Abstract
Objective:
The study aimed to assess the magnitude and factors associated with comprehensive knowledge of HIV/AIDS among pregnant mothers attending antenatal care (ANC) services at health institutions in Arsi zone, Oromia Regional State, Ethiopia.
Methods:
The study employed a health facility-based cross-sectional study design from 18 March to 25 June 2019. Out of an estimated sample size of 4481, a total of 4440 (92.23%) pregnant women were selected by multistage random sampling technique and interviewed. Multivariable binary logistic regression was used to identify the factors associated with comprehensive knowledge of HIV/AIDS. The model fitness was tested by Hosmer and Lemeshow goodness of fit, which provided a p value of 0.72 and deviance reduced (i.e., −2log likelihood was reduced from 5580.38 to 5069.55 with a p value of 0.000).
Results:
Out of the total mothers (4440) interviewed, only 1430 (32.2%; 95% confidence interval: (30.83%, 33.60%)) had comprehensive knowledge about HIV/AIDS. Not knowing safe period to be pregnant (adjusted odds ratio = 0.67; 95% confidence interval: 0.56, 0.81), and not empowering women’s for sexual practice (adjusted odds ratio = 0.50; 95% confidence interval: 0.43, 0.58) let women have less comprehensive knowledge while women who never educated about the sexual matter (adjusted odds ratio = 1.65; 95% confidence interval: 1.42, 1.92), who had a discouraging attitude toward having multiple partners (adjusted odds ratio = 1.53; 95% confidence interval: 1.24, 1.88), who had a discouraging attitude toward premarital sex (adjusted odds ratio = 1.68; 95% confidence interval: 1.38, 2.03), and who had a positive attitude toward accepting HIV/AIDS patients (2.69; 95% confidence interval: 2.34, 3.10) had more comprehensive knowledge of HIV/AIDS.
Conclusion:
Only about one-third (32.2%) of pregnant mothers on ANC follow-up had comprehensive knowledge. Thus, it would be better if the health institutions emphasize educating the mothers attending antenatal care follow-up about HIV/AIDS, for those who do not know pregnancy occurrence date, not empowered of sexual practice, and had an encouraging attitude toward multiple partners, premarital sex, and negative attitude toward accepting HIV/AIDS patients.
Keywords: Comprehensive knowledge of HIV/AIDS, mothers’ HIV/AIDS knowledge, mothers attending ANC
Introduction
Worldwide, mother-to-child transmission (MTCT) of HIV is a significant contributor to the HIV pandemic, accounting for 9% of new infections. The Joint United Nations Programme on HIV/AIDS reported that in 2016 an estimated 160,000 children were newly infected with HIV, and an estimated 3.1 million children were living with HIV globally.1 Although this is still a large number of new infections, at the peak of the HIV epidemic, there were close to 500,000 children infected with HIV through MTCT each year. MTCT of HIV occurs when HIV is transmitted from a woman living with HIV to her baby during pregnancy, labor or delivery, or after delivery through breastfeeding.
Without treatment, approximately 15%–30% of infants born to HIV-positive women will become infected with HIV during gestation and delivery, with a further 5%–15% becoming infected through breastfeeding.2 However, the 2021 Ethiopian guideline of Prevention of Mother to Child Transmission (PMTCT) revealed that the transmission rate was 10%–15%, 35%–40%, and 35%–40% during pregnancy, labor and delivery, and breastfeeding, respectively.3
An estimated 1.3 million women living with HIV become pregnant every year.4 The World Health Organization has developed a campaign aimed at almost eliminating pediatric HIV to reduce the danger of MTCT. A four-pronged approach is implemented as part of the virtual elimination of HIV in children. Primary prevention of HIV infection in women of childbearing age; preventing unintended pregnancies among HIV-positive women; preventing HIV transmission from a woman living with HIV to her infant; and providing appropriate treatment, care, and support to HIV-positive mothers, their children, and their families are among the approaches.5 One of the greatest challenges in preventing HIV transmission from mother to child is a lack of awareness and knowledge about the MTCT and PMTCT. Mothers’ understanding of PMTCT, in particular, plays an important role in implementing preventive measures and utilizing the service.6
Ethiopia has been implementing the PMTCT program since 2001 focusing on equitable access to services without any discrimination (Equity), upholding the right of all persons to the highest attainable standard of health, which includes Antiretroviral therapy (ART), PMTCT, and access to family planning information and services. Respecting the right of persons with HIV to decide on the number and timing of their children (human rights); integrating PMTCT with all appropriate services (Integration); using PMTCT as an entry point to HIV care for family (Family Focused); Prioritization of pregnant women with advanced disease to Highly active antiretroviral therapy (HAART); setting the essential PMTCT package of services as standard for all sectors (Standardization); the health networking of facilities and the community to reduce gaps in coverage (i.e., health centers to hospitals and community to health care facilities) (Referral linkages); HIV counseling and testing services after adequate information and voluntarily following informed consent (Confidentiality and voluntary informed consent); involving the community in offering prevention, treatment, care, and support (Community participation and mobilization); and encouraging male partners and fathers to participate in PMTCT programs and services (Male involvement).3,7
Comprehensive knowledge about HIV/AIDS was considered as knowing that consistent use of condoms during sexual intercourse and having just one uninfected faithful partner can reduce the chance of getting the AIDS virus, knowing that a healthy-looking person can have the AIDS virus.8–10
HIV prevalence depends on the knowledge of preventive actions, the attitude toward the disease, and people’s sexual behaviors.11,12 Studies conducted in different areas of Ethiopia indicated different levels of comprehensive knowledge. It was indicated that 24.5%, 25%, and 35.5% in Eastern Ethiopia (Hararge Zone) among in-school youths,9 Western Ethiopia (Wayu Tuka District) among out-of-school youths,13 and Mekelle city among secondary school students,14 respectively. The Ethiopian demographic and health survey 2016 (Ethiopian Demography and Health Survey (EDHS 2016) indicated 20.5% comprehensive knowledge among women aged 15–49 years which fluctuated from one group to the other, ranging from 3.5% in the Somali region to 24.9% in Tigray region, respectively.15 Other studies among youth in northern Uganda and the Villagers of Comilla District of Bangladesh reported 29% and 36% comprehensive knowledge, respectively.8,9
Different studies revealed that different factors threw in for the instability of the magnitude of comprehensive knowledge of HIV/AIDS among women from country to country as well as from place to place. The study conducted in Hararge Zone, Ethiopia showed that comprehensive knowledge was more common among those who were from families with a relatively middle or high wealth index, who got HIV/AIDS information mainly from friends or mass media, and who received education on HIV/AIDS and sexual matters2; gender, geographic location, marital status, and education were found to be associated with comprehensive knowledge of HIV/AIDS among youth in northern Uganda16 and Palestinian women.17 A study on demographic and health survey (DHS) analysis in Ghana identified that comprehensive knowledge was associated with education, gender, marital status, locality, occupation, and wealth status.18 The DHS analysis from Kenya was identified education, having tested for HIV, knowing someone with HIV, and/or having a small or moderate to great risk perception as predictors of comprehensive knowledge.19 Attitude and religion were other factors found to have an association with comprehensive knowledge of HIV/AIDS in Greece.20 Sources of information, ever being tested for HIV, educational level, and wealth status were significant factors associated with comprehensive knowledge of HIV/AIDS in the reproductive age group of Uganda.21
The study conducted in Wayu Tuka district, Western Ethiopia among out of school youths revealed that comprehensive HIV/AIDS knowledge was more common among youths with secondary and above educational level, who live with their friends/partners or relatives/other persons like a neighbor, who used media as their major HIV/AIDS information source, who knew about sexually transmitted infections other than HIV/AIDS and those who discussed the sexual matter with their parents or other family members.13
Many world countries including Ethiopia have adapted and established sustainable development goal three to end the epidemic of HIV/ADS, and to reduce maternal mortality ratio and neonatal mortality to 70 per 100,000 and 12 per 1000 live births by 2030, respectively, through strengthening the capacity of all developing countries’ early warning, risk reduction, and management of national and global risks.22 Even though the variety of studies showed that the magnitude of comprehensive knowledge about HIV/AIDS among different sub-group of females and factors associated with them; no study was indicating magnitude and factors associated with comprehensive knowledge about HIV/AIDS among pregnant mothers attending antenatal care (ANC) clinic at health institutions in Ethiopia, particularly in the Arsi zone. Thus, the study is aimed to assess the magnitude and factors associated with comprehensive knowledge of HIV/AIDS among pregnant mothers attending ANC services at health institutions in Arsi zone, Oromia Regional State, Ethiopia.
Methods
Study design and area
A quantitative health facility-based cross-sectional study design was conducted among pregnant mothers attending ANC at health institutions in Arsi zone, Oromia Region, Ethiopia from 18 March to 25 June 2019. Administratively, the Arsi zone had 24 districts, one town administration, 58 towns, and 498 rural Kebeles. The zone has been located at southeast Oromia and hemmed in East Showa (in the north), West Arsi (in the south and west), and West Harargie (in the east). The climate condition of the zone is Dega (42%), Weyna Dega (28%), and Kolla (30%). In the zone, there were four governmental hospitals, 96 health centers, and 496 health posts as well as one private hospital, two health centers, and 256 clinics with 96 drug stores. In 2018, the total health coverage in the zone was 88%. The number of health professionals in the zone was estimated to be 12 medical doctors, 102 health officers, 21 pharmacists, 112 druggists, 662 nurses, 82 environmental health professionals, 26 laboratory technologists, 102 laboratory technicians, and 923 health extension workers. The health service delivery system was through four tiers, that is the primary healthcare unit, district hospital, zonal hospital, and referral hospital. The primary healthcare unit in the zone encompassed one primary hospital with one health center and five health posts.23 According to the 2007 Ethiopian census report, Arsi Zone (excluding Asella town, with 67,250 population) has a total population of 2,635,515 with nearly one to one sex ratio.24
Sample size and sampling procedures
The sample size for the study was determined by double population proportion formula of unmatched case–control study by Epi Info version 7 considering 95% confidence level (CI), 80% power, one to one ratio, 11.57% proportion of the population with comprehensive knowledge having low family wealth index (P1), and 15.67% proportion of the population without comprehensive knowledge having low family wealth index (P2) from the study conducted among in-school adolescent at Eastern Ethiopia, Arargie Zone.9 Thus, since the sample size calculated by comparing middle family wealth index with low family wealth index was the largest, it was considered for investigation. By adding a 5% nonresponse rate and considering the design effect of two, the final sample size considered for the investigation was 4814 ((2292 + 115)*2) pregnant mothers of which 4440 (92.23%) were responded to the interview.
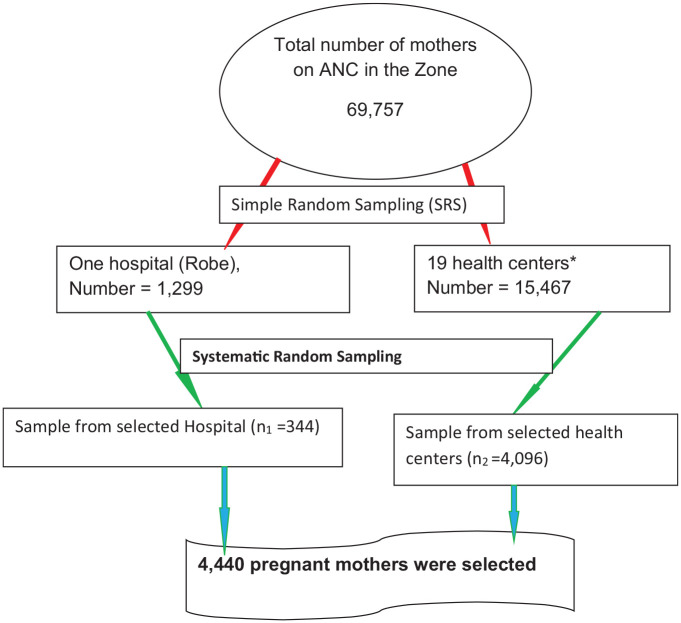
In the Zone, 100 health institutions were providing ANC service. According to Arsi Zone Health bureau report, about 69,757 pregnant mothers were on ANC service in 2010 (2017–2018).23 To select 4440 pregnant mothers for the investigation in the zone, who were on ANC follow-up in the health institutions of the zone, multistage random sampling was employed (Figure 1).
Figure 1.
Schematic presentation of the sampling procedure for selecting pregnant mothers on ANC in health institutions of the Arsi zone, Oromia Regional State, Ethiopia, 2019.
Data collection and data quality
Data were collected by interview, using a structured and pre-tested questionnaire which was developed by reviewing the literature.8,13,15–18,21,25 All pregnant mothers without hearing problems, who can communicate properly and are not seriously ill were interviewed. The questionnaire contains information related to comprehensive knowledge, sociodemographic characteristics, behavioral factors, healthcare services, pregnancy and delivery, information seeking, and family-related factors. Comprehensive knowledge about HIV/AIDS was considered as knowing that consistent use of condoms during sexual intercourse and having just one uninfected faithful partner can reduce the chance of getting the AIDS virus; knowing that a healthy-looking person can have the AIDS virus, and rejecting the two most common local misconceptions about transmission or prevention of the AIDS virus. The two most common local misconceptions in Ethiopia are as follows: (1) AIDS virus can be transmitted by mosquito bites and (2) AIDS virus can be transmitted by supernatural means.8–10 In the study, those who knew these five components were considered knowledgeable (yes), and the magnitude/proportion of knowledgeable mothers was calculated by dividing those who responded “yes” for the five components by total sample size.
Data collection was done by trained health professionals who were working in the ANC clinics nearest to the selected health institutions. One supervisor of health officer from each health institution supervised the data collection procedures in addition to investigators. The questionnaire was prepared originally in English and translated to Afan Oromo and Amharic, and then retranslated back to English by bilingual experts independently to keep the consistency of the questions. Training for data collectors and supervisors was given for 2 days by the investigator at their respective health institutions. The questionnaire was pre-tested to identify a potential problem, unanticipated interpretations, and cultural objections to any of the questions on 241 (5%) respondents having similar characteristics with the study subjects nearby health institutions not selected for the actual investigation. Based on the pre-test results, the questionnaire was additionally adjusted contextually and terminologically and then used for the actual data collection. Counter-checking of the daily filled questionnaires was done by supervisors. Double data entry was done into EPI INFO 7 statistical software. Privacy of the mothers was kept during data collection to get honest responses.
Statistical analysis
The collected data were cleaned, edited, and entered into EPI INFO 7 statistical software and then exported to STATA version 14 for further analysis. Descriptive statistics of the data were done for most variables in the study using different statistical measurements. Bivariable binary logistic regression analysis was conducted primarily to identify variables that had an association with the comprehensive knowledge of mothers. Variables found to have an association with the comprehensive knowledge of pregnant mothers about HIV/AIDS at 0.25 probability were then entered into multivariable binary logistic regression for controlling the possible effect of confounders. Finally, the variables which had significant association were identified by adjusted odds ratio (AOR), with its 95% CI and p values less than 0.05 to fit into the final model. The model fitness was checked for logistic regression by Hosmer and Lemeshow goodness-of-fit, which provided a p value of 0.72 (i.e. >0.05) and deviance reduced (i.e., −2log likelihood was reduced from 5580.38 to 5069.55 with the p value of 0.000). Reliability of the tools used to measure comprehensive knowledge of HIV/AIDS was tested by Cronbach’s alpha which yielded 0.75 with Cronbach’s alpha if item deleted ranging 0.69–0.77.
Results
Sociodemographic characteristics of pregnant mothers attending ANC
Out of the total sample size (4814), 4440 were responded to the interview providing a response rate of 92.23%. The average age of pregnant women attending ANC was 26.21 (±5.5) years. Among these pregnant women, the majority (64.8%) were from urban, 59.5% were Muslim followers, the highest proportion of women was at the primary education level (32.2%), 93.0% were married, about two-thirds were housewives (67.2%) and 18.2% of their husbands were polygamy (Table 1).
Table 1.
Sociodemographic characteristics of pregnant mothers attending antenatal care services in health institutions of Arsi Zone, Oromia Regional State, Ethiopia, 2019 (n = 4440).
| Variables | Frequency (%) |
|---|---|
| Residence | |
| Urban | 1563 (35.2) |
| Rural | 2877 (64.8) |
| Religion | |
| Orthodox | 1481 (33.4) |
| Muslim | 2643 (59.5) |
| Protestant | 276 (6.2) |
| Catholic | 36 (0.8) |
| Others* | 4 (0.1) |
| Educational status | |
| Uneducated | 656 (14.8) |
| Read and write only | 633 (14.3) |
| primary (1–8 grade) | 1429 (32.2) |
| Secondary (9–12 grade) | 792 (17.8) |
| 12 complete | 180 (4.0) |
| Certificate | 138 (3.0) |
| Diploma | 416 (9.4) |
| Degree | 167 (3.8) |
| Masters | 29 (0.7) |
| Marital status | |
| Married (living together) | 4128 (93.0) |
| Single | 118 (2.7) |
| Widowed | 43 (1.0) |
| Separated (not living together) | 100 (2.2) |
| Divorced | 51 (1.1) |
| Work status | |
| Housewife | 2984 (67.2) |
| Government employee | 549 (12.4) |
| None-government employee | 121 (2.7) |
| Farmer | 404 (9.1) |
| Merchant | 330 (7.4) |
| Others** | 52 (1.2) |
| Husband had multiple wives | |
| Yes | 816 (18.4) |
| No | 3312 (74.6) |
| No marriage | 312 (7.0) |
Wakefata and Joba.
Students and daily laborer.
Healthcare service accessibility, availability, and delivery history of mothers
More than half (51.2%) of the pregnant mothers were not visited during their pregnancy period by health extension workers, whereas about one-third (33.9%) of them delivered at home their previous births (Table 2).
Table 2.
Healthcare service accessibility, availability, and delivery history of pregnant mothers attending ANC services in health institutions of Arsi Zone, Oromia Regional State, Ethiopia, 2019 (n = 4440).
| Variables | Frequency (%) |
|---|---|
| Visited by health extension workers | |
| Yes | 2166 (48.8) |
| No | 2274 (51.2) |
| Place of delivery for a previous birth | |
| Home | 1507 (33.9) |
| Health institution | 1388 (31.3) |
| Not given birth | 1545 (34.8) |
| Type of pregnancy | |
| Wanted (planned) | 3268 (73.6) |
| Not wanted (unplanned) | 1172 (26.4) |
| Order of current pregnancy | |
| First | 1559 (35.1) |
| Second | 1079 (24.3) |
| Third | 779 (17.6) |
| Fourth and more | 1023 (23.0) |
| Number of ANC visit | |
| First visit | 1503 (33.9) |
| Second visit | 1455 (32.8) |
| Third visit | 903 (20.3) |
| Fourth visit | 515 (11.6) |
| Fifth and more | 64 (1.4) |
| Mothers’ attitude on premarital pregnancy | |
| Discouraging attitude | 3838 (86.4) |
| Encouraging attitude | 602 (13.6) |
| Parity | |
| Nullipara | 1559 (35.1) |
| Primipara | 1079 (24.3) |
| Multipara | 1802 (40.6) |
| Contraceptive methods mentioned | |
| Female sterilization | 513 (11.6) |
| Male sterilization | 540 (12.2) |
| Pill | 3391 (76.4) |
| IUD | 1971 (44.4) |
| Injectable | 3841 (86.5) |
| Implants | 3392 (76.4) |
| Male condoms | 1682 (37.9) |
| Female condoms | 291 (6.6) |
| Lactation amenorrhea method | 467 (10.5) |
| Emergency contraception | 397 (8.9) |
| The standard days’ method | 255 (5.7) |
| Periodic abstinence (or rhythm) | 189 (4.3) |
| Withdrawal | 254 (5.7) |
| Source of contraception mentioned | |
| Government hospital | 2313 (52.1) |
| Government health center | 3693 (83.2) |
| Government health post/HEW | 2506 (56.4) |
| Private hospital | 1466 (33.0) |
| Private clinic | 1874 (42.2) |
| Pharmacy | 818 (18.4) |
| NGO health facility | 682 (15.4) |
| Voluntary community health workers | 130 (2.9) |
| Drug vendor/store | 90 (2.0) |
| Shop | 195 (4.4) |
| Friend/relative | 127 (2.9) |
ANC, antenatal care; IUD, intrauterine device; NGO, non-governmental organization.
Pregnant mothers’ family history and sexual empowerment
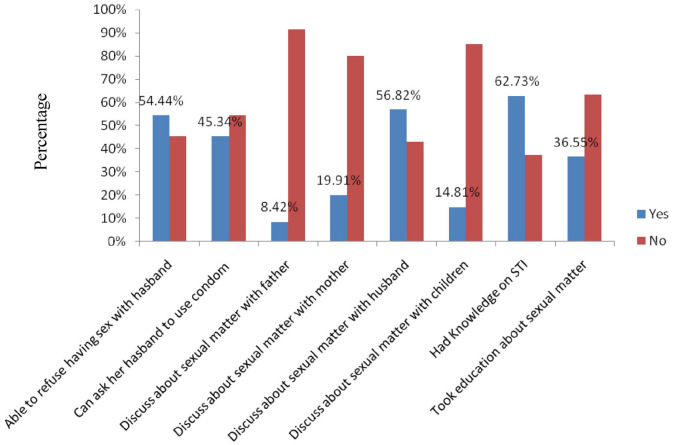
About 10% of pregnant mothers attending ANC were widows while 23.3% and 21.3% of the educational status of their husbands or partners were secondary levels and primary level, respectively. Nearly one-third of pregnant mothers had children who attended primary level education (32.5%); followed by secondary educated (6.7%) children (Table 3). More than half of them reported that they can refuse to have sex when they have no interest and discussion about the sexual matter with their husbands (i.e., 54.44% versus 56.82%), respectively. Nearly two-thirds (62.73%) of mothers knew sexually transmitted infection while only about one-third took education about sexual matters (Figure 2).
Table 3.
Family history of pregnant mothers attending antenatal care services in health institutions of Arsi Zone, Oromia Regional State, Ethiopia, 2019 (n = 4440).
| Variables | Frequency (%) |
|---|---|
| Husband/ partners alive | |
| Yes | 3990 (89.9) |
| No | 450 (10.1) |
| Husband/ partners’ educational status | |
| Uneducated (not read and write) | 681 (15.3) |
| Primary (1–8 grade) | 945 (21.3) |
| Secondary (9–12 grade) | 1033 (23.3) |
| 12 complete | 246 (5.5) |
| Certificate | 177 (4.0) |
| Diploma | 460 (10.4) |
| Degree | 376 (8.5) |
| Masters | 72 (1.60) |
| No husband | 450 (10.10) |
| The highest educational level attained by one of their children | |
| Uneducated (not read and write) | 891 (20.1) |
| Primary (1–8 grade) | 1442 (32.5) |
| Secondary (9–12 grade) | 298 (6.7) |
| 12 complete | 62 (1.4) |
| Certificate | 28 (0.6) |
| Diploma | 79 (1.8) |
| Degree | 89 (1.9) |
| Masters | 29 (0.7) |
| No child | 1525 (34.3) |
Figure 2.
Knowledge of STI and empowerment on sexual matters of pregnant mothers on ANC in health institutions of Arsi Zone, Oromia Regional State, Ethiopia, 2019 (n = 4, 440).
ANC, antenatal care; STI, sexually transmitted infection.
HIV/AIDS magnitude, knowledge, and attitude of pregnant mothers attending ANC
Among the total pregnant mothers interviewed, only one-third, 1430 (32.2% (95% CI: 30.83%, 33.60%)), of mothers were found to have comprehensive knowledge About HIV/AIDS. The study showed about 85.9% were tested for HIV of which 97.96% received their result. The prevalence of HIV/AIDS was found to be 2.82% among pregnant mothers attending ANC in the health institutions of the Arsi Zone (Table 4).
Table 4.
HIV/AIDS Magnitude, knowledge, and attitude of pregnant mothers attending antenatal care services in health institutions of Arsi Zone, Oromia Regional State, Ethiopia, 2019 (n = 4440).
| Variables | Frequency (%) |
|---|---|
| Heard of HIV/AIDS | |
| Yes | 3833 (86.3) |
| No | 607 (13.7) |
| Took education on HIV/AIDS | |
| Yes | 3667 (82.6) |
| No | 773 (17.4) |
| Had a comprehensive knowledge of HIV/AIDS | |
| Yes | 1430 (32.2) |
| No | 3010 (67.8) |
| Attitude toward HIV/AIDS patients | |
| Not accepting attitude | 2930 (66.0) |
| Accepting attitude | 1510 (34.0) |
| Know somebody who died of HIV/AIDS | |
| Yes | 1867 (42.0) |
| No | 2573 (58.0) |
| Had relatives died of HIV/AIDS (n = 1867) | |
| Yes | 961 (21.6) |
| No | 1031 (23.2) |
| Tested for HIV/AIDS | |
| Yes | 3815 (85.9) |
| No | 625 (14.1) |
| Received test result (n = 3815) | |
| Yes | 3737 (97.96) |
| No | 78 (2.04) |
| The magnitude of HIV/AIDS | |
| Positive | 125 (2.82) |
| Negative | 3690 (83.11) |
| Not tested | 625 (14.07) |
| Sources of information mentioned for HIV/AID | |
| Radio | 2712 (61.1) |
| Television | 1610 (36.3) |
| News paper | 716 (16.1) |
| Health institution | 3054 (68.8) |
| School | 1690 (38.1) |
| Church | 653 (14.7) |
Pregnant mothers substance use in the last 12 months
In the last 12 months before data collection, 10.7%, 15.7%, 3%, and 2.3% of pregnant mothers attending ANC services had the habit of alcohol drinking, khat chewing, cigarette smoking, and using Shish, respectively (Table 5).
Table 5.
Substance use in the last twelve months among pregnant mothers attending antenatal care services in health institutions of Arsi Zone, Oromia Regional State, Ethiopia, 2019 (n = 4440).
| Variables | Frequency (%) |
|---|---|
| Drink alcohol | |
| Yes | 473 (10.7) |
| No | 3967 (89.3) |
| Chewed khat | |
| Yes | 697 (15.7) |
| No | 3743 (84.3) |
| Smoked cigarette | |
| Yes | 133 (3.0) |
| No | 4307 (97.0) |
| Used shisha | |
| Yes | 104 (2.3) |
| No | 4336 (97.7) |
Discussion
The study revealed that only about one-third (32.2%; 95% CI: 30.83%, 33.60%) of pregnant mothers attending ANC follow-up had comprehensive knowledge about HIV/AIDS. The result is similar to prevention gap reports of the United Nations which stated that two-thirds of young people do not have correct and comprehensive knowledge of HIV.26
However, this result is lower than studies conducted among staff in public universities of Kenya which reported 83% of females had high knowledge of HIV/AIDS,27 among urban young women in Kenya ( 53.9%),19 Palestinian women in the occupied Palestinian territory (48.1%) which reported that healthy-looking persons can be infected by HIV/AIDS,17 among adult population in Ghana (50%),18 among Indian women, around 70% had awareness of AIDS while 64.2% of the women knew that one can reduce chances of acquiring HIV/AIDS using condoms,28 among the nursing school of a Technological Educational Institute in Greece, 60.2% believed that mosquitoes cannot transmit HIV, whereas 62% believed the virus could not be transmitted via the toilet seat.20 In addition, in Uganda nearly three-fourths, 55%, 88%, and 74% of women, knew that HIV can be prevented using condoms, limiting sexual intercourse to one uninfected partner, HIV cannot be transmitted by mosquito bites, a healthy-looking person can have HIV, and a person cannot be infected by sharing food with a person who has HIV, respectively.29 In Palestine, reports of UNICEF revealed that 34.8% of women knew that they can protect themselves from contracting HIV both using condoms and having sex solely with one faithful uninfected partner,30 In Mekelle City, Ethiopia, 85.5% respondents had good knowledge about HIV/AIDS.14 The possible reason for the difference could be measurement difference as most of these studies used only one criterion to estimate comprehensive knowledge of HIV/AIDS while this study used five criteria. In addition, most of these studies were conducted among educated and/or urban population, whereas this study covered urban and rural as well as uneducated pregnant mothers.
On the other hand, the result of this study is higher than results of the studies conducted among out-of-school youths in Wayu Tuka district, Western Ethiopia, and among in-school adolescents in eastern Ethiopia in which 25% and 24.5% of them had comprehensive knowledge of HIV/AID,9,13 respectively. About 20% of women in India thought that sharing food with an infected person can transmit HIV/AIDS,28 24% of young women aged 15–24 years has comprehensive knowledge of HIV/AIDS in Nigeria31 and in Uganda, 30% of young women have comprehensive knowledge of HIV/AIDS.16 The explanation for the differences could be information exposure as our study was among mothers attending ANC follow-up with the high probability of exposure to information in the health institutions while most of the studies were on general as well as on young population with less probability.
Mothers who knew safe period to be pregnant concerning their menstruations were 32.89% more likely to have comprehensive knowledge compared to those who did not know their safe period to be pregnant concerning menstruation date (AOR = 1.49; 95% CI: 1.24, 1.78). As mothers read about their safe period to be pregnant, the probability of reading about HIV/AIDS has increased which, in turn, increases their comprehensive knowledge. As these mothers intended to prevent pregnancy the likelihood of exposure to information of HIV/AIDS is increased through reading and discussion with the health professionals.
The odds of having comprehensive knowledge among pregnant mothers who took education on any sexual matter were one point six five times more likely compared to those who did not take education (AOR = 1.65; 95% CI: 1.42, 1.92). The result is supported by studies conducted in Palestine, Uganda, Hararge Zone which showed that comprehensive knowledge was more common among those who received education on sexual matters.9,16–18,21 Education is a key to disseminating information about HIV/AIDS, so, currently, a new curriculum on HIV/AIDS is added to the higher education program in Ethiopia.
Women who had no sexual practice empowerment were 50% less likely to have comprehensive knowledge compared to those who were empowered (AOR = 0.50; 95% CI: 0.43, 0.58). As women are getting empowered, the probability of seeking new information and knowledge about what they are practicing to prevent themselves will increase. Other factors associated with comprehensive knowledge of mothers attending ANC were the attitude toward having multiple partners, attitude toward premarital sex, and attitude toward accepting HIV/AIDS patients. Accordingly, mothers who had a discouraging attitude toward having multiple partners were 34.64% more likely to have comprehensive knowledge about HIV/AIDS compared to those who had an encouraging attitude (AOR = 1.53; 95% CI: 1.24, 1.88). Likewise, mothers who had the discouraging attitude toward having premarital sex were 40.48% more likely to have comprehensive knowledge of HIV/AIDS compared to those who had the encouraging attitude (AOR = 1.68; 95% CI: 1.38, 2.03). Mothers who had a positive attitude toward accepting HIV/AIDS patients were about 62.83% more likely to have comprehensive knowledge of HIV/AIDS compared to those who had a negative attitude (AOR = 2.69; 95% CI: 2.34, 3.10) (Table 6). These results are supported by the study conducted in Greece in which attitude was associated with comprehensive knowledge of HIV/AIDS.20 As the mother’s attitude is favorable/positive for comprehensive knowledge, the likelihood of looking for the information will increase.
Table 6.
Factors associated with comprehensive knowledge of HIV/AIDS among pregnant mothers attending antenatal care services in health institutions of Arsi Zone, Oromia Regional State, Ethiopia, 2019 (n = 4440).
| Explanatory variables | Comprehensive knowledge | COR (95% CI) | AOR (95% CI) | p Value | |
|---|---|---|---|---|---|
| Yes | No | ||||
| Residence | |||||
| Urban | 537 | 1026 | 1 | ||
| Rural | 893 | 1984 | 0.86 (0.75, 0.98) | ||
| Number of ANC visit | |||||
| First visit | 498 | 1005 | 1 | ||
| Second visit | 382 | 1073 | 0.72 (0.61, 0.84) | ||
| Third visit | 263 | 640 | 0.83 (0.69, 0.99) | ||
| Fourth visit | 275 | 240 | 2.31 (1.89, 2.84) | ||
| Fifth and more | 12 | 52 | 0.47 (0.25, 0.88) | ||
| Visited by HEW | |||||
| Yes | 588 | 1578 | 1 | ||
| No | 842 | 1432 | 1.58 (1.39, 1.79) | ||
| Know safe period to be pregnant | |||||
| Yes | 332 | 462 | 1.67 (1.42, 1.95) | 1.49 (1.24, 1.78) | 0.000 |
| No | 1098 | 2549 | 1 | ||
| Current pregnancy | |||||
| Planned | 1142 | 2126 | 1 | ||
| Unplanned | 288 | 884 | 0.61 (0.52, 0.71) | ||
| Mother and father live together | |||||
| Yes | 1029 | 2046 | 1 | ||
| No | 401 | 964 | 0.83 (0.72, 0.95) | ||
| Ever taught about a sexual matter | |||||
| Yes | 441 | 1182 | 1 | ||
| No | 989 | 1828 | 1.45 (1.27, 1.66) | 1.65 (1.42, 1.92) | 0.000 |
| Women’s sexual practice empowerment | |||||
| Empowered | 610 | 849 | 1 | ||
| Not empowered | 820 | 2161 | 0.53 (0.46, 0.60) | 0.50 (0.43, 0.58) | 0.000 |
| Attitude toward premarital pregnancy | |||||
| Discouraging | 1196 | 2642 | 1 | ||
| Encouraging | 234 | 362 | 1.41 (1.18, 1.68) | ||
| Attitude toward multiple partners | |||||
| Encouraging | 214 | 761 | 1 | ||
| Discouraging | 1216 | 2249 | 1.92 (1.63, 2.27) | 1.53 (1.24, 1.88) | 0.000 |
| Attitude toward premarital sex | |||||
| Encouraging | 262 | 979 | 1 | ||
| Discouraging | 1168 | 2031 | 2.15 (1.84, 2.51) | 1.68 (1.38, 2.03) | 0.000 |
| Attitude toward accepting HIV/AIDS patients | |||||
| Negative | 692 | 2238 | 1 | ||
| Positive | 738 | 772 | 3.09 (2.71, 3.53) | 2.69 (2.34, 3.10) | 0.000 |
| Attitude toward compensated dating with sex | |||||
| Encouraging | 142 | 518 | 1 | ||
| Discouraging | 1288 | 2492 | 1.89 (1.55, 2.30) | ||
ANC, antenatal care; AOR, adjusted odds ratio; CI, confidence interval; COR, crude odds ratio.
Limitation of the study
Even though the study disclosed the magnitude and factors associated with comprehensive knowledge of HIV/AIDS, the result is not free of the effect of cross-sectional study design (i.e., not indicating temporal relationship). Since most of the information was based on self-report, it is also not free of social desirability biases. In addition, there was a shortage of similar studies so that the comparison and justification of the discussion were not strongly supported.
Conclusion
In conclusion, only about one-third (32.2%) of pregnant mothers attending ANC services had comprehensive knowledge of HIV/AIDS. Knowledge of safe period to be pregnant, education about the sexual matter, women’s sexual practice empowerment, attitude toward having multiple partners, attitude toward premarital sex, and attitude toward accepting HIV/AIDS patients were factors significantly associated with pregnant mothers’ comprehensive knowledge of HIV/AIDS. Thus, it would be better if the health institutions in the zone focused on educating mothers on ANC follow-up about HIV/AIDS, particularly for those with an unplanned pregnancy, who do not know the safe period to be pregnant, not empowered of sexual practice, and had an encouraging attitude toward multiple partners, premarital sex, and negative attitude toward accepting HIV/AIDS patients.
Supplemental Material
Supplemental material, sj-docx-1-smo-10.1177_20503121221145614 for Two-thirds of pregnant mothers attending antenatal care services at Arsi Zone, Oromia Regional State, Ethiopia had no comprehensive knowledge of HIV/AIDS: A cross-sectional study by Teresa Kisi Beyen and Abenet Menene Gurara in SAGE Open Medicine
Acknowledgments
We would like to forward our deepest gratitude to Arsi zone and Asella town health bureau for the permission and information they provided us. A very special thank goes to Guta Tola Debela and Daniele Abebe Mekuriya for the time they devoted to organizing the information required for the research.
Footnotes
Author contributions: Teresa Kisi Beyen, conceived the idea, wrote the proposal, supervised the data collection, analyzed the data, drafted the manuscript, and revised subsequent drafts. Abenet Menene Gurara wrote the proposal, supervised the data collection, analyzed the data, drafted the manuscript, and revised subsequent drafts.
Availability of data and materials: As the study was our original work, we have primary data collected from the study participants and the tool for the collected data. We are happy to share the data and tools through communication.
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval and consent to participate: Ethical approval for this study was obtained from Institutional research ethics review board of Arsi University, College of Health Sciences Research Ethics Review Committee with approval number of A/CHS/R001/15/16. Oral informed consent was obtained from each mother after getting permission from each health institution. The verbal consent was approved by the Institutional Review Board of the Arsi University. Verbal consent was obtained due to difference in mothers’ educational levels and based on Arsi University Institutional Review Board (IRB) recommendation. Each pregnant mother was informed about the objective of the study and those who refused to participate in the study were not forced. Confidentiality was granted for information collected by keeping the privacy of the respondents while interviewing, using means which was not disclose mothers and keeping the collected information in the locked cabinet.
Funding: The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was funded by Arsi University from its annual research and community service grant.
ORCID iD: Abenet Menene Gurara  https://orcid.org/0000-0002-3973-1455
https://orcid.org/0000-0002-3973-1455
Supplemental material: Supplemental material for this article is available online.
References
- 1. UNAIDS. Ending AIDS: progress towards the 90 –90 –90 targets. Global AIDS update 2017. Geneva: UNAIDS, http://www.unaids.Org/sites/default/files/media_asset/Global_AIDS_update_2017_en.pdf (2017, accessed 18 November 2021). [Google Scholar]
- 2. World Health Organization. Global guidance on criteria and processes for validation of elimination of mother-to-child transmission of HIV and syphilis, 2nd edn. Geneva: World Health Organization, 2017. [Google Scholar]
- 3. Federal Ministry of Health. National guideline for prevention of mother-to-child transmission of HIV, Syphilis and Hepatitis B Virus. Ethiopia: ICAP, 2021. [Google Scholar]
- 4. UNAIDS. The gap report 2014: children and pregnant women living with HIV. Geneva: UNAIDS, p.5; http://www.unaids.org/sites/default/files/media_asset/09_ChildrenandpregnantwomenlivingwithHIV.pdf (2014, accessed 18 November 2021). [Google Scholar]
- 5. World Health Organization. Global guidance on criteria and processes for validation: elimination of mother-to-child transmission of HIV and Syphilis. Geneva, Switzerland: WHO, 2017. [Google Scholar]
- 6. Sama CB, Feteh VF, Tindong M, et al. A. Prevalence of maternal HIV infection and knowledge on mother–to–child transmission of HIV and its prevention among antenatal care attendees in a rural area in northwest Cameroon. PLoS One 2017; 12: e0172102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Federal Ministry of Health. Guidelines for prevention of mother-to-child transmission of HIV in Ethiopia, Federal HIV/AIDS Prevention and Control Office. In: Office FHAPaC, editor, 2007. [Google Scholar]
- 8. EDHS. Ethiopia Demographic and Health Survey 2011 Central Statistical Agency, Addis Ababa, Ethiopia ICF International Calverton, MD, 2012. [Google Scholar]
- 9. Oljira L, Berhane Y, Worku A. Assessment of comprehensive HIV/AIDS knowledge level among in-school adolescents in eastern Ethiopia. J Int AIDS Soc 2013; 16(17349): 1–5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Central Statistical Agency (CSA) [Ethiopia] and ICF. Ethiopia Demographic and Health Survey 2016. Addis Ababa, Ethiopia, and Rockville, MD: CSA and ICF, 2016. [Google Scholar]
- 11. Shiferaw Y, Alemu A, Girma A, et al. Assessment of knowledge, attitude and risk behaviors towards HIV/AIDS and other sexual transmitted infection among preparatory students of Gondar town, North West Ethiopia. BMC Res Notes 2011; 4(505): 1–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. WHO. Early marriages, adolescent and young pregnancies Report by the Secretariat Sixty-Fifth World Health Assembly A65/13 Provisional agenda item 2012. Geneva: WHO, 2012. [Google Scholar]
- 13. Kejela G, Oljira L, Dessie Y, et al. Comprehensive HIV/AIDS knowledge level among out-of-school youths in Wayu Tuka district, Western Ethiopia. Eur J Prevent Med 2015; 3(1): 11–6. [Google Scholar]
- 14. Tadese A, Menasbo B. Knowledge, attitude and practice regarding HIV/AIDS among secondary school students in Mekelle City, Ethiopia. Afr JAIDS HIV Res 2013; 1(1): 1–7. [Google Scholar]
- 15. Central Statistical Agency (CSA) [Ethiopia] and ICF. Ethiopia Demographic and Health Survey 2016: Key Indicators Report. Addis Ababa, Ethiopia, and Rockville, MD: CSA and ICF, 2016. [Google Scholar]
- 16. CiCCiò l, Sera D. Assessing the knowledge and behavior towards HIV/AIDS among youth in northern Uganda: a cross-sectional survey. Giornale Italiano di Medicina Tropicale, 2010; 15(1–4): 29–34. [Google Scholar]
- 17. Husseini A, Abu-Rmeileh NM. HIV/AIDS-related knowledge and attitudes of Palestinian women in the occupied Palestinian territory. Am J Health Behav 2007; 31(3): 323–334. [DOI] [PubMed] [Google Scholar]
- 18. Fenny AP, Crentsil AO, Asuman D. Determinants and distribution of comprehensive HIV/AIDS knowledge in Ghana. Global J Health Sci 2017; 9(12): 32–46. [Google Scholar]
- 19. Ochako R, Ulwodi D, Njagi P, et al. Trends and determinants of Comprehensive HIV and AIDS knowledge among urban young women in Kenya. AIDS Res Ther 2011; 8(11): 1–8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Ouzouni C, Nakakis K. HIV/AIDS knowledge, attitudes and behaviours of student nurses. Health Sci J 2012; 6(1): 129–150. [Google Scholar]
- 21. Ankunda D, Asiimwe JB. Determinants of comprehensive knowledge of HIV/AIDS among women of the reproductive age (15-49) in Uganda. Int J Commun Med Public Health 2017; 4(10): 3530–3535. [Google Scholar]
- 22. United Nations. Transforming our World: The 2030 Agenda for Sustainable Development A/RES/70/1, https://www.un.org/sustainabledevelopment/development-agenda/ (2015).
- 23. Arsi Zone Health office. Qajeelcha Eegumsa Fayyaa Godina Arsii, Gabaasa Raawwii Karoora Kurmaana 1FFAA, Fulbaana Bara 2010, 2010, pp. 1–33. [Google Scholar]
- 24. Central Statistical Agency. Summary and statistical report of the 2007 population and housing census: population size by age and sex. Ethiopia Addis Ababa. UNFPA, 2008. [Google Scholar]
- 25. Federal Democratic Republic of Ethiopia. Country progress report on the HIV response, Addis Ababa, Ethiopia: Federal Democratic Republic of Ethiopia, 2014. [Google Scholar]
- 26. UNAIDS. Prevention gap report, Joined United Nation Programme on HIV/AIDS, 20 Avenue Appia 1211 Geneva 27, Switzerland, 2016. [Google Scholar]
- 27. Samuel M, Irene M. HIV/AIDS distigmatisation at work place: more than comprehensive knowledge required international J HIV/AIDS Prevent Educ Behav Sci 2017; 3(6): 63–69. [Google Scholar]
- 28. Agarwal S, Araujo PD. Access to media and HIV knowledge in India. Economies 2014; 2: 124–146. [Google Scholar]
- 29. Uganda Ministry of Health and ICF International. Uganda AIDS indicator survey of 2011: Key findings. Calverton, MD: MOH and ICF International, 2012. [Google Scholar]
- 30. UNICEF. Knowledge, Attitudes and practices survey Healthy lifestyles. New York: UNICEF, 2011. [Google Scholar]
- 31. UNICEF Report. Fact sheet on Comprehensive Knowledge of HIV prevention among young people in Nigeria. Nigeria, 2015. https://www.unicef.org/nigeria/media/1641/file/Nigeria-equity-profile-hiv.pdf. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental material, sj-docx-1-smo-10.1177_20503121221145614 for Two-thirds of pregnant mothers attending antenatal care services at Arsi Zone, Oromia Regional State, Ethiopia had no comprehensive knowledge of HIV/AIDS: A cross-sectional study by Teresa Kisi Beyen and Abenet Menene Gurara in SAGE Open Medicine