Abstract
Objective
To investigate whether improving adherence to healthy dietary patterns interacts with the genetic predisposition to obesity in relation to long term changes in body mass index and body weight.
Design
Prospective cohort study.
Setting
Health professionals in the United States.
Participants
8828 women from the Nurses’ Health Study and 5218 men from the Health Professionals Follow-up Study.
Exposure
Genetic predisposition score was calculated on the basis of 77 variants associated with body mass index. Dietary patterns were assessed by the Alternate Healthy Eating Index 2010 (AHEI-2010), Dietary Approach to Stop Hypertension (DASH), and Alternate Mediterranean Diet (AMED).
Main outcome measures
Five repeated measurements of four year changes in body mass index and body weight over follow-up (1986 to 2006).
Results
During a 20 year follow-up, genetic association with change in body mass index was significantly attenuated with increasing adherence to the AHEI-2010 in the Nurses’ Health Study (P=0.001 for interaction) and Health Professionals Follow-up Study (P=0.005 for interaction). In the combined cohorts, four year changes in body mass index per 10 risk allele increment were 0.07 (SE 0.02) among participants with decreased AHEI-2010 score and −0.01 (0.02) among those with increased AHEI-2010 score, corresponding to 0.16 (0.05) kg versus −0.02 (0.05) kg weight change every four years (P<0.001 for interaction). Viewed differently, changes in body mass index per 1 SD increment of AHEI-2010 score were −0.12 (0.01), −0.14 (0.01), and −0.18 (0.01) (weight change: −0.35 (0.03), −0.36 (0.04), and −0.50 (0.04) kg) among participants with low, intermediate, and high genetic risk, respectively. Similar interaction was also found for DASH but not for AMED.
Conclusions
These data indicate that improving adherence to healthy dietary patterns could attenuate the genetic association with weight gain. Moreover, the beneficial effect of improved diet quality on weight management was particularly pronounced in people at high genetic risk for obesity.
Introduction
Obesity is a multifactorial disorder that has a genetic predisposition but requires environmental influences for it to manifest.1 2 In the US, the past decades witnessed considerable transition of habitual dietary habits from a traditional pattern high in complex carbohydrates and fiber toward one high in sugar, fat, and animal products, which has played a key role in triggering the surge of obesity.3 4 Compelling evidence has shown that certain dietary factors such as sugar sweetened drinks, fried foods, and coffee might modify the genetic susceptibility to elevated body mass index, supporting potential interactions between genetic predisposition and overall dietary patterns on the risk of obesity.5 6 7
On the basis of scientific evidence and dietary recommendations, several diet quality scores have been developed to evaluate the healthfulness of dietary patterns.8 9 10 One such score is the Alternate Healthy Eating Index 2010 (AHEI-2010), which has been consistently associated with lower risk of chronic disease in clinical and epidemiological investigations.8 The other two commonly studied scores are the Dietary Approach to Stop Hypertension (DASH), which represents the DASH-style diet aimed at reducing blood pressure,9 and the Alternate Mediterranean Diet (AMED), which focuses on a Mediterranean dietary pattern.10 Improving adherence to healthy dietary patterns, as assessed by these three diet quality scores, has been associated with less weight gain in previous studies.11 12 13 However, no study has assessed the interactions between changes in adherence to healthy dietary patterns over time and genetic susceptibility to obesity on long term weight gain.
In this study, we prospectively examined the interactions of changes in the AHEI-2010, DASH, and AMED over up to 20 years with genetic predisposition to obesity, as evaluated by a genetic risk score based on 77 genetic variants associated with body mass index, on long term changes in body mass index and body weight in US men and women from two independent, prospective cohorts: the Nurses’ Health Study and the Health Professionals Follow-up Study.
Methods
Study design and population
The Nurses’ Health Study is a cohort of 121 701 female registered nurses aged 30-55 years at enrollment in 1976.14 The Health Professionals Follow-up Study is a cohort of 51 529 male health professionals aged 40-75 years at enrollment in 1986.15 Participants were followed with application of biennial validated questionnaires about medical history and lifestyle. For this study, the baseline year in both studies was 1986, when detailed information of diet and lifestyle was available. Between 1989 and 1990, 32 826 women in the Nurses’ Health Study provided blood samples; likewise, between 1993 and 1995, a blood sample was obtained from 18 225 men in the Health Professionals Follow-up Study. This analysis included 8828 women and 5218 men of European ancestry who had complete baseline information and available genotype data based on genome-wide association studies16 17 18 19 20 and were free from diabetes, cancer, or cardiovascular at baseline.
Assessment of body mass index and body weight
Height was assessed by questionnaires administered at enrollment, and body weight was requested by questionnaires administered at enrollment and at each follow-up. Weights reported in questionnaires and measured by technicians were highly correlated (r=0.97 in both studies) in a validation subsample.21 Body mass index was calculated as weight in kilograms divided by the square of height in meters. Changes in body mass index and weight were evaluated every four years as the differences in body mass index and weight between the beginning and the end of each four year interval, with positive differences representing weight gain and negative differences weight loss.
Assessment of healthy dietary patterns
Dietary intake information was collected by a validated 131 item semiquantitative food frequency questionnaire, administered in 1986 and every four years thereafter.22 Participants were asked how often on average they had consumed each food of a standard portion size over the previous 12 months. The responses had nine frequency categories ranging from “never or less than once per month” to “six or more times per day.” The reproducibility and validity of the food frequency questionnaire showed good correlation of food intake with that measured by multiple diet records.23 24 Diet quality scores were calculated from the food frequency questionnaires every four years. Criteria for computation of each diet quality score are given in supplementary table A.
The AHEI-2010 score was based on 11 foods and nutrients predictive of chronic disease risk,8 emphasizing higher intake of vegetables (excluding potatoes), fruits, whole grains, nuts and legumes, long chain (n-3) fats, and polyunsaturated fatty acids; moderate intake of alcohol; and lower intake of sugar sweetened drinks and fruit juice, red and processed meats, trans fat, and sodium. Each component was scored from 0 (unhealthiest) to 10 (healthiest) points, with intermediate values scored proportionally. All component scores were summed to obtain a total score ranging from 0 (non-adherence) to 110 (best adherence) points.
The DASH score was based on eight foods and nutrients that were either emphasized or de-emphasized in the DASH-style diet.9 Each component was scored from 1 to 5 points according to fifths of intake, with 5 being the best score for higher intake of vegetables, fruits, nuts and legumes, whole grains, and low fat dairy products and for lower intake of sugar sweetened drinks, red and processed meats, and sodium. The total score ranged from 8 to 40 points.
The AMED score was modified and adapted to a Mediterranean diet in a Greek population.25 This score included nine components and awarded 1 point for an intake equal to or above the cohort specific median for vegetables, fruits, whole grains, nuts, legumes, fish, and ratio of monounsaturated to saturated fat and 1 point for an intake below the cohort specific median for red and processed meat and for alcohol intake 5-15 g/d for women and 10-25 g/d for men.10 The total score ranged from 0 to 9 points, with a higher score representing higher resemblance to the Mediterranean diet.
Changes in the diet quality scores were calculated as their differences between the beginning and the end of each four year interval. Therefore, positive differences represented increased adherence to a high quality diet and negative differences decreased adherence to a high quality diet.
Genotyping and calculation of genetic risk score
We selected 77 single nucleotide polymorphisms (SNPs) that represent all 77 loci associated with body mass index identified in people of European descent (supplementary table B).26 The detailed information on SNP genotyping and imputation have been described previously.16 17 18 19 20 Most of the SNPs were genotyped or had a high imputation quality score (r2≥0.8), as assessed with the use of MACH software, version 1.0.16. No proxy SNPs were used.
Consistent with our previous study,27 we used a weighted method to calculate the genetic risk score on the basis of the 77 SNPs. Each SNP was recoded as 0, 1, or 2 according to the number of risk alleles (body mass index increasing alleles), and each SNP was weighted by its relative effect size (β coefficient) on body mass index obtained from the previous genome-wide association study.26 We calculated the genetic risk score by using the equation: GRS=(β1×SNP1+β2×SNP2+…+β77×SNP77) × (77/sum of the β coefficients), where SNPi is the risk allele number of each SNP. The genetic risk score ranges from 0 to 154, with each unit corresponding to one risk allele and higher scores indicating a higher genetic predisposition to obesity.
Assessment of covariates
Information on demographics, lifestyle, and medical history came from the biennial questionnaires. We converted leisure time physical activity to metabolic equivalent hours (METs) per week.28 The reproducibility and validity of physical activity have been described previously.29 Alcohol intake was updated on the food frequency questionnaires every four years, and total energy intake was derived from these questionnaires.
Statistical analysis
In the Nurses’ Health Study and Health Professionals Follow-up Study, data were analyzed within five intervals of four years during a follow-up of 20 years from 1986 to 2006.27 We used multivariable generalized linear models with repeated measures analyses to assess the main associations of the genetic risk score and changes in the AHEI-2010, DASH, and AMED scores with change in body mass index within each four year interval, the associations between each additional 10 risk allele and change in body mass index according to thirds of changes in the three diet quality scores, and the associations between each 1 SD increase in diet scores and change in body mass index according to genetic risk subgroups. We classified genetic risk as low risk, intermediate risk, and high risk on the basis of thirds of the genetic risk score. We tested interactions of the genetic risk score with changes in the three diet quality scores and each dietary components on change in body mass index by including the respective interaction terms in the models (for example, change in the AHEI-2010×genetic risk score), with the main effects included in the models as well. We also examined the genetic associations and interactions on weight change. We used multivariable models to adjust for age, genotyping source, baseline levels of body mass index, respective diet quality scores, physical activity, and other dietary and lifestyle factors at the beginning of each four year interval, as well as concurrent changes in these dietary and lifestyle factors within each four year interval. Missing values for diet, body mass index, and body weight were carried forward only once, and after that the follow-up was censored; for other variables, we coded missing data during any follow-up period as a missing indicator category for categorical variables (for example, smoking status) or used carried forward values for continuous variables.
In sensitivity analyses, considering potential confounding caused by age related or smoking related weight change, we assessed the genetic associations and interactions in participants younger than 65 years by censoring participants who were aged 65 years and in participants who had never smoked throughout the follow-up period. Moreover, we repeated the analyses of genetic association and interactions by using an extensive genetic risk score based on 97 SNPs comprising the 77 SNPs identified in people of European descent and 20 more SNPs identified in a combination of people of European and non-European descent (supplementary table B).26 We pooled the findings across the two cohorts by means of inverse variance weighted fixed effects meta-analysis. All reported P values are nominal and two sided. We used SAS software, version 9.4, for statistical analyses.
Patient involvement
No patients were involved in setting the research question or the outcome measures, nor were they involved in recruitment or the design and implementation of the study. No patients were asked to advice on interpretation or writing up of results. There are no plans to disseminate the results of the research to study participants or the relevant patient community.
Results
Characteristics of the two cohorts
Table 1 shows characteristics at baseline and the first four year changes in characteristics of women in the Nurses’ Health Study and men in the Health Professionals Follow-up Study. Compared with participants with relatively stable adherence to diet quality scores, participants with the greatest increases in diet quality scores seemed to have lower diet quality scores at baseline and increased physical activity and less weight gain during the first four year period. The mean genetic risk score was 69.5 (SD 5.5) in the Nurses’ Health Study and 69.3 (SD 5.6) in the Health Professionals Follow-up Study; the genetic risk score was significantly correlated with body mass index and showed normal distributions across the two cohorts (supplementary figure A).
Table 1.
Characteristics according to first four year changes in three diet quality scores in thirds among 14 046 US men and women in Nurses’ Health Study and Health Professional Follow-up Study
| Variable | Third of AHEI-2010 (score range: 0-110) change | Third of DASH (score range: 8-40) change | Third of AMED (score range: 0-9) change | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 (decrease) | 2 (stable) | 3 (increase) | 1 (decrease) | 2 (stable) | 3 (increase) | 1 (decrease) | 2 (stable) | 3 (increase) | |||
| Nurses’ Health Study (n=8828) | |||||||||||
| No of participants | 2942 | 2943 | 2943 | 3010 | 2903 | 2915 | 3189 | 2308 | 3331 | ||
| Initial diet quality score | 57.7 (11.0) | 51.9 (10.7) | 47.4 (9.8) | 26.9 (4.5) | 24.4 (4.6) | 21.9 (4.5) | 5.1 (1.6) | 4.2 (1.8) | 3.2 (1.7) | ||
| Change in diet quality score | −7.9 (4.7) | 1.0 (1.7) | 10.1 (4.9) | −4.1 (2.0) | 0.0 (0.8) | 4.1 (2.1) | −1.8 (1.0) | 0.0 (0.0) | 1.8 (1.0) | ||
| Age, years | 54.3 (6.6) | 54.1 (6.7) | 54.2 (6.6) | 54.4 (6.7) | 54.1 (6.6) | 54.0 (6.6) | 54.3 (6.6) | 54.1 (6.7) | 54.1 (6.6) | ||
| Initial BMI | 25.5 (4.7) | 25.7 (4.9) | 25.6 (4.8) | 25.5 (4.7) | 25.4 (4.8) | 25.8 (4.9) | 25.5 (4.7) | 25.6 (4.9) | 25.5 (4.9) | ||
| BMI change | 0.63 (2.04) | 0.41 (2.15) | 0.14 (2.09) | 0.63 (2.10) | 0.45 (1.98) | 0.10 (2.18) | 0.50 (2.00) | 0.45 (2.09) | 0.25 (2.20) | ||
| Initial weight, kg | 68.0 (13.6) | 68.5 (13.8) | 68.2 (13.6) | 68.0 (13.5) | 67.9 (13.6) | 68.8 (14.0) | 68.2 (13.4) | 68.5 (14.1) | 68.0 (13.7) | ||
| Weight change, kg | 1.6 (4.7) | 1.0 (4.7) | 0.3 (5.0) | 1.6 (4.7) | 1.1 (4.5) | 0.2 (5.1) | 1.2 (4.6) | 1.1 (4.9) | 0.7 (4.9) | ||
| Initial physical activity, MET-h/wk | 14.6 (20.6) | 13.9 (17.5) | 13.6 (17.9) | 14.8 (17.8) | 14.4 (21.7) | 12.9 (16.3) | 14.5 (20.3) | 14.0 (17.8) | 13.6 (17.7) | ||
| Change in physical activity, MET-h/wk | 1.0 (15.7) | 1.5 (15.8) | 2.0 (15.6) | 0.8 (15.9) | 1.4 (15.6) | 2.2 (15.6) | 0.9 (15.6) | 1.3 (15.7) | 2.1 (15.8) | ||
| Initial alcohol intake, g/d | 5.9 (9.3) | 6.3 (10.5) | 7.5 (12.9) | 6.6 (11.0) | 6.4 (10.9) | 6.6 (11.3) | 6.4 (10.3) | 6.3 (11.1) | 6.9 (11.6) | ||
| Change in alcohol intake, g/d | −0.6 (6.1) | −0.7 (5.2) | −2.0 (7.8) | −1.1 (6.7) | −0.9 (6.0) | −1.4 (6.7) | −1.2 (6.4) | −0.9 (6.2) | −1.2 (6.8) | ||
| Current smoker, No (%) | 461 (15.7) | 495 (16.8) | 572 (19.4) | 426 (14.2) | 538 (18.5) | 564 (19.4) | 487 (15.3) | 413 (17.9) | 628 (18.9) | ||
| Remained current smoker, No (%) | 358 (12.2) | 363 (12.3) | 397 (13.5) | 332 (11.0) | 399 (13.7) | 387 (13.3) | 376 (11.8) | 303 (13.1) | 439 (13.2) | ||
| Total energy intake, kcal/d | 1814 (519) | 1806 (540) | 1731 (491) | 1821 (496) | 1790 (552) | 1739 (502) | 1839 (510) | 1810 (545) | 1713 (500) | ||
| Change in total energy intake, kcal/d | −16 (451) | 0 (408) | −26 (441) | −46 (449) | −12 (405) | 18 (443) | −126 (435) | −17 (389) | 96 (435) | ||
| Genetic risk score | 69.3 (5.5) | 69.6 (5.5) | 69.4 (5.5) | 69.3 (5.5) | 69.4 (5.5) | 69.6 (5.5) | 69.5 (5.4) | 69.4 (5.6) | 69.4 (5.5) | ||
| Health Professionals Follow-up Study (n=5218) | |||||||||||
| No of participants | 1739 | 1740 | 1739 | 1526 | 1922 | 1770 | 1842 | 1599 | 1777 | ||
| Initial diet quality score | 57.2 (11.7) | 52.5 (11.1) | 47.9 (10.5) | 26.6 (4.8) | 24.1 (4.8) | 21.6 (4.6) | 5.2 (1.8) | 4.3 (1.9) | 3.4 (1.7) | ||
| Change in diet quality score | −7.9 (4.7) | 0.8 (1.5) | 10.0 (4.9) | −3.9 (2.0) | 0.0 (0.7) | 4.2 (2.2) | −1.8 (1.0) | 0.0 (0.0) | 1.7 (1.0) | ||
| Age, years | 55.2 (8.7) | 54.7 (8.6) | 55.4 (8.6) | 55.0 (9.0) | 54.8 (8.4) | 55.5 (8.5) | 55.3 (8.7) | 54.7 (8.8) | 55.3 (8.4) | ||
| Initial BMI | 25.8 (3.3) | 25.9 (3.4) | 25.7 (3.1) | 25.6 (3.3) | 25.7 (3.3) | 26.0 (3.2) | 25.7 (3.3) | 25.9 (3.5) | 25.7 (3.1) | ||
| BMI change | 0.35 (1.35) | 0.21 (1.29) | 0.04 (1.29) | 0.36 (1.33) | 0.26 (1.23) | 0.00 (1.37) | 0.28 (1.34) | 0.20 (1.28) | 0.12 (1.33) | ||
| Initial weight, kg | 82.1 (12.3) | 81.9 (12.2) | 81.1 (11.5) | 81.2 (12.0) | 81.8 (12.2) | 82.1 (11.8) | 81.8 (12.1) | 82.1 (12.5) | 81.3 (11.5) | ||
| Weight change, kg | 1.1 (3.8) | 0.7 (3.8) | 0.1 (3.8) | 1.1 (3.7) | 0.8 (3.7) | 0.1 (4.0) | 0.9 (3.8) | 0.6 (3.8) | 0.4 (3.9) | ||
| Initial physical activity, MET-h/wk | 20.5 (27.5) | 19.8 (24.1) | 19.3 (22.5) | 22.1 (28.4) | 19.8 (24.6) | 17.9 (21.3) | 20.3 (25.1) | 20.4 (27.3) | 18.8 (22.0) | ||
| Change in physical activity, MET-h/wk | 16.0 (32.9) | 15.6 (30.8) | 18.2 (34.0) | 15.6 (33.6) | 15.6 (31.4) | 18.5 (33.0) | 17.2 (34.5) | 14.9 (31.3) | 17.5 (31.7) | ||
| Initial alcohol intake, g/d | 11.5 (14.1) | 12.6 (15.9) | 14.1 (18.7) | 12.6 (15.6) | 12.7 (16.9) | 12.9 (16.6) | 12.4 (15.3) | 12.7 (16.9) | 13.1 (17.1) | ||
| Change in alcohol intake, g/d | −0.1 (8.9) | −0.9 (7.4) | −2.9 (10.8) | −1.6 (10.0) | −0.9 (7.9) | −1.5 (9.8) | −1.5 (9.6) | −1.1 (8.5) | −1.4 (9.5) | ||
| Current smoker, No (%) | 161 (9.3) | 158 (9.1) | 140 (8.1) | 119 (7.8) | 174 (9.1) | 166 (9.4) | 165 (9.0) | 136 (8.5) | 158 (8.9) | ||
| Remained current smoker, No (%) | 119 (6.8) | 112 (6.4) | 91 (5.2) | 82 (5.4) | 122 (6.4) | 118 (6.7) | 117 (6.4) | 95 (5.9) | 110 (6.2) | ||
| Total energy intake, kcal/d | 2051 (623) | 2056 (630) | 2003 (597) | 2068 (613) | 2044 (646) | 2001 (588) | 2083 (619) | 2057 (638) | 1971 (592) | ||
| Change in total energy intake, kcal/d | −71 (533) | −69 (428) | −101 (507) | −138 (522) | −55 (450) | −58 (504) | −214 (499) | −63 (450) | 43 (485) | ||
| Genetic risk score | 69.2 (5.7) | 69.3 (5.5) | 69.5 (5.4) | 69.4 (5.5) | 69.2 (5.6) | 69.4 (5.6) | 69.3 (5.5) | 69.3 (5.6) | 69.5 (5.6) | ||
Plus-minus values are mean (SD) for variables of baseline (1986) and first four year changes (1986-90) in Nurses’ Health Study and Health Professional Follow-up Study.
AHEI-2010=Alternate Healthy Eating Index 2010; AMED=Alternate Mediterranean Diet; BMI=body mass index; DASH=Dietary Approach to Stop Hypertension; MET=metabolic equivalent.
Changes in body mass index and body weight according to categories of genetic risk and changes in diet quality scores in thirds
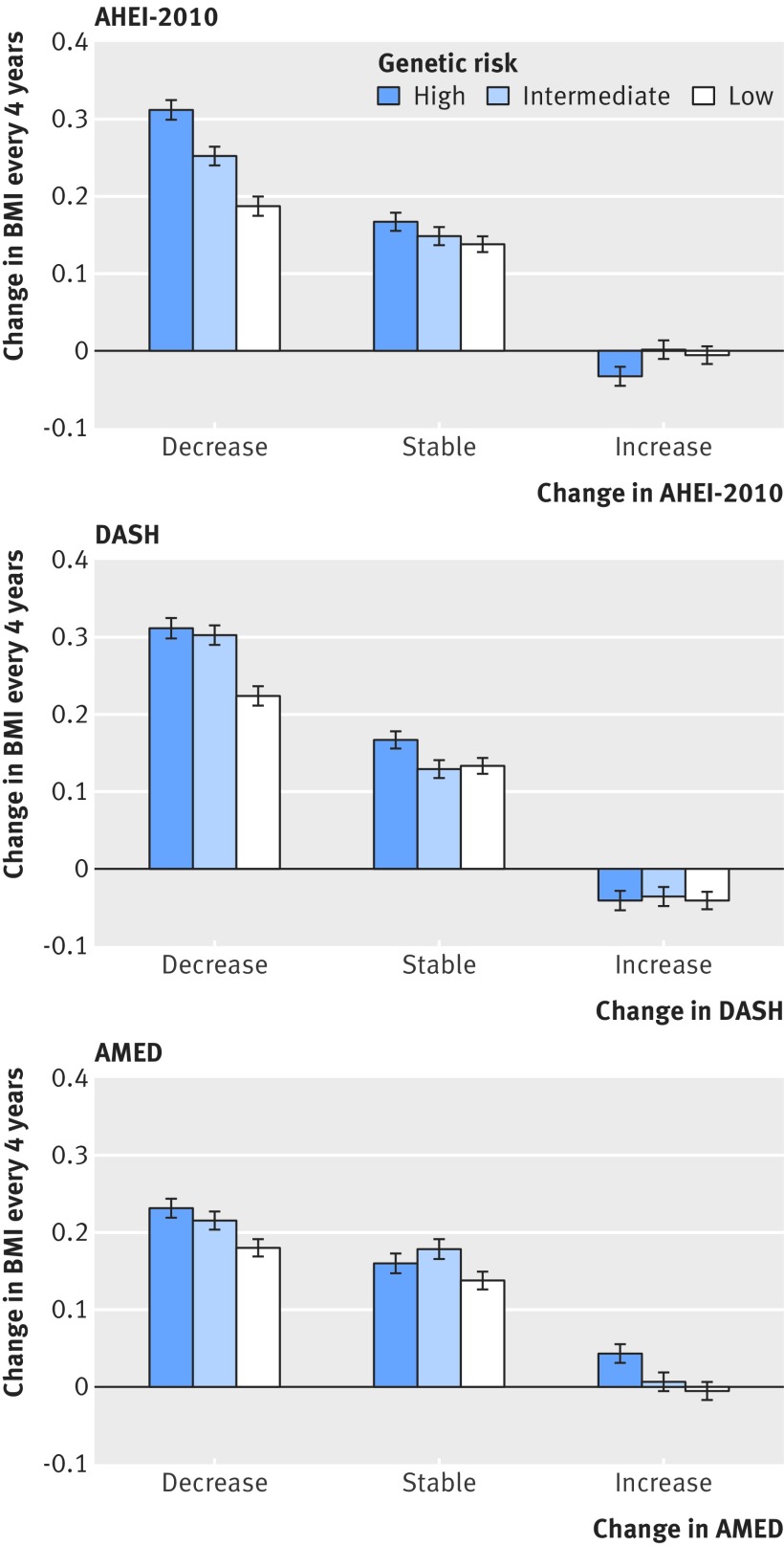
In general, the genetic risk score was associated with increases in body mass index and body weight every four years: in the two cohorts combined, each additional 10 risk allele was associated with 0.02 (SE 0.01) increase in body mass index and 0.05 (SE 0.03) kg increase in body weight (supplementary tables C and D). The difference in body mass index change between people at high genetic risk and those at low genetic risk was more prominent among participants with decreased adherence to the AHEI-2010 (0.12) than those with increased adherence to the AHEI-2010 (−0.03); a similar pattern was observed for DASH but not for AMED (fig 1). When viewed jointly, the genetic associations with change in body mass index attenuated in participants who increased adherence to the AHEI-2010 and DASH; from another perspective, the inverse associations of increased adherence to the AHEI-2010 and DASH with change in body mass index were more prominent in participants at high genetic risk. Similar results were observed for weight change (supplementary figure B).
Fig 1.
Pooled, multivariable adjusted means of change in body mass index (BMI) every four years, according to categories of genetic risk and changes in diet quality scores in thirds. AHEI-2010=Alternate Healthy Eating Index 2010; AMED=Alternate Mediterranean Diet; DASH=Dietary Approach to Stop Hypertension. Histograms and bars are means and SEs. Decreased, stable, and increased adherence to each diet quality score refers to third 1, 2, and 3 of each score, respectively. Data were derived from repeated measurements analyses for women in Nurses’ Health Study (five intervals of four years from 1986 to 2006) and men in Health Professionals Follow-up Study (five intervals of four years from 1986 to 2006). Results were adjusted for same set of variables as in table 2. Results for two cohorts were pooled by means of inverse variance weighted fixed effects meta-analysis
Genetic association with changes in body mass index and body weight according to changes in diet quality scores in thirds
The genetic associations with change in body mass index were significantly attenuated with increased AHEI-2010 score in the Nurses’ Health Study (P=0.001 for interaction) and Health Professionals Follow-up Study (P=0.005 for interaction) (table 2). In the combined cohorts, changes in body mass index per 10 risk allele increment were 0.07 (SE 0.02) among participants in the lowest third with decreased AHEI-2010 score and −0.01 (0.02) among those in the highest third with increased AHEI-2010 score (P<0.001 for interaction), corresponding to a weight change of 0.16 (0.05) kg versus −0.02 (0.05) kg (supplementary table E). Similarly, changes in body mass index per 10 risk allele increment were 0.04 (0.02) among participants with decreased DASH score and 0.01 (0.02) among those with increased DASH score (P=0.01 for interaction); corresponding weight change was 0.07 (0.06) kg versus −0.01 (0.06) kg. No clear interaction pattern was observed for AMED (P=0.33 for interaction).
Table 2.
Body mass index change every four years per 10 risk allele increment, according changes in diet quality scores in thirds*
| Analysis | Thirds of changes in diet quality scores | P for interaction | ||
|---|---|---|---|---|
| 1 (decrease) | 2 (stable) | 3 (increase) | ||
| AHEI-2010 | ||||
| NHS | 0.06 (0.03) | −0.01 (0.03) | 0.01 (0.03) | 0.001 |
| HPFS | 0.08 (0.03) | 0.03 (0.03) | −0.02 (0.03) | 0.005 |
| Pooled results† | 0.07 (0.02) | 0.02 (0.02) | −0.01 (0.02) | <0.001 |
| DASH | ||||
| NHS | 0.03 (0.03) | 0.02 (0.03) | 0.01 (0.03) | 0.008 |
| HPFS | 0.04 (0.03) | 0.04 (0.03) | 0.01 (0.03) | 0.16 |
| Pooled results† | 0.04 (0.02) | 0.03 (0.02) | 0.01 (0.02) | 0.01 |
| AMED | ||||
| NHS | 0.01 (0.03) | 0.01 (0.03) | 0.06 (0.03) | 0.50 |
| HPFS | 0.05 (0.03) | 0.01 (0.03) | 0.02 (0.03) | 0.11 |
| Pooled results† | 0.03 (0.02) | 0.01 (0.02) | 0.04 (0.02) | 0.33 |
AHEI-2010=Alternate Healthy Eating Index 2010; AMED=Alternate Mediterranean Diet; DASH=Dietary Approach to Stop Hypertension; HPFS=Health Professionals Follow-up Study; NHS=Nurses’ Health Study.
Plus-minus values are β coefficient (SE). Data were derived from repeated measurements analyses for women in NHS (five intervals of four years from 1986 to 2006) and men in HPFS (five intervals of four years from 1986 to 2006). Results were adjusted for age, genotyping source, baseline body mass index (fifths), and respective baseline diet quality scores (fifths); baseline lifestyle factors at beginning of each four year period: physical activity (fifths), alcohol intake (0, 0.1-4.9, 5-9.9, 10-14.9, ≥15 g/d; only for DASH score), smoking status (never, former, current), and total energy intake (fifths); and concurrent changes in lifestyle factors: physical activity (fifths), alcohol intake (fifths, only for DASH score), smoking status (never to never, never to current, past to past, past to current, current to past, current to current), and total energy intake (fifths).
Results for two cohorts were pooled by means of inverse variance weighted fixed effects meta-analysis (all P for heterogeneity>0.05).
Association of changes in diet quality scores with changes in body mass index and body weight according to genetic risk
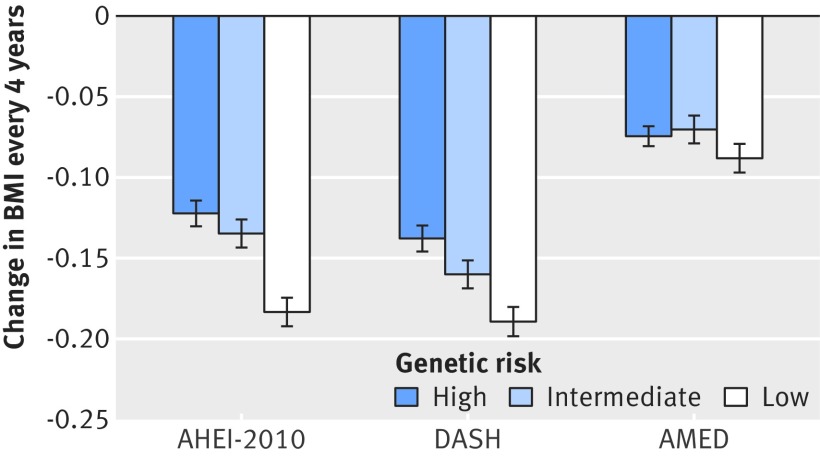
Increase in each diet quality score was associated with decreases in body mass index and body weight every four years in total participants (supplementary tables C and D), and such association seemed to be more prominent in participants at high genetic risk (fig 2). Changes in body mass index per 1 SD increase in AHEI-2010 score were −0.12 (SE 0.01), −0.14 (0.01), and −0.18 (0.01) among participants at low, intermediate, and high genetic risk, respectively, corresponding to weight changes of −0.35 (0.03), −0.36 (0.04), and −0.50 (0.04) kg, respectively (supplementary figure C). Similarly, changes in body mass index per 1 SD increase in DASH score were −0.14 (0.01), −0.16 (0.01), and −0.19 (0.02) across these genetic risk subgroups. Differences in body mass index changes associated with change in the AMED across these subgroups were not evident. Similar results were observed for weight changes (supplementary figure C).
Fig 2.
Pooled, multivariable adjusted body mass index (BMI) change every four years per 1 SD increment of each diet quality score, according to genetic risk. AHEI-2010=Alternate Healthy Eating Index 2010; AMED=Alternate Mediterranean Diet; DASH=Dietary Approach to Stop Hypertension. Histograms and bars are β coefficients and SEs. Value of 1 SD: AHEI-2010: 8.38; DASH: 3.71; AMED: 1.72. Data were derived from repeated measurements analyses for women in Nurses’ Health Study (five intervals of four years from 1986 to 2006) and men in Health Professionals Follow-up Study (five intervals of four years from 1986 to 2006). Results were adjusted for same set of variables as in table 2. Results for two cohorts were pooled by means of inverse variance weighted fixed effects meta-analysis
Modifying effect of diet quality scores and dietary components on genetic associations with changes in body mass index and body weight
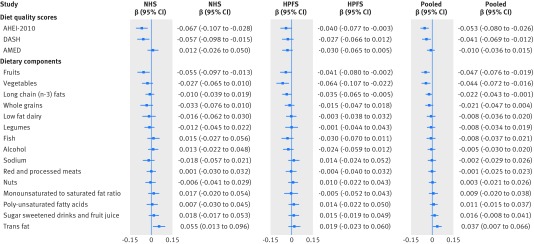
In the combined cohorts, increases in AHEI-2010 and DASH scores significantly attenuated the genetic association with change in body mass index: each 1 SD increase in the AHEI-2010 and DASH score was associated with −0.05 (95% confidence interval −0.08 to −0.03; P<0.001 for interaction) and −0.04 (−0.07 to −0.01; P=0.005 for interaction) change in body mass index attributed to each additional 10 risk allele, respectively (fig 3). Such interaction effect was not statistically significant for AMED. For individual dietary components, each 1 SD increases in fruits (β −0.05, −0.08 to −0.02; P=0.001 for interaction), vegetables (−0.04, −0.07 to −0.02; P=0.002 for interaction), long chain (n-3) fats (−0.02, −0.04 to −0.001; P=0.037 for interaction), and trans fat (0.04, 0.01 to 0.07; P=0.015 for interaction) showed nominally significant interactions with the genetic risk score per additional 10 risk allele on change in body mass index. Similar interactions for weight change are shown in supplementary figure D.
Fig 3.
Interaction of genetic risk score with changes in diet quality scores and dietary components on change in body mass index (BMI) every four years. AHEI-2010=Alternate Healthy Eating Index 2010; AMED=Alternate Mediterranean Diet; DASH=Dietary Approach to Stop Hypertension; NHS=Nurses’ Health Study; HPFS=Health Professionals Follow-up Study. Histograms and bars are β coefficients and 95% CIs for interactions between genetic risk score (per 10 risk allele) and changes in diet quality scores and dietary components (per 1 SD increment) on BMI change. Value of 1 SD: AHEI-2010: 8.38; DASH: 3.71; AMED: 1.72; fruits (servings/d): 1.12; vegetables (servings/d): 2.06; long chain (n-3) fats (mg/d): 300.7; whole grains (g/d): 17.34; low fat dairy (servings/d): 0.88; legumes (servings/d): 0.27; fish (servings/d): 0.38; alcohol (drinks/d): 0.70; sodium (mg/d): 3.10; red and processed meats (servings/d): 0.26; nuts (servings/d): 0.52; ratio of monounsaturated to saturated fat: 0.21; polyunsaturated fatty acids (% of energy): 1.68; sugar sweetened drinks and fruit juice (servings/d): 0.92; trans fat (% of energy): 0.01. Data were derived from repeated measurements analyses for women in Nurses’ Health Study (five intervals of four years from 1986 to 2006) and men in Health Professionals Follow-up Study (five intervals of four years from 1986 to 2006). Results were adjusted for same set of variables as in table 2. Results for two cohorts were pooled by means of inverse variance weighted fixed effects meta-analysis
Sensitivity analyses
In participants younger than 65 years and in those who had never smoked throughout the follow-up period, we observed similar but weaker results for genetic associations and interactions between the genetic risk score and changes in diet quality scores on change in body mass index (supplementary tables F and G). Moreover, analyses using the genetic risk score comprising 97 SNPs yielded consistent results (supplementary table H).
Discussion
In this study, we found consistent interactions between changes in diet quality scores and genetic predisposition related to long term changes in body mass index and body weight in two independent prospective cohorts of US women and men. Our findings show that improving adherence to healthy dietary patterns assessed according to the AHEI-2010 and DASH could significantly attenuate the genetic association with increases in body mass index and body weight. Viewed differently, improving diet quality over time was associated with decreases in body mass index and body weight, and such favorable effect was more prominent in people at high genetic risk for obesity than in those with low genetic risk.
Results in relation to other studies
The dramatic alternations in dietary patterns over the past decades have paralleled the rapid rise in the prevalence of obesity in the US.3 4 Emerging evidence supports a protective effect of improved adherence to healthy dietary patterns on weight gain and other health outcomes such as cardiovascular disease and total and cardiovascular disease mortality.11 12 13 30 31 In previous studies, we have shown that dietary factors such as sugar sweetened drinks and fried foods could amplify the genetic associations with elevated body mass index.5 6 Similar interactions have also been reported by another group.32 Our findings in this study are consistent with these previous reports and for the first time indicate that improving adherence to healthy dietary patterns might diminish the genetic association with weight gain. Here, we evaluated healthy dietary patterns by diet quality scores. Instead of considering individual diets in isolation, diet quality scores provide comprehensive measures of diets incorporating nutrients and foods and therefore represent a broader picture of dietary intake.33 34 In this study, the AHEI-2010 showed the most significant interaction with genetic predisposition to obesity on changes in body mass index and body weight, and we also found a similar interaction pattern for DASH but not for AMED. When evaluating changes over time, the continuous scale and wider range of the AHEI-2010 may allow for greater sensitivity to differentiate dietary changes; in contrast, the wider scale and narrower range of AMED may limit its ability to detect the differences in dietary changes. Additionally, the AHEI-2010 captured all four dietary components (fruits, vegetables, long chain (n-3) fats, and trans fat) that contributed to significant interactions with the genetic risk score at a nominal significance threshold, whereas DASH and AMED each captured two, which might also account for the observed differences between the three diet quality scores.
From another point of view, our findings indicate that people with a greater genetic predisposition seem to be more susceptible to the favorable effect of improving diet quality on weight management. Our results are in line with the findings of a meta-analysis (including 6951 participants from 10 studies) showing that people carrying the homozygous FTO allele predisposing to obesity may lose more weight than non-carriers through diet and lifestyle interventions.35 In a more recent meta-analysis of 9563 participants from eight randomized controlled trials, each copy of the FTO obesity predisposing allele was associated with non-significant reductions in body mass index (−0.02, 95% confidence interval −0.13 to 0.09) and body weight (−0.04, −0.34 to 0.26, kg) (indicative of gene by treatment interactions) after weight loss intervention in the treatment versus control arm.36 Of note, the effect sizes of gene by treatment (dietary, physical activity, or drug based intervention) interaction in this meta-analysis are in similar ranges to the effect sizes of gene by dietary patterns interaction shown in our study, supporting the generalization of the effect sizes yielded by our study.
Biological plausibility
The precise mechanisms underlying the observed interactions remain unclear. The beneficial bioactivities of healthy dietary patterns, such as balancing energy intake, regulating metabolism, and reducing cardiometabolic risk,37 38 may partly explain their modifying effect on genetic predisposition to weight gain. In addition, several genes associated with body mass index have been shown to be involved in central appetite regulation and energy homeostasis,26 which may also be responsible for the observed interactions. However, we cannot exclude the involvement of other biological pathways, and future functional studies are needed to provide biological insights into the gene by diet interactions on weight change.
Strengths and limitations of study
The strengths of our study include the cross validation from two independent prospective cohorts of men and women, the well validated measures of dietary factors and body weight within five repeated four year periods of a 20 year follow-up, and the reliable findings improved by several sensitivity analyses. Notably, we evaluated changes in diet quality scores and changes in body mass index and body weight during the same four year intervals in discrete periods, because this change-on-change analytic approach has been shown to generate more robust, consistent, and biologically plausible relations between diet and long term weight change than the approaches of prevalent diet with weight change (prevalent analysis) or change in diet with weight change in the subsequent four years (lagged changes analysis).39
Our study also has several potential limitations. Firstly, although we have carefully controlled for baseline and concurrent changes of lifestyle and dietary factors in the analyses, unmeasured or unknown confounders may also exist. Secondly, because adherence to healthy dietary patterns was not randomized, the association between dietary factors and weight change may not imply a causal relation. Thirdly, the results could be underestimated by potential reverse causality; for example, people who gained weight might tend to adopt healthier eating patterns to lose weight. Fourthly, our study was restricted to health professionals of European descent in the US, and the generalizability of our findings should be tested in other demographic and racial/ethnic populations.
Implications of findings
Our results suggest that weight gain associated with genetic predisposition can be at least partly counteracted by improving adherence to healthy dietary patterns. Importantly, for people who are genetically predisposed to obesity, improving adherence to a healthy diet is more likely to lead to greater weight loss. Our findings support recommendation of adherence to healthy dietary patterns,37 particularly for people at high genetic risk of obesity. The observed genetic effects were modest in magnitude, compared with lifestyle risk factors. Of note, the changes in body mass index and body weight reported in our study were changes per four years. Because changes in body mass index and body weight are essentially cumulative during the life course, the long term effect size would be substantial. Furthermore, long term, dramatic weight loss is difficult to achieve, even in the context of weight loss interventions. Therefore, even modest weight loss or simply maintaining weight from adulthood onward, compared with gaining weight, may have a substantial effect on population health.
Conclusion
Our study provides reproducible evidence from two prospective cohorts of US men and women that improving adherence to healthy dietary patterns could attenuate the genetic association with body mass index increment and weight gain, and the beneficial effect of improving diet quality on weight management was more prominent in people at high genetic risk. Our findings highlight the importance of improving adherence to a healthy diet in the prevention of weight gain, particularly in people genetically predisposed to obesity.
What is already known on this topic
Improving adherence to healthy dietary patterns, as assessed by various diet scores, has been associated with weight loss in several studies
No study has assessed the interactions between changes in these diet quality scores and genetic predisposition to obesity in relation to long term changes in body mass index and body weight
What this study adds
Improving adherence to healthy dietary patterns as assessed by the Alternate Healthy Eating Index 2010 and Dietary Approach to Stop Hypertension can counteract part of gene related, long term weight gain
People at high genetic risk for obesity are more susceptible to the beneficial effect of improving diet quality on weight loss
This underlines the importance of improving adherence to healthy dietary patterns in the prevention of weight gain, especially in people with greater genetic predisposition to obesity
Acknowledgments
We thank all the participants of the Nurses’ Health Study and the Health Professionals Follow-up Study for their continued cooperation.
Web Extra.
Extra material supplied by the author
Supplementary tables and figures
Contributors: TW and LQ conceived and designed the study. EBR, JEM, FBH, WCW, and LQ acquired the data. TW did the analyses and drafted the manuscript. All authors contributed to the interpretation of the results and critical revision of the manuscript for important intellectual content and approved the final version of the manuscript. LQ is the guarantor.
Funding: The cohorts were supported by grants R01 CA49449, UM1 CA186107, and UM1 CA167552 from the National Institutes of Health. This study was supported by grants from the National Heart, Lung, and Blood Institute (HL071981, HL034594, HL126024, HL35464), the National Institute of Diabetes and Digestive and Kidney Diseases (DK091718, DK100383, DK078616), the National Eye Institute (EY015473), the National Human Genome Research Institute (U01 HG004728), and the National Institute of Health (CA87969, CA49449, CA55075, CA167552). TW is supported by the National Natural Science Foundation of China (81500610). LQ is supported by the American Heart Association Scientist Development Award (0730094N). All investigators are independent from funders.
Competing interests: All authors have completed the ICMJE uniform disclosure form at www.icmje.org/coi_disclosure.pdf and declare: no support from any organization for the submitted work other than that described above; no financial relationships with any organizations that might have an interest in the submitted work in the previous three years; no other relationships or activities that could appear to have influenced the submitted work.
Ethical approval: The study protocol was approved by the institutional review boards of Brigham and Women’s Hospital and Harvard T.H. Chan School of Public Health. The completion of the self administered questionnaire was considered to imply informed consent.
Data sharing: Data, the statistical code, questionnaires, and technical processes are available from the corresponding author at nhlqi@channing.harvard.edu.
Transparency statement: LQ affirms that the manuscript is an honest, accurate, and transparent account of the study being reported; that no important aspects of the study have been omitted; and that any discrepancies from the study as planned (and, if relevant, registered) have been explained.
References
- 1. Qi L, Cho YA. Gene-environment interaction and obesity. Nutr Rev 2008;66:684-94. 10.1111/j.1753-4887.2008.00128.x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. El-Sayed Moustafa JS, Froguel P. From obesity genetics to the future of personalized obesity therapy. Nat Rev Endocrinol 2013;9:402-13. 10.1038/nrendo.2013.57 [DOI] [PubMed] [Google Scholar]
- 3. Ezzati M, Riboli E. Behavioral and dietary risk factors for noncommunicable diseases. N Engl J Med 2013;369:954-64. 10.1056/NEJMra1203528 [DOI] [PubMed] [Google Scholar]
- 4. Swinburn BA, Caterson I, Seidell JC, James WP. Diet, nutrition and the prevention of excess weight gain and obesity. Public Health Nutr 2004;7(1A):123-46. [DOI] [PubMed] [Google Scholar]
- 5. Qi Q, Chu AY, Kang JH, et al. Sugar-sweetened beverages and genetic risk of obesity. N Engl J Med 2012;367:1387-96. 10.1056/NEJMoa1203039 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Qi Q, Chu AY, Kang JH, et al. Fried food consumption, genetic risk, and body mass index: gene-diet interaction analysis in three US cohort studies. BMJ 2014;348:g1610. 10.1136/bmj.g1610 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Wang T, Huang T, Kang JH, et al. Habitual coffee consumption and genetic predisposition to obesity: gene-diet interaction analyses in three US prospective studies. BMC Med 2017;15:97. 10.1186/s12916-017-0862-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Chiuve SE, Fung TT, Rimm EB, et al. Alternative dietary indices both strongly predict risk of chronic disease. J Nutr 2012;142:1009-18. 10.3945/jn.111.157222 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Fung TT, Chiuve SE, McCullough ML, Rexrode KM, Logroscino G, Hu FB. Adherence to a DASH-style diet and risk of coronary heart disease and stroke in women. Arch Intern Med 2008;168:713-20. 10.1001/archinte.168.7.713 [DOI] [PubMed] [Google Scholar]
- 10. Fung TT, Rexrode KM, Mantzoros CS, Manson JE, Willett WC, Hu FB. Mediterranean diet and incidence of and mortality from coronary heart disease and stroke in women. Circulation 2009;119:1093-100. 10.1161/CIRCULATIONAHA.108.816736 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Fung TT, Pan A, Hou T, et al. Long-term change in diet quality is associated with body weight change in men and women. J Nutr 2015;145:1850-6. 10.3945/jn.114.208785 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Tobias DK, Zhang C, Chavarro J, et al. Healthful dietary patterns and long-term weight change among women with a history of gestational diabetes mellitus. Int J Obes (Lond) 2016;40:1748-53. 10.1038/ijo.2016.156 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Cespedes Feliciano EM, Tinker L, Manson JE, et al. Change in Dietary Patterns and Change in Waist Circumference and DXA Trunk Fat Among Postmenopausal Women. Obesity (Silver Spring) 2016;24:2176-84. 10.1002/oby.21589 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Willett WC, Stampfer MJ, Colditz GA, Rosner BA, Hennekens CH, Speizer FE. Dietary fat and the risk of breast cancer. N Engl J Med 1987;316:22-8. 10.1056/NEJM198701013160105 [DOI] [PubMed] [Google Scholar]
- 15. Rimm EB, Giovannucci EL, Willett WC, et al. Prospective study of alcohol consumption and risk of coronary disease in men. Lancet 1991;338:464-8. 10.1016/0140-6736(91)90542-W [DOI] [PubMed] [Google Scholar]
- 16. Hunter DJ, Kraft P, Jacobs KB, et al. A genome-wide association study identifies alleles in FGFR2 associated with risk of sporadic postmenopausal breast cancer. Nat Genet 2007;39:870-4. 10.1038/ng2075 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Qi L, Cornelis MC, Kraft P, et al. Meta-Analysis of Glucose and Insulin-related traits Consortium (MAGIC) Diabetes Genetics Replication and Meta-analysis (DIAGRAM) Consortium Genetic variants at 2q24 are associated with susceptibility to type 2 diabetes. Hum Mol Genet 2010;19:2706-15. 10.1093/hmg/ddq156 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Cornelis MC, Monda KL, Yu K, et al. Genome-wide meta-analysis identifies regions on 7p21 (AHR) and 15q24 (CYP1A2) as determinants of habitual caffeine consumption. PLoS Genet 2011;7:e1002033. 10.1371/journal.pgen.1002033 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Wiggs JL, Kang JH, Yaspan BL, et al. GENEVA Consortium Common variants near CAV1 and CAV2 are associated with primary open-angle glaucoma in Caucasians from the USA. Hum Mol Genet 2011;20:4707-13. 10.1093/hmg/ddr382 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Jensen MK, Pers TH, Dworzynski P, Girman CJ, Brunak S, Rimm EB. Protein interaction-based genome-wide analysis of incident coronary heart disease. Circ Cardiovasc Genet 2011;4:549-56. 10.1161/CIRCGENETICS.111.960393 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Rimm EB, Stampfer MJ, Colditz GA, Chute CG, Litin LB, Willett WC. Validity of self-reported waist and hip circumferences in men and women. Epidemiology 1990;1:466-73. 10.1097/00001648-199011000-00009 [DOI] [PubMed] [Google Scholar]
- 22. Rimm EB, Giovannucci EL, Stampfer MJ, Colditz GA, Litin LB, Willett WC. Reproducibility and validity of an expanded self-administered semiquantitative food frequency questionnaire among male health professionals. Am J Epidemiol 1992;135:1114-26, discussion 1127-36. 10.1093/oxfordjournals.aje.a116211 [DOI] [PubMed] [Google Scholar]
- 23. Salvini S, Hunter DJ, Sampson L, et al. Food-based validation of a dietary questionnaire: the effects of week-to-week variation in food consumption. Int J Epidemiol 1989;18:858-67. 10.1093/ije/18.4.858 [DOI] [PubMed] [Google Scholar]
- 24. Feskanich D, Rimm EB, Giovannucci EL, et al. Reproducibility and validity of food intake measurements from a semiquantitative food frequency questionnaire. J Am Diet Assoc 1993;93:790-6. 10.1016/0002-8223(93)91754-E [DOI] [PubMed] [Google Scholar]
- 25. Trichopoulou A, Costacou T, Bamia C, Trichopoulos D. Adherence to a Mediterranean diet and survival in a Greek population. N Engl J Med 2003;348:2599-608. 10.1056/NEJMoa025039 [DOI] [PubMed] [Google Scholar]
- 26. Locke AE, Kahali B, Berndt SI, et al. LifeLines Cohort Study. ADIPOGen Consortium. AGEN-BMI Working Group. CARDIOGRAMplusC4D Consortium. CKDGen Consortium. GLGC. ICBP. MAGIC Investigators. MuTHER Consortium. MIGen Consortium. PAGE Consortium. ReproGen Consortium. GENIE Consortium. International Endogene Consortium Genetic studies of body mass index yield new insights for obesity biology. Nature 2015;518:197-206. 10.1038/nature14177 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Wang T, Huang T, Heianza Y, et al. Genetic Susceptibility, Change in Physical Activity, and Long-term Weight Gain. Diabetes 2017;66:2704-12. 10.2337/db17-0071 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Ainsworth BE, Haskell WL, Whitt MC, et al. Compendium of physical activities: an update of activity codes and MET intensities. Med Sci Sports Exerc 2000;32(Suppl):S498-504. 10.1097/00005768-200009001-00009 [DOI] [PubMed] [Google Scholar]
- 29. Wolf AM, Hunter DJ, Colditz GA, et al. Reproducibility and validity of a self-administered physical activity questionnaire. Int J Epidemiol 1994;23:991-9. 10.1093/ije/23.5.991 [DOI] [PubMed] [Google Scholar]
- 30. Sotos-Prieto M, Bhupathiraju SN, Mattei J, et al. Changes in Diet Quality Scores and Risk of Cardiovascular Disease Among US Men and Women. Circulation 2015;132:2212-9. 10.1161/CIRCULATIONAHA.115.017158 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Sotos-Prieto M, Bhupathiraju SN, Mattei J, et al. Association of Changes in Diet Quality with Total and Cause-Specific Mortality. N Engl J Med 2017;377:143-53. 10.1056/NEJMoa1613502 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Brunkwall L, Chen Y, Hindy G, et al. Sugar-sweetened beverage consumption and genetic predisposition to obesity in 2 Swedish cohorts. Am J Clin Nutr 2016;104:809-15. 10.3945/ajcn.115.126052 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Hu FB. Dietary pattern analysis: a new direction in nutritional epidemiology. Curr Opin Lipidol 2002;13:3-9. 10.1097/00041433-200202000-00002 [DOI] [PubMed] [Google Scholar]
- 34. Kant AK. Dietary patterns and health outcomes. J Am Diet Assoc 2004;104:615-35. 10.1016/j.jada.2004.01.010 [DOI] [PubMed] [Google Scholar]
- 35. Xiang L, Wu H, Pan A, et al. FTO genotype and weight loss in diet and lifestyle interventions: a systematic review and meta-analysis. Am J Clin Nutr 2016;103:1162-70. 10.3945/ajcn.115.123448 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Livingstone KM, Celis-Morales C, Papandonatos GD, et al. FTO genotype and weight loss: systematic review and meta-analysis of 9563 individual participant data from eight randomised controlled trials. BMJ 2016;354:i4707. 10.1136/bmj.i4707 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.US Department of Health and Human Services, US Department of Agriculture. 2015-2020 dietary guidelines for Americans, 8th ed. 2015. http://health.gov/dietaryguidelines/2015/guidelines/.
- 38. Kant AK, Graubard BI. Energy density of diets reported by American adults: association with food group intake, nutrient intake, and body weight. Int J Obes (Lond) 2005;29:950-6. 10.1038/sj.ijo.0802980 [DOI] [PubMed] [Google Scholar]
- 39. Smith JD, Hou T, Hu FB, et al. A Comparison of Different Methods for Evaluating Diet, Physical Activity, and Long-Term Weight Gain in 3 Prospective Cohort Studies. J Nutr 2015;145:2527-34. 10.3945/jn.115.214171 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplementary tables and figures