Abstract
Importance
Examining life expectancy by county allows for tracking geographic disparities over time and assessing factors related to these disparities. This information is potentially useful for policy makers, clinicians, and researchers seeking to reduce disparities and increase longevity.
Objective
To estimate annual life tables by county from 1980 to 2014; describe trends in geographic inequalities in life expectancy and age-specific risk of death; and assess the proportion of variation in life expectancy explained by variation in socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors.
Design, Setting, and Participants
Annual county-level life tables were constructed using small area estimation methods from deidentified death records from the National Center for Health Statistics (NCHS), and population counts from the US Census Bureau, NCHS, and the Human Mortality Database. Measures of geographic inequality in life expectancy and age-specific mortality risk were calculated. Principal component analysis and ordinary least squares regression were used to examine the county-level association between life expectancy and socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors.
Exposures
County of residence.
Main Outcomes and Measures
Life expectancy at birth and age-specific mortality risk.
Results
Counties were combined as needed to create stable units of analysis over the period 1980 to 2014, reducing the number of areas analyzed from 3142 to 3110. In 2014, life expectancy at birth for both sexes combined was 79.1 (95% uncertainty interval [UI], 79.0-79.1) years overall, but differed by 20.1 (95% UI, 19.1-21.3) years between the counties with the lowest and highest life expectancy. Absolute geographic inequality in life expectancy increased between 1980 and 2014. Over the same period, absolute geographic inequality in the risk of death decreased among children and adolescents, but increased among older adults. Socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors explained 60%, 74%, and 27% of county-level variation in life expectancy, respectively. Combined, these factors explained 74% of this variation. Most of the association between socioeconomic and race/ethnicity factors and life expectancy was mediated through behavioral and metabolic risk factors.
Conclusions and Relevance
Geographic disparities in life expectancy among US counties are large and increasing. Much of the variation in life expectancy among counties can be explained by a combination of socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors. Policy action targeting socioeconomic factors and behavioral and metabolic risk factors may help reverse the trend of increasing disparities in life expectancy in the United States.
This data analysis estimates trends in geographic inequalities in life expectancy and age-specific risk of death by US county from 1980 to 2014.
Key Points
Question
Are inequalities in life expectancy among counties in the United States growing or diminishing, and what factors can explain differences in life expectancy among counties?
Findings
In this population-based analysis, inequalities in life expectancy among counties are large and growing, and much of the variation in life expectancy can be explained by differences in socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors.
Meaning
Policy action targeting socioeconomic factors and behavioral and metabolic risk factors may help reverse the trend of increasing disparities in life expectancy in the United States.
Introduction
Studies have routinely shown that life expectancy in the United States varies geographically, in some cases dramatically. Counties are the smallest administrative unit routinely available in death registration data and represent an opportunity to explore the extent of geographic inequalities in the United States. In particular, tracking inequality at the county level over time is an important means of assessing progress toward the goal of more equitable health outcomes, as enshrined in the Healthy People 2020 objective: “Achieve health equity, eliminate disparities, and improve the health of all groups.” Moreover, county-level information on basic health outcomes is essential for appropriately targeting resources and designing and implementing health and social welfare policy at both the federal and state level.
Previous analyses of life expectancy at the county level have found large and increasing geographic disparities. However, these analyses either excluded or combined a large number of smaller counties, likely leading to an underestimation of geographic inequality. Moreover, recent research has highlighted the need to consider age-specific metrics of survival in addition to life expectancy overall. Case and Deaton identified differential trends in mortality rates among age groups, with middle age mortality rates stagnating or even increasing for certain populations, while mortality rates among older individuals continued to decline. Similarly, Currie and Schwandt identified differential trends in income-based inequalities by age, with inequalities generally declining among children and adolescents and increasing for older ages. To our knowledge, age-specific trends in geographic inequalities have not been previously described at the county level in the United States.
Beyond describing geographic variation in life expectancy, exploring what factors explain this variation might provide import insights into how to reduce inequalities and achieve more equitable health outcomes. Several previous analyses have used local data on all-cause mortality to explore this question and have identified a large number of socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors that are correlated with survival. However, these analyses have not systematically explored the extent to which county-level variation in life expectancy can be explained by the larger social and economic context of a county, the behavioral and metabolic risk profile of county residents, or the availability and quality of health care.
This analysis has 3 specific aims. First, to generate annual estimates of life expectancy and age-specific mortality risk for each county from 1980 to 2014. Second, to quantify geographic inequalities in life expectancy and age-specific mortality risks and to examine trends in geographic inequality over time. Third, to assess the extent to which variation in life expectancy is explained by variation in socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care access and quality.
Methods
Small Area Models for Estimating Life Expectancy and Age-Specific Mortality Risks
Unit of Analysis
All analyses were carried out at the county level. Counties were combined as needed to create stable units of analysis over the period 1980 to 2014, reducing the number of areas analyzed from 3142 to 3110 (eTable 1 in the Supplement). For simplicity, these units are referred to as “counties” throughout.
Data
Deidentified death records from the National Center for Health Statistics (NCHS) and population counts from the census bureau, NCHS, and the Human Mortality Database were used in this analysis. Deaths and population were tabulated by county, age group (0, 1-4, 5-9, …, 80-84, and ≥85), sex, and year. County-level information on levels of education, income, race/ethnicity, Native American reservations, and population density derived from data provided by the census bureau and NCHS was also incorporated (eTable 2 in the Supplement).
Small Area Model
Previously described and validated Bayesian small area models for estimating age-specific mortality rates by county were used in this analysis. These models incorporated 7 covariates (the proportion of the adult population who graduated high school; the proportion of the population that is Hispanic; the proportion of the population that is black; the proportion of the population that is a race other than black or white; the proportion of a county that is contained within a state or federal Native American reservation; the median household income; and the population density) and smooth mortality rates over space, time, and age to produce more stable estimates of the mortality rate in each county, year, and age group. Models were fit using the Template Model Builder Package in R version 3.2.4 (R Foundation). County-level estimates were scaled to ensure consistency with existing national-level estimates from the Global Burden of Disease study.
Life Table Construction and Metrics
The method described by Wang et al was used to extrapolate mortality rates to older ages (5-year age groups up to age 110 years). Standard demographic methods were used to construct period life tables for each county and year from the age-specific mortality rates estimated by the small area model. Life expectancy at birth (e0) and the probability of death for 5 age groups—0 to 5 (5q0); 5 to 25 (20q5), 25 to 45 (20q25), 45 to 65 (20q45), and 65 to 85 (20q65)—were extracted from these life tables.
For each measure, absolute geographic inequality was quantified as the difference between the 99th and 1st percentile level, and relative geographic inequality was quantified as the ratio of the 99th to 1st percentile level. The corresponding measures using the 90th and 10th percentile were calculated as well.
Analysis of County-Level Variation in Life Expectancy
Data
A cross-sectional data set was constructed of variables correlated with life expectancy at the county level. To maximize the number of variables included, 2009, the year with the best data coverage, was used. Three groups of variables were considered. For the first group, variables related to the broader social, economic, and demographic context of a county were identified. Specifically: the poverty rate, median household income, proportion of the adult population who graduated high school, proportion of the adult population who graduated college, the unemployment rate, proportion of the population that are black, proportion of the population that are native American, and proportion of the population that are Hispanic. For the second group, behavioral and metabolic risk factors with high attributable burden in the United States for which reliable estimates were available at the county level were identified. The prevalence of obesity, leisure–time physical inactivity, cigarette smoking, hypertension, and diabetes were included. For the third group, variables related to access to health care and health care quality were identified. Three variables were ultimately included: the percentage of the population younger than 65 years who are insured, a quality index that is a composite of variables related to primary care access and quality based on Medicare data analyzed by the Dartmouth Atlas project, and the number of physicians per capita. eTable 3 in the Supplement provides details about the data sources for each of these variables.
Regression Models
A series of bivariate ordinary least squares regression models were fitted with life expectancy at birth in 2009 as the dependent variable and each of the variables listed above as independent variables to assess the independent relationship between each of these variables and life expectancy.
Many of the variables considered were highly correlated (eFigure 1 in the Supplement), making multivariate models including all of these factors challenging to interpret due to collinearity. Therefore, a principal component analysis was conducted on each group of variables and the first principal component from each (rescaled to run from 0 to 1) was used as a composite index representing the socioeconomic and race/ethnicity, behavioral and metabolic risk, and health care characteristics, respectively, of each county. A series of ordinary least squares regression models were fitted with life expectancy at birth as the dependent variable and each of these indices separately, and then in combination, as the independent variable(s). For all models, the estimated model coefficients and the adjusted and unadjusted R2 were extracted. As a sensitivity analysis, the full multivariate regression models using all of the factors separately were also fitted.
Results
Inequalities in Life Expectancy and Age-Specific Mortality Risk
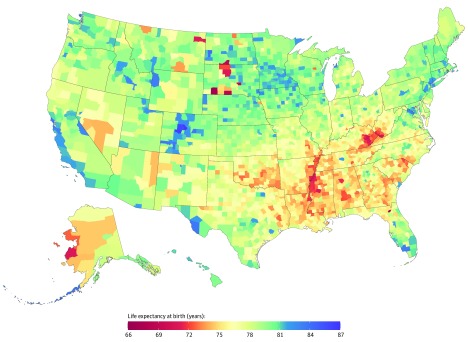
There was considerable variation in mortality risk and life expectancy at the county level in all years. In 2014, life expectancy at birth for both sexes combined at the national level was 79.1 (95% uncertainty interval [UI], 79.0-79.1) years (76.7 [95% UI, 76.7-76.8] years for men, and 81.5 [95% UI, 81.4-81.5] years for women), but there was a 6.2-year gap (95% UI, 6.1-6.2) between the 10th and 90th percentile, a 10.7-year gap (95% UI, 10.5-11.0) between the 1st and 99th percentile, and a 20.1-year gap (95% UI, 19.1-21.3) between the lowest and highest life expectancy among all counties. Several counties in South and North Dakota (typically those with Native American reservations) had the lowest life expectancy, and counties along the lower half of the Mississippi and in eastern Kentucky and southwestern West Virginia also had very low life expectancy compared with the rest of the country. In contrast, counties in central Colorado had the highest life expectancies (Figure 1). Geographical patterns in mortality risk for each age group were similar, but not identical (eFigures 2-6 in the Supplement). Results by sex and for all counties and years are available in an online visualization tool.
Figure 1. Life Expectancy at Birth by County, 2014.
Counties in South Dakota and North Dakota had the lowest life expectancy, and counties along the lower half of the Mississippi, in eastern Kentucky, and southwestern West Virginia also had very low life expectancy compared with the rest of the country. Counties in central Colorado had the highest life expectancies.
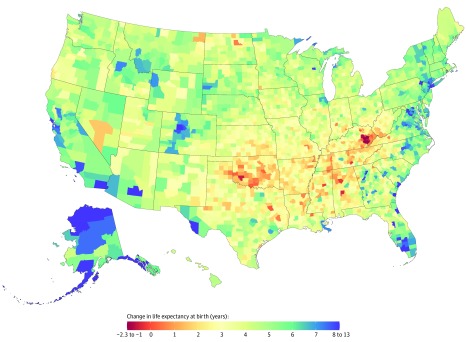
Between 1980 and 2014, life expectancy at birth for both sexes combined in the United States increased by 5.3 (95% UI, 5.3-5.4) years, from 73.8 (95% UI, 73.7-73.8) to 79.1 (95% UI, 79.0-79.1) years (6.7 [95% UI, 6.7-6.8]) years, from 70.0 [95% UI, 70.0-70.0] to 76.7 [95% UI, 76.7-76.8] for men; 3.9 [95% UI, 3.9-4.0] years, from 77.5 [95% UI, 77.5-77.6] to 81.5 [95% UI, 81.4-81.5] for women). This masks massive variation at the county level; however, counties in central Colorado, Alaska, and along both coasts experienced much larger increases, while some southern counties in states stretching from Oklahoma to West Virginia saw little, if any, improvement over this same period (Figure 2). Similarly, there was considerable variation among counties in the percent decline in the mortality risk within each age group (eFigure 7 in the Supplement). While all counties experienced declines in mortality risk for children (ages 0 to 5 years) and nearly all counties (>98%) experienced declines in the mortality risk for adolescents (ages 5 to 25 years) and older adults (ages 45 to 65 and 65 to 85 years), a significant minority of counties (11.5%) experienced increases in the risk of death between ages 25 and 45 years.
Figure 2. Change in Life Expectancy at Birth by County, 1980 to 2014.
Compared with the national average, counties in central Colorado, Alaska, and along both coasts experienced larger increases in life expectancy between 1980 and 2014, while some southern counties in states stretching from Oklahoma to West Virginia saw little, if any, improvement over this same period.
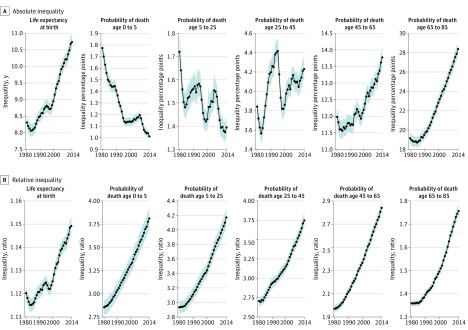
Absolute geographic inequality in life expectancy at birth increased between 1980 and 2014, with the gap between the 1st and 99th percentile increasing by 2.4 (95% UI, 2.1-2.7) years (Figure 3). However, for mortality risks, this pattern varied by age: the difference between the 1st and 99th among counties declined by 42.9% (95% UI, 40.4%-45.1%) among children (ages 0 to 5 years), by 18.9% (95% UI, 15.2%-22.7%) for adolescents (ages 5 to 25years), and increased by 10.1% (95% UI, 6.4%-14.1%), 15.0% (95% UI, 11.6%-18.4%), and 48.2% (95% UI, 42.7%-53.7%) for age groups 25 to 45 years, 45 to 65 years, and 65 to 85 years, respectively. Relative inequality rose for all age groups, likely due to the overall decrease in mortality risk over this period. Similar trends were observed when comparing the 10th and 90th percentiles (eFigure 8 in the Supplement).
Figure 3. Absolute and Relative Inequality Among Counties in Life Expectancy and Age-Specific Mortality Risks, 1980–2014.
Shaded areas along the plotted data represent 95% uncertainty intervals. Absolute geographic inequality was quantified as the difference between the 99th and first percentile level, and relative geographic inequality was quantified as the ratio of the 99th to the first percentile level.
Factors Related to Variation in Life Expectancy
Table 1 provides summary statistics for each of the variables included in the analysis of factors related to variation in life expectancy as well as the bivariate regression results. Statistically significant relationships with life expectancy were found for each variable. Detailed results of the principal component analysis are given in eTables 4 through 6 and eFigure 9 in the Supplement. The first principal component explained 42%, 79%, and 56% of the total variation in socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors, respectively. Table 2 lists the regression results based on these three indices. Socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors, when considered independently, explained 60%, 74%, and 27%, respectively, of the county-level variation in life expectancy. In combination, these 3 factors explained 74% of the variation. The effect size for the behavioral and metabolic risk factors index is similar in the combined model (Model 4) as in the model with just risk factors as a predictor (Model 2). In contrast, the effect size for socioeconomic and race/ethnicity factors is much reduced in the combined model (Model 4) compared with the model with just socioeconomic and race/ethnicity factors (Model 1), and is no longer statistically significant. The effect size for health care factors is also reduced in the combined model (Model 4) compared with the model with just health care factors (Model 3), but the effect is still statistically significant.
Table 1. Variables Included in the Regression Analysis With Summary Statistics and Bivariate Regression Results.
| Variable | Summary Statistics, Mean (SD) [Range] | Bivariate Regression Results | |
|---|---|---|---|
| Coefficient (SE) | R2 | ||
| Socioeconomic and race/Ethnicity factors | |||
| Population below the poverty line, % | 16.3 (6.4) [3.1-62.0] | −0.24 (0.005) | 0.47 |
| Median household income, log $ | 10.6 (0.2) [9.8-11.6] | 6.06 (0.130) | 0.41 |
| Graduates, age ≥25 y, % | |||
| High school | 83.7 (7.2) [46.3-98.6] | 0.20 (0.004) | 0.42 |
| College | 19.2 (8.6) [4.2-72.0] | 0.15 (0.004) | 0.34 |
| Unemployment rate, age ≥16 y, % | 9.1 (3.2) [2.1-27.4] | −0.29 (0.011) | 0.18 |
| Black population, % | 9.4 (14.7) [0-85.8] | −0.07 (0.002) | 0.24 |
| American Indian, Native Alaskan, and Native Hawaiian population, % | 2.3 (7.9) [0-97.2] | −0.06 (0.005) | 0.04 |
| Hispanic population, % | 8.1 (13.1) [0-95.9] | 0.02 (0.003) | 0.01 |
| Behavioral and metabolic risk factors, % | |||
| Obesity prevalence, age ≥20 y | 37.0 (4.3) [18.0-52.0] | −0.39 (0.006) | 0.54 |
| No leisure-time physical activity prevalence, age ≥20 y | 27.0 (5.2) [11.7-47.2] | −0.34 (0.005) | 0.62 |
| Cigarette smoking prevalence, age ≥18 y | 24.7 (4.1) [7.7-42.1] | −0.40 (0.007) | 0.54 |
| Hypertension prevalence, age ≥30 y | 39.5 (3.6) [27.9-56.4] | −0.49 (0.007) | 0.62 |
| Diabetes prevalence, age ≥20 y | 14.0 (2.4) [8.1-25.5] | −0.72 (0.011) | 0.59 |
| Health care factors | |||
| Insured population, age <65 y, % | 81.7 (5.7) [57.3-96.7] | 0.15 (0.007) | 0.14 |
| Quality index | 70.1 (11.5) [0-100] | 0.10 (0.003) | 0.28 |
| Physicians per 1000 population, No. | 1.1 (1.0) [0-4.4] | 0.53 (0.039) | 0.06 |
Abbreviation: SE, standard error.
Table 2. Multivariate Regression Results.
| Variable | Model 1a | Model 2a | Model 3a | Model 4a |
|---|---|---|---|---|
| Intercept, coefficient (SE) | 70.60 (0.10)b | 70.40 (0.08)b | 73.21 (0.13)b | 70.07 (0.09)b |
| Socioeconomic and race/ethnicity factors, coefficient (SE) | 13.13 (0.19)b | NA | NA | −0.10 (0.37) |
| Behavioral and metabolic risk factors, coefficient (SE) | NA | 13.73 (0.15)b | NA | 13.04 (0.33)b |
| Health care factors, coefficient (SE) | NA | NA | 7.88 (0.23)b | 1.37 (0.17)b |
| R2 | 0.60 | 0.74 | 0.27 | 0.74 |
| Adjusted R2 | 0.60 | 0.74 | 0.27 | 0.74 |
Abbreviations: NA, not applicable or no data available; SE, standard error.
Model 1 includes adjustment for socioeconomic and race/ethnicity factors; (ie, poverty; income; education level; unemployment; black population; American Indian, Native Alaskan, and Native Hawaiian population; and Hispanic population); Model 2, behavioral and metabolic risk factors (ie, obesity, inactivity, smoking status, hypertension, and diabetes); Model 3, health care factors (ie, insurance, quality index, number of physicians per 1000 people); and Model 4, combined (ie, all factors from all models).
P < .05.
The corresponding results from the regressions using all variables separately are presented in eTable 7 in the Supplement. The overall amount of variation explained by each group of factors, both separately and in combination, is somewhat higher, but with the same ordering among the different groups of factors: 69% for socioeconomic and race/ethnicity factors, 77% for behavioral and metabolic risk factors, 31% for health care factors, and 82% for all factors combined.
Discussion
This study found large—and increasing—geographic disparities among counties in life expectancy over the past 35 years. The magnitude of these disparities demands action, all the more urgently because inequalities will only increase further if recent trends are allowed to continue uncontested.
The finding that county-level geographic inequalities in life expectancy are large and increasing is consistent with earlier studies. Kulkarni et al reported a 15.2-year and 12.5-year gap between counties with the lowest and highest life expectancy in 2007 for men and women, respectively, while Wang et al reported a 17.8-year and 12.3-year gap in 2010 for men and women, respectively. This study estimates noticeably larger disparities: in recent years, the gap in life expectancy among counties for both sexes combined was more than 20 years. The smaller estimates in Kulkarni et al and Wang et al are likely due to their aggregation of smaller counties into larger merged county units (they analyze 2356 units compared with 3110 in this study). Chetty et al also estimated county-level life expectancy for a subset of counties, with a focus on how life expectancy varies among counties for low-income compared with high-income individuals. As in this analysis, they found substantial variation in life expectancy among counties. There are several important differences in their estimation strategy as compared with the one used in this study, however. In particular, to estimate life expectancy by income level, they use death records from the social security administration rather than from NCHS. This restricts their analysis to individuals aged 40 to 76 years who reported at least some income, and introduces some uncertainty in the county of residence for decedents who relocated after reaching retirement age (62 years). Likely as a consequence of the differences in the underlying data, as well as differences in analysis methods, the correlation between the estimates from Chetty et al and this analysis was lower than might be expected: between 0.38 and 0.65, depending on sex and income quartile.
This study expanded upon earlier analyses of county-level variation in longevity by examining mortality risk by age in addition to life expectancy. There were substantial geographic inequalities in the risk of death in each age group considered; however, the trajectory of inequalities over time differed by age: absolute geographic inequalities in the risk of death declined over the study period for children and adolescents, and increased for adults, especially those aged 65 to 85 years. This is broadly consistent with recent findings by Currie and Schwandt who analyzed age-specific mortality rates among counties grouped by income and found that inequality among income groups decreased for children and adolescents and increased for older adults from 1990 to 2010. Further research should focus on the drivers of these divergent trends. It seems likely that increases in geographic inequality in life expectancy over the past 3 decades have been driven largely by increases in geographic inequality in the risk of death in older ages. Consequently, these age groups are an especially important target for further research and intervention.
A large body of previous research documents a relationship between socioeconomic and race/ethnicity factors and various measures of survival. Consistent with this research, this study found that socioeconomic and race/ethnicity factors alone explained 60% of the variation in life expectancy. At the same time, 74% of the variation was explained by behavioral and metabolic risk factors alone, while only marginally more variation was explained by socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors combined. Furthermore, there was very little additional effect of socioeconomic and race/ethnicity factors when accounting for all 3 sets of factors simultaneously, suggesting that the association between life expectancy and socioeconomic and race/ethnicity factors at the county level is largely mediated through behavioral and metabolic risk factors.
Previous studies examining the relationship between socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and/or health care factors and some measure of survival at a substate level in the United States are not directly analogous because they use different measures of survival, different explanatory factors, and more aggregated geographic units or a subset of larger counties, but certain findings can still be compared. Cullen et al examined the relationship between 22 socioeconomic and environmental variables and the sex-specific and race-specific probability of survival to age 70 years in 510 groups of counties. Consistent with the results of this study, they found that a large proportion of the variation in survival among counties could be explained by these variables (72%-86%, depending on the sex and race). Furthermore, in a small subset of larger counties, they found that additionally considering 8 risk and health care factors increased the amount of variation explained to 86% to 90%. Davids and Jones assessed the relationship between county-level life expectancy and a small set of socioeconomic and race factors (poverty, no high school diploma, black race) and metabolic risk factors (diabetes and hypertension prevalence). As in this study, Davids and Jones found an inverse relationship between life expectancy and markers of low socioeconomic status and metabolic risk factors. Their findings differ from ours, however, in that the effect of the socioeconomic and race factors was only slightly attenuated when considering risk factors concurrently, although this may be due to the much smaller number of factors considered.
The findings on factors related to variation in life expectancy have important policy implications. In particular, policies and programs that target behavioral and metabolic risk factors have the potential to improve health in all locations but especially those that are currently most at a disadvantage, consequently reducing geographic disparities. This is not to say that policies that target socioeconomic drivers of disparities would not also be effective, but rather that there are multiple potential routes to more equitable health outcomes for federal, state, and local policy makers to consider. Furthermore, researchers now recognize that the relationship between socioeconomic status and health likely reflects causal pathways running in both directions (ie, from better health to higher socioeconomic status as well as from higher socioeconomic status to better health). Thus, policies that target inequalities in health may also in the long run be effective mechanisms for addressing inequalities in socioeconomic status as well.
This study has a number of strengths. First, this analysis used recently developed and validated small area models that have been shown to generate more precise estimates than previous methodologies. Second, this study did not exclude small counties or aggregate them beyond what was necessary to address historical boundary changes, allowing for a more complete accounting of geographic inequalities at the county level than previously available. Third, in addition to life expectancy, this study considered geographic inequalities in age-specific mortality risks that have not been previously explored. Fourth, this study is the first to systematically consider to what extent geographic inequalities in life expectancy at the county level can be explained by socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors, both independently and in combination.
Limitations
This analysis also has a number of limitations. The deaths, population, and covariates data used as the basis for estimating life expectancy by county are all subject to error. The small area models are designed to smooth across counties, years, and age groups and may in some cases over-smooth, resulting in an underestimation of geographic inequalities. This study documented increasing geographic inequality in life expectancy among counties but did not assess the extent to which these trends are a reflection of increasing inequality among individuals as opposed to changes in the geographic distribution of low-risk and high-risk individuals as a result of differential migration (eg, increasing segregation of low and high risk populations). In the regression analysis of factors related to county-level variation in life expectancy, the outcome variable (life expectancy) as well as the socioeconomic and race/ethnicity variables, behavioral and metabolic risk variables, and health care variables, are subject to measurement error. Moreover, all of the risk factor variables are themselves based on models that incorporated some socioeconomic factors as covariates, which may induce additional correlation between risk and socioeconomic factors in the regression analysis—this is unlikely to have a substantial effect however, because the relationship between risk factors and socioeconomic factors in the risk factor small area models is not imposed, but rather estimated from the data. A relatively small number of variables were used to represent the overall socioeconomic and race/ethnicity, behavioral and metabolic risk, and health care characteristics of a county, and consequently have likely not captured all relevant factors within each of these groups. There are also likely factors outside of these 3 categories that are related to geographic inequality but that were not considered in this analysis. The regression analysis is cross-sectional and can be used to draw conclusions about associations but not whether these associations are causal. Similarly, it cannot be used to assess the extent to which increasing geographic inequality in life expectancy among counties is due to change in the factors considered in the regression analysis. Furthermore, if socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors are causally related to life expectancy, this effect almost certainly plays out over the life course. However, the regression analysis only incorporates contemporaneous information about life expectancy, and these other factors and a county’s current status in terms of socioeconomic and race/ethnicity, behavioral and metabolic risk, and health care factors may not perfectly represent the lifetime experience of individuals currently living and dying in that county.
Conclusions
Geographic disparities in life expectancy among counties are large and increasing. Much of the variation in life expectancy among counties can be explained by a combination of socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors. Policy action targeting socioeconomic factors and behavioral and metabolic risk factors may help reverse the trend of increasing disparities in life expectancy in the United States.
eTable 1. Counties combined to ensure historically stable units of analysis
eTable 2. Data sources used for covariates in the small area models
eTable 3. Data sources used for the regression analysis of variation in life expectancy
eTable 4. Principal component analysis of socioeconomic and race/ethnicity factors
eTable 5. Principal component analysis of behavioral and metabolic risk factors
eTable 6. Principal component analysis of health care factors
eTable 7. Multivariate regression models
eFigure 1. Correlation matrix for variables included in the regression analysis of variation in life expectancy
eFigure 2. Probability of death between age 0 and 5 (5q0) by county, 2014
eFigure 3. Probability of death between age 5 and 25 (20q5) by county, 2014
eFigure 4. Probability of death between age 25 and 45 (20q25) by county, 2014
eFigure 5. Probability of death between age 45 and 65 (20q45) by county, 2014
eFigure 6. Probability of death between age 65 and 85 (20q65) by county, 2014
eFigure 7. Distribution of county-level declines in age-specific mortality risks, 1980-2014
eFigure 8. Absolute and relative inequality among counties in life expectancy and age-specific mortality risks, 1980-2014
eFigure 9. Index of socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors by county, 2009
References
- 1.Wei R, Anderson RN, Curtin LR, Arias E. U.S. decennial life tables for 1999-2001: state life tables. Natl Vital Stat Rep. 2012;60(9):1-66. [PubMed] [Google Scholar]
- 2.Kulkarni SC, Levin-Rector A, Ezzati M, Murray CJ. Falling behind: life expectancy in US counties from 2000 to 2007 in an international context. Popul Health Metr. 2011;9(1):16. doi: 10.1186/1478-7954-9-16 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Wang H, Schumacher AE, Levitz CE, Mokdad AH, Murray CJ. Left behind: widening disparities for males and females in US county life expectancy, 1985-2010. Popul Health Metr. 2013;11(1):8. doi: 10.1186/1478-7954-11-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.US Department of Health and Human Services Healthy People 2020 Framework. https://www.healthypeople.gov/sites/default/files/HP2020Framework.pdf. Accessed July 13, 2016.
- 5.Chetty R, Stepner M, Abraham S, et al. The association between income and life expectancy in the United States, 2001-2014. JAMA. 2016;315(16):1750-1766. doi: 10.1001/jama.2016.4226 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Case A, Deaton A. Rising morbidity and mortality in midlife among white non-Hispanic Americans in the 21st century. Proc Natl Acad Sci U S A. 2015;112(49):15078-15083. doi: 10.1073/pnas.1518393112 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Currie J, Schwandt H. Inequality in mortality decreased among the young while increasing for older adults, 1990-2010. Science. 2016;352(6286):708-712. doi: 10.1126/science.aaf1437 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Cullen MR, Cummins C, Fuchs VR. Geographic and racial variation in premature mortality in the U.S.: analyzing the disparities. PLoS One. 2012;7(4):e32930. doi: 10.1371/journal.pone.0032930 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Davids B-O, Hutchins SS, Jones CP, Hood JR. Disparities in life expectancy across US counties linked to county social factors, 2009 Community Health Status Indicators (CHSI). J Racial Ethn Health Disparities. 2014;1(1):2-11. doi: 10.1007/s40615-013-0001-3 [DOI] [Google Scholar]
- 10.Centers for Disease Control and Prevention National Vital Statistics System Multiple Cause of Death Data File. 1980-2014. https://www.cdc.gov/nchs/nvss/mortality_public_use_data.htm. Accessed March 22, 2017.
- 11.United States Census Bureau Intercensal County Estimates by Age, Sex, Race: 1980-1989. 2009. http://www.census.gov/popest/data/counties/asrh/1980s/PE-02.html. Accessed January 8, 2015.
- 12.National Center for Health Statistics Bridged-race intercensal estimates of the resident population of the United States for July 1, 1990-July 1, 1999, by year, county, single-year of age (0, 1, 2, ..., 85 years and over), bridged race, Hispanic origin, and sex. 2004. http://www.cdc.gov/nchs/nvss/bridged_race.htm. Accessed November 21, 2011.
- 13.National Center for Health Statistics Bridged-race intercensal estimates of the resident population of the United States for July 1, 2000-July 1, 2009, by year, county, single-year of age (0, 1, 2, ..., 85 years and over), bridged race, Hispanic origin, and sex. 2012. http://www.cdc.gov/nchs/nvss/bridged_race.htm. Accessed October 30, 2012.
- 14.National Center for Health Statistics Vintage 2014 postcensal estimates of the resident population of the United States (April 1, 2010, July 1, 2010-July 1, 2014), by year, county, single-year of age (0, 1, 2, ..., 85 years and over), bridged race, Hispanic origin, and sex. 2015. http://www.cdc.gov/nchs/nvss/bridged_race.htm. Accessed December 18, 2015.
- 15.University of California Berkeley, Max Planck Institute for Demographic Research. Human Mortality Database. http://www.mortality.org/. Accessed July 8, 2013.
- 16.Dwyer-Lindgren L, Bertozzi-Villa A, Stubbs RW, et al. US county-level trends in mortality rates for major causes of death, 1980-2014. JAMA. 2016;316(22):2385-2401. doi: 10.1001/jama.2016.13645 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Kristensen K, Nielsen A, Berg CW, Skaug H, Bell B. TMB: automatic differentiation and Laplace approximation. J Stat Softw. 2016;70(5):1-21. doi: 10.18637/jss.v070.i05 [DOI] [Google Scholar]
- 18.R Core Team R: A Language and Environment for Statistical Computing. Vienna, Austria: R Foundation for Statistical Computing; 2016. http://www.R-project.org/. Accessed March 31, 2016.
- 19.GBD 2015 Mortality and Causes of Death Collaborators Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet. 2016;388(10053):1459-1544. doi: 10.1016/S0140-6736(16)31012-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Wang H, Dwyer-Lindgren L, Lofgren KT, et al. Age-specific and sex-specific mortality in 187 countries, 1970-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380(9859):2071-2094. doi: 10.1016/S0140-6736(12)61719-X [DOI] [PubMed] [Google Scholar]
- 21.Preston SH, Heuveline P, Guillot M. Demography: Measuring and Modeling Population Processes. Wiley-Blackwell; 2001. [Google Scholar]
- 22.Murray CJL, Atkinson C, Bhalla K, et al. ; U.S. Burden of Disease Collaborators . The state of US health, 1990-2010: burden of diseases, injuries, and risk factors. JAMA. 2013;310(6):591-608. doi: 10.1001/jama.2013.13805 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.The Dartmouth Atlas of Health Care Selected measures of primary care access and quality. http://www.dartmouthatlas.org/tools/downloads.aspx#primary. Accessed June 16, 2016.
- 24.Mardia K. Multivariate Analysis. London, New York: Academic Press; 1979. [Google Scholar]
- 25.Rogot E, Sorlie PD, Johnson NJ. Life expectancy by employment status, income, and education in the National Longitudinal Mortality Study. Public Health Rep. 1992;107(4):457-461. [PMC free article] [PubMed] [Google Scholar]
- 26.Singh GK, Siahpush M. Widening socioeconomic inequalities in US life expectancy, 1980-2000. Int J Epidemiol. 2006;35(4):969-979. doi: 10.1093/ije/dyl083 [DOI] [PubMed] [Google Scholar]
- 27.Meara ER, Richards S, Cutler DM. The gap gets bigger: changes in mortality and life expectancy, by education, 1981-2000. Health Aff (Millwood). 2008;27(2):350-360. doi: 10.1377/hlthaff.27.2.350 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Olshansky SJ, Antonucci T, Berkman L, et al. Differences in life expectancy due to race and educational differences are widening, and many may not catch up. Health Aff (Millwood). 2012;31(8):1803-1813. doi: 10.1377/hlthaff.2011.0746 [DOI] [PubMed] [Google Scholar]
- 29.Bloom DE, Canning D. Policy forum: public health. The health and wealth of nations. Science. 2000;287(5456):1207-1209. doi: 10.1126/science.287.5456.1207 [DOI] [PubMed] [Google Scholar]
- 30.Dowd JB, Hamoudi A. Is life expectancy really falling for groups of low socio-economic status? lagged selection bias and artefactual trends in mortality. Int J Epidemiol. 2014;43(4):983-988. doi: 10.1093/ije/dyu120 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
eTable 1. Counties combined to ensure historically stable units of analysis
eTable 2. Data sources used for covariates in the small area models
eTable 3. Data sources used for the regression analysis of variation in life expectancy
eTable 4. Principal component analysis of socioeconomic and race/ethnicity factors
eTable 5. Principal component analysis of behavioral and metabolic risk factors
eTable 6. Principal component analysis of health care factors
eTable 7. Multivariate regression models
eFigure 1. Correlation matrix for variables included in the regression analysis of variation in life expectancy
eFigure 2. Probability of death between age 0 and 5 (5q0) by county, 2014
eFigure 3. Probability of death between age 5 and 25 (20q5) by county, 2014
eFigure 4. Probability of death between age 25 and 45 (20q25) by county, 2014
eFigure 5. Probability of death between age 45 and 65 (20q45) by county, 2014
eFigure 6. Probability of death between age 65 and 85 (20q65) by county, 2014
eFigure 7. Distribution of county-level declines in age-specific mortality risks, 1980-2014
eFigure 8. Absolute and relative inequality among counties in life expectancy and age-specific mortality risks, 1980-2014
eFigure 9. Index of socioeconomic and race/ethnicity factors, behavioral and metabolic risk factors, and health care factors by county, 2009