Abstract
Introduction:
Phentolamine mesylate (OraVerse) is mostly used to reverse soft tissue anesthesia after dental procedures. The aim of the present study was to evaluate the effect of the injection of OraVerse on postoperative pain after root canal treatment in patients with symptomatic irreversible pulpitis.
Methods and Materials:
In this randomized single-blind clinical trial study, 100 patients (50 per group) with symptomatic irreversible pulpitis in the first or second mandibular molars, randomly received either OraVerse or sham treatment after a single-visit root canal therapy. Each patient recorded their pain score, using a Heft Parker visual analogue scale, before and after 6, 12, 24, 36, 48, and 72 h of the treatment. They also monitored their soft-tissue anesthesia every 15 min for 5 h. Data were analyzed by t-test and repeated measured ANOVA statistical tests. The level of significance was set at 0.05.
Results:
Patients who received phentolamine had significantly higher pain scores at 6- and 12-h postoperative intervals compared with those receiving sham treatment (P=0.01 and P=0.00 respectively). Consumption of analgesics in OraVerse group was significantly higher than that of the sham group (P=0.48).
Conclusion:
Although phentolamine accelerated the reversal of normal soft tissue sensation after the dental visit, it increased postoperative pain in patients suffering from symptomatic irreversible pulpitis, which may limit phentolamine administration in this group.
Key Words: Anesthesia, Inferior Alveolar Nerve, Lidocaine, Phentolamine Mesylate, Postoperative Pain
Introduction
Postoperative pain control -in endodontic procedures- might be challenging for both patients and practitioners [1]. Postoperative pain causes patient dissatisfaction, inconvenience and mistrust. Different strategies have been used to reduce postoperative pain [1-4]. Dental anesthesia results in soft-tissue anesthesia in addition to pulpal anesthesia. Numbness of soft-tissue lasts considerably more than pulpal anesthesia [4]. This unwanted prolonged soft-tissue anesthesia makes patients uncomfortable in aspects of physical appearance, diminished sensation and difficulties in routine functions such as speaking, eating, and drinking [5].
Phentolamine mesylate, known as OraVerse (Novalar Pharmaceuticals, Inc, San Diego, CA, USA), is a nonselective, α-adrenergic blocker with the primary action of vasodilation; which has been used to reverse soft tissue anesthesia [5-7]. It is injected using a standard dental syringe at the previous local anesthetic injection site. It provides vasodilation, which removes the anesthetic agents through increasing blood flow at the injection site [8]. Nevertheless, after the submucosal injection, phentolamine would be 100% available and reaches its peak concentration after 10-20 min. Also, the half-life of phentolamine is reported to be approximately 2-3 h in blood [5].
Several clinical studies revealed that phentolamine statistically reduced the duration of soft-tissue numbness [5-7, 9-11]. However, there is no study concerning the use of phentolamine in endodontic procedures; especially in patients encountering symptomatic teeth. The only observation on endodontic fields belongs to Fowler et al. [9] who investigated the administration of phentolamine after root canal therapy in asymptomatic teeth. That study resulted in faster return of soft-tissue to a normal sensation and function.
Benefits of the administration of phentolamine might be doubtful at the end of their endodontic appointment in such patients; because there is a significant relationship between pre- and post-endodontic pain [12, 13]. Hence, the aim of this prospective, randomized, single-blind study was to evaluate the postoperative pain and reversal of soft-tissue anesthesia after the injection of phentolamine mesylate; following root canal treatment in patients with symptomatic irreversible pulpitis in a mandibular molar.
Materials and Methods
Inclusion and exclusion criteria
One hundred patients, who were referred to Faculty of Dentistry, Isfahan University of Medical Sciences (Iran) from January to August 2015, enrolled in this study. The study design was conducted in full accordance with the World Medical Association Declaration of Helsinki. Torabinejad Research Center Committee (Isfahan University of Medical Sciences, Isfahan, Iran) approved the study with the ID number of 393116 (IRCT201512076578N33).
All participants were healthy adults (18 years and older; American society of anesthesiologists class I) as determined by a health history and oral questioning. Also, written informed consent was obtained from each patient. The exclusion criteria were: a) consumption of over-the-counter pain-relieving medications, narcotics, sedatives, anti-anxiety, or anti-depressant medications that might affect pain perception; b) allergy to phentolamine, local anesthetics; and c) any orofacial infection/inflammation or active pathosis at the injection site. Pregnant women and breast-feeding mothers were also excluded.
Each participant had a fully-formed, restorable, vital mandibular permanent molar with symptomatic pulpitis and normal periapical tissue. Molars with pain and prolonged response to the cold test (EndoIce, Hygenic Crop, Akron, Ohio, US) were diagnosed as symptomatic pulpitis. Patients with necrotic teeth [no response to the cold test or 2 consecutive response of 80 to electrical pulp test (EPT)] or partial necrotic molars (determined upon access cavity preparation), periradicular pathosis (other than a widened periodontal ligament), and with teeth sensitive to palpation or percussion were excluded. All the procedure, from diagnosis to complete treatment, was done by an expert endodontist in a blind manner.
Randomization
Sample size was calculated based on similar studies on anesthetic agents (n=50 in each group). On the day of the appointment, five-digit random number was written on papers by a third person who was not involved in the study, and each paper was kept in a separate sealed opaque envelope. Also, the appropriate five-digit random number was written on a label; which was placed on the syringe containing OraVerse or sham treatment (control group). Each patient randomly chose one of the envelopes and was assigned a five-digit random number indicating whether phentolamine solution or sham procedure had to be administered. Only the random number was used on the data collection sheets to further blind the experiment.
Study design
Topical anesthetic gel (20% benzocaine, Patterson Dental Supply Inc., MN, USA) was placed at the injection site for 60 sec using a cotton tip applicator. The inferior alveolar nerve block (IANB) was administered with 1.8 mL of 2% lidocaine and 1:100000 epinephrine (Xylocaine; Dentsply Pharmaceuticals Inc., York, PA, USA). A standard IANB was administered with a 27-gauge 1.5-inch needle (Monoject; Sherwood Services, MA, USA) over a period of 10 sec. Also, the long buccal nerve block was proceeded by 0.6 mL of the same local anesthetic agent.
Fifteen min after injection, the patient was questioned about lip numbness. If profound lip numbness was not obtained within 15 min, the block was considered missed, and the patient was excluded from the study. Meanwhile, the teeth were isolated with a rubber dam. Root canal preparation was performed in one visit. The working length was set at 1 mm shorter than the radiographic apex, and this was confirmed with an apex locator (Morita, Kyoto, Japan). Any teeth with an overestimated working length and over-instrumented or overfilled ones were excluded from the study. A 1.5% solution of sodium hypochlorite was used as an irrigant between each instrumentation. The root canals were instrumented using ProTaper Universal rotary instruments (Dentsply Maillefer, Ballaigues, Switzerland) up to F3 (30/0.09). The smear layer was removed by irrigating with 17% Ethylene diamine tetra acetic acid (EDTA)(Asia Chimi Teb, Tehran, Iran), followed by normal saline. The root canals were then dried and filled with gutta-percha and AH-26 (Dentsply De Tery, Konstanz, Germany) based on lateral condensation technique.
Interventions
Immediately following the treatment, and after rubber dam removal, the patients in OraVerse group received one cartridge (1.7 mL) of phentolamine mesylate (0.4 mg, OraVerse; Septodont Inc, Lancaster, England) at the same site as IANB injection. The cartridge of OraVerse was deposited over a 1-min time period using an aspirating syringe (Becton-Dickinson & Co., Ruther- ford, NJ, USA) equipped with a 27-G, 1.5 inch needle. For the patients assigned to the control (sham) group, a capped 27-G, 1.5 inch needle attached to an aspirating syringe pressed against the alveolar mucosa for 1 min without any soft tissue penetration. This strategy mimicked needle insertion, placement, and solution deposition [14].
Data collection and analysis
The time of the treatment was calculated in minutes. It started with the time when the anesthetic solution was injected, to the time when OraVerse or sham treatment were administered.
The patients were instructed to rate their pain on a Heft Parker visual analogue scale (VAS) in 2 phases: pre-treatment, and post-treatment at 6-, 12-, 24-, 36-, 48- and 72-h intervals after the endodontic treatment. The Heft-Parker VAS scale was divided into four categories. No pain corresponded as 0 mm. Mild pain was defined as greater than 0 mm and less than or equal to 54 mm. Moderate pain was defined as greater than 54 mm and less than 114 mm. Severe pain was defined as equal to or greater than 114 mm.
To evaluate the efficacy of soft-tissue anesthesia after using OraVerse, the patients were trained to accurately palpate the lip and tongue (mandible) on the side of injection. They washed their hands with soap and water before palpating, and palpated these areas every 15 min for 5 h after the treatment. They were asked to record their level of numbness; when a tingling sensation (pins and needles feeling) was present, or when a sensation recovery occurred (absence of pins-and-needles sensations).
Patients were given both verbal and written post-operative instructions. They were asked to consume analgesics; ibuprofen 400 mg with paracetamol 325 mg (Combiflam, Aventis Pharma, Anklesh- war, India), in case of necessity during post-operative period, and record the number of analgesic tablets on their VAS forms.
Statistical analysis
Data were collected in SPSS 20.0 (SPSS Inc., Chicago, IL, USA) for statistical analysis and subjected to t-test and repeated measured ANOVA at a significant level of 0.05.
Results
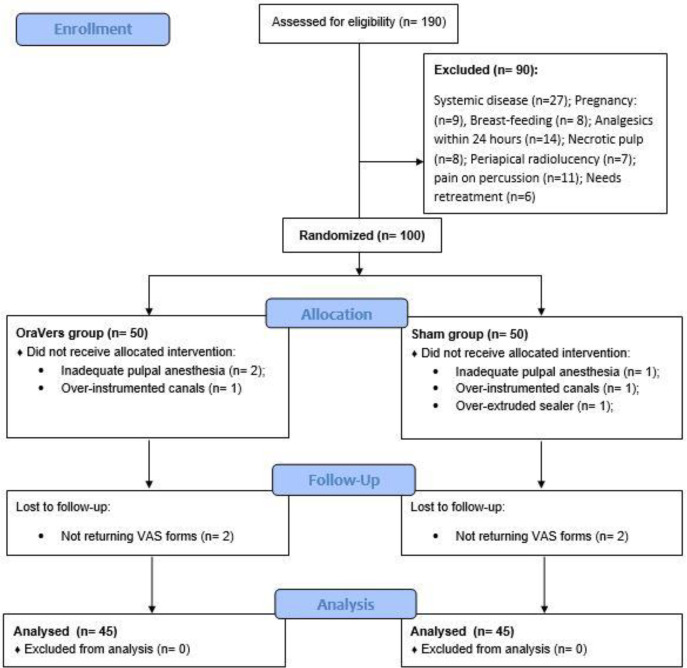
A total of 100 patients enrolled in this study. The data of 90 patients (49 males and 41 females) were used for statistical analysis (45 patients in each group). A total of 10 patients were excluded from the study because of the following reasons (Table 1): Inadequate pulpal anesthesia (3 patients; 1 female in the control group, 1 female and 1 male in the test group), over-instrumented canals (2 patients; 1 male in the control group, 1 female in the test group), Over-extruded root canal sealer through the apical foramen (1 female in the control group) and not returning VAS forms (4 patients; 2 males in the control group, 1 female and 1 male in the test group).
Table 1.
Demographic data of the test and control groups
| Value | OraVerse | Sham | P -Value |
|---|---|---|---|
| Age [Mean(SD)] | 30.42 (1.1) [18-48 yrs] | 28.16 (1.3) [20-52 yrs] | P=0.73 |
| Gender | 17 Females | 24 Females | P=0.78 |
| 28 Males | 21 Males |
Table 1 provides the general biographic and demographic data of the patients. There was no significant difference (P=0.73) between the two groups regarding their mean ages (30.42±1.1 years in OraVerse group, and 28.16±1.3 years in the sham group) based on the repeated measure analysis. In addition, no significant difference was found in gender and tooth type between OraVerse and sham groups (P=0.78 and P=0.16, respectively).
The mean procedure time for the clinical endodontic treatment was 73±1.4 min for OraVerse group and 71±2.1 min for the sham group. There were no statistical differences regarding the procedure time between two groups (P=0.35).
In the present study, there were no significant differences between OraVerse and sham groups considering the patients’ age, sex and initial pain. Mentioned variables did not have noticeable effects on the results between the two groups.
Based on t-test analysis, there were statistically significant differences in the time of reversal to the normal sensation for lip and tongue after IANB injection (P=0.00). Patients who received phentolamine experienced mandibular lip and tongue sensation after 120 and 103 min, respectively. In the sham group, patients experienced mandibular lip and tongue sensation after 152 and 174 min, respectively.
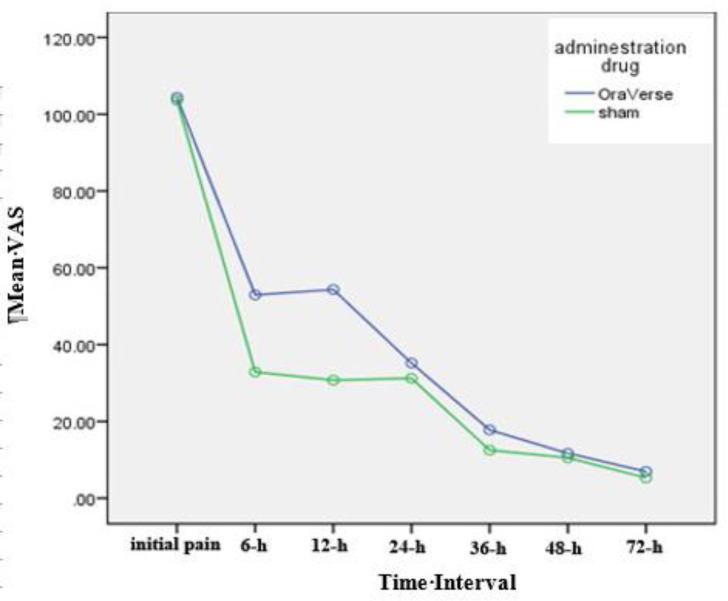
The mean intensity of pain before the treatment and 6, 12, 24, 36, 48 and 72 h after the endodontic treatment are illustrated in Figure 1. There were no significant differences between two groups regarding the mean intensity of initial pain before the endodontic treatment (P=0.81).
Figure 1.
The VAS data of the OraVerse and sham groups which illustrates the mean intensity of pain before the treatment and 6, 12, 24, 36, 48 and 72 h after endodontic treatment
The subjects who received phentolamine reported significantly higher post-operative pain levels after 6 and 12 h compared to the patients who received sham (P=0.01 and P=0.00, respectively). The mean intensity of pain was higher in OraVerse group at the other time intervals but showed no significant differences from the sham group (P>0.05).
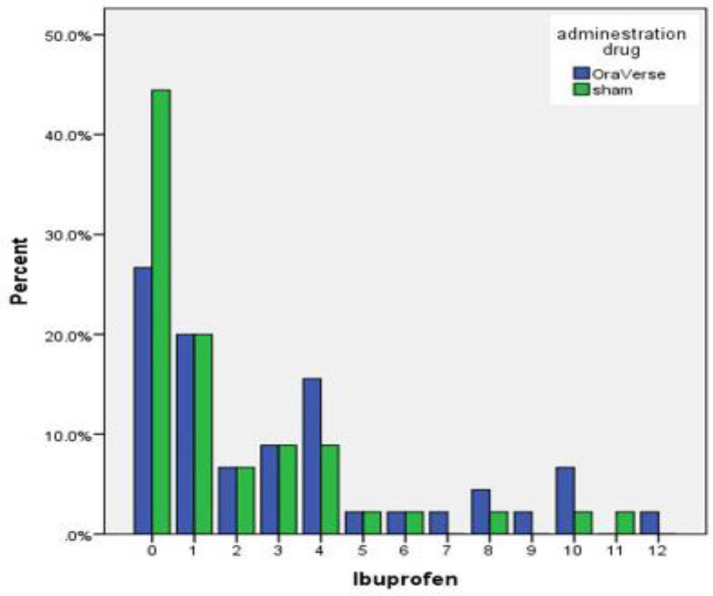
There were also no statistical relationships between age and sex with VAS at any time intervals. There were significant differences in the total of pain killer tablets consumed by the patients. Patients in OraVerse group consumed a total of 140 tablets, which were significantly higher than the 83 tablets used in the sham group (Figure 2).
Figure 2.
The number of analgesic tablets taken by patients in the OraVerse and sham groups during the first 72 h after root canal treatment
Discussion
The null hypothesis of this study was to observe no significant difference in the post-operative pain levels in patients with symptomatic irreversible pulpitis after administration of phentolamine compared with the control group.
Different scales have been introduced to measure pain severity. VAS consists of a line (usually 100 mm in length) with descriptors of ‘‘no pain’’ and “maximum possible pain” at each end [15]. It is simple and quick, and reproducible with validity [15, 16]. The Heft Parker VAS was used in the present study that consists of 4 categories of scales on a 170-mm VAS line. It is a combined scale using both advantages of VAS and verbal scale [17, 18].
The mean severity of initial pain ratings for patients in OraVerse group was 104 mm and mesh group on VAS score. This pain severity represented an irreversible pulpitis similar to other studies [17-19]. OraVerse group showed significantly higher short-term post-operative pain with higher total analgesics consumption.
All patients in this study had symptomatic teeth and were expected to experience more post-operative pain. Mattscheck et al. [20] described that patients, who had higher pretreatment pain, reported considerably increased post-treatment pain up to 24 h after receiving the endodontic treatment. Up to 80% of patients with pre-operative pain continued to report mild to severe pain after the endodontic treatment [21].
The pain was assessed during the first 72 h after the root canal treatment in our study, similar to the studies by Parirokh et al. [22], and Pak and White [23]; who claimed that most patients reported the highest post-operative pain levels in the first 3 days [23].
In the present study, the highest incidence of post-operative pain was at 6 h after the single-visit root canal treatment in both groups. However, the severity of pain in OraVerse group was significantly higher than that of the sham group. This could be related to the faster removal of the anesthetic effect of the block.
All the teeth in this study were treated in one appointment because the number of treatment visits might influence the post-operative pain after root canal therapy [25-26].
Figure 3.
Flowchart of the included patients into the study
In the present study, the patients were instructed to take ibuprofen and acetaminophen as analgesic medications in case of pain. Use of analgesics might have influenced the results, but there are several factors behind the design of the present study. First, ethical practice indicates that medications should be prescribed for patients if they feel pain [27]. Second, if patients, who received medication after treatment, had been excluded from the study, then the protocol would not have followed what typically happens in day-to-day clinical practice. Furthermore, one of the exclusion criteria was gastric diseases since ibuprofen was prescribed for all the patients to ensure that the same medication was used by all patients. This meant that the same effects would be experienced by all the patients, and the number of tablets could be compared for each group. Third, previous investigations have either prescribed or allowed patients to use medications if they felt pain; to evaluate the influence of either procedures or medications on pain [11, 28, 29].
In the present study, the sham treatment was also tested; because injecting a saline solution, as a control, would dilute the anesthetic solution at the site and affect the duration of soft-tissue anesthesia; which could cause invalid clinical results.
The mean VAS and severity of pain after the root canal treatment was less than the initial pain in both groups. This might be related to the removal of the etiological cause of pain which was inflamed pulp. In OraVerse group, after 6 and 12 h, the level of pain was significantly higher than the sham group. It could be due to the earlier return of the sensation in OraVerse group compared to the sham group. When sensation returns, the pain also returns. After 24 h, the level of pain was mild in both groups with no significant difference. After 48 and 72 h, the level of pain was similar in both groups.
Regarding the analgesic consumption, the percentage of patients who did not take any analgesicswere almost double in the sham group compared to OraVerse group. It shows that in the sham group, the level of pain was mild or less. In OraVerse group, the number of patients, who had taken 4 tablet, were almost double than the sham group; which is the indication of severity of pain in OraVerse group.
Considering VAS level of pain and the number of tablets taken by patients in both groups, we can conclude that patients in OraVerse group had more post-operative pain and thus, needed more analgesics than sham group.
Conclusion
Within the limitation of this study, (not being double-blind, using only one analgesic medication, etc.) it could be concluded that phentolamine was not beneficial for patients with symptomatic mandibular molar tooth. Although OraVerse fastened the return-to-normal soft-tissue function and sensation after the dental visit, it increased the post-operative pain in the symptomatic endodontic patients. Thus, administration of phentolamine for such patients ought to be limited.
Conflict of Interest:
‘None declared’.
References
- 1.El Mubarak AH, Abu-bakr NH, Ibrahim YE. Postoperative pain in multiple-visit and single-visit root canal treatment. J Endod. 2010;36(1):36–9. doi: 10.1016/j.joen.2009.09.003. [DOI] [PubMed] [Google Scholar]
- 2.De Oliveira GS Jr, Agarwal D, Benzon HT. Perioperative single dose ketorolac to prevent postoperative pain: a meta-analysis of randomized trials. Anesth Analg. 2012;114(2):424–33. doi: 10.1213/ANE.0b013e3182334d68. [DOI] [PubMed] [Google Scholar]
- 3.Nourbakhsh N, Shirani F, Babaei M. Effect of phentolamine mesylate on duration of soft tissue local anesthesia in children. J Res Pharm Pract. 2012;1(2):55–9. doi: 10.4103/2279-042X.108371. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Fernandez C, Reader A, Beck M, Nusstein J. A prospective, randomized, double-blind comparison of bupivacaine and lidocaine for inferior alveolar nerve blocks. J Endod. 2005;31(7):499–503. doi: 10.1097/01.don.0000167395.61075.38. [DOI] [PubMed] [Google Scholar]
- 5.Moore PA, Hersh EV, Papas AS, Goodson JM, Yagiela JA, Rutherford B, et al. Pharmacokinetics of lidocaine with epinephrine following local anesthesia reversal with phentolamine mesylate. Anesth Prog. 2008;55(2):40–8. doi: 10.2344/0003-3006(2008)55[40:POLWEF]2.0.CO;2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Hersh EV, Moore PA, Papas AS, Goodson JM, Navalta LA, Rogy S, et al. Reversal of soft-tissue local anesthesia with phentolamine mesylate in adolescents and adults. J Am Dent Assoc. 2008;139(8):1080–93. doi: 10.14219/jada.archive.2008.0311. [DOI] [PubMed] [Google Scholar]
- 7.Tavares M, Goodson JM, Studen-Pavlovich D, Yagiela JA, Navalta LA, Rogy S, et al. Reversal of soft-tissue local anesthesia with phentolamine mesylate in pediatric patients. J Am Dent Assoc. 2008;139(8):1095–104. doi: 10.14219/jada.archive.2008.0312. [DOI] [PubMed] [Google Scholar]
- 8.Prasanna JS. OraVerse: Reverses Numbness After Dental Procedures. J Maxillofac Oral Surg. 2012;11(2):212–9. doi: 10.1007/s12663-011-0318-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Fowler S, Nusstein J, Drum M, Reader A, Beck M. Reversal of soft-tissue anesthesia in asymptomatic endodontic patients: a preliminary, prospective, randomized, single-blind study. J Endod. 2011;37(10):1353–8. doi: 10.1016/j.joen.2011.06.019. [DOI] [PubMed] [Google Scholar]
- 10.Froum SJ, Froum SH, Malamed SF. The use of phentolamine mesylate to evaluate mandibular nerve damage following implant placement. Compend Contin Educ Dent. 2010;31(7):520, 2–8. [PubMed] [Google Scholar]
- 11.Laviola M, McGavin SK, Freer GA, Plancich G, Woodbury SC, Marinkovich S, et al. Randomized study of phentolamine mesylate for reversal of local anesthesia. J Dent Res. 2008;87(7):635–9. doi: 10.1177/154405910808700717. [DOI] [PubMed] [Google Scholar]
- 12.Praveen R, Thakur S, Kirthiga M. Comparative Evaluation of Premedication with Ketorolac and Prednisolone on Postendodontic Pain: A Double-blind Randomized Controlled Trial. J Endod. 2017 doi: 10.1016/j.joen.2016.12.012. [DOI] [PubMed] [Google Scholar]
- 13.Parirokh M, P VA. Various strategies for pain-free root canal treatment. Iran Endod J. 2014;9(1):1–14. [PMC free article] [PubMed] [Google Scholar]
- 14.Elmore S, Nusstein J, Drum M, Reader A, Beck M, Fowler S. Reversal of pulpal and soft tissue anesthesia by using phentolamine: a prospective randomized, single-blind study. J Endod. 2013;39(4):429–34. doi: 10.1016/j.joen.2012.12.024. [DOI] [PubMed] [Google Scholar]
- 15.Goddard G, Karibe H, McNeill C. Reproducibility of visual analog scale (VAS) pain scores to mechanical pressure. Cranio. 2004;22(3):250–6. doi: 10.1179/crn.2004.030. [DOI] [PubMed] [Google Scholar]
- 16.Averbuch M, Katzper M. Assessment of visual analog versus categorical scale for measurement of osteoarthritis pain. J Clin Pharmacol. 2004;44:4)368–72. doi: 10.1177/0091270004263995. [DOI] [PubMed] [Google Scholar]
- 17.Simpson M, Drum M, Nusstein J, Reader A, Beck M. Effect of combination of preoperative ibuprofen/acetaminophen on the success of the inferior alveolar nerve block in patients with symptomatic irreversible pulpitis. J Endod. 2011;37(5):57–93. doi: 10.1016/j.joen.2011.02.015. [DOI] [PubMed] [Google Scholar]
- 18.Oleson M, Drum M, Reader A, Nusstein J, Beck M. Effect of preoperative ibuprofen on the success of the inferior alveolar nerve block in patients with irreversible pulpitis. J Endod. 2010;36(3):379–82. doi: 10.1016/j.joen.2009.12.030. [DOI] [PubMed] [Google Scholar]
- 19.Matthews R, Drum M, Reader A, Nusstein J, Beck M. Articaine for supplemental buccal mandibular infiltration anesthesia in patients with irreversible pulpitis when the inferior alveolar nerve block fails. J Endod. 2009;35(3):343–6. doi: 10.1016/j.joen.2008.11.025. [DOI] [PubMed] [Google Scholar]
- 20.Mattscheck DJ, Law AS, Noblett WC. Retreatment versus initial root canal treatment: factors affecting posttreatment pain. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2001;92(3):321–4. doi: 10.1067/moe.2001.115135. [DOI] [PubMed] [Google Scholar]
- 21.Nixdorf DR, Law AS, Lindquist K, Reams GJ, Cole E, Kanter K, et al. Frequency, impact, and predictors of persistent pain after root canal treatment: a national dental PBRN study. Pain. 2016;157(1):159–65. doi: 10.1097/j.pain.0000000000000343. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Parirokh M, Yosefi MH, Nakhaee N, Manochehrifar H, Abbott PV, Reza Forghani F. Effect of bupivacaine on postoperative pain for inferior alveolar nerve block anesthesia after single-visit root canal treatment in teeth with irreversible pulpitis. J Endod. 2012;38(8):1035–9. doi: 10.1016/j.joen.2012.04.012. [DOI] [PubMed] [Google Scholar]
- 23.Pak JG, White SN. Pain prevalence and severity before, during, and after root canal treatment: a systematic review. J Endod. 2011;37(4):429–38. doi: 10.1016/j.joen.2010.12.016. [DOI] [PubMed] [Google Scholar]
- 24.Genet JM, Wesselink PR, Thoden van Velzen SK. The incidence of preoperative and postoperative pain in endodontic therapy. Int Endod J. 1986;19(5):221–9. doi: 10.1111/j.1365-2591.1986.tb00482.x. [DOI] [PubMed] [Google Scholar]
- 25.Su Y, Wang C, Ye L. Healing rate and post-obturation pain of single- versus multiple-visit endodontic treatment for infected root canals: a systematic review. J Endod. 2011;37(2):125–32. doi: 10.1016/j.joen.2010.09.005. [DOI] [PubMed] [Google Scholar]
- 26.Figini L, Lodi G, Gorni F, Gagliani M. Single versus multiple visits for endodontic treatment of permanent teeth: a Cochrane systematic review. J Endod. 2008;34(9):1041–7. doi: 10.1016/j.joen.2008.06.009. [DOI] [PubMed] [Google Scholar]
- 27.Rosner F. The ethics of randomized clinical trials. Am J Med. 1987;82(2):283–90. doi: 10.1016/0002-9343(87)90069-6. [DOI] [PubMed] [Google Scholar]
- 28.Heft MW, Parker SR. An experimental basis for revising the graphic rating scale for pain. Pain. 1984;19(2):153–61. doi: 10.1016/0304-3959(84)90835-2. [DOI] [PubMed] [Google Scholar]
- 29.Hersh EV, Hermann DG, Lamp CJ, Johnson PD, MacAfee KA. Assessing the duration of mandibular soft tissue anesthesia. J Am Dent Assoc. 1995;126(11):1531–6. doi: 10.14219/jada.archive.1995.0082. [DOI] [PubMed] [Google Scholar]
- 30.Hersh EV, Lindemeyer R, Berg JH, Casamassimo PS, Chin J, Marberger A, et al. Phase Four, Randomized, Double-Blinded, Controlled Trial of Phentolamine Mesylate in Two- to Five-year-old Dental Patients. Pediatr Dent. 2017;39(1):39–45. [PubMed] [Google Scholar]