Abstract
No longitudinal study has examined risk factors for future suicide attempts in major depressive disorder in a nationally representative sample. The objective of this study was to investigate baseline sociodemographic characteristics, comorbid mental disorders, specific depressive symptoms, and previous suicidal behavior as potential risk factors for suicide attempts at 3 years follow-up. Data came from the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC), a large nationally representative longitudinal survey of mental illness in adults [Wave 1 (2001–2002); Wave 2 (2004–2005) n=34,653]. Logistic regression examined associations between risk factors present at Wave 1 and suicide attempts at Wave 2 (n=169) among individuals with major depressive disorder at baseline assessment (n=6004). Risk factors for incident suicide attempts at Wave 2 (n=63) were identified among those with major depressive disorder at Wave 1 and no lifetime history of suicide attempts (n=5170). Results revealed specific comorbid anxiety, personality, and substance use disorders to be associated with incident suicide attempts at Wave 2. Comorbid borderline personality disorder was strongly associated with suicide attempts in all models. Several comorbid disorders were strongly associated with suicide attempts at Wave 2 even after adjusting for previous suicidal behavior, notably posttraumatic stress disorder [Adjusted Odds Ratio (AOR) = 2.20; 95% confidence interval (95% CI) 1.27–3.83] and dependent personality disorder (AOR = 4.43; 95% CI 1.93–10.18). These findings suggest that mental illness comorbidity confers an increased risk of future suicide attempts in major depressive disorder that is not solely accounted for by past suicidal behavior.
Keywords: major depressive disorder, suicide attempt, epidemiology, anxiety disorder, personality disorder
INTRODUCTION
Major depressive disorder (MDD) carries a significant risk of suicidal behavior (Kessler et al., 1999). Epidemiologic studies suggest that 15% of individuals with MDD have attempted suicide at some point in their life (Chen et al., 1996) and rates of 40% have been observed in clinical populations (Malone et al., 1996). Studies of suicide completers reveal that depression is present in approximately 60% of suicide deaths (Lesage et al., 1994; Cavanagh et al., 2003), and that depression is associated with a 20-fold increased risk of suicide (Osby et al., 2001). Studying suicide attempts is an important method to identify those at risk of future completion, since they are more common in the general population and strong risk factors for suicide (Suokas et al., 2001; Suominen et al., 2004). Suicide attempts frequently bring at-risk individuals to the attention of care providers, thus emphasizing their role as intervention points in suicide prevention strategies (Mann et al., 2005).
To date, much information has been gleaned from studies examining correlates of suicide attempts in MDD. Depression severity (Roy, 1993), comorbid personality (Corbitt et al., 1996; Soloff et al., 2000), anxiety (Bolton et al., 2008; Stein et al., 2001), and alcohol use disorders (Bulik et al., 1990; Claassen et al., 2007) have all been associated with an elevated risk of suicide attempt. Longitudinal studies have consistently demonstrated the importance of past suicide attempts (Oquendo et al., 2005; Oquendo et al., 2007; Sokero et al., 2005), cigarette smoking (Oquendo et al., 2005; Oquendo et al., 2007), alcohol use disorders (Maser et al., 2002), and comorbid personality disorder (Hansen et al., 2003; Oquendo et al., 2007) as predictors of future suicide attempts in depressed populations.
While these studies have considerably furthered our understanding of risk factors for suicide attempts in depression, there remain areas requiring further clarification. The vast majority of our knowledge is drawn from clinical samples of depressed individuals. To our knowledge, there have been no longitudinal studies examining predictors of suicidal behavior among individuals with MDD in a nationally representative epidemiologic sample. The existing literature on suicide attempts in depression reveals varying assessments of potential risk factors between studies. A recent review of prospective studies stressed the need to study a more comprehensive range of factors such as anxiety disorders (Oquendo et al., 2006). Many studies have established borderline personality disorder as a risk factor for suicidal behavior (Friedman et al., 1983; Soloff et al., 2000), whereas cluster A and C personality disorders have received less attention. Another important limitation in the existing literature relates to previous suicide attempts. Most studies examining suicide risk factors in MDD have included subjects with histories of suicidal ideation or attempts. While it is important to understand the contribution of previous suicide attempts to the risk of future attempts, it is also of interest to examine risk factors for incident suicide attempts in individuals with no history of suicidal behavior.
In this study we sought to examine an extensive range of correlates as possible risk factors for future suicide attempts among individuals with MDD in the general population. Using the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC; Grant et al., 2004a; Grant et al., 2008), we examined correlates including sociodemographic factors, comorbid Axis I and II mental illnesses, specific depressive symptoms, and past suicidal behavior. Predictors of incident suicide attempts were analyzed among depressed people with no previous history of suicidal behavior. Previous suicide attempts and suicidal ideation were also compared with comorbid psychiatric disorders as independent risk factors for future suicide attempts. The NESARC is a large, nationally representative survey of mental illness in community-dwelling adults. Its comprehensive assessment of Axis I disorders and all ten DSM-IV personality disorders, coupled with its longitudinal design and large sample size provided a unique ability to assess risk factors for subsequent suicide attempts in MDD.
METHOD
Sample
The NESARC is a nationally representative longitudinal survey of the adult non-institutionalized, civilian population of the 50 United States conducted by the United States Census Bureau under the direction of the National Institute on Alcohol Abuse and Alcoholism (NIAAA). Wave 1 was conducted in 2001–2002 with a sample of 43,093 respondents age 18 and over (Grant et al., 2003). Wave 2 was a 3-year prospective follow-up comprising 34,653 of the Wave 1 respondents, representing a response rate of 86.7% of eligible respondents (Grant et al., 2005). In combination with the Wave 1 response rate of 81%, the cumulative response rate for Wave 2 is 70.2%. Trained lay interviewers conducted face-to-face assessments using computer-assisted software. Informed consent was obtained from all participants before beginning the interviews. Interviewers retested a random sample of both the Wave 1 and Wave 2 samples in order to assess the reliability of the survey (Grant et al., 2003; Grant et al., 2005). Detailed descriptions of methodology, sampling, and weighting procedures can be found elsewhere (Grant et al., 2003; Ruan et al., 2008).
Measures
Suicide Ideation and Attempts
In the Wave 1 NESARC, suicidal ideation and suicide attempts were assessed only among Wave 1 respondents who endorsed one of the following two MDD symptoms: “In your entire life, have you ever had a time, lasting at least 2 weeks, when you felt sad, blue, depressed, or down most of the time for at least 2 weeks?” or “In your entire life, have you ever had a time, lasting at least 2 weeks, when you didn’t care about the things that you usually cared about, or when you didn’t enjoy the things you usually enjoyed?” In order to assess suicide ideation and attempts, respondents were then asked whether they thought about committing suicide or attempted suicide, respectively, during that time when their mood was at its lowest or they enjoyed or cared the least about things. The exact question assessing suicide attempts was, “During that time when (your mood was at it’s lowest/you enjoyed or cared the least about things), did you attempt suicide?” The exact question assessing suicidal ideation was, “During that time when (your mood was at it’s lowest/you enjoyed or cared the least about things), did you think about committing suicide?”
Suicide attempts that occurred between the Wave 1 and 2 interviews were assessed at Wave 2 among individuals who endorsed depressed mood or anhedonia symptoms of MDD, and also in the general survey among all respondents. Therefore not all suicide attempts at Wave 2 necessarily occurred in the context of a major depressive episode. The exact question assessing suicide attempts was, “During the time since your LAST interview when (your mood was at it’s lowest/you enjoyed or cared the least about things), did you attempt suicide?” The exact question assessing suicidal ideation was, “During the time since your LAST interview when (your mood was at it’s lowest/you enjoyed or cared the least about things), did you think about committing suicide?” The question in the general survey assessing suicide attempts was, “In your ENTIRE life did you EVER attempt suicide?”
Sociodemographic Factors
Sociodemographic factors of sex, race/ethnicity, age, marital status, education, income, urbanicity and region of residence assessed at Wave 1 were examined as predictors of suicide attempts in the current study. Sex and urbanicity (urban vs. rural) were dichotomous variables while all other sociodemographic factors were categorical (See Table 1 for categories).
Table 1.
Demographic Characteristics of the Sample
| Characteristics | Wave I Lifetime MDD (N=6004) Na | Prevalence % (95% CI)a |
|---|---|---|
| Sex | ||
| Male | 1798 | 34.3 (32.8–35.8) |
| Female | 4206 | 65.7 (64.2–67.2) |
| Race/ethnicity | ||
| White | 3983 | 77.7 (75.2–80.0) |
| Hispanic/Latino | 946 | 8.6 (6.9–10.6) |
| Other | 1075 | 13.8 (12.4–15.3) |
| Age | ||
| 18–29 | 1257 | 23.1 (21.6–24.7) |
| 30–44 | 2073 | 33.7 (32.2–35.2) |
| 45+ | 2674 | 43.2 (41.6–44.9) |
| Marital Status | ||
| Married/Common-law | 2706 | 55.8 (54.2–57.4) |
| Widowed/Separated/Divorced | 1914 | 23.2 (21.9–24.5) |
| Never Married | 1384 | 21.0 (19.7–22.4) |
| Education | ||
| Less than high school | 889 | 13.7 (12.5–15.0) |
| High school graduate | 1605 | 26.7 (25.2–28.4) |
| Some college or higher | 3510 | 59.6 (57.8–61.4) |
| Income | ||
| $0–$19,999 | 1664 | 21.8 (20.3–23.4) |
| $20,000–$34,999 | 1302 | 20.3 (18.9–21.7) |
| $35,000–$59,999 | 1515 | 25.8 (24.3–27.4) |
| $60,000 or greater | 1523 | 32.2 (30.1–34.3) |
| Urbanicity | ||
| Urban | 2010 | 28.3 (25.0–31.8) |
| Rural | 3994 | 71.7 (68.2–75.0) |
| Region | ||
| Northeast | 1076 | 17.8 (12.9–24.2) |
| Midwest | 1441 | 25.2 (19.7–31.5) |
| South | 2029 | 32.7 (27.4–38.5) |
| West | 1458 | 24.3 (18.5–31.2) |
| Since Wave I Incident Suicide Attempt | 63 | 1.2 (0.9–1.7)b |
| Since Wave I Suicide Attempt | 169 | 2.7 (2.2–3.3)c |
Ns are unweighted values; percentages are weighted values.
3-year incidence of suicide attempts assessed at Wave 2 among people with MDD at Wave 1 without a history of previous suicide attempt.
3-year prevalence of suicide attempts assessed at Wave 2 among all people with MDD at Wave 1
p < .05,
p < .01,
p < .001.
Psychiatric Disorders
Axis I and II psychiatric disorders were assessed at Waves 1 and 2 according to the Diagnostic and Statistical Manual of Mental Disorders 4th Edition (DSM-IV; American Psychiatric Association, 2000) criteria using the Alcohol Use Disorders and Associated Disabilities Interview (AUDADIS-IV; Grant et al., 2001). This is a fully-structured diagnostic interview that is appropriate for use by trained lay interviewers. At Wave 1, Axis I disorders of major depression, dysthymia, mania, hypomania, panic disorder with or without agoraphobia, agoraphobia without panic disorder, social phobia, specific phobia, generalized anxiety disorder, alcohol abuse and dependence, and drug abuse and dependence were assessed. All Axis II diagnoses, excluding schizotypal, narcissistic and borderline personality disorders, were also assessed at Wave 1. The Wave 2 interview assessed all Axis I diagnoses included in Wave 1 and additionally assessed posttraumatic stress disorder (PTSD). The Wave 2 interview did not reassess the seven personality disorders assessed in Wave 1, but rather assessed the personality disorders excluded from the Wave 1 interview. Fair to excellent test-retest and inter-rater reliability have been demonstrated for diagnoses generated in both Waves 1 and 2 (Grant et al., 2003; Ruan et al., 2008). The validity of drug and alcohol diagnoses have been well-documented (Canino et al., 1999; Hasin et al., 1997) and validity of mood, anxiety and personality diagnoses assessed by the AUDADIS-IV has also been established statistically, using the NESARC data (Grant et al., 2004a; Grant et al., 2004b; Grant et al., 2004c).
For the purposes of the current study all diagnoses were lifetime and occurred previous to the Wave 1 interview. The three personality disorders assessed at Wave 2 were assumed to fit this time frame since personality disorder symptoms, by definition, begin before the age of 18. PTSD with onset after Wave 1 was excluded from the analyses.
Symptoms of Major Depressive Disorder
Seventeen depressive symptoms were assessed in the Wave 1 interview in order to generate a DSM-IV diagnosis of MDD. Many of the DSM-IV major depressive episode A-criteria are composed of more than one of these symptoms, but they were kept separate in analyses in order to present a more accurate characterization of relationships between depressive symptoms and suicide attempts. Depressive symptoms were also combined into a variable reflecting the number of depressive symptoms endorsed, as a proxy measure of depression severity.
Analytic Strategy
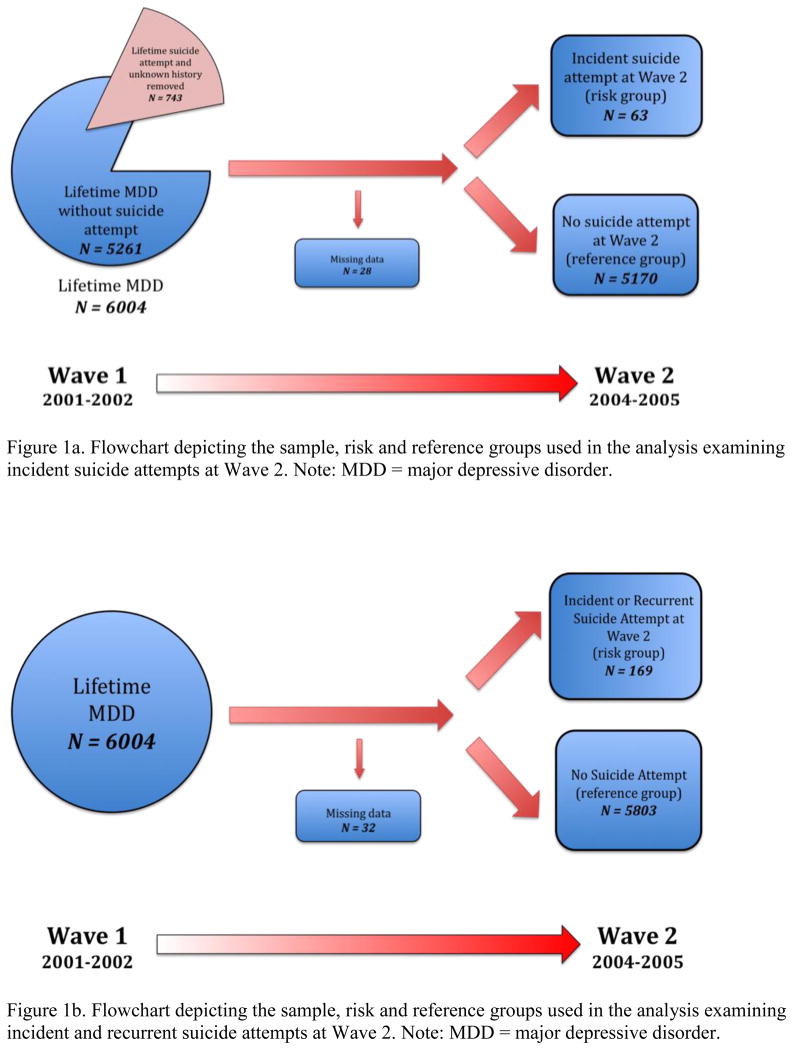
Two parallel sets of analyses were conducted in this study (Figure 1). The first examined associations between the above-mentioned correlates and incident suicide attempts during the 3-year follow-up period (Figure 1a). The second examined correlates of all suicide attempts (incident and recurrent) during the same period (Figure 1b). All analyses were conducted in the SUDAAN program (Shah et al., 1995) using Taylor Series Linearization, a variance estimation procedure that accounts for the complex survey methodology employed in the NESARC. Statistical weights and stratification variables are available specifically for this purpose.
Figure 1.
Analytic models
1. Incident Suicide Attempts at Wave 2
Incident suicide attempts were defined as suicide attempts occurring in the 3-year period between Wave 1 and Wave 2, only among the sub-sample of respondents with a lifetime diagnosis of MDD at Wave 1 who had not made a lifetime suicide attempt prior to Wave 1 (n=5261). By excluding individuals with MDD who had made a suicide attempt prior to Wave 1, only new (or incident) suicide attempts were captured. In this part of the analysis, the risk group consisted of people with an incident suicide attempt (n=63). They were compared to the reference group consisting of the remainder of the depressed persons who had never made a suicide attempt at any point in their lives (n=5170).
The incidence rate of suicide attempts over the 3 years between Waves 1 and 2 is reported as percentage of the at-risk group (i.e., individuals with major depression at Wave 1 without suicide attempts) and per 100 person-years. These incidence rates were calculated in an identical manner as previous studies with the prospective NESARC data (Grant et al., 2008). Specifically, the incidence rate is expressed as a percentage (I/T) × 100 where I is the weighted number of individuals with a first onset of suicide attempt and T is the population at risk (weighted n), or all individuals without a previous suicide attempt. Incidence rates per 100 person-years are calculated using the equation (I/(T − (1.5)I) × 100, which takes into account the population’s total period of exposure. The period of exposure is estimated at 1.5 years (the midpoint of the 3 year follow-up) as the assumption is typically made that the average point when a new case emerges lies halfway through the exposure period (Grant et al., 2008; Shah et al., 1995).
Predictors of incident suicide attempts at Wave 2 included sociodemographic factors, depressive features and lifetime psychiatric disorders occurring before the Wave 1 interview. Predictors were examined in cross-tabulations with the dependent variables and multiple logistic regression models. Sociodemographic factors were first examined in bivariate logistic regression models. Each psychiatric disorder and depressive feature was then examined in a regression model adjusting for sociodemographic factors significantly associated with incident suicide attempts. Each psychiatric disorder was also examined in regression models adjusting for sociodemographic factors and depressive features significantly associated with incident suicide attempts. A final regression model was examined wherein all sociodemographic factors, depressive symptoms and psychiatric diagnoses that were significant in previous models were entered simultaneously to predict incident suicide attempts.
Positive predictive values (PPVs) were calculated for each psychiatric diagnosis, depressive symptom and previous suicidal behavior. The PPV represents the probability that an individual will make a suicide attempt given the presence of one of these variables and is used to evaluate the effectiveness of each variable in predicting suicide attempts. The formula used for these calculations is based on the following:
The way that the formula was utilized in our calculations is the following:
wherein X refers to the presence of a specific variable and SA refers to a suicide attempt.
2. All Suicide Attempts at Wave 2
This part of the analysis examined risk factors for all suicide attempts (both incident and recurrent) during the 3-year period between Wave 1 and Wave 2. Because this analysis did not focus solely on incident suicide attempts, all individuals with a lifetime diagnosis of MDD at Wave 1 were included (n=6004). The risk group in this part of the study consisted of all people who had made a suicide attempt during the 3-year follow-up period (n=169). The reference group consisted of all individuals with lifetime MDD at Wave 1 who did not attempt suicide during the follow-up period (n=5803).
Predictors of all suicide attempts included sociodemographic factors, depressive features (including a history of suicide ideation or suicide attempts) and lifetime psychiatric disorders occurring before the Wave 1 interview. Predictors were examined in cross-tabulations with the dependent variables and multiple logistic regression models. The same pattern of regression models as described in the analyses of incident suicide attempts was employed to examine all suicide attempts.
RESULTS
Demographic characteristics of the sample as well as the incidence of suicide attempts at Wave 2 and the prevalence of suicide attempts at Wave 2 are presented in Table 1. The incidence of a suicide attempt among individuals with major depression was 1.2% for the 3-year period between interviews (1.3 per 100 person-years). The prevalence of suicide attempts in the follow-up period was 2.7%.
1. Incident Suicide Attempts at Wave 2
The only significant sociodemographic predictor of an incident suicide attempt was age (results not shown in tables but available upon request). Respondents age 45 and over were significantly less likely than those age 18–29 to have made an incident suicide attempt between Waves 1 and 2 (OR = 0.30, 95% CI = 0.10–0.87).
After adjusting for age, no depressive symptoms were significantly associated with incident suicide attempts. PPVs for depressive symptoms ranged from 0.8% to 1.5%, with the highest PPV associated with feeling worthless and excessive guilt (results not shown in tables but available upon request).
Psychiatric correlates of incident suicide attempts are presented in Table 2. Among anxiety disorders, panic disorder, specific phobia, posttraumatic stress disorder and any anxiety disorder were significantly associated with incident suicide attempts after adjusting for age. Paranoid, avoidant, borderline, schizotypal and any personality disorder were also predictive of an incident suicide attempt after adjusting for age. Finally, any drug use disorder, any alcohol use disorder, nicotine dependence and any substance use disorder were all significant predictors of an incident suicide attempt between Waves 1 and 2 after adjusting for age. PPVs for psychiatric correlates ranged from 1.3% to 5.0%.
Table 2.
Mental Disorder Correlates of Incident Suicide Attempts in Major Depressive Disordera
| Lifetime Psychiatric Disorders at Wave 1 (N) | No Suicide Attemptb (N=5170) N (%)d | Suicide Attemptc (N=63) N (%)d | AORe (95% CI) | Positive Predictive Valuef % (95% CI) |
|---|---|---|---|---|
| Anxiety disorders | ||||
| Panic disorder (N=761) | 744 (14.4) | 17 (32.6) | 3.01 (1.39–6.50)** | 2.8 (1.4–5.4) |
| Agoraphobia (N=26) | 25 (0.6) | 1 (1.1) | ---g | --- |
| Social phobia (N=712) | 699 (14.4) | 13 (20.8) | 1.51 (0.63–3.61) | 1.8 (0.8–3.8) |
| Specific phobia (N=1048) | 1032 (20.7) | 16 (38.2) | 2.29 (1.01–5.23)* | 2.3 (1.2–4.3) |
| Generalized anxiety disorder (N=832) | 818 (16.6) | 14 (25.3) | 1.85 (0.77–4.47) | 1.9 (0.9–3.8) |
| Posttraumatic stress disorder (N=682) | 663 (13.0) | 19 (28.7) | 2.86 (1.32–6.23)** | 2.3 (1.2–4.1) |
| Any anxiety disorder (N=2494) | 2450 (50.0) | 44 (72.8) | 2.76 (1.29–5.91)** | 1.8 (1.2–2.7) |
| Personality disorders | ||||
| Antisocial (N=343) | 331 (7.2) | 12 (11.8) | 1.44 (0.61–3.42) | 2.0 (0.9–4.5) |
| Dependent (N=48) | 46 (0.8) | 2 (7.0) | --- | --- |
| Obsessive-compulsive (N=934) | 917 (18.8) | 17 (19.9) | 1.03 (0.41–2.58) | 1.3 (0.6–3.0) |
| Paranoid (N=666) | 643 (12.0) | 23 (27.4) | 2.44 (1.21–4.94)* | 2.8 (1.6–4.8) |
| Schizoid (N=428) | 419 (7.8) | 9 (14.4) | 1.91 (0.62–5.84) | 2.3 (0.8–6.2) |
| Histrionic (N=247) | 241 (4.4) | 6 (8.3) | 1.57 (0.42–5.90) | 2.3 (0.7–8.0) |
| Avoidant (N=383) | 369 (7.2) | 14 (22.0) | 3.32 (1.53–7.18)** | 3.7 (1.9–7.0) |
| Narcissistic (N=552) | 540 (9.1) | 12 (10.5) | 1.04 (0.46–2.34) | 1.4 (0.7–2.9) |
| Borderline (N=704) | 670 (12.6) | 34 (53.4) | 7.23 (3.69–14.17)*** | 5.0 (3.3–7.7) |
| Schizotypal (N=431) | 418 (7.8) | 13 (22.0) | 3.11 (1.35–7.18)** | 3.4 (1.6–7.1) |
| Any personality disorder (N=2190) | 2142 (41.5) | 48 (71.3) | 3.12 (1.46–6.69)** | 2.1 (1.4–3.1) |
| Substance use disorders | ||||
| Any drug use disorder (N=937) | 915 (18.7) | 22 (41.0) | 2.57 (1.21–5.47)* | 2.7 (1.6–4.5) |
| Any alcohol use disorder (N=2139) | 2103 (42.5) | 36 (66.8) | 2.57 (1.36–4.86)** | 1.9 (1.2–3.0) |
| Nicotine dependence (N=1516) | 1481 (30.5) | 35 (59.5) | 3.17 (1.69–5.95)*** | 2.4 (1.6–3.5) |
| Any substance use disorder (N=2778) | 2730 (55.0) | 48 (83.6) | 3.85 (1.87–7.90)*** | 1.9 (1.3–2.7) |
Among people with lifetime major depression assessed at Wave 1 with no history of suicide attempt (N=5261)
Reference group is individuals without a suicide attempt between Wave 1 and Wave 2. Individuals with suicidal ideation at Wave 1 were excluded from this group.
Risk group is individuals with a suicide attempt between Wave 1 and Wave 2
Ns are unweighted values; percentages are weighted values
AOR: Adjusted Odds Ratio: adjusted for age.
Positive predictive values are based on weighted N’s. Note: boldface type indicates significance;
p < .05,
p < .01,
p < .001
Dashed lines signify statistics not presented due to cell sizes less than 5.
In the final model predicting incident suicide attempts, age, any anxiety disorder, any personality disorder and any substance use disorder were entered simultaneously (Table 3). These psychiatric disorder categories were entered instead of each disorder separately due to sample size concerns. In this model, any personality disorder and any substance use disorder were the only variables that remained significant predictors of incident suicide attempts.
Table 3.
Final Model of Incident Suicide Attempts In Major Depressive Disordera
| Incident Suicide Attempts (N=63) AORb (95% CI) | |
|---|---|
| Sociodemographics | |
| Age | |
| 18–29 | 1.00 |
| 30–44 | 0.71 (0.32–1.57) |
| 45+ | 0.35 (0.12–1.01) |
| Comorbid Psychiatric Disorders | |
| Any Anxiety Disorder | 2.25 (0.95–4.64) |
| Any Personality Disorder | 2.44 (1.04–5.71)* |
| Any Substance Use Disorder | 4.10 (1.82–9.23)*** |
Among people with lifetime major depression assessed at Wave 1 with no history of suicide attempt (N=5261)
AOR: Adjusted Odds Ratio: all variables in table were entered simultaneously
p < .05,
p < .01,
p < .001;
Note: boldface type indicates significance.
2. All Suicide Attempts at Wave 2
Age, marital status and income emerged as significant predictors of suicide attempts during the follow-up period (results not shown in tables but available upon request). Respondents age 45 and over were significantly less likely than those age 18–29 to have made a suicide attempt between Waves 1 and 2 (OR = 0.30, 95% CI = 0.17–0.53). Respondents who were never married were significantly more likely than respondents who were married or common-law to have made a suicide attempt between Waves 1 and 2 (OR = 1.81, 95% CI = 1.08–3.03). Respondents in all three higher income categories were significantly less likely to have made a suicide attempt between Waves 1 and 2 compared to those in the lowest income category.
Specific features of MDD were associated with suicide attempts occurring between Wave 1 and 2 (results not shown in tables). After adjusting for significant sociodemographic factors (age, marital status, and income), the strongest associations were observed with Wave 1 lifetime suicidal ideation (AOR = 6.04, 95% CI = 3.63–10.05) and a Wave 1 lifetime suicide attempt (AOR = 11.28, 95% CI = 7.19–17.70). Depressive symptoms of anhedonia, feeling worthless and excessive guilt as well as the number of depressive symptoms endorsed were also significantly associated with all suicide attempts at Wave 2 in the adjusted model. PPV’s for depressive symptoms were in the range of 2.7% to 3.7%, with feeling worthless having the highest PPV. PPV’s for suicidal behaviors were slightly higher (5.5% for suicidal ideation and 14.1% for suicide attempts).
After adjusting for sociodemographic factors as well as depressive features, many psychiatric disorders remained significantly associated with all suicide attempts during the follow-up period (Table 4). Panic disorder, generalized anxiety disorder, posttraumatic stress disorder and any anxiety disorder were significantly associated with all suicide attempts at Wave 2. Dependent, paranoid, schizoid, avoidant, borderline, schizotypal and any personality disorder were also significantly associated with all suicide attempts. Finally, any drug use disorder, nicotine dependence and any substance disorder were also significantly associated with all suicide attempts during the 3-year follow-up period.
Table 4.
Mental Disorder Correlates of All Suicide Attempts in Major Depressive Disordera
| Lifetime Psychiatric Disorders at Wave 1 (N) | No Suicide Attemptb (N=5803) N (%)d | Suicide Attemptc (N=169) N (%)d | AORe (95% CI) | AOR-2f (95% CI) | Positive Predictive Valueg % (95% CI) |
|---|---|---|---|---|---|
| Anxiety disorders | |||||
| Panic disorder (N=982) | 919 (15.8) | 63 (39.1) | 3.25 (2.12–4.98)*** | 1.91 (1.14–3.21)* | 6.4 (4.6–8.9) |
| Agoraphobia (N=29) | 28 (0.6) | 1 (0.5) | ---h | --- | --- |
| Social phobia (N=867) | 824 (15.1) | 43 (27.8) | 1.96 (1.21–3.19)** | 1.41 (0.86–2.33) | 4.9 (3.2–7.3) |
| Specific phobia (N=1272) | 1218 (21.8) | 54 (40.0) | 2.24 (1.37–3.66)** | 1.58 (0.91–2.73) | 4.9 (3.3–7.0) |
| Generalized anxiety disorder (N=1019) | 965 (17.2) | 54 (35.5) | 2.78 (1.76–4.38)*** | 1.96 (1.17–3.26)* | 5.4 (3.8–7.6) |
| Posttraumatic stress disorder (N=851) | 800 (14.1) | 51 (33.1) | 3.09 (1.92–4.98)*** | 2.20 (1.27–3.83)** | 5.5 (3.8–7.8) |
| Any anxiety disorder (N=2971) | 2846 (51.5) | 125 (80.6) | 3.82 (2.21–6.60)*** | 3.05 (1.63–5.72)*** | 4.1 (3.2–5.2) |
| Personality disorders | |||||
| Antisocial (N=486) | 444 (8.6) | 42 (21.3) | 2.17 (1.34–3.52)** | 1.05 (0.61–1.80) | 6.5 (4.4–9.5) |
| Dependent (N=99) | 81 (1.4) | 18 (15.8) | 9.87 (5.17–18.85)*** | 4.43 (1.93–10.18)*** | 24.6 (15.0–37.7) |
| Obsessive-compulsive (N=1132) | 1080 (19.7) | 52 (30.1) | 1.64 (0.97–2.77) | 1.13 (0.63–2.01) | 4.1 (2.6–6.3) |
| Paranoid (N=887) | 816 (13.3) | 71 (39.5) | 3.31 (2.10–5.21)*** | 2.13 (1.29–3.51)** | 7.7 (5.6–10.4) |
| Schizoid (N=569) | 527 (8.6) | 42 (31.1) | 4.10 (2.53–6.63)*** | 2.22 (1.31–3.76)** | 9.1 (6.1–13.4) |
| Histrionic (N=341) | 315 (5.2) | 26 (18.1) | 2.93 (1.62–5.29)*** | 1.43 (0.77–2.64) | 8.8 (5.4–14.1) |
| Avoidant (N=537) | 485 (8.3) | 52 (32.6) | 4.27 (2.72–6.70)*** | 2.46 (1.47–4.12)*** | 9.8 (6.9–13.7) |
| Narcissistic (N=679) | 639 (9.7) | 40 (16.7) | 1.48 (0.89–2.44) | 1.16 (0.67–2.01) | 4.6 (3.0–6.9) |
| Borderline (N=999) | 888 (14.7) | 111 (67.8) | 10.27 (6.65–15.86)*** | 6.61 (4.07–10.72)*** | 11.4 (9.1–14.3) |
| Schizotypal (N=595) | 535 (8.7) | 60 (36.5) | 4.91 (3.01–8.00)*** | 3.12 (1.85–5.26)*** | 10.5 (7.2–14.9) |
| Any personality disorder (N=2714) | 2569 (44.2) | 145 (85.5) | 6.25 (3.35–11.67)*** | 4.00 (1.95–8.22)*** | 5.1 (4.1–6.4) |
| Substance use disorders | |||||
| Any drug use disorder (N=1178) | 1110 (20.3) | 68 (44.3) | 2.59 (1.66–4.06)*** | 1.69 (1.05–2.71)* | 5.7 (4.3–7.6) |
| Any alcohol use disorder (N=2516) | 2419 (43.6) | 97 (58.2) | 1.80 (1.19–2.72)** | 1.43 (0.92–2.21) | 3.6 (2.8–4.7) |
| Nicotine dependence (N=1827) | 1733 (31.9) | 94 (54.6) | 2.36 (1.58–3.52)*** | 1.80 (1.18–2.75)** | 4.6 (3.5–5.9) |
| Any substance use disorder (N=3261) | 3131 (56.2) | 130 (80.0) | 2.99 (1.88–4.74)*** | 2.51 (1.56–4.04)*** | 3.8 (3.1–4.7) |
Among people with lifetime major depression assessed at Wave 1 (N=6004)
Reference group is individuals without a suicide attempt between Wave 1 and Wave 2.
Risk group is individuals with a suicide attempt between Wave 1 and Wave 2
Ns are unweighted values; percentages are weighted values
AOR: Adjusted Odds Ratio: adjusted for age, marital status, and income.
AOR-2: Adjusted Odds Ratio: adjusted for age, marital status, income and depression features significantly related to a suicide attempt between Wave 1 and Wave 2 after adjusting for sociodemographics (Anhedonia, Feeling worthless, Excessive Guilt, Wave I Lifetime suicidal ideation, Wave I Lifetime suicide attempt, and Number of depressive symptoms).
Positive predictive values are based on weighted N’s; Note: boldface type indicates significance;
p < .05,
p < .01,
p < .001
Dashed lines signify statistics not presented due to cell sizes less than 5.
In the final model predicting all suicide attempts at Wave 2, age, marital status, income, anhedonia, feeling worthless, excessive guilt, Wave 1 lifetime suicidal ideation, a Wave 1 lifetime suicide attempt, number of depressive symptoms, any anxiety disorder, any personality disorder and any substance use disorder were entered simultaneously (Table 5). In this model, age, income, Wave 1 lifetime suicide attempt, any anxiety disorder, any personality disorder and any substance disorder remained significant predictors of future suicide attempts.
Table 5.
Final Model of All Suicide Attempts In Major Depressive Disordera
| All Suicide Attempts (N=169) AORb (95% CI) | |
|---|---|
| Sociodemographics | |
| Age | |
| 18–29 | 1.00 |
| 30–44 | 1.12 (0.64–1.96) |
| 45+ | 0.49 (0.26–0.96)* |
| Marital Status | |
| Married/Common-law | 1.00 |
| Widowed/Separated/Divorced | 0.76 (0.40–1.46) |
| Never Married | 0.97 (0.51–1.84) |
| Income | |
| $0–$19,999 | 1.00 |
| $20,000–$34,999 | 0.51 (0.27–0.98)* |
| $35,000–$59,999 | 0.54 (0.24–1.19) |
| $60,000 or greater | 0.44 (0.20–0.99)* |
| Depression Features | |
| Anhedonia | 1.60 (0.56–4.57) |
| Feeling Worthless | 1.40 (0.64–3.04) |
| Excessive Guilt | 1.53 (0.84–2.77) |
| Wave I Lifetime Suicidal Ideation | 1.57 (0.81–3.08) |
| Wave I Lifetime Suicide Attempt | 5.57 (3.16–10.17)*** |
| Number of depressive symptoms | 0.96 (0.87–1.05) |
| Comorbid Psychiatric Disorders | |
| Any Anxiety Disorder | 2.31 (1.19–4.47)* |
| Any Personality Disorder | 3.23 (1.47–7.10)** |
| Any Substance Use Disorder | 2.26 (1.32–3.85)** |
Among people with lifetime major depression assessed at Wave 1 (N=6004)
AOR: Adjusted Odds Ratio: all variables in table were entered simultaneously
p < .05,
p < .01,
p < .001;
Note: boldface type indicates significance.
DISCUSSION
For the first time, a longitudinal nationally representative sample was used to examine risk factors for suicide attempts among individuals with MDD. This study was able to explore a more comprehensive range of mental disorders and depressive symptoms than has been previously possible in large epidemiologic samples. It extends our understanding of the spectrum of suicidal behavior by examining correlates of incident suicide attempts among people who have never attempted suicide. This study also confers important information regarding the independent risk associated with mental illness comorbidity when compared to previous suicidal behavior and other features specific to MDD. It overcomes limitations inherent in clinical studies and thus provides new insight into risk factors for suicidal behavior in depressed people who have not necessarily presented to treatment providers. These advantages provide a novel context that increases the importance of the findings from this study and in so doing extends our knowledge on risk factors for suicidal behavior in MDD.
Panic disorder comorbidity in MDD increases the odds of incident suicide attempts threefold when compared to MDD without panic disorder. Previous studies have yielded contradictory results as to the role of panic disorder in suicidal behavior when comorbid with MDD (Bolton et al., 2008a; Placidi et al., 2000). One study found panic disorder to be protective against more lethal suicide attempts (Nakagawa et al., 2009). The current study is the first longitudinal study of depressed individuals to demonstrate an association between panic disorder and future suicide attempts. Posttraumatic stress disorder was also strongly associated with a risk of new-onset suicide attempts. This finding corroborates previous studies demonstrating heightened risk of suicide attempts when PTSD is comorbid with MDD (Oquendo et al., 2003; Oquendo et al., 2005). Although longitudinal epidemiologic studies have found that anxiety disorders independently increase the risk of incident suicide attempts (Boden et al., 2007; Bolton et al., 2008b; Sareen et al., 2005b), longitudinal studies of suicidal behavior specific to depressed cohorts have not identified anxiety disorder comorbidity as a predictor of suicidal behavior (Oquendo et al., 2006). These discrepant findings may be due to methodological differences in study design, including sampling and assessment of comorbidity. Our findings emphasize the role of anxiety disorders in suicidal behavior, and should alert care providers to the presence of panic disorder and PTSD as potential risk factors for future suicidal behavior in individuals presenting with MDD.
The risk of new-onset suicide attempts in MDD is also heightened by personality disorder and substance use disorder comorbidity. Borderline personality disorder increased the odds of incident suicide attempts by a factor of seven. Borderline personality disorder is a well-recognized risk factor for suicidal behavior both independently and when comorbid with MDD (Soloff et al., 2000; Yen et al., 2003). The current results extend these previous findings to a general population sample. The NESARC also allowed an investigation of suicidal behavior in the less-studied Cluster A and C personality disorders, with intriguing results. Baseline avoidant, paranoid, and schizotypal personality disorders comorbid with MDD were all associated with higher rates of suicide attempts at follow-up. This is consistent with our previous cross-sectional analysis of personality disorder comorbidity in MDD, which revealed that avoidant and paranoid personality disorders, among others, were associated with a lifetime history of suicide attempts (Bolton et al., 2008a). All substance use disorders were significantly associated with incident suicide attempts, with nicotine dependence having the strongest association. Longitudinal studies have demonstrated cigarette smoking to be associated with the development of depression (Fergusson et al., 2003), and among depressed people it has emerged as an important independent predictor of future suicidal acts (Oquendo et al., 2004). This mechanism may be partially explained by aggression and impulsivity.
Depressed smokers have higher rates of aggressive and impulsive personality traits (Angst et al., 1998), and these same traits have been identified as risk factors for suicide attempts (Mann et al., 1999). Our finding of an elevated risk of incident suicide attempts in alcohol use disorders is also consistent with previous studies (Maser et al., 2002; Sokero et al., 2003). The disinhibition effect of alcohol and drugs likely contributes to the heightened risk of suicidality associated with these disorders. Clinicians should be aware that comorbid alcohol or drug disorders and nicotine dependence are worrisome signs suggestive of future suicidal acts.
Many interesting findings emerged from analyses examining the entire cohort of people with MDD at Wave 1. As expected, a history of past suicidal ideation and previous suicide attempts at baseline assessment were strong risk factors for suicide attempts within three years follow-up. Previous suicide attempts are one of the most consistently identified risk factors for future suicide attempts in depression (Harrington et al., 1990; Oquendo et al., 2004; Sokero et al., 2005). The effect of previous suicide attempts is strong and often renders associations with other risk factors nonsignificant (Sokero et al., 2005). Surprisingly, after adjusting for the effects of past suicidal ideation, previous suicide attempts, and significant depressive symptoms, many comorbid Axis I and II disorders remained significantly associated with a higher likelihood of suicide attempts at follow-up. Panic disorder, generalized anxiety disorder, and PTSD were anxiety disorders positively correlated with new-onset suicide attempts. Several personality disorders, nicotine dependence, and drug use disorders were also associated with future suicide attempts. Some disorders, such as antisocial personality disorder, fell from significance after controlling for a history of suicide attempts, indicating that the latter may account for a significant portion of the variance in the relationship with suicidal behavior and mental disorders. A multivariable regression model of significant correlates revealed past suicide attempts, anxiety, personality, and substance use disorders to be independently associated with subsequent suicide attempts, whereas higher income and age over 45 were protective. Therefore, while past attempts remain a strong predictor of repeat suicide attempts, comorbid mental illnesses should alert clinicians as independent risk factors.
While there are many correlates significantly associated with suicidal behavior, it is important to consider the predictive ability of these factors. The PPV for many of the associations were low. Most disorders carried a PPV of less than 10%, indicating that individual comorbid disorders have low specificity in predicting future suicide attempts within 3 years. Even a history of suicide attempt, although strongly associated with subsequent suicide attempts in regression models, predicted a future attempt at a rate of only 14%. These PPV findings emphasize the difficulty in accurately identifying people who will later engage in suicidal behavior, despite growing knowledge of correlates that make up the profile of suicidal individuals. It is likely that multiple comorbid disorders would result in higher PPV values; future studies examining specific combinations of risk factors could produce a refined risk assessment for a person’s total burden of mental illness.
The results of this study need to be interpreted in the context of specific limitations. The first pertains to the assessment of suicidal behavior. We were unable to assess the severity or intended lethality of suicide attempts, and could not address indirect severity markers such as health service contacts related to suicide attempts. Highly lethal suicide attempts may differentiate individuals that are closer in profile to suicide completers than their counterparts who choose less lethal means (Linehan, 1986; Mann, 2002). It would be important in future studies to determine whether the subgroup of individuals with MDD with more lethal suicide attempts had a different pattern of correlates when compared to those with less severe suicide attempts. Another limitation of this study was the inability to examine correlates of completed suicide, since information on completed suicide is not available in the NESARC survey. Our study was limited to an examination of non-fatal suicidal behavior, and as a result the potential risk factors identified in our study may not apply to completed suicide. Some evidence suggests that suicide attempters and suicide completers are different populations (Beautrais, 2001) whereas other studies implicate suicide attempts as important risk factors in the trajectory to suicide (Harris et al., 1997; Suominen et al., 2004). Future prospective studies including suicide completers are necessary to elucidate specific risk factors for completion as well as to understand the relationship between suicide attempts and suicide. Specific elements of MDD were not examined as factors influencing the risk of suicide attempts, such as the chronicity or recurrence of depressive episodes. It would also be of interest to further examine the role of suicidal ideation in future suicidal behavior given recent findings showing that suicidal ideation influences the relationship between mental disorders and future suicidal behavior (Borges et al., 2008). Another limitation of the current study is that we did not differentiate people who made multiple suicide attempts from those who attempted only once. Lastly, it is possible that the wording of the specific questions asking about suicidal behavior may have been misinterpreted by respondents, resulting in inaccurate prevalence rates of suicide attempts.
A further limitation potentially influencing our findings is the lack of assessment of other known risk factors for suicide attempts. We were unable to assess personality traits such as impulsivity and aggression which have been shown to be important factors in suicide attempts (Oquendo et al., 2004) and completion (Dumais et al., 2005). Hopelessness is a worrisome cognition that has been implicated in future suicide attempts (Malone et al., 2000), but was not assessed specifically in this survey. Furthermore, we could not assess the temporal relationship between correlates and suicide attempts at a greater level of detail than the two assessment points 3 years apart. Therefore the individual’s mental state at time of attempt could not be determined. This prospective design identified correlates of MDD that increase future risk of suicide attempt, but it does not permit an examination of more proximal factors that lead a person to attempt suicide. Psychological autopsy studies are better suited to capture this level of detail and have shown, for example, that specific stressors and a lack of mental health resource coordination are temporally associated with suicide (Lesage et al., 2008; Seguin et al., 2006). Despite these specific limitations, the NESARC’s longitudinal design and more comprehensive assessment of mental disorders compared to other large mental health surveys allow it to overcome many of the limitations in previous studies addressing risk factors at the population level. The complete assessment of all 10 personality disorders in particular is a major advancement in epidemiologic studies of suicidal behavior, and strengthens the findings of this study.
In summary, this study identifies specific anxiety, personality, and substance use disorders as risk factors for future suicide attempts in MDD. It furthers our understanding by examining depressed individuals with no prior suicidal behavior, a population understudied to date. By examining a nationally representative sample, it overcomes biases inherent in clinical studies and extends findings to a population level. The findings from this study along with its methodological advantages will likely contribute to the ongoing development of suicide prevention strategies. Future large-scale prospective studies including completed suicide as an outcome are necessary to enhance the predictive ability of risk factors in this challenging area of study.
Acknowledgments
The authors would like to acknowledge Shay-Lee Belik, MSc., for her assistance with statistical analysis, and Rae Spiwak, MSc., for her assistance with manuscript preparation.
Footnotes
Previously presented at the 162nd Annual Meeting of the American Psychiatric Association in San Francisco, USA, May 17, 2009, at the Research Colloquium for Junior Investigators
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Reference List
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4. Washington, DC: American Psychiatric Association; 2000. text revision (DSM-IV-TR) [Google Scholar]
- Angst J, Clayton PJ. Personality, smoking and suicide: A prospective study. J Affect Disord. 1998;51:55–62. doi: 10.1016/s0165-0327(98)00156-6. [DOI] [PubMed] [Google Scholar]
- Beautrais AL. Suicides and serious suicide attempts: Two populations or one? Psychol Med. 2001;31:837–845. doi: 10.1017/s0033291701003889. [DOI] [PubMed] [Google Scholar]
- Bolton JM, Belik S, Enns MW, Cox BJ, Sareen J. Exploring the correlates of suicide attempts among individuals with major depressive disorder: Findings from the National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry. 2008a;69:1139–1149. doi: 10.4088/jcp.v69n0714. [DOI] [PubMed] [Google Scholar]
- Bolton JM, Cox BJ, Afifi TO, Enns MW, Bienvenu OJ, Sareen J. Anxiety disorders and risk for suicide attempts: Findings from the Baltimore Epidemiologic Catchment Area follow-up study. Depress Anxiety. 2008b;25:477–481. doi: 10.1002/da.20314. [DOI] [PubMed] [Google Scholar]
- Boden JM, Fergusson DM, Horwood LJ. Anxiety disorders and suicidal behaviors in adolescence and young adulthood: Findings from a longitudinal study. Psychol Med. 2007;37:431–440. doi: 10.1017/S0033291706009147. [DOI] [PubMed] [Google Scholar]
- Borges G, Angst J, Nock MK, Ruscio AM, Kessler RC. Risk factors for the incidence and persistence of suicide-related outcomes: A 10-year follow-up study using the National Comorbidity Surveys. J Affect Disord. 2008;105:25–33. doi: 10.1016/j.jad.2007.01.036. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bulik CM, Carpenter LL, Kupfer DJ, Frank E. Features associated with suicide attempts in recurrent major depression. J Affect Disord. 1990;18:29–37. doi: 10.1016/0165-0327(90)90114-n. [DOI] [PubMed] [Google Scholar]
- Canino GJ, Bravo M, Ramfrez R, Febo V, Fernandez R, Hasin DS. The Spanish Alcohol Use Disorder and Associated Disabilities Interview Schedule (AUDADIS): Reliability and concordance with clinical diagnoses in a Hispanic population. J Stud Alcohol. 1999;60:790–799. doi: 10.15288/jsa.1999.60.790. [DOI] [PubMed] [Google Scholar]
- Cavanagh JT, Carson AJ, Sharpe M, Lawrie SM. Psychological autopsy studies of suicide: A systematic review. Psychol Med. 2003;33:395–405. doi: 10.1017/s0033291702006943. [DOI] [PubMed] [Google Scholar]
- Chen YW, Dilsaver SC. Lifetime rates of suicide attempts among subjects with bipolar and unipolar disorders relative to subjects with other Axis I disorders. Biol Psychiatry. 1996;39:896–899. doi: 10.1016/0006-3223(95)00295-2. [DOI] [PubMed] [Google Scholar]
- Claassen CA, Trivedi MH, Rush AJ, Husain M, Zisook S, Young E, Leuchter A, Wisniewski S, Balasubramani G, Alpert J. Clinical differences among depressed patients with and without a history of suicide attempts: Findings from the STAR*D trial. J Affect Disord. 2007;97:77–84. doi: 10.1016/j.jad.2006.05.026. [DOI] [PubMed] [Google Scholar]
- Corbitt EM, Malone M, Haas GL, Mann JJ. Suicidal behavior in patients with major depression and comorbid personality disorders. J Affect Disord. 1996;39:61–72. doi: 10.1016/0165-0327(96)00023-7. [DOI] [PubMed] [Google Scholar]
- Dumais A, Lesage AD, Alda M, Rouleau G, Dumont M, Chawky MP, Roy M, Mann JJ, Benkelfat C, Turecki G. Risk factors for suicide completion in major depression: A case-control study of impulsive and aggressive behaviors in men. Am J Psychiatry. 2005;162:2116–2124. doi: 10.1176/appi.ajp.162.11.2116. [DOI] [PubMed] [Google Scholar]
- Fergusson DM, Goodwin RD, Horwood LJ. Major depression and cigarette smoking: Results of a 21-year longitudinal study. Psychol Med. 2003;33:1357–1367. doi: 10.1017/s0033291703008596. [DOI] [PubMed] [Google Scholar]
- Friedman RC, Aronoff MS, Clarkin JF, Corn R, Hurt WS. History of suicidal behavior in depressed borderline inpatients. Am J Psychiatry. 1983;140:1023–1026. doi: 10.1176/ajp.140.8.1023. [DOI] [PubMed] [Google Scholar]
- de Graaf R, Bijl RV, Smit F, Vollebergh WAM. Predictors of first incidence of DSM-III-R psychiatric disorders in the general population: Findings from the Netherlands Mental Health Survey and Incidence Study. Acta Psychiatr Scand. 2002;106:303–313. doi: 10.1034/j.1600-0447.2002.01397.x. [DOI] [PubMed] [Google Scholar]
- Grant BF, Dawson DA, Hasin DS. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-DSM-IV Version. Bethesda, MD: National Institute on Alcohol Abuse and Alcoholism; 2001. [Google Scholar]
- Grant BF, Dawson DA, Stinson FS, Chou PS, Kay W, Pickering R. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-IV (AUDADIS-IV): Reliability of alcohol consumption, tobacco use, family history of depression and psychiatric diagnostic modeuls in a general population sample. Drug Alcohol Depend. 2003;71:7–16. doi: 10.1016/s0376-8716(03)00070-x. [DOI] [PubMed] [Google Scholar]
- Grant BF, Goldstein RB, Chou SP, Dawson DA, Saha TD, Smith SM, Pulay AJ, Pickering RP, Ruan WJ, Compton WM. Sociodemographic and psychopathologic predictors of first incidence of DSM-IV substance use, mood and anxiety disorders: Results from the Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions. Mol Psychiatry. 2008;28:1–16. doi: 10.1038/mp.2008.41. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Grant BF, Hasin DS, Stinson FS, Dawson DA, Chou SP, Ruan WJ, Pickering RP. Prevalence, correlates and disability of personality disorders in the United States: Results from the National Epidemiologic Survey on Alcohol and Related Conditions. J Clin Psychiatry. 2004;65:948–958. doi: 10.4088/jcp.v65n0711. [DOI] [PubMed] [Google Scholar]
- Grant BF, Kaplan KD. Source and accuracy statement for the Wave 2 National Epidemiologic Survey on Alcohol and Related Conditions (NESARC) Rockville, Maryland: National Institute on Alcohol Abuse and Alcoholism; 2005. [Google Scholar]
- Grant BF, Kaplan K, Shepard J, Moore T. Source and Accuracy Statement: Wave 1 National Epidemiologic Survey on Alcohol and Related Conditions (NESARC) Bethesda, MD: National Institute on Alcohol Abuse and Alcoholism; 2003. [Google Scholar]
- Grant BF, Stinson FS, Dawson DA, Chou SP, Dufour MC, Compton W, Pickering RP, Kaplan K. Prevalence and co-occurrence of substance use disorders and independent mood and anxiety disorders: Results from the National Epidemiologic survey on Alcohol and Related Conditions. Arch Gen Psychiatry. 2004;61:807–816. doi: 10.1001/archpsyc.61.8.807. [DOI] [PubMed] [Google Scholar]
- Grant BF, Stinson FS, Dawson DA, Chou SP, Ruan WJ, Pickering RP. Co-occurrence of 12-month alcohol and drug use disorders and personality disorders in the United States: Results from the National Epidemiologic Survey on Alcohol and Related Conditions. Arch Gen Psychiatry. 2004;61:361–368. doi: 10.1001/archpsyc.61.4.361. [DOI] [PubMed] [Google Scholar]
- Hansen PE, Wang AG, Stage KB, Kragh-Sorensen P The Danish University Antidepressant Group. Comorbid personality disorder predicts suicide after major depression: A 10-year follow-up. Acta Psychiatr Scand. 2003;107:436–440. [PubMed] [Google Scholar]
- Harrington R, Fudge H, Rutter M, Pickles A, Hill J. Adult outcomes of childhood and adolescent depression. 1 Psychiatric status. Arch Gen Psychiatry. 1990;47:465–473. doi: 10.1001/archpsyc.1990.01810170065010. [DOI] [PubMed] [Google Scholar]
- Harris EC, Barraclough B. Suicide as an outcome for mental disorders. A meta-analysis Br J Psychiatry. 1997;170:205–228. doi: 10.1192/bjp.170.3.205. [DOI] [PubMed] [Google Scholar]
- Hasin D, Carpenter KM, McCloud S, Smith M, Grant B. The Alcohol Use Disorder and Associated Disabilities Interview Schedule (AUDADIS): Reliability of alcohol and drug modules in a clinical sample. Drug Alcohol Depend. 1997;44:133–141. doi: 10.1016/s0376-8716(97)01332-x. [DOI] [PubMed] [Google Scholar]
- Kessler RC, Borges G, Walters EE. Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry. 1999;56:617–626. doi: 10.1001/archpsyc.56.7.617. [DOI] [PubMed] [Google Scholar]
- Lesage AD, Boyer R, Grunberg F, Vanier C, Morissette R, Buteau-Menard C, Loyer M. Suicide and mental disorders: A case-control study of young men. Am J Psychiatry. 1994;151:1063–1068. doi: 10.1176/ajp.151.7.1063. [DOI] [PubMed] [Google Scholar]
- Lesage A, Séguin M, Guy A, Daigle F, Bayle MN, Chawky N, Tremblay N, Turecki G. Systematic services audit of consecutive suicides in New Brunswick: The case for coordinating specialist mental health and addiction services. Can J Psychiatry. 2008;53:671–678. doi: 10.1177/070674370805301006. [DOI] [PubMed] [Google Scholar]
- Linehan MM. Suicidal people. One population or two? Ann NY Acad Sci. 1986;487:16–33. doi: 10.1111/j.1749-6632.1986.tb27882.x. [DOI] [PubMed] [Google Scholar]
- Malone KM, Haas GL, Sweeney JA, Mann JJ. Major depression and the risk of attempted suicide. J Affect Disord. 1995;34:173–185. doi: 10.1016/0165-0327(95)00015-f. [DOI] [PubMed] [Google Scholar]
- Malone KM, Oquendo MA, Haas GL, Ellis SP, Shuhua L, Mann JJ. Protective factors against suicidal acts in major depression: Reasons for living. Am J Psychiatry. 2000;57:1084–1088. doi: 10.1176/appi.ajp.157.7.1084. [DOI] [PubMed] [Google Scholar]
- Mann JJ. A current perspective of suicide and attempted suicide. Ann Intern Med. 2002;136:302–311. doi: 10.7326/0003-4819-136-4-200202190-00010. [DOI] [PubMed] [Google Scholar]
- Mann JJ, Waternaux C, Haas GL, Malone KM. Toward a clinical model of suicidal behavior in psychiatric patients. Am J Psychiatry. 1999;156:181–189. doi: 10.1176/ajp.156.2.181. [DOI] [PubMed] [Google Scholar]
- Mann JJ, Apter A, Bertolote J, Beautrais A, Currier D, Haas A, Hegerl U, Lonnqvist J, Malone K, Marusic A, Mehlum L, Patton G, Phillips M, Rutz W, Rihmer Z, Schmidtke A, Shaffer D, Silverman M, Takahashi Y, Varnic A, Wasserman D, Hendin H. Suicide prevention strategies: A systematic review. JAMA. 2005;294:2064–2074. doi: 10.1001/jama.294.16.2064. [DOI] [PubMed] [Google Scholar]
- Maser JD, Akiskal HS, Schettler P, Scheftner W, Mueller T, Endicott J, Solomon D, Clayton P. Can temperament indentify affectively ill patients who engage in lethal or near-lethal suicidal behavior? A 14-year prospective study. Suicide Life Threat Behav. 2002;32:10–32. doi: 10.1521/suli.32.1.10.22183. [DOI] [PubMed] [Google Scholar]
- Mojtabai R, Olfson M, Mechanic D. Perceived need and help-seeking in adults with mood, anxiety or substance use disorders. Arch Gen Psychiatry. 2002;59:77–84. doi: 10.1001/archpsyc.59.1.77. [DOI] [PubMed] [Google Scholar]
- Nakagawa A, Grunebaum MF, Oquendo MA, Burke AK, Kashima H, Mann JJ. Clinical correlates of planned, more lethal suicide attempts, in major depressive disorder. J Affect Disord. 2009;112:237–242. doi: 10.1016/j.jad.2008.03.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oquendo MA, Brent DA, Birmaher B, Greenhill L, Kolko D, Stanley B, Zelazny J, Burke AK, Firinciogullari S, Ellis SP, Mann JJ. Posttraumatic stress disorder comorbid with major depression: Factors mediating the association with suicidal behavior. Am J Psychiatry. 2005;162:560–566. doi: 10.1176/appi.ajp.162.3.560. [DOI] [PubMed] [Google Scholar]
- Oquendo MA, Bongiovi-Garcia ME, Galfalvy H, Goldberg PJ, Grunebaum MF, Burke AK, Mann JJ. Sex differences in clinical predictors of suicidal acts after major depression: A prospective study. Am J Psychiatry. 2007;164:134–141. doi: 10.1176/appi.ajp.164.1.134. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oquendo MA, Currier D, Mann JJ. Prospective studies of suicidal behavior in major depressive and bipolar disorders: What is the evidence for predictive risk factors? Acta Psychiatr Scand. 2006;114:151–158. doi: 10.1111/j.1600-0447.2006.00829.x. [DOI] [PubMed] [Google Scholar]
- Oquendo MA, Friend JM, Halberstam B, Brodsky BS, Burke AK, Grunebaum MF, Malone KM, Mann JJ. Association of comorbid posttraumatic stress disorder and major depression with greater risk for suicidal behavior. Am J Psychiatry. 2003;160:580–582. doi: 10.1176/appi.ajp.160.3.580. [DOI] [PubMed] [Google Scholar]
- Oquendo MA, Galfalvy H, Russo S, Ellis SP, Gruenbaum MF, Burke A, Mann JJ. Prospective study of clinical predictors of suicidal acts after a major depressive episode in patients with major depressive disorder or bipolar disorder. Am J Psychiatry. 2004;161:1433–1441. doi: 10.1176/appi.ajp.161.8.1433. [DOI] [PubMed] [Google Scholar]
- Osby U, Brandt L, Correia N, Ekbom A, Sparen P. Excess mortality in bipolar and unipolar disorder in Sweden. Arch Gen Psychiatry. 2001;58:844–850. doi: 10.1001/archpsyc.58.9.844. [DOI] [PubMed] [Google Scholar]
- Placidi GP, Oquendo MA, Malone KM, Brodsky B, Ellis SP, Mann JJ. Anxiety in major depression: Relationship to suicide attempts. Am J Psychiatry. 2000;157:1614–1618. doi: 10.1176/appi.ajp.157.10.1614. [DOI] [PubMed] [Google Scholar]
- Ruan WJ, Goldstein RB, Chou SP, Smith SM, Tulshi DS, Pickering RP, Dawson DA, Huang B, Stinson FS, Grant BF. The Alcohol Use Disorder and Associated Disabilities Interview Schedule-IV (AUDADIS-IV): Reliability of new psychiatric diagnostic modules and risk factors in a general population sample. Drug Alcohol Depend. 2008;92:27–36. doi: 10.1016/j.drugalcdep.2007.06.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Roy A. Features associated with suicide attempts in depression: A partial replication. J Affect Disord. 1993;27:35–38. doi: 10.1016/0165-0327(93)90094-z. [DOI] [PubMed] [Google Scholar]
- Sareen J, Cox BJ, Afifi TO, deGraaf R, Asmundson GJG, ten Have M, Stein M. Anxiety disorders and risk for suicidal ideation and suicide attempts: A population-based longitudinal study of adults. Arch Gen Psychiatry. 2005b;62:1249–1257. doi: 10.1001/archpsyc.62.11.1249. [DOI] [PubMed] [Google Scholar]
- Séguin M, Lesage A, Guy A, Daigle F, Turecki G. Suicide cases in New Brunswick from April 2002 to May 2003: The importance of better recognizing substance and mood disorder comorbidity. Can J Psychiatry. 2006;51:581–586. doi: 10.1177/070674370605100906. [DOI] [PubMed] [Google Scholar]
- Shah BV, Barnswell BG, Bieler GS. SUDAAN user’s manual: Software for the analysis of correlated data. Release 6.40 ed. Research Triangle Park, NC: Research Triangle Institute; 1995. [Google Scholar]
- Sokero TP, Melartin TK, Rytsala HJ, Leskela US, Lestela-Melonen PS. Prospective study of risk factors for attempted suicide among patients with DSM-IV major depressive disorder. Br J Psychiatry. 2005;186:314–318. doi: 10.1192/bjp.186.4.314. [DOI] [PubMed] [Google Scholar]
- Sokero TP, Melartin TK, Rytsala HJ, Leskela US, Lestela-Melonen PS, Isometsa ET. Suicidal ideation and attempts among psychiatric patients with major depressive disorder. J Clin Psychiatry. 2003;64:1094–1100. doi: 10.4088/jcp.v64n0916. [DOI] [PubMed] [Google Scholar]
- Soloff PH, Lynch KG, Kelly TM, Malone KM, Mann JJ. Characteristics of suicide attempts of patients with major depressive episode and borderline personality disorder: A comparative study. Am J Psychiatry. 2000;157:601–608. doi: 10.1176/appi.ajp.157.4.601. [DOI] [PubMed] [Google Scholar]
- Stein MB, Fuetsch M, Muller N, Muller N, Hofler M, Lieb R, Wittchen HU. Social anxiety disorder and the risk of depression: A prospective community study of adolescents and young adults. Arch Gen Psychiatry. 2001;58:251–256. doi: 10.1001/archpsyc.58.3.251. [DOI] [PubMed] [Google Scholar]
- Suokas J, Suominen K, Isometsa E, Ostamo A, Lonqvist J. Long-term risk factors for suicide mortality after attempted suicide--Findings of a 14-year follow-up study. Acta Psychiatr Scand. 2001;104:117–121. doi: 10.1034/j.1600-0447.2001.00243.x. [DOI] [PubMed] [Google Scholar]
- Suominen K, Isometsa E, Suokas J, Haukka J, Achte K, Lonnqvist J. Completed suicide after a suicide attempt: A 37-year follow-up study. Am J Psychiatry. 2004;161:562–563. doi: 10.1176/appi.ajp.161.3.562. [DOI] [PubMed] [Google Scholar]
- Yen S, Shea MT, Pagano M, Sanislow CA, Grilo CM, McGlashan TH, Skodol AE, Bender DS, Zanarini MC, Gunderson JG, Morey LC. Axis I and II disorders as predictors of prospective suicide attempts: Findings from the Collaborative Longitudinal Personality Disorders Study. J Abnorm Psychol. 2003;112:375–381. doi: 10.1037/0021-843x.112.3.375. [DOI] [PMC free article] [PubMed] [Google Scholar]