Abstract
Hyponatremia is a common finding after subarachnoid hemorrhaging (SAH) and can be caused by either cerebral salt-wasting syndrome (CSWS) or syndrome of inappropriate antidiuretic hormone (SIADH). Distinguishing between these two entities can be difficult because they have similar manifestations, including hyponatremia, serum hypo-osmolality, and high urine osmolality. We herein report the case of a 60-year-old man who suffered from SAH complicated by hyponatremia. During his initial hospitalization, he was diagnosed with CSWS. He was readmitted one week later with hyponatremia and was diagnosed with SIADH. This is the first report of SAH causing CSWS followed by SIADH. These two different sources of hyponatremia require different treatments.
Keywords: hyponatremia, CSWS, SIADH
Introduction
Hyponatremia after subarachnoid hemorrhaging (SAH) is a common finding. It has been reported that over 50% of patients admitted for SAH develop hyponatremia (1-3). SAH-associated hyponatremia can be caused by excessive intravenous fluid therapy, diuretic therapy, cerebral salt-wasting syndrome (CSWS), and syndrome of inappropriate antidiuretic hormone (SIADH) (4). Both CSWS and SIADH cause hyponatremia by increasing renal excretion of sodium, and both are associated with serum hypo-osmolality and high urine osmolality (5-8). Kao et al. (9) and Hannon et al. (3) reported that SIADH is more likely to occur than CSWS (35.4% vs. 22.9%, 71.4% vs. 0%) in this patient population, yet CSWS has similar mortality rates and duration of hospital stay to SIADH.
CSWS is characterized by extracellular fluid volume depletion (1,10). The high urine sodium level observed in patients with CSWS is secondary to urine sodium wasting rather than volume expansion (11). Although the precise mechanism of salt wasting is poorly understood, several studies have begun to shed light on the pathophysiology of this disease. First, impaired sympathetic neural input to the juxtaglomerular apparatus may reduce proximal tubule sodium, urate, and water reabsorption and decrease renin and aldosterone release (12). Second, brain injury might increase the secretion of human atrial natriuretic peptide (hANP) and brain natriuretic peptide (BNP), leading to an increase in sodium excretion and urine volume (1,10,13).
In contrast, hyponatremia secondary to SIADH is a result of an excess of water rather than a deficiency of sodium. Excessive secretion of antidiuretic hormone (ADH) is caused by stimulation of the hypothalamus after trauma or ischemia. High levels of ADH increase water reabsorption in the distal convoluted renal tubule, causing fluid retention and dilutional hyponatremia (14,15).
Several factors may be useful in differentiating CSWS from SIADH. First, CSWS is characterized by volume depletion, while SIADH is not (5,16). However, the evaluation of extracellular fluid volume is notoriously difficult. Second, changes in uric acid homeostasis may provide clues to the cause of hyponatremia. In SIADH, the correction of serum sodium levels leads to normalization of uric acid levels. In contrast, in CSWS, hypouricemia and increased renal uric acid excretion persist after correction of serum sodium. Furthermore, the fractional excretion of uric acid (FEUA) is greater than 10% after correction of hyponatremia in CSWS but is less than 10% after correction of hyponatremia in SIADH (17).
It is important to distinguish between CSWS and SIADH in patients with hyponatremia because treatment of these two syndromes is very different. We herein report a case of CSWS followed by SIADH after SAH.
Case Report
A 60-year-old man was admitted to our hospital in February 2015. He had been in good health until 4 days prior to presentation, at which point he fell and developed SAH. He was initially admitted for 3 days for treatment of traumatic SAH. Two days following discharge, he developed a headache, nausea, thirst, and impaired consciousness, prompting readmission.
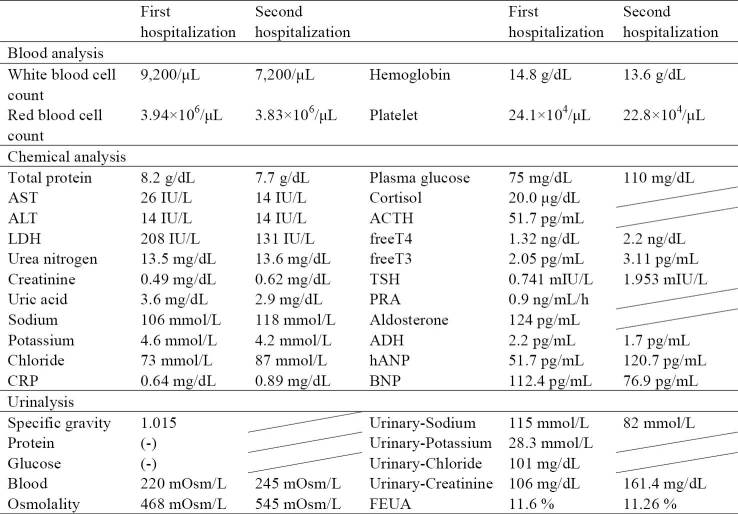
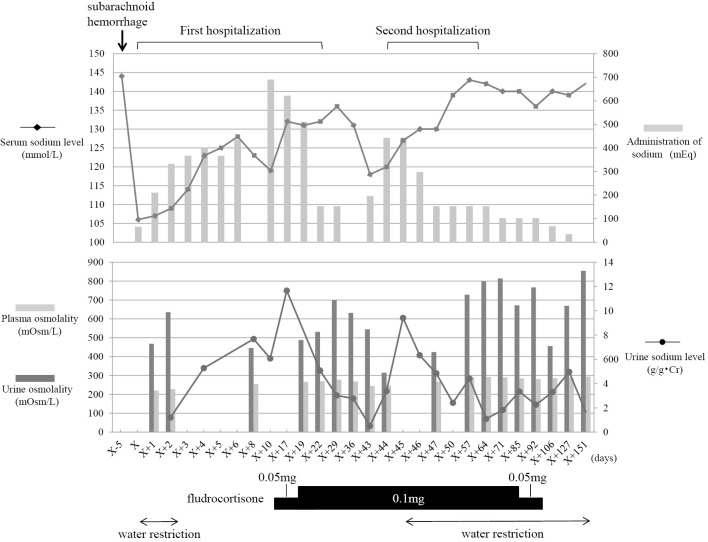
On admission, his Glasgow Coma Scale was 14 points (E4V4M6). His height was 160 cm, and body weight 60 kg. His blood pressure was 127/72 mmHg, pulse rate was 61 beats per minute, and oxygen saturation was 98% while breathing ambient air. His physical examination findings were unremarkable. Table 1 shows the results of blood and urine testing. The laboratory findings included marked hyponatremia (106 mmol/L), plasma hypo-osmolality (220 mOsm/L), urine hyper-osmolality (468 mOsm/L), and elevated urine sodium (115 mmol/L). His serum arginine vasopressin peptide (AVP) level was 2.2 pg/mL, and his serum creatinine, thyroid hormone, and adrenal cortical hormone levels were within normal limits. Although his physical examination findings were normal, he reported increased urination and excessive thirst. Furthermore, his inferior vena cava diameter was 8 mm on ultrasound, indicating volume depletion. He had no response to fluid restriction. Together, the data suggested a diagnosis of CSWS, and he was treated with sodium repletion (300 to 600 mEq daily). However, the serum sodium level did not improve (119 mmol/L), and he continued to excrete high levels of sodium. Starting on hospital day 10, he was treated with fludrocortisone (0.05 to 0.1 mg daily). Shortly thereafter, the serum sodium level gradually improved (135 mmol/L), and the urine sodium level decreased (Figure). The fractional excretion of uric acid was 11.9% after correction of hyponatremia, which is consistent with a diagnosis of CSWS. His symptoms improved and he was discharged on hospital day 37.
Table 1.
Laboratory Data during the First and Second Hospitalizations.
Figure.
Clinical course.
The patient returned 7 days after discharge with a new headache. His body weight was 61.5 kg. His blood pressure was 148/78 mmHg, and his pulse rate was 64 beats per minute. He was again noted to be hyponatremic (118 mmol/L) and was thus readmitted to our hospital. Similar to his prior hospitalization, laboratory tests revealed hypo-osmolality (245 mOsm/L), urine hyper osmolality (545 mOsm/L), and increased renal excretion of sodium (82 mmol/L). Serum AVP level was 1.7 pg/mL (Table 1). Serum creatinine and hormone levels were within normal limits. His physical examination findings were unremarkable, but unlike at his previous hospitalization, the diameter of his inferior vena cava was normal (14 mm) on ultrasound. He was initially treated with sodium repletion (300 to 400 mEq daily) and fludrocortisone (0.1 mg daily) but his serum sodium level did not improve. Together, these findings suggested a new diagnosis of SIADH. He was subsequently treated with fluid restriction (800 mL/day), and his serum sodium level improved (140 mmol/L, Figure). The fractional excretion of uric acid was 4.9% after correction of hyponatremia, which is consistent with a diagnosis of SIADH. His symptoms improved, and he was discharged 13 days after admission. He continued to do well over the next four months, requiring no additional hospitalizations or medications.
Discussion
It has been reported that hyponatremia in patients with central nervous system (CNS) diseases can be attributed to excessive fluid therapy, diuretic use, CSWS, or SIADH (8). Although CSWS and SIADH have similar laboratory findings, including hyponatremia, serum hypo-osmolality, and increased renal excretion of sodium, the pathophysiology and treatment of these syndromes are very different. Hyponatremia due to CSWS improves with fluid repletion and fludrocortisone, while hyponatremia due to SIADH improves with fluid restriction and vasopressin-2 receptor antagonists. Thus, the correct etiology of hyponatremia must be identified before starting the appropriate therapy.
CSWS is characterized by extracellular volume depletion, which stimulates ADH release (1,10). This is accompanied by increased production of hANP and BNP and impaired release of renin, despite fluid depletion. SIADH, which is characterized by excessive extracellular volume, causes similar changes in renin, hANP and BNP. Hence, changes in these serum markers cannot be used to differentiate CSWS from SIADH. Other factors may be more useful in differentiating these two syndromes, including extracellular volume status, changes in uric acid homeostasis, and response to fluid restriction. Table 2 shows the laboratory and physical findings during the patient's first and second hospitalizations, leading to the diagnoses of CSWS and SIADH.
Table 2.
Comparison of Laboratory Data from the First and Second Hospitalizations.
| Points in common | First hospitalization CSWS | Second hospitalization SIADH |
|---|---|---|
| Blood osmolality | 220 mOsm/L (low) | 245 mOsm/L (low) |
| Urine osmolality | 468 mOsm/L (high) | 545 mOsm/L (high) |
| ADH | 2.2 pg/mL (above detection sensitivity) | 1.7 pg/mL (above detection sensitivity) |
| Urinary sodium | 115 mmol/L (high) | 82 mmol/L (high) |
| Uric acid | 3.6 mg/dL (low) | 2.9 mg/dL (low) |
| hANP | 51.7 pg/mL (high) | 120.7 pg/mL (high) |
| BNP | 112.4 pg/mL (high) | 76.9 pg/mL (high) |
| Points of difference | ||
| Volume depletion | + | - |
| FEUA (after improvement of hyponatremia) |
11.9% (more than 10%) |
4.9% (less than 10%) |
| Reaction to fluid restriction | - (Na; 106 → 108 mmol/L) |
+ (Na; 120 → 140 mmol/L) |
For example, the fractional excretion of uric acid was greater than 10% after the correction of hyponatremia during the first hospitalization, but it was less than 10% during the second hospitalization (Table 1, 2). Furthermore, the response to fluid restriction differed between the first and second hospitalizations. The sensitivity and specificity of these findings for the diagnosis of CSWS and SIADH are unknown. Therefore, these differences may simply be diagnostic tools, rather than strict definitions of disease. Nonetheless, the data suggest that his initial presentation was consistent with CSWS and his second presentation was consistent with SIADH.
There are no previous reports suggesting that CSWS may transform into SIADH, and no reports of a temporal association between the two syndromes. The mechanisms underlying the two conditions in this case are uncertain. It is possible that SIADH occurred after CSWS had resolved. SIADH can occur hours to months after brain injury; our patient may therefore have suffered from late-onset SIADH, leading to the observed time difference between CSWS and SIADH (18). In our case, natriuretic factors such as ANP and BNP were initially increased by direct damage to the brain. Natriuretic factors would lead to a diminished activity of the renin-angiotensine-aldosterone system and increased natriuresis in the distal renal tubule (19). Treatment for CSWS may induce excessive secretion of ADH. Inappropriate secretion of ADH increases water reabsorption in the distal renal tubule, which is consistent with late-onset SIADH, resulting in increased natriuresis. It is also possible that the patient developed both syndromes simultaneously but that the laboratory findings during his first admission were most consistent with CSWS. After fluid therapy and fludrocortisone treatment, the CSWS resolved, revealing the residual SIADH. We might also need to consider how much the patient drank, particularly after the first hospital discharge, as excessive drinking can result in an excess of water, which would exacerbate SIADH. However, the patient did not consume a large amount of water at his home. He reported that he consumed 1 to 1.5 liters of water per day, which would not cause an excess of water. Without precise data on the amount he drank after the first hospital discharge, though, conclusions are difficult to make.
We herein report a rare case of CSWS and SIADH following SAH. Distinguishing between CSWS and SIADH may help prevent complications resulting from inappropriate treatment. This is particularly important in patients with hyponatremia and CNS diseases.
The authors state that they have no Conflict of Interest (COI).
References
- 1.Kurokawa Y, Uede T, Ishiguro M, et al. Pathogenesis of hyponatremia following subarachnoid hemorrhage due to ruptured cerebral aneurysm. Surg Neurol 46: 500-507, 1996. [DOI] [PubMed] [Google Scholar]
- 2.Sherlock M, O'Sullivan E, Agha A, et al. The incidence and pathophysiology of hyponatremia after subarachnoid hemorrhage. Clin Endocrinol 64: 250-254, 2006. [DOI] [PubMed] [Google Scholar]
- 3.Hannon MJ, Behan LA, O'Brien MM, et al. Hyponatremia following mild/moderate subarachnoid hemorrhage is due to SIAD and glucocorticoid deficiency and not cerebral salt wasting. J Clin Endocrinol Metab 99: 291-298, 2014. [DOI] [PubMed] [Google Scholar]
- 4.Marupudi NI, Mittal S. Diagnosis and management of hyponatremia in patients with aneurysmal subarachnoid hemorrhage. J Clin Med 4: 756-767, 2015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Milionis HJ, Liamis GL, Elisaf MS. The hyponatremic patient: a systematic approach to laboratory diagnosis. CMAJ 166: 1056-1062, 2002. [PMC free article] [PubMed] [Google Scholar]
- 6.Al-Mufti H. Hyponatremia due to cerebral salt-wasting syndrome: combined cerebral and distal tubular lesion. Am J Med 77: 740-746, 1984. [DOI] [PubMed] [Google Scholar]
- 7.Laville M, Burst V, Peri A, Verbalis JG. Hyponatremia secondary to the syndrome of inappropriate secretion of antidiuretic hormone (SIADH): therapeutic decision-making in real-life cases. Clin Kidney J 6: 1-20, 2013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Sterns RH, Silver SM. Cerebral salt wasting versus SIADH: what difference? J Am Soc Nephrol 19: 194, 2008. [DOI] [PubMed] [Google Scholar]
- 9.Kao L, Al-Lawati Z, Vavao J, Steinberg GK, Katznelson L. Prevalence and clinical demographics of cerebral salt wasting in patients with aneurysmal subarachnoid hemorrhage. Pituitary 12: 347-351, 2009. [DOI] [PubMed] [Google Scholar]
- 10.Isotani E, Suzuki R, Tomita K, et al. Alterations in plasma concentrations of natriuretic peptides and antidiuretic hormone after subarachnoid hemorrhage. Stroke 25: 2198-2203, 1994. [DOI] [PubMed] [Google Scholar]
- 11.Smith DM, McKenna K. Hyponatraemia. Clin Endocrinol 52: 667-678, 2000. [DOI] [PubMed] [Google Scholar]
- 12.Bitew S, Imbriano L, Miyawaki N, Fishbane S, Maesaka JK. More on renal salt wasting without cerebral disease: response to saline infusion. Clin J Am Soc Nephrol 4: 309-315, 2009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Berendes E, Walter M, Cullen P, et al. Secretion of brain natriuretic peptide in patients with aneurysmal subarachnoid haemorrhage. Lancet 349: 245-249, 1997. [DOI] [PubMed] [Google Scholar]
- 14.Fox JL, Falik JL, Schlhoub RJ. Neurosurgical hyponatremia: the role of inappropriate antidiuresis. J Neurosurg 34: 506-514, 1971. [DOI] [PubMed] [Google Scholar]
- 15.Cogan E, Debieve MF, Pepersack T, Abramow M. Natriuresis and atrial natriuretic factor secretion during inappropriate antidiuresis. Am J Med 84: 409-418, 1998. [DOI] [PubMed] [Google Scholar]
- 16.Maesaka JK, Miyawaki N, Palaia T, Fishbane S, Durham JH. Renal salt wasting without cerebral disease: diagnostic value of urate determinations in hyponatremia. Kidney Int 71: 822-826, 2007. [DOI] [PubMed] [Google Scholar]
- 17.Maesaka JK, Gupta S, Fishbane S. Cerebral salt-wasting syndrome: Does it exist? Nephron 82: 100-109, 1999. [DOI] [PubMed] [Google Scholar]
- 18.Ogasawara K, Kinouchi H, Nagamine Y. Cerebral salt wasting syndrome and SIADH. No Shinkei Geka 26: 501-505, 1998(in Japanese, Abstract in English).9635302 [Google Scholar]
- 19.Cerdà-Esteve M, Cuadrado-Godia E, Chillaron JJ, et al. Cerebral salt wasting syndrome: review. Eur J Intern Med 19: 249-254, 2008. [DOI] [PubMed] [Google Scholar]