Abstract
Purpose
Systemic hypertension is a risk factor of age-related retinal diseases such as diabetic retinopathy and age-related macular degeneration. High intake of dietary salt and low intake of water increase extracellular osmolality resulting in hypertension, in particular in salt-sensitive individuals. This review summarizes the present knowledge regarding the impact of salt and water intake on the regulation of blood pressure, retinal function, and the development of age-related retinal diseases.
Methods
A literature search of the Medline database and a summary of recent studies that used human RPE cells.
Results
The salt sensitivity of the blood pressure and plasma osmolality increase with age, and body water deficits are common in older individuals. High plasma osmolality has adverse effects in the retina. In RPE cells, high osmolality induces expression and secretion of angiogenic factors, such as vascular endothelial growth factor (VEGF), placental growth factor, and basic fibroblast growth factor, and expression of aquaporin-5, a water channel implicated in transepithelial water transport. The transcriptional activities of hypoxia-inducible factor-1 (HIF-1) and nuclear factor of activated T cell 5 (NFAT5) are critical for the production of VEGF in response to salt-induced osmotic stress. Salt-induced osmotic stress also induces priming of the NLRP3 inflammasome and activates inflammatory enzymes in RPE cells.
Conclusions
Raised plasma osmolality may aggravate age-related retinal diseases by stimulation of local inflammation and angiogenic factor production in the RPE. Alterations in salt and water consumption, and of minerals that stimulate renal salt excretion, may offer nutritional approaches to prevent age-related retinal disorders, in particular in salt-sensitive individuals and individuals who show signs of body dehydration.
Introduction
Despite new medical and surgical interventions, age-related macular degeneration (AMD) remains the leading cause of irreversible blindness in patients older than 65 years in developed countries [1]. The majority (about 90%) of patients suffer from dry AMD that is, in the early stage, characterized by the thickening of and structural changes in Bruch’s membrane, basal laminar deposits (drusen), and lipofuscin accumulation in the RPE. In the advanced stage, dry AMD is characterized by geographic atrophy and choriocapillaris degeneration. The remaining patients suffer from exudative (neovascular) AMD characterized by choroidal neovascularization (CNV) and subretinal edema. Geographic atrophy, CNV, and edema are associated with photoreceptor damage resulting in progressive loss of visual acuity [2].
The pathogenesis of AMD is still incompletely understood. AMD is caused by age-dependent functional impairment and degeneration of RPE cells, and by a decrease in the choroidal blood flow; both result in hypoglycemia and hypoxia of the outer retina. A major function of the RPE is phagocytosis and digestion of membrane discs that are shed from the tips of photoreceptor outer segments [3]. The discs contain high amounts of peroxidized lipids and protein adducts that are formed due to oxidative stress resulting from light exposure, the high oxygen consumption of photoreceptors, and the high polyunsaturated fatty acid content of photoreceptor membranes [4,5]. The age-dependent dysregulation of protein and lipid recycling and degradation pathways in RPE cells [6,7] impairs the regular degradation of peroxidized photoreceptor lipoproteins; this impairment results in lipofuscin accumulation in RPE cells and deposition of drusen in Bruch’s membrane [8,9]. Accumulated lipoproteins constitute a hydrophobic barrier that adversely affects the transport of oxygen and nutrients from the choriocapillaris to the photoreceptors [10]. The resulting hypoglycemia and hypoxia of the outer retina induce overproduction of angiogenic factors by the RPE that stimulate the growth of choroidal vessels and increase the permeability of the outer blood–retinal barrier [10]. The toxic effects of peroxidized photoreceptor waste products and the decline in cellular clearance systems also cause chronic local inflammation associated with complement-mediated RPE cell injury, for example [5,9-12]. In addition to local inflammation, AMD is associated with systemic inflammation [13-16].
Vascular endothelial growth factor (VEGF) is the most relevant angiogenic factor induced by retinal hypoxia [17]. In addition to glial cells and invading macrophages, RPE cells are an important source of VEGF in the outer retina [18]. The efficiency of the clinical use of anti-VEGF agents in the treatment of CNV [19] underlines the important role of VEGF in pathological neovascularization. However, in more than half of patients visual acuity does not improve after anti-VEGF therapy, and about 10% of patients do not respond to treatment [20]. Therefore, it was suggested that in addition to VEGF, further angiogenic factors are required to promote the development of CNV [10,21]. Such angiogenic factors produced by the RPE are, for example, placental growth factor (PlGF), platelet-derived growth factor (PDGF), basic fibroblast growth factor (bFGF), heparin-binding epidermal growth factor-like growth factor (HB-EGF), and transforming growth factor-β (TGF-β) [10,22-27]. In addition, inflammatory and immune mediators (for example, complement proteins that accumulate in drusen and induce expression of VEGF in RPE cells) play a pathogenic role in CNV [9].
In addition to advanced age, race, and genetic factors, such as complement gene polymorphisms [28], lifestyle factors are associated with the risk of AMD. These factors include sunlight exposure, cigarette smoking, and nutrition [29]. Low levels of nutritional antioxidants and fat-rich nutrition increase the risk of AMD [1,30]. Plasma lipids, such as cholesterol and triglycerides, accumulate in Bruch’s membrane and contribute to drusen formation [31,32]. Obesity is associated with AMD [33,34], possibly because obesity induces oxidative damage and systemic vascular inflammation.
AMD was suggested to represent an ocular manifestation of a systemic disease process [14]. Associations have been reported between AMD and hypertension, cardiovascular disease, cerebrovascular disease, dyslipidemia, chronic kidney disease, and neurodegenerative disorders [14]. Cardiovascular disease and AMD share common risk factors, such as atherosclerosis, systemic markers of inflammation, cigarette smoking, and hyperlipidemia [35-37]. An important aspect of cardiovascular disease is hypertension. Systemic hypertension confers increased risk of AMD. The association between high blood pressure and AMD has been well documented in various population-based studies [36,38-40]. Some studies described an association between neovascular AMD and hypertension, but not geographic atrophy [29,33,34,41,42]. The shared risk factors suggest that cardiovascular disease plays an etiological role in the development of AMD [34]. In the present article, we direct attention to two nutritional factors that may affect directly and indirectly (via the effect on blood pressure) the development of AMD: the intake of dietary salt (sodium chloride) and drinking water. Alterations in salt and water consumption may offer nutritional approaches to prevent age-related retinal disorders, such as AMD.
Hypertension
Systemic hypertension affects a large proportion of the adult population and is a significant cause of morbidity worldwide. It was reported that 27% of adult Americans suffer hypertension (≥140/90 mmHg or use of antihypertensive medications) and another 31% suffer prehypertension (120–139/80–89 mmHg, no medication) [43]. Among adults older than 50 years, the lifetime risk of developing hypertension approaches 90% [44].
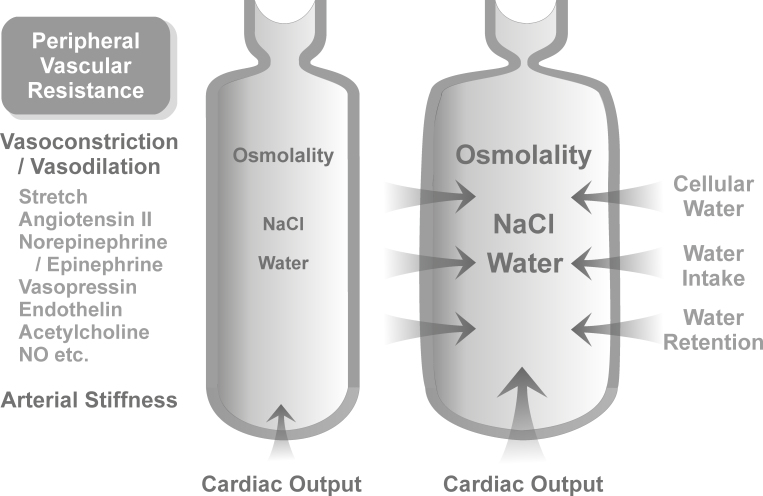
Blood pressure is proportional to cardiac output and vascular resistance to blood flow. Hypertension mainly results from an increase in the blood volume caused by increased osmotic pressure of the plasma (plasma osmolality); the expansion of the blood volume induces increases in cardiac output and in peripheral vascular resistance (Figure 1) [45-47]. Blood pressure increases with age [48] because of various age-related alterations. For example, plasma osmolarity increases [49], and arterial walls become less elastic; the latter is caused by arteriosclerosis and atheromatosis. AMD is associated with increased systemic arterial stiffness [37].
Figure 1.
Factors that influence arterial blood pressure. Blood pressure is proportional to cardiac output and the total peripheral resistance. The latter is dependent on the stiffness of the arterial walls and the level of arteriolar constriction. High intake of dietary salt causes a rise in extracellular (including plasma) osmolality during the postprandial phases. The elevation of extracellular osmolality results in an increase in the extracellular fluid (including blood) volume by various mechanisms: osmotic movement of cellular water to extracellular fluids, stimulation of the thirst center resulting in increased fluid intake, stimulation of renal salt excretion, and secretion of vasopressin that produces increased renal water retention. All of these mechanisms reduce the plasma salt level. The blood volume expansion increases cardiac output and induces arteriolar constriction (to prevent tissue overperfusion); both result in hypertension. The level of arteriolar constriction is regulated by the activities of vasoconstrictory (stretch, sympathetic activity, angiotensin II, epinephrine, vasopression, endothelin, etc.) and vasodilatory factors (acetylcholine, NO, etc.). Peripheral resistance increases with age mainly because the resistance vessels become thicker, stiffer, and narrowed due to arteriosclerosis (the replacement of the medial muscle fibers and intima by collagen) and atheromatosis (the deposition of lipids in vascular walls resulting in vascular inflammation and endothelial dysfunction). High salt also increases the blood pressure independent of blood volume expansion by direct effects on arterial smooth muscles, cardiac myocytes, hypothalamic control of blood pressure, and the local renin-angiotensin system. The blood pressure–raising effect of dietary salt increases with age mainly because of renal malfunction, which impairs salt excretion, and vascular alterations, such as arteriolar stiffening and decreased endothelial NO production. In addition, baseline plasma osmolality increases with age. The scheme shows the transition between an artery and an arteriole that controls tissue perfusion. In salt-resistant individuals, an increase in plasma osmolality induces a dilation of the artery (which prevents hypertension) while tissue perfusion remains constant due to arteriolar vasoconstrictory autoregulation. Age-related vessel stiffening impairs vessel dilation and contributes to the development of salt sensitivity of blood pressure.
Blood pressure can be lowered by decreases in cardiac output, vascular smooth muscle tonus, and plasma osmolality. This can be achieved with antihypertensive medications and with lifestyle modifications, such as increased physical activity, weight loss, and dietary alterations, including the Dietary Approaches to Stop Hypertension (DASH) diet (low-fat foods rich in fruits and vegetables and reduced in saturated fat and cholesterol), and moderation of alcohol intake [50,51]. Plasma osmolality can be decreased by reducing salt intake, increasing potassium intake, and increasing water consumption.
Plasma osmolality and hypertension: The role of salt intake
Plasma osmolality depends on the levels of glucose, lipids, and ions. Elevated plasma glucose frequently occurs during the postprandial phases and is common among elderly individuals because of the high prevalence of glucose intolerance [52,53]. However, the most relevant factor that determines plasma osmolality is the plasma salt level which is dependent on the balance between salt intake and excretion (Figure 1) [51,54]. Consumption of dietary salt is one cause of the age-related increase in blood pressure [48].
High intake of dietary salt is a main risk factor of cardiovascular disease. There is a linear relationship between salt consumption and blood pressure; however, the relationship between salt intake and the incidence of cardiovascular disease is nonlinear [54]. The optimal range of daily salt consumption is 2–3 g sodium/d, corresponding to about 5–8 g salt/d; higher and lower values increase the risk of cardiovascular disease [54]. Low salt consumption (<4 g/d) has various adverse consequences, such as increased insulin resistance, increased aldosterone secretion (which stimulates sodium reabsorption), activation of the renin-angiotensin system, and increased sympathetic nerve activity; all of these effects increase blood pressure [55]. Human societies differ in levels of salt consumption. There are populations with moderate salt intake, such as in North America (about 5–8 g/d), Great Britain (about 9 g/d), and Germany (about 6–9 g/d), and populations with high salt consumption, such as in Finland (about 11 g/d), South Korea (about 12 g/d), and Japan (about 14 g/d) [54]. The main source of salt in the diet (about 70%) is from processed foods [56]. In developed countries, the intake of dietary salt increased rapidly in the past along with the consumption of processed foods. Increased salt consumption may also represent an environmental risk factor for the progression of AMD [57].
Salt sensitivity of blood pressure
Human subjects differ in salt sensitivity of blood pressure. There are salt-resistant individuals; in these subjects, salt-induced variations in blood volume do not cause changes in plasma osmolality and blood pressure [47]. Salt resistance is mediated by effective renal salt excretion and endothelial production of vasodilatory nitric oxide (NO) [58,59]. Salt excretion restores normal blood volume within hours or days [47]. However, in salt-sensitive individuals, even small changes in plasma salt levels induce abnormal changes in blood pressure due to renal malfunction and impairment of endothelial NO production [60]. Thirty to fifty percent of hypertensive individuals, but also many normotensive individuals, are salt-sensitive [61,62]. Salt sensitivity of blood pressure increases with age [63].
Blood pressure–lowering minerals
In spite of the evidence that high salt intake is associated with hypertension, it was suggested that low consumption of minerals that reduce blood pressure (potassium, calcium, magnesium, phosphorus, bicarbonate) is a more important factor that induces hypertension; the blood pressure–lowering effect of these minerals is in part mediated by stimulation of renal salt excretion [64,65]. Potassium intake is inversely related to blood pressure [66]. The decreased content of blood pressure–lowering minerals is a characteristic of modern processed foods [67].
Dietary salt: Blood pressure–independent tissue damage
Excess salt also has direct harmful effects on tissues and vasculature, independent of blood pressure. The blood pressure–independent effects of high salt result in vascular remodeling, including thickening, stiffening, and narrowing of resistance arteries, and vascular fibrosis and inflammation [68,69]. Salt-induced vascular changes are mediated by various mechanisms, including stimulation of aldosterone synthesis [70] and oxidative stress [58]. High salt causes cellular perturbations, such as DNA double-strand breaks, oxidation of DNA and proteins, disruption of the mitochondrial structure and function, cytoskeletal alterations, and apoptotic cell death [71,72]. By inducing oxidative stress in RPE cells, high salt may also contribute to the development of AMD.
Plasma osmolality and hypertension: Role of water intake
Insufficient water intake increases the plasma salt level and osmolality. The baseline plasma osmolality increases, and the total body water decreases with age [49,73]. Body water deficits are common in elderly individuals [74,75]. Among hospitalized patients and long-term care residents, prevalences of body dehydration as high as 80% have been reported [76]. Reduced water intake in aged individuals is a result of various factors, including decreased thirst sensation, poor appetite, decreased kidney function and vasopressin effectiveness, illness, disability, use of medications (e.g., diuretics), social isolation, and cognitive disorders [74]. Body dehydration is associated with chronic disease and functional impairment, including neurologic complications ranging from lethargy to coma, renal failure, cardiovascular disease, cataract, and dry eye [77-80].
Retinal effects of hypertension
Systemic hypertension has widespread effects in the sensory retina. Elevated blood pressure induces retinal vascular changes, including hypertensive retinopathy, choroidopathy, and optic neuropathy, and is associated with increased risks of further vascular complications, such as retinal vein and artery occlusion, arteriolar macroaneurysm, and embolic events [81,82]. Hypertensive retinopathy, a sign of systemic vascular disease [81], is common and seen in nearly 10% of the general adult nondiabetic population [83]. Arteriolar narrowing, the earliest manifestation of hypertensive retinopathy [82], is caused by functional (loss of NO-mediated vasodilation) and structural changes (arteriosclerosis) [84,85]. The resulting retinal malperfusion may contribute to degeneration of retinal neurons and photoreceptors [86].
Hypertension confers increased risk of glaucoma and is the main secondary risk factor of diabetic retinopathy [87]. Control of blood pressure reduces the risk of diabetic retinopathy and prevents microvascular complications independent of glycemia [88]. Systemic hypertension also confers increased risk of AMD. Hypertension may also contribute to age-related structural changes in Bruch’s membrane [40]. However, antihypertensive medications do not alter the risk of AMD [41,89]. Several studies even described that the use of antihypertensive medications is associated with an increased incidence of AMD [90-92]. Differences between retinal and choroidal regulation of vessel perfusion [93] may explain the different associations between the use of antihypertensive medications and the risks of diabetic retinopathy and AMD.
Effects of hypertension on choroidal vasculature
Hypertension increases the risk of AMD via effects on choroidal circulation. Age- and AMD-related reduction in choroidal blood flow and the increase in choroidal blood velocity result from atrophy of the choriocapillaris and decreased parasympathetic perfusion regulation [94-98]. Among patients with AMD, there is a direct association between blood pressure and choroidal blood velocity [99]. Inadequate choroidal perfusion can lead to hypoglycemia and hypoxia of the overlying RPE [100] and is associated with focal RPE hyperpigmentation, drusen formation, and development of CNV [99,101,102]. Choroidal blood flow is also reduced in diabetic retinopathy [103].
Choroidal vascular disease in AMD is caused by hypertension and additional conditions that drive vascular inflammation, such as obesity and complement-induced endothelial injury [104]. Patients with hypertensive AMD display a more severe decrease in choroidal blood flow compared with normotensive patients [99]. Inadequate choroidal blood flow was found in patients with a history of systemic hypertension; both parameters do not correlate with actual blood pressure when antihypertensive medications are used, suggesting that hypertension in the past produces chronic effects on the choroidal vasculature [99].
The cellular mechanisms by which hypertension increases the risk of AMD are little understood. Systemic hypertension increases retinal inflammation [105], and hypertension is associated with mechanical stress on vascular and retinal cells [106]. Raised choroidal blood velocity increases endothelial shear stress that induces fibrinoid necrosis of choroidal arterioles, oxidative stress, and vascular inflammation [58,82,107]. Mechanical stress induces expression of VEGF in retinal endothelial and RPE cells [106,108]. Because VEGF is the most relevant angiogenic factor in the retina [17], hypertension-induced mechanical stress will facilitate the development of neovascular retinal disorders. AMD is associated with a decrease in the expression of NO synthases in choroidal arteries and RPE; lower production of NO increases vasoconstriction and reduces choroidal blood flow [109]. Whether the AMD-related decrease in NO synthase expression is facilitated by high salt as in renal endothelia [58] remains to be clarified.
Retinal effects of osmotic stress
Retinal osmotic stress due to raised plasma osmolality is common in elder and hypertensive individuals. In diabetes, osmotic stress mainly results from hyperglycemia that entails increased systemic osmolality and intracellular sorbitol accumulation [53,110]. Osmotic stress has adverse effects on the retina. High plasma osmolality decreases the standing potential of the eye [111] that originates from the RPE [112]. The standing potential is reduced in retinal diseases that are associated with altered integrity of the RPE, such as chorioretinal dystrophies and diabetic retinopathy [113,114]. High extracellular osmolality also causes decreases in the electroretinogram b-wave and oscillatory potential [115], alters the membrane potential, resistance, and gene expression of the RPE [116,117], induces transmitter release from synaptic terminals [118], and increases the adhesion of neutrophils to vascular endothelia [119] that represents an early step of vascular injury in diabetic retinopathy [120]. Exudative AMD is associated with a breakdown of the outer blood–retinal barrier constituted by the RPE [2]. Osmotic conditions regulate the tightness of this barrier. High osmolality at the basal side of the RPE induces a breakdown of the barrier, while low osmolality increases the tightness of the barrier [121]. Mannitol infusion in human subjects increases plasma osmolality and results in opening of the blood–brain and blood–retinal barriers [122].
Retinal effects of high salt
High salt consumption has various effects in the retina. In treatment-resistant hypertensive patients, salt consumption increases the wall thickness of retinal arterioles independent of blood pressure [123]. In salt-sensitive rats, high salt consumption induces retinal arteriolar spasm and ischemia [124].
Osmotic gradients between the retina and the blood are resolved by glial and RPE cells via mediating transmembrane ion and water fluxes [3,125]. Transmembrane water transport is facilitated and directed by aquaporin (AQP) water channels [126,127]. AQPs are a family of proteins that facilitate the bidirectional movement of water across membranes in dependence on the osmotic gradient and hydrostatic pressure [128]. High salt loading in rats results in retinal glial cell activation, intracellular edema, and mitochondrial swelling in retinal ganglion and glial cells, and increased expression of AQP1 in glial membranes [129]. Similar alterations in glial AQP expression have been observed in experimental ischemic and diabetic retinopathies [130,131]. High salt intake aggravates the changes in glial AQP expression associated with diabetic retinopathy independent of the blood pressure [132]. It is likely that alterations in the expression of additional AQP subtypes, for example, of AQP11 that is upregulated in retinal inflammation [133], may be implicated in the salt- and high osmolarity-induced responses of glial and RPE cells.
Systemic hypertension aggravates experimental diabetic retinopathy by increasing angiotensin II and sympathetic activities [134]. A low-salt diet modulates the retinal renin-angiotensin-aldosterone system that prevents experimental ischemic retinopathy and reduces vascular leakage and production of angiogenic and inflammatory factors, such as VEGF [135]. However, in human subjects, the use of angiotensin converting enzyme inhibitors is associated with a higher risk of AMD [90,91].
High salt: Induction of angiogenic growth factors in RPE cells
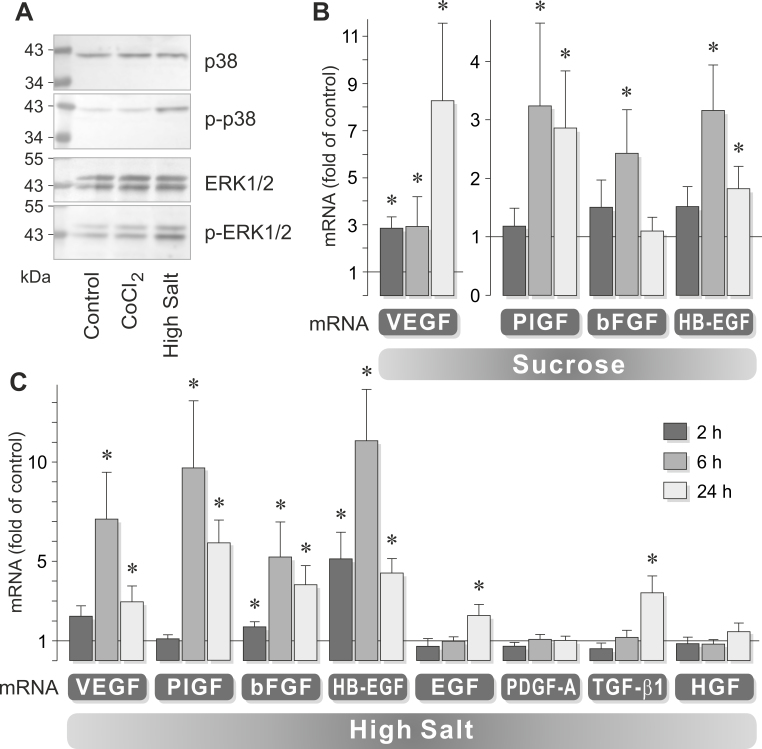
The development of CNV is stimulated by angiogenic factors [10]. The expression of VEGF, TGF-β, and bFGF is elevated in retinal tissues and CNV membranes of patients with AMD [136,137]. High extracellular osmolality may facilitate the development of neovascular AMD via direct effects on the RPE. Whether salt-induced high extracellular osmolality induces angiogenic factor expression in RPE cells has been recently investigated in cultured cells. High salt activates RPE cells, as indicated by the activation of mitogen-activated protein kinase (MAPK) pathways (Figure 2A) [57]. This is associated with increased expression of various angiogenic growth factor genes, including the VEGF, bFGF, PlGF, and HB-EGF genes (Figure 2B,C) [57,138,139]. The time-dependency of VEGF gene expression is different between salt- and sucrose-induced high osmolality (Figure 2B,C) [57]. This suggests that high salt induces VEGF expression by two different mechanisms: via the increase in extracellular osmolality and by alteration of the transmembrane sodium chloride gradient. High salt also induces secretion of VEGF, bFGF, and PlGF proteins from RPE cells [57,138,139]. The salt-induced expression of VEGF, bFGF, and HB-EGF is dependent on autocrine or paracrine activation of growth factor receptors, such as TGF-β and FGF receptors [139]. This suggests that high salt also induces a release of TGF-β and FGF from the cells. The expression of the VEGF gene induced by hypoxia and high salt is not additive (Figure 3A) [57]; this suggests that high extracellular salt may stimulate the expression of VEGF in RPE cells to a similar degree as hypoxia. Triamcinolone acetonide, an anti-inflammatory steroid clinically used for the rapid resolution of retinal edema, completely inhibits the salt-induced expression and secretion of VEGF in RPE cells [57]. Because a decrease in extracellular osmolality results in downregulation of VEGF and PlGF gene expression [57,138], the production of VEGF and PlGF in RPE cells is directly related to extracellular osmolality.
Figure 2.
High extracellular osmolality activates human RPE cells in vitro and stimulates gene expression of angiogenic factors. A: Western blot analysis shows that the addition of 100 mM salt (NaCl) to the culture medium for 20 min induces increased phosphorylation levels of p38 mitogen-activated protein kinase (MAPK) and extracellular signal-regulated kinase (ERK) 1/2 proteins. Phosphorylation of p38 MAPK and ERK1/2 is not stimulated by chemical hypoxia (induced by addition of 150 µM CoCl2) for 20 min. Amounts of total proteins are shown above; amounts of phosphorylated proteins are shown below. B, C: Relative mRNA levels of growth factors in cells cultured in media with high osmolality for 2, 6, and 24 h. High osmolality was induced by the addition of 100 mM sucrose (B) and 100 mM salt (C), respectively, to the culture medium. EGF = epidermal growth factor; HGF = hepatocyte growth factor. *p<0.05 vs. isoosmotic control. Modified after Hollborn et al. [57,138] and Veltmann et al. [139].
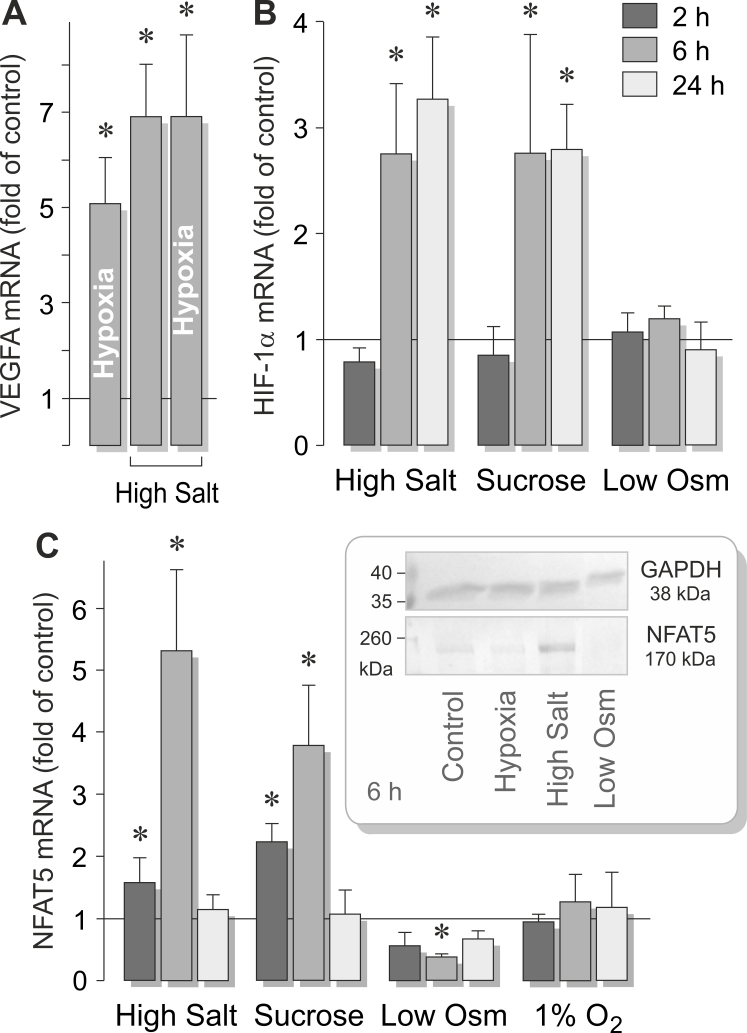
Figure 3.
High osmolality-induced expression of transcription factors in RPE cells. A: Chemical hypoxia (induced by the addition of 150 µM CoCl2) and high salt (+ 100 mM NaCl) do not additively increase the expression of the VEGF gene. B: High osmolality, induced by the addition of 100 mM salt (NaCl) or 100 mM sucrose to the culture medium, induces gene expression of hypoxia-inducible factor-1 alpha (HIF-1α). Low osmolality (Low Osm; 60% osmolality) has no effect. C: High osmolality increases, and low osmolality decreases, the gene expression of nuclear factor of activated T cell 5 (NFAT5). Hypoxia (1% O2) has no effect. Inset: The NFAT5 protein level in RPE cells determined with western blot analysis. High salt increases and low osmolality decreases the cellular NFAT5 protein level. Hypoxia (+ 150 µM CoCl2) has no effect. *p<0.05 vs. control. Modified after Hollborn et al. [57].
High salt: Induction of AQP5 in RPE cells
The development of retinal edema is an important vision-threatening condition of exudative AMD [140]. Normally, RPE cells clear the excess fluid from the subretinal space [3] by transcellular transport of ions and water; water transport is facilitated by AQP water channels [126]. The higher permeability of the outer blood–retinal barrier induced, for example, by VEGF allows increased fluid flux from choroidal vessels into the subretinal space. The fluid clearance capacity of RPE cells can be exceeded when excess blood-derived fluid enters the subretinal space and when the cells alter the expression of ion channels, transporters, and AQPs. RPE cells freshly isolated from human post-mortem donor eyes contain gene transcripts of various AQP subtypes; high salt induces expression of the AQP3, AQP5, and AQP8 genes in RPE cells [57]. Throughout the body, AQP5 plays an important role in transporting water across epithelia. In RPE cells, the expression of the AQP5 gene is directly related to extracellular osmolality; AQP5 gene expression is increased by high osmolality and decreased by low osmolality [57]. AQP5 gene expression in RPE cells is also reduced under hypoxic conditions and in the presence of blood serum [57]. Triamcinolone acetonide does not prevent high salt-induced expression of AQP5 [57].
High salt: Activation of transcription factors in RPE cells
Hypoxia and high salt induce non-additive expression of the VEGF gene (Figure 3A), suggesting the involvement of common mechanisms of transcriptional activation of the VEGF gene under both conditions [57]. Cellular adaptation to hypoxia is mainly mediated by transcriptional activation of target genes by the hypoxia-inducible factor-1 (HIF-1) resulting in increased production of proteins that improve oxygen and nutrient supply [141]. These genes include VEGF, glucose transporter, and erythropoietin genes [142]. HIF-1 also triggers the expression of inducible NO synthase [143]; NO induces vasodilation but also causes nitrosative stress and may contribute to photoreceptor degeneration [144]. HIF-1-induced transcriptional activation of VEGF plays a critical role in the development of experimental CNV [145].
High extracellular salt induces increased transcriptional activation of HIF-1α in RPE cells (Figure 3B) [57]. Inhibition of HIF-1 activity decreases salt-induced transcription of the VEGF gene by approximately 50% and abrogates almost completely salt-induced secretion of VEGF from RPE cells [57]. The salt-induced transcriptional activation of AQP5 is, in part, dependent on the activity of nuclear factor kappa beta (NF-κB) activity, but not on HIF-1 [57]. NF-κB is the main transcription factor that regulates the gene expression of proteins involved in inflammatory cell responses.
Normally, high extracellular osmolality causes water flux from cells resulting in cell shrinkage, an early event of apoptotic cell death [146]. However, cells possess several adaptive mechanisms that allow them to survive in osmotic stress by restoration of the osmotic balance. Cellular survival under high-salt conditions is initially maintained by activation of ion transport systems and thereafter by intracellular accumulation of small organic osmolytes and increased abundance of heat shock proteins and AQPs [71,72]. The classical cellular response to high extracellular osmolality involves the transcription of target genes by the nuclear factor of activated T cell 5 (NFAT5), also known as tonicity-responsive enhancer binding protein (TonEBP/OREBP) [72]. This transcription factor has a large C-terminal region that harbors a high osmolality-sensitive transactivation domain. NFAT5 binds to the tonicity responsive enhancer elements (TonEs) in the 5′ region of the target genes. The target genes of NFAT5 include genes for enzymes and transporters that are implicated in intracellular accumulation of organic osmolytes, such as sorbitol, myo-inositol, betaine, and taurine (aldose reductase, myo-inositol transporter 1, taurine transporter, etc.) [53,72]. Additional target genes of NFAT5 in various cell systems are heat shock protein 70–2, tumor necrosis factor-α, and water channels AQP1 and AQP2 [53,72].
In RPE cells, the expression of NFAT5 is directly related to the level of extracellular osmolality; that is, high osmolality increases and low osmolality decreases the gene and protein expression of NFAT5 (Figure 3C) [57]. High osmolality also induces DNA binding of the NFAT5 protein [57]. Hypoxia has no effect on the expression of NFAT5 (Figure 3C) [57]. Knockdown of NFAT5 expression with siRNA reduces salt-induced transcription of the VEGF, PlGF, bFGF, and AQP5 genes, and salt-induced secretion of VEGF and bFGF from RPE cells [57,138,139]. The data suggest that the transcriptional activity of NFAT5 is critical for salt-induced induction of VEGF and other angiogenic factors in RPE cells. Whether in addition to these transcription factors, additional mechanisms of gene transcription contribute to the effects of high salt in RPE cells (e.g., transcription induced by the increase in the intracellular sodium concentration [147]) remains to be determined.
Aldose reductase, which produces sorbitol from glucose, is a prototypical NFAT5 target gene [148]. Intracellular accumulation of sorbitol is a main pathogenic factor of diabetic retinopathy [149]. In the retinas of diabetic mice and in RPE cells stimulated with high glucose, NFAT5 activity induces (directly or indirectly) the expression of various genes, including aldose reductase and protein kinase Cδ, and the proapoptotic protein Bax, while NFAT5 decreases the expression of the antiapoptotic protein Bcl2; these data suggest that NFAT5 activity is involved in retinal degeneration under hyperglycemic conditions [150]. However, under high-salt conditions, production of sorbitol protects RPE cells from death [151], suggesting that intracellular sorbitol accumulation may also have protective effects. The contradictory effects of sorbitol production on cell viability in dependence on the strength or duration of osmotic imbalances may explain the limited benefits of aldose reductase inhibitors in the treatment of diabetic retinopathy [152].
High salt: Priming of the NLRP3 inflammasome
Chronic inflammation is a key factor that contributes to the development of AMD [13,15,16]. High salt was shown to increase the production of inflammatory factors, such as interleukin (IL)-6 and monocyte chemoattractant protein-1 (MCP-1) by RPE cells [153]. Generally, inflammatory processes are activated by cytosolic protein-signaling complexes, termed inflammasomes, which drive proteolytic activation of caspase-1 and maturation of the inflammatory cytokines IL-1β and IL-18 [154]. Activation of the NLRP3 inflammasome in RPE cells is implicated in mediating RPE cell degeneration in geographic atrophy [155] and may also promote neovascular AMD pathologies, such as RPE barrier breakdown and CNV [156]. In RPE cells, salt-induced osmotic stress induces priming and transient activation of the NLRP3 inflammasome, as well as expression and activation of inflammatory enzymes, such as phospholipases A2 and cyclooxygenases [157] (data not shown). Thus, high-salt consumption may aggravate the development of AMD by stimulation of local inflammation. Salt-induced priming of the NLRP3 inflammasome in RPE cells is, in part, mediated by the activities of HIF-1 and NFAT5 [157]. Full salt-induced expression of NFAT5 is dependent on the release of ATP and autocrine and paracrine activation of purinergic receptors, such as P2Y1 and P2X7 (data not shown). The latter may contribute to the degeneration of the RPE in geographic atrophy [155]. RPE-derived ATP may also promote photoreceptor degeneration [158], a characteristic of AMD, as well as microvascular cell death [159], a hallmark of diabetic retinopathy.
Summary and conclusions
Various studies showed an association between systemic hypertension and the risk of AMD. Hypertension aggravates the age-dependent degeneration of the choroidal vasculature, which reduces choroidal blood flow [99]. Choroidal ischemia and the resulting outer retinal hypoxia promote angiogenic factor production in the RPE and the development of CNV. However, it was shown that the use of antihypertensive medications does not confer a decreased risk of AMD [41,89]; this suggests that additional factors associated with hypertension are also relevant for the pathogenesis of AMD. The main factor that induces acute hypertension is the elevation of the plasma salt level that results from intake of dietary salt and impaired renal salt excretion [45,46,51,54]. Because high salt causes cellular perturbations independently of blood pressure, in part via increasing extracellular osmolality [71,72], direct effects of salt and high osmolality on choroidal and RPE cells may contribute to the pathological processes involved in the development of AMD.
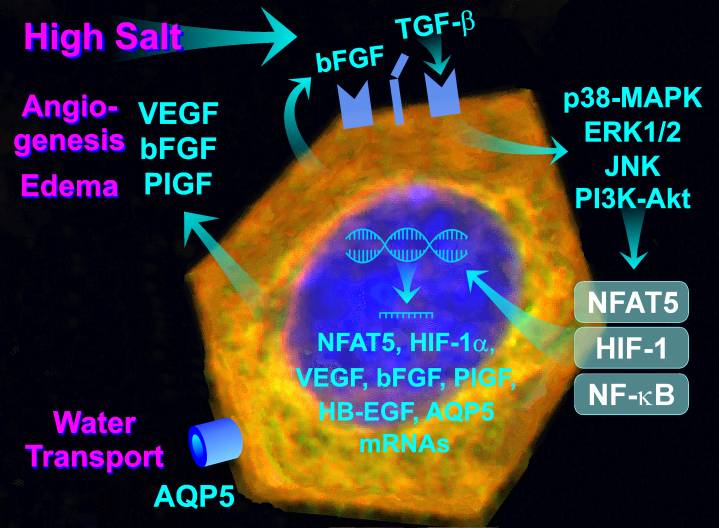
Recent studies showed that high salt and high extracellular osmolality have direct effects on RPE cells, including activation of MAPK pathways, activation of transcription factors, such as HIF-1, NF-κB, and NFAT5, transcriptional activation and secretion of angiogenic and inflammatory factors, such as VEGF, PlGF, bFGF, IL-6, and MCP-1, priming of the NLRP3 inflammasome, and upregulation of AQP5 (Figure 4) [57,138,139,153,157]. Salt-induced production of inflammatory factors may contribute to the development of local inflammation, a characteristic of AMD [13,15,16]. Salt-induced production of angiogenic factors may promote the development of CNV and edema, two hallmarks of neovascular AMD. Salt-induced production of TGF-β may contribute to choroidal fibrosis. Because hypoxia and high salt induce expression of the VEGF gene in a non-additive fashion (Figure 3A), high salt consumption may facilitate the development of CNV and edema under normoxic conditions. The data also suggest that dietary salt may act via three mechanisms: an increase in blood pressure, an increase in plasma osmolality, and alteration of the transmembrane sodium chloride gradient. These mechanisms may independently and additively stimulate the production of VEGF in the RPE (Figure 5). However, whether the increased plasma salt level and high extracellular osmolality are risk factors of AMD, independently of hypertension, remains to be determined in clinical studies.
Figure 4.
High salt consumption may aggravate neovascular retinal diseases by stimulation of angiogenic factor production in RPE cells. Excess salt induces the release of growth factors, such as basic fibroblast growth factor (bFGF) and transforming growth factor-β (TGF-β) from RPE cells. Autocrine and paracrine TGF-β and FGF receptor signaling induces activation of the intracellular signal transduction pathways, including p38 mitogen-activated protein kinase (MAPK), extracellular signal-regulated kinase (ERK) 1/2, c-Jun NH2-terminal kinase (JNK), and phosphatidylinositol-3 kinase (PI3K)-Akt pathways, resulting in activation of the transcription factors nuclear factor of activated T cell 5 (NFAT5), hypoxia-inducible factor-1 (HIF-1), nuclear factor kappa beta (NF-κB). NFAT5 and HIF-1 induce the transcription of the VEGF gene, while NFAT5 and NF-κB induce the transcription of the AQP5 gene. NFAT5 also induces expression of the bFGF gene. The salt-induced secretion of VEGF, bFGF, and placental growth factor (PlGF) may stimulate the development of the central nervous system (CNV) and edema. Increased expression of AQP5 may improve water transport through the RPE, which may facilitate the development and/or resolution of edema, in dependence on the osmotic and hydrostatic gradients across the RPE.
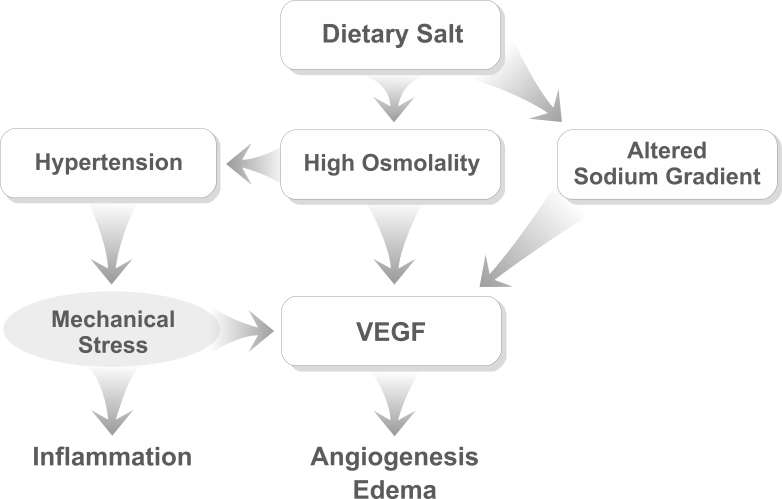
Figure 5.
Dietary salt intake may stimulate the production of VEGF in RPE cells via three independent mechanisms. High salt increases plasma osmolality resulting in raised blood pressure and membrane stretch, and it alters the transmembrane sodium gradient.
NFAT5 is a transcription factor that may contribute to the aggravating effects of high salt on the retinal disease processes in AMD. The expression of VEGF, PlGF, and AQP5 genes in RPE cells is directly related to the level of extracellular osmolality, likely because of the osmolality-dependent activation of NFAT5 (Figure 3C) [57,138]. However, the roles of NFAT5 activity in the regulation of retinal cell responses to osmotic stress and the development of age-related retinal diseases remain to be further investigated. In various cell systems, NFAT5 can be also activated in an osmolality-independent manner by different stimuli, such as cytokines, growth factors, receptor and integrin activation, ions, and reactive oxygen species [160]. It is unclear whether inhibition of NFAT5 may represent an approach to prevent the effects of high salt and osmotic stress on the RPE. Because NFAT5 is a transcription factor that improves cell survival in osmotic stress [71,72,151], it is conceivable that inhibition of NFAT5 may facilitate disease progression. However, downregulation of proapoptotic proteins and upregulation of antiapoptotic proteins induced by knockdown of NFAT5 in the retina of diabetic mice [150] may indicate that inhibition of NFAT5 will decelerate disease progression.
Osmotic conditions at the basal side of the RPE regulate the tightness of the outer blood–retinal barrier; high osmolality increases and low osmolality decreases the permeability of the barrier [121]. Up- and downregulation of VEGF under high- and low-osmolality conditions [57] may represent one mechanism by which osmotic alterations regulate the tightness of the barrier. Alterations in the expression of AQP5 in dependence on the osmotic conditions [57] may be implicated in the resolution of osmotic gradients across the RPE. High plasma osmolality may facilitate AQP5-mediated water transport from the subretinal space through the RPE. This may support the resolution of subretinal edema under conditions of osmotic opening of the outer blood–retinal barrier. Under conditions of low plasma osmolality, downregulation of AQP5 may reduce the water transport through the RPE and thus may diminish the osmotic water flux from the blood to the retinal tissue. However, whether the water permeability of the RPE is regulated by alterations in AQP5 expression remains to be confirmed by further studies. Hypoxic and serum-induced downregulation of AQP5 [57] may counteract the upregulation of AQP5 induced by high plasma osmolality. This will impair the fluid clearance across the RPE under hypoxic conditions and in the case of hemorrhage. Triamcinolone acetonide inhibits the expression and secretion of VEGF induced by high osmolality but does not prevent the upregulation of AQP5 [57]. The inhibitory effect on the production of VEGF and the ineffectiveness on the expression of AQP5 may support the resolution of retinal edema in situ.
Clinical implications
Although hypertension is associated with a higher risk of AMD, the use of antihypertensive medications is associated with an unaltered or even increased risk [41,89-92]. This may suggest that lifestyle modifications are more relevant than antihypertensive medications to decelerate progression of AMD. The effects of salt-induced high osmolality in RPE cells (Figure 4) suggest that a decrease in plasma osmolality may have protective effects. A decrease in plasma osmolality can be achieved by reducing the intake of dietary salt. Many meta-analyses suggest that most people will benefit from a reduction in salt consumption in terms of the risk of stroke and cardiovascular disease (e.g., Li et al. [161] and Aburto et al. [162]). Daily salt intake of <4 or <6 g is recommended by the American Heart Association and the Institute of Medicine, respectively [163]. Reduced dietary salt intake may also improve plasma cholesterol and triglyceride levels [164], known risk factors of AMD [29,32]. Therefore, it might be helpful to monitor dietary salt consumption in patients with AMD. However, there is an ongoing discussion regarding the beneficial effects of dietary salt restriction for cardiovascular disease [54]. There is a wide range of salt consumption (5–8 g/d) that has little effect on the risk of cardiovascular disease; higher (>10 g/d) and lower (<4 g/d) levels of salt intake are associated with increased risks of cardiovascular disease [54]. It is unlikely that dietary salt restriction has beneficial effects in populations with moderate salt consumption, such as in North America, Great Britain, and Germany; here, salt restriction may even be harmful [54]. In populations with high salt consumption, such as in Finland and Japan, dietary salt restriction may have beneficial effects [54].
Another approach to decrease the plasma salt level and osmolality is increased water intake. To obtain adequate body hydration and plasma osmolality, it was recommended to consume 1.5 l/d drinking water for women and 1.9 l/d for men [165]. These values are achieved in European countries (1.5–1.9 l/d) and are exceeded in North America (2.4 l/d) [166-168]. To avoid hyponatremia, lower daily water consumption is recommended for patients with distinct diseases, for example, severe congestive heart failure that requires high-dose diuretics [169]. Excess water intake may also cause hypertension and congestion of the cardiovascular system resulting from the increased blood volume.
Although the beneficial effects of reducing salt consumption and increasing water intake in the whole population are uncertain, there are two exceptions: salt-sensitive individuals and individuals who show signs of body dehydration. Because salt-resistant individuals show minimal changes in plasma osmolality and blood pressure after salt intake [47], dietary salt restriction does not have a benefit. However, salt-sensitive (normotensive and hypertensive) individuals display abnormal changes in plasma osmolality and blood pressure after salt intake [60]. The salt-induced upregulation of angiogenic factors in RPE cells is transient (Figure 2C) [57,139]. This suggests that repetitive salt-induced increases in plasma osmolality during postprandial phases will have greater effects than a persistent elevation of the plasma salt level. The fact that high extracellular osmolality and alteration of the transmembrane sodium chloride gradient induce upregulation of VEGF in RPE cells [57] could, at least in part, explain why the use of antihypertensive medications is not associated with a decreased risk of AMD [41,89]. This may suggest that, in salt-sensitive subjects, approaches to reduce plasma salt levels with dietary salt restriction may be more beneficial than antihypertensive medications. However, it should be kept in mind that the salt sensitivity of blood pressure is induced less by high salt consumption and more by low intake of blood pressure–lowering minerals (potassium, calcium, magnesium, phosphorus, bicarbonate) [64]. Therefore, salt sensitivity can also be attenuated by other dietary modifications, including the DASH diet and adequate dietary mineral intake [50,51,61,64]. Increased consumption of calcium-, magnesium-, potassium- (milk and dairy products), and bicarbonate-rich foods (fruits and vegetables) promotes renal salt excretion and blunts the pressor effect of dietary salt [65,170,171].
Inadequate water intake is common in elderly individuals. Therefore, the water consumption of aged patients should be monitored, and attention should be paid to signs of body dehydration (e.g., decreased skin turgor and increased urine osmolality as indicated by the yellow color of the urine). It is important that dehydrated elderly individuals drink more plain water and less of other fluids, such as fruit juice and soft drinks. The latter have higher osmolalities (550–840 mOsm/kg) than plasma (285–295 mOsm/kg) [172] and thus cause net movement of water from the vascular system into the intestinal lumen; this leads to impaired water intake and increased plasma osmolality. At least, beverages should be diluted with plain water. Dilution of high-energy beverages is also beneficial in terms of another risk factor of AMD, obesity [33,34].
Acknowledgments
Some of the work presented in this review was conducted with grants from the Deutsche Forschungsgemeinschaft (KO 1547/7–1 to L.K.) and the Geschwister Freter Stiftung (Hannover, Germany, to P.W.).
References
- 1.Van Leeuwen R, Klaver CC, Vingerling JR, Hofman A, de Jong PT. Epidemiology of age-related maculopathy: a review. Eur J Epidemiol. 2003;18:845–54. doi: 10.1023/a:1025643303914. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=14561043&dopt=Abstract a. [DOI] [PubMed] [Google Scholar]
- 2.Roth F, Bindewald A, Holz FG. Keypathophysiologic pathways in age-related macular disease. Graefes Arch Clin Exp Ophthalmol. 2004;242:710–6. doi: 10.1007/s00417-004-0976-x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15309554&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 3.Strauss O. The retinal pigment epithelium in visual function. Physiol Rev. 2005;85:845–81. doi: 10.1152/physrev.00021.2004. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15987797&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 4.Kopitz J, Holz FG, Kaemmerer E, Schutt F. Lipids and lipid peroxidation products in the pathogenesis of age-related macular degeneration. Biochimie. 2004;86:825–31. doi: 10.1016/j.biochi.2004.09.029. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15589692&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 5.Hollyfield JG, Bonilha VL, Rayborn ME, Yang X, Shadrach KG, Lu L, Ufret RL, Salomon RG, Perez VL. Oxidative damage-induced inflammation initiates age-related macular degeneration. Nat Med. 2008;14:194–8. doi: 10.1038/nm1709. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=18223656&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Kaarniranta K, Sinha D, Blasiak J, Kauppinen A, Vereb Z, Salminen A, Boulton ME, Petrovski G. Autophagy and heterophagy dysregulation leads to retinal pigment epithelium dysfunction and development of age-related macular degeneration. Autophagy. 2013;9:973–84. doi: 10.4161/auto.24546. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23590900&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Ferrington DA, Sinha D, Kaarniranta K. Defects in retinal pigment epithelial cell proteolysis and the pathology associated with age-related macular degeneration. Prog Retin Eye Res. 2016;51:69–89. doi: 10.1016/j.preteyeres.2015.09.002. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=26344735&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Feeney-Burns L, Berman ER, Rothman H. Lipofuscin of human retinal pigment epithelium. Am J Ophthalmol. 1980;90:783–91. doi: 10.1016/s0002-9394(14)75193-1. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=7446665&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 9.Anderson DH, Mullins RF, Hageman GS, Johnson LV. A role for local inflammation in the formation of drusen in the aging eye. Am J Ophthalmol. 2002;134:411–31. doi: 10.1016/s0002-9394(02)01624-0. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12208254&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 10.Schlingemann RO. Role of growth factors and the wound healing response in age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol. 2004;242:91–101. doi: 10.1007/s00417-003-0828-0. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=14685874&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 11.Hageman GS, Luthert PJ, Victor Chong NH, Johnson LV, Anderson DH, Mullins RF. An integrated hypothesis that considers drusen as biomarkers of immune-mediated processes at the RPE-Bruch's membrane interface in aging and age-related macular degeneration. Prog Retin Eye Res. 2001;20:705–32. doi: 10.1016/s1350-9462(01)00010-6. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11587915&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 12.Piippo N, Korkmaz A, Hytti M, Kinnunen K, Salminen A, Atalay M, Kaarniranta K, Kauppinen A. Decline in cellular clearance systems induces inflammasome signaling in human ARPE-19 cells. Biochim Biophys Acta. 2014;1843:3038–46. doi: 10.1016/j.bbamcr.2014.09.015. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=25268952&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 13.Xu H, Chen M, Forrester JV. Para-inflammation in the aging retina. Prog Retin Eye Res. 2009;28:348–68. doi: 10.1016/j.preteyeres.2009.06.001. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19560552&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 14.Cheung CM, Wong TY. Is age-related macular degeneration a manifestation of systemic disease? New prospects for early intervention and treatment. J Intern Med. 2014;276:140–53. doi: 10.1111/joim.12227. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24581182&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 15.Nita M, Grzybowski A, Ascaso FJ, Huerva V. Age-related macular degeneration in the aspect of chronic low-grade inflammation (pathophysiological parainflammation). Mediators Inflamm. 2014;2014:930671. doi: 10.1155/2014/930671. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=25214719&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Kauppinen A, Paterno JJ, Blasiak J, Salminen A, Kaarniranta K. Inflammation and its role in age-related macular degeneration. Cell Mol Life Sci. 2016;73:1765–86. doi: 10.1007/s00018-016-2147-8. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=26852158&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Witmer AN, Vrensen GF, Van Noorden CJ, Schlingemann RO. Vascular endothelial growth factors and angiogenesis in eye disease. Prog Retin Eye Res. 2003;22:1–29. doi: 10.1016/s1350-9462(02)00043-5. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12597922&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 18.Ishibashi T, Hata Y, Yoshikawa H, Nakagawa K, Sueishi K, Inomata H. Expression of vascular endothelial growth factor in experimental choroidal neovascularization. Graefes Arch Clin Exp Ophthalmol. 1997;235:159–67. doi: 10.1007/BF00941723. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9085111&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 19.Lim LS, Mitchell P, Seddon JM, Holz FG, Wong TY. Age-related macular degeneration. Lancet. 2012;379:1728–38. doi: 10.1016/S0140-6736(12)60282-7. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22559899&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 20.Tranos P, Vacalis A, Asteriadis S, Koukoula S, Vachtsevanos A, Perganta G, Georgalas I. Resistance to antivascular endothelial growth factor treatment in age-related macular degeneration. Drug Des Devel Ther. 2013;7:485–90. doi: 10.2147/DDDT.S43470. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23818759&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Oshima Y, Oshima S, Nambu H, Kachi S, Hackett SF, Melia M, Kaleko M, Connelly S, Esumi N, Zack DJ, Campochiaro PA. Increased expression of VEGF in retinal pigmented epithelial cells is not sufficient to cause choroidal neovascularization. J Cell Physiol. 2004;201:393–400. doi: 10.1002/jcp.20110. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15389527&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 22.Rakic JM, Lambert V, Devy L, Luttun A, Carmeliet P, Claes C, Nguyen L, Foidart JM, Noël A, Munaut C. Placental growth factor, a member of the VEGF family, contributes to the development of choroidal neovascularization. Invest Ophthalmol Vis Sci. 2003;44:3186–93. doi: 10.1167/iovs.02-1092. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12824270&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 23.Jo N, Mailhos C, Ju M, Cheung E, Bradley J, Nishijima K, Robinson GS, Adamis AP, Shima DT. Inhibition of platelet-derived growth factor B signaling enhances the efficacy of anti-vascular endothelial growth factor therapy in multiple models of ocular neovascularization. Am J Pathol. 2006;168:2036–53. doi: 10.2353/ajpath.2006.050588. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16723717&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Hollborn M, Tenckhoff S, Seifert M, Köhler S, Wiedemann P, Bringmann A, Kohen L. Human retinal epithelium produces and responds to placenta growth factor. Graefes Arch Clin Exp Ophthalmol. 2006;244:732–41. doi: 10.1007/s00417-005-0154-9. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16341703&dopt=Abstract a. [DOI] [PubMed] [Google Scholar]
- 25.Hollborn M, Iandiev I, Seifert M, Schnurrbusch UEK, Wolf S, Wiedemann P, Bringmann A, Kohen L. Expression of HB-EGF by retinal pigment epithelial cells in vitreoretinal proliferative disease. Curr Eye Res. 2006;31:863–74. doi: 10.1080/02713680600888807. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17050278&dopt=Abstract b. [DOI] [PubMed] [Google Scholar]
- 26.Hollborn M, Petto C, Steffen A, Trettner S, Bendig A, Wiedemann P, Bringmann A, Kohen L. Effects of thrombin on RPE cells are mediated by transactivation of growth factor receptors. Invest Ophthalmol Vis Sci. 2009;50:4452–9. doi: 10.1167/iovs.08-3194. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19369239&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 27.Hollborn M, Kohen L, Werschnik C, Tietz L, Wiedemann P, Bringmann A. Activated blood coagulation factor X (FXa) induces angiogenic growth factor expression in human retinal pigment epithelial cells. Invest Ophthalmol Vis Sci. 2012;53:5930–9. doi: 10.1167/iovs.11-9214. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22871831&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 28.Coleman HR, Chan CC, Ferris FL, 3rd, Chew EY. Age-related macular degeneration. Lancet. 2008;372:1835–45. doi: 10.1016/S0140-6736(08)61759-6. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19027484&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Klein R, Cruickshanks KJ, Nash SD, Krantz EM, Nieto FJ, Huang GH, Pankow JS, Klein BE. The prevalence of age-related macular degeneration and associated risk factors. Arch Ophthalmol. 2010;128:750–8. doi: 10.1001/archophthalmol.2010.92. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=20547953&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Eye Disease Case-Control Study Group Risk factors for neovascular age-related macular degeneration. Arch Ophthalmol. 1992;110:1701–8. doi: 10.1001/archopht.1992.01080240041025. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=1281403&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 31.Cousins SW, Espinosa-Heidmann DG, Alexandridou A, Sall J, Dubovy S, Csaky K. The role of aging, high fat diet and blue light exposure in an experimental mouse model for basal laminar deposit formation. Exp Eye Res. 2002;75:543–53. doi: 10.1006/exer.2002.2047. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12457866&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 32.Seddon JM, Cote J, Rosner B. Progression of age-related macular degeneration: association with dietary fat, transunsaturated fat, nuts, and fish intake. Arch Ophthalmol. 2003;121:1728–37. doi: 10.1001/archopht.121.12.1728. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=14662593&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Fraser-Bell S, Wu J, Klein R, Azen SP, Hooper C, Foong AW, Varma R. Cardiovascular risk factors and age-related macular degeneration: the Los Angeles Latino Eye Study. Am J Ophthalmol. 2008;145:308–16. doi: 10.1016/j.ajo.2007.10.007. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=18222193&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Hogg RE, Woodside JV, Gilchrist SE, Graydon R, Fletcher AE, Chan W, Knox A, Cartmill B, Chakravarthy U. Cardiovascular disease and hypertension are strong risk factors for choroidal neovascularization. Ophthalmol. 2008;115:1046–52. doi: 10.1016/j.ophtha.2007.07.031. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17953990&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 35.Vingerling JR, Dielemans I, Bots ML, Hofman A, Grobbee DE, de Jong PTVM. Age-related macular degeneration is associated with atherosclerosis. The Rotterdam Study. Am J Epidemiol. 1995;142:404–9. doi: 10.1093/oxfordjournals.aje.a117648. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=7625405&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 36.Van Leeuwen R, Ikram MK, Vingerling JR, Witteman JC, Hofman A, de Jong PT. Blood pressure, atherosclerosis, and the incidence of age-related maculopathy: the Rotterdam Study. Invest Ophthalmol Vis Sci. 2003;44:3771–7. doi: 10.1167/iovs.03-0121. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12939290&dopt=Abstract b. [DOI] [PubMed] [Google Scholar]
- 37.Sato E, Feke GT, Appelbaum EY, Menke MN, Trempe CL, McMeel JW. Association between systemic arterial stiffness and age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol. 2006;244:963–71. doi: 10.1007/s00417-005-0201-6. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16411106&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 38.Sperduto RD, Hiller R. Systemic hypertension and age-related maculopathy in the Framingham Study. Arch Ophthalmol. 1986;104:216–9. doi: 10.1001/archopht.1986.01050140070022. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=3947296&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 39.Goldberg J, Flowerdew G, Smith E, Brody JA, Tso MO. Factors associated with age-related macular degeneration. An analysis of data from the first National Health and Nutrition Examination Survey. Am J Epidemiol. 1988;128:700–10. doi: 10.1093/oxfordjournals.aje.a115023. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=3421236&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 40.Klein R, Klein BE, Tomany SC, Cruickshanks KJ. The association of cardiovascular disease with the long-term incidence of age-related maculopathy: the Beaver Dam Eye Study. Ophthalmology. 2003;110:1273–80. doi: 10.1016/S0161-6420(03)00599-2. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12799274&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 41.Hyman L, Schachat AP, He Q, Leske MC. Hypertension, cardiovascular disease, and age-related macular degeneration. Age-Related Macular Degeneration Risk Factors Study Group. Arch Ophthalmol. 2000;118:351–8. doi: 10.1001/archopht.118.3.351. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=10721957&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 42.Age-Related Eye Disease Study Research Group Risk factors associated with age-related macular degeneration. A case-control study in the Age-Related Eye Disease Study: Age-Related Eye Disease Study report number 3. Ophthalmology. 2000;107:2224–32. doi: 10.1016/s0161-6420(00)00409-7. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11097601&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Wang Y, Wang QJ. The prevalence of prehypertension and hypertension among US adults according to the new joint national committee guidelines: new challenges of the old problem. Arch Intern Med. 2004;164:2126–34. doi: 10.1001/archinte.164.19.2126. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15505126&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 44.Vasan RS, Beiser A, Seshadri S, Larson MG, Kannel WB, D’Agostino RB, Levy D. Residual lifetime risk for developing hypertension in middle-aged women and men: the Framingham Heart Study. JAMA. 2002;287:1003–10. doi: 10.1001/jama.287.8.1003. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11866648&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 45.Lifton RP, Gharavi AG, Geller DS. Molecular mechanisms of human hypertension. Cell. 2001;104:545–56. doi: 10.1016/s0092-8674(01)00241-0. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11239411&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 46.He FJ, Markandu ND, Sagnella GA, de Wardener HE, MacGregor GA. Plasma sodium: ignored and underestimated. Hypertension. 2005;45:98–102. doi: 10.1161/01.HYP.0000149431.79450.a2. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15557392&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 47.Charra B. Fluid balance, dry weight, and blood pressure in dialysis. Hemodial Int. 2007;11:21–31. doi: 10.1111/j.1542-4758.2007.00148.x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17257351&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 48.Anderson DE, Fedorova OV, Morrell CH, Longo DL, Kashkin VA, Metzler JD, Bagrov AY, Lakatta EG. Endogenous sodium pump inhibitors and age-associated increases in salt sensitivity of blood pressure in normotensives. Am J Physiol Regul Integr Comp Physiol. 2008;294:R1248–54. doi: 10.1152/ajpregu.00782.2007. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=18287222&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Kenney WL, Chiu P. Influence of age on thirst and fluid intake. Med Sci Sports Exerc. 2001;33:1524–32. doi: 10.1097/00005768-200109000-00016. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11528342&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 50.Sacks FM, Svetkey LP, Vollmer WM, Appel LJ, Bray GA, Harsha D, Obarzanek E, Conlin PR, Miller ER, 3rd, Simons-Morton DG, Karanja N, Lin PH, DASH-Sodium Collaborative Research Group Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet: DASH-Sodium Collaborative Research Group. N Engl J Med. 2001;344:3–10. doi: 10.1056/NEJM200101043440101. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11136953&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 51.Appel LJ, Brands MW, Daniels SR, Karanja N, Elmer PJ, Sacks FM, American Heart Association Dietary approaches to prevent and treat hypertension: a scientific statement from the American Heart Association. Hypertension. 2006;47:296–308. doi: 10.1161/01.HYP.0000202568.01167.B6. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16434724&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 52.Stookey JD, Pieper CF, Cohen HJ. Is the prevalence of dehydration among community-dwelling older adults really low? Informing current debate over the fluid recommendation for adults aged 70+ years. Public Health Nutr. 2005;8:1275–85. doi: 10.1079/phn2005829. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16372923&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 53.Neuhofer W. Role of NFAT5 in inflammatory disorders associated with osmotic stress. Curr Genomics. 2010;11:584–90. doi: 10.2174/138920210793360961. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=21629436&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Alderman MH. Presidential Address: 21st Scientific Meeting of the International Society of Hypertension: dietary sodium and cardiovascular disease: the 'J'-shaped relation. J Hypertens. 2007;25:903–7. doi: 10.1097/HJH.0b013e3280c14394. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17414648&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 55.Alderman MH. Evidence relating dietary sodium to cardiovascular disease. J Am Coll Nutr. 2006;25:256S–61S. doi: 10.1080/07315724.2006.10719575. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16772637&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 56.Opinion of the Scientific Panel on Dietetic Products Nutrition and Allergies on a request from the Commission related to the Tolerable Upper Intake Level of Sodium. EFSA Journal. 2005;209:1–26. [Google Scholar]
- 57.Hollborn M, Vogler S, Reichenbach A, Wiedemann P, Bringmann A, Kohen L. Regulation of the hyperosmotic induction of aquaporin 5 and VEGF in retinal pigment epithelial cells: Involvement of NFAT5. Mol Vis. 2015;21:360–77. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=25878490&dopt=Abstract [PMC free article] [PubMed] [Google Scholar]
- 58.Sanders PW. Salt intake, endothelial cell signaling, and progression of kidney disease. Hypertension. 2004;43:142–6. doi: 10.1161/01.HYP.0000114022.20424.22. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=14707151&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 59.Ritz E. Salt - friend or foe? Nephrol Dial Transplant. 2006;21:2052–6. doi: 10.1093/ndt/gfi256. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16384834&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 60.De Wardener HE, He FJ, MacGregor GA. Plasma sodium and hypertension. Kidney Int. 2004;66:2454–66. doi: 10.1111/j.1523-1755.2004.66018.x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15569339&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 61.Morris RC, Jr, Sebastian A, Forman A, Tanaka M, Schmidlin O. Normotensive salt sensitivity: effects of race and dietary potassium. Hypertension. 1999;33:18–23. doi: 10.1161/01.hyp.33.1.18. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9931076&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 62.Weinberger MH, Fineberg NS, Fineberg SE, Weinberger M. Salt sensitivity, pulse pressure, and death in normal and hypertensive humans. Hypertension. 2001;37:429–32. doi: 10.1161/01.hyp.37.2.429. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11230313&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 63.Khaw KT, Barrett-Connor E. The association between blood pressure, age and dietary sodium and potassium: a population study. Circulation. 1988;77:53–61. doi: 10.1161/01.cir.77.1.53. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=3257173&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 64.McCarron DA. Role of adequate dietary calcium intake in the prevention and management of salt-sensitive hypertension. Am J Clin Nutr. 1997;65:712S–6S. doi: 10.1093/ajcn/65.2.712S. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9022571&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 65.Gallen IW, Rosa RM, Esparaz DY, Young JB, Robertson GL, Batlle D, Epstein FH, Landsberg L. On the mechanism of the effects of potassium restriction on blood pressure and renal sodium retention. Am J Kidney Dis. 1998;31:19–27. doi: 10.1053/ajkd.1998.v31.pm9428447. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9428447&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 66.Whelton PK, He J. Health effects of sodium and potassium in humans. Curr Opin Lipidol. 2014;25:75–9. doi: 10.1097/MOL.0000000000000033. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24345983&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 67.Ekmekcioglu C, Blasche G, Dorner TE. Too much salt and how we can get rid of it. Forsch Komplement Med. 2013;20:454–60. doi: 10.1159/000357413. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24434760&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 68.Kupari M, Koskinen P, Virolainen J. Correlates of left ventricular mass in a population sample aged 36–37 years. Focus on lifestyle and salt intake. Circulation. 1994;89:1041–50. doi: 10.1161/01.cir.89.3.1041. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=8124789&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 69.Safar ME, Thuilliez C, Richard V, Benetos A. Pressure-independent contribution of sodium to large artery structure and function in hypertension. Cardiovasc Res. 2000;46:269–76. doi: 10.1016/s0008-6363(99)00426-5. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=10773231&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 70.Takeda Y, Yoneda T, Demura M, Miyamori I, Mabuchi H. Sodium-induced cardiac aldosterone synthesis causes cardiac hypertrophy. Endocrinology. 2000;141:1901–4. doi: 10.1210/endo.141.5.7529. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=10803602&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 71.Ferraris JD, Burg MB. Tonicity-dependent regulation of osmoprotective genes in mammalian cells. Contrib Nephrol. 2006;152:125–41. doi: 10.1159/000096320. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17065809&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 72.Cheung CY, Ko BC. NFAT5 in cellular adaptation to hypertonic stress - regulations and functional significance. J Mol Signal. 2013;8:5. doi: 10.1186/1750-2187-8-5. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23618372&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Watson PE, Watson ID, Batt RD. Total body water volumes for adult males and females estimated from simple anthropometric measurements. Am J Clin Nutr. 1980;33:27–39. doi: 10.1093/ajcn/33.1.27. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=6986753&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 74.Hoffman NB. Dehydration in the elderly: insidious and manageable. Geriatrics. 1991;46:35–8. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=2040458&dopt=Abstract [PubMed] [Google Scholar]
- 75.Matz R. Dehydration in older adults. JAMA. 1996;275:911–2. doi: 10.1001/jama.1996.03530360021030. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=8598616&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 76.O’Neill PA, Davies I, Wears R, Barrett JA. Elderly female patients in continuing care: why are they hyperosmolar? Gerontology. 1989;35:205–9. doi: 10.1159/000213024. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=2511083&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 77.Minassian DC, Mehra V, Verrey JD. Dehydrational crises: a major risk factor in blinding cataract. Br J Ophthalmol. 1989;73:100–5. doi: 10.1136/bjo.73.2.100. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=2930754&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Chan J, Knutsen SF, Blix GG, Lee JW, Fraser GE. Water, other fluids, and fatal coronary heart disease: the Adventist Health Study. Am J Epidemiol. 2002;155:827–33. doi: 10.1093/aje/155.9.827. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11978586&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 79.Wilson MM, Morley JE. Impaired cognitive function and mental performance in mild dehydration. Eur J Clin Nutr. 2003;57(Suppl 2):S24–9. doi: 10.1038/sj.ejcn.1601898. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=14681710&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 80.Walsh NP, Fortes MB, Raymond-Barker P, Bishop C, Owen J, Tye E, Esmaeelpour M, Purslow C, Elghenzai S. Is whole-body hydration an important consideration in dry eye? Invest Ophthalmol Vis Sci. 2012;53:6622–7. doi: 10.1167/iovs.12-10175. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22952120&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 81.Wong TY, Mitchell P. The eye in hypertension. Lancet. 2007;369:425–35. doi: 10.1016/S0140-6736(07)60198-6. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17276782&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 82.DellaCroce JT, Vitale AT. Hypertension and the eye. Curr Opin Ophthalmol. 2008;19:493–8. doi: 10.1097/ICU.0b013e3283129779. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=18854694&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 83.Bhargava M, Ikram MK, Wong TY. How does hypertension affect your eyes? J Hum Hypertens. 2012;26:71–83. doi: 10.1038/jhh.2011.37. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=21509040&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 84.Wong TY, Mitchell P. Hypertensive retinopathy. N Engl J Med. 2004;351:2310–7. doi: 10.1056/NEJMra032865. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15564546&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 85.Delles C, Michelson G, Harazny J, Oehmer S, Hilgers KF, Schmieder RE. Impaired endothelial function of the retinal vasculature in hypertensive patients. Stroke. 2004;35:1289–93. doi: 10.1161/01.STR.0000126597.11534.3b. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15073389&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 86.Sabbatini M, Strocchi P, Vitaioli L, Amenta F. Changes of retinal neurons and glial fibrillary acid protein immunoreactive astrocytes in spontaneously hypertensive rats. J Hypertens. 2001;19:1861–9. doi: 10.1097/00004872-200110000-00022. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11593108&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 87.Kostraba JN, Klein R, Dorman JS, Becker DJ, Drash AL, Maser RE, Orchard TJ. The epidemiology of diabetes complications study. IV. Correlates of diabetic background and proliferative retinopathy. Am J Epidemiol. 1991;133:381–91. doi: 10.1093/oxfordjournals.aje.a115892. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=1994702&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 88.UK Prospective Diabetes Study Group Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ. 1998;317:703–13. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9732337&dopt=Abstract [PMC free article] [PubMed] [Google Scholar]
- 89.Van Leeuwen R, Tomany SC, Wang JJ, Klein R, Mitchell P, Hofman A, Klein BE, Vingerling JR, Cumming RG, de Jong PT. Is medication use associated with the incidence of early age-related maculopathy? Pooled findings from 3 continents. Ophthalmology. 2004;111:1169–75. doi: 10.1016/j.ophtha.2003.10.024. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15177967&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 90.McCarty CA, Mukesh BN, Fu CL, Mitchell P, Wang JJ, Taylor HR. Risk factors for age-related maculopathy: the Visual Impairment Project. Arch Ophthalmol. 2001;119:1455–62. doi: 10.1001/archopht.119.10.1455. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11594944&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 91.Etminan M, Brophy JM, Maberley D. Use of statins and angiotensin converting enzyme inhibitors (ACE-Is) and the risk of age-related macular degeneration: nested case-control study. Curr Drug Saf. 2008;3:24–6. doi: 10.2174/157488608783333952. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=18690977&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 92.Klein R, Myers CE, Klein BE. Vasodilators, blood pressure-lowering medications, and age-related macular degeneration: the Beaver Dam Eye Study. Ophthalmology. 2014;121:1604–11. doi: 10.1016/j.ophtha.2014.03.005. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24793737&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Kur J, Newman EA, Chan-Ling T. Cellular and physiological mechanisms underlying blood flow regulation in the retina and choroid in health and disease. Prog Retin Eye Res. 2012;31:377–406. doi: 10.1016/j.preteyeres.2012.04.004. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22580107&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.McLeod DS, Lutty GA. High-resolution histologic analysis of the human choroidal vasculature. Invest Ophthalmol Vis Sci. 1994;35:3799–811. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=7928177&dopt=Abstract [PubMed] [Google Scholar]
- 95.Ramrattan RS, van der Schaft TL, Mooy CM, de Bruijn WC, Mulder PG, de Jong PT. Morphometric analysis of Bruch’s membrane, the choriocapillaris, and the choroid in aging. Invest Ophthalmol Vis Sci. 1994;35:2857–64. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=8188481&dopt=Abstract [PubMed] [Google Scholar]
- 96.Dallinger S, Findl O, Strenn K, Eichler HG, Wolzt M, Schmetterer L. Age dependence of choroidal blood flow. J Am Geriatr Soc. 1998;46:484–7. doi: 10.1111/j.1532-5415.1998.tb02471.x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9560073&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 97.Fitzgerald MEC, Tolley E, Jackson B, Zagvazdin YS, Cuthbertson SL, Hodos W, Reiner A. Anatomical and functional evidence for progressive age-related decline in parasympathetic control of choroidal blood flow in pigeons. Exp Eye Res. 2005;81:478–91. doi: 10.1016/j.exer.2005.03.008. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15935343&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 98.Ehrlich R, Kheradiya NS, Winston DM, Moore DB, Wirostko B, Harris A. Age-related ocular vascular changes. Graefes Arch Clin Exp Ophthalmol. 2009;247:583–91. doi: 10.1007/s00417-008-1018-x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19084984&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 99.Metelitsina TI, Grunwald JE, DuPont JC, Ying GS. Effect of systemic hypertension on foveolar choroidal blood flow in age related macular degeneration. Br J Ophthalmol. 2006;90:342–6. doi: 10.1136/bjo.2005.082974. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16488959&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Coleman DJ, Silverman RH, Rondeau MJ, Lloyd HO, Khanifar AA, Chan RV. Age-related macular degeneration: choroidal ischaemia? Br J Ophthalmol. 2013;97:1020–3. doi: 10.1136/bjophthalmol-2013-303143. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23740965&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Ciulla TA, Harris A, Kagemann L, Danis RP, Pratt LM, Chung HS, Weinberger D, Garzozi HJ. Choroidal perfusion perturbations in non-neovascular age related macular degeneration. Br J Ophthalmol. 2002;86:209–13. doi: 10.1136/bjo.86.2.209. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11815349&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.Mullins RF, Johnson MN, Faidley EA, Skeie JM, Huang J. Choriocapillaris vascular dropout related to density of drusen in human eyes with early age-related macular degeneration. Invest Ophthalmol Vis Sci. 2011;52:1606–12. doi: 10.1167/iovs.10-6476. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=21398287&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Nagaoka T, Kitaya N, Sugawara R, Yokota H, Mori F, Hikichi T, Fujio N, Yoshida A. Alteration of choroidal circulation in the foveal region in patients with type 2 diabetes. Br J Ophthalmol. 2004;88:1060–3. doi: 10.1136/bjo.2003.035345. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15258025&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Lundh von Leithner P, Kam JH, Bainbridge J, Catchpole I, Gough G, Coffey P, Jeffery G. Complement factor H is critical in the maintenance of retinal perfusion. Am J Pathol. 2009;175:412–21. doi: 10.2353/ajpath.2009.080927. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19541934&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Silva KC, Pinto CC, Biswas SK, de Faria JB, de Faria JM. Hypertension increases retinal inflammation in experimental diabetes: a possible mechanism for aggravation of diabetic retinopathy by hypertension. Curr Eye Res. 2007;32:533–41. doi: 10.1080/02713680701435391. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17612969&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 106.Suzuma I, Hata Y, Clermont A, Pokras F, Rook SL, Suzuma K, Feener EP, Aiello LP. Cyclic stretch and hypertension induce retinal expression of vascular endothelial growth factor and vascular endothelial growth factor receptor-2: potential mechanisms for exacerbation of diabetic retinopathy by hypertension. Diabetes. 2001;50:444–54. doi: 10.2337/diabetes.50.2.444. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11272159&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 107.Rodriguez-Iturbe B, Vaziri ND, Herrera-Acosta J, Johnson RJ. Oxidative stress, renal infiltration of immune cells, and salt-sensitive hypertension: all for one and one for all. Am J Physiol Renal Physiol. 2004;286:F606–16. doi: 10.1152/ajprenal.00269.2003. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15001451&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 108.Seko Y, Seko Y, Fujikura H, Pang J, Tokoro T, Shimokawa H. Induction of vascular endothelial growth factor after application of mechanical stress to retinal pigment epithelium of the rat in vitro. Invest Ophthalmol Vis Sci. 1999;40:3287–91. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=10586955&dopt=Abstract [PubMed] [Google Scholar]
- 109.Bhutto IA, Baba T, Merges C, McLeod DS, Lutty GA. Low nitric oxide synthases (NOSs) in eyes with age-related macular degeneration (AMD). Exp Eye Res. 2010;90:155–67. doi: 10.1016/j.exer.2009.10.004. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19836390&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Cheung AK, Lo AC, So KF, Chung SS, Chung SK. Gene deletion and pharmacological inhibition of aldose reductase protect against retinal ischemic injury. Exp Eye Res. 2007;85:608–16. doi: 10.1016/j.exer.2007.07.013. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17727843&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 111.Kawasaka K, Yanagida T, Yamamoto S, Yonemura D. Decrease of electrooculographic potential under osmotic stress in man. Jpn J Ophthalmol. 1977;31:23–8. [Google Scholar]
- 112.Steinberg RH, Linsenmeier RA, Griff ER. Retinal pigment epithelial cell contributions to the electroretinogram and electrooculogram. Prog Retinal Res. 1985;4:33–66. [Google Scholar]
- 113.Yonemura D, Kawasaki K, Madachi-Yamamoto S. Hyperosmolarity response of ocular standing potential as a clinical test for retinal pigment epithelium activity: Chorioretinal dystrophies. Doc Ophthalmol. 1984;57:163–73. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=6432505&dopt=Abstract [PubMed] [Google Scholar]
- 114.Kawasaki K, Yonemura D, Madachi-Yamamoto S. Hyperosmolarity response of ocular standing potential as a clinical test for retinal pigment epithelium activity: Diabetic retinopathy. Doc Ophthalmol. 1984;58:375–84. doi: 10.1007/BF00679800. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=6441696&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 115.Winkler BS. Hyperosmolarity and electroretinogram (ERG) potentials in isolated rat retinas: possible implications in diabetic models. Exp Eye Res. 2003;77:115–6. doi: 10.1016/s0014-4835(03)00085-x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12823995&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 116.Shirao Y, Steinberg RH. Mechanisms of effects of small hyperosmotic gradients on the chick RPE. Invest Ophthalmol Vis Sci. 1987;28:2015–25. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=3679749&dopt=Abstract [PubMed] [Google Scholar]
- 117.Arsenijevic T, Vujovic A, Libert F, Op de Beeck A, Hébrant A, Janssens S, Grégoire F, Lefort A, Bolaky N, Perret J, Caspers L, Willermain F, Delporte C. Hyperosmotic stress induces cell cycle arrest in retinal pigmented epithelial cells. Cell Death Dis. 2013;4:e662. doi: 10.1038/cddis.2013.189. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23744362&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 118.Yu W, Miller RF. Hyperosmotic activation of transmitter release from presynaptic terminals onto retinal ganglion cells. J Neurosci Methods. 1995;62:159–68. doi: 10.1016/0165-0270(95)00071-2. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=8750098&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 119.Gilcrease MZ, Hoover RL. Neutrophil adhesion to endothelium following hyperosmolar insult. Diabetes Res. 1991;16:149–57. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=1802480&dopt=Abstract [PubMed] [Google Scholar]
- 120.Joussen AM, Murata T, Tsujikawa A, Kirchhof B, Bursell SE, Adamis AP. Leukocyte-mediated endothelial cell injury and death in the diabetic retina. Am J Pathol. 2001;158:147–52. doi: 10.1016/S0002-9440(10)63952-1. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=11141487&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 121.Orgül S, Reuter U, Kain HL. Osmotic stress in an in vitro model of the outer blood-retinal barrier. Ger J Ophthalmol. 1993;2:436–43. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=8312831&dopt=Abstract [PubMed] [Google Scholar]
- 122.Millay RH, Klein ML, Shults WT, Dahlborg SA, Neuwelt EA. Maculopathy associated with combination chemotherapy and osmotic opening of the blood-brain barrier. Am J Ophthalmol. 1986;102:626–32. doi: 10.1016/0002-9394(86)90536-2. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=3096140&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 123.Raff U, Harazny JM, Titze SI, Schmidt BM, Michelson G, Schmieder RE. Salt intake determines retinal arteriolar structure in treatment resistant hypertension independent of blood pressure. Atherosclerosis. 2012;222:235–40. doi: 10.1016/j.atherosclerosis.2012.02.006. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22386068&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 124.Thimm F, Frey M, Spitzmüller K, Hofgärtner W, Fleckenstein-Grün G. Arteriolar spasm and ischemia in the ocular fundus of NaCl-loaded salt sensitive Dahl rats: vascular protection by long-term treatment with the calcium antagonist nitrendipine. Adv Exp Med Biol. 1992;317:793–8. doi: 10.1007/978-1-4615-3428-0_97. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=1288206&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 125.Bringmann A, Pannicke T, Grosche J, Francke M, Wiedemann P, Skatchkov SN, Osborne NN, Reichenbach A. Müller cells in the healthy and diseased retina. Prog Retin Eye Res. 2006;25:397–424. doi: 10.1016/j.preteyeres.2006.05.003. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16839797&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 126.Stamer WD, Bok D, Hu J, Jaffe GJ, McKay BS. Aquaporin-1 channels in human retinal pigment epithelium: role in transepithelial water movement. Invest Ophthalmol Vis Sci. 2003;44:2803–8. doi: 10.1167/iovs.03-0001. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12766090&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 127.Nagelhus EA, Mathiisen TM, Ottersen OP. Aquaporin-4 in the central nervous system: cellular and subcellular distribution and coexpression with Kir4.1. Neuroscience. 2004;129:905–13. doi: 10.1016/j.neuroscience.2004.08.053. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15561407&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 128.Verkman AS, Ruiz-Ederra J, Levin MH. Functions of aquaporins in the eye. Prog Retin Eye Res. 2008;27:420–33. doi: 10.1016/j.preteyeres.2008.04.001. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=18501660&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 129.Qin Y, Fan J, Ye X, Xu G, Liu W, Da C. High salt loading alters the expression and localization of glial aquaporins in rat retina. Exp Eye Res. 2009;89:88–94. doi: 10.1016/j.exer.2009.02.017. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19268466&dopt=Abstract a. [DOI] [PubMed] [Google Scholar]
- 130.Iandiev I, Pannicke T, Biedermann B, Wiedemann P, Reichenbach A, Bringmann A. Ischemia-reperfusion alters the immunolocalization of glial aquaporins in rat retina. Neurosci Lett. 2006;408:108–12. doi: 10.1016/j.neulet.2006.08.084. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16997459&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 131.Iandiev I, Pannicke T, Reichenbach A, Wiedemann P, Bringmann A. Diabetes alters the localization of glial aquaporins in rat retina. Neurosci Lett. 2007;421:132–6. doi: 10.1016/j.neulet.2007.04.076. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17566653&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 132.Qin Y, Xu G, Fan J, Witt RE, Da C. High-salt loading exacerbates increased retinal content of aquaporins AQP1 and AQP4 in rats with diabetic retinopathy. Exp Eye Res. 2009;89:741–7. doi: 10.1016/j.exer.2009.06.020. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19596320&dopt=Abstract b. [DOI] [PubMed] [Google Scholar]
- 133.Deeg CA, Amann B, Lutz K, Hirmer S, Lutterberg K, Kremmer E, Hauck SM. Aquaporin 11, a regulator of water efflux at retinal Müller glial cell surface decreases concomitant with immune-mediated gliosis. J Neuroinflammation. 2016;13:89. doi: 10.1186/s12974-016-0554-2. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=27107718&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 134.Qin Y, Ren H, Hoffman MR, Fan J, Zhang M, Xu G. Aquaporin changes during diabetic retinopathy in rats are accelerated by systemic hypertension and are linked to the renin-angiotensin system. Invest Ophthalmol Vis Sci. 2012;53:3047–53. doi: 10.1167/iovs.11-9154. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22491408&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 135.Deliyanti D, Armani R, Casely D, Figgett WA, Agrotis A, Wilkinson-Berka JL. Retinal vasculopathy is reduced by dietary salt restriction: involvement of glia, ENaCα, and the renin-angiotensin-aldosterone system. Arterioscler Thromb Vasc Biol. 2014;34:2033–41. doi: 10.1161/ATVBAHA.114.303792. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=25012132&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 136.Amin R, Puklin JE, Frank RN. Growth-factor localization in choroidal neovascular membranes of age-related macular degeneration. Invest Ophthalmol Vis Sci. 1994;35:3178–88. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=7519180&dopt=Abstract [PubMed] [Google Scholar]
- 137.Kliffen M, Sharma HS, Mooy CM, Kerkvliet S, deJong PTVM. Increased expression of angiogenic growth factors in age-related maculopathy. Br J Ophthalmol. 1997;81:154–62. doi: 10.1136/bjo.81.2.154. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9059252&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 138.Hollborn M, Reichmuth K, Prager P, Wiedemann P, Bringmann A, Kohen L. Osmotic induction of placental growth factor in retinal pigment epithelial cells in vitro: involvement of NFAT5. Mol Biol Rep. 2016;43:803–14. doi: 10.1007/s11033-016-4016-9. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=27230578&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 139.Veltmann M, Hollborn M, Reichenbach A, Wiedemann P, Kohen L, Bringmann A. Osmotic induction of angiogenic growth factor expression in human retinal pigment epithelial cells. PLoS ONE. 2016;11:e0147312. doi: 10.1371/journal.pone.0147312. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=26800359&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 140.Bressler NM, Bressler SB, Fine SL. 2001. Neovascular (exudative) age-related macular degeneration. In: Schachat AP (ed) Retina. Mosby, St Louis, 2001; 1100–35. [Google Scholar]
- 141.Ziello JE, Jovin IS, Huang Y. Hypoxia-Inducible Factor (HIF)-1 regulatory pathway and its potential for therapeutic intervention in malignancy and ischemia. Yale J Biol Med. 2007;80:51–60. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=18160990&dopt=Abstract [PMC free article] [PubMed] [Google Scholar]
- 142.Gleadle JM, Ratcliffe PJ. Induction of hypoxia-inducible factor-1, erythropoietin, vascular endothelial growth factor, and glucose transporter-1 by hypoxia: evidence against a regulatory role for Src kinase. Blood. 1997;89:503–9. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9002952&dopt=Abstract [PubMed] [Google Scholar]
- 143.Kaur C, Sivakumar V, Foulds WS. Early response of neurons and glial cells to hypoxia in the retina. Invest Ophthalmol Vis Sci. 2006;47:1126–41. doi: 10.1167/iovs.05-0518. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16505051&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 144.De Kozak Y, Cotinet A, Goureau O, Hicks D, Thillaye-Goldenberg B. Tumor necrosis factor and nitric oxide production by resident retinal glial cells from rats presenting hereditary retinal degeneration. Ocul Immunol Inflamm. 1997;5:85–94. doi: 10.3109/09273949709085056. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=9234372&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 145.Vinores SA, Xiao WH, Aslam S, Shen J, Oshima Y, Nambu H, Liu H, Carmeliet P, Campochiaro PA. Implication of the hypoxia response element of the Vegf promoter in mouse models of retinal and choroidal neovascularization, but not retinal vascular development. J Cell Physiol. 2006;206:749–58. doi: 10.1002/jcp.20525. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16245301&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 146.Maeno E, Ishizaki Y, Kanaseki T, Hazama A, Okada Y. Normotonic cell shrinkage because of disordered volume regulation is an early prerequisite to apoptosis. Proc Natl Acad Sci USA. 2000;97:9487–92. doi: 10.1073/pnas.140216197. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=10900263&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 147.Orlov SN, Hamet P. Salt and gene expression: evidence for [Na+]i/[K+]i-mediated signaling pathways. Pflugers Arch. 2015;467:489–98. doi: 10.1007/s00424-014-1650-8. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=25479826&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 148.Ruepp B, Bohren KM, Gabbay KH. Characterization of the osmotic response element of the human aldose reductase gene promoter. Proc Natl Acad Sci USA. 1996;93:8624–9. doi: 10.1073/pnas.93.16.8624. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=8710921&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 149.Asnaghi V, Gerhardinger C, Hoehn T, Adeboje A, Lorenzi M. A role for the polyol pathway in the early neuroretinal apoptosis and glial changes induced by diabetes in the rat. Diabetes. 2003;52:506–11. doi: 10.2337/diabetes.52.2.506. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=12540628&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 150.Park J, Kim H, Park SY, Lim SW, Kim YS, Lee DH, Roh GS, Kim HJ, Kang SS, Cho GJ, Jeong BY, Kwon HM, Choi WS. Tonicity-responsive enhancer binding protein regulates the expression of aldose reductase and protein kinase Cδ in a mouse model of diabetic retinopathy. Exp Eye Res. 2014;122:13–9. doi: 10.1016/j.exer.2014.03.001. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24631337&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 151.Winges A, Garcia TB, Prager P, Wiedemann P, Kohen L, Bringmann A, Hollborn M. Osmotic expression of aldose reductase in retinal pigment epithelial cells: involvement of NFAT5. Graefes Arch Clin Exp Ophthalmol. 2016 doi: 10.1007/s00417-016-3492-x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=27628063&dopt=Abstract In press. [DOI] [PubMed] [Google Scholar]
- 152.Ryan GJ. New pharmacologic approaches to treating diabetic retinopathy. Am J Health Syst Pharm. 2007;64:S15–21. doi: 10.2146/ajhp070332. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17720889&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 153.Zhang D, Wang C, Cao S, Ye Z, Deng B, Kijlstra A, Yang P. High-salt enhances the inflammatory response by retina pigment epithelium cells following lipopolysaccharide stimulation. Mediators Inflamm. 2015;2015:197521. doi: 10.1155/2015/197521. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=26783382&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 154.Latz E, Xiao TS, Stutz A. Activation and regulation of the inflammasomes. Nat Rev Immunol. 2013;13:397–411. doi: 10.1038/nri3452. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23702978&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 155.Kerur N, Hirano Y, Tarallo V, Fowler BJ, Bastos-Carvalho A, Yasuma T, Yasuma R, Kim Y, Hinton DR, Kirschning CJ, Gelfand BD, Ambati J. TLR-independent and P2X7-dependent signaling mediate Alu RNA-induced NLRP3 inflammasome activation in geographic atrophy. Invest Ophthalmol Vis Sci. 2013;54:7395–401. doi: 10.1167/iovs.13-12500. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24114535&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 156.Marneros AG. NLRP3 inflammasome blockade inhibits VEGF-A-induced age-related macular degeneration. Cell Rep. 2013;4:945–58. doi: 10.1016/j.celrep.2013.08.002. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24012762&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 157.Prager P, Hollborn M, Steffen A, Wiedemann P, Kohen L, Bringmann A. High salt-induced priming of retinal pigment epithelial cells for NLRP3 inflammasome activation: contribution of P2Y1 receptor signaling. PLoS One. 2016 doi: 10.1371/journal.pone.0165653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 158.Notomi S, Hisatomi T, Murakami Y, Terasaki H, Sonoda S, Asato R, Takeda A, Ikeda Y, Enaida H, Sakamoto T, Ishibashi T. Dynamic increase in extracellular ATP accelerates photoreceptor cell apoptosis via ligation of P2RX7 in subretinal hemorrhage. PLoS ONE. 2013;8:e53338. doi: 10.1371/journal.pone.0053338. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23308196&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 159.Sugiyama T, Kawamura H, Yamanishi S, Kobayashi M, Katsumura K, Puro DG. Regulation of P2X7-induced pore formation and cell death in pericyte-containing retinal microvessels. Am J Physiol. 2005;288:C568–76. doi: 10.1152/ajpcell.00380.2004. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=15496477&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 160.Halterman JA, Kwon HM, Wamhoff BR. Tonicity-independent regulation of the osmosensitive transcription factor TonEBP (NFAT5). Am J Physiol Cell Physiol. 2012;302:C1–8. doi: 10.1152/ajpcell.00327.2011. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=21998140&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 161.Li XY, Cai XL, Bian PD, Hu LR. High salt intake and stroke: meta-analysis of the epidemiologic evidence. CNS Neurosci Ther. 2012;18:691–701. doi: 10.1111/j.1755-5949.2012.00355.x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22742770&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 162.Aburto NJ, Ziolkovska A, Hooper L, Elliott P, Cappuccio FP, Meerpohl JJ. Effect of lower sodium intake on health: systematic review and meta-analyses. BMJ. 2013;346:f1326. doi: 10.1136/bmj.f1326. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23558163&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 163.Chang A, Appel LJ. Public health: Effects of sodium and potassium intake on health outcomes. Nat Rev Nephrol. 2013;9:376–7. doi: 10.1038/nrneph.2013.107. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=23752886&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 164.Parikh NI, Gona P, Larson MG, Wang TJ, Newton-Cheh C, Levy D, Benjamin EJ, Kannel WB, Vasan RS. Plasma renin and risk of cardiovascular disease and mortality: the Framingham Heart Study. Eur Heart J. 2007;28:2644–52. doi: 10.1093/eurheartj/ehm399. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=17895253&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 165.EFSA Panel on Dietetic Products, Nutrition, and Allergies (NDA) Scientific Opinion on Dietary reference values for water. EFSA Journal. 2010;8:1459. [Google Scholar]
- 166.Manz F, Wentz A. Hydration status in the United States and Germany. Nutr Rev. 2005;63:S55–62. doi: 10.1111/j.1753-4887.2005.tb00154.x. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=16028572&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 167.Kant AK, Graubard BI, Atchison EA. Intakes of plain water, moisture in foods and beverages, and total water in the adult US population-nutritional, meal pattern, and body weight correlates: National Health and Nutrition Examination Surveys 1999–2006. Am J Clin Nutr. 2009;90:655–63. doi: 10.3945/ajcn.2009.27749. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=19640962&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 168.Ng SW, Ni Mhurchu C, Jebb SA, Popkin BM. Patterns and trends of beverage consumption among children and adults in Great Britain, 1986–2009. Br J Nutr. 2012;108:536–51. doi: 10.1017/S0007114511006465. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=22186747&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 169.Gibbs CR, Jackson G, Lip GY. ABC of heart failure. Non-drug management. BMJ. 2000;320:366–9. doi: 10.1136/bmj.320.7231.366. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=10657338&dopt=Abstract [DOI] [PMC free article] [PubMed] [Google Scholar]
- 170.Morgan TO. The effect of potassium and bicarbonate ions on the rise in blood pressure caused by sodium chloride. Clin Sci. 1982;63:407S–9S. [Google Scholar]
- 171.Rodrigues SL, Baldo MP, Machado RC, Forechi L, Molina M del C, Mill JG. High potassium intake blunts the effect of elevated sodium intake on blood pressure levels. J Am Soc Hypertens. 2014;8:232–8. doi: 10.1016/j.jash.2014.01.001. https://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&list_uids=24524886&dopt=Abstract [DOI] [PubMed] [Google Scholar]
- 172.Bell SJ, Anderson FL, Bistrian BR, Danner EH, Blackburn GL. Osmolality of beverages commonly provided on clear and full liquid menu. Nutr Clin Pract. 1987;2:241–4. [Google Scholar]