Abstract
Background
In the Children’s Oncology Group ANBL1221 phase 2 trial for patients with first relapse/first declaration of refractory high-risk neuroblastoma, irinotecan and temozolomide (I/T) combined with either temsirolimus (TEMS) or immunotherapy (the anti-GD2 antibody dinutuximab (DIN) and granulocyte macrophage colony stimulating factory (GM-CSF)) was administered. The response rate among patients treated with I/T/DIN/GM-CSF in the initial cohort (n=17) was 53%; additional patients were enrolled to permit further evaluation of this chemoimmunotherapy regimen. Potential associations between immune-related biomarkers and clinical outcomes including response and survival were evaluated.
Methods
Patients were evaluated for specific immunogenotypes that influence natural killer (NK) cell activity, including killer immunoglobulin-like receptors (KIRs) and their ligands, Fc gamma receptors, and NCR3. Total white cells and leucocyte subsets were assessed via complete blood counts, and flow cytometry of peripheral blood mononuclear cells was performed to assess the potential association between immune cell subpopulations and surface marker expression and clinical outcomes. Appropriate statistical tests of association were performed. The Bonferroni correction for multiple comparisons was performed where indicated.
Results
Of the immunogenotypes assessed, the presence or absence of certain KIR and their ligands was associated with clinical outcomes in patients treated with chemoimmunotherapy rather than I/T/TEMS. While median values of CD161, CD56, and KIR differed in responders and non-responders, statistical significance was not maintained in logistic regression models. White cell and neutrophil counts were associated with differences in survival outcomes, however, increases in risk of event in patients assigned to chemoimmunotherapy were not clinically significant.
Conclusions
These findings are consistent with those of prior studies showing that KIR/KIR-ligand genotypes are associated with clinical outcomes following anti-GD2 immunotherapy in children with neuroblastoma. The current study confirms the importance of KIR/KIR-ligand genotype in the context of I/T/DIN/GM-CSF chemoimmunotherapy administered to patients with relapsed or refractory disease in a clinical trial. These results are important because this regimen is now widely used for treatment of patients at time of first relapse/first declaration of refractory disease. Efforts to assess the role of NK cells and genes that influence their function in response to immunotherapy are ongoing.
Trial registration number
Keywords: Clinical Trials as Topic, Genetic Markers, Immunotherapy, Neuroblastoma, Pediatrics
WHAT IS ALREADY KNOWN ON THIS TOPIC
Immune-related biomarkers, including immunogenotypes and/or phenotypic markers that may influence immune cell function, can impact response to immunotherapy in patients with cancer. For patients with high-risk neuroblastoma treated in the front-line setting, certain killer immunoglobulin-like receptor (KIR)/KIR-ligand genotypes have been associated with outcome following immunotherapy directed at the GD2 antigen on the surface of neuroblastoma cells.
WHAT THIS STUDY ADDS
Whether or not those same KIR/KIR-ligand genotypes would influence outcome following immunotherapy (dinutuximab with granulocyte macrophage colony-stimulating factory) in combination with chemotherapy (irinotecan and temzolomide) had not been evaluated prior to this study. The current study demonstrates that KIR and KIR-ligand genotypes also impact response to chemoimmunotherap.
HOW THIS STUDY MIGHT AFFECT RESEARCH, PRACTICE OR POLICY
These findings suggest that these genotypes could potentially serve as biomarkers to aid in selection of patients most likely to respond to this therapy.
Introduction
ANBL1221 (NCT01767194) was a Children’s Oncology Group (COG) phase 2 trial that was designed to evaluate response to temsirolimus (TEMS) or dinutuximab (DIN) with granulocyte macrophage colony-stimulating factory (GM-CSF) combined with irinotecan and temozolomide (I/T) in patients with first relapse or first declaration of refractory neuroblastoma. The objective response (OR) rate was 6% (1 of 18) in the initial cohort of patients assigned to receive I/T/TEMS, and 53% (9 of 17) for the initial cohort of patients assigned to receive I/T/DIN/GM-CSF.1 Therefore, additional patients (n=36) were assigned to I/T/DIN/GM-CSF to permit more accurate assessment of the response rate and therapy-related toxicities associated with this regimen.2 In addition, evaluation of potential biomarkers of activity was undertaken, including evaluation of the association of specific immunogenotypes with clinical outcomes.
Natural killer (NK) cells are regulated by costimulatory and inhibitory receptors that modulate the immune response. It has been shown previously that specific host genotypes are associated with outcome in patients with neuroblastoma who have been treated with immunotherapy, likely due to impact on NK cell function.3–11 Specifically, the presence or absence of inhibitory killer immunoglobulin-like receptors (KIRs) and their KIR-ligands (HLA-C1, HLA-C2, and HLA-Bw4), as well as single-nucleotide polymorphisms (SNPs) found in Fc Gamma Receptors (FCGR3A, FCGR2A, and FCGR2C), have been shown to be associated with improved outcome in the context of immunotherapy that relies on the function of immune cells that bear these receptors. Finally, the quantity and type of regulatory molecules on the surface of NK cells or in the circulation of patients receiving immunotherapy could impact the efficacy of antibody treatment.12 To better understand the relationships between NK-related profiles and outcomes following chemoimmunotherapy, detailed studies of host immune parameters were performed as part of this trial.
Methods
Study design and participants
The initial and revised ANBL1221 study designs have been described previously.1 2 A ‘Pick-the-Winner’ design was used during the randomized portion of this study, and I/T/DIN/GM-CSF met the a priori benchmark for activity.1 Patients were non-randomly assigned to I/T/DIN/GM-CSF after a protocol amendment that permitted expansion of the trial.2 Patients of any age with documentation of a high-risk neuroblastoma diagnosis were eligible at first relapse or first designation of refractory disease status if they had evaluable or measurable disease that was not limited to bone marrow. Performance status (Lansky/Karnofsky) ≥50% and adequate organ function status were required.
Procedures
Subjects received oral temozolomide (100 mg/m2/dose) and intravenous irinotecan (50 mg/m2/dose given over 90 min) on days 1–5 of 21-day cycles. DIN (17.5 mg/m2/day intravenous on days 2–5) and GM-CSF (250 µg/m2/dose subcutaneously on days 6–12) were administered as previously described.1 Disease evaluations were performed after cycles 2, 4, and 6, and every 4 cycles thereafter. Modified International Neuroblastoma Response Criteria in place at the time were used to assess response.13 OR was defined as best overall response of complete response (CR) or partial response (PR) by the end of the sixth cycle. Non-responders included patients with stable or progressive disease (SD, PD), and those who met off protocol therapy criteria due to toxicity before attaining an OR.
Blood samples for KIR genotype, KIR ligand, and FCGR genotype determination as well as NKp30 genotyping and isoform evaluation were collected at baseline. Following DNA extraction, KIR genotype was determined using a SYBR green real time PCR as previously described.5 6 KIR-ligands (including HLA-C1, HLA-C2, and HLA-Bw4 epitopes) were determined by PCR-SSP reactions using the KIR HLA Ligand SSP typing kit (Olerup, West Chester, Pennsylvania, USA) with GoTaq DNA polymerase (Promega, Madison, Wisconsin, USA). FCGR SNP status was determined using primer/probe approaches using Taqman probes for FCGR3A and FCGR2A, and RNaseH primers/probes as previously described.7 14 To determine NKp30 status, both RNA and DNA were extracted from available specimens. The region surrounding NCR3 SNP rs986475 was amplified from genomic DNA, purified and sequenced. Amplification: NCR3-U3F, 5’- CTGAACTTTCCCTTCCACCA-3′; NCR3-U3R, 5’- GGTCCAGCCAGTAAAAACCA-3′, Sequencing: NCR3-U3sF, 5’- TGTCCTGAGAAATGGGAAGG-3′, NCR3-U3sR, 5’- CAGTAAAAACCATGGTCCCC-3′). cDNA was synthesized with an oligo dt primer and SuperScript IV Reverse Transcriptase (Life Technologies). Quantitative PCR was performed as previously described15 and expression was determined using the 2-ΔΔCt algorithm, with each isoform reported as a percentage of the total of all three isoforms encoded by the NCR3 gene. Isoforms A and B are considered stimulatory, while isoform C is inhibitory and generally comprises <10% of the total isoform population. A threshold of isoform C comprising ≥25% of the total population was the criterion for designating a given profile as immunosuppressive.
Blood was collected for limited analyses of blood markers prior to the start of treatment cycles 1 and 2 during the randomized portion of the study, and prior to cycles 1–4 and after completion of cycles 4 and 6 for a more extensive set of analyses after the protocol was amended to include the expanded cohort. Total white cell count (WCC) and counts of neutrophils, lymphocytes and monocytes were obtained at the treating sites at the time of or the day prior to this blood collection. To identify NK cell markers, peripheral blood mononuclear cells (PBMC) were isolated using gradient centrifugation of fresh blood samples and were analyzed using flow cytometry. CD3 FITC (BD Cat #555916), CD56 APC (BD Cat#555518), and the following specific PE-labeled marker of choice: NKp44 (CD336, BD Cat#558563), KIR (CD158b1, BD Cat#556071), NKR-P1A (CD161, KLRB1 gene product, BD Cat#556081) and CD226 (BioLegend Cat#338305). Following incubation and washing, cells were fixed and analyzed via flow cytometry (BD FacsCaliber). After gating for lymphocytes, the populations were sorted for CD3 and CD56 status, followed by gating for the specific subpopulation within the CD3-/CD56+ population. The absolute cell number (cell/μL) was determined by multiplying the total lymphocyte number by the percentage of NK cells in the lymphocyte population as determined by fluorescence activated cell sorting. The number of NK cells expressing a particular marker was obtained by multiplying the absolute number of NK cells by percentage of marker-positive NK cells. Flow data processing was performed using FlowJo software. Soluble CD276 (B7-H3) was assessed in pretreatment patient plasma using Aviva Systems Biology CD276 ELISA Kit (Human) (OKEH01880) according to manufacturer’s directions, with the data presented as arbitrary units (au).
Statistical methods
Genotype analyses
χ2 tests were used to evaluate associations between OR and genotype. Measures of survival were the elapsed time from date of enrollment to date of event (relapse, PD, secondary malignancy, or death) for event-free survival (EFS) and time to date of death for overall survival (OS). Log-rank tests were used to assess associations between time to event or death and genotype. For comparisons between patients who received I/T/TEMS and those who received I/T/DIN, data from all evaluable I/T/DIN patients (including those in the randomized and non-randomized cohorts) were combined. Analyses were performed using SAS (SAS/STAT User’s Guide, V.9.4; SAS Institute) and R (V.3.6.1). Survival curves were created using R (https://www.r-project.org/). As the genotypes evaluated here were associated with significant differences in clinical outcomes in previous studies,5–8 a limited number of a priori hypotheses were tested and no correction for multiple comparisons was required. For genotype analyses, a p<0.05 was considered statistically significant.
Cell count and surface protein analyses
The Wilcoxon rank-sum test was used to test for differences between response groups (patients with OR vs those without OR) in continuous variables including cell counts (WCC, lymphocytes, neutrophils, monocytes, neutrophil:lymphocyte ratio) and cell surface protein levels (KIR, CD226, NKp44, CD161) and soluble CD276. Fisher’s exact test was used to test for association between response and categorical variable NKp30 isoform status (immunostimulatory (AB) vs immunosuppressive (C)). In addition, logistic regression models for OR were fit with these variables as independent predictors. Cox proportional hazards models were used to test for association between survival outcomes and continuous variables; log-rank tests were used to test for association between survival outcomes and categorical variables. Bonferroni corrections for multiple comparisons were used within groups of markers (cell counts or cell surface proteins) being analyzed. For markers related to cell counts, a p<0.01 was considered significant and for markers related to cell surface proteins, a p<0.0125 was considered significant.
Results
Patients and specimens
Blood samples from 45/53 patients assigned to I/T/DIN/GM-CSF and 14/18 patients assigned to I/T/TEMS were available for the laboratory studies presented here. Clinical details for all enrolled patients have been previously published1 2 and details for patients with samples available for analyses presented in this report are provided (online supplemental table 1).
jitc-2022-006530supp001.pdf (91.4KB, pdf)
Associations between KIR/KIR-ligand genotype and outcome
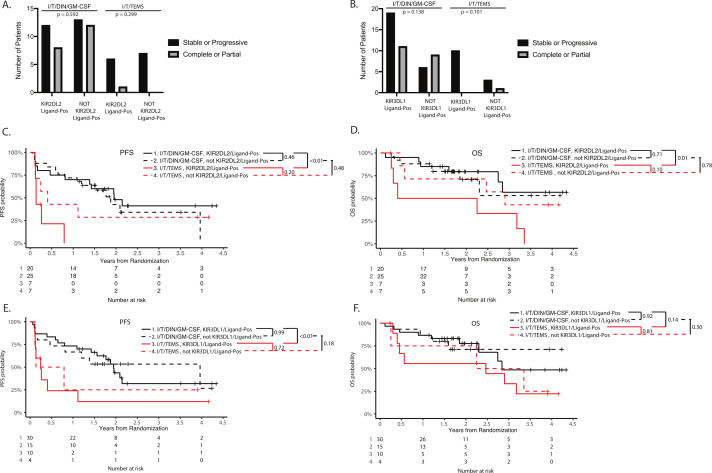
Eighteen patients were assigned to receive I/T/TEMS during the randomized portion of the study. In total, 53 eligible patients were assigned to I/T/DIN/GM-CSF; 17 during the randomized portion and 36 during the non-randomized portion. Previous data suggested that patients with KIR2DL2 with its ligand, HLA-C1, and patients with KIR3DL1 with its ligand, HLA-Bw4, had improved progression-free and OS following treatment with GD2-directed immunotherapy compared with patients who were not treated with this immunotherapy. In contrast, survival outcomes were not improved for patients who did not have these KIR/KIR-ligand genotypes.6 Therefore, KIR/KIR-ligand genotypes were determined and associations with response and survival following I/T/DIN/GM-CSF and I/T/TEMS were evaluated for all patients for whom germline DNA specimens were available (n=14 patients assigned to I/T/TEMS and 45 assigned to I/T/DIN/GM-CSF, figure 1). Neither the presence or absence of KIR2DL2, with or without its ligand (figure 1A), nor the presence or absence of KIR3DL1, with or without its ligand (figure 1B), was associated with response. However, patients with a KIR2DL2+/ligand+genotype had significantly improved EFS and OS when treated with I/T/DIN/GM-CSF compared with treatment with I/T/TEMS (p<0.01, figure 1C, D). Patients who were not positive for both KIR2DL2 and its ligand (not KIR2DL2+/ligand+) appeared to have improved survival outcomes if treated with I/T/DIN/GM-CSF rather than I/T/TEMS, however, differences were not statistically significant (figure 1C). Patients positive for both KIR3DL1 and its ligand (KIR3DL1+/ligand+) had significantly improved EFS (p<0.01), but not OS (p=0.14) if treated with I/T/DIN/GM-CSF and not with I/T/TEMS (figure 1E, F). However, this was not seen for patients who were not KIR3DL1+/ligand+; significant difference in EFS (p=0.18) or OS (p=0.30) was detected based on therapy administered in this group (figure 1E, F). It should be noted that there were only four KIR3DL1+/ligand+ patients in the I/T/TEMS group. There were no significant differences in EFS or OS for patients with or without KIR2DL2 and its ligand, or KIR3DL1 and its ligand within the group of patients treated with I/T/DIN/GM-CSF (figure 1).
Figure 1.
KIR/KIR ligand genotype and outcome. Neither KIR2DL2 with its ligand, nor KIR3DL1 with its ligand are associated with clinical outcome in patients receiving I/T/DIN/GM-CSF, however, these genotypes are associated with improved outcome when comparing I/T/DIN/GM-CSF versus I/T/TEMS. A, B) There were no significant differences in response rate based on KIR2DL2/ligand status (A) or KIR3DL1/ligand status (B). C, D) Patients positive for both KIR2DL2 and its ligand, HLA-C1 (KIR2DL2/Ligand-Pos), had significantly improved EFS (C) and OS (D) when treated with I/T/DIN/GM-CSF compared with those patients treated with I/T/TEMS (black solid line vs red solid line; EFS: p<0.01, OS: p=0.01). However, KIR2DL2/ligand-Pos status was not associated with outcome among patients treated with I/T/DIN/GM-CSF (EFS: p=0.46, OS: p=0.71). E, F) Similarly, those positive for both KIR3DL1 and its ligand, HLA-Bw4 (KIR3DL1/ligand-Pos), had significantly improved EFS (E), but there was no difference in OS (F) in patients treated with I/T/DIN/GM-CSF versus I/T/TEMS (black solid line vs red solid line; EFS: p<0.01, OS: p=0.14). Among patients treated with I/T/DIN/GM-CSF, KIR3DL1/ligand status was not associated with survival outcomes (black solid line vs black dashed line; EFS: p=0.18, OS: p=0.30). DIN, dinutuximab; EFS, event-free survival; GM-CSF, granulocyte macrophage colony stimulating factory; I/T, irinotecan and temozolomide; OS, overall survival; PFS, progression-free survival.
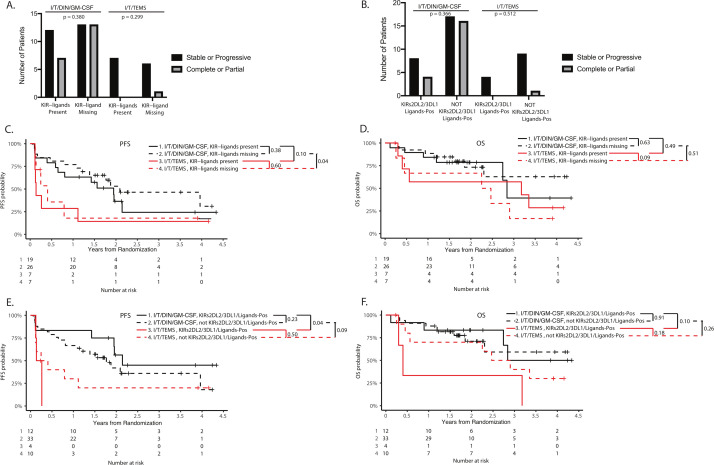
Individuals may have multiple combinations of inhibitory KIRs/KIR-ligands; specific combinations of inhibitory KIR with respective KIR-ligands, have been associated with outcome in patients treated with immunotherapy.3 4 KIR/KIR-ligands can be grouped as ‘KIR-ligands present versus KIR-ligand missing’, a comparison that considers the potential influence of having all inherited inhibitory KIR genes (of the following KIR2DL1, KIR2LD2, KIR2DL3 and KIR3DL1) and their respective ligands present (termed ‘KIR-ligands present’) versus having at least one inhibitory KIR gene (of the four noted above: namely KIR2DL1, KIR2LD2, KIR2DL3 and KIR3DL1) that does not have its respective ligand expressed (termed ‘KIR-ligand missing’). No significant differences in response were observed based on therapy for patients with KIR-ligands present versus with KIR-ligand missing (figure 2A) and no differences were observed in response based on presence or absence of KIRs2DL2/3DL1 and their ligands (figure 2B). Further analysis of KIR/KIR-ligand status and survival outcomes showed that there was a trend toward improved EFS in patients with ‘KIR-ligands present’ for those treated with I/T/DIN/GM-CSF compared with those treated with I/T/TEMS (p=0.10, figure 2C). For patients with ‘KIR-ligand missing’, EFS was significantly higher for those assigned to I/T/DIN-GM-CSF (p=0.04, figure 2C), suggesting that chemoimmunotherapy was associated with similar benefit regardless of KIR-ligand present versus missing status. Improvement in OS for ‘KIR-ligand missing’ patients assigned to I/T/DIN/GM-CSF was not detected, however (figure 2D).
Figure 2.
KIR ligand status (missing vs present) and outcome. Neither KIR ligand missing versus nor KIRs2DL2/3DL1/ligands-present genotype is associated with clinical outcome among patients receiving chemoimmunotherapy, nor are these genotypes associated with improved outcome when comparing I/T/DIN/GM-CSF versus I/T/TEMS. A, C, D) There were no differences in response rate (A) or OS (D) for these genotype groupings based on treatment type, nor were there differences in clinical outcome when comparing KIR-ligand missing genotypes versus KIR-ligand present genotypes based on treatment type. Patients with the KIR-ligand missing genotype and patients with the KIR-ligands present genotype, have improved EFS (C) when treated with I/T/DIN/GM-CSF compared with I/T/TEMS (red lines vs black lines; KIR-ligands present: p=0.10, KIR-ligand missing: p=0.04). B, E, F) No differences in response rate were observed based on KIRs2DL2/3DL1/Ligands status (B). However, patients with the KIRs2DL2/3DL1/Ligands-Pos show significantly improved EFS (E) and a trend for improved OS (F) when treated with chemoimmunotherapy as compared with I/T/TEMS (black solid line vs red solid line; EFS: p=0.04, OS: p=0.10). There was a trend toward improved EFS (E) for patients without the KIRs2DL2/3DL1/ligands-Pos genotype), but there was no difference in OS (F) for those not KIRs2DL2/3DL1/Ligands-Pos (black dashed line vs red dashed line; EFS: p=0.09, OS: p=0.26). However, there were no differences observed in EFS or OS when comparing KIRs2DL2/3DL1/ligands-Pos vs not KIRs2DL2/3DL1/ligands-Pos genotypes based on treatment type. DIN, dinutuximab; EFS, event-free survival; GM-CSF, granulocyte macrophage colony-stimulating factory; I/T, irinotecan and temozolomide; KIRs, killer immunoglobulin-like receptor; OS, overall survival; PFS, progression-free survival; TEMS, temsirolimus.
Previous work has shown that patients with specific combinations of KIR/KIR ligands (KIR2DL2+/HLA-C1+/KIR3DL1+/HLA-Bw4+; termed ‘KIRs2DL2/3DL1/ligands-Pos’) appear to have favorable outcomes when assigned to treatment with anti-GD2 immunotherapy versus treatment without immunotherapy, while those patients without the KIRs2DL2/3DL1/ligands-Pos genotype did not appear to derive a clear benefit from immunotherapy. As shown in figure 2E, F, KIRs2DL2/3DL1/ligands-Pos was associated with improved EFS (p=0.04) and a trend toward improved OS among patients treated with I/T/DIN/GM-CSF versus I/T/TEMS (p=0.10). Statistical power was limited for this analysis, as only four patients with the KIRs2DL2/3DL1/ligands-Pos genotype were treated with I/T/TEMS.
When outcomes for only those patients assigned to I/T/DIN/GM-CSF were examined, there were no significant differences in EFS or OS (figure 2C, D) for patients with KIR-ligands present or KIR-ligand missing, and there were no significant differences in EFS or OS for patients with or without KIRs2DL2/3DL1/ligands-Pos (figure 2E, F).
Associations between FCGR and outcome
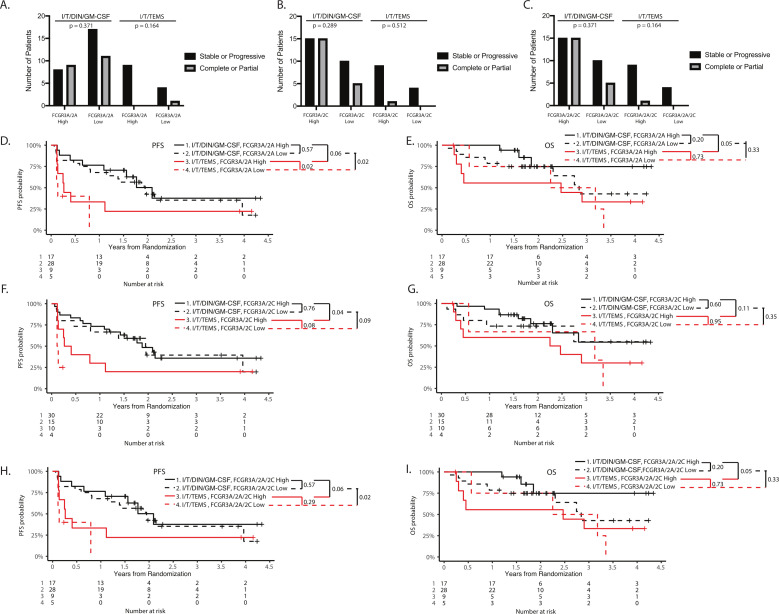
In patients with renal cell carcinoma, specific combinations of FCGR3A, FCGR2A and FCGR2C genotypes, grouped as ‘high-affinity’ FCGRs versus ‘low-affinity’ FCGRs based on SNP status, were associated with response to immunotherapy.7 FCGR genotype has also been associated with outcome in neuroblastoma patients treated with anti-GD2 therapy.16 17 No differences in response were observed based on FCGR genotypes (figure 3A–C). Significantly improved OS (p=0.05) and a trend toward improved EFS (p=0.06) for patients with a high-affinity FCGR3A/2A genotype were detected in patients treated with I/T/DIN/GM-CSF versus those treated with I/T/TEMS in the current study (figure 3D, E). However, those with the low-affinity FCGR3A/2A genotypes also had significantly improved EFS if assigned to I/T/DIN/GM-CSF versus I/T/TEMS (p=0.02, figure 3D). Conversely, there was no difference in OS among patients with the low affinity FCGR3A/2A based on I/T/DIN/GM-CSF versus I/T/TEMS treatment assignment (p=0.33, figure 3E). Evaluation of associations between a combination of FCGR3A/2C genotypes and both EFS and OS yielded a similar finding (figure 3F, G), as did evaluation of associations between a combination of FCGR3A/2A/2C genotypes and both EFS and OS outcomes (figure 3H, I). Overall, these results suggest that the improved outcomes associated with I/T/DIN/GM-CSF were independent of FCGR3A/2A/2C genotypes.
Figure 3.
FCGR3A/2A/2C genotypes and outcome. A, D, E) There were no differences in response to treatment type based of FCGR3A/2A genotype status, and no differences in response rate (A). A trend toward improved EFS (D) and OS (E) was detected for patients with the high-affinity genotype for FCGR3A and FCGR2A (‘FCGR3A/2A high’) following treatment with chemoimmunotherapy as compared with I/T/TEMS (black solid line vs red solid line; EFS: p=0.06, OS: p=0.05). However, EFS among those with the FCGR3A/2A Low genotype was also significantly improved among based on receipt of I/T/DIN/GM-CSF versus I/T/TEMS (black dashed line vs red dashed line; p=0.02). B, F, G) There were no differences in response to treatment type based on FCGR3A/2C genotype status, and there are no differences in response rate (B) Patients with a high-affinity genotype for FCGR3A and FCGR2C (‘FCGR3A/2C high’) had significantly improved EFS (F) and a trend toward improved OS (G) when treated with immunotherapy as compared with I/T/TEMS (black solid line vs red solid line; EFS: p=0.04, OS: p=0.11). However, those with the FCGR3A/2C Low genotype also showed a trend toward improved EFS when treated with I/T/DIN/GM-CSF versus I/T/TEMS (black dashed line vs red dashed line; p=0.09). C, H, I) There were no differences in response to treatment type based on FCGR3A/2A/2C genotype status, and there were no differences in response rate (C) Patients with the a high-affinity genotype for FCGR3A, FCGR2A and FCGR2C (‘FCGR3A/2A/2C high’) had a trend for improved EFS (H) and significantly improved OS (I) when treated with I/T/DIN/GM-CSF vs I/T/TEMS (black solid line vs red solid line; EFS: p=0.06, OS: p=0.05), however, improved EFS was also detected in those with the FCGR3A/2A/2C low genotype when treated with I/T/DIN/GM-CSF versus I/T/TEMS (black dashed line vs red dashed line; p=0.02). DIN, dinutuximab; EFS, event-free survival; GM-CSF, granulocyte macrophage colony-stimulating factory; I/T, irinotecan and temozolomide; OS, overall survival; PFS, progression-free survival; TEMS, temsirolimus.
Association of NKp30 isoform profile with outcome
NKp30 isoform status has previously been shown to predict outcome in patients with gastrointestinal stromal tumors treated with immunotherapy, and in subsets of patients with neuroblastoma.15 18 NKp30 isoform has been previously shown to correlate with SNP rs986475 genotype17 19 In all 47 patients for whom both genotype and transcript data were available in this cohort, NKp30 isoform status correlated with rs986475 genotype. NKp30 status was available for 59 patients enrolled on ANBL1221, including 14 assigned to I/T/TEMS and 45 assigned to I/T/DIN/GM-CSF. Among the latter, 35 (78%) were found to have the immunostimulatory NKp30 AB isoform profile and 10 (22%) were found to have the immunosuppressive C profile. No association between isoform type and OR, EFS or OS was detected, however (tables 1 and 2).
Table 1.
White blood cell types, cell surface markers, and additional candidate biomarkers and response
| N | Median | Uncorrected | OR for responder | P value | |||
| P value | |||||||
| Cell counts* | |||||||
| WCC | Responder | 15 | 4400 | 0.6127 | 1.002† | 0.87 | |
| Non-responder | 18 | 4400 | |||||
| Lymphocytes | Responder | 14 | 1845.5 | 0.1064 | 1.079† | 0.0327 | |
| Non-responder | 18 | 813 | |||||
| Monocytes | Responder | 14 | 643 | 0.0805 | 1.002 | 0.3015 | |
| Non-responder | 18 | 515 | |||||
| Neutrophils | Responder | 14 | 2650 | 0.69 | 0.986† | 0.4037 | |
| Non-responder | 18 | 2573.9 | |||||
| Neutrophil: lymphocyte ratio | Responder | 14 | 1.4 | 0.1656 | 0.862 | 0.2144 | |
| Non-responder | 18 | 2.81 | |||||
| Cell surface proteins | |||||||
| KIR | Responder | 9 | 37.2 | 0.0081‡ | 1.079 | 0.0752 | |
| Non-responder | 8 | 14.56 | |||||
| CD226 | Responder | 9 | 108.75 | 0.0184 | 1.035 | 0.0529 | |
| Non-responder | 8 | 57.28 | |||||
| Nkp44 | Responder | 9 | 10.47 | 0.665 | 0.992 | 0.6388 | |
| Non-responder | 8 | 7.8 | |||||
| CD161 | Responder | 9 | 87.15 | 0.0045‡ | 1.089 | 0.0384 | |
| Non-responder | 8 | 31.34 | |||||
| Additional markers | |||||||
| CD276§ | Responder | 20 | 122.91 | 0.3241 | 1.003 | 0.5378 | |
| Non-responder | 23 | 114.9 | |||||
| CD56 | Responder | 9 | 111 | 0.0304 | 1.023 | 0.0614 | |
| Non-responder | 8 | 49.15 | |||||
| NKp30 | AB | C | |||||
| Responder | 14 | 6 | N/A | 0.3011 | 0.444 | 0.2679 | |
| Non-responder | 21 | 4 | |||||
Bolded values indicate statistically significant differences.
*Units for cell counts—cells/µL.
†OR corresponds to a 100-unit increase in WCC/lymphocytes/neutrophils.
‡With Bonferroni correction for multiple comparisons among the four NK cell surface markers, p<0.0125 was considered significant.
§Units for CD276 - arbitrary units (AU).
N/A, not available; WCC, white cell count.
Table 2.
White blood cell types, cell surface markers, and additional candidate biomarkers and survival outcomes
| N | EFS | OS | ||||
| HR | P value | HR | P value | |||
| Cell counts | ||||||
| WCC | 33 | 1.020* | 0.0073† | 1.021* | 0.0133 | |
| Lymphocytes | 32 | 1.020* | 0.2336 | 1.000* | 0.9904 | |
| Neutrophils | 32 | 1.029* | 0.0029† | 1.022* | 0.0097† | |
| Neutrophil:lymphocyte ratio | 32 | 1.059 | 0.43 | 1.143 | 0.0231 | |
| Monocytes | 32 | 1.003 | 0.0259 | 1.002 | 0.187 | |
| Cell surface markers | ||||||
| KIR | 17 | 0.962 | 0.0898 | 0.944 | 0.3781 | |
| CD226 | 17 | 0.989 | 0.1343 | 0.989 | 0.4825 | |
| NKp44 | 17 | 1.014 | 0.2791 | 0.962 | 0.6728 | |
| CD161 | 17 | 0.989 | 0.2262 | 0.985 | 0.4928 | |
| Other Markers | ||||||
| CD276 | 43 | 1.003 | 0.2545 | 1.004 | 0.2286 | |
| N (%) | 3 years EFS% (SE) | P value | 3 years OS% (SE) | P value | ||
| NKp30 | AB | 35 (77.8) | 35.3 (12.7) | 0.4125 | 44.3 (14.8) | 0.1462 |
| C | 10 (22.2) | 48.0 (34.6) | 90.0 (16.4) | |||
Bolded values indicate statistically significant differences.
*R corresponds to a 100-unit increase in WCC/lymphocytes/neutrophils.
†With Bonferroni correction for multiple comparisons among the five cell counts, p<0.01 was considered significant.
EFS, event-free survival; WCC, white cell count.
Association of WCC types and cell surface markers with outcome
Total WCC numbers and numbers of lymphocytes, monocytes, and neutrophils, as well as the neutrophil:lymphocyte ratio were obtained from blood count data collected at the start of treatment cycles at participating sites for the combined randomized and non-randomized cohorts. Flow cytometry was performed only on PBMC samples from patients enrolled during the non-randomized portion of the study, as a protocol amendment was required to permit collection of these samples. PBMC numbers were insufficient for adequate flow cytometry analyses for a substantial portion of samples, particularly for many samples collected at baseline. Adequate samples for flow cytometric analysis were available from only 17/36 patients non-randomly assigned to I/T/DIN/GM-CSF in the expanded cohort, and these were only available from the start of cycle 3 time point. Only patients who had SD or better after the first disease evaluation were permitted to remain on protocol therapy, and therefore the analyzed samples were only from patients who did not experience early PD. Four of the 36 patients enrolled on the expanded cohort had experienced PD prior to this time point. Acknowledging this limitation, results are shown (tables 1 and 2). Differences in median NK cell (CD56+/CD3-) number and expression of CD161 and KIR between response groups were significant after correction for multiple comparisons as appropriate, while no differences were found when CD226 and CD276 were evaluated. None of these factors was a statistically significant predictor of response in the logistic regression models. Associations between neutrophil count and both EFS and OS as well as associations between WCC and EFS were significant among patients assigned to I/T/DIN/GM-CSF on this study. A 100-unit increase in neutrophil count corresponded to a 2.9% increase in risk of event (p=0.0029) while a 100-unit increase in WCC corresponded to a 2.0% increase in risk of an event (p=0.0073). No significant associations between response status or survival outcomes and additional parameters studied were detected.
Discussion
This study of patients with relapsed or refractory neuroblastoma included a randomized portion in which patients were treated with either I/T/TEMS or I/T/DIN/GM-CSF, permitting evaluation of the hypothesis that patients with certain KIR/KIR-ligand genotypes would have differential survival outcomes based on treatment type. The finding that patients with a KIR2DL2+/ligand+ genotype and those with a KIR3DL1+/ligand+ genotype had improved survival outcomes if treated with I/T/DIN/GM-CSF rather than I/T/TEMS is concordant with what has been previously reported.5–8 Other than results published by Erbe et al regarding the association of KIR/KIR-ligand status with outcome during frontline postconsolidation treatment of children with high-risk neuroblastoma on COG ANBL0032,6 no other published studies demonstrating an association between KIR/KIR-ligand genotype and survival outcome in patients with neuroblastoma have included patients treated with and without immunotherapy.3–11 The findings reported here are important because they confirm the ANBL0032 findings with respect to KIR/KIR-ligand genotype in an independent cohort of patients with relapsed/refractory neuroblastoma treated on a clinical trial. Taken together, the data from ANBL0032 and from the current study demonstrate that the relevance of KIR/KIR-ligand genotype is specific to a treatment context that includes anti-GD2 immunotherapy. As shown in figure 1, the presence of KIR2DL2 or KIR3DL1 and the relevant ligand are associated with improved outcome in the setting of GD2-directed immunotherapy, while there is no difference in outcome when immunotherapy is administered to patients without KIR2DL2 or KIR3DL1 and the relevant ligand. In contrast, in this study, the benefit of immunotherapy seemed to be independent of FCGR genotype, with no differences in outcome seen based on high-affinity versus low-affinity genotype. The findings suggest that clinical outcome is being influenced by cells that express KIR, and that their function is being influenced by the KIR/KIR-Ligand interactions. This would be consistent with the concept that the chemotherapy given with the anti-GD2 antibody therapy may be allowing augmented access of immune cells to the tumor microenvironment, inhibiting progression of disease and resulting in improved survival outcomes.
When results of these analyses are interpreted, limitations of this work must be considered. The number of patients for whom samples were available for assessment of several of the markers studied was small, and results should not be overinterpreted. Also, results for some of the markers studied reflects pooling of data from patients enrolled during the randomized portion of the study and from patients enrolled after the chemoimmunotherapy cohort alone was expanded. Referral patterns may have changed in ways that could make the patients in the latter group differ from those in the former group, and therefore, statistical analyses could potentially be biased. In addition, analysis of OS in this patient population is difficult, as patients with relapsed and refractory disease often receive additional therapy after discontinuation of chemoimmunotherapy, and subsequent therapies may impact survival. The magnitude of this effect may be especially significant among responders with primary refractory disease who went on to high-dose chemotherapy with autologous stem cell transplantation after experiencing a reduction in disease burden following chemoimmunotherapy.2
However, the identification of a context-specific effect of KIR/KIR-ligand genotype in the setting of anti-GD2 immunotherapy is of interest despite these limitations. If validated in additional studies, this finding may have implications for therapy selection in the setting of relapsed and refractory disease, since DIN-based chemoimmunotherapy is now widely used as part of treatment.
Median values for NK cells (CD56+/CD3−) and their expression of CD161 and KIR differed in response groups, but statistical significance was not maintained in logistic regression models. As the antibody used for KIR flow cytometry recognizes both inhibitory and stimulatory forms of KIR, additional studies may be needed to refine the population of KIR being expressed. CD161 is expressed on the majority of mature NK cells and has been shown to participate in triggering NK cell cytotoxicity.20 21 CD161 marks NK cells that have retained the ability to respond to innate cytokines during differentiation.20 A meta-analysis of expression signatures from ~18,000 human tumors of varying histologies showed that expression of the CD161 coding gene KLRB1 was associated with favorable survival outcomes.22 Further study of the potential predictive value of these biomarkers in patients with relapsed or refractory neuroblastoma treated with chemoimmunotherapy may be of interest.
In summary, correlative studies performed using samples from patients treated with I/T/DIN on ANBL1221 have demonstrated that KIR/KIR-ligand genotype is associated with improved outcome when evaluated in the setting of GD2-directed chemoimmunotherapy, and that among all additional markers analyzed, NK cells (CD56+/CD3−) and their expression of CD161 and KIR may possibly be associated with response. Based on this work, focused analysis of these biomarkers in future studies is anticipated. Outcomes for patients treated in a single-center front-line trial that incorporated anti-GD2 therapy into induction appear to be favorable,23 and a randomized cooperative group trial that includes chemoimmunotherapy early in treatment of children with high-risk neuroblastoma is in development. This randomized clinical trial presents an important opportunity to prospectively evaluate the roles of potential biomarkers identified in the current study in a larger cohort of patients randomized to induction chemotherapy with or without DIN.
Footnotes
Contributors: AKE and ASF genotyped the patients, interpreted the patient data regarding the clinical associations with outcome. MBD and VM phenotyped the patients, interpreted the patient data regarding the clinical associations with outcome. AKE, RB, PMS, MBD and ALY were major contributors to the writing of the manuscript. AN, FFZ, JB, KK, J-TH and WBL performed statistical analysis and inference of clinical outcome in association with genotype status and were major contributors to the writing of the manuscript. RB, ALY, PMS, RM, MTP, BLS, SS, SA and JMM, JRP designed and conducted the clinical trial, designed the correlative study components of the trial, and participated in collection and analysis of clinical data. All authors participated in the writing and editing of this manuscript. RB and PMS serve as content guarantors for this study.
Funding: NCTN Operations Center Grant (U10CA180886), the NCTN Statistics and Data Center Grant (U10CA180899), NIH R35 (CA220500 and CA197078, DOD (PR110118), St. Baldrick’s Foundation, Alex’s Lemonade Stand Foundation, Stand Up 2 Cancer, Midwest Athletes Against Childhood Cancer (MACC) Fund, Crawdaddy Foundation; University of Wisconsin Carbone Cancer Center, Children’s Neuroblastoma Cancer Foundation Bridgeman Memorial Fund, and Chang Gung Medical Foundation (OMRP G3C0048, CMRPG3M0441). Dinutuximab was supplied by United Therapeutics Corporation.
Competing interests: None declared.
Provenance and peer review: Not commissioned; externally peer reviewed.
Supplemental material: This content has been supplied by the author(s). It has not been vetted by BMJ Publishing Group Limited (BMJ) and may not have been peer-reviewed. Any opinions or recommendations discussed are solely those of the author(s) and are not endorsed by BMJ. BMJ disclaims all liability and responsibility arising from any reliance placed on the content. Where the content includes any translated material, BMJ does not warrant the accuracy and reliability of the translations (including but not limited to local regulations, clinical guidelines, terminology, drug names and drug dosages), and is not responsible for any error and/or omissions arising from translation and adaptation or otherwise.
Data availability statement
Data are available on reasonable request.
Ethics approval
This study involves human participants. Participants gave informed consent to participate in the study before taking part.
References
- 1.Mody R, Naranjo A, Van Ryn C, et al. Irinotecan-temozolomide with temsirolimus or dinutuximab in children with refractory or relapsed neuroblastoma (COG ANBL1221): an open-label, randomised, phase 2 trial. Lancet Oncol 2017;18:946–57. 10.1016/S1470-2045(17)30355-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Mody R, Yu AL, Naranjo A, et al. Irinotecan, temozolomide, and dinutuximab with GM-CSF in children with refractory or relapsed neuroblastoma: a report from the children’s Oncology Group. J Clin Oncol 2020;38:2160–9. 10.1200/JCO.20.00203 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Cheung N-KV, Sowers R, Vickers AJ, et al. FCGR2A polymorphism is correlated with clinical outcome after immunotherapy of neuroblastoma with anti-GD2 antibody and granulocyte macrophage colony-stimulating factor. J Clin Oncol 2006;24:2885–90. 10.1200/JCO.2005.04.6011 [DOI] [PubMed] [Google Scholar]
- 4.Delgado DC, Hank JA, Kolesar J, et al. Genotypes of NK cell Kir receptors, their ligands, and Fcγ receptors in the response of neuroblastoma patients to hu14.18-IL2 immunotherapy. Cancer Res 2010;70:9554–61. 10.1158/0008-5472.CAN-10-2211 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Erbe AK, Wang W, Carmichael L, et al. Follicular lymphoma patients with KIR2DL2 and KIR3DL1 and their ligands (HLA-C1 and HLA-bw4) show improved outcome when receiving rituximab. J Immunother Cancer 2019;7:70. 10.1186/s40425-019-0538-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Erbe AK, Wang W, Carmichael L, et al. Neuroblastoma patients’ Kir and KIR-ligand genotypes influence clinical outcome for dinutuximab-based immunotherapy: a report from the children’s Oncology Group. Clin Cancer Res 2018;24:189–96. 10.1158/1078-0432.CCR-17-1767 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Erbe AK, Wang W, Goldberg J, et al. FCGR polymorphisms influence response to IL2 in metastatic renal cell carcinoma. Clin Cancer Res 2017;23:2159–68. 10.1158/1078-0432.CCR-16-1874 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Erbe AK, Wang W, Reville PK, et al. HLA-bw4-I-80 isoform differentially influences clinical outcome as compared to HLA-bw4-T-80 and HLA-A-bw4 isoforms in rituximab or dinutuximab-based cancer immunotherapy. Front Immunol 2017;8:675. 10.3389/fimmu.2017.00675 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Pittari G, Liu X-R, Selvakumar A, et al. Nk cell tolerance of self-specific activating receptor KIR2DS1 in individuals with cognate HLA-C2 ligand. J Immunol 2013;190:4650–60. 10.4049/jimmunol.1202120 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Tarek N, Le Luduec J-B, Gallagher MM, et al. Unlicensed NK cells target neuroblastoma following anti-GD2 antibody treatment. J Clin Invest 2012;122:3260–70. 10.1172/JCI62749 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Venstrom JM, Zheng J, Noor N, et al. Kir and HLA genotypes are associated with disease progression and survival following autologous hematopoietic stem cell transplantation for high-risk neuroblastoma. Clin Cancer Res 2009;15:7330–4. 10.1158/1078-0432.CCR-09-1720 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Wu S-Y, Fu T, Jiang Y-Z, et al. Natural killer cells in cancer biology and therapy. Mol Cancer 2020;19:120. 10.1186/s12943-020-01238-x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Brodeur GM, Pritchard J, Berthold F, et al. Revisions of the International criteria for neuroblastoma diagnosis, staging, and response to treatment. J Clin Oncol 1993;11:1466–77. 10.1200/JCO.1993.11.8.1466 [DOI] [PubMed] [Google Scholar]
- 14.Erbe AK, Wang W, Gallenberger M, et al. Genotyping single nucleotide polymorphisms and copy number variability of the fcgrs expressed on NK cells. Methods Mol Biol 2016;1441:43–56. 10.1007/978-1-4939-3684-7_4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Delahaye NF, Rusakiewicz S, Martins I, et al. Alternatively spliced NKp30 isoforms affect the prognosis of gastrointestinal stromal tumors. Nat Med 2011;17:700–7. 10.1038/nm.2366 [DOI] [PubMed] [Google Scholar]
- 16.Siebert N, Jensen C, Troschke-Meurer S, et al. Neuroblastoma patients with high-affinity FCGR2A, -3A and stimulatory kir 2DS2 treated by long-term infusion of anti-GD2 antibody ch14.18/CHO show higher ADCC levels and improved event-free survival. Oncoimmunology 2016;5:e1235108. 10.1080/2162402X.2016.1235108 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Desai AV, Gilman AL, Ozkaynak MF, et al. Outcomes following GD2-directed postconsolidation therapy for neuroblastoma after cessation of random assignment on ANBL0032: a report from the children’s Oncology Group. J Clin Oncol 2022;40:4107–18. 10.1200/JCO.21.02478 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Semeraro M, Rusakiewicz S, Minard-Colin V, et al. Clinical impact of the nkp30/B7-H6 axis in high-risk neuroblastoma patients. Sci Transl Med 2015;7:283ra55. 10.1126/scitranslmed.aaa2327 [DOI] [PubMed] [Google Scholar]
- 19.Hingorani P, Krailo M, Buxton A, et al. Phase 2 study of anti-disialoganglioside antibody, dinutuximab, in combination with GM-CSF in patients with recurrent osteosarcoma: a report from the children’s oncology group. Eur J Cancer 2022;172:264–75. 10.1016/j.ejca.2022.05.035 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Kurioka A, Cosgrove C, Simoni Y, et al. Cd161 defines a functionally distinct subset of pro-inflammatory natural killer cells. Front Immunol 2018;9:486. 10.3389/fimmu.2018.00486 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Konjević G, Vuletić A, Mirjačić Martinović K. Natural killer cell receptors: alterations and therapeutic targeting in malignancies. Immunol Res 2016;64:25–35. 10.1007/s12026-015-8695-4 [DOI] [PubMed] [Google Scholar]
- 22.Gentles AJ, Newman AM, Liu CL, et al. The prognostic landscape of genes and infiltrating immune cells across human cancers. Nat Med 2015;21:938–45. 10.1038/nm.3909 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Furman WL, McCarville B, Shulkin BL, et al. Improved outcome in children with newly diagnosed high-risk neuroblastoma treated with chemoimmunotherapy: updated results of a phase II study using hu14.18K322A. J Clin Oncol 2022;40:335–44. 10.1200/JCO.21.01375 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
jitc-2022-006530supp001.pdf (91.4KB, pdf)
Data Availability Statement
Data are available on reasonable request.