Abstract
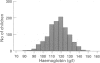
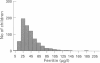
AIM: To identify the optimum age to screen for iron deficiency, the normal distribution of haemoglobin and ferritin in a representative population sample was investigated. METHODS: Normal values for haemoglobin and ferritin were measured from heel prick capillary samples obtained from a representative cohort of 1175 infants at 8 months old who were randomly selected from children taking part in the Avon Longitudinal Study of Pregnancy and Childhood (ALSPAC). RESULTS: Haemoglobin was normally distributed: mean (SD) 117 (11) milligrams, 95% confidence interval (CI) 116 to 118, and range 72-153 milligrams. Ferritin was log normally distributed: geometric mean 38.5 micrograms/l, 95% CI 37.0 to 39.9, range 7.1-224 micrograms/l. The 5th centile for haemoglobin was 97 milligrams and for ferritin 16.9 micrograms/l. No correlation was found between haemoglobin and ferritin. Multiple regression analysis showed ferritin concentrations to be positively related to birth weight (p < 0.0001) and the sex of the child (girls with higher concentrations) (p < 0.0001) but negatively with the child's weight at 8 months (p < 0.0001). Haemoglobin concentrations were positively related to the child's weight at 8 months (p = 0.04). Neither haemoglobin nor ferritin concentrations were related to social class as measured by maternal education level. CONCLUSION: These data define the normal range for haemoglobin and ferritin in capillary samples in the UK population, and suggest that anaemia is common in infancy. Using current recommendations, 23% of infants would be identified as anaemic. For British infants at 8 months of age, a more representative 'cut off' for anaemia would be haemoglobin concentration < 97 milligrams and for iron deficiency ferritin < 16 micrograms/l.
Full text
PDF


Images in this article
Selected References
These references are in PubMed. This may not be the complete list of references from this article.
- Aukett M. A., Parks Y. A., Scott P. H., Wharton B. A. Treatment with iron increases weight gain and psychomotor development. Arch Dis Child. 1986 Sep;61(9):849–857. doi: 10.1136/adc.61.9.849. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Burman D. Haemoglobin levels in normal infants aged 3 to 24 months, and the effect of iron. Arch Dis Child. 1972 Apr;47(252):261–271. doi: 10.1136/adc.47.252.261. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Duggan M. B., Steel G., Elwys G., Harbottle L., Noble C. Iron status, energy intake, and nutritional status of healthy young Asian children. Arch Dis Child. 1991 Dec;66(12):1386–1389. doi: 10.1136/adc.66.12.1386. [DOI] [PMC free article] [PubMed] [Google Scholar]
- James J., Evans J., Male P., Pallister C., Hendrikz J. K., Oakhill A. Iron deficiency in inner city pre-school children: development of a general practice screening programme. J R Coll Gen Pract. 1988 Jun;38(311):250–252. [PMC free article] [PubMed] [Google Scholar]
- Liappis N., Mallmann R., Schlebusch H. Vergleich der Ferritin- und Eisen-Konzentration in Kapillar- und Venenblutserum von Kindern, Jugendlichen und Erwachsenen. Klin Padiatr. 1992 Nov-Dec;204(6):444–446. doi: 10.1055/s-2007-1025386. [DOI] [PubMed] [Google Scholar]
- Mills A. F. Surveillance for anaemia: risk factors in patterns of milk intake. Arch Dis Child. 1990 Apr;65(4):428–431. doi: 10.1136/adc.65.4.428. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oski F. A. Iron deficiency in infancy and childhood. N Engl J Med. 1993 Jul 15;329(3):190–193. doi: 10.1056/NEJM199307153290308. [DOI] [PubMed] [Google Scholar]
- Stevens D. Epidemiology of hypochromic anaemia in young children. Arch Dis Child. 1991 Jul;66(7):886–889. doi: 10.1136/adc.66.7.886. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Walter T., De Andraca I., Chadud P., Perales C. G. Iron deficiency anemia: adverse effects on infant psychomotor development. Pediatrics. 1989 Jul;84(1):7–17. [PubMed] [Google Scholar]
- Yip R., Johnson C., Dallman P. R. Age-related changes in laboratory values used in the diagnosis of anemia and iron deficiency. Am J Clin Nutr. 1984 Mar;39(3):427–436. doi: 10.1093/ajcn/39.3.427. [DOI] [PubMed] [Google Scholar]