Summary
Background
Sudden cardiac arrest is a global public health problem with a mortality rate of more than 90%. Prearrest warning symptoms could be harnessed using digital technology to potentially improve survival outcomes. We aimed to estimate the strength of association between symptoms and imminent sudden cardiac arrest.
Methods
We conducted a case-control study of individuals with sudden cardiac arrest and participants without sudden cardiac arrest who had similar symptoms identified from two US community-based studies of patients with sudden cardiac arrest in California state, USA (discovery population; the Ventura Prediction of Sudden Death in Multi-Ethnic Communities [PRESTO] study), and Oregon state, USA (replication population; the Oregon Sudden Unexpected Death Study [SUDS]). Participant data were obtained from emergency medical services reports for people aged 18–85 years with witnessed sudden cardiac arrest (between Feb 1, 2015, and Jan 31, 2021) and an inclusion symptom. Data were also obtained from corresponding control populations without sudden cardiac arrest who were attended by emergency medical services for similar symptoms (between Jan 1 and Dec 31, 2019). We evaluated the association of symptoms with sudden cardiac arrest in the discovery population and validated our results in the replication population by use of logistic regression models.
Findings
We identified 1672 individuals with sudden cardiac arrest from the PRESTO study, of whom 411 patients (mean age 65·7 [SD 12·4] years; 125 women and 286 men) were included in the analysis for the discovery population. From a total of 76 734 calls to emergency medical services, 1171 patients (mean age 61·8 [SD 17·3] years; 643 women, 514 men, and 14 participants without data for sex) were included in the control group. Patients with sudden cardiac arrest were more likely to have dyspnoea (168 [41%] of 411 vs 262 [22%] of 1171; p<0·0001), chest pain (136 [33%] vs 296 [25%]; p=0·0022), diaphoresis (50 [12%] vs 90 [8%]; p=0·0059), and seizure-like activity (43 [11%] vs 77 [7%], p=0·011). Symptom frequencies and patterns differed significantly by sex. Among men, chest pain (odds ratio [OR] 2·2, 95% CI 1·6–3·0), dyspnoea (2·2, 1·6–3·0), and diaphoresis (1·7, 1·1–2·7) were significantly associated with sudden cardiac arrest, whereas among women, only dyspnoea was significantly associated with sudden cardiac arrest (2·9, 1·9–4·3). 427 patients with sudden cardiac arrest (mean age 62·2 [SD 13·5]; 122 women and 305 men) were included in the analysis for the replication population and 1238 patients (mean age 59·3 [16·5] years; 689 women, 548 men, and one participant missing data for sex) were included in the control group. Findings were mostly consistent in the replication population; however, notable differences included that, among men, diaphoresis was not associated with sudden cardiac arrest and chest pain was associated with sudden cardiac arrest only in the sex-stratified multivariable analysis.
Interpretation
The prevalence of warning symptoms was sex-specific and differed significantly between patients with sudden cardiac arrest and controls. Warning symptoms hold promise for prediction of imminent sudden cardiac arrest but might need to be augmented with additional features to maximise predictive power.
Funding
US National Heart Lung and Blood Institute.
Introduction
Out-of-hospital sudden cardiac arrest is a common cause of death with a high fatality rate (>90%).1,2 Improved methods are needed for predicting and preventing sudden cardiac arrest, and thereby reducing mortality. Approximately half of patients with sudden cardiac arrest report symptoms in the hours, days, or weeks before their cardiac arrest,3-6 and some contact their health-care provider in the week preceding the cardiac arrest.7 We previously reported that, among patients with sudden cardiac arrest in the community-based Oregon Sudden Unexpected Death Study (SUDS), most patients and their families did not act on these early warning signs, with only a minority (81 [19%] of 430) seeking urgent medical care by calling 911 in response to symptoms before their collapse.3 People who called 911 before their collapse had more than five-times higher survival from sudden cardiac arrest. However, given the overlap of common symptoms with conditions other than sudden cardiac arrest, emergency medical services (EMS) systems could be rapidly overwhelmed by false-positive calls if these symptoms were to be used as predictors of sudden cardiac arrest. Therefore, the accuracy of specific symptoms for prediction of imminent sudden cardiac arrest needs to be established. Earlier studies on symptoms before sudden cardiac arrest have identified chest pain, dyspnoea, lightheadedness, palpitations, syncope, and other symptoms but have been limited by absence of comparison groups,5,8,9 small sample sizes (<100 participants),8,10,11 or restriction to particular age groups or people with conditions that increase their risk of sudden cardiac arrest.8,10,11 Harnessing warning symptoms to perform effective triage could lead to early intervention and prevention of death from imminent sudden cardiac arrest.
The dynamic nature of sudden cardiac arrest and the relatively low occurrence in the overall population (ie, 50–100 sudden cardiac arrests per 100000 people annually) present some challenges. A large sample of people with sudden cardiac arrest is needed to perform feasible analyses, and digital technology needs to be designed12 to make triage of high risk versus low risk of sudden cardiac arrest possible. For example, a smartphone algorithm developed using a combination of established high-risk symptoms could assist an individual or bystander in deciding whether symptoms require immediate medical attention by emergency first responders. Therefore, we performed a study in participants from two established and ongoing community-based studies of out-of-hospital sudden cardiac arrest to evaluate the prevalence of individual symptoms and sets of symptoms before sudden cardiac arrest compared with control groups that also sought emergency medical care. The use of data from these population-based studies provided a feasible sample size for analysis to build the foundations for digital technology to perform risk triage for sudden cardiac arrest. Among individuals with symptoms before sudden cardiac arrest, we aimed to estimate the strength of association between prespecified symptoms and sudden cardiac arrest.
Methods
Study design and participants
We conducted a case-control study of individuals with out-of-hospital sudden cardiac arrest and participants without sudden cardiac arrest who had similar symptoms. We used populations from two ongoing studies: the Ventura Prediction of Sudden Death in Multi-Ethnic Communities (PRESTO) study and SUDS.
We used the PRESTO study to select our discovery population. We identified individuals aged 18–85 years with an out-of-hospital sudden cardiac arrest from the study’s start date of Feb 1, 2015, to Jan 31, 2021, from the ongoing study in Ventura County, CA, USA (population of 848 112 people in 2018). All incident cases of presumed sudden cardiac arrest were prospectively identified through collaboration with the county’s two-tiered EMS system.13 People with sudden cardiac arrest who were residents of Ventura County with resuscitation attempted by EMS were subjected to detailed adjudication on the basis of the EMS prehospital care report, medical records from regional hospital systems, death certificates from California state vital statistics records, and the medical examiner report and autopsy if available. Three physicians performed adjudication of sudden cardiac arrest, which was defined as a sudden, unexpected pulseless condition of probable cardiac origin.2 People with an identifiable non-cardiac cause for cardiac arrest, such as trauma, drug overdose, and chronic terminal illness (eg, malignancy not in remission), were excluded. For this project, people with sudden cardiac arrest whose arrests were unwitnessed were excluded, because information about their symptoms before arrest was not uniformly available. By including only people with witnessed sudden cardiac arrest (about half of the total study population with sudden cardiac arrest), we attempted to ensure that assessment of symptom presence or absence and type of symptom was as accurate as possible. Demographic comparisons of people with witnessed and unwitnessed sudden cardiac arrest indicated no substantial differences between the groups, indicating that symptoms in people with witnessed sudden cardiac arrest could be generalisable to the entire patient population with sudden cardiac arrest.
The control group was designed to represent individuals attended by EMS who did not have sudden cardiac arrest, but who had symptoms that could have been mistaken for imminent sudden cardiac arrest. We identified potential control participants from the list of all 911 calls to the Ventura County EMS system from Jan 1 to Dec 31, 2019. We restricted calls to residents of Ventura County who were aged 18–85 years and excluded calls for cardiac arrest, trauma, behaviour, and pregnancy complications (based on EMS primary impression in the field) and calls not resulting in transport to hospital. To select individuals meeting inclusion criteria, we performed a comprehensive automated keyword search of the EMS narrative for any of the predefined inclusion symptoms or their synonyms. From this subset, we selected a simple random sample for manual review of the EMS prehospital care narratives and included people with at least one of the 12 inclusion symptoms. Any individuals already enrolled as participants in the PRESTO study and any that, on manual review, could have been sudden cardiac arrest (ie, any patient receiving CPR or defibrillation) were excluded. No matching was performed for control group selection.
We replicated our results in a separate population using data from the same years (from Feb 1, 2015, to Jan 31, 2021) from SUDS, in the Portland metropolitan region, OR, USA, which uses identical case and control ascertainment methods as the PRESTO study.3 Control participants were selected from 911 calls to Multnomah County’s EMS system from Jan 1–Dec 31, 2019 in the same manner as in the PRESTO study.
The PRESTO study received ethical approval by the Institutional Review Boards of Ventura County Medical Center, Cedars-Sinai Health System, and all other participating hospitals and health systems. SUDS received ethical approval by the Institutional Review Board of Oregon Health and Science University and all participating hospital and health systems. All survivors of cardiac arrest provided written informed consent for the PRESTO study and SUDS, which extends to this analysis; for non-survivors this requirement was waived. This report follows the STROBE guidelines for reporting results of observational studies.14
Procedures
Symptom data and demographics for the PRESTO study population were obtained monthly throughout the study period for patients with sudden cardiac arrest and obtained in a one-time batch for controls from EMS prehospital care reports written by first responders of the Ventura County Health Care Agency in Ventura County, CA, USA. A designated member of the study staff worked with the Ventura County Health Care Agency to obtain monthly case data, and in 2021, the one-time dataset of EMS calls in 2019 for control participants. In the reports, first responders recorded basic patient demographics and the circumstances of the event leading to the 911 call, including symptoms reported by bystanders or, in the approximately 10% of sudden cardiac arrests witnessed by EMS, by the patient themselves. Due to the sudden and unexpected nature of these events, these data were collected verbally at the time of the incident from the individuals or bystanders and recorded by EMS personnel. Race and ethnicity information were not available in most reports. Sex was determined by EMS personnel. Trained study personnel manually reviewed EMS narratives for all people with witnessed sudden cardiac arrest and for control participants randomly selected for detailed review. Symptoms were required to have clearly preceded the collapse; this was determined based on the EMS narrative describing the emergency call and any symptom-related information obtained by first responders at the scene, which often noted the length of time that an individual had experienced symptoms (for example, “patient complained of chest pain one hour before collapse”). Signs occurring as a consequence of the cardiac arrest (eg, gasping or agonal breathing or apparent seizure following collapse) were not recorded as symptoms.
The list of symptoms to be included in this analysis was determined from published literature regarding symptoms of sudden cardiac arrest, including chest pain, dyspnoea, palpitations, syncope, seizure-like activity, and influenza-like symptoms,3,8-11,15 and other symptoms associated with acute coronary syndrome.16-18 The symptoms also included nausea or vomiting, diaphoresis, dizziness, unusual fatigue, abdominal symptoms (ie, pain or discomfort), and weakness. These symptoms of sudden cardiac arrest and acute coronary syndrome comprised the list used for inclusion in our analysis. For analysis, chest pain was defined to include symptoms reported as chest pain, discomfort, or pressure; shoulder, arm, neck, and jaw pain; heartburn; and indigestion.
Both people with sudden cardiac arrest and control participants in this analysis were required to have at least one inclusion symptom, as listed above. Patients with sudden cardiac arrest whose EMS narrative did not report the presence or absence of specific symptoms before arrest were labelled as probably having no symptoms, and those whose narrative specifically indicated an absence of symptoms before arrest were labelled as definitely having no symptoms. The remainder were classified as individuals with at least one inclusion symptom and individuals with other symptoms. Control participants included in analysis were individuals with at least one inclusion symptom identified at manual review of the narrative; people with no inclusion symptoms or whose narrative was not detailed enough to confirm specific symptoms were excluded.
Data for symptoms for the replication population were obtained using the same procedures as for the discovery population from the Multnomah County EMS system’s prehospital reports for each participant.
Our outcome was out-of-hospital sudden cardiac arrest. Our exposure variables were 12 symptoms that occurred before the 911 call, as recorded in EMS reports. We assessed differences in symptom prevalence between patients with sudden cardiac arrest and control participants, and potential associations between these symptoms and the outcome. We also evaluated the frequency of mutually exclusive and sets of symptoms. Finally, we evaluated potential confounding and effect modification by age and sex.
Statistical analysis
The sample size was determined a priori for a power of more than 0·90 to detect a more than 10% difference in symptom prevalence, assuming prevalence ranged from 0·2 to 0·5. Independent samples t tests and Pearson χ2 tests were used for demographic and univariate case-control comparisons of individual symptom prevalence. We also evaluated the frequency of symptoms stratified by sex. There was no evidence of colinearity between individual symptoms or between symptoms and age and sex. We tested for interaction of selected symptoms with age and sex by use of multi-plicative interaction terms in logistic models (p<0·20 indicating potential interaction) and used sex-stratified logistic regression models to evaluate the association of selected symptoms (ie, chest pain, dyspnoea, and diaphoresis) with sudden cardiac arrest, using p values from the Wald test in models including the three symptoms and age. We evaluated the frequency of mutually exclusive single symptoms and sets of symptoms with UpSet plots in R, which is a technique to visualise sets of data points, their intersections, and aggregates of intersection.19 We repeated the same univariate and multivariable analysis in the external validation population. We conducted a sensitivity analysis to assess whether controlling for differences in age and sex by frequency matching would produce similar results. In both the discovery and replication populations, we repeated bivariate comparisons and multiple logistic regression models in datasets in which control participants were frequency-matched to patients with sudden cardiac arrest by use of 10-year age categories (ie, ages 18–34 years, 35–44 years, 45–54 years, 55–64 years, 65–74 years, ≥75 years) by sex. Participants for whom data were missing for sex were excluded from the sex-stratified analysis and multivariable logistic modelling.
All statistical analysis was conducted using SAS, version 9.4.
Role of the funding source
The funder of the study had no role in study design, data collection, data analysis, data interpretation, or writing of the report.
Results
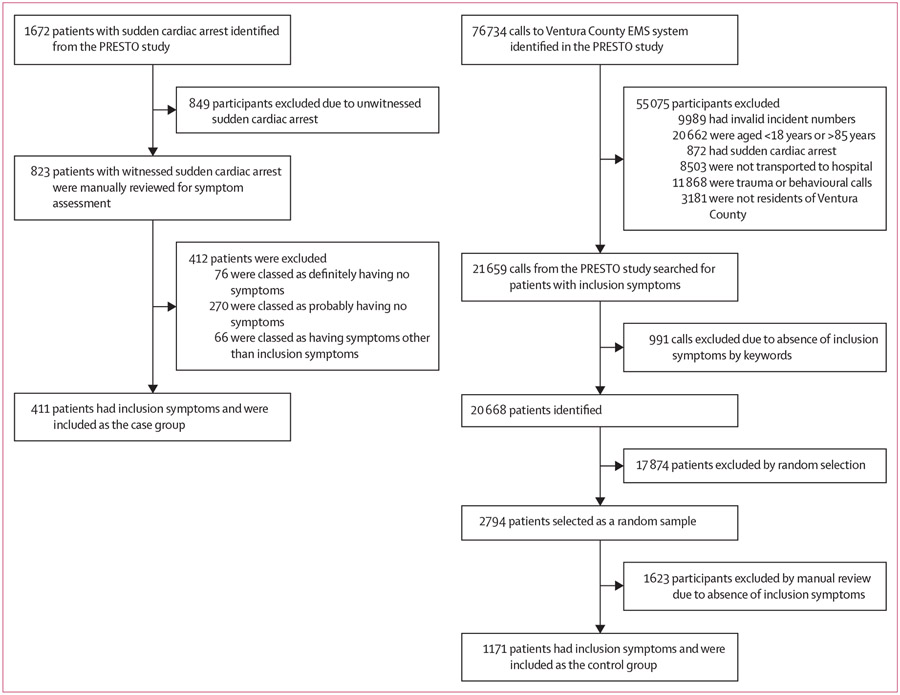
We identified a total of 1672 individuals with out-of-hospital sudden cardiac arrest of probable cardiac cause from the PRESTO study (from Feb 1, 2015, to Jan 31, 2021), of whom 823 (49%) had sudden cardiac arrest witnessed by a bystander or EMS personnel. Review and extraction of symptom data was performed in 2021 for people with sudden cardiac arrest and control participants. Of the 823 participants with sudden cardiac arrest, 411 (50%) had at least one of the inclusion symptoms and were retained for analysis. 76 (9%) of 823 participants had an explicit mention of an absence of symptoms before sudden cardiac arrest, 270 (33%) had no mention of symptom absence or presence in the narrative, and 66 (8%) had none of the inclusion symptoms but had at least one other symptom (figure 1).
Figure 1:
Participant selection for the discovery population
A total of 76 734 calls were made to the Ventura Country EMS system during the selected time period. After restriction to residents of Ventura County aged 18–85 years and exclusion of calls for cardiac arrest, trauma, behaviour, and pregnancy complications and calls not resulting in transport to hospital, 21659 calls remained. 20668 patients with inclusion symptoms were identified through automated keyword search. We selected a random sample of 2794 individuals whose EMS narrative was manually reviewed, and 1171 (42%) had at least one of the inclusion symptoms and were included in this analysis. The remainder had symptoms other than the predetermined inclusion symptoms, or, despite the keyword search, did not have adequate symptom information on manual review.
Among the 411 participants with sudden cardiac arrest and 1171 control participants with at least one inclusion symptom, patients with sudden cardiac arrest were significantly more likely to be male and were older (table 1). 14 control participants were missing data for sex and were excluded from sex-stratified analysis and multivariable logistic modelling.
Table 1:
Demographics of patients with sudden cardiac arrest and control participants across the PRESTO discovery population and the SUDS replication population
| PRESTO |
SUDS |
|||||
|---|---|---|---|---|---|---|
| Participants with sudden cardiac arrest (n=411) |
Controls (n=1171) | p value | Participants with sudden cardiac arrest (n=427) |
Controls (n=1238) | p value | |
| Sex* | ·· | ·· | <0·0001 | ·· | ·· | <0·0001 |
| Female | 125 (30%) | 643/1157 (56%) | ·· | 122 (29%) | 689/1237 (56%) | ·· |
| Male | 286 (70%) | 514/1157 (44%) | ·· | 305 (71%) | 548/1237 (44%) | ·· |
| Age, years | ·· | ·· | <0·0001 | ·· | ·· | 0·0002 |
| 18–34 | 7 (2%) | 114 (10%) | ·· | 15 (4%) | 133 (11%) | ·· |
| 35–44 | 22 (5%) | 107 (9%) | ·· | 29 (7%) | 101 (8%) | ·· |
| 45–54 | 46 (11%) | 142 (12%) | ·· | 75 (18%) | 176 (14%) | ·· |
| 55–64 | 108 (26%) | 208 (18%) | ·· | 117 (27%) | 292 (24%) | ·· |
| 65–74 | 129 (31%) | 281 (24%) | ·· | 113 (26%) | 298 (24%) | ·· |
| 75–85 | 99 (24%) | 319 (27%) | ·· | 78 (18%) | 238 (19%) | ·· |
| Overall mean age, years (SD) | 65·7 (12·4) | 61·8 (17·3) | <0·0001 | 62·2 (13·5) | 59·3 (16·5) | 0·0003 |
| Mean female age, years (SD) | 68·5 (12·6) | 60·8 (17·9) | <0·0001 | 61·8 (14·3) | 58·8 (17·1) | 0·045 |
| Mean male age, years (SD) | 64·5 (12·1) | 63·0 (16·4) | 0·013 | 62·4 (13·2) | 59·9 (15·7) | 0·015 |
Data are n (%) unless otherwise stated. *Data were missing for 14 control participants in the PRESTO study and one control participant in SUDS.
Among patients with sudden cardiac arrest, the most common symptoms were chest pain and dyspnoea (table 2). Nausea or vomiting, diaphoresis, seizure-like activity, and weakness each occurred in approximately one in ten patients with sudden cardiac arrest. All other symptoms were reported in fewer than 6% of patients with sudden cardiac arrest (table 2).
Table 2:
Symptom prevalence among patients with sudden cardiac arrest and control groups across the PRESTO discovery population and the SUDS replication population
| PRESTO |
SUDS |
|||||
|---|---|---|---|---|---|---|
| Participants with sudden cardiac arrest (n=411) |
Controls (n=1171) | p value | Participants with sudden cardiac arrest (n=427) |
Controls (n=1238) | p value | |
| Chest pain | 136 (33%) | 296 (25%) | 0·0022 | 133 (31%) | 387 (31%) | 0·97 |
| Dyspnoea | 168 (41%) | 262 (22%) | <0·0001 | 179 (42%) | 316 (26%) | <0·0001 |
| Nausea or vomiting | 52 (13%) | 353 (30%) | <0·0001 | 42 (10%) | 355 (29%) | <0·0001 |
| Diaphoresis | 50 (12%) | 90 (8%) | 0·0059 | 26 (6%) | 77 (6%) | 0·92 |
| Seizure-like activity | 43 (11%) | 77 (7%) | 0·011 | 75 (18%) | 45 (4%) | <0·0001 |
| Weakness | 42 (10%) | 267 (23%) | <0·0001 | 25 (6%) | 199 (16%) | <0·0001 |
| Dizziness | 26 (6%) | 294 (25%) | <0·0001 | 26 (6%) | 253 (20%) | <0·0001 |
| Syncope | 25 (6%) | 107 (9%) | 0·054 | 21 (5%) | 95 (8%) | 0·054 |
| Abdominal symptoms | 21 (5%) | 234 (20%) | <0·0001 | 24 (6%) | 260 (21%) | <0·0001 |
| Influenza-like symptoms | 19 (5%) | 79 (7%) | 0·12 | 28 (7%) | 87 (7%) | 0·74 |
| Fatigue | 16 (4%) | 56 (5%) | 0·46 | 20 (5%) | 58 (5%) | 0·99 |
| Palpitations | 3 (1%) | 56 (5%) | 0·0002 | 4 (1%) | 41 (3%) | 0·0091 |
Data are n (%) unless otherwise stated. Percentages add to greater than 100% because individuals can have more than one symptom recorded.
Chest pain, dyspnoea, diaphoresis, and seizure-like activity were significantly more common among patients with sudden cardiac arrest than among controls in the discovery population (table 2). The symptoms that were significantly more common among control participants in the discovery population, with a prevalence of more than 20%, were nausea or vomiting, weakness, dizziness, and abdominal symptoms (ie, pain or discomfort; table 2). Palpitations were also more common among control participants, but had a prevalence of less than 5% overall (table 2). In logistic regression models including all participants with sudden cardiac arrest and controls adjusted for age, sex, and each symptom separately, odds of chest pain (p=0·0017), dyspnoea (p<0·0001), diaphoresis (p=0·041), and seizure-like activity (p=0·0003) were at least 45% higher in patients with sudden cardiac arrest (data not shown). When interaction terms were added to the models, significant interaction was observed between chest pain and sex (p<0·0001) but not between chest pain and age (p=0·95; data not shown). There was potential interaction between dyspnoea and sex (p=0·18) but not age (p=0·47; data not shown). No age or sex interaction was observed for diaphoresis (p=0·85 for age and p=0·39 for sex; data not shown). For seizure-like activity, there was potential interaction by both age (p=0·052) and sex (p=0·17; data not shown).
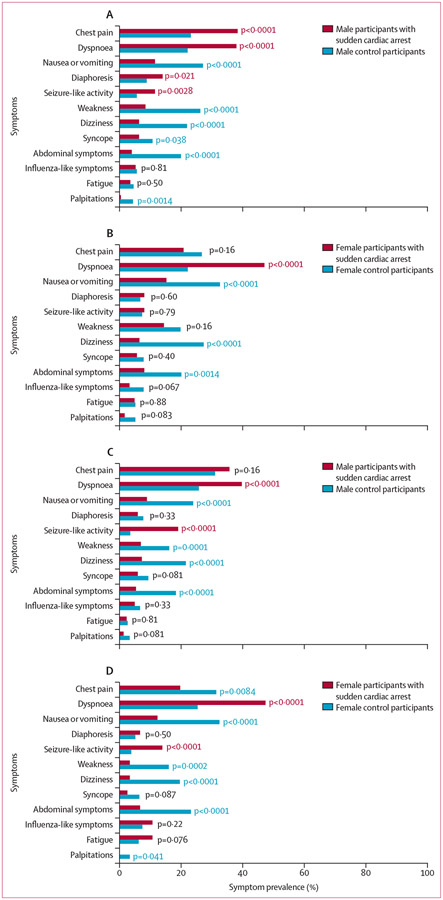
Among men, the prevalence of chest pain, dyspnoea, diaphoresis, and seizure-like activity was significantly higher among patients with sudden cardiac arrest than controls (figure 2A). Among women, only dyspnoea was significantly more prevalent among patients with sudden cardiac arrest than controls (figure 2B). In both men and women, the symptoms observed more commonly in control participants were largely consistent (figure 2A-B).
Figure 2: Symptom frequency in participants with at least one predefined symptom.
Symptom frequency in male participants with sudden cardiac arrest (n=286) and controls (n=514) in the PRESTO discovery population (A), female participants with sudden cardiac arrest (n=125) and controls (n=657) in the PRESTO discovery population (B), male participants with sudden cardiac arrest (n=305) and controls (n=548) in the SUDS replication population (C), and female participants (n=122) and controls (n=690) in the SUDS replication population (D). Data for sex were missing for 14 control participants in the PRESTO discovery population and one control participant in the SUDS replication population.
In sex-stratified age-adjusted multivariable models including chest pain, dyspnoea, and diaphoresis, each symptom was associated with sudden cardiac arrest among men (table 3). Among women, dyspnoea was significantly associated with sudden cardiac arrest, whereas chest pain and diaphoresis were not (table 3). In models with each symptom modelled alone, discrimination was lower, particularly among men (areas under the receiver operating characteristic curve for individual symptoms were <0·585 among men and <0·683 among women (data not shown).
Table 3:
Associations with sudden cardiac arrest in the PRESTO discovery population and SUDS replication population
| PRESTO |
SUDS |
|||||||
|---|---|---|---|---|---|---|---|---|
| Men | p value (AUROC=0·644) |
Women | p value (AUROC=0·686) |
Men | p value (AUROC=0·605) |
Women | p value (AUROC=0·643) |
|
| Chest pain | 2·2 (1·6–3·0) | <0·0001 | 0·7 (0·4–1·1) | 0·14 | 1·3 (1·0–1·8) | 0·058 | 0·6 (0·5–0·9) | 0·018 |
| Dyspnoea | 2·2 (1·6–3·0) | <0·0001 | 2·9 (1·9–4·3) | <0·0001 | 1·9 (1·4–2·6) | <0·0001 | 2·5 (1·7–3·7) | <0·0001 |
| Diaphoresis | 1·7 (1·1–2·7) | 0·027 | 1·0 (0·5–2·1) | 0·99 | 0·8 (0·4–1·4) | 0·37 | 1·2 (0·5–2·7) | 0·68 |
Data are odds ratio (95% CI) unless otherwise stated. All models included chest pain, dyspnoea, and diaphoresis, adjusted for age. p values are from Wald tests in sex-stratified multiple logistic regression models including the three symptoms, adjusted for age. The AUROC indicates the discrimination of the model. AUROC=area under the receiver operating characteristic curve.
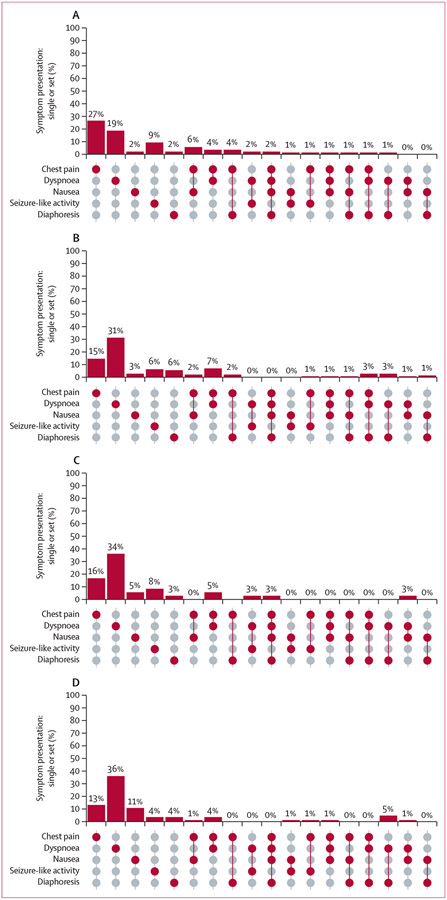
A visual analysis of the five most prevalent symptoms among patients with sudden cardiac arrest (ie, chest pain, dyspnoea, nausea, seizure-like activity, and diaphoresis) showed that, when mutually exclusive single symptoms or sets of symptoms occurring together were considered, most people had only one symptom noted by EMS. A minority had 2 or more symptoms occurring together (figure 3). These single symptoms and sets of symptoms varied by age and sex. For example, among 138 men aged 35–64 years with sudden cardiac arrest (figure 3A), chest pain occurred alone in 37 (27%) men, and occurred together with one or more other symptoms in 29 (21%) men (ie, eight [6%] men aged 35–64 years with chest pain also had nausea; five [4%] also had dyspnoea; five [4%] also had diaphoresis; three [2%] also had nausea, dyspnoea, and diaphoresis; and eight [6%] had one of four different combinations, with two [1%] men having each combination). Among men aged 65 years or older, dyspnoea alone was the most common symptom (figure 3B). Among 38 women aged 35–64 years with sudden cardiac arrest, chest pain occurred as a single symptom in six (16%) women and in a group with other symptoms in three (8%) women (ie, two [5%] women also had dyspnoea and one [3%] woman also had dyspnoea, nausea, and diaphoresis; figure 3C).
Figure 3: UpSet plot of symptoms occurring singly or in sets of symptoms among patients with sudden cardiac arrest in the discovery population.
(A) Men with sudden cardiac arrest aged 35–64 years. (B) Men with sudden cardiac arrest aged ≥65 years. (C) Women with sudden cardiac arrest aged 35–64 years. (D) Women with sudden cardiac arrest aged ≥65 years. The five most prevalent symptoms among patients with sudden cardiac arrest are shown, with each bar representing the mutually exclusive frequency of the single symptom or symptom set in each age–sex group. In the legend below each bar, a single dark circle indicates that symptom occurring alone; two or more dark circles connected with a line indicates those symptoms occurring as a group. This graph does not include the smaller proportion of cases with one or more of the five most common symptoms that occurred with less common symptoms (eg, chest pain plus dizziness) or other less common mutually exclusive individual symptoms or sets of symptoms (eg, palpitations or palpitations plus dizziness).
For all sex–age groups, the majority of symptoms occurred alone (in 82 [59%] of 138 men aged 35–64 years and 87 [60%] of 144 men aged ≥65 years; in 25 [66%] of 38 women aged 35–64 years and 56 [67%] of 84 women aged ≥65 years). A smaller proportion of cases had one or more of the five most common symptoms together with less common symptoms (eg, chest pain plus dizziness) or other less common mutually exclusive individual symptoms or sets of symptoms (eg, palpitations or palpitations plus dizziness). These less common presentations were observed in approximately 15–20% of cases: 20 (14%) of 138 men aged 35–64 years, 27 (19%) of 144 men aged 65 years or older, eight (21%) of 38 women aged 35–64 years, and 16 (19%) of 84 women aged 65 years or older (data not shown). Overall, women aged 35–64 years were less likely than other groups to present with the most common symptoms or sets of symptoms.
In the SUDS replication population, we identified 1640 patients with out-of-hospital sudden cardiac arrest of probable cardiac cause, of which 883 (54%) patients had a witnessed sudden cardiac arrest. 427 (48%) of 883 patients had inclusion symptoms and were included in the analysis. 79 (9%) of 883 patients had an explicit mention of an absence of symptoms before sudden cardiac arrest, 288 (33%) had no mention of symptom absence or presence in the narrative, and 89 (10%) had none of the inclusion symptoms but had at least one other symptom (appendix p 1). From 79 209 total calls to Multnomah County 911 system in 2019, 18 480 calls remained after restricting to individuals aged 18–85 years and excluding calls for cardiac arrest, trauma, behavioural issues, and pregnancy complications and calls not resulting in transport to hospital. An automated keyword search for inclusion symptoms retained 15 867 calls. A random sample of 2090 calls was selected for manual review. 1238 individuals had at least one inclusion symptom and were included as the control population.
Compared with the PRESTO study population, the sex and age distribution of patients with sudden cardiac arrest with an inclusion symptom (n=427) and controls (n=1238) in SUDS were similar, although both patients with sudden cardiac arrest and controls were younger than in the discovery population (table 1). Data were missing for sex for one control participant, who was excluded from the sex-stratified analysis and multivariable logistic modelling.
With a few exceptions, the frequency of individual symptoms and differences in magnitude and direction between patients with sudden cardiac arrest and controls in Oregon were similar to those in the discovery population (table 2). Two important differences were that chest pain and diaphoresis did not differ between patients with sudden cardiac arrest and control participants in the SUDS replication population (table 2). All other findings were consistent.
In sex-stratified analyses of the replication population, individual symptom frequencies were largely similar to those in the discovery population, although some differences were observed (figure 2). Among men, chest pain was not significantly different between patients with sudden cardiac arrest and controls (p=0·16), and neither was diaphoresis (p=0·33). Dyspnoea and seizure-like activity were more prevalent among patients with sudden cardiac arrest than among controls (figure 2C), whereas symptoms more prevalent among controls were largely consistent with those in the discovery population. Among women, results were largely consistent with those in the discovery population: dyspnoea was significantly more common among patients with sudden cardiac arrest than controls, as was seizure-like activity (figure 2D). In sex-stratified age-adjusted multivariable models, results were largely consistent with the discovery population analysis. Among men, chest pain was modestly associated with sudden cardiac arrest, dyspnoea was consistent with the results in the discovery population, and diaphoresis was not associated (table 3). Among women, dyspnoea was significantly associated with sudden cardiac arrest, whereas chest pain was negatively associated with sudden cardiac arrest, and diaphoresis was not associated (table 3).
In frequency-matched datasets (411 patients with sudden cardiac arrest and 411 controls from the PRESTO study; 427 patients with sudden cardiac arrest and 427 controls from SUDS), results were nearly identical to the unmatched analyses for case-control comparisons of individual symptoms (appendix p 2).
Discussion
In this study of warning symptoms before imminent out-of-hospital sudden cardiac arrest versus a comparison group of individuals who called 911 for other reasons but with the same prespecified symptoms, we were able to analyse a large dataset obtained from EMS electronic health records. Symptoms of chest pain and dyspnoea were reported in more than 30% of patients with sudden cardiac arrest. Other symptoms were present in less than 18% of patients with sudden cardiac arrest. Our case-control comparisons indicated significant sex differences in associations of symptoms with sudden cardiac arrest. In sex-specific models, chest pain, dyspnoea, and diaphoresis were associated with sudden cardiac arrest in men, but only dyspnoea was associated with sudden cardiac arrest among women. Dizziness, abdominal symptoms (ie, pain or discomfort), weakness, and nausea or vomiting were significantly less common among patients with sudden cardiac arrest than the control group. Most symptoms occurred alone rather than in sets of symptoms. These findings were replicated in the external, geographically distinct population. To our knowledge, this is the first community-based study to evaluate the association of warning symptoms or sets of symptoms with imminent sudden cardiac arrest using a comparison group with EMS-documented symptoms recorded as part of routine emergency care for both patients with sudden cardiac arrest and control participants.
In the past decade, there has been heightened interest to evaluate whether warning symptoms could be used for prediction of imminent sudden cardiac arrest. However, no previous large community-wide studies of sudden cardiac arrest warning symptoms included a comparison group. A study in Japan obtained symptom information from EMS reports for 1042 people and observed that, among the 644 people with any prodromal symptoms, the three most common symptoms for sudden cardiac arrest of cardiac cause were dyspnoea (178 [28%]), chest pain (133 [21%]), and syncope (82 [13%]),5 similar to our findings. An earlier study in Germany reported that, among 406 patients sudden with cardiac arrest, angina was most common (88 [22%]), followed by dyspnoea (61 [15%]), nausea or vomiting (27 [7%]), and dizziness or syncope (21 [5%]).4 In a study of symptoms and treatment-seeking behaviour in adults with sudden cardiac arrest (n=140), fatigue, chest pain, dyspnoea, diaphoresis, and not feeling well were the most common symptoms reported by witnesses or family members of individuals who died from sudden cardiac arrest.9 Some previous studies included a control group but restricted analysis to small sudden cardiac arrest subgroups. For example, a study in Danish residents aged 1–35 years included a matched accidental-death comparison group but included only sudden cardiac arrest with coronary artery disease before arrest (n=40)10 or with hypertrophic cardiomyopathy (n=38).11
Our findings represent the initial step in the discovery of novel methods to predict imminent sudden cardiac arrest. Although warning symptoms can potentially be harnessed, many people have these symptoms on a daily basis. In a previous publication, we presented a concept for how digital and wireless technologies could save lives by identifying patients at high risk of imminent sudden cardiac arrest.12 A smartphone-based platform could collate features, such as warning symptoms data, with demographic data, the individual’s clinical profile, physiological measurements from biometric sensors, and a smartphone-generated electrocardiogram (ECG) to generate a risk score for impending sudden cardiac arrest. The input features would generate an output by providing a recommendation on whether an individual with warning symptoms should seek an emergent, urgent, or non-urgent evaluation with the goal of preventing sudden cardiac arrest. However, prospective studies might be required to evaluate the effectiveness of warning symptoms to predict imminent sudden cardiac arrest. The findings from this study provide the first basis for designing and performing these prospective studies that will ideally combine these symptoms with other features to enhance prediction of imminent sudden cardiac arrest. Furthermore, investigations in people with sudden cardiac arrest with warning symptoms that include clinical profile or biomarkers, or both, might be useful for prediction of imminent sudden cardiac arrest among those who will not have warning symptoms.
Studies of symptoms of acute coronary syndrome indicate that combining symptoms with additional features might improve their usefulness. In a Swedish study of 2917 EMS patients with acute chest pain, 335 (11%) patients overall suffered acute myocardial infarction.20 A combination of symptom characteristics (ie, pain triggers, pain location, and quality), clinical history (ie, kidney disease, heart failure, and atrial fibrillation), laboratory tests (ie, for troponin T), and ECG findings better differentiated individuals at high risk versus low risk of acute myocardial infarction than did individual symptoms.21
Our findings of lower chest pain and higher dyspnoea prevalence among women with sudden cardiac arrest than among men with sudden cardiac arrest is also consistent with similar studies in the literature regarding acute coronary syndrome. A meta-analysis of 27 studies reported that women with confirmed acute coronary syndrome have higher odds of dyspnoea and lower odds of chest pain and diaphoresis than do men.22 Taken together, earlier data and our present findings on symptoms before sudden cardiac arrest suggest that symptoms vary by patient characteristics, indicating the need to consider the age, sex, and clinical history of patients if symptoms are to be used to predict imminent sudden cardiac arrest. Our visual evaluation of symptoms and sets of symptoms with UpSet plots in R19 is, to our knowledge, unique in the sudden cardiac arrest literature and allowed for a relatively intuitive visual evaluation of symptom presentation in patient subgroups. In our study, men were more likely than women to present with the most common symptom groups, similar to findings from the VIRGO study of acute myocardial infarction,23 emphasising the potential for missed recognition of imminent cardiac events in women.
Although the use of a predefined list of symptoms based on previous literature regarding symptoms of sudden cardiac arrest and acute coronary syndrome allowed for objective comparisons between patients with sudden cardiac arrest and controls, use of a predefined list meant that we were unable to discover potential new symptoms of sudden cardiac arrest. Another potential limitation of the study is that we cannot be certain of the reliability and comprehensive nature of symptoms reported to EMS at the time of the emergency by family members, bystanders, or the individual themselves. Our analysis identified some symptoms typically associated with acute coronary syndrome or cardiac arrest (ie, chest pain, dyspnoea, and diaphoresis), whereas others (ie, palpitations, dizziness, and syncope) were not associated with imminent sudden cardiac arrest. This information might facilitate early recognition of imminent sudden cardiac arrest and timely activation of EMS response to prevent death from sudden cardiac arrest among the subset of individuals who present with symptoms before sudden cardiac arrest (approximately 50% of total patients with sudden cardiac arrest). For the remaining approximately 40–50% of individuals with sudden cardiac arrest without previous symptoms, and the 5–10% who have symptoms besides those that are typical of acute coronary syndrome or sudden cardiac arrest, other approaches will likely be needed to prevent sudden cardiac arrest. Finally, these findings might not be generalisable to other regions within the USA or worldwide. Race and ethnicity data were not available for most participants, which is a limitation.
In conclusion, among individuals with symptomatic out-of-hospital sudden cardiac arrest in the community, chest pain and dyspnoea in men and dyspnoea in women were the most common symptoms and had a moderate association with sudden cardiac arrest when compared with a control group of individuals who also called 911 for emergency care. Symptom type and symptom co-occurrence differed by sex. No individual symptom or set of symptoms was prevalent enough to warrant use alone for prediction of imminent sudden cardiac arrest. Warning symptoms are common but might need to be supplemented with additional features, such as the clinical profile and biometric measures, for improved prediction of imminent sudden cardiac arrest. Potential future directions include combining symptoms with a patient’s clinical profile or dynamic alterations in clinical markers or biomarkers measured by wearables to identify stronger associations with imminent sudden cardiac arrest.
Supplementary Material
Research in context.
Evidence before this study
Overall survival from sudden cardiac arrest is less than 10%; however, effective methods for predicting and preventing this mostly lethal condition are yet to be identified. Many individuals have warning symptoms before sudden cardiac arrest, and early response to symptoms (eg, calling 911 before collapse) is associated with improved survival. Prearrest warning symptoms could be harnessed with digital technology to potentially improve survival outcomes, but the usefulness of symptoms for identification of imminent sudden cardiac arrest is unknown. Given the probable overlap of common symptoms with conditions other than sudden cardiac arrest, there is also the possibility that emergency systems could be rapidly overwhelmed by false-positive calls if symptoms are used for identification of imminent sudden cardiac arrest. Therefore, the association of specific symptoms with imminent sudden cardiac arrest in the community needs to be established. Earlier studies of symptoms before sudden cardiac arrest have not included a control group or have been limited by small sample sizes. We searched PubMed between Jan 1, 1990, and Dec 31, 2022, for original research or review articles published in English using the search terms “symptom” and “cardiac arrest” (which returned 331 articles) or “sudden cardiac death” (which returned 282 articles). After reviewing abstracts, we identified five original research articles on symptoms before sudden cardiac arrest among adults in the community, and four articles on symptoms before sudden cardiac arrest among children and young adults (ie, aged 1–35 years). None of these studies evaluated the effectiveness of warning symptoms or sets of symptoms for prediction of sudden cardiac arrest. For the findings to be relevant to the general population, we identified the need to conduct a large community-based study, across all ages, and include a comparison group.
Added value of this study
We were able to include a comparison group for this study, which was conducted in a large dataset ascertained from emergency medical services (EMS) electronic health records. This case-control study was conducted in a US population of approximately 850 000 residents and replicated in another US community of approximately 800 000 residents. We evaluated the prevalence and potential grouping of symptoms recorded by EMS personnel before sudden cardiac arrest (>400 patients with sudden cardiac arrest in each study) compared with individuals who also had EMS response for emergency medical care (>1000 comparison individuals in each study). To our knowledge, this is the first community-based study to evaluate the association of warning symptoms or sets of symptoms before imminent sudden cardiac arrest compared with a community-based control group.
Implications of all the available evidence
The prevalence of warning symptoms in our study was sex-specific and differed significantly between patients with sudden cardiac arrest and control participants. Warning symptoms are common but will probably need to be augmented with additional features, such as the clinical profile and biometric measures, for improved prediction of imminent sudden cardiac arrest. Digital technology and the use of features identified in patients with prearrest symptoms could facilitate further investigation to reduce mortality from imminent sudden cardiac arrest.
Acknowledgments
We thank Habiba Aziz for preparation of UpSet plots. This work was funded, in part, by National Institutes of Health, with National Heart Lung and Blood Institute grants R01HL145675 and R01HL147358 to SSC. SSC holds the Pauline and Harold Price Chair in Cardiac Electrophysiology at Cedars-Sinai Health System, Los Angeles, CA, USA.
Footnotes
Declaration of interests
We declare no competing interests.
Contributor Information
Kyndaron Reinier, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Bernadine Dizon, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Harpriya Chugh, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Ziana Bhanji, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Madison Seifer, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Arayik Sargsyan, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Audrey Uy-Evanado, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Faye L Norby, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Kotoka Nakamura, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA.
Katy Hadduck, Ventura County Health Care Agency, Ventura, CA, USA.
Daniel Shepherd, Ventura County Health Care Agency, Ventura, CA, USA.
Tristan Grogan, Department of Medicine, David Geffen School of Medicine at UCLA, Los Angeles, CA, USA.
David Elashoff, Department of Medicine, David Geffen School of Medicine at UCLA, Los Angeles, CA, USA.
Jonathan Jui, Department of Emergency Medicine, Oregon Health and Science University, Portland, OR, USA.
Angelo Salvucci, Ventura County Health Care Agency, Ventura, CA, USA.
Sumeet S Chugh, Center for Cardiac Arrest Prevention, Department of Cardiology, Smidt Heart Institute, Cedars-Sinai Health System, Los Angeles, CA, USA; Division of Artificial Intelligence in Medicine, Department of Medicine, Cedars-Sinai Health System, Los Angeles, CA, USA.
Data sharing
De-identified participant data will be made available after publication on reasonable request to the corresponding author, following approval of a proposal and a signed data use agreement.
References
- 1.Tsao CW, Aday AW, Almarzooq ZI, et al. Heart disease and stroke statistics—2022 update: a report from the American Heart Association. Circulation 2022; 145: e153–639. [DOI] [PubMed] [Google Scholar]
- 2.Fishman GI, Chugh SS, Dimarco JP, et al. Sudden cardiac death prediction and prevention: report from a National Heart, Lung, and Blood Institute and Heart Rhythm Society Workshop. Circulation 2010; 122: 2335–48. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Marijon E, Uy-Evanado A, Dumas F, et al. Warning symptoms are associated with survival from sudden cardiac arrest. Ann Intern Med 2016; 164: 23–29. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Müller D, Agrawal R, Arntz HR. How sudden is sudden cardiac death? Circulation 2006; 114: 1146–50. [DOI] [PubMed] [Google Scholar]
- 5.Nishiyama C, Iwami T, Kawamura T, et al. Prodromal symptoms of out-of-hospital cardiac arrests: a report from a large-scale population-based cohort study. Resuscitation 2013; 84: 558–63. [DOI] [PubMed] [Google Scholar]
- 6.Norris RM. Circumstances of out of hospital cardiac arrest in patients with ischaemic heart disease. Heart 2005; 91: 1537–40. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Höglund H, Jansson JH, Forslund AS, Lundblad D. Prodromal symptoms and health care consumption prior to out-of-hospital cardiac arrest in patients without previously known ischaemic heart disease. Resuscitation 2014; 85: 864–68. [DOI] [PubMed] [Google Scholar]
- 8.Drezner JA, Fudge J, Harmon KG, Berger S, Campbell RM, Vetter VL. Warning symptoms and family history in children and young adults with sudden cardiac arrest. J Am Board Fam Med 2012; 25: 408–15. [DOI] [PubMed] [Google Scholar]
- 9.Rosenfeld A, Christensen V, Daya M. Long enough to act? Symptom and behavior patterns prior to out-of-hospital sudden cardiac death. J Cardiovasc Nurs 2013; 28: 166–75. [DOI] [PubMed] [Google Scholar]
- 10.Jabbari R, Risgaard B, Holst AG, et al. Cardiac symptoms before sudden cardiac death caused by coronary artery disease: a nationwide study among young Danish people. Heart 2013; 99: 938–43. [DOI] [PubMed] [Google Scholar]
- 11.Lynge TH, Risgaard B, Jabbari R, et al. Cardiac symptoms before sudden cardiac death caused by hypertrophic cardiomyopathy: a nationwide study among the young in Denmark. Europace 2016; 18: 1801–08. [DOI] [PubMed] [Google Scholar]
- 12.Held EP, Chugh SS. Warning signs of impending acute cardiac events. Circulation 2018; 138: 1617–19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Chugh SS, Reinier K, Uy-Evanado A, et al. Prediction of sudden cardiac death manifesting with documented ventricular fibrillation or pulseless ventricular tachycardia. JACC Clin Electrophysiol 2022; 8: 411–23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Ann Intern Med 2007; 147: 573–77. [DOI] [PubMed] [Google Scholar]
- 15.Skjelbred T, Lynge TH, Nielsen J, Winkel BG, Tfelt-Hansen J. Symptoms and healthcare contact preceding sudden cardiac death in persons aged 1-49 years. Trends Cardiovasc Med 2021; 31: 119–24. [DOI] [PubMed] [Google Scholar]
- 16.Gulati M, Levy PD, Mukherjee D, et al. 2021 AHA/ACC/ASE/CHEST/SAEM/SCCT/SCMR guideline for the evaluation and diagnosis of chest pain: executive summary: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation 2021; 144: e368–454. [DOI] [PubMed] [Google Scholar]
- 17.Khan NA, Daskalopoulou SS, Karp I, et al. Sex differences in prodromal symptoms in acute coronary syndrome in patients aged 55 years or younger. Heart 2017; 103: 863–69. [DOI] [PubMed] [Google Scholar]
- 18.Devon HA, Rosenfeld A, Steffen AD, Daya M. Sensitivity, specificity, and sex differences in symptoms reported on the 13-item acute coronary syndrome checklist. J Am Heart Assoc 2014; 3: e000586. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Lex A, Gehlenborg N, Strobelt H, Vuillemot R, Pfister H. UpSet: visualization of intersecting sets. IEEE Trans Vis Comput Graph 2014; 20: 1983–92. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Wibring K, Lingman M, Herlitz J, Pettersson H, Lerjebo A, Bång A. Clinical presentation in EMS patients with acute chest pain in relation to sex, age and medical history: prospective cohort study. BMJ Open 2022; 12: e054622. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Wibring K, Lingman M, Herlitz J, Ashfaq A, Bång A. Development of a prehospital prediction model for risk stratification of patients with chest pain. Am J Emerg Med 2022; 51: 26–31. [DOI] [PubMed] [Google Scholar]
- 22.van Oosterhout REM, de Boer AR, Maas AHEM, Rutten FH, Bots ML, Peters SAE. Sex differences in symptom presentation in acute coronary syndromes: a systematic review and meta-analysis. J Am Heart Assoc 2020; 9: e014733. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Brush JE Jr, Krumholz HM, Greene EJ, Dreyer RP. Sex differences in symptom phenotypes among patients with acute myocardial infarction. Circ Cardiovasc Qual Outcomes 2020; 13: e005948. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
De-identified participant data will be made available after publication on reasonable request to the corresponding author, following approval of a proposal and a signed data use agreement.