Abstract
Introduction
Partial thickness rotator cuff tears (PTRCT) are a common injury reported in 13–32% of the population, yet most of the current literature focuses on full thickness rotator cuff tears. Therefore, the purpose of this study was to analyze trends among patients with PTRCT including: (1) demographics; (2) comorbidities; (3) cost of care; (4) setting of initial diagnosis; and (5) change in incidence of PTRCT or surgical approach over time.
Methods
A Medicare patient-population consisting of 44 million lives was retrospectively analyzed from 2007 to 2017 using International Classification of Disease, 9th Revision (ICD-9) codes. Patients were identified for PTRCT using ICD-9 code: 726.13. The query yielded a total of 44,978 patients all of which had been previously diagnosed with PTRCT. Primary trends analyzed included: demographics, comorbidities, cost of care, initial setting of diagnosis, and change in incidence of PTRCT or surgical approach over time.
Results
PTRCTs and surgical repair of PTRCTs were most common in patients ages 65 to 69 and least common in patients who were 85 and older. Incidence of PTRCT was greater in females (54.12%) than males (45.88%). Comorbidities found within the population included hypertension, hyperlipidemia, diabetes mellitus, tobacco use, obesity, rheumatoid arthritis, and osteoarthritis of the shoulder. The average cost per episode of care totaled $9,923.26. PTRCTs were most commonly diagnosed in patients who resided in assisted living facilities (n = 27,106), making up 60% of the patient population. Reported incidence of PTRCT has increased substantially along with the surgical repair of PTRCT.
Conclusion
Reported cases of PTRCT and its surgical repair have both increased substantially over time. Approximately 11.70% of patients with PTRCT undergo either open or arthroscopic procedure as a means of surgical repair. With the growing popularity of arthroscopic procedures for rotator cuff repair, further investigation should be performed to analyze trends and risk factors for PTRCT, a seemingly underrepresented orthopedic condition.
Keywords: Shoulder surgery, Partial thickness rotator cuff tear, Arthroscopy, Patient demographics, Sports injury, Medicare
1. Introduction
The rotator cuff consists of 4 tendons converging into the humeral head: the supraspinatus, infraspinatus, teres minor, and subscapularis. Both partial thickness rotator cuff tears (PTRCT) and full thickness rotator cuff tears (FTRCT) can occur as a result of an acute injury as typically seen in overhead and throwing athletes, or degenerative wear, most commonly a chronic condition observed in patients over 50 years of age.1, 2, 3 Causes of both full and partial thickness lesions in the rotator cuff are likely multifactorial in nature. Age related declines in tissue integrity and vascularity have been attributed to degenerative rotator cuff injuries.4, 5, 6
PTRCTs have been estimated to affect anywhere from 13 to 32% of the general population.4,5,7,8 While not all PTRCTs appear to be symptomatic, those that are can result in pain, decreased range of motion, crepitus, and positive impingement signs.9,10 Additionally, a significant proportion of PTRCTs eventually develop into full thickness rotator cuff tears, potentially worsening the pre-existing symptoms.11
Despite the prevalence of PTRCTs, most of the literature on rotor cuff tears is focused on full thickness rotator cuff tears, with little to no present knowledge on the demographics and trends of patients with PTRCTs or their surgical repair.12 Therefore, the purpose of the study was to analyze trends among patients with PTRCT including: (1) demographics; (2) comorbidities; (3) cost of care; (4) setting of initial diagnosis; and (5) change in incidence of PTRCT or surgical approach over time.
2. Methods
2.1. Database
A retrospective review of the Humana patient population database from 2007 to third quarter of 2017 was performed using the PearlDiver (Pearl Diver Technologies, Fort Wayne, Indiana) supercomputer. PearlDiver is compliant with the Health Insurance Portability and Accountability (HIPPA) act and contains the records of over 100 million de-identified patient records. Patients and complications were queried using International Classification of Disease, ninth revision (ICD-9) coding. Since patient records are de-identified, the study was exempt from our institution's Institutional Review Board (IRB) approval.
2.2. Study population
A Medicare patient-population consisting of 44 million lives was retrospectively analyzed from 2007 to 2017 using International Classification of Disease, 9th Revision (ICD-9) codes. Patients with PTRCT were identified for PTRCT using ICD-9 code: 726.13. Patients with PTRCT who underwent open procedure surgical repair were identified using CPT codes: 23410, 23412, and 23420. Patients with PTRCT who underwent arthroscopic repair were identified using CPT code: 29827. The query yielded a total of 44,978 patients, 5,263 of which had undergone either open procedure or arthroscopic surgical repair.
2.3. Primary assessments
Primary trends analyzed included: demographics, comorbidities, cost of care, setting of initial diagnosis, and change in PTRCT incidence or surgical approach over time.
2.4. Data analysis
Statistical analysis was primarily descriptive and was performed using the PearlDiver computing software. A p-value less than 0.05 was considered statistically significant.
3. Results
3.1. Patient demographics and comorbidities
PTRCTs were most common in patients ages 65 to 69 (n = 13,876; 30.85%), followed by 70–74 (10,279; 22.85%), and 75 to 79 (6,255; 13.90%). PTRCTs were least common in patients who were 85 and older (n = 2,280; 5.07%). Incidence of PTRCT was greater in females (24,342; 54.12%) than males (20,636; 45.88%). Comorbidities found within the patient population included: hypertension (35,807; 79.61%), hyperlipidemia (31,112; 69.17%), diabetes mellitus (16,704; 37.13%), tobacco use (8,761; 19.47%), obesity (4,102; 9.12%), rheumatoid arthritis (3,545; 7.88%), and osteoarthritis of the shoulder joint (237; 0.53%) (Table 1).
Table 1.
Demographics of age and comorbidities of patients with partial thickness rotator cuff tears within the medicare population. BMI = Body mass index.
| Demographics | n (%) |
|---|---|
| SEX | |
| Male | 20,636 (45.88) |
| Female | 24,342 (54.11) |
| AGE | |
| 64 and Under | 9,405 (20.91) |
| 65-69 | 13,876 (30.85) |
| 70-74 | 10,279 (22.85) |
| 75-79 | 6,255 (13.90) |
| 80-84 | 3,336 (7.41) |
| 85< | 2,280 (5.06) |
| COMORBIDITIES | |
| Hypertension | 35,807 (79.61) |
| Hyperlipidemia | 31,112 (69.17) |
| Diabetes Mellitus | 16,704 (37.13) |
| Tobacco Use | 8,761 (19.47) |
| Obesity (BMI >30 kg/m2) | 4,102 (9.12) |
| Rheumatoid Arthritis | 3,545 (7.88) |
| Arthritis of Shoulder | 237 (0.53) |
3.2. Cost and setting of initial diagnosis
The average cost per episode of care totaled $9,923.26. Reported incidence of PTRCT within the Medicare population has increased substantially, with 12.8 times growth from 2011 to 2014 and 1.77 times increase from 2012 to 2014. PTRCTs were most commonly diagnosed in patients who resided in assisted living facilities (27,106; 60.26%), followed by doctor's office (5,250; 11.67%) and outpatient hospital settings (2,345; 5.21%). A significant portion of patients (5,976; 13.287%) were diagnosed in either unassigned or unknown facilities (Table 2).
Table 2.
Initial setting of diagnosis in patients with partial thickness rotator cuff tears within the medicare population.
| Setting of Initial Diagnosis | n (%) |
|---|---|
| Assisted Living Facility | 27,106 (60.26) |
| Office | 5,250 (11.67) |
| Outpatient Hospital | 2,345 (5.21) |
| Ambulatory Surgical | 1,732 (3.85) |
| Public Health Clinic | 1,091 (2.42) |
| Emergency Room | 715 (1.58) |
| Group Home | 377 (.83) |
| Impatient Hospital | 222 (.50) |
| Independent Laboratory | 79 (.17) |
| Home | 71 (.16) |
| Urgent Care Facility | 17 (0.037) |
| Hospice | 12 (0.026) |
| Unassigned/Unknown Facility (Aggregate) | 5,976 (13.287) |
3.3. Surgical trends
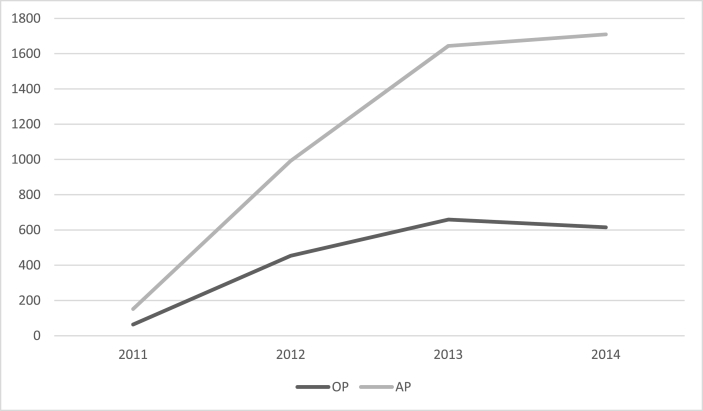
Of the 44,978 identified patients who were diagnosed with PTRCT, 5,263 had undergone surgical repair (11.70%) by either an open or arthroscopic procedure. Of the patients who had undergone surgical approaches, a total of (1,515; 28.77%) patients underwent open procedure, while (3,748; 71.22%) patients underwent an arthroscopic approach. Among both open and arthroscopic procedure groups, patients aged 65 to 69 had the highest rates of surgical repair (1,778; 33.78%), followed by 70–74 (1,336; 25.38%) and 64 and under (1,216; 23.11%) (Table 3). The open method of surgical repair for PTRCT had shown a large increase in prevalence from 2011 to 2013, with a downward trend from 2013 to 2014. Arthroscopic approaches to PTRCT repair increased substantially from 2011 to 2014 and maintained a positive trend throughout (Fig. 1).
Table 3.
Demographic analysis of patients with partial thickness rotator cuff tears undergoing surgical repair within the medicare population. OP= open wound procedure, AP = arthroscopic procedure, PTRCT= partial thickness rotator cuff tear.
| Demographics | OP, n (%) | AP, n (%) | Total Surgically Repaired PTRCTs |
|---|---|---|---|
| AGE | |||
| 64 and Under | 354 (6.73) | 862 (16.38) | 1,216 (23.11) |
| 65-69 | 504 (9.57) | 1,274 (24.21) | 1,778 (33.78) |
| 70-74 | 366 (6.95) | 970 (18.43) | 1,336 (25.38) |
| 75-79 | 206 (3.91) | 463 (8.80) | 669 (12.71) |
| 80-84 | 67 (1.27) | 150 (2.85) | 217 (4.12) |
| 85 and Over | 18 (0.34) | 29 (0.55) | 47 (.89) |
| Total | 1,515 (28.77) | 3,748 (71.22) | 5,263 (100) |
Fig. 1.
Surgical trends among patients with partial thickness rotator cuff tears undergoing surgical repair within the medicare population. OP= open wound procedure, AP = arthroscopic procedure.
4. Discussion
Despite their relatively high incidence, information regarding partial thickness rotator cuff tears (PTRCT) appears to be underrepresented in the literature. Cadaveric studies suggest PTRCTs effect up to 32% of the population.3,4,8,10 The purpose of this study was to analyze reported trends, demographics, comorbidities, cost of care, setting of initial diagnosis, and change in incidence of PTRCT or surgical approach over time in patients with PTRCT within the Medicare population.
While our study has the advantages of being adequately powered with large sample sizes, there are limitations that should be acknowledged. Using an administrative database to acquire patient records relies on ICD-9 procedural and diagnosis codes not intended for research purposes.13 Due to the nature of ICD-9 diagnosis and procedural coding, we were unable to assess the severity of PTRCTs, limiting the degree of granulation to our data. Additionally, while age groups from 64 to 85 were reported in brackets of 5 years, the age group “64 and under” was reported as one large sum, further limiting our demographic assessment. Despite these limitations, this is the first study to our knowledge, that analyzes reported trends, demographics, comorbidities, cost of care, setting of initial diagnosis, and change in incidence of PTRCT or surgical approach over time, in a population of this magnitude among patients with PTRCTs.
This study demonstrates that most of the PTRCTs in the Medicare patient population occur over the age of 65. This is consistent with the current findings in the literature regarding both partial and full thickness rotator cuff tears. In a prospective ultrasonographic study of 411 patients, Tempelhof et al. demonstrated an age dependent trend among patients with nonspecific rotator cuff tears.14 Similarly, in a magnetic resonance imaging study of 96 asymptomatic individuals, Sher et al. reported that 28% and 26% of individuals over the age of 60 had FTRCTs and PTRCTs, respectively.8 These reports support the findings of this study and demonstrate the need for further investigation in elderly patients with PTRCTs.
Additionally, comorbidities were assessed in all patients diagnosed with PTRCTs regardless of whether they had undergone any form of surgical repair. Incidence of hypertension was the greatest, followed by hyperlipidemia, diabetes mellitus, and tobacco use. In a case control study of 401 patients, Gumina et al. demonstrated that hypertensive patients were 2 times more likely to experience a rotator cuff large tear (OR: 2.09, 95%CI: 1.39–3.16) and 4 times more likely to experience a massive rotator cuff tear (OR: 4.30, 95%CI, 2.44–7.58).15 Similarly, a systematic review by Yang et al. suggests an association between dyslipidemia and rotator cuff tears.16 In a retrospective longitudinal population-based cohort study, Huang et al. demonstrated that diabetes mellitus increased risk of rotator cuff repair surgery (HR: 1.33, 95%CI: 1.05–1.68, p < 0.001).17 The literature suggests that diabetes mellitus may play a role in the development of musculoskeletal degeneration as commonly seen in rotator cuff tears due to nonenzymatic glycosylation of collagen, inflammation, and reduced tissue vascularity.18, 19, 20 Furthermore, in a study conducted on 586 orthopedic patients with atraumatic shoulder pain, Baumgarten et al. observed a strong association between cigarette smoking within 10 years of presentation and rotator cuff tears (OR: 4.24, 95%CI: 1.75–10.25, p = 0.0004).21 Tobacco use likely plays a role in the rotator cuff disease by decreasing collagen production, impairing bone to tendon healing, and reducing vascularity.22, 23, 24 These reports support our findings of these comorbidities among patients who suffer from PTRCTs. Further research should be conducted to assess PTRCT risk associated with each of these conditions.
Despite the large volume of data on age related factors for unspecified rotator cuff tears in the elderly, there is paucity in the literature regarding incidence and trends of surgical treatment for PTRCT. The study analyzed the incidence and trends among open and arthroscopic procedures as means of PTRCT repair. Both open and arthroscopic procedures declined with age, with the highest incidence of either being in the 65–69 age group, followed by the 70–74 age group. These results vary slightly from recent reports among patients with FTRCTs. Zhang et al. demonstrated that while arthroscopic rotator cuff repairs decreased with age, open rotator cuff tears increased with age.25 We hypothesize the differences in our findings may be due to unique approaches or risk factors involved with varying rotator cuff severity. Further research should be performed to determine the cause of discrepancy between open wound procedure trends in PTRCT vs FTRCT patients. Furthermore, both arthroscopic and open procedure utilization for PTRCTs increased substantially from 2011 to 2013. From 2013 to 2014, open procedure approaches decline, whereas arthroscopic approaches continue to trend upwards. These findings are consistent with the overall upward trend of arthroscopic utilization for rotator cuff repairs.26
5. Conclusion
The study illustrates that reported cases of PTRCT and its surgical repair have both increased substantially over time. It is important to consider the results of the study in the context of the study design and limitations. Orthopedic surgeons should be aware of these trends and demographics among patients with PTRCTs and consequent surgical repair of PTRCTs. With the growing popularity of arthroscopic procedures for rotator cuff repair, further investigation should be performed to analyze trends and risk factors for PTRCT, a seemingly underrepresented orthopedic condition.
Disclosure of funding related to current work
This research did not receive any grant funding.
Ethical review committee statement
This study was exempt from our institution's International Review Board (IRB) approval.
Conflicts of interest outside submitted work
None.
References
- 1.Shaffer B., Huttman D. Rotator cuff tears in the throwing athlete. Sports Med Arthrosc. 2014;22(2):101–109. doi: 10.1097/JSA.0000000000000022. [DOI] [PubMed] [Google Scholar]
- 2.Clement N.D., Nie Y.X., McBirnie J.M. Management of degenerative rotator cuff tears: a review and treatment strategy. Sport Med Arthrosc Rehabil Ther Technol. 2012;4(1):48. doi: 10.1186/1758-2555-4-48. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Boyer Martin I. AAOS comprehensive orthopaedic review 2. https://books.google.com/books?hl=en&lr=&id=WkNsDwAAQBAJ&oi=fnd&pg=PP55&ots=LkB_pWh_vm&sig=d6wLhmpW5wLBWhv5gvotujkm3_o#v=onepage&q&f=false Google Books.
- 4.Lohr J.F., Uhthoff H.K. The microvascular pattern of the supraspinatus tendon. Clin Orthop Relat Res. 1990;254:35–38. [PubMed] [Google Scholar]
- 5.Sano H., Ishii H., Trudel G., Uhthoff H.K. Histologic evidence of degeneration at the insertion of 3 rotator cuff tendons: a comparative study with human cadaveric shoulders. J Shoulder Elb Surg. 1999;8(6):574–579. doi: 10.1016/s1058-2746(99)90092-7. [DOI] [PubMed] [Google Scholar]
- 6.Rudzki J.R., Adler R.S., Warren R.F. Contrast-enhanced ultrasound characterization of the vascularity of the rotator cuff tendon: age- and activity-related changes in the intact asymptomatic rotator cuff. J Shoulder Elb Surg. 2008;17(1 Suppl):96S–100S. doi: 10.1016/j.jse.2007.07.004. [DOI] [PubMed] [Google Scholar]
- 7.Fukuda H. Partial-thickness rotator cuff tears: a modern view on Codman's classic. J Shoulder Elb Surg. 2000;9(2):163–168. [PubMed] [Google Scholar]
- 8.Sher J.S., Uribe J.W., Posada A., Murphy B.J., Zlatkin M.B. Abnormal findings on magnetic resonance images of asymptomatic shoulders. J Bone Joint Surg Am. 1995;77(1):10–15. doi: 10.2106/00004623-199501000-00002. [DOI] [PubMed] [Google Scholar]
- 9.Edwards P., Ebert J., Joss B., Bhabra G., Ackland T., Wang A. Exercise rehabilitation in the non-operative management of rotator cuff tears: a review of the literature. Int J Sports Phys Ther. 2016;11(2):279–301. [PMC free article] [PubMed] [Google Scholar]
- 10.Ozaki J., Fujimoto S., Nakagawa Y., Masuhara K., Tamai S. Tears of the rotator cuff of the shoulder associated with pathological changes in the acromion. A study in cadavera. J Bone Joint Surg Am. 1988;70(8):1224–1230. [PubMed] [Google Scholar]
- 11.Yamanaka K., Matsumoto T. The joint side tear of the rotator cuff. A followup study by arthrography. Clin Orthop Relat Res. 1994;304:68–73. [PubMed] [Google Scholar]
- 12.Matthewson G., Beach C.J., Nelson A.A. Partial thickness rotator cuff tears: current concepts. Adv Orthop. 2015;2015 doi: 10.1155/2015/458786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Yoshihara H., Yoneoka D. Understanding the statistics and limitations of large database analyses. Spine. 2014;39(16):1311–1312. doi: 10.1097/BRS.0000000000000352. [DOI] [PubMed] [Google Scholar]
- 14.Tempelhof S., Rupp S., Seil R. Age-related prevalence of rotator cuff tears in asymptomatic shoulders. J Shoulder Elb Surg. 1999;8(4):296–299. doi: 10.1016/s1058-2746(99)90148-9. [DOI] [PubMed] [Google Scholar]
- 15.Gumina S., Arceri V., Carbone S. The association between arterial hypertension and rotator cuff tear: the influence on rotator cuff tear sizes. J Shoulder Elb Surg. 2013;22(2):229–232. doi: 10.1016/j.jse.2012.05.023. [DOI] [PubMed] [Google Scholar]
- 16.Yang Y., Qu J. The effects of hyperlipidemia on rotator cuff diseases: a systematic review. J Orthop Surg Res. 2018;13(1):204. doi: 10.1186/s13018-018-0912-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Huang S.-W., Wang W.-T., Chou L.-C., Liou T.-H., Chen Y.-W., Lin H.-W. Diabetes mellitus increases the risk of rotator cuff tear repair surgery: a population-based cohort study. J Diabetes Complicat. 2016;30(8):1473–1477. doi: 10.1016/j.jdiacomp.2016.07.015. [DOI] [PubMed] [Google Scholar]
- 18.Dutta U., Cohenford M.A., Guha M., Dain J.A. Non-enzymatic interactions of glyoxylate with lysine, arginine, and glucosamine: a study of advanced non-enzymatic glycation like compounds. Bioorg Chem. 2007;35(1):11–24. doi: 10.1016/j.bioorg.2006.07.005. [DOI] [PubMed] [Google Scholar]
- 19.Nho S.J., Yadav H., Shindle M.K., Macgillivray J.D. Rotator cuff degeneration: etiology and pathogenesis. Am J Sports Med. 2008;36(5):987–993. doi: 10.1177/0363546508317344. [DOI] [PubMed] [Google Scholar]
- 20.Chen A.L., Shapiro J.A., Ahn A.K., Zuckerman J.D., Cuomo F. Rotator cuff repair in patients with type I diabetes mellitus. J Shoulder Elb Surg. 2003;12(5):416–421. doi: 10.1016/s1058-2746(03)00172-1. [DOI] [PubMed] [Google Scholar]
- 21.Baumgarten K.M., Gerlach D., Galatz L.M. Cigarette smoking increases the risk for rotator cuff tears. Clin Orthop Relat Res. 2010;468(6):1534–1541. doi: 10.1007/s11999-009-0781-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Jorgensen L.N., Kallehave F., Christensen E., Siana J.E., Gottrup F. Less collagen production in smokers. Surgery. 1998;123(4):450–455. [PubMed] [Google Scholar]
- 23.Galatz L.M., Silva M.J., Rothermich S.Y., Zaegel M.A., Havlioglu N., Thomopoulos S. Nicotine delays tendon-to-bone healing in a rat shoulder model. J Bone Joint Surg Am. 2006;88(9):2027–2034. doi: 10.2106/JBJS.E.00899. [DOI] [PubMed] [Google Scholar]
- 24.Abate M., Vanni D., Pantalone A., Salini V. Cigarette smoking and musculoskeletal disorders. Muscles Ligaments Tendons J. 2013;3(2):63–69. doi: 10.11138/mltj/2013.3.2.063. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Zhang A.L., Montgomery S.R., Ngo S.S., Hame S.L., Wang J.C., Gamradt S.C. Analysis of rotator cuff repair trends in a large private insurance population. Arthroscopy. 2013;29(4):623–629. doi: 10.1016/j.arthro.2012.11.004. [DOI] [PubMed] [Google Scholar]
- 26.Colvin A.C., Egorova N., Harrison A.K., Moskowitz A., Flatow E.L. National trends in rotator cuff repair. J Bone Joint Surg Am. 2012;94(3):227–233. doi: 10.2106/JBJS.J.00739. [DOI] [PMC free article] [PubMed] [Google Scholar]