.1200/JCO.2009.23.4732. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Labaj W, Papiez A, Polanski A, Polanska J. Comprehensive analysis of MILE gene expression data set advances discovery of leukaemia type and subtype biomarkers. Interdiscip Sci. 2017;9(1):24–35. doi: 10.1007/s12539-017-0216-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Daver N, Schlenk RF, Russell NH, Levis MJ. Targeting FLT3 mutations in AML: review of current knowledge and evidence. Leukemia. 2019;33(2):299–312. doi: 10.1038/s41375-018-0357-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Cancer Genome Atlas Research N. Ley TJ, Miller C, Ding L, Raphael BJ, Mungall AJ, Robertson A, Hoadley K, Triche TJ, Jr, Laird PW, et al. Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. N Engl J Med. 2013;368(22):2059–2074. doi: 10.1056/NEJMoa1301689. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Tyner JW, Tognon CE, Bottomly D, Wilmot B, Kurtz SE, Savage SL, Long N, Schultz AR, Traer E, Abel M, et al. Functional genomic landscape of acute myeloid leukaemia. Nature. 2018;562(7728):526–531. doi: 10.1038/s41586-018-0623-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Agrawal S, Koschmieder S, Baumer N, Reddy NG, Berdel WE, Muller-Tidow C, Serve H. Pim2 complements Flt3 wild-type receptor in hematopoietic progenitor cell transformation. Leukemia. 2008;22(1):78–86. doi: 10.1038/sj.leu.2404988. [DOI] [PubMed] [Google Scholar]
- 80.Cheng H, Huang C, Xu X, Hu X, Gong S, Tang G, Song X, Zhang W, Wang J, Chen L, et al. PIM-1 mRNA expression is a potential prognostic biomarker in acute myeloid leukemia. J Transl Med. 2017;15(1):179. doi: 10.1186/s12967-017-1287-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Kapelko-Slowik K, Urbaniak-Kujda D, Wolowiec D, Jazwiec B, Dybko J, Jakubaszko J, Slowik M, Kuliczkowski K. Expression of PIM-2 and NF-kappaB genes is increased in patients with acute myeloid leukemia (AML) and acute lymphoblastic leukemia (ALL) and is associated with complete remission rate and overall survival. Postepy Hig Med Dosw (Online) 2013;67:553–559. doi: 10.5604/17322693.1052449. [DOI] [PubMed] [Google Scholar]
- 82.Luo H, Sun R, Zheng Y, Huang J, Wang F, Long D, Wu Y. PIM3 promotes the proliferation and migration of acute myeloid leukemia cells. Onco Targets Ther. 2020;13:6897–6905. doi: 10.2147/OTT.S245578. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Kim KT, Baird K, Ahn JY, Meltzer P, Lilly M, Levis M, Small D. Pim-1 is up-regulated by constitutively activated FLT3 and plays a role in FLT3-mediated cell survival. Blood. 2005;105(4):1759–1767. doi: 10.1182/blood-2004-05-2006. [DOI] [PubMed] [Google Scholar]
- 84.Hu YL, Passegue E, Fong S, Largman C, Lawrence HJ. Evidence that the Pim1 kinase gene is a direct target of HOXA9. Blood. 2007;109(11):4732–4738. doi: 10.1182/blood-2006-08-043356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Lohr JG, Stojanov P, Carter SL, Cruz-Gordillo P, Lawrence MS, Auclair D, Sougnez C, Knoechel B, Gould J, Saksena G, et al. Widespread genetic heterogeneity in multiple myeloma: implications for targeted therapy. Cancer Cell. 2014;25(1):91–101. doi: 10.1016/j.ccr.2013.12.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Kelly LM, Kutok JL, Williams IR, Boulton CL, Amaral SM, Curley DP, Ley TJ, Gilliland DG. PML/RARalpha and FLT3-ITD induce an APL-like disease in a mouse model. Proc Natl Acad Sci U S A. 2002;99(12):8283–8288. doi: 10.1073/pnas.122233699. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Agrawal-Singh S, Koschmieder S, Gelsing S, Stocking C, Stehling M, Thiede C, Thoennissen NH, Kohler G, Valk PJ, Delwel R, et al. Pim2 cooperates with PML-RARalpha to induce acute myeloid leukemia in a bone marrow transplantation model. Blood. 2010;115(22):4507–4516. doi: 10.1182/blood-2009-03-210070. [DOI] [PubMed] [Google Scholar]
- 88.Pogacic V, Bullock AN, Fedorov O, Filippakopoulos P, Gasser C, Biondi A, Meyer-Monard S, Knapp S, Schwaller J. Structural analysis identifies imidazo[1,2-b]pyridazines as PIM kinase inhibitors with in vitro antileukemic activity. Cancer Res. 2007;67(14):6916–6924. doi: 10.1158/0008-5472.CAN-07-0320. [DOI] [PubMed] [Google Scholar]
- 89.Chen LS, Redkar S, Taverna P, Cortes JE, Gandhi V. Mechanisms of cytotoxicity to Pim kinase inhibitor, SGI-1776, in acute myeloid leukemia. Blood. 2011;118(3):693–702. doi: 10.1182/blood-2010-12-323022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Yang Q, Chen LS, Neelapu SS, Miranda RN, Medeiros LJ, Gandhi V. Transcription and translation are primary targets of Pim kinase inhibitor SGI-1776 in mantle cell lymphoma. Blood. 2012;120(17):3491–3500. doi: 10.1182/blood-2012-02-412643. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Keeton EK, McEachern K, Dillman KS, Palakurthi S, Cao Y, Grondine MR, Kaur S, Wang S, Chen Y, Wu A, et al. AZD1208, a potent and selective pan-Pim kinase inhibitor, demonstrates efficacy in preclinical models of acute myeloid leukemia. Blood. 2014;123(6):905–913. doi: 10.1182/blood-2013-04-495366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Puente XS, Bea S, Valdes-Mas R, Villamor N, Gutierrez-Abril J, Martin-Subero JI, Munar M, Rubio-Perez C, Jares P, Aymerich M, et al. Non-coding recurrent mutations in chronic lymphocytic leukaemia. Nature. 2015;526(7574):519–524. doi: 10.1038/nature14666. [DOI] [PubMed] [Google Scholar]
- 93.Quesada V, Conde L, Villamor N, Ordonez GR, Jares P, Bassaganyas L, Ramsay AJ, Bea S, Pinyol M, Martinez-Trillos A, et al. Exome sequencing identifies recurrent mutations of the splicing factor SF3B1 gene in chronic lymphocytic leukemia. Nat Genet. 2011;44(1):47–52. doi: 10.1038/ng.1032. [DOI] [PubMed] [Google Scholar]
- 94.Chapuy B, Stewart C, Dunford AJ, Kim J, Kamburov A, Redd RA, Lawrence MS, Roemer MGM, Li AJ, Ziepert M, et al. Molecular subtypes of diffuse large B cell lymphoma are associated with distinct pathogenic mechanisms and outcomes. Nat Med. 2018;24(5):679–690. doi: 10.1038/s41591-018-0016-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Morin RD, Mungall K, Pleasance E, Mungall AJ, Goya R, Huff RD, Scott DW, Ding J, Roth A, Chiu R, et al. Mutational and structural analysis of diffuse large B-cell lymphoma using whole-genome sequencing. Blood. 2013;122(7):1256–1265. doi: 10.1182/blood-2013-02-483727. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Lohr JG, Stojanov P, Lawrence MS, Auclair D, Chapuy B, Sougnez C, Cruz-Gordillo P, Knoechel B, Asmann YW, Slager SL, et al. Discovery and prioritization of somatic mutations in diffuse large B-cell lymphoma (DLBCL) by whole-exome sequencing. Proc Natl Acad Sci U S A. 2012;109(10):3879–3884. doi: 10.1073/pnas.1121343109. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Reddy A, Zhang J, Davis NS, Moffitt AB, Love CL, Waldrop A, Leppa S, Pasanen A, Meriranta L, Karjalainen-Lindsberg ML, et al. Genetic and functional drivers of diffuse large B cell lymphoma. Cell. 2017;171(2):481–494.e415. doi: 10.1016/j.cell.2017.09.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98.Hoadley KA, Yau C, Hinoue T, Wolf DM, Lazar AJ, Drill E, Shen R, Taylor AM, Cherniack AD, Thorsson V, et al. Cell-of-origin patterns dominate the molecular classification of 10,000 tumors from 33 types of cancer. Cell. 2018;173(2):291–304.e296. doi: 10.1016/j.cell.2018.03.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.da Silva Almeida AC, Abate F, Khiabanian H, Martinez-Escala E, Guitart J, Tensen CP, Vermeer MH, Rabadan R, Ferrando A, Palomero T. The mutational landscape of cutaneous T cell lymphoma and Sezary syndrome. Nat Genet. 2015;47(12):1465–1470. doi: 10.1038/ng.3442. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Bea S, Valdes-Mas R, Navarro A, Salaverria I, Martin-Garcia D, Jares P, Gine E, Pinyol M, Royo C, Nadeu F, et al. Landscape of somatic mutations and clonal evolution in mantle cell lymphoma. Proc Natl Acad Sci U S A. 2013;110(45):18250–18255. doi: 10.1073/pnas.1314608110. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Ma MCJ, Tadros S, Bouska A, Heavican T, Yang H, Deng Q, Moore D, Akhter A, Hartert K, Jain N, et al. Subtype-specific and co-occurring genetic alterations in B-cell non-Hodgkin lymphoma. Haematologica. 2022;107(3):690–701. doi: 10.3324/haematol.2020.274258. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.Rossi D, Berra E, Cerri M, Deambrogi C, Barbieri C, Franceschetti S, Lunghi M, Conconi A, Paulli M, Matolcsy A, et al. Aberrant somatic hypermutation in transformation of follicular lymphoma and chronic lymphocytic leukemia to diffuse large B-cell lymphoma. Haematologica. 2006;91(10):1405–1409. [PubMed] [Google Scholar]
- 103.Zhang J, McCastlain K, Yoshihara H, Xu B, Chang Y, Churchman ML, Wu G, Li Y, Wei L, Iacobucci I, et al. Deregulation of DUX4 and ERG in acute lymphoblastic leukemia. Nat Genet. 2016;48(12):1481–1489. doi: 10.1038/ng.3691. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Andersson AK, Ma J, Wang J, Chen X, Gedman AL, Dang J, Nakitandwe J, Holmfeldt L, Parker M, Easton J, et al. The landscape of somatic mutations in infant MLL-rearranged acute lymphoblastic leukemias. Nat Genet. 2015;47(4):330–337. doi: 10.1038/ng.3230. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Rossi D, Cerri M, Capello D, Deambrogi C, Berra E, Franceschetti S, Alabiso O, Gloghini A, Paulli M, Carbone A, et al. Aberrant somatic hypermutation in primary mediastinal large B-cell lymphoma. Leukemia. 2005;19(12):2363–2366. doi: 10.1038/sj.leu.2403982. [DOI] [PubMed] [Google Scholar]
- 106.Liso A, Capello D, Marafioti T, Tiacci E, Cerri M, Distler V, Paulli M, Carbone A, Delsol G, Campo E, et al. Aberrant somatic hypermutation in tumor cells of nodular-lymphocyte-predominant and classic Hodgkin lymphoma. Blood. 2006;108(3):1013–1020. doi: 10.1182/blood-2005-10-3949. [DOI] [PubMed] [Google Scholar]
- 107.Pasqualucci L, Neumeister P, Goossens T, Nanjangud G, Chaganti RS, Kuppers R, Dalla-Favera R. Hypermutation of multiple proto-oncogenes in B-cell diffuse large-cell lymphomas. Nature. 2001;412(6844):341–346. doi: 10.1038/35085588. [DOI] [PubMed] [Google Scholar]
- 108.Libra M, Capello D, Gloghini A, Laura P, Berra E, Cerri M, Gasparotto D, Franca S, De Re V, Gaidano G, et al. Analysis of aberrant somatic hypermutation (SHM) in non-Hodgkin’s lymphomas of patients with chronic HCV infection. J Pathol. 2005;206(1):87–91. doi: 10.1002/path.1754. [DOI] [PubMed] [Google Scholar]
- 109.Paino T, Garcia-Gomez A, Gonzalez-Mendez L, San-Segundo L, Hernandez-Garcia S, Lopez-Iglesias AA, Algarin EM, Martin-Sanchez M, Corbacho D, Ortiz-de-Solorzano C, et al. The novel Pan-PIM kinase inhibitor, PIM447, displays dual antimyeloma and bone-protective effects, and potently synergizes with current standards of care. Clin Cancer Res. 2017;23(1):225–238. doi: 10.1158/1078-0432.CCR-16-0230. [DOI] [PubMed] [Google Scholar]
- 110.Asano J, Nakano A, Oda A, Amou H, Hiasa M, Takeuchi K, Miki H, Nakamura S, Harada T, Fujii S, et al. The serine/threonine kinase Pim-2 is a novel anti-apoptotic mediator in myeloma cells. Leukemia. 2011;25(7):1182–1188. doi: 10.1038/leu.2011.60. [DOI] [PubMed] [Google Scholar]
- 111.Hiasa M, Teramachi J, Oda A, Amachi R, Harada T, Nakamura S, Miki H, Fujii S, Kagawa K, Watanabe K, et al. Pim-2 kinase is an important target of treatment for tumor progression and bone loss in myeloma. Leukemia. 2015;29(1):207–217. doi: 10.1038/leu.2014.147. [DOI] [PubMed] [Google Scholar]
- 112.Harada T, Hiasa M, Teramachi J, Abe M. Myeloma-bone interaction: a vicious cycle via TAK1-PIM2 signaling. Cancers (Basel) 2021;13(17):4441. doi: 10.3390/cancers13174441. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113.Gomez-Abad C, Pisonero H, Blanco-Aparicio C, Roncador G, Gonzalez-Menchen A, Martinez-Climent JA, Mata E, Rodriguez ME, Munoz-Gonzalez G, Sanchez-Beato M, et al. PIM2 inhibition as a rational therapeutic approach in B-cell lymphoma. Blood. 2011;118(20):5517–5527. doi: 10.1182/blood-2011-03-344374. [DOI] [PubMed] [Google Scholar]
- 114.Landau DA, Carter SL, Stojanov P, McKenna A, Stevenson K, Lawrence MS, Sougnez C, Stewart C, Sivachenko A, Wang L, et al. Evolution and impact of subclonal mutations in chronic lymphocytic leukemia. Cell. 2013;152(4):714–726. doi: 10.1016/j.cell.2013.01.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115.Landau DA, Tausch E, Taylor-Weiner AN, Stewart C, Reiter JG, Bahlo J, Kluth S, Bozic I, Lawrence M, Bottcher S, et al. Mutations driving CLL and their evolution in progression and relapse. Nature. 2015;526(7574):525–530. doi: 10.1038/nature15395. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Brault L, Menter T, Obermann EC, Knapp S, Thommen S, Schwaller J, Tzankov A. PIM kinases are progression markers and emerging therapeutic targets in diffuse large B-cell lymphoma. Br J Cancer. 2012;107(3):491–500. doi: 10.1038/bjc.2012.272. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 117.Gaidano G, Pasqualucci L, Capello D, Berra E, Deambrogi C, Rossi D, Maria Larocca L, Gloghini A, Carbone A, Dalla-Favera R. Aberrant somatic hypermutation in multiple subtypes of AIDS-associated non-Hodgkin lymphoma. Blood. 2003;102(5):1833–1841. doi: 10.1182/blood-2002-11-3606. [DOI] [PubMed] [Google Scholar]
- 118.Peters TL, Li L, Tula-Sanchez AA, Pongtornpipat P, Schatz JH. Control of translational activation by PIM kinase in activated B-cell diffuse large B-cell lymphoma confers sensitivity to inhibition by PIM447. Oncotarget. 2016;7(39):63362–63373. doi: 10.18632/oncotarget.11457. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119.Zhou Y, Liu W, Xu Z, Zhu H, Xiao D, Su W, Zeng R, Feng Y, Duan Y, Zhou J, et al. Analysis of genomic alteration in primary central nervous system lymphoma and the expression of some related genes. Neoplasia. 2018;20(10):1059–1069. doi: 10.1016/j.neo.2018.08.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 120.Hsi ED, Jung SH, Lai R, Johnson JL, Cook JR, Jones D, Devos S, Cheson BD, Damon LE, Said J. Ki67 and PIM1 expression predict outcome in mantle cell lymphoma treated with high dose therapy, stem cell transplantation and rituximab: a cancer and Leukemia Group B 59909 correlative science study. Leuk Lymphoma. 2008;49(11):2081–2090. doi: 10.1080/10428190802419640. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 121.Martin-Sanchez E, Odqvist L, Rodriguez-Pinilla SM, Sanchez-Beato M, Roncador G, Dominguez-Gonzalez B, Blanco-Aparicio C, Garcia Collazo AM, Cantalapiedra EG, Fernandez JP, et al. PIM kinases as potential therapeutic targets in a subset of peripheral T cell lymphoma cases. PLoS One. 2014;9(11):e112148. doi: 10.1371/journal.pone.0112148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 122.Bellon M, Lu L, Nicot C. Constitutive activation of Pim1 kinase is a therapeutic target for adult T-cell leukemia. Blood. 2016;127(20):2439–2450. doi: 10.1182/blood-2015-11-685032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 123.Bellon M, Nicot C. Feedback loop regulation between Pim kinases and tax keeps human T-cell leukemia virus type 1 viral replication in check. J Virol. 2022;96(3):e0196021. doi: 10.1128/jvi.01960-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 124.Decker S, Finter J, Forde AJ, Kissel S, Schwaller J, Mack TS, Kuhn A, Gray N, Follo M, Jumaa H, et al. PIM kinases are essential for chronic lymphocytic leukemia cell survival (PIM2/3) and CXCR4-mediated microenvironmental interactions (PIM1) Mol Cancer Ther. 2014;13(5):1231–1245. doi: 10.1158/1535-7163.MCT-13-0575-T. [DOI] [PubMed] [Google Scholar]
- 125.Chen LS, Redkar S, Bearss D, Wierda WG, Gandhi V. Pim kinase inhibitor, SGI-1776, induces apoptosis in chronic lymphocytic leukemia cells. Blood. 2009;114(19):4150–4157. doi: 10.1182/blood-2009-03-212852. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 126.Huttmann A, Klein-Hitpass L, Thomale J, Deenen R, Carpinteiro A, Nuckel H, Ebeling P, Fuhrer A, Edelmann J, Sellmann L, et al. Gene expression signatures separate B-cell chronic lymphocytic leukaemia prognostic subgroups defined by ZAP-70 and CD38 expression status. Leukemia. 2006;20(10):1774–1782. doi: 10.1038/sj.leu.2404363. [DOI] [PubMed] [Google Scholar]
- 127.Cohen AM, Grinblat B, Bessler H, Kristt D, Kremer A, Schwartz A, Halperin M, Shalom S, Merkel D, Don J. Increased expression of the hPim-2 gene in human chronic lymphocytic leukemia and non-Hodgkin lymphoma. Leuk Lymphoma. 2004;45(5):951–955. doi: 10.1080/10428190310001641251. [DOI] [PubMed] [Google Scholar]
- 128.Kapelko-Slowik K, Dybko J, Grzymajlo K, Jazwiec B, Urbaniak-Kujda D, Slowik M, Potoczek S, Wolowiec D. Expression of the PIM2 gene is associated with more aggressive clinical course in patients with chronic lymphocytic leukemia. Adv Clin Exp Med. 2019;28(3):385–390. doi: 10.17219/acem/90771. [DOI] [PubMed] [Google Scholar]
- 129.Bialopiotrowicz E, Gorniak P, Noyszewska-Kania M, Pula B, Makuch-Lasica H, Nowak G, Bluszcz A, Szydlowski M, Jablonska E, Piechna K, et al. Microenvironment-induced PIM kinases promote CXCR4-triggered mTOR pathway required for chronic lymphocytic leukaemia cell migration. J Cell Mol Med. 2018;22(7):3548–3559. doi: 10.1111/jcmm.13632. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130.Martin-Sanchez E, Sanchez-Beato M, Rodriguez ME, Sanchez-Espiridion B, Gomez-Abad C, Bischoff JR, Piris MA, Garcia-Orad A, Garcia JF. HDAC inhibitors induce cell cycle arrest, activate the apoptotic extrinsic pathway and synergize with a novel PIM inhibitor in Hodgkin lymphoma-derived cell lines. Br J Haematol. 2011;152(3):352–356. doi: 10.1111/j.1365-2141.2010.08401.x. [DOI] [PubMed] [Google Scholar]
- 131.Szydlowski M, Prochorec-Sobieszek M, Szumera-Cieckiewicz A, Derezinska E, Hoser G, Wasilewska D, Szymanska-Giemza O, Jablonska E, Bialopiotrowicz E, Sewastianik T, et al. Expression of PIM kinases in Reed-Sternberg cells fosters immune privilege and tumor cell survival in Hodgkin lymphoma. Blood. 2017;130(12):1418–1429. doi: 10.1182/blood-2017-01-760702. [DOI] [PubMed] [Google Scholar]
- 132.Fowlkes S, Murray C, Fulford A, De Gelder T, Siddiq N. Myeloproliferative neoplasms (MPNs) - part 1: an overview of the diagnosis and treatment of the “classical” MPNs. Can Oncol Nurs J. 2018;28(4):262–268. doi: 10.5737/23688076284262268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 133.Gozgit JM, Bebernitz G, Patil P, Ye M, Parmentier J, Wu J, Su N, Wang T, Ioannidis S, Davies A, et al. Effects of the JAK2 inhibitor, AZ960, on Pim/BAD/BCL-xL survival signaling in the human JAK2 V617F cell line SET-2. J Biol Chem. 2008;283(47):32334–32343. doi: 10.1074/jbc.M803813200. [DOI] [PubMed] [Google Scholar]
- 134.Schwemmers S, Will B, Waller CF, Abdulkarim K, Johansson P, Andreasson B, Pahl HL. JAK2V617F-negative ET patients do not display constitutively active JAK/STAT signaling. Exp Hematol. 2007;35(11):1695–1703. doi: 10.1016/j.exphem.2007.07.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 135.Dutta A, Nath D, Yang Y, Le BT, Rahman MF, Faughnan P, Wang Z, Stuver M, He R, Tan W, et al. Genetic ablation of Pim1 or pharmacologic inhibition with TP-3654 ameliorates myelofibrosis in murine models. Leukemia. 2022;36(3):746–759. doi: 10.1038/s41375-021-01464-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 136.Wernig G, Gonneville JR, Crowley BJ, Rodrigues MS, Reddy MM, Hudon HE, Walz C, Reiter A, Podar K, Royer Y, et al. The Jak2V617F oncogene associated with myeloproliferative diseases requires a functional FERM domain for transformation and for expression of the Myc and Pim proto-oncogenes. Blood. 2008;111(7):3751–3759. doi: 10.1182/blood-2007-07-102186. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 137.Eiring AM, Harb JG, Neviani P, Garton C, Oaks JJ, Spizzo R, Liu S, Schwind S, Santhanam R, Hickey CJ, et al. miR-328 functions as an RNA decoy to modulate hnRNP E2 regulation of mRNA translation in leukemic blasts. Cell. 2010;140(5):652–665. doi: 10.1016/j.cell.2010.01.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 138.Nieborowska-Skorska M, Hoser G, Kossev P, Wasik MA, Skorski T. Complementary functions of the antiapoptotic protein A1 and serine/threonine kinase pim-1 in the BCR/ABL-mediated leukemogenesis. Blood. 2002;99(12):4531–4539. doi: 10.1182/blood.V99.12.4531. [DOI] [PubMed] [Google Scholar]
- 139.Adam M, Pogacic V, Bendit M, Chappuis R, Nawijn MC, Duyster J, Fox CJ, Thompson CB, Cools J, Schwaller J. Targeting PIM kinases impairs survival of hematopoietic cells transformed by kinase inhibitor-sensitive and kinase inhibitor-resistant forms of Fms-like tyrosine kinase 3 and BCR/ABL. Cancer Res. 2006;66(7):3828–3835. doi: 10.1158/0008-5472.CAN-05-2309. [DOI] [PubMed] [Google Scholar]
- 140.Nakano H, Hasegawa T, Kojima H, Okabe T, Nagano T. Design and synthesis of potent and selective PIM kinase inhibitors by targeting unique structure of ATP-binding pocket. ACS Med Chem Lett. 2017;8(5):504–509. doi: 10.1021/acsmedchemlett.6b00518. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 141.Cortes J, Tamura K, DeAngelo DJ, de Bono J, Lorente D, Minden M, Uy GL, Kantarjian H, Chen LS, Gandhi V, et al. Phase I studies of AZD1208, a proviral integration Moloney virus kinase inhibitor in solid and haematological cancers. Br J Cancer. 2018;118(11):1425–1433. doi: 10.1038/s41416-018-0082-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 142.Burger MT, Nishiguchi G, Han W, Lan J, Simmons R, Atallah G, Ding Y, Tamez V, Zhang Y, Mathur M, et al. Identification of N-(4-((1R,3S,5S)-3-Amino-5-methylcyclohexyl)pyridin-3-yl)-6-(2,6-difluorophenyl)- 5-fluoropicolinamide (PIM447), a potent and selective proviral insertion site of Moloney murine leukemia (PIM) 1, 2, and 3 kinase inhibitor in clinical trials for hematological malignancies. J Med Chem. 2015;58(21):8373–8386. doi: 10.1021/acs.jmedchem.5b01275. [DOI] [PubMed] [Google Scholar]
- 143.Koblish H, Li YL, Shin N, Hall L, Wang Q, Wang K, Covington M, Marando C, Bowman K, Boer J, et al. Preclinical characterization of INCB053914, a novel pan-PIM kinase inhibitor, alone and in combination with anticancer agents, in models of hematologic malignancies. PLoS One. 2018;13(6):e0199108. doi: 10.1371/journal.pone.0199108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 144.Byrne M, Donnellan W, Patel MR, Zeidan AM, Cherry M, Baer MR, Fathi AT, Kaplan J, Zhou F, Zheng F, et al. Preliminary results from an ongoing phase 1/2 study of INCB053914, a pan-proviral integration sites for Moloney virus (PIM) kinase inhibitor, in patients with advanced hematologic malignancies. Blood. 2017;130:2585. [Google Scholar]
- 145.Kapoor S, Natarajan K, Baldwin PR, Doshi KA, Lapidus RG, Mathias TJ, Scarpa M, Trotta R, Davila E, Kraus M, et al. Concurrent inhibition of Pim and FLT3 kinases enhances apoptosis of FLT3-ITD acute myeloid leukemia cells through increased mcl-1 proteasomal degradation. Clin Cancer Res. 2018;24(1):234–247. doi: 10.1158/1078-0432.CCR-17-1629. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 146.Brunen D, Garcia-Barchino MJ, Malani D, Jagalur Basheer N, Lieftink C, Beijersbergen RL, Murumagi A, Porkka K, Wolf M, Zwaan CM, et al. Intrinsic resistance to PIM kinase inhibition in AML through p38alpha-mediated feedback activation of mTOR signaling. Oncotarget. 2016;7(25):37407–37419. doi: 10.18632/oncotarget.9822. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 147.Harada M, Benito J, Yamamoto S, Kaur S, Arslan D, Ramirez S, Jacamo R, Platanias L, Matsushita H, Fujimura T, et al. The novel combination of dual mTOR inhibitor AZD2014 and pan-PIM inhibitor AZD1208 inhibits growth in acute myeloid leukemia via HSF pathway suppression. Oncotarget. 2015;6(35):37930–37947. doi: 10.18632/oncotarget.6122. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 148.Chen LS, Yang JY, Liang H, Cortes JE, Gandhi V. Protein profiling identifies mTOR pathway modulation and cytostatic effects of Pim kinase inhibitor, AZD1208, in acute myeloid leukemia. Leuk Lymphoma. 2016;57(12):2863–2873. doi: 10.3109/10428194.2016.1166489. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 149.Meja K, Stengel C, Sellar R, Huszar D, Davies BR, Gale RE, Linch DC, Khwaja A. PIM and AKT kinase inhibitors show synergistic cytotoxicity in acute myeloid leukaemia that is associated with convergence on mTOR and MCL1 pathways. Br J Haematol. 2014;167(1):69–79. doi: 10.1111/bjh.13013. [DOI] [PubMed] [Google Scholar]
- 150.Blanco-Aparicio C, Collazo AM, Oyarzabal J, Leal JF, Albaran MI, Lima FR, Pequeno B, Ajenjo N, Becerra M, Alfonso P, et al. Pim 1 kinase inhibitor ETP-45299 suppresses cellular proliferation and synergizes with PI3K inhibition. Cancer Lett. 2011;300(2):145–153. doi: 10.1016/j.canlet.2010.09.016. [DOI] [PubMed] [Google Scholar]
- 151.Doshi KA, Trotta R, Natarajan K, Rassool FV, Tron AE, Huszar D, Perrotti D, Baer MR. Pim kinase inhibition sensitizes FLT3-ITD acute myeloid leukemia cells to topoisomerase 2 inhibitors through increased DNA damage and oxidative stress. Oncotarget. 2016;7(30):48280–48295. doi: 10.18632/oncotarget.10209. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 152.Scarpa M, Kapoor S, Tvedte ES, Doshi KA, Zou YS, Singh P, Lee JK, Chatterjee A, Ali MKM, Bromley RE, et al. Pim kinase inhibitor co-treatment decreases alternative non-homologous end-joining DNA repair and genomic instability induced by topoisomerase 2 inhibitors in cells with FLT3 internal tandem duplication. Oncotarget. 2021;12(18):1763–1779. doi: 10.18632/oncotarget.28042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 153.Puente-Moncada N, Costales P, Antolin I, Nunez LE, Oro P, Hermosilla MA, Perez-Escuredo J, Rios-Lombardia N, Sanchez-Sanchez AM, Luno E, et al. Inhibition of FLT3 and PIM kinases by EC-70124 exerts potent activity in preclinical models of acute myeloid leukemia. Mol Cancer Ther. 2018;17(3):614–624. doi: 10.1158/1535-7163.MCT-17-0530. [DOI] [PubMed] [Google Scholar]
- 154.Yang C, Boyson CA, Di Liberto M, Huang X, Hannah J, Dorn DC, Moore MA, Chen-Kiang S, Zhou P. CDK4/6 inhibitor PD 0332991 sensitizes acute myeloid leukemia to cytarabine-mediated cytotoxicity. Cancer Res. 2015;75(9):1838–1845. doi: 10.1158/0008-5472.CAN-14-2486. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 155.Lee HJ, Daver N, Kantarjian HM, Verstovsek S, Ravandi F. The role of JAK pathway dysregulation in the pathogenesis and treatment of acute myeloid leukemia. Clin Cancer Res. 2013;19(2):327–335. doi: 10.1158/1078-0432.CCR-12-2087. [DOI] [PubMed] [Google Scholar]
- 156.Pemmaraju N, Kantarjian H, Kadia T, Cortes J, Borthakur G, Newberry K, Garcia-Manero G, Ravandi F, Jabbour E, Dellasala S, et al. A phase I/II study of the Janus kinase (JAK)1 and 2 inhibitor ruxolitinib in patients with relapsed or refractory acute myeloid leukemia. Clin Lymphoma Myeloma Leuk. 2015;15(3):171–176. doi: 10.1016/j.clml.2014.08.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 157.Cao T, Jiang N, Liao H, Shuai X, Su J, Zheng Q. The FLT3-ITD mutation and the expression of its downstream signaling intermediates STAT5 and Pim-1 are positively correlated with CXCR4 expression in patients with acute myeloid leukemia. Sci Rep. 2019;9(1):12209. doi: 10.1038/s41598-019-48687-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 158.Abraham M, Klein S, Bulvik B, Wald H, Weiss ID, Olam D, Weiss L, Beider K, Eizenberg O, Wald O, et al. The CXCR4 inhibitor BL-8040 induces the apoptosis of AML blasts by downregulating ERK, BCL-2, MCL-1 and cyclin-D1 via altered miR-15a/16-1 expression. Leukemia. 2017;31(11):2336–2346. doi: 10.1038/leu.2017.82. [DOI] [PubMed] [Google Scholar]
- 159.Cooper TM, Sison EAR, Baker SD, Li L, Ahmed A, Trippett T, Gore L, Macy ME, Narendran A, August K, et al. A phase 1 study of the CXCR4 antagonist plerixafor in combination with high-dose cytarabine and etoposide in children with relapsed or refractory acute leukemias or myelodysplastic syndrome: a Pediatric Oncology Experimental Therapeutics Investigators’ Consortium study (POE 10–03) Pediatr Blood Cancer. 2017;64(8):e26414. doi: 10.1002/pbc.26414. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 160.Liu CN, Liu B, Xu CP, Zhang P, Li B, Ji B, et al. ETH-155008, a novel selective dual inhibitor of FLT3 and CDK4/6 in preclinical treatment of acute myeloid leukemia. Blood. 2019;134(Supplement_1):5141.
- 161.Solomon SR, Montesinos P, Nazha A, Strickland SA, Martinelli G, Santoro A, et al. Updated results from DIAMOND-01 (CLI24-001) trial: a phase I/II study of SEL24/MEN1703, a first-in-class dual PIM/FLT3 kinase inhibitor, in acute myeloid leukemia. J Clin Oncol. 2021;39(15_suppl):7023.
- 162.Minieri V, De Dominici M, Porazzi P, Mariani SA, Spinelli O, Rambaldi A, Peterson LF, Porcu P, Nevalainen MT, Calabretta B. Targeting STAT5 or STAT5-regulated pathways suppresses leukemogenesis of Ph+ acute lymphoblastic leukemia. Cancer Res. 2018;78(20):5793–5807. doi: 10.1158/0008-5472.CAN-18-0195. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 163.De Smedt R, Peirs S, Morscio J, Matthijssens F, Roels J, Reunes L, Lintermans B, Goossens S, Lammens T, Van Roy N, et al. Pre-clinical evaluation of second generation PIM inhibitors for the treatment of T-cell acute lymphoblastic leukemia and lymphoma. Haematologica. 2019;104(1):e17–e20. doi: 10.3324/haematol.2018.199257. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 164.Ribeiro D, Melao A, van Boxtel R, Santos CI, Silva A, Silva MC, Cardoso BA, Coffer PJ, Barata JT. STAT5 is essential for IL-7-mediated viability, growth, and proliferation of T-cell acute lymphoblastic leukemia cells. Blood Adv. 2018;2(17):2199–2213. doi: 10.1182/bloodadvances.2018021063. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 165.Padi SKR, Luevano LA, An N, Pandey R, Singh N, Song JH, Aster JC, Yu XZ, Mehrotra S, Kraft AS. Targeting the PIM protein kinases for the treatment of a T-cell acute lymphoblastic leukemia subset. Oncotarget. 2017;8(18):30199–30216. doi: 10.18632/oncotarget.16320. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 166.Lin YW, Beharry ZM, Hill EG, Song JH, Wang W, Xia Z, Zhang Z, Aplan PD, Aster JC, Smith CD, et al. A small molecule inhibitor of Pim protein kinases blocks the growth of precursor T-cell lymphoblastic leukemia/lymphoma. Blood. 2010;115(4):824–833. doi: 10.1182/blood-2009-07-233445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 167.Kuang X, Xiong J, Wang W, Li X, Lu T, Fang Q, Wang J. PIM inhibitor SMI-4a induces cell apoptosis in B-cell acute lymphocytic leukemia cells via the HO-1-mediated JAK2/STAT3 pathway. Life Sci. 2019;219:248–256. doi: 10.1016/j.lfs.2019.01.022. [DOI] [PubMed] [Google Scholar]
- 168.De Smedt R, Morscio J, Reunes L, Roels J, Bardelli V, Lintermans B, Van Loocke W, Almeida ARM, Cheung LC, Kotecha RS, et al. Targeting cytokine and therapy induced PIM1 activation in T-cell acute lymphoblastic leukemia and lymphoma. Blood. 2020;135(19):1685–1695. doi: 10.1182/blood.2019003880. [DOI] [PubMed] [Google Scholar]
- 169.Raab MS, Thomas SK, Ocio EM, Guenther A, Goh YT, Talpaz M, Hohmann N, Zhao S, Xiang F, Simon C, et al. The first-in-human study of the pan-PIM kinase inhibitor PIM447 in patients with relapsed and/or refractory multiple myeloma. Leukemia. 2019;33(12):2924–2933. doi: 10.1038/s41375-019-0482-0. [DOI] [PubMed] [Google Scholar]
- 170.Iida S, Sunami K, Minami H, Hatake K, Sekiguchi R, Natsume K, Ishikawa N, Rinne M, Taniwaki M. A phase I, dose-escalation study of oral PIM447 in Japanese patients with relapsed and/or refractory multiple myeloma. Int J Hematol. 2021;113(6):797–806. doi: 10.1007/s12185-021-03096-9. [DOI] [PubMed] [Google Scholar]
- 171.Tian Z, Zhao JJ, Tai YT, Amin SB, Hu Y, Berger AJ, Richardson P, Chauhan D, Anderson KC. Investigational agent MLN9708/2238 targets tumor-suppressor miR33b in MM cells. Blood. 2012;120(19):3958–3967. doi: 10.1182/blood-2012-01-401794. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 172.Reidy M, vanDijk M, Keane N, O'Neill M, O’Dwyer ME. Initial evaluation of novel dual PIM/PI3K and triple PIM/PI3K/mTOR inhibitors in multiple myeloma. Blood. 2014;124(21):5713. doi: 10.1182/blood.V124.21.5713.5713. [DOI] [Google Scholar]
- 173.de Vos S, Krug U, Hofmann WK, Pinkus GS, Swerdlow SH, Wachsman W, Grogan TM, Said JW, Koeffler HP. Cell cycle alterations in the blastoid variant of mantle cell lymphoma (MCL-BV) as detected by gene expression profiling of mantle cell lymphoma (MCL) and MCL-BV. Diagn Mol Pathol. 2003;12(1):35–43. doi: 10.1097/00019606-200303000-00005. [DOI] [PubMed] [Google Scholar]
- 174.Rubenstein JL, Fridlyand J, Abrey L, Shen A, Karch J, Wang E, Issa S, Damon L, Prados M, McDermott M, et al. Phase I study of intraventricular administration of rituximab in patients with recurrent CNS and intraocular lymphoma. J Clin Oncol. 2007;25(11):1350–1356. doi: 10.1200/JCO.2006.09.7311. [DOI] [PubMed] [Google Scholar]
- 175.Decker S, Kissel S, Aumann K, Zenz T, Zirlik K, Claus R, Duyster J, Dierks C. The Pan-PIM kinase inhibitor LGB321 affects apoptotic pathways and microenvironmental interactions in CLL. Blood. 2016;128(22):4370. doi: 10.1182/blood.V128.22.4370.4370. [DOI] [Google Scholar]
- 176.Kuo HP, Ezell SA, Hsieh S, Schweighofer KJ, Cheung LW, Wu S, Apatira M, Sirisawad M, Eckert K, Liang Y, et al. The role of PIM1 in the ibrutinib-resistant ABC subtype of diffuse large B-cell lymphoma. Am J Cancer Res. 2016;6(11):2489–2501. [PMC free article] [PubMed] [Google Scholar]
- 177.Marit MR, Chohan M, Matthew N, Huang K, Kuntz DA, Rose DR, Barber DL. Random mutagenesis reveals residues of JAK2 critical in evading inhibition by a tyrosine kinase inhibitor. PLoS One. 2012;7(8):e43437. doi: 10.1371/journal.pone.0043437. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 178.Mazzacurati L, Lambert QT, Pradhan A, Griner LN, Huszar D, Reuther GW. The PIM inhibitor AZD1208 synergizes with ruxolitinib to induce apoptosis of ruxolitinib sensitive and resistant JAK2-V617F-driven cells and inhibit colony formation of primary MPN cells. Oncotarget. 2015;6(37):40141–40157. doi: 10.18632/oncotarget.5653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 179.Huang SM, Wang A, Greco R, Li Z, Barberis C, Tabart M, Patel V, Schio L, Hurley R, Chen B, et al. Combination of PIM and JAK2 inhibitors synergistically suppresses MPN cell proliferation and overcomes drug resistance. Oncotarget. 2014;5(10):3362–3374. doi: 10.18632/oncotarget.1951. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 180.Mazzacurati L, Collins RJ, Pandey G, Lambert-Showers QT, Amin NE, Zhang L, Stubbs MC, Epling-Burnette PK, Koblish HK, Reuther GW. The pan-PIM inhibitor INCB053914 displays potent synergy in combination with ruxolitinib in models of MPN. Blood Adv. 2019;3(22):3503–3514. doi: 10.1182/bloodadvances.2019000260. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 181.Mascarenhas JO, Orazi A, Bhalla KN, Champlin RE, Harrison C, Hoffman R. Advances in myelofibrosis: a clinical case approach. Haematologica. 2013;98(10):1499–1509. doi: 10.3324/haematol.2013.086348. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 182.Rampal RK, Pinzon-Ortiz M, Somasundara AVH, Durham B, Koche R, Spitzer B, Mowla S, Krishnan A, Li B, An W, et al. Therapeutic efficacy of combined JAK1/2, Pan-PIM, and CDK4/6 inhibition in myeloproliferative neoplasms. Clin Cancer Res. 2021;27(12):3456–3468. doi: 10.1158/1078-0432.CCR-20-4898. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 183.Curi DA, Beauchamp EM, Blyth GT, Arslan AD, Donato NJ, Giles FJ, Altman JK, Platanias LC. Pre-clinical evidence of PIM kinase inhibitor activity in BCR-ABL1 unmutated and mutated Philadelphia chromosome-positive (Ph+) leukemias. Oncotarget. 2015;6(32):33206–33216. doi: 10.18632/oncotarget.5091. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 184.Fan RF, Lu Y, Fang ZG, Guo XY, Chen YX, Xu YC, Lei YM, Liu KF, Lin DJ, Liu LL, et al. PIM-1 kinase inhibitor SMI-4a exerts antitumor effects in chronic myeloid leukemia cells by enhancing the activity of glycogen synthase kinase 3beta. Mol Med Rep. 2017;16(4):4603–4612. doi: 10.3892/mmr.2017.7215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 185.Ma L, Pak ML, Ou J, Yu J, St Louis P, Shan Y, Hutchinson L, Li S, Brehm MA, Zhu LJ, et al. Prosurvival kinase PIM2 is a therapeutic target for eradication of chronic myeloid leukemia stem cells. Proc Natl Acad Sci U S A. 2019;116(21):10482–10487. doi: 10.1073/pnas.1903550116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 186.Li J, Hu XF, Loveland BE, Xing PX. Pim-1 expression and monoclonal antibody targeting in human leukemia cell lines. Exp Hematol. 2009;37(11):1284–1294. doi: 10.1016/j.exphem.2009.08.002. [DOI] [PubMed] [Google Scholar]
- 187.Hu XF, Li J, Vandervalk S, Wang Z, Magnuson NS, Xing PX. PIM-1-specific mAb suppresses human and mouse tumor growth by decreasing PIM-1 levels, reducing Akt phosphorylation, and activating apoptosis. J Clin Invest. 2009;119(2):362–375. doi: 10.1172/JCI33216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 188.Thomas M, Lange-Grunweller K, Weirauch U, Gutsch D, Aigner A, Grunweller A, Hartmann RK. The proto-oncogene Pim-1 is a target of miR-33a. Oncogene. 2012;31(7):918–928. doi: 10.1038/onc.2011.278. [DOI] [PubMed] [Google Scholar]
- 189.Liang C, Yu XJ, Guo XZ, Sun MH, Wang Z, Song Y, Ni QX, Li HY, Mukaida N, Li YY. MicroRNA-33a-mediated downregulation of Pim-3 kinase expression renders human pancreatic cancer cells sensitivity to gemcitabine. Oncotarget. 2015;6(16):14440–14455. doi: 10.18632/oncotarget.3885. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 190.Zhang Y, Lei W, Yan W, Li X, Wang X, Zhao Z, Hui J, Shen Z, Yang J. microRNA-206 is involved in survival of hypoxia preconditioned mesenchymal stem cells through targeting Pim-1 kinase. Stem Cell Res Ther. 2016;7(1):61. doi: 10.1186/s13287-016-0318-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 191.Pan XP, Wang HX, Tong DM, Li Y, Huang LH, Wang C. miRNA-370 acts as a tumor suppressor via the downregulation of PIM1 in hepatocellular carcinoma. Eur Rev Med Pharmacol Sci. 2017;21(6):1254–1263. [PubMed] [Google Scholar]
- 192.Pang W, Tian X, Bai F, Han R, Wang J, Shen H, Zhang X, Liu Y, Yan X, Jiang F, et al. Pim-1 kinase is a target of miR-486-5p and eukaryotic translation initiation factor 4E, and plays a critical role in lung cancer. Mol Cancer. 2014;13:240. doi: 10.1186/1476-4598-13-240. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 193.Qian Z, Zhang L, Chen J, Li Y, Kang K, Qu J, Wang Z, Zhai Y, Li L, Gou D. MiR-328 targeting PIM-1 inhibits proliferation and migration of pulmonary arterial smooth muscle cells in PDGFBB signaling pathway. Oncotarget. 2016;7(34):54998–55011. doi: 10.18632/oncotarget.10714. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 194.Deng D, Wang L, Chen Y, Li B, Xue L, Shao N, Wang Q, Xia X, Yang Y, Zhi F. MicroRNA-124-3p regulates cell proliferation, invasion, apoptosis, and bioenergetics by targeting PIM1 in astrocytoma. Cancer Sci. 2016;107(7):899–907. doi: 10.1111/cas.12946. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 195.Gu H, Liu M, Ding C, Wang X, Wang R, Wu X, Fan R. Hypoxia-responsive miR-124 and miR-144 reduce hypoxia-induced autophagy and enhance radiosensitivity of prostate cancer cells via suppressing PIM1. Cancer Med. 2016;5(6):1174–1182. doi: 10.1002/cam4.664. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 196.Rang Z, Yang G, Wang YW, Cui F. miR-542-3p suppresses invasion and metastasis by targeting the proto-oncogene serine/threonine protein kinase, PIM1, in melanoma. Biochem Biophys Res Commun. 2016;474(2):315–320. doi: 10.1016/j.bbrc.2016.04.093. [DOI] [PubMed] [Google Scholar]
- 197.Liu XY, Liu ZJ, He H, Zhang C, Wang YL. MicroRNA-101-3p suppresses cell proliferation, invasion and enhances chemotherapeutic sensitivity in salivary gland adenoid cystic carcinoma by targeting Pim-1. Am J Cancer Res. 2015;5(10):3015–3029. [PMC free article] [PubMed] [Google Scholar]
- 198.Han W, Li N, Liu J, Sun Y, Yang X, Wang Y. MicroRNA-26b-5p enhances T cell responses by targeting PIM-2 in hepatocellular carcinoma. Cell Signal. 2019;59:182–190. doi: 10.1016/j.cellsig.2018.11.011. [DOI] [PubMed] [Google Scholar]
- 199.Zhang H. Upregulation of PIM2 by underexpression of microRNA-135-5p improves survival rates of skin allografts by suppressing apoptosis of fibroblast cells. Med Sci Monit. 2017;23:107–113. doi: 10.12659/MSM.897613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 200.Du J, Zheng X, Cai S, Zhu Z, Tan J, Hu B, Huang Z, Jiao H. MicroRNA506 participates in pancreatic cancer pathogenesis by targeting PIM3. Mol Med Rep. 2015;12(4):5121–5126. doi: 10.3892/mmr.2015.4109. [DOI] [PubMed] [Google Scholar]