Abstract
Due to the increased interest in their application in the treatment of infectious diseases, boron-containing compounds have received a significant coverage in the literature. Herein, a small set of novel cinnamoly-oxaborole amides were synthesized and screened against nagana Trypanosoma brucei brucei for antitrypanosomal activity. Compound 5g emerged as a new hit with an in vitro IC50 value of 0.086 μM against T. b. brucei without obvious inhibitory activity against HeLa cell lines. The same series was also screened against other human pathogens, including Mycobacterium tuberculosis, the causative agent of tuberculosis (TB), for which moderate to weak activity (10 to >125 μM) was observed. Similarly, these compounds exhibited moderate activity against the human protozoal pathogen Trichomonas vaginalis with no observed effect on common microbiome bacterial species. The cross-species inhibitory activity presents the possibility of these compounds serving as broad-spectrum antibiotics for these prevalent three human pathogens.
Keywords: benzoxaboroles, cinnamic acids, trichomoniasis, trypanosomiasis, Mycobacterium tuberculosis
1. Introduction
Globally, the major tropical infections malaria, tuberculosis (TB), trypanosomiasis, and leishmaniasis remain a serious public health concern. Collectively, these infectious diseases are responsible for more than 2.2 million deaths in developing countries annually [1]. Despite it being a preventable infectious disease, in 2015, approximately 1.8 million people died from TB infection [2]. A complete eradication of TB remains an incomplete task since drugs to treat these diseases are facing several limitations including reduced efficacy, poor safety, and affordability [3]. A further complication is the emergence of multidrug resistant Mycobacterium tuberculosis against clinically proven drugs, which has made the development of new therapies a demanding task for effective management and control of TB. Additionally, TB is considered a primary killer in HIV-positive individuals, and the World Health Organization (WHO) reported that people living with HIV are at higher risk of developing TB compared to healthy individuals [2]. In recent years, there have been reports of an overlap of endemic regions between TB and parasitic diseases, which may result in co-infections of these diseases in the affected population [4].
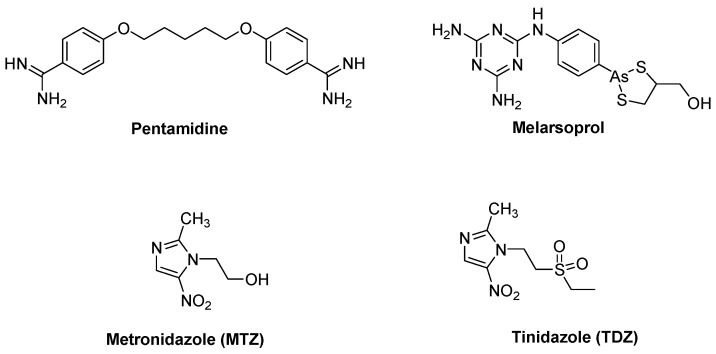
Human African trypanosomiasis (HAT), commonly referred to as a sleeping sickness [5], is a fatal and debilitating disease which is included in the list of 17 neglected tropical diseases (NTDs) prioritized by WHO [6,7,8]. Approximately 70 million people mainly residing in the remote areas of sub-Saharan Africa are at risk of contracting the disease [9,10]. Human African trypanosomiasis is caused by Trypanosoma brucei sub-species, namely T. b. rhodesiense and T. b. gambiense [11,12]. It is spread from one person to another via the bite of an infected tsetse fly [13]. Although the causal agents of HAT have been known for over a century, only four drugs, pentamidine, melarsoprol (Figure 1), suramin, and eflornithine, are registered for the treatment of this disease [14]. These long-discovered drugs have very poor oral bioavailability; as such, they are only administered intravenously, which is expensive [15] and requires expertise and facilities that are inaccessible in disease stricken rural areas [16], hampering treatment implementation [17]. In addition, these drugs also have serious side effects [18] including nephrotoxicity, hypertension, anemia, and neuropathy [19]. Moreover, there are growing concerns over the development of the drug-resistant infections against these drugs [20].
Figure 1.
Chemical structures of drugs for treatment of sleeping sickness and trichomoniasis.
Similarly, individuals affected by parasitic diseases and bacterial infections are also exposed to sexually transmitted diseases [3]. Each year >340 million new cases of sexually transmitted bacterial and protozoal infections (STIs) occur globally [21,22]. Included in the list of STIs is human trichomoniasis, a non-viral disease that is caused by Trichomonas vaginalis. Contrary to infections such as chlamydia, gonorrhea, and syphilis, trichomoniasis receives less attention in terms of control efforts despite it being the most common disease of all [23]. Problems associated with trichomoniasis include premature rupture of membranes during pregnancy, premature birth, low birth weight, and enhancing the acquisition of HIV [24], an infectious virus posing a major threat especially in Africa. Nitroimidazoles, metronidazole, and tinidazole (Figure 1), are preferred drugs for treatment of T. vaginalis infections [25]. With the emerging resistance of T. vaginalis against metronidazole, there is no well-established alternative therapy available.
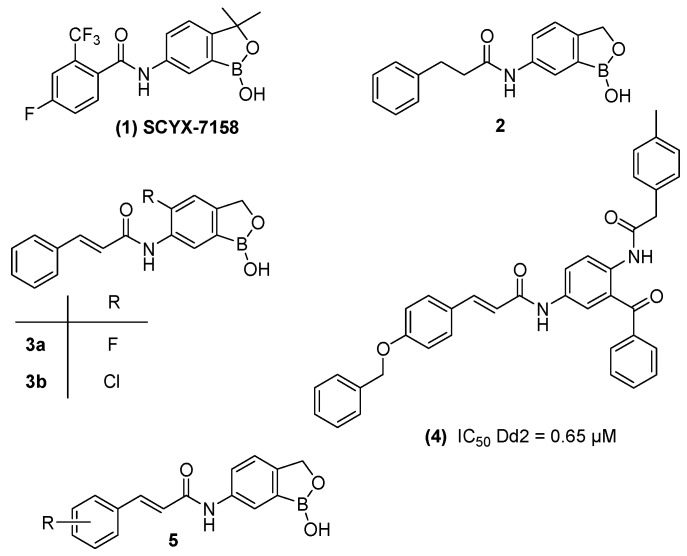
Considering their attractive therapeutic and biological profile, in recent years, boron-containing compounds have received significant attention and are featuring prominently in literature [5,26,27,28,29,30,31,32,33]. Typical examples of these compounds are benzoxaboroles, which are cyclic boronic acids with robust stability under elevated acidic and basic conditions. Initially discovered by Torssell in 1957 [34], benzoxaboroles have been hailed as potent anti-infective agents [26,27,28,29] that are non-toxic and possess desirable chemical properties as well as pharmacokinetic properties [31]. Recent endeavors aimed at discovering novel trypanocidal agents have culminated in new chemical entities (NCEs) entering clinical trials [35], one of which is SCYX-7158 (1)—a benzoxaborole-based compound [36] (Figure 2). Due to high attrition rates during clinical development of NCEs [37], it is imperative to replete the trypanocidal drug development pipeline with numerous and structurally diverse benzoxaborole-based leads. Typical examples of other promising novel benzoxaborole-containing compounds include compound 2 (Figure 2), which showed excellent trypanocidal activity with in vitro IC50 value of 0.14 μg/mL against T. b. brucei S427 [38]. Furthermore, compounds 3a and 3b (Figure 2) are two examples of cinnamic acid-based benzoxaborole derivatives, which have been studied as antifungal agents [39].
Figure 2.
Chemical structures of antifungal, antiplasmodial, and trypanocidal benzoxaboroles including the proposed cinnamoyl-oxaborole amides (5).
More importantly, cinnamic acids are a class of compounds, which have received considerable attention as promising anti-infective agents [40]. Several studies have shown that cinnamic acid and their corresponding phenolic derivatives exhibit a broad spectrum of biological activities including antiproliferative, antioxidant, antiviral, antimicrobial, antimalarial, and anti-cardiovascular activities [40,41,42]. For example, Wiesner and co-workers [43] reported the antimalarial activity of 2,5-bisacylaminobenzonephone (Figure 2, Compound 4) obtained by replacing a 3-phenylpropanamide unit with 3-phenylprop-2-enamide unit. This prompted us to explore the biological activity of compounds containing the-prop-2-enamide unit coupled with 6-aminobenzoxaborole, which is an appealing scaffold with antiprotozoal properties. Except the cinnamic acid-based benzoxaborole derivatives (Figure 2, Compounds 3a and 3b), there is no previous literature report on this class of compounds as potential antiprotozoal agents. Hence, herein we wish to report on the synthesis and in vitro biological evaluation of novel cinnamoyl-oxaborole amides (Figure 2, Compound 5).
2. Results and Discussion
2.1. Chemistry
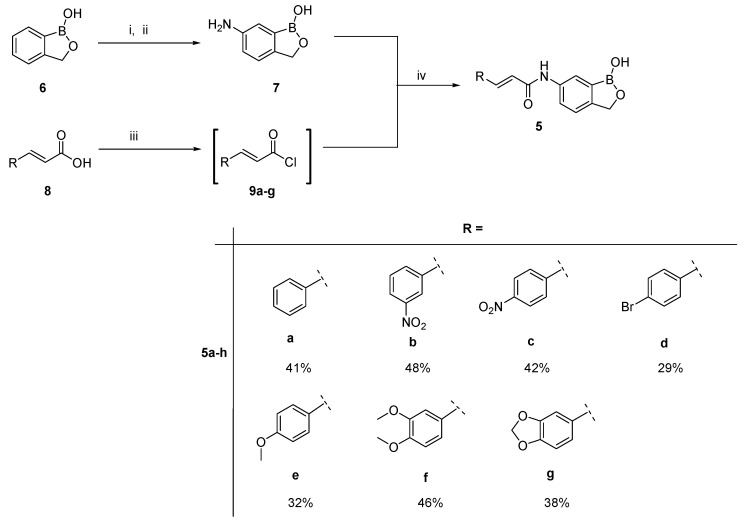
The synthesis of all intermediates and target compounds is presented in Scheme 1 below. Briefly, the commercially accessible benzoxaborole 6 was treated with nitric acid at −30 to −40 °C to form 6-nitrobenzoxaborole intermediate, and subsequently reduced to form 6-aminobenzoxaborole 7 under hydrogen atmosphere using palladium on carbon catalyst [44]. With the 6-aminobenzoxaborole 7 in hand, we turned our attention to the activation of cinnamic acids 8 for coupling with 7 to form the desired target cinnamoly-oxaborole amides 5a–g. Initially, we tried in situ activation of the carboxylic acid group of cinnamic acids for amidation using different coupling agents such as CDI, EDCI, HOBt, HOSu [45], and upon addition of 6-aminobenzoxaborole 7 these coupling agents all gave traces of desired products. We then opted for the conversion of cinnamic acids to their more reactive cinnamoyl chloride derivatives [46]. The common method of converting carboxylic acids to acyl chlorides, which makes use of SOCl2 [47] was attempted, and upon coupling with 6-aminobenzoxaborole 7, the reaction gave poor yields, and in some cases the desired products could not be isolated.
Scheme 1.
Synthesis of cinnamoyl˗benzoxaborole amides 5a–g. Reagents and conditions: (i) 99% HNO3, −30 °C, 3 h; (ii) H2, Pd/C, r.t, 2 h; (iii) DCM, Et3N, POCl3 and then (iv) DMAP.
We then adopted an alternative method using POCl3 in the presence of Et3N, an organic base. The presence of an organic base to maintain a basic environment has been reported to be important for acylation reactions of this type [48]. Thus, cinnamic acids 8 were treated with phosphoryl chloride under nitrogen atmosphere to form in situ the corresponding cinnamoyl chloride intermediates 9a–g. 6-Aminobenzoxaborole 7 was then acylated with the intermediates 9a–g to form targeted compounds 5a–g in 29 to 46% yields.
The synthesized cinnamoyl-oxaboroles (Scheme 1, 5a–g) were characterized using 1H and 13C nuclear magnetic resonance (NMR) as well as high resolution mass spectrometry (HRMS). The 1H-NMR spectra of all compounds showed a signal at δ ca 10.27 ppm assigned to B-OH. The peak at δ ca 9.24 ppm is assigned to -NH of the amide bond. Two doublets (J = 15.0 and 15.6 Hz) at δ ca 6.87 and 7.60 ppm are attributed to the two -CH of prop-2-enamide. These coupling constants are consistent with a trans geometry at the double bond. The signal at δ ca 4.96 ppm is assigned to the oxaborole -CH2. The 13C-NMR spectra of all compounds confirmed the skeletal structures consistent with proposed compounds 5a–g. The non-appearance of the carbon adjacent to the boron atom was noted, which is a common trend in benzoxaborole-containing compounds [49]. Analysis of the HRMS revealed molecular ion peaks agreeing with overall molecular structures of achieved compounds. The purity of all compounds was determined to be greater than 96% using qualitative high performance liquid chromatography (HPLC) (reversed phase).
2.2. Pharmacology
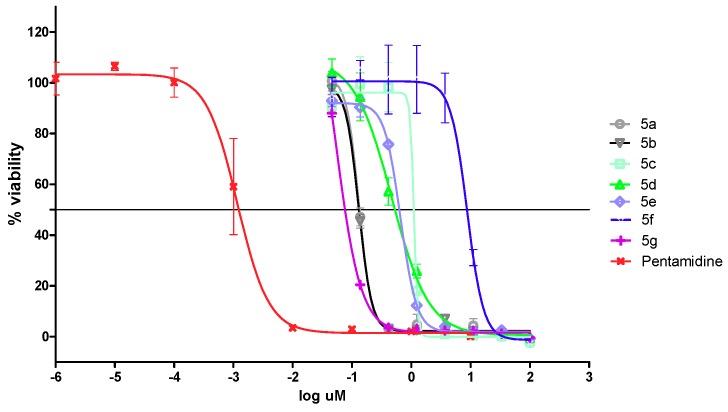
All target compounds were screened for in vitro inhibitory activity against the 427 strain of T. b. brucei, the T. vaginalis parasite, and M. tuberculosis H37Rv. The cytotoxicity of all compounds was assessed against human cervix adenocarcinoma (HeLa) cell line and emetine was used as a control. At a 20 μM concentration of each compound, none of the compounds showed any toxic effects to the HeLa cell line, and >80% cell viability was maintained during a 48 h exposure to the compounds (Table 1. At this concentration, all tested compounds exhibited greater than 90% growth inhibition of trypanosome parasites. Based on the single concentration screening data, the IC50 values were determined for compound 5a–g; the results are summarized in Figure 3 and Table 2. The cinnamoly-oxaborole amides showed promising antitrypanosomal activity with IC50 values in the low micromolar to sub-micromolar range. Despite being slightly less active compared to compounds 1 and 2, compounds 5a–e showed good activity with IC50 values below 1 μM and compound 5g emerged as the most active compound with IC50 value of 0.086 μM against the T. b. brucei parasite. Pentamidine was used as a positive control antitrypanosomal drug (IC50 = 1.2 nM).
Table 1.
In vitro antimycobacterial, antitrichomonas, and cytotoxicity activities of cinnamic acid-benzoxaborole hybrids.
| Compound | IC50 (μM) | MIC99 (μM) | %Viability |
|---|---|---|---|
| T. vaginalis | H37Rv | HeLa Cells | |
| 5a | 15.3 ± 0.33 | 61.8 | 108.5 ± 5.35 |
| 5b | 41.7 ± 0.23 | 107 | 87.0 ± 1.59 |
| 5c | 10.2 ± 0.56 | 26.5 | 94.3 ± 28.8 |
| 5d | 12.6 ± 0.28 | 10.7 | 89.9 ± 5.12 |
| 5e | 11.7 ± 0.28 | 18.7 | 102.5 ± 2.34 |
| 5f | ˃50 | ˃125 | 109.9 ± 0.84 |
| 5g | 22.8 ± 1.02 | 40.7 | 131.5 ± 26.6 |
| EM | - | - | 3.195 |
| ME | 0.53 | - | - |
| RE | - | 0.003 | - |
EM = emetine, ME = metronidazole, RE = rifampicin.
Figure 3.
Percentage viability of the T. b. brucei parasites determined at different compound concentrations and corresponding IC50 values of compounds 5a–g.
Table 2.
In vitro antitrypanosomal activities of cinnamic acid-benzoxaborole hybrids.
| Compound | IC50 (μM) |
|---|---|
| 1 | 0.292 ± 0.019 a |
| 2 | 0.14 b |
| 5a | 0.13 ± 0.02 |
| 5b | 0.13 ± 0.01 |
| 5c | 0.92 ± 0.04 |
| 5d | 0.47 ± 0.04 |
| 5e | 0.66 ± 0.03 |
| 5f | 8.71 ± 0.65 |
| 5g | 0.086 ± 0.002 |
| PE | 0.0012 ± 0.0001 |
a IC50 in μg/mL from reference 33, b IC50 in μg/mL from reference 38, PE = pentamidine.
Consistent with other studies [43,50,51,52,53,54] our data seem to suggest that linking of the cinnamoyl framework with bioactive scaffolds lead to compounds showing superior activity. The more active compounds also displayed excellent selectivity for the trypanosomal parasites over the human HeLa cell line. Thus far, the preliminary structure-activity relationship (SAR) suggested that mono-substituted aryl moieties are preferred for activity. More importantly, bicyclic aryl frameworks as observed for compound 5g emerged as promising ring systems, which are worth further exploration.
Interestingly, inhibitory activity profiles for both mycobacteria and trichomonad parasites revealed similar SAR, suggesting that the cellular targets of these compounds may be similar, even though mycobacteria are prokaryotic and trichomonads are eukaryotic pathogens. Also, given that trichomonad parasites co-exist with a mucosal microbiome, screening of these compounds showed no detectable effects on normal flora bacterial growth in vitro. Taken together, these compounds may present a new scaffold for drug discovery against human trypanosomiasis, tuberculosis, and human trichomoniasis.
Target compounds 5a–g were also evaluated for antimycobacterial activity in vitro. To this end, the compounds were screened in a broth microdilution assay against Mycobacterium tuberculosis H37Rv (Mtb) using rifampicin as a standard. The antimycobacterial activities are reported as minimum inhibitory concentration (MIC99) required to inhibit mycobacterial growth by 99%. Antimycobacterial activities are incorporated in Table 1. More than 50% of the compounds exhibited antimycobacterial activities, although these were moderate with respect to activity of the standard, rifampicin (MIC99 0.003 μM). Starting from compound 5a (MIC99 61.8 μM), di-substitution of the aryl moiety resulted in the loss of activity (e.g., 5f, MIC99 ˃ 50 μM), while mono-substitution enhances activity (e.g., 5e, MIC99 18.7 μM). The para-substituted aryl analogues showed the best activities (5d, MIC99 10.7 μM).
3. Materials and Methods
3.1. General Information
All chemicals and solvents used were purchased from Sigma-Aldrich (Pty) Ltd (Johannesburg, South Africa) and Merck (Pty) Ltd (Johannesburg, South Africa) and were used without further purification. Reactions were monitored by analytical thin layer chromatography (TLC) using Merck F254 silica gel plates (Merck, Johannesburg, South Africa) supported on aluminum sheets and the plates were visualized under ultraviolet (UV 254 and 366 nm) light and in iodine flasks. Where necessary, the crude compounds were purified by a silica gel column chromatography using Merck Kieselgel 60 Å:70–230 (0.068–0.2 mm) silica gel mesh (Merck, Johannesburg, South Africa). The 1H and 13C-NMR spectra were recorded on Bruker Biospin 300, 400 or 600 MHz spectrometers, and were referenced internally using residual solvent signals of deuterated DMSO-d6: 2.50 ppm for 1H and 39.5 ppm for 13C-NMR, or deuterated chloroform CDCl3: 7.26 ppm for 1H and 77.2 ppm for 13C-NMR at ambient temperature. The high-resolution mass spectrometric data (HRS-MS) of the final compounds was recorded on Waters Synapt G2 Mass Spectrometer (Stellenbosch University, Stellenbosch, South Africa) using electron impact (EI) ionization in the positive ionization mode. The starting 6-aminobenzoxaborole 7 was synthesized from the commercial 6-nirobenzoxaborole 6 (see Supplementary Materials) as previously described in the literature [31,55]. Purity was determined by HPLC (Agilent, Santa Clara, CA, USA), and all compounds were confirmed to have a purity of >95%. The chromatographic system consisted of an Agilent HP1100 LC-MSD (Agilent, Santa Clara, CA, USA) and equipped with a quaternary pump, in-line degasser, DAD detector, 1100 MSD and ChemStation for collection and analysis of data. A ZORBAX Elipse Plus C18 4.6 i.d. × 150 mm × 5 μm column was used for reversed-phase HPLC analysis. A mobile phase consisting of a mixture of aqueous solution of monobasic sodium phosphate 0.01 M and acetonitrile (90:10) on isocratic elution mode was used. Five different concentrations (5–500 μg/mL) of samples to be analyzed were made, filtered using 0.45 μm Millipore filters before their injection.
3.2. General Synthetic Procedure for the Cinnamic Acid-Benzoxaborole Hybrids, 5a–g
A mixture of cinnamic acids 2 (0.5 mmol) and Et3N (1.2 mmol) in anhydrous CH2Cl2 (1.5 mL) under N2 atmosphere was stirred at 0 °C for 5 min, then POCl3 (0.5 mmol) in anhydrous CH2Cl2 (1 mL) was added and the resulting mixture allowed to stir at room temperature for 30 min. When the acids were completely consumed (TLC), a solution of DMAP (0.15 mmol) and 6-aminobenzo[c] [1,2]oxaborol-1(3H)-ol (0.6 mmol) in anhydrous CH2Cl2 (0.5 mL) was added dropwise and the mixture stirred overnight at room temperature. Upon completion, the reaction mixture was washed sequentially with ice-cold water (10 mL), 10% aqueous HCl (10 mL), saturated aqueous NaHCO3 solution (10 mL), brine, and dried over anhydrous MgSO4. The solvent was removed in vacuo to give a solid residue, which was purified by flash column chromatography to afford the pure products, 5a–g.
(E)-N-(1-Hydroxy-1,3-dihydrobenzo[c][1,2]oxaborol-6-yl)cinnamamide (5a). Off white solid. Yield = 41%. m.p.: 182–184 °C. 1H-NMR (300 MHz, DMSO-d6) δH (ppm): 10.28 (1H, s, B-OH), 9.25 (1H, s, NH), 8.11 (1H, d, J = 1.8 Hz, Ar-H9), 7.78 (1H, dd, J = 1.8 and 6.3 Hz, Ar-H10), 7.65–7.56 (3H, m, Ar-H7/H6/H2), 7.46–7.34 (4H, m, Ar-H11, Ar-H5, Ar-H4, Ar-H3), 6.90 (1H, d, J = 15.6 Hz, H8), 4.96 (2H, s, H12). 13C-NMR (75 MHz, DMSO-d6) δ (ppm): 163.6, 149.4, 140.4, 138.6, 135.3, 130.1, 129.6, 128.2, 122.9, 122.8, 122.1, 121.5, 70.2. m/z (ESI-MS) found 280.1146 [M + H]+, expected 279.1067. HPLC purity = 99.3%, retention time = 1.01 min.
(E)-N-(1-Hydroxy-1,3-dihydrobenzo[c][1,2]oxaborol-6-yl)-3-(3-nitrophenyl)acrylamide (5b). Yellow solid. Yield = 48%. m.p.: 176–178 °C. 1H-NMR (300 MHz, DMSO-d6) δH (ppm): 10.23 (1H, s, B-OH), 8.09 (1H, d, J = 3.0 Hz, Ar-H9), 8.77 (1H, dd, J = 3.0 and 6.0 Hz, Ar-H10), 7.52 (1H, d, J = 15.0 Hz, H7), 7.35 (1H, d, J = 6.0 Hz, Ar-11), 7.20–7.13 (2H, m, H4, H2),7.03–6.96 (1H, m, Ar-H6), 6.90–6.82 (1H, m, Ar-H5), 6.73 (1H, d, J = 15.0 Hz, H8), 4.94 (2H, s, H12). 13C-NMR (75 MHz, DMSO-d6) δC (ppm):164.5, 149.4, 148.7, 140.4, 138.9, 129.9, 124.1, 122.9, 122.4, 121.7, 121.1, 109.4, 107.0, 102.2, 70.4. m/z (ESI-MS) found 324.1046 [M]+, expected 324.0918. HPLC purity = 92.5%, retention time = 1.43 min.
(E)-N-(1-Hydroxy-1,3-dihydrobenzo[c][1,2]oxaborol-6-yl)-3-(4-nitrophenyl)acrylamide (5c). Yellow solid. Yield = 42%. m.p.: 176–180 °C.1H-NMR (600 MHz, DMSO-d6) δH (ppm): 10.42 (1H, s, B-OH), 9.29 (1H, s, H10), 8.29 (2H, d, J = 9.0 Hz, Ar-Hf), 8.10 (1H, d, J = 1.5 Hz, Ar-H7), 7.90 (2H, d, J = 9.0 Hz, Ar-He), 7.77 (1H, dd, J = 1.8, 9.0 Hz, Ar-H5), 7.70 (1H, d, J = 15.6 Hz, Hb), 7.39 (1H, d, J = 8.4 Hz, Ar-H4), 7.05 (1H, d, J = 15.0 Hz, Hc), 4.96 (2H, s, H3). 13C-NMR (151 MHz, DMSO-d6) δC (ppm): 163.3, 149.6, 148.1, 141.8, 138.4, 138.0, 129.2, 127.2, 124.6, 122.8, 122.2, 121.6. 70.3. ESI-HRMS m/z calcd. for C16H13BN2O5 324.0918, found 325.1005 [M + H]+. HPLC purity = 99.1%, retention time = 1.33 min.
(E)-3-(4-Bromophenyl)-N-(1-hydroxy-1,3-dihydrobenzo[c][1,2]oxaborol-6-yl)acrylamide (5d). Off white solid. Yield = 29%. m.p.: 206–210 °C. 1H-NMR (300 MHz, DMSO-d6) δH (ppm):10.33 (1H, s, B-OH), 9.28 (1H, s, H10), 8.32 (1H, d, J = 2.8 Hz, Ar-H7), 8.06 (1H, dd, J = 3.0, 6.0 Hz, Ar-H5), 7.61–7.51 (4H, m, Ar-He, -Hf), 7.53 (1H, d, J = 15.0 Hz, Hb), 7.36 (1H, d, J = 9.0 Hz, Ar-4), 6.87 (1H, d, J = 15.0 Hz, Hc), 4.94 (2H, s, H3). 13C-NMR (75 MHz, DMSO-d6) δC (ppm): 163.9, 149.6, 139.3, 139.3, 138.3, 134.4, 132.4, 130.2, 123.4, 123.0, 122.2, 121.6, 70.2. ESI-HRMS m/z calcd. for C16H13BBrNO3 357.0172, found 358.0250 [M + H]+. HPLC purity = 98.4%, retention time = 0.67 min.
(E)-N-(1-Hydroxy-1,3-dihydrobenzo[c][1,2]oxaborol-6-yl)-3-(4-methoxyphenyl)acrylamide (5e). Off white solid. Yield = 32%. m.p.: 190–192 °C. 1H-NMR (300 MHz, DMSO-d6) δH (ppm): 10.19 (1H, s, B-OH), 9.25 (1H, s, NH), 8.09 (1H, d, J = 1.2 Hz, Ar-H9), 7.75 (1H, dd, J = 1.8 and 6.6 Hz, Ar-H10), 7.54 (1H, d, J = 15.0 Hz, H7), 7.36 (1H, d, J = 9.0 Hz, Ar-11), 7.01 (2H, d, J = 9.0 Hz, Ar-H2, H6), 6.97 (2H, d, J = 9.0 Hz, Ar-H5, H3), 6.74 (1H, d, J = 15.0, H8), 4.95 (2H, s, H12), 3.15 (3H, s, H4’). 13C-NMR (75 MHz, DMSO-d6) δC (ppm): 168.4, 164.4, 161.1, 149.3, 138.9, 130.5, 130.57, 130.0, 127.8, 127.7, 120.6, 115.1, 70.5, 56.1. m/z (ESI-MS) found 310.1252 [M + H]+, expected 309.1172. HPLC purity = 99.5%, retention time = 0.95 min.
(E)-3-(3,4-Dimethoxyphenyl)-N-(1-hydroxy-1,3-dihydrobenzo[c][1,2]oxaborol-6-yl)acrylamide (5f). Pale yellow solid. Yield = 46%. m.p.: 188–190 °C. 1H-NMR (300 MHz, DMSO-d6) δH (ppm): 10.20 (1H, s, B-OH), 9.35 (1H, s, NH), 8.05 (1H, d, J = 2.6 Hz, Ar-H9), 7.71 (1H, dd, J = 3.0 and 6.0 Hz, Ar-H10), 7.51 (2H, d, J = 15.6 Hz, H7), 7.35 (1H, d, J = 9.0 Hz, Ar-11), 7.20–7.13 (2H, m, H5, H2), 6.98 (1H, d, J = 9.0 Hz, H6), 6.73 (1H, d, J = 15.0, H8), 4.93 (2H, s, H12), 3.79 (6H, s, H4’, H3). 13C-NMR (75 MHz, DMSO-d6) δC (ppm): 168.9, 164.9, 151.2, 151.6, 149.7, 141.2, 138.8, 128.1, 127.7, 123.4, 122.7, 122.5, 122.0, 120.6, 110.9, 56.4, 56.3. m/z (ESI-MS) found 340.1357 [M + H]+, expected 339.1278. HPLC purity = 97.1%, retention time = 1.28 min.
(E)-3-(Benzo[d][1,3]-6-dioxol-5-yl)-N-(1-hydroxy-1,3-dihydrobenzo[c][1,2]oxaborol-6-yl)acrylamide (5g). Pale yellow solid. Yield = 38%. m.p.: 145–148 °C. 1H-NMR (400 MHz, DMSO-d6) δH (ppm): 10.64 (1H, s, B-OH), 9.30 (1H, s, NH), 8.47 (2H, s, Ar-H7), 8.24 (1H, d, J = 8.0 Hz, Ar-H7), 8.14 (1H, s, Ar-He), 7.81 (1H, d, J = 6.3 Hz, Ar-4), 7.76 (1H, d, J = 7.6 Hz, Ar-i), 7.71 (1H, d, J = 16.0 Hz, Hb), 7.37 (1H, d, J = 8.0 Hz, Ar-Hh), 7.20 (1H, d, J = 16.0 Hz, Hc), 4.98 (2H, s, H3), 1.98 (2H, s, Hk). 13C-NMR (75 MHz, DMSO-d6) δC (ppm):170.7, 163.0, 149.4, 148.8, 138.4, 137.8, 134.4, 130.8, 125.9, 124.2, 122.1, 121.5, 70.1, 60.1. ESI-HRMS m/z calcd for C17H14BNO5 323.0965, found 325.0995 [M + H]+. HPLC psurity = 100%, retention time = 1.40 min.
3.3. In Vitro Antitrypanosomal Assay
Trypanosoma brucei brucei 427 trypomastigotes were cultured in Iscove’sss Modified Dulbecco’s medium (IMDM, Lonza, Basel Switzerland) supplemented with 10% fetal calf serum, HMI-9 supplement [56], hypoxanthine, and penicillin/streptomycin at 37 °C in a 5% CO2 incubator. Serial dilutions of test compounds were incubated with the parasites in 96-well plates for 24 h and residual parasite viability in the wells determined by adding 20 μL resazurin toxicology reagent (Sigma-Aldrich) and incubating for an additional 2–4 h. Reduction of resazurin to resorufin by viable parasites was assessed by fluorescence readings (excitation 560 nm, emission 590 nm) in a Spectramax M3 plate reader (Molecular Devices, San Jose, CA, USA). Fluorescence readings were converted to % parasite viability relative to the average readings obtained from untreated control wells. IC50 values were determined by plotting % viability vs. log[compound] and performing non-linear regression using GraphPad Prism (v. 5.02) software [57].
3.4. In Vitro Cytotoxicity Assay
HeLa cells (Cellonex, Johannesburg, South Africa) seeded in 96-well plates were incubated with 20 μM test compounds for 24 h and cell viability assessed using a resazurin fluorescence assay as previously described [57].
3.5. In Vitro Antitrichomonal Assay and Mucosal Normal Flora Susceptibility Assay
Axenic cultures of the Trichomonas vaginalis G3 strain (the genome strain) were grown in 5 mL TYM Diamond’s medium (containing equine serum and antibiotics) in a 37 °C incubator for 24 h. One hundred millimolar stocks of the compounds were made by dissolving in DMSO and were screened against G3 stain of T. vaginalis. Cells that are untreated and treated with 5 μL DMSO (0.1% final concentration) were used as controls. Five milliliters of the 100 mM stocks of the compound library were added for a final concentration of 50 mM. Results were calculated based on manual counts utilizing a hemocytometer after 24 h (parasite motility being the criteria for viability). The IC50 values were determined by titration of the stock solutions and hemocytometer counting as described above. Data were plotted on GraphPad Prism (GraphPad Software Inc., San Diego, CA, USA) and theoretical IC50 values were determined. To confirm the IC50 values, the predicted values were then re-tested as described above. Non-pathogenic mucosal normal flora strains such as Lactobacillus reuteri (ATCC 23272, Lactobacillus acidophilus (ATCC 43560), and Lactobacillus rhamnosus (ATCC 53103) were cultured in Lactobacilli MRS at 37 °C under anaerobic conditions. One hundred milliMolar stock solutions as well as vehicle control DMSO were diluted to 100 μM in media and incubated with empty BDL-sensi-discs (6 mm) for 20 min at room temperature. Discs containing vehicle control, compounds, or various antibiotic discs [levofloxacin (5 μg), gentamicin (10 μg), and gentamicin (120 μg)] were placed onto the bacterial streaked agar plates and incubated overnight at 37 °C. Vehicle, compound, or antibiotic sensitivity was determined via measurement of zones of inhibition around each disc in mm.
3.6. In Vitro Antimycobacterial Assay
The minimum inhibitory concentration (MIC) was determined using the standard broth micro dilution method, where a 10 mL culture of Mycobacterium tuberculosis pMSp12:GFP [58], was grown to an optical density (OD600) of 0.6–0.7. The media used were: (i) Gaste-Fe (glycerol-alanine-salts) medium pH 6.6, supplemented with 0.05% Tween-80 and 1% Glycerol, and (ii) 7H9 supplemented with 10% Albumin Dextrose Catalase supplement (ADC), 0.05% Tween-80 [59,60]. Cultures grown in Gaste-Fe were diluted 1:100, and cultures grown in 7H9 ADC were diluted 1:500, prior to inoculation of the MIC assay. The compounds to be tested are reconstituted to a concentration of 10 mM in DMSO. Two-fold serial dilutions of the test compound are prepared across a 96-well micro titre plate, after which, 50 μL of the diluted M. tuberculosis cultures were added to each well in the serial dilution. The plate layout was a modification of the method previously described [61]. Assay controls used were a minimum growth control (Rifampicin at 2 × MIC), and a maximum growth control (5% DMSO). The micro titre plates were sealed in a secondary container and incubated at 37 °C with 5% CO2 and humidification. Relative fluorescence (excitation 485 nM; emission 520 nM) was measured using a plate reader (FLUOstar OPTIMA, BMG LABTECH, Ortenberg, Germany), at day 7 and day 14. The raw fluorescence data were archived and analyzed using the CDD Vault from Collaborative Drug Discovery, in which, data were normalized to the minimum and maximum inhibition controls to generate a dose response curve (% inhibition), using the Levenberg-Marquardt (Burlingame, CA, USA www.collaborativedrug.com) damped least squares method, from which the MIC90 was calculated. The lowest concentration of drug that inhibits growth of more than 90% of the bacterial population was considered the MIC90.
4. Conclusions
In summary, the current drugs used to treat sleeping sickness have serious side effects, and in most cases, showed poor efficacy. Therefore, there is a need to search for new and better treatment options. Benzoxaborole-containing lead compounds have demonstrated promising efficacy and desirable drug-like properties. Due to high attrition in clinical development, it is essential to replete the drug development pipeline with structurally diverse leads. In this study, a small set of cinnamoyl-oxaborole molecules was synthesized and evaluated for trypanocidal activity; and for activity against other prevalent human pathogens. Compound 5g emerged as new hit with improved activity compared to compound 2 against T. b. brucei. Against other pathogens evaluated in this study, these compounds displayed moderate to weak activity without any obvious cytotoxic effect.
Acknowledgments
The authors (S.D.K and R.M.B.) acknowledge Rhodes University for a Postdoctoral (RMB) support. KML and NL were supported by the Department of Biological Sciences at the University of the Pacific. Our great appreciation from the Stellenbosch University Central Analytical Facility (CAF) for mass spectrometric analysis.
Supplementary Materials
The following are available online (Synthesis of compound 6, 1H and 13C-NMR spectra of 5c, 5d, and 5g).
Author Contributions
G.M. and T.M. synthesized target amides. R.S. and D.F.W. coordinated and performed the anti-mycobacterial assay experiments. C.C.T.; L.W.C.; N.L. and K.M.L. developed and performed the anti-T. vaginalis assays and related antimicrobial experiments. R.M.B. validated the synthesis of amides and compiled the paper. H.C.H, M.I. and D.L. coordinated and performed the T. b. brucei and cytotoxicity assays. S.D.K conceptualized and coordinated the investigation including supervision.
Funding
This work was funded by the National Research Foundation (S.D.K), South Africa, grant number (98894) and Rhodes University Sandisa Imbewu (S.D.K. and H.C.H.). The antiplasmodial bioassay component of the project was funded by the South African Medical Research Council (SAMRC) with funds from National Treasury under its Economic Competitiveness and Support Package. The antimycobacterial assays were funded by a grant (to D.F.W.) from the Strategic Health Innovation Partnerships initiative of the South African Medical Research Council (SAMRC) with funds from National Treasury under its Economic Competitiveness and Support Package. CT and LWC were funded by the United States Department of Agriculture, Agricultural Research Service (National Program 108, Project #5325-42000-039-00D).
Conflicts of Interest
The authors declare no conflict of interest.
Footnotes
Sample Availability: Samples of all the compounds 5a–g are available from the authors.
References
- 1.Njogu P.M., Guantai E.M., Pavadai E., Chibale K. Computer-aided drug discovery approaches against the tropical infectious diseases malaria, tuberculosis, trypanosomiasis, and leishmaniasis. ACS Infect. Dis. 2015;2:8–31. doi: 10.1021/acsinfecdis.5b00093. [DOI] [PubMed] [Google Scholar]
- 2.WHO Global Tubercoulosis Report 2017. [(accessed on 30 May 2018)]; Available online: http://www.who.int/tb/publications/global_report/en/
- 3.Jakobsen P.H., Wang M.W., Nwaka S. Innovative partnerships for drug discovery against neglected diseases. PLoS Negl. Trop. Dis. 2011;5:e1221. doi: 10.1371/journal.pntd.0001221. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Li X.X., Zhou X.N. Con-infection of tuberculosis and parasitic diseases in humans: a systematic review. Parasites Vectors. 2013;6:79. doi: 10.1186/1756-3305-6-79. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Berninger M., Schimidt I., Ponte-Sucre A., Holzgrabe U. Novel lead compounds in pre-clinical development against African sleeping sickness. Med. Chem. Commun. 2017;8:1872–1890. doi: 10.1039/C7MD00280G. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Njoroge M., Njuguna N.M., Mutai P., Ongarora D.S.B., Smith P.W., Chibale K. Recent approaches to chemical discovery and development against malaria and the neglected tropical diseases human African trypanosomiasis and schistosomiasis. Chem. Rev. 2014;114:11138–11163. doi: 10.1021/cr500098f. [DOI] [PubMed] [Google Scholar]
- 7.Castillo-Acosta V., Ruiz-Pérez L., Etxebarria J., Reichardt N., Navarro M., Igarashi Y., Liekens S., Balzarini J., González-Pacanowska D. Open source drug discovery with the malaria box compound collection for neglected diseases and beyong. PLoS Pathog. 2016;12:e1005851. doi: 10.1371/journal.ppat.1005763. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Burrows J.N., Elliott R.L., Kaneko T., Mowbray C.E., Waterson D. The role of modern drug discovery in the fight against neglected and tropical diseases. Med. Chem. Commun. 2014;5:688–700. doi: 10.1039/c4md00011k. [DOI] [Google Scholar]
- 9.Kwofie K.D., Tung N.H., Suzuki-Ohashi M., AmoaBosompem M., Adegle R., Sakyiamah M.M., Ayertey F., Owusu K.B.-A., Tuffour I., Atchoglo P., et al. Antitrypanosomal activities and mechanisms of action of novel tetracyclic iridoids from Morinda lucida benth. Antimicrob. Agents Chemother. 2016;60:3283–3290. doi: 10.1128/AAC.01916-15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.WHO: Trypanosomiasis, Human African (Sleeping Sickness) [(accessed on 30 June 2018)]; Available online: http://www.who.int/mediacentre/factsheets/fs259/en/
- 11.Nwodo N.J., Ibezim A., Ntie-Kang F., Adikwu M.U., Mbah C.J. Anti-trypanosomal activity of Nigerian plants and their constituents. Molecules. 2015;20:7751–7771. doi: 10.3390/molecules20057750. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.CDC Parasites African Trypanosomiasis (Also known as Sleeping Sickness) [(accessed on 30 June 2018)]; Available online: https://www.cdc.gov/parasites/sleepingsickness/
- 13.Franco J.R., Simarro P.P., Diarra A., Jannin J.G. Epidemiology of human African trypanosomiasis. Clin. Epidemiol. 2014;6:257–275. doi: 10.2147/CLEP.S39728. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Babokhov P., Sanyaolu A.O., Oyibo W.A., Fagbenro-Beyioku A.F., Iriemenam N.C. A current analysis of chemotherapy strategies for the treatment of human African trypanosomiasis. Pathog. Glob. Health. 2013;107:242–252. doi: 10.1179/2047773213Y.0000000105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Kaiser M., Bray M.A., Cal M., Trunz B., Torreele E., Brun R. Antitrypanosomal activity of fexinidazole, a new oral nitroimidazole drug candidate for treatment of sleeping sickness. Antimicrob. Agents Chemother. 2011;55:5602–5608. doi: 10.1128/AAC.00246-11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Mishina Y.V., Krishna S., Haynes R.K., Meade J.C. Artemisinins inhibit Trypanosoma cruzi and Trypanosoma bruce rhodesiense in vitro growth. Antimicrob. Agents Chemother. 2007;51:1852–1854. doi: 10.1128/AAC.01544-06. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Willyard C. Putting sleeping sickness to bed. Nat. Med. 2011;17:14–17. doi: 10.1038/nm0111-14. [DOI] [PubMed] [Google Scholar]
- 18.Balasegaram M., Young H., Chappuis F., Priotto G., Raguenaud M.E., Checchi F. Effectiveness of melarsoprol and eflornithine as first-line regimens for gambiense sleeping sickness in nine Médecins Sans Frontières programmes. Trans. R. Soc. Trop. Med. Hyg. 2009;103:280–290. doi: 10.1016/j.trstmh.2008.09.005. [DOI] [PubMed] [Google Scholar]
- 19.Yang P.Y., Wang M., Li L., Wu H., He C.Y., Yao S.Q. Design, synthesis and biological evaluation of potent azadipeptide nitrile inhibitors and activity-based probes as promising anti-Trypanosoma brucei agents. Chem. Eur. J. 2012;18:6528–6541. doi: 10.1002/chem.201103322. [DOI] [PubMed] [Google Scholar]
- 20.Giordani F., Morrison L.J., Rowan T.G., De Koning H.P., Barrett M.P. The animal trypanosomiases and their chemotherapy: A review. Parasitology. 2016;143:1862–1889. doi: 10.1017/S0031182016001268. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.WHO . WHO Report 2007: Global Strategy for the Prevention and Control of Sexually Transmitted Infections: 2006–2015: Breaking the Chain of Transmission. WHO Press; Geneva, Switzerland: 2007. pp. 1–60. WC 142. [Google Scholar]
- 22.World Health Organization Department of Reproductive Health and Research (2011) WHO. [(accessed on 30 June 2018)]; Available online: http://www.who.int/reproductivehealth/publications/rtis/9789241502450/en/index.html/
- 23.Secor W.E., Meites E., Starr M.C., Workowski K.A. Neglected parasitic infections in the United States: Trichomoniasis. Am. J. Trop. Med. Hyg. 2014;90:800–804. doi: 10.4269/ajtmh.13-0723. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Kirkcaldy R.D., Augostini P., Asbel L.E., Bernstein K.T., Kerani R.P., Mettenbrink C.J., Pathela P., Schwebke J.R., Secor W.E., Workowski K.A., et al. Trichomonas vaginalis antimicrobial drug resistance in six US cities, STD surveillance network, 2009–2010. Emerg. Infect. Dis. 2012;18:939–943. doi: 10.3201/eid1806.111590. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Workowski K.A., Bolan G.A. Sexually transmitted diseases treatment guidelines. MMWR Recomm. Rep. 2015;64:1–137. doi: 10.1086/342100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Liu C.T., Tomsho J.W., Benkovic S.J. The unique chemistry of benzoxaboroles: Current and emerging applications in biotechnology and therapeutic treatments. Bioorg. Med. Chem. 2014;22:4462–4473. doi: 10.1016/j.bmc.2014.04.065. [DOI] [PubMed] [Google Scholar]
- 27.Baker S.J., Tomsho J.W., Benkovic S.J. Boron-containing inhibitors of synthetases. Chem. Soc. Rev. 2011;40:4279–4285. doi: 10.1039/c0cs00131g. [DOI] [PubMed] [Google Scholar]
- 28.Jacobs R.T., Plattner J.J., Keenan M. Boron-based drugs as antiprotozoals. Curr. Opin. Infect. Dis. 2011;24:586–592. doi: 10.1097/QCO.0b013e32834c630e. [DOI] [PubMed] [Google Scholar]
- 29.Adamczyk-Woźniak A., Borys K.M., Sporzyński A. Recent developments in the chemistry and biological applications of benzoxaboroles. Chem. Rev. 2015;115:5224–5247. doi: 10.1021/cr500642d. [DOI] [PubMed] [Google Scholar]
- 30.Adamczyk-Woźniak A., Cyrański M.K., Żubrowska A., Sporzyński A. Benzoxaboroles-Old compounds with new applications. J. Organomet. Chem. 2009;694:3533–3541. doi: 10.1016/j.jorganchem.2009.07.022. [DOI] [Google Scholar]
- 31.Zhang J., Zhu M.Y., Lin Y.N., Zhou H.C. The synthesis of benzoxaboroles and their applications in medicinal chemistry. Sci. China Chem. 2013;56:1372–1381. doi: 10.1007/s11426-013-4981-y. [DOI] [Google Scholar]
- 32.Zhang Y.P., Plattner J.J., Easome E.E., Zhou Y., Akama T., Bu W., White W.H., Defauw J.M., Winkle J.R., Balko T.W., et al. Discovery of an orally bioavailable isoxazoline benzoxaborole (AN8030) as a long acting animal ectoparasiticide. Bioorg. Med. Chem. Lett. 2015;25:5589–5593. doi: 10.1016/j.bmcl.2015.10.044. [DOI] [PubMed] [Google Scholar]
- 33.Jacobs R.T., Nare B., Wring S.A., Orr M.D., Chen D., Sligar J.M., Jenks M.X., Noe R.A., Bowling T.S., Mercer L.T., et al. SCYX-7158, an orally-active benzoxaborole for the treatment of stage 2 human African trypanosomiasis. PLoS Negl. Trop. Dis. 2011;5:e1151. doi: 10.1371/journal.pntd.0001151. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Torssell K. Bromination of tolylboronic acids according to Wohl-Ziegler. Ark. Kemi. 1957;10:507–511. [Google Scholar]
- 35.Brun R., Don R., Jacobs R., Wang M., Barrett M. Devlopment of novel drugs for human African trypanosomiasis. Future Microbiol. 2011;6:677–691. doi: 10.2217/fmb.11.44. [DOI] [PubMed] [Google Scholar]
- 36.Drugs for Neglected Diseases Initiative (Dndi) Dndi Announces Successful Completion of SCYX-7158 Phase I Study for Treatment of Sleeping Sicknes. [(accessed on 25 June 2018)]; Available online: http://www.news-medical.net/news/20150909/DNDi-announces-successful-completion-of-SCYX-7158-Phase-I-study-for-treatment-of-sleeping-sickness.aspx.
- 37.Waring M.J., Arrowsmith J., Leach A.R., Leeson P.D., Mandrell S., Owen R.M., Pairaudeau G., Pennie W.D., Pickett S.D., Wang J., et al. An analysis of the attrition of drug candidates from four major pharmaceutical companies. Nat. Rev. Drug Discov. 2015;14:475–486. doi: 10.1038/nrd4609. [DOI] [PubMed] [Google Scholar]
- 38.Jacobs R., Orr M., Wring S., Chen D., Zhou H., Ding D., Feng Y., Ye L., Hernandez V.S., Zhang Y.K., et al. Boron-Containing Small Molecules as Anti-Protozoal Agents. WO2010045503A1. 2016 Nov 15;
- 39.Stierli D., Renold P., Rajan R. Novel microbiocides. WO2014173880A1. 2014 Oct 30;
- 40.De P., Bedos-Belval F., Vanucci-Bacque C., Baltas M. Cinnamic acid derivatives iin tuberculosis, malaria and cardiovascular diseases-a review. Curr. Org. Chem. 2012;16:747–768. [Google Scholar]
- 41.Sharma P. Cinnamic acid derivatives: A new chapter of various pharmacological activities. J. Chem. Pharm. Res. 2011;3:403–423. [Google Scholar]
- 42.Guzman J.D. Natural cinnamic acids, synthetic derivatives and hybrids with antimicrobial activity. Molecules. 2014;19:19292–19349. doi: 10.3390/molecules191219292. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Wiesner J., Wiβner P., Dahse H.M., Jomaa H., Schlitzer M. Discovery of novel lead structure for antimalarials. Bioorg. Med. Chem. 2001;9:785–792. doi: 10.1016/S0968-0896(00)00296-0. [DOI] [PubMed] [Google Scholar]
- 44.Joardar S., Bhattacharyya A., Das S. A palladium on carbon catalyzed one-pot synthesis of substituted benzyimidazoles. Synthesis. 2014;46:3121–3132. doi: 10.1055/s-0034-1378454. [DOI] [Google Scholar]
- 45.Joullié M.M., Lassen K.M. Evolution of bond formation. Arkivoc. 2010:189–250. [Google Scholar]
- 46.Montalbetti C.A.G., Falque V. Amide bond formation and peptide coupling. Tetrahedron. 2005;61:10827–10852. doi: 10.1016/j.tet.2005.08.031. [DOI] [Google Scholar]
- 47.Leggio A., Belsito E.L., De Luca G., Di Gioia M.L., Leotta V., Romio E., Siciliano C., Liguori A. One-pot synthesis of amides from carboxylic acids activated using thionyl chloride. RSC Adv. 2016;6:34468–34475. doi: 10.1039/C5RA24527C. [DOI] [Google Scholar]
- 48.Chen P.J., Wang H.Y., Peng A.Y. A mild and efficient amide formation reaction mediated by P(OEt)3 and iodine. RSC Adv. 2015;5:94328–94331. doi: 10.1039/C5RA18459B. [DOI] [Google Scholar]
- 49.Adamczyk-Woźniak A., Cyrański M.K., Jakubczyk M., Klimentowska P., Koll A., Kołodziejczak J., Pojmaj G., Żubrowska A., Żukowska G.Z., Sporzyński A. Influence of the substituents on the structure and properties of benzoxaboroles. J. Phys. Chem. A. 2010;114:2324–2330. doi: 10.1021/jp9086283. [DOI] [PubMed] [Google Scholar]
- 50.Carvalho S.A., da Silva F., de Souza M.V.N., Lourenco M.C.S., Vincente F.R. Synthesis and antimycobacterial evaluation of trans-cinnamic acid hydrazide derivatives. Bioorg. Med. Chem. Lett. 2008;18:538–541. doi: 10.1016/j.bmcl.2007.11.091. [DOI] [PubMed] [Google Scholar]
- 51.De P., Yoya G.K., Constant P., Bedos-Belval F., Duran H., Saffon N., Daffé M., Baltas M. Design, synthesis, and biological evaluation of new cinnamic derivatives as antituberculosis agents. J. Med. Chem. 2011;54:1449–1461. doi: 10.1021/jm101510d. [DOI] [PubMed] [Google Scholar]
- 52.Kakwani M.D., Suryavanshi P., Ray M., Rajan M.G.R., Majee S., Samad A., Devarajan P., Degani M.S. Design, synthesis and antimycobacterial activity of cinnamide derivatives: A molecular hybridization approach. Bioorg. Med. Chem. Lett. 2011;21:1997–1999. doi: 10.1016/j.bmcl.2011.02.022. [DOI] [PubMed] [Google Scholar]
- 53.Pérez B., Teixeira C., Gut J., Rosenthal P.J., Gomes J.R.B., Gomes P. Cinnamic acid/chloroquinoline conjugates as potent agents against chloroquine-resistant Plasmodium falciparum. Chem. Med. Chem. 2012;7:1537–1540. doi: 10.1002/cmdc.201200257. [DOI] [PubMed] [Google Scholar]
- 54.Chang S., Yin S.L., Wang J., Jing Y.K., Dong J.H. Design and synthesis of novel 2-phenylaminopyrimidine (PAP) derivatives and their antiproliferative effects in human chronic myeloid leukemia cells. Molecules. 2009;14:4166–4179. doi: 10.3390/molecules14104166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Ding C.Z., Zhang Y.K., Li X., Liu Y., Zhang S., Zhou Y., Plattner J.J., Baker S.J., Liu L., Duan M., et al. Synthesis and biological evaluation of P4-benzoxaborole-substituted macrocyclic inhibitors of HCV NS3 protease. Bioorg. Med. Chem. Lett. 2010;20:7317–7322. doi: 10.1016/j.bmcl.2010.10.071. [DOI] [PubMed] [Google Scholar]
- 56.Hirymi H., Hirumi K. Continuous cultivation of Trypanosoma brucei blood stream forms in a medium containing a low concentration of serum protein without feeder cell layers. J. Parasitol. 1989;75:985–989. doi: 10.2307/3282883. [DOI] [PubMed] [Google Scholar]
- 57.Oderinlo O.O., Tukulula M., Isaacs M., Hoppe H.C., Taylor D., Smith V.J., Khanye S.D. New thiazolidine-2,4-dione derivatives compbined with organometallic ferrocene: Synthesis, structure and antiparasitic activity. Appl. Organomet. Chem. 2018;32:e4385. doi: 10.1002/aoc.4385. [DOI] [Google Scholar]
- 58.Abrahams G.L., Kumar A., Savvi S., Hung A.W., Wen S., Abell C., Barry C.E., 3rd, Sherman D.R., Boshoff H.I., Mizrahi V. Pathway-selective sensitization of Mycobacterium tuberculosis for target-based whole-cell screening. Chem. Biol. 2012;19:844–854. doi: 10.1016/j.chembiol.2012.05.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.De Voss J.J., Rutter K., Schroeder B.G., Su H., Zhu Y., Barry III C.E. The salicylate-derived mycobactin siderophores of mycobacterium tuberculosis are essential for growth in macrophages. Proc. Nat. Acad. Sci. USA. 2000;97:1252–1257. doi: 10.1073/pnas.97.3.1252. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Franzblau S.G., DeGroote M.A., Cho S.H., Andries K., Nuermberger E., Orme I.M., Mdluli K., Angulo-Barturen I., Dick T., Dartois W., et al. Comprehensive analysis of methods used for the evaluation of compounds against Mycobacterium tuberculosis. Tuberculosis. 2012;92:453–488. doi: 10.1016/j.tube.2012.07.003. [DOI] [PubMed] [Google Scholar]
- 61.Ollinger J., Bailey A., Moraski C., Casey A., Florio S., Alling T., Miller J., Parish T. A dual read-out assay to evaluate the potency of compounds active against Mycobacterium tuberculosis. PLoS ONE. 2013;8:e60531. doi: 10.1371/journal.pone.0060531. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.