Abstract
Context:
Schools can play an important role in supporting a healthy lifestyle by offering nutritious foods and beverages and providing opportunities for physical activity. A healthy diet and regular physical activity may reduce the risk of obesity. This manuscript reports on a Community Guide systematic review examining the effectiveness of interventions in schools combining school meal or fruit and vegetable snack programs and physical activity.
Evidence acquisition:
Studies meeting the intervention definition were identified from a literature search (search period: January 1990–November 2019). Community Guide systematic review methods were used to assess effectiveness as measured by dietary behavior, physical activity, and weight changes; analyses were conducted in 2020.
Evidence synthesis:
Interventions (n=24 studies) were considered effective for increasing physical activity [median increase 21.8 minutes/day (min/d); interquartile interval (IQI): −0.8 to 27.4 min/d], modestly increasing fruit and vegetable intake (median relative increase of 12.1%; IQI: −4.6 to 73.4%), and decreasing the prevalence of overweight and obesity [median decrease of 2.5 percentage points (pct pts); IQI: −8.1 to −1.6 pct pts] among elementary school students through sixth grade. There were not enough studies to determine effectiveness of interventions for middle and high school students.
Conclusions:
School meal or fruit and vegetable snack interventions combined with physical activity were effective in increasing physical activity, with modest effects for improving fruit and vegetable consumption and reducing the prevalence of overweight and obesity among elementary students. These results may inform researchers and school administrators about healthy eating and physical activity interventions.
CONTEXT
Consuming a healthy diet and participating in regular physical activity during childhood can build stronger bones and muscles, and reduce the risk of developing disease conditions such as obesity, type 2 diabetes, high blood pressure and heart disease, and osteoporosis.1,2 In 2018, about 35% of American children and adolescents aged 2–19 years experienced overweight or obesity.3 More specifically, the prevalence of obesity among children aged 6–11 years was 19.3% and adolescents aged 12–19 years was 20.9%, with Mexican American populations and Black or African American populations having higher prevalence.4 There are many causes of excess weight gain, such as diet, physical activity, genetics, and community factors.5 Schools can play an important role in providing an environment that supports 2 of these factors: healthy eating and physical activity. Schools are an ideal setting because most children in the U.S. attend school 6 hours a day during the school year and consume as much as half their daily calories at school.6,7 A healthy school nutrition and physical activity environment can support healthier choices by increasing availability of nutritious foods and beverages and increasing opportunities for accumulating the recommended guidelines of 60 minutes or more of moderate- to vigorous-intensity physical activity daily for children and adolescents.2,7 Healthier foods and beverages include fruits, vegetables, whole grains, low-fat or fat-free dairy products, lean meats, beans, eggs, nuts, and items that are low in saturated fats, salt, and added sugars, and that have no trans fats.1
The Guide to Community Preventive Services serves as a respected source of information about effective interventions to address public health issues, including obesity prevention and control.8 A number of Community Guide reviews of intervention approaches to prevent and control obesity in schools have been conducted. This review contributes to the existing literature by assessing school meals or fruit and vegetable (FV) snack interventions combined with physical activity interventions and will be referred to hereafter as “school meal, FV snack, and physical activity interventions.” The purpose of this review was to examine the effectiveness on dietary habits, physical activity behavior or weight status, and the applicability of findings to various U.S. populations using Community Guide methods and to provide and evidence-based recommendation.
Conceptual Approach and Analytic Framework
School meal, FV snack, and physical activity interventions aim to improve students’ health behaviors and overall health by increasing the availability of healthier foods and beverages and providing opportunities for physical activity. School meal, FV snack, and physical activity interventions include school meal policies that ensure school breakfasts or lunches meet specific nutrition requirements (e.g., School Breakfast Program,9 National School Lunch Program10) or FV programs that provide fresh FV to students during lunch or snack. Physical activity interventions include physical education classes that engage students in physical activity or school policies or practices that provide opportunities for physical activity during the school day (e.g., physical activities for students such as recess and active classroom breaks).
Interventions also may include additional strategies such as healthy food and beverage marketing strategies (e.g., posters of healthier options); educational programs that address nutrition or build knowledge and skills needed to maintain physically active lifestyles; large-scale infrastructure changes that provide or improve space, facilities, or equipment to make physical activity easy and appealing (e.g., renovating a school playground); addition of small-scale equipment to promote physical activity (e.g., jump ropes, balls, cones, team vests); staff training; or family and community engagement.
The analytic framework (Figure 1) illustrates hypothesized pathways in which school meal, FV snack, and physical activity interventions lead to improved dietary, physical activity, and weight-related outcomes. These interventions may improve the school environment by increasing the availability of healthier foods and non-sugar sweetened beverages (SSB) and opportunities for physical activity. These interventions may also lead to increased knowledge, awareness, motivation, or skills, which may improve psychosocial outcomes including self-efficacy. This may support improvement in the recommendation outcomes of dietary intake11 and physical activity,11 which may lead to improved weight-related and clinical outcomes. In addition, interventions may lead to additional benefits such as increased health-related quality of life and improved academic performance, whereas potential harms may include negative effects on body image. Potential effect modifiers include intervention intensity and duration of exposure to healthier meals, FV snacks, and physical activity, study population characteristics (such as gender, baseline weight status, and race/ethnicity), and peer influence.
Figure 1.
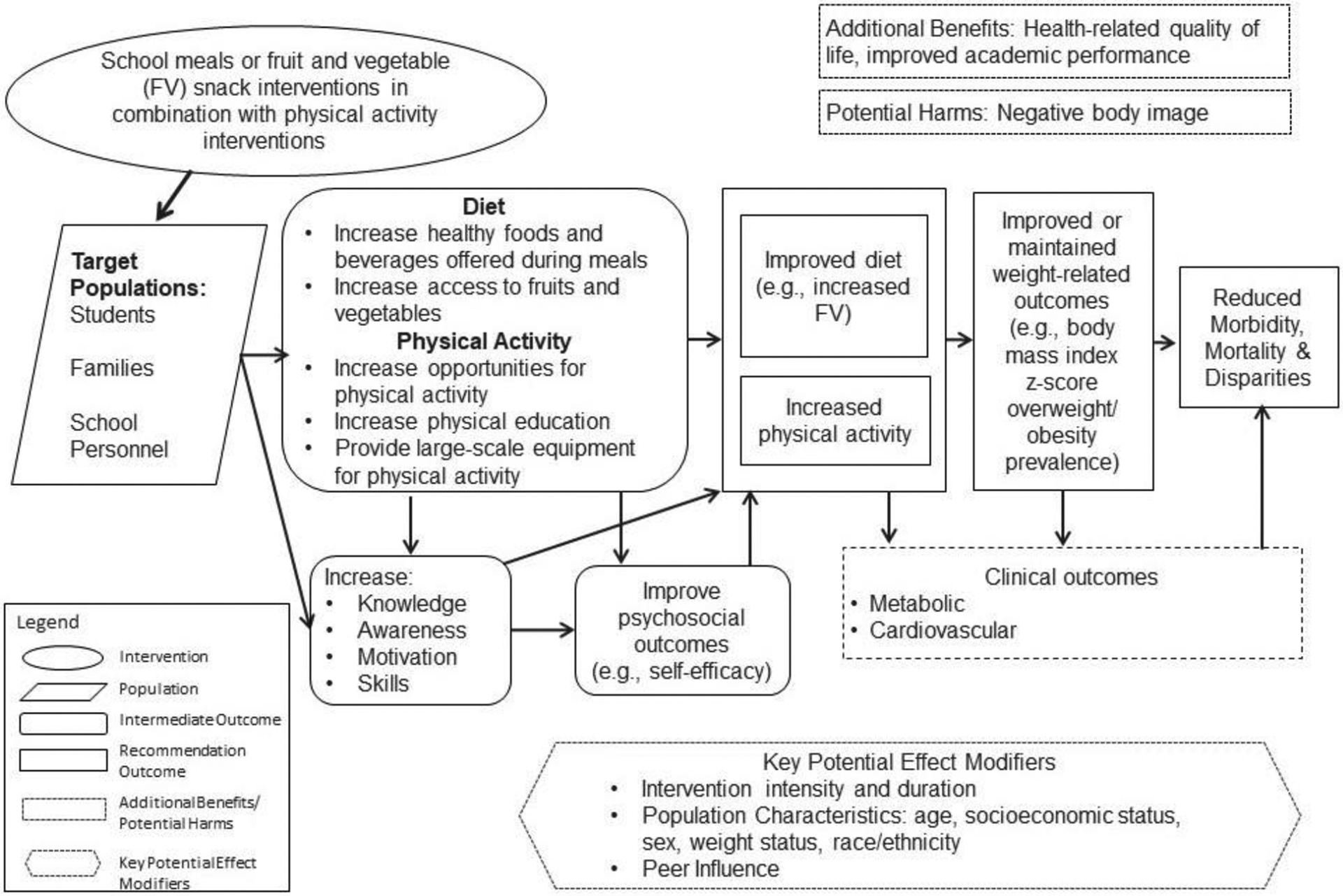
Analytic framework of school meal, fruit and vegetable snack, and physical activity interventions.
EVIDENCE ACQUISITION
Detailed systematic review methods used by The Community Guide are published elsewhere.12 For this review, the team comprised subject matter experts in obesity, nutrition, and physical activity from multiple government agencies (e.g., Centers for Disease Control and Prevention (CDC), NIH and universities along with systematic review experts from the Community Guide Office at CDC. The team worked in collaboration with the independent, nonfederal, unpaid Community Preventive Services Task Force (CPSTF).
Search for Evidence
The search for evidence was conducted in CINAHL, Cochrane, Embase (Ovid), PubMed, PsycINFO (Ovid), and PubMed, and included peer-reviewed journal articles, books, and the gray literature of theses and dissertations (search period: January 1, 1990–November 7, 2019). Reference lists in retrieved articles also were reviewed. The search strategy, found at https://www.thecommunityguide.org/findings/obesity-prevention-control-meal-fruit-vegetable-snack-interventions-combined-physical-activity-interventions-schools.html, combined terms related to school dietary and physical activity interventions, and dietary, physical activity, and weight-related outcomes.
Inclusion and Exclusion Criteria
Studies were included if schools (kindergarten through high school) were the primary setting; they evaluated intervention programs or policies aimed at school meals, or FV snack programs, or both and the intervention included physical education classes or programs or policies aimed at providing increased opportunities for physical activity; they reported a diet, physical activity, or weight-related outcome measured at least 6 months after the intervention program or policy began; they were controlled trials or a quasi-experimental design that included a comparison group, time series, before–after study, or post-only studies with a comparison group; they were conducted in a very high Human Development Index country (for comparability to U.S. populations and settings)13 and they were published in English.
Weight loss specific interventions were excluded as were studies that only recruited participants with overweight or obesity or other chronic diseases or conditions (e.g., eating disorders) so that findings are generalizable to the whole student population.
Data Abstraction and Quality Assessment
Included studies were independently abstracted by 2 review team members. The suitability of each study design was rated as greatest, moderate, or least, depending on the degree to which the design protected against threats to validity.12 Abstraction was based on a standardized abstraction form that included information on study quality, intervention components, participant demographics, and outcomes.14 Disagreements were reconciled by consensus between reviewers. Threats to validity were used to characterize studies as having good (0 to 1 limitation), fair (2 to 4), or limited (5 or more) quality of execution.12 Internal and external threats to validity included poor description of the intervention, population, or sampling frame; poor measurement of exposure or outcome; poor reporting of analytic methods; loss to follow-up; or intervention and comparison groups not being comparable at baseline. Studies with limited quality of execution were excluded from the analyses.
Outcomes of Interest
Effectiveness for outcomes of interest was assessed by the most reported measures that were relevant to the intervention. For dietary effectiveness these included total daily intake of at least 1 of the following: FV, beverages with added sugars, referred to as SSB,1 low-nutrient foods (e.g., foods with too much sodium, saturated fat, and sugar), water, and composite healthy eating measures. The team considered increases in FV intake, water consumption, and composite healthy eating measures (i.e., higher number) and decreases in SSB and low-nutrient food intake as favorable.
Physical activity effectiveness was assessed by cardiorespiratory fitness (i.e., 1 mile run/walk and timed run) or time spent in physical activity. Improved cardiorespiratory fitness and increased time spent in physical activity were considered favorable.
Effectiveness for weight-related outcomes was assessed using BMI z-score or overweight or obesity prevalence. A decrease in BMI z-score, overweight or obesity prevalence was considered favorable. Given national trends demonstrating modest increases in obesity prevalence among children,15 the team considered studies without a control group that reported a decrease or no change in weight-related outcomes as favorable, regardless of statistical significance, as this demonstrated potential for a decreased rate of change in BMI z-score, overweight, or obesity prevalence.
This body of evidence includes both objective and self-reported measures. Most physical activity and height and weight variables were objectively measured. Nearly all dietary consumption outcomes were self-reported using various, validated food and beverage intake instruments; some reported frequency of consumption while others reported quantity or volume consumed.
Calculation of Effect Estimates for Qualifying Studies
Effect estimates were calculated when the adjusted change was not provided; otherwise, the adjusted values provided in the publication were used. The formula for calculating effect estimates was carried out using 1 of 3 methods, depending on study design and variability of the outcome. The preferred method included nontreated comparison (C) and intervention (I) group—the basic unit for the calculation—with measurements made before and after the intervention. For studies with a comparison group, the team calculated the difference between the intervention group and comparison group:14
where Ipost is the posttest for the group of participants receiving the intervention (for studies with multiple measurement points, the time point closest to the conclusion of the intervention was used), Ipre is the pretest for the group receiving the intervention, Cpost is the posttest for the comparison group, and Cpre is the pretest for the comparison group.
In addition, when studies used various measures to assess the same outcome, relative percentage change was calculated as the difference in the relative change in the intervention group and comparison group:14
When studies did not include a comparison group, and the team calculated the difference between post intervention and pre intervention:14
When possible, for each primary outcome measure, the median effect estimates from individual studies was reported, along with the interquartile interval (IQI), which represents the middle 50%, or the range between the first and third quartiles.
EVIDENCE SYNTHESIS
Search Yield
Figure 2 summarizes the search process. The search identified 24,086 records. After removing duplicates, 23,412 titles and abstracts were screened. Two review team members independently screened the full-text of 250 potentially relevant articles, identifying 24 included studies in 3016–45 publications. Table 1 includes the list of interventions and their linked publications used in this review.
Figure 2.

PRISMA flowchart of school meal, fruit and vegetable snack, and physical activity interventions.
Table 1.
Interventions and Associated Publications by Study Design
| Intervention Name | Associated publications used in this review |
|---|---|
| Group RCT | |
| Aventuras Para Niños Study | Crespo 201216 |
| Child and Adolescent Trial for Cardiovascular | Luepker 199617, Nader 199946 |
| Health (CATCH), multi-state | |
| Lifestyle of 7–9 Year-Old Study | Hrafnkelsson 201418, Kristjansdottir 201019 |
| The CHILDREN Study | Angelopoulos 200920 |
| The Energy Balance 4 Kids with Play | Madsen 201521 |
| The HEalth in Adolescents (HEIA) Study | Bjelland 201522, Grydeland 201323, Grydeland 201424 |
| The Heart Smart Program | Arbeit 199225 |
| The Pathways Study | Caballero 200326 |
| Wise Mind Healthy Eating and Exercise, 2007 | Williamson 200728 Williamson 201327 |
| Prospective cohort | |
| Know Your Body Program | Resnicow 199229 |
| Other design with concurrent comparison | |
| Coordinated Approach to Child Health (CATCH) El Paso | Coleman 200530 |
| Go For Health Program | Simons Morton 199131 |
| Healthy Primary School of the Future | Bartelink 201932, Bartelink 201933 |
| Kahnawake Schools Diabetes Prevention Project | Paradis 200534 |
| Group non-randomized trial | |
| APPLE New Zealand (A Pilot Program for Lifestyle and Exercise) | Taylor 200635, Taylor 200836, Taylor 200737 |
| Healthier Options for Public School-children (HOPS) | Hollar 201038, Hollar 201039 |
| The Copenhagen School Child Intervention Study | Bugge 201240 |
| Repeat cross-sectional with comparison | |
| Living 4 Life | Utter 201141 |
| Single group before–after | |
| CATCH BasicPlus (BP) | Hoelscher 201042 |
| CATCH BasicPlus Community (BPC) | Hoelscher 201042 |
| CATCH Midwest | Vogeltanz-Holm 201843 |
| Healthy Children in Sound Communities – Germany | Naul 201244 |
| Healthy Children in Sound Communities – Netherlands | Naul 201244 |
| Wise Mind Healthy Eating and Exercise, 2010 | Newton 201045 |
Quality of Execution Assessment
Regarding study design, 17 studies had a comparison group (greatest suitability of study design),16–31,34–40 1 study was repeat cross-sectional with comparison (moderate suitability of study design),41 and 6 studies were pre-post studies (least suitability of study design).42–45 Appendix Figure 1 (available online) displays the study limitations based on the quality assessment from included studies.12 The most limitations were sampling approaches that were prone to bias (n=15), such as schools self-selecting to implement the intervention, and follow-up rates less than 80% (n=9). Based on the quality assessment, 7 studies had good quality of execution,16,20,21,38–40,42 and the remaining studies had fair quality of execution.17–19,22–31,34–37,41,44,45
Study and Intervention Characteristics
Appendix Table 1 displays study characteristics including country, degree of urbanization, setting, school level, and intervention components. Studies took place primarily in the U.S. (14 studies) and in urban areas (10 studies). Summary evidence tables for all included studies can be found at https://www.thecommunityguide.org/sites/default/files/assets/SET-Obesity-School-Meals-PA.pdf. The majority of studies (17 studies) were implemented in kindergarten through fifth grade, while 5 studies were implemented in elementary and middle combined, 1 in middle school, and 1 in middle and high school combined. Intervention duration ranged from 9 months to 42 months, with a median of 24 months.
Most studies (17 studies) included intervention components outside of the school setting. These additional components may include activities such as distributing newsletters encouraging families to make changes at home, activity packets, or family fun night; community involvement by providing access to sports or offering children’s menus at restaurants; before or after school activities such as walk -or-bike to school and afterschool activities. The most common dietary intervention component was school meal changes (17 studies) while the most common physical activity components were the combination of increasing time spent engaged in physical activity during physical education classes and providing opportunities for physical activity during the school day (e.g., physical activity during classroom breaks) (10 studies).
Demographic Characteristics of Participants in Included Studies
Study participants had a mean age of 8.8 years with roughly equal numbers of males and females. Thirteen studies reported on SES, with 9 interventions implemented among low-income (e.g., proportion qualifying for free or reduced school meals, author reported disadvantaged population) student populations and 4 being implemented in mixed or middle-income student populations.
Fourteen U.S. studies reported on racial and ethnic distributions, with 4 interventions implemented among students of a predominant race/ethnicity: American Indian/Alaska Native (100%; 1 study), Black or African American (100%; 1 study), and Hispanic or Latino (93% and >70%; 2 studies). Of the remaining 10 studies, populations were composed of students in the following groups: White (median 58%; 8 studies), Black or African American (median 14%; 9 studies), Hispanic or Latino (median 52%; 9 studies), and Asian (9%; 2 studies).
Outcomes
Details of outcomes that are included within the CPSTF recommendation statement are described below. Additional outcomes assessed are in Appendix Table 2.
Changes in dietary outcomes.
Ten studies reported FV intake (Table 2). Four studies16,18,20,37 reported a median relative increase of 12.1% (range: −4.6% to 73.4%) for FV intake for the total day. Five studies in 4 publications22,29,34,42 reported a median relative increase of 3.0% (IQI: 2.5% to 9.1%) for frequency of FV intake for the total day. One study21 reported no change in FV intake at lunch.
Table 2.
Recommended Dietary and Physical Activity Outcomes and Overweight and Obesity Prevalence
| Outcome | Result |
|---|---|
| Dietary outcomes | |
| Fruit and vegetable | |
| Number of interventions | 10 |
| Median change (IQI or range) | Relative change in amount/d: |
| Increase 12.1% (range: −4.6 to 73.4%)16,18,20,37 | |
| Relative change in frequency/d: | |
| Increase 3.0% (IQI: 2.5 to 9.1%)22,29,34,42 | |
| Lunchtime intake: no change21 | |
| Physical activity | |
| Cardiorespiratory fitness | |
| 1 Mile run/walk time* | |
| Number of interventions | 3 |
| Change (range) | Decrease 0.20 min (−1.1 to 2.2 min)21,25,34 |
| Timed run | |
| Number of interventions | 4 |
| Change | Timed run: Increase 16 yards17 |
| 9 min run: Boys Increase 15 yards; girls Increase 9 yards30 | |
| 6 min run: Range: Increase 44.4 to 74.4 yards44 | |
| Number of interventions | 2 |
| Change | Max ergometer test: Increase 0.29 watts/kg18 |
| VO2 peak (treadmill): | |
| Increase 0.46 mL/kg/min40 | |
| Counts per minute | |
| Number of interventions | 2 |
| Change | Accelerometer: |
| Range: Increase 0.18 to 20.4 counts/min26,32 | |
| Time spent in physical activity | |
| Minutes per day | |
| Number of interventions | 6 |
| Change (IQI) | Increase 21.8 min/d (−0.8 to 27.4 min/d)20,23,28,35,45,46 |
| Changes in weight-related prevalence | |
| Overweight and obesity prevalence | |
| Number of interventions | 9 |
| Median change (IQI) | Decrease 2.5 pct pts (−8.1 to −1.6 pct pts)16,26,30,36,42–44 |
| Obesity prevalence only | |
| Number of interventions | 1 |
| Change | Increase 1.1 pct pts41 |
d, day; IQI, interquartile interval, kg, kilogram; min, minute; mL, milliliter; no., number; NR, not reported; pct pts, percentage points.
Six studies reported SSB intake (Appendix Table 2). Three studies18,22,37 reported a median relative decrease of 13.3% (range: −29.2% to −4.0%) in SSB intake per day. Three studies in 2 publications21,42 reported a median relative increase of 7.1% (range: −9.0% to 15.4%) in frequency of SSB intake. Information on other dietary behaviors, including water and indices of low-nutrient food intake and healthy eating, is in Appendix Table 2 (available online).
Changes in physical activity outcomes.
Physical activity was reported using several different outcome measures. Studies were grouped into cardiorespiratory fitness outcome measures and time spent in physical activity. Results of cardiorespiratory fitness and time spent in physical activity favored the intervention. Eleven studies reported on cardiorespiratory fitness outcome measures (Table 2). Three of these studies21,25,34 reported a median decrease of 0.20 minutes (range: −1.1 to 2.2 minutes) in the 1-mile run/walk; 4 studies in 3 publications17,30,44 reported an increase in distance covered during a timed run; 2 studies18,40 reported no change in cardiorespiratory fitness measured by a treadmill maximal oxygen uptake test or a maximum ergometer test; and 2 studies reported accelerometer increases of 20.4 counts26 and 0.18 counts per minute, respectively.32 Six studies20,23,28,35,45,46 reported on time spent in physical activity. The median increase was 21.8 minutes (IQI: −0.8 to 27.4 minutes) of physical activity per day. Information on physical activity during the school day is in Appendix Table 2 (available online).
Changes in weight-related outcomes.
Nine studies in 7 publications16,26,30,36,42–44 reported change in overweight and obesity prevalence combined following the CDC or German definitions.44 Results were favorable for the intervention. The baseline median overweight and obesity prevalence combined for these studies was 38.4% with a reported decrease of 2.5 percentage points (IQI: −8.1 to −1.6 pct pts) (Table 2). One additional study41 following the WHO definition47 assessed only obesity prevalence and reported an increase of 1.1 percentage points (Table 2).
Twelve studies reported BMI z-score; 10 studies20,21,24,33,36,39–41,43,45 were able to be combined to calculate a median effect, which was a decrease of 0.07 (IQI: −0.19 to −0.02). Two studies reported BMI-z that could not be combined with the other 10: 1 study27 reported no significant effects related to the comparison group and 1 study16 reported a beta decrease of 0.019 (p=0.54) (Appendix Table 2). Information on other weight-related outcomes is in Appendix Table 2.
Additional Benefits and Potential Harms.
Studies did not report outcomes the CPSTF postulated as additional benefits or potential harms.
DISCUSSION
Based on these findings, the CPSTF recommends school meal, FV snack, and physical activity interventions for elementary students. This is based on evidence of increasing physical activity by providing opportunities for physical activity, modestly increasing fruit and vegetable consumption through school meals and/or snacks, and decreasing the prevalence of overweight and obesity among students up to and including sixth grade. The majority of studies included additional components outside the school setting to reinforce the content of the intervention Too few studies took place in middle and high school students to support a recommendation. The CPSTF recommendation for elementary students, and this systematic review on which it was based, provide evidentiary support for, and underscore the value of CDC’s Comprehensive Framework for addressing the School Nutrition Environment Framework and Services48 and the Increasing Physical Education and Physical Activity: A Framework for Schools,49 which address school-based approaches to improve dietary intake and physical education and physical activity, respectively. In turn, these frameworks provide information, tools, and resources that schools and communities can use to implement such interventions.
Findings from this review are applicable to students in the U.S. and other high human development index countries for kindergarten through sixth grade. However, gaps remain, including the need to assess effectiveness of these interventions among middle and high school students. Additionally, results were generally favorable among studies that included racial and ethnic minority groups, but the available information limited ability to more closely explore potential between-group differences. Few studies conducted sub-population analyses; future studies may consider stratifying results by racial and ethnic groups such as Black or African American, Hispanic or Latino, Asian, American Indian/Alaska Native, and Native Hawaiian/other Pacific Islander students.
Future studies may consider examining if these interventions offer co-benefits such as improvements in academic achievement, which would meet both educational and public health goals and may provide a stronger motivation for schools and communities to adopt these interventions. One included study among elementary students from families with lower income reported significantly more children maintained a healthy weight and achieved improvements in math scores, and higher, although not significant, reading scores.38 Additionally, studies may consider examining these interventions among middle and high school students.
Studies may also examine considerations for implementation which includes what amount and types of training are needed by faculty and school staff to implement these interventions, whether effects differ based on the level of implementation (e.g., district-wide, school, specific grade level, classroom), if schools implement these interventions with fidelity, and to what extent programs are sustained. Studies may also consider identifying barriers (e.g., cost, lack of resources, potential burden on school staff) to implementing interventions that provide meals or FV snacks and physical activity and information on if there were differences across schools with majority lower income families. Even though most studies in this review (85%) lasted longer than a school year, seasonal effects were unable to be examined. Assessing whether benefits are lost over the summer is an important future research area for interventions that span multiple school years. This is an important consideration because physical fitness can decline50 and weight gain during elementary school years may occur primarily during summer break.51
Finally, studies may consider examining potential harms of these interventions on development of weight or body dissatisfaction or unhealthy weight-control behaviors. No included study reported on these types of outcomes, perhaps because the included studies were primarily among elementary students. The American Academy of Pediatrics cautions that obesity prevention programs may trigger unhealthy weight-control behaviors among children 12 years and older.52 It may thus be important for future studies to modify interventions to reduce the potential for weight or body dissatisfaction or unhealthy weight-control behaviors among students of all ages.
Limitations
There were several limitations for this body of evidence. First, most articles were from peer-reviewed literature and there is a potential publication bias. However, not all studies published positive effects. The team attempted to address publication bias further by searching gray literature, but no dissertations or other non-peer reviewed reports met the inclusion criteria. Second, a formal meta-analysis was not possible, due to varied study designs, few studies reporting CIs or SEs, and reported measures being heterogeneous. The team addressed this by grouping measures for relative percent change to provide summary statistics when possible. Lastly, the maintenance of dietary and weight-related outcomes is unknown because too few studies reported long term effects.
CONCLUSIONS
Schools can be an important setting for addressing childhood obesity because of the number of hours children spend in schools, and the role played by schools in providing meals or FV snacks and opportunities for physical activity. Interventions that combine healthy school meals or FV snacks in combination with opportunities for increasing physical activity are an effective way for children to improve FV intake, increase physical activity, and maintain weight status. Findings from this review can inform researchers, school administrators, and public health decision makers about effective strategies to improve students’ dietary behavior and physical activity levels, and positively affect weight outcomes.
Supplementary Material
ACKNOWLEDGMENTS
The authors acknowledge the work of former Community Guide research fellows and interns who contributed to completion of the systematic review: Alyson Haslam and Devon L. Okasako-Schmucker, who were supported with funds from the Oak Ridge Institute for Science and Education, and student intern, Thuy Thai.
The authors acknowledge staff from the Centers for Disease Control and Prevention (CDC) library for assistance with the systematic literature search, and the Community Guide Office at CDC for scientific and dissemination assistance.
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
The content expressed in this paper is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health, U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, or Agency for Toxic Substances and Disease Registry.
Names and affiliations of the Community Preventive Services Task Force members can be found at: www.thecommunityguide.org/about/task-force-members.html.
No financial disclosures were reported by the authors of this paper.
CRediT Author Statement
AJPM-22-0808-1025R
Leigh Ramsey Buchanan: Conceptualization, Methodology, Formal Analysis, Investigation, Writing-Original Daft, Writing-Review & Editing, Supervision, Project administration Holly R. Wethington: Conceptualization, Methodology, Formal Analysis, Investigation, Writing-Original Daft, Writing-Review & Editing, Supervision, Project administration Ramona K.C. Finnie: Conceptualization, Formal Analysis, Writing-Review & Editing Shawna L. Mercer: Conceptualization, Methodology, Writing-Review & Editing, Supervision Caitlin Merlo: Conceptualization, Writing-Review & Editing Shannon Michael: Conceptualization, Writing-Review & Editing Sarah Sliwa: Conceptualization, Writing-Review & Editing Charlotte A. Pratt: Conceptualization, Writing-Review & Editing Emmeline Ochiai: Conceptualization, Writing-Review & Editing Community Preventive Services Task Force: Conceptualization, Writing-Review & Editing
REFERENCES
- 1.U.S. Department of Health and Human Services and U.S. Department of Agriculture. Dietary Guidelines for Americans 2020–2025. https://www.dietaryguidelines.gov/sites/default/files/2021-03/Dietary_Guidelines_for_Americans-2020-2025.pdf. Accessed December 17, 2021.
- 2.U.S. Department of Health and Human Services. Physical Activity Guidelines for Americans, 2nd Edition. https://health.gov/sites/default/files/2019-09/Physical_Activity_Guidelines_2nd_edition.pdf. Accessed May 24, 2021. [Google Scholar]
- 3.Fryar CD, Carroll MD, Afful J. Prevalence of overweight, obesity, and severe obesity among children and adolescents aged 2–19 years: United States, 1963–1965 through 2017–2018. NCHS Health E-Stats. 2020. [Google Scholar]
- 4.Ogden CL, Fryar CD, Martin CB, Freedman DS, Carroll MD, Gu Q, et al. Trends in obesity prevalence by race and Hispanic origin-1999–2000 to 2017–2018. JAMA. 2020;324(12):1208–1210. 10.1001/jama.2020.14590. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.U.S. Department of Health and Human Services. Childhood obesity causes & consequences. 2021. https://www.cdc.gov/obesity/childhood/causes.html. Accessed May 24, 2021.
- 6.National Center for Education Statistics. Schools and Staffing Survey. Average number of hours in the school day and average number of days in the school year for public schools, by state: 2007–08. 2010. https://nces.ed.gov/surveys/sass/tables/sass0708_035_s1s.asp. Accessed May 28, 2021.
- 7.Centers for Disease Control and Prevention. Comprehensive framework for addressing the school nutrition environment and services. 2016. https://www.cdc.gov/healthyschools/nutrition/schoolnutrition.htm. Accessed May 28, 2021.
- 8.Guide to Community Preventive Services. Obesity prevention and control. 2015. https://nces.ed.gov/surveys/sass/tables/sass0708_035_s1s.asp. Accessed May 28, 2021. [Google Scholar]
- 9.U.S. Department of Agriculture Food and Nutrition Services. School breakfast program. 2020. https://www.fns.usda.gov/sbp/school-breakfast-program. Accessed May 14, 2020.
- 10.U.S. Department of Agriculture Food and Nutrition Services. National school lunch program. 2020. https://www.fns.usda.gov/nslp. Accessed May 14, 2020.
- 11.Centers for Disease Control and Prevention. School health guidelines to promote healthy eating and physical activity. MMWR Recomm Rep. 2011;60(RR-5):1–76. [PubMed] [Google Scholar]
- 12.Briss PA, Zaza S, Pappaioanou M, et al. Developing an evidence-based guide to community preventive services - methods. Am J Prev Med. 2000;18(15):35–43. 10.1016/S0749-3797(99)00119-1. [DOI] [PubMed] [Google Scholar]
- 13.United Nations Development Programme. Human development report. 2016. http://hdr.undp.org/en/composite/HDI. Accessed May 28, 2021.
- 14.Zaza S, Wright-De Agüero LK, Briss PA, et al. Data collection instrument and procedure for systematic reviews in the Guide to Community Preventive Services. Task Force on Community Preventive Services. Am J Prev Med. 2000;18(1 Suppl):44–74. 10.1016/S0749-3797(99)00122-1. [DOI] [PubMed] [Google Scholar]
- 15.Ogden CL, Carroll MD, Lawman HG, et al. Trends in obesity prevalence among children and adolescents in the United States, 1988–1994 through 2013–2014. JAMA. 2016;315(21):2292–2299. 10.1001/jama.2016.6361. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Crespo NC, Elder JP, Ayala GX, et al. Results of a multi-level intervention to prevent and control childhood obesity among Latino children: the Aventuras Para Ninos Study. Ann Behav Med. 2012;43(1):84–100. 10.1007/s12160-011-9332-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Luepker RV, Perry CL, McKinlay SM, et al. Outcomes of a field trial to improve children’s dietary patterns and physical activity. The Child and Adolescent Trial for Cardiovascular Health. CATCH collaborative group. JAMA. 1996;275(10):768–776. 10.1001/jama.1996.03530340032026. [DOI] [PubMed] [Google Scholar]
- 18.Hrafnkelsson H, Magnusson KT, Thorsdottir I, et al. Result of school-based intervention on cardiovascular risk factors. Scand J Prim Health Care. 2014;32(4):149–155. 10.3109/02813432.2014.982363. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Kristjansdottir AG, Johannsson E, Thorsdottir I, et al. Effects of a school-based intervention on adherence of 7–9-year-olds to food-based dietary guidelines and intake of nutrients. Public Health Nutr. 2010;13(8):1151–1161. 10.1017/S1368980010000716. [DOI] [PubMed] [Google Scholar]
- 20.Angelopoulos PD, Milionis HJ, Grammatikaki E, et al. Changes in BMI and blood pressure after a school based intervention: the CHILDREN study. Eur J Public Health. 2009;19(3):319–325. 10.1093/eurpub/ckp004. [DOI] [PubMed] [Google Scholar]
- 21.Madsen K, Linchey J, Gerstein D, et al. Energy balance 4 Kids with play: Results from a two-year cluster-randomized trial. Child Obes. 2015;11(4):375–383. 10.1089/chi.2015.0002. [DOI] [PubMed] [Google Scholar]
- 22.Bjelland M, Hausken SES, Bergh IH, et al. Changes in adolescents’ and parents’ intakes of sugar-sweetened beverages, fruit and vegetables after 20 months: results from the HEIA study - a comprehensive, multi-component school-based randomized trial. Food Nutr Res. 2015;59:25932. 10.3402/fnr.v59.25932. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Grydeland M, Bergh IH, Bjelland M, et al. Intervention effects on physical activity: the HEIA study - a cluster randomized controlled trial. Int J Beh Nutr Phys Act. 2013;10:17. 10.1186/1479-5868-10-17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Grydeland M, Bjelland M, Anderssen SA, et al. Effects of a 20-month cluster randomised controlled school-based intervention trial on BMI of school-aged boys and girls: the HEIA study. Br J Sports Med. 2014;48(9):768–773. 10.1136/bjsports-2013-092284. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Arbeit ML, Johnson CC, Mott DS, et al. The heart smart cardiovascular school health promotion: behavior correlates of risk factor change. Prev Med. 1992;21(1):18–32. 10.1016/0091-7435(92)90003-Z. [DOI] [PubMed] [Google Scholar]
- 26.Caballero B, Clay T, Davis SM, et al. Pathways: a school-based, randomized controlled trial for the prevention of obesity in American Indian schoolchildren. Am J Clin Nutr. 2003;78(5):1030–1038. 10.1093/ajcn/78.5.1030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Williamson DA, Han H, Johnson WD, et al. Modification of the school cafeteria environment can impact childhood nutrition. Results from the Wise Mind and LA Health studies. Appetite. 2013;61(1):77–84. 10.1016/j.appet.2012.11.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Williamson DA, Copeland AL, Anton SD, et al. Wise Mind project: a school-based environmental approach for preventing weight gain in children. Obesity (Silver Spring). 2007;15(4):906–917. 10.1038/oby.2007.597. [DOI] [PubMed] [Google Scholar]
- 29.Resnicow K, Cohn L, Reinhardt J, et al. A three-year evaluation of the know your body program in inner-city schoolchildren. HEQ. 1992;19(4):463–480. 10.1177/109019819201900410. [DOI] [PubMed] [Google Scholar]
- 30.Coleman KJ, Tiller CL, Sanchez J, et al. Prevention of the epidemic increase in child risk of overweight in low-income schools: the El Paso coordinated approach to child health. Arch Pediatr Adolesc Med. 2005;159(3):217–224. 10.1001/archpedi.159.3.217. [DOI] [PubMed] [Google Scholar]
- 31.Simons-Morton BG, Parcel GS, Baranowski T, et al. Promoting physical activity and a healthful diet among children: results of a school-based intervention study. Am J Public Health. 1991;81(8):986–991. 10.2105/AJPH.81.8.986. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Bartelink NHM, van Assema P, Kremers SPJ, et al. One- and Two-Year Effects of the Healthy Primary School of the Future on Children’s Dietary and Physical Activity Behaviours: A Quasi-Experimental Study. Nutrients. 2019;11(3). 10.3390/nu11030689. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Bartelink NHM, van Assema P, Kremers SPJ, et al. Can the Healthy Primary School of the Future offer perspective in the ongoing obesity epidemic in young children? A Dutch quasi-experimental study. BMJ Open. 2019;9(10):e030676. 10.1136/bmjopen-2019-030676. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Paradis G, Lévesque L, Macaulay AC, et al. Impact of a diabetes prevention program on body size, physical activity, and diet among Kanien’keha’:ka (Mohawk) children 6 to 11 years old: 8-year results from the Kahnawake Schools Diabetes Prevention Project. Pediatrics. 2005;115(2):333–339. 10.1542/peds.2004-0745. [DOI] [PubMed] [Google Scholar]
- 35.Taylor RW, McAuley KA, Williams SM, et al. Reducing weight gain in children through enhancing physical activity and nutrition: the APPLE project. Int J Pediatr Obes. 2006;1(3):146–152. 10.1080/17477160600881247. [DOI] [PubMed] [Google Scholar]
- 36.Taylor RW, McAuley KA, Barbezat W, et al. Two-year follow-up of an obesity prevention initiative in children: the APPLE project. Am J Clin Nutr. 2008;88(5):1371–1377. 10.3945/ajcn.2007.25749. [DOI] [PubMed] [Google Scholar]
- 37.Taylor RW, McAuley KA, Barbezat W, et al. APPLE Project: 2-y findings of a community-based obesity prevention program in primary school age children. Am J Clin Nutr. 2007;86(3):735–742. 10.1093/ajcn/86.3.735. [DOI] [PubMed] [Google Scholar]
- 38.Hollar D, Messiah SE, Lopez-Mitnik G, et al. Effect of a two-year obesity prevention intervention on percentile changes in body mass index and academic performance in low-income elementary school children. Am J Public Health. 2010;100(4):646–653. 10.2105/AJPH.2009.165746. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Hollar D, Messiah SE, Lopez-Mitnik G, et al. Healthier options for public schoolchildren program improves weight and blood pressure in 6- to 13-year-olds. J Am Diet Assoc. 2010;110(2):261–267. 10.1016/j.jada.2009.10.029. [DOI] [PubMed] [Google Scholar]
- 40.Bugge A, El-Naaman B, Dencker M, et al. Effects of a three-year intervention: the Copenhagen School Child Intervention Study. Med Sci Sports Exerc. 2012;44(7):1310–1317. 10.1249/MSS.0b013e31824bd579. [DOI] [PubMed] [Google Scholar]
- 41.Utter J, Scragg R, Robinson E, et al. Evaluation of the Living 4 Life project: A youth-led, school-based obesity prevention study. Obes Rev. 2011;12(SUPPL. 2):51–60. 10.1111/j.1467-789X.2011.00905.x. [DOI] [PubMed] [Google Scholar]
- 42.Hoelscher DM, Springer AE, Ranjit N, et al. Reductions in child obesity among disadvantaged school children with community involvement: the Travis County CATCH Trial. Obesity (Silver Spring). 2010;18 Suppl 1:S36–44. 10.1038/oby.2009.430. [DOI] [PubMed] [Google Scholar]
- 43.Vogeltanz-Holm N, Holm J. Changes in body bass index during a 3-Year elementary school-based obesity prevention program for American Indian and White rural students. Health Educ Behav. 2018;45(2):277–285. 10.1177/1090198117714825. [DOI] [PubMed] [Google Scholar]
- 44.Naul R, Schmelt D, Dreiskaemper D, et al. ‘Healthy children in sound communities’ (HCSC/gkgk)--a Dutch-German community-based network project to counteract obesity and physical inactivity. Fam Pract. 2012;29 Suppl 1:i110–i116. 10.1093/fampra/cmr097. [DOI] [PubMed] [Google Scholar]
- 45.Newton RL Jr., Han H, Anton SD, et al. An environmental intervention to prevent excess weight gain in African-American students: a pilot study. Am J Health Promot. 2010;24(5):340–343. 10.4278/ajhp.08031224. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Nader PR, Stone EJ, Lytle LA, et al. Three-year maintenance of improved diet and physical activity: the CATCH cohort. Child and Adolescent Trial for Cardiovascular Health. Arch Pediatr Adolesc Med. 1999;153(7):695–704. 10.1001/archpedi.153.7.695. [DOI] [PubMed] [Google Scholar]
- 47.de Onis M, Onyango AW, Borghi E, et al. Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ. 2007;85:660–667. 10.2471/BLT.07.043497. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Centers for Disease Control and Prevention. Comprehensive Framework for Addressing the School Nutrition Environment and Services. Atlanta, GA: Centers for Disease Control and Prevention, US Dept of Health and Human Services; 2019. https://www.cdc.gov/healthyschools/nutrition/pdf/School_Nutrition_Framework_508tagged.pdf. Accessed November 7, 2022. [Google Scholar]
- 49.Centers for Disease Control and Prevention. Increasing Physical Education and Physical Activity: A Framework for Schools. Atlanta, GA: Centers for Disease Control and Prevention, US Dept of Health and Human Services; 2019. https://www.cdc.gov/healthyschools/physicalactivity/pdf/2019_04_25_PE-PA-Framework_508tagged.pdf#:~:text=%28CSPAP%29%20is%20a%20framework%20for%20planning%20and%20organizing,in%20addressing%20this%20aspect%20of%20the%20WSCC%20model. Accessed November 7, 2022. [Google Scholar]
- 50.Brusseau TA, Burns RD. Children’s weight gain and cardiovascular fitness loss over the summer. Int J Eviron. 2018;15(12):2770. 10.3390/ijerph15122770. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Moreno JP, Johnston CA, Woehler D. Changes in weight over the school year and summer vacation: results of a 5-year longitudinal study. J Sch Health. 2013;83(7):473–477. 10.1111/josh.12054. [DOI] [PubMed] [Google Scholar]
- 52.Golden NH, Schneider M, Wood C. Preventing obesity and eating disorders in adolescents. Pediatrics. 2016. 138(3):e20161649. 10.1542/peds.2016-1649. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.


