Abstract
Duodenal perforation is a rare but severe complication during endoscopic ultrasound-guided fine needle aspiration (EUS-FNA) and typically requires surgical intervention. With the widespread clinical use of over-the-scope clips (OTSCs), we aimed to evaluate their efficacy and safety for the closure of a duodenal perforation caused by EUS-FNA. A 79-year-old woman underwent EUS-FNA for a suspected low-density nodule in the head of the pancreas. However, duodenal perforation occurred during EUS-FNA. To minimize the patient’s pain postoperatively compared with surgical intervention, we used an OTSC to close the perforation immediately and administered drug treatment for 2 weeks. The patient was discharged after complete recovery. OTSC is considered an effective and safe choice for closing a perforation at the upper corner of the duodenal bulb without surgical intervention.
Keywords: Over-the-scope clip, duodenal perforation, endoscopic ultrasonography, fine needle aspiration, surgical intervention, drug therapy, complete recovery
Introduction
Endoscopic ultrasonography (EUS) is a unique and useful examination for the diagnosis of hepatobiliary and pancreatic diseases. EUS can be used to visualize, investigate, and intervene in pathological gastrointestinal luminal, mural, or peri-luminal structures, with negligible adverse effects.1 The most common intervention with EUS is transmural fine needle aspiration (FNA), which is an extremely safe procedure. Numerous clinical studies have reported that EUS-FNA is a safe method for biopsy required for pathological examination, given the relatively low risks of complications.2 Although bleeding and perforation are potentially severe complications of EUS-FNA, the incidences and severities of these complications have not been fully evaluated because of their relative rarity.3,4
The over-the-scope clip (OTSC) system is a novel endoscopic device that can be used to manage leaks and fistulas, remove submucosal tumors, and close perforations.5 Additionally, the efficacy of this system in treating high-risk gastrointestinal bleeding has been widely reported.6 Several studies reported that the OTSC system was effective in closing perforated peptic ulcers with a diameter <15 mm.7 We used the OTSC system to successfully close a perforation near the upper corner of the duodenal bulb and the posterior wall during EUS-FNA. We also performed long-term follow-up of the patient.
Case Report
The reporting of this study conforms to the CARE guidelines.8 This study was approved by the Ethics Committee of Lishui Municipal Central Hospital (approval No. 2023-5). Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
The patient, a 79-year-old female farmer, was admitted to Lishui Municipal Central Hospital because of epigastric pain accompanied by jaundice for 2 days. Routine blood tests revealed the following: leukocytes (WBC): 11.2 × 109/L, neutrophils: 79.7%, lymphocytes: 7.1%, and red blood cells (RBCs): 3.47 × 1012/L. The high-sensitivity C-reactive protein (CRP) level was 121 mg/L. Liver function testing revealed the following: gamma glutamyl transpeptidase (GGT): 107 U/L, total bilirubin (TBIL): 145.8 μmol/L, direct bilirubin (DBIL): 116.4 μmol/L, and albumin (ALB): 23.1 g/L. Pancreatic computed tomography (CT) revealed that the patient had acute pancreatitis with peripancreatic exudation and a suspected low-density nodule in the head of the pancreas that was possibly malignant. To clarify the nature of the nodule, we performed EUS using an Olympus ME1 ultrasound machine (Olympus Medical Systems, Tokyo, Japan).
During EUS, a hypoechoic lesion was observed in the pancreatic head. The size of the lesion was approximately 16.1 ×10.1 mm, with unclear boundaries. The echogenicity of the pancreatic body and tail was uniform, the common bile duct was not dilated, and there was no abnormal echogenicity inside the duct. The patient reported feeling anxious regarding whether the suspected low-density nodule in the head of the pancreas was malignant. Pancreatic CT and clinical manifestations indicated that the severity of the acute pancreatitis was mild, and duodenal edema was not found during abdominal CT and EUS. Subsequently, we proposed EUS-FNA to further evaluate the pancreatic head nodule. During EUS-FNA, we forgot to release the fixed knob and directly retracted the scope in the descending duodenum, which caused a sudden empty feeling. We inserted a direct gastroscope and visualized a perforation of approximately 10-mm diameter near the upper corner of the duodenal bulb and the posterior wall (Figure 1). We placed an OTSC (Ovesco Endoscopy GmbH, Tubingen, Germany) to immediately close the perforation (Figures 1 and 2). We did not perform a biopsy. Postoperatively, abdominal CT revealed free gas shadows in the abdominal cavity. We administered 40 mL of contrast agent (iohexol; Shanghai Shanjin Biotechnology Co., Ltd., Shanghai, China) orally, and after 20 minutes, high-density contrast agent shadows were seen in the stomach, duodenum, and proximal jejunum; no contrast agent effusion was observed in the abdominal cavity (Figure 3). Gastrointestinal decompression and fasting; imipenem (Merck, Rahway, NJ, USA) 1.0 ivgtt q 6 h and vancomycin (Eli Lilly, Indianapolis, IN, USA) 500 mg ivgtt q12 h to prevent infection; esomeprazole (AstraZeneca, Södertälje, Sweden) to inhibit gastric acid; and somatostatin (Serono, Aubonne, Switzerland) to inhibit pancreatic secretion were administered for 1 week. The final diagnosis was chronic pancreatitis.
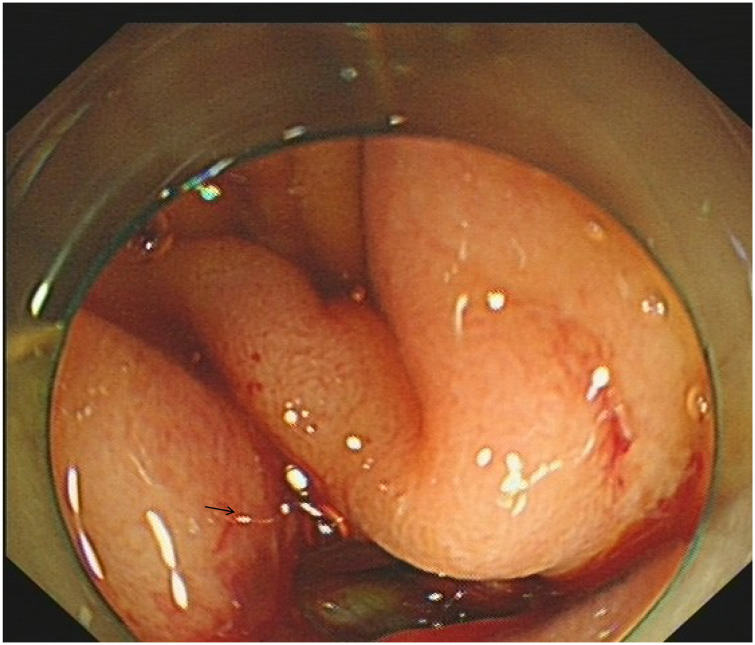
Figure 1.
Endoscopic image showing a perforation measuring approximately 10 mm in diameter near the upper corner of the duodenal bulb and the posterior wall.
Figure 2.
Endoscopic image showing successful closure of the perforation near the upper duodenal bulb using an OTSC.
OTSC, over-the-scope clip.
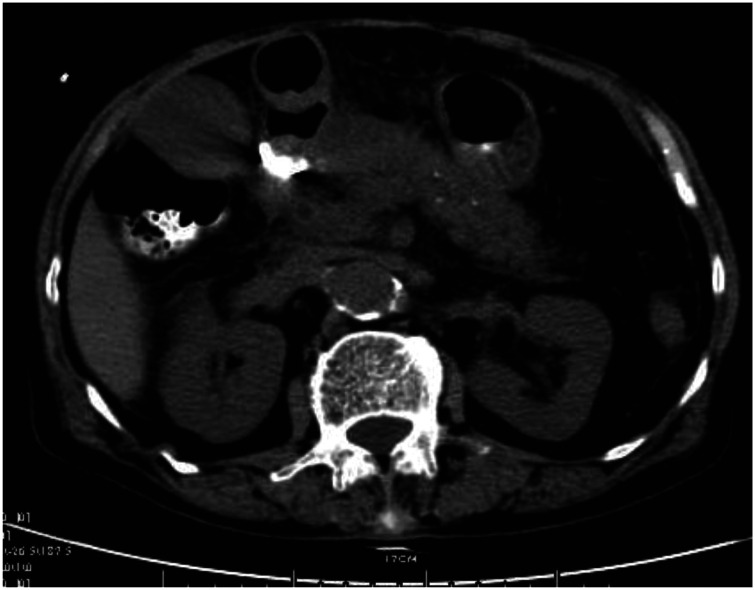
Figure 3.
Oral contrast was administered and abdominal CT was performed immediately after closing the perforation, which showed no contrast agent effusion in the abdominal cavity.
CT, computed tomography.
After completion of the drug therapy, repeat abdominal CT was performed, which showed that the free gas in the retroperitoneal cavity had been absorbed, and there was a small volume of pelvic effusion (Figure 4). We rechecked routine blood tests, CRP levels, and liver function, and the results showed improvement. However, the CRP level was 32 mg/L and the ALB level was 29.6 g/L, which required further treatment. Therefore, esomeprazole was continued, intravenous fluid therapy was administered, and the patient was given a liquid diet. She was discharged 2 weeks after endoscopic treatment and was followed-up for 1 year, remained in good health, and had no specific discomfort.
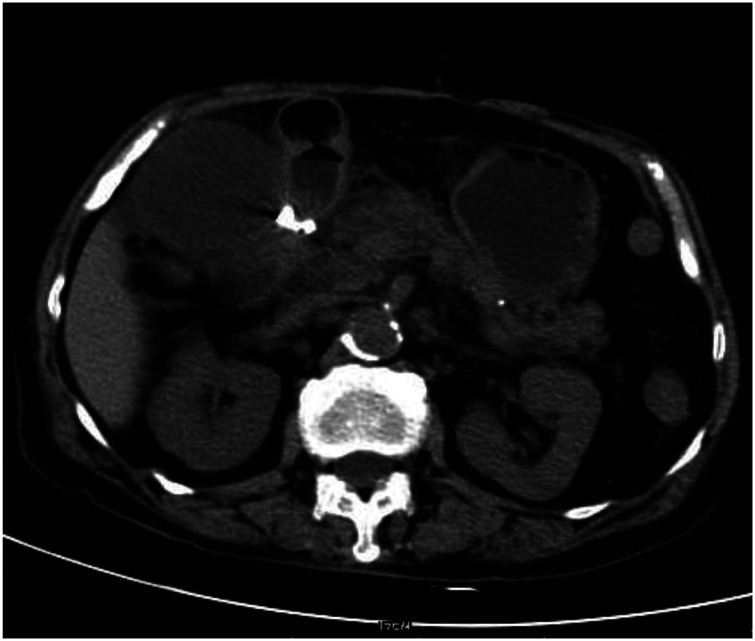
Figure 4.
Abdominal CT was repeated after drug treatment for 1 week and revealed that the free gas in the retroperitoneal cavity had been absorbed, and there was a small volume of intrapelvic effusion.
CT, computed tomography.
Discussion
EUS-FNA is highly sensitive for the diagnosis of hepatobiliary and pancreatic diseases and has unique advantages, such as the avoidance of inadvertent vascular biopsy and minimal trauma; therefore, the technique is widely used. Longitudinal EUS involves using an anterior side-view scope. As it is not possible to directly observe the direction of the digestive tract by longitudinal EUS, this technique is usually performed by physicians by feel and noting complications, such as massive bleeding, acute pancreatitis, and digestive tract perforation, with perforation being the most serious.7 However, the head end of the longitudinal EU scope is blunt, and the complication of upper gastrointestinal perforation caused by direct puncture of the wall of the digestive tract is rare. However, previous studies have reported cases of duodenal perforation with EUS.9–11 Iatrogenic gastrointestinal perforation during longitudinal EUS is mainly caused by retracting the endoscope at the descending duodenum. The upper angle of the duodenum is easily caught by the end of the internal endoscope during retraction, which causes perforation. Occasionally, after completing EUS-FNA at the descending duodenum, physicians forget to release the fixed knob and directly retract the scope, causing perforation. This was the error we made in the current case, which led to duodenal perforation.
Direct surgical intervention is performed after perforations. However, surgery is costly and traumatic as well as difficult for some patients to tolerate because most are elderly and have advanced tumors, jaundice, and poor general health. This situation results in a high mortality rate and often leads to medical litigation. Therefore, perforations should be sutured immediately through endoscopy to promote faster recovery and avoid litigation. Possible methods of closure are direct clamping with metal clips, metal clips combined with a nylon purse string suture, and OTSC. Owing to the narrow intestine at the duodenal bulb and the angle of rotation to the right, endoscopy is difficult to perform with a flexible endoscope. Additionally, it is challenging to completely clamp the tissue around a perforation with metal clips only. It is relatively easy to close perforations in the stomach and rectum with metal clips combined with a nylon purse string suture.12,13 Currently, OTSCs are the best option for closing intestinal perforations.14 The OTSC bite force is large, especially for perforations with diameters less than 15 cm, and a single OTSC can close the perforation.5 OTSCs have been used to completely close digestive tract perforations, with a reported success rate of 75% to 84.6%.5,15 In the current case, the diameter of the perforation was approximately 1.0 cm, which was an indication for the use of a single OTSC.5 The results confirmed that the selection was an excellent choice. After 2 weeks of drug treatment and careful observation, the patient gradually improved and ultimately recovered. She was subsequently discharged from the hospital and followed-up for 1 year. Her general condition was good throughout the follow-up.
Successful management of complications of EUS-FNA is essential. EUS-FNA is technically challenging and operator-dependent. Complications are mainly related to the choice of puncture site, puncture frequency, and puncture proficiency.1 In tertiary-care hospitals, doctors have high proficiency with EUS-FNA, which results in a low incidence of complications, while in primary-care hospitals, complications can occur, given that fewer patients are seen and fewer operations are performed compared with tertiary-care hospitals.16 How to promote the use of EUS-FNA while ensuring patient safety requires more cases and case series. In this study, iatrogenic duodenal perforation occurred due to surgical error. We successfully closed the duodenal perforation intraoperatively with an OTSC. OTSCs are easy to use and have several advantages in primary-care hospitals. This case report provides a reference for clinicians in primary-care hospitals when performing EUS-FNA, indicating that OTSCs can be used if perforation occurs during surgery.
OTSCs might play an important role in rescue therapy of perforations. The use of OTSCs has a high success rate. If an OTSC is placed, it does not preclude subsequent surgical intervention; therefore, OTSCs should be the first treatment choice in EUS-associated gastrointestinal perforations.
Footnotes
Author contributions: Wanlin Zhu and Jianbo Wang designed and conceptualized the article. Wanlin Zhu performed the literature search and literature review. Wanlin Zhu and Jianbo Wang wrote and approved the final version of the article.
The authors declare that there is no conflict of interest.
Funding: The authors disclose receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Lishui Science and Technology Planning Project (No. 2019SJZC60).
ORCID iD: Jianbo Wang https://orcid.org/0000-0002-0575-3023
Availability of data and materials
No datasets were generated or analyzed during the current study.
References
- 1.Lakhtakia S. Complications of diagnostic and therapeutic endoscopic ultrasound. Best Pract Res Clin Gastroenterol 2016; 30: 807–823. doi: 10.1016/j.bpg.2016.10.008. [DOI] [PubMed] [Google Scholar]
- 2.Polkowski M, Jenssen C, Kaye P, et al. Technical aspects of endoscopic ultrasound (EUS)-guided sampling in gastroenterology: European Society of Gastrointestinal Endoscopy (ESGE) Technical Guideline – March 2017. Endoscopy 2017; 49: 989–1006. doi: 10.1055/s-0043-119219. [DOI] [PubMed] [Google Scholar]
- 3.Hamada T, Yasunaga H, Nakai Y, et al. Severe bleeding and perforation are rare complications of endoscopic ultrasound-guided fine needle aspiration for pancreatic masses: an analysis of 3,090 patients from 212 hospitals. Gut Liver 2014; 8: 215–218. doi: 10.5009/gnl.2014.8.2.215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.ASGE Standards of Practice Committee; Early DS, Acosta RD, Chandrasekhara V, et al. Adverse events associated with EUS and EUS with FNA. Gastrointest Endosc 2013; 77: 839–843. doi: 10.1016/j.gie.2013.02.018. [DOI] [PubMed] [Google Scholar]
- 5.Kobara H, Mori H, Nishiyama N, et al. Over-the-scope clip system: a review of 1517 cases over 9 years. J Gastroenterol Hepatol 2019; 34: 22–30. doi: 10.1111/jgh.14402. [DOI] [PubMed] [Google Scholar]
- 6.Wei JJ, Xie XP, Lian TT, et al. Over-the-scope-clip applications for perforated peptic ulcer. Surg Endosc 2019; 33: 4122–4127. doi: 10.1007/s00464-019-06717-x. [DOI] [PubMed] [Google Scholar]
- 7.Carrara S, Arcidiacono PG, Mezzi G, et al. Pancreatic endoscopic ultrasound-guided fine needle aspiration: complication rate and clinical course in a single centre. Dig Liver Dis 2010; 42: 520–523. doi: 10.1016/j.dld.2009.10.002. [DOI] [PubMed] [Google Scholar]
- 8.Gagnier JJ, Kienle G, Altman DG, et al. ; CARE Group. The CARE guidelines: consensus-based clinical case reporting guideline development. Headache 2013; 53: 1541–1547. [DOI] [PubMed] [Google Scholar]
- 9.Grande G, Manno M, Alberghina N, et al. Quick, safe and effective repair of EUS-related duodenal perforation using over-the-scope clip system (with video). Dig Liver Dis 2016; 48: 1099–1100. doi: 10.1016/j.dld.2016.04.013. [DOI] [PubMed] [Google Scholar]
- 10.Ince AT, Kocaman O, Yıldız K, et al. Endoscopic repair of duodenal perforation with over-the-scope clipping system and endoclips: a case report. Turk J Gastroenterol 2014; 25: 103–105. doi: 10.5152/tjg.2014.4314. [DOI] [PubMed] [Google Scholar]
- 11.Li Y, Han Z, Zhang W, et al. Successful closure of lateral duodenal perforation by endoscopic band ligation after endoscopic clipping failure. Am J Gastroenterol 2014; 109: 293–295. doi: 10.1038/ajg.2013.415. [DOI] [PubMed] [Google Scholar]
- 12.Wu N, Liu S, Chen M, et al. The prepurse-string suture technique for gastric defect after endoscopic full-thickness resection (with video). Medicine (Baltimore) 2018; 97: e12118. doi: 10.1097/MD.0000000000012118. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Katsinelos P, Kountouras J, Chatzimavroudis G, et al. Endoscopic closure of a large iatrogenic rectal perforation using endoloop/clips technique. Acta Gastroenterol Belg 2009; 72: 357–359. [PubMed] [Google Scholar]
- 14.Zhong C, Tan S, Ren Y, et al. Endoscopic management of iatrogenic gastrointestinal defects with the over-the-scope clip (OTSC) system: an updated systematic review. Minim Invasive Ther Allied Technol 2021; 30: 63–71. doi: 10.1080/13645706.2019.1683582. [DOI] [PubMed] [Google Scholar]
- 15.Mizrahi I, Eltawil R, Haim N, et al. The clinical utility of over-the-scope clip for the treatment of gastrointestinal defects. J Gastrointest Surg 2016; 20: 1942–1949. doi: 10.1007/s11605-016-3282-0. [DOI] [PubMed] [Google Scholar]
- 16.Kandel P, Wallace MB. Recent advancement in EUS-guided fine needle sampling. J Gastroenterol 2019; 54: 377–387. doi: 10.1007/s00535-019-01552-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
No datasets were generated or analyzed during the current study.