Abstract
Neural abnormalities commonly associated with autism spectrum disorders include prefrontal cortex (PFC) dysfunction and cerebellar pathology in the form of Purkinje cell loss and cerebellar hypoplasia. It has been reported that loss of cerebellar Purkinje cells results in aberrant dopamine neurotransmission in the PFC which occurs via dysregulation of multisynaptic efferents from the cerebellum to the PFC. Using a mouse model we investigated the possibility that developmental cerebellar Purkinje cell loss could disrupt glutamatergic cerebellar projections to the PFC that ultimately modulate DA release. We measured glutamate release evoked by local electrical stimulation using fixed potential amperometry in combination with glutamate selective enzyme-based recording probes in urethane anesthetized Lurcher mutant and wildtype mice. Target sites included the medio-dorsal and ventro-lateral thalamic nuclei, reticulo-tegmental nuclei, pedunculopontine nuclei, and ventral tegmental area. With the exception of the ventral tegmental area, results indicated that in comparison to wildtype mice, evoked glutamate release was reduced in Lurcher mutants by between 9% to 72% at all stimulated sites. These results are consistent with the notion that developmental loss of cerebellar Purkinje cells drives reductions in evoked glutamate release in cerebellar efferent pathways that ultimately influence PFC dopamine release. Possible mechanisms whereby reductions in glutamate release could occur are discussed.
Keywords: Autism, Cerebellum, Dopamine, Glutamate, Fmr1 mice
Introduction
Autism Spectrum Disorders (ASD) are a group of neurodevelopmental disorders that are diagnosed in young children generally before the age of six (American Psychiatric Association, 2000). Individuals diagnosed within this spectrum exhibit deficits in social skills, communication, and repetitive behavior, as well as various cognitive abnormalities including deficits in executive function [1, 2]. Prevalence rates of ASD are rising, making it imperative that insights into the biological bases of these disorders are discovered [2, 3].
There are a number of strategies that can be employed in order to uncover the biological underpinnings of ASD. One strategy that we have used is to concentrate on well documented and consistent evidence of brain damage associated with ASD. Cerebellar neuropathology including cerebellar hypoplasia and reduced cerebellar Purkinje cell numbers are the most consistent neuropathologies linked to ASD, although not all ASD patients exhibit reductions in cerebellar Purkinje cells at autopsy which may partly be related to premortem conditions and methodological differences in histological staining [5–14]. Coupled to this cerebellar neuropathology, abnormalities in another late-developing structure, the frontal cortex have also been reported. Quantitative MRI of autistic children revealed increased volume of the frontal lobe, which was correlated with the degree of cerebellar abnormality [15]. Using stereological methods on postmortem tissue it has also been reported that autistic male children average 67% more neurons in the frontal lobe, in comparison to non-autistic, male controls [16]. As measured by PET, autistic children also show low medial prefrontal cortex (mPFC) dopaminergic activity compared to age and gender matched controls [17].
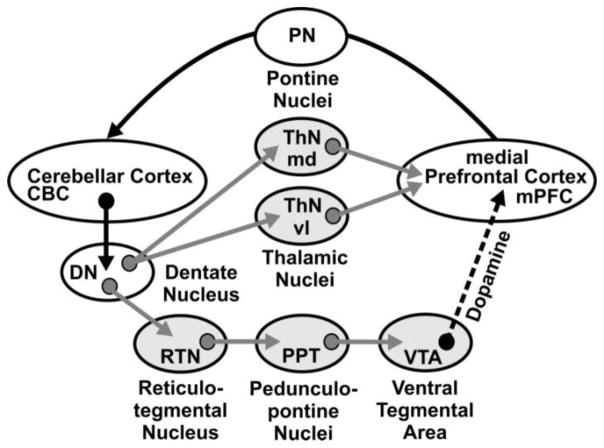
Using a mouse model we have investigated how developmental damage of the cerebellum influences the appearance of autism-like symptoms and cognitive deficits, as well as the neural mechanisms by which these could occur. Lurcher mutant (Lc+) mice have an autosomal dominant mutation that results in a nearly complete loss of cerebellar Purkinje cells between the 2nd and 4th weeks of life [18, 19]. Since these mice are ataxic we used non-ataxic chimeric mice (Lc/+↔+/+), which have a variable loss of Purkinje cells dependent upon the incorporation of the wildtype lineage, to examine the behavioral impact of cerebellar Purkinje cell loss [20]. We found that: (1) Chimeric mice with reduced numbers of cerebellar Purkinje cells show exaggerated repetitive behavior and deficits in executive function that are significantly, negatively correlated with the number of cerebellar Purkinje cells obtained from cell counts [21, 22]. These results directed us to the mPFC because the occurrence of repetitive behavior and deficits in executive function has been linked directly to frontal cortical function [23, 24]. (2) cerebellar output through the cerebellar dentate nucleus (DN) modulates dopamine (DA) release in the mPFC via two independent pathways [25]. As shown in Figure 1, both of these pathways originate in the cerebellar cortex and then project to the DN. The first involves indirect activation of mesocortical dopaminergic neurons in the ventral tegmental area (VTA) via contralateral glutamatergic projections of the DN to reticulotegmental nuclei (RTN) that, in turn, project to pedunculopontine nuclei (PPT) and then project to, and stimulate directly, VTA dopaminergic cell bodies projecting to the mPFC [26–29]. The second pathway involves activation of the contralateral glutamatergic projections of the DN to thalamic mediodorsal and ventrolateral nuclei (ThN md and ThN vl) that send glutamatergic efferents to the mPFC to modulate mesocortical dopaminergic terminal release in the mPFC via appositional excitatory glutamatergic synapses [30–33]. (3) In Lurcher mutant mice, we found that stimulating the cerebellar DN evokes mPFC DA release, although the DA response is significantly attenuated in comparison to Lurcher wildtype mice [25]. (4) In Lurcher wildtype mice, blocking glutamatergic transmission along either of these pathways reduced cerebellar dependent mPFC DA release by around 50% in each case, suggesting that the two pathways contribute equally and that they are primarily, if not entirely, glutamatergic [34]. (5) This 50% balance between the thalamic and VTA pathways in wildtype mice is altered in Lurcher mutants. In addition to the attenuation in cerebellar influence on the mPFC (point 3 above), there is a shift in the balance of influence of these pathways [35]. Thus, in Lurcher mutants the influence of the thalamic pathway is increased to 70% of the cerebellar signal while the VTA pathway is reduced to 30% of this signal. Considered together these findings suggest that cerebellar neuropathology in the form of Purkinje cell loss results in dysregulation of cerebellar neural circuitry modulating mPFC DA release, which can impinge on cognitive functions including repetitive behavior and executive function.
Figure 1.
Neuronal circuitry underlying cerebellar modulation of medial prefrontal cortex (mPFC) dopamine neurotransmission. Cerebellar modulation of dopamine release in the mPFC may occur via polysynaptic inputs from deep cerebellar nuclei, such as the dentate nucleus, to dopamine-containing cells in the ventral tegmental area or via a monosynaptic input to thalamic (md, mediodorsal; vl, ventrolateral) projections making close appositions with dopamine terminals in the mPFC. Glutamatergic pathways are shown as gray arrows and the dopaminergic pathway as a dashed arrow. Black curved arrow represents mPFC feedback to cerebellum via pontine nuclei. Gray ovals correspond to stimulation-evoked glutamate recording sites. Nuclei abbreviations are shown in the ovals
As projections from the DN to the thalamic nuclei and VTA are entirely glutamatergic it is reasonable that alterations in the functional properties of this neurotransmitter are driving the reductions in mPFC evoked dopamine release. Specifically, it is possible that only the first order projections from the DN to the RTN, and DN to ThN md and ThN vl are selectively affected, or alternatively, that there are generalized changes in glutamatergic responsiveness throughout both pathways that additionally encompass PPT and VTA. The purpose of this study was to distinguish between these possibilities. Thus, we evaluated glutamate release in RTP, PPT and VTA (VTA pathway) and ThN md and ThN vl (thalamic pathway) evoked by localized electrical stimulation using fixed potential amperometry in combination with glutamate enzyme-based recording probes in urethane anesthetized Lurcher wildtype and mutant mice in order to distinguish between these possibilities.
Methods
Animals
Experimental subjects were bred and maintained in the Animal Care Facility located in the Department of Psychology at the University of Memphis. Mice were continuously maintained in a temperature controlled environment (21±1°C) on a 12:12 light:dark cycle (lights on at 0800) and were given free access to food and water. Original Lurcher (#001046) breeders were purchased from The Jackson Laboratory (Bar Harbor, Maine). All experiments were approved by a local Institutional Animal Care and Use Committee and conducted in accordance with the National Institutes of Health Guidelines for the Care and Use of Laboratory Animals.
Breeding
To produce Lurcher mutant (Lc+) mice, ataxic male mice heterozygous for the Lurcher spontaneous mutation (B6CBACa Aw-J/A-Grid2Lc) were bred with non-ataxic female wildtype (WT) mice (B6CBACa Aw-J/A-Grid2+). This breeding strategy produced litters composed of both heterozygous mutant and WT mice. Due to their ataxic gait, mice heterozygous for the Lurcher mutation are easily distinguishable from their non-ataxic WT littermates.
Surgery
A total of 61 adult male Lc+ or WT mice were used. Six Lc+ and three WT mice were used for the assays in the ThN md, six Lc+ and six WT mice for the ThN vl, ten Lc+ and ten WT mice for the RTN, seven Lc+ and four WT mice for the VTA, and four Lc+ and five WT mice for the PPT. All were urethane anesthetized (1.5 g/kg i.p.) and placed in a stereotaxic frame. Body temperature was maintained at 36 ± 0.5°C with a temperature-regulated heating pad. Fixed potential amperometry (FPA) was used with a concentric bipolar stimulating electrode (SNE-100, Kopf Instruments) and a glutamate enzyme recording probe (model 7001, Pinnacle Technology), with an Ag/AgCl reference electrode component. In individual mice an electrode was implanted adjacent to the stimulating electrode in the left hemisphere using coordinates with respect to bregma and depth with respect to dura, in either the ThN md (AP −1.35, ML +0.4, and DV −2.75), ThN vl (AP −1.35, ML +1.0, and DV −3.45), RTN (AP −4.6, ML +.3, and DV −4.3), PPT (AP −4.7, ML +1.2, and DV −2.75), or the VTA (AP −3.3, ML +0.35, and DV −4.0). Figure 1 indicates the stimulation/recording sites.
Fixed potential amperometry and electrical stimulation
FPA coupled with glutamate enzyme-based recording probes has been shown to be a valid technique for real-time monitoring of stimulation-evoked glutamate release [36, 37]. Briefly, all glutamate recording probes were calibrated in a flow cell using glutamate solutions (10–400 μM) prior to insertion in the brain. A stock solution of L-glutamic acid (monosodium salt hydrate) and saline was freshly prepared prior to each probe calibration. Five separate concentration steps (10, 50, 100, 200, 400 μM) were injected sequentially through the flow cell over the recording probe. As in vivo, a fixed positive potential (+0.6 V) was applied to the recording probe and oxidation current was monitored continuously. Linear glutamate concentration-oxidation current correlation coefficients equal to or greater than 0.97 were deemed acceptable. Individual probe calibration values were used to establish glutamate concentrations recorded in vivo.
All recording sites were taken from [38]. A fixed positive potential (+0.6 V) was applied to the recording electrode and oxidation current was monitored continuously (10K samples/sec) by an electrometer filtered at 50 Hz. A total of 3 stimulations (100 monophasic 0.5 msec duration pulses at 100 Hz every 600 secs) were applied to the ThN md, ThN vl, RTN, PPT, or VTA (at 800 μAmps). As reviewed recently by [39], the spread of effective current is proportional to the square of the distance between the electrode tip and is highly dependent on the pulse duration and current–distance constant of neurons (low vs. high excitability threshold). Current–distance constants typically range from 100 μA mm2 to 4000 μA mm2 in brain tissue. Myelinated axons such as glutamatergic fibers exhibit a relatively high current–distance constant of 2000–4000 μA mm2 [40]. Thus, for high-threshold neurons (~3500 μA mm2), we estimate that 0.5 ms pulses at 800 μA would activate these neuronal elements ~0.6 mm from the electrode tip. Six hundred seconds after the final stimulation the glutamate probe was withdrawn from the brain and a bipolar stimulating electrode was introduced into the same location. A direct current (100 μA for 10 s) was passed through this electrode to lesion the stimulation/recording site.
Data Analysis
Based upon probe calibration, oxidation current following each of the three stimulations was converted to evoked glutamate concentration (micromoles) at 5 second intervals ranging from 0 to 240 seconds post-stimulation. The initial mixed model analysis of variance involved four factors. Between subjects factors included Site (ThN md, ThN vl, RTN, PPT and VTA) and Group (WT or Lc+), while Stimulation (1, 2, 3) and Time (0 to 240 seconds in 5 second intervals) were the within subjects factors. Results of this initial, omnibus ANOVA necessitated additional 3 factor ANOVAs restricted to each stimulation site. When appropriate, between group differences were further analyzed using simple main effects tests or Dunnett’s t-tests.
Results
Histology
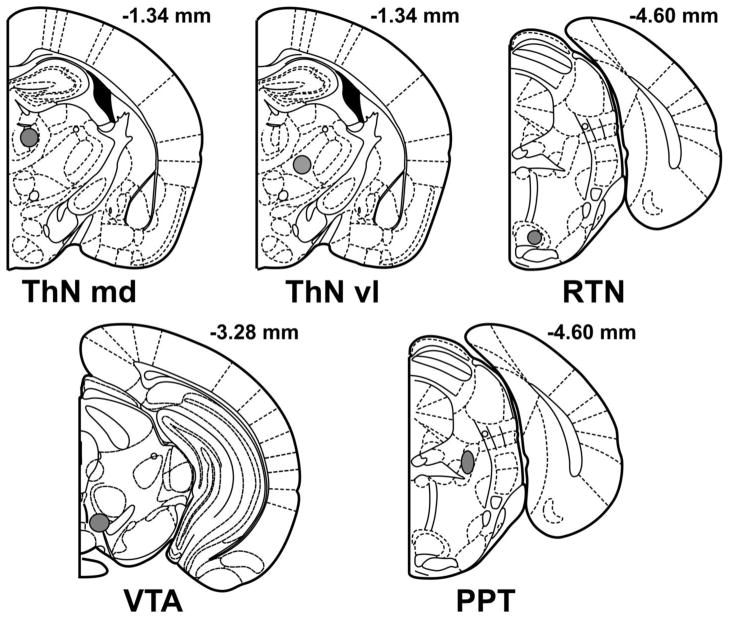
Immediately following each experiment each mouse was euthanized with a lethal intracardial injection of urethane. Brains were removed and preserved in 10 % buffered formalin containing 0.1 % potassium ferricyanide, and then stored in 30 % sucrose/10 % formalin until sectioning. The brains were sectioned on a cryostat at −30 °C. A Prussian blue spot indicative of the redox reaction of ferricyanide and iron deposits labeled the stimulating electrode tip in each stimulation/recording site. As shown in Figure 2, stimulation/recording sites were localized to the target sites. The ranges in localized histology were, in mm, (AP −1.22 to −1.46, ML .25 to .75, DV −2.5 to −3.25; AP −1.06 to −1.46, ML .75 to 1.25, DV −3.25 to −3.75; AP −4.48 to −4.72, ML .20 to .75, DV −4.0 to −4.6; AP −4.48 to −4.72, ML .75 to 1.25, DV −2.5 to −3.25; and AP −3.08 to −3.4, ML .2 to .6, DV −3.75 to −4.25) for the ThN md, ThN vl, RTN, PPT, and VTA respectively.
Figure 2.
Representative coronal sections in Lurcher (Lc+) and wildtype (WT) mice illustrating placements (gray shaded areas) of stimulation/recording electrodes in the mediodorsal nucleus of the thalamus (ThN md), ventrolateral nucleus of the thalamus (ThN vl), reticulotegmental nucleus (RTN), pedunculopontine nuclei (PPT), and ventral tegmental area (VTA). Numbers correspond to mm from bregma. Placements of stimulating/recording overlapped in all groups. Sections were adapted from the mouse atlas of Franklin and Paxinos, (2001).
Evoked Glutamate Release
Figure 3 shows the time course of stimulation-evoked glutamate release averaged across stimulations at the different sites. The omnibus ANOVA indicated that significant differences as occurred as a function of stimulation Site (Site: F=3.44, df=4,51, p<.02) and Group (Group: F=8.44, df=1,51, p=.005), and that group differences in the time course of evoked glutamate release occurred as a function of Site and Stimulation number (Site X Stimulation: F=1.97, df=384,4752, p<.001). Thus, each Site was subsequently analyzed separately. As shown in Figure 3, WT mice had significantly greater evoked glutamate release in the ThN md in comparison to Lc+ animals (Group X Time: F=15.4, df=48,336, p<.001). Dunnett’s t-tests further indicate that groups differed significantly between 5 and 90 seconds post-stimulation. A similar pattern was observed in response to electrical stimulation of the ThN vl (Group X Time: F=3.67, df=48,480, p<.001), although the significantly increased glutamate release in WT mice persisted for up to 100 seconds post-stimulation (Dunnett’s t-test). Lc+ and WT mice also differed significantly in evoked glutamate release in the RTN (Group X Time: F=5.06, df=48,864, p<.001), although this difference was shorter in duration and occurred from 5 to 70 seconds post-stimulation (Dunnett’s t-test). Group differences in evoked glutamate release were somewhat smaller in the PPT (Group X Time: F=2.29, df=48,336, p<.001) and were apparent between 10 and 45 seconds post-stimulation (Dunnett’s t-test). As shown in Figure 3, evoked glutamate release in WT and Lc+ mice was comparable following stimulation of the VTA (Group X Time: F=0.5, df=48,432, p=ns). Table 1 shows the micromolar evoked glutamate release averaged across 3 stimulations over the 240 second recording intervals at each recording site in WT and Lc+ mice. As can be seen in this table, Lc+ mice had the largest reductions in glutamate release in ThN md, ThN vl and RTN.
Figure 3.
The time-course of glutamate release evoked by electrical stimulation of the mediodorsal nucleus of the thalamus (ThN md), ventrolateral nucleus of the thalamus (ThN vl), reticulotegmental nucleus (RTN), pedunculopontine nuclei (PPT), or ventral tegmental area (VTA) in Lucher (Lc+) mutant mice or wildtype (WT) controls. A total of 3 stimulations (100 monophasic 0.5 msec duration pulses at 100 Hz every 600 secs) were applied to the ThN md, ThN vl, RTN, PPT, or VTA (at 800 μAmps). Results averaged across the 3 stimulations are shown. Vertical lines indicate the standard error of the mean.
Table 1.
Difference in evoked glutamate release in Lc+ and WT mice averaged across 3 stimulations*
| Stimulation Site | WT | Lc+ | %Change |
|---|---|---|---|
| ThN md | 129.7 | 51.0 | −60.7 |
| ThN vl | 220.5 | 62.8 | −71.5 |
| RTN | 223.6 | 151.8 | −32.1 |
| PPT | 109.0 | 99.0 | −9.2 |
| VTA | 72.6 | 65.1 | −10.3 |
micromolar values shown
Figure 4 shows the amount of evoked glutamate release for each of the 3 stimulations averaged over the 240 second post-stimulation recording interval. A number of different patterns of response were apparent over successive stimulations. The average amount of evoked glutamate release was maintained in WT and Lc+ animals following repeated electrical stimulations in the ThN md (Stimulation: F=0.54, df=2,14, p=ns), RTN (Stimulation: F=0.19, df=2,34, p=ns), or PPT (Stimulation: F=2.30, df=2,14, p=ns). In the ThN vl there was a group difference in evoked glutamate release (Group X Stimulation: F=3.95, df=2,19, p<.05). Simple main effects tests revealed that in WT mice, glutamate release increased significantly during the second and third stimulations in comparison to the first (Stimulation: F=4.67, df=2,10, p<.05). In contrast, in the ThN vl, glutamate release declined significantly across stimulations in Lc+ animals (F=4.41, df=2,9, p<.05). In the VTA there was a small but significant increase in evoked glutamate release across the 3 stimulations in both WT and Lc+ mice (Stimulation: F=3.97, df=2, 18, p<.05).
Figure 4.
Average glutamate release evoked by electrical stimulation of the mediodorsal nucleus of the thalamus (ThN md), ventrolateral nucleus of the thalamus (ThN vl), reticulotegmental nucleus (RTN), pedunculopontine nuclei (PPT), or ventral tegmental area (VTA) in Lucher (Lc+) mutant mice or wildtype (WT) controls. A total of 3 stimulations (100 monophasic 0.5 msec duration pulses at 100 Hz every 600 secs at 800 μAmps) were applied to each stimulation/recording site. Results of each stimulation are shown. Vertical lines indicate the standard error of the mean. * p<0.05 succesive stimulations vs. first stimulation in WT and Lc+ mice.
Discussion
The present results show that electrical stimulation of glutamatergic axons in the ThN md, ThN vl, RTN, and PPT of Lc+ mice resulted in significantly less evoked glutamate release than in WT control mice (Fig. 3). Evoked glutamate release was equivalent in the VTA of both genotypes. As such, these results are consistent with the idea that both first and second order glutamatergic projections from the DN are abnormal in Lc+ mice possessing developmental cerebellar neuropathology that involves loss of cerebellar Purkinje cells [18, 19]. It thus seems highly likely that it is this cerebellar neuropathology that drives the subsequent reduction in glutamate release observed in cerebellar efferents from the DN. As both pathways participate in the modulation of mPFC dopamine release, it appears reasonable that these reductions in glutamate release can account for the previously observed reduction in mPFC dopamine release elicited by electrical stimulation of the DN in Lc+, compared to WT, mice [25].
It is important to point out that the observed reductions in glutamate release in cerebellar efferent pathways could result from at least two different sources. As a function of loss of Purkinje cells in the cerebellar cortex and subsequent reductions in impulse traffic to the DN, it is possible that reductions in the population of glutamatergic efferents has occurred, which correspond to reductions in glutamate available for release. In support of this proposal, reductions in glutamate release have been shown to correlate with reductions in the numbers of activated glutamatergic neurons in vivo. The concentration of glutamate immunoreactivity and the concentration of glutamate neurons corresponded to associated glutamate evoked neuronal activity in studies of the visual cortex in monkeys [41] and cats [42]. In schizophrenia, another disorder where diverse symptomatology that has been suggested to result from developmental abnormalities in prefrontal cortico-cerebellar-thalamo-prefrontal cortical circuits [43], cerebellar abnormalities including reductions in cerebellar Purkinje cells have been observed [44,45]. Diffusion tensor imaging in schizophrenics has revealed reduced anistropic diffusion in connectivity between cerebellum and thalamus, which was interpreted as a loss of connectivity [46]. It seems reasonable that a reduction in the population of glutamatergic efferents from the DN to the thalamus, including the RTN and its projections to the PPT, could contribute to a loss in connectivity and drive. Indeed, quantitative morphological analysis of deep cerebellar nuclei have shown a 20% and 37% reduction in the number of principal and small neurons, respectively, in the DN of adult Lc+ mice as a result of secondary transneuronal degeneration brought on by the developmental loss of cerebellar Purkinje cells [47]. In addition, volumetric analysis has shown the loss of myelinated axons and boutons accounts for 59% of the atrophy of the DN in Lc+ mice, with the remaining 41% accounted for by a loss in nuclear neurons, dendritic arbors and reduced volume of glial processes, vascular elements, and intercellular space [48].
Alternatively, as a function of loss of Purkinje cells in the cerebellar cortex and subsequent reductions in impulse traffic to the DN, glutamatergic receptors and cellular machinery contributing to the processes of synthesis and release may be altered, resulting in a reduction in glutamatergic transmission and glutamate available for release. For example, autoradiography of glutamate receptor binding in adult Lc+ mice, compared to WT mice, has shown a significant decrease in ionotropic glutamatergic receptors in the DN, as well as in the thalamus, neostriatum, limbic regions, and cerebral cortical regions [49].
As shown in Fig. 5, glutamate can be generated in the mitochondria from glutamine by glutaminase 1 (Gls1 gene products) and then transported into presynaptic vesicles via transporters Vglut1/2 (Slc17a7 and Slc17a6 gene products) or further metabolized to α-ketoglutarate by glutamate dehydrogenase (Glud1 gene product) as part of cellular metabolism. During synaptic transmission, glutamate can bind to a number of ionotropic (NMDA and AMPA/kainate) and group I metabotropic (mGluR1/5) receptors in the postsynaptic cell, as well as group II (mGluR2/3) and group III (mGluR4, 6–8) metabotropic receptors in the presynaptic terminal. For instance, glutamate neurotransmission is inhibited by activation of group I and II metabotropic receptors resulting in a down-regulation of postsynaptic glutamate response or presynaptic glutamate release, respectively. In addition, glutamate is removed from the synaptic cleft by glial transporters EAAT1/Glt2 (Slc1a3 gene product) and EAAT2/GLAST (Slc1a2 gene product). In astrocytes, glutamate is converted to glutamine and transported out by SN1, where it can be taken up by neurons via GLNT and SAT2, and where it is converted back to glutamate by mitochondrial glutaminase (GLS1) in order to replenish the vesicular glutamate pool in the presynaptic terminal. Astrocytes also contain glutamate decarboxylase (GAD) that enzymatically converts glutamate to GABA [50]. Thus, a reduction in glutamate stores could arise from multiple intraneuronal or astrocytic metabolic pathways including an upregulation of astrocytic GAD activity. For example, [51] examined the anterior cingulate cortex and found that the protein levels of kidney-type glutaminase, but not those of the other enzymes, were significantly lower in subjects with autism compared to controls. In addition, using proton magnetic resonance spectroscopy in two brain regions implicated in ASD (the basal ganglia and prefrontal cortex), investigators have recently shown marked reductions in glutamate, and glutamine in autistic patients [52], Thus, it is conceivable that glutamate synthesis, and thus tissue content, may be diminished in astrocytes and/or glutamatergic terminals in first order and second order glutamatergic projections from the DN in Lc+ mice resulting in an overall reduction in stimulation-evoked glutamate release.
Figure 5.
Schematic representation of glutamate release at cerebellar synaptic junctions. Glutamate (glu) released from pre-synaptic glutamatergic neurons acts on post-synaptic and presynaptic neuronal metabotropic and ionotropic (NMDA and AMPA) receptors. See text for details. VGlut, vesicular glutamate transporter; mGluR, metabotropic glutamate receptors; AMPA, α-Amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid; NMDA, N-methyl-D-aspartate; EAAT, excitatory amino acid transporter; GAD, glutamate decarboxylase; GABA, γ-aminobutyric acid; SN1, glutamine transporter; SAT2, system amino acid transporter; GLNT, neutral amino acid transporter; GLS, glutaminase; GLUD1, glutamate dehydrogenase.
We suspect that mechanisms involving reductions in the population of glutamatergic efferents, as well as reductions in the processes governing synthesis and release are reflected in Lc+ mice. Specifically, in Lc+ mice in the ThN md, RTN and PPT we found clear evidence of reductions in evoked glutamate release that were maintained across successive stimulations. We believe this pattern of results is indicative of a reduction in the population of glutamatergic axons in these nuclei. In contrast, evoked glutamate release in Lc+ mice was lower than that of WT mice, and additionally declined significantly with repeated stimulation in the Thn vl. It seems reasonable that this pattern of change is additionally indicative of alterations in the processes contributing to synthesis and release as well as reduced numbers of glutamatergic axons projecting to this nucleus. It should be noted that relatively little is known about glutamatergic projections from the DN to thalamic and brainstem nuclei in Lc+ mice or ASD. Thus, further investigation of these possibilities is warranted.
Acknowledgments
This project was made possible by NINDS grant 1R01NS063009.
Footnotes
Conflicts of Interest: There are no conflicts of interest.
References
- 1.American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders-IV-TR. 4. Washington, D.C: American Psychiatric Association; 2000. [Google Scholar]
- 2.Ozonoff S, South M, Provencal S. Executive functions in autism: Theory and practice. In: Pérez JM, GonzálezPM MC, Comí MC, et al., editors. New Developments in Autism: The Future is Today. Philadelphia: Asociación de Padres de Personas con Autismo; 2007. pp. 185–213. [Google Scholar]
- 3.Centers for Disease Control and Prevention. Prevalence of autism spectrum disorders—Autism and Developmental Disabilities Monitoring Network, 14 sites, United States, 2002. MMWR. 2007;56(SS-1):12–28. [PubMed] [Google Scholar]
- 4.Rogers TD, McKimm E, Dickson PE, Goldowitz D, Blaha CD, Mittleman G. Is autism a disease of the cerebellum? An integration of clinical and pre-clinical research. Front Syst Neurosci. 2013b;7:1–16. doi: 10.3389/fnsys.2013.00015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Bauman ML. Microscopic neuroanatomic abnormalities in autism. Pediatrics. 1991;87:791–96. [PubMed] [Google Scholar]
- 6.Bolduc M, Du Plessis AJ, Sullivan N, Khwaja OS, Zhang X, Barnes K, et al. Spectrum of neurodevelopmental disabilities in children with cerebellar malformations. Dev Med Child Neurol. 2011;53:409–16. doi: 10.1111/j.1469-8749.2011.03929.x. [DOI] [PubMed] [Google Scholar]
- 7.Courchesne E. Brainstem, cerebellar and limbic neuroanatomical abnormalities in autism. Curr Opin Neurobiol. 1997;7:269–78. doi: 10.1016/s0959-4388(97)80016-5. [DOI] [PubMed] [Google Scholar]
- 8.Courchesne E, Townsend J, Akshoomoff NA, Saitoh O, Yeung-Courchesne R, Lincoln AJ, et al. Impairment in shifting attention in autistic and cerebellar patients. Behav Neurosci. 1994;108:848–65. doi: 10.1037//0735-7044.108.5.848. [DOI] [PubMed] [Google Scholar]
- 9.Courchesne E, Yeung-Courchesne R, Press GA, Hesselink JR, Jernigan TL. Hypoplasia of cerebellar vermal lobules VI and VII in autism. N Engl J Med. 1988;318:1349–54. doi: 10.1056/NEJM198805263182102. [DOI] [PubMed] [Google Scholar]
- 10.DiCicco-Bloom E, Lord C, Zwaigenbaum L, Courchesne E, Dager SR, Schmitz C, et al. The developmental neurobiology of autism spectrum disorder. J Neurosci. 2006;26:6897–906. doi: 10.1523/JNEUROSCI.1712-06.2006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Limperopoulos C, Chilingaryan G, Sullivan N, Guizard N, Robertson RL, du Plessis AJ. Injury to the Premature Cerebellum: Outcome is Related to Remote Cortical Development. Cereb Cortex. 2012 Nov 11; doi: 10.1093/cercor/bhs354. Epub ahead of print. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Palmen SJ, van Engeland H, Hof PR, Schmitz C. Neuropathological findings in autism. Brain. 2004;127:2572–83. doi: 10.1093/brain/awh287. [DOI] [PubMed] [Google Scholar]
- 13.Whitney ER, Kemper TL, Bauman ML, Rosene DL, Blatt GJ. Cerebellar Purkinje cells are reduced in a subpopulation of autistic brains: A stereologic experiment using calbindin-D28k. Cerebellum. 2008;7:406–416. doi: 10.1007/s12311-008-0043-y. [DOI] [PubMed] [Google Scholar]
- 14.Whitney ER, Kemper TL, Rosene DL, Bauman ML, Blatt GJ. Calbindin-D28k is a more reliable marker of human Purkinje cells than standard Nissl stains: a stereological experiment. J Neurosci Methods. 2008;168:42–7. doi: 10.1016/j.jneumeth.2007.09.009. [DOI] [PubMed] [Google Scholar]
- 15.Carper RA, Courchesne E. Inverse correlation between frontal lobe and cerebellum sizes in children with autism. Brain. 2000;123:836–44. doi: 10.1093/brain/123.4.836. [DOI] [PubMed] [Google Scholar]
- 16.Courchesne E, Mouton PR, Calhoun ME, Semendeferi K, Ahrens-Barbeau C, Hallet MJ, et al. Neuron number and size in prefrontal cortex of children with autism. JAMA. 2011;306:2001–10. doi: 10.1001/jama.2011.1638. [DOI] [PubMed] [Google Scholar]
- 17.Ernst M, Zametkin AJ, Matochik JA, Pascualvaca D, Cohen RM. Low medial prefrontal dopaminergic activity in autistic children. Lancet. 1997;350:638. doi: 10.1016/s0140-6736(05)63326-0. [DOI] [PubMed] [Google Scholar]
- 18.Caddy KW, Biscoe TJ. Structural and quantitative studies on the normal C3H and Lurcher mutant mouse. Philos Trans R Soc Lond B Biol Sci. 1979;287:167–201. doi: 10.1098/rstb.1979.0055. [DOI] [PubMed] [Google Scholar]
- 19.Zuo J, De Jager PL, Takahashi KA, Jiang W, Linden DJ, Heintz N. Neurodegeneration in Lurcher mice caused by mutation in delta2 glutamate receptor gene. Nature. 1997;388:769–73. doi: 10.1038/42009. [DOI] [PubMed] [Google Scholar]
- 20.Goldowitz D, Moran H, Wetts R. Mouse chimeras in the study of genetic and structural determinants of behavior. In: Goldowitz D, Wahlsten D, Wimer RE, editors. Techniques for the Genetic Analysis of Brain and Behavior: Focus on the Mouse. Amsterdam: Elsevier; 1992. pp. 271–90. [Google Scholar]
- 21.Dickson PE, Rogers TD, Del Mar N, Martin LA, Heck D, Blaha CD, et al. Behavioral flexibility in a mouse model of developmental cerebellar Purkinje cell loss. Neurobiol Learn Mem. 2010;94:220–28. doi: 10.1016/j.nlm.2010.05.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Martin LA, Goldowitz D, Mittleman G. Repetitive behavior and increased activity in mice with Purkinje cell loss: a model for understanding the role of cerebellar pathology in autism. Eur J Neurosci. 2010;31:544–55. doi: 10.1111/j.1460-9568.2009.07073.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Chudasama Y, Passetti F, Rhodes SE, Lopian D, Desai A, Robbins TW. Dissociable aspects of performance on the 5-choice serial reaction time task following lesions of the dorsal anterior cingulate, infralimbic and orbitofrontal cortex in the rat: differential effects on selectivity, impulsivity and compulsivity. Behav Brain Res. 2003;146:105–19. doi: 10.1016/j.bbr.2003.09.020. [DOI] [PubMed] [Google Scholar]
- 24.Robbins TW, Arnsten AF. The neuropsychopharmacology of fronto-executive function: monoaminergic modulation. Annu Rev Neurosci. 2009;32:267–87. doi: 10.1146/annurev.neuro.051508.135535. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Mittleman G, Goldowitz D, Heck DH, Blaha CD. Cerebellar modulation of frontal cortex dopamine release in mice: Relevance to autism and schizophrenia. Synapse. 2008;62:544–50. doi: 10.1002/syn.20525. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Schwarz C, Schmitz Y. Projection from the cerebellar lateral nucleus to precerebellar nuclei in the mossy fiber pathway is glutamatergic: A study combining anterograde tracing with immunogold labeling in the rat. J Comp Neurol. 1997;381:320–34. doi: 10.1002/(sici)1096-9861(19970512)381:3<320::aid-cne5>3.0.co;2-4. [DOI] [PubMed] [Google Scholar]
- 27.Vertes RP, Martin GF, Waltzer R. An autoradiographic analysis of ascending projections from the medullary reticular formation in the rat. Neuroscience. 1986;19:873–98. doi: 10.1016/0306-4522(86)90305-2. [DOI] [PubMed] [Google Scholar]
- 28.Oakman SA, Faris PL, Cozzari C, Hartman BK. Characterization of the extent of pontomesencephalic cholinergic neurons’ projections to the thalamus: comparison with projections to midbrain dopaminergic groups. Neuroscience. 1999;94:529–47. doi: 10.1016/s0306-4522(99)00307-3. [DOI] [PubMed] [Google Scholar]
- 29.Lavoie B, Parent A. Pedunculopontine nucleus in the squirrel monkey: distribution of cholinergic and monoaminergic neurons in the mesopontine tegmentum with evidence for the presence of glutamate in cholinergic neurons. Comp Neurol. 1994;344:190–209. doi: 10.1002/cne.903440203. [DOI] [PubMed] [Google Scholar]
- 30.Middleton FA, Strick PL. Basal ganglia and cerebellar loops: Motor and cognitive circuits. Brain Res Brain Res Rev. 2000;31:236–50. doi: 10.1016/s0165-0173(99)00040-5. [DOI] [PubMed] [Google Scholar]
- 31.Middleton FA, Strick PL. Cerebellar projections to the prefrontal cortex of the primate. J Neurosci. 2001;21:700–12. doi: 10.1523/JNEUROSCI.21-02-00700.2001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Pinto A, Jankowski M, Sesack SR. Projections from the paraventricular nucleus of the thalamus to the rat prefrontal cortex and nucleus accumbens shell: ultrastructural characteristics and spatial relationships with dopamine afferents. J Comp Neurol. 2003;459:142–55. doi: 10.1002/cne.10596. [DOI] [PubMed] [Google Scholar]
- 33.Pirot S, Jay TM, Glowinski J, Thierry AM. Anatomical and electrophysiological evidence for an excitatory amino acid pathway from the thalamic mediodorsal nucleus to the prefrontal cortex in the rat. Eur J Neurosci. 1994;6:1225–34. doi: 10.1111/j.1460-9568.1994.tb00621.x. [DOI] [PubMed] [Google Scholar]
- 34.Rogers TD, Dickson PE, Heck DH, Goldowitz D, Mittleman G, Blaha CD. Connecting the dots of the cerebro-cerebellar role in cognitive function: Neuronal pathways for cerebellar modulation of dopamine release in the prefrontal cortex. Synapse. 2011;65:1204–12. doi: 10.1002/syn.20960. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Rogers TD, Dickson PE, McKimm E, Heck D, Goldowitz D, Blaha C, et al. Developmental cerebellar damage in two mouse models: relevance to the neuropathology of autism. Cerebellum. 2013;12:547–56. doi: 10.1007/s12311-013-0462-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Agnesi F, Blaha CD, Lin J, Lee KH. Local glutamate release in the rat ventral lateral thalamus evoked by high-frequency stimulation. J Neural Eng. 2010;7:1–11. doi: 10.1088/1741-2560/7/2/026009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Agnesi F, Tye SJ, Bledsoe JM, Griessenauer CJ, Kimble CJ, Sieck GC, et al. Wireless instantaneous neurotransmitter concentration system-based amperometric detection of dopamine, adenosine, and glutamate for intraoperative neurochemical monitoring. J Neurosurgery. 2009;111:701–11. doi: 10.3171/2009.3.JNS0990. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Paxinos G, Franklin KBJ. The Mouse Brain in Stereotaxic Coordinates. 2. San Diego, CA: Academic Press; 2001. [Google Scholar]
- 39.Tehovnik EJ. Electrical stimulation of neural tissue to evoke behavioral responses. J Neurosci Methods. 1996;65:1–17. doi: 10.1016/0165-0270(95)00131-x. [DOI] [PubMed] [Google Scholar]
- 40.Yeomans JS, Maidment NT, Bunney BS. Excitability properties of medial forebrain bundle axons of A9 and A 10 dopamine cells. Brain Res. 1988;450:86–93. doi: 10.1016/0006-8993(88)91547-8. [DOI] [PubMed] [Google Scholar]
- 41.Carder RK, Hendry SH. Neuronal characterization, compartmental distribution, and activity-dependent regulation of glutamate immunoreactivity in adult monkey striate cortex. J Neurosci. 1994;14:242–62. doi: 10.1523/JNEUROSCI.14-01-00242.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Arckens L, Schweigart G, Qu Y, Wouters G, Pow DV, Vandesande F, Eysel UT, Orban GA. Cooperative changes in GABA, glutamate and activity levels: the missing link in cortical plasticity. Eur J Neurosci. 2000;12:4222–32. doi: 10.1046/j.0953-816x.2000.01328.x. [DOI] [PubMed] [Google Scholar]
- 43.Andreasen NC, Paradiso S, O’Leary DS. “Cognitive dysmetria” as an integrative theory of schizophrenia: A dysfunction in cortical-subcortical-cerebellar circuitry. Schizophr Bull. 1998;24:203–18. doi: 10.1093/oxfordjournals.schbul.a033321. [DOI] [PubMed] [Google Scholar]
- 44.Kyriakopoulos M, Vyas NS, Barker GJ, Chitnis XA, Frangou S. A diffusion tensor imaging study of white matter in early onset schizophrenia. Biol Psychiatry. 2008;63:519–23. doi: 10.1016/j.biopsych.2007.05.021. [DOI] [PubMed] [Google Scholar]
- 45.Maloku E, Covelo IR, Hanbauer I, Guidotti A, Kadriu B, Hu Q, Davis JM, Costa E. Lower number of cerebellar Purkinje neurons in psychosis is associated with reduced reelin expression. Proc Natl Acad Sci U S A. 2010;107:4407–11. doi: 10.1073/pnas.0914483107. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Magnotta VA, Adix ML, Caprahan A, Lim K, Gollub R, Andreasen NC. Investigating connectivity between the cerebellum and thalamus in schizophrenia using diffusion tensor tractography: a pilot study. Psychiatry Res. 2008;163:193–200. doi: 10.1016/j.pscychresns.2007.10.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Heckroth JA. Quantitative morphological analysis of the cerebellar nuclei in normal and lurcher mutant mice. I. Morphology and cell number. J Comp Neurol. 1994a;343:173–82. doi: 10.1002/cne.903430113. [DOI] [PubMed] [Google Scholar]
- 48.Heckroth JA. A quantitative morphological analysis of the cerebellar nuclei in normal and lurcher mutant mice. II. Volumetric changes in cytological components. J Comp Neurol. 1994b;343:183–92. doi: 10.1002/cne.903430114. [DOI] [PubMed] [Google Scholar]
- 49.Strazielle C, Lalonde R, Reader TA. Autoradiography of glutamate receptor binding in adult Lurcher mutant mice. J Neuropathol Exp Neurol. 2000;59:707–22. doi: 10.1093/jnen/59.8.707. [DOI] [PubMed] [Google Scholar]
- 50.Lee M, Schwab C, McGeer PL. Astrocytes are GABAergic cells that modulate microglial activity. Glia. 2011;59:152–165. doi: 10.1002/glia.21087. [DOI] [PubMed] [Google Scholar]
- 51.Shimmura C, Suzuki K, Iwata Y, Tsuchiya KJ, Ohno K, Matsuzaki H, et al. Enzymes in the glutamate-glutamine cycle in the anterior cingulate cortex in postmortem brain of subjects with autism. Mol Autism. 2013;4:6. doi: 10.1186/2040-2392-4-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Horder J, Lavender T, Mendez MA, O’Gorman R, Daly E, Craig MC, Lythgoe DJ, Barker GJ, Murphy DG. Reduced subcortical glutamate/glutamine in adults with autism spectrum disorders: a [1H]MRS study. Transl Psychiatry. 2013;3:e279. doi: 10.1038/tp.2013.53. [DOI] [PMC free article] [PubMed] [Google Scholar]