Abstract
Background
High-quality cardiopulmonary resuscitation (CPR) is foundational to all resuscitative efforts. Spaced practice improves learners’ skill retention. We evaluated the implementation of a quarterly CPR curriculum and skills training program for a dedicated chest compressor team to improve the quality of CPR performed during in-hospital cardiac arrest (IHCA) events and its impact on patient survival of event.
Methods
Baseline observations on CPR performance within the hospital were collected in October 2018. The CPR quarterly training program was implemented in November 2018. Training included use of high-fidelity simulation manikins and team members received real-time feedback scores related to compression rate, depth and recoil. High-quality CPR scores were set at ≥ 70%. Yearly IHCA event survival data was examined in relation to the implementation of training.
Results
Quarterly CPR training of the team led to retention of CPR skills (chest compression rate, depth, and recoil). The team’s initial CPR training performance average score was 49.1%, increasing to 80.3%, with 95% (n = 37) of participants achieving a higher score after feedback during their initial training. A two-sample t-test was used for numerical data and chi-square was used for proportional data analysis. The survival of event prior to this training was 61.0% January-October 2018. Post -training, event survival rose to 73.5% (p-value 0.03) in 2019.
Conclusion
Implementation of a team that attends quarterly CPR training with a high-fidelity simulation manikin is attainable. This training resulted in improved CPR quality and benefited IHCA event survival.
Keywords: IHCA, Team Training, Quarterly, CPR, Education
Introduction
In-hospital cardiac arrest (IHCA) remains a serious patient safety issue. Each year, approximately 292,000 adults in US hospitals experience an IHCA that requires cardiopulmonary resuscitation (CPR).1 Survival of IHCA to hospital discharge has improved from 17% to 25% between 2000–2016.2
Response to IHCA is performed by code blue teams, where clinicians and healthcare staff work together to deliver high-quality CPR, which improves the survival of IHCA events. Features of top-performing resuscitation teams include dedicated or designated resuscitation personnel; multiple disciplines; clear identification of roles and responsibilities; and use of direct, closed-loop communication during IHCA.3 Team coordination and communication are also relevant factors predicting the performance of high-quality CPR.4
The American Heart Association (AHA) cites that current educational offerings in the form of standardized online and face-to-face courses completed every-two years are insufficient, with CPR providers (licensed and non-licensed healthcare staff) demonstrating a decay of their CPR skills over time.5 Instead, transitioning to quarterly CPR training sessions has been shown to improve providers’ retention of high-quality CPR skills.5 For example, when healthcare providers were trained with spaced practice, the percentage of healthcare providers performing high-quality CPR more than doubled from 25% to 65%.6 Mastery of learning, deliberate practice, and spaced practice has also been shown to improve healthcare provider CPR skills retention.7, 8, 9, 10
High-quality CPR has been defined as minimizing interruptions in chest compressions, providing compressions of adequate rate and depth, avoiding leaning on the chest between compressions, and avoiding excessive ventilation.11 Using an audio-visual feedback manikin during CPR skills practice is a more effective method of training to improve CPR quality.12, 13 In comparison, assessment of CPR skills by human instructors has been shown to be inaccurate when compared with objective measures.14
Literature supports the importance of clearly defining the role of chest compressor at IHCA and increasing the frequency of CPR skills training using feedback devices. Therefore, this quality improvement initiative aimed to develop a customized, quarterly CPR curriculum and skills training program for our Dedicated Chest Compressor Team and improve the quality of compressions performed at IHCA events.
Methods
Design
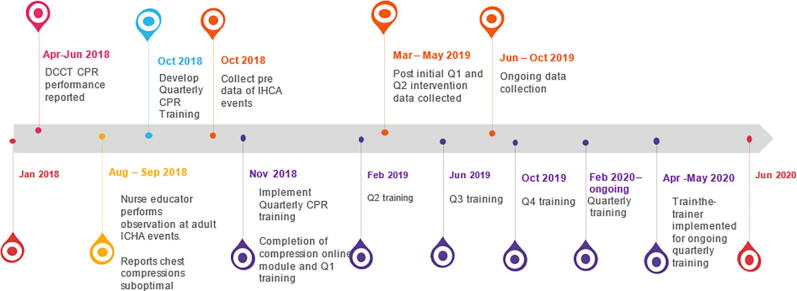
We conducted a quality improvement initiative to evaluate the effectiveness of a quarterly CPR training program for the Dedicated Chest Compressor Team at our 625-bed academic, tertiary, level 1 medical center, from October 2018 to October 2019 (See Fig. 1). Institutional review board was not required by our facility, as this was a quality improvement initiative. The authors declare that all supporting data are available within the article.
Fig. 1.
Timeline of Quality Improvement Initiative, Legend- DCCT = Designated Chest Compressor Team, CPR = Cardiopulmonary Resuscitation, IHCA = In-Hospital Cardiac Arrest, Q1 = Quarter 1 training Q2 = Quarter 2 Training, Q3 = Quarter 3 Training, Q4 = Quarter 4 Training.
Dedicated chest compressor team
The institution’s adult code blue team consists of a surgical resident, medicine resident/fellow, medicine intern, anesthesiologist, respiratory therapist, pharmacist, medical intensive care unit nurse, rapid response nurse, and Lift Team members. Our code blue team is activated by a staff member who calls the code line. The code line operator sends out an overhead page and an alert to the code blue pagers that are held by members of the code blue team. The Lift Team was first designated as the Dedicated Chest Compressor Team in 2016, assuming the role of performing chest compressions at adult IHCA events upon arrival and are members of the code blue team. When an IHCA is identified, the Lift Team members on shift respond to code blue alerts and assume the chest compressor role and rotate every-two minutes or sooner, as needed.
The Lift Team is a department comprised of former firefighters, emergency medical technicians, undergraduate students studying healthcare, and non-licensed staff. They work as ergonomics experts and partner with clinicians within the hospital to ensure proper patient mobilization and safe patient handling techniques to prevent both staff and patient movement injuries.
Historically, Lift Team CPR training consisted of participation in the institution’s CPR skill training every-two years. The biennial training consisted of completing a 60-minute CPR online learning module which covered adult, child and infant CPR skills and use of an automated external defibrillator. Then they attended a 30-minute hands-on skill practice and verification session with a CPR instructor. During the skills verification portion, participants performed five cycles of chest compressions and rescue breaths on a clinical task trainer manikin. Successful CPR skill verification was based on the CPR instructor’s subjective assessment of performance.
Identification of training deficit
High-quality CPR influences survival from IHCA, but there is considerable variation in monitoring, implementation, and quality improvement. Gaps between current knowledge of high-quality CPR and translation to practice exist.11 In 2018, the performance of CPR compressions during adult IHCA events was reported as not meeting the critical components of high-quality CPR (rate, depth, and recoil). Anecdotal feedback suggested compressions were being performed as, “too deep” and “too quickly”. In addition, we identified an opportunity for increased frequency of CPR training, objective compression feedback, and deliberate practice of CPR skills between the two-year renewal cycle.
In 2018, a nurse educator who is a CPR instructor, began attending adult IHCA events to observe chest compression performance and identified a need for more frequent practice and feedback for chest compression skills. It was determined that chest compression performance could improve with the implementation of evidence-based training and quarterly practice of high-quality CPR skills.
Quarterly CPR curriculum and program implementation
We created the Dedicated Chest Compressor Team Quarterly CPR Training Program to improve chest compression performance during IHCA events. In November 2018, quarterly CPR training was implemented for the Dedicated Chest Compressor Team to promote high-quality CPR skills with the intention of optimizing IHCA patient survival. The AHA 2015 guidelines were used to underpin the activity, and an audio-visual simulation high-fidelity manikin (SmartMan, V4EMS Inc., United States) was used to provide objective feedback during training.15 Each training was performed during calendar quarters.
Initial Quarterly CPR Training. The initial training consisted of a newly created CPR online module focusing on high-quality CPR and chest compressions. Once the online module was completed, participants took part in a hands-on CPR skills practice session utilizing the high-fidelity simulation manikin. The manikin, paired with high sensor fidelity, provides objective feedback on CPR compressions depth, rate, and recoil performance, as well as an overall score for compression performance between 0–100%. Target compression scores for trainees were set to a minimum of 70%. This overall score is determined by the high-fidelity manikin computer software. The software combines the average of each component of chest compressions (rate, depth, and recoil) and determines the overall CPR performance score.
Within a group training session, each Dedicated Chest Compressor Team member performed two minutes of chest compressions on the high-fidelity manikin without coaching or audio-visual feedback in a simulated code event. Using data from a high-fidelity manikin, each trainees’ performance was recorded. Utilizing the objective data from the manikin, instructors identified areas of competence and improvement needed, such as compression rate (too fast/too slow), compression depth (too shallow/too deep), allowing for recoil, proper hand placement, or use of a step stool. The training was in a simulation room within the hospital and the manikin was on a hospital bed with a backboard in place. Training instructors held sessions that were accommodating to all shifts (0700, 1500, 2000, 0100, and 0300).
After the initial baseline compression practice and CPR score were recorded, the trainers reviewed the components of high-quality CPR with each trainee. The trainee then received verbal coaching on their CPR technique from the trainers and visual feedback from the high-fidelity manikin. This allowed trainees to receive real-time feedback and adjust their compressions as the skill was practiced. A final CPR score from the high-fidelity manikin, with a program goal to have a higher score than their baseline, was established.
Subsequent Quarterly CPR Trainings. In subsequent quarterly trainings, sessions included CPR practice using the high-fidelity manikin where participants performed two 100-compression practice sessions while receiving audio-visual feedback. The training also incorporated a defibrillator (ZOLL R Series, ZOLL, United States), which is the device that provides audio-visual feedback and is utilized during IHCA events for the duration of the event. Like the high-fidelity manikin, these defibrillators provide real-time CPR feedback for depth, recoil, and compression rate and are used during an IHCA to optimize chest compression performance. The defibrillator is located on each unit’s code blue cart throughout the organization. The same parameters as the initial training were used for compression practice, including repeated rounds if the high-fidelity manikin CPR performance score fell below 70%.
Data collection and analysis
Data from the high-fidelity manikin analytics software program (SmartMan, V4EMS Inc., United States) were used to measure overall chest compression performance scores for each Dedicated Chest Compressor Team member, comprising of CPR rate, depth, and recoil. The data was saved and exported for analysis. Descriptive statistics were performed to summarize team member CPR performance during each quarterly training session.
In addition, we performed chart reviews from each adult IHCA event identified using code blue operator reports between January-October 2018 and January-December 2019. Data extracted included code length, if there was a return of spontaneous circulation (ROSC), patient age, gender, location (intensive care unit vs non-intensive care unit) and discharge disposition. The code blue events were located on adult inpatient units, including both intensive care units and acute care/telemetry units. We excluded the following code blue events from our analysis: no chest compressions performed, pediatric patients, patients with a Ventricular Assist Device, and CPR performed in the emergency department, operating room, labor and delivery suites, radiology procedure areas, or the cafeteria. The emergency department, operating room and labor and delivery run their own codes and our radiology suites, and the cafeteria codes are run by the emergency department staff, not the Code Blue Team. A two-sample t-test was used for numerical data and a chi-square was used for proportional data to see if there is a difference between code blue outcomes between 2018 and 2019. All analyses were performed in Microsoft Excel, or SAS version 9.4 (SAS Institute, Cary, NC). Hypothesis tests were two-sided and evaluated at a significance level of 0.05. One author maintained full access of all data collected, its integrity and analysis.
Results
Dedicated chest Compressor Team performance
In total, 46 Lift Team members participated in the Designated Chest Compressor Team quarterly training program. Due to changes in staffing, the number of participants in each quarterly training ranged from 14-39 (See Table 1). Of the 46 participants, 43 (93.5%) were male and three females (6.5%). One individual completed all five quarterly training sessions, whereas 32 Lift Team members completed between two to four trainings.
Table 1.
Lift Team (LT) Quarterly Training Scores.
| Quarter | Number of Participants | Score 1 Average |
Score 2 Average |
Average Training Score |
|---|---|---|---|---|
| Q4-2018 (Pre) | 39 | 49.1 | 80.3 | 64.7 |
| Q1-2019 (Int) | 24 | 79.8 | 86.1 | 83.0 |
| Q2-2019 (Post) | 14 | 76.7 | 64.4 | 70.6 |
| Q3-2019 (Post) | 14 | 76.1 | 71.4 | 73.8 |
| Q4-2019 (Post) | 23 | 72.3 | 85.3 | 78.8 |
LT indicates Lift Team; Q4 indicates Quarter 4 calendar year; Q1 indicates quarter 1 calendar year; Q2 indicates quarter 2 calendar year; Q3 indicates quarter 3 calendar year; Q4 indicates quarter 4 calendar year.
Quality of CPR performance was scored according to the high-fidelity mannikin system from 0-100%, with a score of 70% indicating good quality CPR. During the initial training, prior to feedback, the average score was 49.1% (See Table 1). After receiving feedback and coaching, the average score increased to 80.3%, with 95% (n = 37) of participants achieving a higher score after feedback. Of the 33 Dedicated Chest Compressor Team members who completed two or more trainings, 91% (n = 30) improved their scores. The effects of this training were evident in the patient outcomes. The survival of event (ROSC achieved), prior to this training, was 61.0% in January-October 2018. Post-training January-December 2019, event survival (ROSC achieved), rose to 73.5% (p = 0.03).
An unexpected result from this training was the increase in confidence of the Dedicate Chest Compressor Team members and receiving positive feedback on the consistency and quality of their chest compressions. During the initial training, Dedicated Chest Compressor Team members shared that they felt undervalued as code blue team members and that others critiqued their compression performance but did not offer feedback. The Dedicated Chest Compressor Team members were strongly encouraged to advocate for themselves by mastering skills and modeling best practices learned during training. Through frequent simulation and objective feedback on CPR performance, this training program helped to empower them to voice concerns and needs during IHCA events. For example, one Dedicated Chest Compressor Team member, noted on their training evaluation form, “During a code blue event, I feel like I have a voice now”. In addition, Dedicate Chest Compressor Team members reported developing a strong rapport during code blue situations. They encouraged each other to provide good chest compressions, using the defibrillator for objective feedback on chest compression rate and depth as well as tracking compression time themselves and switching out compressors as needed. The improvements in CPR quality were also recognized by other code blue team members. In one scenario, a critical care nurse shared with supervisors, “The Lift Team provided phenomenal CPR… I heard a physician say he has never seen compressions like those which were provided”. In addition to improving CPR quality and IHCA event survival, we saw increased confidence within the Dedicated Chest Compressor Team.
IHCA event survival
In comparing code blue events between January-October 2018 and January-December 2019, there was a statistically significant difference between survival event (ROSC achieved: 61.0% vs 73.5%, p = 0.03) and survival to discharge (20.4% vs 34.5%, p = 0.01). There was no significant difference seen in age, event duration, sex, or Intensive Care Units vs Non-Intensive Care Units (See Table 2).
Table 2.
IHCA Outcomes.
| Jan – Oct 2018 (N = 100) |
Jan – Dec 2019 (N = 201) |
||||
|---|---|---|---|---|---|
| N | Mean (SD) | N | Mean (SD) | p-value | |
| Patients’ Age | 98 | 61.3 (15.94) | 201 | 59.3 (17.6) | 0.34 |
| Female | 42 | 42.0% | 68 | 33.8% | 0.17 |
| Event Duration (minutes) | 100 | 19.6 (20.3) | 155 | 16.7 (14.4) | 0.22 |
| N | % | N | % | p-value | |
| ROSC achieved* | 61 | 61.0% | 147 | 73.5% | 0.03 |
| Survived to Discharge** | 20 | 20.4% | 69 | 34.5% | 0.01 |
| Intensive Care Unit | 74 | 74.0% | 150 | 74.6% | 0.91 |
SD indicates standard deviation.
One missing in 2019.
Two missing for 2018 and one missing for 2019.
Discussion
In this quality improvement initiative, we found that implementing a quarterly training program for our Dedicated Chest Compressor Team improved CPR skills and IHCA survival. The quarterly training sessions helped Dedicate Chest Compressor Team members retain CPR psychomotor skills and improve their baseline CPR performance. Team members demonstrated higher scores with frequent training and consistent feedback.
To date, we know of no other projects that have compared more frequent CPR training for dedicated personnel performing compressions and IHCA event survival. Klacman et al. reported the effects of quarterly CPR training and compression skill retention. However, they indicated that more research into how training correlates to real-time IHCA survival is needed.16 This program helps bridge that gap and shows improvement in IHCA survival through achievement of ROSC.
Code blue team member roles, tasks, and compression training using feedback simulation manikins are essential factors in the performance of high-quality CPR.3, 4, 5, 9, 10 The Dedicate Chest Compression Team members who attended the quarterly CPR training program showed improved quality of CPR performance and maintained these skills over the one-year of the initiative. Not only have varying rates of skills acquisition been documented after traditional AHA training classes, but also, universally poor skill performance of providers 3 to 6 months after CPR training has been noted.6 Oerman et al. reported in their 2011 study that participants who practiced frequently had higher compression rates and better compression depths than participants in the control group. Whereas participants in the control group lost their ability to compress between 9 and 12 months.9 By practicing CPR skills quarterly and receiving specific and instructional feedback on delivering high-quality CPR, the Dedicated Chest Compressor Team members retained skills and developed their expertise in CPR performance.
Based on the success of the initial program, in May 2020, we developed a train-the-trainer class to ensure sustainability of the Dedicated Chest Compressor Team Quarterly CPR Skills Training Program. The Lift Team leadership attended the CPR instructor training, which included how to a) use instructor training materials; b) deliver trainee coaching; c) provide an audio-visual skills performance evaluation using the high-fidelity manikin; d) follow quarterly CPR training program guidelines; and e) use, maintain and troubleshoot the manikin and equipment. The Lift Team department was provided with a high-fidelity manikin system.
Utilizing the methods obtained during the train-the-trainer class and the high-fidelity manikin, in Fall 2020, Lift Team leadership assumed responsibility of facilitating ongoing CPR quarterly training. They were provided a high-fidelity manikin system to allow for greater flexibility in scheduling and completing the quarterly training. Each quarter Lift Team provides an attendance roster to the nursing education department, reporting staff attendance of the training for tracking in the hospital’s learning management system.
Limitations
This initiative has several important limitations. First, this initiative was performed at a single, academic, urban institution and may not generalize to other hospitals that do not utilize a Dedicated Chest Compressor Team or employ a Lift Team department. Second, we recognize our Lift Team Department had changes in staffing and members transitioned to employment in different departments within the hospital. This effected the consistency of individual members training and the number of participants coming through each of the quarterly training program, creating a limitation to adherence in training. Third, chest compressions are only one variable contributing to treatment during an IHCA event. We acknowledge that there are many other patient illness severities, treatment factors and post resuscitation processes (therapeutic temperature management and coronary reperfusion strategy)that contribute to patient survival (ROSC) that were not included.
While we provide information regarding patient age and code length, we do not control for these other factors in our analysis examining overall IHCA event survival over the project timeline. Along this line, we examined immediate IHCA event survival rather than survival to hospital discharge, which is a more common patient outcome associated with IHCA but is further impacted by additional factors unrelated to CPR performance. Lastly, we included each code blue as an individual event rather than indexing at the patient level. Therefore, if a patient had more than one code blue event, each event was counted separately, which might lower our IHCA ROSC rate, as the more times a person has an event, their likelihood of survival diminishes.
Conclusion
Our quality improvement initiative provides the preliminary evidence to support implementation of a quarterly chest compression training program to increase the quality of CPR performed by designated personnel performing chest compressions during IHCA. We achieved our goal to provide quarterly CPR training to the Dedicated Chest Compressor Team, improve individuals’ chest compression skills, and sustain the program long-term. More importantly, we also found the Dedicated Chest Compressor Team Quarterly CPR Training Program benefited patient outcomes, as demonstrated through an overall increase in IHCA event survival.
Conflict of Interest
None.
CRediT authorship contribution statement
Amanda O'Leary: Conceptualization, Methodology, Software, Validation, Investigation, Data curation, Writing – original draft, Writing – review & editing, Visualization, Supervision, Project administration. Polly Butler: Conceptualization, Methodology, Software, Validation, Resources, Writing – original draft, Writing – review & editing, Visualization, Supervision, Project administration. Jeffrey Fine: Software, Formal Analysis, Data Curation, Writing – review & editing.
Acknowledgments
We would like to acknowledge the Lift Team for participating in this training program and assuming ongoing leadership in sustaining high-quality CPR practices. Their dedication to improving CPR skills and sustaining the training program is impressive and supports improving patient care. We would also like to thank the Code Blue Committee, Kelly MacPherson, and Marcus Christian for their collaboration, as well as Sarina Fazio and the Center for Nursing Science and the Clinical and Translational Science Center for assistance with manuscript preparation.
Contributor Information
Amanda O'Leary, Email: aamichalski@ucdavis.edu.
Polly Butler, Email: pollybutler206@gmail.com.
Jeffrey R. Fine, Email: jrfine@ucdavis.edu.
References
- 1.Holmberg M.J., Ross C.E., Fitzmaurice G.M., et al. Annual incidence of adult and pediatric in-hospital cardiac arrest in the United States. Circ Cardiovasc Qual Outcomes. 2019;12 doi: 10.1161/circoutcomes.119.005580. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Benjamin E.J., Muntner P., Alonso A., et al. Heart disease and stroke statistics—2019 update: A report from the American Heart Association. Circulation. 2019;139 doi: 10.1161/cir.0000000000000659. [DOI] [PubMed] [Google Scholar]
- 3.Nallamothu B.K., Guetterman T.C., Harrod M., et al. How do resuscitation teams at top-performing hospitals for in-hospital cardiac arrest succeed? Circulation. 2018;138:154–163. doi: 10.1161/circulationaha.118.033674. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Fernandez Castelao E., Russo S.G., Riethmüller M., Boos M. Effects of team coordination during cardiopulmonary resuscitation: A systematic review of the literature. J Crit Care. 2013;28:504–521. doi: 10.1016/j.jcrc.2013.01.005. [DOI] [PubMed] [Google Scholar]
- 5.Cheng A., Nadkarni V.M., Mancini M.B., et al. Resuscitation education science: Educational strategies to improve outcomes from cardiac arrest: A scientific statement from the American Heart Association. Circulation. 2018;138 doi: 10.1161/cir.0000000000000583. [DOI] [PubMed] [Google Scholar]
- 6.Sutton R.M., Niles D., Meaney P.A., et al. Low-dose, high-frequency CPR training improves skill retention of in-hospital pediatric providers. Pediatrics. 2011;128 doi: 10.1542/peds.2010-2105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Hunt E.A., Jeffers J., McNamara L.A., et al. Improved cardiopulmonary resuscitation performance with code aces 2: A resuscitation quality bundle. J Am Heart Assoc. 2018;7 doi: 10.1161/jaha.118.009860. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Saramma P.P., Raj L.S., Dash P.K., Sarma P.S. Assessment of long-term impact of formal certified cardiopulmonary resuscitation training program among nurses. Indian Journal of Critical Care Medicine. 2016;20:226–232. doi: 10.4103/0972-5229.180043. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Oermann M.H., Kardong-Edgren S.E., Odom-Maryon T. Effects of monthly practice on nursing students’ CPR psychomotor skill performance. Resuscitation. 2011;82:447–453. doi: 10.1016/j.resuscitation.2010.11.022. [DOI] [PubMed] [Google Scholar]
- 10.Panchal A.R., Norton G., Gibbons E., Buehler J., Kurz M.C. Low dose- high frequency, case based psychomotor CPR training improves compression fraction for patients with in-hospital cardiac arrest. Resuscitation. 2020;146:26–31. doi: 10.1016/j.resuscitation.2019.10.034. [DOI] [PubMed] [Google Scholar]
- 11.Meaney P.A., Bobrow B.J., Mancini M.E., et al. Cardiopulmonary resuscitation quality: Improving cardiac resuscitation outcomes both inside and outside the hospital. Circulation. 2013;128:417–435. doi: 10.1161/cir.0b013e31829d8654. [DOI] [PubMed] [Google Scholar]
- 12.Wilson-Sands C., Brahn P., Graves K. The effect of instructional method on cardiopulmonary resuscitation skill performance. J Nurses Prof Dev. 2015;31 doi: 10.1097/nnd.0000000000000203. [DOI] [PubMed] [Google Scholar]
- 13.Oermann M.H., Kardong-Edgren S.E., Roberts C.J., Odon-Maryon T. Effects of practice on competency in single-rescuer cardiopulmonary resuscitation. Med Surg Nurs. 2014;23:22–28. [PubMed] [Google Scholar]
- 14.Brennan E.E., McGraw R.C., Brooks S.C. Accuracy of instructor assessment of chest compression quality during simulated resuscitation. CJEM. 2016;18:276–282. doi: 10.1017/cem.2015.104. [DOI] [PubMed] [Google Scholar]
- 15.Kleinman M.E., Brennan E.E., Goldberger Z.D., et al. Part 5: Adult basic life support and cardiopulmonary resuscitation quality. Circulation. 2015;132 doi: 10.1161/cir.0000000000000259. [DOI] [PubMed] [Google Scholar]
- 16.Klacman A., Barnes D., Wang J. The effects of a novel quarterly cardiopulmonary resuscitation training program on hospital basic life support providers’ cardiopulmonary resuscitation skill performance. J Nurses Prof Dev. 2021;37:131–137. doi: 10.1097/nnd.0000000000000727. [DOI] [PubMed] [Google Scholar]