Abstract
The authors report a case of recurrent subarachnoid hemorrhage (SAH) after complete occlusion of an intracranial aneurysm. It is known that regrowth of an aneurysm after the complete clipping is a rare event. For detection of recurrence, however, it may be necessary to follow up with the patient regularly after the initial operation for intracranial aneurysms, because re-rupture of an aneurysm can cause a fatal result, and the cumulative risk of a recurrent SAH is thought to be not low over time.
Keywords: Subarachnoid hemorrhage, Complete occlusion, Recurrence, Intracranial aneurysm
INTRODUCTION
Subarachnoid hemorrhage (SAH) after surgical clipping is a rare incidence. The authors report a rare case of repeated bleeding after complete clipping of a ruptured intracranial aneurysm among 809 patients who were clipped surgically by the same neurosurgeon, along with a review of the literature.
CASE REPORT
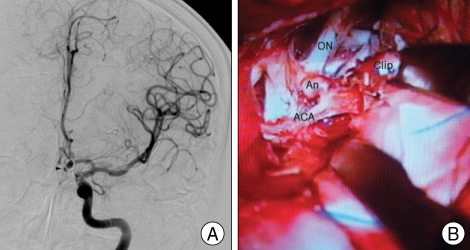
A 30-year-old man was admitted to our hospital presented with an SAH for the first time. Neurological examination showed no abnormal findings. The initial angiogram showed an aneurysm of the left anterior communicating artery (ACoA) (Fig. 1A). The patient underwent neck clipping of the aneurysm with a ring clip through the left pterional approach. The aneurysm observed during the first operation was 3 mm in diameter and directed anterosuperiorly, and it was clipped successfully (Fig. 1B). The postoperative angiogram revealed total aneurysm occlusion without residual neck (Fig. 2). The patient was discharged with no neurological deficits. The patient was alert when he again suffered an SAH six-and-one-half years after the operation. A brain computed tomography (CT) scan revealed an SAH of Fisher grade II. Angiographic studies demonstrated a 6 mm-sized left ACoA aneurysm directed inferiorly (Fig. 3A). During the second operation, the recurrent aneurysm was found near the clip of the previous operation, but the new aneurysm was separated from the old one by some distance and directed anteriorly (Fig. 3B). The ACoA aneurysm was successfully occluded by clipping with a new straight Sugita clip. An angiogram after the second operation showed complete occlusion of the newly developed aneurysm (Fig. 4). The patient was discharged with no neurological deficits.
Fig. 1.
Preoperative (A) angiograms of the initial anterior communicating artery aneurysm and intraoperative inspection (B) of the first operation through the left pterional approach showing preclipped initial anterior communicating artery aneurysm directed superiorly (Rt A1 = A1 segment of right anterior cerebral artery; Lt A1 = A1 segment of left anterior cerebral artery). An : aneurysm, ON : optic nerve.
Fig. 2.

Postoperative angiograms of the initial anterior communicating artery aneurysm. Postoperative angiogram after the first clipping shows no residual neck.
Fig. 3.
Preoperative (A) angiogram of recurrent anterior communicating artery aneurysm at 6.5 years after the first surgery (arrow head = recurrent aneurysm) and intraoperative view (B) of the second operation through the left pterional approach showing the recurrent aneurysm located near the clip of the previous operation, with some distance, and directed anteriorly. ACA : anterior cerebral artery, An : aneurysm, Clip : previous clip in the first clipping, ON : optic nerve.
Fig. 4.

Postoperative angiogram of recurrent anterior communicating artery aneurysm at 6.5 years after the first surgery. Postoperative angiogram after the second clipping shows complete occlusion of the newly developed aneurysm.
DISCUSSION
Some studies have pointed out that re-growth of an aneurysm can develop despite complete obliteration after the first SAH3,13,14). However, it is generally considered an unusual event with a reported incidence of 0.14% to 2%2,4,5,10,12). Recurrent hemorrhage may be divided into early rebleeding due to inadequate clipping and late rebleeding originating from an unruptured aneurysm, de novo aneurysm, and re-growth of the initially treated aneurysm1,15). The authors operated on only one case of repeated bleeding after complete clipping of a ruptured intracranial aneurysm among 809 patients who were clipped surgically by the same neurosurgeon between 1990 and 2005.
Some authors have reported that risk for a recurrent SAH is higher than risk for SAH in the general population6,9,13,14). In one report, cumulative risk for recurrence of SAH was 2.2% at 10 years and 9.0% at 20 years after a first operation, and the recurrence rate for SAH was over 10 times higher than the incidence rate in the general population13).
Some probable causes for the development of recurrent aneurysms have been proposed. Recurrent episodes of SAH may be caused by a de novo aneurysm that results from underlying vascular conditions that have remained despite successful treatment of the ruptured aneurysm14). A remaining arterial medial wall defect is one of these underlying vascular conditions, and the main pathogenesis of aneurysm formation. Re-growth of an aneurysm caused by clip slippage may be another cause of a recurrent aneurysm14). Clip slippage may result from various conditions, such as a wide and partially calcified aneurysmal neck, grasping of the aneurysmal neck with the distal third of the clip blades, or magnetic resonance image investigation2). Aneurysms missed during the first treatment, owing to the limited sensitivity of angiography, may also be another cause of recurrent SAH14). A young age and a small residual neck left after clipping under the operating microscope may be risk factors for aneurysm recurrence7,9,10). Sakaki et al.11) reported that hypertension and hemodynamic stress are likely factors in development of de novo aneurysms causing recurrent hemorrhage.
In our case, clip slippage was not found in postoperative angiograms. Angiogram after the first operation did not show a residual neck. The new aneurysm was considered a de novo aneurysm that developed in the vicinity of the completely clipped previous aneurysm, because it was found located at a distance from the previous aneurysm noted at the second operation, and because directions were different for the first and recurrent aneurysms. Hemodynamic stress combined with an underlying vascular condition, such as an arterial medial wall defect, could be a pathogenetic factor in formation of this recurrent aneurysm11). In one study, most of the recurrent episodes of an SAH were caused by de novo aneurysms. The predominance of de novo aneurysms as a cause for recurrent episodes of SAH indicates that the underlying vascular condition for development of an aneurysm remains despite successful treatment of the ruptured aneurysm. Patients who have experienced an SAH remain prone to new aneurysm formation despite complete treatment of all detected aneurysms after the first SAH14).
Because risk for a recurrent SAH increases as time goes by, screening for new aneurysms in patients who have been treated after an initial SAH may be worthwhile. Various proposals have been made about the appropriate timing for performing a postoperative reassessment to detect recurrent aneurysms after the first operation. Wermer et al.14) have proposed that screening for new aneurysms can be performed from 2.5 to 5 years after clipping of all detected aneurysms10,14). Another study has suggested that angiography might be necessary after 9 to 10 years for patients with completely clipped aneurysms12). On the other hand, some authors have proposed that screening should not be implemented before its frequency, benefits, and risks have been assessed in a clinical study14), and that late angiographic follow-up is probably not required as a routine for completely clipped aneurysms3).
To date, no screening program has been properly assessed for advantages and disadvantages. However, digital subtraction angiography may be an acceptable method for detection of de novo aneurysms or re-growth of original aneurysms, in spite of its risk4,12). Recent advances in MRA and 3-D CT angiography techniques for cerebral arteries will increase opportunities for screening of de novo aneurysms or recurrent aneurysms in the future8,13).
CONCLUSION
The authors present a case of repeated bleeding due to a de novo aneurysm after complete clipping of a ruptured intracranial aneurysm among 809 patients who were clipped surgically by the same neurosurgeon between 1990 and 2005.
References
- 1.Amagasaki K, Higa T, Takeuchi N, Nakizawa T, Shimizu T. Late recurrence of subarachnoid hemorrhage due to regrowth of aneurysm after neck clipping surgery. Neurol Med Chir (Tokyo) 2002;42:496–500. doi: 10.2176/nmc.42.496. [DOI] [PubMed] [Google Scholar]
- 2.Asgari S, Wanke I, Schoch B, Stolke D. Recurrent hemorrhage after initially complete occlusion of intracranial aneurysms. Neurosurg Rev. 2003;26:269–274. doi: 10.1007/s10143-003-0285-6. [DOI] [PubMed] [Google Scholar]
- 3.David CA, Vishteh AG, Spetzler RF, Lemole M, Lawton MT, Partovi S. Late angiographic follow-up review of surgically treated aneurysms. J Neurosurg. 1999;91:396–401. doi: 10.3171/jns.1999.91.3.0396. [DOI] [PubMed] [Google Scholar]
- 4.Feuerberg I, Lindquist C, Lindqvist M, Steiner L. Natural history of postoperative aneurysm rests. J Neurosurg. 1987;66:30–34. doi: 10.3171/jns.1987.66.1.0030. [DOI] [PubMed] [Google Scholar]
- 5.Lin T, Fox AJ, Drake CG. Regrowth of aneurysm sacs from residual neck following aneurysm clipping. J Neurosurg. 1989;70:556–560. doi: 10.3171/jns.1989.70.4.0556. [DOI] [PubMed] [Google Scholar]
- 6.Miller CA, Hill SA, Hunt WE. "De novo" aneurysms. A clinical review. Surg Neurol. 1985;24:173–180. doi: 10.1016/0090-3019(85)90181-8. [DOI] [PubMed] [Google Scholar]
- 7.Nakase H, Kamada Y, Aoki H, Goda K, Morimoto T, Sasaki T. Clinical study on recurrent intracranial aneurysm. Cerebrovasc Dis. 2000;10:255–260. doi: 10.1159/000016067. [DOI] [PubMed] [Google Scholar]
- 8.Park JS, Yim MB, Kim IM, Lee CY, Son EI, Kim DW. Treatment for recurrent cerebral aneurysm. J Korean Neurosurg Soc. 2003;33:472–476. [Google Scholar]
- 9.Rinne JK, Hernesniemi JA. De novo aneurysms : special multiple intracranial aneurysms. Neurosurgery. 1993;33:981–985. doi: 10.1227/00006123-199312000-00004. [DOI] [PubMed] [Google Scholar]
- 10.Sakaki T, Takeshima T, Tominaga M, Hashimoto H, Kawaguchi S. Recurrence of ICA-PCoA aneurysms after neck clipping. J Neurosurg. 1994;80:58–63. doi: 10.3171/jns.1994.80.1.0058. [DOI] [PubMed] [Google Scholar]
- 11.Sakaki T, Tominaga M, Miyamoto K, Tsunoda S, Hiasa Y. Clinical studies of de novo aneurysms. Neurosurgery. 1993;32:512–516. doi: 10.1227/00006123-199304000-00004. discussion 516-517. [DOI] [PubMed] [Google Scholar]
- 12.Tsutsumi K, Ueki K, Morita A, Usui M, Kirino T. Risk of aneurysm recurrence in patients with clipped cerebral aneurysms : results of long-term follow-up angiography. Stroke. 2001;32:1191–1194. doi: 10.1161/01.str.32.5.1191. [DOI] [PubMed] [Google Scholar]
- 13.Tsutsumi K, Ueki K, Usui M, Kwak S, Kirino T. Risk of recurrent subarachnoid hemorrhage after complete obliteration of cerebral aneurysms. Stroke. 1998;29:2511–2513. doi: 10.1161/01.str.29.12.2511. [DOI] [PubMed] [Google Scholar]
- 14.Wermer MJ, Rinkel GJ, Greebe P, Albrecht KW, Dirven CM, Tulleken CA. Late recurrence of subarachnoid hemorrhage after treatment for ruptured aneurysms : patient characteristics and outcomes. Neurosurgery. 2005;56:197–204. doi: 10.1227/01.neu.0000148894.32031.39. discussion 197-204. [DOI] [PubMed] [Google Scholar]
- 15.Yamakawa H, Sakai N, Takanaka K, Yoshimura S, Andoh T, Yamada H, et al. Clinical analysis of recurrent subarachnoid hemorrhage after neck clipping surgery. Neurol Med Chir(Tokyo) 1997;37:380–385. doi: 10.2176/nmc.37.380. discussion 385-386. [DOI] [PubMed] [Google Scholar]