Abstract
Objective
The aim of this investigation was to study the feasibility of a randomised controlled trial (RCT) based on a multicentre fall prevention intervention including exercise with or without motivational interviewing compared to standard care in community-living people 75 years and older.
Method
The feasibility of a three-armed, randomised controlled trial was evaluated according to the following: process, resources, management by questionnaire, and treatment outcomes. The outcome measures were fall frequency, physical performance and falls self-efficacy evaluated after three months. Twelve physiotherapists conducted the measurements and treatments and responded to the questionnaire. The first 45 participants recruited to the ongoing RCT were included: 16 individuals in the Otago Exercise Program group (OEP), 16 individuals in the OEP combined with motivational interviewing group (MI), and 13 individuals in the control group. The study was conducted from November 2012 to December 2013.
Results
The feasibility of the study process, resources and management reached the set goals in most aspects; however, the set goal regarding the MI guide and planned exercise for the participating older people was not completely reached. No significant differences were found between the groups regarding the outcome measures.
Conclusion
This study confirmed the acceptable feasibility for the study protocol in the ongoing RCT.
Keywords: Exercise, Feasibility study, Motivational interviewing, Older adults, Community-living
Highlights
-
•
Feasibility in this study was sufficient and evaluated from the physiotherapist's perspective.
-
•
Motivational interviewing takes time to learn and implement in trials.
-
•
The physiotherapists were well motivated to perform the interventions.
Background
Over one-third of all people 65 years and older fall each year (Cotter et al., 2006), and approximately 10% of all falls result in serious physical injuries, half of which are fractures (Wijlhuizen, 2008). The number of falls and the associated costs are expected to increase with an increasing older population (Merom et al., 2012). The common individual consequences among older people after a fall are anxiety, fear of falling, loss of independence, and balance and strength impairments (Sipilä et al., 2011). A Cochrane review by Gillespie (Gillespie et al., 2012) showed that home-based exercise programs that include balance and strength-training exercises reduce falls and appear to reduce fractures in older people. Adherence to exercise programs increases, according to the elderly themselves, if the program is individually adapted, professionally guided and performed at home (Yardley et al., 2006).
The Otago exercise program (OEP), developed in New Zeeland, is a home-based exercise program including strength, balance and endurance training (Campbell et al., 2001). The program is individualised and progressive. A trained health professional gives instructions to the patient about the program during a home visit and makes regular follow-ups, either at home or by phone. The OEP has been shown to reduce falls, fall-related injuries and mortality in people 80 years and older (Thomas et al., 2010).
Regular physical activity can help reduce fall injuries in older persons (Chodzko-Zajko et al., 2009). In a systematic review of 53 studies (Fei et al., 2013), only two studies reported sufficient physical activity (150 min per week of moderate to high intensity activity) (Gómez et al., 2010, Hillsdon et al., 2008). A current challenge is to motivate older people to perform physical activity over time. It is important to increase the understanding of how intervention programs for the elderly should be presented to maximise the acceptance and participation and, at the same time, fit the recommendations (Yardley et al., 2006).
Motivational interviewing (MI) is a method used to initiate and support behaviour change, and it aims to help people detect and resolve their ambivalence about a behavioural change (Miller, 1983). A characteristic of MI is that the patient stimulates the motivation to change a behaviour; the therapist then uses a supportive approach to increase self-efficacy for the behavioural change process. Physical exercise, in combination with programs aiming to obtain behavioural change in the elderly, has rarely been evaluated, and there is a need to assess the feasibility of using exercise in the behavioural change process.
The aim of this study was to assess the feasibility of a multi-centre, fall prevention randomised controlled study (RCT) conducted in three Swedish municipalities and including either OEP, OEP combined with MI (onwards termed MI), or standard care (control group) for older people in the community by evaluating A) the study process, resources and management and B) the effects of the intervention programs on fall frequency, physical performance, balance and falls self-efficacy.
Method
The design of this study was a descriptive feasibility investigation of an RCT.
The Consolidated Standards of Reporting Trials - CONSORT checklist was used for reporting the RCT (Schulz et al., 2011).
Participants and recruitment
Twelve licenced physiotherapists (PTs) from three different municipalities in Sweden conducted the assessments and interventions within the RCT. Four PTs performed the measurements single blindly, and eight PTs administered the treatment, of which five PTs administered the OEP treatment and three administered the MI treatment.
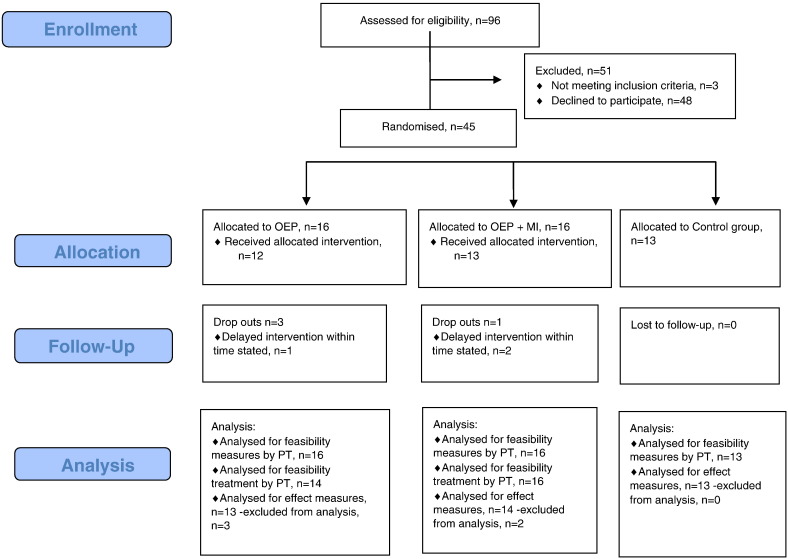
The participants were older community-living individuals seeking walking aid from health centres or seeking home care in a municipality that participated in the study (Table 1). Care managers, occupational therapists or physiotherapists in the three communities collaborated with the research team to recruit participants. Older individuals who fulfilled the inclusion criteria were invited to participate and were reported to the study leaders and then to the PTs. The eligibility criteria for study participation were as follows: being 75 years or older, being able to walk independently in their home and being able to understand written and oral information in the Swedish language. The exclusion criteria were as follows: a score less than 25 on the Mini Mental State Examination (MMSE), ongoing, regular physical therapy treatment due to injury and/or illness or being in terminal care. The study leaders contacted possible participants and patients who had given their consent, and those who met the study criteria were included and randomised by an independent PT. Forty-eight of the 96 eligible older people agreed to participate, but three of the 48 participants did not meet the criteria on the MMSE. Forty-five participants were included in the study: 16 individuals were randomised to the OEP group, 16 individuals were randomised to the MI group, and 13 were randomised to the control group (Fig. 1). There were no significant baseline differences between the three groups (Table 1). The median (min–max) age for the entire group was 83 years (75–96). The questionnaires for the feasibility procedure were analysed for all 45 participants for measurements and on 30 participants who were allocated to the treatment, OEP or MI groups. Each participant's flow through the trial is presented in Fig. 1. Three-month follow-ups were conducted for 40 participants.
Table 1.
Baseline characteristics.
| Total n = 45 | OEP n = 16 | MI n = 16 | Control n = 13 | Analysis p-value | |
|---|---|---|---|---|---|
| Age median (min–max) | 83.0 (75–103) | 82.0 (75–103) | 84.5 (77–92) | 81.0 (76–91) | .11 |
| Gender, (%) | .91 | ||||
| Female | 32 (71) | 12 (75) | 11 (69) | 9 (69) | |
| Male | 13 (29) | 4 (25) | 5 (31) | 4 (31) | |
| Education level | .55 | ||||
| Elementary school | 21 | 9 | 8 | 4 | |
| Secondary school/girl school | 6 | 2 | 4 | 4 | |
| High school/trade school | 7 | 2 | 4 | 1 | |
| University | 11 | 3 | 4 | ||
| Marital status | .85 | ||||
| Married | 19 | 8 | 5 | 6 | |
| Unmarried | 4 | 1 | 3 | 7 | |
| Widowed | 21 | 7 | 7 | ||
| Cohabitation | 1 | 1 | |||
| Falls during the past year | .60 | ||||
| No | 30 | 12 | 9 | 9 | |
| Yes, 1 time | 7 | 2 | 4 | 1 | |
| Yes, 2–3 times | 8 | 2 | 3 | 3 | |
| Walking aid | .20 | ||||
| No | 4 | 1 | 2 | 1 | |
| Yes | 21 | 15 | 14 | 12 | |
| Help in daily living | .29 | ||||
| No | 27 | 11 | 8 | 8 | |
| Yes from relatives/friends | 10 | 5 | 3 | 2 | |
| Yes from home help services/private firm | 8 | 5 | 3 | ||
| Activity level during the past six months | .09 | ||||
| Mostly sedentary | 13 | 3 | 7 | 3 | |
| Light physical effort | 27 | 12 | 9 | 6 | |
| More strenuous exercise 1–2 h/week | 5 | 1 | 4 | ||
| Health condition, median (min–max) | .99 | ||||
| EQ5DVAS scale (0–100) | 65.0 (35–90) | 70.0 (40–80) | 62.5 (40–90) | 60.0 (35–90) | |
OEP = Otago Exercise Program, MI = Motivational Interviewing.
Fig. 1.
Participant's flow through the trial1. 1CONSORT flow chart.
The main RCT was estimated to include 414 participants, and the present study was performed according to recommendations for feasibility studies with 30 or more participants (Lancaster et al., 2004).
Measurements
Feasibility was evaluated with close monitoring in the first three months of the main RCT.
A) Process, resources and management
Feasibility was measured using two questionnaires, one answered by all PTs conducting the measurements, and the other answered by all PTs conducting the treatment. The questions that referred to the MI treatment were only answered by the three PTs who administered this treatment. The questionnaires covered the following study areas: process, resource, and management of conducting the present RCT (Thabane et al., 2010). Process was defined as steps that needed to be considered to assess the feasibility of the process. Factors affecting data collection and how the study protocols worked were a part of the study procedure. Resources was defined as how much time the measurements and treatments required. Management covered environmental issues and management of the measurements and treatments.
The response options were rated on numeric rating scale (NRS) questions, 0 = lowest level and 10 = highest level, and dichotomous responses (yes/no or pos/neg). Most questions provided an opportunity to make comments in connection to the answers. One open-ended question about obstacles and advantages to performing the exercise in the home environment was presented in the questionnaire. A median rate of eight or more for each feasibility area (process, resource, management) for the NRS questions was decided as a limit for acceptable feasibility, and the corresponding limit for dichotomous responses was a positive rate of 80%.
B) Effect measures
Fall frequency was reported by all participants on a fall calendar, which was followed up by the PT every month. The current recommendations for reporting falls are daily reports from the older persons and a monthly report to the responsible practitioner (Lamb et al., 2005). All measurements were completed in the participant's home or at a health care centre formed by an independent PT who was blinded for group randomisation. Balance was measured by the Mini-BESTest, which includes 14 different tasks in four sub scales: anticipatory, reactive postural control, sensory orientation and dynamic gait. All tasks were graded 0–2 points, with a total maximum score of 28 points; zero indicated the lowest level of balance, and 2 indicated the highest level in each task (Franchignoni et al., 2010). The Mini-BESTest has a high test–retest reliability and inter-rater reliability (Tsang et al., 2013). Physical performance was measured using the Short Physical Performance Battery (SPPB), which evaluates lower extremity functioning, i.e., standing balance, gait speed, and repetitive chair stands in older persons (Guralnik et al., 1994), and is reported to be predictive for disability and risk of falls (Gawel et al., 2012). The tasks were graded on a 4-point scale, with a maximum score of 12 points and a minimum score of 0 points for the worst performance. The test has good test–retest reliability (Guralnik et al., 1994). Confidence in the participant's ability to perform various daily activities without falling was measured by the Falls Efficacy Scale Swedish version FES(S) (Hellström et al., 2003). The instrument had 13 items that were rated on a 0–10 scale, with a maximum total score of 130. For each item, 0 represented the lowest and 10 represented the highest level of self-efficacy. The test has high internal reliability (Nordell et al., 2009) and test–retest reliability (Hellström and Lindmark, 1999).
Randomisation
After baseline assessments were completed, the participants were randomised to one of the three groups. A predetermined randomisation list was made by an independent statistician. Randomisation was performed in blocks to minimise the risk of revealing treatment group membership, with a variable size of three, six, nine or twelve participants.
Intervention
All three groups received written recommendations for fall prevention, which is standard care. In the OEP and MI groups, the OEP program was performed and the exercises were supervised on five occasions during the first three months.
OEP group
The Otago Exercise Program (OEP) is a home-based exercise program designed to improve strength, balance and endurance. The exercise program should be individually tailored with a successively increasing level of difficulty. A walking program was given as a complement to the OEP. The PT adjusted the program individually to ensure that the exercise level was safe and intense enough for the participant according to the OEP protocol. The exercises were performed by the participants in their home three times per week, and walks were performed on the days when no exercises were performed. An exercise diary was reported in every month by the participant. The OEP instruction session was estimated to take one hour, and the exercises were estimated to take 30 min in total to complete and could be divided up during the day. All participants received ankle cuff weights, all according to the OEP (Thomas et al., 2010).
MI group
MI was used to stimulate autonomy and evoke motivation for behavioural change by strengthening the person in collaborative conversation about exercising according to the OEP. In the MI group, adjustments of exercises were made, not only according to the OEP protocol, but also in line with the participant's motivation to change. An MI guide including the MI processes of engagement, focusing, evoking and planning was used to guide the PTs during the conversation. “The engagement” referred to going in the same direction with the participant; and “the focusing” concerned finding out, together, what the collaboration was about, and this was a prerequisite for evoking motivation to change. “The planning” occurred after the first collaborative processes of engagement, focusing and evoking (Miller and Rollnick, 2013). Open-ended questions, affirmations, reflective listening and summaries, (OARS) (Miller and Rollnick, 1991) were included in the MI session. The instruction session was calculated to last approximately one hour and consisted of the OEP combined with MI.
Control group
The control group was given standard care.
Treatment fidelity
The PTs supervising the OEP program had meetings before the study began and during the study period to assure concordance on how the program was administered. Minor adjustments were made in agreement with all involved PTs. MI was adjusted in cooperation with guidance from an authorised Motivational Interviewing Network of Trainers (MINT) instructor during a three-day education session before the study began and at two follow-ups during the first year. All PTs who conducted the motivational interviews were experienced with the method before the study began. An MI guide was developed as support for the conversations with the participant. Every other MI conversation was recorded and discussed by the PTs during the meetings to secure MI quality.
Ethics
The study was approved by the Regional Ethics Committee in Uppsala, Dnr. 2012/147. The participants received no compensation for their participation.
Data-analyses
The questionnaires answered by the participating PTs were summarised using descriptive statistics, and the data were presented as frequencies, medians, min–max and percentages. Comments were categorised and calculated with the frequencies and summarised as descriptive text. Differences between groups were analysed using Fisher's exact test for nominal data and the Kruskal–Wallis test for ordinal data. Changes within the groups over time (pre–post) were analysed using the Wilcoxon signed rank test and effect size, ES, using the following formula: r = Z/√n. Differences between the groups over time were analysed using the General Linear Model, and repeated measures were analysed using Tukey's post hoc comparison. Statistical significance was set at p < 0.05, and data analysis was performed using IBM SPSS statistics 19.
Results
A) Process, resources and management
Process-measurements and treatment
Questions referring to how well the demographic questionnaire was filled in by the participants had a median (min–max) value of 9 (0–10), and there were comments concerning the participant's need for support to complete the questionnaire. Most tests, 82%, were conducted in the participant's home, and 87% of the tests were completed as planned. The physiotherapists rated adherence to the given instructions regarding the tests and measurements as high as 9 (7–10) (Table 2). Some comments revealed limitations when the tests were performed in the participant's home. The median rating on how well the OEP protocol worked was 9 (7–10), and that for the MI guide was 7 (5–10). There were comments regarding the OEP protocol, which was judged as being suitable and served its purpose. The PTs expressed criticism regarding the MI guide being limited. The PTs rated 90% of the participants' attitude to treatment as positive (Table 2).
Table 2.
Participating physiotherapist's ratings and answers regarding measurements (n = 4) and treatment (n = 8) feasibility.
| Questions for measurement's feasibility, n = 45 | Median (min–max) | Percentage |
|---|---|---|
| To what extent was the demographic questionnaire filled in? (scale 0–10) | 9 (0–10) | |
| Where were the tests performed? Home/public location? | 82/18 | |
| Did the physical tests work as planned? Yes/no | 87/13 | |
| How important did you think it was that the tests were carried out according to the instructions? (scale 0–10) | 9 (7–10) | |
| Resources | ||
| How long was the measurement session, in minutes? | 90 (60–90) | |
| Management | ||
| Did you have the right competence to perform the measurements? Yes/no | 100 | |
| How did you perceive your own motivation to perform the measurements? (scale 0–10) | 10 (5–10) | |
| Questions for treatment feasibility, n = 30 | Median (min–max) | Percentage |
| Process | ||
| How did you perceive the participants attitude towards the treatment? positive/negative | 90/10 | |
| How did the OEP protocol work? (scale 0–10) | 9 (7–10) | |
| For MI group only, n = 16 How well did the MI guide work? (scale 0–10) |
7 (5–10) | |
| Resources | ||
| How long was the treatment session in minutes? | 60 (30–90) | |
| Management | ||
| Did you have the right competence for the OEP? Yes/no | 100 | |
| How was your own motivation for the OEP? (scale 0–10) | 9 (6–10) | |
| Questions for MI group only, n = 16 | ||
| Did you have the right competence for the MI part of the treatment? Yes/no | 82/18 | |
| How was your own motivation for the MI part? (scale 0–10) | 10 (8–10) | |
| Was the exercise carried out as planned? Yes/no | 73/27 | |
| How well did the OEP work in the home environment? (scale 0–10) | 9 (8–10) | |
| How well did the individual adjustment of the OEP work? (scale 0–10) | 8 (4–10) | |
| Did the adherence of reporting the exercise diary work? Yes/no | 97/3 | |
| Where there any health risks during treatment? Yes/no | 0/100 | |
|
Obstacles/advantages to performing the intervention in the home environment? Four areas emerged: |
Prerequisite for participation, applicable, time, external factors | |
OEP = Otago Exercise Program, MI = Motivational interviewing
Resources and management — measurements and treatment
The median (min–max) time used for the measurements was 90 min (60–90), and that for the treatment was 60 min (30–90) (Table 2). The PTs performing the measurements rated their motivation as very high 10 (5–10), and their competence to perform the measurements was rated yes on 100% of the questionnaires (Table 2). Motivation for performing the OEP treatment was rated 9 (6–10), and that for the PTs performing the MI was rated 10 (8–10). Despite the highly rated motivation score for providing the MI intervention, the PTs requested more support in conducting the MI and several treatment sessions with the participants. The median rating for how well the OEP worked in the home environment was 9 (8–10), and that of the individual adjustment of the OEP was 8 (4–10). According to the PTs, the OEP program was easy to use in the home environment, and the individual adjustment of the OEP was easy to apply. The PTs valued their competence to perform the OEP as 100% and that for performing the MI as 82%. Comments on competence for the MI required more time and practice. Exercises that were performed as planned were rated as ‘yes’ in 73% of the questionnaires, and the comments addressing this included health-related issues, e.g., illness, pain and hospitalisation, lack of motivation and external factors, e.g., weather. The training diary was adequately reported to the PTs, and no health risks related to the treatment emerged.
Answers to the open-ended question about obstacles or advantages to performing exercises in the home environment noted exercising at home as an advantage for the target group and as a prerequisite for participation. The exercise instructions were easy to apply and understand for the participants in the environment where the exercises should be performed.
B) Effect measures
Falls
Eight participants reported one fall and two participants reported two falls. No differences between the groups were found regarding falls.
Balance
There were no significant differences in balance, measured by the Mini-BESTest, between the groups or within any of the three groups over time (Table 3).
Table 3.
Effect measures by time and within groups.
| Effect measures | Baseline median (min–max) | Three-month median (min–max) | p-value | Effect size (r) |
|---|---|---|---|---|
| Mini-BESTest score (0–28) | ||||
| OEP (n = 13) | 16.0 (5–26) | 18.0 (8–26) | 0.21 | 0.24 |
| MI (n = 14) | 19.0 (7–26) | 20.5 (7–26) | 0.33 | 0.19 |
| Control group (n = 13) | 18.0 (8–24) | 20.0 (12–24) | 0.49 | 0.14 |
| SPPB score (0–12) | ||||
| OEP (n = 13) | 8.0 (4–12) | 8.0 (2–12) | 0.91 | 0.02 |
| MI (n = 14) | 8.0 (3–12) | 9.0 (6–12) | 0.046 | 0.38 |
| Control group (n = 13) | 8.0 (3–12) | 10.0 (5–12) | 0.02 | 0.47 |
| FES score (0–130) | ||||
| OEP (n = 13) | 98.0 (62–130) | 107.0 (66–128) | 0.18 | 0.27 |
| MI (n = 14) | 97.5 (60–130) | 124.0 (91–130) | 0.02 | 0.45 |
| Control group (n = 13) | 110.0 (44–130) | 121.0 (70–130) | 0.15 | 0.28 |
SPPB = Short Physical Performance Battery, FES = Falls Efficacy Scale, OEP = Otago Exercise Program, MI = Motivational Interviewing.
Physical performance
No significant differences between the groups were observed over time. Within groups, the median (min–max) on the SPPB for the MI group was 8 (3–12) at baseline and 9 (6–12) at the three-month follow-up (p = 0.046, ES (r) = 0.38). Likewise, a significant improvement was observed in the control group from 8 (3–12) to 10 (5–12) (p = 0.02, ES (r) = 0.47); however, the corresponding difference in the OEP group was not significant (Table 3).
Falls efficacy scale
No significant differences between the groups were observed over time. Within groups, the median (min–max) fall-related self-efficacy for the MI group was 97.5 points (60–130) at baseline, and this value improved significantly (p = 0.02, ES (r) = 0.45) to 124 points (91–130) at the three-month follow-up. The corresponding differences in any of the two other groups were not significant (Table 3).
Discussion
In this study, feasibility was analysed from the physiotherapist's perspective, which is often overlooked in intervention studies. Conducting a multicentre study includes many factors that must be considered and covered thoroughly in the preparatory work. Meetings and preparations for the PTs were one of the important aspects and were contributors to collaboration between the three municipalities. The positive motivation and high competence among the PTs was also interpreted as strong predictors of positive results of the study. In most aspects, the results indicated acceptable feasibility; however, the MI guide and planned exercise did not fully meet the established goals.
At the beginning of the study, an MI guide was used but was found to be insufficient for the PTs performing the MI. Therefore, the guide will be improved and used as a support rather than as a guide to attain treatment fidelity further on in the RCT. The possibility of performing the exercises as planned did not fully meet the acceptable feasibility in this study.
Among older community-living people, upcoming, unexpected contextual factors and intrapersonal factors affected exercise performance. Obstacles to accomplishing the planned exercise included external factors and health-related issues. Responsible PTs, irrespective of the treatment group, were highly motivated to perform the treatment.
Before the study began, the research group had a three-day MI education session that was specifically designed for this study and was supported by a MINT instructor. Two follow-up sessions were conducted during this first year of the project. The PT's comments to their answers regarding competence and motivation to perform MI expressed the need of more support and rehearsal with a MINT instructor. However, the ratings of motivation to perform the MI were generally high, and the competence for MI was experienced as good. The specific challenges regarding the results from this study suggest adjustments to the motivational counselling by the PTs. Limited practice of MI could explain the need of support; however, all of the PTs had previous experience with MI. The use of a MI guide has both advantages and disadvantages. In a meta-analysis by Hettema, Steele and Miller, the authors concluded that a MI manual may not be effective and was not recommended (Hettema et al., 2005). The need for support when MI is used was also highlighted in a recent review by Schwalbe, Oh and Zweben. The authors recommended approximately three to four contacts over a six-month period to sustain MI skills after a workshop or similar provided rehearsal (Schwalbe et al., 2014). This finding indicates that our study protocol had limitations. The clinical implementation of the MI communication method was also discussed in a recent article by Miller and Rollnick, where the importance of obtaining treatment fidelity was highlighted (Miller and Rollnick, 2014). However, necessary steps will be taken to obtain treatment fidelity for the MI treatment in the ongoing RCT.
Outcome variables of falls frequency, balance and physical functions three months after randomisation were based on a small study sample. Nevertheless, small but significant differences were found for the SPPB both in the MI group and in the control group (p = 0.046, ES (r) = 0.38 and p = 0.02, r = 0.47); these findings indicate some changes in physical performance behaviour for these two groups. The FES(S) was only significantly improved over time in the MI group (p = 0.02, ES (r) = 0.45), which possibly reflects an important effect of MI treatment.
The possibility of performing exercises as planned, as viewed by the PTs, was still considered acceptable in this study due to upcoming life events of the participants, which cannot be controlled for in a study protocol. Some studies report adherence to exercise programs for falls prevention in the elderly to be as low as 10% (Day et al., 2002, Yardley et al., 2006). Adherence to exercises expected to be performed at home is often challenging (Campbell et al., 2001), and obedience to the treatment protocol is important in intervention studies. Furthermore, insufficient supervision and a drift from the treatment protocol can lead to low adherence (Sandborgh et al., 2010). However, this was not a problem in this study because the PTs thoroughly followed and registered the exercise protocols and participated in regular meetings during the study.
The improvement in the FES(S) and SPPB in the MI group supports the importance of MI as a factor by which physical activity behaviour might change (Emmons and Rollnick, 2001, Miller and Rollnick, 2002). However, improvement in the control group is a well-known phenomenon in intervention studies (Waters et al., 2012) due to the amount of assessment at baseline where the participants raise awareness of their physical ability. However, it must be emphasised that conclusions regarding the outcomes of this study are uncertain because of the limited study sample.
One strength of the study was that we captured feasibility from the PTs perspective and that we considered feasibility on the basis of process, resources and management. The two questionnaires that were used could be sources of error, as they were not psychometrically evaluated, and the authors are well aware of this limitation.
Conclusion
This study confirmed that the study protocol in a planned RCT had acceptable feasibility. In most aspects, the results indicated acceptable feasibility. However, the MI guide and adherence to planned exercises did not quite meet the goals of the study. Our research program needs to be improved in those areas.
Conflict of interest
The authors declare that there are no conflicts of interest.
Acknowledgments
We acknowledge the support of the MINT trainers Staffan Hultgren and Lena Lindhe Söderlund for providing the MI rehearsal for the PTs in the study.
References
- Campbell R., Evans M., Donovan J.L., Tucker M., Quilty B., Dieppe P. Why don't patients do their exercises? Understanding non-compliance with physiotherapy in patients with osteoarthritis of the knee. J. Epidemiol. Community Health. 2001;55(2):132–138. doi: 10.1136/jech.55.2.132. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chodzko-Zajko W.J., Proctor D.N., Fiatarone Singh M.A., Minson C.T., Nigg C.R., Salem G.J., Skinner J.S. American College of Sports Medicine position stand. Exercise and physical activity for older adults. Med. Sci. Sports Exerc. 2009;41(7) doi: 10.1249/MSS.0b013e3181a0c95c. [DOI] [PubMed] [Google Scholar]
- Cotter P.E., Timmons S., O'Connor M., Twomey C., O'Mahony D. The financial implications of falls in older people for an acute hospital. Ir. J. Med. Sci. 2006;175(2):11–13. doi: 10.1007/BF03167941. [DOI] [PubMed] [Google Scholar]
- Day L., Fildes B., Fitzharris M., Gordon I., Flamer H., Lord S. Randomised factorial trial of falls prevention among older people living in their own homes. Br. Med. J. 2002;325(7356):128–131. doi: 10.1136/bmj.325.7356.128. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Emmons K.M., Rollnick S. Motivational interviewing in health care settings: opportunities and limitations. Am. J. Prev. Med. 2001;20(1):68–74. doi: 10.1016/s0749-3797(00)00254-3. [DOI] [PubMed] [Google Scholar]
- Fei S., Norman I.J., While A.E. Physical activity in older people: a systematic review. BMC Public Health. 2013;13(1):1–17. doi: 10.1186/1471-2458-13-449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Franchignoni F., Horak F., Godi M., Nardone A., Giordano A. Using psychometric techniques to improve the Balance Evaluation Systems Test: the mini-BESTest. J. Rehabil. Med. (Stiftelsen Rehabiliteringsinformation) 2010;42(4):323–331. doi: 10.2340/16501977-0537. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gawel J., Vengrow D., Collins J., Brown S., Buchanan A., Cook C. The short physical performance battery as a predictor for long term disability or institutionalization in the community dwelling population aged 65 years old or older. Phys. Ther. Rev. 2012;17(1):37–44. [Google Scholar]
- Gillespie L.D., Robertson M.C., Gillespie W.J., Sherrington C., Gates S., Clemson L.M., Lamb S.E. Interventions for preventing falls in older people living in the community. Cochrane Database Syst. Rev. 2012;9 doi: 10.1002/14651858.CD007146.pub3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gómez L.F., Parra D.C., Moreno J., Brownson R.C., Buchner D., Sarmiento O.L., Lobelo F. Built environment attributes and walking patterns among the elderly population in Bogotá. Am. J. Prev. Med. 2010;38(6):592–599. doi: 10.1016/j.amepre.2010.02.005. [DOI] [PubMed] [Google Scholar]
- Guralnik J.M., Simonsick E.M., Ferrucci L., Glynn R.J., Berkman L.F., Blazer D.G., Wallace R.B. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J. Gerontol. 1994;49(2):M85–M94. doi: 10.1093/geronj/49.2.m85. [DOI] [PubMed] [Google Scholar]
- Hellström K., Lindmark B. Fear of falling in patients with stroke: a reliability study. Clin. Rehabil. 1999;13(6):509–517. doi: 10.1191/026921599677784567. [DOI] [PubMed] [Google Scholar]
- Hellström K., Fugl-Meyer A.R., Lindmark B., Wahlberg B. Self-efficacy in relation to impairments and activities of daily living disability in elderly patients with stroke: a prospective investigation. J. Rehabil. Med. 2003;35(5):202–207. doi: 10.1080/16501970310000836. [DOI] [PubMed] [Google Scholar]
- Hettema J., Steele J., Miller W.R. Motivational interviewing. Annu. Rev. Clin. Psychol. 2005;1(1):91. doi: 10.1146/annurev.clinpsy.1.102803.143833. [DOI] [PubMed] [Google Scholar]
- Hillsdon M., Lawlor D.A., Ebrahim S., Morris J.N. 2008. Evidence-based Policy and Practice: Physical Activity in Older Women: Associations with Area Deprivation and with Socioeconomic Position over the Life Course: Observations in the British Women's Heart and Health Study. 344. [DOI] [PubMed] [Google Scholar]
- Lamb S.E., Jørstad-Stein E.C., Hauer K., Becker C. Development of a common outcome data set for fall injury prevention trials: the Prevention of Falls Network Europe consensus. J. Am. Geriatr. Soc. 2005;53(9):1618–1622. doi: 10.1111/j.1532-5415.2005.53455.x. [DOI] [PubMed] [Google Scholar]
- Lancaster G.L., Dodd S., Williamson P.R. Design and analysis of pilot studies: recommendations for good practice. J. Eval. Clin. Pract. 2004;10(2):307–312. doi: 10.1111/j..2002.384.doc.x. [DOI] [PubMed] [Google Scholar]
- Merom D., Pye V., Macniven R., van der Ploeg H., Milat A., Sherrington C., Bauman A. Prevalence and correlates of participation in fall prevention exercise/physical activity by older adults. Prev. Med. 2012;55(6):613–617. doi: 10.1016/j.ypmed.2012.10.001. [DOI] [PubMed] [Google Scholar]
- Miller W.R. Motivational interviewing with problem drinkers. Behav. Psychother. 1983;11(2):147–172. [Google Scholar]
- Miller W.R., Rollnick S. Guilford Press; New York: 1991. Motivational Interviewing: Preparing People to Change Addictive Behavior/William R. Miller, Stephen Rollnick. [Google Scholar]
- Miller W.R., Rollnick S. 2nd ed. Guilford Publications The Guilford Press; New York, New York: 2002. Motivational Interviewing: Preparing People for Change. [Google Scholar]
- Miller W.R., Rollnick S. 3rd edition. Guilford Press; New York, NY, US: 2013. Motivational Interviewing: Helping People Change. [Google Scholar]
- Miller W.R., Rollnick S. The effectiveness and ineffectiveness of complex behavioral interventions: impact of treatment fidelity. Contemp. Clin. Trials. 2014;37(2):234–241. doi: 10.1016/j.cct.2014.01.005. [DOI] [PubMed] [Google Scholar]
- Nordell E., Thorngren K.G., Andreasson M., Gall K. Evaluating the Swedish version of the Falls Efficacy Scale-International (FES-I) Adv. Physiother. 2009;11(2):81–87. [Google Scholar]
- Sandborgh M., Åsenlöf P., Lindberg P., Denison E. Implementing behavioural medicine in physiotherapy treatment: Part II: adherence to treatment protocol, from. 2010. http://ep.bib.mdh.se/login?url=http://search.ebscohost.com/login.aspx?direct=true&db=edsswe&AN=edsswe.oai.DiVA.org.uu.131506&site=eds-live
- Schulz K.F., Altman D.G., Moher D. CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. Int. J. Surg. 2011;9(8):672–677. doi: 10.1016/j.ijsu.2011.09.004. [DOI] [PubMed] [Google Scholar]
- Schwalbe C.S., Oh H.Y., Zweben A. Sustaining motivational interviewing: a meta-analysis of training studies. Addiction. 2014;109(8):1287–1294. doi: 10.1111/add.12558. [DOI] [PubMed] [Google Scholar]
- Sipilä S., Salpakoski A., Edgren J., Kauppinen M.A., Rantanen T., Heinonen A., Kallinen M. Promoting mobility after hip fracture (ProMo): Study protocol and selected baseline results of a year-long randomized controlled trial among community-dwelling older people. [Article] BMC Musculoskelet. Disord. 2011;12 doi: 10.1186/1471-2474-12-277. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thabane L., Ma J., Chu R., Cheng J., Ismaila A., Rios L.P., Goldsmith C.H. A tutorial on pilot studies: the what, why and how. BMC Med. Res. Methodol. 2010;10:1-1. doi: 10.1186/1471-2288-10-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thomas S., Mackintosh S., Halbert J. Does the ‘Otago exercise programme’ reduce mortality and falls in older adults? A systematic review and meta-analysis. Age Ageing. 2010;39(6):681–687. doi: 10.1093/ageing/afq102. [DOI] [PubMed] [Google Scholar]
- Tsang C.S.L., Lin-Rong L., Chung R.C.K., Pang M.Y.C. Psychometric properties of the Mini-Balance Evaluation Systems Test (Mini-BESTest) in community-dwelling individuals with chronic stroke. Phys. Ther. 2013;93(8):1102–1115. doi: 10.2522/ptj.20120454. [DOI] [PubMed] [Google Scholar]
- Waters L., Reeves M., Fjeldsoe B., Eakin E. Control group improvements in physical activity intervention trials and possible explanatory factors: a systematic review. J. Phys. Act. Health. 2012;9(6):884–895. doi: 10.1123/jpah.9.6.884. [DOI] [PubMed] [Google Scholar]
- Wijlhuizen G.J. 2008. Physical Activity and Falls in Older Persons: Development of the Balance Control Difficulty Homeostasis Model: TNO Quality of Life, Faculty of Medicine/Leiden University Medical Center (LUMC), Leiden University, 2009-02-12. [Google Scholar]
- Yardley L., Bishop F.L., Lanta K., Beyer N., Holt A.R., Hauer K., Horne M. Older people's views of falls—prevention interventions in six European countries. Gerontologist. 2006;46(5):650–660. doi: 10.1093/geront/46.5.650. [DOI] [PubMed] [Google Scholar]