Abstract
Study Design
Systematic review.
Objective
In patients with extradural metastatic spine disease, we sought to systematically review the outcomes and complications of patients with intermediate Spinal Instability Neoplastic Score (SINS) lesions undergoing radiation therapy, percutaneous interventions, minimally invasive surgeries, or open spinal surgeries.
Methods
Following PRISMA guidelines for systematic reviews, MEDLINE, EMBASE, Web of Science, the Cochrane Database of Systematic Reviews and the Cochrane Center Register of Controlled Trials were queried for studies that reported on SINS intermediate patients who underwent: 1) radiotherapy, 2) percutaneous intervention, 3) minimally invasive, or 4) open surgery. Dates of publication were between 2013-22. Patients with low- or high-grade SINS were excluded. Outcome measures were pain score, functional status, neurological outcome, ambulation, survival, and perioperative complications.
Results
Thirty-nine studies (n = 4554) were included that analyzed outcomes in the SINS intermediate cohort. Radiotherapy appeared to provide temporary improvement in pain score; however, recurrent pain led to surgery in 15%–20% of patients. Percutaneous vertebral augmentation provided improvement in pain. Minimally invasive surgery and open surgery offered improvement in pain, quality of life, neurological, and ambulatory outcomes. Open surgery may be associated with more complications. There was limited evidence for radiofrequency ablation.
Conclusion
In the SINS intermediate group, radiotherapy was associated with temporary improvement of pain but may require subsequent surgery. Both minimally invasive surgery and open spinal surgery achieved improvements in pain, quality of life, and neurological outcomes for patients with spine metastases. Open surgery may be associated with more complications.
Keywords: tumor, metastases, oncology, SINS, mechanical stability, surgery
Introduction
Treatment for spinal metastatic disease benefits from a multidisciplinary approach, often involving pain control, chemotherapy, radiotherapy (RT), percutaneous treatment and surgery. 1 Surgical indications for patients with spinal metastases include spinal instability, spinal cord or nerve root compression, and the need for circumferential tumor separation in preparation for stereotactic radiation, all of which can be achieved with an open approach.1-4 In recent years, the advancement of minimally invasive surgery (MIS) techniques including open kyphoplasty, open vertebroplasty, and mini-open procedures have been shown to decrease operative morbidity.1-4 Additionally, even less invasive procedures such as percutaneous kyphoplasty,5-7 vertebroplasty,5-7 and radiofrequency ablation are increasingly being employed as treatments.8,9
Mechanical stability is an important aspect in the treatment of spinal metastases. According to the NOMS framework (neurologic, oncologic, mechanical, systemic), mechanical instability represents an independent reason to operate, even without any epidural disease. The Spinal Instability Neoplastic Score (SINS) was developed by the Spine Oncology Study Group as a referral-based tool to identify patients who may require spinal stabilization prior to radiation or systemic chemotherapy treatment and was primarily meant for non-surgeons as a means of communication across specialties.10-13 SINS consists of 6 components, each scored separately from 0-2/3/4. A stable spine has a SINS of less than 7, while an unstable spine has a SINS of more than 12. A score between 7 to 12 is frequently labeled as intermediate stability, potentially unstable, or impending instability. The management of the SINS intermediate category is uncertain and remains controversial amongst clinicians,14-17 yet it remains critically important due to its prevalence.
Currently, there are limited studies examining treatment outcomes for SINS intermediate patients, and there are no reviews focusing on such outcomes among this specific patient population. We sought to conduct a systematic review regarding the treatment of SINS intermediate lesions to assess outcomes and complications from four possible treatment options: 1) radiation therapy, 2) percutaneous procedure, 3) minimally invasive surgery, and 4) open surgery.
Methodology
Search Strategy
Comprehensive and systematic electronic searches were conducted on October 3, 2022, and again on December 15, 2022 following the PRISMA guidelines. 18 The search was performed in the following databases: PubMed (MEDLINE), Cochrane Library databases (Wiley), Ovid Embase (Elsevier), Web of Science (Clarivate), Cochrane Central Register of Controlled Trials and Cochrane Database of Systematic Reviews. The search terms are included in Supplemental Table 1. This was supplemented with review of pertinent article bibliographies. Database-specific control vocabulary and keyboard terms related to SINS intermediate, spinal metastases, open spinal surgery and minimally invasive surgery were utilized. No language restriction was imposed, and the search date ranged from the inception of each database to the date of search. All references were uploaded to screening platform (Rayyan) and underwent deduplication. 19 The reference lists of retrieved articles that were reviewed independently by 3 investigators (ND, SZ, WCK) to identify studies systematically as per the search criteria. Due to the nature of the study, inform consent and Institutional Review Board approval was not necessary. All authors have been deemed exempt from these approvals.
Selection Criteria
A set of a priori inclusion and exclusion criteria was determined as follows: 1) full-length article (randomized, nonrandomized trials, and observational studies) in a peer-reviewed journal; 2) inclusion of the population of interest, specifically, patients with spinal metastases and SINS intermediate stability; 3) date of publication after the establishment of SINS intermediate criteria, 4) treatment ranging from nonsurgical (radiation therapy), percutaneous procedures, minimally invasive surgery, or open surgery; and 5) report of measurable or comparable outcomes. Exclusion criteria included: 1) review articles, meta-analyses, editorials, and opinion pieces; and 2) cohorts with less than 5 patients. Disagreements between the reviewers were resolved by discussion and consensus.
Data Extraction and Appraisal
Titles and abstracts were screened for potential relevance with successful articles undergoing full-text assessments. Data from selected articles were extracted and entered into a spreadsheet (Microsoft Excel). When appropriate, foreign language articles were reviewed by native speakers. Disagreements were reviewed and resolved by discussion and consensus.
Results
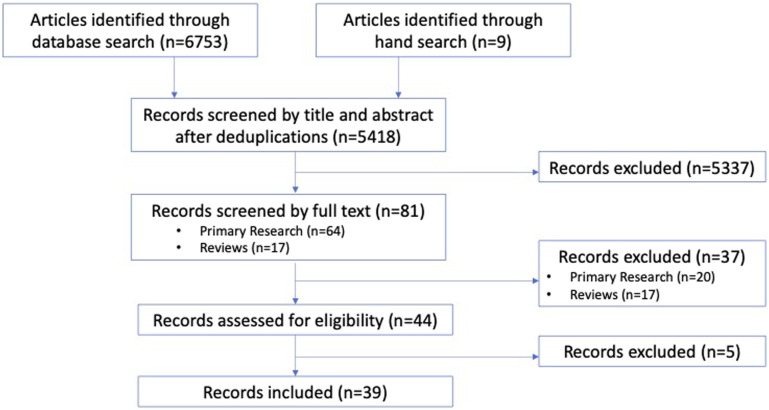
Our search yielded a total of 5481 studies after de-duplication. Title and abstract screening yielded 64 relevant primary research articles for full-text review, as well as 17 meta-analyses for reference. Forty-four articles met the inclusion criteria and were analyzed based on their discussion and analysis of SINS intermediate. Seven articles exclusively studied patients in the SINS intermediate category, and 13 articles studied patient in all SINS categories and performed analysis specific to the SINS intermediate category. Seventeen articles reported on SINS intermediate, but performed analysis by combining SINS intermediate and SINS unstable. These articles had more than 50% of their combined population in the SINS intermediate category and were included in our analysis. One article presented an averaged intermediate SINS with a confidence interval within the SINS intermediate category; this study was included in our analysis. 20 Two articles were excluded as they combined SINS intermediate and SINS unstable without a clear distribution of patients.21,22 Three articles were excluded as they presented averaged intermediate SINSs with a wide confidence interval, making their results uncertain to be applicable to the SINS intermediate category.23-25 A total of 39 articles were included in this review. A flowchart of the articles is presented in Figure 1 with an itemized summary of data collected in Table 1. Supplemental Table 2 illustrates the distribution of patients in SINS intermediate in each study included.
Figure 1.
Flowchart summarizing literature search and study selection process.
Table 1.
Itemized Summary of Articles Included in This Review With Details on Interventions and Outcomes Provided in Each Article.
| Author | Intervention | Pain | Neurology | HRQOL | Survival | VCF | Complication |
|---|---|---|---|---|---|---|---|
| Van der Velden 31 | Radiotherapy (RT) | Yes | |||||
| Huisman 29 | Radiotherapy | Yes | |||||
| Versteeg 30 | Radiotherapy | Yes | Yes | Yes | |||
| Versteeg 16 | Radiotherapy | Yes | Yes | ||||
| Germano 30 | Radiotherapy | Yes | Yes | Yes | |||
| Bollen 32 | Radiotherapy | Yes | Yes | ||||
| Lam 33 | Radiotherapy | Yes | |||||
| Sahgal 35 | Radiotherapy | Yes | Yes | ||||
| Lee 36 | Radiotherapy | Yes | Yes | ||||
| Shi 37 | Radiotherapy | Yes | Yes | ||||
| Sullivan 38 | RT vs RT + surgery | Yes | Yes | ||||
| Dial34,39 | RT vs RT + surgery | Yes | Yes | ||||
| Vargas 39 | RT+surgery | Yes | |||||
| Kim 40 | RT+surgery | Yes | |||||
| Dosani 41 | RT+surgery | Yes | |||||
| Park 44 | Percutaneous screw | Yes | Yes | Yes | |||
| Hem 26 | Percutaneous screw | Yes | Yes | Yes | |||
| Nakanishi 45 | Percutaneous screw | Yes | Yes | Yes | Yes | ||
| Silva 9 | Percutaneous screw | Yes | |||||
| Ragheb 9 | Radiofrequency ablation | Yes | Yes | Yes | |||
| Sebaaly 42 | Open vertebroplasty | Yes | Yes | Yes | |||
| Molloy 43 | Kyphoplasty | Yes | |||||
| Shao 20 | Vertebroplasty | Yes | |||||
| Ntilikina 47 | MIS vs open | Yes | Yes | Yes | |||
| Kumar 48 | MIS vs open | Yes | Yes | Yes | Yes | Yes | |
| Kumar 49 | MIS vs open | Yes | |||||
| Han 50 | Open surgery | Yes | Yes | Yes | Yes | ||
| Li 51 | Circumferential decompression and stabilization | Yes | Yes | Yes | Yes | Yes | |
| Cavalcante 52 | Circumferential decompression and stabilization | Yes | Yes | Yes | |||
| Masuda 53 | Posterior decompression and stabilization | Yes | Yes | Yes | |||
| Donnellan 54 | Vertebrectomy and stabilization | Yes | Yes | Yes | |||
| Wanman 55 | Open surgery | Yes | Yes | Yes | |||
| Zadnik 56 | Open surgery | Yes | |||||
| Barzilai 57 | Open surgery | Yes | |||||
| Chang 58 | Open surgery | Yes | |||||
| Pennington 17 | Instrumented fusion | Yes | |||||
| Hussain 28 | Open and MIS surgery | Yes | Yes | ||||
| Lenschow 14 | Instrumented fusion | Yes | Yes |
From the included articles, one article was written in Spanish and reviewed by a native Spanish orthopedics surgical resident. 26 Two articles provided separate analysis on the same group of patients as verified by the data in the patient characteristic table; their conclusions were combined for the analysis.27,28 One article analyzed a patient population that was a subset of a subsequent publication; the methodology and data presented were complementary.15,16
Radiotherapy
RT in SINS intermediate lesions were evaluated in 12 studies. As studies report either patient or lesions, these 12 studies include 1205 SINS intermediate patients in 8 studies, and 376 SINS intermediate lesions in 4 studies. Despite the heterogenous analysis of the studies, 5 reported on pain response following RT,15,16,29-31 three on spinal adverse events,32-34 and five on risk factors for development of vertebral compression fracture (VCF).30,32,35-37 No studies focused on neurological outcomes. Three studies compared outcomes in SINS intermediate between RT alone vs RT combined with surgery with a focus on health-related quality of life outcomes (HRQOL).15,16,38 One study exclusively analyzed outcomes in the SINS intermediate group between RT only in comparison to combined RT and surgery and combined RT and kyphoplasty. 34
Five studies, including 286 SINS intermediate patients (as reported in 4 studies) and 114 SINS intermediate lesions (as reported in 1 study), evaluated the relationship between SINS and response to RT based on patient-reported pain response.15,16,29-31 Patients experienced a significant temporary improvement in pain outcomes within 7 days following stereotactic body radiotherapy. 30 However, recurrence of pain in patients led to a non-significant pain response at 52 weeks.15,16,30 Three studies analyzed complications and adverse events though the definition of adverse events varied. Two studies, including 198 SINS intermediate patients, defined adverse events as the development of new pathologic fracture, progression of an existing pathologic fracture, or deterioration of alignment requiring surgical stabilization. The percentage of patients experiencing an adverse event that required retreatment was between 15%–20%.32,34 Another definition of adverse event included symptomatic vertebral fracture, hospitalization for site-related pain, salvage surgery or interventional procedure, new neurological symptoms or cord compression. 33 This study, including 173 SINS intermediate lesions, found that the cumulative incidence of adverse event ranged from 9% for multi-fraction RT to 24% for single-fraction RT by 180 days, emphasising that SINS ≥11 was a predictor of the incidence of adverse event.
Five studies, including 70 SINS intermediate patients and 176 SINS intermediate lesions, evaluated risk factors for VCF in patients undergoing RT.30,32,35-37 Identified risk factors included pre-existing VCF,30,35,36 severe pain,30,37 lesion location, 32 extensive vertebral body involvement, 35 lytic tumor,35,37 and spinal misalignment being components of the SINS classification. 35 In contrast, two multivariate analyses found no association with location, 37 extent of vertebral body involvement,32,37 lytic tumor 32 or spinal misalignment. 35
When comparing outcomes in SINS intermediate between RT alone vs RT combined with surgery, the current body of literature has one descriptive study and two comparative studies. A retrospective study analyzed 126 patients undergoing RT, of which 98 (78%) were SINS intermediate, and 109 patients undergoing surgery, of which 63 (61%) were SINS intermediate. 38 This analysis did not provide further outcome information on the SINS intermediate cohort. With a focus on HRQOL, Versteeg et al 15 compared patients with SINS intermediate score treated with RT alone (N = 84) or combined surgery and RT (N = 136). In the combined surgical and RT group, significant improvements in pain and HRQOL metrics were maintained up to 52-week following the treatments, while no significant changes were observed in the cohort treated with RT alone. Based on numeric rating scale (NRS) pain scores and the Spine Oncology Study Group Outcomes Questionnaire (SOSGOQ2.0), the combined surgical and RT cohort experienced a 3.0-point decrease in NRS pain score and a 12.7-point increase in SOSGOQ2.0 score. Meanwhile, the RT alone cohort experienced a 1.4-point decrease in NRS pain score and a 6.2-point increase in SOSGOQ2.0 score. Patients in the surgical group were noted to have mechanical back pain, lytic lesions and vertebral compression fractures. In a subsequent study that incorporated this aforementioned patient data, Versteeg et al 16 confirmed that the presence of mechanical pain on the SINS scale was demonstrated to be less responsive to RT and often required surgical intervention.
One comparative study analyzed 211 patients with SINS intermediate score divided into 3 treatment groups: external beam radiation therapy alone (EBRT, n = 57), surgery with EBRT (S + E, n = 128), and cement augmentation with EBRT (K + E, n = 27). 34 Dial et al 34 concluded that length of survival, maintenance of ambulation and revision treatment rates were all improved following surgical management and RT compared to RT alone. 34 The 1-year survivorship was 26%, 31%, and 60% for EBRT, K + E, and S + E respectively. The ambulatory status at death was 77%, 92%, and 91% for EBRT, K + E, and S + E respectively. The number of patients requiring revision were 26 (20.3%), 2 (7.4%), and 9 (15.8%) for EBRT, K + E, and S + E respectively. Patients in the EBRT group were the only ones requiring revision due to persistent pain, while patients in S + E were the only ones requiring revision due to deep infection. Other causes of revision included neurological symptoms for 7%, 7%, and 3% of EBRT, K + E, and S + E respectively. 34 The aforementioned study showed that a high percentage of RT only patients needed subsequent surgery. While addition of surgery or vertebral augmentation was associated with higher survival, though revision surgery was sometimes needed.
Since patients with a SINS intermediate score and significant mechanical pain or neurological symptoms often respond less favorably to nonoperative treatment, two studies have analyzed the risk factor for conversion to surgical treatment.39-41 These studies analyzed a combined 58 SINS intermediate patients undergoing surgical stabilization with 96 SINS intermediate patients undergoing nonoperative treatment. SINS >11 (OR 8.09, CI 1.96-33.4) and Karnofsky Performance Scale (KPS) score <60 (OR .94) were associated with an increased risk of salvage surgery. 39 With a conversion rate of about 33% from nonoperative to surgery, consideration for surgical treatment in patients with tumors in T3-T10 and even less than 50% of vertebral body collapse has been recommended. 40 No relationship between radiosensitivity of the tumor and conversion to surgery was found.
Percutaneous Interventions
Less invasive techniques such as radiofrequency ablation (RFA), vertebroplasty, and kyphoplasty have been shown to be effective alternatives for SINS intermediate patients. One study evaluated pain in patients undergoing RFA. 9 Two studies analyzed patient-related outcomes for pain, HRQOL and complications for closed balloon kyphoplasty.42,43 No studies for percutaneous vertebroplasty in SINS intermediate group was found.
A cohort of 23 females with metastatic breast cancer, all with SINS intermediate scores, underwent RFA with kyphoplasty. Significant reductions in pain levels were observed postoperatively, at discharge (Visual Analog Scale (VAS) = 3.5), at 1-month follow-up (VAS = 2.8), at 3-month follow-up (VAS = 1.1), and at 6-month follow-up (VAS = .7). However, this study did not have a control group and was combined with kyphoplasty. The authors recommended that the addition of RFA to kyphoplasty may reduce local tumor recurrence while providing similar pain relief benefits. 9
Two studies on balloon kyphoplasty, with a pooled 174 SINS intermediate patients, demonstrated that pain was significantly decreased in the postoperative period along with a reduction of up to 56% in analgesic and opioid dosage.42,43 Pain reduction was equally significant for patients with a posterior vertebral body wall (PVBW) deficit and patients with an intact PVBW. There were no new neurological complications reported. HRQOL was improved following treatment as measure by increase in EQ5D from .39 to .48 and decrease in Oswestry Disability Index Quality of life from 50 to 42. Length of stay averaged 2.6 days. The amount of bleeding reported in the studies were less than 20 mL and 100 mL. Complications reported in both studies included 64 cases (31%) of cement leakage; none of which led to neurological complications even in patients with PVBW defect. There were no reported cases of cardiovascular complications or infection. Out of 174 patients, one patient developed pulmonary embolism and another patient with pre-existing emphysema developed respiratory decompensation leading to death.
Minimally Invasive Surgery
Minimally Invasive Surgery (MIS), including percutaneous instrumentation, microscope assisted mini-open, open vertebroplasty and open kyphoplasty, has been analyzed by 8 studies including 333 SINS intermediate patients. Four studies reported on outcomes for percutaneous pedicle screw stabilization,26,44-46 with two studies reporting on pain scores,26,44 two on functional outcomes,44,45 four on ambulation and neurological outcomes,26,44-46 and three on perioperative complications.26,45,46 One study compared the outcomes in open vertebroplasty and kyphoplasty. 20 Two studies compared MIS and surgical outcomes for pain, neurology, survival, and perioperative complications.47,48 One final study also compared MIS and surgical outcomes with focus on construct failure. 49 The last three studies are discussed in a separate section.
Four studies including 117 SINS intermediate patients analyzed outcomes for percutaneous pedicle screw stabilization. All four studies reported their finding combining all SINS categories; SINS intermediate made up between 58%–83% of the study population, averaging 73% of the combined cohort. VAS scores improved from 8 to 2.75 with significant improvement on 77% of cases.26,44 Overall, 91.8% of patients experienced improvement in their Eastern Cooperative Oncology Group (ECOG) score postoperatively.44,45 Out of 117 patient, neurological recovery (Frankel grade) showed improvements between 16%–67% of cases, with two cases of neurological deterioration.44,46 Survival was reported between 8 to 22 months.44,45 Pooled perioperative complications for 149 patients included 1 case of paraplegia, 4 dural tears managed intraoperatively with no postoperative CSF leak, 3 implant failures, 4 cases of wound dehiscence, and 2 hematomas requiring revision surgery, 2 cases of UTI, and 2 cases of DVT.
In a study comparing open vertebroplasty (VP) and open kyphoplasty (KP) combined with open pedicle screw fixation, Shao et al 20 followed 55 patients with mean SINS of 10.93 +/− .99 and 11.25 +/− .97, respectively. The VAS score improved from 8.19 to 3.04 in the VP cohort, and from 8.36 to 2.68 in the KP cohort at their last follow-up at 1 year. No significant differences were found in surgery time, time from surgery to discharge, blood loss and complications between both groups postoperatively, suggesting either VP or KP can be utilised as treatment adjuvant for patients with spinal metastases undergoing open posterior instrumentation, including cases with posterior vertebral body wall (PVBW) defect.
Open Surgical Intervention
Open surgical decompression and stabilization has been a traditional strategy to address spinal instability and associated mechanical pain. Nine studies including 472 SINS intermediate patients analyzed outcome for patient undergoing surgery. Five studies (160 SINS intermediate patients) underwent spinal decompression and stabilization, while 4 studies (320 SINS intermediate patients) did not specify the surgical approach. From these 9 studies, three reported on pain scores,50-52 three on functional outcomes,50,51,53 five on neurological outcomes and ambulation,50,51,53-55 six on survival outcomes,51-56 and seven on complications.50-52,54-58 All nine studies reported their findings by combining all SINS categories with SINS intermediate compromising between 35%–83% of the study population, averaging 60% of all the patients in the studies.
Three studies focusing on pain scores included 88 SINS intermediate patients out of 163. They demonstrated statistically significant decreased in VAS scores postoperatively.50-52 A statistically significant correlation was found between severe preoperative pain (VAS 9-10) and unstable SINS, but not SINS intermediate. 52 Three separate studies, including 84 SINS intermediate patients out of 128 patients, showed significant improvement in European Organization for the Research and Treatment of Cancer Quality of Life Questionnaire, Karnofsky Performance Scale, and ECOG-PS scale.50,51,53 Five studies, including 244 SINS intermediate patients out of 372 patients, showed maintenance or improvement of Frankel grade.50,51,53,54 In a subgroup analysis, the ability to ambulate one month after surgery was statistically significantly improved in the SINS intermediate cohort compared with SINS unstable, while, and there was no statistically significant difference between the SINS intermediate and SINS unstable when analyzing ambulatory status before surgery and after surgery in a different subgroup analysis. 55 Six studies, including 245 SINS intermediate patients out of 425 patients showed the median survival for the SINS potentially unstable group ranged from 6.5 -28.1 months.51-56 Three studies showed no statistically significant difference in survival between SINS intermediate and unstable SINS categories,51,55,56 while two studies indicated a survival difference between SINS intermediate and unstable SINS.53,54 Seven studies reported on complications, but these complications could not be attributed to the SINS intermediate cohort specifically.50-52,54,55,57,58 Pooled complications for 670 patients include 3 cases of massive bleeding ≥3000 mL, 7 cases of wound dehiscence, 11 surgical site infections requiring surgical debridement, 2 DVT, 1 pulmonary embolism, 1 hematoma requiring surgical evacuation, 3 CSF leaks, and 2 cases of pneumonias. Additionally, there were 82 complications that were not described. 54
Comparing MIS and Open Surgery
Two studies, Kumar et al and Ntilikina et al, directly compared MIS techniques with open surgery, including 38 SINS intermediate patients in the MIS cohort of 51 patients and 38 SINS intermediate patient in the open surgery cohort of 53 patients.47,48 The analysis from both studies combined for all SINS categories with SINS intermediate accounting for 75% of the cohort across both studies. In terms of pain for the MIS cohort, the VAS improved from 5.8-7 to 1.9-1.8; in the open surgery cohort, VAS improved from 6-7 to 1.4-3.5. Ambulation was improved, but not significantly, 3-month post-surgery. Ambulation was impaired, or not possible, in 21%–59% of MIS patient and 27%–36% of open surgery patients. One study reported full normal function (Frankel grade E) was achieved in 88% of patients in the MIS group compared with 61% in the open group postoperatively. 48 A significant improvement in ECOG score was observed in postoperative period as compared with preoperative period in both groups, and the median survival was 7-7.5 months for the MIS cohort and 7-12 months for open surgery cohort. MIS procedures included less blood loss (184cc vs 961cc, respectively) and shorter time to radiation therapy (13 days vs 24 days, respectively). No difference was found in operating time, duration of hospital stays or time in ICU. The postoperative complication rate was equal in one study while higher in the open surgery group (16% vs 3%) in another study. 25 The MIS cohort reported 1 transfusion, one transient paralytic ileus, and 1 deep wound infection. The open surgery cohort reported 2 deep wound infection, four other infections, and 1 DVT. A separate study analyzing construct failure in MIS and open surgery, including 178 (72%) SINS intermediate patients, reported symptomatic failure in 4/49 patients in the MIS cohort and 10/194 in the open surgery cohort. Multivariate regression for all SINS patients showed that preoperative ECOG, preoperative ambulatory status, and junctional region lesions were predictive of construct failure.
Regrouping in SINS Intermediate
Given the paucity of guidelines in SINS intermediate cohorts, three studies with a combined 206 SINS intermediate patients, have suggested subdividing SINS 7-12 into two groups in which a lower SINS intermediate cohort would not require stabilization while a higher SINS intermediate cohort would benefit the spinal stabilization.17,27,39 The cut-off value for the SINS also varied; two studies suggested stabilization for SINS 10-12 while one study suggested stabilization for SINS 11-12. The modalities of stabilization in these studies were variable including percutaneous and open instrumentation and fusion. Following stabilization, patients in the higher SINS intermediate cohort exhibited greater improvement in pain and disability PRO scores compared to the lower SINS intermediate cohort; though the latter cohort also exhibited a statistically significant improvement in pain and disability PRO scores.
In contrast, one study found no evidence to support differentiating SINS 7-9 from SINS 10-12. Lenschow et al 14 studied 331 patients with SINS intermediate lesions and compared a decompression with instrumentation cohort vs a non-instrumented cohort undergoing radiation and vertebral augmentation. In a subgroup analysis for SINS intermediate patients, SINS 10-12 showed no significant difference between the instrumentation and non-instrumentation group in terms of neurological function at first examination, changes in their Frankel grade, or ambulatory status. Given the complications, the study suggested that a SINS intermediate score alone might not warrant spinal instrumentation. This is in contrast to Wanman et al 55 who advocated that patients from both SINS intermediate and SINS unstable would benefit equally from surgical decompression and possible instrumentation. This study found no statistically significant difference in the overall risk for death or in the risk of loss of ambulation 1 month after surgery between the SINS Intermediate and unstable categories.
Discussion
The current review summarizes outcomes and complications in the current literature for patients in the SINS intermediate group (SINS 7-12) undergoing one of the following treatments: 1) radiotherapy, 2) radiofrequency ablation, percutaneous vertebral augmentation, 3) minimally invasive decompression, percutaneous stabilization and 4) open surgical decompression or stabilization.
RT has been foundational in the treatment of symptomatic spinal metastases with effectiveness reported between 50%–80%.59,60 In the SINS intermediate patients undergoing RT, despite a temporary improvement in pain outcomes, recurrent pain requiring retreatment or surgery occurred in 15%–20% of patients. Alternatively, up to 85% of patients with SINS intermediate lesions won’t require additional treatment after RT alone, demonstrating that patient selection is crucial. Additionally, adverse events of patients treated with RT alone include symptomatic vertebral fractures, hospitalization for site-related pain, salvage surgery or interventional procedure, new neurological symptoms, or cord compression. These occurred more frequently in single-fraction RT than in multi-fraction RT. The risk factors for vertebral compression fracture after RT in SINS intermediate cohort include component location, extensive vertebral body involvement, lytic tumor, and spinal misalignment, which are components of the SINS. In contrast, other studies in the literature have shown that the total SINS is not predictive for new or progressive vertebral compression fractures (VCFs) in patients receiving high-dose stereotactic radiotherapy.61,62
When comparing RT alone with combined RT and surgery in SINS intermediate patients, pain scores and HRQOL were significant improved and maintain up to 52 weeks in the surgical group only. Additionally, there was improvement in 1-year survivorship and ambulatory status in the surgical group. These studies provide evidence to consider surgical intervention the SINS intermediate cohort, especially when mechanical pain is present. Some authors even advocated for more aggressive consideration for surgery in the T3-T10 location even when there is less than 50% of vertebral body collapse. 40
The evidence on radiofrequency ablation for SINS intermediate patients is limited, with one study showing significantly decreased in pain scores at 6-month 9 Similarly, there was only one study focused on open vertebroplasty and kyphoplasty including the SINS intermediate cohort. 20 Pain scores and HRQOL were improved with no new neurological complications, with similar outcomes in patient with and without a posterior vertebral body wall deficit.
When comparing MIS with open surgery, pain scores were improved in both MIS and open cohorts, but ambulation was not significantly improved in the MIS group. There was less blood loss and shorter time to radiation therapy in the MIS cohort, but no difference was found in operating time, duration of hospital stays or time in ICU. The postoperative complication rate was equal in one study while higher in the open surgery group in another study. There was no difference between open and MIS surgery in terms of pain changes, neurological function, or survival time in SINS intermediate patients. While there were no clear advantages of MIS over open surgery in this specific patient population, MIS have been shown to be associated with better AE profile in the metastatic spine population as a whole. 63 Limiting the surgical footprint in the oncological population is physiologically sound and should be promoted and further studied. It is unclear if subdividing SINS intermediate in 2 groups leads to any advantages in term of treatment recommendations.
Different treatment options are available for the heterogeneous clinical conditions related to spinal bone metastases, especially in the SINS intermediate cohort. Comprehensive and multi-disciplinary treatment must be individualized to the needs and goals of each patient and should also incorporate patient preferences. Nonoperative treatment like radiotherapy and radiofrequency ablation can provide temporary palliation and a good outcome in many patients, which may be the most appropriate option in some cases. The results of this systematic review should not be misinterpreted as a recommendation that surgery should be recommended for every patient in the SINS intermediate category. It should however be considered when mechanical pain is present. The SINS on its own was not designed to determine the need for surgery. As such, understanding which other clinical and radiological factors are associated with failure of nonoperative management in this patient population is an important knowledge gap. A range of surgical approaches may be required for others to maintain or improve the patient’s quality of life, offer more durable pain control, and maximize ambulatory capability. More comprehensive studies are needed to better understand the impact of various treatment options in different outcomes for the SINS intermediate cohort. As such, a meta-analysis of the papers presented in this study is underway to help bridge this knowledge gap.
Supplemental Material
Supplemental Material for What is the Optimal Management of Metastatic Spine Patients With Intermediate Spinal Instability Neoplastic Scores: To Operate or Not to Operate? by William Chu Kwan, MD, Scott L. Zuckerman, MD, Charles G. Fisher, MD, Ilya Laufer, MD, Dean Chou, MD, John E. O'Toole, MD, Markus Schultheiss, MD, Michael H. Weber, MD, PhD, Daniel M. Sciubba, MD, Markian Pahuta, MD, PhD, John H. Shin, MD, Michael G. Fehlings, MD, PhD, Anne Versteeg, MD, PhD, Matthew L. Goodwin, MD, Stefano Boriani, MD, Chetan Bettegowda, MD, PhD, Aron Lazary, MD, Alessandro Gasbarrini, MD, Jeremy J. Reynolds, MD, Jorrit-Jan Verlaan, MD, PhD, Arjun Sahgal, MD, Ziya L. Gokaslan, MD, Laurence D. Rhines, MD, and Nicolas Dea, MD, MSc, FRCSC in Global Spine Journal.
Supplemental Material for What is the Optimal Management of Metastatic Spine Patients With Intermediate Spinal Instability Neoplastic Scores: To Operate or Not to Operate? by William Chu Kwan, MD, Scott L. Zuckerman, MD, Charles G. Fisher, MD, Ilya Laufer, MD, Dean Chou, MD, John E. O'Toole, MD, Markus Schultheiss, MD, Michael H. Weber, MD, PhD, Daniel M. Sciubba, MD, Markian Pahuta, MD, PhD, John H. Shin, MD, Michael G. Fehlings, MD, PhD, Anne Versteeg, MD, PhD, Matthew L. Goodwin, MD, Stefano Boriani, MD, Chetan Bettegowda, MD, PhD, Aron Lazary, MD, Alessandro Gasbarrini, MD, Jeremy J. Reynolds, MD, Jorrit-Jan Verlaan, MD, PhD, Arjun Sahgal, MD, Ziya L. Gokaslan, MD, Laurence D. Rhines, MD, and Nicolas Dea, MD, MSc, FRCSC in Global Spine Journal.
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was organized and funded by AO Spine through the AO Spine Knowledge Forum Tumor, a focused group of international Tumor experts. AO Spine is a clinical division of the AO Foundation, which is an independent medically-guided not-for-profit organization.
Supplemental Material: Supplemental material for this article is available online.
ORCID iDs
William Chu Kwan https://orcid.org/0000-0001-6803-0669
Michael G. Fehlings https://orcid.org/0000-0002-5722-6364
Anne Versteeg https://orcid.org/0000-0003-3251-9694
Aron Lazary https://orcid.org/0000-0002-0157-719X
References
- 1.Benhabib H, Meirovich H, David E. Evolving role of minimally invasive techniques in the management of symptomatic bone metastases. Curr Opin Support Palliat Care. 2021;15(2):91-98. doi: 10.1097/SPC.0000000000000548. [DOI] [PubMed] [Google Scholar]
- 2.Flynn SC, Eli IM, Ghogawala Z, Yew AY. Minimally invasive surgery for spinal metastasis: a review. World Neurosurg. 2022;159:e32-e39. doi: 10.1016/j.wneu.2021.11.097. [DOI] [PubMed] [Google Scholar]
- 3.Papalexis N, Parmeggiani A, Peta G, Spinnato P, Miceli M, Facchini G. Minimally invasive interventional procedures for metastatic bone disease: a comprehensive review. Curr Oncol. 2022;29(6):4155-4177. doi: 10.3390/curroncol29060332. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Perna A, Smakaj A, Vitiello R, et al. Posterior percutaneous pedicle screws fixation versus open surgical instrumented fusion for thoraco-lumbar spinal metastases palliative management: a systematic review and meta-analysis. Front Oncol. 2022;12:884928. doi: 10.3389/fonc.2022.884928. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Yimin Y, Zhiwei R, Wei M, Jha R. Current status of percutaneous vertebroplasty and percutaneous kyphoplasty - a review. Med Sci Mon Int Med J Exp Clin Res. 2013;19(1):826-836. doi: 10.12659/MSM.889479. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.De la Garza-Ramos R, Benvenutti-Regato M, Caro-Osorio E. Vertebroplasty and kyphoplasty for cervical spine metastases: a systematic review and meta-analysis. Internet J Spine Surg. 2015;10. doi: 10.14444/3007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Sørensen ST, Kirkegaard AO, Carreon L, Rousing R, Andersen MØ. Vertebroplasty or kyphoplasty as palliative treatment for cancer-related vertebral compression fractures: a systematic review. Spine J. 2019;19(6):1067-1075. doi: 10.1016/j.spinee.2019.02.012. [DOI] [PubMed] [Google Scholar]
- 8.Senol N, Oguzoglu AS, Goksel HM. Radiofrequency ablation and augmentation in the management of spinal metastases: clinical experience in 41 patients. World Neurosurg. 2022;163:e420-e425. doi: 10.1016/j.wneu.2022.03.140. [DOI] [PubMed] [Google Scholar]
- 9.Ragheb A, Vanood A, Fahim DK. The addition of radiofrequency tumor ablation to kyphoplasty may reduce the rate of local recurrence in spinal metastases secondary to breast cancer. World Neurosurg. 2022;161:e500-e507. doi: 10.1016/j.wneu.2022.02.052. [DOI] [PubMed] [Google Scholar]
- 10.Fisher CG, Schouten R, Versteeg AL, et al. Reliability of the Spinal Instability Neoplastic Score (SINS) among radiation oncologists: an assessment of instability secondary to spinal metastases. Radiat Oncol. 2014;9(1):69. doi: 10.1186/1748-717X-9-69. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Fisher CG, Dipaola CP, Ryken TC, et al. A novel classification system for spinal instability in neoplastic disease: an evidence-based approach and expert consensus from the Spine Oncology Study Group. Spine (Phila Pa 1976). 2010;35, E1221-E1229. doi: 10.1097/BRS.0B013E3181E16AE2 [DOI] [PubMed] [Google Scholar]
- 12.Fourney DR, Frangou EM, Ryken TC, et al. Spinal instability neoplastic score: an analysis of reliability and validity from the spine oncology study group. J Clin Oncol. 2011;29(22):3072-3077. doi: 10.1200/JCO.2010.34.3897. [DOI] [PubMed] [Google Scholar]
- 13.Fisher CG, Versteeg AL, Schouten R, et al. Reliability of the spinal instability neoplastic scale among radiologists: an assessment of instability secondary to spinal metastases. AJR Am J Roentgenol. 2014;203(4):869-874. doi: 10.2214/AJR.13.12269. [DOI] [PubMed] [Google Scholar]
- 14.Lenschow M, Lenz M, von Spreckelsen N, et al. Impact of spinal instrumentation on neurological outcome in patients with intermediate spinal instability neoplastic score (SINS). Cancers. 2022;14(9):2193. doi: 10.3390/cancers14092193. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Versteeg AL, Sahgal A, Rhines LD, et al. Health related quality of life outcomes following surgery and/or radiation for patients with potentially unstable spinal metastases. Spine J. 2021;21(3):492-499. doi: 10.1016/j.spinee.2020.10.017. [DOI] [PubMed] [Google Scholar]
- 16.Versteeg AL, Sahgal A, Laufer I, et al. Correlation between the spinal instability neoplastic score (SINS) and patient reported outcomes. Global Spine J. 2023;13:1358-1364. doi: 10.1177/21925682211033591. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Pennington Z, Ahmed AK, Westbroek EM, et al. SINS score and stability: evaluating the need for stabilization within the uncertain category. World Neurosurg. 2019;128:e1034-e1047. doi: 10.1016/j.wneu.2019.05.067. [DOI] [PubMed] [Google Scholar]
- 18.Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372:n71. doi: 10.1136/bmj.n71. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A. Rayyan—a web and mobile app for systematic reviews. Syst Rev. 2016;5(1):210. doi: 10.1186/S13643-016-0384-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Shao X, Wu J, Zhou Z, et al. Bone cement and pedicle screw for the treatment of spinal tumors with spinal cord compression and posterior wall defects. Orthop Surg. 2022;14(8):1827-1835. doi: 10.1111/os.13316. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Aiba H, Kimura T, Yamagami T, et al. Prediction of skeletal-related events in patients with non-small cell lung cancer. Support Care Cancer. 2016;24(8):3361-3367. doi: 10.1007/S00520-016-3167-5/FIGURES/3. [DOI] [PubMed] [Google Scholar]
- 22.Xing D, Dong Z, Zheng X, et al. The protective effects of surgery according to the spinal instability neoplastic score for patients with the EGFR mutation, lung adenocarcinoma and spinal metastatic instability, 2019. https://www.ijcem.com/ [Google Scholar]
- 23.Telera S, Caroli F, Raus L, et al. Spine surgery in patients with metastatic breast cancer: a retrospective analysis. World Neurosurg. 2016;90:133-146. doi: 10.1016/j.wneu.2016.02.065. [DOI] [PubMed] [Google Scholar]
- 24.Telera S, Gorgoglione N, Raus L, et al. Open kyphoplasty for metastatic spine disease: a retrospective clinical series. World Neurosurg. 2019;127:e751-e760. doi: 10.1016/j.wneu.2019.03.258. [DOI] [PubMed] [Google Scholar]
- 25.Hubertus V, Gempt J, Mariño M, et al. Surgical management of spinal metastases involving the cervicothoracic junction: results of a multicenter, European observational study. Neurosurg Focus. 2021;50(5):E7-E9. doi: 10.3171/2021.2.FOCUS201067. [DOI] [PubMed] [Google Scholar]
- 26.Hem S, Beltrame S, Rasmussen J, Vecchi E, Landriel F, Yampolsky C. Usefulness of minimally invasive spine surgery for the management of thoracolumbar spinal metastases. Surg Neurol Int. 2019;10(2):S1-S11. doi: 10.4103/sni.sni_288_18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Hussain I, Barzilai O, Reiner AS, et al. Spinal Instability Neoplastic Score component validation using patient-reported outcomes. J Neurosurg Spine. 2019;30(4):432-438. doi: 10.3171/2018.9.SPINE18147. [DOI] [PubMed] [Google Scholar]
- 28.Hussain I, Barzilai O, Reiner AS, et al. Patient-reported outcomes after surgical stabilization of spinal tumors: symptom-based validation of the Spinal Instability Neoplastic Score (SINS) and surgery. Spine J. 2018;18(2):261-267. doi: 10.1016/j.spinee.2017.07.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Huisman M, Van Der Velden JM, Van Vulpen M, et al. Spinal instability as defined by the spinal instability neoplastic score is associated with radiotherapy failure in metastatic spinal disease. Spine J. 2014;14(12):2835-2840. doi: 10.1016/j.spinee.2014.03.043. [DOI] [PubMed] [Google Scholar]
- 30.Germano IM, Carai A, Pawha P, Blacksburg S, Lo YC, Green S. Clinical outcome of vertebral compression fracture after single fraction spine radiosurgery for spinal metastases. Clin Exp Metastasis. 2016;33(2):143-149. doi: 10.1007/S10585-015-9764-8. [DOI] [PubMed] [Google Scholar]
- 31.van der Velden JM, Versteeg AL, Verkooijen HM, et al. Prospective evaluation of the relationship between mechanical stability and response to palliative radiotherapy for symptomatic spinal metastases. Oncol. 2017;22(8):972-978. doi: 10.1634/theoncologist.2016-0356. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Bollen L, Groenen K, Pondaag W, et al. Clinical evaluation of the spinal instability neoplastic score in patients treated with radiotherapy for symptomatic spinal bone metastases. Spine (Phila Pa 1976). 2017;42(16):E956-E962. doi: 10.1097/BRS.0000000000002058 [DOI] [PubMed] [Google Scholar]
- 33.Lam TC, Uno H, Krishnan M, et al. Adverse outcomes after palliative radiation therapy for uncomplicated spine metastases: role of spinal instability and single-fraction radiation therapy. Int J Radiat Oncol Biol Phys. 2015;93(2):373-381. doi: 10.1016/J.IJROBP.2015.06.006. [DOI] [PubMed] [Google Scholar]
- 34.Dial BL, Catanzano AA, Esposito V, et al. Treatment outcomes in spinal metastatic disease with indeterminate stability. Global Spine J. 2022;12(3):373-380. doi: 10.1177/2192568220956605. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Sahgal A, Whyne CM, Ma L, Larson DA, Fehlings MG. Review Vertebral Compression Fracture after Stereotactic Body Radiotherapy for Spinal Metastases, 2013. https://www.thelancet.com/oncology [DOI] [PubMed] [Google Scholar]
- 36.Lee CH, Hong JT, Lee SH, et al. Reliable in predicting vertebral compression fractures for spinal metastasis? A systematic review and qualitative analysis. J Korean Neurosurg Soc. 2021;64(1):4-12. doi: 10.3340/jkns.2020.0105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Shi DD, Hertan LM, Lam TC, et al. Assessing the utility of the spinal instability neoplastic score (SINS) to predict fracture after conventional radiation therapy (RT) for spinal metastases. Pract Radiat Oncol. 2018;8(5):e285-e294. doi: 10.1016/J.PRRO.2018.02.001. [DOI] [PubMed] [Google Scholar]
- 38.Sullivan PZ, Albayar A, Ramayya AG, et al. Association of spinal instability due to metastatic disease with increased mortality and a proposed clinical pathway for treatment. J Neurosurg Spine. 2020;32:950-957. doi: 10.3171/2019.11.SPINE19775. [DOI] [PubMed] [Google Scholar]
- 39.Vargas E, Lockney DT, Mummaneni PV, et al. An analysis of tumor-related potential spinal column instability (Spine Instability Neoplastic Scores 7-12) eventually requiring surgery with a 1-year follow-up. Neurosurg Focus. 2021;50(5):E6-E7. doi: 10.3171/2021.2.FOCUS201098. [DOI] [PubMed] [Google Scholar]
- 40.Kim YH, Kim J, Chang SY, Kim H, Chang BS. Treatment strategy for impending instability in spinal metastases. Clin Orthop Surg. 2020;12(3):337-342. doi: 10.4055/cios20014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Dosani M, Lucas S, Wong J, et al. Impact of the spinal instability neoplastic score on surgical referral patterns and outcomes. Curr Oncol. 2018;25(1):53-58. doi: 10.3747/co.25.3835. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Sebaaly A, Najjar A, Wang Z, Boubez G, Masucci L, Shedid D. Anterolateral cervical kyphoplasty for metastatic cervical spine lesions. Asian Spine J. 2018;12(5):823-829. doi: 10.31616/ASJ.2018.12.5.823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Molloy S, Sewell MD, Platinum J, et al. Is balloon kyphoplasty safe and effective for cancer-related vertebral compression fractures with posterior vertebral body wall defects? J Surg Oncol. 2016;113(7):835-842. doi: 10.1002/jso.24222. [DOI] [PubMed] [Google Scholar]
- 44.Park HY, Lee SH, Park SJ, Kim ES, Lee CS, Eoh W. Minimally invasive option using percutaneous pedicle screw for instability of metastasis involving thoracolumbar and lumbar spine : a case series in a single center. J Korean Neurosurg Soc. 2015;57(2):100-107. doi: 10.3340/jkns.2015.57.2.100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Nakanishi K, Uchino K, Watanabe S, Misaki K, Iba H. Effect of minimally invasive spine stabilization in metastatic spinal tumors. Medicina (Lithuania). 2022;58(3):358. doi: 10.3390/medicina58030358. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Silva A, Yurac R, Guiroy A, et al. Low implant failure rate of percutaneous fixation for spinal metastases: a multicenter retrospective study. World Neurosurg. 2021;148:e627-e634. doi: 10.1016/j.wneu.2021.01.047. [DOI] [PubMed] [Google Scholar]
- 47.Ntilikina Y, Collinet A, Tigan LV, Fabacher T, Steib JP, Charles YP. Comparison of open versus minimally invasive surgery in the treatment of thoracolumbar metastases. Orthop Traumatol Surg Res. 2022;108(4):103274. doi: 10.1016/j.otsr.2022.103274. [DOI] [PubMed] [Google Scholar]
- 48.Kumar N, Malhotra R, Maharajan K, et al. Metastatic Spine Tumor Surgery A Comparative Study of Minimally Invasive Approach Using Percutaneous Pedicle Screws Fixation versus Open Approach; 2016. https://www.clinicalspinesurgery.com [DOI] [PubMed] [Google Scholar]
- 49.Kumar N, Patel R, Tan JH, et al. Symptomatic construct failure after metastatic spine tumor surgery. Asian Spine J. 2021;15(4):481-490. doi: 10.31616/asj.2020.0166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Han XX, Tao F, Wang GW, et al. Effect of combined treatment including surgery and postoperative adjuvant therapy on spinal metastases of Tomita type 7. Clin Neurol Neurosurg. 2019;181:112-118. doi: 10.1016/j.clineuro.2019.04.007. [DOI] [PubMed] [Google Scholar]
- 51.Li Z, Long H, Guo R, et al. Surgical treatment indications and outcomes in patients with spinal metastases in the cervicothoracic junction (CTJ). J Orthop Surg Res. 2018;13(1):20. doi: 10.1186/s13018-018-0732-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Cavalcante RAC, Fernandes YB, Marques RAS, et al. Is there a correlation between the spinal instability neoplastic score and mechanical pain in patients with metastatic spinal cord compression? A prospective cohort study. J Craniovertebr Junction Spine. 2017;8(3):187-192. doi: 10.4103/jcvjs.JCVJS_64_17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Masuda K, Ebata K, Yasuhara Y, Enomoto A, Saito T. Outcomes and prognosis of neurological decompression and stabilization for spinal metastasis: is assessment with the Spinal Instability Neoplastic Score useful for predicting surgical results? Asian Spine J. 2018;12(5):846-853. doi: 10.31616/ASJ.2018.12.5.846. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Donnellan CJ, Roser S, Maharaj MM, Davies BN, Ferch R, Hansen MA. Outcomes for vertebrectomy for malignancy and correlation to the spine instability neoplastic score (SINS): a 10-year single-center perspective. World Neurosurg. 2020;138:e151-e159. doi: 10.1016/j.wneu.2020.02.048. [DOI] [PubMed] [Google Scholar]
- 55.Wänman J, Jernberg J, Gustafsson P, et al. Predictive value of the spinal instability neoplastic score for survival and ambulatory function after surgery for metastatic spinal cord compression in 110 patients with prostate cancer. Spine (Phila Pa 2020). 2021;46(8):550-558. doi: 10.1097/BRS.0000000000003835. [DOI] [PubMed] [Google Scholar]
- 56.Zadnik PL, Hwang L, Ju DG, et al. Prolonged survival following aggressive treatment for metastatic breast cancer in the spine. Clin Exp Metastasis. 2014;31(1):47-55. doi: 10.1007/s10585-013-9608-3. [DOI] [PubMed] [Google Scholar]
- 57.Barzilai O, Versteeg AL, Goodwin CR, et al. Association of neurologic deficits with surgical outcomes and health-related quality of life after treatment for metastatic epidural spinal cord compression. Cancer. 2019;125(23):4224-4231. doi: 10.1002/cncr.32420. [DOI] [PubMed] [Google Scholar]
- 58.Chang SY, Ha JH, Seo SG, Chang BS, Lee CK, Kim H. Prognosis of single spinal metastatic tumors: predictive value of the Spinal Instability Neoplastic Score system for spinal adverse events. Asian Spine J. 2018;12(5):919-926. doi: 10.31616/ASJ.2018.12.5.919. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Lutz S, Berk L, Chang E, et al. Palliative radiotherapy for bone metastases: an ASTRO evidence-based guideline. Int J Radiat Oncol Biol Phys. 2011;79(4):965-976. doi: 10.1016/J.IJROBP.2010.11.026. [DOI] [PubMed] [Google Scholar]
- 60.Chow E, Harris K, Fan G, Tsao M, Sze WM. Palliative radiotherapy trials for bone metastases: a systematic review. J Clin Oncol. 2007;25(11):1423-1436. doi: 10.1200/JCO.2006.09.5281. [DOI] [PubMed] [Google Scholar]
- 61.Cunha MVR, Al-Omair A, Atenafu EG, et al. Vertebral compression fracture (VCF) after spine stereotactic body radiation therapy (SBRT): analysis of predictive factors. Int J Radiat Oncol Biol Phys. 2012;84(3):e343-e349. doi: 10.1016/J.IJROBP.2012.04.034. [DOI] [PubMed] [Google Scholar]
- 62.Sung SH, Chang UK. Evaluation of risk factors for vertebral compression fracture after stereotactic radiosurgery in spinal tumor patients. Korean J Spine. 2014;11(3):103-108. doi: 10.14245/KJS.2014.11.3.103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Zuckerman SL, Laufer I, Sahgal A, et al. When less is more: the indications for MIS techniques and separation surgery in metastatic spine disease. Spine (Phila Pa 1976). 2016;41(Suppl 20):S246-S253. doi: 10.1097/BRS.0000000000001824. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental Material for What is the Optimal Management of Metastatic Spine Patients With Intermediate Spinal Instability Neoplastic Scores: To Operate or Not to Operate? by William Chu Kwan, MD, Scott L. Zuckerman, MD, Charles G. Fisher, MD, Ilya Laufer, MD, Dean Chou, MD, John E. O'Toole, MD, Markus Schultheiss, MD, Michael H. Weber, MD, PhD, Daniel M. Sciubba, MD, Markian Pahuta, MD, PhD, John H. Shin, MD, Michael G. Fehlings, MD, PhD, Anne Versteeg, MD, PhD, Matthew L. Goodwin, MD, Stefano Boriani, MD, Chetan Bettegowda, MD, PhD, Aron Lazary, MD, Alessandro Gasbarrini, MD, Jeremy J. Reynolds, MD, Jorrit-Jan Verlaan, MD, PhD, Arjun Sahgal, MD, Ziya L. Gokaslan, MD, Laurence D. Rhines, MD, and Nicolas Dea, MD, MSc, FRCSC in Global Spine Journal.
Supplemental Material for What is the Optimal Management of Metastatic Spine Patients With Intermediate Spinal Instability Neoplastic Scores: To Operate or Not to Operate? by William Chu Kwan, MD, Scott L. Zuckerman, MD, Charles G. Fisher, MD, Ilya Laufer, MD, Dean Chou, MD, John E. O'Toole, MD, Markus Schultheiss, MD, Michael H. Weber, MD, PhD, Daniel M. Sciubba, MD, Markian Pahuta, MD, PhD, John H. Shin, MD, Michael G. Fehlings, MD, PhD, Anne Versteeg, MD, PhD, Matthew L. Goodwin, MD, Stefano Boriani, MD, Chetan Bettegowda, MD, PhD, Aron Lazary, MD, Alessandro Gasbarrini, MD, Jeremy J. Reynolds, MD, Jorrit-Jan Verlaan, MD, PhD, Arjun Sahgal, MD, Ziya L. Gokaslan, MD, Laurence D. Rhines, MD, and Nicolas Dea, MD, MSc, FRCSC in Global Spine Journal.