Abstract
BACKGROUND
Indications and optimal timing for surgical treatment of degenerative cervical myelopathy (DCM) remain unclear, and data from daily clinical practice are warranted.
OBJECTIVE
To investigate clinical outcomes following decompressive surgery for DCM.
METHODS
Data were obtained from the Norwegian Registry for Spine Surgery. The primary outcome was change in the neck disability index (NDI) 1 yr after surgery. Secondary endpoints were the European myelopathy score (EMS), quality of life (EuroQoL 5D [EQ-5D]), numeric rating scales (NRS) for headache, neck pain, and arm pain, complications, and perceived benefit of surgery assessed by the Global Perceived Effect (GPE) scale.
RESULTS
We included 905 patients operated between January 2012 and June 2018. There were significant improvements in all patient-reported outcome measures (PROMs) including NDI (mean −10.0, 95% CI −11.5 to −8.4, P < .001), EMS (mean 1.0, 95% CI 0.8-1.1, P < .001), EQ-5D index score (mean 0.16, 95% CI 0.13-0.19, P < .001), EQ-5D visual analogue scale (mean 13.8, 95% CI 11.7-15.9, P < .001), headache NRS (mean −1.1, 95% CI −1.4 to −0.8, P < .001), neck pain NRS (mean −1.8, 95% CI −2.0 to −1.5, P < .001), and arm pain NRS (mean −1.7, 95% CI −1.9 to −1.4, P < .001). According to GPE scale assessments, 229/513 patients (44.6%) experienced “complete recovery” or felt “much better” at 1 yr. There were significant improvements in all PROMs for both mild and moderate-to-severe DCM. A total of 251 patients (27.7%) experienced adverse effects within 3 mo.
CONCLUSION
Surgery for DCM is associated with significant and clinically meaningful improvement across a wide range of PROMs.
Keywords: Cervical spine, Decompressive surgery, Degenerative, Degenerative cervical myelopathy, Observational study, Spine disorder, Spine surgery
Graphical Abstract
Graphical Abstract.
ABBREVIATIONS
- DCM
degenerative cervical myelopathy
- EMS
European myelopathy score
- EQ-5D
EuroQoL-5D
- GPE
Global Perceived Effect
- MCIC
minimal clinically important change
- mJOA
modified Japanese Orthopedic Association
- NDI
neck disability index
- NORspine
Norwegian Registry for Spine Surgery
- NRS
numeric rating scales
- PROM
patient-reported outcome measure
Degenerative cervical myelopathy (DCM) is a progressive spine disorder and the most common cause of spinal cord impairment in adults over 55 yr.1-4 The cervical spine is prone to degenerative changes such as disk herniation, ligament hypertrophy or ossification, and osteophyte formation that may lead to spinal cord compression and dysfunction.4,5 DCM should be considered in patients >50 yr with progressive neurological symptoms, such as pain and stiffness in the neck, pain and numbness in limbs, poor coordination, imbalance, loss of dexterity, frequent falls, and bowel and/or urinary incontinence.6,7 As nonspecific and subtle initial early features of DCM overlap with other neurological conditions, it is frequently challenging to catch the diagnosis early. Lack of awareness and incomplete neurological assessments can also delay diagnosis,8 and this may also increase patients’ risk of developing life-long disability and impaired quality of life.9,10 Magnetic resonance imaging (MRI) is the investigation of choice to detect spinal cord compression with or without intramedullary signal abnormalities and electrophysiologic testing can sometimes help exclude alternative diagnoses.7,11 Incidental degenerative changes in the cervical spine with spinal cord compression are commonly encountered on MRI and do not correlate well with the severity of symptoms.4 As the oldest sector of the population continues to grow and wishes to remain active, physicians will be required to manage an increasing number of patients with degenerative changes in the spine and DCM.4,12
Indications and optimal timing for surgical treatment of DCM remain unclear, and additional high-quality data from daily clinical practice including all disease severities are warranted. According to current guidelines, surgery is recommended for moderate-to-severe or progressive DCM to prevent further deterioration.5 Two prospective multicenter AOSpine studies showed that decompressive surgery in selected patients can halt disease progression and achieve meaningful, albeit limited, recovery in pain, function, and quality of life.13,14 These 2 large studies were instrumental in driving the development of the 2017 AOSpine and Cervical Spine Research Society guidelines for management of DCM.5 Still, it is a common perception among health-care providers that chances of clinically relevant improvement following surgery for DCM are slim.
In this nationwide study with prospectively collected data from the Norwegian Registry for Spine Surgery (NORspine), we investigated clinical outcomes in patients undergoing decompressive surgery for DCM.
METHODS
Reporting is consistent with the STROBE (Strengthening the Reporting of Observational Studies in Epidemiology) statement.15 The Regional Committee for Medical Research Ethics approved the study (2016/840), and all participants provided written informed consent.
Study Population
NORspine is a comprehensive registry for quality control and research and includes all eight centers performing cervical spine surgery in Norway.16,17 Currently, approximately 81% of patients who undergo surgery in the cervical spine in Norway are included in NORspine. The inclusion rate for DCM surgery is probably higher as these procedures typically are scheduled. NORspine participation was not a requirement for patients to gain access to treatment or for a provider to be eligible for reimbursement and payment. Patients were eligible if they were ≥18 yr, underwent decompressive surgery for DCM between January 1, 2012 and June 15, 2018, had a preoperative European myelopathy score (EMS) <18 points, and were registered in NORspine.
Surgical Procedures
All patients underwent decompressive surgery of the cervical spine. The surgical approach, the number of operated levels, and the use and type of instrumentation were performed at the surgeons’ discretion.
Outcome Measures
The primary outcome was change in the neck disability index (NDI) between baseline and 1 yr. Secondary outcome measures were changes at 1 yr in EMS, EuroQoL-5D (EQ-5D), and numeric rating scales (NRS) for headache, neck pain, and arm pain. In addition, we report complications occurring within 3 mo and patients’ perceived benefit of surgery assessed by the Global Perceived Effect (GPE) scale at 1 yr.
The NDI is a self-rated questionnaire developed for patients with neck disability.18 The questionnaire is composed of 10 items: 7 related to activities of daily living, 2 to pain, and 1 to concentration. The sum of the 10 items is recalculated into a percentage NDI score from 0 to 100 (no to maximum disability). The minimal clinically important change (MCIC) is approximately 7.5 percentage points.19,20
The EMS has 5 subscores obtained by patient questionnaires to evaluate the 4 major neural systems, the impairment of which contributes to the clinical picture of DCM: (a) the upper motor neuron with signs of spasticity as well as bladder and bowel disturbances; (b) the lower motor neuron with impairment of hand function; (c) the posterior roots with upper limb radicular deficits and paresthesias; and (d) the posterior columns with proprioceptive sensory loss, disturbed coordination, and ataxia.21,22 The total score ranges between 5 and 18, and the lower the score, the more severe the deficits. Scores ≥13 were classified as mild DCM and scores between 5 and 12 points were classified as moderate-to-severe DCM.21 There is no consensus of the MCIC for EMS, but even a small change in severe DCM might be considered important in daily function.
Changes in health-related quality of life were measured with EQ-5D.23 An index value for health status is generated for each patient. Scores range from −0.6 to 1, in which 1 corresponds to perfect health. Effect size estimations were used to evaluate the magnitude of changes.24 EQ-5D also contains a vertical visual analogue scale, ranging from 0 to 100 (lower scores indicate poorer health).
Intensities of headache, neck pain, and arm pain were assessed on 0 to 10 NRS, with response options ranging from 0 (no pain) to 10 (worst imaginable pain). The MCIC for NRS is approximately 1.5 points.25
The GPE has 7 response categories: (1) complete recovery, (2) much better, (3) slightly better, (4) unchanged, (5) slightly worse, (6) much worse, and (7) worse than ever.26
Surgeons provided the following data on perioperative complications: unintentional durotomy, nerve root injury, wrong level surgery, misplacement of implant, intraoperative hemorrhage requiring blood replacement, respiratory complications, anaphylactic reaction, spinal cord injury, esophageal injury, major vessel injury, cardiovascular complications, and other nerve injury. Patients reported the following complications if occurring within 3 mo: wound infection, urinary tract infection, pneumonia, pulmonary embolism, deep vein thrombosis, dysphagia, dysphonia, and new-onset arm or leg weakness.
Data Collection
On admission for surgery, the patients completed a self-administered questionnaire, which included questions about demographics, personal characteristics, and patient-reported outcome measures (PROMs). Using a standard registration form, surgeons recorded data on diagnosis, severity of DCM according to the Ranawat27 classification of myelopathy, comorbidity, American Society of Anesthesiologists grade, image findings, and surgical procedure. NORspine distributed self-administered questionnaires to the patients by mail 3 and 12 mo after surgery. Nonresponders received 1 reminder with a new copy of the questionnaire.
Statistical Analysis
Statistical analyses were performed with SPSS (IBM Corp) version 26.0 and Software R (R Foundation for Statistical Computing) version 3.6.3. For statistical comparison tests, we defined the significance level as P ≤ .05. Frequencies were used for demographic variables at baseline, and changes in PROMs were compared with paired-sample T-test.
Missing data were managed with mixed linear model analyses. Previous studies have shown that imputations are not required before performing a mixed model analysis on longitudinal data.28,29 Patients were not excluded from mixed model analyses if a variable was missing at some, but not all, time points following baseline.
Patient and Public Involvement
A member from The Norwegian Back Pain Association reviewed the study protocol and provided feedback concerning the study design.
RESULTS
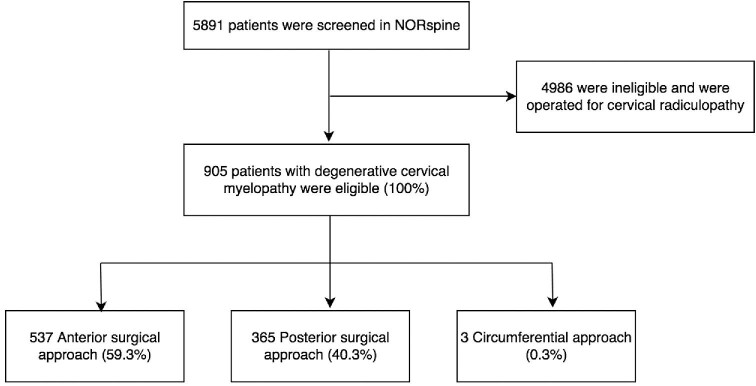
Figure 1 shows the inclusion and exclusion process leading to 905 eligible patients. Baseline characteristics are presented in Table 1. Participants underwent surgery at 8 neurosurgical departments. The mean age was 57.5 +/−12.4 yr, 365 (40.3%) were female, and 163 patients (18.0%) had moderate-to-severe DCM at baseline. In total, 697 participants (77%) provided patient reported outcome measures at 3 and/or 12 mo. The only differences in baseline characteristics between responders and non-responders were tobacco use (32.1% vs 47.6%, P < .001), age (58.3 vs 54.9 yr, P < .001), and life partner (73.1% vs 59.1%, P < .001). Preoperative EMS was missing in 89 patients (9.8%).
FIGURE 1.
Flow diagram with study enrolment and surgical treatment.
TABLE 1.
Personal Characteristics, Coexisting Illnesses, and Measures of Health
| Variables | |
|---|---|
| Age, years (standard deviation [SD]) | 57.5 (+/−12.4) |
| Female | 365 (40.3) |
| Married or partner | 627 (69.3) |
| Current tobacco user | 324 (35.8) |
| College education | 281 (31.0) |
| Prior cervical spine surgery | 102 (11.3%) |
| Body mass index (SD) | 27.2 (+/−4.8) |
| Comorbidity | 508 (56.1) |
| American Society of Anesthesiologists grade > 2 | 190 (21.0) |
| Ranawat grade 3A or 3B | 339 (37.5) |
| Symptoms >1 yr | 183 (20.2) |
| Preoperative EMS (SD) | 14.3 (+/−2.4) |
| Preoperative NDI (SD) | 34.9 (+/−16.8) |
| Preoperative EQ-5D (SD) | 0.45 (+/−0.33) |
| Preoperative diagnostic imaging: | |
| MRI | 885 (97.8) |
| Computed tomography | 112 (13.5) |
| Myelography | 2 (0.2) |
| Electrophysiologic testing | 5 (0.6) |
Values are numbers (percentages) unless stated otherwise.
Primary Outcome
The mean NDI score at baseline was 35.1 and at 1-yr follow-up was 25.1 (difference −10.0, 95% CI −11.5 to −8.4, P < .001). In patients with mild DCM, the mean NDI score at baseline was 32.2 and at 1-yr follow-up was 22.7 (difference −9.5, 95% CI −11.7 to −7.9, P < .001). In patients with moderate-to-severe DCM, the mean NDI score at baseline was 48.7 and at 1-yr follow-up was 34.9 (difference −13.8, 95% CI −19.0 to −8.6, P < .001). The mean change in NDI exceeded the MCIC of 7.5 points for all DCM severities.
Secondary Outcomes
PROMs are presented in Table 2. There were significant improvements in all PROMs at 1 yr including EMS (mean 1.0, 95% CI 0.8–1.1, P < .001), EQ-5D index score (mean 0.16, 95% CI 0.13–0.19, P < .001), EQ-5D visual analogue scale (mean 13.8, 95% CI 11.7–15.9, P < .001), headache NRS (mean −1.1, 95% CI −1.4 to −0.8, P < .001), neck pain NRS (mean −1.8, 95% CI −2.0 to −1.5, P < .001), and arm pain NRS (mean −1.7, 95% CI −1.9 to −1.4, P < .001).
TABLE 2.
Complete Case Analysis and Mixed Linear Model Analysis for Outcomes at 1 yr in Patients With DCM
| Variable | Baseline | 1 yr | Mean change | 95% CI | P-value |
|---|---|---|---|---|---|
| Complete case analyses: | |||||
| All categories | |||||
| NDI (N = 385) | 35.1 | 25.1 | −10.0 | −11.5 to −8.4 | <.001 |
| EMS (N = 416) | 14.3 | 15.2 | 1.0 | 0.8 to 1.1 | <.001 |
| EQ-5D summary score (N = 453) | 0.45 | 0.61 | 0.16 | 0.13 to 0.19 | <.001 |
| EQ-5D VAS (N = 470) | 49.1 | 62.9 | 13.8 | 11.7 to 15.9 | <.001 |
| Headache NRS (N = 435) | 3.3 | 2.2 | −1.1 | −1.4 to −0.8 | <.001 |
| Neck pain NRS (N = 457) | 4.8 | 3.0 | −1.8 | −2.0 to −1.5 | <.001 |
| Arm pain NRS (N = 459) | 5.1 | 3.5 | −1.7 | −1.9 to −1.4 | <.001 |
| Mild myelopathy | |||||
| NDI (N = 298) | 32.2 | 22.7 | −9.5 | −11.7 to −7.9 | <.001 |
| EMS (N = 330) | 15.3 | 15.8 | 0.5 | 0.4 to 0.7 | <.001 |
| EQ-5D summary score (N = 338) | 0.52 | 0.66 | 0.14 | 0.11 to 0.18 | <.001 |
| EQ-5D VAS (N = 345) | 52.8 | 65.5 | 12.7 | 10.3 to 15.1 | <.001 |
| Headache NRS (N = 314) | 3.1 | 2.1 | −1.0 | −1.4 to −0.7 | <.001 |
| Neck pain NRS (N = 332) | 4.6 | 2.9 | −1.7 | −2.0 to −1.4 | <.001 |
| Arm pain NRS (N = 336) | 4.8 | 3.2 | −1.6 | −1.9 to −1.3 | <.001 |
| Moderate-to-severemyelopathy | |||||
| NDI (N = 64) | 48.7 | 34.9 | −13.8 | −19.0 to −8.6 | <.001 |
| EMS (N = 86) | 10.4 | 13.0 | 2.6 | 2.0 to 3.2 | <.001 |
| EQ-5D summary score (N = 83) | 0.18 | 0.44 | 0.26 | 0.16 to 0.36 | <.001 |
| EQ-5D VAS (N = 86) | 35.3 | 53.1 | 17.8 | 12.0 to 23.5 | <.001 |
| Headache NRS (N = 83) | 3.7 | 2.8 | −0.9 | −1.6 to −0.2 | .009 |
| Neck pain NRS (N = 83) | 5.3 | 3.4 | −1.9 | −2.6 to −1.3 | <.001 |
| Arm pain NRS (N = 82) | 5.8 | 4.1 | −1.7 | −2.5 to −0.9 | <.001 |
| Mixed linear model analyses | |||||
| All categories | |||||
| NDI (N = 854) | 35.1 | 25.8 | −9.4 | −10.6 to −8.1 | <.001 |
| EMS (N = 880) | 14.3 | 15.2 | 0.9 | 0.7 to 1.0 | <.001 |
| EQ-5D summary score (N = 887) | 0.44 | 0.60 | 0.16 | 0.14 to 0.19 | <.001 |
| EQ-5D VAS (N = 884) | 49.1 | 62.5 | 13.4 | 11.6 to 15.2 | <.001 |
| Headache NRS (N = 870) | 3.2 | 2.1 | −1.0 | −1.3 to −0.8 | <.001 |
| Neck pain NRS (N = 882) | 4.8 | 3.0 | −1.7 | −2.0 to −1.5 | <.001 |
| Arm pain NRS (N = 882) | 5.0 | 3.4 | −1.6 | −1.9 to −1.4 | <.001 |
| Mild myelopathy | |||||
| NDI (N = 633) | 32.3 | 23.1 | −9.2 | −10.6 to −7.8 | <.001 |
| EMS (N = 653) | 15.3 | 15.8 | 0.5 | 0.3 to 0.6 | <.001 |
| EQ-5D Summary score (N = 647) | 0.52 | 0.66 | 0.14 | 0.11 to 0.17 | <.001 |
| EQ-5D VAS (N = 645) | 52.8 | 65.5 | 12.7 | 10.7 to 14.8 | <.001 |
| Headache NRS (N = 633) | 3.0 | 2.0 | −1.0 | −1.3 to −0.7 | <.001 |
| Neck pain NRS (N = 642) | 4.6 | 2.9 | −1.7 | −2.0 to −1.4 | <.001 |
| Arm pain NRS (N = 642) | 4.8 | 3.2 | −1.6 | −1.9 to −1.3 | <.001 |
| Moderate-to-severe myelopathy | |||||
| NDI (N = 144) | 48.8 | 35.3 | −13.5 | −17.3 to −9.7 | <.001 |
| EMS (N = 163) | 10.4 | 13.0 | −2.6 | −2.1 to −3.0 | <.001 |
| EQ-5D Summary score (N = 162) | 0.14 | 0.43 | 0.29 | 0.21 to 0.36 | <.001 |
| EQ-5D VAS (N = 159) | 36.0 | 53.6 | 17.6 | 12.8 to 22.3 | <.001 |
| Headache NRS (N = 156) | 3.5 | 2.6 | −0.9 | −1.5 to −0.4 | <.001 |
| Neck pain NRS (N = 158) | 5.5 | 3.4 | −2.1 | −2.6 to −1.5 | <.001 |
| Arm pain NRS (N = 157) | 5.8 | 4.0 | −1.8 | −2.4 to −1.1 | <.001 |
The change in EQ-5D index score represents a moderate clinical change, with an effect size of 0.51. Further, there were significant improvements in all PROMs for both mild and moderate-to-severe DCM. The mean changes in neck and arm pain NRS exceeded the MCIC of 1.5 points. Mixed linear model analyses showed similar results for all PROMs
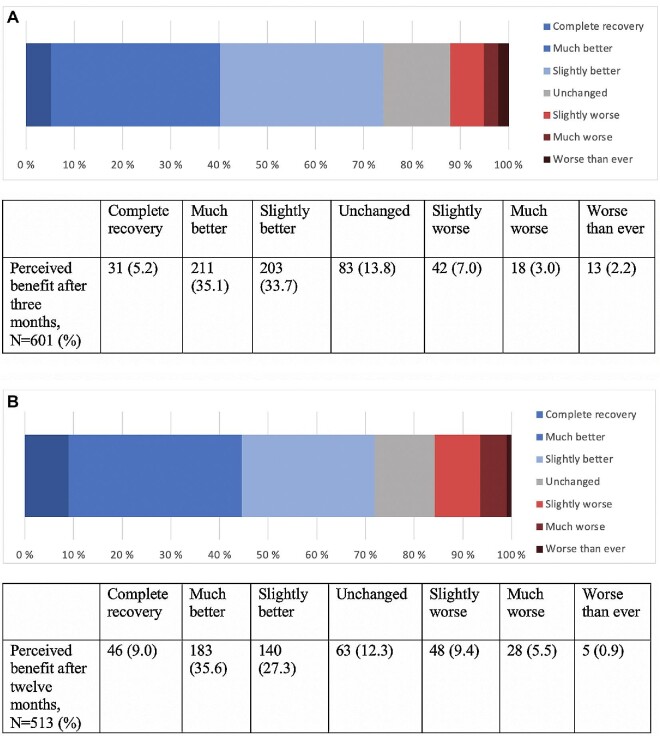
Patients’ perceived benefit of surgery assessed by the GPE at 3 mo and 1 yr is presented in Figure 2A and 2B, respectively. According to GPE assessments, 229 out of 513 patients (44.6%) reported complete recovery or feeling much better at 1 yr. In total, 81 out of 513 patients (15.8%) reported feeling “slightly worse,” “much worse,” or “worse than ever” at 1 yr.
FIGURE 2.
A, Patients’ perceived benefit of surgery for DCM after 3 mo. B, Patients’ perceived benefit of surgery for DCM after 1 yr.
Table 3 provides details of surgical treatments and complications. There were no deaths within 30 d of surgery. In total, 251 patients (27.7%) experienced complications or adverse effects within 3 mo.
TABLE 3.
Surgical Treatment, Complications, and Events
| Variables | |
|---|---|
| Emergency surgery | 137 (15.1) |
| Surgical approach | |
| Anterior | 537 (59.3) |
| Posterior | 365 (40.3) |
| Instrumented fusion | 17 (1.9) |
| Circumferential | 3 (0.3) |
| Number of levels decompressed, median (range) | 2 (1-6) |
| Spine level of surgery | |
| C0-C1 | 3 (0.3) |
| C1-C2 | 4 (0.4) |
| C2-C3 | 54 (6.0) |
| C3-C4 | 258 (28.5) |
| C4-C5 | 389 (43.0) |
| C5-C6 | 580 (64.1) |
| C6-C7 | 327 (36.1) |
| C7-TH1 | 35 (3.9) |
| Operation time, min (SD) | 92.5 (+/−42.7) |
| Number of days in hospital (SD) | 1.7 (+/−1.8) |
| Reoperation within 90 d | 5 (0.6) |
| Patients with complications | 251 (27.7) |
| Perioperative complications | 13 (1.4) |
| Unintentional durotomy | 4 (0.4) |
| Nerve root injury | 0 |
| Iatrogenic spinal cord injury | 2 (0.2) |
| Wrong level surgery | 0 |
| Postoperative hematoma | 2 (0.2) |
| Misplacement of implant | 0 |
| Esophageal injury | 0 |
| Major blood vessel injury | 0 |
| Cardiovascular complications | 1 (0.1%) |
| Respiratory complications | 1 (0.1) |
| Anaphylactic reaction | 0 |
| Other complications | 5 (0.6%) |
| Complications within 3 mo | 244 (27.0) |
| Deep wound infection | 9 (1.0%) |
| Superficial wound infection | 35 (3.9%) |
| Urinary tract infection | 41 (4.5%) |
| Pneumonia | 12 (1.3%) |
| Pulmonary embolism | 5 (0.6%) |
| Deep venous thrombosis | 7 (0.8%) |
| New-onset arm or leg weakness | 120 (13.3%) |
| Dysphagia | 72 (8.0%) |
| Dysphonia | 62 (6.9%) |
Values are numbers (percentages) of participants unless stated otherwise.
DISCUSSION
This nationwide study shows that surgery for DCM is associated with significant and clinically relevant improvements across the whole range of PROMs at 1 yr. Favorable outcomes were observed for both mild and moderate-to-severe DCM, with the largest effects observed in the latter more severely disabled group. Our study adds to the evidence from previous observational studies that surgical treatment cannot only arrest further progression of myelopathy, but also improve functional status, neurological outcomes, and quality of life.13,14,30 Although >70% of responders perceived a benefit from surgery, a substantial placebo effect cannot be ruled out following such complex treatment.31 Risk associated with surgery for DCM is not negligible and should be clearly communicated to patients prior to surgery. Patients should also be informed that complete resolution of symptoms is unlikely following surgery. Life-threatening complications and early reoperations are fortunately rare. In our study, 27.7% of responders experienced adverse effects or complications within 3 mo and 15.8% perceived a clinical worsening.
The epidemiology of DCM is poorly understood, and exact numbers of prevalence or incidence are not known. The prevalence of surgically treated DCM in Europe has been estimated between 1.6 and 4.7 per 100 000 inhabitants.32,33 It is important to refer patients with suspected DCM promptly to MRI and a specialist for consideration of decompressive surgery, as delayed diagnosis and treatment can lead to unnecessary residual symptoms and worsening of disability. For nonmyelopathic patients without radiculopathy and only radiological evidence of cervical cord compression, prophylactic surgery is not recommended.5,6 These patients should be followed clinically if feasible and counseled as to potential risks of progression and advised to seek medical attention if symptoms should develop.
Until recently, there has been limited evidence to guide clinical management of mild DCM.5 In a large and recent prospective study on mild DCM with 2 yr follow-up, significant gains in a wide range of PROMs were observed following surgery.34 Two small randomized trials in patients with mild-to-moderate DCM found no differences in neurological outcomes at 2 yr between those who received conservative vs surgical treatment.35,36 Still, the majority of patients in our study had mild DCM and significant improvements were observed for all PROMs. However, these improvements were smaller compared to patients with moderate-to-severe DCM. Although we have detailed clinical data at the time of surgery, little is known about the dynamics of symptoms, disability, and neurological functioning preceding surgery. A recent study showed that machine learning algorithms might become useful to identify patients with mild DCM that will benefit from surgery.37 The phenotype of mild DCM needs to be acknowledged, and a recent study reported that neck pain, motor symptoms, and female gender were associated with greater impairment of quality of life and greater response to surgery.38 Additional observational studies or clinical trials should be encouraged to clarify the natural course of the disease and evaluate surgery and structured rehabilitation for patients with mild DCM.
There are no randomized trials comparing surgical and nonsurgical management of patients with moderate-to-severe DCM. In a recent trial, adjuvant treatment perioperatively with riluzole (Aventis Pharma) did not improve functional recovery beyond decompressive surgery in patients with moderate-to-severe DCM.39 Age-related degeneration of the cervical spine encompasses a complex set of anatomical changes that can result in DCM.4 Spine surgeons can draw from a repertoire of different operations to treat DCM, and the surgical strategy is typically based on patient specific factors and preferences of the surgeon. An interesting topic is the comparative efficacy and effectiveness of different surgical treatments.30,40-42 Unfortunately, this is beyond the scope of our study as we did not have detailed enough information in order to compare the effectiveness of different surgical procedures. Interestingly, a recent trial showed that an anterior surgical approach did not significantly improve outcomes compared with a posterior surgical approach.43
Limitations
The modified Japanese Orthopedic Association (mJOA) scale is currently the recommended disease-specific PROM. The use of the EMS might make it more challenging to compare results across more recent studies. This is to some extent alleviated by the use of the NDI and EQ-5D, which are included in recent studies on DCM. NORspine started including patients several years prior to the current practice guidelines.5 Solely assessing the myelopathy is likely insufficient to fully understand clinical outcome in its totality, and combinations of questionnaires are recommended.38,44,45 A study comparing 7 different scales, including mJOA and EMS, found that all of them detected significant improvement following surgery.46 Still, each scale had differing qualities of reliability, validity, and responsiveness. Lack of randomization is an obvious limitation. Loss to follow-up is another concern, but a previous NORspine study showed no difference in outcomes between responders and nonresponders.47 Follow-up exceeding 1 yr may be warranted to detect the effect of surgery on progression of symptoms. Some patients may have received physical therapy, but our study cannot assess the impact of such interventions.
CONCLUSION
Surgery for DCM is associated with significant improvements across the whole range of PROMs. Favorable outcomes were observed at 1 yr for both mild and moderate-to-severe DCM. Surgical treatment cannot only arrest further progression of myelopathy but also improve functional status, neurological outcomes, and quality of life.
Funding
This study did not receive any funding or financial support.
Disclosures
The authors have no personal, financial, or institutional interest in any of the drugs, materials, or devices described in this article.
Acknowledgments
This work is in memory of Stein Andresen, former user representative in NORspine. The authors thank NORspine and are greatly indebted to all patients and spine surgeons who participated in NORspine registration.
Contributor Information
Sasha Gulati, Department of Neuromedicine and Movement Science, Norwegian University of Science and Technology, Trondheim, Norway; Department of Neurosurgery, St. Olavs Hospital, Trondheim, Norway; National Advisory Unit on Spinal Surgery, St. Olavs Hospital, Trondheim, Norway.
Vetle Vangen-Lønne, Department of Neuromedicine and Movement Science, Norwegian University of Science and Technology, Trondheim, Norway; Department of Neurosurgery, St. Olavs Hospital, Trondheim, Norway.
Øystein P Nygaard, Department of Neuromedicine and Movement Science, Norwegian University of Science and Technology, Trondheim, Norway; Department of Neurosurgery, St. Olavs Hospital, Trondheim, Norway; National Advisory Unit on Spinal Surgery, St. Olavs Hospital, Trondheim, Norway.
Agnete M Gulati, Department of Rheumatology, St. Olavs Hospital, Trondheim, Norway.
Tommy A Hammer, Department of Radiology, St. Olavs Hospital, Trondheim, Norway.
Tonje O Johansen, Department of Neuromedicine and Movement Science, Norwegian University of Science and Technology, Trondheim, Norway; Department of Neurosurgery, St. Olavs Hospital, Trondheim, Norway.
Wilco C Peul, Department of Neurosurgery, Leiden University Medical Centre, Leiden, Netherlands; Department of Neurosurgery, Haaglanden Medical Centre, The Hague, Netherlands.
Øyvind O Salvesen, Department of Public Health and General Practice, Norwegian University of Science and Technology, Trondheim, Norway.
Tore K Solberg, Department of Neurosurgery, University Hospital of North Norway, Norwegian Registry for Spine Surgery, Tromsø, Norway; Institute for Clinical Medicine, The Arctic University of Norway, Tromsø, Norway.
Neurosurgery Speaks! Audio abstracts available for this article at www.neurosurgery-online.com.
Neurosurgery Speaks (Audio Abstracts)
Listen to audio translations of this paper's abstract into select languages by choosing from one of the selections below.
REFERENCES
- 1.Kalsi-Ryan S, Karadimas SK, Fehlings MG. Cervical spondylotic myelopathy: the clinical phenomenon and the current pathobiology of an increasingly prevalent and devastating disorder. Neuroscientist. 2013;19(4):409-421. [DOI] [PubMed] [Google Scholar]
- 2.Moore AP, Blumhardt LD. A prospective survey of the causes of non-traumatic spastic paraparesis and tetraparesis in 585 patients. Spinal Cord. 1997;35(6):361-367. [DOI] [PubMed] [Google Scholar]
- 3.Theodore N. Degenerative cervical spondylosis. N Engl J Med. 2020;383(2):159-168. [DOI] [PubMed] [Google Scholar]
- 4.Nouri A, Tetreault L, Singh A, Karadimas SK, Fehlings MG. Degenerative cervical myelopathy: epidemiology, genetics, and pathogenesis. Spine. 2015;40(12):E675-E693. [DOI] [PubMed] [Google Scholar]
- 5.Fehlings MG, Tetreault LA, Riew KDet al. A clinical practice guideline for the management of patients with degenerative cervical myelopathy: recommendations for patients with mild, moderate, and severe disease and nonmyelopathic patients with evidence of cord compression. Global Spine J. 2017;7(3 Suppl):70S-83S. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Davies BM, Mowforth OD, Smith EK, Kotter MR. Degenerative cervical myelopathy. BMJ. 2018;360:k186. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Tracy JA, Bartleson JD. Cervical spondylotic myelopathy. Neurologist. 2010;16(3):176-187. [DOI] [PubMed] [Google Scholar]
- 8.Behrbalk E, Salame K, Regev GJ, Keynan O, Boszczyk B, Lidar Z. Delayed diagnosis of cervical spondylotic myelopathy by primary care physicians. Neurosurg Focus. 2013;35(1):E1. [DOI] [PubMed] [Google Scholar]
- 9.Oh T, Lafage R, Lafage Vet al. Comparing quality of life in cervical spondylotic myelopathy with other chronic debilitating diseases using the short form survey 36-health survey. World Neurosurg. 2017;106:699-706. [DOI] [PubMed] [Google Scholar]
- 10.Tetreault LA, Côté P, Kopjar B, Arnold P, Fehlings MG. A clinical prediction model to assess surgical outcome in patients with cervical spondylotic myelopathy: internal and external validations using the prospective multicenter AOSpine North American and international datasets of 743 patients. Spine J. 2015;15(3):388-397. [DOI] [PubMed] [Google Scholar]
- 11.Okada E, Matsumoto M, Ichihara Det al. Aging of the cervical spine in healthy volunteers: a 10-year longitudinal magnetic resonance imaging study. Spine. 2009;34(7):706-712. [DOI] [PubMed] [Google Scholar]
- 12.Kovalova I, Kerkovsky M, Kadanka Zet al. Prevalence and imaging characteristics of nonmyelopathic and myelopathic spondylotic cervical cord compression. Spine. 2016;41(24):1908-1916. [DOI] [PubMed] [Google Scholar]
- 13.Fehlings MG, Ibrahim A, Tetreault Let al. A global perspective on the outcomes of surgical decompression in patients with cervical spondylotic myelopathy: results from the prospective multicenter AOSpine international study on 479 patients. Spine. 2015;40(17):1322-1328. [DOI] [PubMed] [Google Scholar]
- 14.Fehlings MG, Wilson JR, Kopjar Bet al. Efficacy and safety of surgical decompression in patients with cervical spondylotic myelopathy: results of the AOSpine North America prospective multi-center study. J Bone Joint Surg Am. 2013;95(18):1651-1658. [DOI] [PubMed] [Google Scholar]
- 15.von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP. The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370(9596):1453-1457. [DOI] [PubMed] [Google Scholar]
- 16.Nerland US, Jakola AS, Solheim Oet al. Minimally invasive decompression versus open laminectomy for central stenosis of the lumbar spine: pragmatic comparative effectiveness study. BMJ. 2015;350:h1603. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Madsbu MA, Salvesen Ø, Carlsen SMet al. Surgery for herniated lumbar disc in private vs public hospitals: a pragmatic comparative effectiveness study. Acta Neurochir. 2020;162(3):703-711. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Johansen JB, Andelic N, Bakke E, Holter EB, Mengshoel AM, Røe C. Measurement properties of the Norwegian version of the neck disability index in chronic neck pain. Spine. 2013;38(10):851-856. [DOI] [PubMed] [Google Scholar]
- 19.Young BA, Walker MJ, Strunce JB, Boyles RE, Whitman JM, Childs JD. Responsiveness of the neck disability index in patients with mechanical neck disorders. Spine J. 2009;9(10):802-808. [DOI] [PubMed] [Google Scholar]
- 20.MacDermid JC, Walton DM, Avery Set al. Measurement properties of the neck disability index: a systematic review. J Orthop Sports Phys Ther. 2009;39(5):400-C12. [DOI] [PubMed] [Google Scholar]
- 21.Herdmann JLM, Krzan M, Dvorak J, Bock WJ. The European myelopathy score. Cerebellar Infarct Midline Tumors Minimally Invasive Endoscopic Neurosurgery (MIEN) Advances in Neurosurgery, vol 22. Springer; 1994. [Google Scholar]
- 22.Vitzthum HE, Dalitz K. Analysis of five specific scores for cervical spondylogenic myelopathy. Eur Spine J. 2007;16(12):2096-2103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Solberg TK, Olsen JA, Ingebrigtsen T, Hofoss D, Nygaard OP. Health-related quality of life assessment by the EuroQol-5D can provide cost-utility data in the field of low-back surgery. Eur Spine J. 2005;14(10):1000-1007. [DOI] [PubMed] [Google Scholar]
- 24.Kazis LE, Anderson JJ, Meenan RF. Effect sizes for interpreting changes in health status. Med Care. 1989;27(3 Suppl):S178-S189. [DOI] [PubMed] [Google Scholar]
- 25.Dworkin RH, Turk DC, Wyrwich KWet al. Interpreting the clinical importance of treatment outcomes in chronic pain clinical trials: IMMPACT recommendations. J Pain. 2008;9(2):105-121. [DOI] [PubMed] [Google Scholar]
- 26.Kamper SJ, Ostelo RW, Knol DL, Maher CG, de Vet HC, Hancock MJ. Global perceived effect scales provided reliable assessments of health transition in people with musculoskeletal disorders, but ratings are strongly influenced by current status. J Clin Epidemiol. 2010;63(7):760-766.e1. [DOI] [PubMed] [Google Scholar]
- 27.Ranawat CS, O’Leary P, Pellicci P, Tsairis P, Marchisello P, Dorr L. Cervical spine fusion in rheumatoid arthritis. J Bone Joint Surg Am. 1979;61(7):1003-1010. [PubMed] [Google Scholar]
- 28.Twisk J, de Boer M, de Vente W, Heymans M. Multiple imputation of missing values was not necessary before performing a longitudinal mixed-model analysis. J Clin Epidemiol. 2013;66(9):1022-1028. [DOI] [PubMed] [Google Scholar]
- 29.Madsbu MA, Solberg TK, Salvesen O, Nygaard OP, Gulati S. Surgery for herniated lumbar disk in individuals 65 years of age or older: a multicenter observational study. JAMA Surg. 2017;152(5):503-506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Lau D, Winkler EA, Than KD, Chou D, Mummaneni PV. Laminoplasty versus laminectomy with posterior spinal fusion for multilevel cervical spondylotic myelopathy: influence of cervical alignment on outcomes. J Neurosurg Spine. 2017;27(5):508-517. [DOI] [PubMed] [Google Scholar]
- 31.Turner JA, Deyo RA, Loeser JD, Von Korff M, Fordyce WE. The importance of placebo effects in pain treatment and research. JAMA. 1994;271(20):1609-1614. [PubMed] [Google Scholar]
- 32.Boogaarts HD, Bartels RH. Prevalence of cervical spondylotic myelopathy. Eur Spine J. 2015;24(S2):139-141. [DOI] [PubMed] [Google Scholar]
- 33.Kristiansen JA, Balteskard L, Slettebø Het al. The use of surgery for cervical degenerative disease in Norway in the period 2008–2014 : a population-based study of 6511 procedures. Acta Neurochir. 2016;158(5):969-974. [DOI] [PubMed] [Google Scholar]
- 34.Badhiwala JH, Witiw CD, Nassiri Fet al. Efficacy and safety of surgery for mild degenerative cervical myelopathy: results of the AOSpine North America and international prospective multicenter studies. Neurosurgery. 2019;84(4):890-897. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Bednarík J, Kadanka Z, Vohánka S, Stejskal L, Vlach O, Schröder R. The value of somatosensory- and motor-evoked potentials in predicting and monitoring the effect of therapy in spondylotic cervical myelopathy. Prospective randomized study. Spine. 1999;24(15):1593-1598. [DOI] [PubMed] [Google Scholar]
- 36.Kadanka Z, Bednarík J, Vohánka Set al. Conservative treatment versus surgery in spondylotic cervical myelopathy: a prospective randomised study. Eur Spine J. 2000;9(6):538-544. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Khan O, Badhiwala JH, Witiw CD, Wilson JR, Fehlings MG. Machine learning algorithms for prediction of health-related quality-of-life after surgery for mild degenerative cervical myelopathy [published online ahead of print: February 08, 2020]. Spine J. doi:10.1016/j.spinee.2020.02.003. [DOI] [PubMed] [Google Scholar]
- 38.Badhiwala JH, Hachem LD, Merali Zet al. Predicting outcomes after surgical decompression for mild degenerative cervical myelopathy: moving beyond the mJOA to identify surgical candidates. Neurosurgery. 2020;86(4):565-573. [DOI] [PubMed] [Google Scholar]
- 39.Fehlings MG, Badhiwala JH, Ahn Het al. Safety and efficacy of riluzole in patients undergoing decompressive surgery for degenerative cervical myelopathy (CSM-Protect): a multicentre, double-blind, placebo-controlled, randomised, phase 3 trial. Lancet Neurol. 2021;20(2):98-106. [DOI] [PubMed] [Google Scholar]
- 40.Bartels RH, van Tulder MW, Moojen WA, Arts MP, Peul WC. Laminoplasty and laminectomy for cervical sponydylotic myelopathy: a systematic review. Eur Spine J. 2015;24 (S2):160-167. [DOI] [PubMed] [Google Scholar]
- 41.Kotter MRN, Tetreault L, Badhiwala JHet al. Surgical outcomes following laminectomy with fusion versus laminectomy alone in patients with degenerative cervical myelopathy. Spine. 2020;45(24):1696-1703. [DOI] [PubMed] [Google Scholar]
- 42.van Geest S, de Vormer AM, Arts MP, Peul WC, Vleggeert-Lankamp CL. Long-term follow-up of clinical and radiological outcome after cervical laminectomy. Eur Spine J. 2015;24 (S2):229-235. [DOI] [PubMed] [Google Scholar]
- 43.Ghogawala Z, Terrin N, Dunbar MRet al. Effect of ventral vs dorsal spinal surgery on patient-reported physical functioning in patients with cervical spondylotic myelopathy: a randomized clinical trial. JAMA. 2021;325(10):942-951. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Kalsi-Ryan S, Singh A, Massicotte EMet al. Ancillary outcome measures for assessment of individuals with cervical spondylotic myelopathy. Spine. 2013;38(22 Suppl 1):S111-S122. [DOI] [PubMed] [Google Scholar]
- 45.Lubelski D, Alvin MD, Nesterenko Set al. Correlation of quality of life and functional outcome measures for cervical spondylotic myelopathy. J Neurosurg Spine. 2016;24(3):483-489. [DOI] [PubMed] [Google Scholar]
- 46.Singh A, Crockard HA. Comparison of seven different scales used to quantify severity of cervical spondylotic myelopathy and post-operative improvement. J Outcome Meas. 2001;5(1):798-818. [PubMed] [Google Scholar]
- 47.Solberg TK, Sorlie A, Sjaavik K, Nygaard OP, Ingebrigtsen T. Would loss to follow-up bias the outcome evaluation of patients operated for degenerative disorders of the lumbar spine? Acta Orthopaedica. 2011;82(1):56-63. [DOI] [PMC free article] [PubMed] [Google Scholar]