Abstract
Behavioral health integration (BHI) within primary care settings is shown to improve outcomes. However, achieving BHI requires identifying best practices and a reliable tool that can be used to measure existing levels and progress toward BHI. The objective of this study was to develop and apply a conceptual framework to measure BHI, test the approach, and examine challenges to achieving BHI. Surveys and interviews were conducted with key informants within 17 designated public hospitals in California at the midpoint of participating in a 5-year project to establish BHI. A framework and coding methodology were developed to assess BHI best practices at each hospital. BHI status was assessed in the domains of infrastructure and process. Each domain included 5 themes such as electronic health record integration and functionality (infrastructure) and interprovider communication (process). Themes were assessed using a 6-point scale for various activities under a theme and associated weights. Theme-specific values were standardized from 0% to 100% to compare BHI scores between hospitals. Overall progress toward BHI ranged from scores of 52% to 83% (mean 63%) and indicated greater contribution of infrastructure versus process implementation. Within the infrastructure domain, scores were higher for having institutional and provider support, but lagged in establishing provider proximity. Within the process domain, scores were highest for implementation of behavioral health screening, but were frequently lower for other themes such as use of care coordination and referral processes. Further research is needed to test the robustness of this approach in other settings.
Keywords: behavioral health care, primary care, integrated health care, public hospitals
Introduction
The majority of behavioral health (BH) conditions are diagnosed and treated with medications by primary care providers (PCPs), but providers frequently lack adequate training, resources, or support to diagnose and treat such conditions.1–3 Furthermore, treatment of patients with comorbid BH conditions is more challenging and such comorbidities can exacerbate and complicate treatment for individual conditions.4 In 2001, the National Academy of Medicine report on “Crossing the Quality Chasm” identified fragmentation in care delivery as a major problem in the United States and prompted a greater focus on delivery of integrated care as a solution to improving health and lowering the costs of care.5
Evidence indicates that behavioral health integration (BHI) within primary health settings improves communication and knowledge and skill transfer between medical and behavioral health providers (BHPs), promotes more effective referrals, and facilitates increased access to care.6 BHI also improves health outcomes, particularly for patients with chronic conditions and co-occurring BH conditions, including depression, anxiety, and substance use disorders.7–9 However, BHI remains challenging because of the historical silos limiting interaction between medical and BH providers.2,10,11
Organizations seeking to implement full integration face additional challenges, including difficulties in BH staffing, obtaining resources or funding, receiving reimbursement for integrated services, and implementing the necessary health information technology to support integrated care.10,12,13 These challenges are likely more prominent in safety net health care settings, in which competing priorities, lack of resources, and higher complexity of patient care may impede the comprehensive implementation of BHI.14
BHI also occurs at different levels and along a continuum in which activities are focused solely on coordination among providers working separately in primary care and BH settings, to colocated providers who may practice separately or interact to some degree in care delivery, and to fully integrated practices that have joint infrastructure and closely collaborate to deliver care.15,16 Depending on level of BHI, it requires significant effort in developing the needed infrastructure and implementation of care processes, such as having a multidisciplinary team that includes primary care and BH providers and other relevant staff, and protocols for screening and referring patients, huddles, warm hand offs, joint care planning, and joint quality improvement activities.2,9,15–19
Numerous BH integrated care initiatives and multiple clinical practice manuals on how to integrate care are available.2,16,20–22 In a review of models of integrated care, the most common components of integration included standardized care coordination processes, patient education, care supervision by care managers, and systematic screening for BH conditions in primary care settings.19 Other BHI components include decision support, provider linkages, colocation of providers, and team-based care.16,23
However, these initiatives and practice manuals may differ in the conceptual frameworks used and elements included in integration, do not include measurement tools that home in on individual components of BHI, or lack broad applicability. In addition, studies have focused on measuring BHI implementation in specific settings such as primary care practices, community health centers, and Veterans Administration.16,24–26
Most importantly, there is a dearth of practical assessment tools that examine the level of BHI in organizations to establish the starting point or assess progress toward full BHI, particularly in primary care settings in safety net hospitals that often provide care to more complex patients.15,16 In particular, fewer assessment tools have included components of infrastructure that enable and prepare health systems to implement BHI processes.27 Such a tool is particularly of value as BHI is increasing as a priority for improving quality of care and patient outcomes.
This study addresses this gap by (1) providing a conceptual framework that measures BHI along the BHI continuum, (2) presenting a tool for measuring best practices related to infrastructure and processes that lead to BHI, (3) examining the utility of this tool in measuring BHI in the safety net hospitals providing primary care and focusing on low-income and uninsured populations, and (4) identifying challenges to BHI by participating hospitals.
Methods
Conceptual framework for assessing BHI
This study developed a conceptual framework for delivery of integrated BH care following the standard framework for levels of integrated health care and identified 3 levels including coordination, colocation, and integration with broad description of how care is delivered under each level.15,28–30 The authors examined the existing literature and expanded on this framework by identifying specific best practices in infrastructure and care delivery that could lead to full BHI and better care outcomes.16,24–26,31
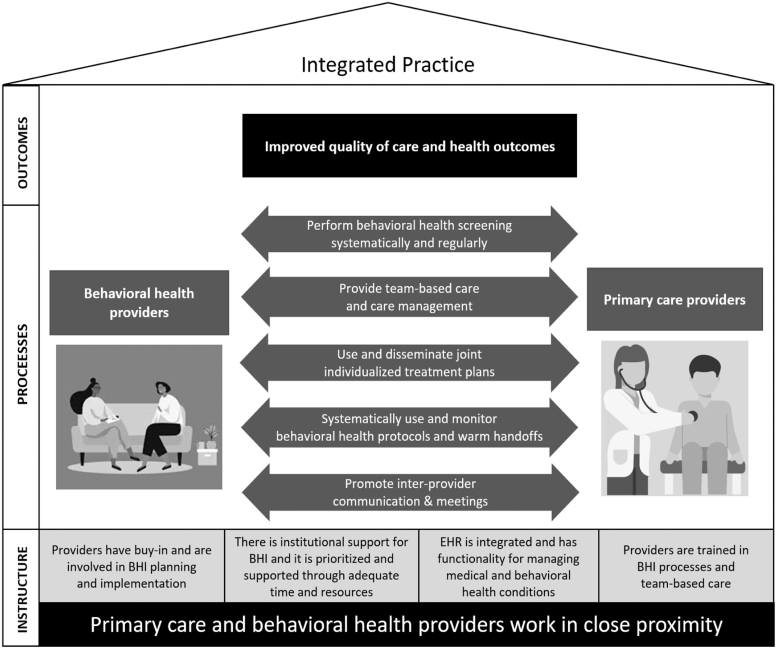
Six levels of BHI were identified, ranging from 1, minimal collaboration to, 6, full collaboration in a transformed/merged integrated practice (Fig. 1). The authors identified 5 themes for infrastructure and 5 themes for care delivery processes. Infrastructure-related themes included concepts such as provider buy-in for BHI, electronic health record (EHR) integration and functionality between primary care and BH care, and physical proximity of primary care and BHPs. Process-related themes included concepts such as implementation of team-based care and care management, use of referral methods and monitoring, and frequency of interprovider communication and meetings.
FIG. 1.
Conceptual framework for measuring BHI. BHI, behavioral health integration.
Each theme included as few as 4 and as many as 9 best practices. For example, EHR integration and functionality was measured by the following themes: joint access to EHR by BHPs and PCPs, functionality of EHR for care coordination, availability of electronic consultation tool, availability of electronic decision support tool for referrals, and availability of BH registry.32 Full details are presented in Supplementary Table S1. The authors conceptualized that BHI will lead to better care outcomes but did not examine that concept in this study.
Measurement of and challenges to BHI
Data were obtained from the evaluation of a California Section 1115(a) Medicaid Waiver demonstration program called Public Hospital Redesign and Incentives in Medi-Cal (PRIME), implemented from 2015 to 2020. A total of $7.4 billion was available to 54 public hospitals to implement projects to promote health care delivery and outcomes for achievement in pay for reporting and pay for performance metrics. One project focused on promoting BHI within primary care outpatient settings, in which all 17 designated public hospitals (DPHs) within California were required to participate.33,34
DPHs consisted of 12 county-owned and operated organizations and 5 University of California hospitals. Participating hospitals were asked to choose specific core components from a list of activities that were considered instrumental in BHI such as colocation of BHPs and PCPs within the same care settings and standardizing processes for BH care coordination and referrals.33
Key informant surveys and interviews
Data were collected using 2 online surveys of the key informants closely involved with project implementation at participating hospitals, including chief medical officers, project-level managers, and quality improvement staff. The first survey was conducted from April to May 2018 and included questions related to implementation of each BHI core component by hospitals. A follow-up survey was conducted from January to May 2019 with additional questions to clarify ambiguous responses in the first survey and to gather more specific information (questions from both surveys are provided in Supplementary Table S2).
Collectively, these surveys reflected the progress of hospitals at ∼2.5 years following PRIME implementation. Survey responses were reviewed and validated in interviews or follow-up correspondence. Interviews with key informants were conducted after the first survey from June to August 2018. Key informants were asked to expand on or clarify their survey responses. Interviews were transcribed and analyzed using NVivo to identify information pertaining to implementation of BHI.
A coding methodology was developed to measure BHI from survey responses following the 6 levels identified in the study's conceptual framework with level 1 representing the lowest BHI and level 6 identifying the highest BHI (Supplementary Table S1). For example, within the theme of EHR access and functionality, achievement of the best practice joint access to EHR by BHPs and PCPs was rated as 6 if respondents reported that primary care and BHPs had read/write access to both types of records within a single EHR, and rated as 1 if they reported that there were separate EHRs for primary care and BH records, and neither provider had read or write access to the other record.
Separate EHRs with unilateral or bilateral access by primary care and BHPs were rated at 4 and 5 accordingly. Three team members independently rated each best practice, assigned a weight (0.5 or 1.0) reflecting the contribution of the best practice to the theme, and resolved all discrepancies jointly. For example, within the her integration and functionality theme, the best practices of joint access herEHR by BHPs and PCPs, availability of electronic consultation tool, availability of decision support tool for referrals, and availability of BH registry had a weight of 1.0 and functionaliherof EHR for care coordination had a weight of 0.5.
This coding methodology was then applied to the survey data to assess BHI within each hospital. The sum of weighted ratings of best practices for each theme was divided by the number of best practices and multiplied it by 100 to create a standardized score that ranged from 1 to 100 per theme. The mean of theme scores was obtained for each domain. Therefore, each theme contributed equally to each domain and each domain contributed equally to the final BHI score, which also ranged from a low of 0 to a high of 100%.
The authors reported DPH characteristics to describe the context in which hospitals implemented the BHI project under PRIME. The final overall BHI score and the contribution of each domain to the final score were reported. The authors also reported the domain-specific scores and the contribution of each theme to the domain. An examination of additional evaluation data including hospital reports and follow-up interviews to surveys was conducted to gain insights into challenges to BHI as reported by hospitals.
The study was approved by the University of California, Los Angeles Institutional Review Board.
Results
Sample characteristics
The characteristics of hospitals are displayed in Table 1. On average, participating hospitals were relatively large institutions with 14.2 primary care and 76.0 specialty clinics, 498.9 beds, 20,841 annual discharges, and 578,553 annual outpatient visits. Many (47%) of their patients were enrolled in Medicaid managed care on average.
Table 1.
Hospital Characteristics
| Characteristic, mean (SD) | County DPH (n = 12) | UC DPH (n = 5) | Total DPH (n = 17) |
|---|---|---|---|
| Hospital capacity | |||
| Primary care facilities | 11.5 (8.1) | 20.8 (22.1) | 14.2 (13.6) |
| Specialty clinics | 58.4 (109.8) | 118.2 (84.0) | 76.0 (104.1) |
| Hospital beds | 453.0 (437.9) | 609.2 (131.0) | 498.9 (376.1) |
| Annual discharges | 17,033 (16,113) | 29,980 (7275) | 20,841 (15,123) |
| Annual outpatient visits | 475,567 (338,163) | 825,720 (222,996) | 578,553 (343,651) |
| Patient mix | |||
| % of Primary care patients enrolled in Medicaid-managed care | 62% (18.0) | 10% (10.3) | 47% (29.0) |
| Case mix index | 1.2 (0.1) | 1.8 (0.1) | 1.4 (0.3) |
County, county owned and operated; DPH, designated public hospital; SD, standard deviation; UC, University of California.
BHI scores
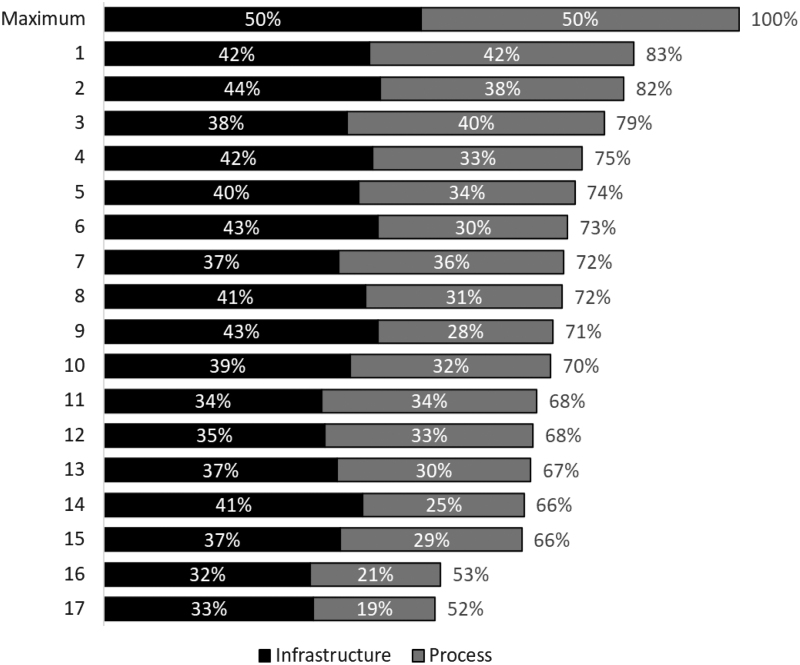
Figure 2 shows the overall BHI score ranked by the 17 hospitals in the sample and the maximum possible score for comparison. Overall scores ranged from a high of 84% to a low of 52% (mean 63%). Among hospitals with the highest ranking, the infrastructure (ranging from 42% to 33%) and process (ranging from 42% to 19%) domains frequently contributed nearly equally to the overall BHI score. However, infrastructure often contributed more toward the overall score than process among lower ranking hospitals.
FIG. 2.
Ranking of public hospitals by the overall BHI score and relative contribution of infrastructure and process scores. BHI, behavioral health integration.
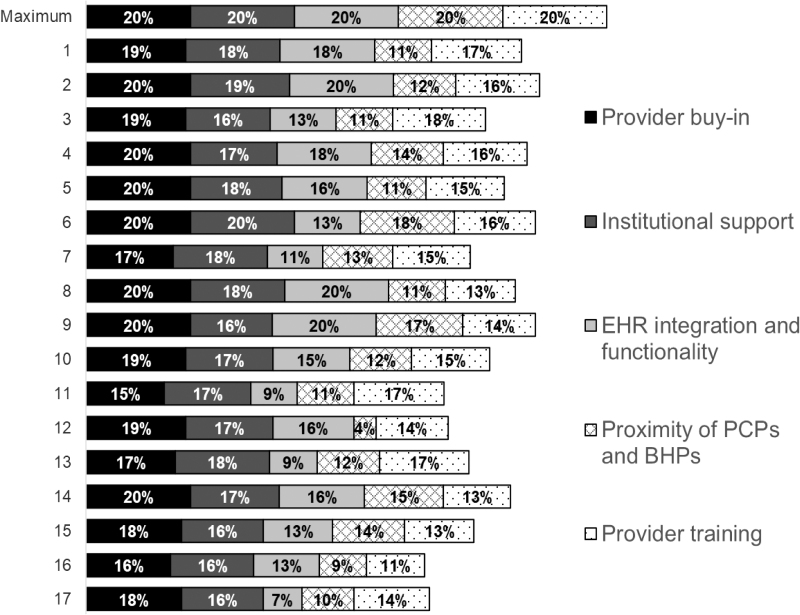
Figure 3 shows the relative contribution of themes toward the overall infrastructure score and following the rankings displayed in Figure 2. The maximum possible score for each theme was 20%. Overall, provider buy-in (ranging from 15% to 20%) and institutional support (ranging from 16% to 20%) were relatively high. Variation was greater for EHR integration (ranging from 7% to 20%), proximity of PCPs and BHPs (ranging from 11% to 18%), and training providers to provide integrated care (ranging from 11% to 18%).
FIG. 3.
Contribution of infrastructure themes to the overall infrastructure score, ranked by the hospitals' overall BHI score. BHI, behavioral health integration; PCP, primary care provider.
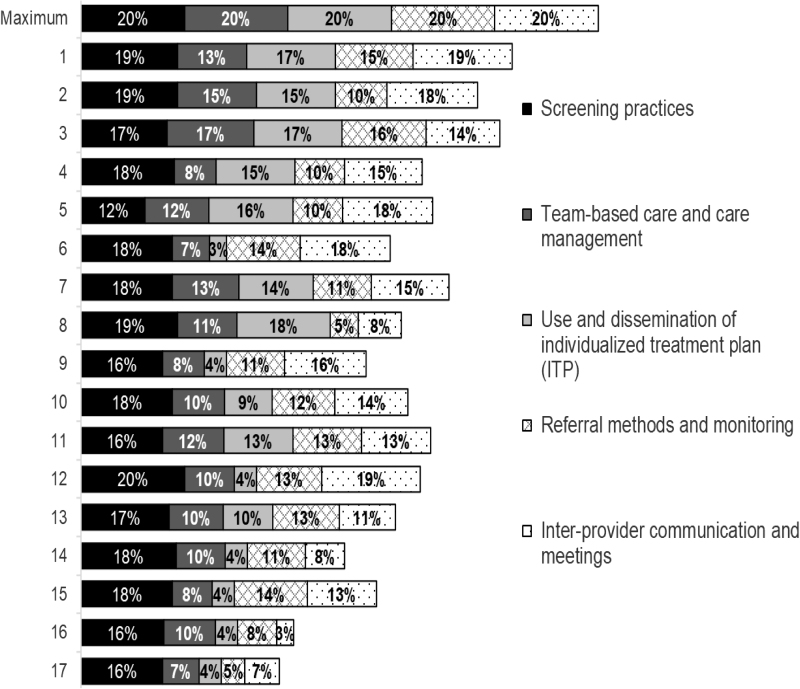
Figure 4 displays the relative contribution of themes toward the overall process score and following the rankings displayed in Figure 2. The maximum possible score for each theme was 20%. Data showed a relatively high level of screening practices (ranging from 12% to 18%) but more variations in other themes such as use and dissemination of individualized treatment plan (ranging from 4% to 18%).
FIG. 4.
Contribution of process themes to the overall process score, ranked by the hospitals' overall BHI score. BHI, behavioral health integration.
In interviews, hospitals reported challenges to BHI implementation under the infrastructure and process domains. Relating to infrastructure, hospitals reported challenges to implementing proximity of PCPs and BHPs including lack of clinic structure or space requirements, difficulty employing and retaining BHPs due to workforce shortages and turnover, substantial costs and effort associated with integrating EHRs with higher functionality, and effort to implement shared data access within and outside of the hospital system.
Challenges to implementing BHI processes included limitations in provider time to engage in integrated care, competing priorities due to high acuity of care in safety net settings, coordinating workflows across different sites, and the complexities of initiating and managing care for patients who require care and follow-up after screening positive for BH conditions.
Discussion
The authors developed a conceptual framework of BHI with 2 domains, 5 themes per domain, and 1 or more best practices per theme. This framework included a core set of best practices similar to other studies measuring BHI including measurement of specific provider-driven processes and implementing BHI best practices including screening, referral, decision support, and care management.16,24,25,27 However, this framework is one of few that measure BHI along a continuum.16
Departing from other frameworks that heavily focus on the measurement of BHI processes, this framework also includes the measurement of essential infrastructure such as EHR operability, institutional support, provider buy-in, and provider training, which are important in supporting the delivery of integrated care.27 Other research confirms these are common barriers to BHI.35
The authors developed a methodology to score BHI using this framework and measured it among 17 public hospitals that had participated in a Section 1115 Medicaid Waiver demonstration project designed to promote BHI. In general, the case mix of participating hospitals was higher than those of private hospitals, indicating that participating hospitals provided care to more complex patients.36 Nevertheless, it was found that the BHI scores per hospital ranged from 52% to 83% of the maximum possible scores that represented the highest level of BHI best practices, within ∼2.5 years after start of the project. The study also found more variation in process scores with the highest overall ranking hospitals having higher process scores than lowest ranking hospitals.
Furthermore, variations in best practices that led to the overall BHI scores in themes and subsequent domains were found. Lower scores in infrastructure themes and self-reported challenges to BHI appeared to indicate that proximity or colocation of PCPs and BHPs, and EHR integration and functionality were more difficult to accomplish for many hospitals. The findings are consistent with other research that indicates that BHI staffing is costly and challenging due to provider shortages and staff turnover.19,37 Other research also supports the findings that BHI requires significant staff time for BH management, care coordination, and implementing information technology necessary for BHI such as registries and clinical decision support.19,37–40
Some studies have noted increasing demand on providers and complexity of practicing under BHI.11,35,38,39 The findings of lower scores in process themes and self-reported challenges to BHI appeared to indicate difficulties in activities such as communication and coordination between providers specially for patients with multiple conditions.10,27 Studies in various health settings have described infrastructure barriers such as lack of sufficient resources, space, and time to meeting the increased need for treatment for BH conditions resulting from increased screening.10,12,35,38
Limitations
This study was based on self-reported data and may be subject to social desirability or recall bias as well as the knowledge of key informants providing information. The results are primarily generalizable to California public safety net hospitals that participated in a specific project and these findings may not be generalizable to solo providers and providers in other group or clinic-based settings. All likely BHI best practices may not have been included and the scoring methodology such as weights for specific activities may not be appropriate for all settings. We measured BHI before the COVID-19 pandemic and the rapid escalation in delivery of mental health care through telehealth, which may have negatively impacted hospitals' ability to deliver integrated care.
Yet, our framework is relatively robust as it includes best practices that facilitate (eg, bidirectional EHR access, electronic consultation tool) or negatively impact BHI (eg, warm handoffs, joint previsit planning or huddles) when care is provided through telehealth. Despite limitations, this study provided a comprehensive and practical conceptual framework and scoring methodology that can be modified for use in various settings.
Implications
This study has implications for research, practice, and policy. Further research is needed to test the conceptual framework and scoring methodology in other settings and to assess the robustness of the themes and activities the study has identified in measuring BHI. The findings also imply the importance of addressing challenges to integration through provision of needed resources to develop the necessary infrastructure and carry out integrated care delivery. Depending on the robustness of the approach, the tool can be used to measure the existing levels of BHI in organizations ready to promote integration, identify areas in need of improvement, and measure progress after implementation of BHI projects.
Since the data used in this study were collected, the use of telehealth as a modality for delivery of mental health care has greatly accelerated after the start of the COVID-19 pandemic. This change implies adaptations in workflows and a greater focus on best practices that promote rather than compromise BHI. These efforts include escalating EHR integration, colocation and scheduling of PCPs and BHPs for virtual handoffs, training providers on BHI when using telehealth as a care delivery modality, and providing opportunities for virtual care management and planning, and provider communication if using remote BHPs.
Furthermore, the BHI best practices identified in this study can be used by federal, state, or local policy makers to promote BHI by public and private organizations operating within the safety net. Additional research is needed to assess the outcomes of BHI in integrated practices.
Ultimately, a major advantage of measuring BHI levels is the ability to assess the impact of integration on access to care, quality of care, and patient outcomes. This approach provides a pathway to measuring the value of BHI in the broader context of the triple aim of better care, better health, and increased efficiencies.
Supplementary Material
Acknowledgments
The authors thank the key informants for participating in the surveys and interviews used for this study. In addition, we thank Leigh Ann Haley, Denisse Huerta, Maria Ditter, and Sarah Andebrhan for contributing to data collection and review.
Authors' Contributions
Prof. Pourat contributed to conceptualization, methodology, visualization, supervision, funding acquisition, and writing—original draft. Ms Tieu was involved in methodology, formal analysis, writing—original draft, and visualization. Ms Martinez carried out conceptualization, methodology, writing—review and editing, supervision, project administration, and funding acquisition.
Disclaimer
The findings and conclusions in this article are those of the authors and do not necessarily represent the views or opinions of the funder.
Author Disclosure Statement
The authors have no potential conflicts of interest to disclose.
Funding Information
This study was supported by funding from the California Department of Health Care Services (DHCS, Contract No. 16-93440). Ms Tieu was also supported by NIH/National Center for Advancing Translational Science (NCATS) UCLA CTSI TL1 TR001883.
Supplementary Material
References
- 1. Blount FA, Miller BF. Addressing the workforce crisis in integrated primary care. J Clin Psychol Med Settings 2009;16:113–119. [DOI] [PubMed] [Google Scholar]
- 2. Gerrity M. Evolving models of behavioral health integration: evidence update 2010-2015. Milbank Memorial Fund. New York, NY, 2016. [Google Scholar]
- 3. McGough PM, Bauer AM, Collins L, Dugdale DC. Integrating behavioral health into primary care. Pop Health Manage 2016;19:81–87. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Mental health and chronic diseases. Atlanta, GA: Centers for Disease Control and Prevention, 2012. [Google Scholar]
- 5. Crossing the quality chasm: a new health system for the 21st century. Washington, DC: Institute of Medicine, 2001. [PubMed] [Google Scholar]
- 6. Beil H, Feinberg RK, Patel SV, Romaire MA. Behavioral health integration with primary care: implementation experience and impacts from the State Innovation Model Round 1 States. Milbank Quart 2019;97:543–582. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Coventry PA, Hudson JL, Kontopantelis E, et al. Characteristics of effective collaborative care for treatment of depression: a systematic review and meta-regression of 74 randomised controlled trials. PLoS One 2014;9:e108114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Archer J, Bower P, Gilbody S, et al. Collaborative care for depression and anxiety problems. Cochrane Database Syst Rev 2012;10:Cd006525. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Pace CA, Uebelacker LA. Addressing unhealthy substance use in primary care. Med Clin North Am 2018;102:567–586. [DOI] [PubMed] [Google Scholar]
- 10. Fong HF, Tamene M, Morley DS, et al. Perceptions of the implementation of pediatric behavioral health integration in 3 Community Health Centers. Clin Pediatr 2019;58:1201–1211. [DOI] [PubMed] [Google Scholar]
- 11. Aggarwal M, Knifed E, Howell NA, et al. A qualitative study on the barriers to learning in a Primary Care-Behavioral Health Integration Program in an Academic Hospital: the family medicine perspective. Acad Psychiatry 2020;44:46–52. [DOI] [PubMed] [Google Scholar]
- 12. Blasi PR, Cromp D, McDonald S, et al. Approaches to behavioral health integration at high performing primary care practices. J Am Board Fam Med 2018;31:691–701. [DOI] [PubMed] [Google Scholar]
- 13. Yin I, Staab EM, Beckman N, et al. Improving primary care behavioral health integration in an academic internal medicine practice: 2-year follow-up. Am J Med Qual 2021; 36(6):379–386. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Gilmer TP, Avery M, Siantz E, et al. Evaluation of the behavioral health integration and complex care initiative in Medi-Cal. Health Aff 2018;37:1442–1449. [DOI] [PubMed] [Google Scholar]
- 15. Standard Framework for Levels of Integrated Healthcare, 2013. SAMHSA-HRSA Center for Integration Health Solutions, Washington, DC. [Google Scholar]
- 16. Goldman ML, Smali E, Richkin T, Pincus HA, Chung H. A novel continuum-based framework for translating behavioral health integration to primary care settings. Transl Behav Med 2020;10:580–589. [DOI] [PubMed] [Google Scholar]
- 17. Reiter JT, Dobmeyer AC, Hunter CL. The Primary Care Behavioral Health (PCBH) Model: an overview and operational definition. J Clin Psychol Med Settings 2018;25:109–126. [DOI] [PubMed] [Google Scholar]
- 18. Dissemination of integrated care within adult primary care settings: the Collaborative Care Model. American Psychiatric Association, Academy of Psychosomatic Medicine. Washington, DC, 2016. [Google Scholar]
- 19. Tice JA, Ollendor DA, Reed SJ, Shore KK, Weissberg J, Pearson SD. Integrating behavioral health into primary care: a technology assessment: final report. Boston, MA: Institute for Clinical and Economic Review, California Technology Assessment Forum, 2015. [Google Scholar]
- 20. Scheirer M, Leonard B, Ronan L, Boober B. Site Self Assessment Tool for the Maine Health Access Foundation Integrated Care Initiative. Augusta, Maine: Maine Health Access Foundation, 2010. [Google Scholar]
- 21. Scott VC, Kenworthy T, Godly-Reynolds E, et al. The Readiness for Integrated Care Questionnaire (RICQ): an instrument to assess readiness to integrate behavioral health and primary care. Am J Orthopsychiatry 2017;87:520–530. [DOI] [PubMed] [Google Scholar]
- 22. Waxmonsky J, Auxier A, Romero PW, Heath B. Integrated Practice Assessment Tool. Colorado Access, ValueOptions, Axis Health System. Aurora, CO, 2014. [Google Scholar]
- 23. Behavioral Health Integration Capacity Assessment (BHICA). Institute for Healthcare Improvement. The Lewin Group, Falls Church, VA. 2014. [Google Scholar]
- 24. Beehler GP, Funderburk JS, Possemato K, Vair CL. Developing a measure of provider adherence to improve the implementation of behavioral health services in primary care: a Delphi study. Implement Sci 2013;8:19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Mullin DJ, Hargreaves L, Auxier A, et al. Measuring the integration of primary care and behavioral health services. Health Serv Res 2019;54:379–389. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Pourat N, Hadler MW, Dixon B, Brindis C. One-stop shopping: efforts to integrate physical and behavioral health care in five California community health centers. Policy Brief (UCLA Center for Health Policy Research) 2015(Pb2015-1):1–11. [PubMed] [Google Scholar]
- 27. Zivin K, Miller BF, Finke B, et al. Behavioral Health and the Comprehensive Primary Care (CPC) Initiative: findings from the 2014 CPC behavioral health survey. BMC Health Serv Res 2017;17:612. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Doherty WJ, McDaniel SH, Baird MA. Five levels of primary care/behavioral healthcare collaboration. Behav Healthc Tomorrow 1996;5:25–27. [PubMed] [Google Scholar]
- 29. Blount A. Integrated primary care: organizing the evidence. Fam Syst Health 2003;21:121–133. [Google Scholar]
- 30. Parks J, Pollack D, Bartels S, Mauer B. Integrating behavioral health and primary care services: opportunities and challenges for State Mental Health Authorities. Alexandria, VA: National Association of State Mental Health Program Directors, 2005. [Google Scholar]
- 31. Pourat N, Martinez AE, Haley LA, Crall JJ. Colocation does not equal integration: identifying and measuring best practices in Primary Care Integration of Children's Oral Health Services in Health Centers. J Evid-Based Dent Pract 2020;20:101469. [DOI] [PubMed] [Google Scholar]
- 32. Faulkner LR. Implications of a needs-based approach to estimating psychiatric workforce requirements. Acad Psychiatry 2003;27:241–246. [DOI] [PubMed] [Google Scholar]
- 33. Attachment Q—PRIME Projects and Metrics Protocol. Sacramento, CA: CA Department of Health Care Services, 2016. [Google Scholar]
- 34. Pagel L, Schwartz T. The Public Hospital Redesign and Incentives in Medi-Cal (PRIME) Program: continuing California's Delivery System Transformation. Sacramento, CA: Harbage Consulting, 2017. [Google Scholar]
- 35. Wakida EK, Talib ZM, Akena D, et al. Barriers and facilitators to the integration of mental health services into primary health care: a systematic review. Syst Rev 2018;7:211. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Mendez CM, Harrington DW, Christenson P, Spellberg B. Impact of hospital variables on case mix index as a marker of disease severity. Pop Health Manage 2014;17:28–34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37. Yeung K, Richards J, Goemer E, et al. Costs of using evidence-based implementation strategies for behavioral health integration in a large primary care system. Health Serv Res 2020;55:913–923. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38. Goldman ML, Smali E, Richkin T, Pincus HA, Chung H. Implementation of behavioral health integration in small primary care settings: lessons learned and future directions. Community Mental Health J 2022;58(1):136–144. [DOI] [PubMed] [Google Scholar]
- 39. Davis MM, Balasubramanian BA, Cifuentes M, et al. Clinician staffing, scheduling, and engagement strategies among primary care practices delivering integrated care. J Am Board Fam Med 2015;28 Suppl 1(Suppl 1):S32–S40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Burke BT, Miller BF, Proser M, et al. A needs-based method for estimating the behavioral health staff needs of community health centers. BMC Health Serv Res 2013;13:245. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.