Abstract
Analogous to the clinical use of recombinant high-affinity antibodies, transfer of T cell receptor genes may be used to create a T cell compartment specific for self-antigens to which the endogenous T cell repertoire is immune tolerant. Here we show in a spontaneous prostate carcinoma model that the combination of vaccination with adoptive transfer of small numbers of T cells that are genetically modified with a tumor-specific TCR results in a marked suppression of tumor development, even though both treatments are by themselves without effect. These results demonstrate the value of TCR gene transfer to target otherwise non-immunogenic tumor-associated self-antigens provided that adoptive transfer occurs under conditions that allow in vivo expansion of the TCR-modified T cells.
This is an author-produced version of a manuscript accepted for publication in The Journal of Immunology (The JI). The American Association of Immunologists, Inc. (AAI), publisher of The JI, holds the copyright to this manuscript. This version of the manuscript has not yet been copyedited or subjected to editorial proofreading by The JI; hence, it may differ from the final version published in The JI (online and in print). AAI (The JI) is not liable for errors or omissions in this author-produced version of the manuscript or in any version derived from it by the U.S. National Institutes of Health or any other third party. The final, citable version of record can be found at www.jimmunol.org.
Introduction
The shared tumor-associated antigens (TAAs) that are potential targets of cancer immunotherapy primarily consist of non-mutated self-antigens that are either lineage-specific or overexpressed. Due to immunological tolerance towards these proteins, B cells producing high affinity antibodies and T cells expressing high-affinity T cell receptors (TCRs) are often deleted, making the remaining repertoire relatively unresponsive to active immunization. Furthermore, for those antigens for which self tolerance is incomplete, the process of tumor development can actively tolerize the remaining T cells (1). In the absence of an effective endogenous TAA-specific immune repertoire, passive immunization with TAA-specific antibodies or T cells may be considered a preferred approach (2). In line with this, the clinical use of recombinant antibodies such as Rituximab that targets CD20 and Trastuzumab that targets Her2/Neu has been a major advance in the treatment of human cancer over the past decade (3).
Analogous to the transfer of high-affinity antibodies, adoptive transfer of exogenous tumor-specific TCRs into endogenous T cells (a process hereafter referred to as TCR gene transfer) might be used to generate T cells directed towards TAAs such as WT-1 and PRAME. Like the HER-2/neu protein targeted by Trastuzumab, these antigens are non-mutated proteins that are over expressed by cancer cells, being either leukemic (4) or melanoma cells (5). Furthermore, for all these proteins, over-expression contributes to cellular transformation, making tumor escape a less likely event (6-8). In the present study, we set out to analyse the value of TCR gene transfer in the targeting of this class of tumor-associated antigens in a murine spontaneous tumor model. These experiments assess the feasibility of TCR gene therapy for tumor types for which classical forms of adoptive T cell therapy may be precluded and compare it to the value of active vaccination.
Materials and Methods
Mice
C57BL/6 (B6) and TRAMP mice (9) were obtained from the Experimental Animal Department of The Netherlands Cancer Institute. For all experiments F1 offspring of B6 * TRAMP mice was used. All animal experiments were performed in accordance with institutional and national guidelines and were approved by the Experimental Animal Committee of The Netherlands Cancer Institute.
Retroviral constructs and retroviral transduction of T cells
The SV40IV specific TCR α and β chains were cloned by standard procedures from the cytotoxic T lymphocyte clone Y-4. The Y-4 clone was isolated by limiting dilution from CTL derived from B6 mice immunized with SV40 large T antigen transformed syngeneic kidney cells and has been described previously (10). A pMX-SV40α-IRES-SV40β vector was generated and used to transfect Phoenix-E packaging cells to generate retrovirus (11). Mouse splenocytes were modified by retroviral transduction as described previously (12).
Flow cytometry
Surface TCR expression was measured 24 hours post transduction by flow cytometry. Cells wecd anti-TCR Vβ9 mAb and PE-labeled anti-TCR Vβ2, 3, 4, 5.1, 8, 11 and 10b mAb (anti Vβ-pool), or with MHC tetramers, in combination with PE- or APC-conjugated anti-CD8α mAb (all mAbs from Pharmingen, except PE-conjugated anti-CD8α mAb from Caltag). Propidium iodide (Sigma) was used to select for live cells. For the measurement of antigen-specific T cell responses in peripheral blood, samples were taken at the indicated days post-transfer. Following removal of erythrocytes by NH4Cl treatment, cells were stained with the above-mentioned antibodies and analyzed by flow cytometry. For analysis of SV40-specific T cell responses in spleen and prostate, mice were sacrificed 11 days post-vaccination, spleen and prostate tissue were harvested and single cell suspensions were obtained by macerating tissues through a 40 μm nylon cell strainer. Intracellular IFN-γ staining was performed as previously described (12). Data acquisition and analysis was done on a FacsCalibur (Becton Dickinson, MountainView, CA) with FCS Express software (De Novo Software, Thornhill, Ontario, Canada) or CELLQuest-Pro software (BD Biosciences).
Viral infection
For live influenza A infections, anesthetized mice were infected by intranasal administration of 50 μl of HBSS (Life Technologies, Grand Island, NY) containing 1000 plaque forming units (PFU) of influenza A/WSN/33 (WSN)-SV40(IV) virus (flu-T) (Schepers et al, unpublished data). For vaccinia infections, 1×105 PFU rVV-ES-IV (rVV-T) was injected intraperitoneally (13).
Histopathology
Tissues were sampled in buffered formalin, and stained with haematoxylin and eosin. The sections were reviewed with a Zeiss Axioskop2 Plus microscope (Carl Zeiss Microscopy, Jena, Germany) equipped with Plan-Apochroma (×5/0.16, ×10/0.45, ×20/0.60, and ×40/0.95) and Plan-Neofluar (×2.5/0.075) objectives. In addition to the objectives, there was an extra enlargement device included in the body of the microscope. Images were captured with a Zeiss AxioCam HRc digital camera and processed with AxioVision 4 software (both from Carl Zeiss Vision, München, Germany). Pathological examination and classification of the prostate gland, coagulation gland and seminal vesicles was performed blindly, according to The Consensus Report from the Bar Harbor Meeting of the Mouse Models of Human Cancer Consortium (14).
Immunohistochemistry
Immunohistochemistry was carried out on buffered formalin sections. Sections were pre-incubated with PBS/ 4% BSA. For large T immunostaining, sections were stained for 1hr with SV40 pb 101 primary antibody (1:500, Becton Dickinson), followed by a two-step immunoenzymatic procedure. First, biotin labeled goat-anti mouse immunoglobulins (DAKO, 1:500, 1hr) were applied, followed by HRP-labeled avidin-biotin complex (ABC) (DAKO, 1hr). AEC (Sigma) was used as a substrate-chromagen and slides were counterstained with haematoxylin. Images were acquired using an Axiocam HR digital camera and processed with Axiovision 4 software (Carl Zeiss Vision GmbH, München, Germany).
Statistical analysis
To test whether two treatments had the same underlying multinomial (ordered) distribution of type of pathology, a Stratified Wilcoxon-Mann-Whitney test for ordered categorical responses was used. Two-sided p-values are reported.
Results
Development of neoplastic lesions and SV40 expression in TRAMP mice
TRAMP (transgenic adenocarcinoma of mouse prostate) mice express the transforming protein SV40 large T under control of the prostate specific Probasin promoter, resulting in the development of prostatic intraepithelial neoplasia (PIN) lesions from 8-12 weeks of age and carcinomas by 18 weeks of age ((9); see below). The epithelial cells within prostate areas that undergo pathologic alterations (ranging from atypical hyperplasia to carcinomas) display high SV40 large T expression, as evidenced by immunohistochemistry (Fig. 1, A-C). In contrast, SV40 large T expression in prostate cells with a normal morphology is generally below the limit of detection (Fig. 1, A-C).
FIGURE 1. Detection of SV40 Large T expression in transformed cells.

A-C, Large T expression in the prostate gland of a 9-week old TRAMP mouse. Prostate cells in areas undergoing atypical hyperplasia are large T immunostaining positive (B), whereas prostate cells with a normal morphology are large T immunostaining negative (C). Original magnifications: 10× (A) and 40× (B-C).
The endogenous T cell repertoire of TRAMP mice is tolerant towards SV40IV at the time neoplastic lesions first develop
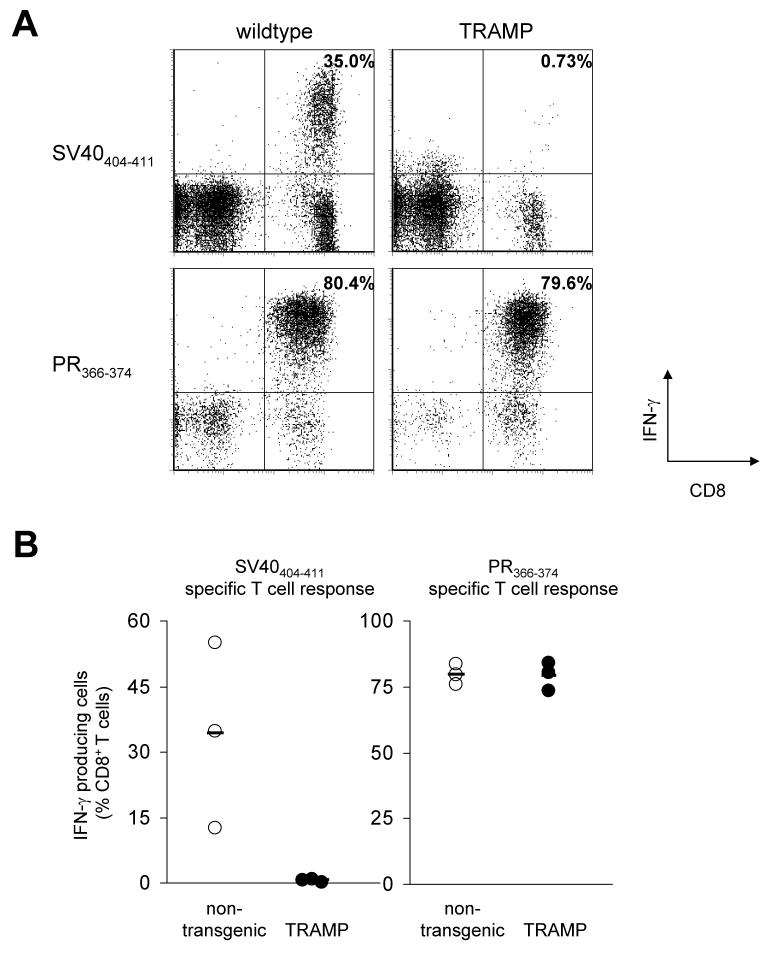
Prior work has demonstrated that young (4-7 week) male TRAMP mice harbour a residual low avidity T cell repertoire specific for SV40IV, the immunodominant epitope of the large T oncoprotein. However, from 10 weeks of age onwards this low avidity T cell repertoire is no longer detectable (15). To corroborate these data, 11-week old TRAMP mice and non-transgenic littermates were infected with an influenza A strain expressing SV40IV, the immunodominant epitope of large T (flu-T). Analysis of ex vivo spleen samples (data not shown) or in vitro restimulated T cell cultures revealed that IFN-γ producing SV40IV-specific T cells were barely detectable in TRAMP mice, but abundantly present in non-transgenic littermates (Fig. 2, A-B). Furthermore, when reactivity against the SV40IV epitope was monitored by MHC tetramer staining, SV40IV,-specific T cell responses were also highly reduced in vaccinated TRAMP mice (data not shown). Consistent with prior peptide and DC vaccination studies (15, 16), these data demonstrate that the endogenous T cell repertoire of TRAMP mice is tolerant towards SV40IV at the time prostatic lesions first develop. The restricted over-expression of large T in (pre)malignant tissue, its role in transformation and the induction of tolerance towards large T in TRAMP mice, make this protein comparable to tumor-associated self antigens such as WT-1 and PRAME.
FIGURE 2. TRAMP mice are tolerant towards the tumor-associated SV40IV epitope.
A-B, TRAMP mice and as a control non-transgenic littermates received an intranasal flu-T infection. 10 days post infection, spleen cells were isolated and cultured in the presence of either SV40404-411 or (as a control) the influenza A nucleoprotein derived PR366-374 epitope (5×10-4 μg/ml) for 14 days. Antigen specific T cells were measured by intracellular IFNγ staining after incubation with 100 ng/ml of the relevant peptide. Shown are dot-plots of 2 representative cultures (A) and cumulative data of all cultures (B). Numbers in upper right corner of dot-plots refer to percentage of IFNγ+ CD8+ cells of total CD8+ cells. Circles in graphs represent individual mice, bars indicate averages.
TCR gene transfer can be used to create a SV40IV-reactive T cell compartment that is otherwise absent in TRAMP mice
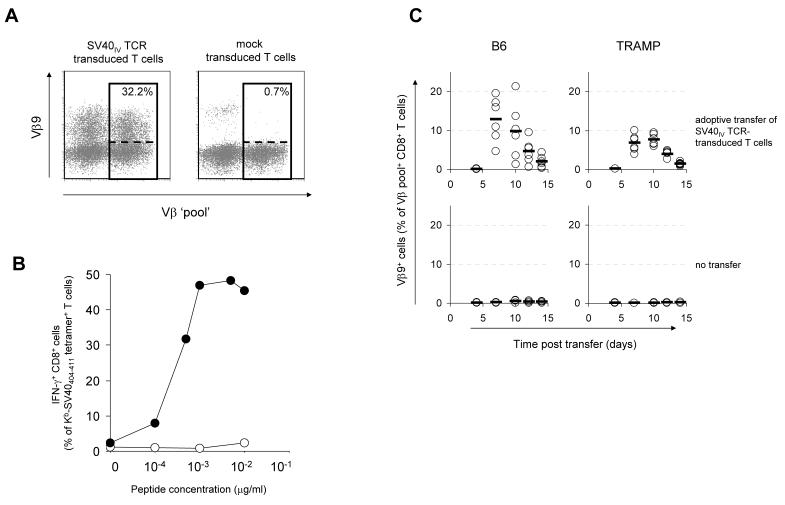
Prior work has shown that the combination of vaccination with adoptive transfer of T cells modified with a relevant TCR - but not a control TCR - can be used to induce self antigen-specific T cell responses (17). To assess the value of the induction of self antigen-reactive T cell responses by TCR gene transfer in the targeting of developing tumors, we isolated an SV40IV-specific TCR (11) and used this TCR to modify T cells of TRAMP mice. Following retroviral transduction, on average 25-40% of CD8+ T cells expressed the SV40IV TCR, and these cells produced IFNγ upon incubation with the relevant antigen in vitro (Fig. 3, A-B). To address whether SV40IV TCR modified T cells could proliferate upon in vivo antigen encounter, TRAMP mice and as a control B6 mice received an adoptive transfer of 1×105 SV40IV TCR CD8+ T cells, followed by an intranasal flu-T infection. Subsequently, TCR-modified T cell responses were monitored by measuring the fraction of T cells expressing one of a set of endogenous Vβ elements together with the Vβ element used by the introduced TCR (17). Although an endogenous SV40IV-specific T cell response could not be detected in TRAMP mice (Fig. 2), SV40IV-TCR transduced T cells proliferated strongly upon antigen encounter in vivo, as assessed by the emergence of a Vβ9+Vβ-pool+ T cell population. In line with the notion that the Vβ9+Vβ-pool+ T cell population consists of TCR-modified T cells, no increase in Vβ9+Vβ-pool+ T cell numbers was seen in recipients of mock-transduced T cells (Fig. 3C, bottom panels). Frequencies of Vβ9+Vβ-pool+ T cells peaked around day 10 post-transfer and subsequently decreased significantly. This contraction of the TCR-modified-specific T cell response is consistent with prior data on the kinetics of endogenous vaccine-induced influenza A-specific T cell responses (18) and is also observed for the endogenous SV40IV-specific T cell response in B6 mice (data not shown). These experiments show that TCR gene transfer can be used to create a TAA-reactive T cell compartment that is otherwise absent (Fig. 3C). Interestingly, SV40IV-TCR transduced T cell responses in TRAMP mice are on average approximately 1.5-2 fold lower than those in B6 controls (average peak T cell response of 8.0% versus 12.9%), suggesting that tolerizing mechanisms may have some impact on the in vivo potential of TCR-modified T cells.
FIGURE 3. SV40IV-TCR transduced T cells recognize antigen in vitro and in vivo.
A, Flow cytometric analysis of SV40IV-TCR (left panel) or mock (right panel) transduced T cells. The transduction efficiency of the SV40IV-TCR was determined by calculating the percentage of Vβ9+ cells within the population of Vβ-pool+ cells (represented in right upper corner of dot plot). Average transduction percentage was 25-40%. B, Functional analysis of SV40IV-TCR transduced splenocytes. Cells were incubated in the presence of SV40404-411 (closed circles) or control OVA257-264 peptide (open circles) at the indicated concentrations. Prior to incubation, a sample of the transduced T cells was stained with Kb-SV40404-411 tetramers and PE-anti-CD8α antibodies to determine the percentage of SV40IV-specific CD8+ cells. Post peptide stimulation, cells were stained with APC-anti-CD8α, permeabilized and stained with PE-anti-IFNγ. C, Flow cytometric analysis of blood cells of B6 (left panels) and TRAMP mice (right panels) that received 1×105 SV40IV-TCR transduced T cells (top panels) or no transfer of T cells (bottom panels) followed by an i.n. infection with 1000 p.f.u. of flu-T. Blood was sampled 3-14 days post infection. Circles represent TCR-transduced T cell responses in individual mice; bars indicate averages.
In vivo distribution and function of SV40IV TCR-modified T cells
To examine the in vivo distribution and function of SV40IV TCR-modified T cells, prostate glands and spleen samples were isolated from TRAMP and B6 mice at day 11-post vaccination. As expected, Vβ9+Vβ-pool+ T cells were detected in spleen samples from B6 and TRAMP mice that had received SV40IV TCR-modified T cells, whereas in control mice that were only vaccinated this population was absent (Figure 4A-B). Furthermore, Vβ9+Vβ-pool+ T cells were also detected in prostate samples from B6 and TRAMP mice, indicating that homing to the prostate can occur independent of antigen expression. Splenic T cells in B6 and TRAMP mice produced high levels of IFNγ after stimulation with the SV40IV antigen. In TRAMP but not B6 mice, this production was dependent upon adoptive T cell transfer, reflecting that an endogenous SV40IV-specific T cell repertoire is lacking in TRAMP but not B6 mice. Notably, no substantial antigen-specific IFNγ production was detected within prostate tissue, suggesting that the effector function of TCR-modified T cells may possibly be suppressed at this site (Figure 4).
FIGURE 4. Homing and functional properties of SV40IV-TCR modified T cells.
10-week old TRAMP mice and control non-transgenic littermates received an adoptive transfer of 5×105 SV40IV-TCR transduced T cells, followed by vaccination by i.p. infection with 1×105 p.f.u. of rVV-T. Control mice were solely vaccinated with rVV-T. 11 days post vaccination, the frequency of TCR transduced cells in spleen and prostate was assessed by analysing the percentage of Vβ9+Vβ-pool+ CD8+ cells of total Vβ-pool+ CD8+ cells. Functionality of SV40IV-specific T cells was measured by intracellular IFN-γ staining after incubation for 4 hours with 100 ng/ml of the relevant peptide (SV40404-411) or control peptide (OVA257-264). Shown are dot-plots from a mouse in each of the treatment groups (A) and cumulative data from all mice (B). Numbers in upper right corner of dot-plots refer to percentage of Vβ9+Vβpool+ cells of total CD8+ cells or IFNγ+CD8+ cells of total CD8+ cells. Circles in graphs represent individual mice, bars indicate averages.
A combination of adoptively transferred SV40IV TCR-modified T cells and vaccination leads to the long-term suppression of tumor progression in TRAMP mice
To determine the potential impact of adoptive cell therapy (ACT) with TCR-modified T cells on tumor development, a pilot study was performed. A first group of TRAMP mice (n=5) received vaccination with two SV40IV-recombinant viruses at week 10 (when PIN lesions are detectable in prostate and coagulation glands in the majority of animals), and at week 16. A second group of mice received vaccination with the same recombinant viruses plus ACT with a small number of TCR-modified T cells (5*105) at the same time points. Two weeks after the second treatment (week 18), mice were sacrificed and analysed ‘blindly’ for tumor development in prostate glands, coagulation glands and seminal vesicles. In 5/5 mice that only received vaccination microinvasive or invasive carcinomas had developed (Table 1). In marked contrast, microinvasive carcinoma development was only seen in 1 out of 5 mice treated by ACT and atypical hyperplasia and PIN were observed in all other mice (Table 1). This first experiment suggested that ACT with TCR-modified T cells may be effective in preventing tumor outgrowth. However it did not address the long-term effect of ACT with TCR-modified T cells.
Table 1.
| Prostate | |||||
|---|---|---|---|---|---|
| No abnormality | Atypical hyperplasia | Intraepithelial neoplasia | Microinvasive Carcinoma | Invasive carcinoma | |
| TCR gene transfer | 0/5 | 4/5 | 1/5 | 0/5 | 0/5 |
| Vaccinia | 0/4 | 0/4 | 0/4 | 2/4 | 2/4 |
| No treatment | 0/4 | 0/4 | 0/4 | 0/4 | 4/4 |
| Non transgenic littermates | 2/3 | 1/3 | 0/3 | 0/3 | 0/3 |
| Coagulation glands | |||||
|---|---|---|---|---|---|
| No abnormality | Atypical hyperplasia | Intraepithelial neoplasia | Microinvasive Carcinoma | Invasive carcinoma | |
| TCR gene transfer | 0/5 | 0/5 | 3/5 | 2/5 | 0/5 |
| Vaccinia | 0/4 | 0/4 | 0/4 | 1/4 | 3/4 |
| No treatment | 0/4 | 0/4 | 0/4 | 0/4 | 4/4 |
| Non transgenic | |||||
| littermates | 3/3 | 0/3 | 0/3 | 0/3 | 0/3 |
| Seminal Vesicles | ||||
|---|---|---|---|---|
| No abnormality | Atypical hyperplasia | Adenoma | Adeno carcinoma | |
| TCR gene transfer | 5/5 | 0/5 | 0/5 | 0/5 |
| Vaccinia | 0/4 | 0/4 | 4/4 | 0/5 |
| No treatment | 0/4 | 1/4 | 2/4 | 1/4 |
| Non transgenic | ||||
| littermates | 3/3 | 0/3 | 0/3 | 0/3 |
To address this issue, a large cohort of mice was treated with the same protocol and then left without further intervention until week 28 (4 months after the start of ACT/vaccination). Furthermore, to test for a potential effect of vaccination by itself on tumor progression, a third group of mice was included that was left fully untreated (experimental setup in Fig. 5A, analysis of TCR-modified T cell responses in Fig. 5B). At week 28, mice were sacrificed to analyse tumor development in prostate glands, coagulation glands and seminal vesicles (Fig. 5, C-D). In untreated mice, carcinomas developed in all prostate glands (100% of mice) as well as in coagulation glands (60% of mice). In the seminal vesicles, atypical hyperplasia (50% of mice) and adenomas (40% of mice) were detected. Importantly, in mice treated by vaccination only, the incidence of carcinomas in prostate glands (100% of mice) and coagulation glands (55% of mice), and the incidence of adenomas in the seminal vesicles (67% of mice) was not reduced to any measurable extent (p=0.9152, Wilcoxon-Mann-Whitney test). However, when mice received the same vaccination protocol in combination with infusion of SV40IV-TCR modified TRAMP T cells, the incidence of carcinomas and adenomas was substantially reduced. In both prostate and coagulation glands, only premalignant lesions were detected in the majority of mice (73% and 64% of mice, respectively). In the seminal vesicles, no abnormalities were detected in 10/11 mice (Fig. 5, C-D).
FIGURE 5. Adoptive transfer of SV40IV-TCR transduced T cells results in a marked delay in tumor development.
A, Outline of experiment. 10-week old TRAMP mice received an adoptive transfer of 2.5-5×105 SV40IV-TCR-transduced T cells, followed by vaccination by means of an i.p. infection with 1×105 p.f.u. of rVV-T. 6 weeks later the same mice received a 2nd infusion of 2.5-5 × 105 SV40IV-TCR transduced T cells, followed by i.n. infection with 1000 p.f.u. of flu-T. Control mice were either vaccinated with the 2 recombinant viruses, or were left untreated. Blood was sampled at various time points for 2 weeks post each infusion and analysed blindly by flow cytometry. At 28 weeks, mice were sacrificed and indicated sites were analysed for tumor development by histopathology. B, The percentage of Vβ9+Vβpool+ CD8+ cells of total Vβpool+ CD8+ cells in peripheral blood. Circles represent individual mice, bars indicate averages. Shown are results of 1 out of 2 experiments. C, Classification of tumor development in prostate gland, coagulation gland and seminal vesicles in treated and non-treated TRAMP mice. Bars depict the percentage of mice with the indicated lesion type within that cohort. In cases where multiple types of lesions were detected within one organ, the most severe type was used for scoring. Shown are the pooled results of two independent experiments, compared to pathology found in 9-weeks old TRAMP mice (top row). To test for treatment effects, Wilcoxon-Mann-Whitney tests were performed, adjusting for organ type. Vaccination only versus no treatment, p=0.9152; TCR gene transfer versus no treatment, p < 0.0001; TCR gene transfer versus vaccination only, p < 0.0001; TCR gene transfer versus the pathology found in 9 week old mice, p=0.3775. D, Macroscopic analysis of the male reproductive tract of a representative TRAMP mouse of each of the three treatment groups, compared to the male reproductive tract of a 28-week old non-transgenic littermate. E, SV40 large T expression in prostate and coagulation gland of a 28-weeks old TRAMP mouse after 2 transfers of SV40IV-TCR transduced T cells in combination with viral vaccination. Dorsal prostate gland (D); lateral prostate gland (L); coagulation gland (C). Cells showing atypical hyperplasia are SV40 large T immunostaining positive (bottom panels), whereas cells with a normal morphology in the same coagulation gland are SV40 Large T immunostaining negative (left bottom panel). Original magnifications: 2.5x (top panel) and 40x (bottom panels).
These data show in a spontaneous tumor model that the combination of TCR gene transfer and vaccination significantly suppresses tumor progression (p <0.0001) and that this effect is long-lasting (months upon ACT). Notably, the low-grade lesions that are still detected in tissue sections of mice that were treated by TCR gene therapy remain large T-positive (Fig. 5E, lower left panel). In a recent study that showed that vaccination of 8 week old TRAMP mice against Prostate Stem Cell Antigen can lead to the long-term suppression of tumor development, low-grade lesions were also still detectable in treated mice (19). However, in this case the remaining lesions were largely antigen-negative. To provide a possible explanation for the persistence of low-grade lesions in the current setting, in which an antigen essential for tumor growth is targeted, we analysed SV40IV-specific T cell responses of 28 week old TRAMP mice treated by TCR gene therapy. Interestingly, this analysis revealed that SV40IV TCR-modified T cells were barely detectable at this time point in ex vivo spleen samples and could not be expanded in in vitro T cell cultures (data not shown). These data suggest that the prolonged presence of TCR-modified T cells in an antigen-bearing host may lead to deletion. Previous studies in TRAMP mice have demonstrated that both deletion and mechanisms of non-deletional tolerance can impede prostate tumor specific T cell responses (15, 20-23). Future studies will be required to determine which mechanisms of tolerance induction can impair the long-term function of adoptively transferred SV40IV TCR-modified T cells in TRAMP mice.
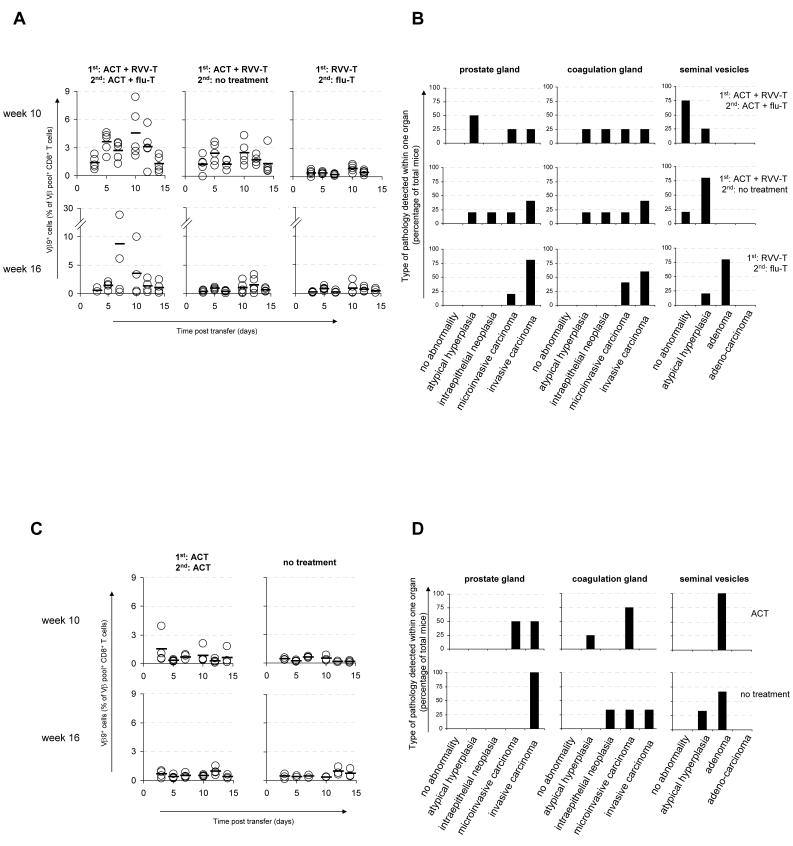
To directly test whether multiple T cell infusions are required for the long-term suppression of tumor progression, TRAMP mice received either a single cycle of TCR-modified T cell transfer/ vaccination at week 10, or two cycles of TCR-modified T cell transfer/ vaccination at week 10 and 16. In both groups of mice tumor progression was significantly (p < 0.01 and p < 0.001 for one and two cycle groups respectively) inhibited as compared to recipients of vaccination only. Thus, whilst there is a (non-significant; p =0.2166) trend towards an increased anti-tumor effect in mice receiving two cycles of ACT, a single cycle of ACT at week 10 can greatly reduce prostate carcinoma development in the following 4 months (Figure 6, A-B).
FIGURE 6. Effect of vaccination and number of treatment cycles on anti-tumor efficacy of SV40IV-TCR modified T cells.
A & B, 10-week old TRAMP mice received an adoptive transfer of 2.5-5×105 SV40IV-TCR-transduced T cells, followed by vaccination by means of an i.p. infection with 1×105 p.f.u. of rVV-T. 6 weeks later, mice did or did not receive a 2nd infusion of 2.5-5 × 105 SV40IV-TCR transduced T cells, followed by i.n. infection with 1000 p.f.u. of flu-T. Control mice were vaccinated with the 2 recombinant viruses without ACT. C & D, 10-week old TRAMP mice received an adoptive transfer of 2.5-5×105 SV40IV-TCR-transduced T cells, followed by a second infusion 6 weeks later. Control mice were left untreated. A & C, Blood was sampled at the indicated time points to determine the percentage of Vβ9+Vβpool+ CD8+ cells of total Vβpool+ CD8+ cells. Circles represent individual mice, bars indicate averages. B & D, At 28 weeks, mice were sacrificed and indicated sites were analysed for tumor development by histopathology. Bars depict the percentage of mice with the indicated lesion type within that cohort. In cases where multiple types of lesions were detected within one organ, the most severe type was used for scoring. To test for treatment effects, Wilcoxon-Mann-Whitney tests were performed. B: Two cycles of ACT/ vaccination versus vaccination only, p < 0.001 ; One cycle of ACT/ vaccination versus vaccination only, p < 0.01; Two cycles of ACT/ vaccination versus one cycle of ACT/ vaccination, p =0.2166; D: TCR gene transfer without concomitant vaccination versus no treatment, p =0.5055.
Concomitant vaccination is an essential requirement for the suppression of prostate carcinoma by adoptively transferred SV40IV TCR-modified T cells in TRAMP mice
The above data demonstrate that the combination of vaccination with TCR-modified T cell transfer suppresses tumor outgrowth. However, these experiments do not address whether vaccination is in fact required to achieve this effect. To address this issue, a group of TRAMP mice received two adoptive transfers of SV40IV TCR-modified T cells at week 10 and week 16 without further vaccination. Analysis of Vβ9+Vβ-pool+ T cell responses in peripheral blood of these animals showed that frequencies of TCR-modified T cells stayed close to background in the absence of vaccination, (Figure 6C). In line with the observation that vaccination is essential to drive expansion of the TCR-modified T cell pool, tumor progression was not measurably affected by the sole transfer of TCR modified T cells (Figure 6D).
Discussion
Approaches for adoptive T cell therapy of human cancer can be divided into two broad categories, based on the use of either allogeneic or of autologous T cells. In allogeneic T cell therapy -as exemplified by donor lymphocyte infusions (DLI) for patients with CML- the infused T cells can recognize polymorphic epitopes expressed by tumor cells as truly foreign antigens, and thus with high avidity (24). The very high response rate seen after DLI treatment (over 50% for patients with relapsed CML (25)) underscores the clinical value of T cells that can recognize tumor-associated antigens with such high avidity. However, the requirement for an allogeneic hematopoietic stem cell transplant, plus the frequent development of Graft-versus-Host-Disease (GvHD), due to T cell recognition of polymorphic antigens expressed by other cell types, form two very substantial limitations of allogeneic T cell therapy. Autologous T cell therapy -by means of infusion of ex vivo expanded patient-derived tumor infiltrating lymphocytes (TILs)- has a substantial clinical effect in patients with metastatic melanoma, with an objective response rate of approximately 50% (26-28). Autologous T cell therapy is not complicated by the development of GvHD, however, it is restricted to those patient groups for which tumor-infiltrating lymphocytes can be isolated. Specifically, while melanoma-reactive T cell responses can be observed rather frequently, for most other tumor types, the detection of T cell infiltrates with a clear potential for tumor recognition is a rare event.
A comparison of the advantages and disadvantages of allogeneic and autologous T cell therapy suggests that the adoptive transfer of T cells that are autologous, but do express high affinity tumor specific TCRs would be an attractive approach, and this has been the goal of efforts to generate redirected T cells by TCR gene transfer (29).
Following a series of in vitro analyses, the in vivo function of TCR gene-modified T cells has been established in mouse models (12, 17, 30, 31). Furthermore, a recent phase I clinical trial in patients with metastatic melanoma has demonstrated that the transfer of TCR modified T cells is clinically feasible and that the resultant cells show long term engraftment in some patients (32). Although the objective response rate in this trial has been low, this study provided the first evidence that -at least for a tumor type that was previously shown to be responsive to TIL treatment- TCR gene therapy is a realistic option.
The goals of the current study were two-fold. First, to establish whether TCR gene therapy could be developed into a realistic option for tumor types for which TIL transfer is not feasible. Second, to make such an assessment in a spontaneous tumor model rather than a transplantable tumor model. The latter issue is of some importance as immunogenicity of unknown neo-antigens that have been introduced or have accumulated during in vitro growth can severely complicate the interpretation of immunological interventions in transplantable tumor models (33). In addition, the aberrant interaction of newly injected tumor cells with the surrounding stroma, and the draining of injected tumor cells to the secondary lymphoid organs may also lead to an over-interpretation of the efficacy of immunotherapeutic intervention (34). In the spontaneous tumor model that was used here, the numbers of endogenous T cells specific for the tumor-associated epitope that is targeted are close to background levels at the age tumor development is first seen ((15); Fig. 2), thereby representing a T cell target antigen for which TIL transfer appears to be precluded. Within this model we show that, whereas vaccination or TCR gene transfer by itself is entirely without effect, the combination of vaccination with TCR gene transfer is highly synergistic. These data directly demonstrate the potential of TCR modified T cells to target tumor types for which classical T cell therapy with autologous tumor-specific T cells has not been possible. As TCRs for antigens such as p53 (35), WT-1 (31), PRAME (unpublished observations) and MDM2 (36) have been isolated, clinical assessment of such therapies can be expected in the coming years.
It seems reasonable to expect that in order to obtain strong T cell responses in such trials, (at least) three ingredients will be required. First, it should be feasible to generate a sufficient number of autologous gene-modified T cells for infusion. As the current data demonstrate that the infusion of a small number of gene modified T cells (1-5×105 of gene-modified T cells; which equals approximately 1% of the total CD8+ T cell compartment) suffices to delay tumor progression, this is unlikely to pose the major problem in future clinical tests. It may however be important to ensure that the infused gene-modified T cells have not undergone terminal differentiation (37).
Second, the sole infusion of TCR gene-modified T cells without further treatment is insufficient for the generation of robust tumor-specific T cell responses (Figure 6). Therefore, a clinically acceptable strategy to promote the expansion of TCR gene-modified T cells is required. Whilst in the current manuscript, in vivo expansion is achieved by vaccination, host conditioning regimens that have originally been developed for TIL therapy may prove equally or even more effective in this respect (de Witte et al., unpublished observations). The development of effective strategies to promote in vivo activation of the TCR-modified T cells also appear to be essential to prevent the tolerization of infused TCR-modified T cell populations. In the current study, SV40IV-TCR transduced T cell responses directly after infusion were on average approximately 1.5-2 fold lower in TRAMP mice than in B6 controls. More importantly, when TCR-modified T cell responses in TRAMP mice were examined months after transfer, reactivity was highly limited. These data are consistent with the notion that the long-term presence of self antigen-reactive T cells in an antigen-bearing host can lead to progressive tolerization (20, 21, 38) and strategies to prevent such tolerization will be valuable.
Third, a collection of (publicly available) high affinity T cell receptors for a series of tumor-associated antigens will need to be created. Biotechnological platforms for TCR isolation may perhaps best be designed by analogy with platforms for recombinant antibody isolation. Specifically, Muromonab-CD3, the first monoclonal antibody registered for clinical use, was obtained by vaccination of mice and immunogenicity of this fully murine antibody and other antibodies of mouse origin has limited their clinical application (39). To avoid the immunogenicity of mouse antibodies in clinical use, increasingly sophisticated approaches for the generation of mAbs with a partial or fully human sequence have been developed in subsequent years, eventually resulting in the creation of mouse strains transgenic for the unrearranged human immunoglobulin loci (40). By analogy to the use of these hIg mouse models for the generation of human antibodies against human self antigens, mouse models that carry the human TCR loci should be of substantial value. Human TCRs obtained from such models may then be used to produce a tumor-reactive T cell repertoire by modification of pre-existing patient derived T cells, or - in the more distant future - such cells may be generated from scratch, through in vitro differentiation of TCR modified T cells from hematopoietic stem cells (41-43).
Acknowledgements
We would like to thank Erwin Swart and Martin van der Valk for technical assistance, Shalin Naik for reading the manuscript and Andrea Vogel for breeding the TRAMP mice.
This research was supported by grants from the Dutch Cancer Society (NKI 2003-2860), the EU 6th Framework program (ATTACK), the National Cancer Institute of the U. S. National Institutes of Health (CA-25000), the American Cancer Society (Research Scholar Grant 04-059-01-LIB) and the Leukaemia Research Fund (06037).
References
- 1.Willimsky G, Blankenstein T. Sporadic immunogenic tumours avoid destruction by inducing T-cell tolerance. Nature. 2005;437:141–146. doi: 10.1038/nature03954. [DOI] [PubMed] [Google Scholar]
- 2.Overwijk WW. Breaking tolerance in cancer immunotherapy: time to ACT. Curr Opin Immunol. 2005;17:187–194. doi: 10.1016/j.coi.2005.01.011. [DOI] [PubMed] [Google Scholar]
- 3.Adams GP, Weiner LM. Monoclonal antibody therapy of cancer. Nat Biotechnol. 2005;23:1147–1157. doi: 10.1038/nbt1137. [DOI] [PubMed] [Google Scholar]
- 4.Gao L, Bellantuono I, Elsasser A, Marley SB, Gordon MY, Goldman JM, Stauss HJ. Selective elimination of leukemic CD34(+) progenitor cells by cytotoxic T lymphocytes specific for WT1. Blood. 2000;95:2198–2203. [PubMed] [Google Scholar]
- 5.Ikeda H, Lethe B, Lehmann F, van Baren N, Baurain JF, de Smet C, Chambost H, Vitale M, Moretta A, Boon T, Coulie PG. Characterization of an antigen that is recognized on a melanoma showing partial HLA loss by CTL expressing an NK inhibitory receptor. Immunity. 1997;6:199–208. doi: 10.1016/s1074-7613(00)80426-4. [DOI] [PubMed] [Google Scholar]
- 6.Inoue K, Tamaki H, Ogawa H, Oka Y, Soma T, Tatekawa T, Oji Y, Tsuboi A, Kim EH, Kawakami M, Akiyama T, Kishimoto T, Sugiyama H. Wilms’ tumor gene (WT1) competes with differentiation-inducing signal in hematopoietic progenitor cells. Blood. 1998;91:2969–2976. [PubMed] [Google Scholar]
- 7.Di Fiore PP, Pierce JH, Kraus MH, Segatto O, King CR, Aaronson SA. erbB-2 is a potent oncogene when overexpressed in NIH/3T3 cells. Science. 1987;237:178–182. doi: 10.1126/science.2885917. [DOI] [PubMed] [Google Scholar]
- 8.Epping MT, Wang L, Edel MJ, Carlee L, Hernandez M, Bernards R. The human tumor antigen PRAME is a dominant repressor of retinoic acid receptor signaling. Cell. 2005;122:835–847. doi: 10.1016/j.cell.2005.07.003. [DOI] [PubMed] [Google Scholar]
- 9.Greenberg NM, DeMayo F, Finegold MJ, Medina D, Tilley WD, Aspinall JO, Cunha GR, Donjacour AA, Matusik RJ, Rosen JM. Prostate cancer in a transgenic mouse. Proc Natl Acad Sci U S A. 1995;92:3439–3443. doi: 10.1073/pnas.92.8.3439. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Tanaka Y, Tevethia MJ, Kalderon D, Smith AE, Tevethia SS. Clustering of antigenic sites recognized by cytotoxic T lymphocyte clones in the amino terminal half of SV40 T antigen. Virology. 1988;162:427–436. doi: 10.1016/0042-6822(88)90483-7. [DOI] [PubMed] [Google Scholar]
- 11.Kessels HW, Schepers K, van den Boom MD, Topham DJ, Schumacher TN. Generation of T cell help through a MHC class I-restricted TCR. J Immunol. 2006;177:976–982. doi: 10.4049/jimmunol.177.2.976. [DOI] [PubMed] [Google Scholar]
- 12.Kessels HW, Wolkers MC, van den Boom MD, van der Valk MA, Schumacher TN. Immunotherapy through TCR gene transfer. Nat Immunol. 2001;2:957–961. doi: 10.1038/ni1001-957. [DOI] [PubMed] [Google Scholar]
- 13.Blaney JE, Jr., Nobusawa E, Brehm MA, Bonneau RH, Mylin LM, Fu TM, Kawaoka Y, Tevethia SS. Immunization with a single major histocompatibility complex class I-restricted cytotoxic T-lymphocyte recognition epitope of herpes simplex virus type 2 confers protective immunity. J Virol. 1998;72:9567–9574. doi: 10.1128/jvi.72.12.9567-9574.1998. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Shappell SB, Thomas GV, Roberts RL, Herbert R, Ittmann MM, Rubin MA, Humphrey PA, Sundberg JP, Rozengurt N, Barrios R, Ward JM, Cardiff RD. Prostate pathology of genetically engineered mice: definitions and classification. The consensus report from the Bar Harbor meeting of the Mouse Models of Human Cancer Consortium Prostate Pathology Committee. Cancer Res. 2004;64:2270–2305. doi: 10.1158/0008-5472.can-03-0946. [DOI] [PubMed] [Google Scholar]
- 15.Degl’Innocenti E, Grioni M, Boni A, Camporeale A, Bertilaccio MT, Freschi M, Monno A, Arcelloni C, Greenberg NM, Bellone M. Peripheral T cell tolerance occurs early during spontaneous prostate cancer development and can be rescued by dendritic cell immunization. Eur J Immunol. 2005;35:66–75. doi: 10.1002/eji.200425531. [DOI] [PubMed] [Google Scholar]
- 16.Grossmann ME, Davila T, Celis T. Avoiding tolerance against prostatic antigens with subdominant peptide epitopes. J Immunother (1997) 2001;24:237–241. [PubMed] [Google Scholar]
- 17.de Witte MA, Coccoris M, Wolkers MC, van den Boom MD, Mesman EM, Song JY, van der Valk M, Haanen JB, Schumacher TN. Targeting self-antigens through allogeneic TCR gene transfer. Blood. 2006;108:870–877. doi: 10.1182/blood-2005-08-009357. [DOI] [PubMed] [Google Scholar]
- 18.Haanen JB, Toebes M, Cordaro TA, Wolkers MC, Kruisbeek AM, Schumacher TN. Systemic T cell expansion during localized viral infection. Eur J Immunol. 1999;29:1168–1174. doi: 10.1002/(SICI)1521-4141(199904)29:04<1168::AID-IMMU1168>3.0.CO;2-J. [DOI] [PubMed] [Google Scholar]
- 19.Garcia-Hernandez Mde L, Gray A, Hubby B, Klinger OJ, Kast WM. Prostate stem cell antigen vaccination induces a long-term protective immune response against prostate cancer in the absence of autoimmunity. Cancer Res. 2008;68:861–869. doi: 10.1158/0008-5472.CAN-07-0445. [DOI] [PubMed] [Google Scholar]
- 20.Anderson MJ, Shafer-Weaver K, Greenberg NM, Hurwitz AA. Tolerization of tumor-specific T cells despite efficient initial priming in a primary murine model of prostate cancer. J Immunol. 2007;178:1268–1276. doi: 10.4049/jimmunol.178.3.1268. [DOI] [PubMed] [Google Scholar]
- 21.Mihalyo MA, Hagymasi AT, Slaiby AM, Nevius EE, Adler AJ. Dendritic cells program non-immunogenic prostate-specific T cell responses beginning at early stages of prostate tumorigenesis. Prostate. 2007;67:536–546. doi: 10.1002/pros.20549. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Degl’Innocenti E, Grioni M, Capuano G, Jachetti E, Freschi M, Bertilaccio MT, Hess-Michelini R, Doglioni C, Bellone M. Peripheral T-cell tolerance associated with prostate cancer is independent from CD4+CD25+ regulatory T cells. Cancer Res. 2008;68:292–300. doi: 10.1158/0008-5472.CAN-07-2429. [DOI] [PubMed] [Google Scholar]
- 23.Tseng-Rogenski SS, Arredouani MS, Neeley YC, Lu B, Chinnaiyan AM, Sanda MG. Fas-mediated T cell deletion potentiates tumor antigen-specific tolerance in a mouse model of prostate cancer. Cancer Immunol Immunother. 2008 doi: 10.1007/s00262-008-0471-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Kolb HJ, Schattenberg A, Goldman JM, Hertenstein B, Jacobsen N, Arcese W, Ljungman P, Ferrant A, Verdonck L, Niederwieser D, van Rhee F, Mittermueller J, de Witte T, Holler E, Ansari H. Graft-versus-leukemia effect of donor lymphocyte transfusions in marrow grafted patients. Blood. 1995;86:2041–2050. [PubMed] [Google Scholar]
- 25.Collins RH, Jr., Shpilberg O, Drobyski WR, Porter DL, Giralt S, Champlin R, Goodman SA, Wolff SN, Hu W, Verfaillie C, List A, Dalton W, Ognoskie N, Chetrit A, Antin JH, Nemunaitis J. Donor leukocyte infusions in 140 patients with relapsed malignancy after allogeneic bone marrow transplantation. J Clin Oncol. 1997;15:433–444. doi: 10.1200/JCO.1997.15.2.433. [DOI] [PubMed] [Google Scholar]
- 26.Dudley ME, Wunderlich JR, Robbins PF, Yang JC, Hwu P, Schwartzentruber DJ, Topalian SL, Sherry R, Restifo NP, Hubicki AM, Robinson MR, Raffeld M, Duray P, Seipp CA, Rogers-Freezer L, Morton KE, Mavroukakis SA, White DE, Rosenberg SA. Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science. 2002;298:850–854. doi: 10.1126/science.1076514. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Gattinoni L, Powell DJ, Jr., Rosenberg SA, Restifo NP. Adoptive immunotherapy for cancer: building on success. Nat Rev Immunol. 2006;6:383–393. doi: 10.1038/nri1842. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Yee C, Thompson JA, Byrd D, Riddell SR, Roche P, Celis E, Greenberg PD. Adoptive T cell therapy using antigen-specific CD8+ T cell clones for the treatment of patients with metastatic melanoma: in vivo persistence, migration, and antitumor effect of transferred T cells. Proc Natl Acad Sci U S A. 2002;99:16168–16173. doi: 10.1073/pnas.242600099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Schumacher TN. T-cell-receptor gene therapy. Nat Rev Immunol. 2002;2:512–519. doi: 10.1038/nri841. [DOI] [PubMed] [Google Scholar]
- 30.Morris EC, Tsallios A, Bendle GM, Xue S, Stauss HJ. A critical role of T cell antigen receptor-transduced MHC class I-restricted helper T cells in tumour protection. Proc Natl Acad Sci U S A. 2005;102:7934–7939. doi: 10.1073/pnas.0500357102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Xue S, Gao L, Hart D, Gillmore R, Qasim W, Thrasher A, Apperley J, Engels B, Uckert W, Morris E, Stauss H. Elimination of human leukemia cells in NOD/SCID mice by WT1-TCR gene-transduced human T cells. Blood. 2005;106:3062–3067. doi: 10.1182/blood-2005-01-0146. [DOI] [PubMed] [Google Scholar]
- 32.Morgan RA, Dudley ME, Wunderlich JR, Hughes MS, Yang JC, Sherry RM, Royal RE, Topalian SL, Kammula US, Restifo NP, Zheng Z, Nahvi A, de Vries CR, Rogers-Freezer LJ, Mavroukakis SA, Rosenberg SA. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science. 2006;314:126–129. doi: 10.1126/science.1129003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.van Hall T, van de Rhee NE, Schoenberger SP, Vierboom MP, Verreck FA, Melief CJ, Offringa R. Cryptic open reading frames in plasmid vector backbone sequences can provide highly immunogenic cytotoxic T-lymphocyte epitopes. Cancer Res. 1998;58:3087–3093. [PubMed] [Google Scholar]
- 34.Ochsenbein AF, Klenerman P, Karrer U, Ludewig B, Pericin M, Hengartner H, Zinkernagel RM. Immune surveillance against a solid tumor fails because of immunological ignorance. Proc Natl Acad Sci U S A. 1999;96:2233–2238. doi: 10.1073/pnas.96.5.2233. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Kuball J, Schmitz FW, Voss RH, Ferreira EA, Engel R, Guillaume P, Strand S, Romero P, Huber C, Sherman LA, Theobald M. Cooperation of human tumor-reactive CD4+ and CD8+ T cells after redirection of their specificity by a high-affinity p53A2.1-specific TCR. Immunity. 2005;22:117–129. doi: 10.1016/j.immuni.2004.12.005. [DOI] [PubMed] [Google Scholar]
- 36.Stanislawski T, Voss RH, Lotz C, Sadovnikova E, Willemsen RA, Kuball J, Ruppert T, Bolhuis RL, Melief CJ, Huber C, Stauss HJ, Theobald M. Circumventing tolerance to a human MDM2-derived tumor antigen by TCR gene transfer. Nat Immunol. 2001;2:962–970. doi: 10.1038/ni1001-962. [DOI] [PubMed] [Google Scholar]
- 37.Gattinoni L, Klebanoff CA, Palmer DC, Wrzesinski C, Kerstann K, Yu Z, Finkelstein SE, Theoret MR, Rosenberg SA, Restifo NP. Acquisition of full effector function in vitro paradoxically impairs the in vivo antitumor efficacy of adoptively transferred CD8+ T cells. J Clin Invest. 2005;115:1616–1626. doi: 10.1172/JCI24480. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Rocha B, Grandien A, Freitas AA. Anergy and exhaustion are independent mechanisms of peripheral T cell tolerance. J Exp Med. 1995;181:993–1003. doi: 10.1084/jem.181.3.993. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Richards J, Auger J, Peace D, Gale D, Michel J, Koons A, Haverty T, Zivin R, Jolliffe L, Bluestone JA. Phase I evaluation of humanized OKT3: toxicity and immunomodulatory effects of hOKT3gamma4. Cancer Res. 1999;59:2096–2101. [PubMed] [Google Scholar]
- 40.Lonberg N. Human antibodies from transgenic animals. Nat Biotechnol. 2005;23:1117–1125. doi: 10.1038/nbt1135. [DOI] [PubMed] [Google Scholar]
- 41.La Motte-Mohs RN, Herer E, Zuniga-Pflucker JC. Induction of T-cell development from human cord blood hematopoietic stem cells by Delta-like 1 in vitro. Blood. 2005;105:1431–1439. doi: 10.1182/blood-2004-04-1293. [DOI] [PubMed] [Google Scholar]
- 42.Zhao Y, Parkhurst MR, Zheng Z, Cohen CJ, Riley JP, Gattinoni L, Restifo NP, Rosenberg SA, Morgan RA. Extrathymic generation of tumor-specific T cells from genetically engineered human hematopoietic stem cells via Notch signaling. Cancer Res. 2007;67:2425–2429. doi: 10.1158/0008-5472.CAN-06-3977. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.van Lent AU, Nagasawa M, van Loenen MM, Schotte R, Schumacher TN, Heemskerk MH, Spits H, Legrand N. Functional human antigen-specific T cells produced in vitro using retroviral T cell receptor transfer into hematopoietic progenitors. J Immunol. 2007;179:4959–4968. doi: 10.4049/jimmunol.179.8.4959. [DOI] [PubMed] [Google Scholar]