Abstract
INTRODUCTION
As one of the most rapidly aging societies globally, Korea's efforts to mitigate the social burden of Alzheimer's disease and related dementias (ADRD) may provide valuable insights.
METHODS
We conducted a mixed‐methods review of studies and policies related to dementia care in Korea over the past 25 years, including quantitative analysis of administrative and comparative data.
RESULTS
Estimates suggest a high social burden from ADRD, with annual costs increasing from 0.9% to 3.8% of gross domestic product between 2019 and 2050. Pilot programs for integrated community care and hospice palliative care reveal the advantages of innovating from a foundation of national health insurance and long‐term care insurance, as well as the continuing challenges of appropriately designing programs and incentives for early detection, integrated care, and late‐life palliative care.
DISCUSSION
A rigorous analysis of programs addressing uneven quality and a study of the impact of integrated care models for home‐ and community‐based services would be valuable.
Highlights
A mixed‐method review highlights the challenges of rapid aging in Korea.
Universal health and long‐term care systems support innovation for dementia care.
Dementia costs are projected to increase from 0.9% to 3.8% of gross domestic product in 2019–2050.
Pilots of integrated community care and hospice palliative care show promise.
Rigorous analysis of programs to address uneven quality would be valuable.
Keywords: Alzheimer's disease, caregiving, dementia, gender roles, Korea, long‐term care, long‐term care insurance, Long‐Term Services and Supports
1. BACKGROUND
As one of the most rapidly aging societies globally, the Republic of Korea (hereafter Korea) is home to an increasing number of older adults at risk of developing dementia as well as people currently living with Alzheimer's disease and related dementias (ADRD). Improving prevention and early detection while addressing the social burden of care for people living with ADRD (PwADRD) is especially important given this dramatic demographic shift. Koreans 65 years of age or older constitute 19.2% of the population in 2024, whereas as recently as 2007—the year that Korea enacted a system of Long Term Care Insurance (LTCI)—the fraction of Koreans who were 65 years of age or older was only 10%. 1 Demographic projections indicate that the population 65 years of age or older will represent fully 46.4% of the population by year 2070, and over 30% already by 2035. 2 Continuing extremely low fertility may bring these projections even closer, whereas any rebound in fertility would postpone their realization. Several regions of the country have already become “super‐aged societies,” with populations 65 years of age or older accounting for 20% or more of the total population.
In this review, we summarize Korean efforts to promote healthy aging and diagnose, treat, and care for PwADRD, focusing especially on recent policies to enhance “aging in place” for older adults capable of autonomous living as well as palliative care for those in need of greater supports and often toward the end of life. Drawing insights from key informant interviews and quantitative analyses of administrative data, we provide an overview of the economic implications and policy responses, including the roles of national health insurance and long‐term care insurance, plans for integrated community care, and the relative roles of and coordination across health care and social care, across public versus private entities, and across in‐home and community‐based services, residential care, and hospice palliative care, highlighting the challenges for caregivers, care recipients, and mitigating the social burden of ADRD.
2. METHODS
We conducted a mixed‐methods review and synthesis of studies and policies related to dementia care in Korea over the past 25 years. Our critical review of the social science and health policy literature emphasized peer‐reviewed articles in health economics, health services research, and health policy (including both English‐language and Korean‐language studies). The review was supplemented by quantitative analysis of Korean statistical agency data and comparative data from the other high‐income economies of the Organization for Economic Development and Cooperation (OECD), as well as informed by interviews conducted in the summer of 2023 of local government policymakers, researchers, and social welfare organization administrators in an area with an above‐average proportion of older adults (Chuncheon, Korea).
RESEARCH IN CONTEXT
Systematic review: We conducted a mixed‐methods review and synthesis of studies and policies related to dementia care in Korea.
Interpretation: Despite the strengths of universal health and long‐term care insurance, Korea faces challenges from rapid aging, widespread poverty among older adults, and a relatively weak system of primary care. Of particular note are Korea's efforts in establishing a national network of “dementia relief centers” as well as of pilot programs for integrated community care and hospice palliative care.
Future directions: Advancing the science of dementia care and caregiving requires evidence from different institutional and cultural contexts, and Korea's experience offers distinctive insights. Although epidemiological and health services research studies shed much light on current strengths and challenges, larger‐scale data with rigorous study designs to identify the causal impact of innovations in care delivery models could contribute significantly to a virtuous cycle of improvement in evidence‐based policy.
3. RESULTS
3.1. Insurance and service delivery
Societies take different approaches to financing and delivering services to older adults. South Korea has opted for social insurance—first, with more than four decades of consolidating and expanding the coverage of National Health Insurance (NHI), and then in 2008, launching LTCI. This latter system of social insurance for Long‐Term Services and Supports (LTSS) replaced the previous local government‐run programs funded by tax revenues. 3 Korea's LTCI constitutes a universal, mandatory program administered alongside Korea's health insurance system by the NHI Service.
The LTCI program, by separating long‐term services from NHI, contributed to enhanced accessibility, “de‐medicalizing” social care, and supporting more community‐based care settings for people with care needs appropriately addressed in the community. Indeed, one of the primary goals of adopting LTCI was to reduce “social hospitalizations”— that is, hospitalizations primarily to seek assistance with activities of daily living rather than medical care. 3 , 4 , 5 , 6 , 7
Korea's LTCI program provides subsidies for LTC services for individuals 65 years of age or older as well as those with age‐related needs such as ADRD or Parkinson's disease. There are copayment requirements (15% for home care services, 20% for institutional care services), with reduced copayments or exemptions for those with the least ability to pay. LTCI covers several categories of service benefits, including home care, day care, or night care centers, and residential institutional care. Originally, the eligibility criteria for LTC services in Korea emphasized activities of daily living and physical capacity or functioning; only later was eligibility expanded to better account for the needs of those with living with dementia. 8 Eligibility for benefits must be renewed regularly. The validity period varies by dependence level (a useful resource on the nuances of these requirements and other aspects of the historical evolution of Korea's LTCI system is provided by the Gateway to Global Aging Data 9 ).
Korea's health and LTC system relies on “contracting out” most of care, in the sense that organized, public financing is paid to mostly non‐government providers of services. Nationally, 9.6% of hospital beds are public, with some variation by location (e.g., Seoul's hospital beds are 11.1% public, compared to less than 5% in Incheon and Ulsan, and more than 20% in Sejong City (23.8%) and Jeju Island [30.4%]). 10
Within this private‐dominated service delivery system, there remains considerable variation in the public–private mix across services, partly in line with what would be expected from a conceptual model of the trade‐offs in promoting access, quality, and efficiency in delivery of tax‐financed services. 11 For example, the private sector completely dominates for pharmacies and clinics (including dental, Korean medicine, and midwifery clinics), but is absent from public health services such as health centers and subcenters and primary health care posts. The private sector runs 83% of general hospitals and 73% of tertiary hospitals as of 2022. 12 For LTSS, the role of non‐government service providers is even more pronounced, a pattern common across many countries. 11
3.2. Prevalence of ADRD and estimates of associated social burden
As the life expectancy of Koreans increases to among the highest in the world, subsidized health check‐ups under NHI and other policies explicitly target prevention with the goal of “compressing” years lived with frailty and low functional status toward later in life (“compression of morbidity”). Korea's age‐standardized health outcomes are quite good. Indeed, a recent comparative study 13 finds Korea among the global leaders in health outcomes after taking account of its population age structure, right after Switzerland and Singapore, and just ahead of Japan and Italy. Focusing on specific age groups, Chang and colleagues found that globally, Korea had the best outcomes for individuals 65–69 years of age in terms of age‐standardized mortality rates. 13 Yet the overall increase in the number of older Koreans implies an increasing number of individuals requiring social supports in the face of loss of physical and cognitive functions, including PwADRD.
Several studies describe current trends of ADRD in Korea and the projected future incidence and prevalence. 14 , 15 Although specific estimates differ, they all agree on the increase in prevalence despite generally declining age‐specific incidence, given Koreans’ longevity. Table 1 shows the current rate of ADRD in Korea nationally for different groups as well as the differential rates across selected regions.
TABLE 1.
People living with dementia in the Republic of Korea, 2022.
| Gender | Age | Population of that age | Population with dementia | Prevalence of dementia | |
|---|---|---|---|---|---|
| South Korea, 2022 | |||||
| Nationwide | Total | 65+ | 8,974,643 | 924,870 | 10.31 |
| Nationwide | Total | 85+ | 907,881 | 353,670 | 38.96 |
| Nationwide | Male | 85+ | 258,660 | 139,647 | 53.99 |
| Nationwide | Female | 85+ | 649,221 | 214,022 | 32.97 |
| Select regions | |||||
| Seoul | Total | 65+ | 1,620,545 | 154,989 | 9.56 |
| Busan | Total | 65+ | 686,167 | 64,747 | 9.44 |
| Daegu | Total | 65+ | 427,261 | 42,282 | 9.90 |
| Gyeonggi Province | Total | 65+ | 1,945,767 | 195,209 | 10.03 |
| Gangwon Province | Total | 65+ | 331,882 | 36,766 | 11.08 |
| South Jeolla Province | Total | 65+ | 428,235 | 51,746 | 12.08 |
| Jeju Province | Total | 65+ | 111,895 | 12,505 | 11.18 |
Source: Statistics Korea.
Shon and Yoon 16 estimate that in 2019, the health‐economic cost per capita due to dementia was approximately USD $6957, with indirect costs from family members’ informal care accounting for 48%. Their estimates suggest that this economic burden has grown significantly (about 1.5 times) since 2015, totaling about USD $4218 million. 16 The Ministry of Health and Welfare, which forecasts PwADRD to grow to 15.9% of Koreans 65 years of age or older by 2050, has collaborated with the Ministry of Science and ICT (information and communication technology) to launch the national Korea Dementia Research Center and supported research estimating that the annual cost of dementia care will increase from 0.9% to 3.8% of gross domestic product (GDP) between 2019 and 2050. 10 , 17 This estimate underscores the formidable pace of population aging and associated social cost of dementia care in Korea, although the estimate's accuracy depends on multiple assumptions (e.g., incidence rates, costs and coverage of any new treatments, or whether family caregiver costs are included based on formal care worker wages for equivalent hours of care or the predicted wage of the family caregiver if he or she were working). This large projected economic cost of almost 4% of GDP by 2050 could prove to be an underestimate because of factors not included in the model. For example, the economic and social costs of dementia will impose an even greater burden if population aging further slows GDP growth in Korea beyond current projections (for example, because of labor shortages and lower productivity growth in specific sectors of the economy). Slower growth would raise the percentage of GDP for any given cost of formal and informal care, as well as leave less fiscal space for tax revenue supporting long‐term care.
Korea's demographic transition, like its economic development, has been compressed into just a few generations. As a result, its triumph of longevity and current extra‐low fertility engender social strains and policy pressures to address the burgeoning needs for LTSS—including prevention of ADRD, investing in early detection, and providing appropriate care for PwADRD, which often involve addressing the broader social issue of financial support for older adults and detecting cognitive decline in those still engaged in the labor force.
3.3. Financial support: LTSS copayments
Social insurance like Korea's NHI and LTCI provide a solid foundation for pooling the risks associated with frailty and care needs, avoiding the adverse selection that market‐based insurance suffers from in other economies such as in the United States. 18 Accessibility is relatively high. Indeed, some analysts argue that there is an over‐supply of LTC providers in Korea, albeit juxtaposed with inadequate assurance of quality of care. 17
However, social insurance is no panacea for mitigating disparities and securing financial support for the most vulnerable citizens such as PwADRD and their families. In Korea, out‐of‐pocket payments for medical care constitute a substantial portion of household consumption. In 2021, 64.8% of Korean health care expenditures were covered by public financing (government or compulsory schemes, mostly NHI and some Medical Aid for the poor). 19 , 20 Private voluntary schemes covered 8.7% of medical care expenditures, with out‐of‐pocket spending representing the remaining 26.6% of expenditures—one of the highest out‐of‐pocket shares of any high‐income economy. 19 , 20 These copayments represent a comparatively large share of average household budgets. Indeed, according to OECD statistics, Koreans pay more of such copayments than any other OECD country except Switzerland, double the average share in the United States. 20 Specifically, the average Korean household spent 5.6% of final household consumption on out‐of‐pocket medical spending, compared to 2.8% in the United States in 2017. 20 For older adults with limited incomes and higher medical needs, that share can be considerably higher, although the poorest receive support through Korea's Medical Aid program.
Recognizing the problems associated with out‐of‐pocket payments for medical and long‐term care services, Korean policymakers have introduced a series of reforms to expand coverage and protect the most vulnerable populations from catastrophic medical spending or illness‐induced poverty. Examples include introducing NHI copayment ceilings based on income decile, and special arrangements for Koreans eligible for the Medical Aid program. 21 These reforms apply to services covered by NHI or Medical Aid; co‐payments paid for non‐covered services do not enjoy a copayment ceiling, 21 since copayments and non‐covered service designation are designed to control wasteful overuse and concentrate limited insurance funds on preventing catastrophic expenditures for services deemed worthy of coverage.
3.4. Livelihoods and labor force participation
One result of longer, healthier lives would be the ability to work longer and retire later or contribute to society in other ways, with older adults a vital social resource (e.g., in care for grandchildren, frail spouses, or other informal care services). Korea has relatively high labor force participation (LFP) among older men, compared to most other OECD countries. 19 Many Korean households conventionally relied on a single earner, constraining the household's ability to afford retirement when pension support is limited. The gender gap in employment in Korea is higher than in most OECD countries, 22 although gender differences in employment and in educational attainment are changing rapidly over time, like many other aspects of Korea's demography and society. For example, employment rates of women 55–64 years of age in Korea were more than 10 percentage points lower than in the United States as recently as 2008, but they have increased and overtaken those of the United States by 2023. 19 , 23 The share of housework done by men has increased over time, although according to analysis of data from a time use survey collected by Statistics Korea, women shouldered 77% even in dual‐earner households in 2019. 23 Many jobs taken by older adults (such as men after retirement and women re‐entering the labor force after raising children) are relatively low‐paying, low‐productivity positions in the service sector. 23
Part of the reason for Korea's high LFP among older adults, especially men, has been limited to other sources of financial support. Korea's net pension replacement ratio based on pre‐retirement income is 35%, ranking toward the bottom of the OECD. 24 The poverty rate among Koreans 65 years of age or older was higher than in many other OECD countries: 43.2% compared to 23% in the United States, 11.6% in Spain, and 4.4% in France. 10 , 19 Korea's future older adults may experience lower poverty and greater pension support as the structure of public and private retirement savings continues to evolve. For example, the basic old‐age pension is improving, and those who retire in 2028 or after will benefit from having had the opportunity to contribute a full 40 years into Korea's National Pension Scheme (begun in 1988). 25
Fieldwork in Gangwon province supports the view that the high LFP of older Koreans may be problematic. As one manager of a senior welfare center explained, “Currently, 70% of the elderly population do “senior jobs”. But now, most of these 70% are public service jobs. Public interest jobs were created to provide income security. However, if an elderly person almost 100 years old is working that way, it's a useless job. Because even the elderly who have difficulty walking come out to pick up trash. Some get hurt just by trying to walk and falling,” 26 although comprehensive data about such injuries are not currently available. It also is unclear how those “senior employment” positions are related to depression 27 or other adverse health outcomes and comorbidities, given the dearth of research with a plausible study design to identify impact rather than association.
This livelihood challenge, along with rapid social change and intergenerational inequalities, is also perceived to be closely related to mental health challenges and social isolation of older adults, our interviewees reported. Giving a lonely elderly person a reason to get up in the morning to go outside to socialize has its benefits; however, having 70‐ and 80‐year‐olds picking up garbage in public parks does not seem like a sustainable way to support livelihoods and healthy aging. Indeed, it may lead to accidents for those who are most frail and most in need of this supplemental income, so this policy could be self‐defeating in reducing their welfare and raising other (e.g., health care) costs. A rigorous evaluation could help to answer this question. As one senior center manager recommends, it probably would be preferable to raise the basic pension and eliminate or at least better target the government‐created jobs for the elderly. 26
Another important financial consideration stems from cognitive decline not being detected until late in the process when it is already severe, leaving those experiencing the early phases of ADRD susceptible to financial fraud and mismanagement of assets and income. This issue is little studied in Korea, although the intergenerational detrimental impact has been well documented elsewhere. 28 How decision‐making by cognitively impaired individuals affects health and financial well‐being can be considered the defining feature of the economics perspective on ADRD and its social impacts, as emphasized in an excellent recent review. 18 Indeed, the economic impacts of ADRD go beyond the assessed direct and even indirect costs on individuals and caregivers, since there are multiple channels through which ADRD also impacts the fiscal sustainability of health and social care systems, and the national economy, 29 as well as global public goods of knowledge and innovation about prevention and treatment.
3.5. Prevention and early detection
Ensuring timely and accurate diagnoses will be critical going forward. It is not clear that caregivers have the awareness, knowledge, and incentives to correctly identify and appropriately manage behavioral and psychological symptoms of dementia. Detection in health care settings remains challenging. According to the 2020 Survey of the Actual Conditions of the Elderly by the Korean Institute for Health and Family Affairs (KIHASA), ≈13% of Koreans 65 years of age or older have physical dysfunction or disabilities. 30 Only 55% of the elderly in need of care were found to be receiving care, suggesting an important gap between reality and the policy goal of appropriate and comprehensive support for all older Koreans in need of care. 30
To address this service gap over the long term, Korean policy seeks to strengthen screening and diagnosis while also promoting a reduction in risk factors associated with dementia, including low education, smoking, physical inactivity, and uncontrolled chronic disease such as hypertension and diabetes. 31
First, consider educational attainment. Large increases in Koreans’ educational attainment, especially among women, imply that Korea's future older adults may not be as burdened by the adverse impacts of limited educational opportunities as the current elderly. Education has been shown to be associated with cognitive reserve, including among older Koreans with varying levels of education. 32 As one of the countries with the highest levels of educational attainment per capita, Korea's future burden of dementia will be smaller than it would have been under simple projections of dementia by age and sex for previous cohorts. For example, Kasajima and colleagues find that Japan's official projections of dementia prevalence were incorrect because they did not account for the enhanced educational attainment of Japan's future elderly and the protective effects that brings for dementia risk. 33 Similarly, Hudomiet and colleagues find that for the United States, increases in education between 2000 and 2016, statistically explained about 40% of the reduction in dementia prevalence among men and 20% among women. 34
Policy to support the most vulnerable may be even more important in light of a steepening educational gradient in health, including a wider gap in the prevalence of functional disability between those with low and high educational attainment. Demographic modeling for Korea, compared to Singapore, shows that improved survival of those with low education and their declining share of the population leads to their concentration among the oldest‐old and therefore with the highest disability burden. 35
A second vital issue is improving healthy behaviors, many of which are manifest in specific groups. For men especially, accelerating the decline in smoking would contribute to reduced premature mortality, and help to control a risk factor for dementia. 31 Reducing sedentary lifestyles and promoting healthy sleep habits from a young age can have positive impacts across a lifetime. For example, an analysis of the impact of a law requiring private tutoring schools to close by 10 p.m. showed that a 1 h increase in sleep duration was associated with a 0.56 kg/m2 reduction in body mass index and a decreased risk of being overweight or obese by 4.2% points. 36
Hypertension is an important risk factor associated with dementia. 31 Korea's NHI system promotes access to care to facilitate control of chronic conditions like hypertension. However, analysis of data from 2007 to 2015, through the Korean National Health and Nutrition Examination Survey shows that 34.8% of Korean adults with hypertension were not aware of their condition and not being treated for it. 37 Younger age, lower education, and male gender were among the risk factors associated with undiagnosed and untreated hypertension, reinforcing the risks of the more vulnerable low‐income Koreans who may also smoke. Indeed, the authors find a significant correlation between several unhealthy behaviors (including risky alcohol consumption, high salt intake, insufficient physical activity, and lack of health check‐ups) and lack of control of hypertension. 37 Although improvements in blood pressure control and narrowing disparities in hypertension control are encouraging, substantial room still exists for improvement.
Diabetes constitutes a second critical chronic disease that is also a risk factor for cardiovascular disease, dementia, and premature mortality. Kim and Cheng analyze diabetes‐related avoidable hospitalizations as a metric of the quality of primary health care, showing that both the Korean and Taiwan systems of primary care management for diabetes could be improved. 38
Finally, mental health is of salient importance, as depression is a risk factor for dementia and mental disorders account for a large share of the burden of chronic disease in Korea, including at older ages. 39 Social pressures are tragically apparent from the high rates of suicide in Korea—including among older adults. “Self‐harm” increased from the #7 cause of premature mortality in 1990 to #2, second only to stroke, by 2010, according to the Global Burden of Disease, even as once‐rampant scourges such as tuberculosis and other infectious diseases decreased appreciably. 39 Some local governments in Korea have experimented with pilot programs targeting elderly individuals who are living alone to screen for depression and enhance case management for individuals deemed at high risk of suicide; such an approach has appeared to help reduce the elderly suicide rate in Gangwon, for example, and might be usefully subject to rigorous evaluation and scaled up, if found to be effective. 40
3.6. At‐home and community‐based care
Traditions of inter‐generational living have deep and lasting roots but are coming under strain due to demographic and social change. Many Koreans, like in other aging societies, express a desire to remain in their local communities as they age. Cultural practices and norms, such as filial obligation, establish a general sentiment that caring for the elderly and disabled is the responsibility of family members (usually the eldest daughter or daughter‐in‐law). However, rapid demographic change has been accompanied by changes in social norms regarding responsibilities and caregiving, arguably in part because of policies such as public LTCI. Significantly fewer people think that it is solely the responsibility of family members to care for older parents: 67.3% in 2006, declining to only 32.6% by 2016. 3
Accordingly, Korean policies aim to establish an environment in which the elderly with functional disabilities can receive medical care and social care delivered in their own home or community before receiving institutional care such as a nursing facility, while leveraging social resources for LTSS. Indeed, policymakers and local experts we interviewed all emphasized that Korea seeks to strengthen home‐ and community‐based services (HCBS) and delay institutionalization.
Data reveal both progress and opportunities for further improvement in HCBS. According to OECD data, Korea's share of LTC recipients who receive services at home rather than in institutions remains lower than many peer economies but has been increasing gradually over recent years (increasing 2018–2022 from 17.5% to 22.7% of individuals 80 years of age and older, and from 6.2% to 8.1% of individuals 65 years of age and older; see Figure 1). 41 , 42 This increase is partially the result of the desires and social norms of Korean households, as well as concerted policy efforts to increase emphasis on HCBS and support families and individuals who are living alone in achieving quality outcomes. In‐home care has been shown to assist with mitigating pressure ulcers among individuals who are vulnerable and frail. 43
FIGURE 1.
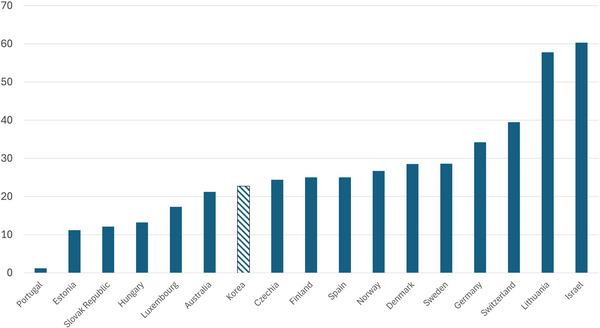
At‐home long‐term care recipients aged 80+, percentage of total population aged 80+. Source: OECD Statistics.
Making the vision of quality HCBS a reality involves multiple dimensions of financing and service delivery, tailored to local and individual circumstances while supporting equitable access nationally for those in need. November 2018 saw the launch of Korea's “Comprehensive Plan for Community Care.” The next month, in December 2018, through the revision of the National Health Insurance Act, a new provision for visiting (at‐home) treatment benefits was established. The following year, in October 2019, the community care pilot project was launched, with December 2019 seeing the corresponding launch of the pilot project for primary care visits, targeting patients with reduced mobility due to illness or injury. 44 Despite the onset of the pandemic soon thereafter, the efforts to strengthen home care continued as conditions allowed.
This community care pilot project, active since 2019 (see Figure 2), involves input and coordination among multiple levels of government, including at the central, local, and community levels. 44 The roles of the central government are budgetary, legal, and institutional support. City or provincial governments take the lead in project planning and case management for some particularly difficult cases, whereas the local government agencies (Eup, Myeon, Dong, or village) take responsibility for the overall implementation of projects, overseeing delivery of services and regular case management.
FIGURE 2.
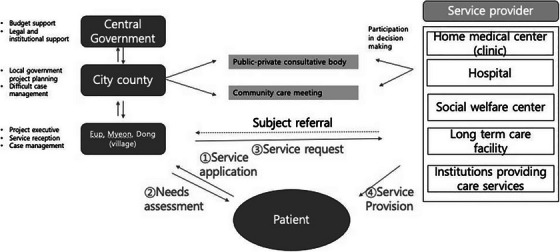
Community care pilot project in Korea. Source: Author adaptation of Figure 4 of Yoo and Park (2022).
The service providers encompass home medical centers and clinics, hospitals, social welfare centers, long‐term care facilities, and other organizations providing care services. Individuals (patients) first submit a service application; they then receive a needs assessment from the relevant government agency at the local level (village or district dong), and if deemed eligible, a service request is submitted to the service providers, which then directly provide the service(s) to the patient. 44
The vision for the “home medical center for long‐term care patients in Korea” includes several components (see Figure 2). The first step is application and initial consultation, in which relevant personnel visit the patient's home to understand the patient's health condition and treatment needs. Second, those parties discuss and establish a care plan after comprehensive evaluation, detailing services and connecting individuals to resources. Third, the PwADRD or other frail patient receives regular visits for medical treatment and care services, usually with a physician visiting at least once a month and a nurse twice a month, as well as case management according to patient severity and assessed needs. 44 However, limited evidence yet exists on whether the program has attained is goals and if there have been any positive or negative spillovers on other aspects of care service or other populations.
In addition, there is the perennial question of what constitutes an optimal compensation scheme to promote appropriate, integrated, quality care, while controlling cost. The current home medical service fee includes three parts: a basic fee for home medical services, a visiting treatment fee per visit, and additional compensation for other nursing services. 44 Studies of the payment scheme's impact on cost and quality would be valuable.
Local experiments with integrated care are also of note. For example, a public–private partnership in one “super‐aging” area (with individuals 65+ constituting 27% of the population) in the northeast of the country brought together multiple parties and sectors to try to provide an integrated service to the local older adult population. The collaboration spanned personnel from multiple government agencies including housing, social care, safety, and health services, alongside private advocates and service providers, possibly providing a model for other areas to emulate. That experience and others in the region demonstrated that in addition to addressing fragmentation of service delivery, the economic incentives for integration need to be considered carefully. Currently, separate budgets, administrative processes, and regulatory authority (e.g., NHI, local governments, community social care) hamper achieving integrated HCBS for services for older adults. 45 Both organizational and financial integration may be needed before incentives can be aligned and appropriate coordination sustained.
Regarding HCBS for dementia, of particular note are Korea's efforts in establishing a national network of “dementia relief centers.” LTSS offered through these centers include a variety of components that may vary by location, such as support for screening and early detection of ADRD, self‐help groups, basic counseling, in‐depth and one‐on‐one customized counseling, case management, and efforts to support family and community caregivers. 45 As these dementia centers become more established in their communities and evidence is collected on their effectiveness in providing LTSS to PwADRD, policies may be updated to reflect the latest knowledge about best practices and components of programming that are most appropriate for different population subgroups.
3.7. Residential care
Although HCBS may be the emphasis, frail older PwADRD with multiple comorbidities often require institutional care in residential facilities such as nursing homes. While the supply of such LTSS providers has greatly improved and the affordability for families has been enhanced by LTCI coverage, several issues remain to be addressed.
Like many countries, Korean families and officials have suspicions, backed up with some evidence, that the social care services delivered in institutions such as nursing homes is of uneven quality. Some concerns center on the use of potentially inappropriate medications 46 ; others highlight issues with adequate staffing and processes of care. 47 , 48 Some analysts suggest that the nexus between medical care and LTSS needs special attention to prevent lapses in quality and coordination. 8 A recent KIHASA report also highlights concerns with quality of care for those in residential facilities, framing their care as an issue of the right to self‐determination. 49 A natural response would be strengthening training of staff providing LTSS and enhancing the quality evaluation system for services both in institutions and in HCBS.
Studies to date suggest a variety of determinants of the quality of care and policies that might help to raise the average level and reduce the wide disparities in quality. Kim and Kwon 3 argue that:
“The quality of care is higher in government‐owned institutions than their counterparts, but the majority of private providers are individual‐owned, small‐size homes, and their numbers have rapidly increased, resulting in fierce competition… often based on more tangible aspects of care (e.g., buildings/structures, etc.) or illegal price discounts rather than actual quality of care (outcomes)…. Competition is not likely to improve social efficiency in the Korean LTCI context. Several policies to address such issues have been implemented, including improving the quality of nursing home inspections, provision of care guidelines, and financial support for direct‐care workers” (p. 25). 3
With investments in systematic monitoring and evaluation of these efforts, LTSS policies can contribute to improved quality of care.
3.8. Complexities revealed by the COVID‐19 pandemic
The coronavirus disease 2019 (COVID‐19) pandemic (2020–2023) significantly impacted care for the at‐risk elderly in Korea, as elsewhere. According to a World Bank report prepared by faculty at Seoul National University School of Public Health, 50 early in the pandemic (2020), the government prioritized the supply of masks for LTC service providers; strengthened containment measures and mandated reimbursement of employee screening tests; and prioritized vaccination for those residing in or working in LTC facilities, as well as those age 75 and older living in the community. 50 The closure of many community‐based care facilities for an extensive period in 2020—including senior welfare centers, dementia care centers, senior day/night care centers, and employment centers for older people—impacted users and their caregivers/families, protecting them from infection with severe acute respiratory syndrome coronavirus 2 (SARS‐CoV‐2) infection but removing valuable services and supports, as our interviewees reported. One effect was strain from social distancing, delayed or foregone medical care for fear of infection, and compounding of social isolation, especially among those already living alone. As Lee et al. note,
“The Korean government aimed at transparent communication and information disclosure for effective contact tracing and tried to provide as much information as the law prescribed. However, facing criticism on privacy issues, the [Infectious Disease Control and Prevention Act] IDCPA was revised to reduce the scope of information disclosure while maintaining some essential information for contact tracing. This enhanced the transparency and openness of the government responses and, in turn, led to fostering the public's trust in them” (p. 56). 50
Successful social adaptation to population aging and a strengthened dementia‐care support system both call for similar dedication to evidence, adjustment, and high‐priority open communication without descending into divisive politicization.
3.9. Interactions between NHI and LTCI
Care transitions for PwADRD expose frailty and the costs of poorly integrated care. Despite the strengths of universal health coverage and compulsory LTCI, in Korea, these care transitions can be difficult, given the gray areas between NHI and LTCI that patients and their families must navigate.
An important aspect of the design and adoption of LTCI in South Korea was the aim to encourage substitution between informal and formal care services, relieving the burden of informal care for family caregivers by subsidizing formal care services and thereby reducing the need for “social hospitalizations” under NHI. Some studies suggest that adding LTCI to Korea's existing coverage by NHI did promote some reduction in related NHI services, such as inpatient services or LTC hospitals, while increasing others (e.g., outpatient care and pharmaceuticals). 3 , 4 , 5 , 6
In an empirically rigorous study, Kim and Lim 7 study how South Korea's LTCI system, by subsidizing formal care, impacts informal care use and medical expenditures. Studying over 171,000 individuals with a regression discontinuity design using administrative data on the eligibility thresholds, Kim and Lim show that the LTCI subsidies lead to increases in formal LTC utilization, concluding that “publicly financed home care may have limited impact among the more able, but that it may be both more cost‐effective and beneficial than institutional care for the least able” (p. 128). 7
Careful analysis of health care use by Cho and Kwon 4 found that LTCI probably did contribute to reducing social hospitalizations, because its introduction is associated with fewer inpatient admissions for the target population and a reduction in the length of stay for such admissions. In particular, by caring for the daily needs of older adults through accessible LTC, Korea's LTCI program appears to have helped to ameliorate the rate of growth of health care spending, especially for the largest component of NHI spending, that of inpatient services. Cho and Kwon document that LTCI led to a 2.7% reduction in hospitalization rates, and that for those who were still hospitalized, length of stay and inpatient expenses decreased by 15.6% and 9.5%, respectively. 4
3.10. Workforce
As in many countries, Korea's workforce furnishing care to people with AD/ADRD is under considerable strain. Korea needs more strategies to recruit, retain, and empower a knowledgeable and resilient caregiving workforce. 51 Although low fertility may free up care time previously absorbed by young dependents, care work for older adults rapidly fills that space and cumulatively leaves smaller families with substantial caregiving responsibilities. Care partners may be at risk for cognitive decline themselves, or other adverse impacts on health and social engagement. 52 Although some research has studied caregivers in Korea, including unpaid family informal care and its associated burden according to the severity of ADRD symptoms, 53 little generalizable results on their resilience and effective support strategies is yet available 54 , 55 ; more research would be valuable.
Fahle and McGarry, analyzing the U.S. Health and Retirement Study (HRS), document significant reductions in caregivers’ labor force attachment when providing informal care to parents and parents‐in‐law, the burden of which falls mostly on women in their 50s. 56 Thus, these caregiving responsibilities provide headwinds for the trend toward longer working lives, and contributes to a continued “M” shaped LFP rate for Korean women, with lower rates in prime ages that then rebound in their later years. 23
3.11. Palliative care, hospice, and end‐of‐life care
Hospice and palliative care aim to reduce the suffering of individuals within the last few months of life and provide psychological and spiritual support for patients and their families. 57 , 58 Although the terms end‐of‐life care, hospice care, and palliative or comfort care are often used interchangeably, we focus here on the context of Korea's legal mandates to provide hospice palliative care, which did not target individuals with severe dementia and related conditions, but rather started with a focus on cancer care (regardless of comorbidities). 59 Nevertheless, this policy framework and gradually expanding system of care and social awareness suggest that hospice care may soon become a more broadly available option for late‐stage PwADRD and their caregivers.
Unlike other countries where hospice care originated from charity work by religious groups and was later funded by public foundations and social insurance, Korea previously lacked a convention of hospice palliative care. Some religious groups had started hospice care services informally, but only recently has the government taken the lead in funding hospice care and shaping the method of service provision. Financial support effectively began when Korea started a government‐designed hospice palliative care pilot project in 2002. In 2016, the “Act on Hospice Palliative Care and Decisions on Life‐Sustaining Treatment for Patients in the Terminal Stage” (the Life‐Sustaining Treatment Decision Act) was enacted and has been in effect since February 2018.
Looking at the contents of the current law, this Life‐Sustaining Treatment Decisions Act defines the target recipients of “hospice and palliative care” as individuals diagnosed as terminally ill by a physician or a patient otherwise medically designated as at the end‐of‐life. 60 The law refers to medical and social care aimed at comprehensive support for the physical, psychosocial, and spiritual impacts of terminal illness. This includes relief of pain and symptoms and may encompass not only individuals with cancer, but also those with acquired immunodeficiency syndrome, chronic obstructive respiratory disease, chronic liver cirrhosis, or chronic respiratory failure. However, currently only cancer patients can be admitted to the hospice ward of a hospital; others receive home‐based care.
For a service provider to participate in hospice care, the provider must be a licensed medical institution that meets certain standards for hospice care such as personnel, equipment, and facilities. Services may commence once the provider obtains confirmation of designation from the office of the Minister of Health and Welfare. 61
Under this program, 15,819 terminally ill cancer patients were admitted to hospice wards at specialized institutions in 2022, with a range of support provides to their families. 62 Hospice teams from specialized institutions designated by the Ministry of Health and Welfare also visit homes to provide care and specialized palliative care services to terminally ill patients and their families who wish to remain at home. As of 2023, 39 such locations were in operation, but the number of users remained limited (e.g., only 2359 total beneficiaries in 2022). 62 In the case of home‐based care, the hospice team provides specialized palliative care services together with the attending physician for terminally ill patients and their families who have received or may still be receiving some treatment in general wards, outpatient clinics, and emergency rooms. As of 2022, a total of 6630 beneficiaries had utilized this combined‐type hospice care. 62
Overall, a limited number of service providers have joined the program, and there are many people waiting. In addition, even for users who do currently use the service, accessibility remains constrained, since, as noted, inpatient services are limited to terminally ill cancer patients. For this reason, the hospice care utilization rate (number of hospice users/number of cancer deaths) as of 2022 is 24.5%, which is relatively low compared to the utilization rate of 40%–50% in other high‐income countries. 62 In terms of securing financial resources, hospice care is currently compensated through health insurance, but it might be possible to consider having public interest foundations shoulder a portion of the financial resources by activating a donation culture, as in many other industrialized countries.
4. DISCUSSION
As one of the most rapidly aging societies globally, Korea's efforts to mitigate the social burden of ADRD may provide valuable insights for other countries. Our mixed‐methods review of studies and policies related to dementia care in Korea over the past 25 years reveals the advantages of having national health coverage both for medical care and for LTC. Several of the key aims of adopting LTCI—such as decreasing unnecessary “social hospitalizations” and “de‐medicalizing” social care—appear to be partially realized. As Kim and Kwon 3 emphasize, the adoption of LTCI in 2008 helped to address regional disparities by providing nationwide risk pooling for LTSS, although this parallel system of financing and care also creates its own challenges for the coordination of health care and LTC and for local community input for the design of appropriate HCBS care models.
Korea's rapid socioeconomic and demographic change exacerbates many of the social pressures associated with a transition to a large population of frail older adults, including PwADRD. Demographic and economic projections suggest that the annual cost of ADRD in Korea may increase to almost 4% of GDP by 2050. 10 , 17 Although the accuracy of this estimate depends on a series of assumptions about the costs of formal and informal care and the growth of GDP, it underscores the importance of investing in prevention and supporting families caring for PwADRD. Korea is aging more rapidly than the United States, where Gruber and McGarry estimate that informal care by family caregivers accounts for more than one‐third of the nearly 2% of GDP devoted to all LTC. 63 Korea enjoys the foundational advantage of nation‐wide social insurance coverage for both health care and LTC (both of which the United States lacks); yet the rapidity of population aging suggests even greater urgency in policy response, given projected doubling of dementia care costs as a share of Korea's economy over the next 25 years.
Korea's efforts to appropriately design programs and incentives for early detection, integrated care, and late‐life palliative care confront at least three important challenges. First, there is the question of supporting an aging workforce by providing services to older adults and encouraging coordinated, person‐centered HCBS. The shortage of caregivers and the aging workforce constitute key dilemmas, raising questions about immigration as a continuing supply of labor for LTC. Pilot programs for integrated community care appear encouraging, if adequate human resources and financial support enables more coordinated, person‐centered care.
A related challenge is the low utilization of some LTSS programs already put in place, such as the program supporting hospice and palliative care. Both demand‐ and supply‐side factors appear to contribute to relatively low utilization. Because the incentive for supplying palliative care is relatively low, providers may hesitate to devote resources to meeting these patients’ needs (including hiring appropriate care providers). Moreover, on the demand side, family members and patients themselves may find it difficult to forego further curative treatments. The option of hospice palliative care may become more acceptable in the future, given the desire of many patients and their families to focus on quality of life rather than medical interventions at the end of life.
A second set of challenges involves expanding the target group of beneficiaries and diversifying LTSS. It will be important for policy to carefully consider how best to define the priority target group and clarify selection criteria. Diversification of service contents, including leveraging emerging technologies to improve service delivery, are pressing concerns. This includes enhancing support for complementary medical care services and responding to additional health care needs such as on‐site rehabilitation. Better care support for daily life would involve the development of additional care service types such as hospital companion services and nutrition support services. Aging‐in‐place also relies on effective housing support and would benefit from integrating support for care using ICT technology, such as telemedicine services and home‐based monitoring devices.
Third, consistent policy coordination and evaluation merits consideration. To utilize limited resources most effectively, it will be critical to design and collect policy‐relevant evidence about what works for PwADRD and their care partners. Korea has used pilots and other policy experiments to inform policy for PwADRD to some extent, but the scope has been limited compared to the burgeoning need and demand. These scattered efforts to assess program impact could be formally endorsed and provided with ongoing resources and channels for informing policy. Several other OECD economies have systems in place to generate evidence, beyond health technology assessment, to encompass LTSS and other programs especially relevant for frail older adults. For example, in the United States, the National Institute on Aging (NIA) has supported several Roybal Centers that conduct pilot research aimed at strengthening the design of dementia care interventions. In addition, the NIA IMPACT Collaboratory has partnered with health care systems across the country to conduct pragmatic clinical trials. 64 Given concerns that quality falls short of what Koreans expect and deserve, rigorous analysis of programs to address uneven quality would be useful, including efforts related to staff training and staff ratio regulation, monitoring quality processes and outcomes, and studying the impact of HCBS integrated care models for quality and satisfaction among participating PwADRD.
CONFLICT OF INTEREST STATEMENT
The authors declare no conflicts of interest. Author disclosures are available in the Supporting Information
CONSENT STATEMENT
All human subjects provided informed consent.
Supporting information
Supporting Information
ACKNOWLEDGMENTS
Although this review did not receive any specific grant from funding agencies in the public, commercial, or not‐for‐profit sectors, Karen Eggleston gratefully acknowledges support from an East‐West Center POSCO fellowship and a Fulbright scholar award in the Republic of Korea during 2022–2023, when initiating the broader project of which this is a part. Eggleston also thanks Professor Jiyoung Lyu and Dr. Jung‐Eun Lee of Hallym University Institute of Aging for their kind assistance with the qualitative interviews conducted in Korea in 2023, and Jenny Seo Jin Lee of Stanford University for excellent research assistance funded by the Shorenstein Asia‐Pacific Research Center at Stanford University. Note: The views expressed in this article are those of the authors and do not reflect the official policy positions of the Korea Institute for Health and Social Affairs (KIHASA) or any other organization.
Eggleston K, Kim D. Dementia care in a rapidly aging society. Alzheimer's Dement. 2025;21:e70268. 10.1002/alz.70268
REFERENCES
- 1. Korean Statistical Information Service (KOSIS), Projected Population by Age Group. https://kosis.kr/statHtml/statHtml.do?orgId=101&tblId=DT_1BPA003&conn_path=I2&language=en
- 2. Statistics Korea, Population Projections: 2020–2070. https://kostat.go.kr/anse/
- 3. Kim H, Kwon S. A decade of public long‐term care insurance in South Korea: policy lessons for aging countries. Health Policy. 2021;125(1):22‐26. [DOI] [PubMed] [Google Scholar]
- 4. Cho YM, Kwon S. Effects of public long‐term care insurance on the medical service use by older people in South Korea. Health Econo Policy Law. 2023;18(2):154‐171. [DOI] [PubMed] [Google Scholar]
- 5. Rhee JC, Done N, Anderson GF. Considering long‐term care insurance for middle‐income countries: comparing South Korea with Japan and Germany. Health Policy. 2015;119(10):1319‐1329. [DOI] [PubMed] [Google Scholar]
- 6. Kim H, Jung YI, Kwon S. Delivery of institutional long‐term care under two social insurances: lessons from the Korean experience. Health Policy. 2015;119(10):1330‐1337. [DOI] [PubMed] [Google Scholar]
- 7. Kim HB, Lim W. Long‐term care insurance, informal care, and medical expenditures. J Public Econ. 2015;125:128‐142. [Google Scholar]
- 8. Jeon B, Kwon S. Health and long‐term care systems for older people in the Republic of Korea: policy challenges and lessons. Health Syst Reform. 2017;3(3):214‐223. [DOI] [PubMed] [Google Scholar]
- 9. Gateway to Global Aging Data . Gateway Policy Explorer: Republic of Korea, Long‐Term Care In‐Kind Benefit Plan Details, 2008‐2023, Version: 1.0 (January 2024), University of Southern California, Los Angeles. 2024. doi: 10.25553/gpe.ltc.kb.kor [DOI] [Google Scholar]
- 10. Korean Statistical Information Service (KOSIS). https://kosis.kr/eng/
- 11. Eggleston K. Nonprofits and the scope of government: Theory and an application to the health sector. National Bureau of Economic Research; January 2024. Working Paper 32020.
- 12. Health Insurance Review & Assessment Service, National Health Insurance Statistical Yearbook . https://kosis.kr/statHtml/statHtml.do?orgId=354&tblId=DT_HIRA43&language=en&conn_path=I3
- 13. Chang AY, Skirbekk VF, Tyrovolas S, Kassebaum NJ, Dieleman JL. Measuring population ageing: an analysis of the Global Burden of Disease Study 2017. The Lancet Public Health. 2019;4(3):e159‐e167. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Kim YJ, Han JW, So YS, Seo JY, Kim KY, Kim KW. Prevalence and trends of dementia in korea: a systematic review and meta‐analysis. J Korean Med Sci. 2014;29(7):903‐912. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Moon W, Han JW, Bae JB, et al. Disease burdens of Alzheimer's disease, vascular dementia, and mild cognitive impairment. J Am Med Dir Assoc. 2021;22(10):2093‐2099.e3. [DOI] [PubMed] [Google Scholar]
- 16. Shon C, Yoon H. Health‐economic burden of dementia in South Korea. BMC Geriatr. 2021;21(1):549. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Song K. Korea Times [Internet]. 2024. [cited 2024 October 1]. Population aging and dementia management. https://www.koreatimes.co.kr/www/opinion/2024/10/791_369122.html
- 18. Chandra A, Coile C, Mommaerts C. What can economics say about Alzheimer's disease? J Econ Lit. 2023;61(2):428‐470. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. OECD Statistics . https://www.oecd‐ilibrary.org/statistics
- 20. OECD Health Statistics 2019 . OECD National Accounts Database.
- 21. National Health Insurance Service (NHIS), Republic of Korea . Insurance benefits. 2025. https://www.nhis.or.kr/english/wbheaa02600m01.do
- 22. OECD Statistics , OECD family database, Gender differences in employment outcomes. https://www.oecd.org/content/dam/oecd/en/data/datasets/family‐database/lmf_1_6_gender_differences_in_employment_outcomes.pdf
- 23. Kim J, Lee CH, Eggleston K. The Evolution of Age‐Friendly Jobs in a Rapidly Ageing Economy. Stanford Asia Health Policy Program, February 2025. Working paper.
- 24. Chung JW, Lee CH. Technology, Job characteristics, and retirement of aged workers: evidence from automation and IT adoption of firms in Korea. Ind Corp Change. 2023;32:831‐847. [Google Scholar]
- 25. Gateway to Global Aging Data . Gateway Policy Explorer: Republic of Korea, Public Old‐Age Social Assistance Plan Details, 1992‐2020, Version: 1.1 (August 2023), University of Southern California; 2023. doi: 10.25553/gpe.ret.sa.kor [DOI] [Google Scholar]
- 26. Interview, June 7th 2023, Director So‐Young Kim, Manager of a Senior Welfare Center.
- 27. Roh HW, Park S, Park S, et al. Association of geriatric depressive symptoms and government‐initiated senior employment program: a community based cross‐sectional study in Korea. Alzheimers Dement. 2023;19(S23):e073973. [Google Scholar]
- 28. Mazzonna F, Peracchi F. Are older people aware of their cognitive decline? Misperception and financial decision‐making. J Polit Econ. 2024;132(6):1793‐1830. [Google Scholar]
- 29. Knapp M, Wong G. Economics and dementia: challenges and responses. Dementia. 2024;23(3):512‐522. [DOI] [PubMed] [Google Scholar]
- 30. Korea Institute for Health and Social Affairs (KIHASA) , 2020 Survey of the Actual Conditions of the Elderly by KIHASA. https://www.kihasa.re.kr/
- 31. Livingston G, Huntley J, Liu KY, et al. Dementia prevention, intervention, and care: 2024 report of the Lancet standing Commission. The Lancet. 2024;404(10452):572‐628. [DOI] [PubMed] [Google Scholar]
- 32. Kim Y, Stern Y, Seo SW, et al. Factors associated with cognitive reserve according to education level. Alzheimers Dement. 2024;20(11):7686‐7697. https://onlinelibrary.wiley.com/doi/abs/10.1002/alz.14236 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Kasajima M, Eggleston K, Kusaka S, et al. Projecting prevalence of frailty and dementia and the economic cost of care in Japan from 2016 to 2043: a microsimulation modelling study. The Lancet Public Health. 2022;7(5):e458‐e468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34. Hudomiet P, Hurd MD, Rohwedder S. Trends in inequalities in the prevalence of dementia in the United States. Proc Natl Acad Sci U S A. 2022;119(46):e2212205119. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Chen C, Lim JT, Chia NC, et al. Educational Gradients in Disability among Asia's future elderly: projections for the Republic of Korea and Singapore. Asian Dev Rev. 2022;39(01):51‐89. [Google Scholar]
- 36. Do YK. Causal effect of sleep duration on body weight in adolescents: a population‐based study using a natural experiment. Epidemiology. 2019;30(6):876‐884. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37. Park JE, Park JH, Chang SJ, Lee JH, Kim SY. The Determinants of and Barriers to Awareness and Treatment of Hypertension in the Korean Population. Asia Pac J Public Health. 2019;31(2):121‐135. [DOI] [PubMed] [Google Scholar]
- 38. Kim H, Cheng SH. Assessing quality of primary diabetes care in South Korea and Taiwan using avoidable hospitalizations. Health Policy. 2018;122(11):1222‐1231. [DOI] [PubMed] [Google Scholar]
- 39. Global Burden of Disease (GBD), data and analysis. https://www.healthdata.org/research‐analysis/gbdandGlobalHealthDataExchange(GHDx), https://ghdx.healthdata.org/
- 40. Interview with Professor Kang Lee of Hallym University, June 2023.
- 41. Grabowski DC. The future of long‐term care requires investment in both facility‐ and home‐based services. Nat Aging. 2021;1(1):10‐11. [DOI] [PubMed] [Google Scholar]
- 42. OECD data explorer, Long‐Term Care Resources and Utilization. September 28, 2024. https://data‐explorer.oecd.org/vis
- 43. Lee E. Longitudinal outcomes of home care in Korea to manage pressure ulcers. Res Nurs Health. 2017;40(3):255‐262. [DOI] [PubMed] [Google Scholar]
- 44. Yoo AJ, Park HK. Evaluation of the integrated care policy: performance and future directions. Public Health Affairs. 2022;6(1):e7 (in Korean). doi: 10.29339/pha.22.7 [DOI] [Google Scholar]
- 45. Interview with Professor Kang Lee. Hallym University. June 2023. [Google Scholar]
- 46. Hwang HJ, Kim SH, Lee KS. Potentially inappropriate medications in the elderly in Korean long‐term care facilities. Drugs Real World Outcomes. 2015;2(4):355‐361. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47. Shin JH, Hyun TK. Nurse staffing and quality of care of nursing home residents in Korea. J Nurs Scholarsh. 2015;47(6):555‐564. [DOI] [PubMed] [Google Scholar]
- 48. Cho E, Min D, Heo SJ, Lee K, Kim H. Effects of registered nurses' staffing levels, work environment and education levels on nursing home residents' quality of life and nurse outcomes. J Clin Nurs. 2023;32(17‐18):6494‐6503. [DOI] [PubMed] [Google Scholar]
- 49. Lee SJ. Human Rights and Protection of Residential Facility Users: Focusing on the Right to Self‐Determination, Research report 2023‐26. 25 September 2024. https://www.kihasa.re.kr/en/publish/paper/research/view?seq=60904
- 50. Lee TJ, Kim H, Cho S, You MS, Chung W, Moon J. Country Case Study: The Republic of Korea (English). World Bank Group. [Google Scholar]
- 51. Pace D, Betts S, Reda L, et al. Empowering a person‐centered long‐term care workforce. Alzheimers Dement. 2024;20(9):6647‐6653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52. Jeon SY, Kim JL. Spousal caregiver burden among patient with cognitive impairment: effects on nutrition and other lifestyle factors. Alzheimers Dement. 2022;18(S8):e062066. [Google Scholar]
- 53. Kim B, Kim JI, Na HR, Lee KS, Chae K‐h, Kim S. Factors influencing caregiver burden by dementia severity based on an online database from Seoul dementia management project in Korea. BMC Geriatr. 2021;21(1):649. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54. Seo HJ, Park SI, Choi YM, Choi MJ, Choo IH, Park JH. Resilience of family caregivers of PwD in Korea: a scoping review. Alzheimers Dement. 2023;19(S19):e071450. [Google Scholar]
- 55. Kim B, Noh GO, Kim K. Behavioral and psychological symptoms of dementia in patients with Alzheimer's disease and family caregiver burden: a path analysis. BMC Geriatr. 2021;21(1):160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56. Fahle S, McGarry K. Women working longer: labor market implications of providing family care. Women Working Longer: Increased Employment at Older Ages. University of Chicago Press; 2017. p. 157‐181. [Google Scholar]
- 57. National Health Service (NHS), UK . End of Life Care. 2022. https://www.nhs.uk/conditions/end‐of‐life‐care/what‐it‐involves‐and‐when‐it‐starts
- 58. Connor SR. Development of hospice and palliative care in the United States. Omega (Westport). 2008;56(1):89‐99. doi: 10.2190/om.56.1.h [DOI] [PubMed] [Google Scholar]
- 59. Ministry of Health and Welfare . The 1st Comprehensive Plan for Hospice and Palliative Care (2019‐2023). 2019. (in Korean). Bogeon bogjibu. Je1cha Hoseupiseu Yeonmyeong‐uilyo Jonghabgyehoeg.
- 60. The Act on Decisions on Life‐Sustaining Treatment for Patients in Hospice and Palliative Care or at the End‐of‐Life Stage (Enforced on April 7, 2020, Act No. 17218, April 7, 2020) (in Korean).
- 61. Ministry of Health and Welfare 2024 Hospice and Palliative Care Project Guidelines (in Korean).
- 62. National Cancer Center . Current Status and Statistics. https://hospice.go.kr:8444/?menuno=53 (in Korean)
- 63. Gruber J, McGarry KM. Long‐term Care in the United States. National Bureau of Economic Research working paper No. 31881. November 2023.
- 64. Assitant Secretary for Planning and Evaluation (ASPE), US Department of Health and Human Services . National Plan to Address Alzheimer's Disease: 2023 Update. 2024. [Accessed 2024 Sep 26]. https://aspe.hhs.gov/reports/national‐plan‐2023‐update
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supporting Information


