Abstract
Background
Despite an acknowledged need to improve communication between staff and family caregivers of non-communicative care recipients (i.e., care recipients who are unable to engage in discussions with the medical staff about their treatment and care at geriatric facilities), no tools exist to measure the quality of this communication nor the extent to which family caregivers’ communication needs are met.
Objective
To develop and test two assessment tools to evaluate the extent to which family caregivers' communication needs are met according to family caregivers and for evaluating the quality of communication with the staff member most often consulted.
Design
Instrument development, including reliability, validity, and construct testing.
Settings
Five geriatric facilities (two geriatric medical centers and three nursing homes) in Israel.
Participants
128 family caregivers of non-communicative care recipients at geriatric facilities.
Methods
Based on our previous findings, we developed the Family Caregiver’s Communication Needs Questionnaire, which assesses the extent to which family caregivers' communication needs are met according to them, and the Staff-Family Quality of Communication Questionnaire, which evaluates the quality of communication with the staff member most often consulted. We conducted personal interviews with the participants to explore both tools’ items and reliability and examined the reliability and convergent validity of the Family Caregiver’s Communication Needs Questionnaire in a different sub-sample. The Family Caregiver’s Communication Needs Questionnaire’s construct was tested using a factor analysis.
Results
Both tools’ internal consistency reliabilities were high (Family Caregiver’s Communication Needs Questionnaire, Cronbach’s α = 0.92, 23 items; Staff-Family Quality of Communication Questionnaire, α = 0.86, 8 items). Exploratory factor analysis for the Family Caregiver’s Communication Needs Questionnaire reinforced the four factors that emerged in a prior study (staff's availability and attitude, relating to family caregivers' caregiving experience, clarity and reliability of information, and language barriers), accounting together for 63.3 % of the variance. Both tools demonstrated good convergent validity.
Conclusions
The Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire are valid and reliable tools for assessing the quality of staff-family communication, assisting in identifying communication strengths and weaknesses, suggesting potential interventions for improved communication, and providing outcome measures for such interventions.
Keywords: Caregiving, Geriatric facilities, Non-communicative care recipients, Staff-family communication, Scale development
What is already known.
-
•
Poor communication between geriatric facilities' staff and family caregivers is associated with negative consequences for all parties (staff, family, and care recipients).
-
•
No tools exist for assessing staff-family communication at geriatric facilities during care recipients’ stay at the facilities and the communication needs of family caregivers of non-communicative care recipients.
Alt-text: Unlabelled box
What this paper adds.
-
•
We introduced two valid and reliable tools, one to assess family-caregivers’ communication needs and the other to assess communication between staff and family of non-communicative care recipients at geriatric facilities.
-
•
The combined use of these tools can assist in identifying aspects of communication that need improvement in a specific unit.
-
•
The tools may inform interventions to improve staff-family communication and serve as outcome measures for such interventions.
Alt-text: Unlabelled box
1. Background
Many older care recipients residing in geriatric facilities are non-communicative; i.e., they are unable to effectively communicate with staff members regarding their care. Thus, the communication shifts to their family caregivers. Good staff-family communication has been associated with lower risk of psychological distress among family caregivers (Barken and Lowndes, 2018). Poor staff-family communication has been associated with increased suffering and discomfort among family caregivers and care recipients (Ibañez-Masero et al., 2019; McCarthy, 2011), greater psychological and emotional distress for family caregivers (Bidwell et al., 2017; Dionne-Odom et al., 2017; Oh, 2017), and lower family caregiver trust in staff members (Bidwell et al., 2017). Poor communication may lead to burnout (Schmitz et al., 2022) and high levels of strain among staff members (Sánchez-Martínez et al., 2020).
These negative consequences of poor staff-family communication suggest the importance of assessing it while care recipients reside in the facility to provide an opportunity to improve the communication. However, the closest existing tools evaluate communication only with physicians (Biola et al., 2007; Engelberg et al., 2006), physician care skills (Engelberg et al., 2010), a specific care conversation (Engelberg et al., 2006), a specific stage of care; e.g., the dying process (Biola et al., 2007), or a specific setting; e.g., home hospice (Ewing et al., 2013) or hospital (Brazil et al., 2013). One tool addresses family caregivers’ needs in various settings but was developed primarily in the context of cancer patients receiving home hospice care (Demiris et al., 2020). Another tool originally involved lung/respiratory patients (Engelberg et al., 2006). The development of other tools has been limited to retrospective assessments of bereaved family caregivers concerning various aspects of care (Biola et al., 2007; Brazil et al., 2013; Ewing et al., 2013). No existing tool focuses on the communication needs of family caregivers for non-communicative care recipients while they reside in the facility or on the quality of communication between such caregivers and staff members.
Given the limited available tools, it is crucial to develop reliable and valid tools for assessing staff-family communication when the care recipients are unable to communicate. Such tools should (1) elucidate family caregivers’ needs, experiences, thoughts, and beliefs concerning communication with staff; (2) identify strengths and weaknesses of staff-family care and general communication; and (3) suggest potential interventions for improving such communication. Thus, in the current study we aim to develop and examine two communication quality assessment tools for family caregivers: (1) a tool that examines the extent to which family caregivers’ needs are addressed, and (2) a tool for examining the quality of communication between family caregivers and the staff member who is most often consulted.
2. Methods
Tool Development. We developed two questionnaires to evaluate quality of communication between family caregivers of non-communicative care recipients and staff members at geriatric facilities based on our qualitative analysis of previous interviews with family caregivers in a prior study (Cohen et al., 2024). These data were used to assure the content validity of the questionnaires, as the questionnaires represent all the communication-related topics that emerged in our previous study with family caregivers (Cohen et al., 2024). The questionnaires were reviewed by four geriatric experts and five family caregivers to ensure face validity. All items in the questionnaires were reviewed by the study's team members for clarity, redundancy, and phrasing and were modified accordingly.
Family Caregiver Communication Needs Questionnaire. The Family Caregiver’s Communication Needs Questionnaire was developed to assess the extent to which family caregivers' communication needs are met according to family caregivers. See Supplementary Material Table A.1. The questionnaire is based on the communication needs reported by family caregivers in a previous study (Cohen et al., 2024): (1) availability of communication, (2) family caregivers’ information needs, (3) staff attitude, and (4) language/cultural barriers. We developed several items for each category; e.g., “when I need something, I have someone to approach;” “when I ask staff members for something, I feel as if they try to avoid me.” The first version involved 42 items rated on a 5-point Likert scale (1 = 'not at all', 5= 'to a very large extent'). The Family Caregiver’s Communication Needs Questionnaire pertains to family caregivers’ general experience on the unit in relation to all staff roles.
Staff-Family Quality of Communication Questionnaire. The Staff-Family Quality of Communication Questionnaire evaluates the quality of communication with the staff member most often interacting with the family caregiver. See Supplementary Material Table A.2. Its items elicit information concerning problems in day-to-day communication between a family caregiver and the staff member with whom the contact is most frequent, according to the family caregiver (Cohen et al., 2024). It includes eight items: the first item refers to the professional role of the staff member, such as nurse, nurse assistant, physician; Items 2–8 inquire into the nature of the parties’ communication rated on a 5-point Likert scale (1= 'not at all', 5= 'to a very large extent'), such as the level of difficulty accessing the staff member (“When you want to talk to this staff member, how difficult is it to reach her/him?”); the extent to which the family caregiver and staff member understand each other (“When you talk to this staff member, to what extent do you understand what s/he says?”); and the staff member's attitude (“When you talk to this staff member, to what extent do you feel that s/he treats you with respect?”).
Participants. Participants were 128 family caregivers of non-communicative care recipients who resided at five facilities (two geriatric medical centers and three nursing homes). Inclusion criteria were: (1) being family caregivers of care recipients aged 65 years or older residing in a geriatric facility non-rehabilitation unit for at least 2 weeks (i.e., complex care, assisted ventilation care, skilled nursing care, frail/mentally-frail care, and oncology care); (2) being family caregivers of care recipients who could not effectively communicate with staff about their condition and medical issues; and (3) the interviewee- family caregiver was 18 years old or older and could complete the interview in Hebrew.
Assessments. Sociodemographic information regarding the family caregivers (age, sex, relation to the care recipient, marital status, place of birth, religion, education, and frequency and duration of visits), and care recipients (age, sex, main diagnosis, reported dementia or major cognitive impairments, family caregiver opinion of the care recipient’s communication ability, and the degree to which communication is held with the care recipient according to the family caregiver).
Quality of Staff-Family Communication. We used the Quality of Communication questionnaire (Engelberg et al., 2006) to examine the convergent validity of the Family Caregiver’s Communication Needs Questionnaire and the Staff-Family Quality of Communication Questionnaire. The Quality of Communication questionnaire is a 13-item questionnaire rated on an 11-point scale (0 = 'the very worst,' 10 = 'the very best') to assess physician performance during a specific conversation. It includes two subscales: general communication skills and end-of-life care specific communication skills.
Procedure. This study was part of a larger study concerning staff-family communication.
All interviews were conducted face-to-face in Hebrew by trained interviewers at locations convenient to participants (e.g., geriatric facility, home, or coffee shop) and lasted 1–1.5 h. The interviewers asked the family caregiver participants pre-prepared multiple-choice questions (as detailed under “Assessments”) and marked the participants’ answers. When participants provided detailed narrative answers, these answers were transcribed verbatim during the interview. The Family Caregiver’s Communication Needs Questionnaire was the first questionnaire used, followed by the Staff-Family Quality of Communication Questionnaire and the Quality Of Communication questionnaire (Engelberg et al., 2006).
Recruitment. In the first stage, two geriatric medical centers and one nursing home provided contact information for eligible family caregivers who were contacted by research staff who explained the study and requested their consent to participate. The other nursing home preferred to contact the family caregivers directly. The second stage involved one geriatric medical center and one nursing home. When lower family caregiver participation was encountered during the second stage, facility staff approached family caregivers to request their consent to be contacted by the study team.
Data Analysis. Missing data for the Family Caregiver’s Communication Needs Questionnaire were replaced by analyzing the content of the participants' detailed verbal responses for each item. When detailed verbal responses lacked relevant data, the item was coded as a missing value.
Stage 1:
-
•
We examined the internal consistency reliabilities for the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire in the first sub-sample (n = 93 family caregivers).
-
•
We calculated Cronbach's α reliability for the full version of the Family Caregiver’s Communication Needs Questionnaire (42 items). We then excluded items whose missing values exceeded 10 % (some of these items also did not address staff-family communication and others were difficult because they involved several topics in one item) and items with a discrimination index (item-total correlation) lower than 0.3 (Benson and Clark, 1982; Domino and Domino, 2006), resulting in a shorter version of the Family Caregiver’s Communication Needs Questionnaire (30 items).
Items of the Staff-Family Quality of Communication Questionnaire did not reach >10 % missing values.
Stage 2:
-
•
We tested the internal consistency reliability of both questionnaires in the second sub-sample (n = 35).
-
•
Since the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire examine different dimensions of staff-family communication, we tested their convergent validity by examining the correlations between them.
-
•
We calculated the correlations between the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire separately with the Quality Of Communication questionnaire (Engelberg et al., 2006) and its subscales.
Stage 3: We examined the construct of the shortened Family Caregiver’s Communication Needs Questionnaire by performing an exploratory factor analysis (EFA) (principal axis factoring [PAF]) using data from both sub-samples [N = 128]. Several criteria were used to retain the factors (Hayton et al., 2004; Kaiser, 1960): (1) Factors with Eigenvalue greater than 1; (2) Items with loadings greater than 0.4; and (3) The theoretical meaning of the extracted factors. We took into account potential correlations among the factors via direct oblimin rotation. We performed several iterations to reach a simple solution.
Analyses were performed using IBM SPSS Statistics Version 29 software (IBM, Armonk, NY, USA).
3. Ethics
The study was approved by the institutional review board of Tel Aviv University (January 19, 2016) and the Helsinki Committees of Rabin Medical Center (#0139-16-RMC) and Dorot Geriatric Medical Center (#03/2016). All participants provided informed consent to participate in the study.
4. Results
4.1. Full-sample characteristics
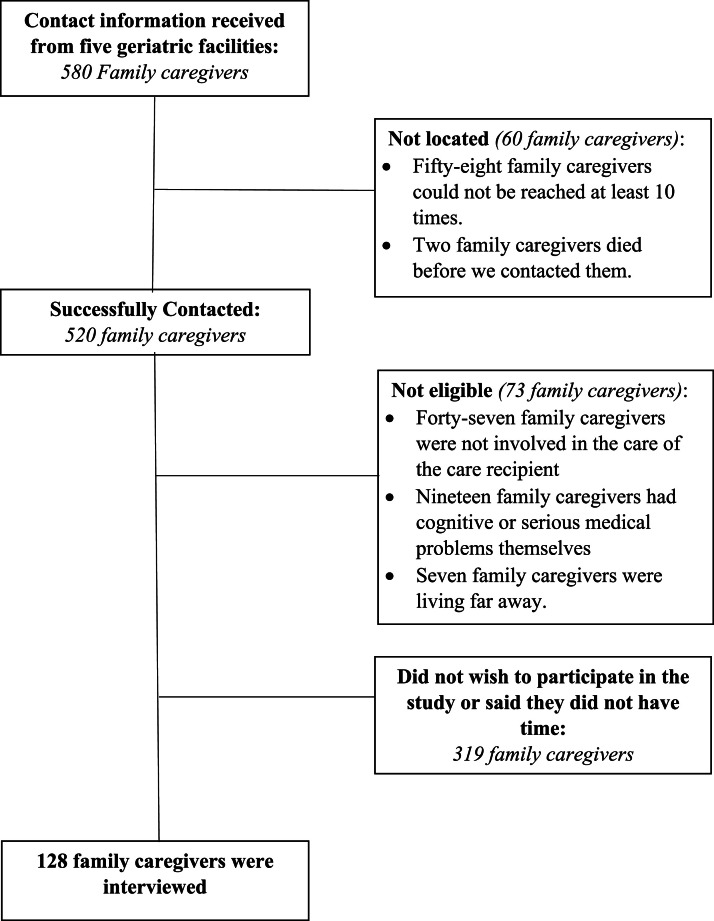
We received contact information for 580 eligible family caregivers. See Fig. 1. About a fifth of them (22.9 %) could not be reached or were not eligible to participate. Of the family caregivers eligible to participate, 71.4 % did not wish to participate or did not have time to do so. This resulted in a response rate of 28.6 % (128 family caregivers).
Fig. 1.
Enrollment of Study Participants for Questionnaires Development.
We interviewed 128 family caregivers (one family caregiver for each care recipient). See Table 1. The first stage, during which both tools were developed and tested, included 93 family caregivers. The second, during which the construct of the Family Caregiver’s Communication Needs Questionnaire and the convergent validity of both tools were tested, involved 35 family caregivers.
Table 1.
Characteristics of Older Care Recipients and Family Caregivers (N = 128) From Five Geriatric Facilities.
| Characteristics | First Sub-Sample: Questionnaires Development Stage (n = 93 family caregivers) Mean (SD) / n ( %) |
Second Sub-Sample: Questionnaires Examination Stage (n = 35 family caregivers) Mean (SD) / n ( %) |
Full Sample (N = 128 family caregivers) Mean (SD) / n ( %) |
|---|---|---|---|
| Facility type ( % older care recipients) * Geriatric medical centers Nursing homes |
65 (69.9 %)1 28 (30.1 %)3 |
20 (57.1 %)2 15 (42.9 %)4 |
85 (66.4 %) 43 (33.6 %) |
| Unit type ( % older care recipients) * Complex Nursing Care Assisted Ventilation Skilled Nursing Care Frail/ Mentally frail Oncology |
25 (26.9 %) 29 (31.2 %) 17 (18.3 %) 17 (18.3 %) 5 (5.4 %) |
10 (28.6 %) 10 (28.6 %) 15 (42.9 %) - - |
35 (27.3 %) 39 (30.5 %) 32 (25 %) 17 (13.3 %) 5 (3.9 %) |
| Care recipient | |||
| Age (years) [Range] | 80.9 (8.8) [65–99] | 83.4 (8.9) [65–99] | 81.6 (8.9) [65–99] |
| Sex ( % women) | 55 (59.1 %) | 19 (54.3 %) | 74 (57.8 %) |
| Main diagnosis ( %): Dementia/Alzheimer's disease Lung diseases Cardiovascular accident Pressure sores Major ADL difficulties Other |
36 (38.5 %) 16 (17.2 %) 15 (16.1 %) 11 (11.8 %) 6 (6.5 %) 9 (9.7 %)5 |
9 (25.7 %) 7 (20.0 %) 4 (11.4 %) 4 (11.4 %) 7 (20.0 %) 4 (11.4 %)6 |
45 (35.2 %) 23 (17.9 %) 19 (14.8 %) 15 (11.7 %) 13 (10.2 %) 13 (10.2 %) |
| Reported dementia or major cognitive impairments ( % yes) |
79 (94.1 %)7 |
29 (82.9 %) |
108 (90.8 %)8 |
| Care recipient ability to communicate about care according to the family caregiver ( %): Not at all To a small extent |
60 (64.5 %) 33 (35.5 %) |
20 (57.2 %) 11 (31.4 %) |
80 (62.5 %) 48 (37.5 %) |
| Communication conducted with care recipient according to the family caregiver ( %): Not at all To a small extent |
73 (78.5 %) 20 (21.5 %) |
27 (77.1 %) 7 (20.0 %) |
100 (78.1 %) 28 (21.9 %) |
| Length of stay in current care facility (months) Median (Interquartile range; IQR) [Range] |
10 (IQR, 2–24) [.5–144] |
6 (IQR, 1.5–36) [.8–84] |
9 (IQR, 2–24) [.5–144] |
| Family Caregiver | |||
| Age (years) [Range] | 56.6 (12.8) [21–93] | 58.6 (11.7) [33–83.5] | 57.1 (12.5) [21–93] |
| Sex ( % women) | 54 (58.1 %) | 25 (71.4 %) | 79 (61.7 %) |
| Relationship to care recipient ( %) Child Spouse Other |
72 (77.4 %) 18 (19.4 %) 3 (3.2 %)9 |
29 (82.9 %) 3 (8.6 %) 3 (8.6 %)10 |
101 (78.9 %) 21 (16.4 %) 6 (4.7 %) |
| Marital status ( % married/ in a relationship) | 70 (75.3 %) | 30 (85.7 %) | 100 (78.1 %) |
| Place of birth ( % Israel) | 65 (69.9 %) | 25 (71.4 %) | 90 (70.3 %) |
| Religion ( % Jews) | 90 (96.6 %) | 35 (100.0 %) | 125 (97.7 %) |
| Years of education [Range] | 14.7 (2.9) [8–22] | 15.17 (2.3) [12–21] | 14.8 (2.8) [8–22] |
| Frequency of visits ( %) Once a day or more Once to several times a week Once to several times a month Less than once a month |
32 (34.5 %) 56 (60.2 %) 3 (3.2 %) 2 (2.1 %) |
13 (37.1 %) 20 (57.1 %) 2 (5.7 %) - |
45 (35.1 %) 76 (59.3 %) 5 (3.9 %) 2 (1.7 %) |
| Duration of visits (minutes) Median (IQR) [Range] |
90 (IQR, 60–180) [10–720] |
60 (IQR, 60–120) [10–360] |
90 (IQR, 60–175) [10–720] |
Note: SD: Standard Deviation; ADL: Activities of Daily Living; IQR: Interquartile range; N: number of family caregivers in the total sample; n: number of family caregivers in the subsamples).
Two geriatric medical centers
One geriatric medical center.
Two nursing homes.
One nursing home.
Cancer, cardiovascular diseases, gastrointestinal disorders, sepsis.
Cardiovascular diseases, gastrointestinal disorders, diabetes mellitus.
n = 84.
n = 119.
One cousin, one granddaughter and one niece.
One sibling and two daughters in law.
Statistically significant differences between the two subsamples were found for the following variables: Facility type (X24 = 58.4, p = 6.111E-12) and Unit type X211 = 57.5, p = 2.658E-08).
The family caregivers in the full sample tended to be Jewish, married, born in Israel, women, with a mean of 57.1 years of age. Most of the family caregivers were the children of the care recipients. The vast majority of family caregivers reported visiting the care recipients at least weekly, with a median visit duration of 90 min.
Over half of the care recipients in the full sample were women (57.8 %). Care-recipients had a mean age of 81.6 years. They resided at the facilities for periods between two weeks and 144 months. All family caregivers described the care recipients as unable to communicate concerning their care or able to communicate only to a small extent. In describing the communication limitations of the care recipients, family caregivers reported communication via facial expressions of physical pain, happiness when seeing loved-ones, or indications of agreement or disagreement in response to simple yes/no questions. All family caregivers reported that communication about care or treatment either was not conducted with care recipients or conducted with them only to a small extent. Most family caregivers’ descriptions of such communication involved staff members informing the care recipient what action the staff member was going to undertake for the care recipient.
When comparing the first and second sub-samples, statistically significant differences were found regarding facility and unit types but not regarding demographic, functional, and medical variables (See Table 1 footnote).
Stage 1: Development of the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire
Piloting the First Versions
The original versions of both questionnaires were piloted in the interviews using the first five participants, whose feedback provided the basis for revising the wording of some items to improve clarity but did not warrant the deletion of any items outright.
Examining Internal Consistency Reliability
Family Caregiver’s Communication Needs Questionnaire. The original version consisted of 42 items. Its internal consistency reliability was 0.93 (n = 47 due to missing values) after reverse-coding the responses to 17 negative items so that higher scores represented better communication. Exclusion of 12 items (six due to not addressing staff-family communication or being too difficult to answer and six due to discrimination indices lower than 0.3) resulted in Cronbach's α of 0.93 (n = 87) for 30 items.
Staff-Family Quality of Communication Questionnaire. There were no missing values, and Cronbach's α was 0.79 (n = 93). One item could have been removed to increase the reliability to 0.86. However, it was crucial to include that item because it involved the level of difficulty the family caregiver encountered in trying to reach the specific staff member.
Stage 2: Testing both questionnaires in a second sub-sample
We examined the internal consistency reliability of the Family Caregiver’s Communication Needs Questionnaire (30 items) and the Staff-Family Quality of Communication Questionnaire in a different sub-sample of 35 family caregivers. Table 1 presents the characteristics of these sub-samples). Reliabilities of both questionnaires were higher than 0.86. See Table 2.
Table 2.
Exploratory Factor Analysis of the Family Caregiver’s Communication Needs Questionnaire - Short Version (23 items): Factors, Items, Eigenvalue, Variances and Reliabilities.
| Items | Communalities | Factor 1 (Loadings)1 | Factor 2 (Loadings)2 | Factor 3 (Loadings)3 | Factor 4 (Loadings)4 |
|---|---|---|---|---|---|
| 1. Staff members treat me with respect. | 0.67 | 0.77 | |||
| 2. When I visit, there are available nurses I can approach. | 0.53 | 0.77 | |||
| 3. When I ask staff members for something, I feel as if they try to avoid me.5 | 0.64 | 0.74 | |||
| 4. I ask for something and don’t get a response.5 | 0.52 | 0.70 | |||
| 5. I feel that staff members listen when I talk to them. | 0.71 | 0.68 | |||
| 6. When I need something, I have someone to approach. | 0.57 | 0.66 | |||
| 7. When I approach staff members, they treat me as if I’m interrupting them.5 | 0.50 | 0.63 | |||
| 8. I feel as if staff members’ answers are meant only to ‘blow me off.’5 | 0.53 | 0.63 | |||
| 9. I’m afraid to criticize staff members out of concern for the wellbeing of my family member.5 | 0.44 | 0.61 | |||
| 10. I receive responses to my requests. | 0.50 | 0.61 | |||
| 11. When I approach staff members, they treat me with patience. | 0.69 | 0.56 | |||
| 12. I feel as if staff members talk to me as an equal. | 0.49 | 0.39 | |||
| 13. Staff members provide the best service they can. | 0.48 | 0.35 | |||
| 14. Staff members relate to me, my feelings, and my emotions. | 0.86 | 0.96 | |||
| 15. I feel as if staff members care about me and what I’m going through. | 0.71 | 0.77 | |||
| 16. Staff members are attentive to my experience as a family caregiver. | 0.59 | 0.74 | |||
| 17. I feel as if staff members understand that for me, my family member is the most important thing. | 0.47 | 0.44 | |||
| 18. I feel as if staff members act with full transparency. | 0.81 | 0.83 | |||
| 19. Sometimes I feel as if staff members don’t tell me the whole truth.5 | 0.54 | 0.72 | |||
| 20. I think staff members tell me what is really going on - whether it’s good or bad. | 0.61 | 0.66 | |||
| 21. I’m concerned that information regarding my family member or her/his care is being hidden from me.5 | 0.42 | 0.66 | |||
| 22. I think there’s a language barrier between me and staff members.5 | 0.36 | 0.52 | |||
| 23. Some staff members don’t speak Hebrew, and it is impossible to communicate with them.5 | 0.22 | 0.43 | |||
| Eigenvalue | 9.23 | 1.98 | 1.78 | 1.58 | |
| % of variance | 40.13% | 8.6% | 7.7% | 6.9% | |
| Cronbach's α | Total scale: 0.92 (23 items; 125 family caregivers) | 0.92 (13 items; 126 family caregivers) | 0.84 (4 items; 128 family caregivers) | 0.82 (4 items; 127 family caregivers) | 0.616 (2 items; 128 family caregivers) |
The extraction method was principal axis factoring with an oblique (direct oblimin with Kaiser normalization) rotation. Rotation converged in six iterations.
Factor 1: Staff's availability and attitude when being approached.
Factor 2: Relating to family caregivers' caregiving experience.
Factor 3: Clarity of information and reliability.
Factor 4: Language barriers.
Scores of these items were inverted prior to data analysis so that higher scores indicate higher quality of communication.
Spearman-Brown coefficient.
Stage 3: Examining the construct of the Family Caregiver’s Communication Needs Questionnaire
We examined the construct of the Family Caregiver’s Communication Needs Questionnaire (30 items) by performing an EFA (PAF) using data from both sub-samples (N = 128). The Kaiser-Meyer-Olkin (KMO) measure of sampling adequacy was greater than 0.5 (KMO= 0.86), and the Bartlett's test of sphericity was statistically significant (p = 2.278E-216), both results implying suitability of the data for EFA.
After we omitted seven items with loadings lower than 0.4, the EFA yielded four interpretable factors regarding family caregivers’ communication needs in the context of communication with staff members, accounting together for 63.3 % of the variance: Staff's availability and attitude when being approached (accounting for 40.1 %), Relating to family caregivers' caregiving experience (8.6 %), Clarity and reliability of information provided by staff (7.7 %), and Language barriers (6.9 %). See Table 2. The further shortened version of the Family Caregiver’s Communication Needs Questionnaire (four-factor solution) comprised 23 items with moderate to very good discrimination indices (0.44 - 0.86), except for the two items regarding language barriers (0.36, 0.22).
Three factors had good internal consistency reliabilities: Staff's availability and attitude when being approached (α = 0.92; 13 items; 126 family caregivers); Family caregivers' caregiving experience (α = 0.84; 4 items; 128 family caregivers); Clarity of information and reliability (α = 0.82; 4 items; 127 family caregivers). The language barrier factor involved only two items. Therefore, its reliability was calculated as a Spearman-Brown coefficient (Eisinga et al., 2013) (0.61; two items, 128 family caregivers). We retained this factor despite its low reliability and its inclusion of only two items because family caregivers reported that language posed a serious communication barrier, especially in nursing homes. In our previous study (Cohen et al., 2024), family caregivers attributed this barrier to staff members’ lack of Hebrew proficiency (for example, nursing assistants from Sudan and Eritrea) and staff members who preferred to speak among themselves in a language other than Hebrew, even in the presence of people who did not understand that language. These issues posed a challenge to staff-family communication, and foreclosed the possibility of effective communication in many cases (Cohen et al., 2024).
4.2. Convergent validity of both questionnaires
Convergent validities of the final version of the Family Caregiver’s Communication Needs Questionnaire and the Staff-Family Quality of Communication Questionnaire were tested by calculating correlations between them and between each of them and the Quality of Communication questionnaire (Engelberg et al., 2006). See Table 3. Most correlations of the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire with the Quality of Communication questionnaire (Engelberg et al., 2006, including its subscales) were of moderate to high, but not perfect, magnitude (r = 0.43 to r = 0.75), indicating good convergent validity. The correlation between the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire was high (r = 0.70, p = 4.260E-20), suggesting that they both fit within a close, but not identical, theoretical concept.
Table 3.
Convergent Validity of the Family Caregiver’s Communication Needs Questionnaire - Short Version (23 items) and the Staff-Family Quality of Communication Questionnaire: Pearson Correlations with the Quality of Communication Questionnaire (N=128 family caregivers).
| Scale | Family Caregiver’s Communication Needs Questionnaire | Staff-Family Quality of Communication Questionnaire |
|---|---|---|
| Staff-Family Quality of Communication Questionnaire | 0.70 (p = 4.260E-20) | |
| Quality of Communication questionnaire - Total score | 0.62 (p = 6.917E-15) | 0.52 (p = 5.158E-10) |
| Quality of Communication questionnaire - General Communication | 0.71 (p = 1.078E-20) | 0.75 (p = 3.482E-24) |
| Quality of Communication questionnaire - End-of-Life Communication | 0.43 (p = 2.996E-07) | 0.29 (p = 0.001) |
5. Discussion
The questionnaires we developed and tested, the Family Caregiver’s Communication Needs Questionnaire and the Staff-Family Quality of Communication Questionnaire, assessed the quality of communication between staff members and family caregivers of non-communicative care recipients who resided at geriatric facilities. The four factors of the Family Caregiver’s Communication Needs Questionnaire accounted together for a notable part of the variance (63.3 %), and reflected the communication needs of family caregivers that emerged in a prior study: Staff's availability and attitude when approached; Relating to family caregivers' caregiving experience; Clarity and reliability of information provided by staff; and Language barriers (Cohen et al., 2024). In contrast to the literature (Candrian et al., 2018; Collins et al., 2018; Soong et al., 2020) and as reflected in the majority of existing tools (Biola et al., 2007; Brazil et al., 2013; Engelberg et al., 2006) in which communication needs usually equaled information needs, the Family Caregiver’s Communication Needs Questionnaire broadens the inquiry by including other important dimensions, such as staff availability, family caregivers’ caregiving experiences, and language barriers. Even the Caregiver-Centered Communication Questionnaire does not inquire into staff availability or language barriers (Demiris et al., 2020).
Existing tools provide a fragmented and incomplete picture of communication; e.g., assessing only specific dimensions, such as staff's perceptions of relationships with family caregivers (Bauer et al., 2014) or family caregivers' support needs during palliative care at home (Ewing and Grande, 2013); inquiry that is retrospective (Biola et al., 2007; Brazil et al., 2013; Ewing and Grande, 2013) or limited to a specific stage of care (Biola et al., 2007); and inquiry only about a specific conversation with a physician (Engelberg et al., 2006). In contrast, the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire provide a more comprehensive assessment of quality of staff-family communication on two levels – a general perspective, including all staff (the Family Caregiver’s Communication Needs Questionnaire) and an individual perspective concerning a specific staff member (the Staff-Family Quality of Communication Questionnaire).
On the general – all staff – level, the Family Caregiver’s Communication Needs Questionnaire evaluates quality of communication via family caregivers’ perceptions of the degree to which their communication needs are met by the geriatric staff members, while the Staff-Family Quality of Communication Questionnaire assesses the quality of family caregivers’ regular communication with the staff member most often consulted. In contrast to the Quality of Communication questionnaire (Engelberg et al., 2006), the Staff-Family Quality of Communication Questionnaire is not about whether a physician made eye-contact with the family caregiver or used words the family caregiver could understand in a specific conversation but about the core elements of the parties’ communications. These elements involve the extent to which (a) the family caregiver and staff member understand each other and (b) the staff member acts with respect, care and patience. While the correlation between the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire was high, it was not perfect, suggesting that they fit in similar, but not identical, constructs.
Clinically, the combined use of the two questionnaires provides a comprehensive view of staff-family communication in a specific unit and can assist in identifying aspects of communication that need to be improved. The Staff-Family Quality of Communication Questionnaire is much shorter than the Family Caregiver’s Communication Needs Questionnaire and may serve as a preliminary screening tool. The Family Caregiver’s Communication Needs Questionnaire can be used to provide staff members with detailed information about aspects of communications that need to be improved. Given the harmful consequences of poor staff-family communication for family caregivers (Dionne-Odom et al., 2017; Nipp et al., 2016; Oh, 2017) and staff (Sánchez-Martínez et al., 2020; Schmitz et al., 2022), the two tools are important for assessing and improving staff-family communication and can serve as a crucial function for all stakeholders.
Empirically, both the Family Caregiver’s Communication Needs Questionnaire and the Staff-Family Quality of Communication Questionnaire demonstrated good psychometric properties when tested with a sample different from that used in developing the original versions. The Family Caregiver’s Communication Needs Questionnaire and three of its factors had high internal consistency reliability (α = 0.82–0.92) and satisfactory convergent validity (r = 0.43-0.71). The language barrier factor, which includes only two items, presented satisfactory reliability (r = 0.61). The Staff-Family Quality of Communication Questionnaire had good reliability (α = 0.86) and good convergent validity (r = 0.29–0.75).
6. Limitations
The vast majority of participants were Jewish Israelis. Thus, generalizability of the findings needs to be established. Future research should include geriatric facilities serving care recipients of other regions, religions, languages, and cultures. Additionally, the sample size was not sufficient to conduct a confirmatory factor analysis to check the construct validity of the Family Caregiver’s Communication Needs Questionnaire’s subscales, thus warranting further examination of its validity with larger samples. Since the study was conducted in Hebrew, no psychometrics evaluations were conducted for the English versions of the tests. Future researchers should examine the psychometrics of the English versions.
With regard to care recipients’ communication ability, the degree of this ability is a continuous variable, and, therefore, the utility of the questionnaires in cases of different levels of communication ability by care-recipients should be examined in future research.
7. Conclusions
The Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire provide valid, reliable, and practical means for understanding and improving the quality of communication between staff and family caregivers of non-communicative care recipients residing at geriatric facilities. These tools can be used as outcome measures in interventions for improving staff-family communication and as clinical tools that identify communication strengths and weaknesses.
In contrast to existing tools, the Family Caregiver’s Communication Needs Questionnaire and Staff-Family Quality of Communication Questionnaire were designed based on data gained through interviews with family caregivers in a previous study (Cohen et al., 2024), rather than relying on researchers’ perceptions of family caregiver needs. Additionally, unlike other questionnaires (Biola et al., 2007; Brazil et al., 2013; Engelberg et al., 2006), the two questionnaires we developed were designed for family caregivers to complete during the care recipients’ residence at a geriatric facility, thus providing staff members with data pertinent to concurrent decisions that increases the opportunity to better meet family caregivers’ communication needs and provide improved care.
CRediT authorship contribution statement
Rinat Cohen: Writing – review & editing, Writing – original draft, Visualization, Validation, Supervision, Software, Project administration, Methodology, Investigation, Formal analysis, Data curation, Conceptualization. Gal Maydan: Writing – review & editing, Supervision, Investigation. Shai Brill: Writing – review & editing, Resources, Investigation, Funding acquisition. Jiska Cohen-Mansfield: Writing – review & editing, Visualization, Validation, Supervision, Software, Resources, Project administration, Methodology, Investigation, Funding acquisition, Conceptualization.
Declaration of competing interest
None.
Acknowledgments
Funding
This work was supported by the Israel’s Ministry of Science and Technology [grant number 3–12807]; and the Minerva Foundation [grant number 3158329500]. The funders did not exercise any role in the conduct of the study or any decision regarding its publication.
Acknowledgments
The authors would like to express their gratitude to the geriatric institutions and their staff that collaborated with our research team, and the family caregivers who shared their experiences with us at a time that was very challenging for many of them.
Footnotes
Supplementary material associated with this article can be found, in the online version, at doi:10.1016/j.ijnsa.2025.100333.
Appendix. Supplementary materials
References
- Barken R., Lowndes R. Supporting family involvement in long-term residential care: promising practices for relational care. Qual. Health Res. 2018;28(1):60–72. doi: 10.1177/1049732317730568. [DOI] [PubMed] [Google Scholar]
- Bauer M., Fetherstonhaugh D., Lewis V. Attitudes towards family-staff relationships in Australian residential aged care settings: development and psychometric evaluation of the 'Family and Staff Relationship Attitude Tool' (FASRAT) Aust. J. Ageing. 2014;33(3):170–173. doi: 10.1111/ajag.12006. [DOI] [PubMed] [Google Scholar]
- Benson J., Clark F. A guide for instrument development and validation. Am. J. Occupat. Therapy. 1982;36(12):789–800. doi: 10.5014/ajot.36.12.789. [DOI] [PubMed] [Google Scholar]
- Bidwell J.T., Lyons K.S., Mudd J.O., Gelow J.M., Chien C.V., Hiatt S.O., Grady K.L., Lee C.S. Quality of life, depression, and anxiety in Ventricular Assist device therapy: longitudinal outcomes for patients and Family caregivers. J. Cardiovasc. Nurs. 2017;32(5):455–463. doi: 10.1097/JCN.0000000000000378. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Biola H., Sloane P.D., Williams C.S., Daaleman T.P., Williams S.W., Zimmerman S. Physician communication with family caregivers of long-term care residents at the end of life. J. Am. Geriatr. Soc. 2007;55(6):846–856. doi: 10.1111/j.1532-5415.2007.01179.x. [DOI] [PubMed] [Google Scholar]
- Brazil K., Cupido C., Taniguchi A., Howard M., Akhtar-Danesh N., Frolic A. Assessing family members' satisfaction with information sharing and communication during hospital care at the end of life. J. Palliat. Med. 2013;16(1):82–86. doi: 10.1089/jpm.2012.0362. [DOI] [PubMed] [Google Scholar]
- Candrian C., Tsantes A., Matlock D.D., Tate C., Kutner J.S. I just need to know they are going to do what they say they’re going to do with my mom.” understanding hospice expectations from the patient, caregiver and admission nurse perspective. Patient Educ. Couns. 2018;101(11):2025–2030. doi: 10.1016/j.pec.2018.08.005. [DOI] [PubMed] [Google Scholar]
- Cohen R., Maydan G., Brill S., Cohen-Mansfield J. Communications needs of family caregivers of geriatric unit residents at end-of-life. Gerontologist. 2024;65(2):gnae174. doi: 10.1093/geront/gnae174. [DOI] [PubMed] [Google Scholar]
- Collins A., McLachlan S.A., Philip J. How should we talk about palliative care, death and dying? A qualitative study exploring perspectives from caregivers of people with advanced cancer. Palliat. Med. 2018;32(4):861–869. doi: 10.1177/0269216317746584. [DOI] [PubMed] [Google Scholar]
- Demiris G., Ganz F.D., Han C.J., Pike K., Oliver D.P., Washington K. Design and preliminary testing of the caregiver-centered communication questionnaire (CCCQ) J. Palliat. Care. 2020;35(3):154–160. doi: 10.1177/0825859719887239. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dionne-Odom J.N., Demark-Wahnefried W., Taylor R.A., Rocque G.B., Azuero A., Acemgil A., Martin M.Y., Astin M., Ejem D., Kvale E., Heaton K., Pisu M., Partridge E.E., Bakitas M.A. The self-care practices of family caregivers of persons with poor prognosis cancer: differences by varying levels of caregiver well-being and preparedness. Support Care Cancer. 2017;25(8):2437–2444. doi: 10.1007/s00520-017-3650-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Domino G., Domino M.L. Cambridge University Press; 2006. Psychological Testing: An Introduction. [Google Scholar]
- Eisinga R., Grotenhuis M.t., Pelzer B. The reliability of a two-item scale: pearson, Cronbach, or Spearman-Brown? Int. J. Public Health. 2013;58:637–642. doi: 10.1007/s00038-012-0416-3. [DOI] [PubMed] [Google Scholar]
- Engelberg R., Downey L., Curtis J.R. Psychometric characteristics of a quality of communication questionnaire assessing communication about end-of-life care. J Palliat Med. 2006;9(5):1086–1098. doi: 10.1089/jpm.2006.9.1086. [DOI] [PubMed] [Google Scholar]
- Engelberg R.A., Downey L., Wenrich M.D., Carline J.D., Silvestri G.A., Dotolo D., Nielsen E.L., Curtis J.R. Measuring the quality of end-of-life care. J Pain Symptom Manag. 2010;39(6):951–971. doi: 10.1016/j.jpainsymman.2009.11.313. [DOI] [PubMed] [Google Scholar]
- Ewing G., Brundle C., Payne S., Grande G. The Carer Support Needs Assessment Tool (CSNAT) for use in palliative and end-of-life care at home: a validation study. J. Pain Symptom Manage. 2013;46(3):395–405. doi: 10.1016/j.jpainsymman.2012.09.008. [DOI] [PubMed] [Google Scholar]
- Ewing G., Grande G. Development of a Carer support Needs Assessment tool (CSNAT) for end-of-life care practice at home: a qualitative study. Palliat. Med. 2013;27(3):244–256. doi: 10.1177/0269216312440607. [DOI] [PubMed] [Google Scholar]
- Hayton J.C., Allen D.G., Scarpello V. Factor retention decisions in exploratory factor analysis: a tutorial on parallel analysis. Organ Res. Methods. 2004;7(2):191–205. [Google Scholar]
- Ibañez-Masero O., Carmona-Rega I.M., Ruiz-Fernández M.D., Ortiz-Amo R., Cabrera-Troya J., Ortega-Galán Á.M. Communicating health information at the end of life: the caregivers' Perspectives. Int. J. Environ. Res. Public Health. 2019;16(14) doi: 10.3390/ijerph16142469. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kaiser H.F. The application of electronic computers to factor analysis. Educ. Psychol. Meas. 1960;20(1):141–151. [Google Scholar]
- McCarthy B. Family members of patients with cancer: what they know, how they know and what they want to know. Eur. J. Oncol. Nurs. 2011;15(5):428–441. doi: 10.1016/j.ejon.2010.10.009. [DOI] [PubMed] [Google Scholar]
- Nipp R.D., El-Jawahri A., Fishbein J.N., Gallagher E.R., Stagl J.M., Park E.R., Jackson V.A., Pirl W.F., Greer J.A., Temel J.S. Factors associated with depression and anxiety symptoms in family caregivers of patients with incurable cancer. Ann. Oncol. 2016;27(8):1607–1612. doi: 10.1093/annonc/mdw205. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oh Y.S. Communications with health professionals and psychological distress in family caregivers to cancer patients: a model based on stress-coping theory. Appl. Nurs. Res. 2017;33:5–9. doi: 10.1016/j.apnr.2016.09.008. [DOI] [PubMed] [Google Scholar]
- Sánchez-Martínez I., Vilar R., Irujo J., Ulsamer D., Cano D., Casaca Soares C., Acevedo Á., Jerez-Roig J., Celdrán M. Effectiveness of the validation method in work satisfaction and motivation of Nursing Home care professionals: a literature review. Int. J. Environ Res. Public Health. 2020;18(1) doi: 10.3390/ijerph18010201. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Schmitz A.C., da Rosa Witeck C., de Oliveira J.M.D., Clemons M., Paiva C.E., Porporatti A.L., de Luca Canto G., Grosseman S. Coping strategies to prevent or reduce stress and burnout among oncology physicians: a systematic review. Braz. J. Oncol. 2022;18 continuous publication. [Google Scholar]
- Soong A., Au S.T., Kyaw B.M., Theng Y.L., Tudor Car L. Information needs and information seeking behaviour of people with dementia and their non-professional caregivers: a scoping review. BMC Geriatr. 2020;20(1):61. doi: 10.1186/s12877-020-1454-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.