Abstract
We investigated the associations of body fat percentage, objectively assessed moderate-to-vigorous physical activity (MVPA), and different types of physical activity assessed by a questionnaire with neuromuscular performance. The participants were 404 children aged 6–8 years. Body fat percentage (BF%) was assessed using dual-energy x-ray absorptiometry and physical activity by combined heart rate and movement sensing and a questionnaire. The results of 50-metre shuttle run, 15-metre sprint run, hand grip strength, standing long jump, sit-up, modified flamingo balance, box and block, and sit-and-reach tests were used as measures of neuromuscular performance. Children who had a combination of higher BF% and lower levels of physical activity had the poorest performance in 50-metre shuttle run, 15-metre sprint run, and standing long jump tests. Higher BF% was associated with slower 50-metre shuttle run and 15-metre sprint times, shorter distance jumped in standing long jump test, fewer sit-ups, more errors in balance test, and less cubes moved in box and block test. Higher levels of physical activity and particularly MVPA assessed objectively by combined accelerometer and heart rate monitor were related to shorter 50-metre shuttle run and 15-metre sprint times. In conclusion, higher BF% and lower levels of physical activity and particularly the combination of these two factors were associated with worse neuromuscular performance.
Keywords: Adiposity, physical activity, DXA, physical fitness, children
Introduction
Neuromuscular performance, a combination of attributes such as motor skills and muscular strength, is an essential part of children´s daily life (Shumway-Cook & Woollacott, 1995). However, neuromuscular performance, and particularly motor proficiency, has declined over the past decades in children (Hardy, King, Espinel, Cosgrove, & Bauman, 2010; Olesen, Kristensen, Ried-Larsen, Grøntved, & Froberg, 2014; Runhaar et al., 2010). Overweight and physical inactivity have become one of the most important public health problems among children and adolescents in developed countries (Haug et al., 2010; Lee et al., 2012; Ng et al., 2014). This could be one of the explanations for the decreased neuromuscular performance among children (Rodriques, Stodden, & Lopes, 2015).
Increased body mass index (BMI) and waist circumference have been associated with impaired neuromuscular performance in children and adolescents (Artero et al., 2010; Cattuzzo et al., 2014; Malina et al., 1995; Rauner, Mess, & Woll, 2013; Smith et al., 2014), whereas the results of some studies suggest that higher levels of habitual physical activity are associated with better neuromuscular performance among children (Fisher et al., 2005; Iivonen et al., 2013; Lubans, Morgan, Cliff, Barnett, & Okely, 2010; Williams et al., 2008). Nevertheless, there are few studies on the associations of body fat percentage assessed by dual-energy x-ray absorptiometry (DXA) with neuromuscular performance in children (Rauner et al., 2013). The results of some previous studies suggest a weak and partly inconsistent relationship of physical activity with neuromuscular performance (Holfelder & Schott, 2014, Iivonen et al., 2013; Laukkanen, Pesola, Havu, Sääkslahti, & Finni, 2013; Okely, Booth, & Patterson, 2001). These inconsistencies may be partly due to different methods, such as accelerometers, electromyography, and questionnaires, used to assess physical activity (Holfelder & Schott, 2014, Iivonen et al., 2013; Laukkanen, Pesola, Havu, Sääkslahti, & Finni, 2013; Okely, Booth, & Patterson, 2001).
Adiposity and physical activity are interrelated (Jiménez-Pavón, Kelly, & Reilly, 2010) and increasing evidence indicates that impaired neuromuscular performance combined with low levels of physical activity is associated with increased risk of overweight and obesity in children (Robinson et al. 2015). Overweight or obese children are more often physically inactive and have poorer neuromuscular performance than children with higher levels of physical activity suggesting multidirectional associations between adiposity, physical activity, and neuromuscular performance (Robinson et al. 2015). However, little is known about the combined associations of adiposity and physical activity with neuromuscular performance among children. The findings by Morrison et al. (2012) suggest that children with a low body fat percentage assessed by skin fold-thickness who also have high levels of physical activity have better neuromuscular performance than children with a high body fat percentage and low levels of physical activity.
We aimed to investigate the independent and combined associations of body fat percentage and different types of physical activity with several components of neuromuscular performance in a population sample of children.
Methods
Study design and study population
The Physical Activity and Nutrition in Children (PANIC) Study is an ongoing physical activity and diet intervention study in a population sample of children from the city of Kuopio, Finland (Eloranta et al., 2014). Altogether 736 children 6–8 years of age were invited to participate in the baseline study in 2007–2009. Of the invited children, 512 (70%) agreed to participated. The participants did not differ in sex distribution or BMI-standard deviation score (BMI-SDS) from other children of the same age whose data were obtained from school health examinations (data not shown). Complete data on neuromuscular performance, body fat percentage, and physical activity assessed by questionnaire were available for 404 children (200 boys, 204 girls) and complete data on neuromuscular performance, body fat percentage, and physical activity assessed objectively by combined accelerometer and heart rate monitor were available for 343 children (162 boys, 181 girls). The children included in the analyses did not differ in physical activity, body fat percentage, or neuromuscular performance from those excluded from the analyses. The PANIC Study protocol was approved by the Research Ethics Committee of the Hospital District of Northern Savo. All participating children and their parents provided written informed consent.
Assessment of body size and composition
Body fat mass, body fat percentage, and lean body mass were measured by the Lunar Prodigy Advance® DXA device (GE Medical Systems, Madison, WI, USA) using standardised protocols (Tompuri et al., 2015). Body weight was measured twice to the nearest 0.1kg after overnight fasting, bladder emptying, and whilst standing in light underwear using the InBody® 720 bioelectrical impedance device (Biospace, Seoul, Korea). The mean of the two values was used for analyses. Body height was measured three times to the nearest 0.1cm using a wall-mounted stadiometer whilst barefoot and with the head positioned in the Frankfurt plane. The mean of the nearest two values was used for analyses. The prevalence of overweight and obesity was defined using cut-offs published by Cole and co-workers (Cole, Bellizzi, Flegal, & Dietz, 2000).
Assessment of physical activity
Physical activity was assessed using a combined heart rate and movement sensing monitor (Actiheart®, CamNtech Ltd., Papworth, UK) (Brage, Brage, Franks, Ekelund, & Wareham, 2005) which was attached to the children´s chest with two standard ECG electrodes. The children were asked to wear the monitor continuously for seven days (including sleep and water-based activities) without changing their usual behaviour. The heart rate data were individually calibrated with a maximal cycle ergometer exercise test. Free-living heart rate data were pre-processed before final analysis (Stegle, Fallert, & Brage, 2008). We used a branched equation modelling to integrate the acceleration signal and heart rate into estimates of physical activity energy expenditure (Brage et al., 2007). We defined time spent in moderate-to-vigorous physical activity (MVPA) using a threshold of ≥ 3 METs intensity. We included children who had at least 48 hours (32 hours during week-days, 16 hours during weekend days) of valid activity recording into the analyses (Collings et al. 2015). The median recording time was 67.8 hours (interquartile range, IQR = 35.3) for week-days and 39.3 hours (IQR = 14.0) for weekend days.
We also assessed different types of physical activity using the PANIC Physical Activity Questionnaire (Haapala et al., 2014; Väistö et al., 2014). The types of physical activity included organised sports, supervised exercise other than sports (e.g. afterschool exercise clubs), unsupervised physical activity, physically active school transportation (such as walking and bicycling), and physical activity during recess. In Finnish schools, 1.5 hours of physical education per week are compulsory for all children in Grades 1–9. We did not include physical education in analyses concerning the different types of physical activity because time spent in physical education was the same for all children. Data regarding the frequency of each type of physical activity and the average duration of each of the sessions was reported. The amount of physical activity was calculated by multiplying the frequency with the average duration of the physical activity session and was expressed in minutes per week.
Neuromuscular performance
Running speed and agility were assessed by the 50-metre shuttle run test (European Council, 1988). The children were asked to run five metres from a start line to another line as fast as possible, to turn on the line, run back to the start and to continue until five shuttles were completed. The test score was the running time in seconds, with a longer time indicating a poorer performance.
Sprint running speed was assessed by the 15-metre sprint test. The children were asked to run five times 18 metres as fast as possible at 50-second intervals. After a recovery period of four minutes, the children were again asked to repeat the same test again. Time spent in each run was measured using two photo cells (ALGE-TIMING GmbH, Lustenau, Austria). The first photocell was placed at 2.5 metres from the start allowing the children to speed up before the timer started. The second photocell was placed 0.5 metres before the finish line. The test score was the time of the fastest 15-metre run.
Hand grip strength was assessed by the Martin vigorimeter (Martin, Tuttlingen, Germany). The children were asked to keep the elbow close to the body with the arm flexed at 90° and to squeeze a rubber bulb as hard as possible three times with each hand. The mean of the best result from each hand was used in the analyses. Hand grip strength was expressed in kilopascals.
Lower limb explosive strength was assessed by the standing long jump test (European Council, 1988). The children were asked to stand with their feet together, then jump as far as possible and to land on both feet. The test score was the longest jump of three attempts in centimetres.
The sit-up test was used to assess abdominal muscle strength and endurance (European Council, 1988). The children were asked to lie down with knees flexed at 90°, feet positioned on the ground and arms behind the neck. The children were told to do as many sit-ups as possible in 30 seconds with the elbows coming up to touch the knees with the assistant holding their feet on the floor. The test score was the number of technically correct sit-ups completed in 30 seconds.
Static balance was assessed by the modified flamingo balance test. The children were asked to stand barefoot on one leg with eyes closed for 30 seconds. The test score was the number of times the free foot touched the floor or eyes opened during the test, a larger number indicating a poorer static balance.
Manual dexterity and upper limb movement speed were assessed by the box and block test (Jongbloed-Pereboom, Nijhuis-van der Sanden, & Steenbergen, 2013). The tests were performed using a wooden box (53.7cm x 25.4cm x 8cm) divided into two identical compartments by a partition. At the beginning of the test, 150 small wooden cubes (2.5cm/side) were placed in one compartment. The children were asked to pick up the cubes one by one with the dominant hand from one side of the wooden box and to move as many cubes as possible over the partition to the other side of the box in a random order during 60 seconds. The same task was repeated with the non-dominant hand. The test score was the total number of cubes moved to the other side of the box in two minutes, a smaller number of cubes moved indicating a poorer manual dexterity.
Lower back and hamstring muscle flexibility was assessed using the sit-and-reach test (European Council, 1988). The children were asked to sit down with the heels at the zero line and the heels 25 centimetres apart. The measuring stick was placed to -38 centimetres from the zero line. The children were asked to reach forward slowly, as far as possible keeping the hands parallel and knees extended and to repeat the test three times. The test score was the longest distance in centimetres reached with the fingertips from the starting line of -38 centimetres.
Other assessments
The research physician assessed pubertal status using the 5-stage criteria described by Tanner (Tanner, 1962). The boys were defined as having entered clinical puberty, if their testicular volume assessed by an orchidometer was >3 ml (Stage ≥2). The girls were defined having entered clinical puberty if their breast development had started (Stage ≥2).
The parents were asked to report in a questionnaire their annual household income, (≤ 30,000 €, 30,001–60,000 € and ≥ 60,001 €) and their highest completed or ongoing educational degrees (vocational school or less, polytechnic, university). The degree of the more educated parent was used in the analyses.
Statistical methods
Statistical analyses were performed using SPSS software, Version 21.0 (IBM, Armonk, NY, USA). We compared basic characteristics between boys and girls using the Student´s t-test, the Mann-Whitney´s U-test, and the Chi Square-test. We examined the associations of body fat percentage and the measures of physical activity with the measures of neuromuscular performance using linear regression analyses adjusted for age and sex. The data on the associations of body fat percentage with neuromuscular performance were also adjusted for physical activity and the data of the relationships of physical activity to neuromuscular performance were adjusted for body fat percentage. Data on the associations of objectively measured MVPA with the measures of neuromuscular performance were additionally adjusted for wear time on week days and weekend days.
The combined associations of body fat percentage and objectively measured MVPA with the measures of neuromuscular performance were analysed by dichotomizing body fat percentage and MVPA at the sex-specific medians and by comparing the measures of neuromuscular performance in the four groups using General Linear Models (GLM) adjusted for age and sex. We used GLM to study whether there was an interaction between body fat percentage and physical activity on neuromuscular performance.
We estimated the effect sizes (R2 for linear regression and eta squared (η2) for the GLM analyses). We defined small, medium, and large effect sizes for R2 as 0.02, 0.15, and 0.35 and for η2 as 0.01, 0.09, and 0.25, respectively, according to Cohen (1992) and Miles & Shevlin (2005). Given that maturity may have an effect on the associations of adiposity and physical activity with neuromuscular performance, we performed all analyses also without children who had entered clinical puberty.
Results
Characteristics of children
Boys were more physically active, had lower body fat mass, lower body fat percentage, faster 50-metre shuttle run, faster 15-metre sprint test time, higher absolute pressing power in the hand grip strength test, longer jump in the standing long jump test, more errors in the modified flamingo balance test, fewer cubes moved in the box and block test, and shorter distance reached in the sit-and-reach test than girls (Table 1).
Table 1. Basic characteristics.
| All N=404 |
Boys N=200 |
Girls N=204 |
P-value | |
|---|---|---|---|---|
| Basic characteristics | ||||
| Age (years) | 7.6 (0.4) | 7.6 (0.4) | 7.6 (0.4) | 0.339 |
| Pubertal status (%) | ||||
| Prepubertal | 98.0 | 99.0 | 97.0 | 0.161 |
| Pubertal | 2.0 | 1.0 | 3.0 | |
| Parental education | 0.025 | |||
| Vocational school or less (%) | 20.8 | 21.1 | 18.9 | |
| Polytechic | 46.1 | 39.7 | 52.7 | |
| University | 33.1 | 39.2 | 28.4 | |
| Household income (%) | 0.390 | |||
| ≤ 30 000 € | 22.2 | 20.4 | 22.6 | |
| 30 001 – 60 000€ | 42.5 | 40.3 | 44.7 | |
| > 60 000 € | 35.3 | 39.3 | 32.7 | |
| Physical activity | ||||
| Objectively assessed moderate-to-vigorous physical activity (min/d)1 | 89.9 (49.6) | 103.2 (52.0) | 78.1 (44.2) | <0.001 |
| Unsupervised physical activity (min/wk)2 | 343.6 (220.0) | 371.0 (220.7) | 316.7 (216.4) | 0.013 |
| Organised sports (min/wk)2 | 52.7 (71.8) | 60.3 (79.5) | 45.3 (62.6) | 0.036 |
| Supervised exercise other than sports (min/wk)2 | 43.3 (70.0) | 52.2 85.3) | 34.6 (48.5) | 0.011 |
| Physical activity during recess (min/wk)2 | 111.3 (29.1) | 116.1 (28.3) | 106.9 (27.3) | 0.002 |
| Physically active school transportation (min/wk)2 | 17.6 (16.0) | 17.0 (15.6) | 18.2 (16.5) | 0.469 |
| Body size and composition | ||||
| Body height (cm) | 128.8 (5.7) | 129.6 (5.6) | 128.1 (5.6) | 0.006 |
| Body weight (kg) | 27.0 (5.1) | 27.3 (5.1) | 26.7 (5.1) | 0.119 |
| Prevalence of overweight and obesity (%) | 12.9 | 11.0 | 14.7 | 0.266 |
| Body fat mass (kg) | 5.8 (3.6) | 5.2 (3.6) | 6.4 (3.6) | <0.001 |
| Body fat percentage3 | 20.0 (8.4) | 17.4 (8.1) | 22.6 (7.9) | <0.0014 |
| Neuromuscular performance | ||||
| Time in 50-metre shuttle run test (s) | 24.1 (2.2) | 23.8 (2.2) | 24.4 (2.1) | 0.003 |
| Time in 15-metre sprint test (s) | 3.1 (0.2) | 3.1 (0.2) | 3.2 (0.2) | <0.001 |
| Pressing power in hand grip strength test (kilopascals) | 47.0 (8.3) | 48.7 (8.1) | 45.2 (8.1) | <0.001 |
| Distance jumped in standing long jump test (cm) | 125 (16.5) | 129.6 (15.86 | 120.7 (16.0) | <0.001 |
| Number of repetitions in sit-up test in 30 seconds | 11.0 (6.0) | 10.7 (4.9) | 10.5 (4.8) | 0.855 |
| Number of errors in modified flamingo balance test in 30 seconds3 | 3.0 (3.0) | 4.0 (4.0) | 3.0 (4.0) | <0.0014 |
| Cubes moved in box and block test in two minutes | 101.2 (13.2) | 99.1 (12.8) | 104.5 (13.0) | <0.001 |
| Distance reached in sit-and-reach test (cm) | -3.1 (7.8) | -5.9 (7.2) | 0.42 (7.3) | <0.001 |
Physical activity assessed objectively by combined movement and heart rate monitoring defined as time spent ≥3 metabolic equivalents (METs), N=343.
Different types of physical activity assessed by questionnaire.
Median (interquartile range).
Mann-Whitney U-test. The prevalence of overweight and obesity was determined based on International Obesity Task Force reference values (Cole et al., 2000).
Independent associations of body fat percentage and physical activity with neuromuscular performance
Higher body fat percentage was related to slower 50-metre shuttle run time (R2 change = 0.055) and 15-metre sprint run time (R2 change = 0.165, shorter standing long jump (R2 change = 0.166), lower number of sit-ups in the sit-up test (R2 change = 0.047), higher number of errors in the modified flamingo balance test (R2 change = 0.015), and fewer number of cubes moved in the box and block test (R2 change = 0.011) (Table 2). Higher levels of objectively measured MVPA were associated with faster 50-metre shuttle run time (R2 change = 0.023), 15-metre sprint time (R2 change = 0.046), and longer distance jumped in the standing long jump test (R2 change = 0.049). Higher levels of organised sports and unsupervised physical activity assessed by a questionnaire were associated with faster 50-metre shuttle run time (R2 change = 0.012 and 0.011, respectively) and faster 15-metre sprint time (R2 change = 0.014 and 0.017, respectively). Self-reported organised sports participation was also directly related to distance jumped in the standing long jump test (R2 change = 0.013). Physically active school transportation assessed by a questionnaire was inversely associated with the number of sit-ups in the sit-up test (R2 change = 0.011). These associations remained similar when the analyses were performed without children who had entered clinical puberty (data not shown).
Table 2. The associations of body fat percentage and physical activity with neuromuscular performance among 404 children aged 6–8 years.
| 50-metre shuttle run test time (s) | 15-metre sprint time (s) | Pressing power in the hand grip strength test (kPa) | Pressing power in the hand grip strength test adjusted for lean mass (kPa) | Distance jumped in standing long jump test (cm) | Sit-ups completed in 30 seconds | Errors in the flamingo balance test | Cubes moved in the box and block test | Distance reach in the Sit-and-reach test (cm) | |
|---|---|---|---|---|---|---|---|---|---|
| Body fat percentage | 0.236† | 0.402† | 0.136** | 0.007 | -0.417† | -0.253† | 0.119* | -0.112* | -0.070 |
| Objectively assessed moderate-to-vigorous physical activity1 | -0.162** | -0.228† | 0.090 | 0.004 | 0.235† | -0.008 | 0.019 | 0.053 | 0.041 |
| Unsupervised physical activity2 | -0.101* | -0.130** | 0.090 | 0.045 | 0.075 | -0.034 | 0.020 | 0.042 | 0.021 |
| Organised sports2 | -0.118* | -0.122** | 0.031 | -0.024 | 0.120** | 0.060 | -0.037 | 0.062 | 0.062 |
| Supervised exercise other than sport2 | 0.002 | 0.009 | 0.073 | 0.066 | 0.068 | 0.018 | 0.013 | 0.089 | 0.082 |
| Physical activity during recess2 | -0.024 | 0.039 | 0.025 | 0.044 | 0.016 | 0.013 | 0.021 | -0.078 | -0.035 |
| Physically active school transportation2 | 0.063 | 0.032 | 0.020 | -0.019 | 0.004 | -0.110* | -0.023 | -0.008 | -0.036 |
The data are standardized regression coefficients adjusted for age and sex from linear regression analyses.
Physical activity assessed objectively by combined movement and heart rate monitoring defined as time spent ≥3 metabolic equivalents (METs), N=343.
The components of physical activity were assessed using the PANIC Physical Activity Questionnaire.
*P<0.05; **P<0.01; †P<0.001
The association of objectively measured MVPA (β=−0.430 and P<0.001 for boys vs. β=−0.139 and P=0.063 for girls, P = 0.046 for interaction between sex and MVPA) and self-reported unsupervised physical activity (β=−0.352 and P<0.001 for boys vs. β=−0.086 and P=0.245 for girls, P = 0.016 for interaction between sex and unsupervised physical activity) with 15-metre sprint time was stronger in boys than in girls. Other associations between body fat percentage and physical activity with neuromuscular performance were similar in boys and girls.
Combined associations of body fat percentage and objectively assessed physical activity with neuromuscular performance
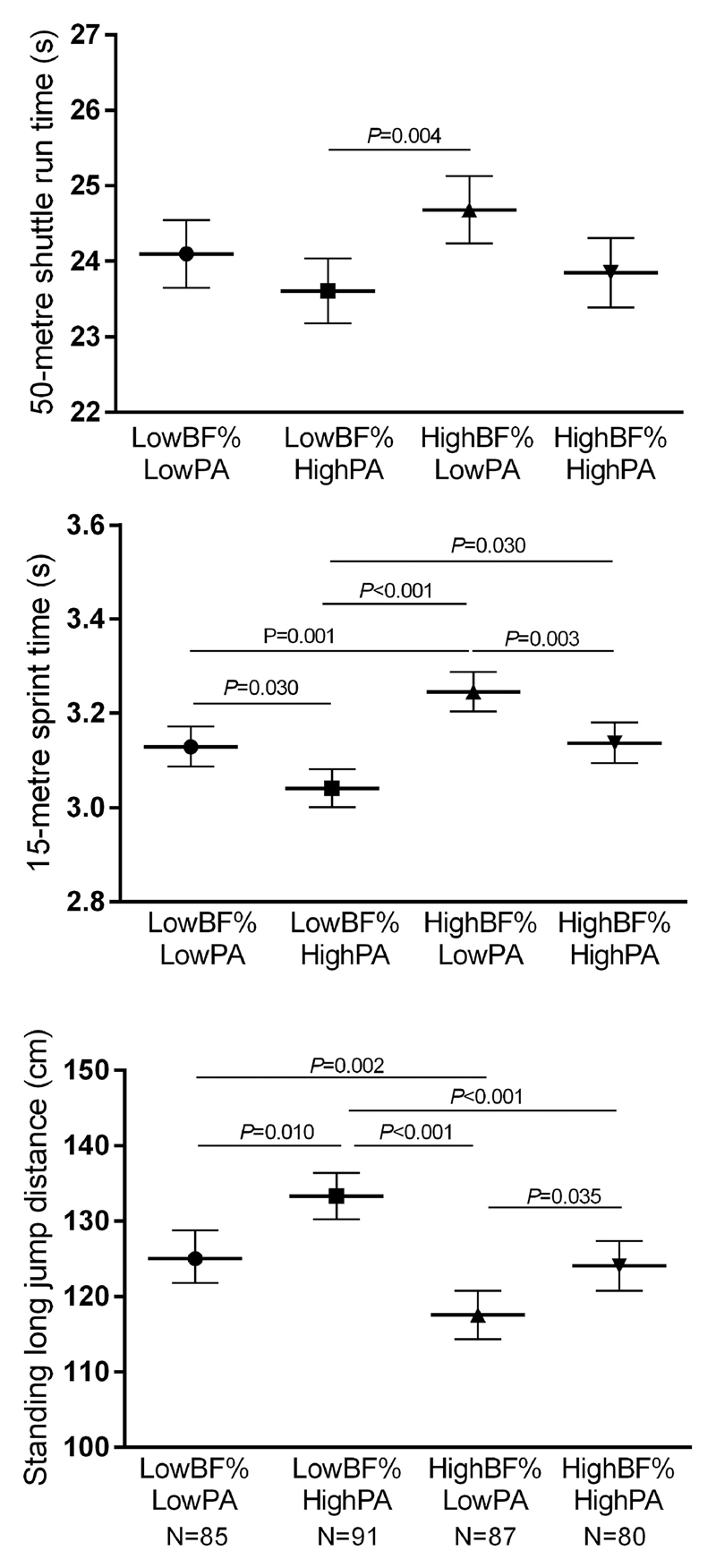
Overall, there were statistically significant differences in 50-metre shuttle run test time (F3,335 =4.241, P=0.006, η2=0.03), 15-metre sprint time (F3,335=15.909, P<0.001, η2=0.12), and distance jumped in standing long jump test (F3,335=16.407, P<0.001, η2=0.12) between the four groups in which body fat percentage and objectively assessed MVPA were dichotomized at sex-specific medians (Figure 1). Children who were below the sex-specific median of body fat percentage (<15% for boys, <21% for girls) and at or above the sex-specific median of MVPA (≥99 min/d for boys, ≥72 min/d for girls) had faster 50-metre shuttle run time than children with higher body fat percentage and lower levels of MVPA (Figure 1). Children with lower body fat percentage and higher levels of MVPA had faster 15-metre sprint time and longer standing long jump than other children. Moreover, children with higher body fat percentage and higher levels of MVPA were faster in the 15-metre sprint test and had longer standing long jump than children with higher body fat percentage and lower levels of MVPA. There was no statistically significant interaction between body fat percentage and MVPA on 50-metre shuttle run time, 15-metre sprint run time, distance jumped in the standing long jump test, pressing power in the hand grip strength, number of sit-ups, errors in the modified flamingo balance test, or distance reach in the sit-and-reach test (P >0.100 for interactions).
Figure 1.
Estimated marginal means and their 95% confidence intervals for measures of neuromuscular performance among children in combined groups of lower and higher levels of body fat percentage (BF%, sex-specific median of 15% for boys and 21% for girls as cut-off) and objectively assessed moderate-to-vigorous physical activity (PA, sex-specific median of 99 min for boys and 72 min for girls as cut-off) adjusted for age and sex.
Higher levels of MVPA were associated with higher number of cubes moved in the box and block test among children with higher body fat percentage (mean 100.2 vs. mean 104.3, P=0.033) but not among children with lower body fat percentage (P = 0.015 for interaction).
Discussion
We performed one of the first studies on the combined associations of adiposity and physical activity with neuromuscular performance in children. We found in a population sample of children 6–8 years of age, that children who had higher body fat percentage and lower levels of MVPA had poorer neuromuscular performance in running and jumping tests than leaner and more physically active children. We also observed that children who had a higher body fat content and higher levels of MVPA outperformed children who were more overweight and less active in 15-metre sprint and standing long jump test.
Children aged 6–8 years with a combination of higher body fat percentage and lower levels of physical activity have been found to have poorer overall neuromuscular performance, assessed by the Koordinations Test für Kinder (KTK) and throwing accuracy tests, than other children (Morris et al., 2012). These results support our observation that children who had higher body fat percentage and lower levels of physical activity had poorer neuromuscular performance than leaner and more physically active children. However, Morris and co-workers (2012) also found that low levels of physical activity were associated with worse neuromuscular performance only in children with a higher body fat percentage. This observation contradicts our finding that body fat percentage did not modify the associations of physical activity with performance in the 50-metre shuttle run, 15-metre sprint, and standing long jump tests. Nevertheless, higher levels of physical activity were related to better manual dexterity only in children with a higher body fat percentage. One explanation of these partly inconsistent findings is that manual dexterity assessed by the box and block test as well as tests included in the overall neuromuscular performance score computed from tests for dynamic balance and coordination skills in the study by Morris et al. (2012), require greater amounts of cognitive control than running and jumping tests (Roebers & Kauer, 2009). Obesity has been linked to a poorer cognitive control (Kamijo et al. 2014) whereas higher levels of physical activity have been associated with enhanced cognitive control in children (Hillman et al. 2014). Moreover, a perceptual-motor deficit has been hypothesised to cause the association between overweight and poor manual dexterity (D’Hondt, Deforche, De Bourdeaudhuij, & Lenoir, 2009; D’Hondt, Deforche, De Bourdeaudhuij, & Lenoir, 2008; Gentier et al., 2013). Therefore, it is possible that physical activity has positive effects on manual dexterity particularly in overweight children.
The results of previous studies that have mainly used BMI as a measure of adiposity support the present findings on weak to moderate associations of higher body fat percentage with a poorer neuromuscular performance in tests that are considered weight-bearing, such as the 50-metre shuttle run test, the 15-metre sprint test, and the standing long jump test (Castetbon & Andreyeva, 2012; Cliff et al., 2012; D Hondt, Deforche, De Bourdeaudhuij, & Lenoir, 2009; Slotte, Sääkslahti, Metsämuuronen, & Rintala, 2014). Children with overweight and obesity have also been observed to have poorer balance and manual dexterity than normal weight children (D’Hondt, Deforche, De Bourdeaudhuij, & Lenoir, 2008; Gentier et al., 2013; Niederer et al., 2012), although not all studies have found such differences (Deforche et al., 2009). Consistent with these results, we found that higher body fat percentage has a weak but statistically significant association with poorer static balance and manual dexterity in children. This observation suggests that increased body fat percentage is related to decreased neuromuscular performance in tests that require moving or bearing body weight but higher body fat percentage may also decrease performance in tasks that are not considered weight-bearing.
We found that higher levels of objectively measured MVPA were related to better neuromuscular performance particularly in tests requiring running and jumping, but the magnitude of the associations were rather small. Similarly, some previous studies have observed a direct association of objectively measured physical activity with running and jumping performance but not with balance skills or abdominal and upper body strength (Iivonen et al., 2013; Laukkanen et al., 2013; Ng et al., 2014). Moreover, we found that higher levels of participation in organized sports and unsupervised physical activity has weak associations with faster 50-metre shuttle run and 15-metre sprint times, and that sports participation was directly related to distance jumped in the standing long jump test. Although some evidence suggests that supervised exercise may lead to greater improvements in neuromuscular performance than unsupervised physical activity (Morgan et al., 2013), our results indicate that higher levels of habitual physical activity may improve 50-metre shuttle run, 15-metre sprint, and standing long jump performance in children. These results emphasise the potential of habitual unsupervised physical activity for improving neuromuscular performance in children.
The strengths of the present study include the population sample of boys and girls, the use of DXA that is the gold standard method for the assessment of adiposity, the opportunity to use both objective and self-reported measures of physical activity, and a number of valid measures of neuromuscular performance. The weaknesses of our study are the cross-sectional design which does not allow us to draw firm conclusions about the time order or causality of the relationships. Our study also lacks data on some important motor skills, such as throwing and kicking. The modified flamingo balance test is a relatively crude measure of static balance, so using more sophisticated and varied measures of balance skills would have provided more detailed understanding of the associations of adiposity and physical activity with these skills. In addition, although our results suggest that body fat percentage was more strongly associated with running and jumping performance than physical activity, these results should be interpreted cautiously because the method used for the assessment of body composition is more precise than that used for the assessment of physical activity.
Our study showed that higher body fat percentage, lower levels of MVPA, and particularly the combination of these two factors were associated with poorer neuromuscular performance in tests that required bearing body weight in children. Higher body fat percentage was also inversely related to worse static balance and manual dexterity in children. These findings emphasise preventing overweight and particularly increasing physical activity to prevent impaired neuromuscular performance among children. Longitudinal studies on the associations of different types of physical activity and adiposity with neuromuscular performance are warranted to further explore the complex relationships between these three factors.
Acknowledgement
We thank the children and their families who volunteered to participate in this study. We also thank Stefanie Hollidge (MRC Epidemiology Unit) for assistance in the objective physical activity data processing. This work was financially supported by grants from Ministry of Social Affairs and Health of Finland, Ministry of Education and Culture of Finland, University of Eastern Finland, Finnish Innovation Fund Sitra, Social Insurance Institution of Finland, Finnish Cultural Foundation, Juho Vainio Foundation, Foundation for Pediatric Research, Paulo Foundation, Paavo Nurmi Foundation, Diabetes Research Foundation, Kuopio University Hospital (EVO funding number 5031343), the Research Committee of the Kuopio University Hospital Catchment Area for the State Research Funding, City of Kuopio, and Päivikki and Sakari Sohlberg Foundation.
Footnotes
The authors declare no conflicts of interest.
References
- Artero EG, España-Romero V, Ortega FB, Jiménez-Pavón D, Ruiz JR, Vicente-Rodríguez G, et al. Castillo MJ. Health-related fitness in adolescents: underweight, and not only overweight, as an influencing factor. The AVENA study. Scandinavian Journal of Medicine and Science in Sports. 2010;20:418–27. doi: 10.1111/j.1600-0838.2009.00959.x. [DOI] [PubMed] [Google Scholar]
- Brage S, Brage N, Franks PW, Ekelund U, Wareham NJ. Reliability and validity of the combined heart rate and movement sensor Actiheart. European Journal of Clinical Nutrition. 2005;59:561–570. doi: 10.1038/sj.ejcn.1602118. [DOI] [PubMed] [Google Scholar]
- Brage S, Ekelund U, Brage N, Hennings MA, Froberg K, Franks PW, Wareham NJ. Hierarchy of individual calibration levels for heart rate and accelerometry to measure physical activity. Journal of Applied Physiology. 2007;103:682–692. doi: 10.1152/japplphysiol.00092.2006. [DOI] [PubMed] [Google Scholar]
- Castetbon K, Andreyeva T. Obesity and motor skills among 4 to 6-year-old children in the United States: nationally-representative surveys. BMC Pediatrics. 2012;12:28. doi: 10.1186/1471-2431-12-28. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cattuzzo MT, Henrique RDS, Ré AHN, Oliveira IS, De Melo BM, de Sousa Moura M, et al. Stodden D. Motor competence and health related physical fitness in youth: a systematic review. Journal of Science and Medicine in Sport. 2014 doi: 10.1016/j.jsams.2014.12.004. Advance online publication. [DOI] [PubMed] [Google Scholar]
- Cliff DP, Okely AD, Morgan PJ, Jones RA, Steele JR, Baur LA. Proficiency deficiency: mastery of fundamental movement skills and skill components in overweight and obese children. Obesity. 2012;20:1024–1033. doi: 10.1038/oby.2011.241. [DOI] [PubMed] [Google Scholar]
- Cohen K. A power primer. Psychological Bulletin. 1992;112:155–159. doi: 10.1037//0033-2909.112.1.155. [DOI] [PubMed] [Google Scholar]
- Cole T, Bellizzi M, Flegal K, Dietz W. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ. 2000;320:1240–1243. doi: 10.1136/bmj.320.7244.1240. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Collings PJ, Wijndaele K, Corder K, Westgate K, Ridgway CL, Sharp SJ, et al. Brage S. Magnitude and determinants of change in objectively-measured physical activity, sedentary time and sleep duration from ages 15 to 17.5y in UK adolescents: the ROOTS study. Int J Behav Nutr Phys Act. 2015;12:61. doi: 10.1186/s12966-015-0222-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- D´Hondt E, Deforche B, De Bourdeaudhuij I, Lenoir M. Relationship between motor skill and body mass index in 5- to 10-year-old children. Adapted Physical Activity Quarterly. 2009;26:21–37. doi: 10.1123/apaq.26.1.21. [DOI] [PubMed] [Google Scholar]
- D’Hondt E, Deforche B, De Bourdeaudhuij I, Lenoir M. Childhood obesity affects fine motor skill performance under different postural constraints. Neuroscience Letters. 2008;440:72–75. doi: 10.1016/j.neulet.2008.05.056. [DOI] [PubMed] [Google Scholar]
- Deforche BI, Hills AP, Worringham CJ, Davies PSW, Murphy AJ, Bouckaert JJ, De Bourdeaudhuij IM. Balance and postural skills in normal-weight and overweight prepubertal boys. International Journal of Pediatric Obesity. 2009;4:175–182. doi: 10.1080/17477160802468470. [DOI] [PubMed] [Google Scholar]
- Eloranta AM, Lindi V, Schwab U, Kiiskinen S, Venäläinen T, Lakka HM, et al. Lakka TA. Dietary factors associated with metabolic risk score in Finnish children aged 6-8 years: the PANIC Study. European Journal of Nutrition. 2014;53:1431–1439. doi: 10.1007/s00394-013-0646-z. [DOI] [PubMed] [Google Scholar]
- European Council. EUROFIT: handbook for the EUROFIT tests of physical fitness. Rome: Council of Europe; 1988. [Google Scholar]
- Fisher A, Reilly JJ, Kelly LA, Montgomery C, Williamson A, Paton JY, Grant S. Fundamental movement skills and habitual physical activity in young children. Medicine and Science in Sports and Exercise. 2005;37(6 d):684–688. doi: 10.1249/01.mss.0000159138.48107.7d. [DOI] [PubMed] [Google Scholar]
- Gentier I, D’Hondt E, Shultz S, Deforche B, Augustijn M, Hoorne S, et al. Lenoir M. Fine and gross motor skills differ between healthy-weight and obese children. Research in Developmental Disabilities. 2013;34(11):4043–4051. doi: 10.1016/j.ridd.2013.08.040. [DOI] [PubMed] [Google Scholar]
- Haapala EA, Poikkeus A-M, Kukkonen-Harjula K, Tompuri T, Lintu N, Väistö J, et al. Lakka TA. Associations of physical activity and sedentary behavior with academic skills – A follow-up study among primary school children. PloS One. 2014;10:e107031. doi: 10.1371/journal.pone.0107031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hardy L, King L, Espinel P, Cosgrove C, Bauman A. NSW Schools Physical Activity and Nutrition Survey (SPANS) 2010 Full report. Sydney: NSW Ministry of Health; 2010. [Google Scholar]
- Haug E, Rasmussen M, Samdal O, Iannotti R, Kelly C, et al. Vereecken C, The Health Behaviour in School-aged Children Obesity Working Group Overweight in school-aged children and its relationship with demographic and lifestyle factors: Results from the WHO-Collaborative Health Behaviour in School-aged Children (HBSC) Study. International Journal of Public Health. 2010;54:167–179. doi: 10.1007/s00038-009-5408-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hillman CH, Pontifex MB, Castelli DM, Khan NA, Raine LB, Scudder MR, et al. Kamijo K. Effects of the FITKids randomized controlled trial on executive control and brain function. Pediatrics. 2014;134:e1063–e1071. doi: 10.1542/peds.2013-3219. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Holfelder B, Schott N. Relationship of fundamental movement skills and physical activity in children and adolescents: A systematic review. Psychology of Sport Exercise. 2014;15:382–391. [Google Scholar]
- Iivonen KS, Sääkslahti AK, Mehtälä A, Villberg JJ, Tammelin TH, Kulmala JS, Poskiparta M. Relationship between fundamental motor skills and physical activity in 4-year-old preschool children. Perceptual and Motor Skills. 2013;117:627–646. doi: 10.2466/10.06.PMS.117x22z7. [DOI] [PubMed] [Google Scholar]
- Jiménez-Pavón D, Kelly J, Reilly JJ. Associations between objectively measured habitual physical activity and adiposity in children and adolescents: Systematic review. International Journal of Pediatric Obesity. 2010;5:3–18. doi: 10.3109/17477160903067601. [DOI] [PubMed] [Google Scholar]
- Jongbloed-Pereboom M, Nijhuis-van der Sanden MWG, Steenbergen B. Norm scores of the box and block test for children ages 3-10 years. American Journal of Occupational Therapy. 2013;67:312–318. doi: 10.5014/ajot.2013.006643. [DOI] [PubMed] [Google Scholar]
- Kamijo K, Pontifex MB, Khan NA, Raine LB, Scudder MR, Drollette ES, et al. Hillman CH. The negative association of childhood obesity to cognitive control of action monitoring. Cerebral Cortex. 2014;24:654–662. doi: 10.1093/cercor/bhs349. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Laukkanen A, Pesola A, Havu M, Sääkslahti A, Finni T. Relationship between habitual physical activity and gross motor skills is multifaceted in 5- to 8-year-old children. Scandinavian Journal of Medicine & Science in Sports. 2014;24(2):102–110. doi: 10.1111/sms.12116. [DOI] [PubMed] [Google Scholar]
- Lee IM, Shiroma EJ, Lobelo F, Puska P, Blair SN, Katzmarzyk PT, Lancet Physical Activity Series Working Group Effect of physical inactivity on major non-communicable diseases worldwide: an analysis of burden of disease and life expectancy. Lancet. 2012;380:219–229. doi: 10.1016/S0140-6736(12)61031-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lubans DR, Morgan PJ, Cliff DP, Barnett LM, Okely AD. Fundamental movement skills in children and adolescents: review of associated health benefits. Sports Medicine. 2010;40:1019–1035. doi: 10.2165/11536850-000000000-00000. [DOI] [PubMed] [Google Scholar]
- Malina RM, Beunen GP, Classens AL, Lefevre J, Vanden Eynde BV, Renson R, et al. Simons J. Fatness and physical fitness of girls 7 to 17 years. Obesity Research. 1995;3:221–231. doi: 10.1002/j.1550-8528.1995.tb00142.x. [DOI] [PubMed] [Google Scholar]
- Miles J, Shevlin M. Applying regression and correlation. A guide for students and researchers. London: Sage Publications ltd; 2005. [Google Scholar]
- Morgan PJ, Barnett LM, Cliff DP, Okely AD, Scott HA, Cohen KE, Lubans DR. Fundamental movement skill interventions in youth: a systematic review and meta-analysis. Pediatrics. 2013;132:e1361–1383. doi: 10.1542/peds.2013-1167. [DOI] [PubMed] [Google Scholar]
- Morrison KM, Bugge A, El-Naaman B, Eisenmann JC, Froberg K, et al. Andersen LB. Inter-relationships among physical activity, body fat, and motor performance in 6- to 8-year-old Danish children. Pediatric Exercise Science. 2012;24:199–209. doi: 10.1123/pes.24.2.199. [DOI] [PubMed] [Google Scholar]
- Ng M, Fleming T, Robinson M, Thomson B, Graetz N, Margono C, et al. Gakidou E. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet. 2014;384(9945):766–781. doi: 10.1016/S0140-6736(14)60460-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Niederer I, Kriemler S, Zahner L, Bürgi F, Ebenegger V, Marques-Vidal P, Puder JJ. BMI group-related differences in physical fitness and physical activity in preschool-age children: a cross-sectional analysis. Research Quarterly for Exercise and Sport. 2012;83:12–19. doi: 10.1080/02701367.2012.10599820. [DOI] [PubMed] [Google Scholar]
- Okely AD, Booth ML, Patterson JW. Relationship of physical activity to fundamental movement skills among adolescents. Medicine and Science in Sports and Exercise. 2001;33:1899–1904. doi: 10.1097/00005768-200111000-00015. [DOI] [PubMed] [Google Scholar]
- Olesen L, Kristensen P, Ried-Larsen M, Grøntved A, Froberg K. Physical activity and motor skills in children attending 43 preschools: a cross-sectional study. BMC Pediatrics. 2014;14:229. doi: 10.1186/1471-2431-14-229. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rauner A, Mess F, Woll A. The relationship between physical activity, physical fitness and overweight in adolescents: a systematic review of studies published in or after 2000. BMC Pediatrics. 2013;13:19. doi: 10.1186/1471-2431-13-19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Robinson LE, Stodden DF, Barnett LM, Lopes VP, Logan SW, et al. D’Hondt E. Motor competence and its effect on positive developmental trajectories of health. Sports Medicine. 2015;45:1273–1284. doi: 10.1007/s40279-015-0351-6. [DOI] [PubMed] [Google Scholar]
- Rodriques LP, Stodden DF, Lopes VP. Developmental pathways of change in fitness and motor competence are related to overweight and obesity status at the end of primary school. Journal of Science and Medicine in Sport. 2015;2015 doi: 10.1016/j.jsams.2015.01.002. in press. [DOI] [PubMed] [Google Scholar]
- Roebers C, Kauer M. Motor and cognitive control in a normative sample of 7-year-olds. Developmental Science. 2009;12:175–181. doi: 10.1111/j.1467-7687.2008.00755.x. [DOI] [PubMed] [Google Scholar]
- Runhaar J, Collard DCM, Singh AS, Kemper HCG, van Mechelen W, Chinapaw M. Motor fitness in Dutch youth: differences over a 26-year period (1980-2006) Journal of Science and Medicine in Sport. 2010;13:323–328. doi: 10.1016/j.jsams.2009.04.006. [DOI] [PubMed] [Google Scholar]
- Saari A, Sankilampi U, Hannila M-L, Kiviniemi V, Kesseli K, Dunkel L. New Finnish growth references for children and adolescents aged 0 to 20 years: Length/height-for-age, weight-for-length/height, and body mass index-for-age. Annals of Medicine. 2011;43:235–48. doi: 10.3109/07853890.2010.515603. [DOI] [PubMed] [Google Scholar]
- Shumway-Cook A, Woollacott M. Motor Control. Theory and Practical Applications. Philadelphia: Lippincott-Williams, & Wilkins; 1995. [Google Scholar]
- Slotte S, Sääkslahti A, Metsämuuronen J, Rintala P. Fundamental movement skill proficiency and body composition measured by dual energy X-ray absorptiometry in eight-year-old children. Early Child Development and Care. 2014;185:475–485. [Google Scholar]
- Smith JJ, Eather N, Morgan PJ, Plotnikoff RC, Faigenbaum AD, Lubans DR. The health benefits of muscular fitness for children and adolescents: A systematic review and meta-analysis. Sports Medicine. 2014;44:1209–1223. doi: 10.1007/s40279-014-0196-4. [DOI] [PubMed] [Google Scholar]
- Stegle O, Fallert S, DJC M, Brage S. Gaussian process robust regression for noisy heart rate data. IEEE Transactions on Biomedical Engineering. 2008;55:2143–2151. doi: 10.1109/TBME.2008.923118. [DOI] [PubMed] [Google Scholar]
- Tanner J. Growth at adolescence. Oxford: Blackwell; 1962. [Google Scholar]
- Tompuri TT, Lakka TA, Hakulinen M, Lindi V, Laaksonen DE, Kilpeläinen TO, et al. Laitinen T. Assessment of body composition by dual-energy X-ray absorptiometry, bioimpedance analysis and anthropometrics in children: the Physical Activity and Nutrition in Children study. Clinical Physiology and Functional Imaging. 2015;35:21–33. doi: 10.1111/cpf.12118. [DOI] [PubMed] [Google Scholar]
- Williams HG, Pfeiffer Ka, O’Neill JR, Dowda M, McIver KL, Brown WH, Pate RR. Motor skill performance and physical activity in preschool children. Obesity. 2008;16:1421–1426. doi: 10.1038/oby.2008.214. [DOI] [PubMed] [Google Scholar]
- Väistö J, Eloranta A-M, Viitasalo A, Tompuri T, Lintu N, Karjalainen P, et al. Lakka TA. Physical activity and sedentary behaviour in relation to cardiometabolic risk in children: cross-sectional findings from the Physical Activity and Nutrition in Children (PANIC) Study. International Journal of Behavioral Nutrition and Physical Activity. 2014;11:55. doi: 10.1186/1479-5868-11-55. [DOI] [PMC free article] [PubMed] [Google Scholar]