Abstract
Background
This study aims to compare the potential short-term effects of non-pharmacological interventions (NPIs) on prehypertensive people, and provide evidence for intervention models with potential in future community-based management.
Methods
In this Bayesian network meta-analysis, Pubmed, Embase, and Web of science were screened up to 16 October 2021. Prehypertensive patients (systolic blood pressure, SBP 120–139 mmHg/diastolic blood pressure, DBP 80–89 mmHg) with a follow-up period longer than 4 weeks were targeted. Sixteen NPIs were identified during the scope review and categorized into five groups. Reduction in SBP and DBP was selected as outcome variables and the effect sizes were compared using consistency models among interventions and intervention groups. Grade approach was used to assess the certainty of evidence.
Results
Thirty-nine studies with 8,279 participants were included. For SBP, strengthen exercises were the most advantageous intervention group when compared with usual care (mean difference = −6.02 mmHg, 95% CI −8.16 to −3.87), and combination exercise, isometric exercise, and aerobic exercise were the three most effective specific interventions. For DBP, relaxation was the most advantageous intervention group when compared with usual care (mean difference = −4.99 mmHg, 95% CI −7.03 to −2.96), and acupuncture, meditation, and combination exercise were the three most effective specific interventions. No inconsistency was found between indirect and direct evidence. However, heterogeneity was detected in some studies.
Conclusion
NPIs can bring short-term BP reduction benefits for prehypertensive patients, especially exercise and relaxation. NPIs could potentially be included in community-based disease management for prehypertensive population once long-term real-world effectiveness and cost-effectiveness are proven.
Systematic review registration
https://www.crd.york.ac.uk/PROSPERO/display_record.php?RecordID=151518, identifier: CRD42020151518.
Keywords: Bayesian network meta-analysis, prehypertension, non-pharmacological intervention, chronic disease management, blood pressure reduction
Introduction
Hypertension is one of the leading risk factors for morbidity and mortality around the world, which affect approximately one billion people (1–3). Elevated blood pressure, called prehypertension, defined as a blood pressure of 120–139/80–89 mmHg, is common and affects 25–50% of adults all over the world (4–6). Prehypertension confers a high risk of progression to hypertension and increases the risk of cardiovascular diseases with a 5-year progression rate of 40% (4, 7, 8). High prevalence and risk of prehypertension call for effective and cost-effective interventions. Current anti-hypertensive treatments include drug interventions and non-pharmacological interventions (NPIs) (9, 10), but previous research points out that there is a lack of evidence that early medication can bring benefits to prehypertensive people with no cardiovascular risk (5, 6), less to mention the unnecessary harm and economic loss brought by the resistance and side effects of anti-hypertensive drugs (11, 12). On the contrary, current available NPIs including exercises (e.g., aerobic exercise, resistance exercise), dietary intervention (e.g., salt reduction, alcohol reduction), relaxation (e.g., acupuncture, yoga), and so on Verma et al. (13), may be equally effective. Since NPIs focus more on changes in patient's behavior and lifestyle, they have no side effects and may be with potential cost-effectiveness (14). NPIs have been recommended by recent guidelines, which can be considered a priority in treating and managing prehypertensive people (6). Quite a few studies have proved that intensive lifestyle intervention as well as other NPIs can reduce the blood pressure (BP) of hypertensive and prehypertensive people in a short term (4, 15–18). However, the relative effects of NPIs are still unknown.
Although prehypertension has a large prevalence worldwide (6, 19), but patients are not managed in most countries currently. Simply using drug interventions may not be suitable to manage such a huge population since the economic burden can be large. NPIs are widely available and with low costs, can be good choices to be applied in management (20). However, implementing NPIs in current community-based chronic disease management still faced some barriers (21). NPIs require community-based chronic disease-management staff to have a medical background and additional professional training, and delivering NPIs is highly dependent on provider services (14, 22–24). However, these staffs are scarce, especially in many low- and middle-income countries (25). It is therefore necessary to explore the most effective and efficient type of service model which had the potential to be implemented. However, the evidence in this field is extremely lacking.
In this study, we aim to conduct a network meta-analysis to rank the short-term effects of NPIs among current available studies. The results will provide evidence for non-pharmacological treatment for prehypertensive patients from a global perspective, and hopefully lay a basis for the future inclusion of prehypertensive patients in community-based chronic disease management.
Methods
We used a network meta-analysis to evaluate the short-term efficacy of NPIs on prehypertension. This research was reported following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) checklist (26). This research was registered with PROSPERO (registration number: CRD42020151518) and the protocol has been published (27).
Patient and public involvement
Patients were not involved in this study.
Literature search
We conducted a systematic search in PubMed, Web of Science, Embase, and the Cochrane Library up to 16 October 2021. We included randomized controlled trials and reasonably designed non-randomized controlled trials but excluded observational studies such as cross-sectional or cohort studies, systematic reviews and meta-analyses, and economic evaluations. We carried out a scope review and systematic review: the scope review was used to determine the NPIs included in the study, and the systematic review was then conducted to determine the studies included in the network meta-analysis. International guidelines were used to double-check the eligibility of interventions (6, 13, 28). The reference lists of relevant meta-analyses were scanned to identify other articles of interest. There was no limitation on the publication date of studies. The language of included studies was limited to English. Our search strategies and process are given in Supplementary material 1.
Inclusion and exclusion criteria
All retrieved articles were imported into Noteexpress (3.2.0.7535, China Pharmaceutical University). Two independent researchers (THS and LYL) screened the literature for inclusion. Disagreements were discussed and consensus was reached in all cases. Literature was included in the systematic review if it met the following criteria.
Population
Study targets of adults aged >18 years whose BP status met the following two criteria were included: (1) diagnosed with prehypertension; (2) baseline BP between 120–139/80–89 mmHg. Subjects were excluded when they: (1) received antihypertensive agents; (2) had cardiovascular diseases (e.g., stroke, myocardial infarction); (3) had pregnancy-induced hypertension or pulmonary hypertension.
Intervention and control
Studies with at least one study arm using the following 15 NPIs were included: acupuncture, aerobic exercise, combination exercise, Dietary Approaches to Stop Hypertension (DASH), high Potassium, isometric exercise, lifestyle, meditation, normal exercise, alcohol reduction, resistance exercise, salt restriction, weight loss, yoga, and usual care. We merged these 15 interventions into five groups: relaxation, dietary intervention, strengthen exercise, lifestyle modification, and usual care, based on a comprehensive consideration of the type of interventions (exercise or dietary) and the intensity of intervention (strengthen or relax). The standardized descriptions of the interventions are shown in Table 1.
Table 1.
Non-pharmacological interventions for prehypertensive patients.
| Name | Content | Intensity | Name | Content | Intensity |
|---|---|---|---|---|---|
| Acupuncture | Including acupuncture and moxibustion. Acupuncture refers to acupuncture of certain acupoints by professionals, leaving the needle for 30 mins after getting qi. Moxibustion refers to the use of prefabricated moxibustion grass on certain acupoints on the body's surface, burning and ironing, using heat to stimulate the acupuncture points | Average 3 times/week, 30 min each time, lasting 6 weeks | Relaxation | Receive physical therapy by professionals. Or receive training by professionals, learn relaxing exercises, combine learning materials for independent exercises, including yoga, meditation | Average 4 times/week, 45 mins each time, lasting 12 weeks |
| Meditation | Transcendental meditation is aim to reduce stress. Participants are instructed by professional meditation instructors and then study and practice in groups to finish the mindfulness-based meditation program | Average 2 h/week, lasting 12 weeks | |||
| Yoga | Guide by a professional yoga instructor to perform yoga exercises, including asanas, breathing and meditation | 6–7 days a week, 45–60 min/d, lasting for 12 weeks | |||
| Aerobic exercise | Use oxygen for energy, moderate to intensity exercise that lasts for a long time and has a rhythm, and the exercise intensity is 50–70% of the maximum heart rate. Including fast walking, jogging, cycling, mountain climbing and so on | 3–4 times/week, 30–60 min/time, lasting 12 weeks | Strengthen exercise | Under the guidance of professionals, perform aerobic exercise (such as jogging, brisk walking, cycling, etc.), resistance exercise, isometric exercise or a combination of multiple forms of exercise at different target intensities | Average 4 times/week, 45 mins each time, lasting 8 weeks |
| Resistance exercise | Complete the specified actions according to the requirements and the purpose of the action design is to exercise the main muscle groups of the body. Totally seven actions, each action is repeated 10–15 times as a group, do 2–3 groups. Elastic ropes and other props are used under the supervision of the professionals | 1 group of 12 reps; total 2 groups lasting 45 min; 3 times/week; lasting 6 months | |||
| Normal exercise | Stretching or walking briskly for 30–60 mins under the supervision of professionals, the exercise intensity is about 5 km/h | 45 mins/time; 3 times/week; lasting 8 weeks | |||
| Isometric exercise | Use isometric handle equipment to exercise at the intensity of 20–30% MVC | 10 min/d; every day; lasting 6 weeks | |||
| Combination exercise | A comprehensive exercise program that combines endurance exercise, isometric exercise and aerobic exercise | 3 times/week, an average of 50 min each time; lasting 7 weeks | |||
| Salt reduction | Provide a measuring spoon, limit salt intake (maximum 3 g/day), or use alternative salt | ≤ 3 g/day | Dietary | Reasonable diet, reduce sodium intake, reduce fat intake, reduce alcohol, increase potassium intake or adopt DASH diet | Adhere to certain diet every day. Conduct education every certain times |
| DASH | Emphasize a comprehensive diet, increase the intake of fruits, vegetables, whole grains and low-fat dairy products, and limit the intake of sodium, saturated fat and total fat | Eat according to DASH every day | |||
| Alcohol reduction | Participants reduce their alcohol intake by substitute their drink to low-alcohol beer (0.9% v/v). Researchers provide 24 × 375 ml every 2 weeks | 0.9% alcohol by volume drink 24 × 375 ml every 2 weeks | |||
| High potassium | Participants either receive a salt substitute (potassium chloride) or receive dietary education by investigator to reduce sodium intake and increase potassium intake | Reduce sodium intake and increase potassium intake every day; education is conducted once a week | |||
| Lifestyle | Give lifestyle suggestions, such as reasonable diet, reducing fat intake, proper exercise, weight control, reducing sodium intake, quitting smoking and alcohol, reducing mental stress. Then participants are required to change lifestyle according to these suggestions | Everyday | Lifestyle | Participants are required to change lifestyle or lose weight according to education | Everyday |
| Weight loss | Participants use the physical exercise plus low-calorie diet as well as specific nutrition intake for weight loss which are designed by researchers to achieve weight and BMI target | Dietary: every day. Physical exercise is recommended 30–45 min/d, 4–5 per week | |||
| Usual care | No intervention, keep the original lifestyle habits unchanged | Everyday | Usual care | Regular blood pressure monitoring and health education is conducted without specific intervention | Follow up once a month and conduct health education once every 6 months |
min, minute; d, day; MVC, maximum voluntary contraction; v/v, volume per volume; BMI, body mass index; DASH, dietary approaches to stop hypertension.
Left three columns represented the standardized description of 15 available non-pharmacological interventions for prehypertensive patients; Right three columns represented the standardized description of five non-pharmacological intervention groups (according to previous 15 specific interventions).
Outcome indicators
The main outcome indicators were changes in SBP and DBP whose follow-up time was no more than a year. We used mean differences instead of median differences as the effect size. The follow-up period of included studies did not exceed 1 year, the risk of cardiovascular events was therefore not reported. In addition, adverse events were not reported in most studies.
Data extraction
Study characteristics extracted by four researchers (THS, LYL, YQT, and WQG) were as follows: title, first author, publication date, randomization, baseline characteristics (age, sex, country, number of participants, and lost to follow-up), details of interventions, follow-up time, baseline value as well as the changes of SBP and DBP after intervention.
Risk of bias and evidence quality assessment
Two investigators (YST and YY) used the Cochrane Risk of Bias Tool 1.0 to evaluate the following items: random sequence generation, allocation concealment, blinding of outcome assessors, completeness of outcome data, selective outcome reporting, and other potential biases (29, 30). All six aspects would be evaluated as (1) low risk of bias, (2) unknown risk of bias, and (3) high risk of bias; a high-quality study should include more than four aspects with low risk of bias. However, blinding and allocation concealment would be difficult to achieve in NPIs. Therefore, we would make particular note of articles that did not involve blinding and allocation concealment but had valuable data (27).
We assessed the certainty of evidence using the grading of recommendations assessment, development and evaluation (GRADE) approach for network meta-analysis (31–35). Two people (THS and LYL) with experience in using GRADE rated each domain for each comparison separately and resolved discrepancies by consensus. We rated the certainty for each comparison and outcome as high, moderate, low, or very low, based on considerations of risk of bias, inconsistency, indirectness, publication bias, intransitivity, incoherence (difference between direct and indirect effects), and imprecision. Judgments of imprecision were made using a minimally contextualized approach, with a null effect as the threshold of importance (36). A recommended four-step approach was used in this study (35). In the first step, the effect sizes and confidence intervals of the direct evidence, indirect evidence, and network meta-analysis evidence were presented separately. In the second step, the quality of the direct evidence for each comparison group was graded without considering the imprecision. If the direct evidence was graded “high” and the contribution to the network meta-analysis results was greater than or equal to indirect evidence, no indirect evidence quality grading was required. The network meta-analysis evidence quality was directly assessed based on the direct evidence quality. Otherwise, indirect evidence quality grading was required. In the third step, based on the quality of direct evidence in the first-order loop of indirect evidence, the quality of indirect evidence was determined. The intransitivity should also be considered. In the fourth step, based on the level of direct evidence and/or indirect evidence, and considering inconsistency and imprecision, the quality of evidence for network meta-analysis was finalized and presented.
Statistical analysis
We carried out a network meta-analysis using the Bayesian framework with the same priors for the variance and effect parameters. A plausible prior for the variance parameter and a uniform prior for the effect parameter suggested in a previous study based on empirical data were used in this network meta-analysis (37). We calculated the mean difference (MD) as the effect size using the reported means and standard deviations (SD) of changes in SBP and DBP. If the original study reported the standard error (SE), we would convert it to the SD through the sample size (n):
If the changes were not reported in the article but the BP at the start and end of the follow-up period were reported, we calculated the mean and SD using the following formula recommended in the Cochrane Handbook (29):
The two most widely used models in network meta-analysis were the fixed effect model and the random effects model (38). The fixed effect model was built under the assumption of existing no heterogeneity. But this assumption was recognized to be unrealistic. If the fixed effect model was applied when heterogeneity existed, uncertainty intervals become artificially narrow. Therefore, the random effects model was preferred since it assumed and accounted for unexplained heterogeneity. In this network meta-analysis, we used a random effects model as the most appropriate and conservative method to explain the heterogeneity among the included studies (38, 39). We used a Markov chain Monte Carlo simulation with four chains with scattered initial values, a total of 50,000 iterations, and annealed after 5,000 iterations. The convergence of the model was judged by the Brooks–Gelman–Rubin method (40).
A ranking probability curve of each treatment was provided by calculating the probability of each arm to achieve the best rank among all. We judged the inconsistency by comparing the deviance information criterion (DIC) between the consistency and inconsistency models (41). Evaluating local incoherence between the direct and indirect comparisons, and obtaining indirect estimation was done by the node-splitting models (42). We calculated the Bayesian P value to estimate the measure of the conflict between direct and indirect evidence (43). The heterogeneity between studies was determined by heterogeneity analysis (including unrelated study effects model, unrelated mean effects model, and consistency model), and Q test and I2 statistic were used to reflect the heterogeneity (I2higher than 75% was considered with high heterogeneity; smaller than 25% was considered with low heterogeneity) (44).
All statistical tests were conducted as two-sided, and a P < 0.05 was considered as being statistically significant. The network meta-analysis was performed using R software (https://www.r-project.org).
Results
Study selection
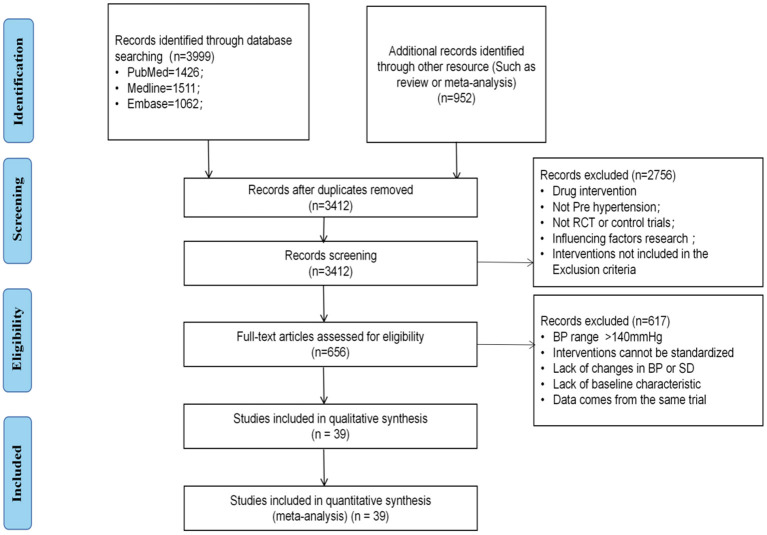
Our search identified a total of 4,951 references. After duplication, 3,412 studies underwent further analysis, of which 2,756 were excluded after reading the title or abstract and a further 617 were excluded after reading the full text. The remaining 39 studies involved 15 interventions and 8,279 patients were included in the analysis (45–83). The study flow chart is shown in Figure 1. The baseline patient characteristics are shown in the Supplementary material 2.
Figure 1.
Flow chart of literature search and article inclusion. RCT, randomized controlled trials; BP, blood pressure; SD, standard difference.
Network meta-analysis
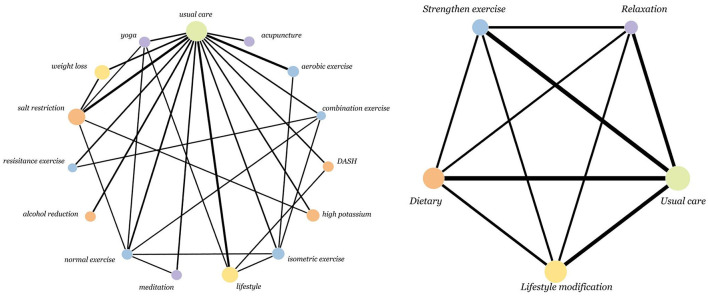
The network evidence plots for SBP and DBP were the same (as shown in Figure 2).
Figure 2.
Network of intervention treatments included in meta-analysis. The size of the nodes represents the sample size. The thickness of the lines represents the number of studies included in the comparison.
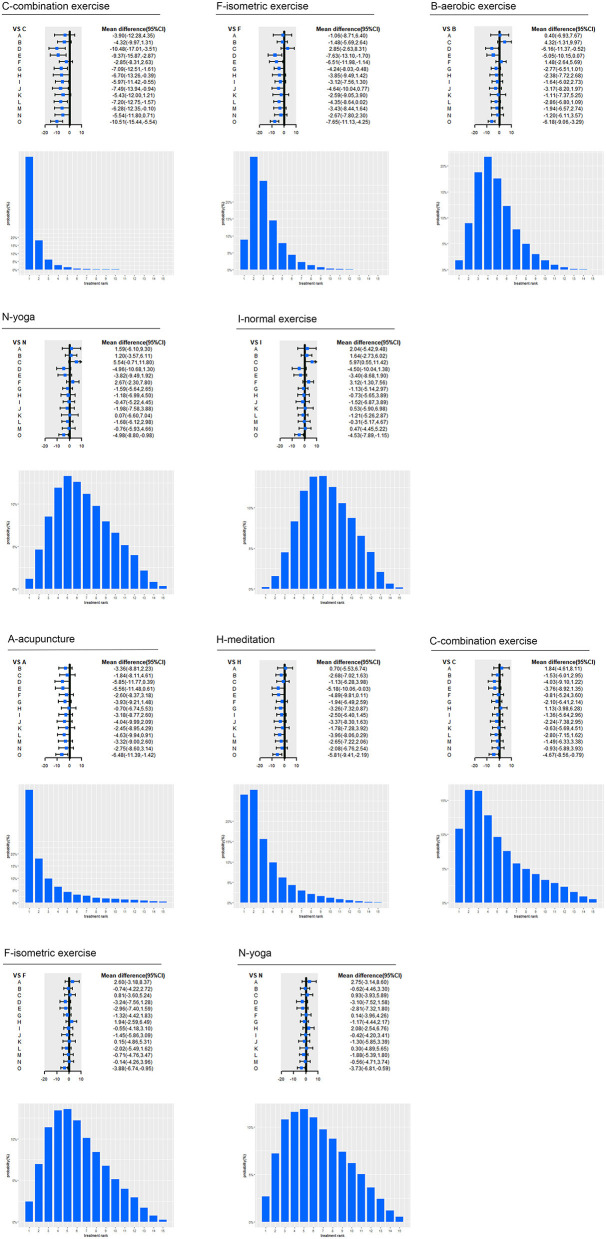
Among the included intervention strategies, combination exercise (69.71%) ranked first in the reduction of SBP, followed by isometric exercise (33.30%), aerobic exercise (18.75%), yoga (11.90%) and normal exercise (12.08%). And acupuncture (46.09%) ranked first in the reduction of DBP, followed by meditation (27.67%), combination exercise (16.39%), isometric exercise (13.42%), yoga (11.86%) (as shown in Figure 3).
Figure 3.
Effect of top five interventions on SBP and DBP. A, acupuncture; B, aerobic exercise; C, combination exercise; D, DASH; E, high Potassium; F, isometric exercise; G, lifestyle; H, meditation; I, normal exercise; J, reduced alcohol; K, resistance exercise; L, salt restriction; M, weight loss; N, yoga; O, usual care; CI, confidence interval; SBP, systolic blood pressure; DBP, diastolic blood pressure. Forest plot represents the relative effects of the other interventions with one intervention as a reference (mean difference, 95% CI, mmHg); Bar plot represents the probability of ranking of the reference intervention.
Specifically, for SBP, aerobic exercise (−6.18 mmHg, 95% CI −9.06 to −3.29; moderate certainty), combination exercise (−10.51 mmHg, −15.44 to −5.54; moderate certainty), isometric exercise (−7.65 mmHg, −11.13 to −4.25; moderate certainty), lifestyle (−3.4 mmHg, −5.89 to −0.94; moderate certainty), normal exercise (−4.53 mmHg, −7.89 to −1.15; low certainty), salt restriction (−3.3 mmHg, −6.02 to −0.7; moderate certainty), weight loss (−4.23 mmHg, −7.97 to −0.58; moderate certainty) and yoga (−4.98 mmHg, −8.8 to −0.98; low certainty) significantly lowered SBP compared with usual care. Aerobic exercise (−6.16 mmHg, −11.37 to −0.52; moderate certainty) had a significant SBP reduction compared with DASH. Combination exercise had a significant SBP reduction compared with DASH (−10.48 mmHg, −17.01 to −3.51; moderate certainty), high potassium (−9.37 mmHg, −15.87 to −2.87; moderate certainty), lifestyle (−7.09 mmHg, −12.51 to −1.61; moderate certainty), meditation (−6.7 mmHg, −13.26 to −0.39; moderate certainty), normal exercise (−5.97 mmHg, −11.42 to −0.55; low certainty), alcohol reduction (−7.49 mmHg, −13.94 to −0.94; moderate certainty), salt restriction (−7.2 mmHg, −12.75 to −1.57; moderate certainty) and weight loss (−6.28 mmHg, −12.35 to −0.1; moderate certainty). Isometric exercise significantly lowered SBP compared with lifestyle (−4.24 mmHg, −8.03 to −0.48; very low certainty), DASH (−7.63 mmHg, −13.1 to −1.7; low certainty), and high Potassium (−6.51 mmHg, −11.98 to −1.14; low certainty). For DBP, acupuncture (−6.48 mmHg, −11.39 to −1.42; moderate certainty), aerobic exercise (−3.12 mmHg, −5.51 to −0.73; moderate certainty), combination exercise (−4.67 mmHg, −8.56 to −0.79; moderate certainty), isometric exercise (−3.88 mmHg, −6.74 to −0.95; low certainty), lifestyle (−2.56 mmHg, −4.56 to −0.58; moderate certainty), meditation (−5.81 mmHg, −9.41 to −2.19; moderate certainty), normal exercise (−3.32 mmHg, −6.05 to −0.59; low certainty), weight loss (−3.16 mmHg, −6.14 to −0.29; moderate certainty) and yoga (−3.73 mmHg, −6.81 to −0.59; moderate certainty) significantly lowered BP compared with usual care. Meditation (−5.18 mmHg, −10.06 to −0.03; moderate certainty) had a significant BP reduction than DASH.
Among the categorized intervention groups, Strengthen exercise (72.54%) ranked first in the reduction of SBP, followed by relaxation (54.56%), lifestyle modification (59.6%), dietary (71.62%), and usual care (99.08%). And relaxation (87.66%) ranked first in the reduction of DBP, followed by Strengthen Exercise (61.93%), lifestyle modification (60.55%), dietary (82.34%), and usual care (98.73%).
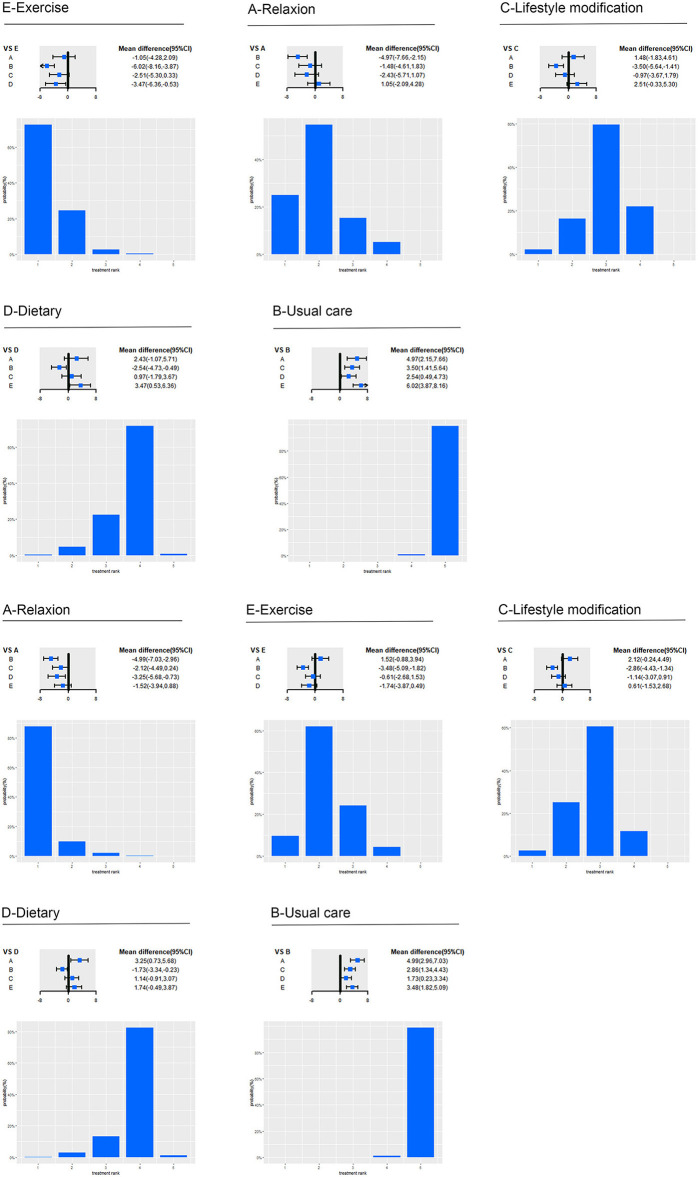
Specifically, for SBP (as shown in Figure 4), relaxation (−4.97 mmHg, −7.66 to −2.15; low certainty), lifestyle modification (−3.5 mmHg, −5.64 to −1.41; moderate certainty), dietary (−2.54 mmHg, −4.73 to −0.49; low certainty) and strengthen exercise (−6.02 mmHg, −8.16 to −3.87; low certainty) significantly reduced BP compared with usual care. Strengthen exercise (−3.47 mmHg, −6.36 to −0.53; moderate certainty) significantly reduced BP compared with dietary. For DBP, relaxation (−4.99 mmHg, −7.03 to −2.96; moderate certainty), lifestyle modification (−2.86 mmHg, −4.43 to −1.34; moderate certainty), dietary (−1.73 mmHg, −3.34 to −0.23; very low certainty) and strengthen exercise (−3.48 mmHg, −5.09 to −1.82; low certainty) significantly reduced BP compared with usual care. Relaxation (−3.25 mmHg, −5.68 to −0.73; moderate certainty) significantly reduced BP compared with dietary.
Figure 4.
Effect of five intervention groups on SBP and DBP. A, relaxation; B, usual care; C, lifestyle; D, Dietary; E, strengthen exercise; CI, confidence interval; SBP, systolic blood pressure; DBP, diastolic blood pressure. Forest plot represents the relative effects of the other intervention groups with one intervention group as a reference (mean difference, 95% CI, mmHg). Bar plot represents the probability of ranking of the reference intervention group.
Inconsistency and heterogeneity
Results of node-splitting and heterogeneity tests are shown in Supplementary material 3 for detail.
When compared among specific intervention programs, no inconsistency was found in SBP nor DBP, as indicated by the model parameters (consistency test for SBP and DBP were DIC = 162.70) and DIC = 164.43, respectively; inconsistency test for SBP and DBP were DIC = 166.97 and DIC = 167.49, respectively. The results of node-splitting analysis showed that there was no local incoherence in both of the models since every Bayesian P > 0.05.
When compared among intervention groups, no inconsistency was found in SBP nor DBP, as indicated by the model parameters (consistency test for SBP and DBP were DIC = 138.37 and DIC = 139.59, respectively; inconsistency test for SBP and DBP were DIC = 140.64 and DIC = 141.31, respectively). The results of node-splitting analysis showed that there was no local incoherence in both of the models since every Bayesian P > 0.05.
The heterogeneity test showed that there was high heterogeneity between some studies for both pair-wise pooled effects and consistency effects. Potential explanations are given in a later discussion.
Risk of bias
The specific literature quality assessment diagram and risk of bias summary are shown in Supplementary material 4. After assessing the quality of the literature by the Cochrane Handbook, we found that 27 studies reported the implementation of randomization, 8 studies reported the allocation concealment, and 15 studies reported on the implementation of blinding. There was no selective reporting bias or result bias in all studies. Because these studies were aimed at NPIs, some study designs could not apply the blinding. In summary, the quality of the articles included in this network meta-analysis was moderate. Detailed results of the certainty evaluation of evidence are shown in Supplementary material 5. Overall, most evidence was concentrated in the moderate and low grades since the existence of the risk of bias, inconsistency, indirectness, intransitivity, and imprecision.
Discussion
This study evaluated the short-term effects of 16 NPIs in patients with prehypertension. Considering the impact on community-based chronic disease-management staff and their need for professional cooperation (25), we merged 16 intervention items into five intervention groups. We evaluated the effects using a network meta-analysis with BP reduction as the outcome indicator and found that combination exercise, isometric exercise, aerobic exercise, yoga, and normal exercise were the top five in SBP reduction, and acupuncture, meditation, combination exercise, isometric exercise and yoga for DBP reduction. Also, according to our studies, sports intervention had more absolute SBP reduction and relaxation had more absolute DBP reduction than other interventions. Strengthen exercise and relaxation rank top two in both SBP and DBP reduction.
There were no inconsistencies but slight heterogeneity in this study. This was likely due to differences in the baseline characteristics (e.g., age, sex, and ethnicity) of the patients included in each study, as well as differences in the interventions adopted by each of the studies. Although the interventions share the same purpose, their contents were slightly different, given that current guidelines did not give standardized strategies for non-pharmacological intervention. Patient compliance and completion rates may also differ among studies. However, this type of heterogeneity was unavoidable.
Numerous studies have examined the short-term anti-hypertensive effects of NPIs. Williamson et al. (18) found that 3–6 months of exercise effectively reduced SBP (−4.40 mmHg, 95% CI −5.78 to −3.01) and DBP (−4.17 mmHg, 95% CI −5.42 to −2.93) in patients aged 18–40 years with both prehypertension and hypertension. Ndanuko et al. (84) conducted a meta-analysis on the BP-reducing effects of MBSR (Mindfulness-Based Stress Reduction) program in both prehypertensive and hypertensive patients and showed that MBSR reduced SBP by 6.64 mmHg and DBP by 2.47 mmHg. Khandekar et al. (85) conducted a meta-analysis of the anti-hypertensive effects of yoga and showed that both SBP (standard MD = −0.62, 95% CI −0.83 to −0.41) and DBP (standard MD = −0.81, 95% CI −1.39 to −0.22) were significantly reduced in the yoga group compared with the control group. According to Liao et al.'s study (86), massage significantly reduced SBP (−7.39 mmHg) and DBP (−5.04 mmHg) in people with both prehypertension and hypertension. Fu et al. (20) reported that the DASH diet was most effective for adults with prehypertension to established hypertension, followed by aerobic exercise and isometric training, which also had obvious effects on BP reduction. Population in current evidence are hypertensive patients or combined with prehypertensive people. Population in current evidence are hypertensive patients or combined with prehypertensive people. Pooled evidence studies target on the BP reduction effect of NPIs in prehypertensive people were lacking. In addition, current studies of the anti-hypertensive effects of NPIs have tended to target one specific intervention. So the current results filled a gap in proving and comparing the short-term effects of NPIs in people with prehypertension.
This was the first study to evaluate the short-term efficacy of NPIs in prehypertensive people. Our results not only supplemented existing evidence in this area but also had important implications for the management of chronic diseases in countries who had a high disease burden of hypertension but with limited medical resources and community-based chronic disease-management staff. Early prevention of hypertension through NPIs can be a potential way to reduce the disease burden. This meant that government administrators in these countries can start to initiate training programs that could reduce the BP of people with prehypertension effectively for community-based chronic disease-management staff to be prepared. For decision-makers, a comprehensive analysis of which types of interventions could be more effective will provide useful evidence to make the optimal health decision. In this study, strengthen exercise and relaxation, which could bring more short-term BP reduction than other interventions according to current evidence, may be considered the priority for government administrators and community-based chronic disease-management staff. Nevertheless, long-term effects of these NPIs with great short-term BP reduction benefits should be further examined (including the number of CVD events avoided), which can provide more evidence for decision-makers.
It is necessary to note that this study is not without shortcomings. First, the standardization of interventions in this study was carried out following the guidelines, still it may leave to subjectivity. Second, due to differences in population baseline of included studies, the heterogeneity could not be avoided. Therefore, in our certainty of the evidence analysis, most comparisons were downgraded in the indirectness of evidence due to the differences in population and intervention. Third, since individual patient data were not available, subgroup analyses were not conducted in this study. However, the heterogeneity caused by some key subgroups (e.g., baseline blood pressure, age) should not be ignored. Fourth, since long-term studies were lacking, only BP change could be selected as the outcome indicator in this study. Without outcome indicators like cardiovascular events or hypertension progression, long-term real-world effectiveness of NPIs could not be recognized. Even though we had proved that NPIs are effective for prehypertensive people, whether they are cost-effective was still unknown. For further research, more high-quality research with long-term outcome projections should be published to fill the gap in this field. Studies are needed to target people with different clinical characteristics. Empirical studies on the inputs and outputs of NPIs in prehypertensive people are also needed to explore the cost-effectiveness and feasibility of implementation in a specific region.
Conclusion
To date, there is no systematic study revealing the comparative effects of NPIs for prehypertensive patients. Our study indicates that strengthening exercise (including combination exercise, isometric exercise and aerobic exercise) and relaxation (including acupuncture, meditation, and yoga) have potential to be educated and applied in community-based chronic disease management. This will provide evidence for countries who have a high disease burden of hypertension but with limited medical resources and staff to prevent or delay the disease progression from prehypertension to hypertension. However, to have a decision on whether prehypertensive patients should be regularly managed and which strategy to be considered, further studies on cost-effectiveness and affordability are needed.
Data availability statement
The original contributions presented in the study are included in the article/Supplementary material, further inquiries can be directed to the corresponding authors.
Author contributions
WT and TS designed the study and interpreted findings. TS and LL wrote initial drafts of the manuscript, developed the model, performed all model analyses, and visualized the data. TS, LL, YTa, WG, YTu, and YY conducted the literature search, screen, and extract the data. TS, LL, CZ, WT, and DM revised and polished the initial manuscript drafts. All authors reviewed the manuscript. All authors had full access to all the data in the study and the corresponding authors had final responsibility for the decision to submit for publication.
Acknowledgments
We thank Susan Furness, PhD, from Liwen Bianji (Edanz) (www.liwenbianji.cn), for basic language editing of a draft of this manuscript.
Funding Statement
This work was supported by General Program of National Natural Science Foundation of China (72174207).
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Publisher's note
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article, or claim that may be made by its manufacturer, is not guaranteed or endorsed by the publisher.
Supplementary material
The Supplementary Material for this article can be found online at: https://www.frontiersin.org/articles/10.3389/fpubh.2022.1051581/full#supplementary-material
Search strategies of this study. Including reverse search and forward search.
Main characteristics of included trials.
Results of node-splitting and heterogeneity test.
“Quality assessment diagram” and “Risk of bias summary.”
Detailed results of the certainty of the evidence analysis.
References
- 1.Gakidou E, Afshin A, Abajobir AA, Abate KH, Abbafati C, Abbas KM, et al. Global, regional, and national comparative risk assessment of 84 behavioural, environmental and occupational, and metabolic risks or clusters of risks, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet. (2017) 390:1345–422. 10.1016/S0140-6736(17)32366-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Forouzanfar MH, Liu P, Roth GA, Ng M, Biryukov S, Marczak L, et al. Global burden of hypertension and systolic blood pressure of at least 110 to 115 mm Hg, 1990–2015. JAMA J Am Med Assoc. (2017) 317:165–82. 10.1001/jama.2016.19043 [DOI] [PubMed] [Google Scholar]
- 3.Rahimi K, Emdin CA, MacMahon S. The epidemiology of blood pressure and its worldwide management. Circ Res. (2015) 116:925–36. 10.1161/CIRCRESAHA.116.304723 [DOI] [PubMed] [Google Scholar]
- 4.Egan BM, Stevens-Fabry S. Prehypertension–prevalence, health risks, and management strategies. Nat Rev Cardiol. (2015) 12:289–300. 10.1038/nrcardio.2015.17 [DOI] [PubMed] [Google Scholar]
- 5.Izzo R, Mancusi C, de Simone G. Are we underestimating prehypertension? Hypertension. (2019) 73:541–2. 10.1161/HYPERTENSIONAHA.118.12310 [DOI] [PubMed] [Google Scholar]
- 6.Foldes C, Fisher JW. Hypertension. Ann Intern Med. (2019) 171:525. 10.7326/L19-0447 [DOI] [PubMed] [Google Scholar]
- 7.Kanegae H, Oikawa T, Kario K. Should pre-hypertension be treated? Curr Hypertens Rep. (2017) 19:91. 10.1007/s11906-017-0789-z [DOI] [PubMed] [Google Scholar]
- 8.Materson BJ, Garcia-Estrada M, Degraff SB, Preston RA. Prehypertension is real and can be associated with target organ damage. J Am Soc Hypertens. (2017) 11:704–8. 10.1016/j.jash.2017.09.005 [DOI] [PubMed] [Google Scholar]
- 9.National Cardiovascular Disease Center Office . National basic hypertension prevention and management guidelines 2020 edition. China Recycling Magazine. (2021) 36:209–20. 10.12037/YXQY.2021.04-06 [DOI] [Google Scholar]
- 10.Whelton PK, Carey RM, Aronow WS, Casey DE, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Hypertension. (2018) 71:65. 10.1161/HYP.0000000000000065 [DOI] [PubMed] [Google Scholar]
- 11.Hong D, Shan W. Improvement in hypertension management with pharmacological and non-pharmacological approaches: current perspectives. Curr Pharm Design. (2021) 27:548–55. 10.2174/1381612826666200922153045 [DOI] [PubMed] [Google Scholar]
- 12.Intarakamhang U, Macaskill A, Prasittichok P. Mindfulness interventions reduce blood pressure in patients with non-communicable diseases: a systematic review and meta-analysis. Heliyon. (2020) 6:e3834. 10.1016/j.heliyon.2020.e03834 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Verma N, Rastogi S, Chia YC, Siddique S, Turana Y, Cheng HM, et al. Non-pharmacological management of hypertension. J Clin Hypertens. (2021) 23:1275–83. 10.1111/jch.14236 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Zhou YF, Liu N, Wang P, Jeong YJ, Song XY, Pan XF, et al. Cost-effectiveness of drug treatment for chinese patients with stage I hypertension according to the 2017 hypertension clinical practice guidelines. Hypertension. (2020) 76:750–8. 10.1161/HYPERTENSIONAHA.119.14533 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Herrod P, Doleman B, Blackwell J, O'Boyle F, Williams JP, Lund JN, et al. Exercise and other nonpharmacological strategies to reduce blood pressure in older adults: a systematic review and meta-analysis. J Am Soc Hypertens. (2018) 12:248–67. 10.1016/j.jash.2018.01.008 [DOI] [PubMed] [Google Scholar]
- 16.Park S, Han KS. Blood pressure response to meditation and yoga: a systematic review and meta-analysis. J Altern Complement Med. (2017) 23:685–95. 10.1089/acm.2016.0234 [DOI] [PubMed] [Google Scholar]
- 17.Patnode CD, Evans CV, Senger CA, Redmond N, Lin JS. Behavioral counseling to promote a healthful diet and physical activity for cardiovascular disease prevention in adults without known cardiovascular disease risk factors. JAMA J Am Med Assoc. (2017) 318:175. 10.1001/jama.2017.3303 [DOI] [PubMed] [Google Scholar]
- 18.Williamson W, Foster C, Reid H, Kelly P, Lewandowski AJ, Boardman H, et al. Will exercise advice be sufficient for treatment of young adults with prehypertension and hypertension? A systematic review and meta-analysis. Hypertension. (2016) 68:78–87. 10.1161/HYPERTENSIONAHA.116.07431 [DOI] [PubMed] [Google Scholar]
- 19.Li W, Chen D, Liu S, Wang X, Chen X, Chen J, et al. The rates and the determinants of hypertension according to the 2017 definition of hypertension by ACC/AHA and 2014 evidence-based guidelines among population aged ≥40 years old. Glob Heart. (2021) 16:34. 10.5334/gh.914 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Fu J, Liu Y, Zhang L, Zhou L, Li D, Quan H, et al. Nonpharmacologic interventions for reducing blood pressure in adults with prehypertension to established hypertension. J Am Heart Assoc. (2020) 9:e16804. 10.1161/JAHA.120.016804 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Mills KT, Stefanescu A, He J. The global epidemiology of hypertension. Nat Rev Nephrol. (2020) 16:223–37. 10.1038/s41581-019-0244-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Dhungana RR, Pedisic Z, de Courten M. Implementation of non-pharmacological interventions for the treatment of hypertension in primary care: a narrative review of effectiveness, cost-effectiveness, barriers, and facilitators. BMC Prim Care. (2022) 23:298. 10.1186/s12875-022-01884-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Anderson P, Bendtsen P, Spak F, Reynolds J, Drummond C, Segura L, et al. Improving the delivery of brief interventions for heavy drinking in primary health care: outcome results of the Optimizing Delivery of Health Care Intervention (ODHIN) five-country cluster randomized factorial trial. Addiction. (2016) 111:1935–45. 10.1111/add.13476 [DOI] [PubMed] [Google Scholar]
- 24.Morgan F, Battersby A, Weightman AL, Searchfield L, Turley R, Morgan H, et al. Adherence to exercise referral schemes by participants—what do providers and commissioners need to know? A systematic review of barriers and facilitators. BMC Public Health. (2016) 16:227. 10.1186/s12889-016-2882-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Anand TN, Joseph LM, Geetha AV, Prabhakaran D, Jeemon P. Task sharing with non-physician health-care workers for management of blood pressure in low-income and middle-income countries: a systematic review and meta-analysis. Lancet Glob Health. (2019) 7:e761–71. 10.1016/S2214-109X(19)30077-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev Lond. (2015) 4:1. 10.1186/2046-4053-4-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Shao T, Li X, Zhou C, Zang X, Malone DC, Zhang L, et al. Effectiveness and efficiency of non-drug therapy among community-dwelling adults with hypertension in China: a protocol for network meta-analysis and cost-effectiveness analysis. Front Med-Lausanne. (2021) 8:651559. 10.3389/fmed.2021.651559 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Mahmood S, Shah KU, Khan TM, Nawaz S, Rashid H, Baqar S, et al. Non-pharmacological management of hypertension: in the light of current research. Irish J Med Sci. (2019) 188:437–52. 10.1007/s11845-018-1889-8 [DOI] [PubMed] [Google Scholar]
- 29.Higgins JP, Green S. Cochrane Handbook for Systematic Reviews of Interventions. Hoboken, NJ: Wiley-Blackwell; (2008). [Google Scholar]
- 30.Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, et al. The Cochrane Collaboration's tool for assessing risk of bias in randomised trials. BMJ Brit Med J. (2011) 343:d5928. 10.1136/bmj.d5928 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Brignardello-Petersen R, Bonner A, Alexander PE, Siemieniuk RA, Furukawa TA, Rochwerg B, et al. Advances in the GRADE approach to rate the certainty in estimates from a network meta-analysis. J Clin Epidemiol. (2018) 93:36–44. 10.1016/j.jclinepi.2017.10.005 [DOI] [PubMed] [Google Scholar]
- 32.Bonner A, Alexander PE, Brignardello-Petersen R, Furukawa TA, Siemieniuk RA, Zhang Y, et al. Applying GRADE to a network meta-analysis of antidepressants led to more conservative conclusions. J Clin Epidemiol. (2018) 102:87–98. 10.1016/j.jclinepi.2018.05.009 [DOI] [PubMed] [Google Scholar]
- 33.Brignardello-Petersen R, Mustafa RA, Siemieniuk R, Murad MH, Agoritsas T, Izcovich A, et al. GRADE approach to rate the certainty from a network meta-analysis: addressing incoherence. J Clin Epidemiol. (2019) 108:77–85. 10.1016/j.jclinepi.2018.11.025 [DOI] [PubMed] [Google Scholar]
- 34.Brignardello-Petersen R, Murad MH, Walter SD, McLeod S, Carrasco-Labra A, Rochwerg B, et al. GRADE approach to rate the certainty from a network meta-analysis: avoiding spurious judgments of imprecision in sparse networks. J Clin Epidemiol. (2019) 105:60–7. 10.1016/j.jclinepi.2018.08.022 [DOI] [PubMed] [Google Scholar]
- 35.Puhan MA, Schunemann HJ, Murad MH Li T, Brignardello-Petersen R, Singh JA, et al. A GRADE Working Group approach for rating the quality of treatment effect estimates from network meta-analysis. BMJ Brit Med J. (2014) 349:g5630. 10.1136/bmj.g5630 [DOI] [PubMed] [Google Scholar]
- 36.Hultcrantz M, Rind D, Akl EA, Treweek S, Mustafa RA, Iorio A, et al. The GRADE Working Group clarifies the construct of certainty of evidence. J Clin Epidemiol. (2017) 87:4–13. 10.1016/j.jclinepi.2017.05.006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Turner RM, Jackson D, Wei Y, Thompson SG, Higgins JP. Predictive distributions for between-study heterogeneity and simple methods for their application in Bayesian meta-analysis. Stat Med. (2015) 34:984–98. 10.1002/sim.6381 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Mills EJ, Thorlund K, Ioannidis JP. Demystifying trial networks and network meta-analysis. BMJ Brit Med J. (2013) 346:f2914. 10.1136/bmj.f2914 [DOI] [PubMed] [Google Scholar]
- 39.Dias S, Welton NJ, Sutton AJ, Caldwell DM, Lu G, Ades AE. Evidence synthesis for decision making 4: inconsistency in networks of evidence based on randomized controlled trials. Med Decis Making. (2013) 33:641–56. 10.1177/0272989X12455847 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Brooks SP, Gelman A. General methods for monitoring convergence of iterative simulations. J Comput Graph Stat. (1998) 7:434–55. 10.2307/1390675 [DOI] [Google Scholar]
- 41.Mason A, Richardson S, Best N. Using DIC to Compare Selection Models With Non-Ignorable Missing Responses. Southampton: National Centre for Research Methods; (2010). [Google Scholar]
- 42.van Valkenhoef G, Dias S, Ades AE, Welton NJ. Automated generation of node-splitting models for assessment of inconsistency in network meta-analysis. Res Synth Methods. (2016) 7:80–93. 10.1002/jrsm.1167 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Dias S, Welton NJ, Caldwell DM, Ades AE. Checking consistency in mixed treatment comparison meta-analysis. Stat Med. (2010) 29:932–44. 10.1002/sim.3767 [DOI] [PubMed] [Google Scholar]
- 44.Van Valkenhoef G, Kuiper J., gemtc. (2021). Available online at: https://cran.r-project.org/web/packages/gemtc/gemtc.pdf (accessed December 3, 2022).
- 45.Seo B, Kwon O, Lee S, Kim H, Kang K, Seol IC, et al. Effects of acupuncture on lowering blood pressure in postmenopausal women with prehypertension or stage 1 hypertension: A propensity score-matched analysis. J Clin Med. (2021) 10:1426. 10.3390/jcm10071426 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Son W, Pekas EJ, Park S. Twelve weeks of resistance band exercise training improves age-associated hormonal decline, blood pressure, and body composition in postmenopausal women with stage 1 hypertension: a randomized clinical trial. Menopause. (2020) 27:199–207. 10.1097/GME.0000000000001444 [DOI] [PubMed] [Google Scholar]
- 47.Tantiprasoplap S, Piaseu N, Kanungsukkasem V, Taneepanichskul S. A randomized controlled trial comparing the effects of an arm swing exercise and low sodium intake education program with low sodium intake education alone on cardiovascular outcomes in postmenopausal women with prehypertension. J Med Assoc Thailand. (2020) 103:22–31. [Google Scholar]
- 48.Ankolekar VH, Reddy GG, Sanju CSV, Mamatha H. Role of yoga intervention on quality of life and prehypertension. Indian J Tradit Know. (2019) 18:351–5. [Google Scholar]
- 49.Ogbutor GU, Nwangwa EK, Uyagu DD. Isometric handgrip exercise training attenuates blood pressure in prehypertensive subjects at 30% maximum voluntary contraction. Niger J Clin Pract. (2019) 22:1765. 10.4103/njcp.njcp_240_18 [DOI] [PubMed] [Google Scholar]
- 50.Pengpid S, Peltzer K, Puckpinyo A, Chantarasongsuk IJ. Effectiveness of a cluster-randomized controlled trial community-based lifestyle intervention program to control prehypertension and/or prediabetes in Thailand. Int J Diabetes Dev C. (2019) 39:123–31. 10.1007/s13410-018-0641-2 [DOI] [Google Scholar]
- 51.Shin K, Park J, Yook T, Kim J, Kwon O, Choi S. Moxibustion for prehypertension and stage I hypertension: a pilot randomized controlled trial. Integr Med Res. (2019) 8:1–7. 10.1016/j.imr.2018.11.002 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Taylor KA, Wiles JD, Coleman DA, Leeson P, Sharma R, O Driscoll JM. Neurohumoral and ambulatory haemodynamic adaptations following isometric exercise training in unmedicated hypertensive patients. J Hypertens. (2019) 37:827–36. 10.1097/HJH.0000000000001922 [DOI] [PubMed] [Google Scholar]
- 53.Ponte Márquez PH, Feliu-Soler A, Solé-Villa MJ, Matas-Pericas L, Filella-Agullo D, Ruiz-Herrerias M, et al. Benefits of mindfulness meditation in reducing blood pressure and stress in patients with arterial hypertension. J Hum Hypertens. (2019) 33:237–47. 10.1038/s41371-018-0130-6 [DOI] [PubMed] [Google Scholar]
- 54.Glodzik J, Rewiuk K, Adamiak J, Marchewka J, Salakowski A, Mazur M, et al. Controlled aerobic training improves endothelial function and modifies vascular remodeling in healthy adults with high normal blood pressure. J Physiol Pharmacol. (2018) 69:699–707. 10.26402/jpp.2018.5.04 [DOI] [PubMed] [Google Scholar]
- 55.Goessler KF, Buys R, VanderTrappen D, Vanhumbeeck L, Cornelissen VA. A randomized controlled trial comparing home-based isometric handgrip exercise versus endurance training for blood pressure management. J Am Soc Hypertens. (2018) 12:285–93. 10.1016/j.jash.2018.01.007 [DOI] [PubMed] [Google Scholar]
- 56.Juraschek SP, White K, Tang O, Yeh H, Cooper LA, Miller ER. Effects of a dietary approach to stop hypertension (DASH) diet intervention on serum uric acid in African Americans with hypertension. Arthrit Care Res. (2018) 70:1509–16. 10.1002/acr.23515 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Neupane D, McLachlan CS, Mishra SR, Olsen MH, Perry HB, Karki A, et al. Effectiveness of a lifestyle intervention led by female community health volunteers versus usual care in blood pressure reduction (COBIN): an open-label, cluster-randomised trial. Lancet Glob Health. (2018) 6:e66–73. 10.1016/S2214-109X(17)30411-4 [DOI] [PubMed] [Google Scholar]
- 58.Staffileno BA, Tangney CC, Fogg L. Favorable outcomes using an ehealth approach to promote physical activity and nutrition among young African American women. J Cardiovasc Nurs. (2018) 33:62–71. 10.1097/JCN.0000000000000409 [DOI] [PubMed] [Google Scholar]
- 59.Allaert F. Effect of NaCl + Chitosan 3% vs. NaCl on high blood pressure parameters of healthy volunteers with prehypertension. Minerva Cardiol Angi. (2017) 65:563–76. 10.23736/S0026-4725.17.04451-6 [DOI] [PubMed] [Google Scholar]
- 60.Azadpour N, Tartibian B, Koşar SN. Effects of aerobic exercise training on ACE and ADRB2 gene expression, plasma angiotensin II level, and flow-mediated dilation: a study on obese postmenopausal women with prehypertension. Menopause. (2017) 24:269–77. 10.1097/GME.0000000000000762 [DOI] [PubMed] [Google Scholar]
- 61.Baross AW, Hodgson DA, Padfield SL, Swaine IL. Reductions in resting blood pressure in young adults when isometric exercise is performed whilst walking. J Sports Med. (2017) 2017:1–6. 10.1155/2017/7123834 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Naseem S, Ghazanfar H, Assad S, Ghazanfar A. Role of sodium-restricted dietary approaches to control blood pressure in Pakistani hypertensive population. J Pak Med Assoc. (2016) 66:837–42. [PubMed] [Google Scholar]
- 63.Rubinstein A, Miranda JJ, Beratarrechea A, Diez-Canseco F, Kanter R, Gutierrez L, et al. Effectiveness of an mHealth intervention to improve the cardiometabolic profile of people with prehypertension in low-resource urban settings in Latin America: a randomised controlled trial. Lancet Diab Endocrinol. (2016) 4:52–63. 10.1016/S2213-8587(15)00381-2 [DOI] [PubMed] [Google Scholar]
- 64.Thiyagarajan R, Pal P, Pal GK, Subramanian SK, Trakroo M, Bobby Z, et al. Additional benefit of yoga to standard lifestyle modification on blood pressure in prehypertensive subjects: a randomized controlled study. Hypertens Res. (2015) 38:48–55. 10.1038/hr.2014.126 [DOI] [PubMed] [Google Scholar]
- 65.Lim S, Min S, Kwon Y, Park S, Park H. Effects of intermittent exercise on biomarkers of cardiovascular risk in night shift workers. Atherosclerosis. (2015) 242:186–90. 10.1016/j.atherosclerosis.2015.06.017 [DOI] [PubMed] [Google Scholar]
- 66.Beck DT, Martin JS, Casey DP, Braith RW. Exercise training improves endothelial function in resistance arteries of young prehypertensives. J Hum Hypertens. (2014) 28:303–9. 10.1038/jhh.2013.109 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Zhao XS, Wang R, Bin LR, Wa SQG. Intervention for prehypertension and its cardiovascular risk factors in Inner Mongolia. Genet Mol Res. (2014) 13:4867–82. 10.4238/2014.July.4.1 [DOI] [PubMed] [Google Scholar]
- 68.Kamalakkannan K, Kumar SM. Effect of land and shallow water aerobic exercises on selected physiological and biochemical variables of obese adult. J Phys Educ Sport. (2014) 14:532. 10.7752/jpes.2014.04082 [DOI] [Google Scholar]
- 69.Hughes JW, Fresco DM, Myerscough RH, Van Dulmen M, Carlson LE, Josephson R. Randomized controlled trial of mindfulness-based stress reduction for prehypertension. Psychosom Med. (2013) 75:721–8. 10.1097/PSY.0b013e3182a3e4e5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Kim J, Kim D. Effects of aerobic exercise training on serum sex hormone binding globulin, body fat index, and metabolic syndrome factors in obese postmenopausal women. Metab Syndr Relat D. (2012) 10:452–7. 10.1089/met.2012.0036 [DOI] [PubMed] [Google Scholar]
- 71.Marquez-Celedonio FG, Texon-Fernandez O, Chavez-Negrete A, Hernandez-Lopez S, Marin-Rendon S, Berlin-Lascurain S. Clinical effect of lifestyle modification on cardiovascular risk in prehypertensives: PREHIPER I study. Rev Esp Cardiol. (2009) 62:86–90. 10.1016/S0300-8932(09)70025-9 [DOI] [PubMed] [Google Scholar]
- 72.Saptharishi L, Soudarssanane M, Thiruselvakumar D, Navasakthi D, Mathanraj S, Karthigeyan M, et al. Community-based randomized controlled trial of non-pharmacological interventions in prevention and control of hypertension among young adults. Indian J Commun Med. (2009) 34:329–34. 10.4103/0970-0218.58393 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Zilkens RR, Rich L, Burke V, Beilin LJ, Watts GF, Puddey IB. Effects of alcohol intake on endothelial function in men: a randomized controlled trial. J Hypertens. (2003) 21:97–103. 10.1097/00004872-200301000-00019 [DOI] [PubMed] [Google Scholar]
- 74.Rakic V, Puddey IB, Burke V, Dimmitt SB, Beilin LJ. Influence of pattern of alcohol intake on blood pressure in regular drinkers: a controlled trial. J Hypertens. (1998) 16:165–74. 10.1097/00004872-199816020-00006 [DOI] [PubMed] [Google Scholar]
- 75.Jessup JV, Lowenthal DT, Pollock ML, Turner T. The effects of endurance exercise training on ambulatory blood pressure in normotensive older adults. Geriatr Nephrol Urol. (1998) 8:103–9. 10.1023/a:1008287320868 [DOI] [PubMed] [Google Scholar]
- 76.Wenneberg SR, Schneider RH, Walton KG, Maclean CRK, Levitsky DK, Salerno JW, et al. A controlled study of the effects of the transcendental meditation® program on cardiovascular reactivity and ambulatory blood pressure. Int J Neurosci. (1997) 89:15–28. 10.3109/00207459708988461 [DOI] [PubMed] [Google Scholar]
- 77.The Trials of Hypertension Prevention Collaborative Research Group . Effects of weight loss and sodium reduction intervention on blood pressure and hypertension incidence in overweight people with high-normal blood pressure. The Trials of Hypertension Prevention, phase II. Arch Intern Med. (1997) 157:657–67. [PubMed] [Google Scholar]
- 78.Anderssen S, Holme I, Urdal P, Hjermann I. Diet and exercise intervention have favourable effects on blood pressure in mild hypertensives: the Oslo Diet and Exercise Study (ODES). Blood Press. (1995) 4:343. [DOI] [PubMed] [Google Scholar]
- 79.Whelton PK, Buring J, Borhani NO, Cohen JD, Cook N, Cutler JA, et al. The effect of potassium supplementation in persons with a high-normal blood pressure: results from phase I of the Trials of Hypertension Prevention (TOHP) Trials of Hypertension Prevention (TOHP) Collaborative Research Group. Ann Epidemiol. (1995) 5:85–95. 10.1016/1047-2797(94)00053-v [DOI] [PubMed] [Google Scholar]
- 80.Stevens VJ, Corrigan SA, Obarzanek E, Bernauer E, Cook NR, Hebert P, et al. Weight loss intervention in phase 1 of the trials of hypertension prevention the TOHP Collaborative Research Group. Arch Intern Med. (1993) 153:849–58. [PubMed] [Google Scholar]
- 81.Puddey IB, Parker M, Beilin LJ, Vandongen R, Masarei JRL. Effects of alcohol and caloric restrictions on blood pressure and serum lipids in overweight men. Hypertension (Dallas, Tex. 1979). (1992) 20:533–41. 10.1161/01.HYP.20.4.533 [DOI] [PubMed] [Google Scholar]
- 82.Hypertension Prevention Trial Research Group . The Hypertension Prevention Trial: three-year effects of dietary changes on blood pressure. Arch Intern Med. (1990) 150:153–62. [PubMed] [Google Scholar]
- 83.Puska P, Iacono JM, Nissinen A, Korhonen HJ, Vartianinen E, Pietinen P, et al. Controlled, randomised trial of the effect of dietary fat on blood pressure. Lancet. (1983) 1:1–5. 10.1016/s0140-6736(83)91556-8 [DOI] [PubMed] [Google Scholar]
- 84.Lee E, Yeung N, Xu Z, Zhang D, Yu CP, Wong S. Effect and acceptability of mindfulness-based stress reduction program on patients with elevated blood pressure or hypertension: a meta-analysis of randomized controlled trials. Hypertension. (2020) 76:1992–2001. 10.1161/HYPERTENSIONAHA.120.16160 [DOI] [PubMed] [Google Scholar]
- 85.Khandekar JS, Vasavi VL, Singh VP, Samuel SR, Sudhan SG, Khandelwal B. Effect of yoga on blood pressure in prehypertension: a systematic review and meta-analysis. ScientificWorldJournal. (2021) 2021:4039364. 10.1155/2021/4039364 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Liao IC, Chen SL, Wang MY, Tsai PS. Effects of massage on blood pressure in patients with hypertension and prehypertension: a meta-analysis of randomized controlled trials. J Cardiovasc Nurs. (2016) 31:73–83. 10.1097/JCN.0000000000000217 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Search strategies of this study. Including reverse search and forward search.
Main characteristics of included trials.
Results of node-splitting and heterogeneity test.
“Quality assessment diagram” and “Risk of bias summary.”
Detailed results of the certainty of the evidence analysis.
Data Availability Statement
The original contributions presented in the study are included in the article/Supplementary material, further inquiries can be directed to the corresponding authors.