Abstract
Sleep is characterized by coordinated cortical and cardiac oscillations reflecting communication between the central (CNS) and autonomic (ANS) nervous systems. Here, we review fluctuations in ANS activity in association with CNS-defined sleep stages and cycles, and with phasic cortical events during sleep (e.g., arousals, K-complexes). Recent novel analytic methods reveal a dynamic organization of integrated physiological networks during sleep and indicate how multiple factors (e.g., sleep structure, age, sleep disorders) affect “CNS-ANS coupling”. However, these data are mostly correlational and there is a lack of clarity of the underlying physiology, making it challenging to interpret causality and direction of coupling. Experimental manipulations (e.g., evoking K-complexes or arousals) provide information on the precise temporal sequence of cortical-cardiac activity, and are useful for investigating physiological pathways underlying the CNS-ANS coupling. With the emergence of new analytical approaches and a renewed interest in ANS and CNS communication during sleep, future work may reveal novel insights into sleep and cardiovascular interactions during health and disease, in which coupling could be adversely impacted.
Keywords: Cortico-cardiac interplay, sleep, autonomic nervous system, central nervous system, heart rate variability, baroreflex, sympathetic, vagal, electroencephalography, electrocardiography
1. Introduction
Sleep is a complex physiological process involving multiple biological systems, fundamental for the health of an individual. It is typically defined as a central nervous system (CNS) phenomenon in which the state of cortical activation determines the individuals’ state of consciousness. Sleep regulatory systems are closely associated, anatomically and physiologically, with the autonomic nervous system (ANS), as described in this review. The ANS regulates the majority of the body’s internal processes (e.g., blood pressure, myocardial function, breathing, body temperature, digestion, urination) via afferent and efferent sympathetic and parasympathetic pathways, allowing adaptive responses to internal and external stressors, guaranteeing the body homeostatic milieu.
A growing body of research has investigated ANS function during sleep, mainly focusing on cardiovascular (CV) functioning, using measures derived from heart rate such as heart rate variability (HRV) analysis of the electrocardiography (ECG) signal. Importantly, measures reflecting ANS function fluctuate across a night of sleep, depending on both homeostatic (i.e., related to the duration of sleep and of prior wakefulness) and circadian processes, and in association with phasic events during sleep. These interactions, which reflect the dynamic interplay between the CNS and the ANS, are the focus of the current review.
Over recent years, a number of studies have explored the association between the CNS and the ANS during sleep using various approaches and rationales, while offering promising new perspectives to understand the brain-body interplay during sleep in humans. Here, we review CNS-ANS coupling during sleep, consider the methodologies for measuring sleep and ANS activity (Sections 1.1), identify limitations in assessing ANS function indirectly in humans (Section 1.1), and discuss the underlying physiological basis for the presence of coupling between the two systems (Section 1.2). We then review the body of work investigating ANS-CNS coupling during sleep, ranging from observations of changes in heart rate, HRV, and blood pressure across sleep stages (Section 2) to an analysis of the temporal dynamics between outputs of the two systems (Sections 3 – 4). Finally, we discuss clinical implications for the interdependency between the CNS and ANS during sleep and conclude with suggestions for future research directions (Section 5 and 6).
For the purpose of this review, we will consider the relationship between CNS indices and ANS measures as part of the concept of “CNS-ANS coupling”. We conceptualize different levels of evidence and methods (arbitrarily defined for clarity of presentation) supporting CNS-ANS coupling during sleep, which forms the framework for this review:
-
▪
Observations. For example, changes in ANS control of cardiovascular effectors, such as changes in cardiac vagal modulation, according to CNS-defined sleep stages.
-
▪
ANS and/or CNS mediated perturbations. For example, heart rate and blood pressure fluctuations associated with, or in response to, CNS-defined phasic sleep events including spontaneous cortical arousals and slow waves.
-
▪
Analytics of continuous CNS-ANS dynamics, which integrate continuous, simultaneous measures of both ANS and CNS function to explore their interconnections. For example, continuous linear and non-linear relationships between time-series of cortical and cardiac function, considering strength, time-course, and directionality.
1.1. Assessment of ANS during sleep
Polysomnography (PSG) is the gold-standard method to objectively assess sleep using multiple sources of information. The characterization of sleep-wake states (i.e., wakefulness, the stages N1, N2, and N3 of non-rapid-eye-movement [NREM] sleep, and rapid-eye-movement [REM] sleep) is fully described in the scoring manual of the American Academy of Sleep Medicine (AASM) (see Berry et al., 2017). This characterization follows standardized rules based on visual detection and discrimination of electroencephalography (EEG), electromyography, and electrooculography features within fixed discrete time windows (30 s epochs) across the night. EEG is typically sampled at ≥ 200 Hz to fully capture high frequency activity.
Sleep can be broadly divided into two main states characterized by specific features and EEG patterns. In humans, REM sleep is characterized by a “wake-like” low-amplitude high frequency EEG activity, irregular and sharp eye movements, and low muscle tone. NREM sleep, which constitutes between 75% and 80% of the total sleep period, is characterized by progressive EEG synchronization. It begins with low amplitude and mixed frequency EEG activity with a predominant theta (4–7 Hz) rhythm in NREM sleep stage N1. This is followed by NREM sleep stage N2, characterized by the appearance of spontaneous K-complexes (the largest event in the human EEG, consisting of a positive-negative-positive waveform ≥ 0.5 s) and sleep spindles (bursts of distinct 11–16 Hz waves, ≥ 0.5 s). There is then a predominance of high-voltage slow wave oscillations (1–4 Hz) in NREM sleep stage N3. Sleep shows a strong ultradian rhythm such that REM and NREM alternate with a cycle length of ~90 min across the night. There is predominance of N3 sleep during cycles in the first part of the night with a progressive increase in time spent in REM sleep across the night (Kryger et al., 2015). Importantly, both sleep states (NREM and REM), as well as phasic sleep events (e.g., arousals, K-complexes) are accompanied by distinct patterns of tonic and phasic ANS activation (see Section 1.2).
Conventional sleep staging offers an overall picture of a night’s sleep, and can be clinically useful in assessing sleep quality and composition. However, it is limited by being visually determined, arbitrary, and providing discrete characterization of sleep. The current scoring guidelines (Berry et al., 2017) are essentially similar to those codified 50 years ago by a committee led by Rechtschaffen and Kales (Kales and Rechtschaffen, 1968) for use with analog data recorded on pen chart recorders. These criteria were, in turn, largely based on visual scoring systems developed 80 years ago (Loomis et al., 1937). Importantly, this approach constrains the analysis of all aspects of human physiology (e.g., cardiovascular measures, hormonal variations) within arbitrarily-defined, discrete, and CNS-defined sleep periods.
Automated quantitative EEG analysis has the potential to overcome limitations inherent in visual scoring and provides continuous and detailed information on the state of cortical activation and EEG complexity. Typically, an EEG spectrum is obtained by applying a fast Fourier transform to the signal, after which power spectral density (µV2/Hz) can be calculated for somewhat arbitrarily defined EEG bands: delta (1–4 Hz), theta (4–7 Hz), alpha (8–12 Hz), sigma (12–15 Hz), low- (16–23 Hz) and high- (23–30 Hz) beta, and gamma (>30 Hz) frequencies. Power in each frequency band can then be summarized per epoch, across the night, or within sleep stages and sleep cycles. For example, EEG delta power declines over sequential NREM-REM sleep cycles, a phenomenon interpreted as reflecting a decrease in homeostatic pressure across the night (Dijk, 2009). Several factors including age, sex, menstrual cycle, medications, and presence of insomnia, influence elements of the EEG power spectrum. EEG spectral indices are the principal CNS indices used in studies directly assessing CNS-ANS coupling (see Section 4).
Daytime assessment of ANS function mainly relies on classic ANS tests reflecting the ANS response to standardized maneuvers such as isometric exercises (handgrip), cold pressure test, cognitive load (mental arithmetic), orthostatic testing (including head-up tilt-test), Valsalva maneuver, deep breathing, cold face test of the diving reflex, and more invasive tests such as pharmacological (e.g., intravenous phenylephrine) or mechanical (e.g., neck suction) challenges to stimulate and evaluate baroreflex functioning (see Zygmunt and Stanczyk, 2010). These tests are used in clinical settings to identify ANS abnormalities for the diagnosis and treatment of diseases involving ANS dysfunction.
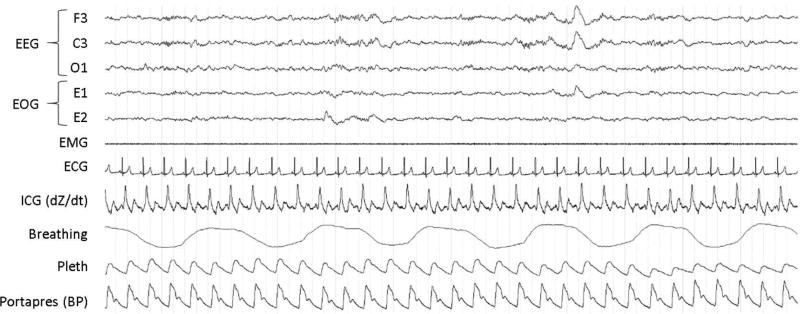
A number of other techniques, more suitable for research purposes, are available to continuously assess ANS and cardiovascular functioning without active engagement from participants, and can, therefore, be applied during sleep (See Table 1 for a summary of these measures and their limitations). These differ as to the particular property of cardiovascular functioning they assess (e.g., cardiac function such as heart rate, or peripheral sympathetic nerve activity [SNA] using microneurography); whether they measure tonic or acute/transient properties (e.g., average heart rate during NREM sleep, or the heart rate response to a brief arousal from sleep); the ease with which the technique can be applied over prolonged periods of time such as during sleep (e.g., challenges associated with inserted electrodes that need to be kept in position across the night); and the degree of ambiguity in the interpretation of the measure (e.g., the relatively straightforward interpretation of average heart rate, or the more complex interpretation of indices of HRV). Figure 1 offers an example of co-registration of EEG, ANS and cardiovascular indices during a PSG night of a sample participant at the SRI Human Sleep Research Lab.
Table 1.
Techniques to assess autonomic nervous system (ANS) functioning during sleep applicable to understanding central nervous system(CNS)-ANS coupling: processing, interpretation, and limitations
| Method | Signal processing | Indices derived | Interpretation | Limitations |
|---|---|---|---|---|
| Heart rate and heart rate variability (HRV) Assesses beat-to-beat variability in the intervals between successive electrocardiographic (ECG) R-waves, generally at frequencies below 0.4 Hz |
|
|
|
|
| Impedance cardiography A noninvasive technology that monitors the electromechanical activity of the heart in combination with the ECG by measuring beat-to-beat changes in electrical impedance across the chest, allowing the measurement of several cardiodynamic parameters (see Sherwood et al., 1990). |
|
|
|
|
| Microneurography Records efferent activity of sympathetic nerve fibers to muscle blood vessels and provides a direct measure of peripheral sympathetic drive (Victor et al., 1987) |
|
|
|
|
| Ambulatory blood pressure monitoring and beat-to-beat blood pressure assessment Ambulatory blood pressure monitoring provides automated, intermittent, sphygmomanometer-based blood pressure measurements. The Finapres/Portapres system (Finapres Medical Systems, Enschede, NL) is arguably the most employed option to continuously and relatively noninvasively measure systolic and diastolic blood pressure with high temporal resolution over long periods of time |
|
|
|
|
| Photoplethysmographic-type methods Provides indirect information on ANS innervation of peripheral vessels |
|
|
|
|
Figure 1.
Co-registration of standard PSG, and ANS and cardiovascular signals in N2 sleep (30 s) from a sample participant at the SRI Human Sleep Research Lab. Signals include: electroencephalogram (EEG), electrooculogram (EOG), electromyogram (EMG), electrocardiogram (ECG), change in impedance over time (dZ/dt) from impedance cardiography (ICG), abdominal breathing recorded using piezoelectric bands, finger plethysmography (PPG), and beat-to-beat blood pressure (BP)
The most widely used indicators of ANS activity during sleep are heart rate and HRV. Heart rate may be readily and non-invasively assessed by appropriately placed surface recording electrodes, typically over thoracic regions, producing the ECG. The ECG is an integral component of clinical sleep assessment and, while not being used as a main source of information to determine sleep state, is recommended by the AASM for standard clinical PSG assessments (Berry et al., 2017).
Heart rate (or heart period, which is its reciprocal) has the advantage of enabling assessment of cardiac ANS tone (i.e., average ANS activity) and of transient (beat-to-beat) cardiac modulation, and thus it has been repeatedly applied in studies of CNS-ANS coupling. The available evidence indicates that heart period is linearly related to the frequency of cardiac parasympathetic and sympathetic activity (Berntson et al., 1995). The mean value of heart period is thus a simple and powerful index to assess changes in the balance (i.e., linear sum) of cardiac parasympathetic and sympathetic tone. Since heart rate and heart period are related by a non-linear (hyperbolic) function, it should be noted that they are not equivalent for the purpose of assessing cardiac ANS tone.
HRV quantifies the beat-to-beat variability of heart periods (the time intervals between subsequent R waves on the ECG), generally at frequencies < 0.4 Hz, and has been widely used with the purpose of estimating specific components of ANS functioning (Cacioppo et al., 2007). HRV may be analyzed in the time domain or in the frequency domain (in the latter technique by integrating HRV spectral power density, in ms2 Hz−1, over specified frequency bands), within specified time-windows, ideally of 5-minute length for the purpose of standardization (Camm et al., 1996), across the sleep period.
HRV spectral power at frequencies below 0.04 Hz (the very low frequency range, VLF) is a measure with dubious interpretation, particularly when assessed from recordings with durations ≤ 5 min. In contrast, HRV power in the 0.15 to 0.40 Hz frequency range (high-frequency, HF) reflects respiratory sinus arrhythmia and as a consequence is a useful measure of cardiac vagal modulation (Camm et al., 1996). Cardiac vagal modulation may also be estimated from HRV in the time domain by computing the indices RMSSD, the root mean square of the differences between successive R-R intervals, and pNN50, the percentage of the values of RR-interval that differ from the preceding value by > 50 ms (Camm et al., 1996).
HRV spectral power in the low frequency (LF) range (0.04 to 0.15 Hz) has often been interpreted to reflect sympathetic activity. This interpretation has been particularly controversial because of conceptual shortcomings and because multiple sources contribute to variability in this range (Billman, 2013; Trinder, 2007). Importantly, the sinoatrial node responses to sympathetic and vagal activity indicate that HRV in the LF range may be driven by both sympathetic and vagal modulations (Rossi et al., 2016). In an attempt to provide a solution to this problem, the power ratio LF/HF has been proposed under the assumption that the vagal component contributing to HRV LF power would be at least partially neutralized, such that the ratio would reflect sympathetic modulation or sympatho-vagal balance (Camm et al., 1996). However, the very concept of sympatho-vagal balance has been challenged (Eckberg, 1997) and there is no reason to think that the vagal modulation contributing to LF HRV power is equal to, or from the same source, as that contributing to HF HRV power. Consistent with this, the interpretation of LF/HF ratio in terms of cardiac sympathetic activity has been recently questioned by direct experimentation on a sheep model of heart failure (Martelli et al., 2014). Nevertheless, even in the absence of a clear-cut physiological interpretation, the LF/HF ratio may nonetheless be of some value as a descriptor of HRV during sleep.
However, papers reporting the LF/HF ratio in the sleep field have often overlooked other computational issues (Burr, 2007). The LF and HF components of HRV power are often expressed in normalized units (nu), as the % of the total power of HRV. In normalizing LF and HF power, however, it is common practice to remove the VLF component from total power, i.e., to divide LF and HF by the sum (LF+HF) (Camm et al., 1996). As a consequence, the quantities LF/HF, LFnu and HFnu (mathematically identical values) are equivalent carriers of information that reflect the same features of cardiac ANS control. Thus it becomes redundant to report more than one of these variables. This limitation is not substantially lessened if total power of HRV is used as the denominator instead of the sum of LF and HF power, because any difference in information among LF/HF, LFnu, and HFnu will then come from the HRV VLF power, which, as noted above, is hardly interpretable in terms of sympathetic or vagal modulation (Burr, 2007).
If the assumptions of linearity and stationarity of the heart period time series are abandoned, several non-liner methods are available to assess ANS function. For example, the Poincaré plot is a non-linear geometric approach to qualitatively picture and quantitatively assess HRV metrics. It is produced by plotting each RR interval (RRn+1, ms; y axis) against the previous RR interval (RRn, ms; x axis) for a specific time window (e.g., 1 min, 2 min, 5 min). The inter-beat autocorrelation coefficient is a quantitative HRV index derived from the Poincaré plot, and has been frequently used in investigating the dynamics of CNS-ANS coupling (see Section 4). It is calculated as the Pearson product-moment correlation coefficient between RRn+1 and RRn+1. The inter-beat autocorrelation coefficient is highly correlated with the frequency-domain HRV LF/HF index during night-time sleep (Otzenberger et al., 1998), whose physiological interpretation is, as previously discussed, a topic of much debate. Moreover, being a linear measure, the inter-beat autocorrelation index is not sensitive to the nonlinear features displayed by the Poincaré plot (Brennan et al., 2001).
Entropy-derived non-linear indices based on HRV (e.g., detrending fluctuation analysis, approximate entropy, sample entropy, multiscale entropy analyses) have also been used. These and even more sophisticated methods (see Valenza et al., 2017) which measure non-linear HRV features might be better suited to track HRV changes associated with human high-level functioning such as emotional and cognitive processing (see de la Torre-Luque et al., 2016; Young and Benton, 2015). However, their readouts are difficult to interpret in terms of specific anatomic pathways.
Limitations of HRV analysis (see Table 1), are critical when considering the physiological interpretation of the even more complex relationships between the temporal EEG-HRV dynamics, as we will further discuss in Section 4.
Given the lack of a pure sympathetic nervous system measure derived from HRV analysis, sympathetic nerve activity (SNA) has been measured using other techniques. Impedance cardiography allows a noninvasive measure of pre-ejection period, a cardiac ANS index calculated as the time from the electrical systole to the opening of the aortic valve (blood ejection). It is thought to reflect β-adrenergic sympathetic control of the heart (Sherwood et al., 1990). To our knowledge, no study has investigated the temporal dynamics of the relationship between the pre-ejection period and CNS indices (e.g., EEG) during sleep. A different direct measure of (non-cardiac) peripheral SNA is obtained by microneurography, an invasive method measuring the SNA to muscle blood vessels and skin. Despite being used in some sleep studies (see Mano et al., 2006), microneurography cannot be easily adopted in sleep research and is impractical in clinical sleep medicine due to its invasiveness and methodological challenges (e.g., the requirement of immobilization). For example, Tank et al. (2003) recorded muscle SNA from the right peroneal nerve using microneurography together with intra-arterial blood pressure before and after EEG K-complexes. None of the 8 participants studied, were able to reach REM sleep and only 5 were able to reach NREM N3. Skin conductance/resistance can offer a non-invasive continuous measure of electrodermal activity, reflecting cutaneous sudomotor activity and indicating skin sympathetic outflow. The most frequently used method to assess electrodermal activity consist of passing a small current between two surface electrodes usually placed on the palm of the hand. The resulting voltage, when the current is held constant, is proportional to skin resistance (or alternatively, a measure of conductance is obtained using a constant voltage system). Although it is generally accepted that sweat glands have predominant sympathetic cholinergic innervations, neural mechanisms and pathways involved in the central control of electrodermal activity are not fully clarified (Cacioppo et al., 2007). Most of the research on electrodermal activity has been conducted in the context of cognitive and emotional processing, and the application and interpretation of this technique during sleep is questionable. The measurement of circulating catecholamines (plasma epinephrine and norepinephrine concentration) has been also used to evaluate peripheral sympathetic ANS functioning during sleep, although it is invasive, and not suitable to assess CNS-ANS coupling during sleep at high temporal resolution.
In summary, as shown in Table 1, there is no unobtrusive and unconfounded measure of central sympathetic tone which can be used in sleep studies. In light of the methodological constraints of sympathetic assessment and in the face of reliable indices of cardiac vagal modulation, it is surprising that research on CNS-ANS coupling during sleep has over-emphasized the sympathetic over the vagal system.
Other measures reflecting ANS function (however, less frequently used in the context of CNS-ANS coupling) are available and may ultimately further advance the understanding of CNS-ANS dynamics during sleep by providing windows on other aspects of the ANS. These measures include beat-to-beat blood pressure monitoring and others obtainable with photoplethysmographic-type sensors (see Table 1 for details).
1.2. Physiological mechanisms underlying CNS-ANS coupling during sleep
The brain is connected to cardiac myocytes and arteriolar smooth muscle cells, which are the CV autonomic effectors, by di-synaptic pathways involving preganglionic and ganglionic autonomic neurons (Silvani et al., 2016). In the afferent direction, changes in blood vessel stretch and skin temperature, which are affected by skin vessel tone, are detected by baroreceptors and thermoreceptors and fed back to the brain (Silvani, 2017; Silvani et al., 2015). Changes in breathing such as those seen when transitioning from wakefulness to sleep (Trinder and Nicholas, 2000), also modulate the ANS both directly, through CNS circuits, and reflexively, for example by changing lung stretch as a function of sleep-related reduction in tidal volume (Colrain et al., 1987). These efferent and afferent pathways constitute the anatomical and functional substrate of the coupling between the CNS and the ANS.
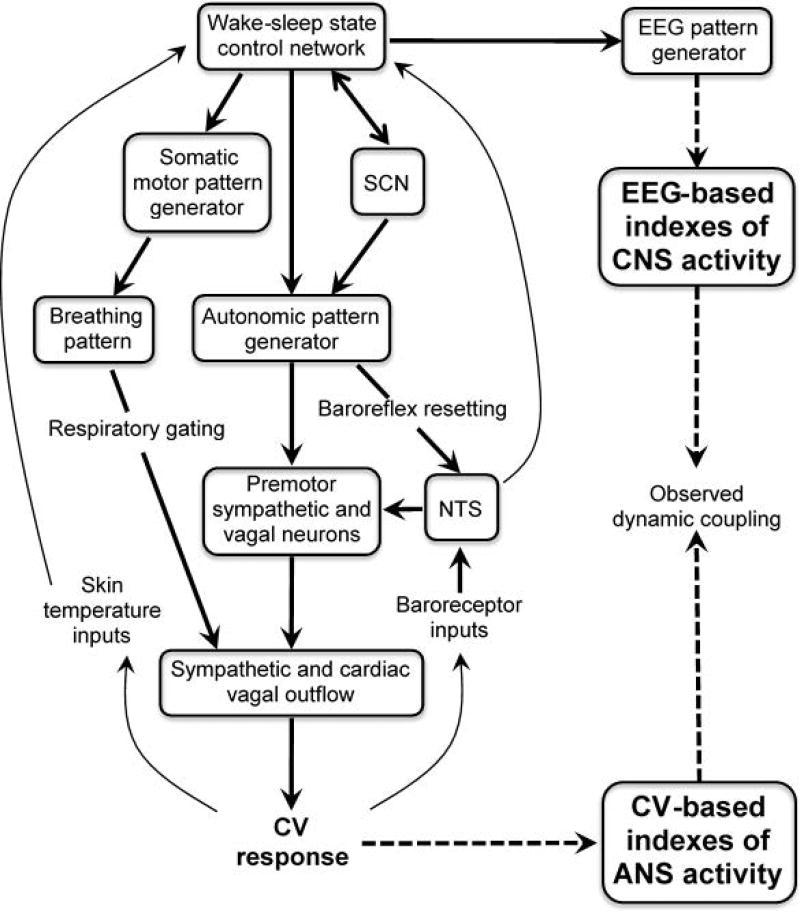
The coexistence of top-down (efferent) and bottom-up (afferent) pathways complicates inferences of causality from observed correlations between CNS and ANS variables (Figure 2). For example, parasympathetic preganglionic neurons in the medullary nucleus ambiguous are subjected to a respiratory modulation (McAllen and Spyer, 1978) that gates inputs from baroreceptors, chemoreceptors and nasopharyngeal receptors (Gilbey et al., 1984). The cardiac sinoatrial node responds to parasympathetic activity with minimal delay and is responsive to modulations of parasympathetic activity at least up to 0.4 Hz (Berger et al., 1989). As a result, the inspiratory gating of nucleus ambiguous neural activity is one of the mechanisms responsible for respiratory sinus arrhythmia (Eckberg, 2003).
Figure 2.
Schematic diagram illustrating the general physiological mechanisms that may underlie the observed dynamic coupling between indexes of central nervous system (CNS) function based on the electroencephalogram (EEG) and indexes of autonomic nervous system (ANS) modulation based on cardiovascular (CV) variables. NTS, nucleus of the solitary tract. SCN, suprachiasmatic nucleus. Modified from Silvani and Dampney (Silvani and Dampney, 2013), with permission.
The specific neural pathways that couple CNS to ANS during sleep are still uncharted. It has been suggested (Silvani and Dampney, 2013) that the activities of thalamo-cortical neurons, skeletal muscles, and the ANS, which explain the EEG, electromyographic, and cardiovascular features of the sleep states, respectively, are modulated in parallel by sleep-state control circuits, which are mainly located in the hypothalamus and brainstem (Scammell et al., 2017). This conceptual model predicts that measures of CNS-ANS coupling during sleep, such as correlations between EEG and HRV spectral indexes, do not necessarily imply direct causal links from EEG to HRV. Rather, the CNS-ANS coupling may reflect the common dependence of EEG and HRV variables on the activity of specific hypothalamic and brainstem circuits. The brainstem appears critical in this respect, as key neural elements of autonomic, respiratory, and cardiovascular control are located within the medulla, pons, and midbrain (Silvani and Dampney, 2013), together with key elements of the ascending pathways that control EEG activity through the thalamus and basal forebrain (Scammell et al., 2017).
This conceptual model bears resemblance to that of central pattern generators coordinating skeletal muscle motor neurons, autonomic preganglionic neurons, and neuroendocrine neurons (Swanson, 2011). In the context of physical exercise, the autonomic counterpart of the skeletal muscle activity produced by these central pattern generators is classically termed the central autonomic command (Goodwin et al., 1972). This conceptual model of central autonomic commands in the context of CNS-ANS coupling during sleep provides a framework for future work to examine which sleep-state control circuits modulate cardiovascular activity, how circuits may differ during NREM versus REM sleep as well as during transition periods between NREM and REM sleep, and whether outputs from sleep state circuits to thalamo-cortical and ANS neurons are indeed precisely temporally coupled. In this respect, the coupling between pattern generators should not be viewed as rigid, and may be actually relatively weak, as is thought for the neural oscillators underlying resting brain fluctuations (Deco et al., 2009). Sleep-related central autonomic commands may result from the summation of activity of different central pattern generators (Silvani and Dampney, 2013), either at the same time, as occurs for thermoregulation (Romanovsky, 2007), or at different times, because of the asynchronous development of the sleep process in different neuronal groups (Kim et al., 2017; Pigarev et al., 1997). A summary of the data-driven hypotheses on the similarities and differences in central autonomic control between wakefulness and NREM sleep, and REM sleep is provided in Table 2.
Table 2.
Summary of data-driven hypotheses on the similarities and differences in central autonomic control across wake-sleep states. See text and primary references (Silvani and Dampney, 2013) and (Silvani et al., 2016), for further details. Upward and downward arrows indicate the direction of changes in neural activity. Rightward arrows indicate synaptic connections. CV, cardiovascular. l/vl PAG, lateral/ventrolateral periaqueductal gray. MnPO, median preoptic nucleus. MPO, medial preoptic area of the hypothalamus. NAmb, nucleus ambiguous. NTS, nucleus of the solitary tract. PBN, parabrachial nucleus. PNA, parasympathetic nerve activity. PPT, pedunculopontine tegmental nucleus. PVN, paraventricular nucleus of the hypothalamus. rMR, rostral medullary raphe. RVLM, rostral ventrolateral medulla. SLD, sublaterodorsal nucleus. SNA, sympathetic nerve activity. NRO, nucleus of the raphe obscurus. IVe/MVe: inferior/medial vestibular nucleus. The question mark (?) indicates that the contribution of parasympathetic withdrawal to the increase in heart rate on passing from NREM sleep to REM sleep is still unclear (see Lo Martire et al., IN PRESS).
| NREM sleep vs. wakefulness | |
|
| |
| ↑ cardiac PNA | ↓ PBN → ↑ NTS → ↑ NAmb |
| ↓ skin SNA | ↓ MnPO → ↑ MPO → ↓ rMR |
| ↓ cardiac, muscle, and renal SNA | ↓ PBN → ↑ NTS → ↓ RVLM |
| ↓ PVN | |
| ↓ PPT → ↓ RVLM | |
| REM sleep vs. NREM sleep | |
|
| |
| ↓ cardiac PNA (?) | ↑ PBN → ↓ NTS → ↓ NAmb |
| ↑ cardiac and muscle SNA, | ↑ PBN → ↓ NTS → ↑ RVLM |
| ↓ mesenteric and renal SNA | ↑ PPT → ↑ RVLM |
| ↑ SLD → ↑ RVLM | |
| ↑↓ l/vl PAG → ↑↓ RVLM | |
| ↑ NRO | |
| ↑ CV variability | ↑ IVe/MVe → ↑ NTS/PBN/PPT |
1.2.1. Central autonomic commands during NREM sleep
Increases in the activity of the hypothalamic ventrolateral preoptic nucleus may modulate ANS activity during NREM sleep through at least four different pathways (Sherin et al., 1996). The lower values of SNA to the skin during NREM sleep compared to wakefulness (Takeuchi et al., 1994) may result from inhibition of a thermoregulatory pathway for heat generation and retention, which includes the preoptic hypothalamus and the medullary raphe (Morrison, 2016). On the other hand, the occurrence of lower values of SNA to the skeletal muscles (Somers et al., 1993) and kidneys (Miki et al., 2003) during NREM sleep may result from (Silvani, 2017; Silvani and Dampney, 2013): a) inhibition of the hypothalamic paraventricular nucleus (Uschakov et al., 2006), a master ANS controller that integrates neuroendocrine, homeostatic and stress responses during wakefulness (Thompson and Swanson, 2003); b) inhibition of the pedunculopontine nucleus between the caudal midbrain and rostral pons (el Mansari et al., 1989), a region potentially contributing to central autonomic commands associated with locomotion during wakefulness (Garcia-Rill et al., 1987; Padley et al., 2007); and c) potentiation of the baroreceptor reflex, through a pathway that involves the pontine parabrachial nucleus (Saito et al., 1977) and the medullary nucleus of the solitary tract (Eguchi and Satoh, 1980). In particular, increases in parabrachial nucleus activity may inhibit the baroreflex at the level of the first afferent relay, which is the nucleus of the solitary tract (Felder and Mifflin, 1988). Therefore, the tonic decrease in parabrachial nucleus activity during NREM sleep may disinhibit the baroreflex in this state. Conversely, transient increases in parabrachial nucleus activity during autonomic arousals in NREM sleep may contribute to simultaneous increases of blood pressure and heart rate because of transient baroreflex inhibition (Silvani et al., 2015; Silvani and Dampney, 2013). These central neural pathways may also explain other features of the baroreflex during NREM sleep, such as the baroreflex resetting toward lower values of heart rate, blood pressure, and SNA, and the greater baroreflex contribution to cardiac control than in wakefulness (Silvani et al., 2008). Taken together, these changes in baroreflex function may represent an important mechanism of the CNS-ANS coupling during sleep.
Neurons of the nucleus of the solitary tract control both cardiac parasympathetic activity, by means of a direct projection to preganglionic parasympathetic neurons in the nucleus ambiguus of the medulla, and cardiac SNA, by means of indirect projections to the rostral ventrolateral medulla (Silvani et al., 2016). At least in mice, the decrease in heart rate from wakefulness to NREM sleep is caused by strikingly balanced increases and decreases in parasympathetic and sympathetic tone to the heart, respectively (Lo Martire et al., IN PRESS). Sleep-related changes in the neural circuit involving the parabrachial nucleus and the nucleus of the solitary tract may thus contribute to drive the decrease in heart rate during NREM sleep. The hypothalamic paraventricular nucleus also receives synaptic projections from the hypothalamic suprachiasmatic nucleus, which control separate populations of pre-sympathetic and pre-parasympathetic neurons (Buijs et al., 2003). The suprachiasmatic nucleus is the master circadian clock responsible for the circadian rhythms of sleep (Easton et al., 2004) and cardiovascular variables (Janssen et al., 1994). Neurons in the suprachiasmatic nucleus decrease their activity during NREM sleep and increase it during REM sleep, suggesting that the link between suprachiasmatic nucleus activity and sleep is, actually, bidirectional (Deboer et al., 2003). Although much critical evidence is still missing, including on the neurochemical features of the suprachiasmatic neurons projecting to the paraventricular nucleus (Buijs et al., 2003), it is conceivable that this circuit plays a role in the integration of circadian and sleep-dependent central autonomic commands (Silvani et al., 2016).
1.2.2. Central autonomic commands during REM sleep
Episodes of REM sleep can be described as tonic or phasic. Tonic REM sleep refers to relatively long period of stable N1-like EEG and muscle atonia with relatively regular heart rate. Tonic REM sleep is interrupted by phasic burst in which eye movements occur and cardiovascular physiology becomes more unstable.
The cardiovascular changes that occur during episodes of REM sleep are largely distinct from those of NREM sleep, but may also be driven by central autonomic commands capable of biasing the arterial baroreflex (Silvani and Dampney, 2013). The neural circuitry responsible for the occurrence and control of REM sleep involves the glutamatergic sublaterodorsal nucleus of the pons as well as multiple GABAergic cell groups in the brainstem and hypothalamus (Luppi et al., 2017). The tonic periods of REM sleep entail disparate changes in SNA, consisting of decreases in renal and mesenteric SNA and simultaneous increases in skeletal muscle SNA (Yoshimoto et al., 2011). Moreover, recent data on mice indicate that the increase in heart rate on passing from NREM sleep to REM sleep is mediated, at least in part, by an increase in cardiac SNA (Lo Martire et al., IN PRESS). The increases in muscle and cardiac SNA during REM sleep may result from direct excitatory projections from the pontine sublaterodorsal nucleus to the pre-sympathetic neurons in the rostral medulla, which project to the sympathetic preganglionic neurons. Moreover, REM sleep reverses the reductions in the activity of the pedunculopontine nucleus and the parabrachial and solitary tract nuclei, which may underlie the reduction in muscle and cardiac SNA during NREM sleep (Silvani and Dampney, 2013). The disparate changes in SNA to the skeletal muscle, cardiac, mesenteric, and renal vascular beds during REM sleep may reflect modulations of pre-sympathetic neurons by neurons of the medullary raphe obscurus and the ventrolateral and lateral regions of the midbrain periaqueductal gray, which include both sympathoexcitatory and sympatho-inhibitory neurons (Futuro-Neto and Coote, 1982; Silvani and Dampney, 2013). Incidentally, the finding that SNA to different cardiovascular effectors undergoes opposing changes at the same time during REM sleep seriously challenges the concept of a unique central sympathetic tone during sleep. In this light, the existence of a global ANS index/measurement that can closely reflect the central ANS control during sleep appears unlikely, especially if the picture is broadened to include cardiac vagal control, the sympathetic control of thermoregulatory effectors such as brown adipose tissue, and the control of breathing, which is tightly linked to that of the cardiovascular system (Eckberg, 2003).
The occurrence of wide and bizarre fluctuations (‘unpredictable fugues’) of blood pressure and heart rate, which may or may not be associated with bursts of rapid eye movements, ponto-geniculo-occipital waves, and transient changes in the breathing pattern, characterizes the phasic periods of REM sleep (Silvani, 2008; Snyder et al., 1964). The medial and inferior vestibular nuclei in the medulla may play a key role in driving the autonomic and neurophysiological variability during phasic REM sleep (Morrison and Pompeiano, 1970). These nuclei may receive sleep-related synaptic input from the hypothalamic ventrolateral preoptic nucleus, and may modulate the activity of the pedunculopontine tegmental nucleus, the pontine parabrachial nucleus, and the medullary nucleus of the solitary tract (Silvani and Dampney, 2013). The centrally-driven changes in breathing pattern may also contribute to baroreflex modulation and cardiovascular variability during phasic REM sleep, at least in part, by modulating barosensitive neurons in the caudal ventrolateral medulla (Mandel and Schreihofer, 2006; Silvani and Dampney, 2013).
2. Observations: changes in ANS tone and modulation according to CNS-defined sleep stages
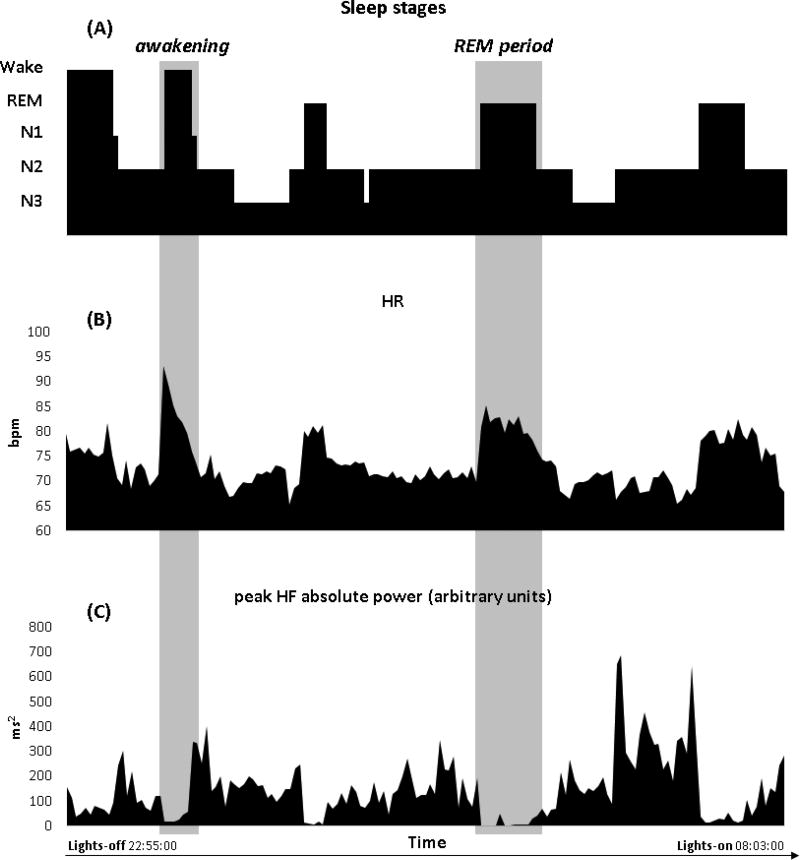
As described above, there are multiple top-down and bottom-up pathways that potentially could underlie the observed dynamic coupling between indices reflecting CNS (EEG) and ANS (cardiovascular variables) modulation during NREM and REM sleep and in relation to phasic sleep events within each sleep state. This section broadly describes how indices reflecting ANS tone and modulation, as measured non-invasively in humans, differ between sleep states. Figure 3 shows the temporal dynamic of heart rate and HRV indices plotted as a function of time of the night and stages of sleep from a PSG night of a sample participant from the SRI Human Sleep Research Laboratory. As indicated, ANS tone and modulation are profoundly influenced by the sleep – wake cycle such that sleep, or sleep related mechanisms, impose regulatory control over the cardiovascular system. The reader is also referred to more extensive reviews of this topic elsewhere (see Trinder, 2007; Trinder et al., 2012).
Figure 3.
In the top panel (A), sleep stages from a PSG night of a randomly selected participant from the SRI Human Sleep Research Program are plotted as a function of time of the night. Heart rate (HR) (B) and peak absolute power of heart rate variability (HRV) in the high-frequency (HF) range (C) were calculated within consecutive 2-min bins, and plotted as a function of time of the night and stages of sleep. Frequency domain HRV analysis was performed and parameters calculated according to Trinder et al. (2001)| It is noticeable how each variable showed specific variations with regard to sleep stage transitions (NREM sleep-to-wakefulness and NREM sleep-to-REM sleep transitions are highlighted in the figure).
The specific effect of the sleep – wake cycle on ANS function is masked by the influence of the circadian system, with the relative influences of the sleep – wake cycle and circadian system varying over different components of the ANS (see Trinder, 2007). Studies that have employed techniques (e.g., constant routine or forced desynchrony) to isolate circadian influences over cardiac function have shown that heart rate is strongly influenced by the circadian system, such that in the absence of sleep, heart rate has a marked sinusoidal pattern, being elevated during the time of normal wakefulness and depressed during the period of normal sleep (Burgess et al., 1997; Kerkhof et al., 1998; Kräuchi and Wirz-Justice, 1994; Van Dongen et al., 2001; van Eekelen et al., 2004). Two studies have identified a circadian influence over vagal modulation as assessed by respiratory sinus arrhythmia, but not over sympathetic activity as assessed by the pre-ejection period and other measures (Burgess et al., 1997; van Eekelen et al., 2004). Evidence of the effect of the circadian system on blood pressure is conflicting. Shea et al. (2011), in a series of 3 experiments with both constant routine and forced desynchrony designs, consistently identified a small circadian effect on blood pressure. In contrast, two previous studies using constant routine procedures did not find a circadian effect (Kerkhof et al., 1998; Van Dongen et al., 2001). These discrepant findings with respect to blood pressure may depend on whether participants in constant routine or forced desynchrony studies became sleep deprived.
While the diurnal rhythm in heart rate is largely determined by the circadian system, heart rate does show a small sleep-related fall at sleep onset, as previously mentioned (Burgess et al., 1999; Burgess et al., 1997). In contrast, blood pressure is strongly influenced by sleep (Carrington et al., 2003; Trinder et al., 2001). Blood pressure shows a substantial fall from wakefulness to stable N2 sleep and typically reaches its minimum diurnal value during the first hour of sleep (Trinder et al., 2001). This can be shown to be an effect of sleep as the fall in blood pressure is delayed in association with a delay in sleep (Carrington et al., 2003). Blood pressure also typically shows a small rise on passing from NREM sleep to REM sleep (Silvani, 2008). The resulting diurnal variation in blood pressure resembles a square-wave like function with a rapid fall at sleep onset and a rapid rise late in sleep and during morning wakefulness (Trinder et al., 2001). The fall in blood pressure early in the sleep period is referred to as a “Dipping Profile” and is considered to be beneficial (“a cardiovascular holiday”) and an indication of cardiovascular health (Staessen et al., 2001).
The fall in blood pressure over sleep onset is irregular. Initially there appears to be a small reduction of approximately 4 mmHg at the point that the decision is made to go to sleep, presumably at lights out under normal circumstances. This is followed by the onset of N1 sleep, a period of sleep-wake state instability characterized by fluctuations between dominant EEG alpha and dominant EEG theta rhythm. Each transient entry into dominant EEG theta rhythm is associated with a fall in blood pressure and each transient period of dominant EEG alpha rhythm is associated with an increase in blood pressure. However, once stable N2 sleep is attained (i.e., sleep onset is achieved) the resulting state stability is associated with lower and stable blood pressure (Carrington and Trinder, 2008).
During sleep, ANS function is influenced by sleep state. Heart rate and blood pressure levels are decreased below the levels of relaxed wakefulness during NREM sleep, and rise again towards the levels of wakefulness during REM sleep. HRV analysis suggests stronger vagal modulation during NREM sleep, while sympathetic vascular tone presumably falls in skeletal muscles, kidneys, and skin as previously described (Silvani and Dampney, 2013), resulting in peripheral vasodilation (Trinder et al., 2001; Van de Borne et al., 1994). In particular, data from microneurography has indicated a progressive drop in muscle SNA in NREM sleep with increased burst rate of muscle SNA in REM states (Hornyak et al., 1991a; Okada et al., 1991; Somers et al., 1993). While NREM sleep may be associated with an increase in baroreflex sensitivity (Conway et al., 1983), which is initiated during sleep onset (Carrington et al., 2005), this is not a consistent finding (Silvani, 2008). Nonetheless, the simultaneous falls in heart rate and blood pressure during NREM sleep suggest downward resetting of the baroreflex. With the exception of heart rate, cardiovascular function within each given sleep stage tends not to vary across the night. Thus, the over-night profile for a cardiovascular variable is mainly a consequence of the changing distribution of sleep stages over the night. Changes in heart rate within a sleep stage as a function of time most likely reflect the strong circadian influence on this variable. Finally, two additional features of REM sleep should be noted. First, both the average level of cardiovascular activity and its variability are higher during REM sleep than during NREM sleep. Second, the cardiovascular features of REM sleep are initiated before other overt features, such as eye movements and muscle atonia (Cajochen et al., 1994).
Sleep-dependent changes in central autonomic and baroreflex control of heart rate have been investigated by the analysis of the coupling (cross-correlation functions) between spontaneous fluctuation in heart period (the reciprocal of heart rate) and systolic blood pressure at < 0.15 Hz (and thus independent of the coupling between heart period and systolic blood pressure at the breathing frequency). Specifically, the greatest baroreflex contribution to the coupling (baroreflex coupling: highest positive correlation between heart period and the previous values of systolic blood pressure) occurred in NREM sleep stage N3 (Silvani et al., 2008).
Summary of observational evidence of CNS-defined sleep stage dependent changes in ANS modulation.
Cardiovascular function during sleep results both from the influence of the circadian system and from the effects of the wake-sleep states (wakefulness, NREM sleep, and REM sleep). The circadian rhythm elicits a stronger effect on heart rate than on blood pressure. While the return of sustained wakefulness stably reasserts wakefulness functioning, the process of arousing from sleep elicits a transient, large, ANS activation response, the waking reflex (see section 3.1). As will be discussed in the following section, when arousals are frequent, the waking reflex introduces substantial instability in the cardiovascular system. This is an important aspect to consider when interpreting within-night variations in EEG-ECG coupling (Section 4).
Few laboratories are equipped to comprehensively assess ANS function during sleep. The behavior of the sympathetic nervous system during sleep is not yet fully understood, partly due to measurement limitations (e.g., invasiveness of microneurography, making it difficult to assess SNA without disturbing sleep, and limitations in interpretation of HRV indices in terms of sympathetic modulation). Conversely, assessment of cardiac vagal ANS modulation with HRV analysis is now widely accessible in routine PSG assessment. However, its integration with measures of the sympathetic nervous system is still limited. Studies employing the simultaneous registration of multiple sources of ANS modulation are necessary.
3. ANS and/or CNS mediated perturbations: CNS-ANS coupling across phasic sleep events (grand-average and ERP designs)
A clear manifestation of the CNS-ANS interplay during sleep is evident from the reciprocal cortical and autonomic fluctuations during phasic, transient sleep events. Phasic sleep events are mainly considered manifestations of transient cortical synchronization and/or desynchronization. The majority of studies directly investigating cortico-cardiac coupling during transient sleep events have time-aligned the analysis to the EEG-defined phasic sleep events, and considered the peripheral changes as ANS correlates of the cortical events. One exception is in the study of heartbeat-evoked potentials, where the causality assumption is reversed and the EEG data are time aligned with the ECG R-waves. A heartbeat-evoked potential is considered a cortical EEG brain wave that appears contiguous with the heartbeat, and is thought to reflect cortical processing of cardiac afferent inputs. However, although findings using intracranial EEG in human seem to support the neuronal origin of heartbeat-evoked potentials (Kern et al., 2013; Park et al., 2017), it is still debatable whether it is possible to separate cortical and non-cortical electrical activity. This leads to question whether the heartbeat-evoked potential reflects a true neuronal response to afferent ANS signals or merely results from ECG artifacts on the EEG recording or confounders from other brain and non-brain pulsing sources. The reader is referred to Lechinger et al. (2015) for an example of a study investigating heartbeat-evoked potentials during sleep.
3.1. Phasic EEG desynchronizations: arousals
In the context of sleep, the term arousal, or arousal response, refers to the transition from sleep to wakefulness, as defined by changes in the EEG (e.g. from theta/delta to predominantly alpha rhythm), along with activation of other physiological systems such as CV and respiratory systems (Silvani et al., 2015). Thus, arousal from sleep is associated with large, rapid and transient increases in both heart rate and blood pressure with peak responses of around 8 bpm at ~4 s for heart rate and of around 15 mmHg at ~5 s for blood pressure. Both heart rate and blood pressure return to the pre-arousal baseline after ~12 s, and may rebound below this level, particularly if the participant has returned to sleep; thus the initial arousal response and the subsequent return to sleep have independent effects on the profile of the cardiovascular response (Trinder et al., 2003, experiment 3). There is also a vasoconstriction response which is considered the primary mediator of the blood pressure increase. The response profile is similar whether arousals are elicited by an external stimulus or are apparently spontaneous, although in the latter arousals the heart rate response (tachycardia) precedes cortically indicated arousal by approximately 2 beats. The cardiovascular response to an arousal from sleep is thought to be a reflex response during which normal regulatory control is suspended (Horner et al., 1997), the response being elicited by the arousal itself, while its magnitude appears to be independent of the sleeper’s physiological status, such as the level of respiratory drive provided by the partial pressure of CO2 in the blood (Trinder et al., 2006), or psychological status, such as elevated anxiety (Trinder et al., 2003, experiment 2A). The cardiovascular arousal response occurs in response to the vast majority of arousals; its assumed functional significance being to rapidly reinstate wakefulness levels of cardiovascular functioning in anticipation of the possibility that the cause of the arousal is threatening. From this perspective it has been referred to as “The Waking Reflex” (Trinder et al., 2003). The occurrence of a substantial cardiovascular response at arousal from sleep is considered to be one cause of the elevated risk of cardiovascular disease in patients with sleep disorders such as obstructive sleep apneas, that are characterized by frequent arousals (see Trinder et al., 2012). The blood pressure response to repeated arousals in particular may lead to a non-dipping hypertensive profile (Wolf et al., 2010).
3.2. Phasic EEG synchronization: K-complexes
Evidence shows that ANS fluctuations also occur in association with some forms of EEG cortical synchronization, i.e. K-complexes. K-Complexes are thought to reflect the synchronized activity of a large number of cortical neurons and can be viewed as phasic changes in the excitability of cortical and thalamic circuitry in the brain. K-complexes are characterized by a positive-negative-positive EEG waveform which lasts at least half a second; they can be evoked by an external stimulus, such as sound, or they can occur spontaneously (Colrain, 2005); they are exclusively seen in NREM sleep and are more likely to occur in N3 than in N2 (Cote et al., 1999). Both spontaneous (De Gennaro et al., 2000) and evoked (Nicholas et al., 2006) K-complexes in N2 are more likely to occur preceding transitions to N3 than transitions to REM. Consistent with delta rhythm generally, spontaneous K-complex density progressively lessens across sleep cycles (De Gennaro et al., 2000; Halász et al., 1985).
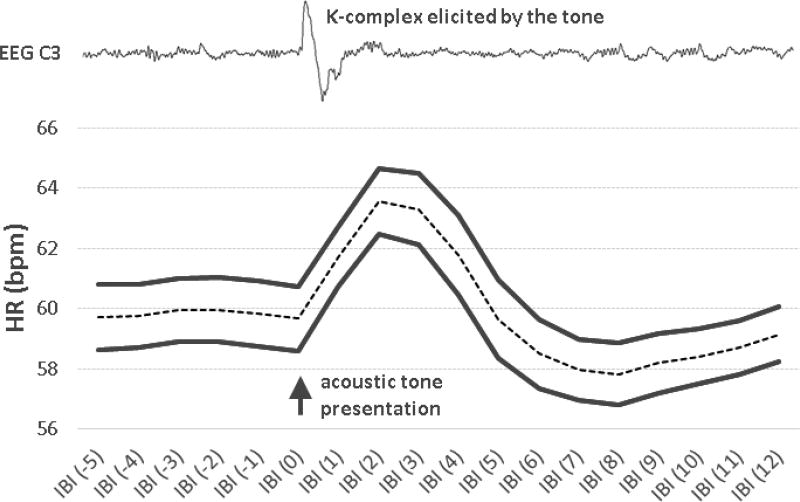
Research has mainly focused on CNS processes involved in K-complex generation, with less attention given to the related peripheral ANS physiology, although ANS activation associated with a K-complex (reported in terms of heart rate, blood pressure, muscle SNA (Colrain, 2005)) has historically been used in the debate over whether a K-complex is an arousal or a sleep-promoting response (see Sforza et al., 2000). In this context, both synchronous EEG (K-complexes, or bursts of slow waves) and cardiovascular activations are seen as responses to arousal from sleep, where arousal is conceptualized as a change in the direction of wakefulness. Recently, our team investigated the temporal dependency between K-complexes (auditory-evoked and spontaneous) and heart rate in young adults (de Zambotti et al., 2016b). Specifically, we showed that, as with EEG-defined arousals from sleep (Trinder et al., 2003), spontaneous and tone-evoked K-complexes were accompanied by a biphasic fluctuation in heart rate. This fluctuation was characterized by initial tachycardia (exceeding pre-tone baseline levels by more than 5%) occurring on average 1–2 beats after the beginning of the K-complex, followed by bradycardia which peaked, on average, between 7 to 10 beats after the K-complex (Figure 4). Also, our results clearly indicated that when acoustic tones played during N2 sleep were not accompanied by a K-complex, the biphasic heart rate fluctuation was reduced or absent (the small heart rate acceleration in the no-K-complex trials most likely reflected phasic EEG synchronizations or desynchronizations which were not recognizable through the visual selection of the trials). This indicates that the biphasic heart rate fluctuation was not simply a reaction to the tone, but, rather, reflected some dependency between CNS and ANS processes (de Zambotti et al., 2016b). A biphasic fluctuation in heart rate (cardiac acceleration and following deceleration) is not only related to isolated K-complexes but is also associated with K-bursts (a sequence of two or more K-complexes) and delta bursts (a sequence of delta waves) (Johnson and Karpan, 1968; Sforza et al., 2000), which can be considered as other forms of phasic EEG synchronization events. In this context, investigations of other alterations in EEG synchronization during sleep such as the Cyclic Alternating Pattern have also shown associated changes in heart rate and HRV (Ferini-Strambi et al., 2000; Ferri et al., 2000).
Figure 4.
Biphasic (initial tachycardia followed by bradycardia) cardiac response, displayed across subsequent inter-beat-intervals (IBIs), to evoked electroencephalographic (EEG) K-complexes in a sample of 37 adolescents. Means (dotted line) and standard errors (thick solid lines) of heart rate (HR) are displayed. Data from de Zambotti et al. (2016b).
As indicated above, in addition to heart rate changes, K-complexes are also associated with a rise in blood pressure (Monstad and Guilleminault, 1999; Somers et al., 1993; Tank et al., 2003) and an increase in muscle SNA (Somers et al., 1993; Tank et al., 2003). A stereotypical temporal sequence of ANS fluctuations, with increases in heart rate followed by a surge in blood pressure, and then a return to or below baseline seems to be associated with both phasic EEG synchronization (e.g., K-complexes) and desynchronization (e.g., arousal events; in which case, the occurrence of the full biphasic sequence possibly reflects the resumption of sleep) (Silvani and Dampney, 2013). A summation of the effects of central autonomic commands time-locked to the phasic sleep events and of the underlying baroreflex control may explain this pattern (Silvani et al., 2011): the initial rise in heart rate and blood pressure may be caused by central commands temporarily overriding or “biasing” (resetting) the baroreflex, whereas the later reduction in heart rate may indicate the resumption of the pre-arousal features of baroreflex control, such as a return to sleep following an arousal, once the central commands are over. Accordingly, Hornyak et al. (1991b) also argued that “the K-complex is associated with a non-baroreflex-mediated increase of vasoconstrictor drive to skeletal muscle vessels.” (p1291) However, whether ANS correlates of K-complexes and arousals share similar physiological pathways still needs to be determined. It is also possible that both the EEG response and cardiovascular activation are responses to arousal mechanisms operating at a sub-cortical level and thus not identifiable by conventional EEG recordings, according to the conceptual model shown in Figure 2. Further, it is possible that in the case of the K-complex, the recruited synchronized EEG response acts as a mechanism to prevent cortical arousal from occurring (Colrain, 2005).
Centering attention on ANS events, there is evidence suggesting that specific ANS states and/or phases of cardiovascular rhythms are associated with the occurrence of specific sleep EEG manifestations. Several typical cardiovascular oscillatory rhythms exist. For example, the myocardium cyclically alternates between phases of depolarization and repolarization of ventricles and atria, thus determining the cardiac rhythmicity or heart rate, approximately on a second-by-second basis. On a different time-scale, the cardiac rhythm accelerates and decelerates in synchrony with alternation of inspiration and expiration within the breathing cycle (a phenomenon known as respiratory sinus arrhythmia). Also, blood pressure spontaneously fluctuates during both day and night at a slower frequency than breathing (reported at around 0.1 Hz, an oscillatory rhythm frequently known and possibly misnamed as “Mayer waves”) (Julien, 2006). Interestingly, in our previous investigation we found that the relationship between tone-elicited K-complexes and associated heart rate changes differed based on the time within the cardiac cycle in which the tone occurred (de Zambotti et al., 2016b). This suggests that there is a specific window in the cardiac cycle in which the K-complex can have an effect on subsequent heart rate, perhaps reflecting time-dependent sensitivity of the sinoatrial node to parasympathetic modulation (Eckberg, 1976). We also found that tone-evoked K-complexes were more likely to be elicited when the pre-K-complex rhythm of heart rate was slower, leading to the possibility that specific ANS states may facilitate cortical synchronization (de Zambotti et al., 2016b; Otzenberger et al., 1997; Trinder, 2007). This hypothesis is supported by other lines of evidence concerning the arterial baroreflex and the activity of the nucleus of the solitary tract in the medulla (Silvani et al., 2015). Additional evidence of possible CV/ANS facilitation of K-complexes comes from Monstad and Guilleminault (1999), who found that spontaneous K-complexes predominantly occurred during the downward slope of the so-called Mayer wave (~0.1 Hz) of blood pressure, implicating a relationship between blood pressure oscillatory state and K-complex occurrence. However, Tank and coworkers (2003) showed that not all the K-complexes are secondary to changes in blood pressure as evidenced by the fact that in their study, about half of the large isolated K-complexes were preceded neither by a drop in blood pressure nor by an increase in muscle SNA. This suggests that some K-complexes may occur in the presence of a baroreflex-mediated sympathetic activation, while other K-complexes do not.
Summary of the analysis of ANS and/or CNS mediated perturbations.
Phasic EEG sleep events are accompanied by stereotypical ANS fluctuations, such as increases in heart rate and blood pressure temporally coupled to the events. Of clinical relevance, frequent transient cardiovascular surges due to repeated arousals could lead to long-term impact on the cardiovascular system.
It is still unclear whether phasic EEG desynchronizations and synchronizations share similar physiological pathways. The role of both central commands and autonomic reflexes (e.g., baroreflex-mediated sympathetic activation) are among the mechanisms thought to be responsible for this stereotypical ANS pattern.
Most attention has been paid to the ANS fluctuations occurring during and after CNS-mediated phasic events. More insight is needed to understand temporal CNS-ANS coupling before the CNS as well as ANS events are “triggered” to understand how different CNS-ANS coupling dynamics may potentially lead to EEG synchronization/desynchronization events, or specific ANS oscillations.
Study of ANS and/or CNS mediated perturbations in populations with selective CNS or ANS lesions/dysfunction, or under medications acting on selective CNS and or ANS function may further advance the understanding of directionality and causality of the coupling.
4. Analytics of continuous CNS-ANS dynamics
Advanced signal processing techniques promise to offer new insights into the relationships underlying the complex dynamic interplay between CNS and ANS processes during sleep. A number of observational studies have focused on the coupling between spontaneous fluctuations of the EEG and either heart rate or HRV indices. The reason for this emphasis is that sleep is principally defined by the EEG, eye movements (measured with the electrooculogram), and muscle activity (measured with electromyograms), and ECG is a standard additional signal routinely recorded in PSG assessments, which allows easy extraction of non-invasive measures of cardiac ANS function. Thus, a growing body of data relating EEG spectral indices to HRV metrics is now available using different techniques, particularly linear methods including scatterplots, cross-correlation coefficients, spectral gain and coherence, across the whole-night sleep period or within specific time windows across the night.
4.1. Characteristics, time delay and directionality
While there have been several attempts to evaluate EEG-ECG coupling during sleep using variants of cross-correlation analysis, the generalizability of study outcomes is questionable due to small subject numbers and the almost exclusive study of male subjects. In addition, studies suffer from a relatively gross time assessment, with units of time being between 1 and 10 minutes, and lack of specificity in terms of EEG analyses. For example, Otzenberger et al. (1997) used 1-minute averages and found that variations in the non-linear Poincaré plot inter-beat autocorrelation coefficient (See section 1.1) were correlated with changes in mean EEG frequency within a broad 0.5–35 Hz band in all 12 healthy male subjects under study (r values ranging between 0.267 and 0.638). Changes in the inter-beat autocorrelation coefficient preceded the changes in EEG by 1–2 minutes. Unfortunately, as previously mentioned, specific ANS contributions to the inter-beat autocorrelation coefficient are difficult to disentangle. Also, the use of the EEG mean frequency does not allow inference as to which specific EEG oscillatory rhythms were involved in the CNS-ANS relationship. Focusing on power within the delta EEG band (0.5–3.5 Hz), Charloux et al. (1998) conducted a similar analysis using broader (10 min) time windows, taking into account also plasma renin activity, which plays a role in the control of blood pressure. Previous studies had shown that plasma renin activity strongly follows sleep stage fluctuations, increasing during NREM sleep and decreasing during REM sleep (see Brandenberger et al., 1985). Charloux et al. (1998) reported that decreases in the inter-beat autocorrelation coefficient preceded both increases in EEG delta power (5 out of 9 male subjects under study, with the remaining 4 subjects showing zero-lag correlations; r values ranging between −0.30 and −0.65) and increases in plasma renin activity (all subjects, r values ranging between −0.29 and −0.65). Increases in EEG delta power were concomitant with (4 subjects) or preceded (5 subjects) those in plasma renin activity, with r values ranging between 0.29 and 0.65. These associations were detectable during sleep, but not during the waking period. In a subsequent study (Charloux et al., 2002), the same group showed that the fluctuations in plasma renin activity occurred concomitantly with or after (0–10 min) increases in EEG delta power, and were preceded (10–20 min) by a drop in both HRV LF/(LF + HF) ratio and intra-arterially-measured mean blood pressure. Unfortunately, the use of the inter-beat autocorrelation coefficient and of the HRV LF/(LF + HF) ratio did not allow the authors to draw definite conclusions on the sympathetic involvement in the fluctuation of renin release. The mechanism underlying the near-simultaneous fluctuations in plasma renin activity and EEG delta power is also still unclear. A plausible explanation is that, according to the discussed in section 1.2, NREM sleep entails both increases in EEG delta power and decreases in blood pressure. The decrease in blood pressure during NREM sleep is sensed by smooth muscle (i.e., renal afferent arteriole) and neural baroreceptors, triggering an increase in plasma renin activity (Charloux et al., 2002). Importantly, both sympathetic ANS and renin-angiotensin system are involved in the regulatory control of blood pressure; the study of their interdependency and relation with EEG cortical synchronization should adopt more direct measures of sympathetic ANS function and greater temporal resolution to disentangle their functional organization.
Specific sleep stage-dependent relationships between EEG and HRV seem to exist. Brandenberger et al. (2001) using 5-minute intervals showed that the fluctuation in LF power of HRV mirrored (inverse coupling) the oscillations in EEG delta power across sleep cycles with a −5 ± 5 minute lag (r values ranging between 0.38 and 0.73) in 9 male subjects. In a subsequent investigation, the same group (Brandenberger et al., 2005) used 10-minute intervals to evaluate differences between N3 and REM sleep across three sleep cycles in 14 healthy male subjects and showed that changes in HRV indices (total variability–SDNN index–, LF/(LF+HF) HRV ratio, and inter-beat autocorrelation coefficient) preceded changes in EEG delta power by one time interval in all subjects but one.
In the only study to evaluate temporal relations between EEG and ECG indices on a sub-minute time frame, using large numbers of women and men (n= 3150), Thomas et al. (2014) evaluated the temporal relations between the ratio of HF (0.1–0.4 Hz) to LF (0.01–0.1 Hz) cardiopulmonary coupling (reflecting the coupling between heart period and respiratory-related changes in amplitude of ECG QRS complexes) and delta EEG power (0.3–4 Hz). Results varied as a function of whether absolute (mean r = 0.34 ± 0.19) or normalized (mean r = 0.40 ± 0.18) values of EEG delta power were used, and depending on the time of night evaluated. Increases in the HF/LF ratio of cardiopulmonary coupling tended to precede increases in delta EEG. The median (25th, 75th percentile) lag for absolute EEG delta power was −6.4 (−8.53, −2.13) min but the mean (± SE) lag was essentially zero (0.01 ± 1.16 min). Of note, they reported that both slow-wave sleep (corresponding to N3) and HF cardiopulmonary coupling were significantly higher in women than in men. Although the correlation between EEG delta power and HF cardiopulmonary coupling did not differ with sex across the whole night, men did show a small but significant increase relative to women in the second half of the night (r = 0.35 vs. 0.33). The study included data from a large dataset of at-home PSG recordings of adults of ≥ 40 y. The authors restricted the analysis to those participants with apnea-hypopnea index ≤5 events per hour of sleep, and excluded subjects with atrial fibrillation, ventricular bigeminy, and pacemakers. However, some participants reported medical conditions such as diabetes (8%), prior myocardial infarction (5%), angina (6%), stroke (2.7%) and hypertension (33.7%). This is relevant because sample characteristics may affect CNS-ANS coupling (see section 4.3).
Some attempts have been made to assess the directionality of the CNS-ANS coupling. Abdullah et al. (2010a) used a combination of the traditional linear cross-correlation method, information theory (mutual information method, which allows the capture of linear and non-linear dependence) and non-linear interdependence (which allows the derivation of directionality in the relation between time series) to study the relationships between EEG and ECG time series during sleep. Results from the mutual information approach revealed an increase in information transfer between heart and brain in deep sleep (N3). However, by using a different phase synchronization approach the same authors (Abdullah et al., 2012) found that the directionality in the cortico-cardiac coupling tended to be unidirectional from brain to heart, contrasting with the previous results and raising the question whether these methods will be ultimately able to disentangle the dynamics of both afferent and efferent projections between brain and heart. Faes et al. (2015) analyzed the EEG-HRV coupling in ten healthy young subjects. By using Granger causality and transfer entropy (measuring directed interaction in multivariate time series) the authors suggested that the causal heart-to-brain direction predominated for the transfer of information between the strength of the cardiac vagal component of HRV and the amplitude of sleep EEG signal.
While the extant literature is limited, and the temporal and directional relations between ANS and CNS changes in sleep are unclear, it would appear that cardiac ANS measures oscillate in phase with cortical CNS measures between sleep states in which delta EEG is dominant or not, with some indication that the cardiac changes may precede the EEG changes.
4.2. Influence of time of night and sleep stages
A number of studies have investigated the relationship between the time courses of EEG spectral power and HRV indices during sleep. However, methods have not been consistent. Some studies have considered a single EEG frequency band (e.g., alpha), used absolute or normalized EEG power, used different HRV indices, focused on different time periods across the night, as well as used different statistical methods ranging from simple correlations to more complex non-linear approaches. Not surprisingly, these studies have elicited a variety of different results. Ehrhart et al. (2000) found that different relationships between EEG alpha power and HRV indices were dependent on sleep state in 10 young male participants. The time course of EEG alpha power during sleep was in counterphase with heart rate and the HRV LF/HF ratio in NREM sleep and REM sleep: alpha power was high in NREM sleep in association with low values of heart rate and HRV LF/HF ratio, whereas alpha power was low in REM sleep in association with high values of heart rate and HRV LF/HF ratio. In contrast, EEG alpha power and HRV indices were in phase during intra-sleep awakenings, when values of EEG alpha power, heart rate, and HRV LF/HF ratio were all high. Kuo et al. (2016) investigated relationships between HRV indices and EEG alpha or beta power in eighteen healthy young participants (9 women). The authors found no relationships between EEG alpha power and HRV indices. However, there was a significant positive correlation between HRV LF/HF ratio and EEG beta power in NREM sleep, and significant positive correlations between EEG beta power and HRV HF power and LF/HF ratio in REM sleep. Ako et al. (2003) considered EEG power in the delta, sigma and beta frequency bands in seven healthy males and showed that EEG delta power correlated negatively with HRV LF power and the HRV LF/HF ratio but not with HRV HF power; none of the other EEG frequency bands had power that correlated with any HRV indices. Similarly, in ten young healthy subjects (7 women), Yang et al. (2002), found that during “quiet sleep” (characterized by delta waves), HRV LF/HF ratio, but neither HRV HF power nor mean RR interval, was related to EEG delta power (although HRV HF power was higher in “quiet sleep” than in wakefulness, as expected). Based on these data, the authors suggested that changes in HRV HF power may be independent of changes in EEG delta power. In contrast, a large and comprehensive assessment of the dynamic relationship between EEG delta power and HRV in 197 midlife women revealed strong, positive correlations in whole-night delta EEG power and HRV HF power, although the dynamics of this relationship varied within and across NREM sleep periods (Rothenberger et al., 2015). Within the first and second NREM periods, the time-varying correlation between EEG delta power and HRV HF power had a bi-modal profile, with strongest correlations before and following the peak of EEG delta power. Interestingly, time-varying correlations between EEG delta power and HRV HF power dropped dramatically in the third NREM sleep period. Similarly, Thomas et al. (2014) showed that the relationship between HF (0.1–0.4 Hz) cardiopulmonary coupling and EEG delta power was weaker in the second than in the first half of the night.
Studying a sample of nine healthy young men, Jurysta et al. (2003) considered all the main conventional EEG frequency bands and demonstrated high spectral coherence (> 0.50) between HRV HFnu power and EEG power in each frequency band (delta, 0.5–3 Hz; theta, 3–8 Hz; alpha, 8–12 Hz; sigma, 12–16 Hz; beta, 16–25 Hz). The highest transfer function gain (greatest magnitude of linear changes in the cortical oscillation per unit change in autonomic oscillation) was found for the delta band. Importantly, HRV HF power fluctuations consistently preceded (the phase shift differed from zero) those in the EEG delta power by about 12 min, suggesting that increases in vagal modulation may precede increases in EEG delta power. In subsequent work, Dumont at al. (2004) further investigated the non-linear properties of this relationship using synchronization likelihood in eight healthy young men. The authors showed that for some EEG frequencies (delta, theta and alpha), the EEG-HRV interdependency was non-linear. This work illustrates the complex dynamics of brain-heart communication, in which integrated CNS-ANS mechanisms work at different time-scales resulting in outcome signals of great complexity, which non-linear methods may be more suitable to capture than linear methods.
It is also important to emphasize that the physiological mechanisms of cortico-cardiac pathways underlying any relationship involving HRV LF power or LF/HF ratio or other HRV indices remain unclear. For example, the slow HRV oscillations (initial cardiac acceleration and following deceleration) accompanying phasic EEG desynchronizations (e.g., arousals from sleep) and synchronizations (e.g., spontaneous isolated K-complexes, which have a frequency similar to delta waves) across the night increase the HRV LF power (see de Zambotti et al., 2016b) and may partially explain the stronger EEG-HRV correlations found when HRV indices based on LF power are considered. The complexity of the EEG-HRV relationship is further highlighted by the fact that HRV changes across sleep stage transitions may not be uniform. For example, evidence indicates that HRV LF/(LF+HF) ratio (as well as the total variability of heart period -SDNN index- and the inter-beat autocorrelation coefficient) progressively decrease across an N2 period that evolves into N3, whereas a stable HRV LF/(LF+HF) ratio characterizes N2 periods preceding REM sleep (Brandenberger et al., 2005). Also, transitions between wakefulness and sleep and between light and deep NREM sleep are characterized by negative EEG-HRV time lags (−3 to −1 min), with changes in HRV preceding those in EEG (Long et al., 2015). Differently, no time lag was found for NREM-REM sleep transitions (Long et al., 2015). Together, these data complement the view that N2 sleep is not a uniform state in terms of K-complex density. In particular, the density of phasic K-complexes linearly increase when N2 sleep precedes N3. On the contrary, the density of K-complexes remains unchanged in the condition in which NREM sleep stage N2 evolves into REM sleep (De Gennaro et al., 2000).
4.3. Influence of demographic factors
ANS functioning (Bonnemeier et al., 2003; Brandenberger et al., 2003; Umetani et al., 1998) and CNS-defined sleep macro- and micro-structure (Carrier et al., 2001) undergo profound changes across the lifespan, exhibiting age- and sex-specific differences as well as sex-by-age interactions. This begs the question of whether the EEG-HRV coupling is also sensitive to the effects of age and sex.
The majority of studies investigating sleep-dependent EEG-HRV relationships have primarily included young healthy male participants. Further, the few studies that included women, and participants across a wide age span, did not consider or were underpowered to explore potential sex differences, age effects, and sex-by-age interactions. Thus, few studies accounted for these factors as well as other potentially relevant demographic (e.g., ethnicity, reproductive state) and behavioral (e.g., alcohol and caffeine consumption, use of sleep aids) factors known to affect ANS and/or CNS.
Jurysta et al. (2005) performed a cross-sectional study to investigate the relationship between the HRV HFnu power and normalized EEG delta power (0.5–3.0 Hz) during the first three NREM-REM sleep cycles in a group of middle-age (36–54 y) males compared to a group of younger males (16–28 y). Their results indicated that spectral coherence (which was greater than 0.50 in all participants) and transfer function gain and phase shift did not differ between healthy young and middle-age participants, suggesting that age does not alter the interaction between ANS and CNS processes. In agreement with previous studies (see above), HRV HF power changes preceded EEG changes in both young and middle-age participants. However, consistent with the literature, the authors found that middle-age participants compared to the younger group had reduced duration of slow-wave sleep (corresponding to N3) and percentage of EEG delta power, shorter RR intervals (faster heart rate) and increased HRV LFnu power. Thus, age may have independent effects on the ANS and CNS system without influencing the CNS-ANS interaction.
Similarly, Thomas et al. (2014) showed that the relationship between EEG delta power and HF cardiopulmonary coupling was maintained across different age groups (<40 y, 41–49 y, 50–59 y, 60–69 y, 70–79 y, >80 y) with the exception of the >80 y group, in which the relationship was significantly weaker than in all the other age groups. Results were maintained after adjusting for the amount of N3 sleep. In the same investigation, the authors reported the lack of sex differences in the coefficient of correlation between EEG delta power and HF cardiopulmonary coupling (r = ~ 0.46 in both men and women). However, during periods of rapid development of the CNS and ANS, such as across adolescence, sex differences in CNS-ANS coupling may manifest (de Zambotti et al., 2016b). In a study from our group on healthy male and female adolescents and young adults, girls had different ANS fluctuations associated to K-complexes than boys. Specifically, despite having similar K-complex features on cortical EEG (similar mean N550 latency and amplitude), girls had blunted and delayed heart rate accelerations associated with phasic tone-evoked K-complexes (de Zambotti et al., 2016b). Given the sparse literature, further studies are needed to investigate potential sex differences in CNS-ANS coupling at different life stages.
Despite not directly addressing the effect of demographic factors, individual characteristics and behaviors, Rothenberger et al. (2015) demonstrated that the relationship between EEG delta power and HRV HF power survived after adjustment for age, race, body mass index, reproductive stage (pre-, early-, late- and post-menopausal status), presence of vasomotor symptoms, caffeine consumption and use of medication affecting sleep (e.g., hypnotic and sedatives, antidepressants) in midlife women. In contrast, Thomas et al. (2014) showed a moderate effect of ethnicity in the relationship between HF cardiopulmonary coupling and EEG delta power with the highest correlations in the Asian/Pacific Islanders whereas the black and Native American/Alaskan subjects showed smaller correlations compared to white subjects.
4.4. Sleep disorders and other mental and medical conditions
The previous sections show that a dynamic interplay between brain and heart normally occurs in healthy sleep. It is possible that the efficiency of CNS-ANS coupling is a prerequisite for system homeostasis. Sleep disruption (alterations in macro- and/or micro-structure) such as may occur in association with medical conditions and/or sleep disorders (e.g., breathing-related disorders, insomnia disorder, restless legs syndrome, narcolepsy, REM sleep behavior disorder) may be associated with ANS and cardiovascular dysfunction (Calandra-Buonaura et al., 2015; Miglis, 2016; Silvani et al., 2016), and also potentially with alterations in EEG-HRV coupling.
A handful of studies have investigated the impact of sleep apneas and hypopneas on EEG-ECG coupling. Thomas et al. (2014) explored the strength of the CNS-ANS relationship as a function of the apnea hypopnea index and found a moderate reduction in the strength of the relationship only in the group of subjects with >30 apnea/hypopnea events per hour of sleep. In contrast, Rothenberger and colleagues (2015) showed that the strength of the EEG-HRV relationship within NREM sleep periods was stronger in women with sleep disordered breathing and self-reported insomnia compared to controls. Jurista and colleagues (2006) showed that the EEG-HRV relationship is altered (decrease in coherence and gain between HRV HF power and EEG delta power) in patients with obstructive sleep apneas. Later, they showed that the altered EEG-HRV relationship in patients with obstructive sleep apneas normalizes to some extent under long-term treatment with continuous positive airway pressure (Jurysta et al., 2013). When the same group (Dumont et al., 2007) re-analyzed the EEG and ECG data series from Jurysta et al. (2006) using a non-linear approach (synchronization likelihood) instead of a conventional linear investigation, they obtained different results: obstructive sleep apneas did not affect the non-linear interdependence between HRV HF power and EEG delta power either using the whole night data or restricting the analysis to specific NREM-REM sleep cycles. These opposing findings from the same dataset illustrate the dramatic effect that different methodologies have on outcomes, and highlight that interpretation of the data arising from studies using sophisticated linear or non-linear analyses needs to be interpreted cautiously. Given such contrasting findings between studies and when applying different analytical techniques to the same dataset, it remains unclear whether there is any impact of sleep-disordered breathing on EEG-HRV coupling.
An altered EEG-HRV relationship was also found in insomnia disorder (Jurysta et al., 2009), as well as in major depressive disorder (Jurysta et al., 2010). Jurysta and colleagues (2009) reported decreased linear coupling and a more variable phase shift between normalized HRV HF power and EEG delta power in patients with insomnia compared to controls, even in the absence of group differences in standard HRV indices and sleep stage-dependent shifts in ANS control. The study of CNS-ANS coupling in insomnia disorder may provide new information about the state of hyperarousal – thought to be a key factor in insomnia pathophysiology (Bonnet and Arand, 2010; Riemann et al., 2010). In particular, the study of CNS-ANS dynamics may be relevant across the sleep onset period, in which cognitive alterations (e.g., intrusive thoughts, anxiety, over worry) (Harvey, 2000) together with cortical (Lamarche and Ogilvie, 1997) and autonomic (de Zambotti et al., 2011) alterations in insomnia seem to be magnified.
Almost no information is available on the investigation of CNS-ANS coupling in cardiovascular disorders. Surprisingly, Thomas et al. (2014) indicated that the nighttime correlation between HF cardiopulmonary coupling and EEG delta power was not affected by the presence of self-reported diabetes, ischemic heart disease, stroke, hypertension, and chronic obstructive pulmonary disease, and that it did not differ significantly between subjects who took sleep medications like benzodiazepines and antidepressants and those who did not.
Recent work has explored the potential use of computational methods in assessing the functional interdependency between EEG and HRV oscillations as a diagnostic tool for screening for insomnia and schizophrenia (Chaparro-Vargas et al., 2016) or sleep apnea (Abdullah et al., 2010b) as well as to monitor post-treatment recovery (e.g., evaluate the effect of positive airway pressure therapy) (Faes et al., 2016). However, given the contradictory findings about the impact of sleep disorders on EEG-HRV coupling, more work is clearly needed before determining whether these computational methods are clinically useful.
4.5. Network physiology
ANS-CNS coupling could be considered within the framework of an emerging interdisciplinary field, “network physiology“. Network physiology considers the human organism as an integrated network in which different biological systems with their own structure, regulatory mechanisms and complexity dynamically interact and coordinate their behavior to generate an individual’s psychophysiological state (Ivanov et al., 2016). Time delay stability has been proposed as a novel concept and method that allows the study of outcomes from multiple systems with diverse dynamics and time frames by measuring the stability of their interactions in terms of coordinated bursting activities in output signals (long periods of constant lag between output signals indicate strong physiological coupling) (see Bartsch et al., 2015; Bashan et al., 2012).
An example of a dynamic network reorganization using the time delay stability approach is provided by Bashan et al. (2012). The authors analyzed the interactions among different systems (brain cortical, and peripheral cardiac, respiratory, ocular, and muscle activity), which are considered nodes within a network, across stages of sleep in 36 healthy young participants. The results indicated that across stages of sleep, the network undergoes profound changes (reorganization in connectivity and topology): the strength of the connections between nodes was higher in wake and “light” NREM sleep (i.e., N1–2: high network connectivity), lower in REM and substantially reduced in “deep” NREM sleep (i.e., N3). Different sub-networks (brain-brain, brain-periphery and periphery-periphery) behave differently across different stages of sleep. Specifically, there was a greater sleep stage modulation of brain-periphery and periphery-periphery links compared to the brain-brain network, which showed a stable topology across sleep stages. On a local network level, the cardiac system, as assessed by heart rate, was highly connected with the other systems during wakefulness and “light” NREM sleep, to a lesser during REM sleep, and to no significant extent in “deep” NREM sleep. However, surprisingly, no connection was reported for cardiac-respiratory systems in any of the sleep stages. Overall, it is possible that these results may simply reflect a greater presence of isolated perturbations in “light” NREM sleep and wakefulness (e.g., body movements, arousals, K-complexes) rather than specific stage-dependent shifting in the functional organization of the network.
Using the same dataset, Bartsch et al., (2015) further explored the dynamics of system interactions across stages of sleep. The authors further increased the complexity of the network by exploring different EEG leads (Fp1, Fp2, C3, C4, O1, O2) which allowed exploration of inter- and intra-channel network characteristics. To emphasize the complexity, we should consider that just within the brain-brain sub-network, the authors explored 861 possible links. Then, they explored the interaction between this brain sub-network and each of the other measured outputs (eye movements, chin and leg muscle activity, cardiac and respiratory activity), and finally integrated all data within a single network, making interpretation of the results challenging. The authors reported a strong spatial asymmetry in the network of brain-eye interactions, stronger in Fp1 and Fp2 than in central and occipital EEG derivations, particularly in the delta frequencies. However, these results might mirror the dynamics of the frequency and pattern of eye movement artifacts within different EEG derivations rather than brain-eye regulatory mechanisms.
Recent work specifically focused on brain-heart interactions has extended the time delay stability method and proposed a new approach to identify and quantify the evolution of the dynamical interactions between EEG and ECG recordings during sleep (Lin et al., 2016). A delay correlation landscape was used to characterize how individual brain rhythms are coupled to heart rate, and how modulations in brain and cardiac dynamics are coordinated in time. The approach takes into account information on the type of correlation (positive or negative) and directionality of interactions. The results indicated a high level of complexity in brain-heart communication. For example, the probability distribution pattern showed a synchronous activity peak (no time delay) when EEG delta power or EEG total power and heart rate were modulated in the same direction (positive correlation: increase-increase or decrease-decrease of EEG power and heart rate). In contrast, a positive delay of about 6 s (suggesting a directional interaction from brain to heart) characterized the coupling between EEG delta power or EEG total power and heart rate when brain-heart communications showed a negative correlation (i.e., the modulation of the two signals occurred in the opposite direction. The opposite occurred for the coupling between EEG theta power and heart rate. In addition, double peaks (reflecting the highest correlation at time delay of 0 or > 0) were also manifest in brain-heart interactions with positive correlation involving EEG power in specific frequency bands. Overall, none of the interactions suggested that heart dynamics preceded brain dynamics. Finally, the time-delay profiles showed minimal variation across participants, indicating a universal pattern. However, the pattern of negative correlations with brain changes preceding heart changes by ~ 6 s progressively disappeared from “deep” NREM sleep to “light” NREM sleep, REM SLEEP, and wakefulness.
While the “network physiology” approach may offer an attractive and comprehensive picture of the complex functional dynamics of CNS-ANS coupling during sleep, it is unclear whether it can ultimately inform on the physiological network organization of the coupling. The field of network physiology is still in its infancy, and further work is needed to refine the interpretation of the results obtained by these tools when applied to physiological and pathological sleep data.
Summary of analytics of continuous CNS-ANS dynamics.
Analyses of continuous CNS-ANS dynamics clearly support the interdependency between cortical and cardiac function during sleep, although directionality in the brain-heart communication (brain-to-heart or heart-to-brain) remains unclear. Overall, HRV measures predominantly reflecting vagal modulation fluctuate together with measures of EEG delta power, with current evidence suggesting that cardiac changes temporally precede cortical changes. Results of cortical-cardiac dynamics outside the EEG delta frequency band remain unclear. Demographic factors such as age and sex, known to impact both sleep EEG and ANS measures, do not seem to alter the CNS-ANS interplay, although specific transitional periods for CNS and ANS development (e.g., adolescence) still need to be investigated. Current data suggests that the presence of sleep disorders, particularly sleep-disordered breathing, seems to alter (decrease) CNS-ANS coupling. However, all studies are observational and most of the studies involved small samples of young, healthy, male participants studied on a single night. Interpretation of these data is therefore still problematic.
Interpretation of data derived from methods used to assess CNS-ANS connectivity (e.g. cross-correlation) is limited by index complexity, debates over the physiological meaning of indices used (e.g., LF/HF ratio), and insufficient scope (e.g., exclusive focus on EEG power in a specific frequency band without considering the potential information contained outside the selected frequency). Most of these methods cannot be used to infer causality. The emerging interdisciplinary field of “Network physiology” views changes in global behaviors such as wakefulness and sleep from the perspective of a functional reorganization of multiple networks. In these networks, the links (presence, amount and direction of interactions) between virtually infinite nodes representing different systems and sub-systems, evolve over time. One of the advantages of this approach is to provide a graphic representation of the complexity of the interactions among systems (see the radar-charts in Bartsch et al., 2015). However, more work is needed in the field of network physiology to better understand the implications of the complex readouts of this approach.
5. Conclusion and future directions
A growing body of evidence at anatomical, physiological, and behavioral levels is converging in support of a tight coupling between CNS and ANS measures during sleep, showing that a dynamic interplay across multiple bio-systems occurs. Thus, (1) cyclic oscillations in CNS (cortical synchronizations and desynchronizations) and co-occurring changes in peripheral ANS control characterize the “sleep cycles”; (2) on a shorter time scale, phasic cortical synchronizations and desynchronizations are strongly temporally associated with phasic ANS perturbations; (3) different analytical models used to analyze EEG and ECG time series reveal complex temporal dynamics of the EEG-HRV relationship across the sleep period. These models provide evidence of strong cortico-cardiac dependencies at different levels of analysis, timing and network complexity. While there is some evidence that demographic factors and sleep disorders may modulate this cortico-cardiac dependency during sleep, findings are still sparse and further work is needed to determine the clinical applications of EEG-HRV coupling. Finally, basic research is making advancements towards understanding the neural pathways that couple the CNS and ANS during different stages of sleep.
Most of the literature has either explicitly, or implicitly, taken the view that CNS-defined sleep imposes regulatory control on the ANS system, resulting in measurable changes in cardiovascular function. However, it has also been suggested that ANS modulation may influence particular features of sleep, based primarily on evidence that vagal modulation (as indexed by HRV HF power) precedes cortical synchronization (as indexed by EEG delta power) during sleep. However, while this evidence clearly indicates a relationship between cardiac vagal modulation and cortical synchronization, it is correlational and does not give a clear indication of causality.
Several potential applications are directly and/or indirectly based on CNS-ANS coupling. Particularly promising is the attempt to use information about ANS function as a surrogate of CNS state/events. ANS-derived signals such as the ECG are easier to measure with relatively inexpensive sensors in real-life contexts than CNS-derived signals such as the EEG, and could be useful to predict CNS tonic state or phasic events. For example, sleep scoring could be enhanced by using ECG-derived ANS features in addition to (or even instead of) EEG and motion. The consumer market in the wearable tech space is already exploring this possibility, with consumer-based sleep-trackers moving away from the simple measurement of motion to determine sleep/wake states, and now using multiple bio-signals (mainly the extraction of ANS features from HRV data obtained by plethysmographic-type sensors) that in conjunction with motion are used to assess sleep stages (de Zambotti et al., 2016a; de Zambotti et al., 2017). While still limited in accuracy, using HRV measures as well as other ANS information to aid in the detection of different sleep stages holds promise (de Zambotti et al., IN PRESS; de Zambotti et al., 2017). The use of EEG-HRV information or even the use of HRV information alone seems to also be a promising direction in epileptic seizure detection and prediction (Greene et al., 2007; Ramgopal et al., 2014; Van de Vel et al., 2013). Overall, a thorough understanding of the dynamics of the mathematical relations between EEG and HRV signals during sleep may reveal new diagnostic/prognostic biomarkers of disease by capturing subtle changes in systems interdependency during sleep. On the other hand, despite their appeal and promise, the computation of sophisticated mathematical relationships between metrics of uncertain or complex origin (e.g., HRV LF power and LF-HF ratio) does not necessarily advance the understanding of the physiological mechanisms behind the CNS-ANS link. Thus, the extent to which the growing popularity of these mathematical approaches will provide new insight into the physiology of the communication between brain and heart remains unclear.
System perturbation (experimental manipulation) and beat-to-beat (or sec-to-sec) co-registration of multiple source of ANS information (e.g., ECG, impedance cardiography, blood pressure) capturing the complexity of ANS function is needed to further provide insight on the link between CNS and ANS. Future studies also need to investigate further the reciprocity of CNS-ANS coupling across the main ANS oscillatory rhythms during sleep (e.g., EEG dynamics across slow oscillations of blood pressure [so-called “Mayer waves”], breathing, HRV slow oscillations). For example, the analysis of the timing and distribution of synchronized and desynchronized phasic EEG events (e.g., distribution of K-complexes and EEG arousals) as a function of the phase of ANS oscillations may further advance the understanding of the involvement of baroreflex in CNS-ANS coupling (see Silvani et al., 2015).
In conclusion, CNS-ANS coupling is evident during sleep based on multiple levels of investigation and supports a vision of sleep as a dynamic complex interaction between multiple systems and subsystems. Further exploration of CNS-ANS interactions will lead to new opportunities to understand the fascinating reciprocal influences between brain and body during sleep.
Highlights.
-
▪
Central (CNS) and autonomic (ANS) nervous systems are tightly coupled during sleep
-
▪
Complex regulatory mechanisms (CNS commands and ANS reflexes) drive the coupling
-
▪
Analytic methods reveal a complex interplay between cortico-cardiac dynamics
-
▪
Analysis of coupling between CNS events and ANS changes gives physiological insight
-
▪
Changes in ANS-CNS coupling might be useful as a biomarker of disease
Practical points and research agenda.
Practical points
-
▪
CNS and ANS are tightly coupled during sleep, as evident from different levels of analysis and different time-scales
-
▪
The complexity of the indices used in analyzing CNS-ANS coupling (mainly spectral EEG and HRV indices) makes the physiological interpretation of cortico-cardiac dynamics during sleep challenging. For example, in the evaluation of the cortico-cardiac relationship, the physiology underlying the oscillatory rhythms responsible for the HRV phenomenon is frequently ignored. HRV metrics of uncertain physiological meaning (e.g., LF/HF ratio) are frequently used, further confounding the interpretation of the complex relationships between CNS and ANS
-
▪
The dynamics of EEG-HRV coupling may be useful to improve screening, severity assessment, and treatment outcomes for sleep disorders, but data need to be interpreted cautiously given different results based on linear and non-linear analytical approaches.
-
▪
The analysis of the bidirectional coupling between transient ANS changes and transient CNS events (e.g. arousals from sleep) is a useful approach to further investigate the physiology underlying CNS-ANS coupling
Research agenda
-
▪
Direct and selective manipulations (perturbations) of CNS- and/or ANS-dependent function are needed to further understand the underlying physiology and the directionality of CNS-ANS coupling
-
▪
Experimental protocols such as sleep deprivation and constant routine protocols are needed to advance understanding of homeostatic and circadian regulation of CNS-ANS coupling
-
▪
Recording of multiple sources of information reflecting ANS function (e.g., beat-to-beat blood pressure, ECG, impedance cardiography) and CNS function (EEG) during sleep is needed to better characterize and understand the physiology of the complex hemodynamic changes occurring in synchrony with cortical events
-
▪
Future research should test the potential predictive role of indices reflecting CNS-ANS coupling during sleep as diagnostic/prognostic biomarkers of disease. Also, more work is needed to determine whether it is practical and valid to predict CNS states based on ANS measures obtained with wearable technology
Acknowledgments
Funding sources: This study was supported by National Institutes of Health (NIH) grants, AA021696 (to IMC+FCB), HL103688 (to FCB), AA020565 (to IMC), AA024841 (to IMC + MdZ), and National Health and Medical Research Council (NHMRC) of Australia (grant ID: 1027076, to JT). The content is solely the responsibility of the authors and does not necessarily represent the official views of the funding agencies.
Main acronyms
- ANS
Autonomic nervous system
- CNS
Central nervous system
- ECG
Electrocardiography
- EEG
Electroencephalography
- HF
High frequency
- HRV
Heart rate variability
- LF
Low frequency
- NREM
non-REM
- PSG
polysomnography
- REM
Rapid-eye-movement
- SNA
Sympathetic nerve activity
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Disclosure Statement: MdZ, FB, and IC have received research funding unrelated to this work from Fitbit Inc., Ebb Therapeutics Inc., and International Flavors & Fragrances Inc. JT and AS have nothing to disclose.
References
- Abdullah H, Maddage N, Cosic I, Cvetkovic D. Biomedical Engineering and Sciences (IECBES), 2010 IEEE EMBS Conference on. IEEE; 2010a. Brain and heart interaction during sleep in the healthy and sleep apnoea; pp. 276–280. [Google Scholar]
- Abdullah H, Maddage N, Cosic I, Cvetkovic D. Cross-correlation of EEG frequency bands and heart rate variability for sleep apnoea classification. Med Biol Eng Comput. 2010b;48:1261–1269. doi: 10.1007/s11517-010-0696-9. [DOI] [PubMed] [Google Scholar]
- Abdullah H, Maddage N, Cvetkovic D. Biomedical Engineering and Sciences (IECBES), 2012 IEEE EMBS Conference on. IEEE; 2012. Phase synchronization and directional coupling between brain and heart during sleep; pp. 659–663. [Google Scholar]
- Ako M, Kawara T, Uchida S, Miyazaki S, Nishihara K, Mukai J, Hirao K, Ako J, Okubo Y. Correlation between electroencephalography and heart rate variability during sleep. Psychiatry Clin Neurosci. 2003;57:59–65. doi: 10.1046/j.1440-1819.2003.01080.x. [DOI] [PubMed] [Google Scholar]
- Bartsch RP, Liu KK, Bashan A, Ivanov PC. Network Physiology: How Organ Systems Dynamically Interact. PLoS ONE. 2015;10:e0142143. doi: 10.1371/journal.pone.0142143. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bashan A, Bartsch RP, Kantelhardt JW, Havlin S, Ivanov PC. Network physiology reveals relations between network topology and physiological function. Nat Commun. 2012;3:702. doi: 10.1038/ncomms1705. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Berger RD, Saul JP, Cohen RJ. Transfer function analysis of autonomic regulation. I. Canine atrial rate response. Am. J. Physiol. 1989;256:H142–H152. doi: 10.1152/ajpheart.1989.256.1.H142. [DOI] [PubMed] [Google Scholar]
- Berntson G, Cacioppo J, Quigley K. The metrics of cardiac chronotropism: biometric perspectives. Psychophysiology. 1995;32:162–171. doi: 10.1111/j.1469-8986.1995.tb03308.x. [DOI] [PubMed] [Google Scholar]
- Berry R, Brooks R, Gamaldo C, Harding S, Lloyd R, Quan S, Troester M, Vaughn B. AASM Scoring Manual Updates for 2017 (Version 2.4) J Clin Sleep Med. 2017;13:665–666. doi: 10.5664/jcsm.6576. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Billman GE. The LF/HF ratio does not accurately measure cardiac sympatho-vagal balance. Front Physiol. 2013;4:26. doi: 10.3389/fphys.2013.00026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bonnemeier H, Richardt G, Potratz J, Wiegand U, Brandes A, Kluge N, Katus H. Circadian profile of cardiac autonomic nervous modulation in healthy subjects: differing effects of aging and gender on heart rate variability. J Cardiovasc Electrophysiol. 2003;14:791–799. doi: 10.1046/j.1540-8167.2003.03078.x. [DOI] [PubMed] [Google Scholar]
- Bonnet M, Arand D. Hyperarousal and insomnia: state of the science. Sleep Med Rev. 2010;14:9–15. doi: 10.1016/j.smrv.2009.05.002. [DOI] [PubMed] [Google Scholar]
- Brandenberger G, Ehrhart J, Buchheit M. Sleep stage 2: an electroencephalographic, autonomic, and hormonal duality. Sleep. 2005;28:1535–1540. doi: 10.1093/sleep/28.12.1535. [DOI] [PubMed] [Google Scholar]
- Brandenberger G, Ehrhart J, Piquard F, Simon C. Inverse coupling between ultradian oscillations in delta wave activity and heart rate variability during sleep. Clin Neurophysiol. 2001;112:992–996. doi: 10.1016/s1388-2457(01)00507-7. [DOI] [PubMed] [Google Scholar]
- Brandenberger G, Follenius M, Muzet A, Ehrhart J, Schieber J. Ultradian oscillations in plasma renin activity: their relationships to meals and sleep stages. J Clin Endocrinol Metab. 1985;61:280–284. doi: 10.1210/jcem-61-2-280. [DOI] [PubMed] [Google Scholar]
- Brandenberger G, Viola A, Ehrhart J, Charloux A, Geny B, Piquard F, Simon C. Age-related changes in cardiac autonomic control during sleep. J Sleep Res. 2003;12:173–180. doi: 10.1046/j.1365-2869.2003.00353.x. [DOI] [PubMed] [Google Scholar]
- Brennan M, Palaniswami M, Kamen P. Do existing measures of Poincare plot geometry reflect nonlinear features of heart rate variability? IEEE Trans Biomed Eng. 2001;48:1342–1347. doi: 10.1109/10.959330. [DOI] [PubMed] [Google Scholar]
- Buijs R, la Fleur S, Wortel J, Van Heyningen C, Zuiddam L, Mettenleiter T, Kalsbeek A, Nagai K, Niijima A. The suprachiasmatic nucleus balances sympathetic and parasympathetic output to peripheral organs through separate preautonomic neurons. J Comp Neurol. 2003;464:36–48. doi: 10.1002/cne.10765. [DOI] [PubMed] [Google Scholar]
- Burgess H, Holmes A, Dawson D. The relationship between slow-wave activity, body temperature, and cardiac activity during nighttime sleep. Sleep. 2001;24:343–349. doi: 10.1093/sleep/24.3.343. [DOI] [PubMed] [Google Scholar]
- Burgess H, Kleiman J, Trinder J. Cardiac activity during sleep onset. Psychophysiology. 1999;36:298– 306. doi: 10.1017/s0048577299980198. [DOI] [PubMed] [Google Scholar]
- Burgess H, Trinder J, Kim Y, Luke D. Sleep and circadian influences on cardiac autonomic nervous system activity. Am J Physiol. 1997;273:H1761–H1768. doi: 10.1152/ajpheart.1997.273.4.H1761. [DOI] [PubMed] [Google Scholar]
- Burr RL. Interpretation of Normalized Spectral Heart Rate Variability Indices In Sleep Research: A Critical Review. Sleep. 2007;30:913–919. doi: 10.1093/sleep/30.7.913. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cacioppo J, Berntson G, Binkley P, Quigley K, Uchino B, Fieldstone A. Autonomic cardiac control. II. Noninvasive indices and basal response as revealed by autonomic blockades. Psychophysiology. 1994;31:586–598. doi: 10.1111/j.1469-8986.1994.tb02351.x. [DOI] [PubMed] [Google Scholar]
- Cacioppo J, Tassinary L, Berntson G. Handbook of psychophysiology. 3. Cambridge University Press; New York, NY: 2007. [Google Scholar]
- Cajochen C, Pischke J, Aeschbach D, Borbély AA. Heart rate dynamics during human sleep. Physiol Behav. 1994;55:769–774. doi: 10.1016/0031-9384(94)90058-2. [DOI] [PubMed] [Google Scholar]
- Calandra-Buonaura G, Provini F, Guaraldi P, Plazzi G, Cortelli P. Cardiovascular autonomic dysfunctions and sleep disorders. Sleep Med Rev. 2015;26:43–56. doi: 10.1016/j.smrv.2015.05.005. [DOI] [PubMed] [Google Scholar]
- Camm AJ, Malik M, Bigger J, Breithardt G, Cerutti S, Cohen R, Coumel P, Fallen E, Kennedy H, Kleiger R. Heart rate variability: standards of measurement, physiological interpretation and clinical use. Task Force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Circulation. 1996;93:1043–1065. [PubMed] [Google Scholar]
- Carney R, Saunders R, Freedland K, Stein P, Rich M, Jaffe A. Association of depression with reduced heart rate variability in coronary artery disease. Am J Cardiol. 1995;76:562–564. doi: 10.1016/s0002-9149(99)80155-6. [DOI] [PubMed] [Google Scholar]
- Carrier J, Land S, Buysse D, Kupfer D, Monk T. The effects of age and gender on sleep EEG power spectral density in the middle years of life (ages 20–60 years old) Psychophysiology. 2001;38:232–242. [PubMed] [Google Scholar]
- Carrington M, Barbieri R, Colrain I, Crowley K, Kim Y, Trinder J. Changes in cardiovascular function during the sleep onset period in young adults. J Appl Physiol (1985) 2005;98:468–476. doi: 10.1152/japplphysiol.00702.2004. [DOI] [PubMed] [Google Scholar]
- Carrington M, Trinder J. Blood pressure and heart rate during continuous experimental sleep fragmentation in healthy adults. Sleep. 2008;31:1701–1712. doi: 10.1093/sleep/31.12.1701. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Carrington M, Walsh M, Stambas T, Kleiman J, Trinder J. The influence of sleep onset on the diurnal variation in cardiac activity and cardiac control. J Sleep Res. 2003;12:213–221. doi: 10.1046/j.1365-2869.2003.00364.x. [DOI] [PubMed] [Google Scholar]
- Chaparro-Vargas R, Schilling C, Schredl M, Cvetkovic D. Sleep electroencephalography and heart rate variability interdependence amongst healthy subjects and insomnia/schizophrenia patients. Med Biol Eng Comput. 2016;54:77–91. doi: 10.1007/s11517-015-1297-4. [DOI] [PubMed] [Google Scholar]
- Charloux A, Otzenberger H, Gronfier C, Lonsdorfer-Wolf E, Piquard F, Brandenberger G. Oscillations in sympatho-vagal balance oppose variations in delta-wave activity and the associated renin release. J Clin Endocrinol Metab. 1998;83:1523–1528. doi: 10.1210/jcem.83.5.4762. [DOI] [PubMed] [Google Scholar]
- Charloux A, Piquard F, Ehrhart J, Mettauer B, Geny B, Simon C, Brandenberger G. Time-courses in renin and blood pressure during sleep in humans. J Sleep Res. 2002;11:73–79. doi: 10.1046/j.1365-2869.2002.00277.x. [DOI] [PubMed] [Google Scholar]
- Colrain I, Trinder J, Fraser G, Wilson G. Ventilation during sleep onset. J Appl Physiol. 1987;63:2067–2074. doi: 10.1152/jappl.1987.63.5.2067. [DOI] [PubMed] [Google Scholar]
- Colrain IM. The K-complex: a 7-decade history. Sleep. 2005;28:255–273. doi: 10.1093/sleep/28.2.255. [DOI] [PubMed] [Google Scholar]
- Conway J, Boon N, Jones J, Sleight P. Involvement of the baroreceptor reflexes in the changes in blood pressure with sleep and mental arousal. Hypertension. 1983;5:746–748. doi: 10.1161/01.hyp.5.5.746. [DOI] [PubMed] [Google Scholar]
- Cote K, de Lugt D, Langley S, Campbell K. Scalp topography of the auditory evoked K-complex in stage 2 and slow wave sleep. J Sleep Res. 1999;8:263–272. doi: 10.1046/j.1365-2869.1999.00164.x. [DOI] [PubMed] [Google Scholar]
- De Gennaro L, Ferrara M, Bertini M. The spontaneous K-complex during stage 2 sleep: is it the 'forerunner' of delta waves? Neurosci Lett. 2000;291:41–43. doi: 10.1016/s0304-3940(00)01366-5. [DOI] [PubMed] [Google Scholar]
- de la Torre-Luque A, Bornas X, Balle M, Fiol-Veny A. Complexity and nonlinear biomarkers in emotional disorders: A meta-analytic study. Neurosci Biobehav Rev. 2016;68:410. doi: 10.1016/j.neubiorev.2016.05.023. [DOI] [PubMed] [Google Scholar]
- de Zambotti M, Cellini N, Baker F, Colrain I, Sarlo M, Stegagno L. Nocturnal cardiac autonomic profile in young primary insomniacs and good sleepers. Int J Psychophysiol. 2014;93:332–339. doi: 10.1016/j.ijpsycho.2014.06.014. [DOI] [PubMed] [Google Scholar]
- de Zambotti M, Covassin N, De Min Tona G, Sarlo M, Stegagno L. Sleep onset and cardiovascular activity in primary insomnia. J Sleep Res. 2011;20:318–325. doi: 10.1111/j.1365-2869.2010.00871.x. [DOI] [PubMed] [Google Scholar]
- de Zambotti M, Godino JG, Baker FC, Cheung J, Patrick K, Colrain IM. The Boom in Wearable Technology: Cause for Alarm or Just What is Needed to Better Understand Sleep? Sleep. 2016a;39:1761–1762. doi: 10.5665/sleep.6108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- de Zambotti M, Goldstone A, Claudatos S, Colrain I, Baker F. A validation study of Fitbit Charge 2™ compared with polysomnography in adults. Chronobiol Int. doi: 10.1080/07420528.2017.1413578. IN PRESS. [DOI] [PubMed] [Google Scholar]
- de Zambotti M, Rosas L, Colrain IM, Baker FC. The Sleep of the Ring: Comparison of the ŌURA Sleep Tracker Against Polysomnography. Behav Sleep Med. 2017;21:1–15. doi: 10.1080/15402002.2017.1300587. [DOI] [PMC free article] [PubMed] [Google Scholar]
- de Zambotti M, Willoughby A, Franzen P, Clark D, Baker F, Colrain I. K-Complexes: Interaction between the Central and Autonomic Nervous Systems during Sleep. Sleep. 2016b;39:1129–1137. doi: 10.5665/sleep.5770. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Deboer T, Vansteensel M, Détári L, Meijer J. Sleep states alter activity of suprachiasmatic nucleus neurons. Nat Neurosci. 2003;6:1086–1890. doi: 10.1038/nn1122. [DOI] [PubMed] [Google Scholar]
- Deco G, Jirsa V, McIntosh A, Sporns O, Kötter R. Key role of coupling, delay, and noise in resting brain fluctuations. Proc Natl Acad Sci U S A. 2009;106:10302–10307. doi: 10.1073/pnas.0901831106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dijk D-J. Regulation and functional correlates of slow wave sleep. J Clin Sleep Med. 2009;5:S6–S15. [PMC free article] [PubMed] [Google Scholar]
- Dumont M, Jurysta F, Lanquart J, Migeotte P, van de Borne P, Linkowski P. Interdependency between heart rate variability and sleep EEG: linear/non-linear? Clin Neurophysiol. 2004;115:2031–2040. doi: 10.1016/j.clinph.2004.04.007. [DOI] [PubMed] [Google Scholar]
- Dumont M, Jurysta F, Lanquart J, Noseda A, van de Borne P, Linkowski P. Scale-free dynamics of the synchronization between sleep EEG power bands and the high frequency component of heart rate variability in normal men and patients with sleep apnea-hypopnea syndrome. Clin Neurophysiol. 2007;118:2752–2764. doi: 10.1016/j.clinph.2007.08.018. [DOI] [PubMed] [Google Scholar]
- Easton A, Meerlo P, Bergmann B, Turek F. The suprachiasmatic nucleus regulates sleep timing and amount in mice. Sleep. 2004;27:1307–1318. doi: 10.1093/sleep/27.7.1307. [DOI] [PubMed] [Google Scholar]
- Eckberg D. Temporal response patterns of the human sinus node to brief carotid baroreceptor stimuli. J Physiol. 1976;258:769–782. doi: 10.1113/jphysiol.1976.sp011445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eckberg D. Sympathovagal balance: a critical appraisal. Circulation. 1997;96:3224–3232. doi: 10.1161/01.cir.96.9.3224. [DOI] [PubMed] [Google Scholar]
- Eckberg DL. The human respiratory gate. J Physiol. 2003;548:339–352. doi: 10.1113/jphysiol.2003.037192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Eguchi K, Satoh T. Convergence of sleep-wakefulness subsystems onto single neurons in the region of cat's solitary tract nucleus. Arch. Ital. Biol. 1980;118:331–345. [PubMed] [Google Scholar]
- Ehrhart J, Toussaint M, Simon C, Gronfier C, Luthringer R, Brandenberger G. Alpha activity and cardiac correlates: three types of relationships during nocturnal sleep. Clin Neurophysiol. 2000;111:940–946. doi: 10.1016/s1388-2457(00)00247-9. [DOI] [PubMed] [Google Scholar]
- el Mansari M, Sakai K, Jouvet M. Unitary characteristics of presumptive cholinergic tegmental neurons during the sleep-waking cycle in freely moving cats. Exp. Brain Res. 1989;76:519–529. doi: 10.1007/BF00248908. [DOI] [PubMed] [Google Scholar]
- Faes L, Marinazzo D, Jurysta F, Nollo G. Linear and non-linear brain-heart and brain-brain interactions during sleep. Physiol Meas. 2015;36:683–698. doi: 10.1088/0967-3334/36/4/683. [DOI] [PubMed] [Google Scholar]
- Faes L, Marinazzo D, Stramaglia S, Jurysta F, Porta A, Giandomenico N. Predictability decomposition detects the impairment of brain-heart dynamical networks during sleep disorders and their recovery with treatment. Philos Trans A Math Phys Eng Sci. 2016;374 doi: 10.1098/rsta.2015.0177. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Felder RB, Mifflin SW. Modulation of carotid sinus afferent input to nucleus tractus solitarius by parabrachial nucleus stimulation. Circ. Res. 1988;63:35–49. doi: 10.1161/01.res.63.1.35. [DOI] [PubMed] [Google Scholar]
- Ferini-Strambi L, Bianchi A, Zucconi M, Oldani A, Castronovo V, Smirne S. The impact of cyclic alternating pattern on heart rate variability during sleep in healthy young adults. Clin Neurophysiol. 2000;111:99–101. doi: 10.1016/s1388-2457(99)00212-6. [DOI] [PubMed] [Google Scholar]
- Ferri R, Parrino L, Smerieri A, Terzano M, Elia M, Musumeci S, Pettinato S. Cyclic alternating pattern and spectral analysis of heart rate variability during normal sleep. J Sleep Res. 2000;9:13. doi: 10.1046/j.1365-2869.2000.00190.x. [DOI] [PubMed] [Google Scholar]
- Forouzanfar M, Baker F, de Zambotti M, McCall McCall C, Giovangrandi L, Kovacs G. Toward a better noninvasive assessment of pre-ejection period: a novel automatic algorithm for B-point detection and correction on thoracic impedance cardiogram. Psychophysiology. doi: 10.1111/psyp.13072. in press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Futuro-Neto HA, Coote JH. Desynchronized sleep-like pattern of sympathetic activity elicited by electrical stimulation of sites in the brainstem. Brain Res. 1982;252:269–276. doi: 10.1016/0006-8993(82)90394-8. [DOI] [PubMed] [Google Scholar]
- Garcia-Rill E, Houser CR, Skinner RD, Smith W, Woodward DJ. Locomotion-inducing sites in the vicinity of the pedunculopontine nucleus. Brain Res. Bull. 1987;18:731–738. doi: 10.1016/0361-9230(87)90208-5. [DOI] [PubMed] [Google Scholar]
- Gilbey MP, Jordan D, Richter DW, Spyer KM. Synaptic mechanisms involved in the inspiratory modulation of vagal cardio-inhibitory neurones in the cat. J. Physiol. 1984;356:65–78. doi: 10.1113/jphysiol.1984.sp015453. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Goodwin GM, McCloskey DI, Mitchell JH. Cardiovascular and respiratory responses to changes in central command during isometric exercise at constant muscle tension. J. Physiol. 1972;226:173–190. doi: 10.1113/jphysiol.1972.sp009979. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Greene B, Boylan G, Reilly R, de Chazal P, Connolly S. Combination of EEG and ECG for improved automatic neonatal seizure detection. Clin Neurophysiol. 2007;118:1348–1359. doi: 10.1016/j.clinph.2007.02.015. [DOI] [PubMed] [Google Scholar]
- Halász P, Pál I, Rajna P. K-complex formation of the EEG in sleep. A survey and new examinations. Acta Physiol Hung. 1985;65:3–35. [PubMed] [Google Scholar]
- Harvey A. Pre-sleep cognitive activity: a comparison of sleep-onset insomniacs and good sleepers. Br J Clin Psychol. 2000;39:275–286. doi: 10.1348/014466500163284. [DOI] [PubMed] [Google Scholar]
- Heathers J. Sympathovagal balance from heart rate variability: an obituary. Exp Physiol. 2012;97:556. doi: 10.1113/expphysiol.2011.063867. [DOI] [PubMed] [Google Scholar]
- Horner R, Sanford L, Pack A, Morrison A. Activation of a distinct arousal state immediately after spontaneous awakening from sleep. Brain Res Rev. 1997;778:127–134. doi: 10.1016/s0006-8993(97)01045-7. [DOI] [PubMed] [Google Scholar]
- Hornyak M, Cejnar M, Elam M, Matousek M, Wallin B. Sympathetic muscle nerve activity during sleep in man. Brain: a journal of neurology. 1991a;114:1281–1295. doi: 10.1093/brain/114.3.1281. [DOI] [PubMed] [Google Scholar]
- Hornyak M, Cejnar M, Elam M, Matousek M, Wallin B. Sympathetic muscle nerve activity during sleep in man. Brain. 1991b;114:1281–1295. doi: 10.1093/brain/114.3.1281. [DOI] [PubMed] [Google Scholar]
- Imholz B, Wieling W, van Montfrans G, Wesseling K. Fifteen years experience with finger arterial pressure monitoring: assessment of the technology. Cardiovasc Res. 1998;38:605–616. doi: 10.1016/s0008-6363(98)00067-4. [DOI] [PubMed] [Google Scholar]
- Ivanov PC, Liu KK, Bartsch RP. Focus on the emerging new fields of network physiology and network medicine. New Journal of Physics. 2016;18:100201. doi: 10.1088/1367-2630/18/10/100201. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Janssen B, Tyssen C, Duindam H, Rietveld W. Suprachiasmatic lesions eliminate 24-h blood pressure variability in rats. Physiol Behav. 1994;55:307–311. doi: 10.1016/0031-9384(94)90138-4. [DOI] [PubMed] [Google Scholar]
- Johnson L, Karpan W. Autonomic correlates of the spontaneous K-complex. Psychophysiology. 1968;4:444–452. doi: 10.1111/j.1469-8986.1968.tb02785.x. [DOI] [PubMed] [Google Scholar]
- Julien C. The enigma of Mayer waves: Facts and models. Cardiovasc Res. 2006;70:12–21. doi: 10.1016/j.cardiores.2005.11.008. [DOI] [PubMed] [Google Scholar]
- Jurysta F, Kempenaers C, Lancini J, Lanquart J, van de Borne P, Linkowski P. Altered interaction between cardiac vagal influence and delta sleep EEG suggests an altered neuroplasticity in patients suffering from major depressive disorder. Acta Psychiatr Scand. 2010;121:236–239. doi: 10.1111/j.1600-0447.2009.01475.x. [DOI] [PubMed] [Google Scholar]
- Jurysta F, Kempenaers C, Lanquart J-P, Noseda A, van de Borne P, Linkowski P. Long-term CPAP treatment partially improves the link between cardiac vagal influence and delta sleep. BMC Pulm Med. 2013;13:29. doi: 10.1186/1471-2466-13-29. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jurysta F, Lanquart J, Sputaels V, Dumont M, Migeotte P, Leistedt S, Linkowski P, van de Borne P. The impact of chronic primary insomnia on the heart rate--EEG variability link. Clin Neurophysiol. 2009;120:1054–1060. doi: 10.1016/j.clinph.2009.03.019. [DOI] [PubMed] [Google Scholar]
- Jurysta F, Lanquart J, van de Borne P, Migeotte P, Dumont M, Degaute J, Linkowski P. The link between cardiac autonomic activity and sleep delta power is altered in men with sleep apnea-hypopnea syndrome. Am J Physiol Regul Integr Comp Physiol. 2006;291:R1165–R1171. doi: 10.1152/ajpregu.00787.2005. [DOI] [PubMed] [Google Scholar]
- Jurysta F, van de Borne P, Lanquart J, Migeotte P, Degaute J, Dumont M, Linkowski P. Progressive aging does not alter the interaction between autonomic cardiac activity and delta EEG power. Clin Neurophysiol. 2005;116:871–877. doi: 10.1016/j.clinph.2004.10.005. [DOI] [PubMed] [Google Scholar]
- Jurysta F, van de Borne P, Migeotte P, Dumont M, Lanquart J, Degaute J, Linkowski P. A study of the dynamic interactions between sleep EEG and heart rate variability in healthy young men. Clin Neurophysiol. 2003;114:2146–2155. doi: 10.1016/s1388-2457(03)00215-3. [DOI] [PubMed] [Google Scholar]
- Kales A, Rechtschaffen A. A manual of standardized terminology, techniques and scoring system for sleep stages of human subjects. Bethesda, MD: 1968. [DOI] [PubMed] [Google Scholar]
- Kerkhof G, Van Dongen H, Bobbert A. Absence of endogenous circadian rhythmicity in blood pressure? Am J Hypertens. 1998;11:373–377. doi: 10.1016/s0895-7061(97)00461-5. [DOI] [PubMed] [Google Scholar]
- Kern M, Aertsen A, Schulze-Bonhage A, Ball T. Heart cycle-related effects on event-related potentials, spectral power changes, and connectivity patterns in the human ECoG. NeuroImage. 2013;81:178–190. doi: 10.1016/j.neuroimage.2013.05.042. [DOI] [PubMed] [Google Scholar]
- Khoo M, Kim T, Berry R. Spectral indices of cardiac autonomic function in obstructive sleep apnea. Sleep. 1999;22:443–451. doi: 10.1093/sleep/22.4.443. [DOI] [PubMed] [Google Scholar]
- Kim B, Kocsis B, Hwang E, Kim Y, Strecker R, McCarley R, Choi J. Differential modulation of global and local neural oscillations in REM sleep by homeostatic sleep regulation. Proc Natl Acad Sci U S A. 2017;114:E1727–E1736. doi: 10.1073/pnas.1615230114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kräuchi K, Wirz-Justice A. Circadian rhythm of heat production, heart rate, and skin and core temperature under unmasking conditions in men. Am J Physiol. 1994;267:R819–R829. doi: 10.1152/ajpregu.1994.267.3.R819. [DOI] [PubMed] [Google Scholar]
- Kryger MH, Roth T, Dement WC. Principles and Practice of Sleep Medicine. Elsevier Health Sciences 2015 [Google Scholar]
- Kuo T, Chen C, Hsu Y, Yang C. EEG beta power and heart rate variability describe the association between cortical and autonomic arousals across sleep. Auton Neurosci. 2016;194:32–37. doi: 10.1016/j.autneu.2015.12.001. [DOI] [PubMed] [Google Scholar]
- Lamarche C, Ogilvie R. Electrophysiological changes during the sleep onset period of psychophysiological insomniacs, psychiatric insomniacs, and normal sleepers. Sleep. 1997;20:724–733. [PubMed] [Google Scholar]
- Lavie P, Schnall R, Sheffy J, Shlitner A. Peripheral vasoconstriction during REM sleep detected by a new plethysmographic method. Nat Med. 2000;6:606. doi: 10.1038/76135. [DOI] [PubMed] [Google Scholar]
- Lechinger J, Heib D, Gruber W, Schabus M, Klimesch W. Heartbeat-related EEG amplitude and phase modulations from wakefulness to deep sleep: Interactions with sleep spindles and slow oscillations. Psychophysiology. 2015;52:1441–1450. doi: 10.1111/psyp.12508. [DOI] [PubMed] [Google Scholar]
- Lin A, Liu K, Bartsch R, Ivanov P. Delay-correlation landscape reveals characteristic time delays of brain rhythms and heart interactions. Philos Trans A Math Phys Eng Sci. 2016;374 doi: 10.1098/rsta.2015.0182. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lo Martire V, Silvani A, Alvente S, Bastianini S, Berteotti C, Valli A, Zoccoli G. Modulation of sympathetic vasoconstriction is critical for the effects of sleep on arterial pressure in mice. J Physiol. doi: 10.1113/JP275353. IN PRESS. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Long X, Arends JB, Aarts RM, Haakma R, Fonseca P, Rolink J. Time delay between cardiac and brain activity during sleep transitions. Appl Phys Lett. 2015;106:143702. [Google Scholar]
- Loomis AL, Harvey EN, Hobart G. Cerebral states during sleep, as studied by human brain potentials. J Exp Psychol. 1937;21:127–144. [Google Scholar]
- Luppi PH, Peyron C, Fort P. Not a single but multiple populations of GABAergic neurons control sleep. Sleep Med. Rev. 2017;32:85–94. doi: 10.1016/j.smrv.2016.03.002. [DOI] [PubMed] [Google Scholar]
- Mandel DA, Schreihofer AM. Central respiratory modulation of barosensitive neurones in rat caudal ventrolateral medulla. J. Physiol. 2006;572:881–896. doi: 10.1113/jphysiol.2005.103622. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Mano T, Iwase S, Toma S. Microneurography as a tool in clinical neurophysiology to investigate peripheral neural traffic in humans. Clin Neurophysiol. 2006;117:2357–2384. doi: 10.1016/j.clinph.2006.06.002. [DOI] [PubMed] [Google Scholar]
- Martelli D, Silvani A, McAllen R, May C, Ramchandra R. The low frequency power of heart rate variability is neither a measure of cardiac sympathetic tone nor of baroreflex sensitivity. Am J Physiol Heart Circ Physiol. 2014;307:H1005–H1012. doi: 10.1152/ajpheart.00361.2014. [DOI] [PubMed] [Google Scholar]
- McAllen RM, Spyer KM. The baroreceptor input to cardiac vagal motoneurones. J. Physiol. 1978;282:365–374. doi: 10.1113/jphysiol.1978.sp012469. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Miglis M. Autonomic dysfunction in primary sleep disorders. Sleep Med. 2016;19:40–49. doi: 10.1016/j.sleep.2015.10.001. [DOI] [PubMed] [Google Scholar]
- Miki K, Kato M, Kajii S. Relationship between renal sympathetic nerve activity and arterial pressure during REM sleep in rats. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2003;284:R467–R473. doi: 10.1152/ajpregu.00045.2002. [DOI] [PubMed] [Google Scholar]
- Monstad P, Guilleminault C. Cardiovascular changes associated with spontaneous and evoked K-complexes. Neurosci Lett. 1999;263:211–213. doi: 10.1016/s0304-3940(99)00142-1. [DOI] [PubMed] [Google Scholar]
- Morrison AR, Pompeiano O. Vestibular influences during sleep. VI. Vestibular control of autonomic functions during the rapid eye movements of desynchronized sleep. Arch. Ital. Biol. 1970;108:154– 180. [PubMed] [Google Scholar]
- Morrison SF. Central neural control of thermoregulation and brown adipose tissue. Auton. Neurosci. 2016;196:14–24. doi: 10.1016/j.autneu.2016.02.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Newlin D, Levenson R. Pre-ejection period: measuring beta-adrenergic influences upon the heart. Psychophysiology. 1979;16:546–553. doi: 10.1111/j.1469-8986.1979.tb01519.x. [DOI] [PubMed] [Google Scholar]
- Nicholas C, Trinder J, Crowley K, Colrain I. The impact of slow wave sleep proximity on evoked K-complex generation. Neurosci Lett. 2006;404:127–131. doi: 10.1016/j.neulet.2006.05.022. [DOI] [PubMed] [Google Scholar]
- Nisbet LC, Yiallourou SR, Biggs SN, Nixon GM, Davey MJ, Trinder JA, Walter LM, Horne RS. Preschool Children with Obstructive Sleep Apnea: The Beginnings of Elevated Blood Pressure? Sleep. 2013;36:1219–1226. doi: 10.5665/sleep.2890. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Okada H, Iwase S, Mano T, Sugiyama Y, Watanabe T. Changes in muscle sympathetic nerve activity during sleep in humans. Neurology. 1991;41:1961–1966. doi: 10.1212/wnl.41.12.1961. [DOI] [PubMed] [Google Scholar]
- Otzenberger H, Gronfier C, Simon C, Charloux A, Ehrhart J, Piquard F, Brandenberger G. Dynamic heart rate variability: a tool for exploring sympathovagal balance continuously during sleep in men. Am J Physiol. 1998;275:H946–H950. doi: 10.1152/ajpheart.1998.275.3.H946. [DOI] [PubMed] [Google Scholar]
- Otzenberger H, Simon C, Gronfier C, Brandenberger G. Temporal relationship between dynamic heart rate variability and electroencephalographic activity during sleep in man. Neurosci Lett. 1997;229:173–176. doi: 10.1016/s0304-3940(97)00448-5. [DOI] [PubMed] [Google Scholar]
- Padley JR, Kumar NN, Li Q, Nguyen TB, Pilowsky PM, Goodchild AK. Central command regulation of circulatory function mediated by descending pontine cholinergic inputs to sympathoexcitatory rostral ventrolateral medulla neurons. Circ. Res. 2007;100:284–291. doi: 10.1161/01.RES.0000257370.63694.73. [DOI] [PubMed] [Google Scholar]
- Park H, Bernasconi F, Salomon R, Tallon-Baudry C, Spinelli L, Seeck M, Schaller K, Blanke O. Neural Sources and Underlying Mechanisms of Neural Responses to Heartbeats, and their Role in Bodily Self-consciousness: An Intracranial EEG Study. Cereb Cortex. 2017;7:1–14. doi: 10.1093/cercor/bhx136. [DOI] [PubMed] [Google Scholar]
- Pigarev IN, Nothdurft HC, Kastner S. Evidence for asynchronous development of sleep in cortical areas. Neuroreport. 1997;8:2557–2560. doi: 10.1097/00001756-199707280-00027. [DOI] [PubMed] [Google Scholar]
- Ramgopal S, Thome-Souza S, Jackson M, Kadish N, Sánchez FI, Klehm J, Bosl W, Reinsberger C, Schachter S, Loddenkemper T. Seizure detection, seizure prediction, and closed-loop warning systems in epilepsy. Epilepsy Behav. 2014;37:291–307. doi: 10.1016/j.yebeh.2014.06.023. [DOI] [PubMed] [Google Scholar]
- Reyes dPG, Langewitz W, Mulder L, van Roon A, Duschek S. The utility of low frequency heart rate variability as an index of sympathetic cardiac tone: a review with emphasis on a reanalysis of previous studies. Psychophysiology. 2013;50:477–487. doi: 10.1111/psyp.12027. [DOI] [PubMed] [Google Scholar]
- Riemann D, Spiegelhalder K, Feige B, Voderholzer U, Berger M, Perlis M, Nissen C. The hyperarousal model of insomnia: A review of the concept and its evidence. Sleep Med Rev. 2010;14:19–31. doi: 10.1016/j.smrv.2009.04.002. [DOI] [PubMed] [Google Scholar]
- Rossi S, Santarnecchi E, Valenza G, Ulivelli M. The heart side of brain neuromodulation. Philos Trans A Math Phys Eng Sci. 2016;374 doi: 10.1098/rsta.2015.0187. [DOI] [PubMed] [Google Scholar]
- Rothenberger S, Krafty R, Taylor B, Cribbet M, Thayer J, Buysse D, Kravitz H, Buysse E, Hall M. Time-varying correlations between delta EEG power and heart rate variability in midlife women: The SWAN Sleep Study. Psychophysiology. 2015;52:572–584. doi: 10.1111/psyp.12383. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Saito H, Sakai K, Jouvet M. Discharge patterns of the nucleus parabrachialis lateralis neurons of the cat during sleep and waking. Brain Res. 1977;134:59–72. doi: 10.1016/0006-8993(77)90925-8. [DOI] [PubMed] [Google Scholar]
- Scammell TE, Arrigoni E, Lipton JO. Neural circuitry of wakefulness and sleep. Neuron. 2017;93:747–765. doi: 10.1016/j.neuron.2017.01.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Schächinger H, Weinbacher M, Kiss A, Ritz R, Langewitz W. Cardiovascular indices of peripheral and central sympathetic activation. Psychosom Med. 2001;63:788–796. doi: 10.1097/00006842-200109000-00012. [DOI] [PubMed] [Google Scholar]
- Schnall R, Shlitner A, Sheffy J, Kedar R, Lavie P. Periodic, profound peripheral vasoconstriction--a new marker of obstructive sleep apnea. Sleep. 1999;22:939–946. [PubMed] [Google Scholar]
- Sforza E, Jouny C, Ibanez V. Cardiac activation during arousal in humans: further evidence for hierarchy in the arousal response. Clin Neurophysiol. 2000;111:1611–1619. doi: 10.1016/s1388-2457(00)00363-1. [DOI] [PubMed] [Google Scholar]
- Shea SA, Hilton MF, Hu K, Scheer FA. Existence of an Endogenous Circadian Blood Pressure Rhythm in Humans that Peaks in the Evening. Circ Res. 2011;108:980–984. doi: 10.1161/CIRCRESAHA.110.233668. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sherin JE, Shiromani PJ, McCarley RW, Saper CB. Activation of ventrolateral preoptic neurons during sleep. Science. 1996;271:216–219. doi: 10.1126/science.271.5246.216. [DOI] [PubMed] [Google Scholar]
- Sherwood A, Allen MT, Fahrenberg J, Kelsey RM, Lovallo WR, van Doornen LJ. Methodological guidelines for impedance cardiography. Psychophysiology. 1990;27:1–23. doi: 10.1111/j.1469-8986.1990.tb02171.x. [DOI] [PubMed] [Google Scholar]
- Silvani A. Physiological sleep-dependent changes in arterial blood pressure: central autonomic commands and baroreflex control. Clinical and experimental pharmacology & physiology. 2008;35:987–994. doi: 10.1111/j.1440-1681.2008.04985.x. [DOI] [PubMed] [Google Scholar]
- Silvani A. Orexins and the cardiovascular events of awakening. Temperature. 2017 doi: 10.1080/23328940.2017.1295128. in press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Silvani A, Calandra-Buonaura G, Benarroch EE, Dampney RA, Cortelli P. Bidirectional interactions between the baroreceptor reflex and arousal: an update. Sleep Med. 2015;16:210–216. doi: 10.1016/j.sleep.2014.10.011. [DOI] [PubMed] [Google Scholar]
- Silvani A, Calandra-Buonaura G, Dampney RA, Cortelli P. Brain-heart interactions: physiology and clinical implications. Philos. Trans. A Math. Phys. Eng. Sci. 2016;374:20150181. doi: 10.1098/rsta.2015.0181. [DOI] [PubMed] [Google Scholar]
- Silvani A, Dampney RA. Central control of cardiovascular function during sleep. Am. J. Physiol. Heart Circ. Physiol. 2013;305:H1683–H1692. doi: 10.1152/ajpheart.00554.2013. [DOI] [PubMed] [Google Scholar]
- Silvani A, Grimaldi D, Vandi S, Barletta G, Vetrugno R, Provini F, Pierangeli G, Berteotti C, Montagna P, Zoccoli G, Cortelli P. Sleep-dependent changes in the coupling between heart period and blood pressure in human subjects. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2008;294:R1686–R1692. doi: 10.1152/ajpregu.00756.2007. [DOI] [PubMed] [Google Scholar]
- Silvani A, Magosso E, Bastianini S, Lenzi P, Ursino M. Mathematical modeling of cardiovascular coupling: Central autonomic commands and baroreflex control. Auton Neurosci. 2011;162:66–71. doi: 10.1016/j.autneu.2011.04.003. [DOI] [PubMed] [Google Scholar]
- Smith L, Dawes P, Galland B. The use of pulse transit time in pediatric sleep studies: A systematic review. Sleep Med Rev. doi: 10.1016/j.smrv.2016.11.006. IN PRESS. [DOI] [PubMed] [Google Scholar]
- Snyder F, Hobson JA, Morrison DF, Goldfrank F. Changes in respiration, heart rate, and systolic blood pressure in human sleep. J. Appl. Physiol. 1964;19:417–422. doi: 10.1152/jappl.1964.19.3.417. [DOI] [PubMed] [Google Scholar]
- Somers V, Dyken M, Mark A, Abboud F. Sympathetic-nerve activity during sleep in normal subjects. N Engl J Med. 1993;328:303–307. doi: 10.1056/NEJM199302043280502. [DOI] [PubMed] [Google Scholar]
- Staessen J, Wang J, Thijs L. Cardiovascular protection and blood pressure reduction: a meta-analysis. Lancet. 2001;358:1305–1315. doi: 10.1016/S0140-6736(01)06411-X. [DOI] [PubMed] [Google Scholar]
- Stein P, Pu Y. Heart rate variability, sleep and sleep disorders. Sleep Med Rev. 2012;16:47–66. doi: 10.1016/j.smrv.2011.02.005. [DOI] [PubMed] [Google Scholar]
- Swanson LW. Understanding the basic plan. second. Oxford University Press; New York: 2011. Brain architecture. [Google Scholar]
- Swenne C. Baroreflex sensitivity: mechanisms and measurement. Neth Heart J. 2013;21:58–60. doi: 10.1007/s12471-012-0346-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Takeuchi S, Iwase S, Mano T, Okada H, Sugiyama Y, Watanabe T. Sleep-related changes in human muscle and skin sympathetic nerve activities. J Auton Nerv Syst. 1994;47:121–129. doi: 10.1016/0165-1838(94)90073-6. [DOI] [PubMed] [Google Scholar]
- Tank J, Diedrich A, Hale N, Niaz FE, Furlan R, Robertson RM, Mosqueda-Garcia R. Relationship between blood pressure, sleep K-complexes, and muscle sympathetic nerve activity in humans. Am J Physiol Regul Integr Comp Physiol. 2003;285:R208–R214. doi: 10.1152/ajpregu.00013.2003. [DOI] [PubMed] [Google Scholar]
- Taylor CE, Witter T, El Sayed K, Hissen SL, Johnson AW, Macefield VG. Relationship between spontaneous sympathetic baroreflex sensitivity and cardiac baroreflex sensitivity in healthy young individuals. Physiol Rep. 2015;3:e12536. doi: 10.14814/phy2.12536. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thayer J, Sternberg E. Beyond heart rate variability: vagal regulation of allostatic systems. Ann N Y Acad Sci. 2006;1088:361–372. doi: 10.1196/annals.1366.014. [DOI] [PubMed] [Google Scholar]
- Thayer JF, Yamamoto SS, Brosschot JF. The relationship of autonomic imbalance, heart rate variability and cardiovascular disease risk factors. Int J Cardiol. 2010;141:122–131. doi: 10.1016/j.ijcard.2009.09.543. [DOI] [PubMed] [Google Scholar]
- Thomas RJ, Mietus JE, Peng C-K, Guo D, Gozal D, Montgomery-Downs H, Gottlieb DJ, Wang C-Y, Goldberger AL. Relationship between delta power and the electrocardiogram-derived cardiopulmonary spectrogram: possible implications for assessing the effectiveness of sleep. Sleep Med. 2014;15:125–131. doi: 10.1016/j.sleep.2013.10.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Thompson RH, Swanson LW. Structural characterization of a hypothalamic visceromotor pattern generator network. Brain Res Rev. 2003;41:153–202. doi: 10.1016/s0165-0173(02)00232-1. [DOI] [PubMed] [Google Scholar]
- Trinder J. Cardiac activity and sympathovagal balance during sleep. Sleep Med Clin. 2007;2:199–208. [Google Scholar]
- Trinder J, Allen N, Kleiman J, Kralevski V, Kleverlaan D, Anson K, Kim Y. On the nature of cardiovascular activation at an arousal from sleep. Sleep. 2003;26:543–551. [PubMed] [Google Scholar]
- Trinder J, Ivens C, Kleiman J, Kleverlaan D, White DP. The cardiorespiratory activation response at an arousal from sleep is independent of the level of CO2. J Sleep Res. 2006;15:174–182. doi: 10.1111/j.1365-2869.2006.00513.x. [DOI] [PubMed] [Google Scholar]
- Trinder J, Kleiman J, Carrington M, Smith S, Breen S, Tan N, Kim Y. Autonomic activity during human sleep as a function of time and sleep stage. J Sleep Res. 2001;10:253–264. doi: 10.1046/j.1365-2869.2001.00263.x. [DOI] [PubMed] [Google Scholar]
- Trinder J, Nicholas CL. Respiratory and cardiac activity at sleep onset. In: Douglas BT, Floras JS, editors. Sleep Disorders and Cardiovascular and Cerebrovascular Disease. Marcel Dekker; New York: 2000. pp. 337–354. [Google Scholar]
- Trinder J, Waloszek J, Woods M, Jordan A. Sleep and cardiovascular regulation. Pflugers Arch. 2012;463:161–168. doi: 10.1007/s00424-011-1041-3. [DOI] [PubMed] [Google Scholar]
- Tsuji H, Larson M, Venditti F, Jr, Manders E, Evans J, Feldman C, Levy D. Impact of reduced heart rate variability on risk for cardiac events. The Framingham Heart Study. Circulation. 1996;94:2850–2855. doi: 10.1161/01.cir.94.11.2850. [DOI] [PubMed] [Google Scholar]
- Umetani K, Singer D, McCraty R, Atkinson M. Twenty-four hour time domain heart rate variability and heart rate: relations to age and gender over nine decades. J Am Coll Cardiol. 1998;31:593–601. doi: 10.1016/s0735-1097(97)00554-8. [DOI] [PubMed] [Google Scholar]
- Uschakov A, Gong H, McGinty D, Szymusiak R. Sleep-active neurons in the preoptic area project to the hypothalamic paraventricular nucleus and perifornical lateral hypothalamus. Eur. J. Neurosci. 2006;23:3284–3296. doi: 10.1111/j.1460-9568.2006.04860.x. [DOI] [PubMed] [Google Scholar]
- Valenza G, Citi L, Garcia RG, Taylor JN, Toschi N, Barbieri R. Complexity Variability Assessment of Nonlinear Time-Varying Cardiovascular Control. Sci Rep. 2017;7:42779. doi: 10.1038/srep42779. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Van de Borne P, Nguyen H, Biston P, Linkowski P, Degaute J. Effects of wake and sleep stages on the 24-h autonomic control of blood pressure and heart rate in recumbent men. Am J Physiol. 1994;266:H548–H554. doi: 10.1152/ajpheart.1994.266.2.H548. [DOI] [PubMed] [Google Scholar]
- Van de Vel A, Cuppens K, Bonroy B, Milosevic M, Jansen K, Van Huffel S, Vanrumste B, Lagae L, Ceulemans B. Non-EEG seizure-detection systems and potential SUDEP prevention: state of the art. Seizure. 2013;22:345–355. doi: 10.1016/j.seizure.2013.02.012. [DOI] [PubMed] [Google Scholar]
- Van Dongen H, Maislin G, Kerkhof G. Repeated assessment of the endogenous 24-hour profile of blood pressure under constant routine. Chronobiol Int. 2001;18:85–98. doi: 10.1081/cbi-100001178. [DOI] [PubMed] [Google Scholar]
- van Eekelen A, Houtveen J, Kerkhof G. Circadian variation in base rate measures of cardiac autonomic activity. Eur J Appl Physiol. 2004;93:39–46. doi: 10.1007/s00421-004-1158-6. [DOI] [PubMed] [Google Scholar]
- Verdecchia P. Prognostic value of ambulatory blood pressure: current evidence and clinical implications. Hypertension. 2000;35:844–851. doi: 10.1161/01.hyp.35.3.844. [DOI] [PubMed] [Google Scholar]
- Victor R, Leimbach W, Jr, Seals D, Wallin B, Mark A. Effects of the cold pressor test on muscle sympathetic nerve activity in humans. Hypertension. 1987;9:429–436. doi: 10.1161/01.hyp.9.5.429. [DOI] [PubMed] [Google Scholar]
- Wolf J, Hering D, Narkiewicz K. Non-dipping pattern of hypertension and obstructive sleep apnea syndrome. Hypertension research: official journal of the Japanese Society of Hypertension. 2010;33:867–871. doi: 10.1038/hr.2010.153. [DOI] [PubMed] [Google Scholar]
- Yang C, Lai C, Lai H, Kuo T. Relationship between electroencephalogram slow-wave magnitude and heart rate variability during sleep in humans. Neurosci Lett. 2002;329:213–216. doi: 10.1016/s0304-3940(02)00661-4. [DOI] [PubMed] [Google Scholar]
- Yoshimoto M, Yoshida I, Miki K. Functional role of diverse changes in sympathetic nerve activity in regulating arterial pressure during REM sleep. Sleep. 2011;34:1093–1101. doi: 10.5665/SLEEP.1168. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Young H, Benton D. We should be using nonlinear indices when relating heart-rate dynamics to cognition and mood. Sci Rep. 2015;5:16619. doi: 10.1038/srep16619. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zygmunt A, Stanczyk J. Methods of evaluation of autonomic nervous system function. Arch Med Sci. 2010;6:11–18. doi: 10.5114/aoms.2010.13500. [DOI] [PMC free article] [PubMed] [Google Scholar]