This meta-analysis examines whether sickle cell trait is associated with a higher risk of incident ischemic stroke among African Americans.
Key Points
Questions
Is sickle cell trait a genetic risk factor for increased risk of ischemic stroke among African Americans?
Findings
In this meta-analysis of 4 studies with 19 464 African American participants, no association was found between heterozygosity for the sickle cell mutation or sickle cell trait and incidence of ischemic stroke among African Americans.
Meaning
Among African Americans, sickle cell trait may not be a genetic risk factor for ischemic stroke.
Abstract
Importance
African Americans and individuals of African ancestry have a higher risk of stroke compared with non-Hispanic white individuals. Identifying the source of this disparity could provide an opportunity for clinical stroke risk stratification and more targeted therapy. Whether sickle cell trait (SCT) is an indicator of increased risk of ischemic stroke among African Americans is still unclear.
Objective
To examine whether SCT is associated with a higher risk of incident ischemic stroke among African Americans.
Design, Setting, and Participants
This meta-analysis assessed the association of SCT with the risk of incident ischemic stroke. Four large, prospective, population-based studies with African American cohorts were assessed: Jackson Heart Study (September 1, 2005, through December 31, 2012), Multi-Ethnic Study of Atherosclerosis (July 1, 2002, through December 31, 2012), Reasons for Geographic and Racial Differences in Stroke (January 1, 2003, through December 31, 2014), and Women’s Health Initiative (October 1, 1998, through December 31, 2012). Using a Cox proportional hazards regression model adjusted for major stroke risk factors, this study estimated the hazard ratio for incident ischemic stroke associated with SCT. Data analysis was performed from July 10, 2016, to February 2, 2017.
Interventions or Exposures
Participants’ SCT status determined by polymerase chain reaction assay genotyping or a combination of whole-exome sequencing and imputation.
Main Outcomes and Measures
Incident ischemic stroke.
Results
This meta-analysis included 19 464 African American individuals (1520 with SCT, 17 944 without SCT, and 620 with ischemic stroke) from 4 studies, with a mean (SD) age of 60.0 (13.0) years (5257 [27.0%] men and 14 207 [73.0%] women). No differences were found in the distribution of risk factors for ischemic stroke comparing participants with and those without SCT at study visit 1 in each cohort. The crude incidence of ischemic stroke was 2.9 per 1000 person-years (95% CI, 2.2-4.0 per 1000 person-years) among those with SCT and 3.2 per 1000 person-years (95% CI, 2.7-3.8 per 1000 person-years) among those without SCT. After stroke risk factors were adjusted for, the hazard ratio of incident ischemic stroke independently associated with SCT in the meta-analysis of all 4 cohorts was 0.80 (95% CI, 0.47-1.35; P = .82). The results of the meta-analysis were similar to those of individual cohorts, in which the results were also similar.
Conclusions and Relevance
Sickle cell trait may not be associated with incidence of ischemic stroke among African Americans. The results of this study suggest performing a more thorough clinical evaluation of a stroke patient with SCT rather than assuming that SCT is the etiologic factor for the stroke.
Introduction
Stroke is the fifth leading cause of death in the United States and a major cause of morbidity and loss of economic productivity.1 The prevalence of stroke is higher among African American individuals compared with non-Hispanic white individuals (4.5% vs 2.5%).2 In this regard, the incidence of stroke has been steadily decreasing among non-Hispanic white individuals but not among African American individuals, who also tend to experience stroke at a younger age.1,3 For instance, the overall age-adjusted incidence rate ratio for stroke between African American and non-Hispanic white individuals is 1.51, whereas it is 4.05 at ages 45 to 54 years but 0.86 at 85 years or older.3 A possible genetic contribution has been hypothesized as a reason for this observed disparity because traditional risk factors were only able to explain half of the observed disparity.4 One common potential genetic risk factor, and the focus of this article, is the sickle hemoglobin (β-globin) mutation.
The sickle cell mutation is an A/T point mutation that results in the substitution of valine for glutamic acid at the sixth position of the β-globin chain.5 The homozygous form (sickle cell anemia or HbSS), which is seen in 1 in 312 African Americans, has been associated with a wide array of complications,6 including stroke.7 The heterozygous state, sickle cell trait (SCT) or HbAS, which is prevalent in approximately 8% of African Americans,8,9 has been associated with an increased incidence and prevalence of venous thromboembolism10 and pulmonary embolism,11,12 with a population attributable risk of 6% to 9% for venous thromboembolism.10 Hypercoagulability attributable to SCT is a proposed mechanism for this association because those with SCT have higher circulating levels of D-dimer, thrombin-antithrombin complex, prothrombin fragment 1.2, and C-reactive protein compared with those without SCT.13,14 In addition, SCT has been associated with blood hyperviscosity,15 tendency for polymerization of hemoglobin,16,17 adherence of red blood cells to the endothelial surface,18 and increased levels of adhesion molecules.19 In general, these pathobiological processes increase the predisposition to microvascular occlusion and ischemic stroke, but whether there is an association between SCT and incidence of stroke in African Americans has been the subject of much debate.20,21
Several case reports22,23,24,25,26 have suggested an association with ischemic stroke, with a previous prospective, population-based study27 reporting an association between SCT and incident stroke in African Americans. The aim of our study was to provide more definitive data on the association between SCT and incident ischemic stroke in African Americans.
Methods
We conducted a meta-analysis of 4 prospective studies that were established to determine the risk factors for cardiovascular disease among diverse race/ethnicity groups in the United States. The cohorts are the Jackson Heart Study (JHS), Multi-Ethnic Study of Atherosclerosis (MESA), Reasons for Geographic and Racial Differences in Stroke (REGARDS), and Women’s Health Initiative (WHI). The design and methods for each study have been previously published.3,28,29,30,31,32 For each participant, baseline clinical information was collected by in-person examination and self-report. For this analysis, we included baseline covariate data and follow-up data on ischemic stroke from African American participants covering September 1, 2005, through December 31, 2012, for the JHS; July 1, 2002, through December 31, 2012, for MESA; January 1, 2003, through December 31, 2014, for REGARDS; and October 1, 1998, through December 31, 2012, for the WHI. All studies received institutional review board approval, and all participants provided written informed consent. Data analysis was performed from July 10, 2016, to February 2, 2017.
Genetic Assessment of SCT
Sickle cell trait was defined based on the presence of the minor allele of the rs334 single-nucleotide polymorphism encoding the HBB (OMIM 141900) p.Glu7Val mutation. The REGARDS sample was directly genotyped using a real-time polymerase chain reaction assay (TaqMan; Thermo Fisher Scientific),27,33 whereas the JHS, MESA, and WHI were assessed using a combination of whole-exome sequencing and imputation.34 Further details of the genotyping procedures, including imputation and quality control methods, have been published and are summarized in the eMethods in the Supplement.9,33
Identification of Incident Ischemic Stroke
The studies followed up participants annually or semiannually to identify occurrence of cardiovascular events, including stroke. Stroke events were obtained from hospitalizations or self-report and were then adjudicated by a panel of neurologists using a combination of clinical and radiologic information. Incident ischemic stroke was defined as the first adjudicated ischemic stroke event that occurred after participants completed their study enrollment and baseline examination. The World Health Organization’s definition of stroke35 was used but without strict adherence to the duration of symptoms when clinical and radiologic evidence of a stroke was present. Additional details on case definition are provided in the eMethods in the Supplement. Individuals who self-reported a history of stroke at the baseline examination were excluded from this analysis. We also censored those with incident hemorrhagic stroke (subarachnoid and intracerebral hemorrhages).
Statistical Analysis
Participants missing relevant covariate or genotype data were excluded before data analysis except when the specific covariate was missing for all individuals in the entire cohort. In addition, individuals who were genotyped or imputed to be homozygous for rs334 or determined to have compound heterozygosity, such as HbSC, were excluded from further analysis (n = 5; 3 from the JHS and 2 from the WHI). Data on the prevalence of SCT as well as baseline demographic, risk factor, and follow-up data were tabulated as proportions or means with SDs as appropriate. The crude incidence rate of ischemic stroke in each study cohort was estimated per 1000 person-years and then meta-analyzed using inverse variance weighting a priori assuming a random-effects model because of the small number of cohorts (n = 4) and inherent heterogeneity among the study cohorts.
We used Cox proportional hazards regression analysis to determine the hazard ratio (HR) for ischemic stroke among individuals with SCT compared with those without SCT, adjusting for relevant covariates. Three levels of covariate adjustment were performed. In model 1, we adjusted for age, sex, and region of residence (in REGARDS only). In model 2, in addition to the covariates in model 1, we adjusted for the components of the Framingham stroke risk score, systolic blood pressure, diabetes mellitus, cigarette smoking (current vs noncurrent except in the WHI, in which it was ever- vs never-smokers), history of cardiovascular disease, hypertension status (defined as diagnosed hypertension or current use of antihypertensive medication), history of atrial fibrillation, and history of left ventricular hypertrophy.36,37 In model 3, in addition to the covariates in model 2, we adjusted for principal components of global ancestry derived from the genome-wide array genotyping data. The results from the Cox proportional hazards regression model and from models 1, 2, and 3 were then combined using inverse variance-weighted meta-analysis, assuming a random-effects model. We also presented the result of the meta-analysis of the fully adjusted model in a forest plot. P < .05 was considered statistically significant based on an inverse variance–weighted approach assuming a random-effects model.
Results
Baseline Characteristics
The total sample size of 19 464 African Americans (mean [SD] age, 60.0 [13.0] years; 5257 [27.0%] men and 14 207 [73.0%] women) included 1520 individuals with SCT and 620 individuals with incident ischemic stroke. The prevalence of SCT among the cohorts ranged from 7.7% to 9.0%, with a mean prevalence of 7.8%, which is consistent with prevalence estimates in African Americans from the general US population.8,38 Table 1 indicates that there was no difference in the distribution of risk factors, number of strokes, or age at ischemic stroke event between those with SCT compared with those without SCT in each cohort.
Table 1. Baseline Characteristics and Distribution of Risk Factors Among Participants by Study Cohort and SCT Statusa.
| Variable | JHS (n = 2133) | MESA (n = 1556) | REGARDS (n = 9759) | WHI (n = 6016) | ||||
|---|---|---|---|---|---|---|---|---|
| SCT | No SCT | SCT | No SCT | SCT | No SCT | SCT | No SCT | |
| Frequency of rs334 | 177 (8.3) | 1956 (91.7) | 141 (9.0) | 1415 (91.0) | 741 (7.6) | 9018 (92.4) | 460 (7.7) | 5555 (92.3) |
| Age, mean (SD), y | 50.4 (12.3) | 50.2 (11.9) | 61.0 (10.0) | 62.0 (10.0) | 63.4 (9.4) | 63.8 (9.2) | 63.6 (7.1) | 63.2 (7.1) |
| Female | 97 (54.8) | 1203 (61.5) | 77 (54.6) | 764 (53.9) | 476 (64.2) | 5575 (61.8) | 460 (100) | 5555 (100) |
| Systolic blood pressure, mean (SD), mm Hg | 123.3 (16.1) | 125.5 (16.5) | 131.0 (20.0) | 132.0 (22.0) | 131.1 (17.4) | 130.7 (17.3) | 133.0 (18.9) | 134.0 (18.0) |
| Diabetes mellitus | 28 (15.8) | 363 (18.6) | 32 (23) | 241 (17) | 217 (29.7) | 2573 (28.4) | 60 (13.0) | 596 (10.7) |
| Hypertension | 82 (46.3) | 971 (49.6) | 80 (57) | 835 (59) | 503 (68.1) | 6338 (70.4) | 223 (47.5) | 3028 (54.5) |
| Current cigarette smoking | 26 (14.7) | 284 (14.5) | 27 (19) | 269 (19) | 127 (17.2) | 1546 (17.3) | 51 (11.1)b | 582 (10.5)b |
| Atrial fibrillation (self-report or ECG evidence) | 1 (0.6) | 5 (0.3) | 0 | 0 | 67 (9.3) | 647 (7.4) | 22 (4.8) | 243 (4.4) |
| LVH (12 lead)c | 11 (6.2) | 77 (3.9) | NA | NA | 43 (8.3) | 447 (7.2) | 25 (5.4) | 376 (6.8) |
| History of CVD | 14 (17.9) | 169 (8.6) | 0 | 0 | 106 (14.6) | 1244 (14.1) | 12 (2.6) | 198 (3.6) |
| Incident ischemic stroke | 2 (1.1) | 38 (1.9) | 2 (1.4) | 36 (2.5) | 19 (2.6) | 287 (3.2) | 17 (3.7) | 219 (3.9) |
| Follow-up time, median (SD), y | 9.6 | 9.8 | 8.4 | 8.4 | 9.5 | 9.5 | 8.8 | 9.0 |
| Total follow-up, No. of person-years | 1593.4 | 17 785.8 | 1020 | 10 575 | 7042.6 | 85 990.9 | 4719.6 | 60 380.8 |
| Age at ischemic stroke event, mean (SD), yd | 74.0 (1.3) | 64.8 (11.8) | 72 (10.1) | 70.0 (10.0) | 72.6 (9.2) | 71.8 (8.9) | 71.8 (7.0) | 73.7 (8.4) |
| Framingham stroke risk, mean (SD) | NA | NA | 16.0 | 16.0 | 10.9 (11.4) | 10.9 (11.2) | 15.5 (10.3) | 15.5 (10.4) |
Abbreviations: CVD, cardiovascular disease; ECG, echocardiography; JHS, Jackson Heart Study; LVH, left ventricular hypertrophy; MESA, Multi-Ethnic Study of Atherosclerosis; NA, not applicable; REGARDS, Reasons for Geographic and Racial Differences in Stroke; SCT, sickle cell trait; WHI, Women’s Health Initiative.
Data are presented as number (percentage) unless otherwise indicated.
Represents individuals who have ever smoked cigarettes.
Variable missing for more than half of the WHI cohort.
Estimated for the WHI participants.
Association of SCT With Incident Stroke
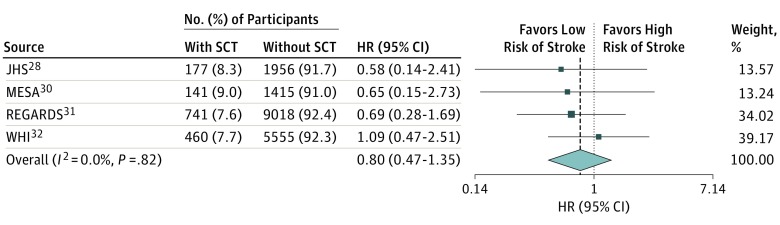
The analysis within each cohort and the subsequent meta-analysis (Table 2) indicate that the crude incidence rate for ischemic stroke was not different between individuals with SCT (2.9 per 1000 person-years; 95% CI, 2.2-4.0 per 1000 person-years) and those without SCT (3.2 per 1000 person-years; 95% CI, 2.7-3.8 per 1000 person-years). Similarly, as indicated in Table 3, the adjusted HR for ischemic stroke was not significantly different between participants with SCT and those without SCT (meta-analysis HR, 0.80; 95% CI, 0.47-1.35; P = .82) (Figure). No associations were observed in the cohort-specific analyses or in the meta-analysis for any of the sequentially adjusted models.
Table 2. Crude Incidence of Ischemic Stroke Among Patients With SCT and Those Without SCT.
| Study | Incidence per 1000 Person-Years (95% CI) |
|---|---|
| JHS | |
| SCT | 1.2 (0.2-4.1) |
| No SCT | 2.1 (1.5-2.9) |
| MESA | |
| SCT | 2.0 (0.3-6.5) |
| No SCT | 3.4 (2.4-4.7) |
| REGARDS | |
| SCT | 2.7 (1.7-4.1) |
| No SCT | 3.4 (2.4-4.7) |
| WHI | |
| SCT | 3.6 (2.2-5.6) |
| No SCT | 3.6 (3.2-4.1) |
| Meta-analysis | |
| SCT | 2.9 (2.2-4.0) |
| No SCT | 3.2 (2.7-3.8) |
Abbreviations: JHS, Jackson Heart Study; MESA, Multi-Ethnic Study of Atherosclerosis; REGARDS, Reasons for Geographic and Racial Differences in Stroke; SCT, sickle cell trait; WHI, Women’s Health Initiative.
Table 3. HRs for Stroke Among Patients With SCT Compared With Those Without SCT.
| Adjusted Modela | JHS | MESA | REGARDS | WHI | Meta-analysis | |||||
|---|---|---|---|---|---|---|---|---|---|---|
| HR (95% CI) | P Value | HR (95% CI) | P Value | HR (95% CI) | P Value | HR (95% CI) | P Value | HR (95% CI) | P Value | |
| Model 1 | 0.59 (0.14-2.44) | .46 | 0.60 (0.14-2.49) | .48 | 0.82 (0.51-1.30) | .39 | 1.01 (0.61-1.65) | .98 | 0.87 (0.63-1.20) | .39 |
| Model 2 | 0.56 (0.13-2.32) | .42 | 0.56 (0.14-2.34) | .43 | 0.84 (0.52-1.35) | .46 | 0.97 (0.47-1.99) | .93 | 0.83 (0.57-1.20) | .31 |
| Model 3 | 0.58 (0.14-2.41) | .45 | 0.65 (0.15-2.73) | .55 | 0.69 (0.28-1.69) | .41 | 1.09 (0.47-2.51) | .84 | 0.80 (0.47-1.35) | .82 |
Abbreviations: HR, hazard ratio; JHS, Jackson Heart Study; MESA, Multi-Ethnic Study of Atherosclerosis; REGARDS, Reasons for Geographic and Racial Differences in Stroke; SCT, sickle cell trait; WHI, Women’s Health Initiative.
A description of the models is given in the Statistical Analysis subsection of the Methods section.
Figure. Forest Plot of the Association Between Sickle Cell Trait (SCT) Status and Incidence of Stroke in the 4 African American Cohorts.
The fully adjusted Cox proportional hazards regression model (adjusted model 3) is shown. Weights are from random-effects analysis. Boxes indicate hazard ratios (HRs); error bars, 95% CIs; and diamond, overall results. HR indicates hazard ratio; JHS, Jackson Heart Study; MESA, Multi-Ethnic Study of Atherosclerosis; REGARDS, Reasons for Geographic and Racial Differences in Stroke; and WHI, Women’s Health Initiative.
Discussion
In this meta-analysis of 4 large, population-based studies, there was no evidence of a statistically significant association between SCT and risk of incident ischemic stroke in African Americans. Neither the crude incidence rate nor the Cox proportional hazards regression models indicated that SCT is a risk factor for ischemic stroke. The absence of an association between SCT and risk of ischemic stroke was consistent among the cohorts and suggests that SCT is not an independent genetic risk factor for ischemic stroke among African Americans.
Although sickle cell anemia is associated with stroke risk, previous evidence of an association between SCT and stroke was limited to case reports22,23,24,26,39,40,41 and a single-cohort longitudinal study.27 The latter study found a 1.4-fold (95% CI, 1.0-2.0) increased risk of ischemic stroke in SCT carriers compared with noncarriers in a population-based cohort of 3497 African Americans. A first possible reason for the inconsistency of results among studies could be because of differences in methods, such as in case ascertainment and definition. However, this reason is unlikely because all the studies used similar surveillance and clinical and radiologic criteria for case identification and definition. A second possible reason is that in our study, the sample of participants with SCT who were in the age groups at greater risk of stroke (in each cohort) was relatively small; thus, differences among studies were likely caused by chance. A third possible reason relates to differences in the covariates considered. For instance, in our study, we adjusted for left ventricular hypertrophy, a component of the Framingham stroke risk score, which was not done in the prior published study.27 However, in our analysis, adjusting for left ventricular hypertrophy did not change the direction of estimate effects.
Limitations
A limitation of our study is that approximately 48% of our sample was not directly genotyped; thus, there is a risk of misclassification of SCT status. We do not believe that misclassification accounts for our lack of association because the κ statistic for imputed vs sequenced genotypes was 0.91 (95% CI, 0.87-0.95), which is considered to indicate high-quality imputation.34 Furthermore, the effect estimates and lack of association that we observed were similar for REGARDS and the JHS, in which all participants were directly genotyped. Finally, we were unable to test the association of SCT with ischemic stroke subtypes. Thus, it remains possible that SCT is associated with 1 or more ischemic stroke subtypes.
Conclusions
In this meta-analysis, we did not observe an association between SCT and an increased risk of stroke in African Americans. Future studies with large numbers of African Americans, longer follow-up, and carefully subtyped ischemic stroke events are needed to further elucidate the possible association of SCT with incident ischemic stroke overall and by specific ischemic stroke subtypes.
eMethods. Supplemental Methods
References
- 1.Ovbiagele B, Goldstein LB, Higashida RT, et al. ; American Heart Association Advocacy Coordinating Committee and Stroke Council . Forecasting the future of stroke in the United States: a policy statement from the American Heart Association and American Stroke Association. Stroke. 2013;44(8):2361-2375. doi: 10.1161/STR.0b013e31829734f2 [DOI] [PubMed] [Google Scholar]
- 2.Benjamin EJ, Blaha MJ, Chiuve SE, et al. ; American Heart Association Statistics Committee and Stroke Statistics Subcommittee . Heart disease and stroke statistics—2017 update: a report from the American Heart Association. Circulation. 2017;135(10):e146-e603. doi: 10.1161/CIR.0000000000000485 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Howard VJ, Kleindorfer DO, Judd SE, et al. . Disparities in stroke incidence contributing to disparities in stroke mortality. Ann Neurol. 2011;69(4):619-627. doi: 10.1002/ana.22385 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Howard G, Cushman M, Kissela BM, et al. ; Reasons for Geographic and Racial Differences in Stroke (REGARDS) Investigators . Traditional risk factors as the underlying cause of racial disparities in stroke: lessons from the half-full (empty?) glass. Stroke. 2011;42(12):3369-3375. doi: 10.1161/strokeaha.111.625277 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Pauling L, Itano HA, et al. . Sickle cell anemia, a molecular disease. Science. 1949;110(2865):543-548. [DOI] [PubMed] [Google Scholar]
- 6.Tsaras G, Owusu-Ansah A, Boateng FO, Amoateng-Adjepong Y. Complications associated with sickle cell trait: a brief narrative review. Am J Med. 2009;122(6):507-512. doi: 10.1016/j.amjmed.2008.12.020 [DOI] [PubMed] [Google Scholar]
- 7.Driss A, Asare KO, Hibbert JM, Gee BE, Adamkiewicz TV, Stiles JK. Sickle cell disease in the post genomic era: a monogenic disease with a polygenic phenotype. Genomics Insights. 2009;2009(2):23-48. doi: 10.4137/GEI.S2626 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Ojodu J, Hulihan MM, Pope SN, Grant AM; Centers for Disease Control and Prevention (CDC) . Incidence of sickle cell trait—United States, 2010. MMWR Morb Mortal Wkly Rep. 2014;63(49):1155-1158. [PMC free article] [PubMed] [Google Scholar]
- 9.Bello NA, Hyacinth HI, Roetker NS, et al. . Sickle cell trait is not associated with an increased risk of heart failure or abnormalities of cardiac structure and function. Blood. 2017;129(6):799-801. doi: 10.1182/blood-2016-08-705541 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Austin H, Key NS, Benson JM, et al. . Sickle cell trait and the risk of venous thromboembolism among blacks. Blood. 2007;110(3):908-912. doi: 10.1182/blood-2006-11-057604 [DOI] [PubMed] [Google Scholar]
- 11.Folsom AR, Tang W, Roetker NS, et al. . Prospective study of sickle cell trait and venous thromboembolism incidence. J Thromb Haemost. 2015;13(1):2-9. doi: 10.1111/jth.12787 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Heller P, Best WR, Nelson RB, Becktel J. Clinical implications of sickle-cell trait and glucose–6-phosphate dehydrogenase deficiency in hospitalized black male patients. N Engl J Med. 1979;300(18):1001-1005. doi: 10.1056/NEJM197905033001801 [DOI] [PubMed] [Google Scholar]
- 13.Pradhan RK, Mishra R, Nag C. Diurnal variations of C-reactive protein in trait and sickle cell disease patients. Biol Rhythm Res. 2013;44(2):277-285. doi: 10.1080/09291016.2012.681846 [DOI] [Google Scholar]
- 14.Westerman MP, Green D, Gilman-Sachs A, et al. . Coagulation changes in individuals with sickle cell trait. Am J Hematol. 2002;69(2):89-94. doi: 10.1002/ajh.10021 [DOI] [PubMed] [Google Scholar]
- 15.Monchanin G, Connes P, Wouassi D, et al. . Hemorheology, sickle cell trait, and alpha-thalassemia in athletes: effects of exercise. Med Sci Sports Exerc. 2005;37(7):1086-1092. doi: 10.1249/01.mss.0000170128.78432.96 [DOI] [PubMed] [Google Scholar]
- 16.Connes P, Sara F, Hardy-Dessources MD, et al. . Effects of short supramaximal exercise on hemorheology in sickle cell trait carriers. Eur J Appl Physiol. 2006;97(2):143-150. doi: 10.1007/s00421-006-0155-3 [DOI] [PubMed] [Google Scholar]
- 17.Tripette J, Hardy-Dessources MD, Sara F, et al. . Does repeated and heavy exercise impair blood rheology in carriers of sickle cell trait? Clin J Sport Med. 2007;17(6):465-470. doi: 10.1097/JSM.0b013e31815aed23 [DOI] [PubMed] [Google Scholar]
- 18.Hebbel RP, Yamada O, Moldow CF, Jacob HS, White JG, Eaton JW. Abnormal adherence of sickle erythrocytes to cultured vascular endothelium: possible mechanism for microvascular occlusion in sickle cell disease. J Clin Invest. 1980;65(1):154-160. doi: 10.1172/JCI109646 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Monchanin G, Serpero LD, Connes P, et al. . Effects of progressive and maximal exercise on plasma levels of adhesion molecules in athletes with sickle cell trait with or without alpha-thalassemia. J Appl Physiol (1985). 2007;102(1):169-173. doi: 10.1152/japplphysiol.00272.2006 [DOI] [PubMed] [Google Scholar]
- 20.Golomb MR. Sickle cell trait is a risk factor for early stroke. Arch Neurol. 2005;62(11):1778-1779. doi: 10.1001/archneur.62.11.1778 [DOI] [PubMed] [Google Scholar]
- 21.Dowling MM. Sickle cell trait is not a risk factor for stroke. Arch Neurol. 2005;62(11):1780-1781. doi: 10.1001/archneur.62.11.1780 [DOI] [PubMed] [Google Scholar]
- 22.Gines R, Truemper E. Stroke in a 9-year-old with sickle cell trait. Am J Emerg Med. 1998;16(1):104-105. doi: 10.1016/S0735-6757(98)90085-7 [DOI] [PubMed] [Google Scholar]
- 23.Greenwald JG. Stroke in a woman with sickle cell trait taking oral contraceptives. Conn Med. 1971;35(4):231-232. [PubMed] [Google Scholar]
- 24.Partington MD, Aronyk KE, Byrd SE. Sickle cell trait and stroke in children. Pediatr Neurosurg. 1994;20(2):148-151. [DOI] [PubMed] [Google Scholar]
- 25.Swanson TH, Zinkel JL, Peterson PL. Bilateral anterior cerebral artery occlusion in an alcohol abuser with sickle-cell trait. Henry Ford Hosp Med J. 1987;35(1):67-70. [PubMed] [Google Scholar]
- 26.Favale F, Gardembas M, Pajot O, et al. . Southeast Asian ovalocytosis and a sickle cell trait in a young patient with sudden retinal stroke: a fortuitous association? Hemoglobin. 2009;33(6):475-479. doi: 10.3109/03630260903344440 [DOI] [PubMed] [Google Scholar]
- 27.Caughey MC, Loehr LR, Key NS, et al. . Sickle cell trait and incident ischemic stroke in the Atherosclerosis Risk in Communities study. Stroke. 2014;45(10):2863-2867. doi: 10.1161/STROKEAHA.114.006110 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Taylor HA Jr, Wilson JG, Jones DW, et al. . Toward resolution of cardiovascular health disparities in African Americans: design and methods of the Jackson Heart Study. Ethn Dis. 2005;15(4 suppl 6):4-17. [PubMed] [Google Scholar]
- 29.Keku E, Rosamond W, Taylor HA Jr, et al. . Cardiovascular disease event classification in the Jackson Heart Study: methods and procedures. Ethn Dis. 2005;15(4 suppl 6):62-70. [PubMed] [Google Scholar]
- 30.Bild DE, Bluemke DA, Burke GL, et al. . Multi-Ethnic Study of Atherosclerosis: objectives and design. Am J Epidemiol. 2002;156(9):871-881. doi: 10.1093/aje/kwf113 [DOI] [PubMed] [Google Scholar]
- 31.Howard VJ, Cushman M, Pulley L, et al. . The Reasons for Geographic and Racial Differences in Stroke study: objectives and design. Neuroepidemiology. 2005;25(3):135-143. doi: 10.1159/000086678 [DOI] [PubMed] [Google Scholar]
- 32.The Women’s Health Initiative Study Group Design of the Women’s Health Initiative clinical trial and observational study. Control Clin Trials. 1998;19(1):61-109. doi: 10.1016/S0197-2456(97)00078-0 [DOI] [PubMed] [Google Scholar]
- 33.Naik RP, Derebail VK, Grams ME, et al. . Association of sickle cell trait with chronic kidney disease and albuminuria in African Americans. JAMA. 2014;312(20):2115-2125. doi: 10.1001/jama.2014.15063 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Auer PL, Johnsen JM, Johnson AD, et al. . Imputation of exome sequence variants into population-based samples and blood-cell-trait–associated loci in African Americans: NHLBI GO Exome Sequencing Project. Am J Hum Genet. 2012;91(5):794-808. doi: 10.1016/j.ajhg.2012.08.031 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Stroke—1989: recommendations on stroke prevention, diagnosis, and therapy: report of the WHO Task Force on Stroke and Other Cerebrovascular Disorders. Stroke. 1989;20(10):1407-1431. [DOI] [PubMed] [Google Scholar]
- 36.Wolf PA, D’Agostino RB, Belanger AJ, Kannel WB. Probability of stroke: a risk profile from the Framingham Study. Stroke. 1991;22(3):312-318. doi: 10.1161/01.str.22.3.312 [DOI] [PubMed] [Google Scholar]
- 37.D’Agostino RB, Wolf PA, Belanger AJ, Kannel WB. Stroke risk profile: adjustment for antihypertensive medication: the Framingham Study. Stroke. 1994;25(1):40-43. doi: 10.1161/01.str.25.1.40 [DOI] [PubMed] [Google Scholar]
- 38.Grant AM, Parker CS, Jordan LB, et al. . Public health implications of sickle cell trait: a report of the CDC meeting. Am J Prev Med. 2011;41(6)(suppl 4):S435-S439. doi: 10.1016/j.amepre.2011.09.012 [DOI] [PubMed] [Google Scholar]
- 39.Greenwald JG. Stroke, sickle cell trait, and oral contraceptives. Ann Intern Med. 1970;72(6):960. [DOI] [PubMed] [Google Scholar]
- 40.Radhakrishnan K, Thacker AK, Maloo JC, el-Mangoush MA. Sickle cell trait and stroke in the young adult. Postgrad Med J. 1990;66(782):1078-1080. doi: 10.1136/pgmj.66.782.1078 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Riggs JE, Ketonen LM, Wang DD, Valanne LK. Cerebral infarction in a child with sickle cell trait. J Child Neurol. 1995;10(3):253-254. doi: 10.1177/088307389501000323 [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
eMethods. Supplemental Methods