Abstract
Introduction
The addition of compulsive sexual behavior disorder (CSBD) into the ICD-11 chapter on mental, behavioral, or neurodevelopmental disorders has greatly stimulated research and controversy around compulsive sexual behavior, or what has been termed “hypersexual disorder,” “sexual addiction,” “porn addiction,” “sexual compulsivity,” and “out-of-control sexual behavior.”
Objectives
To identify where concerns exist from the perspective of sexual medicine and what can be done to resolve them.
Methods
A scientific review committee convened by the International Society for Sexual Medicine reviewed pertinent literature and discussed clinical research and experience related to CSBD diagnoses and misdiagnoses, pathologizing nonheteronormative sexual behavior, basic research on potential underlying causes of CSBD, its relationship to paraphilic disorder, and its potential sexual health consequences. The panel used a modified Delphi method to reach consensus on these issues.
Results
CSBD was differentiated from other sexual activity on the basis of the ICD-11 diagnostic criteria, and issues regarding sexual medicine and sexual health were identified. Concerns were raised about self-labeling processes, attitudes hostile to sexual pleasure, pathologizing of nonheteronormative sexual behavior and high sexual desire, mixing of normative attitudes with clinical distress, and the belief that masturbation and pornography use represent “unhealthy” sexual behavior. A guide to CSBD case formulation and care/treatment recommendations was proposed.
Conclusions
Clinical sexologic and sexual medicine expertise for the diagnosis and treatment of CSBD in the psychiatric-psychotherapeutic context is imperative to differentiate and understand the determinants and impact of CSBD and related “out-of-control sexual behaviors” on mental and sexual well-being, to detect forensically relevant and nonrelevant forms, and to refine best practices in care and treatment. Evidence-based, sexual medicine–informed therapies should be offered to achieve a positive and respectful approach to sexuality and the possibility of having pleasurable and safe sexual experiences.
Keywords: compulsive sexual behavior, hypersexuality, impulse control disorder, ICD-11, sex/porn “addiction”, comorbidity, paraphilias, assessment, diagnosis, treatment
Introduction
The notion that “out of control,” driven sexual behavior associated with distress and negative consequences is considered a mental disorder is still quite controversial.1 On one hand, compulsive sexual behavior (CSB) has a diagnostic formulation as a CSB disorder (CSBD) that was included as an impulse control disorder in the International Classification of Diseases, Eleventh Revision (ICD-11).2 On the other, it was not included as “hypersexual disorder” in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5).3 Moreover, treatment centers have profited from it being labeled an “addiction,” and current social media, periodicals, and online self-help forums have provided a venue for an enormous spread of misinformation regarding its potential causes, severity, and base rates among different populations, especially in North America. This controversy illustrates the lack of consensus regarding the definition and diagnosis and is one in which sexual medicine has a unique perspective and responsibility to address. Therefore, the International Society for Sexual Medicine convened an expert scientific panel to provide a comprehensive review of the current understanding of CSBD as a clinical entity and to what extent empirical data support its potential causes, levels of severity, expression in the population, and comorbidity with other disorders. We then consider what might be best practices in potential care and treatment.
The history of clinical sexology includes attempts to classify “addiction-like” or compulsive forms of sexual behavior. This starts in the clinical literature with von Krafft-Ebing’s description of hyperaesthesia sexualis.4 Since then, various discourses have ensued to describe this clinical phenomenon, and these have been influenced by changing sociopolitical-cultural climates. One of the important discourses has been centered on the boundary between nonnormative sexual behavior (eg, higher sex drive) and a clinical diagnosis of hypersexual disorder or CSB. There is a serious risk of pathologizing sexual behavior that is outside the norm or subject to moral or cultural disapproval. Another discourse has dealt with the etiologic or classification question: Is the phenomenon a sexual disorder, an “addiction,” an “impulse control disorder,” or an “obsessive-compulsive disorder”? Does the phenomenon have paraphilic and nonparaphilic modes of expression? How can it be assessed, the differences distinguished, and what are the underlying mechanisms or correlates?
There is not enough space here to go into detail about the different disputes that marked the consideration of this phenomenon for inclusion in the DSM and ICD historically. Nevertheless, regarding the DSM-5, there was a proposal for the conception and criteria of a diagnosis of hypersexual disorder for inclusion, as well as careful literature reviews from the working group,5 available measurement instruments, and a completed field trial.6 However, the Board of Trustees of the American Psychiatric Association decided in the end not to include the diagnostic category in the DSM-5 or its 2022 text revision. The 2 overarching reasons involved insufficient scientific evidence that the proposed criteria represented a distinct clinical syndrome and concerns about potential misuse of the hypersexual disorder diagnosis in forensic settings.7-9
The initial situation for the ICD-11 was considerably different. Although the diagnosis of “excessive sexual drive” had a shadowy existence without empirical research support, it had existed in the form of “satyriasis” and “nymphomania” in early versions of the ICD and as part of the chapter on sexual dysfunctions within the ICD-10. However, a more precise description of the diagnostic prerequisites and detailed research criteria were absent. The diagnosis was hardly used according to our clinical impression but also according to data from published research (eg, no hits if one enters the terms “excessive sexual drive” and “ICD-10” in MEDLINE). This raised the question of whether a new diagnostic category of the phenomenon should exist and to which chapter it should be assigned.
Aspects associated with the clinical syndrome might affect various aspects of sexual health and well-being at the individual and cultural levels.10-13 CSBD is often associated with negative attitudes about sexuality and excessive guilt about one’s sexual behavior that can interfere with feelings of pleasure and satisfaction and create distress. That guilt may be due to religious or cultural values, which might stigmatize certain sexual behaviors (eg, masturbation, use of erotica, same-sex relationships).14 CSBD can also be associated with coercive sexual behavior involving experiences of being a victim of sexual violence.12 There can be an increased risk of sexually transmitted infections or other health problems.15,16 In addition, CSBD can be associated with difficulty developing or sustaining intimate relationships, as well as communication and relationship problems.17 Thus, sexual health and well-being are hindered among people with CSBD, and given the currently known prevalence, this is a serious public health problem for societies.11,17-19
Thus, since there is public health relevance for CSBD, the elimination of this category was less in question than a revision of the terminology and its placement as a diagnostic category. There was quite a debate of whether to place this syndrome in disorders due to addictive behavior, along with gambling or gaming disorder, or to place it as a type of impulse control disorder. Other considerations were to place it within obsessive-compulsive disorders (OCDs) or with sexual dysfunctions, which were moved out of the chapter on mental and behavioral disorders and into a new chapter of “conditions related to sexual health.” The final decision was to place this in the subchapter of impulse control disorders and to name it CSBD. Central to the diagnostic criteria were difficulties with sexual self-control over a prolonged time that are associated with distress. In the ICD-11 guidelines,2,20 however, a deliberate attempt was made to prevent the risk of overpathologizing. Distress caused by overpathologizing nonnormative sexual behavior, especially by moral judgments and disapproval, does not qualify for the diagnosis. The description of CSBD says that it is “characterized by a persistent pattern of failure to control intense, repetitive sexual impulses or urges resulting in repetitive sexual behavior. Symptoms may include repetitive sexual activities becoming a central focus of the person’s life to the point of neglecting health and personal care or other interests, activities, and responsibilities; numerous unsuccessful efforts to significantly reduce repetitive sexual behavior; and continued repetitive sexual behavior despite adverse consequences or deriving little or no satisfaction from it. The pattern of failure to control intense sexual impulses or urges and resulting repetitive sexual behavior is manifested over an extended period of time (eg, six months or more), and causes marked distress or significant impairment in personal, family, social, educational, occupational, or other important areas of functioning. Distress that is entirely related to moral judgments and disapproval about sexual impulses, urges, or behaviors is not sufficient to meet this requirement.”2
CSBD may be expressed in a variety of behaviors, such as sexual behavior with others, masturbation, use of pornography, or cybersex (internet sex). Although precise diagnostic requirements for CSBD are an important step, the potential for overpathologizing still exists on the basis of moral judgments or societal disapproval, indeed even in misguided self-diagnosis. CSBD must be carefully differentiated from other mental or sexual disorders, such as paraphilic disorder; it must be determined whether it stems from moral guilt; and it must be distanced from the kind of unscientific information and misguided beliefs that proliferate on social media, such as the notion that plasma androgens are lost during sexual activity21 or that watching pornography results in “pornography-induced erectile dysfunction.”22-24
What CSBD is and what it is not
Despite the proliferation of CSB-related studies in the past 2 decades and the inclusion of an official diagnosis for CSBD in the ICD-11,2,25,26 one of the most fundamental questions regarding CSBD still pertains to the accurate identification of those experiencing CSBD. This is critical to avoid pathologizing normal sexual behaviors or misdiagnosing individuals and to provide adequate care for everyone seeking treatment for one’s sexual behaviors.27-29 Persons with CSBD present themselves clinically and socially with a perception of out-of-control sexual behavior, extreme guilt over sexual gratification, and distress related to the adverse consequences of repetitive sexual behavior and/or the lack of satisfaction from it. This might include guilt and shame over masturbation, online pornography use, intrusive sexual thoughts, and sexual activity with others outside a relationship or established social boundaries. This has been popularized in the media as a “sex addiction” or “porn addiction” and therefore as a disorder, but it is also portrayed in some scientific publications as being “reminiscent” of addiction and attributed to the kind of sensitized brain dopamine function observed in drug addiction.30 Sex or pornography addiction, in turn, has been used in the media as a catch-all physiologic process underlying the perceived behavior that leads to guilt, shame, or feelings of distress or to perceived conditions in which sexual responses are blunted (eg, in pornography-induced erectile dysfunction), in which people who view pornography and presumably masturbate compulsively become unable to gain or sustain erections to their partners or indeed to previously utilized pornography vignettes. Instead, they seek out new pornography vignettes or partners that they find exciting enough to induce erection and allow masturbation or sexual activity. An industry based on the principles of Alcoholics Anonymous has grown around the treatment of “sex addiction” and “porn addiction” since the 1980s.31,32 This industry is directly related to the increased concept of addiction to describe any excessive, out-of-control behavior and to the proliferation of self-help groups, which are modeled after 12-step groups and treatment programs that have been helpful for people with substance use disorders.
From a diagnostic perspective, CSBD should be recognized as a distinct and clearly defined clinical disorder2 that is differentiated from other disorders (eg, paraphilias, persistent genital arousal disorder33). In addition, it must be acknowledged that feeling a loss of control and the perceived consequences of uncontrolled sexual behavior represent subjective experiences largely influenced by individual values, beliefs, cultural norms, environmental expectations, and personality characteristics.34 To avoid overpathologizing individually unacceptable, socially unacceptable, or high-frequency sexual behavior, a restriction was added to the diagnostic requirements that one’s distress should not be exclusively related to moral judgment or social disapproval.2,26 However, some clinicians have argued that feelings of moral incongruence toward pornography viewing, masturbation, extramarital sex, or other sexual behaviors should not arbitrarily disqualify one from receiving a diagnosis of CSBD, and its role in the etiology and definition of CSBD warrants additional understanding and further study.28,29
Another challenge of the initial clinical assessment is to rule out “false CSBD presentations,” as a CSBD mental disorder diagnosis may be used by a patient or partner as a convenient excuse for sexual misconduct (eg, when a sexual affair is discovered by a partner). Therefore, assessing one’s motivation to seek treatment is an important part of the evaluation.35
Clinicians may be misled by the fact that emotional dysregulation was not included in the ICD-11 diagnostic guidelines of CSBD. However, it is recognized as an “additional clinical feature” in which “individuals with CSBD often engage in sexual behavior in response to feelings of depression, anxiety, boredom, loneliness, or other negative affective states,”2 and the relationship between emotional regulation and sexual behavior was described as an important aspect of treatment planning.2,36,37
Several important limitations of CSBD research are pertinent. First, CSBD research has been conducted mainly in Western countries18 and largely on cisgender heterosexual males. Less is known about the specific needs for CSBD assessment of males in non-Western cultures or in the context of women and sexually diverse people.38 Clinical presentations of CSBD and therapeutic needs in those populations may differ. For example, women more commonly report engaging in sexual fantasies and/or seductive behaviors that lead to multiple affairs, participating in sadomasochistic behavior or sex work, and describing themselves as “love addicted.” Relative to men, women also exhibit higher sexual anxiety and depression, external sexual control, and fear of sexual relationships.39-43 More research is needed to improve clarity and instrumentation adapted to clinical assessments of these understudied groups and cultures, especially since the etiology and expression of CSBD may vary as a function of culture.
How much is too much?
Two of the important aspects of the CSBD diagnostic criteria are impulse control problems and moral disapproval. First, we review the scientific evidence on whether the quantity of engagement in sexual behaviors might be considered an objective, reliable indicator of control problems in CSBD. Then we discuss the role of moral disapproval in self-labeling one’s sexual behavior as out of control, compulsive, or addictive-like and thus in need of therapy. To explore these issues, we examine the literature on problematic pornography, as >80% of those seeking treatment for CSBD report problematic pornography use (PPU),7,44 which is the most commonly studied CSB in scientific reports.25
The frequency or amount of a given behavior or activity is a potential objective indicator of control problems (eg, frequency of alcohol consumption45-47). However, when we examine behaviors that derive from natural appetitive drives, such as sexual behavior, it is more challenging to draw the line between “normal” and “dysregulated” behavior, as people’s sexual desires and experiences may vary substantially. This variability, even extreme forms, is normal if the behavior does not cause distress, impairment, or other functional problems.5,48 For example, findings from a recent meta-analysis of 61 studies suggest that the quantity of pornography use has a positive moderate association with PPU,49 indicating that a higher quantity of pornography use is associated with more severe PPU. Yet, the association was only moderate, and the frequency of pornography use was identified as the most peripheral symptom of PPU in particular and CSBD in general in network analytical studies of general and treatment-seeking populations.50,51 Thus, the frequency or quantity of pornography use alone might not accurately differentiate those with and without control problems.
This notion was supported by large-scale studies in general and treatment-seeking populations.52-54 In addition to the groups that rarely used pornography and did not experience control problems (ie, nonproblematic users, 68%-76% of users) and those that used pornography frequently and identified as PPUs (ie, problematic users, 3%-12%),52,54 2 other groups emerged that might be important for differential diagnosis. Some used pornography as frequently as problematic users but did not report control problems.53-55 Still others used pornography rarely but experienced self-perceived PPU. In one study, the high-frequency nonproblematic group comprised 19% to 29% of the users52 and may represent those with high sexual desire whose sexual behaviors align with their needs and do not cause adverse consequences in their lives.56,57 Indeed, the number of people with nonproblematic high-frequency use was 3 to 6 times higher than that with problematic high-frequency use, suggesting that frequent pornography use, per se, is not necessarily problematic.
The fourth group of pornography users were those who watched pornography rarely yet were highly distressed about it (approximately 12% of users54). This occurred presumably due to moral disapproval of pornography use and perhaps masturbation.58 According to the early propositions of the moral incongruence model of pornography use,59,60 PPU may appear due to not only control problems or dysregulation but also high levels of religiosity and/or moral incongruence toward pornography use, making the associations between self-perceived PPU and religiosity, moral disapproval, and incongruence complex. Based on findings of nationally representative and large-scale cross-sectional and longitudinal studies, moral incongruence may be best conceptualized as a moderator of the association between pornography use frequency and moral disapproval of pornography use (“ie, feeling as if one’s behaviors and one’s values about those behaviors are misaligned”60). The associations between pornography use frequency and self-perceived PPU can be stronger among those with higher levels of moral disapproval, resulting in feelings of PPU despite the relatively low frequency of pornography use.61 Similarly, according to a recent systematic review,62 although small to moderate direct positive associations can be seen between religiosity and PPU, the interaction between religiosity and pornography use frequency may be a more accurate predictor of self-perceived PPU. Studies including adults and adolescents also reported that pornography use frequency was more strongly related to self-perceived PPU at higher levels of religiosity.63,64 Thus, religiosity and moral disapproval of pornography use may play crucial roles in self-perceived PPU, as evidenced by findings suggesting that 1 in 4 treatment-seeking men may not have objectively dysregulated or high-frequency pornography use but still seek help due to moral incongruence.53,65
In sum, the frequency and amount of pornography use is not, in itself, a reliable indicator of control problems in PPU or CSBD. Using it as an exclusive measure of PPU or CSBD could easily result in overestimation of people with PPU and associated pathologizing of high sexual desire or passion,56,57,66–68 in addition to the erroneous loss of cases with self-perceived PPU who may not use pornography frequently.29,53,54 Therefore, a precise assessment (eg, with well-validated scales69-71 and/or clinical interviews adapted culturally for diverse populations) and differential diagnosis are needed to determine whether PPU stems from sexual self-control problems, moral disapproval of pornography use, or both, as all may trigger treatment seeking but not all be diagnosed as CSBD. Self-identifying as having PPU purely due to the distress driven by moral disapproval of pornography use is not and should never be sufficient to diagnose PPU.28 Similarly, high-frequency pornography use without impaired control and related adverse consequences should not be diagnosed as PPU.52 We note that much of the data so far on PPU have come from the United States, Poland, and China, and it is possible that other cultures exist where pornography use is not considered a problem.
Neurochemical and neuroanatomic mechanisms
To understand the potential neural bases of CSBD and especially how moral incongruence could lead to more sexual arousal associated with the prospect of engaging in sexual activity, it is necessary to understand how sexual behavior is organized in the nervous system. Different aspects of sexual behavior are controlled by excitatory and inhibitory neurochemical mechanisms in the brain and the spinal cord72 (Figure 1). These form the biological basis of the dual control model first proposed by Bancroft and Janssen73 and later augmented by Perelman,74 who added the idea of a labile tipping point between the two. These systems place the behavior into a flow from appetitive to consummatory to satiety, which overlaps with the 4-stage models proposed by Moll75 and Masters and Johnson,76 as refined by Kaplan68 and Georgiadis et al.77 Excitatory systems such as mesolimbic dopamine and hypothalamic melanocortin activate sexual desire and attention toward external sexual cues, while hypothalamic dopamine, noradrenaline, and oxytocin help to switch on the parasympathetic control of genital blood flow that creates and augments genital arousal.72 As sympathetic tone ramps up during sexual interaction, a spinal switch releases it to create sexual climax, which is registered in the brain as orgasm. The ecstatic pleasure of orgasm is likely mediated by endogenous opioid release (eg, β-endorphin), whereas the longer-lasting state of satiety and relaxation is likely mediated by serotonin.72 The inhibition induced by satiety is consonant with sexual refractoriness.
Figure 1.

Dual control model shows the neurochemical mechanisms of excitation and inhibition derived from Bancroft and Janssen73 and Perelman74 and detailed by Pfaus.72 Drugs or psychological states that activate those mechanisms can shift an individual into general sexual excitation or inhibition. In cases of compulsive sexual behavior disorder, individuals are in states of excitation and/or disinhibition.
Mesolimbic dopamine activation is a common neurochemical mediator of motivation, desire, and wanting/craving for all motivational systems.78,79 It does not mediate sexual reward per se; rather, it underlies the process of sustained attention to and movement toward cues that predict sexual reward, especially those related to pleasure and orgasm.80 Mesolimbic dopamine release can be phasic or tonic in response to cues, and these release patterns correspond in sexual behavior to appetitive and consummatory processes, respectively.81 Thus, in this conceptualization, seeking out stimuli associated with a goal would be an appetitive response, whereas acting on the goal once it is obtained would be a consummatory response. Some cues are prepotent, produce arousal, and are innately preferred (eg, visual sexual cues depicting primary and secondary sex characteristics, beautiful faces/bodies, stimulating or comforting auditory cues, music that gives one “chills,” certain food- or fluid-related cues, preferred pet animals, smells). Preference for other cues is learned through their pairing with and thus prediction of arousal and pleasurable gratification. In all cases, mesolimbic dopamine is a mediator of cue strength, and its transmission in regions of the brain, such as the amygdala and ventral striatum or nucleus accumbens, will be augmented in response to cues that predict reward (Figure 2). This has been observed in brain imaging and functional magnetic resonance imaging studies of self-identified problematic pornography users or “sex addicts” relative to controls.82,83
Figure 2.

Modified inverted optimality curve. (A) Response competence as a function of reward strength. (B) Mesolimbic/mesocortical dopamine transmission intensity (straight line and arrow) overlaid on panel A. Dopamine release mediates goal and cue seeking, with the conscious interpretation of “wanting,” “liking,” and “needing,” depending on the intensity of the dopamine response.78,79 Thus, dopamine mediates normal reactivity and hyperreactivity to cues that generate sexual arousal and anticipate sexual reward. But as this moves from attentional balance to attentional bias and lock, the dopamine response mediates the compulsivity observed in compulsive sexual behavior disorder, leading ultimately to the kind of attentional lock reminiscent of drug addiction. The shaded area is where the dopamine response mediates the type of hyperattention to sexual stimuli observed in compulsive sexual behavior disorder.
In addition to prepotent cues, a potent driver of mesolimbic dopamine transmission is “reward prediction error,”84 in which the real reward intensity or occurrence does not conform to the prediction based on past experience. When this happens, dopamine transmission is augmented, resulting in a focus of attention on other details or responses that might explain the discrepancy and bring the predicted reward back. With respect to CSBD, guilt and forced abstinence are hypothesized to create a reward prediction error (ie, individuals want something that they “should not have” and try to avoid). The augmented dopamine response to cues that predict reward under such circumstances (eg, fantasy, pornographic imagery) contributes to intrusive thoughts and arousal,85,86 and sexual rewards experienced on high arousal can become highly preferred and garner preferential attention.35,87,88 This can feed back to strengthen the feeling of guilt as a preparatory state that predicts highly arousing rewards. Thus, although guilt, as a form of frontal lobe–mediated inhibition that is part of “executive function,” can lead to short-term decreases in unwanted behaviors, such decreases might create a schedule of intermittent reinforcement in the long term that strengthens the arousal-reward connection.89
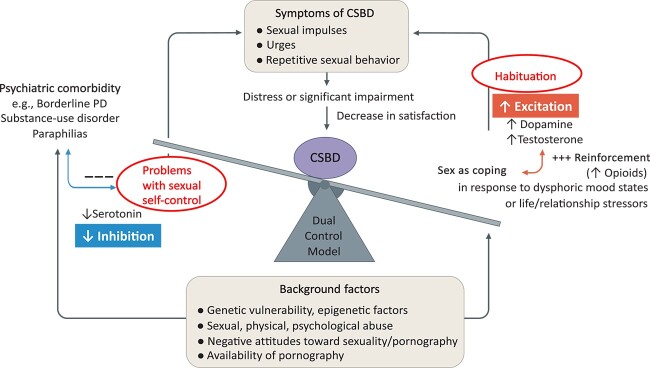
As mentioned earlier, what prevents sexual behavior and pornography use from being an “addiction” are the natural inhibitory states activated with orgasm and climax that give rise to refractoriness.72*,77 At the level of the spinal cord, these involve the activation of sympathetic outflow in spinal circuits that generate climax and open blood vessels so that blood can move from the periphery back to the core, thus preventing erection for a time. In the brain, orgasms activate opioid and serotonin transmission. Both inhibit dopamine release and cell body activation in the short term, but opioids in particular sensitize dopamine release in the long term to unconditioned and conditioned cues that predict reward.72 Refractoriness and satiety occur after natural rewards, but they do not occur—or they occur differently—from drug reward or electrical brain stimulation reward. Thus, there is no withdrawal state after sex. The inability to experience genital arousal in self-perceived pornography-induced erectile dysfunction, for example, would be predicted to reverse itself if the individual allows the refractory state to wear off. This will strengthen the dopamine response to erotic cues as one will no longer be in a state of chronic refractoriness from compulsive masturbation. Instead, one will seek out more stimulating erotic material on the internet or elsewhere, which can then activate excitatory neural systems under residual refractoriness. This is often interpreted as evidence of “tolerance” in behavioral addiction models.30,31,90 Figure 3 shows psychological and neurobiological processes that conspire to excite and disinhibit sexual responses in CSBD.
Figure 3.
Psychological and neurobiological mechanisms that underlie the maintenance of excitation and disinhibition in compulsive sexual behavior disorder. After Briken.102
As with autonomic function, arousal states can habituate if the appetitive behaviors become routine, leading to less potent gratification and a dampening of mesolimbic dopamine response over time. This also leads to the perception that “normal” sexual stimuli no longer arouse the person because the individual is “addicted” to abnormally high arousal states to function sexually. An analogy here would be to those who are risk takers vs those who are risk averse.84,91,92 Dishabituation can occur in response to different erotic stimuli that are perceived to be of higher arousing potential. If people spend inordinate amounts of time seeking out stimuli of ever-higher arousing potential, to the exclusion of other need states or rewards, such behavior can resemble an OCD or an “addiction.” All of this is driven in large part by the focused attention and appetitive responses mediated by mesolimbic dopamine in states of high transmission due to reward prediction error (Figures 2 and 3). In this case, reward prediction error can be produced by guilt, intermittent reinforcement, and seeking more and more arousing stimuli to overcome the effects of habituation or chronic refractoriness.
In contrast, in drug addiction, withdrawal typically results in a hyperaccentuation of physiologic processes that the drug suppresses. For example, opiates induce a state of analgesia. Withdrawal from opiates results in hyperalgesia where simple touch can be experienced as painful.93 Thus, instead of pornography-induced erectile dysfunction, the experience of withdrawal from a chronic inhibitory state induced by masturbation should be hyperexcitation that would mitigate against the apparent need for more and more arousing imagery or actions. Indeed, withdrawal (abstinence) from pornography use by persons who self-identify as PPUs or are diagnosed with CSBD induces frequent intrusive sexual thoughts, higher sexual arousal, and increased out-of-control sexual desire as compared with nonabstinent periods.86
Although there are no a priori data predicting who will and will not display CSBD, some neuroanatomic correlates have emerged in brain studies of CSBD cases relative to non-CSBD cases. This goes back to the original findings of hypersexuality in individuals with frontal lobe damage or Kluver-Bucy syndrome.94 In addition to hyperresponsiveness of mesolimbic dopamine, there is a general finding that the regions in the left hemisphere that mediate excitation are hyperresponsive, whereas regions in the right hemisphere that mediate inhibition are hyporesponsive. This includes greater left amygdala volume in CSBDs and other OCDs95 and greater activation in the left striatum, inferior parietal lobe, dorsal anterior cingulate gyrus, thalamus, and dorsolateral prefrontal cortex in response to visual sexual stimuli in CSBDs relative to non-CSBDs.96 Conversely, more pornography consumption is correlated with lower right striatum volume (gray matter) and increased activation of the right striatum by visual sexual stimuli, although lower functional connectivity of the right striatum to the left dorsolateral prefrontal cortex is observed.97 However, it is not known whether functional differences in these neuroanatomic correlates mediate CSBD or hypersexual responses or whether they are caused by the experiential mechanisms previously described. Most important, finding increased activation of these sites or mesolimbic dopamine (DA) terminal regions, such as the nucleus accumbens, in response to visual sexual stimuli or fantasies is not by itself evidence of CSBD.
Comorbidities and differential diagnoses
Another concern regarding the accurate assessment of CSBD stems from the fact that CSB can manifest secondary to other mental health or medical conditions. It is well documented that CSB commonly co-occurs with anxiety disorders (46%-96%), mood disorders (39%-81%), attention-deficit/hyperactivity disorder (18.7%), as well as substance use disorders (46%-71%).42,98-101 Clinicians should be able to distinguish CSBD from CSB that stems from comorbid conditions, especially when the CSB does not meet the diagnostic criteria for CSBD. A differential diagnosis is important because it leads to different therapeutic approaches.102
Impaired control over sexual impulses, urges, or behaviors may occur in patients during manic, hypomanic, or mixed episodes,103-105 as well as in people with neurocognitive impairment (ie, brain lesions within frontal lobes and temporolimbic areas, in some cases of Tourette’s syndrome)106-108 or personality disorders (especially borderline)109-112 or while under the influence of alcohol, illicit drugs, or some medications.113-118 Dysregulation of emotion has been found as a predisposing factor to CSB, where sexual arousal and its release through sexual activity may serve as a learned way of coping with negative mood states.102 In fact, CSB co-occurs with social anxiety and all types of mood disorders, such as major depression, bipolar disorder, and dysthymia.99,105,119-122 These cases need additional evaluation to decide whether CSBD should be diagnosed as a separate condition or whether the pattern of behavior should be more appropriately diagnosed as a different mental health disorder or medical condition. Despite use of the term compulsive within the diagnostic category, CSBD is not considered a subtype of OCD. Contrary to CSBD, compulsions in OCD commonly occur in response to intrusive, unwanted, anxiety-provoking thoughts and are not considered pleasurable.2 Nevertheless, OCD and CSBD may be diagnosed as separate comorbid conditions123 that influence each other.
According to the ICD-11, CSBD diagnosis should not be assigned if (1) there is no evidence of a persistent failure to control sexual impulses, urges, or behaviors and the presence of all other diagnostic requirements outside of mood episodes; (2) sexual disinhibition due to neurocognitive disorder is attributed to primary disease; and (3) impaired control over sexual impulses, urges, or behaviors is due to the direct effect of psychoactive substances, including recreational drugs or medications, on the central nervous system, with the onset corresponding to use of the substance or medication.2 Clinicians should be aware that the use of drugs such as methamphetamine, gamma-hydroxybutyric acid, gamma-butyrolactone, and alkyl nitrites (“poppers”) to facilitate engagement in sexual activity or to enhance pleasure from it, described as “chemsex,” may also lead to uncontrolled and risky sexual behavior124 given their common disinhibitory actions on brain dopamine turnover.125 The patterns of substance use (ie, contexts) and their relationship with sexual behavior (motivation, sequencing, impact) should be carefully investigated. As pointed out in the ICD-11, diagnosis of CSBD may be assigned with a disorder due to substance use if the diagnostic requirements for both disorders are met.
Paraphilic disorders represent another diagnostic entity that partially overlaps with CSBD. One diagnosis does not necessarily exclude the other, as they may be present as comorbid conditions in up to 30% of cases.126-128 In CSBD, sexual fantasies, urges, or behaviors occur regardless of the focus of sexual arousal, while in paraphilic disorder they are related to patterns of atypical sexual arousal. According to the ICD-11, comorbid CSBD would not be diagnosed if an individual is able to exercise some degree of control over the behavioral expressions of the arousal pattern.2 In those who are sexually compulsive, craving for more and more differentiated excitement may lead to searching for deviant, even preference-dystonic, paraphilia-related content and penalized behavior.31 However, co-occurrence of paraphilias such as pedophilia, sexual sadism, or exhibitionism with CSB may pose an increased risk for sexual (re)offending.129,130 For these cases, recognition of CSB features may become especially relevant for the development of successful treatment strategy and reoffense prevention.
CSBD and the forensic context
Evidence of the dynamic risk factors characterizing sexual offenders suggests that CSB predicts sexual offending recidivism in male criminal samples.131-133 CSB or markers of CSB (eg, excessive pornography use) also predicted sexual violence in the context of domestic violence and intimate partner sexual aggression.134,135 Furthermore, community women reporting sexual aggression against men revealed increased sexual compulsivity as compared with their nonaggressive female counterparts.136 Despite the general desire to destigmatize and limit overpathologizing, the predictive role of CSB in sexual offending gives the CSBD diagnosis potentially detrimental implications in the forensic context.137-139 Indeed, understanding the dynamics of CSBD symptomatology is of practical interest to establish the mental state of an offender and hence to make inferences about his or her criminal responsibility.139 Within that regard, the concept of “control” is a fundamental aspect to determine whether the offender was mentally capable of reasoning about and taking control over his or her actions. The legal concept of guilt or criminal responsibility involves such a capacity. However, we must stress that the legal definitions and implications associated with the concept of criminal responsibility vary substantially across countries and legal systems. Accordingly, while some legal systems consider sexual compulsivity a proxy of diminished ability to control, other systems do not.102,139 Criminal sentences will likely differ between those systems.
Although a discussion of legal systems is beyond the scope of this article, it is worth noting that many health professionals, including professionals in the field of sexual medicine, could have a role as expert witnesses in sexual offender cases. In that regard, understanding the core presentation and dynamics of CSBD is paramount. The placement of CSBD in the impulsivity disorders section of the ICD-11 highlights the capacity to control sexual impulses or urges as a central feature of the disorder. While the DSM-5 task force rejected hypersexual disorder, arguing about the potential misuse of the diagnosis, especially in forensic settings,7 the inclusion of CSBD in the ICD-11 legitimately opens the discussion again and calls for insights on how the lack of control can be conceptualized, assessed, and intervened. Evidence of attempts to resist and reduce CSB may suggest the willingness but incapacity to control. Even when CSB is not accepted as a proxy of diminished culpability—possibly the most frequent scenario—it does have a role in the prevention of criminal recidivism. Therefore, discussion of the forensic implications of CSBD extends to the rehabilitation context of individuals who have sexually offended, including the danger risk assessment before parole or release. Despite the fact that CSBD and sexual offending behavior may co-occur, the former must not be regarded as a criminal entity or as evidence that criminal activity was involved. CSBD cases where criminal activity is suspected must be handled by clinical forensic experts, following their national legislation.
Role of the sexual medicine expert in diagnosis and treatment
Making a diagnosis of CSBD requires a careful assessment, which would include a thorough sexual history and examination of current symptomology. It would also involve taking a somatic and psychiatric history to exclude somatic causes of CSB (eg, neurologic disease or side effects of drugs or medication). In addition, the examining person must be able to perform a psychiatric assessment to make a differential psychiatric diagnosis and identify mental health comorbidities. These include mood and anxiety disorders, substance use disorders, posttraumatic stress disorder, and personality disorders. Diagnosticians should be able to select and evaluate suitable psychometric assessments of CSBD (eg, the CSBD-19, currently available in almost 30 languages18) and other appropriate psychometric instruments designed to help diagnose common mental health comorbidity.
With regard to etiology or predisposing factors, sexual medicine experts have the ability to ask about possible sexual or other traumatic experiences,12 which are known to create attachment problems commonly observed in patients with CSBD140 and other mental disorders (eg, borderline personality disorder, posttraumatic stress disorder).15 In addition, a differential diagnosis related to comorbidity with paraphilic disorders is important. Thus, the expert must also have basic knowledge of paraphilias and in taking a sexual forensic history. This careful assessment should lead to a comprehensive diagnosis to develop an integrative biopsychosocial treatment plan (Figure 4).15,102
Figure 4.
Considerations for diagnostic and case formulation processes.
Sexual medicine experts are uniquely equipped to provide this type of comprehensive assessment and treatment planning. They are also uniquely trained to perform a detailed, thorough, nonjudgmental sexual history, unlike many other medical practitioners. Learning to separate one’s values and take a nonjudgmental professional stance in evaluating a person’s sexual history, current sexual behaviors, and practices is essential.141 Attitudes toward sexuality-related behaviors, such as the use of pornography and casual sex, must be understood within the patient’s sociocultural but also legal context. It is crucial to keep the social dimensions of sexuality and sexual disorders in mind. For example, there are likely to be significant transcultural differences in CSBD and clinical characteristics (eg, attitudes toward PPU).142 In addition, sexual medicine experts have knowledge and expertise regarding a range of sexual behaviors and sexual disorders, as well as an understanding of sociocultural influences, including an appreciation of the effects of minority stress.143 They possess the medical background to understand links to a variety of medical conditions, medications, and drugs known to affect sexual functioning and behavior. There needs to be knowledge about substances that can be used to initiate sex or that may support sexual compulsivity or about the practice of taking substances in different social contexts to enhance sex (eg, practices of chemsex).15 Finally, there should be knowledge of, and thorough inquiries about, the potential connections between sexual dysfunctions and CSBD. Questions about partners and taking a history of the couple’s sexuality should be included in the diagnostic process, as well as an offer of couples counseling if necessary.15,102
After diagnosing CSBD and recognizing the potential comorbid and contributing factors, the crucial step is to develop a biopsychosocial case formulation considering all the complex factors with the broadest possible understanding of the specific role that sexuality plays in contributing to or maintaining the dysfunctional behavior.144 It is important to also explore the nonsexual reasons for the sexual behavior and why that particular sexual behavior was used for those nonsexual reasons. What is the functionality of the sexual symptom, and where does it become dysfunctional? What is repeated in a dysfunctional way, and what goal is the individual trying to achieve? What are typical triggers, emotions, and previous thoughts in connection with and after sexual behaviors? What roles do guilt and shame play, and do they prevent one from talking about sexual fantasies, thoughts, and behaviors? What role do early sexual experiences play (ie, not only of a traumatic nature)? What role do religion, spirituality, and attitudes toward sexuality play? What role do the couple or family system dynamics play in the maintenance of the symptomatology? How are the symptoms involved in partnered or solo sexual behavior? Are there typical patterns of the dysfunctional sexual behavior here—for example, only brief sexual activity with casual partners; only routine, or “vanilla,” sex in the relationship; masturbation to BDSM sex (ie, bondage, discipline [or domination], sadism, and masochism) but no integration of BDSM practices in the relationship; and sexual dysfunction in partnered sex but no sexual dysfunction with masturbation or when using pornography? Again, these are questions that can be answered only by clinicians who have the training and experience of sexual medicine experts.
With the current state of knowledge, we strongly oppose therapeutic interventions that increase the experience of discrimination, stigma, and moral incongruence. This includes approaches that pathologize sexual behavior of sexually diverse individuals, prohibit unilaterally certain sexual behaviors (eg, viewing pornography, masturbation), apply an addiction model with notions of abstinence from sexual behavior, or seek to impose the professional’s moral or religious values on patients under the guise of evidence-based treatment.
Once all of this is clarified, the clinician can develop a theory-based formulation based on integrated models of CSBD treatment (Figure 4).15,102 While there is a commonality among these integrative models, they emphasize different theoretical perspectives and models of sexual and mental health disorders. A primary perspective is a sexological/sexual medicine and sex-positive perspective. Again, to varying degrees, they recognize the influence of the dual control73,145 and tipping point models74,146 but incorporate other theories (eg, family systems and social learning, cognitive and behavioral, attachment and interpersonal15,102) and address the importance of sociocultural influences (eg, moral incongruence,14,59,60 erotic conflicts, and minority stress143).
Processes of care and treatment recommendations
From what has been described so far, we have derived some basic recommendations for the treatment of people with CSBD with special reference to sexual medicine expertise (Table 1). The dual control model provides an evidence-based system that can also be easily communicated with patients. We assume that in CSBD the relationship between excitatory and inhibitory factors is imbalanced toward excitation due to sensitized neurochemical processes that strengthen excitation and produce disinhibition15 (Figure 3). The goal of treatment is for the patient to achieve a satisfactory balance that supports the control of sexual fantasies and compulsive behaviors to reduce the risk of self-harm or harm to others and to reduce distress associated with CSBD.15 The goal is not to renounce sexuality. However, omitting certain sexual behaviors, such as problematic use of online pornography to the exclusion of other sexual behaviors, can be an intermediate goal of treatment. Treatment for CSBD focuses on the functions (including nonsexual functions) that sexual behaviors serve in a person’s life via a sex-positive approach.147
Table 1.
Recommendations regarding intervention trajectories in CSBD: expert opinion.
| Area to be approached | Recommendations |
|---|---|
| Assessment of comorbidities | • Assess the co-occurrence of other mental health and medical conditions, including medications and substance use (alcohol, drugs, other) • Prioritize critical conditions or symptomatology (eg, manic episodes, substance abuse) |
| Risk assessment | • Assess if there is a specific risk posed to partners (eg, sexually aggressive behavior, encounters with nonconsenting individuals, maltreatment) or a sexually transmitted infection risk to the patient/sexual partners, a specific risk of self-harm (eg, suicidal ideation, injuries due to intensive masturbation, or patterns associated with partnered or autoerotic behavior such as smothering) |
| CSBD and detected criminal sexual activity | • Assign criminal cases to experts with a background in forensic sexology (dependent on countries’ legislation) |
| CSBD case formulation a | • Consider the function of the sexual symptom (eg, does it play a role in individual or couple homeostasis?). Special attention to emotional regulation difficulties and relationship dynamics is needed • Consider the context where the symptoms become dysfunctional and what are the consequences of sexually compulsive behavior • Identify the symptom’s triggers (emotional, cognitive, or behavioral triggers) • Identify maintenance factors (eg, lifestyle and routines, rewarding contexts, relationship context) • Consider how the symptoms evolve in solo and/or partner sex or extramarital sex • Consider the role of cultural specificities, religion or spirituality, and sexual attitudes |
| Impact of the intervention | • Identify personal and social barriers to improvement or treatment adherence (eg, guilt, shame, social stigma, partner’s pressure, lack of motivation) • Identify and incorporate treatment opportunities (eg, social support, partner’s awareness) • Identify the need for medication |
| Need of referrals | • In the context of critical pathology/psychopathology, a history of sexual abuse (child or otherwise), or aversive relationship dynamics, consider the referral to other specialties (eg, trauma intervention, couples therapy) as a first-line intervention |
Abbreviation: CSBD, compulsive sexual behavior disorder.
a Need of expertise in sexual medicine/clinical sexology.
This approach is based on a biopsychosocial understanding of sexuality and sexual disorders, and biopsychosocial factors should be considered in the individual treatment plan. As already mentioned, knowledge about sexuality, sexual rights and norms, attitudes, behaviors, motives, and motivation is crucial for the biopsychosocial understanding of CSBD. CSBD is recognized as an impulse control disorder that manifests itself sexually. It deeply affects sexual well-being and the ability to form and maintain satisfactory emotional and sexual relationships; therefore, it should be treated with a transtheoretical and multimodal approach to provide more holistic and individualized therapeutic care.15,102,147,148-150 This needs specific training since it is not automatically taught in medical or psychological education (eg, training in psychiatry, psychotherapy, clinical psychology).
Different psychotherapeutic modalities and techniques can be used, depending on the patient, resources, possibilities, and abilities. Individual therapy, group therapy, and couples therapy are possible modalities. Medical treatment is often utilized.
These treatment choices depend on the following15:
Motivation and compliance
Severity of CSBD symptoms with a special focus on failure to control sexual impulses and urges
Type of CSBD (autoerotic or partnered) and relationship status
Previous medical, psychiatric, sexual, and criminal history
Comorbid somatic disorders (eg, sexually transmitted infection) and psychiatric disorders (especially the association of CSBD with paraphilic disorders or chemsex practices)
In terms of timing, it makes sense to distinguish an initial phase targeting stabilization, motivation, and self-management15,147,148,149 from later, medium-, and longer-term treatment phases that focus on the understanding of the aforementioned functions of sexual behavior, intimacy concerns, and relationship issues.
In a recent systematic review, Antons et al151 identified 24 studies with interventions for CSBD, including 4 randomized controlled studies. In the reviewed studies, the most widely used cognitive behavior therapy components were as follows:
Psychoeducation
Stimulation of motivation and motivation for change (eg, motivational interviewing)
Identification of goals
Awareness of thoughts, emotions, and beliefs
Training on self-regulation and urge management
Skill training: development of problem-solving skills, conflict management, time management, and coping strategies
Mindfulness and meditation exercises
Relapse prevention and maintenance program
Acceptance and commitment therapy has also been used.151 Many of these techniques are especially useful for the initial treatment phase. However, it is remarkable how treatment programs to date have paid little attention to the specificity of the sexual symptom itself,144 the significance of moral incongruence, erotic conflicts, and previous traumatic experiences and have neglected to address attachment, intimacy, and authenticity.
A group of experts from the World Federation of Societies of Biological Psychiatry recently proposed an algorithm15 for the pharmacologic treatment of CSBD (based on Briken and Turner152 and Thibaut et al153). The procedure—and thus the degree of intervention—depends on the severity of the CSBD symptoms. Specifically, it focuses on evidence for the use of pharmacologic treatment, and it describes 3 levels of CSBD (mild, moderate, severe) that guide the proposals for treatment. Roughly described, psychotherapy alone is used at the level 1 treatment and as a basis of all treatment going forward. At level 2, either selective serotonin reuptake inhibitors (eg, escitalopram) or the opioid receptor antagonist naltrexone is considered. At level 3, the combination of these 2 drugs is recommended. These medications have shown some efficacy in the treatment of CSBD but are prescribed “off-label.” For the simultaneous presence of CSBD with paraphilic disorders, there is a separate, longer established algorithm153 that is predominantly oriented toward the risk for other persons and includes testosterone-lowering medications (eg, cyproterone acetate) or gonadotropin-releasing hormone agonists (eg, triptorelin). While these algorithms exist, more evidence is needed on pharmacologic interventions in CSBD. Until now, only 1 randomized controlled trial for paroxetine, naltrexone, and placebo154; 1 prospective open open-label trial with naltrexone155; and some retrospective analyses and case studies15 have been published.
Conclusion
With this article, we have attempted to clarify the role of sexual medicine experts in the diagnosis and treatment of CSBD. We are convinced that the expertise from sexual medicine is essential in adequately assessing and treating those with CSBD. At the same time, we express our concern about treatment approaches that reinforce sex-negative moralizing attitudes about sexuality and are not informed from sexology and sexual medicine training. Without this training and expertise supported by multicultural perspectives, we see a risk of overdiagnosing conditions that do not actually meet the criteria for CSBD, thus increasing moral incongruence and distress. In addition, we strongly recommend that patients with CSBD receive integrated, comprehensive, biopsychosocial, and sexologically informed treatment that goes beyond control over sexual behavior and reduction of sexually dysfunctional behavior but assists patients to achieve sexually healthy and satisfied lives. To accomplish this, the expertise of sexual medicine specialists is indispensable.
Acknowledgments
J.G.P. is chair of the ISSM Subcommittee on Compulsive Sexual Behavior Disorder and Hypersexuality.
The views expressed in this article are those of the authors and do not represent the official policies or positions of the World Health Organization.
Contributor Information
Peer Briken, Institute for Sex Research, Sexual Medicine, and Forensic Psychiatry, University Medical Center, Hamburg-Eppendorf, Hamburg 20251, Germany.
Beáta Bőthe, Department of Psychology, Université de Montréal, Montréal, QC H3C 3J7, Canada; Centre de Recherche Interdisciplinaire Sur Les Problèmes Conjugaux Et Les Agressions Sexuelles, Montréal, QC H3C 3J7, Canada.
Joana Carvalho, William James Center for Research, Department of Education and Psychology, University of Aveiro, Aveiro 3810-193, Portugal.
Eli Coleman, Eli Coleman Institute for Sexual and Gender Health, University of Minnesota, Minneapolis, MN 55454, United States.
Annamaria Giraldi, Sexological Clinic, Mental Health Center, Copenhagen University Hospital, Mental Health Services, Copenhagen CPH 2200, Denmark; Department of Clinical Medicine, Faculty of Health and Medical Sciences, University of Copenhagen, Copenhagen 2200, Denmark.
Shane W Kraus, Department of Psychology, University of Nevada Las Vegas, Las Vegas, NV 5030, United States.
Michał Lew-Starowicz, Department of Psychiatry, Centre of Postgraduate Medical Education, Warsaw 01-809, Poland.
James G Pfaus, Center for Sexual Health and Intervention, Czech National Institute of Mental Health, Klecany 25067, Czech Republic; Department of Psychology and Life Sciences, Faculty of Humanities, Charles University, Prague 18200, Czech Republic.
Author contributions
Conception and design: P.B., J.C., M.L.-S., J.G.P. Acquisition of data: P.B., B.B., J.C., E.C., A.G., S.W.K., M.L.-S., J.G.P. Analysis and interpretation of data: P.B., B.B., J.C., E.C., A.G., S.W.K., M.L.-S., J.G.P. Drafting the manuscript: P.B., B.B., J.C., E.C., A.G., S.W.K., M.L.-S., J.G.P. Revising it for intellectual content: P.B., B.B., J.C., E.C., A.G., S.W.K., M.L.-S., J.G.P. Final approval of the completed manuscript: P.B., B.B., J.C., E.C., A.G., S.W.K., M.L.-S., J.G.P.
Funding
Research from J.G.P.’s laboratory was supported in part by the Canadian Institutes of Health Research (project grant 162264) and by the Grantová agentura České republiky (GA23-06662S). M.L.-S. was supported by the Centre of Postgraduate Medical Education statutory research funding (project 501-1-065-38-22) and receives funding for noncommercial research on pharmacologic interventions in compulsive sexual behavior disorder from the Polish Medical Research Agency (grant 2022/ABM/03/00039). B.B. was supported by a postdoctoral fellowship from the SCOUP Team–Sexuality and Couples–Fonds de recherche du Québec, Société et Culture, and by the Banting Postdoctoral Fellowship from the Social Sciences and Humanities Research Council of Canada. S.W.K. has been supported by grants from the International Center for Responsible Gaming, MGM Resorts International, Center for the Application of Substance Abuse Technologies (University of Nevada, Reno), Massachusetts General Hospital, and Kindbridge Research Institute (GR15685).
Conflicts of interest
J.G.P. is a consultant for FirmTech, Kanna Health, Ovoca Bio/IVIX, Reunion Neuroscience, SmartBod/Lioness, and Vella Bioscience and serves as editor in chief of Current Sexual Health Reports. E.C. serves on the Sexual Health Advisory Committee for Ro, Inc. A.G. has received honoraria for lectures or participation in advisory boards or being a consultant for Viatris, Eli Lilly, Pfizer, Sandoz, Futura Medical/Exeron, Astellas, Novo Nordic, Freya, and Lundbeck. S.W.K. is a board member for the Nevada Advisory Committee on Problem Gambling and the Society for the Advancement of Sexual Health and serves as editor in chief of Sexual Health & Compulsivity. M.L.-S. has received honoraria as a consultant for AbbVie, Angelini, Apotex, Bayer, Berlin Chemie, Biogen, Bristol Myers Squibb, Eli Lilly, European House Ambrosetti, European Foundation of Art Therapy, Lundbeck, Novo Nordisk, OCInfo, Pfizer, Polpharma, Servier, Stada, and Verco. P.B. was a consultant to the World Health Organization regarding the development of the ICD-11 classification of sexual disorders and sexual health.
References
- 1. Fuss J, Lemay K, Stein DJ, et al. Public stakeholders’ comments on ICD-11 chapters related to mental and sexual health. World Psychiatry. 2019;18(2):233–235. 10.1002/wps.20635. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. World Health Organization . International Classification of Diseases, Eleventh Revision. WHO Press; 2019/2021. [Google Scholar]
- 3. American Psychiatric Association . Diagnostic and Statistical Manual of Mental Disorders. 5th ed. American Psychiatric Publishing; 2013. [Google Scholar]
- 4. von Krafft-Ebing R. Psychopathia Sexualis. Rebman FJ, trans. Physicians and Surgeons Book Company; 1886/1929. [Google Scholar]
- 5. Kafka MP. Hypersexual disorder: a proposed diagnosis for DSM-V. Arch Sex Behav. 2010;39(2):377–400. 10.1007/s10508-009-9574-7. [DOI] [PubMed] [Google Scholar]
- 6. Reid RC, Carpenter BN, Hook JN, Garos S, Manning JC. Report of findings in a DSM-5 field trial for hypersexual disorder. J Sex Med. 2012;9(11):2868–2877. 10.1111/j.1743-6109.2012.02936.x. [DOI] [PubMed] [Google Scholar]
- 7. Kafka MP. What happened to hypersexual disorder? Arch Sex Behav. 2014;43(7):1259–1261. 10.1007/s10508-014-0326-y. [DOI] [PubMed] [Google Scholar]
- 8. Halpern AL. The proposed diagnosis of hypersexual disorder for inclusion in DSM-5: unnecessary and harmful. Arch Sex Behav. 2011;40(3):487–488. 10.1007/s10508-011-9727-3. [DOI] [PubMed] [Google Scholar]
- 9. Moser C. Hypersexual disorder: just more muddled thinking. Arch Sex Behav. 2011;40(2):227–229. 10.1007/s10508-010-9690-4. [DOI] [PubMed] [Google Scholar]
- 10. Bőthe B, Vaillancourt-Morel MP, Bergeron S. Hypersexuality in mixed-sex couples: a dyadic longitudinal study. Arch Sex Behav. 2021;50(5):2139–2150. 10.1007/s10508-021-01959-0. [DOI] [PubMed] [Google Scholar]
- 11. Grubbs JB, Floyd CG, Kraus SW. Pornography use and public health: examining the importance of online sexual behavior in the health sciences. Am J Pub Health. 2023;113(1):22–26. 10.2105/AJPH.2022.307146. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Slavin MN, Scoglio AA, Blycker GR, Potenza MN, Kraus SW. Child sexual abuse and compulsive sexual behavior: a systematic literature review. Curr Addict Rep. 2020;7(1):76–88. 10.1007/s40429-020-00298-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Slavin MN, Blycker GR, Potenza MN, Bőthe B, Demetrovics Z, Kraus SW. Gender-related differences in associations between sexual abuse and hypersexuality. J Sex Med. 2020;17(10):2029–2038. 10.1016/j.jsxm.2020.07.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Coleman E, Jennings T, Gleason N, et al. The relationship between compulsive sexual behavior, religiosity, and moral disapproval. J Sex Marital Ther. 2023;49(3):314–330. 10.1080/0092623X.2022.2117746. [DOI] [PubMed] [Google Scholar]
- 15. Turner D, Briken P, Grubbs J, et al. The World Federation of Societies of Biological Psychiatry guidelines on the assessment and pharmacological treatment of compulsive sexual behaviour disorder. Dialogues Clin Neurosci. 2022;24(1):10–69. 10.1080/19585969.2022.2134739. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Gleason N, Smith G, Canning JR, et al. The relationship between alcohol and drug use, compulsive sexual behavior, and condomless anal sex in men who have sex with men: analysis of retrospectively-reported sexual behavior. AIDS Behav. 2023;27(7):2317–2327. 10.1007/s10461-022-03961-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Dickenson JA, Gleason N, Coleman E, Miner MH. Prevalence of distress associated with difficulty controlling sexual urges, feelings, and behaviors in the United States. JAMA Netw Open. 2018;1(7):e184468. 10.1001/jamanetworkopen.2018.4468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Bőthe B, Koós M, Nagy L, et al. Compulsive sexual behavior disorder in 42 countries: insights from the International Sex Survey and introduction of standardized assessment tools. J Behav Addict. 2023;12(2):393–407. 10.1556/2006.2023.00028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Briken P, Wiessner C, Štulhofer A, et al. Who feels affected by “out of control” sexual behavior? Prevalence and correlates of indicators for ICD-11 compulsive sexual behavior disorder in the German Health and Sexuality Survey (GeSiD). J Behav Addict. 2022;11(3):900–911. 10.1556/2006.2022.00060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Reed GM, Drescher J, Krueger RB, et al. Disorders related to sexuality and gender identity in the ICD-11: revising the ICD-10 classification based on current scientific evidence, best clinical practices, and human rights considerations. World Psychiatry. 2016;15(3):205–221. 10.1002/wps.20354. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Prause N. Dhāt syndrome emerges in the United States from anti-masturbation semen retention/NoFap groups. Int J Impot Res. Published online July 8, 2023. 10.1038/s41443-023-00732-2. [DOI] [PubMed] [Google Scholar]
- 22. Landripet I, Štulhofer A. Is pornography use associated with sexual difficulties and dysfunctions among younger heterosexual men? J Sex Med. 2015;12(5):1136–1139. 10.1111/jsm.12853. [DOI] [PubMed] [Google Scholar]
- 23. Ley DJ. The Myth of Sex Addiction. Rowman & Littlefield; 2012. [Google Scholar]
- 24. Park BY, Wilson G, Berger J, et al. Is internet pornography causing sexual dysfunctions? A review with clinical reports. Behav Sci (Basel). 2016;6(3):17. 10.3390/bs6030017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Grubbs JB, Hoagland C, Lee B, et al. Sexual addiction 25 years on: a systematic and methodological review of empirical literature and an agenda for future research. Clin Psychol Rev. 2020;82:101925. 10.1016/j.cpr.2020.101925. [DOI] [PubMed] [Google Scholar]
- 26. Kraus SW, Krueger RB, Briken P, et al. Compulsive sexual behaviour disorder in the ICD-11. World Psychiatry. 2018;17(1):109–110. 10.1002/wps.20499. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Billieux J, Schimmenti A, Khazaal Y, Maurage P, Heeren A. Are we overpathologizing everyday life? A tenable blueprint for behavioral addiction research. J Behav Addict. 2015;4(3):119–123. 10.1556/2006.4.2015.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Gola M, Lewczuk K, Potenza MN, et al. What should be included in the criteria for compulsive sexual behavior disorder. J Behav Addict. 2020;11(2):160–165. 10.1556/2006.2020.00090. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Kraus SW, Sweeney PI. Hitting the target: considerations for differential diagnosis when treating individuals for problematic use of pornography. Arch Sex Behav. 2019;48(2):431–435. 10.1007/s10508-018-1301-9. [DOI] [PubMed] [Google Scholar]
- 30. Toates F. A motivation model of sex addiction—relevance to the controversy over the concept. Neurosci Biobehav Rev. 2022;142:104872. 10.1016/j.neubiorev.2022.104872. [DOI] [PubMed] [Google Scholar]
- 31. Carnes P. Out of the Shadows: Understanding Sexual Addiction. 3rd ed. Hazeldon; 2001. [Google Scholar]
- 32. Coleman E. Evolution of the field of impulsive/compulsive sexual behavior and sexual addiction: a lost opportunity for dialogue. In: Schneider JP, Kaplan D, Lasser M eds. Reflections on the History of the Sex Addiction Field. CreateSpace Independent Publishing Platform; 2017: 23–43. [Google Scholar]
- 33. Goldstein I, Komisaruk BR, Pukall CF, et al. International Society for the Study of Women’s Sexual Health (ISSWSH) review of epidemiology and pathophysiology, and a consensus nomenclature and process of care for the management of persistent genital arousal disorder/genito-pelvic dysesthesia (PGAD/GPD). J Sex Med. 2021;18(4):665–697. 10.1016/j.jsxm.2021.01.172. [DOI] [PubMed] [Google Scholar]
- 34. Grubbs JB, Tahk R, Fernandez DP, Fernandez EF, Ley D. Pornography and pride: antagonism drives links between narcissism and perceived addiction to pornography. J Res Pers. 2023;107:104419. 10.1016/j.jrp.2023.104419. [DOI] [Google Scholar]
- 35. Lew-Starowicz M, Gola M. Compulsive- and other out-of-control sexual behaviors. In: Lew-Starowicz M, Giraldi A, Krüger THC eds. Psychiatry and Sexual Medicine: A Comprehensive Guide for Clinical Practitioners. Springer; 2020: 457–469. [Google Scholar]
- 36. Lew-Starowicz M, Lewczuk K, Nowakowska I, Kraus S, Gola M. Compulsive sexual behavior and dysregulation of emotion. Sex Med Rev. 2020;8(2):191–205. 10.1016/j.sxmr.2019.10.003. [DOI] [PubMed] [Google Scholar]
- 37. Miner MH, Dickenson J, Coleman E. Effects of emotions on sexual behavior in men with and without hypersexuality. Sex Addict Compulsivity. 2019;26(1-2):24–41. 10.1080/10720162.2018.1564408. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38. Kowalewska E, Gola M, Kraus SW, Lew-Starowicz M. Spotlight on compulsive sexual behavior disorder: a systematic review of research on women. Neuropsychiatr Dis Treat. 2020;16:2025–2043. 10.2147/NDT.S221540. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39. Kürbitz LI, Briken P. Is compulsive sexual behavior different in women compared to men? J Clin Med. 2021;10(15):3205. 10.3390/jcm10153205. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40. Ferree MC. Females and sex addiction: myths and diagnostic implications. Sex Addict Compulsivity. 2001;8(3-4):287–300. 10.1080/107201601753459973. [DOI] [Google Scholar]
- 41. Kowalewska E, Kraus SW, Lew-Starowicz M, Gustavsson K, Gola M. Which dimensions of human sexuality are related to compulsive sexual behavior disorder (CSBD)? Study using a multidimensional sexuality questionnaire on a sample of Polish males. J Sex Med. 2019;16(8):1264–1273. 10.1016/j.jsxm.2019.05.006. [DOI] [PubMed] [Google Scholar]
- 42. Kuzma JM, Black DW. Epidemiology, prevalence, and natural history of compulsive sexual behavior. Psychiatr Clin N Am. 2008;31(4):603–611. 10.1016/j.psc.2008.06.005. [DOI] [PubMed] [Google Scholar]
- 43. Sussman S. Love addiction: definition, etiology, treatment. Sex Addict Compulsivity. 2010;17(1):31–45. 10.1080/10720161003604095. [DOI] [Google Scholar]
- 44. Wordecha M, Wilk M, Kowalewska E, et al. “Pornographic binges” as a key characteristic of males seeking treatment for compulsive sexual behaviors: qualitative and quantitative 10-week-long diary assessment. J Behav Addict. 2018;7(2):433–444. 10.1556/2006.7.2018.33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45. Babor TF, Higgins-Biddle JC, Saunders JB, Monteiro MG. AUDIT: The Alcohol Use Disorders Identification Test: Guidelines for Use in Primary Care. 2nd ed. World Health Organization; 2001. [Google Scholar]
- 46. Di Castelnuovo A, Costanzo S, Bagnardi V, et al. Alcohol dosing and total mortality in men and women. Arch Int Med. 2006;166(22):2437–2445. 10.1001/archinte.166.22.2437. [DOI] [PubMed] [Google Scholar]
- 47. Doll R, Peto R, Boreham J, Sutherland I. Mortality in relation to smoking: 50 years’ observations on male British doctors. BMJ. 2004;328(7455):1519–1528. 10.1136/bmj.38142.554479.AE. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48. Reid RC. How should severity be determined for the DSM-5 proposed classification of hypersexual disorder? J Behav Addict. 2015;4(4):221–225. 10.1556/2006.4.2015.041. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49. Chen L, Jiang X, Wang Q, Bőthe B, Potenza M, Wu H. The association between the quantity and severity of pornography use: a meta-analysis. J Sex Res. 2022;59(6):704–719. 10.1080/00224499.2021.1988500. [DOI] [PubMed] [Google Scholar]
- 50. Bőthe B, Lonza A, Štulhofer A, Demetrovics Z. Symptoms of problematic pornography use in a sample of treatment considering and treatment non-considering men: a network approach. J Sex Med. 2020;17(10):2016–2028. 10.1016/j.jsxm.2020.05.030. [DOI] [PubMed] [Google Scholar]
- 51. Werner M, Štulhofer A, Waldorp L, Jurin T. A network approach to hypersexuality: insights and clinical implications. J Sex Med. 2018;15(3):373–386. 10.1016/j.jsxm.2018.01.009. [DOI] [PubMed] [Google Scholar]
- 52. Bőthe B, Tóth-Király I, Potenza MN, Orosz G, Demetrovics Z. High-frequency pornography use may not always be problematic. J Sex Med. 2020;17(4):793–811. 10.1016/j.jsxm.2020.01.007. [DOI] [PubMed] [Google Scholar]
- 53. Chen L, Jiang X, Luo X, Kraus SW, Bőthe B. The role of impaired control in screening problematic pornography use: evidence from cross-sectional and longitudinal studies in a large help-seeking male sample. Psychol Addict Behav. 2022;36(5):537–546. 10.1037/adb0000714. [DOI] [PubMed] [Google Scholar]
- 54. Vaillancourt-Morel M-P, Blais-Lecours S, Labadie C, Bergeron S, Sabourin S, Godbout N. Profiles of cyberpornography use and sexual well-being in adults. J Sex Med. 2017;14(1):78–85. 10.1016/j.jsxm.2016.10.016. [DOI] [PubMed] [Google Scholar]
- 55. Prause N, Pfaus JG. Viewing sexual stimuli associated with greater sexual responsiveness, not erectile dysfunction. Sex Med. 2015;3(2):90–98. 10.1002/sm2.58. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56. Štulhofer A, Bergeron S, Jurin T. Is high sexual desire a risk for women’s relationship and sexual well-being? J Sex Res. 2016;53(7):882–891. 10.1080/00224499.2015.1084984. [DOI] [PubMed] [Google Scholar]
- 57. Štulhofer A, Jurin T, Briken P. Is high sexual desire a facet of male hypersexuality? Results from an online study. J Sex Marital Ther. 2016;42(8):665–680. 10.1080/0092623X.2015.1113585. [DOI] [PubMed] [Google Scholar]
- 58. Prause N. Porn is for masturbation. Arch Sex Behav. 2019;48(8):2271–2277. 10.1007/s10508-019-1397-6. [DOI] [PubMed] [Google Scholar]
- 59. Grubbs JB, Perry SL, Wilt JA, Reid RC. Pornography problems due to moral incongruence: an integrative model with a systematic review and meta-analysis. Arch Sex Behav. 2019;48(2):397–415. 10.1007/s10508-018-1248-x. [DOI] [PubMed] [Google Scholar]
- 60. Grubbs JB, Perry SL. Moral incongruence and pornography use: a critical review and integration. J Sex Res. 2019;56(1):29–37. 10.1080/00224499.2018.1427204. [DOI] [PubMed] [Google Scholar]
- 61. Grubbs JB, Kraus SW, Perry SL, Lewczuk K, Gola M. Moral incongruence and compulsive sexual behavior: results from cross-sectional interactions and parallel growth curve analyses. J Abnorm Psychol. 2020;129(3):266–278. 10.1037/abn0000501. [DOI] [PubMed] [Google Scholar]
- 62. Jennings TL, Lyng T, Gleason N, Finotelli I, Coleman E. Compulsive sexual behavior, religiosity, and spirituality: a systematic review. J Behav Addict. 2021;10(4):854–878. 10.1556/2006.2021.00084. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63. Grubbs JB, Lee BN, Hoagland KC, Kraus SW, Perry SL. Addiction or transgression? Moral incongruence and self-reported problematic pornography use in a nationally representative sample. Clin Psychol Sci. 2020;8(5):936–946. 10.1177/2167702620922966. [DOI] [Google Scholar]
- 64. Rousseau A, Bőthe B, Štulhofer A. Theoretical antecedents of male adolescents’ problematic pornography use: a longitudinal assessment. J Sex Res. 2021;58(3):331–341. 10.1080/00224499.2020.1815637. [DOI] [PubMed] [Google Scholar]
- 65. Jiang X, Wu Y, Zhang K, Bőthe B, Hong Y, Chen L. Symptoms of problematic pornography use among help-seeking male adolescents: latent profile and network analysis. J Behav Addict. 2022;11(3):912–927. 10.1556/2006.2022.00065. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66. Leonhardt ND, Busby DM, Willoughby BJ. Do you feel in control? Sexual desire, sexual passion expression, and associations with perceived compulsivity to pornography and pornography use frequency. Sex Res Social Pol. 2020;18(2):377–389. 10.1007/s13178-020-00465-7. [DOI] [Google Scholar]
- 67. Rosenberg H, Kraus SW. The relationship of “passionate attachment” for pornography with sexual compulsivity, frequency of use, and craving for pornography. Addict Behav. 2014;39(5):1012–1017. 10.1016/j.addbeh.2014.02.010. [DOI] [PubMed] [Google Scholar]
- 68. Kaplan HS. The Sexual Desire Disorders. Brunner-Routledge; 1995. [Google Scholar]
- 69. Bőthe B, Potenza MN, Griffiths MD, et al. The development of the Compulsive Sexual Behavior Disorder Scale (CSBD-19): an ICD-11 based screening measure across three languages. J Behav Addict. 2020;9(2):247–258. 10.1556/2006.2020.00034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70. Bőthe B, Tóth-Király I, Zsila Á, Griffiths MD, Demetrovics Z, Orosz G. The development of the Problematic Pornography Consumption Scale (PPCS). J Sex Res. 2018;55(3):395–406. 10.1080/00224499.2017.1291798. [DOI] [PubMed] [Google Scholar]
- 71. Kraus SW, Gola M, Grubbs JB, et al. Validation of a brief pornography screen across multiple samples. J Behav Addict. 2020;9(2):259–271. 10.1556/2006.2020.00038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72. Pfaus JG. Pathways of sexual desire. J Sex Med. 2009;6(6):1506–1533. 10.1111/j.1743-6109.2009.01309.x. [DOI] [PubMed] [Google Scholar]
- 73. Bancroft J, Janssen E. The dual control model of male sexual response: a theoretical approach to centrally mediated erectile dysfunction. Neurosci Biobehav Rev. 2000;24(5):571–579. 10.1016/S0149-7634(00)00024-5. [DOI] [PubMed] [Google Scholar]
- 74. Perelman MA. The sexual tipping point: a mind/body model for sexual medicine. Sex Med. 2009;6(3):629–632. 10.1111/j.1743-6109.2008.01177.x. [DOI] [PubMed] [Google Scholar]
- 75. Moll A. The Sexual Life of the Child. Macmillan; 1908. [Google Scholar]
- 76. Masters WH, Johnson V. Human Sexual Response. Little Brown; 1966. [Google Scholar]
- 77. Georgiadis JR, Kringelbach ML, Pfaus JG. Sex for fun: a synthesis of human and animal neurobiology. Nat Rev Urol. 2012;9(9):486–498. 10.1038/nrurol.2012.151. [DOI] [PubMed] [Google Scholar]
- 78. Berridge KC, Robinson TE. What is the role of dopamine in reward: hedonic impact, reward learning, or incentive salience? Brain Res Brain Res Rev. 1998;28(3):309–369. 10.1016/S0165-0173(98)00019-8. [DOI] [PubMed] [Google Scholar]
- 79. Koob GF. Hedonic valence, dopamine and motivation. Mol Psychiatry. 1996;1(3):186–189. [PubMed] [Google Scholar]
- 80. Pfaus JG, Kippin TE, Coria-Avila GA, et al. Who, what, where, when (and maybe even why)? How the experience of sexual reward connects sexual desire, preference, and performance. Arch Sex Behav. 2012;41(1):31–62. 10.1007/s10508-012-9935-5. [DOI] [PubMed] [Google Scholar]
- 81. Blackburn JR, Pfaus JG, Phillips AG. Dopamine functions in appetitive and defensive behaviours. Prog Neurobiol. 1992;39(3):247–279. 10.1016/0301-0082(92)90018-A. [DOI] [PubMed] [Google Scholar]
- 82. Golec K, Draps M, Stark R, Pluta A, Gola M. Aberrant orbitofrontal cortex reactivity to erotic cues in compulsive sexual behavior disorder. J Behav Addict. 2021;10(3):646–656. 10.1556/2006.2021.00051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83. Voon V, Mole TB, Banca P, et al. Neural correlates of sexual cue reactivity in individuals with and without compulsive sexual behaviours. PLoS One. 2014;9(7):e102419. 10.1371/journal.pone.0102419. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84. Schultz W. Multiple functions of dopamine neurons. F1000 Biol Rep. 2010;2:2. 10.3410/B2-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85. Lewczuk K, Wizła M, Glica A, Potenza MN, Lew-Starowicz M, Kraus SW. Withdrawal and tolerance as related to compulsive sexual behavior disorder and problematic pornography use—preregistered study based on a nationally representative sample in Poland. J Behav Addict. 2022;11(4):979–993. 10.1556/2006.2022.00076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86. Zimmer F, Imhoff R. Abstinence from masturbation and hypersexuality. Arch Sex Behav. 2020;49(4):1333–1343. 10.1007/s10508-019-01623-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87. Ismail N, Gelez H, Lachapelle I, Pfaus JG. Pacing conditions contribute to the conditioned ejaculatory preference for a familiar female in the male rat. Physiol Behav. 2009;96(2):201–208. 10.1016/j.physbeh.2008.09.013. [DOI] [PubMed] [Google Scholar]
- 88. Kilimnik CD, Meston CM. Sexual shame in the sexual excitation and inhibition propensities of men with and without nonconsensual sexual experiences. J Sex Res. 2021;58(2):261–272. 10.1080/00224499.2020.1718585. [DOI] [PubMed] [Google Scholar]
- 89. Ferster CB, Skinner BF. Schedules of Reinforcement. Appleton-Century-Crofts; 1957. [Google Scholar]
- 90. Blinka L, Ševčíková A, Dreier M, Škařupová K, Wölfling K. Online sex addiction: a qualitative analysis of symptoms in treatment-seeking men. Front Psychiatry. 2022;13:907549. 10.3389/fpsyt.2022.907549. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91. Kahneman D, Tversky A. Prospect theory: an analysis of decision under risk. Econometrica. 1979;47(2):263–292. 10.2307/1914185. [DOI] [Google Scholar]
- 92. Mukherjee K. A dual system model of preferences under risk. Psychol Rev. 2010;117(1):243–255. 10.1037/a0017884. [DOI] [PubMed] [Google Scholar]
- 93. Leng C, Chen L, Gong X, et al. Upregulation of P2X2 and P2X3 receptors in rats with hyperalgesia induced by heroin withdrawal. Neuroreport. 2018;29(8):678–684. 10.1097/WNR.0000000000001018. [DOI] [PubMed] [Google Scholar]
- 94. Klüver H, Bucy P. Preliminary analysis of functions of the temporal lobes in monkeys. Arch Neurol Psychiatr. 1939;42(6):979–1000. 10.1001/archneurpsyc.1939.02270240017001. [DOI] [PubMed] [Google Scholar]
- 95. Schmidt C, Morris LS, Kvamme TL, Hall P, Birchard T, Voon V. Compulsive sexual behavior: prefrontal and limbic volume and interactions. Hum Brain Mapp. 2017;38(3):1182–1190. 10.1002/hbm.23447. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96. Seok JW, Sohn JH. Gray matter deficits and altered resting-state connectivity in the superior temporal gyrus among individuals with problematic hypersexual behavior. Brain Res. 2018;1684:30–39. 10.1016/j.brainres.2018.01.035. [DOI] [PubMed] [Google Scholar]
- 97. Kühn S, Gallinat J. Neurobiological basis of hypersexuality. Int Rev Neurobiol. 2016;129:67–83. [DOI] [PubMed] [Google Scholar]
- 98. Black DW, Kehrberg LLD, Flumerfelt DL, Schlosser SS. Characteristics of 36 subjects reporting compulsive sexual behavior. Am J Psychiatry. 1997;154(2):243–249. 10.1176/ajp.154.2.243. [DOI] [PubMed] [Google Scholar]
- 99. Kafka MP, Prentky RA. Preliminary observations of DSM-III-R Axis I comorbidity in men with paraphilias and paraphilia-related disorders. J Clin Psychiat. 1994;55:481–487. [PubMed] [Google Scholar]
- 100. Raymond NC, Coleman E, Miner MH. Psychiatric comorbidity and compulsive/impulsive traits in compulsive sexual behavior. Compr Psychiatry. 2003;44(5):370–380. 10.1016/S0010-440X(03)00110-X. [DOI] [PubMed] [Google Scholar]
- 101. Ballester-Arnal R, Castro-Calvo J, Gimenez-Garcia C, Gil-Julia B, Gil-Llario MD. Psychiatric comorbidity in compulsive sexual behavior disorder (CSBD). Addict Behav. 2020;107:106384. 10.1016/j.addbeh.2020.106384. [DOI] [PubMed] [Google Scholar]
- 102. Briken P. An integrated model to assess and treat compulsive sexual behaviour disorder. Nat Rev Urol. 2020;17(7):391–406. 10.1038/s41585-020-0343-7. [DOI] [PubMed] [Google Scholar]
- 103. Dvorak RD, Wray TB, Kuvaas NJ, Kilwein TM. Mania and sexual risk: associations with behavioral self-regulation. J Affect Disord. 2013;150(3):1076–1081. 10.1016/j.jad.2013.04.023. [DOI] [PubMed] [Google Scholar]
- 104. Kopeykina I, Kim H-J, Khatun T, et al. Hypersexuality and couple relationships in bipolar disorder: a review. J Affective Disord. 2016;195:1–14. 10.1016/j.jad.2016.01.035. [DOI] [PubMed] [Google Scholar]
- 105. Kowatch RA, Youngstrom EA, Danielyan A, Findling RL. Review and meta-analysis of the phenomenology and clinical characteristics of mania in children and adolescents. Bipolar Disord. 2005;7(6):483–496. 10.1111/j.1399-5618.2005.00261.x. [DOI] [PubMed] [Google Scholar]
- 106. Baird AD, Wilson SJ, Bladin PF, Saling MM, Reutens DC. Neurological control of human sexual behavior: insights from lesion studies. J Neurol Neurosurg Psychiatry. 2007;78(10):1042–1049. 10.1136/jnnp.2006.107193. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107. Freeman RD, Tourette Syndrome International Database Consortium . Tic disorders and ADHD: answers from a world-wide clinical dataset on Tourette syndrome. Eur Child Adosesc Psychiatry. 2007;16(suppl 1):15–23. 10.1007/s00787-007-1003-7. [DOI] [PubMed] [Google Scholar]
- 108. Mendez MF, Shapira JS. Hypersexual behavior in frontotemporal dementia: a comparison with early-onset Alzheimer’s disease. Arch Sex Behav. 2013;42(3):501–509. 10.1007/s10508-012-0042-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109. Schulte-Herbruggen O, Ahlers CJ, Kronsbein JM, et al. Impaired sexual function in patients with borderline personality disorder is determined by history of sexual abuse. J Sex Med. 2009;6(12):3356–3363. 10.1111/j.1743-6109.2009.01422.x. [DOI] [PubMed] [Google Scholar]
- 110. Hull JW, Clarkin JF, Yeomans F. Borderline personality disorder and impulsive sexual behavior. Hospital Community Psychiatry. 1993;44(10):1000–1002. 10.1176/ps.44.10.1000. [DOI] [PubMed] [Google Scholar]
- 111. Jardin C, Sharp C, Garey L, et al. Compelled to risk: does sexual compulsivity explain the connection between borderline personality disorder features and number of sexual partners? J Personal Disord. 2017;31(6):738–752. 10.1521/pedi_2017_31_277. [DOI] [PubMed] [Google Scholar]
- 112. Elmquist J, Shorey RC, Anderson S, Stuart GL. Are borderline personality symptoms associated with compulsive sexual behaviors among women in treatment for substance use disorders? An exploratory study. J Clin Psychol. 2016;72(10):1077–1087. 10.1002/jclp.22310. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113. Rawson RA, Washton A, Domier CP, Reiber C. Drugs and sexual effects: role of drug type and gender. J Subst Abuse Treatment. 2002;22(2):103–108. 10.1016/S0740-5472(01)00215-X. [DOI] [PubMed] [Google Scholar]
- 114. Abernathy K, Chandler LJ, Woodward JJ. Alcohol and the prefrontal cortex. Int Rev Neurobiol. 2010;91:289–320. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115. Heatherton TF, Wagner DD. Cognitive neuroscience of self-regulation failure. Trends Cogn Sci. 2011;15(3):132–139. 10.1016/j.tics.2010.12.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116. O’Sullivan SS, Evans AH, Lees AJ. Dopamine dysregulation syndrome: an overview of its epidemiology, machanisms and management. CNS Drugs. 2009;23(2):157–170. 10.2165/00023210-200923020-00005. [DOI] [PubMed] [Google Scholar]
- 117. Moore TJ, Glenmullen J, Mattison DR. Reports of pathological gambling, hypersexuality, and compulsive shopping associated with dopamine receptor agonist drugs. JAMA Int Med. 2014;174(12):1930–1933. 10.1001/jamainternmed.2014.5262. [DOI] [PubMed] [Google Scholar]
- 118. Corvol J-C, Artaud F, Cormier-Dequaire F, et al. Longitudinal analysis of impulse control disorders in Parkinson disease. Neurology. 2018;91(3):e189–e201. 10.1212/WNL.0000000000005816. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119. Zlot Y, Goldstein M, Cohen K, Weinstein A. Online dating is associated with sex addiction and social anxiety. J Behav Addict. 2018;7(3):821–826. 10.1556/2006.7.2018.66. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 120. Weiss D. The prevalence of depression in male sex addicts residing in the United States. Sex Addict Compuls. 2004;11(1-2):57–69. 10.1080/10720160490458247. [DOI] [Google Scholar]
- 121. Kalra G. The depressive façade in a case of compulsive sex behavior with frottage. Indian J Psychiatr. 2013;55(2):183–185. 10.4103/0019-5545.111460. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 122. Di Nicola M, Tedeschi D, Mazza M, et al. Behavioural addictions in bipolar disorder patients: role of impulsivity and personality dimensions. J Affect Disord. 2010;125(1-3):82–88. 10.1016/j.jad.2009.12.016. [DOI] [PubMed] [Google Scholar]
- 123. Fuss J, Briken P, Stein DJ, Lochner C. Compulsive sexual behavior disorder in obsessive-compulsive disorder: prevalence and associated comorbidity. J Behav Addict. 2019;8(2):242–248. 10.1556/2006.8.2019.23. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 124. Lafortune D, Blais M, Miller G, Dion L, Lalonde F, Dargis L. Psychological and interpersonal factors associated with sexualized drug use among men who have sex with men: a mixed-methods systematic review. Arch Sex Behav. 2021;50(2):427–460. 10.1007/s10508-020-01741-8. [DOI] [PubMed] [Google Scholar]
- 125. Pfaus JG, Wilkins MF, DiPietro N, et al. Inhibitory and disinhibitory effects of psychomotor stimulants and depressants on the sexual behavior of male and female rats. Horm Behav. 2010;58(1):163–176. 10.1016/j.yhbeh.2009.10.004. [DOI] [PubMed] [Google Scholar]
- 126. Kafka MP, Hennen J. A DSM-IV Axis I comorbidity study of males (n=120) with paraphilias and paraphilia related disorders. Sex Abus. 2002;14(4):349–366. 10.1177/107906320201400405. [DOI] [PubMed] [Google Scholar]
- 127. Kafka MP, Hennen J. Hypersexual desire in males: are males with paraphilias different from males with paraphilia-related disorders? Sex Abus. 2003;15(4):307–321. 10.1177/107906320301500407. [DOI] [PubMed] [Google Scholar]
- 128. Briken P, Habermann N, Kafka MP, Berner W, Hill A. The paraphilia-related disorders: an investigation of the relevance of the concept in sexual murderers. J Forensic Sci. 2006;51(3):683–688. 10.1111/j.1556-4029.2006.00105.x. [DOI] [PubMed] [Google Scholar]
- 129. Klein V, Schmidt AF, Turner D, Briken P. Are sex drive and hypersexuality associated with pedophilic interest and child sexual abuse in a male community sample? PLoS One. 2015;10(7):e0129730. 10.1371/journal.pone.0129730. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130. Hertz PG, Rettenberger M, Turner D, Briken P, Eher R. Hypersexual disorder and recidivism risk in individuals convicted of sexual offenses. J Forens Psychiatry Psychol. 33:572–591. [Google Scholar]
- 131. Kingston DA, Bradford JM. Hypersexuality and recidivism among sexual offenders. Sex Addict Compulsivity. 2013;20(1-2):91–105. [Google Scholar]
- 132. Langevin S, Proulx J, Lacourse E. Sexual aggressors against women’s sexual lives: a latent class analysis. Int J Offender Ther Comp Criminol. 2018;62(6):1430–1451. 10.1177/0306624X17694374. [DOI] [PubMed] [Google Scholar]
- 133. Marshall LE, Marshall WL, Moulden HM, Serran GA. The prevalence of sexual addiction in incarcerated sexual offenders and matched community nonoffenders. Sex Addict Compulsivity. 2008;15(4):271–283. 10.1080/10720160802516328. [DOI] [Google Scholar]
- 134. Simmons CA, Lehmann P, Collier-Tenison S. Linking male use of the sex industry to controlling behaviors in violent relationships: an exploratory analysis. Violence Against Women. 2008;14(4):406–417. 10.1177/1077801208315066. [DOI] [PubMed] [Google Scholar]
- 135. Gardner AR, Grigorian H, Florimbio AR, Brem MJ, Wolford-Clevenger C, Stuart GL. The association between compulsive sexual behavior and sexual aggression perpetration among men arrested for domestic violence. Sex Addict Compulsivity. 2018;25(2-3):226–240. 10.1080/10720162.2018.1532361. [DOI] [Google Scholar]
- 136. Carvalho J, Nobre PJ. Psychosexual characteristics of women reporting sexual aggression against men. J Interpers Violence. 2016;31(15):2539–2555. 10.1177/0886260515579504. [DOI] [PubMed] [Google Scholar]
- 137. Abdalla-Filho E, de Jesus MJ, Diehl A, et al. Forensic implications of the new classification of ICD-11 paraphilic disorders in Brazil. J Sex Med. 2019;16(11):1814–1819. 10.1016/j.jsxm.2019.07.025. [DOI] [PubMed] [Google Scholar]
- 138. Martínez-López JNI, Robles R, Fresán A, et al. Legal and policy implications in Mexico of changes in ICD-11 paraphilic disorders. J Sex Med. 2019;16(10):1623–1637. 10.1016/j.jsxm.2019.07.022. [DOI] [PubMed] [Google Scholar]
- 139. Briken P, Boetticher A, Krueger RB, Kismödi E, Reed GM. Current legal situation for patients with paraphilic disorders and implications of the ICD-11 for paraphilic disorders for Germany. J Sex Med. 2019;16(10):1615–1622. 10.1016/j.jsxm.2019.07.011. [DOI] [PubMed] [Google Scholar]
- 140. Coleman E, Jennings T, Gleason N, et al. The relationship between boredom proneness, attachment styles and compulsive sexual behavior. J Sex Marital Ther. 2023;49(2):172–188. 10.1080/0092623X.2022.2086511. [DOI] [PubMed] [Google Scholar]
- 141. Althof SE, Rosen RC, Perelman MA, Rubio-Aurioles E. Standard operating procedures for taking a sexual history. J Sex Med. 2013;10(1):26–35. 10.1111/j.1743-6109.2012.02823.x. [DOI] [PubMed] [Google Scholar]
- 142. Ahorsu D, Adjorlolo S, Nurmala I, Ruckwongpatr K, Strong C, Lin C-Y. Problematic porn use and cross-cultural differences: a brief review. Current Addiction Reports. 2023;10(3):572–580. 10.1007/s40429-023-00505-3. [DOI] [Google Scholar]
- 143. Jennings TL, Gleason N, Kraus SW. Assessment of compulsive sexual behavior disorder among lesbian, gay, bisexual, transgender, and queer clients: commentary to the debate: “Behavioral addictions in the ICD-11.”. J Behav Addict. 2022;11(2):216–221. 10.1556/2006.2022.00028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 144. Briken P, Turner D. What does “sexual” mean in compulsive sexual behavior disorder? J Behav Addict. 2022;11(2):222–225. 10.1556/2006.2022.00026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 145. Janssen E, Bancroft J. The dual control model of sexual response: a scoping review, 2009-2022. J Sex Res. 2023;60(7):948–968. 10.1080/00224499.2023.2219247. [DOI] [PubMed] [Google Scholar]
- 146. Perelman MA. Sex coaching for non-sexologist physicians: how to use the sexual tipping point model. J Sex Med. 2018;15(12):1667–1672. 10.1016/j.jsxm.2018.10.010. [DOI] [PubMed] [Google Scholar]
- 147. Coleman E, Dickenson JA, Girard A, et al. An integrative biopsychosocial and sex positive model of understanding and treatment of impulsive/compulsive sexual behavior. Sex Addict Compuls. 2018;25(2-3):125–152. 10.1080/10720162.2018.1515050. [DOI] [Google Scholar]
- 148. Munns R, Dickenson J, Candelario-Perez L, et al. Psychotherapies in the treatment of compulsive sexual behavior disorder. In: Balon R, Briken P eds. Compulsive Sexual Behavior Disorder: Understanding, Assessment, and Treatment. American Psychiatric Association; 2021: 109–128. [Google Scholar]
- 149. Braun-Harvey D, Vigorito D. Treating out of Control Sexual Behavior : Rethinking Sexual Addiction: Springer; 2016. [Google Scholar]
- 150. Lew-Starowicz M, Coleman E. Mental and sexual health perspectives of the International Classification of Diseases (ICD-11) compulsive sexual behavior disorder. J Behav Addict. 2022;11(2):226–229. 10.1556/2006.2022.00032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 151. Antons S, Engel J, Briken P, Krüger THC, Brand M, Stark R. Treatments and interventions for compulsive sexual behavior disorder with a focus on problematic pornography use: a preregistered systematic review. J Behav Addict. 2022;11(3):643–666. 10.1556/2006.2022.00061. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 152. Briken P, Turner D. Pharmacotherapy for patients with CSBD. In: Balon R, Briken P eds. Compulsive Sexual Behavior Disorder: Understanding, Assessment, and Treatment. American Psychiatric Association; 2021: 109–128. [Google Scholar]
- 153. Thibaut F, Cosyns P, Fedoroff JP, et al. The World Federation of Societies of Biological Psychiatry (WFSBP) 2020 guidelines for the pharmacological treatment of paraphilic disorders. World J Biol Psychiatry. 2020;21(6):412–490. 10.1080/15622975.2020.1744723. [DOI] [PubMed] [Google Scholar]
- 154. Lew-Starowicz M, Draps M, Kowalewska E, Obarska K, Kraus SW, Gola M. Tolerability and efficacy of paroxetine and naltrexone for treatment of compulsive sexual behaviour disorder. World Psychiatry. 2022;21(3):468–469. 10.1002/wps.21026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 155. Savard J, Oberg KG, Chatzittofis A, Dhejne C, Arver S, Jokinen J. Naltrexone in compulsive sexual behavior disorder: a feasibility study of twenty men. J Sex Med. 2020, 2020;17(8):1544–1552. [DOI] [PubMed] [Google Scholar]