Abstract
Scant research has explored the healthcare experiences of people with Down syndrome (DS) in the United States who are Black, African American, of African descent, or of mixed race. The purpose of this study was to identify and describe the barriers and facilitators that such patients and their caregivers face when accessing healthcare. We gathered data in three ways: focus groups with caregivers, a national survey completed by caregivers, and in-depth interviews with primary care providers. Many caregivers and primary care physicians felt that patients with DS who are Black, African American, of African descent, or of mixed race receive a lower quality of medical care than their white counterparts with DS. Caregivers mentioned feeling tired of being reminded by the medical community about their race and wanting acknowledgment that raising a child with DS can be hard at times. Many felt that the medical community’s conscious and unconscious racial biases do negatively impact the care of their loved ones with DS. Caregivers desired more race concordant medical providers or, when not possible, medical providers who are willing to learn more about DS and build trusted, longitudinal relationships. Primary care providers discussed the need for funded resources and support services to effectively care for their patients with DS.
Keywords: Down syndrome, trisomy 21, race, Black, African American, diversity, equity, inclusion, disparity
1. INTRODUCTION
The overwhelming majority of people with Down syndrome (DS) do not have access to DS specialty clinics, a disparity resulting in delayed or missed diagnoses and significant untreated co-morbidities.1–4 Research further suggests that this unfortunate reality is likely far worse for families who are Black/African American and/or primarily Spanish-speaking.5–8
Racial and ethnic disparities impact access to health services.9 Such disparities cannot be solely attributed to prejudice and discrimination on an individual level. Disparities such as these largely stem from systemic and structural roots, reflecting both racist beliefs but also culturally reinforced and historically rooted institutional practices in healthcare.10,11
Recent research has begun to examine these issues more closely. The 2018 National Healthcare Quality and Disparities Report showed that for over 70 measures of care coordination, effective treatment, healthy living, patient safety, and person-centered care, Black patients, in general, received worse quality of care compared to white patients.12 Other studies have shown that harmful beliefs about biological differences between Black and white people are often present during early years of medical training.13 In a 2016 study that assessed racial attitudes among white medical students and residents, researchers found that about half believed that Black patients’ pain is less severe than that of white patients.13
Racial and ethnic disparities have also been found for children with DS.5,8,14 Previous research demonstrated that compared to children with DS of non-Hispanic white mothers, children with DS of non-Hispanic Black mothers incurred significantly greater medical costs and hospital use, as well as greater cardiac disease burden.7
While DS occurs naturally in all races and ethnicities, population size, maternal age differences, and selective termination preferences influence the number of live births for different races and ethnicities. As of 2010, more than 27,000 non-Hispanic Blacks with DS are estimated to be living in the U.S.15 As a result of ethnic differences in childhood survival, there are also some racial and ethnic differences in life expectancy. For people with DS who are non-Hispanic blacks, researchers estimated the mean and median life expectancy were 22 years (mean) and 2 (median) years in 1950 and 50 (mean) and 57 (median) years in 2010. For people with DS who are non-Hispanic whites, they estimated that mean and median life expectancy rates were 26 years (mean) and 4 years (median) in 1950 and 54 years (mean) and 58 years (median) as of 2010. As such, racial differences in life expectancy for people with DS remain, but the gap appears to be decreasing.15
We were not able to identify any previous work assessing the lived experiences of caregivers of a loved one with DS who is Black or African American. Previous research, though, has examined racial barriers for other populations with intellectual or developmental disabilities. One study examined families from different racial/ethnic minority backgrounds who had a loved one with autism spectrum disorder (ASD), attention deficit hyperactivity disorder (ADHD), or intellectual disability.16 While white and racial/ethnic minority families raising a child with ASD or ADHD showed some similarities in experiencing wellbeing as caregivers, racial/ethnic minority families faced additional barriers including racial discrimination, smaller support network, and more severe stigma within the family and community.16 Another study identified a sense of distrust among Black adults with intellectual or developmental disabilities toward their healthcare providers.17
For this pilot study, we seek to uncover and understand the barriers and facilitators to quality health care, per the caregivers who have a child with DS who is Black, African American, of African descent, or mixed race. The purpose of this study is to build on this previous literature and (1) identify what barriers and facilitators Black families face when accessing health care for their loved ones with DS and (2) synthesize culturally appropriate recommendations to improve healthcare experiences.
2. MATERIALS AND METHODS
2.1. Project leaders
The Massachusetts General Hospital Down Syndrome Program (MGH DSP) is a DS specialty clinic in Boston, Massachusetts, that provides multidisciplinary, comprehensive care across the lifespan for people with DS. This research study was conducted by several MGH DSP team members, including physicians, research assistants, and a Diversity Outreach Specialist, whose role was crafted to specifically implement the aims of this research. Our team was complemented by a survey methodologist from the MGH Mongan Institute. Key stakeholders, including an Expert Advisory Group, Caregiver Working Group, and Primary Care Provider (PCP) Working group, contributed regularly to all aspects of this project (Supplementary Figure 1). The Expert Advisory Group consisted of leaders from two non-profit organizations: the LuMind IDSC Down Syndrome Foundation and the Massachusetts Down Syndrome Congress (MDSC). The Caregiver Working Group consisted of five Black/African American and/or Spanish-speaking caregivers who have a loved one with DS living in the United States. The PCP Working Group consisted of five Black/African American and/or Spanish-speaking PCPs who care for people with DS in the United States. Our project was reviewed and approved by the Massachusetts General Brigham Institutional Review Board.
2.2. Participants
Caregivers invited to participate in the focus groups and online survey were required to have a son or daughter with DS who lived in the U.S. and identified as Black, African American, of African descent, or of mixed race. (For purposes of this paper, we will shorten the phrasing to “Black/African American.”)
For this study, caregivers needed to identify English as their primary language. This study was part of a larger effort that also included key findings from Spanish-speaking families, whose findings will be reported elsewhere.
PCPs invited to participate were required to practice in the United States and take care of at least one patient with DS that is Black/African American and/or Spanish-speaking. PCPs could be physicians, nurse practitioners, or physician assistants (associates).
2.3. Data collection
We collected our data from three sources: (1) caregiver focus groups, (2) caregiver questionnaires, and (3) in-depth interviews from PCPs (Supplementary Figure 1).
Caregiver Focus Groups:
Eligible caregivers were grouped and asked to meet over an encrypted Zoom meeting for a discussion lasting approximately one hour. A moderator from the MGH Research Team asked a set of predetermined questions to prompt a discussion among the caregivers. The questions were generated and revised based on critical inputs from our physician, caregiver, and advocacy stakeholders (Supplementary Materials). Caregivers were compensated $50.00 for their participation in a focus group. Informed consent was obtained verbally from all participants prior to participation.
PCP interviews:
Eligible PCPs were invited to talk individually with an interviewer from the MGB Research Team for a 30-minute encrypted Zoom meeting. The interviewer followed an interview guide of questions generated and revised by our physician, caregiver, and advocacy stakeholders (Supplementary Materials). PCPs were compensated $50.00 for their participation. Informed consent was obtained verbally from all participants prior to participation.
Caregiver Survey:
A novel questionnaire consisting of 20 forced-choice and free-response questions was distributed to caregivers online and by mail (Supplementary Materials). Some survey items were adapted from validated survey instruments including the National Institute of Health’s Health Information National Trends Survey (HINTS) and the Agency for Healthcare Research and Quality’s Consumer Assessment of Healthcare Providers and Systems (CAHPS) Clinician & Group Survey 3.0.18,19 Many survey items were developed in consultation with Dr. Karen Donelan, ScD, EdM, Director of Survey Research at the MGH Mongan Institute. The survey instrument was also revised based on the critical inputs from our physicians, caregivers, and advocacy stakeholders. Study data were collected and managed using REDCap electronic data capture tools hosted at Massachusetts General Hospital.20,21 Eligible caregivers were asked to fill out the survey but were not required to answer every question. Caregivers who completed the online survey were not compensated for their time. Written informed consent was waived; participants needed to read and acknowledge an informational page before proceeding with the survey.
2.4. Recruitment
Caregiver focus groups:
Caregivers were recruited mostly through social media platforms, including the Facebook, Twitter, and Instagram pages of the MGH DSP, MDSC, LuMind IDSC Down Syndrome Foundation. Dr. Brian Skotko and some members of the Caregiver and PCP Working Groups also posted the invitations on their personal social media accounts. The Caregiver Working Group also spread the opportunity throughout their personal networks and through word-of-mouth. This focus group opportunity was also mentioned in MGH DSP, MDSC, and LuMind IDSC Foundation newsletters and e-newsletters. The PCP working group shared this opportunity with caregivers that may be eligible. Some caregivers were recruited directly if they were eligible and had previously participated in a research project with the MGH DSP in the past, noting that they would like to hear about our future projects. Any person interested in participating in a focus group filled out a screening survey to determine their eligibility.
In total, we conducted three focus groups in English with a total of 14 primary caregivers of a loved one with DS that identify as Black/African American. All focus groups were conducted on an encrypted Zoom meeting, recorded with permission, and transcribed.
Caregiver surveys:
We used all of the same recruitment strategies employed for the caregiver focus groups. In addition, we sent an e-mail to 321 DS non-profit organizations, asking them to share the survey link with their members and also gave them the opportunity to request hard-paper copies of the survey for local distribution. We also sent the opportunity out to caregivers through DS-Connect, which serves as a central place for families to receive information about research studies related to DS. Finally, we identified all MGH patients with DS identifying as Black/African American using a hospital systems-wide centralized clinical data registry (Research Patient Data Registry or RPDR) and sent an electronic message to their caregivers via the electronic health portal (Patient Gateway).
We attempted to reach caregivers who may not have access to a laptop or the Internet by providing paper surveys to outreach organizations. We prepared 100 paper copies in English and Spanish of the survey, complete with a self-addressed stamped envelope. We had requests from DS non-profit groups for 65 paper surveys, and we did not receive any completed surveys through the mail prior to our analysis.
PCP interviews:
PCPs were recruited from social media platforms, including the Facebook, Twitter, and Instagram pages of the MGH DSP and LuMind IDSC Down Syndrome Foundation. Dr. Brian Skotko and some members of the Caregiver and PCP Working Groups also posted the invitations on their personal social media accounts and also made personal outreach by e-mail and telephone to eligible PCPs. Our team also contacted the following professional medical organizations, asking them to share our recruitment notices with eligible members. These organizations were either not able to support this request or did not respond to our outreach.
American Academy of Family Physicians
American Academy of Pediatrics
American Board of Family Practitioners
American Board of Internal Medicine
American Board of Pediatrics
American College of Osteopathic Family Physicians
American Medical Association
Association of American Medical Colleges
Florida Medical Association
Medical Society of District of Columbia
Medical Society of the State of New York
Mississippi State Medical Association
National Medical Association
In total, we conducted 20 in-depth interviews on an encrypted Zoom meeting with PCPs. Each interview was recorded and transcribed.
2.5. Analyses
Caregiver Focus Groups and PCP interviews:
A preliminary topic guide was developed for survey interviews and focus groups. The caregiver focus groups and PCP interviews were conducted virtually over Zoom, audio-recorded, and transcribed verbatim for data analysis through TranscribeMe. Qualitative analyses were performed with Dedoose, version 9.0.17. Qualitative data analysis used a rapid, pragmatic approach used in mental health services research and successfully by research collaborators in prior work.22,23 We used an inductive coding approach in which predetermined codes were applied to the data. A team of three coders worked independently to code each transcript and then met to review code applications. Each coded passage in the transcripts was reviewed and discussed until consensus on code application was achieved. Where the codebook was unclear or needed additional examples, modifications were identified and incorporated. This process of codebook application, refinement, and consensus-building was repeated for each transcript until coding was complete. Code frequencies and the strength and quality of the coded passages were used to inform a final set of codes sorted into themes.
Caregiver Survey:
Standard summary statistics were used to analyze the quantitative responses. Open-ended responses were analyzed using qualitative coding methods described above to identify key themes. Fisher’s exact test was used to compare some of the results from our respondents to those from previous publications.24
3. RESULTS
3.1. Demographics
In total, we had 14 parents/caregivers participate in our 3 focus groups of English speaking Black/African American caregivers (Table 1). An additional 68 English-speaking parents/caregivers of a child with DS who was Black, African American, of African descent, or of mixed race completed our online survey (Table 1). The respondents came from a variety of U.S. states, with the majority being from Massachusetts, Pennsylvania, California, Florida, Georgia, Maryland, and Virginia (Supplementary Figure 2). We also conducted in-depth videoconference interviews, over Zoom, with 20 PCPs.
Table 1:
Demographics
| Focus Groups (N = 14) | Number of Participants | % of Participants |
|---|---|---|
| Gender of person with Down syndrome represented by caregiver | ||
| Male | 11 | 78.6 |
| Female | 2 | 14.3 |
| Unknown | 1 | 7.1 |
| Race of person with Down syndrome represented by caregiver | ||
| Black/African American | 14 | 100.0 |
| Ethnicity of person with Down syndrome represented by caregiver | ||
| Non-Hispanic | 14 | 100.0 |
| Age of person with Down syndrome (years) represented by caregiver | ||
| 0–4 | 1 | 7.1 |
| 5–12 | 7 | 50.0 |
| 13–20 | 5 | 35.7 |
| 21 or older | 1 | 7.1 |
| Unknown | 0 | 0 |
| Caregiver race | ||
| Black/African American | 11 | 78.6 |
| White | 1 | 7.1 |
| Unknown | 2 | 14.3 |
| Caregiver ethnicity | ||
| Non-Hispanic | 14 | 100.0 |
| Caregiver relationship to person with Down syndrome | ||
| Mother | 10 | 71.4 |
| Father | 2 | 14.3 |
| Uncle | 1 | 7.1 |
| Unknown | 1 | 7.1 |
| U.S. region where caregiver resides | ||
| West | 0 | 0.0 |
| Midwest | 2 | 14.3 |
| Northeast | 8 | 57.1 |
| South | 0 | 0.0 |
| Southwest | 1 | 7.1 |
| Unknown | 3 | 21.4 |
| PCP Interviews (N=20) | ||
| PCP Gender | ||
| Male | 1 | 5.0 |
| Female | 19 | 95.0 |
| PCP Race | ||
| Black/African American | 3 | 15.0 |
| White | 12 | 60.0 |
| Multi-race | 2 | 10.0 |
| Asian | 2 | 10.0 |
| Unknown | 1 | 5.0 |
| PCP Ethnicity | ||
| Hispanic/Latino(a) | 7 | 35.0 |
| Non-Hispanic | 13 | 65.0 |
| U.S. Region where PCP practices medicine | ||
| West | 10 | 50.0 |
| Midwest | 3 | 15.0 |
| Northeast | 5 | 25.0 |
| South | 0 | 0.0 |
| Southwest | 2 | 10.0 |
| English-speaking caregivers who had children with Down syndrome who were Black, African American, of African descent, or of mixed race (N=68) | ||
| Relation to the person with DS | ||
| Mother or step-mother | 50 | 73.5 |
| Father or step-father | 6 | 8.8 |
| Sibling, half-sibling, or step-sibling | 1 | 1.5 |
| Blank | 11 | 16.2 |
| Race of caregiver | ||
| Black/African American | 44 | 64.7 |
| White | 8 | 11.8 |
| Multi race | 5 | 7.4 |
| Other | 2 | 2.9 |
| Blank | 9 | 13.2 |
| Hispanic, Latino/a, or Spanish origin | ||
| No | 52 | 76.5 |
| Yes | 6 | 14.7 |
| Blank | 10 | 8.8 |
| Caregiver’s last grade completed | ||
| More than college | 26 | 38.2 |
| College graduate (B.S. or B.A.) | 11 | 16.2 |
| Some college or technical/vocational school | 16 | 23.5 |
| High school graduate (grade 12 or GED) | 5 | 7.4 |
| Blank | 10 | 14.7 |
| Insurance for person with DS* | ||
| Private health insurance | 31 | |
| Medicaid | 31 | |
| Medicare | 4 | |
| Military health care (TRICARE/VA/CHAMP) | 4 | |
| Indian health service | 1 | |
| Other | 5 |
More than one option available; as such, counts do not add up to total number of respondents.
3.2. Perspectives from PCPs who take care of patients with DS who are Black, African American, of African descent, mixed race, or whose household is primarily Spanish-speaking
PCPs identified many barriers that prevented them from providing high-quality medical care for their patients with DS who are Black (Supplementary Table 1). Limited time and resources often prevent the necessary care coordination and team-based approach that is desired. PCPs consider the American Academy of Pediatrics a helpful clinical resource, while underscoring the importance of continued medical education about DS (Supplementary Table 2).
PCPs emphasized that time is needed to build a longitudinal relationship centered around trust with families who have Black loved ones with DS (Supplementary Table 3). PCPs should encourage parents to ask questions, while being careful to listen to their specific needs. Whenever feasible, PCPs also recommended that Black families also access DS specialty clinics for care augmentation. Medical costs, transportation barriers, competing demands on parents, and medical literacy were all cited as perceived barriers for these families (Supplementary Table 4).
3.3. Healthcare experiences of people with DS who are Black, African American, of African descent, or of mixed race
3.31. Caregivers’ Experience with Healthcare
Of the 68 caregivers who responded to our online survey, 53% of caregivers feel that patients with DS who are Black receive lower quality of medical care than most white patients with DS (Figure 1). Approximately, 59% of them felt that patients with DS who do not speak English receive lower quality of medical care than most white patients with DS, and about 37% of caregivers feel that patients with DS who are Latino/a receive lower quality of medical care than most white patients with DS.
Figure 1.
“For each of the following groups of patients with Down syndrome, do you think most receive a higher quality of medical care, same quality of medical care, or lower quality of medical care than most white patients with Down syndrome?” N = 68 people with Down syndrome who are Black, African American, of African descent, or of mixed race, as reported by their caregivers (counts per response choice listed in bars)
Within the past year, 26% of caregivers have personally felt that doctors, nurses, or other hospital staff treated their loved one with DS unfairly or with disrespect because of their race or ethnicity (Figure 2). Approximately 25% of caregivers felt the same because of their loved one’s disability. Respondents were less likely to feel disrespected because of their ability to pay for care or because of their religious or cultural beliefs.
Figure 2.
“Please think about all of the experiences you have had with health care visits in the LAST YEAR. Have you personally felt that doctors, nurses, or other hospital staff treated your loved one with Down syndrome unfairly or with disrespect because…” N = 68 people with Down syndrome who are Black, African American, of African descent, or of mixed race, as reported by their caregivers (counts per response choice listed in bars)
When it comes to personal preferences, 63% of caregivers felt it is important for clinicians to be from the same racial or ethnic background as their loved one with DS (Figure 3). Approximately 53% of caregivers felt it is important for clinicians to share the same religious or cultural beliefs, and approximately 37% of caregivers felt it is important for clinicians to be of the same gender as their loved one with DS.
Figure 3.
“In general, how important is it to you to have your loved one be cared for by…” N = 68 people with Down syndrome who are Black, African American, of African descent, or of mixed race, as reported by their caregivers (counts per response choice listed in bars)
3.32. Barriers Accessing Healthcare and Sources for Health Information
Of the 68 caregivers who responded to our online survey, 59% of them worried to some extent that their loved one with DS will be treated with respect when referred for a diagnostic test or appointment (Figure 4). There were 53% of parents who worried about taking time off from work to attend these tests and appointments. Approximately 51% of caregivers worried about themselves being treated with respect, and about half worries about the associated out-of-pocket expenses. Fewer families worried about transportation barriers.
Figure 4.
“When your loved one with Down syndrome has been referred for a diagnostic test or appointment, have you worried about any of the following?” N = 68 people with Down syndrome who are Black, African American, of African descent, or of mixed race, as reported by their caregivers (counts per response choice listed in bars)
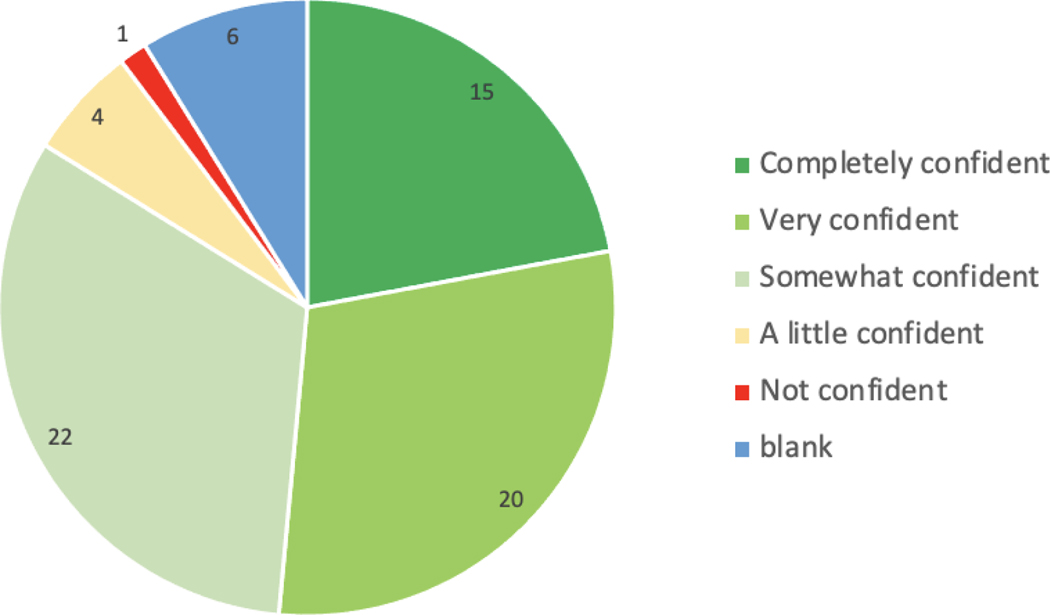
When it comes to searching for information about DS, 54% of caregivers felt some degree of frustration and 47% reported that it took a lot of effort to find that information (Figure 5). However, 84% of caregivers felt at least somewhat confident that they could get information about DS if they needed it (Figure 6). The most trusted messengers of healthcare information are, in decreasing order of importance, doctors, hospital/clinic web pages, charitable organizations, the Internet, government health agencies, family/friends, and religious organizations/leaders (Figure 7). The parents who participated in the focus groups cited many of the same trusted messengers (Supplementary Table 5).
Figure 5.
“Based on the results of your most recent search for information about Down syndrome, how much do you agree or disagree with each of the following statements?” Two statements: “It took a lot of effort to get the information you needed”; “You felt frustrated during your search for information.” N = 68 people with Down syndrome who are Black, African American, of African descent, or of mixed race, as reported by their caregivers (counts per response choice listed in bars)
Figure 6.
“Overall, how confident are you that you could get advice or information about Down syndrome if you needed it?” N = 68 people with Down syndrome who are Black, African American, of African descent, or of mixed race, as reported by their caregivers (counts per response choice listed in bars)
Figure 7.
“In general, how much would you trust information about Down syndrome from each of the following?” N = 68 people with Down syndrome who are Black, African American, of African descent, or of mixed race, as reported by their caregivers (counts per response choice listed in bars).
3.33. In Their Own Words: Role of Race and Ethnicity in Experience of Care, According to Caregivers
In our focus groups, some, but not all, caregivers who have Black loved ones with DS preferred clinicians who were racially and ethnically concordant (Supplementary Table 6). They were more likely to trust the medical system if they perceived the medical care to be high quality and coming from a compassionate provider. Endorsements from other caregivers are often important, and many families are looking to develop long-term relationships with their loved one’s providers. Among the biggest barriers to medical care occurred when parents perceived providers to be dismissive or not knowledgeable of the needs for their loved one with DS (Supplementary Table 7). Insurance and medical costs can be roadblocks to care. Many perceived episodes of systemic racism in the medical system.
In our survey, 63% of caregivers reported that race and/or ethnicity impacted the care of their loved one with DS. Said one parent, “We as parents are treated like we’re stupid and can’t make educated decisions for our child. We are also treated as if we can’t afford quality treatment and care. When our son excels, people are extremely condescending.” About 86% of respondents believe that there is an environment of bias and discrimination. Said one parent, “My child is biracial; his mother is black, and father is white. When attending an appointment with his mother, he is treated with less respect, and procedures are not explain[ed] thoroughly and questions are not treat[ed] [with] respect or concern.”
There were 13 respondents who felt that the medical community was condescending and not always taking their loved one with DS seriously. Said one parent, “I believe I have always had to demonstrate the fact that I was educated in the first meeting with doctors so they would treat us with respect.” Ten parents shared personal stories of discrimination. Said one caregiver, “During her hospital stay, a NP and the doctor-on-call attempted to discharge her for inexplicable reasons since they decided she was not as sick as the pediatrician believed. We refused to allow them to discharge her knowing that she was in crisis.” Eight parents reported difficulty in accessing high quality care and services. Said one parent, “…I notice that in underfunded areas that have black doctors, he is treated well but they have a lack of resources and a huge over run of patients so the time and attention is NOT up to par.” Six parents mentioned that more competent DS specific care is needed. “I am my child’s advocate. Our experiences have been positive so far after 17 years. I just wish doctors had more information, training, and resources for people with DS. It’s a problem,” said one parent. Five parents felt that their loved one had received good care with no concerns. Said one parent, “I’ve felt that all providers have treated my child with care and love regardless of their race or ethnicity.” There were four parents who felt medical care was often rushed. Said one caregiver, “[I] Feel as if they didn’t check in as much, and was spoken to as if I couldn’t understand what my baby was going through. Also rushed conversations.” Three or fewer parents mentioned that language could be a barrier. Facilitations could include living in diverse, urban areas. Some parents felt that “lighter-skinned” Black families received better medical care.
4. DISCUSSION
Many caregivers and PCPs felt that patients with DS who are Black, African American, of African descent, or of mixed race receive a lower quality of medical care than their white counterparts. Their responses were also similar to non-Hispanic Black respondents on the latest Health Information National Trends Survey (HINTS), a national survey about health information seeking, confidence, and trust of health information sources.24 Both populations reported similar levels of being completely or very confident in getting health information (our respondents: 56.5%; HINTS: 63.5%, p = 0.20). Both groups also similarly reported “not a lot” of trust in family and friends (our respondents: 91.7%; HINTS: 92.0%, p = 0.82), the Internet (our respondents: 86.9%; HINTS: 81.0%, p = 0.27), charitable organizations (our respondents: 82.0%; HINTS: 88.9%, p = 0.12). Our respondents differed from the national sample on being more likely to have “not a lot” of trust doctors and health professionals (our respondents: 50.8%; HINTS: 29.3%, p < 0.001), governmental agencies (our respondents: 78.7%; HINTS: 65.0%, p = 0.01), and religious organizations (our respondents: 98.8%; HINTS: 89.0%, p = 0.008). This may be due to the specific nature of a DS diagnosis, as measured in our study, versus the more general nature of health care, as measured in HINTS. There are specific medical guidelines for people with DS, which families have noted might not always be known to the practicing medical provider. People with DS are also eligible for certain governmental benefits throughout their lifetime based on their diagnosis (e.g., Early Intervention, Social Security Income, Medicaid), but enrollment is not always automatic and can be time-consuming and frustrating for some families.
Participants in this pilot study offered many take-home messages, informed by their lived experiences, for constructive improvement. These can be summarized as follows:
Relationships built on trust are crucial for establishing long-lasting medical care. Caregivers need to trust the healthcare system, the PCP, and other specialists. Caregivers are also asking that they be trusted by providers and others. They often feel dismissed due to perceived “lack of knowledge.” Once a trusted clinician is found, parents often share referrals with other parents.
More physicians of color are needed to take care of patients with DS. Some, but not all families, preferred that their loved one with DS be treated, whenever possible, by a race-concordant medical provider. A lack of such providers makes this unattainable in many parts of the U.S.
Caregivers are looking for medical providers who demonstrate a willingness to learn more about DS. Caregivers mentioned that they prefer medical providers who treat their loved one as an individual, and not as a condition. A provider’s responsiveness, availability, and access were crucial for relationship-building for many families.
It takes a funded village. Caregiver mentioned that healthcare professionals are their top sources of trusted information. However, PCPs report they cannot do everything alone. Funded resources and support services are similarly desired by families and PCPs, but frequently unavailable in resource-poor medical environments. Collateral support staff (e.g., social workers) might be especially important for families with low health literacy levels. Having access to such resources would help caregivers develop a sense of self-efficacy, understanding when and how to get support, and how to further engage in the medical community and research opportunities.
Cultural humility and competency need to be part of continual education for the healthcare system. Some parents felt that the medical community’s conscious and unconscious biases based on race affected their loved one’s care. Multiple opportunities for shared dialogue and enhanced learning could be helpful.
The medical community needs to recognize that raising a child with DS can be hard. Some caregivers said that even though they are doing the best that they can do, they still feel marginalized in some healthcare settings. Some parents mention that their loved ones with DS do not just have higher medical needs, but they also have specialized social, emotional, and educational needs. Primary care teams do not always have this expertise, and DS specialists are lacking around the nation. Medical care needs can sometimes be complex spanning different specialties. Switching providers is not always easy, so longitudinal care becomes increasingly important.
Some caregivers felt that they are too often reminded by the medical community about their race. Often such references are subtle, but many caregivers want their loved one with DS to be treated for who they are as a person and not always evaluated through the lens of race or ethnicity. Parents often want their loved one to be known as who they are, and not necessarily categorized as a “person with Down syndrome” or a “Black person.”
Structural barriers and systemic racism can become heightened with a diagnosis of DS. Barriers are often compounded for Black/African-American families, where the ability to build relationships for their loved one with DS may be compromised by cultural differences, systemic issues (lack of time or inability to craft more nuanced schedules so that patients with higher needs are offered more time), mistrust, and overt racism.
Telemedicine and other healthcare technology advances may offer some solutions to these identified barriers and facilitate a democratization of health care. One possibility is “Down Syndrome Clinic to You” (DSC2U, dsc2u.org). DSC2U is a novel, web-based tool created for caregivers of individuals with DS, which collects an extensive array of symptoms and historical data to automatically generate personalized recommendations for the caregiver and the patient’s PCP. Through a national randomized controlled trial, DSC2U was effective in bringing high-cost specialty care to low-cost primary care settings.25 DSC2U is available in both English and Spanish.
DSC2U recognizes that raising a child with DS can be challenging at times, as many caregivers mentioned in this study. The goal of DSC2U is to provide the busy caregiver with curated resources and information accessible from their own home. DSC2U was also created with the input of caregiver stakeholders, including parents who identified as Black and/or primarily Spanish-speaking. The tool’s images intentionally represent the diversity of the DS community. PCPs in this study mentioned that a lack of funded support services often hampered their ability to meet the needs of their patients with DS. DSC2U addresses that gap by providing caregivers with a corresponding plan that can be shared with the PCP. This plan is rich in resources that PCPs can use to help their patients with DS, with no additional cost to the provider. Used effectively, DSC2U can help to build trust between the caregiver, patient, and the medical provider.25
The deepening of this trust will also necessitate more conversations within the DS community. In particular, DS non-profit organizations can play a vital role in addressing some of the healthcare disparities identified in this study. Some local DS non-profit organizations, like the Massachusetts Down Syndrome Congress (www.mdsc.org), have developed specific support groups for families who come from diverse backgrounds (e.g., specific groups for parents who are Black/African American, primarily Portuguese speaking, and primarily Spanish speaking). National DS organizations, such as the National Down Syndrome Congress, have held Town Hall Meetings on “race relations” (https://www.ndsccenter.org/programs-resources/race-relations/) and host a luncheon for diverse families and allies at their annual Convention. Efforts such as these are sorely needed and should be replicated by other organizations to continue this important work.
4.1. Study Limitations
This work is not without limitations. While we remain incredibly grateful for the caregivers and PCPs who participated in this study, their recommendations might not be generalizable to the larger community of families with DS who are Black, African American, of African descent, or of mixed race. Nevertheless, their voices remain powerful, and we hope that this pilot study will motivate further dialogue and research into this area. We recruited through all of the available mechanisms within the DS community, but until a population-based database is established, research will always be limited by selection bias.
Our survey instrument was primarily distributed online. While a paper version was offered to DS non-profit organizations, we did not receive any responses by the time that the data were analyzed. This could imply that DS non-profit organizations did not have the time or capacity to help recruit for research studies like ours or that eligible caregivers, once reached, were uninterested or did not have sufficient time to respond. As such, the results reported in this paper might be skewed to represent the views of families who have a higher access to technology and higher technology literacy.
Our survey also had a 7th grade reading level, which falls into “average difficulty” for questionnaires. We borrowed some questions from pre-existing validated survey instruments and were not able to adjust the wording on those questions. Otherwise, we aimed for “plain language,” but it is possible that some portions of our survey were not fully accessible to families with lower literacy levels. Our survey did not ask caregivers to specify the ages of their loved ones with DS, so we cannot make any distinguishing conclusions based on age.
Recruiting PCPs to participate in the in-depth interviews was challenging. Our team had reached out to the major medical organizations representing medical professionals who are underrepresented minorities. These organizations either (1) did not respond to our request or (2) were not able to accommodate our request to send research opportunities to their membership lists. Collaboration among researchers and such organizations will improve our ability to study the voices, opinions, and lived experiences of such clinicians.
5. CONCLUSION
People with DS who are Black, African American, of African descent, or of mixed race often have suboptimal healthcare experiences, according to their caregivers and PCPs. The intersectionality of ableism and structural racism brings heightened challenges for many of these families. With increased funding, resources, and support, we can help mitigate some of these barriers. However, a deeper dive is necessary for long-lasting trust to be earned. Caregivers are looking for medical professionals who demonstrate an earnest willingness to learn more about DS, recognizing that the journey might be hard at times, but one that is filled with immense hope and possibility.
Supplementary Material
ACKNOWLEDGEMENTS
The authors acknowledge the contribution of DS-Connect® (The Down Syndrome Registry) which is supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), NIH, for participant recruitment. We further thank Weixing Huang from the MGH Biostatistics Unit for help with some of the statistics.
Funding information
This work was supported through a Patient-Centered Outcomes Research Institute (PCORI) Research Award (PCORI-19659-MGH)
Abbreviations
- DS
Down syndrome
- DSC2U
Down Syndrome Clinic to You
- DSP
Down Syndrome Program
- MDSC
Massachusetts Down Syndrome Congress
- MGH
Massachusetts General Hospital
- PCP
Primary care provider
Footnotes
IRB Statement
The Mass General Brigham Institutional Review Board approved this study.
CONFLICTS OF INTEREST
Dr. Skotko occasionally consults on the topic of Down syndrome through Gerson Lehrman Group. He receives remuneration from Down syndrome non-profit organizations for speaking engagements and associated travel expenses. Dr. Skotko receives annual royalties from Woodbine House, Inc., for the publication of his book, Fasten Your Seatbelt: A Crash Course on Down Syndrome for Brothers and Sisters. Within the past two years, he has received research funding from F. Hoffmann-La Roche, Inc., AC Immune, and LuMind IDSC Down Syndrome Foundation to conduct clinical trials for people with Down syndrome. Dr. Skotko is occasionally asked to serve as an expert witness for legal cases where Down syndrome is discussed. Dr. Skotko serves in a non-paid capacity on the Honorary Board of Directors for the Massachusetts Down Syndrome Congress and the Professional Advisory Committee for the National Center for Prenatal and Postnatal Down Syndrome Resources. Dr. Skotko has a sister with Down syndrome.
DATA AVAILABILITY STATEMENT
The data that support the findings of this study are available from the corresponding author upon reasonable request.
6. REFERENCES
- 1.O’Neill ME, Ryan A, Kwon S, Binns HJ. Evaluation of Pediatrician Adherence to the American Academy of Pediatrics Health Supervision Guidelines for Down Syndrome. Am J Intellect Dev Disabil. 2018;123(5):387–398. doi: 10.1352/1944-7558-123.5.387 [DOI] [PubMed] [Google Scholar]
- 2.Skotko BG, Davidson EJ, Weintraub GS. Contributions of a specialty clinic for children and adolescents with Down syndrome. Am J Med Genet A. 2013;161A(3):430–437. doi: 10.1002/ajmg.a.35795 [DOI] [PubMed] [Google Scholar]
- 3.Santoro SL, Martin LJ, Pleatman SI, Hopkin RJ. Stakeholder Buy-In and Physician Education Improve Adherence to Guidelines for Down Syndrome. J Pediatr. 2016;171:262–268.e1–2. doi: 10.1016/j.jpeds.2015.12.026 [DOI] [PubMed] [Google Scholar]
- 4.Santoro SL, Bartman T, Cua CL, Lemle S, Skotko BG. Use of Electronic Health Record Integration for Down Syndrome Guidelines. Pediatrics. 2018;142(3):e20174119. doi: 10.1542/peds.2017-4119 [DOI] [PubMed] [Google Scholar]
- 5.Wang Y, Liu G, Canfield MA, et al. Racial/ethnic differences in survival of United States children with birth defects: a population-based study. J Pediatr. 2015;166(4):819–826.e1–2. doi: 10.1016/j.jpeds.2014.12.025 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Zuckerman KE, Chavez AE, Regalado Murillo C, Lindly OJ, Reeder JA. Disparities in Familiarity With Developmental Disabilities Among Low-Income Parents. Acad Pediatr. 2018;18(8):944–951. doi: 10.1016/j.acap.2018.06.011 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Derrington TM, Kotelchuck M, Plummer K, et al. Racial/ethnic differences in hospital use and cost among a statewide population of children with Down syndrome. Res Dev Disabil. 2013;34(10):3276–3287. doi: 10.1016/j.ridd.2013.06.022 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Flores G, Committee On Pediatric Research. Technical report--racial and ethnic disparities in the health and health care of children. Pediatrics. 2010;125(4):e979–e1020. doi: 10.1542/peds.2010-0188 [DOI] [PubMed] [Google Scholar]
- 9.Mayberry R, Mili F, Ofili E. Racial and Ethnic Differences in Access to Medical Care. Med Care Res Rev MCRR. 2000;57 Suppl 1:108–145. doi: 10.1177/107755800773743628 [DOI] [PubMed] [Google Scholar]
- 10.Bailey ZD, Feldman JM, Bassett MT. How Structural Racism Works — Racist Policies as a Root Cause of U.S. Racial Health Inequities. N Engl J Med. 2021;384(8):768–773. doi: 10.1056/NEJMms2025396 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Bailey ZD, Krieger N, Agénor M, Graves J, Linos N, Bassett MT. Structural racism and health inequities in the USA: evidence and interventions. Lancet Lond Engl. 2017;389(10077):1453–1463. doi: 10.1016/S0140-6736(17)30569-X [DOI] [PubMed] [Google Scholar]
- 12.2018. National Healthcare Quality and Disparities Report: Appendix A. Published online 2016:166. [Google Scholar]
- 13.Hoffman KM, Trawalter S, Axt JR, Oliver MN. Racial bias in pain assessment and treatment recommendations, and false beliefs about biological differences between blacks and whites. Proc Natl Acad Sci U S A. 2016;113(16):4296–4301. doi: 10.1073/pnas.1516047113 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Egan JFX, Smith K, Timms D, Bolnick JM, Campbell WA, Benn PA. Demographic differences in Down syndrome livebirths in the US from 1989 to 2006. Prenat Diagn. 2011;31(4):389–394. doi: 10.1002/pd.2702 [DOI] [PubMed] [Google Scholar]
- 15.de Graaf G, Buckley F, Skotko BG. Estimation of the number of people with Down syndrome in the United States. Genet Med. 2017;19(4):439–447. doi: 10.1038/gim.2016.127 [DOI] [PubMed] [Google Scholar]
- 16.Emmanuel CJ, Knafl KA, Hodges EA, Docherty SL, O’Shea TM, Santos HP. Family members’ experience of well-being as racial/ethnic minorities raising a child with a neurodevelopmental disorder: A qualitative meta-synthesis. Res Nurs Health. 2022;45(3):314–326. doi: 10.1002/nur.22217 [DOI] [PubMed] [Google Scholar]
- 17.Li H, Parish SL, Magaña S, Morales MA. Racial and Ethnic Disparities in Perceived Barriers to Health Care Among U.S. Adults With Intellectual and Developmental Disabilities. Intellect Dev Disabil. 2021;59(1):84–94. doi: 10.1352/1934-9556-59.1.84 [DOI] [PubMed] [Google Scholar]
- 18.CAHPS Clinician & Group Survey. Accessed January 24, 2022. https://www.ahrq.gov/cahps/surveys-guidance/cg/index.html
- 19.Health Information National Trends Survey | HINTS. Accessed January 24, 2022. https://hints.cancer.gov/
- 20.Harris PA, Taylor R, Minor BL, et al. The REDCap consortium: Building an international community of software platform partners. J Biomed Inform. 2019;95:103208. doi: 10.1016/j.jbi.2019.103208 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–381. doi: 10.1016/j.jbi.2008.08.010 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Aschbrenner KA, Naslund JA, Gill LE, Bartels SJ, Ben-Zeev D. A Qualitative Study of Client-Clinician Text Exchanges in a Mobile Health Intervention for Individuals With Psychotic Disorders and Substance Use. J Dual Diagn. 2016;12(1):63–71. doi: 10.1080/15504263.2016.1145312 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Watkins DC. Rapid and Rigorous Qualitative Data Analysis: The “RADaR” Technique for Applied Research. Int J Qual Methods. 2017;16(1):1609406917712131. doi: 10.1177/1609406917712131 [DOI] [Google Scholar]
- 24.Fareed N, Swoboda CM, Jonnalagadda P, Walker DM, Huerta TR. Differences Between Races in Health Information Seeking and Trust Over Time: Evidence From a Cross-Sectional, Pooled Analyses of HINTS Data. Am J Health Promot AJHP. 2021;35(1):84–92. doi: 10.1177/0890117120934609 [DOI] [PubMed] [Google Scholar]
- 25.Chung J, Donelan K, Macklin EA, et al. Correction: A randomized controlled trial of an online health tool about Down syndrome. Genet Med Off J Am Coll Med Genet. 2021;23(1):236. doi: 10.1038/s41436-020-01033-5 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.