Abstract
Background: The COVID-19 pandemic has highlighted a correlation between cardiac complications and elevated cardiac biomarkers, which are linked to poorer clinical outcomes. Objective: This study aims to determine the clinical impact of cardiac biomarkers in COVID-19 patients in Latin America. Subjects and methods: The CARDIO COVID 19-20 Registry is a multicenter observational study across 44 hospitals in Latin America and the Caribbean. It included hospitalized COVID-19 patients (n = 476) who underwent troponin, natriuretic peptide, and D-dimer tests. Patients were grouped based on the number of positive biomarkers. Results: Among the 476 patients tested, 139 had one positive biomarker (Group C), 190 had two (Group B), 118 had three (Group A), and 29 had none (Group D). A directly proportional relationship was observed between the number of positive biomarkers and the incidence of decompensated heart failure. Similarly, there was a proportional relationship between the number of positive biomarkers and increased mortality. In Group B, patients with elevated troponin and natriuretic peptide and those with elevated troponin and D-dimer had 1.4 and 1.5 times higher mortality, respectively, than those with elevated natriuretic peptide and D-dimer. Conclusions: In Latin American COVID-19 patients, a higher number of positive cardiac biomarkers is associated with increased cardiovascular complications and mortality. These findings suggest that cardiac biomarkers should be utilized to guide acute-phase treatment strategies.
Keywords: COVID-19, SARS-CoV-2, biomarkers, cardiovascular disease, mortality, prognosis
1. Introduction
The SARS-CoV-2 virus is a β-coronavirus belonging to the Coronaviridae family, formed by a single positive-sense RNA strand. It causes the severe acute respiratory syndrome known as COVID-19, a global epidemic disease responsible for more than 7.04 million as of May 2024, according to WHO estimates [1,2,3,4,5]. While COVID-19 primarily affects the respiratory system, current evidence suggests significant impacts on the cardiovascular system as well, leading to various cardiac manifestations, including chest pain, palpitations, myocardial injury, and exacerbation of underlying cardiovascular diseases [6,7]. Myocardial injury has been reported in up to 27.8% of hospitalized COVID-19 patients in China [8].
Patients with COVID-19 and underlying cardiovascular diseases generally present with more severe symptoms and a higher mortality rate compared to those with other comorbidities, such as diabetes or chronic respiratory diseases [9,10,11,12,13,14,15]. Cardiac biomarkers are proposed to play a critical role in the diagnosis, prognosis, and management of COVID-19 patients. Robust evidence links elevated biomarkers of myocardial damage and stress, such as cardiac troponin and natriuretic peptides, with increased morbidity and mortality in these patients [9,11,16,17].
Among cardiac biomarkers, troponin is the most strongly associated with adverse outcomes and mortality during COVID-19, with an almost universal increase observed in critically ill or deceased patients. The one-month mortality rate in patients with elevated troponin levels exceeds 50% [8,18,19]. Natriuretic peptides have also been shown to predict COVID-19 severity, with higher values reported in patients who died, suggesting their use as a tool to discriminate severe cases [19,20,21]. Elevated D-dimer levels have been associated with adverse outcomes and increased mortality, although the data is limited and based on small, heterogeneous cohorts. D-dimer values ≥ 1 mg/mL are proposed to have moderate sensitivity and specificity for predicting severe outcomes and fatal events [22].
Cardiovascular diseases are the leading cause of death worldwide, and their prevalence is increasing [23]. This underscores the importance of close monitoring and diagnosis, particularly in the context of COVID-19, which continues to trigger cardiovascular complications and remains a frequent cause of consultation [24].
Given this context, we aim to describe the relationship between cardiac injury biomarkers and the presence of cardiovascular complications and in-hospital mortality in patients hospitalized due to COVID-19 in Latin America.
2. Subjects and Methods
2.1. Supervision and Data Collection
This study was observational, analytical, retrospective, and multicenter, focusing on patients hospitalized due to confirmed SARS-CoV-2 infection. The included subjects were part of the CARDIO COVID 19-20 registry (Latin American Registry of Cardiovascular Diseases and COVID-19), established by the Inter-American Heart Failure Council (CIFACAH) of the Inter-American Society of Cardiology (SIAC).
The study population consisted of adult patients aged 18 years or older who met the following inclusion criteria: serologically confirmed diagnosis of SARS-CoV-2 infection according to the WHO definition, hospitalization for more than 24 h for the treatment of COVID-19, and available results for troponin, natriuretic peptide, and d-dimer. Patients without complete clinical histories were excluded. Follow-up for recruited patients occurred 30 days after hospital discharge. Both patients with and without previous cardiovascular comorbidities reported in their clinical history were included.
The registry was designed, developed, and conducted by CIFACAH of the SIAC, and coordinated by the Clinical Research Center (CRC) of the Fundación Valle de Lili (FVL) in Cali, Colombia. The study complied with the Declaration of Helsinki and did not require informed consent as no additional interventions were performed. The protocol was approved by the CRC and the Human Ethics Committee of FVL (1835), as well as the Executive Committee of CIFACAH/SIAC. The data were obtained from medical records and collected using the REDCap (Research Electronic Data Capture) electronic database system. REDCap 14.3.13—© 2024 Vanderbilt University
2.2. Participants
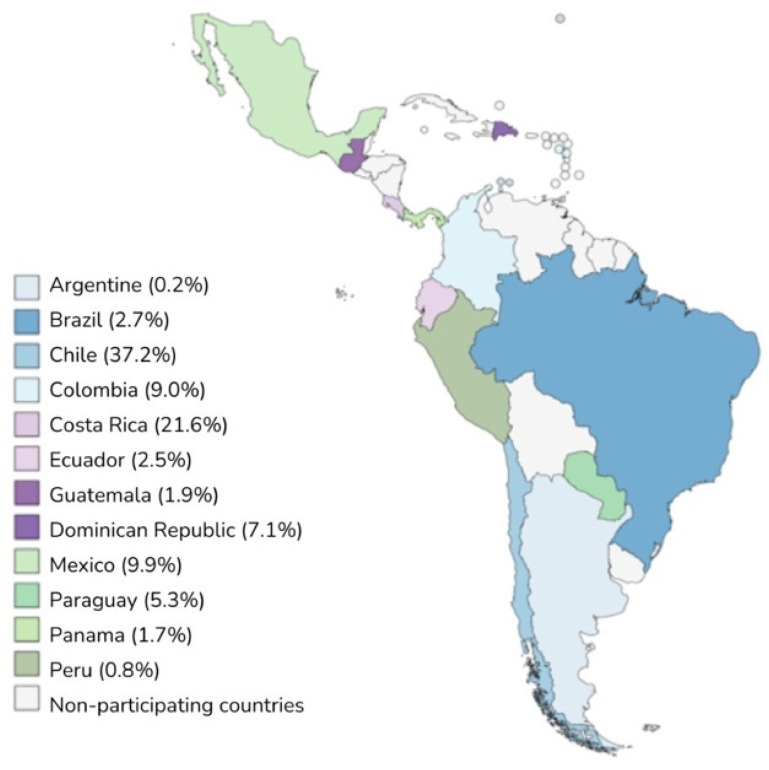
The CARDIO COVID 19-20 registry included 3260 patients admitted to hospitalization, emergency, or intensive care units (ICU) in 44 hospitals across 14 Latin American countries between 1 May 2020 and 30 June 2021 (Figure 1). Of these, 476 patients had all three biomarkers measured.
Figure 1.
Distribution of patients in the participating countries.
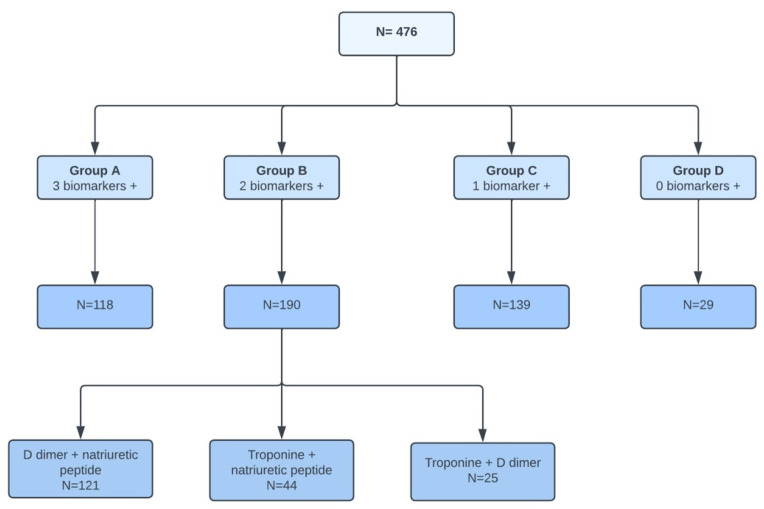
These patients were divided into four groups (Figure 2) based on the number of abnormal or positive biomarkers:
Group A: 3 positive biomarkers, with 118 patients
Group B: 2 positive biomarkers, with 190 patients
Group C: 1 positive biomarker, with 139 patients
Group D: No positive biomarkers, with 29 patients
Figure 2.
Flowchart of patient distribution.
2.3. Para-Clinical Tests
The laboratory tests were conducted according to the institutional protocols of each participating center. The measured parameters included inflammatory, metabolic, cardiac, and coagulation markers, among other paraclinical tests. Specifically, cardiac serum biomarkers measured included d-dimer, various types of natriuretic peptides (NP), and different types of troponins. Cardiac biomarkers were grouped by type and classified according to their results as normal/negative or abnormal/positive.
2.4. Statistical Analysis
A univariate descriptive analysis was conducted to characterize the behavior of the numerical variables. The normality of the quantitative variables was assessed using the Shapiro–Wilk test. Variables with a p-value > 0.05 were considered normally distributed and were presented as means and standard deviations. Variables that did not meet the normality assumption were presented as medians and interquartile ranges. Categorical variables were expressed as proportions, and comparisons between groups were performed using the Chi-square test or Fisher’s exact test, as appropriate. Quantitative variables with a normal distribution were compared using the Student’s t-test, while those with a non-normal distribution were compared using the Mann–Whitney test. For paired samples, the Wilcoxon test was employed.
A subclassification of the data obtained in group B (2 positive biomarkers) was performed, depending on the biomarkers that were elevated or abnormal. This subclassification was made with three groups: Troponin + NP, troponin + d-dimer, and NP + d-dimer, with which the comparisons were made according to the condition at discharge.
Subsequently, the association between each of these groups and the outcome of mortality was evaluated. For this comparison, the subgroup with elevated d-dimer plus NP was taken as the reference, considering the group with the lowest mortality and highest prevalence.
All statistical analyses were performed using R V.4.1.1 (R Foundation for Statistical Computing, Vienna, Austria) through R Studio V.1.4.1717.
3. Results
3.1. Clinical Characteristics at Admission
Of 3260 patients admitted, only 476 were included in various subgroups as given in Table 1. The median age was 64 years, range 52–73 years with a predominance of male gender (68.3% vs. 31.7%). Group A had a median age of 69 years (IQR: 58–77), with a progressive decrease observed across the groups, reaching a median age of 49 years (IQR: 40–69) in group D. The most frequent comorbidities across the four groups were obesity/overweight, which predominated in groups B and C (63.7% and 58.3%, respectively) and were less common in groups A and D (50.8% and 51.7%, respectively) (p = 0.14). Hypertension prevalence decreased significantly as the number of positive biomarkers decreased (group A: 66.9%, group B: 60%, group C: 49.6%, and group D: 37.9%; p = 0.005). Similarly, dyslipidemia followed the same trend as hypertension, with a statistically significant decrease in prevalence corresponding to a lower number of positive biomarkers (group A: 23.7%, group B: 20.5%, group C: 7.2%, and group D: 6.9%; p < 0.001) (Table 1).
Table 1.
Demographics and comorbidities.
| Variables | N | Number of Positive Biomarkers | p-Value 2 | ||||
|---|---|---|---|---|---|---|---|
| Overall, | Group A, | Group B, | Group C, | Group D, | |||
| N = 476 1 | N = 118 1 | N = 190 1 | N = 139 1 | N = 29 1 | |||
| Sociodemographic characteristics | |||||||
| Age | 476 | 64.0 | 69.0 | 65.5 | 58.0 | 49.0 | <0.001 |
| (52.0–73.0) | (58.0–77.0) | (55.2–74.0) | (46.5–68.0) | (40.0–69.0) | |||
| Gender | 476 | 0.3 | |||||
| Female | 151 (31.7%) | 44 (37.3%) | 60 (31.6%) | 41 (29.5%) | 6 (20.7%) | ||
| Male | 325 (68.3%) | 74 (62.7%) | 130 (68.4%) | 98 (70.5%) | 23 (79.3%) | ||
| Comorbidities | |||||||
| Hypertension | 476 | 273 (57.4%) | 79 (66.9%) | 114 (60.0%) | 69 (49.6%) | 11 (37.9%) | 0.005 |
| Diabetes mellitus | 476 | 162 (34.0%) | 43 (36.4%) | 71 (37.4%) | 41 (29.5%) | 7 (24.1%) | 0.3 |
| Dyslipidemia | 476 | 79 (16.6%) | 28 (23.7%) | 39 (20.5%) | 10 (7.2%) | 2 (6.9%) | <0.001 |
| Overweight/obesity | 476 | 277 (58.2%) | 60 (50.8%) | 121 (63.7%) | 81 (58.3%) | 15 (51.7%) | 0.14 |
| Coronary heart disease | 476 | 0.5 | |||||
| Clinical | 29 (6.1%) | 13 (11.0%) | 9 (4.7%) | 6 (4.3%) | 1 (3.4%) | ||
| Stent | 18 (3.8%) | 7 (5.9%) | 7 (3.7%) | 3 (2.2%) | 1 (3.4%) | ||
| Myocardial revascularization | 5 (1.1%) | 1 (0.8%) | 2 (1.1%) | 2 (1.4%) | 0 (0.0%) | ||
| Both | 1 (0.2%) | 0 (0.0%) | 1 (0.5%) | 0 (0.0%) | 0 (0.0%) | ||
| Heart failure | 476 | 41 (8.6%) | 21 (17.8%) | 14 (7.4%) | 4 (2.9%) | 2 (6.9%) | <0.001 |
| LVEF | 36 | 0.3 | |||||
| LVEF < 40% | 23 (63.9%) | 12 (66.7%) | 7 (53.8%) | 3 (100.0%) | 1 (50.0%) | ||
| LVEF 40–50% | 5 (13.9%) | 4 (22.2%) | 1 (7.7%) | 0 (0.0%) | 0 (0.0%) | ||
| LVEF > 50% | 8 (22.2%) | 2 (11.1%) | 5 (38.5%) | 0 (0.0%) | 1 (50.0%) | ||
| Atrial fibrillation | 476 | 25 (5.3%) | 9 (7.6%) | 10 (5.3%) | 5 (3.6%) | 1 (3.4%) | 0.5 |
| Stroke | 476 | 10 (2.1%) | 3 (2.5%) | 6 (3.2%) | 1 (0.7%) | 0 (0.0%) | 0.4 |
1 Median (IQR); n (%). 2 Kruskal-Wallis rank sum test; Pearson’s Chi-squared test. IQR: Interquartile range; LVEF: Left ventricular ejection fraction.
The most frequent clinical manifestation at admission was dyspnea, with a similar prevalence across all groups (79.7%, 83.2%, 75.5%, and 69%, respectively; p = 0.2). No significant differences were observed in vital signs, except for arterial oxygen saturation. The median arterial oxygen saturation values were: group A: 90.5% (IQR: 83–96%), group B: 90% (IQR: 84–94%), group C: 90% (IQR: 86–94%), and group D: 94% (IQR: 92–96%). This indicates that group D had significantly higher saturation compared to the other groups (p = 0.013).
3.2. Paraclinical Tests at Admission
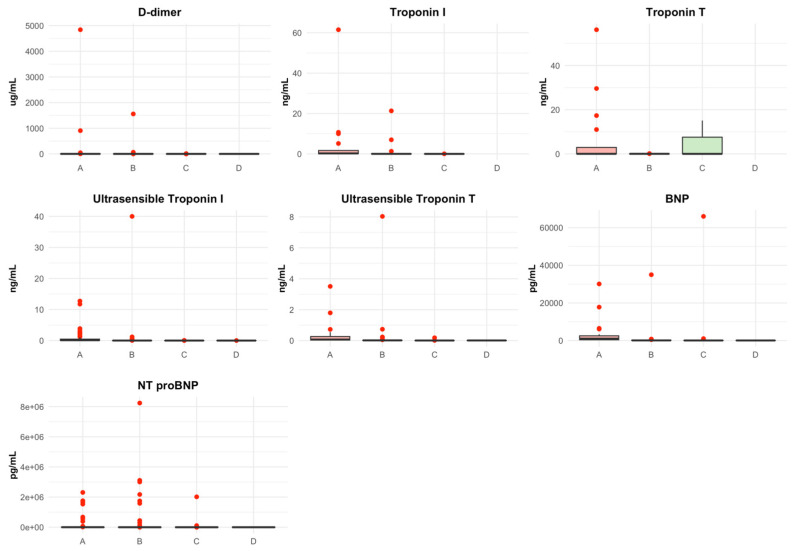
The cardiac biomarkers exhibited a similar trend across the groups, with higher levels observed in patients with more positive or abnormal markers. D-dimer levels were highest in group A (median: 1.54) and decreased progressively in groups C and D (median: 0.30 and 0.28, respectively). Similarly, BNP and NT-proBNP levels decreased as the groups progressed. Troponin I, Troponin T, high-sensitivity Troponin I, and high-sensitivity Troponin T also followed this trend, showing lower values in groups with fewer or no abnormal biomarkers. The distribution of biomarker values is represented in Figure 3.
Figure 3.
Box plot of Biomarkers value distribution. Abnormal or positive biomarker value: D-dimer, >0.5 ug/mL, Troponin I high sensitivity (men), >0.0342 ng/mL, Troponin I high sensitivity (women), >0.0156 ng/mL, Troponin T high sensitivity, >0.014 ng/mL, Troponin T, >0.1 ng/mL, Troponin I (men), >0.033 ng/mL, Troponin I (women), >0.013 ng/mL, BNP, >266 pg/mL, NT-proBNP, >125 pg/mL. BNP: B-type natriuretic peptide; NT-proBNP: N-terminal pro-brain natriuretic peptide; Pg: Picogram; Ng: Nanogram; Ug: Microgram; mL: milliliters.
3.3. Imaging Studies during Hospital Stay
On chest X-ray, pulmonary congestion was observed in 36.6% of patients in group A, decreasing significantly as the number of positive biomarkers decreased, reaching 0.0% in group D (p < 0.001). Echocardiographic abnormalities, including decreased systolic function, right ventricular dysfunction, pericardial effusion, and valvular dysfunction, were predominantly found in group A, with their incidence progressively decreasing across the groups, reaching the lowest levels in group D (Table 2).
Table 2.
Imaging Studies.
| Variables | N | Number of Positive Biomarkers | p-Value 2 | ||||
|---|---|---|---|---|---|---|---|
| Overall, | Group A, | Group B, | Group C, | Group D, | |||
| N = 476 1 | N = 118 1 | N = 190 1 | N = 139 1 | N = 29 1 | |||
| Chest X-ray | 476 | 455 (95.6%) | 112 (94.9%) | 180 (94.7%) | 135 (97.1%) | 28 (96.6%) | 0.7 |
| Pulmonary infiltrates | 455 | 0.032 | |||||
| Unilateral | 35 (7.7%) | 4 (3.6%) | 17 (9.4%) | 10 (7.4%) | 4 (14.3%) | ||
| Bilateral | 371 (81.5%) | 99 (88.4%) | 142 (78.9%) | 113 (83.7%) | 17 (60.7%) | ||
| cardiomegaly | 455 | 84 (18.5%) | 36 (32.1%) | 32 (17.8%) | 15 (11.1%) | 1 (3.6%) | <0.001 |
| Lung congestion | 455 | <0.001 | |||||
| Unilateral | 11 (2.4%) | 3 (2.7%) | 5 (2.8%) | 3 (2.2%) | 0 (0.0%) | ||
| Bilateral | 93 (20.4%) | 41 (36.6%) | 34 (18.9%) | 18 (13.3%) | 0 (0.0%) | ||
| Pleural effusion | 455 | <0.001 | |||||
| Unilateral | 25 (5.5%) | 8 (7.1%) | 14 (7.8%) | 2 (1.5%) | 1 (3.6%) | ||
| Bilateral | 27 (5.9%) | 16 (14.3%) | 8 (4.4%) | 2 (1.5%) | 1 (3.6%) | ||
| Transthoracic echocardiogram | 476 | 120 (25.2%) | 44 (37.3%) | 46 (24.2%) | 26 (18.7%) | 4 (13.8%) | 0.002 |
| Systolic function | 119 | 0.3 | |||||
| Normal | 78 (65.5%) | 22 (50.0%) | 32 (71.1%) | 21 (80.8%) | 3 (75.0%) | ||
| Focal decrease | 14 (11.8%) | 8 (18.2%) | 4 (8.9%) | 1 (3.8%) | 1 (25.0%) | ||
| Global decrease | 25 (21.0%) | 13 (29.5%) | 8 (17.8%) | 4 (15.4%) | 0 (0.0%) | ||
| Right ventricular dysfunction | 118 | 17 (14.4%) | 14 (32.6%) | 2 (4.4%) | 1 (3.8%) | 0 (0.0%) | <0.001 |
1 n (%); Median (IQR). 2 Pearson’s Chi-squared test; Kruskal-Wallis rank sum test.
3.4. Cardiovascular Complications during Hospitalization
The most frequent cardiovascular complications were acute decompensated heart failure (ADHF) (p < 0.001) and cardiac arrhythmias (CA) (p = 0.004). ADHF occurred in 17.6% of patients, primarily in group A (35.6%), followed by group B (8.4%) and group C (5%) (p < 0.001). Among the ADHF clinical profiles, congestion was the most prevalent (10.9%), followed by cardiogenic shock (4.2%) and pulmonary edema (2.1%). Conversely, CA occurred in 13% of patients, with supraventricular arrhythmias being the most prevalent type at 7.8%, mainly present in group A (22.9%), with fewer events occurring in groups C and D (Table 3).
Table 3.
CV complications.
| Variables | N | Number of Positive Biomarkers | p-Value 2 | ||||
|---|---|---|---|---|---|---|---|
| Overall, | Group A, | Group B, | Group C, | Group D, | |||
| N = 476 1 | N = 118 1 | N = 190 1 | N = 139 1 | N = 29 1 | |||
| Acute heart failure | 476 | 84 (17.6%) | 42 (35.6%) | 35 (18.4%) | 7 (5.0%) | 0 (0.0%) | <0.001 |
| Cardiac arrythmia | 476 | 62 (13.0%) | 27 (22.9%) | 26 (13.7%) | 7 (5.0%) | 2 (6.9%) | <0.001 |
| Miocarditis | 476 | 13 (2.7%) | 6 (5.1%) | 5 (2.6%) | 2 (1.4%) | 0 (0.0%) | 0.2 |
| Pulmonary tromboembolism | 476 | 22 (4.6%) | 5 (4.2%) | 8 (4.2%) | 9 (6.5%) | 0 (0.0%) | 0.5 |
| Other | 476 | 75 (15.8%) | 30 (25.4%) | 27 (14.2%) | 17 (12.2%) | 1 (3.4%) | 0.004 |
1 n (%); Median (IQR). 2 Pearson’s Chi-squared test; Kruskal-Wallis rank sum test.
3.5. Treatment for COVID-19
The hospital treatment for COVID-19 provided to patients was similar across the four groups, with notable use of oral and parenteral corticosteroids, chloroquine, lopinavir, and ritonavir. However, anticoagulation therapy was significantly more prevalent in group A and decreased progressively across the groups (group A: 61.9%, group B: 47.9%, group C: 52.5%, group D: 27.6%; p = 0.005). Additionally, the use of azithromycin and hydroxychloroquine was highest in group C, with a statistically significant difference compared to the other groups (p < 0.001).
3.6. Respiratory and Cardiovascular Support
Invasive mechanical ventilation (IMV) was the primary intervention performed, applied to 50.4% of patients. The prevalence of IMV was similar among groups A, B, and C (53.4%, 52.1%, and 51.1%, respectively), but significantly lower in group D (24.1%; p = 0.034). Inotropes were used in 17.4% of patients, with a predominance in group A (28.8%) and a progressive decrease to group D in a statistically significant manner (0.0%, p < 0.001). On the other hand, vasodilators were used in 6.3% of participants, predominating in group A (11.9%) and decreasing progressively in a significant manner until reaching group D (0.0%, p = 0.024) (Table 4).
Table 4.
Treatment administered.
| Variables | N | Number of Positive Biomarkers | p-Value 2 | ||||
|---|---|---|---|---|---|---|---|
| Overall, | Group A, | Group B, | Group C, | Group D, | |||
| N = 476 1 | N = 118 1 | N = 190 1 | N = 139 1 | N = 29 1 | |||
| Vasopressors | 476 | 208 (43.7%) | 59 (50.0%) | 83 (43.7%) | 60 (43.2%) | 6 (20.7%) | 0.043 |
| Inotropes | 476 | 83 (17.4%) | 34 (28.8%) | 32 (16.8%) | 17 (12.2%) | 0 (0.0%) | <0.001 |
| Vasodilators | 476 | 30 (6.3%) | 14 (11.9%) | 10 (5.3%) | 6 (4.3%) | 0 (0.0%) | 0.024 |
| IMV | 476 | 240 (50.4%) | 63 (53.4%) | 99 (52.1%) | 71 (51.1%) | 7 (24.1%) | 0.034 |
| NIVM | 476 | 87 (18.3%) | 15 (12.7%) | 43 (22.6%) | 25 (18.0%) | 4 (13.8%) | 0.2 |
1 n (%). 2 Pearson’s Chi-squared test. IMV: Invasive mechanical ventilation; NIVM: Noninvasive mechanical ventilation.
3.7. Outcomes during Hospitalization
Admission to the ICU was numerically more prevalent in groups A and C (73.7% and 74.1%, respectively) compared to groups B and D (67.9% and 55.2%, respectively), but without statistical significance (p = 0.15). Mortality was an event exclusive and statistically significant to the groups with positive biomarkers, unlike group D, and was considerably higher in group A (group A = 50%, group B = 31.1%, group C = 18%, and group D = 0%, p < 0.001). Additionally, it was observed that patients in group A had a higher prevalence of cardiovascular death (37.3%) compared to groups B and C (28.8%, 12%), (p = 0.066). (Table 5)
Table 5.
Outcomes during hospitalization.
| Variables | N | Number of Positive Biomarkers | p-Value 2 | ||||
|---|---|---|---|---|---|---|---|
| Overall, | Group A, | Group B, | Group C, | Group D, | |||
| N = 476 1 | N = 118 1 | N = 190 1 | N = 139 1 | N = 29 1 | |||
| ICU admission | 476 | 335 (70.4%) | 87 (73.7%) | 129 (67.9%) | 103 (74.1%) | 16 (55.2%) | 0.15 |
| Condition at discharge | 476 | <0.001 | |||||
| Alive | 333 (70.0%) | 59 (50.0%) | 131 (68.9%) | 114 (82.0%) | 29 (100.0%) | ||
| Dead | 143 (30.0%) | 59 (50.0%) | 59 (31.1%) | 25 (18.0%) | 0 (0.0%) | ||
| Type of death | 143 | 0.066 | |||||
| Cardiovascular | 42 (29.4%) | 22 (37.3%) | 17 (28.8%) | 3 (12.0%) | 0 (NA%) | ||
| Not cardiovascular | 101 (70.6%) | 37 (62.7%) | 42 (71.2%) | 22 (88.0%) | 0 (NA%) | ||
1 n (%). 2 Pearson’s Chi-squared test. ICU: Intensive care unit. NA: Not applicable.
3.8. Outcomes at 30-Day Follow-Up after Hospital Discharge
After 30 days of hospital discharge, no statistically significant differences were observed regarding rehospitalization (p = 0.6) or mortality (p = 0.2) among the different groups studied (Table 6).
Table 6.
Outcomes after follow-up of 30-day.
| Variables | N | Number of Positive Biomarkers | p-Value 2 | ||||
|---|---|---|---|---|---|---|---|
| Overall, | Group A, | Group B, | Group C, | Group D, | |||
| N = 333 1 | N = 59 1 | N = 131 1 | N = 114 1 | N = 29 1 | |||
| Status | 307 | 0.2 | |||||
| Alive | 305 (99.3%) | 50 (100.0%) | 125 (99.2%) | 102 (100.0%) | 28 (96.6%) | ||
| Dead | 2 (0.7%) | 0 (0.0%) | 1 (0.8%) | 0 (0.0%) | 1 (3.4%) | ||
| Rehospitalization | 293 | 19 (6.5%) | 5 (10.6%) | 7 (5.8%) | 6 (6.1%) | 1 (3.7%) | 0.6 |
| Death cause | 2 | ||||||
| Non cardiovascular | 2 (100.0%) | 0 (NA%) | 1 (100.0%) | 0 (NA%) | 1 (100.0%) | ||
1 n (%); Median (IQR). 2 Pearson’s Chi-squared test; Kruskal–Wallis rank sum test.
3.9. Comparison between Two Abnormal Biomarkers (Group B)
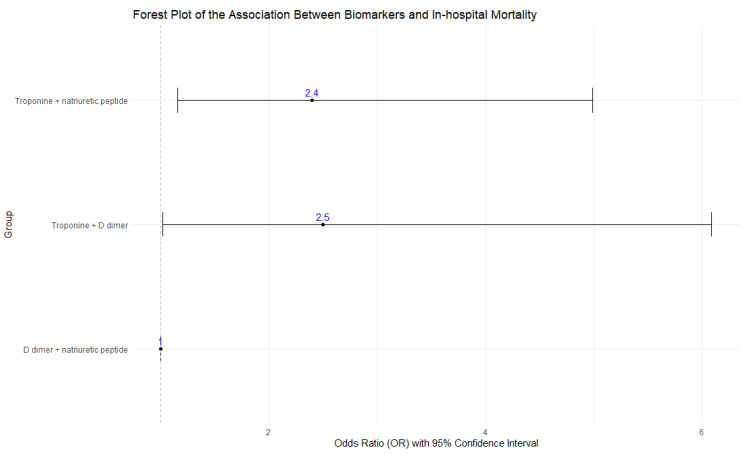
When grouping abnormal biomarkers in pairs, the subgroup with elevated D-dimer and NP (used as the reference) had the lowest mortality (24.0%) and the highest prevalence (n = 121). The subgroup with elevated troponin and D-dimer reported the highest mortality (44.0%), with a 1.5 times higher risk of death compared to the reference group (OR = 2.5; p = 0.045). However, this subgroup was also the least prevalent (n = 25). Finally, the group with elevated troponin and NP (n = 44) had a mortality rate of 43.2%, with a 1.4 times higher risk of death than the reference group (OR = 2.4; p = 0.018). Both associations were statistically significant (Table 7, Figure 4).
Table 7.
Relation of biomarkers with mortality.
| Overall, N = 190 | Troponine + Natriuretic Peptide. N = 44 | Troponine + D-Dimer. N = 25 | D-Dimer + Natriuretic Peptide. N = 121 | ||
|---|---|---|---|---|---|
| Condition at discharge | 190 | ||||
| Alive | 131 (68.9%) | 25 (56.9%) | 14 (56.0%) | 92 (76.0%) | |
| Dead | 59 (31.1%) | 19 (43.2%) | 11 (44.0%) | 29 (24.0%) | |
| N | OR | CI 95% | p-value | ||
| D dimer + natriuretic peptide | 121 | 1 | |||
| Troponine + natriuretic peptide | 44 | 2.4 | 1.16–4.99 | 0.018 | |
| Troponine + D dimer | 25 | 2.5 | 1.02–6.09 | 0.045 |
Figure 4.
Forest plot of Comparison between two abnormal biomarkers.
4. Discussion
4.1. General Information
4.1.1. General Characteristics
In general, male patients were more prone to hospitalization secondary to COVID-19, but without statistically significant differences. Conversely, a direct relationship was found between age and the number of positive biomarkers, likely due to a greater number of underlying conditions. Similarly, pathologies associated with metabolic syndrome, such as obesity, hypertension, diabetes, and dyslipidemia, were the most prevalent comorbidities in patients with positive biomarkers. This aligns with findings from other studies conducted in China and the United States, where diabetes, hypertension, and obesity were comorbidities associated with disease severity [25,26,27,28].
4.1.2. Clinical Manifestations
Patients with positive biomarkers presented more symptoms compared to patients with negative or normal biomarkers. However, the group with three positive biomarkers, which corresponds to the group with the highest morbidity and mortality, was not the most symptomatic. Considering that evidence suggests the severity of symptoms is associated with worse clinical outcomes [29], it is proposed that the most severely ill patients may have difficulty expressing their complaints, thus reporting fewer symptoms. It is important to highlight that there is evidence associating dyspnea with a two-fold higher probability of severe disease [30]. However, in our study, there was no significant difference in the frequency of dyspnea across different patient groups.
4.1.3. Paraclinical Tests on Admission
A study conducted at the University Hospital in Wuhan, China, which evaluated various biomarker levels in COVID-19 patients, including Troponin I and NT-proBNP, found that a higher number of positive biomarkers and higher median values were associated with increased severity and mortality [31]. Our study corroborated these findings, showing that group A had higher medians of biomarkers than groups B and C, with group B medians being higher than those of group C. Additionally, a higher median of biomarkers was linked to an increased number of complications and hospital mortality.
4.1.4. In-Hospital Complications
Our study found that patients with positive biomarkers had a higher prevalence of complications during their hospital stay, consistent with previous studies [31,32,33]. Zhu et al.’s meta-analysis reported that elevated biomarkers, including Troponins I and NT-proBNP, were associated with severe COVID-19 forms, similar to Cersosimo et al., who highlighted the role of troponins in predicting mortality [32,33]. The most common complication in our study was acute decompensated heart failure (ADHF), exclusively observed in patients with at least one abnormal biomarker (A = 35.6% vs. D = 0%). These findings are consistent with other studies reporting ADHF as a common complication, associated with more severe disease and worse outcomes [34,35,36,37].
4.1.5. ICU Interventions
Our study showed that the presence of at least one positive cardiovascular biomarker (Troponin, natriuretic peptide, and/or D-dimer) doubled the need for mechanical ventilation compared to patients with negative biomarkers (Table 5). The need for mechanical ventilation increased with the number of positive biomarkers. Furthermore, patients with at least one positive biomarker had a greater need for vasopressor drugs, with the requirement for such drugs increasing with the number of positive biomarkers (Table 5). This is consistent with literature indicating that elevated troponin levels suggest poor prognosis, correlating with a greater need for high-complexity care [38,39].
4.1.6. Anticoagulant Treatment
In this study, a higher need for anticoagulation therapy was observed with an increasing number of positive biomarkers (A = 61.9% vs. D = 27.6%), correlating with the most severe cases of SARS-CoV-2 infection. The literature extensively describes the hematological complications caused by this virus, including thrombotic events [40,41,42,43]. Consequently, a greater need for anticoagulation can be associated with the presence of positive biomarkers and more severe cases [44,45].
4.1.7. Hospital Outcomes
Literature suggests that cardiac biomarkers in COVID-19 patients can predict ICU needs [46,47,48]. However, our study did not find a significant difference in ICU requirements between patients with positive and negative biomarkers. In-hospital mortality was exclusively related to patients with at least one positive biomarker, with a 50% mortality rate in group A and a higher incidence of cardiovascular mortality. Similar findings were reported by Cersosimo et al., indicating that higher levels of Troponin-T and NT-proBNP predict mortality, with troponins having the greatest impact (50%) [33]. Huang et al. also described that D-dimer, NT-proBNP, and Troponin-I were mainly positive in the most severe cases [49]. Qin et al.’s pioneering study identified that elevated troponins or NT-proBNP were highly predictive of all-cause mortality at 28 days [50]. Our study found similar outcomes regarding 30-day mortality. Based on these findings, biomarkers can serve as prognostic tools.
4.1.8. Outcomes at 30-Day Follow-Up
The positivity of evaluated biomarkers is associated with disease severity and in-hospital mortality. However, after 30 days post-discharge, there was no statistically significant difference in mortality or readmission rates among the different groups (6.5%), though this was better than the 7.1% reported by Peiris et al. [51]. This result contrasts with Lionte et al., who found that NT-proBNP and Troponin I were predictors of 30-day mortality in an emergency hospital setting [52].
4.1.9. Comparison between Subgroups
Among patients in group B (two abnormal or positive biomarkers), those with elevated troponins had the highest mortality and significant odds ratios (ORs), with ORs of 2.5 for the troponin + D-dimer group and 2.4 for the troponin + natriuretic peptide group. Current evidence is insufficient to relate COVID-19 mortality with concomitant positive biomarkers. Future research with a larger participant pool could provide a more accurate OR.
4.2. Strengths and Limitations
The strengths of this study include its multicenter design, encompassing various care centers across the continent and yielding a significant sample size (476 patients). All participants underwent thorough cardiac biomarker measurements, with a 30-day follow-up, collecting data from over 90% of participants.
However, the study’s prospective cohort design has intrinsic limitations, including the lack of randomization and susceptibility to selection biases due to the wide range of COVID-19 severity and variability in test protocols across institutions and regions. Additionally, the absence of quantitative follow-up of these biomarkers limits definitive conclusions regarding their evolution over time and their clinical utility.
5. Conclusions
In patients with COVID-19 requiring hospitalization in Latin America, the presence of at least one altered cardiovascular biomarker (Troponin, natriuretic peptide, and/or D-dimer) is associated with an increased number of cardiovascular complications, ICU admission, ICU respiratory/cardiovascular support, and in-hospital mortality. Thus, measuring these cardiovascular biomarkers during hospitalization could aid in patient stratification and the implementation of individualized treatment and follow-up strategies.
Acknowledgments
We extend our gratitude to all individuals and institutions involved in the design and execution of the CARDIO COVID 19-20 study, whose contributions have been invaluable to its success.
Author Contributions
J.E.G.-M.: project administration, methodology, investigation, writing—review and editing. M.E.: investigation, writing original draft—review and editing. J.A.M.-O., V.A.-R. and J.D.P.-M.: investigation, writing original draft—review and editing. A.A.A.-T.: writing original draft—review and editing. H.L.-G.: methodology, data analysis, visualization, writing. A.V.-O.: methodology, data analysis. E.R.P., A.R., I.M., F.W., J.L.B., M.S., W.A., C.H., J.L.-P., L.P.C.-A., V.R. and D.S.: writing—review and editing. All authors have read and agreed to the published version of the manuscript.
Institutional Review Board Statement
The study protocol was approved by the Centro de Investigaciones Clínicas (CIC), the Comité de Ética Institucional (ethics committee) of the Fundación Valle del Lili (#1835) in Cali, Colombia, and by the Comité Científico y Académico of the Sociedad Interamericana de Cardiología (SIAC).
Informed Consent Statement
Patient consent was waived by the ethics committee that reviewed the protocol, as no interventions were intended for the participants. Additionally, the anonymization of participants’ personal information was guaranteed.
Data Availability Statement
The data presented in this study are available in article.
Conflicts of Interest
The authors declare no competing interests.
Funding Statement
This research received no external funding.
Footnotes
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content.
References
- 1.COVID-19 Map—Johns Hopkins Coronavirus Resource Center. [(accessed on 23 July 2023)]. Available online: https://coronavirus.jhu.edu/map.html.
- 2.Hu B., Guo H., Zhou P., Shi Z.-L. Characteristics of SARS-CoV-2 and COVID-19. Nat. Rev. Microbiol. 2021;19:141–154. doi: 10.1038/s41579-020-00459-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Mohamadian M., Chiti H., Shoghli A., Biglari S., Parsamanesh N., Esmaeilzadeh A. COVID-19: Virology, biology and novel laboratory diagnosis. J. Gene Med. 2021;23:e3303. doi: 10.1002/jgm.3303. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Wang H., Paulson K.R., Pease S.A., Watson S., Comfort H., Zheng P., Aravkin A.Y., Bisignano C., Barber R.M., Alam T., et al. Estimating excess mortality due to the COVID-19 pandemic: A systematic analysis of COVID-19-related mortality, 2020–2021. Lancet. 2022;399:1513–1536. doi: 10.1016/S0140-6736(21)02796-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Datadot COVID-19 Deaths | WHO COVID-19 Dashboard. [(accessed on 25 May 2024)]. Available online: https://data.who.int/dashboards/covid19/cases.
- 6.Liu F., Liu F., Wang L. COVID-19 and cardiovascular diseases. J. Mol. Cell Biol. 2021;13:161–167. doi: 10.1093/jmcb/mjaa064. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.González-Calle D., Eiros R., Sánchez P.L. Corazón y SARS-CoV-2. Med. Clin. 2022;159:440–446. doi: 10.1016/j.medcli.2022.07.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Guo T., Fan Y., Chen M., Wu X., Zhang L., He T., Wang H., Wan J., Wang X., Lu Z. Cardiovascular Implications of Fatal Outcomes of Patients with Coronavirus Disease 2019 (COVID-19) JAMA Cardiol. 2020;5:811–818. doi: 10.1001/jamacardio.2020.1017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Zhou F., Yu T., Du R., Fan G., Liu Y., Liu Z., Xiang J., Wang Y., Song B., Gu X., et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: A retrospective cohort study. Lancet. 2020;28:1054–1062. doi: 10.1016/S0140-6736(20)30566-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Wu Z., McGoogan J.M. Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72 314 Cases from the Chinese Center for Disease Control and Prevention. JAMA. 2020;323:1239–1242. doi: 10.1001/jama.2020.2648. [DOI] [PubMed] [Google Scholar]
- 11.Shi X., Chen M., Zhang Y. The cardiovascular disorders and prognostic cardiac biomarkers in COVID-19. Mol. Biol. Rep. 2021;48:1763–1771. doi: 10.1007/s11033-021-06148-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Grasselli G., Zangrillo A., Zanella A., Antonelli M., Cabrini L., Castelli A., Cereda D., Coluccello A., Foti G., Fumagalli R., et al. Baseline Characteristics and Outcomes of 1591 Patients Infected with SARS-CoV-2 Admitted to ICUs of the Lombardy Region, Italy. JAMA. 2020;323:1574–1581. doi: 10.1001/jama.2020.5394. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Speranza M., López-López J.D., Schwartzmann P., Morr I., Rodríguez-González M.J., Buitrago A., Pow-Chon-Long F., Passos L.C., Rossel V., Perna E.R., et al. Cardiovascular Complications in Patients with Heart Failure and COVID-19: CARDIO COVID 19-20 Registry. J. Cardiovasc. Dev. Dis. 2024;11:34. doi: 10.3390/jcdd11020034. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Márquez-Murillo M.F., Echeverri J.M.M., Torres W.B., Alarcón N.A.F., Escalante M., Figueiredo E.L., Gómez R.E.L., Sierra-Lara D., Herrera C., Lugo J., et al. Desenlaces cardiovasculares en fibrilación auricular y COVID-19 grave en Latinoamérica: Registro CARDIO COVID 19-20. REC CardioClin. 2024;59:23–34. doi: 10.1016/j.rccl.2023.09.003. [DOI] [Google Scholar]
- 15.Gomez-Mesa J.E., Galindo S., Escalante-Forero M., Rodas Y., Valencia A., Perna E., Romero A., Mendoza I., Wyss F., Barisani J.L., et al. Latin-American Registry of Cardiovascular Disease and COVID-19: Final Results. Glob. Heart. 2023;18:60. doi: 10.5334/gh.1272. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Metkus T.S., Sokoll L.J., Barth A.S., Czarny M.J., Hays A.G., Lowenstein C.J., Michos E.D., Nolley E.P., Post W.S., Resar J.R., et al. Myocardial Injury in Severe COVID-19 Compared with Non–COVID-19 Acute Respiratory Distress Syndrome. Circulation. 2021;143:553–565. doi: 10.1161/CIRCULATIONAHA.120.050543. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Rehman A., Yousuf S., Maken G.R., Naqvi S.R.A., Murtaza G., Ahmad A. Cardiac Troponin-I, A Biomarker for Predicting COVID-Induced Myocardial Damage Prognosis. J. Coll. Physicians Surg. Pak. JCPSP. 2023;33:498–503. doi: 10.29271/jcpsp.2023.05.498. [DOI] [PubMed] [Google Scholar]
- 18.Sandoval Y., Januzzi J.L., Jr., Jaffe A.S. Cardiac Troponin for Assessment of Myocardial Injury in COVID-19: JACC Review Topic of the Week. J. Am. Coll. Cardiol. 2020;76:1244–1258. doi: 10.1016/j.jacc.2020.06.068. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Chen T., Wu D.I., Chen H., Yan W., Yang D., Chen G., Ma K., Xu D., Yu H., Wang H., et al. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: Retrospective study. BMJ. 2020;368:m1091. doi: 10.1136/bmj.m1091. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Sorrentino S., Cacia M., Leo I., Polimeni A., Sabatino J., Spaccarotella C.A.M., Mongiardo A., De Rosa S., Indolfi C. B-Type Natriuretic Peptide as Biomarker of COVID-19 Disease Severity—A Meta-Analysis. J. Clin. Med. 2020;9:2957. doi: 10.3390/jcm9092957. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Yang C., Liu F., Liu W., Cao G., Liu J., Huang S., Zhu M., Tu C., Wang J., Xiong B. Myocardial injury and risk factors for mortality in patients with COVID-19 pneumonia. Int. J. Cardiol. 2021;326:230–236. doi: 10.1016/j.ijcard.2020.09.048. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Zhan H., Chen H., Liu C., Cheng L., Yan S., Li H., Li Y. Diagnostic Value of D-Dimer in COVID-19: A Meta-Analysis and Meta-Regression. Clin. Appl. Thromb. 2021;27:10760296211010976. doi: 10.1177/10760296211010976. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Díez J.M.B., García J.L.d.V., Pelegrina J.T., Martínez J.L.M., Peñacoba R.M., Tejón I.G., Quintana E.M.R., Sajkiewicz M.P., Boronat A.A., Pérez B., et al. Epidemiología de las enfermedades cardiovasculares y factores de riesgo en atención primaria. Rev. Esp. Cardiol. 2005;58:367–373. doi: 10.1157/13073893. [DOI] [PubMed] [Google Scholar]
- 24.Barzallo P. Fin de la Pandemia COVID-19. [(accessed on 24 July 2023)];Rev. Med. Ateneo. 2023 25:12–15. Available online: http://www.colegiomedicosazuay.ec/ojs/index.php/ateneo/article/view/286. [Google Scholar]
- 25.Yang J., Zheng Y., Gou X., Pu K., Chen Z., Guo Q., Ji R., Wang H., Wang Y., Zhou Y. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: A systematic review and meta-analysis. Int. J. Infect. Dis. 2020;94:91–95. doi: 10.1016/j.ijid.2020.03.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Richardson S., Hirsch J.S., Narasimhan M., Crawford J.M., McGinn T., Davidson K.W. Presenting Characteristics, Comorbidities, and Outcomes among 5700 Patients Hospitalized with COVID-19 in the New York City Area. JAMA. 2020;323:2052–2059. doi: 10.1001/jama.2020.6775. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Kompaniyets L., Pennington A.F., Goodman A.B., Rosenblum H.G., Belay B., Ko J.Y., Chevinsky J.R., Schieber L.Z., Summers A.D., Lavery A.M., et al. Underlying Medical Conditions and Severe Illness among 540,667 Adults Hospitalized with COVID-19, March 2020–March 2021. Prev. Chronic Dis. 2021;18:E66. doi: 10.5888/pcd18.210123. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Chatterjee S., Nalla L.V., Sharma M., Sharma N., Singh A.A., Malim F.M., Ghatage M., Mukarram M., Pawar A., Parihar N., et al. Association of COVID-19 with Comorbidities: An Update. ACS Pharmacol. Transl. Sci. 2023;6:334–354. doi: 10.1021/acsptsci.2c00181. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Fu L., Wang B., Yuan T., Chen X., Ao Y., Fitzpatrick T., Li P., Zhou Y., Lin Y.-F., Duan Q., et al. Clinical characteristics of coronavirus disease 2019 (COVID-19) in China: A systematic review and meta-analysis. J. Infect. 2020;80:656–665. doi: 10.1016/j.jinf.2020.03.041. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Talukder A., Razu S.R., Alif S.M., Rahman M.A., Islam S.M.S. Association between Symptoms and Severity of Disease in Hospitalised Novel Coronavirus (COVID-19) Patients: A Systematic Review and Meta-Analysis. J. Multidiscip. Healthc. 2022;15:1101–1110. doi: 10.2147/JMDH.S357867. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Han H., Xie L., Liu R., Yang J., Liu F., Wu K., Chen L., Hou W., Feng Y., Zhu C. Analysis of heart injury laboratory parameters in 273 COVID-19 patients in one hospital in Wuhan, China. J. Med. Virol. 2020;92:819–823. doi: 10.1002/jmv.25809. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Zhu Z., Wang M., Lin W., Cai Q., Zhang L., Chen D., Liu F., Xiong X., Chu J., Peng J., et al. Cardiac biomarkers, cardiac injury, and comorbidities associated with severe illness and mortality in coronavirus disease 2019 (COVID-19): A systematic review and meta-analysis. Immun. Inflamm. Dis. 2021;9:1071–1100. doi: 10.1002/iid3.471. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Cersosimo A., Cimino G., Amore L., Calvi E., Pascariello G., Inciardi R.M., Lombardi C.M., Vizzardi E., Metra M. Cardiac biomarkers and mortality in COVID-19 infection: A review. Monaldi Arch. Chest Dis. 2022;93:2276. doi: 10.4081/monaldi.2022.2276. [DOI] [PubMed] [Google Scholar]
- 34.Standl E., Schnell O. Heart failure outcomes and COVID-19. Diabetes Res. Clin. Pract. 2021;175:108794. doi: 10.1016/j.diabres.2021.108794. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Rey J.R., Caro-Codón J., Rosillo S.O., Iniesta M., Castrejón-Castrejón S., Marco-Clement I., Martín-Polo L., Merino-Argos C., Rodríguez-Sotelo L., García-Veas J.M., et al. Heart failure in COVID-19 patients: Prevalence, incidence and prognostic implications. Eur. J. Heart Fail. 2020;22:2205–2215. doi: 10.1002/ejhf.1990. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Bader F., Manla Y., Atallah B., Starling R.C. Heart failure and COVID-19. Heart Fail. Rev. 2021;26:1–10. doi: 10.1007/s10741-020-10008-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Bader M.W., Adeen A.M.A., Hetta O.E., Fallata M.H., Alsiraihi A.A., Ahmed M.E., Kinsara A.J., Hetta O.E., Aloufi A.K., Alsiraihi A.A., et al. Association between COVID-19 Infection and Cardiac Biomarkers in Hospitalized Patients at a Tertiary Care Center. Cureus. 2023;15:e41527. doi: 10.7759/cureus.41527. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Al Oweidat K., Al-Amer R., Saleh M.Y., Albtoosh A.S., Toubasi A.A., Ribie M.K., Hasuneh M.M., Alfaqheri D.L., Alshurafa A.H., Ribie M., et al. Mortality, Intensive Care Unit Admission, and Intubation among Hospitalized Patients with COVID-19: A One-Year Retrospective Study in Jordan. J. Clin. Med. 2023;12:2651. doi: 10.3390/jcm12072651. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Singh N., Anchan R.K., Besser S.A., Belkin M.N., Cruz M.D., Lee L., Yu D., Mehta N., Nguyen A.B., Alenghat F.J. High sensitivity Troponin-T for prediction of adverse events in patients with COVID-19. Biomarkers. 2020;25:626–633. doi: 10.1080/1354750X.2020.1829056. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Azevedo R.B., Botelho B.G., de Hollanda J.V.G., Ferreira L.V.L., de Andrade L.Z.J., Oei S.S.M.L., Mello T.d.S., Muxfeldt E.S. Covid-19 and the cardiovascular system: A comprehensive review. J. Hum. Hypertens. 2021;35:4–11. doi: 10.1038/s41371-020-0387-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Chung M.K., Zidar D.A., Bristow M.R., Cameron S.J., Chan T., Harding C.V., Kwon D.H., Singh T., Tilton J.C., Tsai E.J., et al. COVID-19 and Cardiovascular Disease. Circ. Res. 2021;128:1214–1236. doi: 10.1161/CIRCRESAHA.121.317997. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Gómez-Mesa J.E., Galindo-Coral S., Montes M.C., Martin A.J.M. Thrombosis and Coagulopathy in COVID-19. Curr. Probl. Cardiol. 2021;46:100742. doi: 10.1016/j.cpcardiol.2020.100742. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Lo Y.A., Jok C., Tse H. Cardiovascular complications of COVID-19. Hong Kong Med. J. 2022;28:249–256. doi: 10.12809/hkmj209217. [DOI] [PubMed] [Google Scholar]
- 44.Asakura H., Ogawa H. COVID-19-associated coagulopathy and disseminated intravascular coagulation. Int. J. Hematol. 2021;113:45–57. doi: 10.1007/s12185-020-03029-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Flumignan R.L., Civile V.T., Tinôco J.D.d.S., Pascoal P.I., Areias L.L., Matar C.F., Tendal B., Trevisani V.F., Atallah N., Nakano L.C. Anticoagulants for people hospitalised with COVID-19. Cochrane Database Syst. Rev. 2022;2022:CD013739. doi: 10.1002/14651858.CD013739.pub2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Cipriani A., Capone F., Donato F., Molinari L., Ceccato D., Saller A., Previato L., Pesavento R., Sarais C., Fioretto P., et al. Cardiac injury and mortality in patients with Coronavirus disease 2019 (COVID-19): Insights from a mediation analysis. Intern. Emerg. Med. 2021;16:419–427. doi: 10.1007/s11739-020-02495-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Lombardi C.M., Carubelli V., Iorio A., Inciardi R.M., Bellasi A., Canale C., Camporotondo R., Catagnano F., Dalla Vecchia L.A., Giovinazzo S., et al. Association of Troponin Levels with Mortality in Italian Patients Hospitalized with Coronavirus Disease 2019: Results of a Multicenter Study. JAMA Cardiol. 2020;5:1274–1280. doi: 10.1001/jamacardio.2020.3538. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Battaglini D., Lopes-Pacheco M., Castro-Faria-Neto H.C., Pelosi P., Rocco P.R.M. Laboratory Biomarkers for Diagnosis and Prognosis in COVID-19. Front. Immunol. 2022;13:857573. doi: 10.3389/fimmu.2022.857573. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Huang J., Gao J., Zhu W., Feng R., Liu Q., Chen X., Huang J., Yang Z., Lin X., Zhang Z., et al. Indicators and prediction models for the severity of Covid-19. Int. J. Clin. Pract. 2021;75:e14571. doi: 10.1111/ijcp.14571. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Qin J.-J., Cheng X., Zhou F., Lei F., Akolkar G., Cai J., Zhang X.-J., Blet A., Xie J., Zhang P., et al. Redefining Cardiac Biomarkers in Predicting Mortality of Inpatients with COVID-19. Hypertension. 2020;76:1104–1112. doi: 10.1161/HYPERTENSIONAHA.120.15528. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Peiris S., Nates J.L., Toledo J., Ho Y.-L., Sosa O., Stanford V., Aldighieri S., Reveiz L. Hospital readmissions and emergency department re-presentation of COVID-19 patients: A systematic review. Rev. Panam. Salud Pública. 2022;46:e142. doi: 10.26633/RPSP.2022.142. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Lionte C., Sorodoc V., Haliga R.E., Bologa C., Ceasovschih A., Petris O.R., Coman A.E., Stoica A., Sirbu O., Puha G., et al. Inflammatory and Cardiac Biomarkers in Relation with Post-Acute COVID-19 and Mortality: What We Know after Successive Pandemic Waves. Diagnostics. 2022;12:1373. doi: 10.3390/diagnostics12061373. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
The data presented in this study are available in article.