Abstract
Aging is associated with an increased susceptibility to neurodegenerative disorders which has been linked to chronic inflammation. This process generates oxygen-reactive species, ultimately responsible for a process known as oxidative stress, leading to changes in nitric oxide (NO), and cyclic guanosine monophosphate (cyclic GMP) signaling pathway. In previous studies, we showed that human aging was associated with an increase in NO Synthase (NOS) activity, a decrease in basal cyclic GMP levels in human platelets, and an increase in thiobarbituric acid-reactant substances (TBARS) in erythrocytes. The aim of the present work was to evaluate NOS activity, TBARS and cyclic GMP levels in hippocampus and frontal cortex and its correlation to platelets and erythrocytes of 4-, 12-, and 24-month-old rats. The result showed an age-related decrease in cyclic GMP levels which was linked to an increase in NOS activity and TBARS in both central areas as well as in platelets and erythrocytes of rats. The present data confirmed our previous studies performed in human platelets and erythrocytes and validate NOS activity and cyclic GMP in human platelet as well as TBARS in erythrocytes as biomarkers to study age-related disorders and new anti-aging therapies.
Electronic supplementary material
The online version of this article (doi:10.1007/s11357-011-9365-7) contains supplementary material, which is available to authorized users.
Keywords: Nitric oxide, Aging, Cyclic GMP, TBARS, Peripheral markers
Introduction
Aging is the progressive accumulation of humoral, neural, and endocrine changes with time that are associated with or responsible for the ever-increasing susceptibility to disease and death which accompanies advancing senescence (Yu 1996). The nature of the aging process has been the subject of considerable speculation and there are many evidences suggesting that the sum of the deleterious free radical reactions going on continuously throughout the cells and tissues constitutes the aging process or is a major contributor to it (Harman 1981). According to the “free radical theory of aging”, proposed by Denham Harman in 1956 (Halliwell and Gutteridge 2007; Harman 1998), aging is a result of the accumulation of biomolecules damaged by free radicals, produced during normal metabolism, such as the superoxide anion (O•−2) and hydroxyl radical (OH•). These reactive species can cause oxidative damage to proteins, lipids, and nucleic acids, leading for example to lipid peroxidation and DNA mutations (Mamelak 2007; Valko et al. 2007).
It is believed that those changes can be more intense in neurodegenerative disorders, including Alzheimer’s disease (AD), Parkinson’s disease, and amyotrophic lateral sclerosis which have an age-related great incidence (Floyd 1999; Smith et al. 1991).
The most abundant source of reactive oxygen species (ROS) in the central nervous system (CNS) is the respiratory burst system of activated microglia. When the system is turned on, large amounts of O•−2 are generated on the microglial external membrane, from where they are released as a purposeful attack system. Nitric oxide (NO•) is synthesized from its precursor l-arginine by a highly regulated family of enzymes called NO synthases (NOS) that utilize O2 and NADPH as co-substrates and generate citrulline as co-product. Three isoforms of NOS (types 1–3) encoded by distinct genes have been identified. Two of these isoforms, NOS-1 and NOS-3, first identified in neurons and endothelial cells, respectively, are expressed constitutively. Both bind calmodulin in a reversible calcium-dependent manner and thus activities are stimulated by agonists that increase intracellular calcium. In contrast, NOS-2, originally identified in macrophages, is regulated by transcriptional induction and does not require calcium increases for activity, apparently because it has tightly bound calmodulin. All isoforms contain flavin adenine dinucleotide, flavin adenine mononucleotide, iron protoporphyrin IX, and tetrahydrobiopterin as prosthetic groups (for reviews, see (Knowles and Moncada 1994; Förstermann and Kleinert 1995; Nathan 1997).
NO• in the presence of O2•− forms peroxynitrite anion (ONOO−), which is quite unstable (T1/2 less than 1 s) leading to the formation of OH•, one of the responsibles for cellular death. NO• activates soluble guanylyl cyclase (sGC) with the formation of the second messenger cyclic GMP. Superoxide dismutase (SOD) is responsible for the dismutation of O2•− leading to hydrogen peroxide (H2O2) production, which can be eliminated as water (H2O) and O2 after the action of the enzymes catalase and glutathione peroxidase (GPx). In the presence of transition metals as iron (Fe2+) and copper (Cu+), OH• can also be formed through Fenton reaction (Lipton et al. 1993; Beckman and Koppenol 1996; Bolanos et al. 1997).
In previous studies, we showed an age-related increase in NOS activity and a decrease in cyclic GMP contents in platelets, and an increase in erythrocytes TBARS levels of healthy young and elderly subjects (Kawamoto et al. 2005). In addition, we have reported a basal age-related decline in cyclic GMP–PKG pathway in rat cerebellum (Kawamoto et al. 2007). However, the relationship between biochemical platelets and erythrocytes changes and impairments of oxidative stress, NOS enzyme activity and second messengers in CNS is still an open issue. The aim of the present work was to evaluate if age-related changes in NOS activity, and TBARS and cyclic GMP levels in hippocampus and frontal cortex are also present in platelets and erythrocytes of 4-, 12-, and 24-month-old rats.
Material and methods
Animal and tissue preparation
Four, 12- and 24-month-old male Wistar rats (Biomedical Sciences Institute, University of São Paulo) were kept under 12 h light/dark cycle (lights on at 7:00 A.M.) and allowed free access to food and water. All animals were euthanized by decapitation (between 9:00 and 11:00 AM) following procedure approved by the Biomedical College of Animal Experimentation (COBEA). All procedures were also approved by the Ethical Committee for Animal Research (CEEA) of the Biomedical Sciences Institute of the University of São Paulo. The brain was immediately removed and immersed in cold PBS. The frontal cortex and hippocampus were rapidly dissected, quickly immersed in liquid nitrogen, and stored at −80°C for later use.
Blood sampling and platelet preparation
Blood (5 mL) was drawn after each animal decapitation into citric acid dextrose anticoagulant solution (2.73% citric acid, 3.68% sodium citrate, 2% glucose). Platelet-rich plasma was isolated within 30 min after blood collection by centrifuging the blood at 394×g for 15 min. The plasma was then centrifuged at 1,500×g to obtain the platelet pellet. The pellet was washed twice in Krebs buffer (pH 6.0) containing (in millimolar): 140 NaCl, 5 KCl, 12 sodium citrate, 10 glucose, 12.5 sucrose and centrifuged at 1,500×g. All centrifugations were performed for 15 min at room temperature.
Preparation of erythrocytes membrane fragments
Erythrocytes membrane fragments were prepared according to a previously described method (Baba et al. 1999). Briefly, 5 mL of whole blood was collected in a glass tube containing sodium citrate, centrifuged at 394×g for 10 min and plasma and buffy coat were removed. Erythrocytes were washed with saline three times and then hemolyzed by addition of five volumes of distilled water. Hemolysate was centrifuged at 1,100×g for 5 min and clear red supernatant was discarded by decanting. The pink sediment, composed of membrane fragments, was resuspended at 4°C in erythrocyte buffer, containing (in millimolar): HEPES 2, NaCl 150, MgCl2 1, and EGTA 0.1 (pH 7.4) and centrifuged three times in 1,100×g (5, 10, and 15 min). The liquid was drained from the washed membrane fragments by placing the centrifuge tubes upside down.
TBARS determination in erythrocytes and brain samples
Thiobarbituric acid reacts with products of lipid peroxidation, mainly malondialdehyde, producing a colored compound. Lipid peroxidation in erythrocytes was determined through the production of TBARS, as previously described (Kawamoto et al. 2005). Briefly, 100 μL of 3% sodium dodecyl sulfate was thoroughly mixed to 100 μL of RBC. Then, 400 μL of 0.1 N HCl and 60 μL of 10% phosphotungstic acid were added. Mixture was centrifuged at 900×g for 15 min and supernatant was transferred to 200 μL of 0.7% 2-thiobarbituric acid. Reaction was incubated at 100°C for 30 min and TBARS were extracted into 1.5 mL of n-butanol. After a brief centrifugation, butanol layer fluorescence was measured spectrophotometrically at 535 nm, using an extinction coefficient of 1.56×105. Brain tissues were homogenized in saline buffer and precipitated proteins were removed by centrifugation at 12,000×g for 10 min. The supernatant was mixed with thiobarbituric acid (1% in NaOH 50 mm) and HCl 25%. The samples were then heated in a boiling water bath for 10 min and, after cooling, were extracted with 1.5 mL of butanol. The mixture was centrifuged at 12,000×g for 10 min and the absorbance of the supernatant was determined (Freitas et al. 2001).
NOS activity assay in platelets and brain samples
Tissue sample (frontal cortex or hippocampus) of each rat was individually homogenized in ice-cold 0.32 M sucrose/20 mM HEPES buffer (pH 7.4) containing 1 mM dithiothreitol (DTT) in an ice bath for 1 min using a Teflon homogenizer. Each homogenate was centrifuged at 10,000×g for 30 min at 4°C. The supernatant was passed through a Dowex AG 50 Wx-8 (Na+ form) column to remove the endogenous arginine. The arginine-free eluent was used to assay the NOS activity. The platelets were sonicated at 4°C in a buffer (pH 7.4; 20 mM HEPES, 0.32 M sucrose, 1 mM dithiothreitol, 10 μg/mL leupeptin, 1 mM EDTA, 1 mM pepstatin, 1 mM PMFS), after treatment with an ion-exchange resin (Dowex 50WX8-400, sodium form) to remove endogenous arginine, and this homogenate was used to assay NOS activity. NOS activity in frontal cortex, hippocampus and platelet from 4-, 12-, and 24-month-old rats was determined by enzymatic conversion of [3H]arginine to [3H]citrulline as described by (Mckee et al. 1994) with some modifications. Briefly, the NOS assay reaction medium of 200 μL, containing 100 mM HEPES, pH 7.4; 1 mM NADPH; 0.45 mM CaCl2; 1 μM l-[2,3-3H]-arginine (0.5 μCi), and 100 μL of hippocampus/frontal cortex cytosolic protein (0.2 μg/μL) or platelet homogenate (0.8 μg/μL). The reaction mixture was incubated for 30 min at 37°C and stopped by the addition of stop buffer containing 20 mM Hepes at pH 5.5. The entire reaction mixture was passed through a column packed with Na+ form of Dowex AG 50 Wx-8 resin. The flow through fraction containing [3H]-citrulline was counted for radioactivity using a Beckman 6000 liquid scintillation counter. The NOS activity was expressed as picomoles citrulline per milligram protein per minute. Samples of rat cerebellum were analyzed simultaneously as a positive control. Inhibition of the enzyme was evaluated in all tissues using N-nitro-l-arginine methyl ester hydrochloride (l-NAME, 10−6–10−4 M).
Measurement of cyclic GMP levels and platelets and brain samples
Cyclic GMP levels in the hippocampus, frontal cortex and platelets were determined in triplicate by using direct, competitive enzyme immunoassay kits (Stressgen, Enzo Life Sciences, Inc., USA). Hippocampi and frontal cortex were homogenized in 10 volumes of 0.1 M HCl and centrifuged at 2,500×g for 20 min at room temperature. The supernatant was acetylated to improve signal detection and samples were run in duplicate. The concentration of cyclic GMP is expressed as picomoles per milliliter. Platelets (3 × 108 platelets/mL) were incubated for 15 min at room temperature with theophylline (10 mM) and 3-isobuthylmethylxanthine (1 mM). For platelet disruption, 2 mL of ice-cold ethanol/HCl (1%) was added and mix was kept in ice for 30 min. Supernatant was obtained through centrifugation at 2,500×g for 20 min at 4°C. To assure total platelet disruption, 0.5 mL of ice-cold ethanol/HCl (1%) was added to the pellet, and centrifuged again under similar conditions. The two supernatants were put together and evaporated to dryness at 50°C under compressed air stream. Residue was resuspended in sodium acetate buffer (0.05 M) and stored at −20°C until analysis.
Chemicals and kits
L[2,3,4,5−3H]Arginine monohydrochloride (sp. act. 63.0 Ci/mmol) was purchased from Amersham International, Buckinghamshire, England. Cyclic GMP Enzyme Immunoassay kits were purchased from Enzo Life Sciences, Inc., USA. Resin Dowex AG50WX-8 (H+ form converted to Na+ form using 1 N NaOH), sucrose, HEPES, EDTA, DTT, CaCl2, calmodulin, FMN, FAD, NADPH, l-arginine, Tris–HCl, and l-NAME were purchased from Sigma Chemical Co., St. Louis, USA. Protein assay dye reagent from Bio-Rad Laboratories, CA, USA. All solutions were prepared immediately before use.
Statistics
The data, expressed as mean ± standard error of the mean were obtained from three independent experiments. In each experiment three replicate samples were quantified. Statistical comparisons were made by one-way ANOVA, followed by the Newman–Keuls test. All p values <0.05 were considered to reflect a statistically significant difference.
Results
Age-related NOS activity in hippocampus, frontal cortex, and platelets of rats
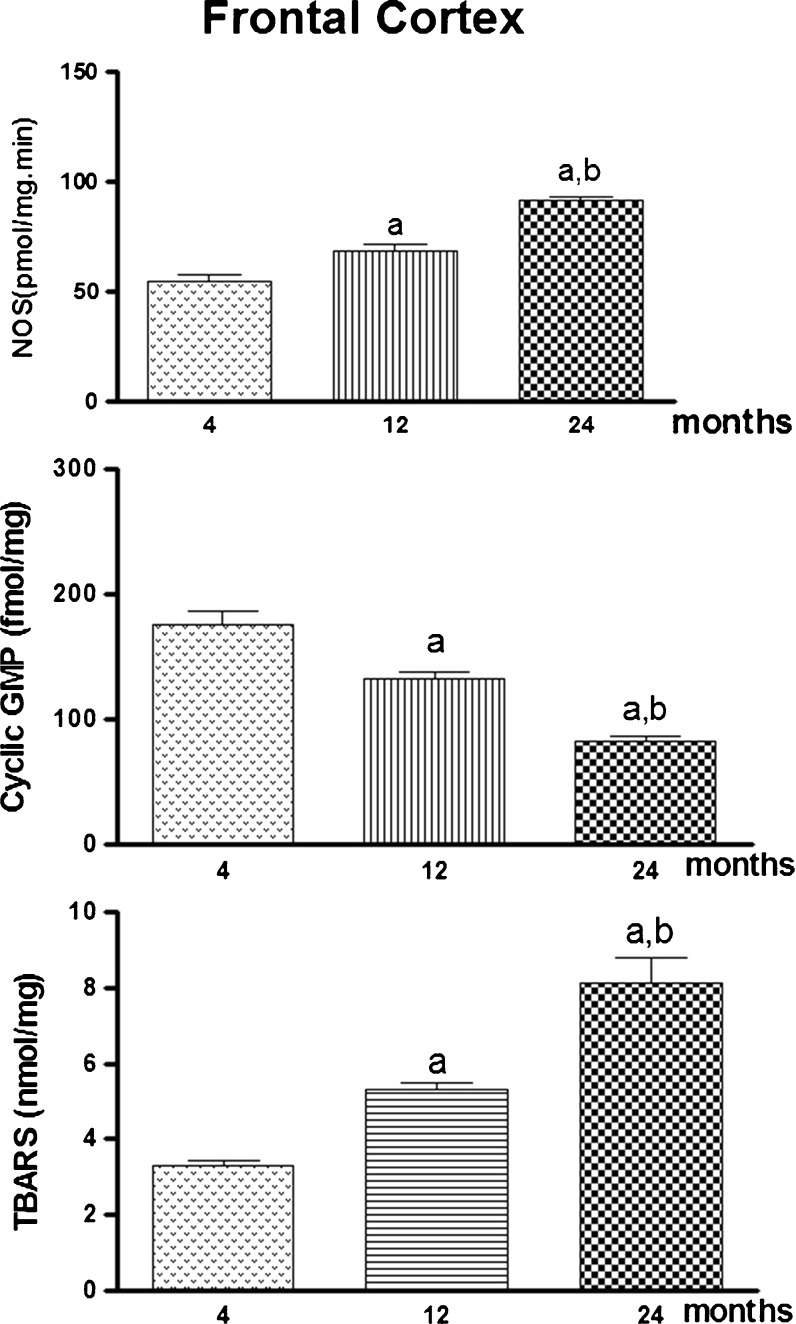
Aging induces a progressive increase of calcium-dependent NOS activity in frontal cortex. The NOS activity at 12 and 24 months is increased to 26.5% and 67.8% of the values detected at 4 months, respectively. In addition, the enzyme activity at 24 months is also increased (32.6%) when compared to the activity obtained in frontal cortex from 12-month-old animals (Fig. 1a) [F(2, 20) = 41.91, p < 0.001].
Fig. 1.
NOS activity, TBARS, and cyclic GMP levels in 4-, 12-, and 24-month-old rat frontal cortex. Values are the mean ± S.E.M. of three individual experiments. Statistical analysis: ANOVA followed by Newman–Keuls. a p < 0.05 vs. 4-month-old basal sample, b p < 0.05 vs. 12-month-old basal sample
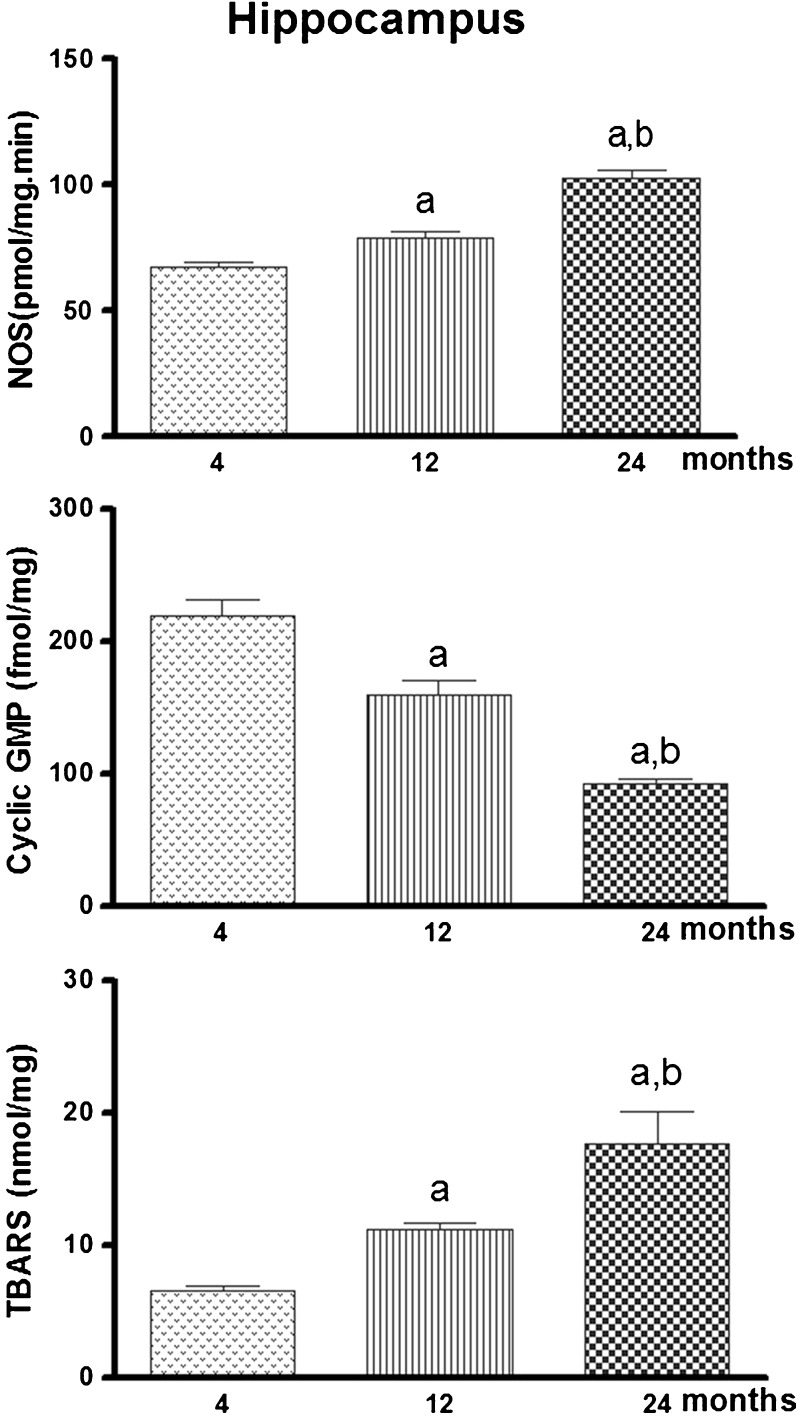
A similar result was observed in hippocampus as NOS activity increased to 16.8% at 12 months and 51.8% at 24 months of the basal values measured at 4 months. NOS activity at 24 months is also increased to 29.9% compared to values observed at 12 months (Fig. 2a) [F (2, 18) = 47.67, p < 0.001].
Fig. 2.
NOS activity, TBARS, and cyclic GMP levels in 4-, 12-, and 24-month-old rat hippocampus. Values are the mean ± S.E.M. of three individual experiments. Statistical analysis: ANOVA followed by Newman–Keuls. a p < 0.05 vs. 4-month-old basal sample, b p < 0.05 vs. 12-month-old basal sample
Regarding platelet samples, NOS activity in 24-month-old rat platelets also exhibited an age-related increase of 38.8% when compared to 12-month-old rat platelets and 121.4% when compared to platelets preparation from 4-month-old animals. The enzyme activity in platelets preparation from 12-month-old animals is also increased (59.5%) when compared tissue preparation from 4 months (Fig. 3) [F (2, 15) = 11.54, p < 0.001].
Fig. 3.
Platelet NOS activity and Cyclic GMP levels, and erythrocyte TBARS levels in 4-, 12-, and 24-month-old rats. Values are the mean ± S.E.M. of three individual experiments. Statistical analysis: ANOVA followed by Newman–Keuls. a p < 0.05 vs. 4-month-old basal sample, b p < 0.05 vs. 12-month-old basal sample
Age-related cyclic GMP content in hippocampus, frontal cortex, and platelets of rats
Changes in cyclic GMP content showed that aging is linked to progressive decrease in this second messenger in frontal cortex and hippocampus. The cyclic GMP levels at 12 and 24 months are decreased to 24.3% and 53.0% of the values detected at 4 months in frontal cortex. The cyclic GMP levels at 24 months is also decreased (38.0%) when compared to values obtained from samples of 12-month-old animals (Fig. 1b) [F(2, 20) = 30.54, p < 0.001].
Samples from rat hippocampus also showed that cyclic GMP levels decrease to 25.6% at 12 months and 57.0% at 24 months when compared to the basal values measured at 4-month-old animals. The enzyme activity at 24 months is also decreased (42.2%) when compared to values obtained at 12 months (Fig. 2b) [F (2, 17) = 40.78, p < 0.001].
Platelet cyclic GMP levels showed a similar result when compared to data obtained in brain tissues since cyclic GMP levels in 24-month-old rat platelets also exhibited a decrease of 37.5% and 12-month-old rat of 11.3% when compared to platelets preparation from 4-month-old animals. In addition, cyclic GMP levels at 24 months also decreased to 29.5% when compared to values obtained from platelets preparation of 12-month-old animals (Fig. 3) [F (2, 15) = 123.7, p < 0.001].
Age-related TBARS content in hippocampus, frontal cortex, and erythrocytes of rats
TBARS determinations showed that aging is linked to progressive increase in products of lipid peroxidation in frontal cortex and hippocampus. The TBARS levels at 12 and 24 months are increased to 60.6% and 145.4% of the values detected at 4 months in frontal cortex. The TBARS levels at 24 months are also increased (52.8%) when compared to values obtained from samples of 12-month-old animals (Fig. 1c) [F(2, 15) = 31.73, p < 0.001].
Samples from rat hippocampus also showed that TBARS levels increase to 69.6% at 12 months and 166.6% at 24 months when compared to the basal values measured at 4-month-old animals. TBARS levels at 24 months are also increased (57.1%) when compared to values obtained at 12 months (Fig. 2c) [F (2, 15) = 13.89, p < 0.001].
TBARS levels in erythrocytes showed similar results when compared to data obtained in brain tissues. In fact, TBARS levels in 12- and 24-month-old rat erythrocytes are increased to 59.2% and 121.4% respectively when compared to platelets preparation from 4-month-old animals. In addition, the increase in products of lipid peroxidation levels at 24 months is also increased to 38.8% when compared to values obtained from erythrocytes preparation of 12-month-old animals (Fig. 3c) [F (2, 15) = 27.97, p < 0.001].
Discussion
The study of peripheral biological samples in order to identify biomarkers either in aging or in neurodegenerative disorders could accelerate research on the etiology, pathophysiology, disease progression, and therapeutic development of many prevalent and devastating diseases. However, progress in the development and use of biomarkers for diseases of the central nervous system has been limited by a number of difficulties of development of reliable biomarkers for brain disorders. Biomarkers of aging are biochemical or physical properties in the human body which indicate that the body is aging. This is important to consider that a biological age is more indicative of healthy conditions than a chronological age since some people reach the age of 85 in a very good physical and mental condition while others have cognitive deficits and physical disturbances around 60. The present work showed an age-related correlation of platelet NOS activity and cyclic GMP levels, and erythrocyte TBARS levels with the same biochemical assays in hippocampus and frontal cortex of rats. These two structures are implicated in learning and memory and are related through a direct excitatory pathway (Fuster 1991; Férino et al. 1987; Swanson 1981).
The presence of toxins in the environment can cause damage to mitochondrial enzymes, leading to increased reactive oxygen species (Koutsilieri et al. 2002). Stimulation of this pathway during the life appears to play an important role in the induction of molecular changes that modify the cellular adaptive responses, leading to a decreased function of several systems (Sapolsky 1992; McCann et al. 1998). This ongoing process is the fundamental basis for the establishment of the aging process, so it is always associated with processes involving prolonged exposure to agents that induce some kind of toxicity.
During the aging process, mitochondrial oxidative phosphorylation becomes less efficient, and this probably contributes to an increase in the production of free radicals. The increase in O2•− production would lead to an accumulation of intracellular calcium and activation of calcium-dependent enzymes, like nitric oxide synthase, which is responsible for the formation of NO•. In fact, our data showed an age-related increase in NOS activity in frontal cortex, hippocampus, and in platelets of rats (Harman 1995; Harman 1998).
This increase in NOS activity in aging may be partly due to the reduction of Ca2+-ATPase, with consequent increase in intracellular concentration of this ion (Tanaka and Ando 1990; Hanahisa and Yamaguchi 2001). Several studies showed that NO• protector or deleterious effect is based on its redox status. NO• donors or synthesized endogenously after NMDA (N-methyl-d-aspartate) receptor activation, can lead to neurotoxicity (Harman 1998; Yu 1996).
NO•-mediated neurotoxicity is engendered, at least in part, by reaction with O•−2, apparently leading to formation of ONOO-, and not by NO• alone. However, if there is NO+ formation, NMDA receptor will be inhibited and a neuroprotective effect will appear. Therefore, NO behavior as a free radical or as an antioxidant agent will be dependent on O•−2 levels. If the concentration of this anion is high, NO will lead to lipid peroxidation, otherwise NO will have an antioxidant behavior (Wink et al. 1996). In fact, studies in rat cerebellum have showed no variation in the expression of NOS isoforms with aging, confirming that the increase in nitric oxide synthase activity is associated to oxidative status linked to aging process (Blanco et al. 2010; Siles et al. 2002).
Most of the neurodegenerative conditions are associated with a chronic inflammation. Although there is controversy whether inflammation is causative or a consequence of the disease process, it is now clear that it can greatly influence its pathogenesis (Floyd 1999; Teunissen et al. 2003). Even though aging and neurodegeneration share the same basic mechanisms, it is difficult to establish the limits between these two processes; there are mounting evidences that neurodegeneration might be an extension of the normal aging process, which might increase the susceptibility for neurotoxic events (Smith et al. 1991; Swerdlow 2007).
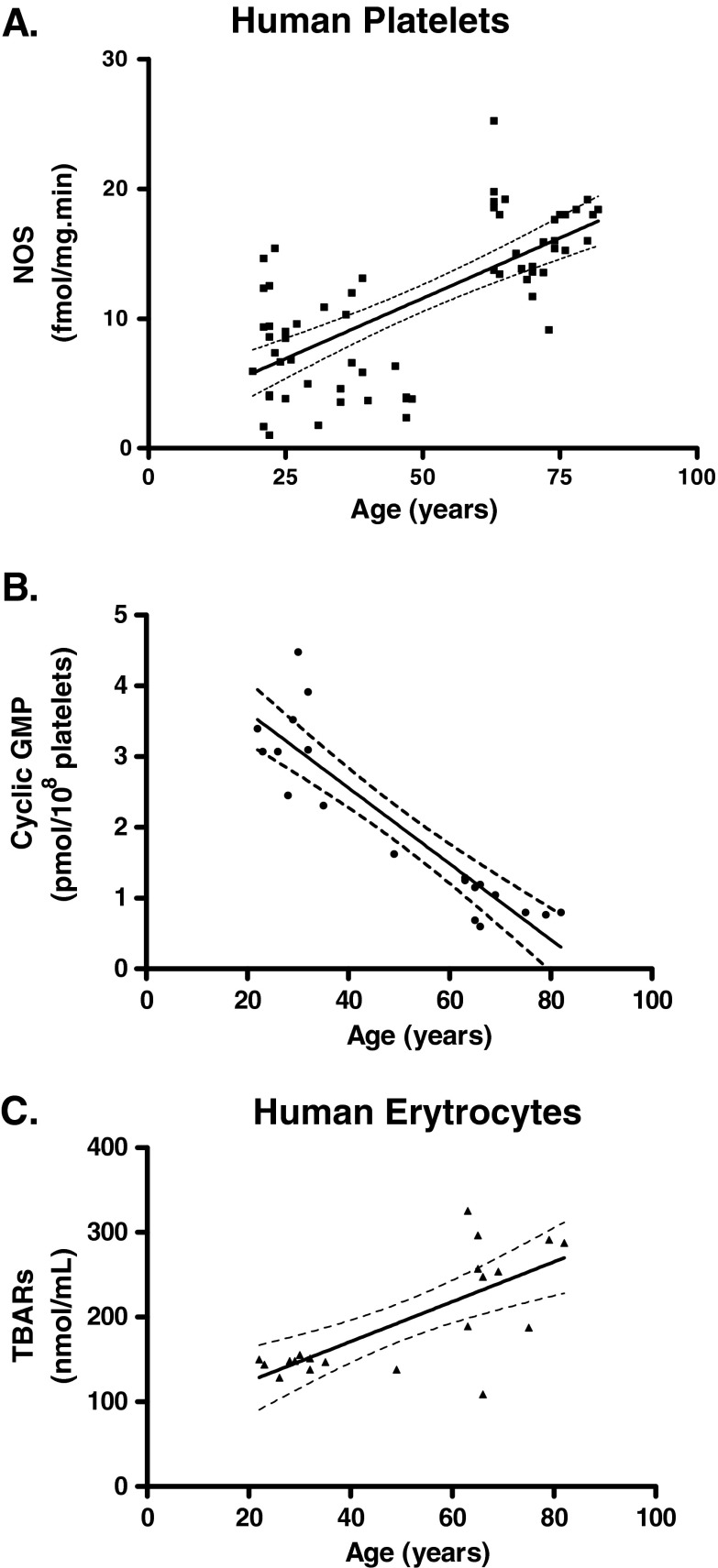
Although not a consensus (Ahlskog et al. 1995), the presence of increased oxidative stress at peripheral level in AD was evidenced in some studies. Kawamoto et al. (2005) detected in platelets and erythrocytes the involvement of ONOO− anion in aging and AD. Aging was associated to an increase in NOS activity, a decrease in basal cyclic GMP content as showed in the Fig. 4a and b. Data from these studied also showed an increase in TBARS (Fig. 4c) and no change in SOD and Na,K-ATPase activities. AD patients showed a higher level of TBARS and an increase in NOS, SOD, and Na,K-ATPase activities, without changes in cyclic GMP, when compared to aged controls. Na,K-ATPase is the enzyme responsible for the cell response to oxidative damage, as it maintains electrochemical sodium and potassium gradient. Its catalytic α subunit is sensitive to damage by free radicals and it has been described that ONOO− can cause cell membrane damage, which in turn leads to the disruption of Na,K-ATPase activity (Xie et al. 1995; Gloor 1997; Kim and Ko 1998). In addition, studies also showed that APOE e4 allele carriers has higher platelet NOS activity than non-carriers in AD patients when compared to aged controls (Marcourakis et al. 2008). The results presented by (Kawamoto et al. 2007) demonstrated a disruption in systemic modulation of oxidative stress in aging and with more intensity in AD and are consistent with the suggestion that neurodegeneration and aging could share a common pathogenic pathway.
Fig. 4.
Age-related NOS activity and Cyclic GMP levels in platelets, and human erythrocyte TBARS from young and aged human (data obtained from previous studies reported in Kawamoto et al. 2005). a Correlation and linear regression between values of NOS (in femtomoles per milligram per minute) activity from human platelets (n = 65). b Correlation and linear regression between values of cyclic GMP (picomoles per 108 platelets) levels from human platelets (n = 20). c Correlation and linear regression between values of TBARS (in femtomoles per milliliter) levels from human erythrocytes (n = 20). Analyses were performed based on Motulsky (1995) by using GraphPad Prism Software. NOS activity—Pearson correlation coefficient, r = 0.69; p < 0.001; linear regression, r 2 = 0.48, F = 59.7, p < 0.001. Cyclic GMP levels—Pearson correlation coefficient, r = 0.90; p < 0.001; linear regression, r 2 = 0.82, F = 84.7, p < 0.001. c TBARS levels—Pearson correlation coefficient, r = 0.73; p < 0.001; linear regression, r 2 = 0.52, F = 20.1, p < 0.001
Evidence suggests that part of the physiologic NO• effects occur mainly through stimulation of soluble GC, with a consequent increase in levels of cyclic GMP (Garthwaite 1991; Chiavegatto et al. 1998). The cyclic GMP, in turn, may act on ion channels or activate protein kinases (Garthwaite and Boulton 1995). Thus, the increased NOS activity of elderly people without dementia compared to healthy young people was not accompanied by a similar increase in the levels of intracellular cyclic GMP.
To evaluate cyclic GMP levels in rats in the present study, the interval between decapitation and experimental procedure was kept to <75 s, and testing of 4-, 12-, and 24-month-old animals were alternated. According to Steiner et al. (1972) levels of the nucleotide cyclic GMP in mouse brain are stable after 60 s of ischemia. Our data showed a similar age-related decrease in cyclic GMP contents in platelets as well as in hippocampus and frontal cortex of rats. These results also confirmed previous studies that showed an age-related reduction in the levels of cyclic GMP in the cerebral cortex, striatum, cerebellum, hippocampus, and hypothalamus of rats (Chalimoniuk and Strosznajder 1998; Puri and Volicer 1981; Schmidt and Thornberry 1978). These results also confirmed our previous evidences that showed a decrease in cyclic GMP levels and Na,K-ATPase activity in rat cerebellum (Scavone et al. 2005; Kawamoto et al. 2007).
These results therefore suggest that NO produced in excess in the elderly is not activating soluble GC, which may be due to the increase in ONOO− production. In fact, the present results showed that rat age-related increase in TBARS in hippocampus and frontal cortex also occurred in erythrocytes, confirming previous data obtained in human erythrocytes (Kawamoto et al. 2005). There is also evidence that excessive production of ONOO− may be responsible for the reduction in cyclic GMP levels by inactivation of the center iron and sulfur in proteins (Beckman and Koppenol 1996). Finally, we cannot rule out that an increase in phosphodiesterase (PDE) activity as responsible for the decrease in cyclic GMP content. In fact, aging process has been associated with an increase in PDE expression and activity and a decrease in cyclic GMP concentration (for review, see Domek-Łopacińska and Strosznajder 2010). This notion is in agreement with data indicating that inhibitors of PDE2 and PDE9 improve learning and memory in older rats (van der Staay et al. 2008) as well as in rat model of hepatic encephalopathy (Montoliu et al. 2010; Cauli et al. 2010).
In fact, studies performed in slices of rat cerebellum showed that incubation of slices preparation with sodium nitrate or carbon monoxide (CO) induced increases in the levels of cyclic GMP in the three age groups (Scavone et al. 2005). The same age-related response was also obtained in human platelets when incubated with NO donor (Kawamoto et al. 2005). Therefore, although there is a reduction in basal levels of cyclic GMP with time, stimulation of soluble GC by NO or CO remains unchanged suggesting that aging is affecting the modulation of the enzyme activity, instead of the total amount of protein.
The aberrant NO–cyclic GMP cascade is not only observed in neurodegenerative diseases, but in several other diseases states, such as hypertension, atherosclerosis, and diabetes which has been linked to cognitive deficits. Our data support that NO–sGC–cyclic GMP dysfunction can arise as a consequence of ROS-mediated decreases in NO bioavailability and an impairment of soluble GC activity through the oxidation of its prosthetic heme moiety. The relevance of impaired NO-dependent cyclic GMP production in aging process is unknown at present but it might predispose or potentiate an effect of specific factor(s) in the manifestation of age-related degenerative disorders.
Experimental data suggest that the hippocampal–prefrontal network can participate in the formation and consolidation of memories (Laroche et al. 1990; Dégenètais et al. 2003). Therefore, the similar changes observed in NOS activity and TBARS/cyclic GMP levels and the characteristics of the excitatory synaptic transmission in the hippocampal–prefrontal cortex pathway further supports the existence of a cooperative relationship between two structures known to be involved in higher cognitive processes. Taken together, the present data suggest that platelet NOS activity and cyclic GMP levels as well as erythrocytes TBARS are potential biomarkers that could be used to test anti-aging therapies and new compounds that affect NO–cyclic GMP signaling pathway in CNS.
Electronic supplementary material
(PDF 11.9 MB)
Acknowledgments
The authors thank Larissa de Sá Lima for technical support and Fernando Kok for his helpful comments. E.M.K. and A.E.B. are supported by postdoc fellowship from FAPESP; A.R.V and S.D. are Ph.D. student research fellowship from FAPESP and Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES), respectively, and L.S.L. is supported by grants from Universidade de São Paulo. Work in the laboratory of the authors was supported by FAPESP, CNPq and Neuroscience Research Support Centers from University of São Paulo (NAPNA). C.S. and T.M. are research fellows of CNPq. The authors report no biomedical financial interests or potential conflicts of interest.
References
- Ahlskog JE, Uitti RJ, Low PA, Tyce GM, Nickander KK, Peterson RC, Kokmen E. No evidence for systemic oxidant stress in Parkinson’s or Alzheimer’s disease. Mov Disord. 1995;10:566–573. doi: 10.1002/mds.870100507. [DOI] [PubMed] [Google Scholar]
- Baba A, Yoshikawa T, Mitamura H, Ogawa S (1999) Erythrocyte Naþ, Kþ-ATPase activity in patients with congestive heart failure. Int J Cardiol 69:117–125 [DOI] [PubMed]
- Beckman JS, Koppenol WH. Nitric oxide, superoxide and peroxynitrite: the good, the bad and ugly. Am J Physiol. 1996;271:C1424–C1437. doi: 10.1152/ajpcell.1996.271.5.C1424. [DOI] [PubMed] [Google Scholar]
- Blanco S, Molina FJ, Castro L, Del Moral ML, Hernandez R, Jimenez A, Rus A, Martinez-Lara E, Siles E, Peinado MA. Study of the nitric oxide system in the rat cerebellum during aging. BMC Neurosci. 2010;11(78 11):78–91. doi: 10.1186/1471-2202-11-78. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bolanos JP, Almeida A, Stewart V, Peuchen S, Land JM, Clark JB, Heales SJ. Nitric oxide-mediated mitochondrial damage in the brain: mechanisms and implications for neurodegenerative diseases. J Neurochem. 1997;68:2227–2240. doi: 10.1046/j.1471-4159.1997.68062227.x. [DOI] [PubMed] [Google Scholar]
- Cauli O, Rodrigo R, Llansola M, Montoliu C, Monfort P, Piedrafita B, el Mlili N, Boix J, Agustí A, Felipo V. Cyclic GMP pathways in hepatic encephalopathy. Neurological and therapeutic implications. Metab Brain Dis. 2010;1:69–80. doi: 10.1007/s11011-010-9184-z. [DOI] [PubMed] [Google Scholar]
- Chalimoniuk M, Strosznajder JB. Aging modulates nitric oxide synthesis and cGMP levels in hippocampus and cerebellum. Effects of amyloid beta peptide. Mol Chem Neuropathol. 1998;35(1–3):77–95. doi: 10.1007/BF02815117. [DOI] [PubMed] [Google Scholar]
- Chiavegatto S, Scavone C, Canteras NS. Nitric oxide synthase activity in the dorsal periaqueductal gray of rats expressing innate fear response. NeuroReport. 1998;9:571–576. doi: 10.1097/00001756-199803090-00002. [DOI] [PubMed] [Google Scholar]
- Dégenètais E, Thierry A-M, Glowinski J, Gioanni Y. Synaptic influence of hippocampus on pyramidal cells of the rat prefrontal cortex: an in vivo intracellular recording study. Cereb Cortex. 2003;13(7):782–792. doi: 10.1093/cercor/13.7.782. [DOI] [PubMed] [Google Scholar]
- Domek-Łopacińska KU, Strosznajder JB. Cyclic GMP and nitric oxide synthase in aging and Alzheimer’s disease. Mol Neurobiol. 2010;41(2–3):129–137. doi: 10.1007/s12035-010-8104-x. [DOI] [PubMed] [Google Scholar]
- Férino F, Thierry AM, Glowinski J. Anatomical and electrophysiological evidence for a direct projection from Ammon’s horn to the medial prefrontal cortex in the rat. Exp Brain Res. 1987;65:421–426. doi: 10.1007/BF00236315. [DOI] [PubMed] [Google Scholar]
- Floyd RA. Neuroinflammatory processes are important in neurodegenerative diseases: an hypothesis to explain the increased formation of reactive oxygen and nitrogen species as major factors involved in neurodegenerative disease development. Free Radic Biol Med. 1999;26:1346–1355. doi: 10.1016/S0891-5849(98)00293-7. [DOI] [PubMed] [Google Scholar]
- Förstermann U, Kleinert H. Nitric oxide synthase: expression and expressional control of the three isoforms. Naunyn Schmiedebergs Arch Pharmacol. 1995;352:351–364. doi: 10.1007/BF00172772. [DOI] [PubMed] [Google Scholar]
- Freitas JJ, Pompéia C, Miyasaka CK, Curi R (2001) Walker-256 tumor growth causes oxidative stress in rat brain. J Neurochem 77(2):655–663 [DOI] [PubMed]
- Fuster JM. The prefrontal cortex and its relation to behavior. Prog Brain Res. 1991;87:201–211. doi: 10.1016/S0079-6123(08)63053-8. [DOI] [PubMed] [Google Scholar]
- Garthwaite J. Glutamate, nitric oxide and cell-cell signaling in the nervous system. Trends Neurosci. 1991;14(2):60–67. doi: 10.1016/0166-2236(91)90022-M. [DOI] [PubMed] [Google Scholar]
- Garthwaite J, Boulton CL. Nitric oxide signaling in the central nervous system. Annu Rev Physiol. 1995;57:683–706. doi: 10.1146/annurev.ph.57.030195.003343. [DOI] [PubMed] [Google Scholar]
- Gloor SM. Relevance of Na, K-ATPase to local extracellular potassium homeostasis and modulation of synaptic transmission. FEBS Lett. 1997;412:1–4. doi: 10.1016/S0014-5793(97)00774-6. [DOI] [PubMed] [Google Scholar]
- Halliwell B, Gutteridge JMC. Free radical in Biology and Medicine., vol 4th. Free radical in Biology and Medicine. New York: Oxford University Press; 2007. [Google Scholar]
- Hanahisa Y, Yamaguchi M. Decrease in Ca2+-ATPase activity in the brain plasma membrane of rats with increasing age: involvement of brain calcium accumulation. Int J Mol Med. 2001;7(4):407–411. doi: 10.3892/ijmm.7.4.407. [DOI] [PubMed] [Google Scholar]
- Harman D. The aging process. Proc Natl Acad Sci U S A. 1981;78(11):7124–7128. doi: 10.1073/pnas.78.11.7124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Harman D. Free radical theory of aging: Alzheimer’s disease pathogenesis. Age. 1995;18:97–119. doi: 10.1007/BF02436085. [DOI] [Google Scholar]
- Harman D. Aging: phenomena and theories. Ann N Y Acad Sci. 1998;854:1–7. doi: 10.1111/j.1749-6632.1998.tb09886.x. [DOI] [PubMed] [Google Scholar]
- Kawamoto EM, Munhoz CD, Glezer I, Bahia VS, Caramelli P, Nitrini R, Gorjão R, Curi R, Scavone C, Marcourakis T. Oxidative stress in platelets and erythrocytes in aging and Alzheimer’s disease. Neurobiol Aging. 2005;26:857–864. doi: 10.1016/j.neurobiolaging.2004.08.011. [DOI] [PubMed] [Google Scholar]
- Kawamoto EM, Munhoz CD, Lepsch LB, De Sá Lima L, Markus RP, Marcourakis T, Scavone C. Age-related changes in cerebellar Phosphatase-1 and Na,K-ATPase activities. Neurobiol Aging. 2007;9:1149–1159. [Google Scholar]
- Kim WK, Ko KH. Potenciation of N-methyl-d-aspartate-mediated neurotoxicity by immunostimulated murine microglia. J Neurosci Res. 1998;54:17–26. doi: 10.1002/(SICI)1097-4547(19981001)54:1<17::AID-JNR3>3.0.CO;2-K. [DOI] [PubMed] [Google Scholar]
- Knowles RG, Moncada S. Nitric oxide synthases in mammals. Biochem J. 1994;298:249–258. doi: 10.1042/bj2980249. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Koutsilieri E, Scheller C, Grünblatt E, Nara K, Li J, Riederer P. Free radicals in Parkinson’s disease. J Neurol. 2002;249 249(Suppl 2):II/1–II/5. doi: 10.1007/s00415-002-1201-7. [DOI] [PubMed] [Google Scholar]
- Laroche S, Jay TM, Thierry AM. Long-term potentiation in the prefrontal cortex following stimulation of the hippocampal CA1/subicular region. Neurosci Lett. 1990;114:184–190. doi: 10.1016/0304-3940(90)90069-L. [DOI] [PubMed] [Google Scholar]
- Lipton SA, Choi YB, Pan ZH, Lei SZ, Chen HSV, Sucher NJ, Loscalzo J, Singel DJ, Stamler JS. A redox-based mechanism for the neuroprotective and neurodestructive effects of nitric oxide and related nitroso-compounds. Nature. 1993;364:626–632. doi: 10.1038/364626a0. [DOI] [PubMed] [Google Scholar]
- Mamelak M. Alzheimer’s disease, oxidative stress and gammahydroxybutyrate. Neurobiol Aging. 2007;28:1340–1360. doi: 10.1016/j.neurobiolaging.2006.06.008. [DOI] [PubMed] [Google Scholar]
- Marcourakis T, Bahia VS, Kawamoto EM, Munhoz CD, Gorjão R, Artes R, Kok F, Caramelli P, Nitrini R, Curi R, Scavone C. Apolipoprotein E genotype is related to nitric oxide production in platelets. Cell Biochem Funct. 2008;26(8):852–858. doi: 10.1002/cbf.1516. [DOI] [PubMed] [Google Scholar]
- McCann SM, Licinio J, Wong M-L, Yu WH, Karanth S, Rettorri V. The nitric oxide hypothesis of aging. Exp Gerontol. 1998;7(8):813–826. doi: 10.1016/S0531-5565(98)00050-3. [DOI] [PubMed] [Google Scholar]
- Mckee M, Scavone C, Nathanson JA. Nitric oxide, cGMP, and hormone regulation of active sodium transport. Proc Natl Acad Sci U S A. 1994;91(25):12056–12060. doi: 10.1073/pnas.91.25.12056. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Montoliu C, Rodrigo R, Monfort P, Llansola M, Cauli O, Boix J, Elmlili N, Agusti A, Felipo V. Cyclic GMP pathways in hepatic encephalopathy. Neurological and therapeutic implications. Metab Brain Dis. 2010;25(1):39–48. doi: 10.1007/s11011-010-9184-z. [DOI] [PubMed] [Google Scholar]
- Motulsky H, editor. Intuitive biostatistics. New York: Oxford University Press; 1995. [Google Scholar]
- Nathan C. Inducible nitric oxide synthase: what difference does it make? J Clin Invest. 1997;100:2417–2423. doi: 10.1172/JCI119782. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Puri SK, Volicer L. Age-related changes of cyclic nucleotide levels in rat brain regions. Mech Ageing Dev. 1981;15:239–242. doi: 10.1016/0047-6374(81)90132-9. [DOI] [PubMed] [Google Scholar]
- Sapolsky RM. Stress, the aging brain, and the mechanism of neuron death. Cambridge: MIT Press; 1992. [Google Scholar]
- Scavone C, Munhoz CD, Kawamoto EM, Glezer I, de Sá LL, Marcourakis T, Markus RP. Age-related changes in cyclic GMP and PKG-stimulated cerebellar Na, K-ATPase activity. Neurobiol Aging. 2005;26(6):907–916. doi: 10.1016/j.neurobiolaging.2004.08.013. [DOI] [PubMed] [Google Scholar]
- Schmidt MJ, Thornberry JF. Cyclic AMP and cyclic GMP accumulation in vitro in brain regions of young, old and aged rats. Brain Res. 1978;139:169–177. doi: 10.1016/0006-8993(78)90070-7. [DOI] [PubMed] [Google Scholar]
- Siles E, Martinez-Lara E, Canuelo A, Sanchez M, Hernandez R, Lopez-Ramos JC, Del Moral ML, Esteban FJ, Blanco S, Pedrosa JA, Rodrigo J, Peinado MA. Age related changes of the nitric oxide system in the rat brain. Brain Res. 2002;956:385–392. doi: 10.1016/S0006-8993(02)03575-8. [DOI] [PubMed] [Google Scholar]
- Smith CD, Carney JM, Starke-Reed PE, Oliver CN, Stadtman ER, Floyd RA, Markesbery WR. Excess brain protein oxidation and enzyme dysfunction in normal aging and in Alzheimer disease. Proc Natl Acad Sci U S A. 1991;88:10540–10543. doi: 10.1073/pnas.88.23.10540. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Steiner AL, Parker CW, Kipnis DM. Radioimmunoassay for cyclic nucleotides. J Biol Chem. 1972;247:1106. [PubMed] [Google Scholar]
- Swanson LW. A direct projection from Ammon’s horn to prefrontal cortex in the rat. Brain Res. 1981;217:150–154. doi: 10.1016/0006-8993(81)90192-X. [DOI] [PubMed] [Google Scholar]
- Swerdlow RH. Is aging part of Alzheimer’s disease, or is Alzheimer’s disease part of aging? Neurobiol Aging. 2007;28:1465–1480. doi: 10.1016/j.neurobiolaging.2006.06.021. [DOI] [PubMed] [Google Scholar]
- Tanaka Y, Ando S. Synaptic aging as revealed by changes in membrane potential and decreased activity of Na+, K+-ATPase. Brain Res. 1990;506:46–52. doi: 10.1016/0006-8993(90)91197-O. [DOI] [PubMed] [Google Scholar]
- Teunissen CE, Lütjohann D, von Bergmann K, Verhey F, Vreeling F, Wauters A, Bosmans E, Bosma H, van Boxtel MP, Maes M, Delanghe J, Blom HJ, Verbeek MM, Rieckmann P, De Bruijn C, Steinbusch HW, de Vente J. Combination of serum markers related to several mechanisms in Alzheimer’s disease. Neurobiol Aging. 2003;24:893–902. doi: 10.1016/S0197-4580(03)00005-8. [DOI] [PubMed] [Google Scholar]
- Valko M, Leibfritz D, Moncol J, Cronin MTD, Mazur M, Telser J. Free radicals and antioxidants in normal physiological functions and human disease. Int J Biochem Cell Biol. 2007;39:44–84. doi: 10.1016/j.biocel.2006.07.001. [DOI] [PubMed] [Google Scholar]
- van der Staay FJ, Rutten K, Barfacker L, Devry J, Erb C, Hea H. The novel selective PDE9 inhibitor BAY 73–6691 improves learning and memory in rodents. Neuropharmacology. 2008;55:908–918. doi: 10.1016/j.neuropharm.2008.07.005. [DOI] [PubMed] [Google Scholar]
- Wink DA, Cook JA, Pacelli REA. The effects of various nitric oxide-donor agents on hydrogen peroxide toxicity: a direct correlation between nitric oxide formation and protection. Arch Biochem Biophys. 1996;331:241–248. doi: 10.1006/abbi.1996.0304. [DOI] [PubMed] [Google Scholar]
- Xie Z, Jack-Hays M, Wang Y, Periyasamy SM, Blanco G, Huang WH, Askari A. Different oxidant sensitivities of the alpha 1 and alpha 2 isoforms of Na/K-ATPase expressed in baculovirus-infected insect cells. Biochem Biophys Res Commun. 1995;207:155–159. doi: 10.1006/bbrc.1995.1166. [DOI] [PubMed] [Google Scholar]
- Yu BP. Aging and oxidative stress: modulation by dietary restriction. Free Radic Biol Med. 1996;21:651–668. doi: 10.1016/0891-5849(96)00162-1. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
(PDF 11.9 MB)