Abstract
Objective
To characterize subsequent pregnancy outcomes among women with a history of previable, preterm prelabor rupture of membranes (PROM) and assess factors associated with recurrent preterm birth.
Methods
This was a retrospective cohort study of women cared with a history of ≥1 singleton pregnancy complicated by preterm PROM <24.0 weeks of gestation between 2002–2013 who cared for in 2 tertiary care health systems by a single group of maternal-fetal medicine specialists. Women were identified using ICD-9 codes and obstetric databases. Those with iatrogenic preterm PROM and those whose index preterm PROM <24.0 weeks was preceded by advanced cervical dilation were excluded. All women with ≥1 pregnancy reaching the second trimester after an index previable, preterm PROM pregnancy were included. The primary outcome was recurrent preterm birth <37 weeks. Data were analyzed by chi-square, Fisher’s exact, t-test, Wilcoxon rank-sum, and logistic regression.
Results
Two hundred ninety four women had ≥1 pregnancy complicated by previable, preterm PROM. One hundred eight out of 294 (37%) had ≥1 subsequent pregnancy in our healthcare systems and50/108 (46%) had ≥2. In the pregnancy immediately after the index delivery, the risk of prematurity was high: 50 (46%) delivered at <37 weeks, 31 (30%) at <34 weeks, 25 (23%) <28 weeks, and 18 (17%) before 24 weeks of gestation. Fewer than half (N=49, 45%) of women received preterm birth prophylaxis (progesterone or cerclage) in a subsequent pregnancy; rates of recurrent preterm birth were similar among women who received preterm birth prophylaxis compared to those who did not. In regression models, the only factor significantly associated with recurrent preterm birth <37 weeks was a history of preterm birth preceding previable, preterm PROM delivery (aOR 3.23, 95% CI 1.32–7.93).
Conclusion
Patients with history of previable, preterm PROM are at high risk of recurrent preterm birth.
Introduction
Preterm prelabor rupture of membranes (PROM) complicates 3–4.5% of all pregnancies and is responsible for approximately 1/3 of all premature births.(1, 2) Previable, preterm PROM (< 24.0 weeks) is associated with high rates of neonatal morbidity and mortality and occurs in <1% of all pregnancies.(3–6)
Traditionally, women delivering <20.0 weeks of gestation have not been regarded to have a preterm birth history, but rather, a miscarriage; such women have been excluded from intervention trials [including the Meis, et al. RCT of 17 alpha hydroxyprogesterone caproate vs. placebo].(7) Recently, experts have challenged this arbitrary 20.0 week cutoff to distinguish between “preterm birth” and “miscarriage.” Studies suggest that women with a history of a prior preterm birth between 16 and 20 weeks of gestation have an increased risk of recurrent second trimester loss and recurrent early preterm birth.(8) Thus, many experts recommend treating women with pregnancy loss due to spontaneous preterm labor, asymptomatic cervical dilation, or preterm PROM at 16–20 weeks similarly to those with this history >20.0 weeks. Management options include prematurity prevention clinic enrollment, prophylactic 17-alpha hydroxyprogesterone caproate, prophylactic cerclage, or increased cervical length surveillance.(9–13) In this investigation, we sought to characterize subsequent pregnancy outcomes among women with a history of preterm PROM <24.0 weeks and assess utilization of preterm birth prophylaxis modalities.
Materials and Methods
This was a retrospective cohort study that included all women with one or more documented singleton pregnancies complicated by preterm PROM between 14.0 and 24.0 weeks of gestation between 2002–2013 (index pregnancy) who then had at least one subsequent pregnancy reaching at least the 2nd trimester (≥14.0 weeks of gestation) between 2003 and 2015. Those with recognized cervical insufficiency (advanced cervical dilation in the absence of uterine contractions) preceding the occurrence of the index previable, preterm PROM were excluded. Women were also excluded if their fetus had major structural congenital malformations or aneuploidy, or if preterm PROM occurred within 1 week of amniocentesis or cervical cerclage placement. Women with a history of previable, preterm PROM who received care at one of 2 tertiary healthcare systems (The University of Utah and Intermountain Healthcare Hospitals) from a single group of maternal-fetal medicine specialists were identified using International Classification of Diseases (ninth revision) using established obstetric databases, and all cases were verified by manual chart review. Women referred for preconception counseling or prenatal care in a subsequent pregnancy following previable, preterm PROM were also included. All subsequent pregnancies reaching at least 14 weeks of gestation in the same 2 healthcare systems were studied..
Data abstracted from the medical records were collected and managed using REDCap (Research Electronic Data Capture) electronic data collection tool hosted at the University of Utah Center for Clinical and Translational Science.(16) Data were de-identified and therefore informed consent was waived. The University of Utah and Intermountain Healthcare Institutional Review Boards approved this study.
The primary outcome was recurrent preterm birth <37.0 weeks of gestation due to any indication in the first pregnancy following the index previable, preterm PROM. Secondary outcomes included recurrent preterm birth <34.0 weeks, <28.0 weeks, and prior to fetal viability (<24.0 weeks), as well as recurrent previable, preterm PROM <24.0 weeks, subsequent pregnancy surveillance with transvaginal cervical length ultrasound, or use of prophylactic progesterone or cerclage. We also sought to examine pregnancy outcomes for the second and third subsequent pregnancies following index previable, preterm PROM, as applicable.
Univariable analyses were by Chi-square analysis, Fisher exact test, Student t-test, Wilcoxon rank-sum as appropriate. Multivariable logistic regression was performed including variables selected using stepwise backward elimination; factors with p<0.20 remained in final models. All data were analyzed using STATA software version 13.1 (STATA Corp, College Station, TX).
Results
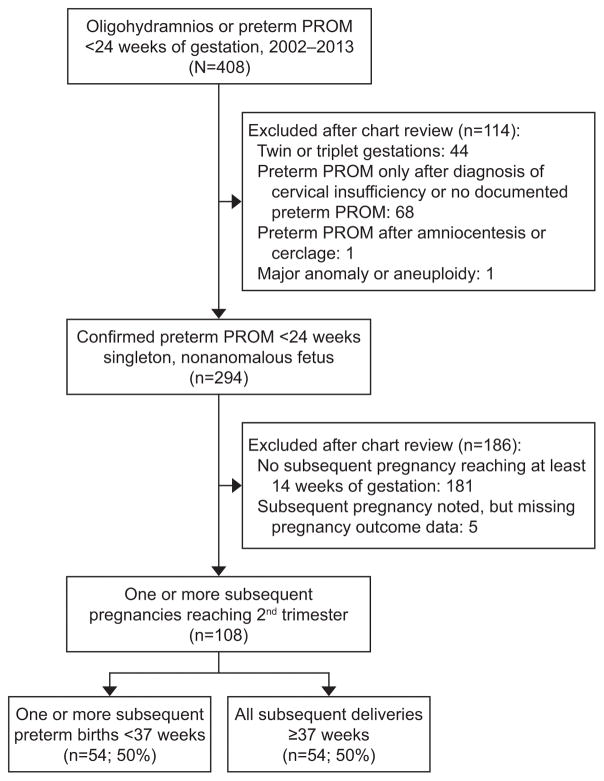
We identified 294 women with at least 1 pregnancy complicated by previable, preterm PROM <24.0 weeks of gestation during the study period (2002–2013). Of these, 108/294 (37%) had at least one subsequent pregnancy in our healthcare system and met inclusion criteria (Figure 1).
Figure 1.
Study enrollment
Four women were found to have had their first previable, preterm PROM deliveries prior to the previable, preterm PROM delivery that occurred during 2002–2013. For the purposes of data analysis, the earliest pregnancy where previable, preterm PROM could be documented was considered the index previable, preterm PROM case, and the next documented subsequent pregnancy to reach the second trimester was studied, even if these pregnancies were earlier than the initial time window specified by the inclusion criteria, provided the woman was confirmed to have a delivery complicated by previable, preterm PROM during the 2002–2013 search window.
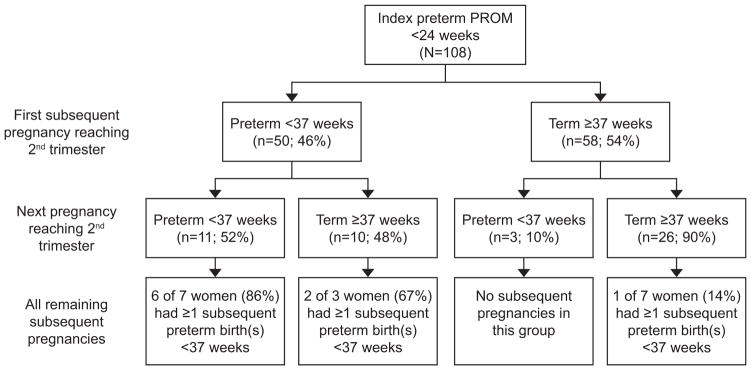
Women with a history of previable, preterm PROM were at high risk for preterm birth <37.0 weeks of gestation in subsequent pregnancies (Figure 2). Overall, 50% had at least one subsequent preterm birth (Figure 1). When only the first subsequent pregnancy reaching the second trimester was considered, 50 women (46%, 95% CI 37–56%) delivered preterm <37.0 weeks of gestation, 31 (30%, 95% CI 23–41%) delivered <34.0 weeks, 25 (23%, 95% CI 16–32%) <28.0 weeks, and 18 (17%, 95% CI 11–25%) delivered <24.0 weeks of gestation. There were no indicated preterm deliveries (e.g., for maternal or fetal indications) in this cohort; all preterm birth were attributed to spontaneous preterm labor, preterm PROM, or cervical insufficiency. Women whose first pregnancy after previable, preterm PROM delivered preterm <37.0 weeks were more likely to have a history of a prior preterm birth and less likely to have had a prior term delivery, but were otherwise similar to those who delivered at term in the subsequent pregnancy. Specifically, the median gestational ages at previable, preterm PROM and at delivery of the index previable, preterm PROM pregnancy were similar between groups (Table 1). Recurrent previable, preterm PROM was also common; 20 women (19%, 95% CI 12–27%) had one or more subsequent pregnancies complicated by recurrent preterm PROM <24.0 weeks of gestation.
Figure 2.
Subsequent pregnancy outcomes following pre-viable preterm premature rupture of membranes, by pregnancy sequence.
Table 1.
Demographic, baseline, and prior pregnancy characteristics dichotomized by the delivery gestational age of the next pregnancy reaching the second trimester.
| Characteristic | Next Pregnancy after previable, Preterm PROM Delivered Preterm <37 weeks of gestation N=50 |
Next Pregnancy after previable, Preterm PROM delivered at Term ≥37 weeks of gestation N=58 |
p-value |
|---|---|---|---|
| Maternal age at due date of next pregnancy after previable, preterm PROM, (mean ± SD) | 31.3 ± 5.6 | 31.0 ± 5.3 | 0.758 |
| White race, n(%) | 43 (86) | 51 (88) | 0.766 |
| Married, n(%) | 36 (72) | 50 (86) | 0.068 |
| Pregestational diabetes mellitus, n(%) | 3 (6) | 1 (2) | 0.241 |
| Chronic hypertension, n(%) | 4 (8) | 3 (5) | 0.552 |
| Maternal psychiatric disorder (anxiety, depression, and/or bipolar), n(%) | 13 (26) | 10 (17) | 0.268 |
| Median rupture GA of index previable, preterm PROM pregnancy, weeks (IQR) | 20.1 (18.6 – 22.0) | 20.9 (18.7 – 22.1) | 0.720 |
| Median delivery GA of index previable, preterm PROM pregnancy, weeks (IQR) | 22.0 (20.0–24.0) | 23.3 (20.7–25.4) | 0.105 |
| Index previable, preterm PROM occurred in first pregnancy (G1), n(%) | 12 (24) | 16 (28) | 0.672 |
| History of one or more preterm birth prior to previable, preterm PROM (among multiparous patients), n(%) | 19 (38) | 7 (12) | 0.002 |
| History of one or more term births prior to previable, preterm PROM (among multiparous patients), n(%) | 17/38 (45) | 28/42 (67) | 0.048 |
| Known Müllerian anomaly, n(%), among those with uterine cavity evaluation or delivering by cesarean | 5/24 (21) | 1/21 (5) | 0.193 |
| Index previable, preterm PROM complicated by chorioamnionitis, n(%) | 14 (28) | 8 (14) | 0.068 |
Fifty of the 108 women (46%, 95%CI 37–56%) had two or more subsequent pregnancies reaching the second trimester. For those with multiple subsequent pregnancies, if the first subsequent pregnancy delivered at term, there was an increased rate of term delivery in the second subsequent pregnancy (90%, 95% CI 71–97%), Figure 2. Six women of 46 (13%, 95% CI 6–27%) with uterine cavity evaluations were found to have uterine cavity abnormalities, including 2 with a uterine septum and 4 with a bicornuate uterus.
Use of prematurity prevention interventions (including 17-alpha hydroxyprogesterone caproate administration and cervical cerclage placement) occurred in 49/108 (45%, 95% CI 36–54%) of women in their first pregnancy after previable, preterm PROM (Table 2). There were no changes over the study period in use of cervical cerclage or vaginal progesterone. However, there was increased use of 17-alpha hydroxyprogesterone caproate among those who had their first subsequent pregnancy later in the study period (Pearson’s correlation coefficient r=0.433, p<0.001). Eight women delivered their next pregnancy before 2004. Although use of 17-alpha hydroxyprogesterone caproate increased later in the study period, of the 100 women who delivered in an era of 17-alpha hydroxyprogesterone caproate use (2004 or later), 17-alpha hydroxyprogesterone caproate use was low, and our ability to make conclusions regarding efficacy in this population are limited by small numbers (Table 2). Specifically, overall 13% (n=7, 95% CI 7–29%) women used 17-alpha hydroxyprogesterone caproate from 2004–2009, vs. 50% (n=23, 95% CI 35–65%) from 2010–2014. In the time of increased use from 2010–2014, 34% (95% CI 17–57%) of those receiving 17-alpha hydroxyprogesterone caproate delivered preterm; although this rate was lower than the 48% (95% CI 27–69%) preterm birth rate among the 23 women who did not receive 17-alpha hydroxyprogesterone caproate, it was not statistically significant (p=0.369).
Table 2.
Management or characteristics of next pregnancy after previable, preterm PROM dichotamized by delivery gestational age.
| Characteristic | Next Pregnancy After Previable Preterm PROM Delivered Preterm N=50 |
Next Pregnancy After Previable Preterm PROM Delivered at Term N=58 |
p-value |
|---|---|---|---|
| Median interpregnancy interval, years (IQR) | 2 (1–3) | 2 (1–3) | 0.565 |
| At least one cervical length assessment by transvaginal ultrasound, n(%) | 22 (44) | 14 (24) | 0.029 |
| Cervical cerclage placement, n(%) | 18 (36) | 12 (21) | 0.077 |
| Received vaginal progesterone, n(%) | 2 (4) | 2 (3) | >0.99 |
| Intramuscular progesterone supplementation, n(%)* | 13/46 (28) | 17/54 (31) | 0.726 |
| Any preterm birth prophylaxis (vaginal progesterone, intramuscular progesterone, or cerclage), n(%) | 26 (52) | 23 (40) | 0.199 |
| Clinical and/or pathologic evidence of chorioamnionitis noted at delivery, n(%) | 13 (26) | 3 (5) | 0.003 |
Only the 100 pregnancies delivering in 2004 or later considered
There was also a lower rate of pre-viable delivery (<24.0 weeks of gestation) with 17-alpha hydroxyprogesterone caproate use across the entire study period, but this analysis was also limited by small numbers (2/28, 6.7% delivered <24.0 weeks with 17-alpha hydroxyprogesterone caproate compared with 16/62, 21% delivered <24.0 weeks without 17-alpha hydroxyprogesterone caproate, p=0.147). We also examined the proportion of women who were “eligible” to receive 17-alpha hydroxyprogesterone caproate using strict inclusion criteria by limiting “eligibility” to delivery at or beyond 20.0 weeks of gestation as per the original study by Meis et al. We found that 42/66 (63%, 95% CI 53–72%) women who delivered their previable, preterm PROM pregnancy ≥20.0 weeks (who had a subsequent pregnancy delivering in or beyond 2004) were not given 17-alpha hydroxyprogesterone caproate in any subsequent pregnancy.
In regression models, a history of preterm birth prior to the previable, preterm PROM delivery was associated with recurrent preterm birth <37.0 weeks (Table 3).
Table 3.
Multivariable regression of factors associated with delivery <37 weeks of gestation of the next pregnancy after previable, preterm PROM.
| Characteristic | Crude OR | p-value | aOR | p-value |
|---|---|---|---|---|
| History of a preterm delivery prior to previable, preterm PROM | 3.39 (1.46–7.86) | 0.004 | 3.23 (1.32–7.93) | 0.010 |
| Index previable, preterm PROM complicated by chorioamnionitis | 2.43 (0.92–6.40) | 0.072 | 2.26 (0.80–6.43) | 0.125 |
| Müllerian anomaly | 6.33 (0.71–56.2) | 0.097 | 8.56 (0.90–81.4) | 0.062 |
| Married | 0.41 (0.16–1.08) | 0.072 | 0.45 (0.16–1.30) | 0.142 |
Other factors considered for inclusion in model but removed (p>0.20) included treatment with any preterm birth preventative intervention (cerclage, vaginal progesterone, and/or intramuscular progesterone – considered as a single variable)
Discussion
In our cohort, nearly half of subsequent pregnancies after previable, preterm PROM resulted in preterm birth, and women with this history were at risk for recurrent preterm birth at <34.0, <28.0, and <24.0 weeks of gestation, as well as recurrent previable, preterm PROM. More alarmingly, 17% of women in this cohort delivered their immediately-ensuing pregnancy <24.0 weeks of gestation.
Recent studies have emphasized the importance of precisely determining the preterm birth phenotype in order to predict clinical outcomes. (17–19) This cohort exemplifies these concepts, as women with a prior preterm birth who then have previable, preterm PROM carry an extremely high risk for subsequent recurrent preterm birth and recurrent previable delivery. In all, 6/46 (13%, 95% CI 6–27%) women had an abnormal uterine cavity. For comparison, the expected rate of Mullerian anomalies in an unselected population is 3–6%; our study design prevents direct comparison of these rates.(20, 21) Previous studies have also found an association between uterine anomalies and preterm birth, second trimester pregnancy loss, miscarriage and infertility.(21–23) If some preterm birth may be attributed to mechanical causes, this may aid counseling and management; surgical repair of uterine anomalies may prolong gestation for some women.(24–26)
Various approaches to preterm birth prophylaxis are recommended for pregnant women with a history of spontaneous preterm birth. All women with ≥1 prior spontaneous preterm birth should receive prophylaxis with weekly intramuscular 17-alpha hydroxyprogesterone caproate injections between 16–36 weeks of gestation.(11, 27) In this cohort, only 30% of those with a history of previable, preterm PROM reaching the 2nd trimester received 17-alpha hydroxyprogesterone caproate. Though 17-alpha hydroxyprogesterone caproate use was higher from 2010 to 2014, it was still only 50%. This low rate of 17-alpha hydroxyprogesterone caproate utilization does not appear unique to our study population. Several recent reports have demonstrated 17-alpha hydroxyprogesterone caproate utilization among eligible women ranges from 39% to 47%.(28, 29). The reasons for our observed low utilization rate of 17-alpha hydroxyprogesterone caproate are unclear.
Our study has limitations. Due to the sample size, our ability to make conclusions regarding the efficacy of certain preterm birth prevention strategies (including vaginal and intramuscular progesterone) was limited. Interpretation of results should take into account the study population. For example, rates of recurrence in other populations, in the setting of increased cervical length screening and more widespread 17-OHPC use may be lower. In contrast, cohorts with more African-American women may have higher rates due to known increased risk of recurrent preterm birth. We were also limited by data available in the electronic medical record; some factors (e.g., maternal smoking) were inconsistently collected and therefore could not be included. We considered previable, preterm PROM to be <24 weeks of gestation in accordance with local practice patterns and ACOG recommendations regarding resuscitation. (30)
This study has several strengths. This is a relatively large cohort of women with a strictly defined history of previable, preterm PROM, all with at least one subsequent pregnancy reaching the second trimester. It adds to the limited data describing subsequent pregnancy outcomes in this specific high risk population. Due to the structure of healthcare delivery system in Utah, two-thirds of women delivering in the State of Utah are captured by our database, reducing the possibility that our data are biased towards worse outcomes and that individuals with subsequent healthy pregnancies would have received care and delivered elsewhere.29
Because previable, preterm PROM is relatively uncommon, adequately powered RCTs of management strategies for future pregnancies are unlikely. Thus, consideration should be given to uterine cavity evaluation (with consideration of repair if an abnormality is found) and using evidence-based treatments extrapolated from more heterogeneous preterm birth intervention studies. In all cases, care should be individualized but should include counseling regarding the likelihood of recurrence of this severe preterm birth phenotype.
Acknowledgments
Supported by the Center for Clinical and Translational Sciences grant 8UL1TR000105 NCATS/NIH, and by NICHD 5K23HD067224 (Dr. Manuck).
Footnotes
Locations of Study:
Department of Obstetrics and Gynecology, Division of Maternal Fetal Medicine, University of Utah School of Medicine, Salt Lake City, UT
Intermountain Healthcare Department of Maternal Fetal Medicine, Salt Lake City, Utah
Financial Disclosure
The authors did not report any potential conflicts of interest.
Presented as a poster at the 36th Annual Society of Maternal Fetal Medicine Meeting (February 1–6, 2016, Atlanta, GA).
References
- 1.Goldenberg RL, Culhane JF, Iams JD, Romero R. Epidemiology and causes of preterm birth. Lancet. 2008;371(9606):75–84. doi: 10.1016/S0140-6736(08)60074-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Lee T, Silver H. Etiology and epidemiology of preterm premature rupture of the membranes. Clin Perinatol. 2001;28(4):721–34. doi: 10.1016/s0095-5108(03)00073-3. [DOI] [PubMed] [Google Scholar]
- 3.Yeast JD. Preterm premature rupture of the membranes before viability. Clin Perinatol. 2001;28(4):849–60. doi: 10.1016/s0095-5108(03)00082-4. [DOI] [PubMed] [Google Scholar]
- 4.Manuck TA, Eller AG, Esplin MS, Stoddard GJ, Varner MW, Silver RM. Outcomes of expectantly managed preterm premature rupture of membranes occurring before 24 weeks of gestation. Obstet Gynecol. 2009;114(1):29–37. doi: 10.1097/AOG.0b013e3181ab6fd3. [DOI] [PubMed] [Google Scholar]
- 5.Wong LF, Holmgren CM, Silver RM, Varner MW, Manuck TA. Outcomes of expectantly managed pregnancies with multiple gestations and preterm premature rupture of membranes prior to 26 weeks. Am J Obstet Gynecol. 2015;212(2):215e1–9. doi: 10.1016/j.ajog.2014.09.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Manuck TA, Varner MW. Neonatal and early childhood outcomes following early vs later preterm premature rupture of membranes. Am J Obstet Gynecol. 2014;211(3):308e1–6. doi: 10.1016/j.ajog.2014.05.030. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Meis PJ, Klebanoff M, Thom E, Dombrowski MP, Sibai B, Moawad AH, et al. Prevention of recurrent preterm delivery by 17 alpha-hydroxyprogesterone caproate. N Engl J Med. 2003;348(24):2379–85. doi: 10.1056/NEJMoa035140. [DOI] [PubMed] [Google Scholar]
- 8.Edlow AG, Srinivas SK, Elovitz MA. Second-trimester loss and subsequent pregnancy outcomes: What is the real risk? Am J Obstet Gynecol. 2007;197(6):581e1–6. doi: 10.1016/j.ajog.2007.09.016. [DOI] [PubMed] [Google Scholar]
- 9.Markham KB, Walker H, Lynch CD, Iams JD. Preterm birth rates in a prematurity prevention clinic after adoption of progestin prophylaxis. Obstet Gynecol. 2014;123(1):34–9. doi: 10.1097/AOG.0000000000000048. [DOI] [PubMed] [Google Scholar]
- 10.Manuck TA, Henry E, Gibson J, Varner MW, Porter TF, Jackson GM, et al. Pregnancy outcomes in a recurrent preterm birth prevention clinic. American journal of obstetrics and gynecology. 2011;204(4):320e1–6. doi: 10.1016/j.ajog.2011.01.011. [DOI] [PubMed] [Google Scholar]
- 11.Committee on Practice Bulletins-Obstetrics TACoO, Gynecologists. Practice bulletin no. 130: prediction and prevention of preterm birth. Obstet Gynecol. 2012;120(4):964–73. doi: 10.1097/AOG.0b013e3182723b1b. [DOI] [PubMed] [Google Scholar]
- 12.Berghella V. Every 30 seconds a baby dies of preterm birth. What are you doing about it? American journal of obstetrics and gynecology. 2010;203(5):416–7. doi: 10.1016/j.ajog.2010.05.042. [DOI] [PubMed] [Google Scholar]
- 13.Boelig RC, Orzechowski KM, Berghella V. Cervical length, risk factors, and delivery outcomes among women with spontaneous preterm birth. The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal Obstet. 2015:1–5. doi: 10.3109/14767058.2015.1105957. [DOI] [PubMed] [Google Scholar]
- 14.Mercer BM, Goldenberg RL, Moawad AH, Meis PJ, Iams JD, Das AF, et al. The preterm prediction study: effect of gestational age and cause of preterm birth on subsequent obstetric outcome. National Institute of Child Health and Human Development Maternal-Fetal Medicine Units Network. American journal of obstetrics and gynecology. 1999;181(5 Pt 1):1216–21. doi: 10.1016/s0002-9378(99)70111-0. [DOI] [PubMed] [Google Scholar]
- 15.Lee T, Carpenter MW, Heber WW, Silver HM. Preterm premature rupture of membranes: risks of recurrent complications in the next pregnancy among a population-based sample of gravid women. Am J Obstet Gynecol. 2003;188(1):209–13. doi: 10.1067/mob.2003.115. [DOI] [PubMed] [Google Scholar]
- 16.Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–81. doi: 10.1016/j.jbi.2008.08.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Manuck TA, Esplin MS, Biggio J, Bukowski R, Parry S, Zhang H, et al. The phenotype of spontaneous preterm birth: application of a clinical phenotyping tool. Am J Obstet Gynecol. 2015;212(4):487e1–e11. doi: 10.1016/j.ajog.2015.02.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Esplin MS. The Importance of Clinical Phenotype in Understanding and Preventing Spontaneous Preterm Birth. Am J Perinatol. 2016 doi: 10.1055/s-0035-1571146. [DOI] [PubMed] [Google Scholar]
- 19.Goldenberg RL, Gravett MG, Iams J, Papageorghiou AT, Waller SA, Kramer M, et al. The preterm birth syndrome: issues to consider in creating a classification system. Am J Obstet Gynecol. 2012;206(2):113–8. doi: 10.1016/j.ajog.2011.10.865. [DOI] [PubMed] [Google Scholar]
- 20.Chan YY, Jayaprakasan K, Zamora J, Thornton JG, Raine-Fenning N, Coomarasamy A. The prevalence of congenital uterine anomalies in unselected and high-risk populations: a systematic review. Human reproduction update. 2011;17(6):761–71. doi: 10.1093/humupd/dmr028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Sugiura-Ogasawara M, Ozaki Y, Kitaori T, Kumagai K, Suzuki S. Midline uterine defect size is correlated with miscarriage of euploid embryos in recurrent cases. Fertility and sterility. 2010;93(6):1983–8. doi: 10.1016/j.fertnstert.2008.12.097. [DOI] [PubMed] [Google Scholar]
- 22.Chan YY, Jayaprakasan K, Tan A, Thornton JG, Coomarasamy A, Raine-Fenning NJ. Reproductive outcomes in women with congenital uterine anomalies: a systematic review. Ultrasound in obstetrics & gynecology : the official journal of the International Society of Ultrasound in Obstetrics and Gynecology. 2011;38(4):371–82. doi: 10.1002/uog.10056. [DOI] [PubMed] [Google Scholar]
- 23.Venetis CA, Papadopoulos SP, Campo R, Gordts S, Tarlatzis BC, Grimbizis GF. Clinical implications of congenital uterine anomalies: a meta-analysis of comparative studies. Reproductive biomedicine online. 2014;29(6):665–83. doi: 10.1016/j.rbmo.2014.09.006. [DOI] [PubMed] [Google Scholar]
- 24.Sugiura-Ogasawara M, Lin BL, Aoki K, Maruyama T, Nakatsuka M, Ozawa N, et al. Does surgery improve live birth rates in patients with recurrent miscarriage caused by uterine anomalies? Journal of obstetrics and gynaecology : the journal of the Institute of Obstetrics and Gynaecology. 2015;35(2):155–8. doi: 10.3109/01443615.2014.936839. [DOI] [PubMed] [Google Scholar]
- 25.Zlopasa G, Skrablin S, Kalafatic D, Banovic V, Lesin J. Uterine anomalies and pregnancy outcome following resectoscope metroplasty. International journal of gynaecology and obstetrics: the official organ of the International Federation of Gynaecology and Obstetrics. 2007;98(2):129–33. doi: 10.1016/j.ijgo.2007.04.022. [DOI] [PubMed] [Google Scholar]
- 26.Lolis DE, Paschopoulos M, Makrydimas G, Zikopoulos K, Sotiriadis A, Paraskevaidis E. Reproductive outcome after strassman metroplasty in women with a bicornuate uterus. The Journal of reproductive medicine. 2005;50(5):297–301. [PubMed] [Google Scholar]
- 27.Society for Maternal-Fetal Medicine Publications Committee waoVB. Progesterone and preterm birth prevention: translating clinical trials data into clinical practice. Am J Obstet Gynecol. 2012;206(5):376–86. doi: 10.1016/j.ajog.2012.03.010. [DOI] [PubMed] [Google Scholar]
- 28.Stringer EM, Vladutiu C, Manuck T, Verbiest S, Ollendorff A, Stringer JS, et al. 17-Hydroxyprogesterone Caproate (17P) Coverage Among Eligible Women Delivering at two North Carolina Hospitals in 2012 and 2013: a retrospective cohort study. Am J Obstet Gynecol. 2016 doi: 10.1016/j.ajog.2016.01.180. [DOI] [PubMed] [Google Scholar]
- 29.Bousleiman SZ, Rice MM, Moss J, Todd A, Rincon M, Mallett G, et al. Use and attitudes of obstetricians toward 3 high-risk interventions in MFMU Network hospitals. American journal of obstetrics and gynecology. 2015;213(3):398e1–11. doi: 10.1016/j.ajog.2015.05.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Obstetric Care Consensus No. 4: Periviable Birth. Obstet Gynecol. 2016;127(6):e157–69. doi: 10.1097/AOG.0000000000001483. [DOI] [PubMed] [Google Scholar]