Abstract
Background
Electronic health literacy is an emerging skill that needs to be focused on by the health system. Adopting and utilizing digital/electronic health tools helps healthcare providers with evidence-based decision-making during patient care. Therefore, pooling robust evidence could help determine the magnitude of health professionals’ level of electronic health literacy.
Methods
We used PubMed, Science Direct, EMBASE, African Journal Online, Google Scholar, and HINARI to search for systematic review studies. The study procedure was performed using the PRISMA flow diagram. We employed the revised version of the Assessment of Multiple Systematic Reviews (AMSTAR-2) checklist to score the quality of the included studies. The pooled effect size of the outcome variable was determined via a forest plot.
Results
Generally, three systematic review studies addressing 16 primary studies were included. Nearly 6435 study participants with an outcome of interest were included in this umbrella review. The overall pooled magnitude of good e-health literacy among health professionals was 55% (95% CI: 50, 60; I2 = 94.4%). The average pooled effect-size of good eHealth literacy was positively associated with perceived usefulness, educational status, favorable attitudes, internet access, and perceived ease of use, 2.29 (95% CI: 1.82, 2.76), I2 = 0.0, P = 0.990.
Conclusions
A moderate level of eHealth literacy was discovered. It is mandatory to improve healthcare professionals’ internet access, as they are the first front-line information users in their duty of care. It is desirable to design programs and policies to strengthen national eHealth literacy by providing pertinent digital skill booster training regarding electronic health tools, enhancing the positive attitudes of health professionals toward easing and using digital tools to help patients access the most up-to-date information across the area of care. Furthermore, building mechanisms to gain and increase the knowledge of health professionals is a mandatory task for every sector of the health system.
Keywords: Electronic health literacy, digital health, review of reviews, health professionals, Ethiopia
Introduction
Electronic health, also known as eHealth or digital health, is the application of information and communication technologies (ICTs) in healthcare and public health.1–3 Electronic health contains important features, such as electronic health records (EHRs), which are digital representations of a patient's medical history and include diagnoses, treatments, test results, and other medical information. 4 EHRs enable healthcare professionals to securely store, access, and share medical data. Broadly, digital health includes categories such as telemedicine, mobile health (mHealth), wearable devices, health information technologies, and other personalized medicine. Owing to rapid digital technology growth in the healthcare environment, health professionals, such as medical doctors, nurses, health informaticians, and medical imaging radiographers, intensively utilize digital equipment to provide health services to patients.5–7 According to the explanations of the WHO (World Health Organization), electronic health/digital health is a tool that can assist healthcare providers in providing a more holistic approach to viewing patients’ health by accessing their data and providing more control over their health status. 7 Additionally, digital health has benefited both health institutions and patients by offering real opportunities to improve medical outcomes and enhance efficiency.
According to the report highlighted by the WHO, establishing a global digital health system that will help facilitate global mobility and protect citizens across the world from ongoing and future health threats, such as pandemics, and developing a wide range of digital technologies to deliver better health for all is the first building block for the global initiative on digital health. 8 Similarly, evidence from the WHO indicates that effectively delivering potential national or regional digital health initiatives must be guided by a robust strategy that can integrate financial, organizational, human, and technology resources. Hence, the global strategy of digital health is mapped to promote healthy lives and well-being for everyone everywhere, at all ages, without discrepancies.7,9
The application of electronic or digital 10 health technologies would empower clients/patients to make informed and better decisions regarding their health and provide a new care approach for facilitating prevention, early diagnosis of life-threatening diseases, and management of chronic diseases in addition to traditional healthcare environments.1,2,11–13 The use of digital health technologies by health professionals in developing countries is usually affected or challenged by different factors, such as the limited availability of infrastructure (availability and reliability of electricity, internet connectivity, and mobile network coverage) and cultural acceptance (due to cultural bias, mistrust, or resistance toward new digital technologies). In addition, healthcare service delivery via digital tools might be affected by poor digital literacy and skills, which can hamper the users, health professionals, and patients’ technical skills required to use these technologies effectively. Similarly, a lack of technical training among healthcare providers could affect the implementation of digital health in developing countries such as Ethiopia.14–19 Based on the national electronic health strategy, eHealth should be viewed as an essential infrastructure underpinning the exchange of information between the participants in the healthcare system as a key enabler and driver for improved health outcomes for the population. 20
Research has revealed that having good digital health or electronic health literacy alone is not enough unless the confidence of health professionals in making health decisions is scaled up. 21 Thus, bridging the gaps that health professionals face while using digital technologies in healthcare service delivery is necessary to advance the culture of digital health information usage. Owing to the variety of digital/electronic health literacy levels in Ethiopia, many systematic reviews and meta-analyses3,13,17 have reported inconsistent results ranging from 49.6% to 59.4%, with varying degrees of quality scores. Furthermore, there is conflicting information on the effects of many of the variables regarding the outcome (level of electronic or digital health literacy) of interest. Therefore, performing a comprehensive overview of the conducted systematic and meta-analysis results of the outcome of interest would bring and narrow the conflicts arising from the variations inflicted. As a result, the purpose of conducting this umbrella review was tailored to narrow the gaps and consolidate the results of the systematic reviews and meta-analysis studies on eHealth literacy by bringing a single result that could be mapped to publish an all-inclusive finding that might be compared and contrasted. To the best of our knowledge, this umbrella review is the first of its kind conducted in Ethiopia to delve into eHealth literacy and associated factors. The results of this umbrella review support the ability of the country to meet the digital health strategy outlined by the WHO for future advancements. Similarly, the findings of this analysis can help health professionals’ digital health literacy levels meet the demands of the country's digital thinking. Furthermore, decision-makers will also benefit from the findings.
Methods
Definition of umbrella reviews
An umbrella review is a review that combines findings from many systematic reviews and meta-analyses on a single topic. It aims to provide a complete summary of the evidence by examining the breadth of available research, detecting trends, and highlighting areas for additional investigation. 22 Umbrella reviews, or systematic reviews of previous systematic reviews, provide a comprehensive overview of what is available on a particular topic and are used for clinical and policy decisions. 23 Through systematic and meta-analyses, umbrella reviews employ a methodological strategy to search for studies and evaluate the quality, synthesis, and reporting of the results.24,25 Umbrella reviews draw intuitive conclusions by conducting systematic reviews with a consistent approach to variables, allowing for a full evaluation that incorporates previously published systematic reviews or meta-analyses. 25 An umbrella review can also be used to quickly evaluate a large body of evidence and compare results from previous systematic reviews. 26
Eligibility criteria
The current study reported the following Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) reporting guidelines. 27 The umbrella review was registered in PROSPERO, and the registration number is CRD42024581952.
We included all eligible systematic reviews and meta-analyses (SRMAs) that used observational study designs (cross-sectional) to examine the level of digital/electronic health literacy and the relationships between digital or electronic literacy and several associated factors (perceived ease of use, perceived usefulness, ICT training, attitudes, knowledge, and internet use). These studies fulfilled the eligibility criteria: study area (studies conducted in Ethiopia), published in the English language, published including health professionals as the study population, study design, all SRMA studies, and the conditions for publication, as published and unpublished. In this study, we were forced to exclude study results that did not disclose the magnitude of digital or eHealth literacy.
Search strategy
Mulugeta Desalegn Kasaye (MDK) and Asressie Molla Tessema (AMT) searched published systematic reviews and meta-analyses regarding digital or electronic health literacy from August to 20 September 2024. We first checked whether the title was registered via the Epistemonikos database and found no results. A combination of Boolean logic operators (AND, OR, NOT), Medical Subject Headings (MeSH), and keywords was used to search the SRMA studies. We used PubMed, ScienceDirect, EMBASE, African Journal Online, Google Scholar, and HINARI.
We applied the following key search terms to the current umbrella review.
((((((digital health) OR (electronic health)) AND (digital literacy)) OR (electronic literacy)) AND (Health literacy) AND (health professionals)) AND (Ethiopia)) AND (systematic review [Publication Type])) OR (systematic reviews [Publication Type])) AND (Meta-analysis [Publication Type]).
Study selection process
All the search results were exported to EndNote 20 for identification within the scope of the inclusion criteria. After identifying the systematic reviews and meta-analysis results through our search method, we removed duplicate studies. Articles with titles, abstracts, and full texts were screened and assessed. The retrieved publications were reviewed independently in duplicate (AGG and NY). Any disagreements between the authors on the admissibility of individual studies were resolved by discussion with two of the reviewers (AAA and MHK).
Data extraction
Duplicate data extraction was performed. We extracted the data for this umbrella review, which consisted of data related to the publication year of the studies, publication year of the primary studies, number of studies in each systematic review and meta-analysis, authors, number of study participants, primary outcome (magnitude of electronic health or digital health literacy), and associated factors, via Microsoft Excel 16.
Primary outcome
The primary outcome of the umbrella study was electronic health literacy or digital health literacy, which can be defined as the ability of individuals to find, comprehend, and use health information from electronic sources. This involves the ability to navigate digital platforms, critically analyze online health information, and use that knowledge to make informed healthcare decisions. In our context, digital health or electronic health literacy is about health professionals’ ability to use digital platforms and search for health information for their clinical decision-making practice.28,29 Therefore, we used electronic health literacy or digital health literacy interchangeably for the sake of this umbrella review.
The quality assessment report for systematic review and meta-analysis studies
Owing to the subjective nature of systematic reviews and the presence of bias, assessing and evaluating the quality of these systematic reviews and meta-analysis papers would increase the quality of the umbrella review. Although many instruments have been designed to evaluate different aspects of reviews, the AMSTRA was developed to critically appraise systematic reviews of randomized trials. Currently, there is a new modified critical appraisal tool (i.e. AMSTRA-2) for systematic reviews of both randomized and nonrandomized studies on healthcare interventions. Therefore, we assessed the quality of the relevant systematic reviews and meta-analysis studies via the AMSTRA-2 (Assessment of Multiple Systematic Reviews) quality assessment tool. 23 The update tool includes 16 items that assess different domains of systematic reviews, yielding a more comprehensive evaluation than the original tool (AMSTRA). 30 The domains consist of whether the authors: Did the authors provide an explicit statement that the review methods were established before the conduct of the review? Were the included studies appropriately selected? Did the authors use a comprehensive literature search strategy? Did the authors perform a study selection in duplicate? Did the authors extract data in duplicate? Did the authors provide a list of excluded studies and justify the exclusions? Did the authors assess the risk of bias for included studies? and Did the authors consider the risk of bias when interpreting the results? Were the methods for statistical analysis described?
Did the authors account for the risk of bias in the individual studies when concluding? Did the authors discuss the limitations of the included studies? Did the authors provide a funding source for the systematic review? Were the included studies randomized? Did the authors assess the applicability of the findings? Did the authors assess the presence of publication bias? And, did the authors provide a rationale for their conclusions?. 23 The responses are listed in the tool as “Yes,” “Partial Yes,” “No,” or “No meta-analysis conducted.” Two of the review authors for each of the included SRM studies scored the 16-item questions. Disagreements observed during the scoring were resolved by EBE. The final results of our umbrella review were categorized as high, moderate, low, or critically low on the basis of the updated AMSTRA-2 23 and previous studies.3,13,17
Data analysis
During the current umbrella review, the tasks for complete data synthesis and statistical analysis were performed via the statistical software STATA 17. A summary of estimates of the magnitude of digital or electronic health literacy and several associated factors is presented. A clear narrative synthesis was used to describe the findings of the included SRMA studies, which were sequenced by an overall meta-analysis. The pooled magnitude and effect sizes were analyzed and presented via a random effects model. The Higgins et al. 31 recommendation for meta-analysis of SRMA studies was employed for studies representing significant heterogeneity (i.e. I2 = 75/100% or higher).
Results
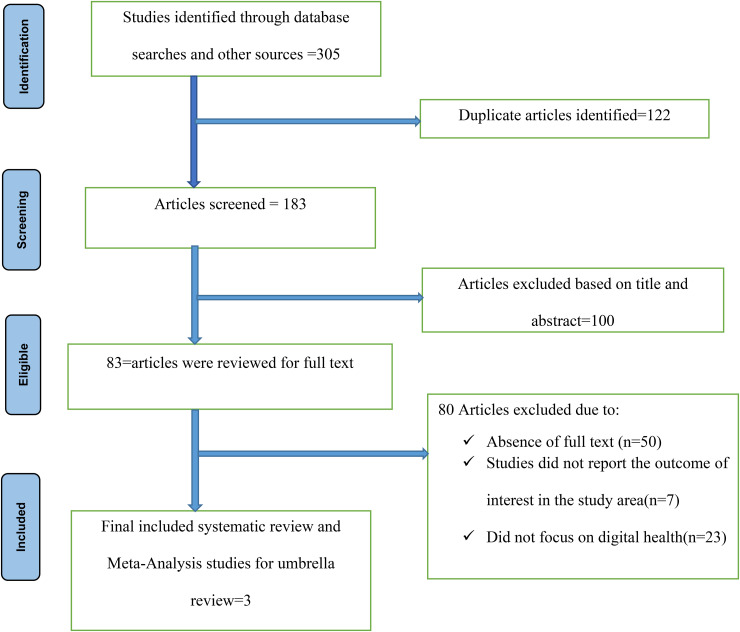
From a total of 305 studies retrieved from the main electronic databases, 183 studies were eligible for additional screening. Owing to the course of duplication, 122 articles were removed from all identified studies. After a critical evaluation, 100 articles were eliminated on the basis of title and abstract as selection criteria. In this umbrella review, 80 of the screened articles were excluded because of the absence of the full text, which does not report the outcome of interest (Figure 1).
Figure 1.
Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) for searching for and identifying systematic reviews and meta-analyses.
Characteristics of the included systematic review and meta-analysis studies for the current Umbrella review
The current umbrella review was endorsed based on 16 observational studies (i.e. cross-sectional studies). The median number of studies included in each SRMA was five, ranging from three to six. The median number of studies included in each SRMA with the outcome of interest (digital/electronic health literacy) was 5, equal to the median value for the separate studies. This umbrella review consists of 1758–2739 study participants. The selected systematic review and meta-analysis studies were published in recent years. All of the included SRMA studies reported and assessed the quality of the primary studies via the Newcastle Ottawa Scale (NOS). All the included studies reported the magnitude and determinants of digital or electronic health literacy. The magnitude of digital/electronic health literacy ranged from 49.85% (95% CI: 37.22–62.47) 3 to 59.39% (95% CI: 47.10–71.68). 17 The PubMed, Google Scholar, Global Health, and HINARI databases were the most frequently searched outlets for systematic review studies (Table 1).
Table 1.
Characteristics of the included systematic review and meta-analysis studies on the digital health literacy of health professionals in Ethiopia.
| S. no. | Author and year | Publication period of primary studies | Databases covered in the search strategy | Included studies | Sample size | Risk of bias | Primary Outcome of the review | Reported magnitude | Reporter factor |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Wubante et al., 2023 | 2019–2022 | PubMed, Embrace, Web of Science, Scopus, Google Scholar, and the African Journal Online | Five institutional cross-sectional studies | 1758 | Clear quality appraisal using NOS | eHealth literacy | 59.39% | Perceived usefulness (AOR = 2.46; 95% CI: 1.36, 3.12), educational status (AOR = 2.28; 95% CI: 1.11, 4.68), internet access (AOR = 2.35; 95% CI: 1.67, 3.30), knowledge on electronic health information sources (AOR = 2.60; 95% CI: 1.78, 3.78) |
| 2. | Chereka et al., 2022, 2024 | 2020–2023 | Google Scholar, PubMed, Cochrane Library, Hinari, CINAHL, and Global Health | Five cross-sectional studies | 1938 | Clear quality appraisal using NOS | Digital literacy | 49.85% | Monthly incomes AOR = 3.89 (95% CI:1.03–14.66), computer literacy 2.93 (95% CI: 1.27–6.74), perceived usefulness 1.68 (95% CI:1.59–4.52), educational status 2.56 (95% CI: 1.59–4.13), attitude 2.23 (95% CI: 1.49–3.35), perceived ease of use 2.22 (95% CI: 1.52–3.23) |
| 3 | Kasaye et al., 2024 | 2022–2023 | Medline, PubMed, Cochrane Library, CINAHL, HINARI, Science Direct, Google Scholar, and Global Health. | Six cross-sectional studies | 2739 | Clear quality appraisal using NOS | Digital health literacy | 56% | internet use (AOR = 2.72, 95% CI: 1.86, 3.98), perceived ease of use (AOR = 2.79, 95% CI: 1.83, 4.25), favorable-attitude (AOR = 2.49, 95% CI:1.61,3.85), perceived usefulness (AOR = 2.29,95% CI:1.65,3.18), information-communication-technology training (AOR = 6.09, 95% CI: 1.83, 24.27), and educational-level (AOR = 3.60, 95% CI: 2.96, 4.37). |
Nature of the included primary studies
We mapped the primary studies within the three SRMA studies that were included, and whether the reviews were based on the same primary evidence was determined.
From a total of 16 primary studies included in our review (Table 1), only four studies32–35 were included in two of the systematic reviews and meta-analyses,3,13 and the papers reported about the same concept of our research title (i.e. digital health or e-health literacy as mapped into the same context). Similarly, one primary study 36 was included in two of the SRMA studies13,17 and reported on the eHealth literacy of health professionals. Five primary studies were included in the SRMA studies after a critical evaluation of the three SRMA studies. Among the five primary studies included in one of the SRMA studies, 17 only one primary study 36 was included, which was then incorporated into another SRMA study. 13 In addition, one of the primary studies 37 was mapped to two of the identified SRMA13,17 studies. In this case, we can conclude that any umbrella review could result from the overlapping nature of the primary studies mapped in each systematic review and meta-analysis study. This is the main drawback of any umbrella review. However, three primary37–39 studies were specific to only Wubante et al., 17 and one primary study 40 was included by Kasaye et al. 13 These specific studies showed no overlap (Table 2).
Table 2.
Quality assessment via AMSTAR-2.
| AMSTAR-2 items a | Quality score | ||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Authors | year | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | Total | |
| Wubante et al. 17 and Chereka et al. 3,34 | 2023 | 2 | 2 | 0 | 2 | 2 | 2 | 2 | 1 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 29 | Moderate |
| Chereka et al.3,34 | 2024 | 2 | 1 | 2 | 2 | 2 | 2 | 2 | 1 | 2 | 0 | 2 | 2 | 2 | 2 | 2 | 0 | 26 | Moderate |
| Kasaye et al. 13 | 2024 | 2 | 2 | 0 | 2 | 2 | 2 | 2 | 1 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 2 | 29 | Moderate |
AMSTAR: assessment of multiple systematic reviews.
Scores for each item are between 0 and 2, where one point is awarded if the study has partial inclusion methods that reduce bias, and two points are awarded for full inclusion of methods to reduce the risk of bias. The tool was adapted from https://amstar.ca/Amstar_Checklist.php.
Meta-analysis of the magnitude of eHealth literacy
All of the studies included in this umbrella review reported the magnitude of eHealth literacy. The overall pooled magnitude of eHealth literacy among health professionals in Ethiopia under this umbrella review was estimated to be 55% (95% CI: 50, 60; I2 = 94.4%) (Figure 2). The magnitude of the outcome of interest in the SRMA studies ranged from 49.85% (95% CI: 37.22–62.47) 3 to 59.39% (95% CI: 47.10–71.68). 17 This indicates that the magnitude of health professionals with good eHealth Literacy was moderate. The conclusion that 55% of health professionals had “good” eHealth literacy indicates that slightly more than half of those polled have the abilities required to effectively use digital health information and tools.
Figure 2.
Magnitude of eHealth literacy among health professionals in Ethiopia, umbrella review analysis.
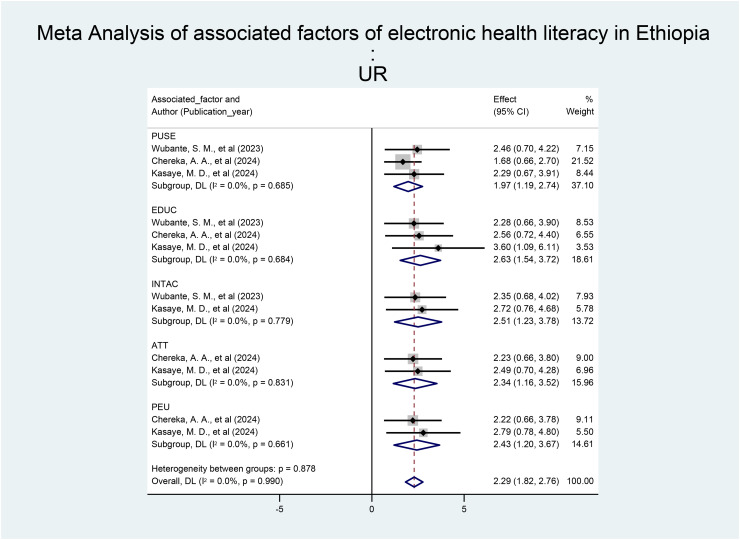
Meta-analysis of factors associated with electronic health literacy
In this umbrella review, we tried to identify predictors of eHealth literacy among health professionals in Ethiopia. In this review of meta-analyses of studies concerning eHealth literacy, all of the included studies3,13,17 reported that perceived usefulness (PU) was positively associated with health professionals’ eHealth literacy. The odds of good eHealth literacy among health professionals who perceived the usefulness of electronic tools for healthcare service delivery as useful were 1.97 (95% CI: 1.19, 2.74) times greater than those who had not perceived them as useful. In this umbrella review, with all the included SRMA articles, the educational level of health professionals was found to be positively associated with good eHealth literacy. The pooled odds of good eHealth literacy among health professionals with master's degree holders and above were 2.63 times (95% CI: 1.54, 3.72) greater than those among health professionals with bachelor's degrees and diplomas. With respect to access to the internet, two studies13,17 yielded positive and significant information, and for health professionals who had access to the internet, the level of electronic/digital health literacy was found to be good. The pooled odds of good e-health literacy among health professionals who had internet access were 2.51 times (95% CI: 1.23, 3.78) greater than those among health professionals who had no internet access.
In addition, for the SRMA studies included in our current umbrella review, two studies3,13 indicated that health professionals had favorable attitudes toward good eHealth literacy. The pooled odds of good electronic health among health professionals with favorable attitudes were 2.34 times (95% CI: 1.16, 3.52) greater than those among health professionals who had unfavorable attitudes. Furthermore, in this review of systematic reviews, perceived ease of use (PEU) was observed to have a positive and significant effect on two3,13 of the included studies. The pooled odds of good eHealth literacy among health professionals who had greater perceived ease of use were 2.43 times (95% CI: 1.20, 3.67) greater than those among health professionals who had lower perceived ease of use (Figure 3).
Figure 3.
Factors associated with eHealth literacy among health professionals in Ethiopia, umbrella review analysis.
Quality assessment
AMSTAR-2 critical appraisal for SRMA studies was used to evaluate the methodological quality of the included studies in the current umbrella review. 23 The final quality score was moderate after scoring the 16 items, with each item scoring 0 to 2 points (Table 2). We identified the quality of the included SRMA studies, and the limitations included the third, 10th, and 16th items for assessing the quality of these included systematic and meta-analytic studies. This indicates that the included SRMA studies were limited in the selection of the study designs for inclusion, and reports regarding sources of funding and potential conflicts of interest were not indicated.
Discussions
In our current umbrella review, we attempt to aggregate the findings from the three systematic reviews and meta-analyses and provide a comprehensive overview of the eHealth literacy levels of healthcare professionals in the Ethiopian context. Umbrella reviews can indeed identify an overall trend, pattern, and consensus in the area of different research landscapes that may not be apparent from a single review. Therefore, our currently conducted umbrella review summarized the existing reviews regarding electronic or digital health literacy among healthcare professionals and yielded less time-consuming findings for readers in the area of interest, and presented them in a single output. 41 Similarly, in this umbrella review, the author assessed the quality of the included studies, which could allow the readers to gauge the reliability of the evidence presented above. We tried to uncover the main limitations of umbrella reviews as their reliance on the quality and comprehensiveness of the underlying systematic review, and the umbrella review synthesize, findings from multiple systematic reviews; any biases, methodological flaws, or gaps in the original reviews may affect the overall conclusions. Umbrella reviews, while useful, have limitations. One significant disadvantage is their reliance on the quality and reporting of the included systematic reviews and meta-analyses, which may result in the exclusion of original studies that have not yet been included. Furthermore, variation in exposure and outcome assessment among studies can pose a problem.
Hence, this umbrella review pointed out that the magnitude of eHealth literacy was mapped in a single study and presented a summary estimate of 55% (95% CI: 50,60), which is higher than that reported in the primary study conducted in Amhara, 34 Malaysia. 42 Similarly, our findings in the present study were greater than the pooled estimated effect size (magnitude) of e-health literacy (37%) reported in Korea, 43 (36%), and Canada. 44 The possible discrepancy might be because the current study showed that the estimated effect of e-health literacy among health professionals in Ethiopia is currently the adoption of digital tools as a public health initiative, which has led the country to focus more on these digital platforms, enhancing access to information and services. The other possible reason might be the large number of participants we employed, as we summarized the different systematic review and meta-analysis studies, rather than the small number of participants included in those primary studies.
However, the pooled result of our umbrella review revealed a smaller proportion of electronic health literacy than the pooled estimate of a study performed on the association between digital health literacy and health outcomes. 45
In our current study, we identified factors contributing to the eHealth literacy of health professionals. Thus, in this review of meta-analyses of studies, the pooled estimate of PU, Pooled-OR-PU = 1.97 (95% CI: 1.19, 2.74), was positively associated with health professionals’ eHealth literacy.3,13,17 This study is in line with a synthesis review study that examined the advocacy of health literacy and eHealth literacy in large longitudinal studies. 46 The possible justification might be that health professionals with good eHealth literacy are likely to perceive digital health tools as more useful, as they can propagate and evaluate these resources effectively during patient care. With the same level of knowledge, health professionals who perceived digital health tools as useful were 1.97 times more likely than health professionals who perceived digital health tools to be useful. This result is in line with the pooled estimate of the study performed.3,47
The educational status of health professionals was significantly associated with their good eHealth literacy level. The pooled odds of good eHealth literacy among Ethiopian health professionals in the included studies3,13,17 were 2.63 times (95% CI: 1.54, 3.72) greater than those among health professionals with bachelor's degrees and diplomas. 45 The reason we found is that the higher educational level of health professionals allows them to make informed decisions on the basis of the latest evidence they retrieved via online platforms, which might impact their clinical practice more than professionals with low-level education.16,45,48
In our review, two studies13,17 revealed a significant positive association between internet access and health professionals’ good electronic or digital health literacy levels. For those who had internet access, the level of electronic/digital health literacy was good. The pooled odds of good e-health literacy among health professionals who had internet access were 2.51 times (95% CI: 1.23, 3.78) greater than those among health professionals who had no internet access. This result is consistent with the results of a systematic review performed in China 49 and Thailand, 50 possibly because having access to the internet plays a crucial role in the ability of healthcare providers to acquire and evaluate health-related information.1,11,51,52
Additionally, in our recent umbrella review, two studies3,13 indicated that health professionals had a favorable attitude toward good eHealth literacy. The pooled odds of good electronic health among health professionals with favorable attitudes were 2.34 times (95% CI: 1.16, 3.52) greater than those among health professionals who had unfavorable attitudes. This finding is consistent with a scoping research output.3,25,52,53
Furthermore, in this review of systematic reviews, PEU was observed to have a positive and significant effect among two3,13 of the included studies. The pooled odds of good eHealth literacy among health professionals who had greater perceived ease of use were 2.43 times (95% CI: 1.20, 3.67) greater than those among health professionals who had lower perceived ease of use (Figure 3). This means that greater perceived ease of use is associated with a greater likelihood of adopting electronic health tools. If health professionals find a tool easy to use, they are more likely to incorporate it into their routine healthcare activities.3,54
Conclusions and recommendations
This systematic review of reviews revealed a moderate level of electronic health (digital health literacy) among health professionals in Ethiopia. In addition, the study revealed a significant association between health professionals’ good e-health literacy and their ability to adopt and utilize e-health information sources via internet access. Similarly, the study revealed five significant and positively associated factors: health professionals’ attitudes, educational status, perceived ease of use, perceived usefulness, and internet access. Providing good internet access, improving positive attitudes, and building mechanisms to gain and increase the knowledge of health professionals are mandatory tasks to be considered by every sector of the health system. The national digital health policy should target adopting digital tools to ensure equitable access to electronic health-based technologies that could promote the implementation of data-driven decision making through technology. Similarly, incorporating digital literacy into CPD frameworks, integrating ICT into pre-service training is recommended to improve the digital health literacy of these health professionals.
Acknowledgements
The authors would like to extend their gratitude to the systematic reviews of the published articles for providing valuable information for this study.
Footnotes
ORCID iD: Mulugeta Desalegn Kasaye https://orcid.org/0000-0002-3968-2518
Author contributions: This review was developed and investigated by Mulugeta Desalegn Kasaye (MDK). Mulugeta Desalegn Kasaye (MDK), Anas Ali Alhur (AAA), and Dr. Asressie Molla Tessema (AMT) searched published systematic reviews and meta-analyses regarding digital or electronic health literacy. The retrieved publications were reviewed independently in duplicate by Dr. Amare Gebrie Getahun (AGG) and Nega Yimer (NY). Any disagreements between the authors on the admissibility of individual studies were resolved by discussion with two of the reviewers (AAA and MHK). The manuscript was drafted by MDK, AMT, MHK, NY, and AAA. Data analyses were performed and reviewed by all the authors equally. The final paper was read and approved by all the authors.
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Availability of data and materials: The data sets that could aid the reviews of this review might be available from the corresponding author (Mulugeta Desalegn Kasaye) on a reasonable request.
Guarantor: Mulugeta Desalegn Kasaye
References
- 1.Brørs G, Larsen MH, Hølvold LBet al. et al. Ehealth literacy among hospital health care providers: a systematic review. BMC Health Serv Res 2023; 23: 1144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Castiglia P, Dettori M, Arghittu A, et al. Use of digital technologies in public health: a narrative review. Acta bio-medica: Atenei Parmensis 2023; 94: e2023164. [DOI] [PubMed] [Google Scholar]
- 3.Chereka AA, Walle AD, Kassie SY, et al. Evaluating digital literacy of health professionals in Ethiopian health sectors: a systematic review and meta-analysis. PloS One 2024; 19: e0300344. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Honavar SG. Electronic medical records – the good, the bad and the ugly. Indian J Ophthalmol 2020; 68: 417–418. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Sharma S, Mohanty V, Balappanavar AY, et al. Role of digital Media in promoting oral health: a systematic review. Cureus 2022; 14: e28893. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Stewart E, Milton A, Yee HF, et al. Ehealth tools that assess and track health and well-being in children and young people: systematic review. J Med Internet Res 2022; 24: e26015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.World Health Organization. What is Digital Health? Available from: https://www.fda.gov/medical-devices/digital-health-center-excellence/what-digital-health.
- 8.World Health Organization. The European Commission and WHO launch landmark digital health initiative to strengthen global health security 2023 [Available from: https://www.who.int/news/item/05-06-2023-the-european-commission-and-who-launch-landmark-digital-health-initiative-to-strengthen-global-health-security.
- 9.WHO. Global strategy on digital health 2020-2025 2021 [Available from: https://www.who.int/publications/i/item/9789240020924. [PubMed]
- 10.Slevin P, Kessie T, Cullen J, et al. Exploring the potential benefits of digital health technology for the management of COPD: a qualitative study of patient perceptions. ERJ Open Res 2019; 5: 1–10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Biggs JS, Willcocks A, Burger Met al. et al. Digital health benefits evaluation frameworks: building the evidence to support Australia's national digital health strategy. Med J Aust 2019; 210: S9–S11. [DOI] [PubMed] [Google Scholar]
- 12.Cheung J, Chan CY, Cheng HY. The effectiveness of interventions on improving the mental health literacy of health care professionals in general hospitals: a systematic review of randomized controlled trials. J Am Psychiatr Nurses Assoc 2023; 31: 10783903231194579. [DOI] [PubMed] [Google Scholar]
- 13.Kasaye MD, Kebede N, Kalayou MH, et al. Digital health literacy and associated factors among health professionals during the outbreak of coronavirus pandemic in Ethiopia: a systematic review and meta-analysis. Digital Health 2024; 10: 20552076241271799. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Manyazewal T, Woldeamanuel Y, Blumberg HM, et al. The potential use of digital health technologies in the African context: a systematic review of evidence from Ethiopia. NPJ Digital Med 2021; 4: 125. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Walle AD, Demsash AW, Adem JB, et al. Exploring facilitators and barriers of the sustainable acceptance of e-health system solutions in Ethiopia: a systematic review. PloS One 2023; 18: e0287991. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Watson J, Hanna K, Talbot C, et al. A systematic review of digital access to post-diagnostic health and social care services for dementia. Int J Geriatr Psychiatry 2024; 39: e6119. [DOI] [PubMed] [Google Scholar]
- 17.Wubante SM, Tegegne MD, Melaku MS, et al. Ehealth literacy and its associated factors in Ethiopia: systematic review and meta-analysis. PloS one 2023; 18: e0282195. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Yehualashet DE, Seboka BT, Tesfa GA, et al. Barriers to the adoption of electronic medical record system in Ethiopia: a systematic review. J Multidiscip Healthc 2021; 14: 2597–2603. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Yeo G, Reich SM, Liaw NAet al. et al. The effect of digital mental health literacy interventions on mental health: systematic review and meta-analysis. J Med Internet Res 2024; 26: e51268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.World Health Organization. National eHealth strategies crucial to achieving universal health coverage 2013 [Available from: https://www.afro.who.int/news/national-ehealth-strategies-crucial-achieving-universal-health-coverage.
- 21.De Santis K, Jahnel T, Sina E, et al. Digital health literacy and COVID-19 pandemic: results of a nationwide survey in Germany. Eur J Public Health 2021; 31: ckab164.274. [Google Scholar]
- 22.Higgins J. Cochrane handbook for systematic reviews of interventions. Chichester, UK: Cochrane Collaboration and John Wiley & Sons Ltd, 2008. [Google Scholar]
- 23.Shea BJ, Reeves BC, Wells G, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. bmj. 2017;358. [DOI] [PMC free article] [PubMed]
- 24.Smith V, Devane D, Begley CMet al. et al. Methodology in conducting a systematic review of systematic reviews of healthcare interventions. BMC Med Res Methodol 2011; 11: 15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Aromataris E, Riitano D. Systematic reviews: constructing a search strategy and searching for evidence. AJN Am J Nurs 2014; 114: 49–56. [DOI] [PubMed] [Google Scholar]
- 26.JBI. JBI Evidence Synthesis releases first issue for 2024 2024 [Available from: https://jbi.global/news/article/jbi-evidence-synthesis-releases-first-issue-2024.
- 27.Parums DV. Review articles, systematic reviews, meta-analysis, and the updated preferred reporting items for systematic reviews and meta-analyses (PRISMA) 2020 guidelines. Med Sci Monitor: Int Med J Exp Clin Res 2021; 27: e934475–1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Norman CD, Skinner HA. eHEALS: the eHealth literacy scale. J Med Internet Res 2006; 8: e507. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Richtering SS, Morris R, Soh S-E, et al. Examination of an eHealth literacy scale and a health literacy scale in a population with moderate to high cardiovascular risk: Rasch analyses. PLoS One 2017; 12: e0175372. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Shea BJ, Grimshaw JM, Wells GA, et al. Development of AMSTAR: a measurement tool to assess the methodological quality of systematic reviews. BMC Med Res Methodol 2007; 7: 10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med 2002; 21: 1539–1558. [DOI] [PubMed] [Google Scholar]
- 32.Ahmed MH, Guadie HA, Ngusie HS, et al. Digital health literacy during the COVID-19 pandemic among health care providers in resource-limited settings: cross-sectional study. JMIR Nurs 2022; 5: e39866. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Assaye BT, Kassa M, Belachew M, et al. Association of digital health literacy and information-seeking behaviors among physicians during COVID-19 in Ethiopia: a cross-sectional study. Digital Health 2023; 9: 20552076231180436. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Chereka AA, Demsash AW, Ngusie HSet al. et al. Digital health literacy to share COVID-19 related information and associated factors among healthcare providers worked at COVID-19 treatment centers in Amhara region, Ethiopia: a cross-sectional survey. Inform Med Unlocked 2022; 30: 100934. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Tegegne MD, Tilahun B, Mamuye A, et al. Digital literacy level and associated factors among health professionals in a referral and teaching hospital: an implication for future digital health systems implementation. Front Public Health 2023; 11: 1187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Tesfa GA, Yehualashet DE, Ewune HA, et al. Ehealth literacy and its associated factors among health professionals during the COVID-19 pandemic in resource-limited settings: cross-sectional study. JMIR Form Res 2022; 6: e36206. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Shiferaw KB, Mehari EA, Eshete T. Ehealth literacy and internet use among undergraduate nursing students in a resource limited country: a cross-sectional study. Inform Med Unlocked 2020; 18: 100273. [Google Scholar]
- 38.Mengestie ND, Yilma TM, Beshir MAet al. et al. Ehealth literacy of medical and health science students and factors affecting eHealth literacy in an Ethiopian university: a cross-sectional study. Appl Clin Inform 2021; 12: 301–309. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Chakilu Tilahun B, Fikadie Endehabtu B, Gullslett MKet al. et al. E-health literacy and associated factors among chronic patients in a low-income country: a cross-sectional survey. 2020. [DOI] [PMC free article] [PubMed]
- 40.Assaye BT, worku Shimie A. Telemedicine use during COVID-19 pandemics and associated factors among health professionals working in health facilities at resource-limited setting 2021. Inform Med Unlocked 2022; 33: 101085. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Aromataris E, Fernandez R, Godfrey CM, et al. Summarizing systematic reviews: methodological development, conduct and reporting of an umbrella review approach. JBI Evid Implement 2015; 13: 132–140. [DOI] [PubMed] [Google Scholar]
- 42.Marzo RR, Su TT, Ismail R, et al. Digital health literacy for COVID-19 vaccination and intention to be immunized: a cross sectional multi-country study among the general adult population. Front Public Health 2022; 10: 998234. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Kim K, Shin S, Kim Set al. et al. The relation between eHealth literacy and health-related behaviors: systematic review and meta-analysis. J Med Internet Res 2023; 25: e40778. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Elgamal R. Meta-analysis: eHealth literacy and attitudes towards internet/computer technology. Patient Educ Couns 2024; 123: 108196. [DOI] [PubMed] [Google Scholar]
- 45.Yuen E, Winter N, Savira F, et al. Digital health literacy and its association with sociodemographic characteristics, health resource use, and health outcomes: rapid review. Interact J Med Res 2024; 13: e46888. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Neter E, Brainin E. Association between health literacy, eHealth literacy, and health outcomes among patients with long-term conditions. Eur Psychol 2019; 24: 1–12. [Google Scholar]
- 47.Sham S, Shiwlani S, Kumar SK, et al. Empowering patients through digital health literacy and access to electronic medical records (EMRs) in the developing world. Cureus 2024; 16: 1–4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Verweel L, Newman A, Michaelchuk W, et al. The effect of digital interventions on related health literacy and skills for individuals living with chronic diseases: a systematic review and meta-analysis. Int J Med Inf 2023; 177: 105114. [DOI] [PubMed] [Google Scholar]
- 49.Zhang Y, Xu P, Sun Q, et al. Factors influencing the e-health literacy in cancer patients: a systematic review. J Cancer Surviv 2023; 17: 425–440. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Rojanasumapong A, Jiraporncharoen W, Nantsupawat N, et al. Internet use, electronic health literacy, and hypertension control among the elderly at an urban primary care center in Thailand: a cross-sectional study. Int J Environ Res Public Health 2021; 18: 9574. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Mitsutake S, Shibata A, Ishii Ket al. et al. Associations of eHealth literacy with health behavior among adult internet users. J Med Internet Res 2016; 18: e192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Belfrage SL, Husted M, Fraser S, et al. A systematic review of the effectiveness of community-based interventions aimed at improving health literacy of parents/carers of children. Perspect Public Health 2023; 145: 17579139231180746. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Verma R, Saldanha C, Ellis U, et al. Ehealth literacy among older adults living with cancer and their caregivers: a scoping review. J Geriatr Oncol 2022; 13: 555–562. [DOI] [PubMed] [Google Scholar]
- 54.Davis FD. Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Q 1989; 13: 319–340. [Google Scholar]