Abstract
AIM
To compare the subjective refraction data with auto-refraction findings in high astigmatisms.
METHODS
In a cross-sectional study, sampling was done from in different geographic regions in Iran using a multistage random cluster sampling method. All study participants underwent cycloplegic auto-refraction and subjective refraction using the red-green test.
RESULTS
In this study, 277 eyes of 158 students aged 8 to 15y were analyzed. According to the results, the mean difference between subjective refraction and autorefraction in measuring sphere, cylinder, spherical equivalent, J0, and J45 was -0.18±0.76, -0.36±0.40, -0.36±0.79, 0.15±0.20, and 0.05±0.21 respectively. The correlation of these two refraction methods in measuring the aforementioned indices was 0.963, 0.898, 0.960, 0.931, and 0.948 respectively. The 95% limits of agreement of the two methods in measuring the above indices were -1.66 to 1.31, -1.14 to 0.42, -1.91 to 1.19, -0.24 to 0.54, and -0.36 to 0.47 respectively. The agreement between the two methods decreased with increasing cylinder power, and the best agreement was found in myopic individuals.
CONCLUSION
The measurements obtained by autorefractometer have a significantly higher cylinder average compared to subjective refraction. However, in the cylinder range of 4–5 diopters, the values of J0 and J45 do not have a high correlation.
Keywords: subjective refraction, autorefraction, astigmatism
INTRODUCTION
Astigmatism is a common refractive error in the human eye[1]–[5]. According to a Meta-analysis, the prevalence of astigmatism in children and adults worldwide is 15.3% and 40.4%, respectively[4].
Studies have shown that high degrees of astigmatism during childhood (especially from infancy to school age) are associated with various disorders such as strabismus, myopia, and amblyopia[6]–[7]. Therefore, given the high prevalence of astigmatism, its timely diagnosis and determination of its characteristics and quality for timely correction are crucial[8]–[9]. Moreover, high degrees of astigmatism (2 D or more) are associated with important ocular diseases such as keratoconus[10]–[11].
To correct astigmatism, its severity and quality must first be accurately determined[12]–[14].
However, both subjective and objective methods (autorefractometer) are used today to investigate astigmatism in optometry and ophthalmology, with the autorefractometer providing accurate assessment of refractive error and the prescription of corrective glasses and contact lenses performed with the help of subjective refraction examinations[12]–[18].
In clinical settings, refractive examinations usually begin with objective examination and are followed by subjective examinations for the patient[19]. To date, studies evaluating the determination of axis of high astigmatism have not been comprehensive, and often these studies have only focused on a few subjective examinations. Additionally, many of these studies have only compared subjective examinations with each other and have not examined the value of subjective tests compared to objective examinations[15]–[16],[20].
Given the high dependence of visual acuity on the astigmatism axis in its high values, refraction requires very high accuracy, and the refractive error obtained will be incorrect if refraction is performed outside the visual axis. Since higher-order aberrations also affect the value and axis of astigmatism, it is sometimes difficult to obtain the correct refractive error in subjective refraction. So, practitioners rely on objective results in some situations. Subjective findings in corneal ectasi as may also be erroneous due to corneal irregularity[11]. For this reason, it seems important to examine the results of object and subjective refraction based on the severity of astigmatism. In view of the above, the present report aimed to evaluate the agreement between auto-refraction and subjective refraction in cases of astigmatism.
PARTICIPANTS AND METHODS
Ethical Approval
The study was conducted in accordance with the Helsinki Declaration. All procedures involving children were approved by the Ethics Committee of Shahid Beheshti University of Medical Sciences. We obtained written informed consent from all parents or students' legal guardians and also oral consent from all the students.
The present report is part of a cross-sectional study conducted in Iran. In this study, seven cities of Iran were randomly selected from different geographical locations using a multi-stage cluster sampling method. The selected cities were from different parts of Iran and the geographical and economic distribution was observed in the sampling. In each city (cluster), a number of boys' and girls' schools were randomly selected in equal numbers, and then all students in each school were selected for sampling. The major part of the sample were 7-year-old children (grade 1), some of whose reports have already been published[21]. In addition to 7-year-children, other school grades (children aged 8 to 15y) were also sampled, and their data were used in this report.
A suitable space was selected on the school site one day before the study. In each school, examinations were started with first graders, and students in each class were examined in alphabetical order.
Examinations
After the interview, students were guided into the examination room to have non-cycloplegic auto-refraction with the Topcon RM8800 autorefractor (Topcon Corporation, Japan) by a single skilled technician. Then, students had their visual acuity tested with their present spectacles, if any, using a Snellen E chart distanced at 6.0 m from the examinee. For these students, lensometry was done with the Topcon LM 800 lensometer (Topcon Corporation, Japan), results of which were recorded along with their prescription data. In the next step, uncorrected visual acuity (UCVA) was tested for all participants, and auto-readings results were refined through retinoscopy (HEINE BETA, Heine Optotechnik, Germany) and trial lenses (MSD, Italy). The lighting of the examination room was set according to the standard conditions. To ensure the accuracy of the measurements, the repeatability of visual acuity results was evaluated in a sample of 20 participants [intraclass correlation coefficient (ICC)=0.913].
The congruence between UCVA and objective refraction findings were used as a starting point for subjective refraction. The steps of subjective refraction included sphere power check, cylinder axis and cylinder power determination using Jackson cross-cylinder (JCC), and binocular balancing, respectively. Finally, cycloplegic refraction was tested with the autorefractometer and retinoscopy 35min after instilling cyclopentolate 1% eye drops twice in each eye with a 5-minute interval. If a significant difference between dry objective, subjective, and cycloplegic refractions was observed, subjective re-examination was performed the next day after removing the effect of cycloplegia. Schoolchildren with corrected visual acuity less than 20/25 and cylinder power better than 2 D were excluded from this study.
Statistical Analysis
The mean differences between autorefraction and subjective refraction of sphere, cylinder, spherical equivalent, J0, and J45 values were determined using paired t-test. Pearson correlation coefficients were used for showing the correlation between autorefraction and subjective refraction measurements of sphere, cylinder, spherical equivalent, J0, and J45.
The J0 vector is the horizontal and vertical components of astigmatism in each eye, and the J45 vector is the oblique component of astigmatism. These vectors were calculated using the following formulas:
J0=(-C/2) cos(2α)
J45=(-C/2) sin(2α)
Where C and α represent the magnitude and direction of cylindrical refraction, respectively.
To demonstrate inter-device agreement, Bland and Altman graphs with 95% limits of agreement (LoA) was used where horizontal and vertical axes indicated the average of a variable with two refraction and the inter-refraction difference for the variable, respectively.
The 95% LoA was calculated as “mean±1.96×standard deviation” of the inter-refraction difference.
RESULTS
In this study, 277 eyes from 158 patients were examined. Of this number, 97 (52.4%) were male, and the mean age of the participants was 12.71y with a standard deviation of 1.77y (age range: 8 to 15y). Table 1 preseted the mean sphere, cylinder, spherical equivalent, J0, and J45 values for each type of refraction with their mean difference and 95% LoA. As can be seen, there is a significant difference between the two methods in all these components.
Table 1. Comparison of autorefraction and subjective refraction in refractive error components.
| Refraction measurement | Autorefraction | Subjective refraction | Paired differences | P a | ICC | LoA |
| Sphere (D) | -0.57±2.68 | -0.40±2.35 | -0.18±0.76 | <0.001 | 0.963 | -1.66 to 1.31 |
| Cylinder (D) | -3.20±0.87 | -2.84±0.89 | -0.36±0.40 | <0.001 | 0.898 | -1.14 to 0.42 |
| Spherical equivalent (D) | -2.18±2.73 | -1.82±2.41 | -0.36±0.79 | <0.001 | 0.960 | -1.91 to 1.19 |
| J0 | 1.43±0.54 | 1.28±0.51 | 0.15±0.20 | <0.001 | 0.931 | -0.24 to 0.54 |
| J45 | 0.04±0.64 | -0.02±0.56 | 0.05±0.21 | <0.001 | 0.948 | -0.36 to 0.47 |
aPaired t-test. ICC: Intraclass correlation coefficient; SD: Standard deviation; LoA: Limit of agreement.
mean±SD
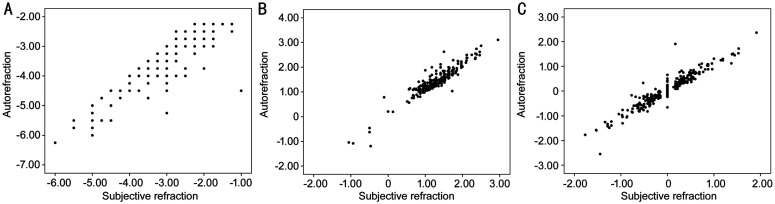
Figure 1 showed the correlation of the autorefraction and subjective refraction in cylinder, J0 and J45 measurement. As observed in Figures 1 and 2, there is a high correlation between the values of cylinder power, J0 and J45 based on autorefraction and subjective refraction. Figure 2 showed the Bland-Altman plot for the agreement of refraction measurements between the autorefraction and subjective refraction.
Figure 1. Scatter plot between subjective refraction and autorefraction measurements of the cylinder power (A), J0 (B), and J45 (C).
Figure 2. Agreement between subjective refraction and autorefraction measurements of the spherical error (A), cylinder power (B), spherical equivalent (C), J0 (D), and J45 (E).
The middle line indicates the mean difference and the two dashed side lines show the 95% limits of agreement.
Table 2 preseted the mean sphere, cylinder, spherical equivalent, J0, and J45 values for each type of measurement with their mean difference and 95% LoA according cylinder power severity.
Table 2. Comparison of autorefraction and subjective refraction in refractive error components according severity of astigmatism.
| Cylinder power | Refraction measurement | Autorefraction | Subjective refraction | Paired differences | P a | ICC | LoA |
| 2–3 diopter | Sphere (D) | -0.62±2.58 | -0.49±2.33 | -0.14±0.66 | 0.024 | 0.969 | -1.42 to 1.15 |
| Cylinder (D) | -2.47±0.21 | -2.14±0.34 | -0.33±0.29 | <0.001 | 0.541 | -0.89 to 0.23 | |
| Spherical equivalent (D) | -1.86±2.59 | -1.56±2.34 | -0.30±0.67 | <0.001 | 0.968 | -1.61 to 1.02 | |
| J0 | 1.09±0.39 | 0.94±0.38 | 0.15±0.16 | <0.001 | 0.915 | -0.16 to 0.46 | |
| J45 | 0.03±0.44 | -0.01±0.38 | 0.04±0.12 | <0.001 | 0.968 | -0.20 to 0.28 | |
| 3–4 diopter | Sphere (D) | -0.36±2.74 | -0.21±2.37 | -0.16±0.84 | 0.067 | 0.956 | -1.80 to 1.48 |
| Cylinder (D) | -3.34±0.30 | -3.04±0.43 | -0.30±0.33 | <0.001 | 0.644 | -0.95 to 0.34 | |
| Spherical equivalent (D) | -2.03±2.74 | -1.72±2.39 | -0.31±0.86 | <0.001 | 0.953 | -2.00 to 1.38 | |
| J0 | 1.53±0.27 | 1.40±0.3.0 | 0.13±0.17 | <0.001 | 0.836 | -0.19 to 0.46 | |
| J45 | 0.04±0.63 | 0.00±0.55 | 0.04±0.17 | 0.024 | 0.965 | -0.30 to 0.38 | |
| 4–5 diopter | Sphere (D) | -0.85±3.03 | -0.49±2.62 | -0.36±0.76 | 0.005 | 0.974 | -1.85 to 1.13 |
| Cylinder (D) | -4.27±0.27 | -3.76±0.67 | -0.51±0.65 | <0.001 | 0.278 | -1.79 to 0.76 | |
| Spherical equivalent (D) | -2.98±2.99 | -2.37±2.67 | -0.61±0.86 | <0.001 | 0.96 | -2.31 to 1.08 | |
| J0 | 1.85±0.57 | 1.68±0.44 | 0.17±0.28 | <0.001 | 0.879 | -0.37 to 0.72 | |
| J45 | 0.04±0.92 | -0.07±0.8 | 0.11±0.35 | 0.047 | 0.928 | -0.57 to 0.79 | |
| >5 diopter | Sphere (D) | -0.77±2.39 | -0.59±1.79 | -0.17±0.98 | 0.495 | 0.930 | -2.10 to 1.75 |
| Cylinder (D) | -5.39±0.40 | -4.83±0.65 | -0.56±0.55 | <0.001 | 0.535 | -1.64 to 0.52 | |
| Spherical equivalent (D) | -3.46±2.42 | -3.01±1.94 | -0.45±0.93 | 0.071 | 0.932 | -2.28 to 1.38 | |
| J0 | 2.43±0.46 | 2.22±0.36 | 0.21±0.35 | 0.027 | 0.667 | -0.47 to 0.90 | |
| J45 | 0.00±1.13 | -0.08±0.96 | 0.08±0.42 | 0.448 | 0.930 | -0.74 to 0.91 |
aPaired t-test. ICC: Intraclass correlation coefficient; SD: Standard deviation; LoA: Limit of agreement.
mean±SD
As shown in Table 2, the mean cylinder value obtained by autorefraction was significantly higher than that obtained by subjective refraction. In Table 2, it can be observed that in cylinder power severity, the values of cylinder, J0, and J45 are highly correlated with each other except for the cylinder range of 4–5 D. As seen in this table, the 95% LoA between the two methods become wider (less agreement) with increasing cylinder power.
Table 3 showed the paired comparison between the refraction values obtained by autorefraction and subjective refraction according refractive errors. In all types of refractive errors, the measured values were statistically significantly correlated (P<0.01).
Table 3. Comparison of autorefraction and subjective refraction in refractive error components according refractive errors.
| Refractive errors | Refraction measurement | Autorefraction | Subjective refraction | Paired differences | P a | ICC | LoA |
| Emmetropia | Sphere (D) | 1.43±0.61 | 1.08±0.59 | 0.36±0.38 | <0.001 | 0.805 | -0.38 to 1.09 |
| Cylinder (D) | -3.14±1.01 | -2.68±0.84 | -0.46±0.39 | <0.001 | 0.925 | -1.23 to 0.31 | |
| Spherical equivalent (D) | -0.14±0.35 | -0.26±0.42 | 0.13±0.29 | 0.078 | 0.730 | -0.45 to 0.70 | |
| J0 | 1.41±0.44 | 1.24±0.40 | 0.16±0.27 | 0.018 | 0.803 | -0.37 to 0.69 | |
| J45 | -0.09±0.76 | -0.07±0.53 | -0.03±0.3 | 0.695 | 0.956 | -0.61 to 0.55 | |
| Myopia | Sphere (D) | -1.32±2.03 | -1.03±1.79 | -0.29±0.76 | <0.001 | 0.930 | -1.78 to 1.19 |
| Cylinder (D) | -3.22±0.88 | -2.87±0.91 | -0.35±0.41 | <0.001 | 0.895 | -1.16 to 0.45 | |
| Spherical equivalent (D) | -2.93±2.08 | -2.46±1.85 | -0.47±0.8 | <0.001 | 0.923 | -2.04 to 1.10 | |
| J0 | 1.44±0.53 | 1.29±0.52 | 0.15±0.20 | <0.001 | 0.931 | -0.24 to 0.53 | |
| J45 | 0.04±0.66 | -0.01±0.58 | 0.06±0.21 | <0.001 | 0.950 | -0.35 to 0.47 | |
| Hyperopia | Sphere (D) | 4.41±2.45 | 3.96±2.33 | 0.44±0.48 | <0.001 | 0.981 | -0.49 to 1.38 |
| Cylinder (D) | -3.08±0.76 | -2.74±0.68 | -0.34±0.25 | <0.001 | 0.945 | -0.84 to 0.15 | |
| Spherical equivalent (D) | 2.87±2.46 | 2.59±2.32 | 0.27±0.44 | 0.003 | 0.985 | -0.58 to 1.13 | |
| J0 | 1.42±0.64 | 1.26±0.56 | 0.16±0.15 | <0.001 | 0.977 | -0.13 to 0.45 | |
| J45 | 0.05±0.33 | -0.02±0.31 | 0.07±0.12 | 0.006 | 0.934 | -0.17 to 0.30 |
aPaired t-test. ICC: Intraclass correlation coefficient; SD: Standard deviation; LoA: Limit of agreement.
mean±SD
DISCUSSION
The present study is one of the few studies that have investigated the difference in axis of high astigmatism (two diopters and above) in refractive examinations using autorefractometer and subjective refraction. In this study, astigmatism was differentiated based on J0 and J45 vectors.
Comparison of auto-refraction with subjective refraction shows that auto-refraction estimates astigmatism by an average 0.36 D higher than subjective refraction. Although this value is not clinically significant, given that the average is affected by extreme small and large data values, the standard deviation of this average and the LoA of the two methods should be considered. As seen, the wide LoA (from -1.14 to 0.42) suggests that the agreement between the two methods is low in cylinder measurement.
In a study by Kozlov et al[16], there was a significant statistical difference in spherical equivalent and cylindrical power values between the two methods. Like us, they showed that the auto-refractometer measures astigmatism about 0.23 D higher than the subjective refraction. Hashemi et al[15] also found that the measurement of astigmatism with auto-refraction is estimated to be at least 0.21 D higher than the subjective refraction in normal and cataractous individuals. Since our study participants had high astigmatism, the difference between the two refraction methods in our study is slightly higher than in other studies.
According to our findings, the best agreement between the two methods was obtained in individuals with myopic refractive errors, which may be attributed to the active matching involvement in hyperopes.
As seen in the Bland-Altman plots, there was a proportion bias in the sphere agreement between the two methods of auto-refraction and subjective refraction, so that in myopes, auto-refraction yielded more negative values. In children, although gold standard is standard cycloplegic refraction[22]–[23], there is a possibility of accommodation even under cycloplegia which is caused by stimulation of convergence. The basis for subjective refraction is to achieve maximum visual acuity with a minimum minus lens (maximum plus lens). Therefore, despite the fact that less myopia (more hyperopia) is expected in the cycloplegic refraction, the cyclorefraction values were more negative as a constant bias.
We examined the difference between the two methods in astigmatism values in different refractive error groups and found that in different refractive error ranges, the values of cylinder and J0 and J45 in all ranges except for 4–5 D of cylinder, astigmatism values have high correlation. The difference between the two methods was above 4 D, which could be due to higher error rates in myopes and hyperopes in autorefractometer due to lack of active matching control. According to a cohort study conducted by Vesely et al[19] in 2019, all subjective and objective methods are statistically sufficient for detecting astigmatism above 2 D; however, in our study, there was a significant difference between autorefraction and subjective refraction in cases of astigmatism above 4–5 D. Therefore, our results were not consistent with their findings. This may be due to differences in sample size or age group, as our sample size was much larger and our age range was broader.
Since the two methods have a statistically significant difference but clinically insignificant and have a high correlation and good agreement, they can be used interchangeably. However, in cases of astigmatism above 4 D, caution is needed and the subjective method is more important and has a significant difference with autorefraction.
In addition to comparing the spherical values, the spherical equivalent values were also compared and it was found that there is a statistically significant difference but not a clinically significant difference. In a similar study[16], the equivalent values of autorefractometer and subjective refraction had differences which may be due to the different types of methods used and the level of patient cooperation.
In addition to the spherical and spherical equivalent values, the cylindrical values were compared in terms of J0 and J45 vectors. As seen in the results, the vertical and horizontal astigmatism components showed statistically significant differences between the two measurement devices. The greatest difference was found in J0 for astigmatisms that are in line with the rule.
In conclusion, based on the findings of this study, there is no significant correlation between autorefractometer and subjective methods in astigmatism values of 4–5 D. Therefore, optometrists and ophthalmologists should exercise caution when using autorefractometer in studies and screenings within this diopter range, as well as in cases where individuals with disabilities, children, and those who do not have good cooperation with the device.
Footnotes
Foundation: Supported by Shahid Beheshti University of Medical Sciences.
Conflicts of Interest: Kangari H, None; Hashemi H, None; Rahmani S, None; Ahmadian E, None; Yekta A, None; Khabazkhoob M, None.
REFERENCES
- 1.Kanclerz P, Bazylczyk N, Lanca C. The prevalence of astigmatism and spectacle wear in Polish schoolchildren. J Binocul Vis Ocul Motil. 2023;73(4):124–130. [PubMed] [Google Scholar]
- 2.Valluru G, Klawe J, Liu B, et al. Characterizing astigmatism in the United States. J Cataract Refract Surg. 2022;48(5):519–527. doi: 10.1097/j.jcrs.0000000000000786. [DOI] [PubMed] [Google Scholar]
- 3.Hashemi H, Asharlous A, Yekta A, et al. Astigmatism profile in the elderly population: Tehran geriatric eye study. Jpn J Ophthalmol. 2022;66(5):461–473. doi: 10.1007/s10384-022-00936-x. [DOI] [PubMed] [Google Scholar]
- 4.Hashemi H, Fotouhi A, Yekta A, et al. Global and regional estimates of prevalence of refractive errors: systematic review and meta-analysis. J Curr Ophthalmol. 2018;30(1):3–22. doi: 10.1016/j.joco.2017.08.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Fotouhi A, Hashemi H, Ali Yekta A, et al. Characteristics of astigmatism in a population of schoolchildren, dezful, Iran. Optom Vis Sci. 2011;88(9):1054–1059. doi: 10.1097/OPX.0b013e318221727d. [DOI] [PubMed] [Google Scholar]
- 6.Lai YH, Hsu HT, Wang HZ, et al. Astigmatism in preschool children in Taiwan. J Am Assoc Pediatr Ophthalmol Strabismus. 2010;14(2):150–154. doi: 10.1016/j.jaapos.2009.12.168. [DOI] [PubMed] [Google Scholar]
- 7.Wen G, Tarczy-Hornoch K, McKean-Cowdin R, et al. Prevalence of myopia, hyperopia, and astigmatism in non-Hispanic white and Asian children: multi-ethnic pediatric eye disease study. Ophthalmology. 2013;120(10):2109–2116. doi: 10.1016/j.ophtha.2013.06.039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Aljohani S, Aldakhil S, Alrasheed SH, et al. The clinical characteristics of amblyopia in children under 17 years of age in qassim region, Saudi Arabia. Clin Ophthalmol. 2022;16:2677–2684. doi: 10.2147/OPTH.S379550. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Read SA, Vincent SJ, Collins MJ. The visual and functional impacts of astigmatism and its clinical management. Ophthalmic Physiol Opt. 2014;34(3):267–294. doi: 10.1111/opo.12128. [DOI] [PubMed] [Google Scholar]
- 10.Gordon-Shaag A, Millodot M, Shneor E. The epidemiology and etiology of keratoconus. Int J Keratoconus Ectatic Corneal Dis. 2012;1(1):7–15. [Google Scholar]
- 11.Bui AD, Truong A, Pasricha ND, et al. Keratoconus diagnosis and treatment: recent advances and future directions. Clin Ophthalmol. 2023;17:2705–2718. doi: 10.2147/OPTH.S392665. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Grzybowski A, Kanclerz P. Beginnings of astigmatism understanding and management in the 19th century. Eye Contact Lens. 2018;44(Suppl 1):S22–S29. doi: 10.1097/ICL.0000000000000449. [DOI] [PubMed] [Google Scholar]
- 13.Asharlous A, Khabazkhoob M, Yekta A, et al. Comprehensive profile of bilateral astigmatism: rule similarity and symmetry patterns of the axes in the fellow eyes. Ophthalmic Physiol Opt. 2017;37(1):33–41. doi: 10.1111/opo.12344. [DOI] [PubMed] [Google Scholar]
- 14.Benedi-Garcia C, Velasco-Ocana M, Dorronsoro C, et al. Perceptual impact of astigmatism induction in presbyopes. Vision Res. 2019;165:143–151. doi: 10.1016/j.visres.2019.10.008. [DOI] [PubMed] [Google Scholar]
- 15.Hashemi H, Asharlous A, Jamali A, et al. Auto-refraction versus subjective refraction in different phakic and pseudophakic conditions: the Tehran Geriatric Eye Study (TGES) Int J Ophthalmol. 2023;16(8):1309–1316. doi: 10.18240/ijo.2023.08.18. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Kozlov Y, Kinori M, Armarnik S, et al. Subjective versus objective refraction in healthy young adults. BMC Ophthalmol. 2024;24(1):79. doi: 10.1186/s12886-024-03340-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Galindo-Ferreiro A, De Miguel-Gutierrez J, González-Sagrado M, et al. Validity of autorefractor based screening method for irregular astigmatism compared to the corneal topography—a cross sectional study. Int J Ophthalmol. 2017;10(9):1412–1418. doi: 10.18240/ijo.2017.09.14. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Chen XJ, Liu LJ, Sun B, et al. Two different autorefractors for vision screening in children and adolescents. Int J Ophthalmol. 2024;17(2):331–338. doi: 10.18240/ijo.2024.02.16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Vesely P, Petrova S, Benes P. Sensitivity and specificity in methods for examination of the eye astigmatism. Cesk Slov Oftalmol. 2020;75(6):310–314. doi: 10.31348/2019/6/3. [DOI] [PubMed] [Google Scholar]
- 20.Guo R, Shi L, Xu K, et al. Clinical evaluation of autorefraction and subjective refraction with and without cycloplegia in Chinese school-aged children: a cross-sectional study. Transl Pediatr. 2022;11(6):933–946. doi: 10.21037/tp-22-226. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Hashemi H, Yekta A, Saatchi M, et al. The met and unmet need for refractive correction and its determinants in 7-year-old children. Br J Vis Impair. 2017;35(1):69–80. [Google Scholar]
- 22.Sankaridurg P, He XG, Naduvilath T, et al. Comparison of noncycloplegic and cycloplegic autorefraction in categorizing refractive error data in children. Acta Ophthalmol. 2017;95(7):e633–e640. doi: 10.1111/aos.13569. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Guo XX, Shakarchi AF, Block SS, et al. Noncycloplegic compared with cycloplegic refraction in a Chicago school-aged population. Ophthalmology. 2022;129(7):813–820. doi: 10.1016/j.ophtha.2022.02.027. [DOI] [PubMed] [Google Scholar]