Abstract
Obesity traits are causally implicated with risk of cardiometabolic diseases. It remains unclear whether there are similar causal effects of obesity traits on other non-communicable diseases. Also, it is largely unexplored whether there are any sex-specific differences in the causal effects of obesity traits on cardiometabolic diseases and other leading causes of death. We constructed sex-specific genetic risk scores (GRS) for three obesity traits; body mass index (BMI), waist-hip ratio (WHR), and WHR adjusted for BMI, including 565, 324, and 337 genetic variants, respectively. These GRSs were then used as instrumental variables to assess associations between the obesity traits and leading causes of mortality in the UK Biobank using Mendelian randomization. We also investigated associations with potential mediators, including smoking, glycemic and blood pressure traits. Sex-differences were subsequently assessed by Cochran’s Q-test (Phet). A Mendelian randomization analysis of 228,466 women and 195,041 men showed that obesity causes coronary artery disease, stroke (particularly ischemic), chronic obstructive pulmonary disease, lung cancer, type 2 and 1 diabetes mellitus, non-alcoholic fatty liver disease, chronic liver disease, and acute and chronic renal failure. Higher BMI led to higher risk of type 2 diabetes in women than in men (Phet = 1.4×10−5). Waist-hip-ratio led to a higher risk of chronic obstructive pulmonary disease (Phet = 3.7×10−6) and higher risk of chronic renal failure (Phet = 1.0×10−4) in men than women. Obesity traits have an etiological role in the majority of the leading global causes of death. Sex differences exist in the effects of obesity traits on risk of type 2 diabetes, chronic obstructive pulmonary disease, and renal failure, which may have downstream implications for public health.
Author summary
Obesity is increasing globally and has been linked to major causes of death, such as diabetes and heart disease. Still, the causal effects of obesity on other leading causes of death is relatively unexplored. It is also unclear if any such effects differ between men and women. Mendelian randomization is a method that explores causal relationships between traits using genetic data. Using Mendelian randomization, we investigated the effects of obesity traits on leading causes of death and assessed if any such effects differ between men and women. We found that obesity increases the risks of heart disease, stroke, chronic obstructive pulmonary disease, lung cancer, diabetes, kidney disease, non-alcoholic fatty liver disease and chronic liver disease. Higher body mass index led to a higher risk of type 2 diabetes in women than in men, whereas a higher waist-hip ratio increased risks of chronic obstructive pulmonary disease and chronic kidney disease more in men than in women. In summary, obesity traits are causally involved in the majority of the leading causes of death, and some obesity traits affect disease risk differently in men and women. This has potential implications for public health strategies and indicates that sex-specific preventative measures may be needed.
Introduction
It is increasingly evident that obesity negatively impacts human health and the prevalence of obesity is increasing world-wide [1]. Both overall obesity (body mass index (BMI) >30 kg/m2) and fat distribution (waist-hip-ratio (WHR) >1.0 in men and >0.85 in women indicative of abdominal fat accumulation) have been linked to cardiometabolic diseases and death in observational studies [2–5]. Previous studies have found causal relationships between higher BMI and WHR adjusted for BMI (WHRadjBMI) and type 2 diabetes (T2D) and coronary artery disease (CAD), using a limited number of previously known obesity-associated single nucleotide polymorphisms (SNPs) [6–11]. However, sex-specific relationships are largely unexplored as is the the role that obesity traits play in the leading causes of death beyond these cardiometabolic diseases.
Obesity traits are known to differ between women and men; regional obesity prevalence rates often vary between the sexes [12,13], women have higher SNP-based heritability for WHR [14], and >90% of WHRadjBMI-associated SNPs that show evidence of sexual dimorphism have larger effect sizes in women than men [14]. It has been suggested that fat distribution related traits might be more strongly associated with cardiometabolic outcomes in women, although many previous studies are inconclusive [15–19]. Only a few studies have investigated sex differences in the effect of genetic risk for obesity-related traits on disease risk [6,9,11] and have mostly been restricted to waist-related traits and T2D and CAD, using a limited number of analyses and/or SNPs, but without finding evidence of differences in disease risk between men and women [6,9,11].
Expanding to a larger set of robustly associated SNPs may identify previously undetected sexual heterogeneity in obesity-related disease risk. A sex difference in the effect of obesity traits on major causes of death could signify that the disease burden arising from obesity may be differential in women and men, allowing prioritizing of public health resources and potentially, sex-specific preventative strategies. We therefore investigated the extent to which obesity traits causally impact the risk of the major global causes of death, and whether relationships with disease are differential between women and men, exploiting recent advances in discovery of obesity-associated SNPs [14].
Methods
Overview of methods
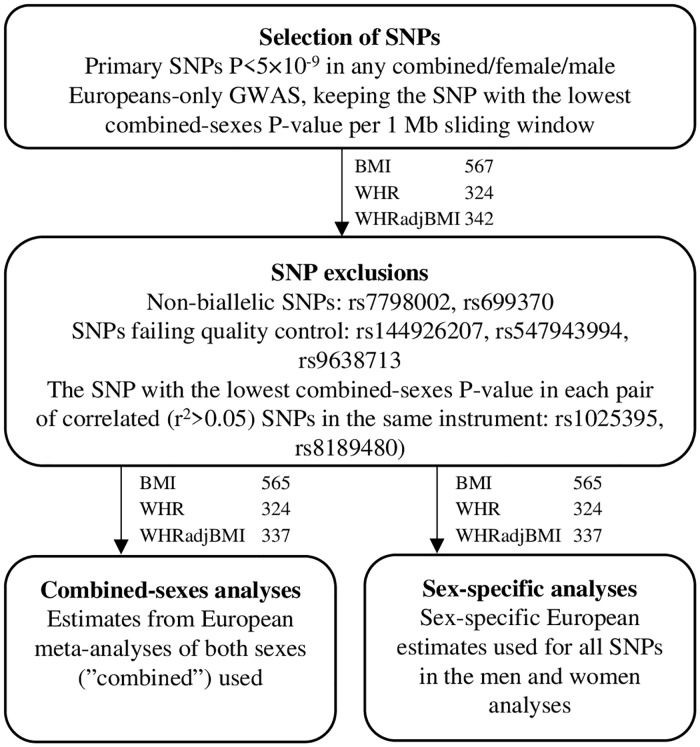
Sex-specific genetic risk scores (GRSs) were constructed and evaluated for BMI, WHR, and WHRadjBMI using genome-wide significant (P<5×10−9) SNPs from a recent genome-wide association study (GWAS) in the Genetic Investigation of ANthropometric Traits (GIANT) [20,21] and UK Biobank [14,22]. These were then investigated for associations with diseases and risk factors in the UK Biobank using regression in a sex-stratified manner. Obesity GRS-outcome combinations that surpassed the multiple testing correction threshold were then analysed with Mendelian randomization (MR) to compute formal causal estimates, and sexual heterogeneity was assessed. In addition, we performed 2-sample MR for outcomes for which we only had access to summary-level data. We also performed sensitivity analyses to explore the robustness of our findings. For an overview of the methods see Fig 1.
Fig 1. Overview of methods.
BMI, body mass index; CLD, chronic liver disease; COPD, chronic obstructive pulmonary disease; DBP, diastolic blood pressure; GRS, genetic risk score; MAGIC, Meta-Analyses of Glucose and Insulin-related traits Consortium; MR, Mendelian randomization; NAFLD, non-alcoholic fatty liver disease; PC, principal component; SBP, systolic blood pressure; T1D, type 1 diabetes; T2D, type 2 diabetes; WHR, waist-hip ratio; WHRadjBMI, waist-hip ratio adjusted for body mass index.
The UK Biobank
The UK Biobank is a prospective UK-based cohort study, with 488,377 genotyped individuals aged 40–69 when recruited [22]. UK Biobank has a Research Tissue Bank approval (Research Ethics Committee reference 16/NW/0274, this study’s application ID 11867), and all participants gave informed consent.
Genotyping, primary genotype quality control, and imputation were performed by the UK Biobank, described in detail elsewhere [23]. Briefly, the UK Biobank samples were genotyped using one of two different arrays, the UK biobank BiLEVE array or the UK biobank array [23]. The genotype data were then imputed using the HRC reference panel [24] or a merged reference panel consisting of UK10K [25] and 1000 Genomes phase 3 [26], with preference given to the HRC reference panel [23]. The imputed genotype data in BGEN v1.2 format were converted into hard calls (--hard-call-threshold 0.1) using PLINK v2.00aLM [14,27,28]. We then performed post-imputation quality control [14,27]. Only SNPs with imputation info score >0.3, minor allele frequency ≥0.01%, and Hardy-Weinberg equilibrium exact test threshold P≥1×10−6 were kept. In addition, SNPs with a missing call rate >0.05 and non-biallelic SNPs were excluded (for details see S1 Text).
General sample quality control was performed (for details see S1 Text) and samples of non-European ancestry excluded, resulting in a final sample size of up to 423,507 individuals. Participant characteristics are in Table A in S1 Text.
Instruments
We evaluated several approaches to construct sex-specific GRSs for BMI, WHR, and WHRadjBMI (Fig A-B in S1 Text). The approach with the highest ranges of trait variance explained and F-statistics for the relevant obesity trait, and with no demonstrable heterogeneity between men and women, was selected as the main model. In this model, GRSs were constructed by combining the primary (“index”) genome-wide significant (P<5×10−9) SNPs in the men, women, or combined-sexes analyses in the largest GWAS available with sex-specific European summary statistics, a meta-analysis of GIANT [20,21] and the UK Biobank (Fig 2, S1 Text and S1 Table) [14,22]. Primary SNPs were identified in the original GWAS [14] by proximal and joint conditional analysis using GCTA in associated loci. Associated loci were established around top SNPs associated with the obesity trait P<5×10−9, and included all SNPs associated with the obesity trait P<0.05, within ±5 Mb of the top SNPs, and in linkage disequlibrium (LD; r2>0.05) with the top SNP; overlapping loci were merged [14].
Fig 2. SNP- and weight selection flowchart with number of SNPs for each obesity trait.
SNPs were selected by combining the primary (“index”) variants associated with the obesity traits P<5×10−9 in a meta-analysis of GIANT and UK Biobank [14,22]. All SNPs were weighted by their sex-specific European estimates for the men- and women-specific analyses, and by the combined-sexes European estimates for the combined-sexes analyses, using estimates from the original genome-wide association study. BMI, body mass index; SNP, single nucleotide polymorphism; WHR, waist-hip-ratio; WHRadjBMI, waist-hip-ratio adjusted for body mass index.
We then kept the SNP with the lowest combined-sexes P-value within each 1 Mb sliding window to limit correlation between SNPs discovered in different sex-strata in each obesity trait. We excluded non-biallelic SNPs (N = 2), SNPs that failed quality control (N = 3), and one SNP per pair with long-distance linkage disequilibrium (r2>0.05, N = 2) (S1 Text). For the combined-sexes analyses, SNPs were weighted using estimates from the combined-sexes European meta-analyzed GWASs. For the men- and women-only analyses, SNPs were weighted by their sex-specific European estimates. All SNPs were orientated so that the effect allele corresponded to a higher level of the investigated obesity trait. Genetic risk scores were then computed using PLINK v1.90b3 (--score, with sum option) [28].
Exposures: Obesity traits
Baseline measurements were used for BMI, WHR, and WHRadjBMI. They were then standardized by rank inverse normal transformation of the residuals after regression of the trait on baseline age, age2, assessment centre, and, if applicable, sex. This was done separately in the men and women only analyses, but jointly in the combined analyses, after any sample quality exclusions (S1 Text). For WHRadjBMI we also adjusted for BMI.
Outcomes: Diseases
We investigated associations between the three obesity traits (BMI, WHR, and WHRadjBMI) with all non-communicable diseases on the World Health Organization’s (WHO) list of leading mortality causes world-wide and in high-income countries [29]; CAD, stroke (including ischemic, hemorrhagic, and of any cause), chronic obstructive pulmonary disease (COPD), dementia, lung cancer, T2D and type 1 diabetes (T1D), colorectal cancer, renal failure (including acute, chronic and of any cause) and breast cancer in women (Table B in S1 Text). In addition, we included infertility, non-alcoholic fatty liver disease (NAFLD) and chronic liver disease (CLD) as they have previously been linked to obesity and represent important and increasing burdens of disease [30–36]. For T2D and T1D, we drew case definitions from a validated algorithm for prevalent T2D and T1D (using “probable” and “possible” cases) and those the algorithm denoted as “diabetes unlikely” were used as controls [37]. For CAD, we used the same case and control definitions as a large GWAS [38]. Case and control criteria for the other disease outcomes were defined using self-reported data, data from an interview with a trained nurse, and hospital health outcome codes (also including death and cancer registry) in discussion between two licensed medical practitioners (Table B in S1 Text). For CAD, acute renal failure, chronic renal failure, stroke of any cause, ischemic stroke and hemorrhagic stroke, exclusions for certain codes were also made in the control groups after defining the case groups. All available information was used to decide on case and control status (except for diabetes), including information collected after the baseline assessment (including repeat assessments and hospital health outcome codes).
Outcomes: Risk factors
To assess the relationship of obesity traits with risk factors that might mediate the disease associations, we also investigated associations between the obesity traits and the cardiometabolic risk factors systolic blood pressure (SBP), diastolic blood pressure (DBP), fasting glucose (FG), fasting insulin (FI), and smoking status.
The mean of the baseline measurements was used for SBP and DBP. Fifteen mmHg to SBP and 10 mmHg to DBP were added if blood pressure lowering medications were used (defined as self-reported use of such in data-fields 6153 and 6177), as in previous blood pressure GWASs and as suggested in simulation studies [39,40]. We then standardized the blood pressure traits by rank inverse normal transformation of the residuals after regression of the trait on baseline age, age2, assessment centre, and, if applicable, sex. This was done separately in the men and women only analyses, but jointly in the combined analyses, after any sample quality exclusions (S1 Text).
Smoking status was defined as self-report of being a current or previous smoker or having smoked or currently smoking (most days or occasionally; any code 1 or 2 in any of the data fields 1239, 1249, and 20116 for the baseline assessment).
Sex-specific summary-level data for plasma FG (in mmol/L, untransformed, corrected to plasma levels using a correction factor of 1.13 if measured in whole blood in the original GWAS) and serum FI (in pmol/L, ln-transformed) were kindly provided by the Meta-Analyses of Glucose and Insulin-related traits Consortium (MAGIC) investigators and can be downloaded from https://www.magicinvestigators.org/downloads/ [41]. SNPs in chromosome:position format were converted to rsIDs using the file All_20150605.vcf.gz from the National Center for Biotechnology Information (NCBI) [42] (available at ftp://ftp.ncbi.nih.gov/snp/organisms/archive/human_9606_b144_GRCh37p13/VCF/). All SNPs were then updated to dbSNP build 151 using the file RsMergeArch.bcp.gz, also from the NCBI [42] (available at ftp://ftp.ncbi.nlm.nih.gov/snp/organisms/human_9606/database/organism_data/).
Statistical analyses: Evaluation of instruments
The GRSs were first assessed if they were robustly associated with their respective obesity traits by computing trait variance explained and the F-statistics using linear regression (Table C in S1 Text). Adjustments were made for array type and 10 PCs, as we had previously adjusted for age, age2, assessment centre, and if applicable sex and BMI, in the rank inverse normal transformation of the obesity traits. Sexual heterogeneity was assessed using Cochran’s Q test [43], with the Phet-threshold set at <0.002 (= 0.05/21) for 21 male-female instrument comparisons.
Statistical analyses: Primary association testing
We then explored the associations of the sex-specific GRSs with diseases and risk factors available in the UK Biobank to see if there were any indications of a causal relationship between the obesity traits and the outcomes [44]. Logistic regression was used for disease outcomes and smoking status and linear regression was used for SBP and DBP. Adjustments were made for baseline age, age2, array type, assessment centre, 10 principal components, and sex if applicable, for all traits when in clinical units and for binary outcomes, and array and 10 principal components if rank inverse normal transformed (where adjustment for age, age2, assessment centre, and if applicable sex had already been performed in the rank inverse normal transformation of the residuals).
Associations between the sex-specific GRSs with outcome traits that surpassed our P-value thresholds were taken forward for MR to more formally quantify the effect of the obesity trait on the outcome. For the obesity trait-disease analyses, the P-value threshold was set at <0.001 (= 0.05/51) for 51 obesity trait-disease combinations investigated in the study. For the obesity trait-risk factor analyses, the P-value threshold was set at <0.003 (= 0.05/15), for the total of 15 obesity trait-risk factor combinations investigated in the study (as we also assessed fasting glucose and fasting insulin using summary data). If a combined-sexes regression analysis identified evidence against the null hypothesis it was taken forward for MR; if a regression analysis identified evidence against the null hypothesis in either men or women, MR was performed in both the men and women-only stratified analyses so sexual heterogeneity could be assessed. Since we conducted the MR analyses both with and without adjusting for smoking status, we conducted MRs for all obesity traits with smoking status for completeness.
Statistical analyses: Secondary computation of MR estimates
Individual-level MR was performed using the Wald method, with the instrumental variable estimate being the ratio between the computed betas for the outcome and risk factor regressed separately on each GRS [45]. In this step, logistic regression was used for binary outcomes using the log(odds ratio(OR)) in the ratio and linear regression used for continuous outcomes. For the binary outcomes, MR regressions of the obesity traits on the GRSs were performed only including the controls for each outcome. Standard errors were adjusted to take the uncertainty in both regressions into account by using the first two terms of the delta method [44,46,47].
Adjustments were made for baseline age, age2, array type, assessment centre, 10 principal components, and sex if applicable, for all traits when in clinical units and for binary outcomes, and array and 10 principal components if rank inverse normal transformed (where adjustment for age, age2, assessment centre, and if applicable sex had already been performed in the rank inverse normal transformation of the residuals).
For the obesity trait-disease analyses, the P-value threshold was set at <0.001 (= 0.05/51) for the total of 51 obesity trait-disease combinations investigated in the study. For the obesity trait-risk factor analyses, the P-value threshold was set at <0.003 (= 0.05/15), for the total of 15 obesity trait-risk factor combinations investigated in the study.
Statistical analyses: 2-sample Mendelian randomization
We performed 2-sample summary-level MRs for the potential risk factors FG and FI directly, as we only had summary-level data for these traits. The main estimates were computed using the inverse-variance weighted (IVW) method. We then computed MR-Egger and weighted median estimates as a sensitivity analysis [48–51]. The P-value threshold was set at <0.003 (= 0.05/15) for the total of 15 obesity trait-risk factor combinations investigated in the study (including individual-level MRs for DBP, SBP, and smoking status).
Statistical analyses: Assessment of sexual heterogeneity
Sexual heterogeneity between male and female estimates from the regressions and the MRs was assessed using P-values from Cochran’s Q test [43]. To facilitate comparisons between the obesity traits and sex-strata, MR estimates were computed per 1 standard deviation (SD) higher obesity trait. The Phet-threshold for obesity trait-disease analyses was set at <0.001 (= 0.05/48) for 48 male-female estimates comparisons, since breast cancer was investigated in women only. For the obesity trait-risk factor analyses, the Phet-threshold was set at <0.003 (= 0.05/15) for the 15 male-female estimates comparisons.
Sensitivity analyses
We performed several sensitivity analyses to ascertain robustness; we conducted (a) analyses adjusting for smoking status and (b) analyses restricted to those of genetically confirmed British ancestry only (S1 Text). We also (c) evaluated the robustness of the MR findings by comparing different weighting strategies, including use of unweighted and externally weighted (using weights from the GIANT 2015 studies [20,21]) GRSs, and (d) investigated for pleiotropy and performed more pleiotropy-robust sensitivity analyses [50,51] (S1 Text). We also (e) performed logistic regressions using the same number of cases and controls in men and women for the disease outcomes and (f) conducted analyses using stricter T2D and T1D case definitions (S1 Text). In addition, we (g) recomputed the MR estimates for the obesity trait-disease combinations with evidence of sexual heterogeneity using additional SNP-selection and weighting approaches (S1 Text).
Software
The diabetes case and control definition scripts were kindly provided by the authors to ‘Algorithms for the Capture and Adjudication of Prevalent and Incident Diabetes in UK Biobank’ [37]. The other code and GRSs related to this project will be available at https://github.com/lindgrengroup/causal.relationships.between.obesity.and.leading.causes.of.death.in.men.and.women. The genotype data was handled using PLINK v2.00aLM and PLINK v1.90b3 [28] (S1 Text). Further data handling was performed in Python 3.5.2 [52] using the packages “pandas” [53] and “numpy” [54], R version 3.4.3 [55] and the package “dplyr” [56], bash version 4.1.2(2) [57] and awk [58]. Statistical analyses and plots were performed using R version 3.4.3 [55] and packages “ggplot2” [59], “mada” [60], “dplyr” [56], “gridExtra” [61], “lattice” [62], “grid” [55], “grDevices” [55], “ggpubr” [63], and “MendelianRandomization” [48].
Results
Evaluation of genetic risk scores
The three GRSs included 565 SNPs for BMI, 324 for WHR and 337 for WHRadjBMI. Trait variance explained varied between 2.5–7.1% and the F-statistic between 4,921–26,466, depending on trait and sex-stratum (Table C in S1 Text).
Primary association testing: Disease outcomes and risk factors
We first assessed the associations of the GRSs with diseases and risk factors using linear or logistic regression (Table D-F and Fig C in S1 Text). Obesity GRSs were associated with diabetes, CAD, COPD, lung cancer, stroke (of any cause and ischemic), renal failure, liver diseases, as well as blood pressure traits (Table D-F and Fig C in S1 Text). Several instruments also associated with smoking status and with higher estimate magnitudes in men than in women for both BMI and WHR (BMI: Phet = 2.2×10−4; WHR: Phet = 8.0×10−14; WHRadjBMI Phet = 0.008) (Table E in S1 Text). The GRS-outcome (diseases and risk factors) associations that surpassed correction for multiple testing were taken forward for MR to compute formal estimates of effect–if surpassed in one sex only, both men and women-only stratified analyses were conducted so that sexual heterogeneity could be assessed.
No obesity GRS showed evidence for association in any sex-strata for colorectal cancer, breast cancer (investigated in women only), dementia, hemorrhagic stroke, and infertility, and these endpoints were therefore not taken forward for computation of formal MR estimates (Table F and Fig C in S1 Text).
Mendelian randomization of obesity with disease outcomes: All individuals
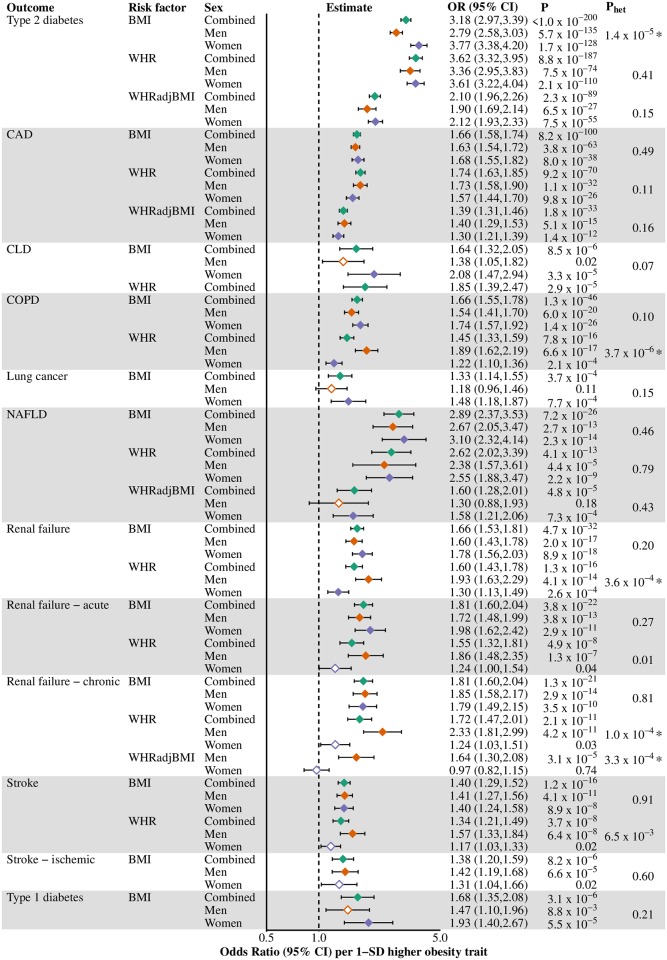
Obesity traits were causally implicated with diseases that represent the major causes of death (Figs 3 and 4). All measures of obesity were strongly causally related to risk of CAD OR ranging from 1.39 for WHRadjBMI to 1.74 for WHR in the combined analyses per 1-SD higher obesity trait). For stroke, both BMI and WHR conferred higher risk (ORs 1.40 and 1.34, respectively). Strong effects were seen for all obesity traits with T2D (OR range 2.10 to 3.62) and BMI also associated with risk of T1D (OR 1.68), with highly similar results using stricter diabetes type criteria (S1 Text). Obesity traits increased the risk of kidney disease, including both acute (ORs 1.55 for WHR and 1.81 for BMI) and chronic (ORs 1.72 for WHR and 1.81 for BMI) renal failure. Strong effects were also seen for risk of NAFLD (OR range 1.60–2.89) and CLD (ORs 1.64 for BMI and 1.85 for WHR).
Fig 3. Causal effects of obesity traits on disease outcomes, overall and stratified by sex.
Endpoints that showed an association with obesity GRSs were taken forward for Mendelian randomization, with estimates reported as odds ratio (95% CI) per 1-SD higher obesity trait. Filled diamonds indicate that the P-value for the obesity trait to disease endpoint surpasses our threshold for multiple testing; empty diamonds indicate that the P-value does not surpass this threshold (Bonferroni-adjusted P-value-threshold set at <0.001 (= 0.05/51) for 51 obesity trait-disease outcome combinations in the study). * denotes that the P-value for heterogeneity (from Cochran’s Q test) surpasses our threshold for multiple testing; Phet-threshold set at <0.001 (= 0.05/48) for 48 male-female comparisons in the study (fewer since breast cancer analyses were performed in women only). Green diamond, combined-sexes estimates; orange diamond, male estimates; purple diamond, female estimates; BMI, body mass index; CAD, coronary artery disease; COPD, chronic obstructive pulmonary disease; NAFLD, non-alcoholic fatty liver disease; SD standard deviation; WHR, waist-hip-ratio; WHRadjBMI, waist-hip-ratio adjusted for body mass index.
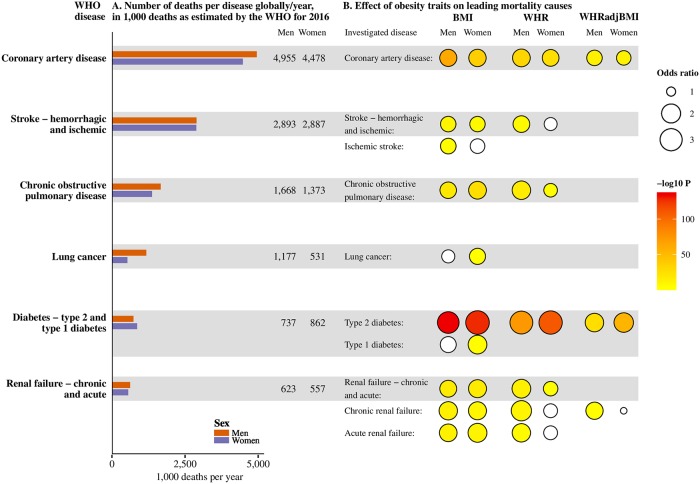
Fig 4. Overview of the sex-specific effect magnitudes and strengths of association of obesity traits on leading causes of death.
Leading causes of death defined as non-communicable diseases on the WHO top 10 lists of causes of death, globally and in high-income countries, with additional separate analyses for subclasses of stroke, diabetes, and renal disease. No obesity trait (BMI, WHR, or WHRadjBMI) genetic risk score associated with dementia, colorectal cancer, breast cancer (investigated in women only) or hemorrhagic stroke–these are not shown on the plot (for the regression results see Table F in S1 Text). (A) Total number of deaths globally, in 1,000 deaths, as estimated by the WHO for 2016 [64], stratified by sex. For diabetes, estimates for annual number of deaths are for type 1 and type 2 diabetes combined. (B) Obesity trait-disease combinations taken forward for Mendelian randomization showed with circles. Mendelian randomization associations with P-values surpassing our threshold in yellow to red fill depending on P-value (-log10 P-value), white fill indicates a P-value not surpassing our threshold. The size of the circles corresponds to the magnitude of the odds ratio estimate for the Mendelian randomization estimate. Estimates and P-values from the MR analyses of the obesity traits with the disease outcomes using the sex-specific estimates approach. BMI, body mass index; P, P-value; WHR, waist-hip-ratio; WHRadjBMI, waist-hip-ratio adjusted for body mass index; WHO, World Health Organization.
Measures of obesity also causally impacted on risks of COPD (OR 1.66 for BMI and 1.45 for WHR) and lung cancer (BMI OR 1.33). As several GRSs had associated with smoking status, we repeated the individual-level MRs adjusting for smoking status to assess potential mediation. Whereas most obesity-disease associations were largely similar, adjusting for smoking status resulted in diminished magnitudes of effect for COPD and lung cancer, suggesting potential mediation (Table G in S1 Text).
Sensitivity analyses, including restricting to those of genetically confirmed British ancestry only, use of different weighting strategies, analyses using more pleiotropy-robust methods, using the same number of cases and controls in men and women, and use of more stringent diabetes case definitions supported the main findings (Tables H,I and Fig D-F in S1 Text).
Mendelian randomization of obesity with disease outcomes: Sex-stratified analyses
Five out of the 24 obesity trait-disease associations differed between women and men (Fig 3). The effect of BMI on T2D risk was higher in women than men, with strong evidence for sexual heterogeneity (women: OR 3.77; 95% CI 3.38–4.20, P = 1.7×10−128; men: OR 2.79; 95% CI 2.58–3.03, P = 5.7×10−135, per 1-SD higher BMI, Phet = 1.4×10−5). This sexual heterogeneity could also be observed in sensitivity analyses where the number of cases in women and men was similar (Phet = 5.6×10−6) (Table I in S1 Text) and when performing the analysis using stricter T2D diagnosis criteria (Phet = 3.5×10−5) (S1 Text).
The estimate for the effect of higher WHR on COPD risk was greater in men than in women (men: OR 1.89; 95% CI 1.62–2.19, P = 6.6×10−17; and women: OR 1.22; 95% CI 1.10–1.36, P = 2.1×10−4, per 1-SD higher BMI, Phet = 3.7×10−6). Similarly, higher WHR was also associated with a greater risk of being a smoker in men than in women (Phet = 2.2×10−14) (Table J in S1 Text). Despite this, the effect estimates for the effect of WHR on COPD risk remained higher in men after adjusting for smoking (Phet = 8.8×10−5) (Table G in S1 Text).
There was also evidence of higher WHR increasing the risk of renal failure more in men than in women (Phet = 3.6×10−4). This sexual heterogeneity may originate from a risk difference in the effect of WHR on chronic renal failure, as men had higher risk estimates than women in that analysis (Phet = 1.0×10−4, with a similar sexual heterogeneity seen in the effect of WHRadjBMI). A 1-SD higher WHR was also associated with higher magnitudes of risk for acute renal failure in men than women, although the Phet-value did not pass our Phet-threshold (men: OR 1.86; 95% CI 1.48–2.35, P = 1.3×10−7; women: OR 1.24; 95% CI 1.00–1.54, P = 0.04, Phet = 0.01).
Sensitivity analyses using different GRS weighting strategies strongly supported sex-differences in the effect of BMI on T2D and WHR on chronic renal failure and COPD, but only weakly supported a sex-difference in the effect of WHR on renal failure of any cause (Fig D,E and G-I in S1 Text).
Potential mechanisms
To identify associations of obesity markers with risk factors that could mediate the disease risks, we assessed the relationship of obesity traits with blood pressure (SBP, DBP), glycemic traits (FG, FI), and smoking status (Figs 5 and 6, Tables J-N in S1 Text). All obesity traits causally increased SBP, DBP, FG and FI (Fig 5). The increase in DBP arising from elevated BMI was greater in women than men (Phet = 5.2×10−5).
Fig 5. Causal effects of obesity traits on continuous risk factors, overall and stratified by sex.
The obesity-risk factor combinations brought forward for Mendelian randomization. Estimates in plasma mmol/L levels for FG, serum pmol/L levels (ln-transformed) for FI and SD-units for SBP and DBP, per 1-SD higher obesity trait. Filled diamonds indicate that the P-value for the obesity trait to risk factor endpoint surpasses our threshold for multiple testing; empty diamonds indicate that the P-value does not surpass this threshold (Bonferroni-adjusted P-value-threshold set at <0.003 (= 0.05/15) for 15 obesity trait-risk factor combinations in the study). * denotes that the P-value for heterogeneity (from Cochran’s Q test) surpasses our threshold for multiple testing; Phet-threshold set at <0.003 (= 0.05/15). Green diamond, combined-sexes estimates; orange diamond, male estimates; purple diamond, female estimates; BMI, body mass index; DBP, diastolic blood pressure; FG, fasting glucose; FI, fasting insulin; SBP, systolic blood pressure; WHR, waist-hip-ratio; WHRadjBMI, waist-hip-ratio adjusted for body mass index.
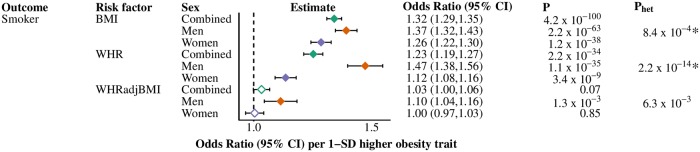
Fig 6. Causal effects of obesity traits on having been or being a smoker, overall and stratified by sex.
Estimates given in odds ratio (95% CI) per 1-SD higher obesity trait. Filled diamonds indicate that the P-value for the obesity trait to disease endpoint surpasses our threshold for multiple testing; empty diamonds indicate that the P-value does not surpass this threshold (Bonferroni-adjusted P-value-threshold set at <0.003 (= 0.05/15) for 15 obesity trait-risk factor combinations in the study). * denotes that the P-value for heterogeneity (from Cochran’s Q test) surpasses our threshold for multiple testing; Phet-threshold set at <0.003 (= 0.05/15). Green diamond, combined-sexes estimates; orange diamond, male estimates; purple diamond, female estimates; BMI, body mass index; SD standard deviation; WHR, waist-hip-ratio; WHRadjBMI, waist-hip-ratio adjusted for body mass index.
We computed MR estimates for smoking status in all sex-strata for completeness, since we performed MRs adjusted for smoking status as a sensitivity analysis. BMI and WHR both associated with higher risk of being a smoker, with the effect magnitudes being larger in men than women (BMI Phet = 8.4×10−4; WHR Phet = 2.2×10−14) (Fig 6). WHRadjBMI was only associated with smoking status in men.
Discussion
Our work shows that obesity is causally implicated in the etiology of two thirds of the globally leading causes of death from non-communicable diseases [29]. Furthermore, we identify that for some diseases, obesity conveys altered magnitudes of risk in men and women. Such sexual dimorphism could be observed in the effects of BMI on T2D and waist-related traits on COPD and renal failure. These findings have potential implications for public health policy.
Diabetes
Obesity traits were causally related to higher risk of T2D, in keeping with previous studies [6–11,19,65]. We could not detect a sex difference in risk of T2D from higher WHR or WHRadjBMI. Even though some observational studies have suggested that WHR may be a stronger predictor of T2D risk in women than in men [18,19], studies investigating the effect on T2D risk from genetic predisposition to higher WHRadjBMI have not found evidence of sexual heterogeneity [6,9,11]. In contrast, we found that BMI conferred a higher T2D risk in women than in men. Whereas men tend to be diagnosed with T2D at lower BMI than women [66], there may be a stronger association between increase of BMI and T2D risk in women than in men [15,18,65,67–70]. Whether this reflects a stronger causal effect of BMI on T2D risk in women has hitherto been unknown. There was no evidence for sexual heterogeneity of the causal effect of BMI on potential glycemic trait risk mediators (FG and FI). There have been indications of higher BMI being observationally associated with lower insulin sensitivity more in men than in women, but this observed sex-difference may not reflect a causal pathway or we are not capturing it by our glycemic measurements [71–73]. We also found evidence of BMI causally increasing risk of T1D. Previous observational [74] and MR [75] studies have implicated childhood BMI in risk of T1D. As SNPs associated with adult BMI have also been found to affect childhood BMI [75,76], our results may reflect the consequences of childhood BMI on T1D rather than adult BMI. The results were robust to use of stricter diabetes case definition criteria, minimizing risk of erroneous findings due to misclassification of diabetes type.
Cardiovascular disease
All obesity traits increased risk of CAD in both sexes, with no difference detected in the magnitude of effect between women and men. The associations with risk of CAD in men and women combined are consistent with previous studies [4,6–8,10,11,15,17]. While observational studies have indicated that waist-related traits may be more strongly associated with cardiovascular disease in women than men, they have not been conclusive [15,17,77,78]. However, a recent study [11] investigated the effect of higher WHRadjBMI, lower gluteofemoral fat distribution, and higher abdominal fat distribution, proxied by genetic variants, on CAD and T2D risk and found no evidence that relationships differed between men and women, similar to our findings. BMI and WHR have previously been observationally associated with risk of stroke [79–81] and a previous MR study found a causal effect of BMI on ischemic stroke [82]. However, some studies have found WHR to be an epidemiological risk factor for stroke in men only [79,80]. Our results confirm BMI as a causal risk factor for stroke (and particulary ischaemic stroke) in both men and women. In women, the effects of WHR were directionally consistent with harm, but the estimates were imprecise, probably reflecting insufficient power in the sex-stratified analysis.
Lung disease
BMI and WHR increased the risk of COPD and BMI increased the risk of lung cancer; a likely common mechanism is smoking. BMI has previously been implicated in the aetiology of COPD, but is not an established epidemiological risk factor [7,83–85]. Obesity may directly contribute to COPD as its diagnosis is partly based on spirometry values, and obesity is associated with lower lung function [85,86]. Higher BMI also increased risk of lung cancer in our study, similar to a previous MR study [87]. Observational studies tend to identify associations between smoking and lower body weight, but whereas smoking lowers body weight, higher BMI is associated with increased smoking [87–90]. We found associations between particularly BMI and WHR with smoking propensity. To assess mediation, we therefore conducted analyses adjusting for smoking status. This attenuated the associations between the obesity markers and risks of COPD and lung cancer, providing some evidence that smoking may lie on the causal pathway between obesity and lung disease. This diminution does not discredit the validity of the MR analyses unadjusted for smoking provided that the obesity instruments only affect smoking propensity through altered obesity [91]. Rather, they suggest that higher BMI impacts on disease beyond the immediate physiological effects of obesity: by altering human behavior (i.e. increased smoking, possibly motivated as a weight loss strategy [92,93]) and this increased propensity to smoking has additional, far-reaching, deleterious effects on human health, as evidenced by the higher risks of serious lung disease. Higher WHR was associated with greater risks of both COPD and being a smoker in men than in women. Whilst the sex difference in the effect of WHR on COPD persisted after adjustment for smoking status, we cannot rule out that WHR has a higher effect on COPD in men than women through its effect on smoking propensity, but that our smoking phenotype does not fully capture the life-long effects of smoking in men as compared to women.
Kidney disease
Our results also provide further evidence for a causal role of obesity traits in both acute and chronic renal disease—previous MR studies assessing these relationships have not been conclusive [6,7,94–96]. Obesity may affect chronic renal disease through a number of mechanisms, including structural changes in the kidney, higher blood pressure and through higher risks of mediating diseases, such as T2D [96–99]. We found central fat distribution (as measured by WHR and WHRadjBMI) to have higher effects on chronic renal failure in men than in women, with evidence of sexual heterogeneity, but the reason for this sex difference is unclear.
Liver disease
Obesity traits associated with increased risk of NAFLD and CLD (important and emerging causes of chronic disease and mortality [32–35]), with the effect of obesity on CLD possibly mediated by NAFLD [33]. A previous MR study found BMI to increase hepatic triglyceride content [100]. Our study confirms a role of both general obesity and central fat distribution in NAFLD and CLD using an MR design. This strengthens evidence of a causal effect and, given that the prevalence of NAFLD is on the rise (with an estimated one billion people affected globally [101]), emphasizes the potential of an increased burden of CLD as a consequence of global obesity [1,32–35].
Other diseases
No obesity GRS showed evidence of association in any sex-strata for colorectal cancer, dementia, hemorrhagic stroke, breast cancer (investigated in women only) and infertility. Whereas this may be due to obesity traits not having an effect on these diseases, there are also other potential explanations. For example, previous observational studies have indicated that higher BMI may be protective in premenopausal breast cancer but harmful in postmenopausal breast cancer [102,103]. It is thus possible that opposing effect directions of BMI on breast cancer risk depending on menopausal state counteract each other in our study. For some diseases, it may be that we have too few cases to detect an association. For example, previous MR studies found evidence in support of a causal role of BMI with risk of colorectal cancer but used larger sample sizes [104,105], meaning that our findings may be false negatives due to inadequate statistical power: we also had relatively few cases for dementia, hemorrhagic stroke, and infertility.
Strengths and limitations
Genetic instruments should only affect the outcome through the risk factor of interest and not through any confounders [106,107]. We performed sensitivity analyses (MR-Egger, weighted-median based methods) more robust to such bias, which supported the main findings [50,51].
If instruments are weakly associated with their respective traits, it can introduce bias in MR studies [108]. We therefore only used instruments strongly associated with their respective risk factor, and performed sensitivity analyses using a variety of SNP-selection and weighting approaches, including unweighted and externally weighted scores, which also supported the main results [44,108,109]. These sensitivity analyses and the strict P-value threshold to denote evidence in support of the presence of sexual heterogeneity should also lessen the risk of the observed sex-differences being due to winner’s curse, although such bias cannot be completely ruled out.
Recent studies have also indicated that there may be slight population stratification in both GIANT and UK Biobank, although such bias is likely to be minor [110,111]. Our study was restricted to individuals of Europeans ancestry; limiting our analyses to those of British ancestry only, yielded near-identical results. Associations between the obesity traits and outcomes may differ in other ancestries.
It is possible that our genetic instrument for WHRadjBMI might show features of collider bias whereby SNPs included in the GRS associate with both higher WHR and lower BMI leading to potentially spurious findings [112]. We note that a recent GWAS [14] evaluated the potential for collider bias in the WHRadjBMI GWAS and found limited evidence for such, although the GRS was associated with higher WHR and lower BMI. The directional consistency of associations between WHR and WHRadjBMI and disease endpoints in our analysis suggests that collider bias is unlikely to represent a major source of error in this study.
Most MR studies to date have weighted instruments for the exposure by estimates derived from analyses in which women and men were combined and thus investigated the average causal effect of both sexes. However, this may obscure causal effects that differ between women and men, and can, in addition, cause less precise estimates [109] or an over/underestimation of the effect of the instrument on the exposure in each sex. Our results indicate that weighting SNPs by their sex-specific estimates improves instrument strength and precision compared to using weights derived in a combined-sexes sample. While the work we perform makes important inroads into the development of sex-specific Mendelian randomization approaches, we recognize that, for example, imbalances in the proportion of women and men in included studies, differential availability of summary-level sex-stratified GWAS data and the potential for biases to operate differentially between women and men pose additional complexities in deciphering underlying causal effects.
Conclusion
Our results implicate obesity in the etiology of the leading causes of death globally, including CAD, stroke, type 2 and 1 diabetes, COPD, lung cancer and renal failure, as well as NAFLD and CLD. This increased risk arising from obesity differs between men and women for T2D, renal failure and COPD. Our findings emphasize the importance of improved preventative measures and treatment of obesity-related disorders and implies that women and men may experience different disease sequelae from obesity, with potential implications for provision of health services and public health policy.
Supporting information
(DOCX)
(XLSX)
Acknowledgments
Computation used the Oxford Biomedical Research Computing (BMRC) facility, a joint development between the Wellcome Centre for Human Genetics and the Big Data Institute supported by Health Data Research UK and the NIHR Oxford Biomedical Research Centre. The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health.
We thank the UK Biobank (application 11867; http://www.ukbiobank.ac.uk/).
Data Availability
Summary-level data for fasting glucose and fasting insulin can be downloaded from https://www.magicinvestigators.org/downloads/. Individual-level data from UK Biobank cannot be shared publicly because of confidentiality but is available from the UK Biobank (https://www.ukbiobank.ac.uk/) for researches who meet the criteria for access to confidential data. The diabetes case and control definition scripts were kindly provided by the authors to ‘Algorithms for the Capture and Adjudication of Prevalent and Incident Diabetes in UK Biobank’ (pone.0162388). The other code and GRSs related to this project will be available at https://github.com/lindgrengroup/causal.relationships.between.obesity.and.leading.causes.of.death.in.men.and.women. All other relevant data are within the manuscript and its supporting information files.
Funding Statement
JCC is funded by an NDM Prize Studentship (17/18_MSD_1108275) from the Oxford Medical Research Council Doctoral Training Partnership (Oxford MRC DTP; https://www.medsci.ox.ac.uk) and the Nuffield Department of Clinical Medicine (https://www.ndm.ox.ac.uk/), University of Oxford. SAEP is supported by a UK Medical Research Council Skills Development Fellowship (MR/P014550/1). JB is supported by funding from the Rhodes Trust (https://www.rhodeshouse.ox.ac.uk/), Clarendon Fund (http://www.ox.ac.uk/clarendon/about) and the Medical Sciences Doctoral Training Centre (https://www.medsci.ox.ac.uk/), University of Oxford. TF is supported by the NIHR Biomedical Research Centre, Oxford. SLP was funded by a Veni Fellowship (016.186.071; ZonMW; https://www.nwo.nl/) from the Dutch Organization for Scientific Research, Nederlandse Organisatie voor Wetenschappelijk Onderzoek (NWO) during the course of the study. MVH works in a unit that receives funding from the Medical Research Council (MRC; https://mrc.ukri.org/) and is supported by a British Heart Foundation Intermediate Clinical Research Fellowship (FS/18/23/33512; https://www.bhf.org.uk/) and the National Institute for Health Research Oxford Biomedical Research Centre (https://oxfordbrc.nihr.ac.uk). CML is supported by the Li Ka Shing Foundation (https://www.lksf.org/), WT-SSI/John Fell funds (https://researchsupport.admin.ox.ac.uk/), the National Institute for Health Research Biomedical Research Centre, Oxford (https://oxfordbrc.nihr.ac.uk/), Widenlife (H2020-TWINN-2015-692065; https://cordis.europa.eu/), and National Institute of Health (NIH; 5P50HD028138-27; https://www.nih.gov/). Computation used the Oxford Biomedical Research Computing (BMRC) facility, a joint development between the Wellcome Centre for Human Genetics and the Big Data Institute supported by Health Data Research UK and the NIHR Oxford Biomedical Research Centre, and with financial support provided by the Wellcome Trust Core Award Grant Number 203141/Z/16/Z. The funders had not role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
References
- 1.GBD 2015 Obesity Collaborators, Afshin A, Forouzanfar MH, Reitsma MB, Sur P, Estep K, et al. Health Effects of Overweight and Obesity in 195 Countries over 25 Years. N Engl J Med. 2017;377: 13–27. 10.1056/NEJMoa1614362 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Seidell JC, Oosterlee A, Thijssen MA, Burema J, Deurenberg P, Hautvast JG, et al. Assessment of intra-abdominal and subcutaneous abdominal fat: relation between anthropometry and computed tomography. Am J Clin Nutr. 1987;45: 7–13. 10.1093/ajcn/45.1.7 [DOI] [PubMed] [Google Scholar]
- 3.Prospective Studies Collaboration. Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009;373: 1083–1096. 10.1016/S0140-6736(09)60318-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Taylor AE, Ebrahim S, Ben-Shlomo Y, Martin RM, Whincup PH, Yarnell JW, et al. Comparison of the associations of body mass index and measures of central adiposity and fat mass with coronary heart disease, diabetes, and all-cause mortality: a study using data from 4 UK cohorts. Am J Clin Nutr. 2010;91: 547–556. 10.3945/ajcn.2009.28757 [DOI] [PubMed] [Google Scholar]
- 5.WHO. Obesity: Preventing and Managing the Global Epidemic Report of a WHO consultation. Geneva: World Health Organization; 2000. [PubMed] [Google Scholar]
- 6.Emdin CA, Khera AV, Natarajan P, Klarin D, Zekavat SM, Hsiao AJ, et al. Genetic Association of Waist-to-Hip Ratio With Cardiometabolic Traits, Type 2 Diabetes, and Coronary Heart Disease. JAMA. 2017;317: 626–634. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Millard LAC, Davies NM, Tilling K, Gaunt TR, Davey Smith G. Searching for the causal effects of body mass index in over 300 000 participants in UK Biobank, using Mendelian randomization. Ripatti S, editor. PLOS Genet. 2019;15: e1007951 10.1371/journal.pgen.1007951 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Lyall DM, Celis-Morales C, Ward J, Iliodromiti S, Anderson JJ, Gill JMR, et al. Association of Body Mass Index With Cardiometabolic Disease in the UK Biobank. JAMA Cardiol. 2017;2: 882 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Huang T, Qi Q, Zheng Y, Ley SH, Manson JE, Hu FB, et al. Genetic Predisposition to Central Obesity and Risk of Type 2 Diabetes: Two Independent Cohort Studies. Diabetes Care. 2015;38: 1306–11. 10.2337/dc14-3084 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Dale CE, Fatemifar G, Palmer TM, White J, Prieto-Merino D, Zabaneh D, et al. Causal Associations of Adiposity and Body Fat Distribution With Coronary Heart Disease, Stroke Subtypes, and Type 2 Diabetes Mellitus: A Mendelian Randomization Analysis. Circulation. 2017;135: 2373–2388. 10.1161/CIRCULATIONAHA.116.026560 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Lotta LA, Wittemans LBL, Zuber V, Stewart ID, Sharp SJ, Luan J, et al. Association of Genetic Variants Related to Gluteofemoral vs Abdominal Fat Distribution With Type 2 Diabetes, Coronary Disease, and Cardiovascular Risk Factors. JAMA. 2018;320: 2553 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Finucane MM, Stevens GA, Cowan MJ, Danaei G, Lin JK, Paciorek CJ, et al. National, regional, and global trends in body-mass index since 1980: systematic analysis of health examination surveys and epidemiological studies with 960 country-years and 9·1 million participants. Lancet. 2011;377: 557–567. 10.1016/S0140-6736(10)62037-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Ng M, Fleming T, Robinson M, Thomson B, Graetz N, Margono C, et al. Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet (London, England). 2014;384: 766–81. 10.1016/S0140-6736(14)60460-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Pulit SL, Stoneman C, Morris AP, Wood AR, Glastonbury CA, Tyrrell J, et al. Meta-analysis of genome-wide association studies for body fat distribution in 694,649 individuals of European ancestry. Hum Mol Genet. 2018; 10.1093/hmg/ddy327 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Rost S, Freuer D, Peters A, Thorand B, Holle R, Linseisen J, et al. New indexes of body fat distribution and sex-specific risk of total and cause-specific mortality: a prospective cohort study. BMC Public Health. 2018;18: 427 10.1186/s12889-018-5350-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Lind L, Ärnlöv J, Lampa E. The Interplay Between Fat Mass and Fat Distribution as Determinants of the Metabolic Syndrome Is Sex-Dependent. Metab Syndr Relat Disord. 2017;15: 337–343. 10.1089/met.2017.0006 [DOI] [PubMed] [Google Scholar]
- 17.Dagenais GR, Yi Q, Mann JFE, Bosch J, Pogue J, Yusuf S. Prognostic impact of body weight and abdominal obesity in women and men with cardiovascular disease. Am Heart J. 2005;149: 54–60. 10.1016/j.ahj.2004.07.009 [DOI] [PubMed] [Google Scholar]
- 18.Meisinger C, Döring A, Thorand B, Heier M, Löwel H. Body fat distribution and risk of type 2 diabetes in the general population: are there differences between men and women? The MONICA/KORA Augsburg Cohort Study. Am J Clin Nutr. 2006;84: 483–489. 10.1093/ajcn/84.3.483 [DOI] [PubMed] [Google Scholar]
- 19.Wannamethee SG, Papacosta O, Whincup PH, Carson C, Thomas MC, Lawlor DA, et al. Assessing prediction of diabetes in older adults using different adiposity measures: a 7 year prospective study in 6,923 older men and women. Diabetologia. 2010;53: 890–898. 10.1007/s00125-010-1670-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Locke AE, Kahali B, Berndt SI, Justice AE, Pers TH, Day FR, et al. Genetic studies of body mass index yield new insights for obesity biology. Nature. 2015;518: 197–206. 10.1038/nature14177 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Shungin D, Winkler TW, Croteau-Chonka DC, Ferreira T, Locke AE, Mägi R, et al. New genetic loci link adipose and insulin biology to body fat distribution. Nature. 2015;518: 187–196. 10.1038/nature14132 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Sudlow C, Gallacher J, Allen N, Beral V, Burton P, Danesh J, et al. UK Biobank: An Open Access Resource for Identifying the Causes of a Wide Range of Complex Diseases of Middle and Old Age. PLOS Med. 2015;12: e1001779 10.1371/journal.pmed.1001779 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Bycroft C, Freeman C, Petkova D, Band G, Elliott LT, Sharp K, et al. The UK Biobank resource with deep phenotyping and genomic data. Nature. 2018;562: 203–209. 10.1038/s41586-018-0579-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Mccarthy S, Das S, Kretzschmar W, Delaneau O, Wood AR, Teumer A, et al. A reference panel of 64,976 haplotypes for genotype imputation. 2016;48 10.1038/ng.3643 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.The UK10K Consortium. The UK10K project identifies rare variants in health and disease. Nature. 2015;526: 82–90. 10.1038/nature14962 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Durbin RM, Altshuler DL, Durbin RM, Abecasis GR, Bentley DR, Chakravarti A, et al. A map of human genome variation from population-scale sequencing. Nature. 2010;467: 1061–1073. 10.1038/nature09534 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Yengo L, Sidorenko J, Kemper KE, Zheng Z, Wood AR, Weedon MN, et al. Meta-analysis of genome-wide association studies for height and body mass index in ∼700000 individuals of European ancestry. Hum Mol Genet. 2018;27: 3641–3649. 10.1093/hmg/ddy271 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Purcell S, Neale B, Todd-Brown K, Thomas L, Ferreira MAR, Bender D, et al. PLINK: A Tool Set for Whole-Genome Association and Population-Based Linkage Analyses. Am J Hum Genet. 2007;81: 559–575. 10.1086/519795 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.World Health Organization. The top 10 causes of death [Internet]. 2018 [cited 7 Jul 2018]. http://www.who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death
- 30.Campbell JM, Lane M, Owens JA, Bakos HW. Paternal obesity negatively affects male fertility and assisted reproduction outcomes: a systematic review and meta-analysis. Reprod Biomed Online. 2015;31: 593–604. 10.1016/j.rbmo.2015.07.012 [DOI] [PubMed] [Google Scholar]
- 31.van der Steeg JW, Steures P, Eijkemans MJC, Habbema JDF, Hompes PGA, Burggraaff JM, et al. Obesity affects spontaneous pregnancy chances in subfertile, ovulatory women. Hum Reprod. 2007;23: 324–328. 10.1093/humrep/dem371 [DOI] [PubMed] [Google Scholar]
- 32.Williams CD, Stengel J, Asike MI, Torres DM, Shaw J, Contreras M, et al. Prevalence of Nonalcoholic Fatty Liver Disease and Nonalcoholic Steatohepatitis Among a Largely Middle-Aged Population Utilizing Ultrasound and Liver Biopsy: A Prospective Study. Gastroenterology. 2011;140: 124–131. 10.1053/j.gastro.2010.09.038 [DOI] [PubMed] [Google Scholar]
- 33.Chalasani N, Younossi Z, Lavine JE, Diehl AM, Brunt EM, Cusi K, et al. The diagnosis and management of non-alcoholic fatty liver disease: Practice Guideline by the American Association for the Study of Liver Diseases, American College of Gastroenterology, and the American Gastroenterological Association. Hepatology. 2012;55: 2005–2023. 10.1002/hep.25762 [DOI] [PubMed] [Google Scholar]
- 34.Vernon G, Baranova A, Younossi ZM. Systematic review: the epidemiology and natural history of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis in adults. Aliment Pharmacol Ther. 2011;34: 274–285. 10.1111/j.1365-2036.2011.04724.x [DOI] [PubMed] [Google Scholar]
- 35.Estes C, Razavi H, Loomba R, Younossi Z, Sanyal AJ. Modeling the epidemic of nonalcoholic fatty liver disease demonstrates an exponential increase in burden of disease. Hepatology. 2018;67: 123–133. 10.1002/hep.29466 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Macaluso M, Wright-Schnapp TJ, Chandra A, Johnson R, Satterwhite CL, Pulver A, et al. A public health focus on infertility prevention, detection, and management. Fertil Steril. 2010;93: 16.e1–16.e10. 10.1016/J.FERTNSTERT.2008.09.046 [DOI] [PubMed] [Google Scholar]
- 37.Eastwood SV, Mathur R, Atkinson M, Brophy S, Sudlow C, Flaig R, et al. Algorithms for the Capture and Adjudication of Prevalent and Incident Diabetes in UK Biobank. Herder C, editor. PLoS One. 2016;11: e0162388 10.1371/journal.pone.0162388 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Nelson CP, Goel A, Butterworth AS, Kanoni S, Webb TR, Marouli E, et al. Association analyses based on false discovery rate implicate new loci for coronary artery disease. Nat Genet. 2017;49: 1385–1391. 10.1038/ng.3913 [DOI] [PubMed] [Google Scholar]
- 39.Tobin MD, Sheehan NA, Scurrah KJ, Burton PR. Adjusting for treatment effects in studies of quantitative traits: antihypertensive therapy and systolic blood pressure. Stat Med. 2005;24: 2911–2935. 10.1002/sim.2165 [DOI] [PubMed] [Google Scholar]
- 40.International Consortium for Blood Pressure Genome-Wide Association Studies, Ehret GB, Munroe PB, Rice KM, Bochud M, Johnson AD, et al. Genetic variants in novel pathways influence blood pressure and cardiovascular disease risk. Nature. 2011;478: 103–9. 10.1038/nature10405 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Lagou V, Mägi R, Hottenga J-JJ. Fasting glucose and insulin variability: sex-dimorphic genetic effects and novel loci. Prep. 2018; [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Sherry ST, Ward MH, Kholodov M, Baker J, Phan L, Smigielski EM, et al. dbSNP: the NCBI database of genetic variation. Nucleic Acids Res. 2001;29: 308–11. http://www.ncbi.nlm.nih.gov/pubmed/11125122 10.1093/nar/29.1.308 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Cochran W. The combination of estimates from different experiments. Biometrics. 1954;10: 101–29. [Google Scholar]
- 44.Burgess S, Thompson SG. Mendelian Randomization—Methods for Using Genetic Variants in Causal Estimation. 1st ed Boca Raton, FL, USA: CRC Press, Taylor & Francis Group, Chapman and Hall; 2005. [Google Scholar]
- 45.Wald A. The Fitting of Straight Lines if Both Variables are Subject to Error. Ann Math Stat. 1940;11: 284–300. 10.1214/aoms/1177731868 [DOI] [Google Scholar]
- 46.Bautista LE, Smeeth L, Hingorani AD, Casas JP. Estimation of Bias in Nongenetic Observational Studies Using “Mendelian Triangulation”. Ann Epidemiol. 2006;16: 675–680. 10.1016/j.annepidem.2006.02.001 [DOI] [PubMed] [Google Scholar]
- 47.Thomas DC, Lawlor DA, Thompson JR. Re: Estimation of Bias in Nongenetic Observational Studies Using “Mendelian Triangulation” by Bautista et al. Ann Epidemiol. 2007;17: 511–513. 10.1016/j.annepidem.2006.12.005 [DOI] [PubMed] [Google Scholar]
- 48.Yavorska OO, Burgess S. MendelianRandomization: an R package for performing Mendelian randomization analyses using summarized data. Int J Epidemiol. 2017;46: 1734–1739. 10.1093/ije/dyx034 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Burgess S, Butterworth A, Thompson SG. Mendelian randomization analysis with multiple genetic variants using summarized data. Genet Epidemiol. 2013;37: 658–65. 10.1002/gepi.21758 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Bowden J, Davey Smith G, Burgess S. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol. 2015;44: 512–525. 10.1093/ije/dyv080 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Bowden J, Davey Smith G, Haycock PC, Burgess S. Consistent Estimation in Mendelian Randomization with Some Invalid Instruments Using a Weighted Median Estimator. Genet Epidemiol. 2016;40: 304–14. 10.1002/gepi.21965 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Python Software Fondation. Python, version 3.5.2 [Internet]. https://www.python.org/
- 53.McKinney W. Data Structures for Statistical Computing in Python. Proc 9th Python Sci Conf. 2010; 51–56.
- 54.Oliphant TE. A guide to NumPy. USA: Trelgol Publishing; 2006. [Google Scholar]
- 55.R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria [Internet]. 2017. https://www.r-project.org/
- 56.Wickham H, Francois R, Henry L, Müller K. dplyr: A Grammar of Data Manipulation. R package version 0.7.4. 2017; https://cran.r-project.org/package=dplyr%0A
- 57.Free Software Foundation. bash 4.1.2(2) [Internet]. 2007. https://www.gnu.org/software/bash/
- 58.Free Software Foundation. GNU AWK 3.1.7 [Internet]. 1989. https://www.gnu.org/software/gawk/manual/gawk.html
- 59.Wickham H. ggplot2: Elegant Graphics for Data Analysis. New York: Springer-Verlag; 2009. [Google Scholar]
- 60.Doebler P. mada: Meta-Analysis of Diagnostic Accuracy. R package version 0.5.8. In: 2017 [Internet]. https://cran.r-project.org/package=mada%0A
- 61.Auguie B. gridExtra: Miscellaneous Functions for “Grid” Graphics. In: R package version 2.3 [Internet]. 2017. https://cran.r-project.org/package=gridExtra
- 62.Sarkar D. Lattice: Multivariate Data Visualization with R. New York: Springer; 2008. [Google Scholar]
- 63.Kassambara A. ggpubr: “ggplot2” Based Publication Ready Plots. In: R package version 0.1.7. 2018.
- 64.World Health Organization. Global Health Estimates 2016: Deaths by Cause, Age, Sex, by Country and by Region, 2000–2016. Geneva; 2018.
- 65.Vazquez G, Duval S, Jacobs DR, Silventoinen K. Comparison of Body Mass Index, Waist Circumference, and Waist/Hip Ratio in Predicting Incident Diabetes: A Meta-Analysis. Epidemiol Rev. 2007;29: 115–128. 10.1093/epirev/mxm008 [DOI] [PubMed] [Google Scholar]
- 66.Logue J, Walker JJ, Colhoun HM, Leese GP, Lindsay RS, McKnight JA, et al. Do men develop type 2 diabetes at lower body mass indices than women? Diabetologia. 2011;54: 3003–3006. 10.1007/s00125-011-2313-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Bray GA. Medical Consequences of Obesity. J Clin Endocrinol Metab. 2004;89: 2583–2589. 10.1210/jc.2004-0535 [DOI] [PubMed] [Google Scholar]
- 68.Kautzky-Willer A, Harreiter J, Pacini G. Sex and Gender Differences in Risk, Pathophysiology and Complications of Type 2 Diabetes Mellitus. Endocr Rev. 2016;37: 278–316. 10.1210/er.2015-1137 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Colditz GA, Willett WC, Rotnitzky A, Manson JE. Weight gain as a risk factor for clinical diabetes mellitus in women. Ann Intern Med. 1995;122: 481–6. http://www.ncbi.nlm.nih.gov/pubmed/7872581 10.7326/0003-4819-122-7-199504010-00001 [DOI] [PubMed] [Google Scholar]
- 70.Chan JM, Rimm EB, Colditz GA, Stampfer MJ, Willett WC. Obesity, fat distribution, and weight gain as risk factors for clinical diabetes in men. Diabetes Care. 1994;17: 961–9. http://www.ncbi.nlm.nih.gov/pubmed/7988316 10.2337/diacare.17.9.961 [DOI] [PubMed] [Google Scholar]
- 71.Sierra-Johnson J, Johnson BD, Bailey KR, Turner ST. Relationships between insulin sensitivity and measures of body fat in asymptomatic men and women. Obes Res. 2004;12: 2070–7. 10.1038/oby.2004.258 [DOI] [PubMed] [Google Scholar]
- 72.Masharani U, Goldfine ID, Youngren JF. Influence of gender on the relationship between insulin sensitivity, adiposity, and plasma lipids in lean nondiabetic subjects. Metabolism. 2009;58: 1602–8. 10.1016/j.metabol.2009.05.012 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Quon MJ. Limitations of the Fasting Glucose to Insulin Ratio as an Index of Insulin Sensitivity. J Clin Endocrinol Metab. 2001;86: 4615–4617. 10.1210/jcem.86.10.7952 [DOI] [PubMed] [Google Scholar]
- 74.Verbeeten KC, Elks CE, Daneman D, Ong KK. Association between childhood obesity and subsequent Type 1 diabetes: a systematic review and meta-analysis. Diabet Med. 2011;28: 10–18. 10.1111/j.1464-5491.2010.03160.x [DOI] [PubMed] [Google Scholar]
- 75.Censin JC, Nowak C, Cooper N, Bergsten P, Todd JA, Fall T. Childhood adiposity and risk of type 1 diabetes: A Mendelian randomization study. Langenberg C, editor. PLoS Med. 2017;14: e1002362 10.1371/journal.pmed.1002362 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Felix JF, Bradfield JP, Monnereau C, van der Valk RJP, Stergiakouli E, Chesi A, et al. Genome-wide association analysis identifies three new susceptibility loci for childhood body mass index. Hum Mol Genet. 2016;25: 389–403. 10.1093/hmg/ddv472 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Li C, Engström G, Hedblad B, Calling S, Berglund G, Janzon L. Sex differences in the relationships between BMI, WHR and incidence of cardiovascular disease: a population-based cohort study. Int J Obes. 2006;30: 1775–1781. 10.1038/sj.ijo.0803339 [DOI] [PubMed] [Google Scholar]
- 78.Dhana K, Kavousi M, Ikram MA, Tiemeier HW, Hofman A, Franco OH. Body shape index in comparison with other anthropometric measures in prediction of total and cause-specific mortality. J Epidemiol Community Health. 2016;70: 90–6. 10.1136/jech-2014-205257 [DOI] [PubMed] [Google Scholar]
- 79.Hu G, Tuomilehto J, Silventoinen K, Sarti C, Männistö S, Jousilahti P. Body Mass Index, Waist Circumference, and Waist-Hip Ratio on the Risk of Total and Type-Specific Stroke. Arch Intern Med. 2007;167: 1420 [DOI] [PubMed] [Google Scholar]
- 80.Abete I, Arriola L, Etxezarreta N, Mozo I, Moreno-Iribas C, Amiano P, et al. Association between different obesity measures and the risk of stroke in the EPIC Spanish cohort. Eur J Nutr. 2015;54: 365–375. 10.1007/s00394-014-0716-x [DOI] [PubMed] [Google Scholar]
- 81.The Global Burden of Metabolic Risk Factors for Chronic Diseases Collaboration (BMI Mediated Effects). Metabolic mediators of the effects of body-mass index, overweight, and obesity on coronary heart disease and stroke: a pooled analysis of 97 prospective cohorts with 1·8 million participants. Lancet. 2014;383: 970–983. 10.1016/S0140-6736(13)61836-X [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Hagg S, Fall T, Ploner A, Magi R, Fischer K, Draisma HH, et al. Adiposity as a cause of cardiovascular disease: a Mendelian randomization study. Int J Epidemiol. 2015;44: 578–586. 10.1093/ije/dyv094 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Vozoris NT, O’Donnell DE. Prevalence, risk factors, activity limitation and health care utilization of an obese, population-based sample with chronic obstructive pulmonary disease. Can Respir J. 2012;19: e18–24. 10.1155/2012/732618 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Hanson C, Rutten EP, Wouters EFM, Rennard S. Influence of diet and obesity on COPD development and outcomes. Int J Chron Obstruct Pulmon Dis. 2014;9: 723–33. 10.2147/COPD.S50111 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Vestbo J, Hurd SS, Agustí AG, Jones PW, Vogelmeier C, Anzueto A, et al. Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease. Am J Respir Crit Care Med. 2013;187: 347–365. 10.1164/rccm.201204-0596PP [DOI] [PubMed] [Google Scholar]
- 86.Bedell GN, Wilson WR, Seebohm PM. Pulmonary function in obese persons. J Clin Invest. 1958;37: 1049–60. 10.1172/JCI103686 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Carreras-Torres R, Johansson M, Haycock PC, Wade KH, Relton CL, Martin RM, et al. Obesity, metabolic factors and risk of different histological types of lung cancer: A Mendelian randomization study. Hu C, editor. PLoS One. 2017;12: e0177875 10.1371/journal.pone.0177875 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Morris RW, Taylor AE, Fluharty ME, Bjørngaard JH, Åsvold BO, Elvestad Gabrielsen M, et al. Heavier smoking may lead to a relative increase in waist circumference: evidence for a causal relationship from a Mendelian randomisation meta-analysis. The CARTA consortium. BMJ Open. 2015;5: e008808 10.1136/bmjopen-2015-008808 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Audrain-McGovern J, Benowitz NL. Cigarette smoking, nicotine, and body weight. Clin Pharmacol Ther. 2011;90: 164–8. 10.1038/clpt.2011.105 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Rásky E, Stronegger WJ, Freidl W. The relationship between body weight and patterns of smoking in women and men. Int J Epidemiol. 1996;25: 1208–12. http://www.ncbi.nlm.nih.gov/pubmed/9027526 10.1093/ije/25.6.1208 [DOI] [PubMed] [Google Scholar]
- 91.Burgess S, Scott RA, Timpson NJ, Davey Smith G, Thompson SG, EPIC- InterAct Consortium. Using published data in Mendelian randomization: a blueprint for efficient identification of causal risk factors. Eur J Epidemiol. 2015;30: 543–52. 10.1007/s10654-015-0011-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Chiolero A, Faeh D, Paccaud F, Cornuz J. Consequences of smoking for body weight, body fat distribution, and insulin resistance. Am J Clin Nutr. 2008;87: 801–809. 10.1093/ajcn/87.4.801 [DOI] [PubMed] [Google Scholar]
- 93.Fulkerson JA, French SA. Cigarette smoking for weight loss or control among adolescents: gender and racial/ethnic differences. J Adolesc Health. 2003;32: 306–13. http://www.ncbi.nlm.nih.gov/pubmed/12667735 10.1016/s1054-139x(02)00566-9 [DOI] [PubMed] [Google Scholar]
- 94.Geng T, Smith CE, Li C, Huang T. Childhood BMI and Adult Type 2 Diabetes, Coronary Artery Diseases, Chronic Kidney Disease, and Cardiometabolic Traits: A Mendelian Randomization Analysis. Diabetes Care. 2018;41: 1089–1096. 10.2337/dc17-2141 [DOI] [PubMed] [Google Scholar]
- 95.Todd JN, Dahlström EH, Salem RM, Sandholm N, Forsblom C, FinnDiane Study Group the FS, et al. Genetic Evidence for a Causal Role of Obesity in Diabetic Kidney Disease. Diabetes. 2015;64: 4238–46. 10.2337/db15-0254 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.van Zuydam NR, Ahlqvist E, Sandholm N, Deshmukh H, Rayner NW, Abdalla M, et al. A Genome-Wide Association Study of Diabetic Kidney Disease in Subjects With Type 2 Diabetes. Diabetes. 2018;67: 1414–1427. 10.2337/db17-0914 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Tsuboi N, Utsunomiya Y, Kanzaki G, Koike K, Ikegami M, Kawamura T, et al. Low glomerular density with glomerulomegaly in obesity-related glomerulopathy. Clin J Am Soc Nephrol. 2012;7: 735–41. 10.2215/CJN.07270711 [DOI] [PubMed] [Google Scholar]
- 98.Kovesdy CP, Furth SL, Zoccali C, World Kidney Day Steering Committee on behalf of the WKDS. Obesity and Kidney Disease: Hidden Consequences of the Epidemic. Can J kidney Heal Dis. 2017;4: 2054358117698669 10.1177/2054358117698669 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Hall ME, do Carmo JM, da Silva AA, Juncos LA, Wang Z, Hall JE. Obesity, hypertension, and chronic kidney disease. Int J Nephrol Renovasc Dis. 2014;7: 75–88. 10.2147/IJNRD.S39739 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Stender S, Kozlitina J, Nordestgaard BG, Tybjærg-Hansen A, Hobbs HH, Cohen JC. Adiposity amplifies the genetic risk of fatty liver disease conferred by multiple loci. Nat Genet. 2017;49: 842–847. 10.1038/ng.3855 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Loomba R, Sanyal AJ. The global NAFLD epidemic. Nat Rev Gastroenterol Hepatol. 2013;10: 686–690. 10.1038/nrgastro.2013.171 [DOI] [PubMed] [Google Scholar]
- 102.Al-Ajmi K, Lophatananon A, Ollier W, Muir KR. Risk of breast cancer in the UK biobank female cohort and its relationship to anthropometric and reproductive factors. Meyre D, editor. PLoS One. 2018;13: e0201097 10.1371/journal.pone.0201097 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Liu K, Zhang W, Dai Z, Wang M, Tian T, Liu X, et al. Association between body mass index and breast cancer risk: evidence based on a dose-response meta-analysis. Cancer Manag Res. 2018;10: 143–151. 10.2147/CMAR.S144619 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Jarvis D, Mitchell JS, Law PJ, Palin K, Tuupanen S, Gylfe A, et al. Mendelian randomisation analysis strongly implicates adiposity with risk of developing colorectal cancer. Br J Cancer. 2016;115: 266–272. 10.1038/bjc.2016.188 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Thrift AP, Gong J, Peters U, Chang-Claude J, Rudolph A, Slattery ML, et al. Mendelian Randomization Study of Body Mass Index and Colorectal Cancer Risk. Cancer Epidemiol Biomarkers Prev. 2015;24: 1024–1031. 10.1158/1055-9965.EPI-14-1309 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Greenland S. An introduction to instrumental variables for epidemiologists. Int J Epidemiol. 2000;29: 722–9. http://www.ncbi.nlm.nih.gov/pubmed/10922351 10.1093/ije/29.4.722 [DOI] [PubMed] [Google Scholar]
- 107.Martens EP, Pestman WR, de Boer A, Belitser S V, Klungel OH. Instrumental variables: application and limitations. Epidemiology. 2006;17: 260–7. 10.1097/01.ede.0000215160.88317.cb [DOI] [PubMed] [Google Scholar]
- 108.Burgess S, Davies NM, Thompson SG. Bias due to participant overlap in two-sample Mendelian randomization. Genet Epidemiol. 2016;40: 597–608. 10.1002/gepi.21998 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Burgess S, Thompson SG. Use of allele scores as instrumental variables for Mendelian randomization. Int J Epidemiol. 2013;42: 1134–1144. 10.1093/ije/dyt093 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Berg JJ, Harpak A, Sinnott-Armstrong N, Joergensen AM, Mostafavi H, Field Y, et al. Reduced signal for polygenic adaptation of height in UK Biobank. bioRxiv. 2018; 354951. [DOI] [PMC free article] [PubMed]
- 111.Haworth S, Mitchell R, Corbin L, Wade KH, Dudding T, Budu-Aggrey A, et al. Common genetic variants and health outcomes appear geographically structured in the UK Biobank sample: Old concerns returning and their implications. bioRxiv. 2018; 294876.
- 112.Davey Smith G, Paternoster L, Relton C. When Will Mendelian Randomization Become Relevant for Clinical Practice and Public Health? JAMA. 2017;317: 589 [DOI] [PubMed] [Google Scholar]