Abstract
Study Objectives
Nurses are a group at high risk for nightmares, yet little is known about the rate of nightmare disorder and associated psychosocial factors in this group in part attributable to the lack of a self-report questionnaire to assess DSM-5 criteria for nightmare disorder. Aims of the current study were to (1) report on development and initial validity of a self-report measure of DSM-5 nightmare disorder, and (2) examine the rate and associated factors of nightmare disorder among nurses.
Methods
Nurses (N = 460) completed baseline measures online including Nightmare Disorder Index (NDI), psychosocial and demographic questionnaires. A subset (n = 400) completed 14 days of sleep diaries and actigraphy.
Results
NDI demonstrated satisfactory psychometric characteristics as indicated by good internal consistency (α = 0.80), medium inter-item correlations (r = 0.50), medium to large item-total (r = 0.55–0.85) and convergent correlations (0.32–0.45), and small to medium discriminant correlations (–0.12–0.33). Per NDI, 48.7% of nurses reported no nightmares in the past month, 43.9% met partial/subthreshold criteria and 7.4% met full criteria for probable nightmare disorder. Nurses with nightmare disorder demonstrated significantly poorer psychosocial functioning (i.e. posttraumatic stress, depression, anxiety, stress) than those with subthreshold nightmare symptoms, who had poorer functioning than those with no nightmares.
Conclusions
NDI is an efficient and valid self-report assessment of nightmare disorder. Nurses have high rates of nightmares and nightmare disorder which are associated with poorer psychosocial functioning. We recommend increased nightmare screening particularly for high-risk populations such as healthcare workers.
Keywords: nightmares, psychometrics, nurses, insomnia, health, psychosocial
Statement of Significance.
The Nightmare Disorder Index is the first brief, valid screening measure for nightmare disorder as defined by the Diagnostic and Statistical Manual – 5th Edition. Increased screening for nightmare disorder is currently very limited but is urgently needed among essential workers like nurses. Among nurses, almost half reported experiencing nightmares in the past month. Nightmares were associated with increased psychosocial distress including symptoms of posttraumatic stress, depression, anxiety, and stress. Further, greater severity of nightmare disorder symptoms was associated with greater severity of psychosocial distress. In the future, the Nightmare Disorder Index should be validated in a variety of populations to help determine the generalizability of the measure and used broadly to increase frequency of nightmare screening.
Introduction
Nightmare disorder, characterized by dysphoric, recurring, well-remembered dreams which result in awakening and are associated with daytime impairment, occurs in 2%–5% of the general population [1, 2] and approximately 30% of psychiatric outpatients [3]. Nightmare disorder can present alone, but is frequently associated with comorbid sleep and/or psychological disorders including insomnia [4], posttraumatic stress disorder (PTSD), depression and anxiety [5, 6]. Nightmare disorder is also associated with increased risk for self-harm, self-directed violence, and completed suicide [7–9]. Despite the severity of nightmare disorder and its sequelae, nightmare disorder is rarely assessed or diagnosed [10], underreported to medical providers, and thus likely undertreated [11, 12].
The lack of a brief, validated assessment tool to assess nightmare disorder according to the Diagnostic and Statistical Manual of Mental Disorders – 5th edition (DSM-5) [13] is one current problem that limits the examination of the occurrence and correlates of nightmares and nightmare disorder. Most studies of nightmares rely on a single questionnaire item about nightmares drawn from questionnaires assessing other constructs (e.g. PTSD). Structured clinical interview [14] is the gold standard for assessing nightmare disorder, but interviews are not always feasible in research settings and rarely do they include this disorder. Therefore, self-report retrospective questionnaires are currently the most common method for assessing nightmares [15]. Although retrospective questionnaires could be subject to recall bias and therefore sacrifice some diagnostic accuracy, they offer several important benefits that are commensurate or superior to other methods (e.g. structured clinical interview, sleep diary). First, retrospective questionnaires are brief, affordable, and easily distributed. Second, retrospective questionnaires can be used to assess relatively longer time periods than may be feasible by prospective measures (e.g. sleep diary) without increasing participant burden. Finally, retrospective questionnaires are able to distinguish nightmare frequency from nightmare distress, which is important given evidence that distress may be the more salient factor in predicting negative outcomes [10, 16].
No validated self-report measure thoroughly assesses nightmare disorder as defined by the DSM-5 [13]. We surveyed the literature to collect the most commonly used validated measures of nightmares, which are presented in Table 1. Unfortunately, extant measures use inconsistent definitions of nightmares and nightmare disorder, which makes comparison across studies difficult [17]. As seen in Table 1, a large majority of the previously created nightmare measures fail to directly asses the chronicity (i.e. the length of time the individual has experienced nightmares) and the ability of the individual to recall the nightmare (a diagnostic criterion for nightmare disorder). Further, none of the nightmare measures identified assessed for all DSM-5 criteria of nightmare disorder (i.e. frequency, intensity, chronicity, recall, sleep disruption, daytime impact) of DSM-5 nightmare disorder.
Table 1.
List of previously developed self-report nightmare measures and the dimensions assessed.
| Nightmare dimensions assessed | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| First author (year) | N | Name of measure | # of items | Frequency | Intensity | Chronicity | Recall | Sleep disruption | Daytime impact | DSM-5 nightmare disorder |
| Belicki (1992) [51] | 540 | Nightmare Distress Questionnaire | 13 | X | X | X | ||||
| Belicki et al. (1997) [52] | –* | Nightmare Effects Survey | 12 | X | X | |||||
| Ağargün et al. (1999) [53] | 76 | Van Dream Anxiety Scale | 13 | X | X | X | X | X | ||
| Krakow et al. (2000) [54] | 169 | Nightmare Frequency Questionnaire | 2 | X | ||||||
| Davis et al. (2001) [55] | 59 | Trauma-Related Nightmare Survey | 16 | X | X | X | X | X | ||
| Köthe et al. (2001) [56] | 41 | Nightmare Behavior Questionnaire | 30 | X | X | X | ||||
| Krakow et al. (2002) [57] | 69 | Disturbing Dreams and Nightmare Severity Index | 5 | X | X | X | ||||
| Spoormaker et al. (2005) [58] | 699 | Subscale of SLEEP-50 | 5 | X | X | X | ||||
| Chen et al. (2014) [59] | 321 | Nightmare Experience Questionnaire | 21 | X | X | X | X | |||
| Schredl et al. (2014) [60] | 2929 | Mannheim Dream Questionnaire | 27 | X | X | X | X | X | ||
| Gorzka et al. (2019) [61] | 707 | Hamburg Nightmare Questionnaire | 30 | X | X | X | X | X | ||
| Kelly & Mathe (2019) [62] | 819 | Nightmare Experience Scale | 4 | X | X | |||||
| Current study | 460 | Nightmare Disorder Index | 5 | X | X | X | X | X | X | X |
Note. Intensity refers to the intensity of the nightmare (e.g. difficult to push out of your mind, difficulty falling back to sleep). Chronicity refers to the length of time the individual has suffered from nightmares.
*Original article and thus N is unavailable; measure information drawn from description in Krakow et al. [54].
Nurses may be at increased risk for nightmare disorder due to factors including irregular shift schedules, high stress work environment, and high exposure to trauma, yet little is known about the rate and associated psychosocial factors in this population. Nurses serve as the front line of patient care and thus are by nature frequently exposed to traumatic events (e.g. witnessing serious injury and death) and vicarious traumas [18]. Approximately 5% of the population reports nightmares and the rate of nightmares increase drastically in populations who have experienced a traumatic event (e.g. up to 50% of trauma-exposed adults [19]; approximately 24% of nurses) [20]. In one study, [21] 35% of nurses (N = 332) reported nightmares related to their work experiences on a single-item self-report item, which queried the presence of nightmares related to the job description or environment. Nurses reported triggers associated with nightmares included performing end of life care, feeling overextended, caring for combative individuals, and visualizing open wounds or bleeding [21]. Unfortunately, nightmares in the nurse population are discussed in the literature almost exclusively in the context of PTSD, despite the fact that nightmares are commonly reported among individuals without PTSD. Indeed, one study of N = 173 pediatric acute care nurses found 49% of nurses reported nightmares associated with their work, though only 21% of the sample reported significant PTSD symptoms (91% of whom reported nightmares) [22]. Nightmares are associated with increased suicide risk above the effects of depression and PTSD [7, 8], and frequently persist even after successful treatment for PTSD [23]. Although the two aforementioned studies [21, 22] established an estimate of the rate of nightmares in nurses using a single item measure, to our knowledge, there is no existing estimate of the rate of nurses who meet full criteria for nightmare disorder.
One potential consequence of the lack of a screening questionnaire for nightmare disorder is that little is known about the rate of nightmares and associated psychosocial and sleep factors, especially among nurses. Thus, the aims of the current study were twofold. The primary aim was to report on the development and preliminary validation of the Nightmare Disorder Index (NDI), a brief self-report screening questionnaire for DSM-5 nightmare disorder. The secondary aim was to describe the rate and compare the psychosocial functioning and sleep parameters of nurses with (1) no nightmares, (2) subthreshold nightmare disorder symptoms, and (3) probable nightmare disorder.
Methods
Procedure
Participants were nurses at two area hospitals in north Texas recruited for a parent study, “Sleep and Vaccine Response in Nurses (SAV-RN)” (R01AI128359-01: PIs: Taylor & Kelly). Nurses (N = 460) completed baseline measures online and a subset of nurses (n = 400) subsequently completed 14 days of sleep and nightmare diaries and actigraphy.
Sample
Participant characteristics (N = 460) are reported in Table 2. In brief, the majority of participants were female (91.0%), white (77.3%), and non-Hispanic (89.2%), currently married (61.2%) and had children (63.7%). The larger and smaller samples were compared and did not significantly differ on any of the characteristics examined in the current study.
Table 2.
Participant characteristics by nightmare status on the Nightmare Disorder Index
| Total sample (N = 460) | No nightmares (N = 224) | Subthreshold nightmare symptoms (N = 202) | Probable nightmare disorder (N = 34) | ||||
|---|---|---|---|---|---|---|---|
| n (% of sample) or M (SD) | n (% of column) or M (SD) | n (% of column) or M (SD) | n (% of column) or M (SD) | F or χ2 | p | Part. η2, φ, or V | |
| Age | 39.02 (11.08) | 40.19 (11.43) | 37.89 (10.69) | 38.06 (10.46) | 2.43 | 0.089 | .011 |
| Sex | 5.74 | 0.057 | .112 | ||||
| Male | 41 (8.9%) | 27 (12.0%) | 13 (6.4%) | 1 (2.9%) | |||
| Female | 419 (91.1%) | 197 (87.9%) | 189 (93.6%) | 33 (97.1%) | |||
| Race* | 0.46 | 0.794 | .032 | ||||
| White | 357 (77.6%) | 176 (78.6%) | 156 (77.2%) | 25 (73.5%) | |||
| Black/African American | 31 (6.7%) | 12 (5.4%) | 15 (7.4%) | 4 (11.8%) | |||
| Asian | 51 (11.1%) | 25 (11.2%) | 22 (10.9%) | 4 (11.8%) | |||
| Multiracial/other | 21 (4.6%) | 11 (4.9%) | 9 (4.5%) | 1 (2.9%) | |||
| Ethnicity+ | 0.91 | 0.633 | .045 | ||||
| Hispanic/Latino | 47 (10.3%) | 22 (9.8%) | 20 (9.9%) | 5 (14.7%) | |||
| Not Hispanic/Latino | 410 (89.7%) | 200 (89.3%) | 182 (90.0%) | 28 (82.4%) | |||
| Marital status | 7.53 | 0.110 | .090 | ||||
| Married | 282 (61.3%) | 137 (61.2%) | 131 (64.9%) | 14 (41.2%) | |||
| Single | 125 (27.2%) | 59 (26.3%) | 51 (25.2%) | 15 (44.1%) | |||
| Divorced/separated/ widowed | 53 (11.5%) | 28 (12.5%) | 20 (9.9%) | 5 (14.7%) | |||
| Children | 4.82 | 0.090 | .102 | ||||
| No children | 167 (36.3%) | 70 (31.3%) | 83 (41.1%) | 14 (41.2%) | |||
| Has children | 293 (63.7%) | 154 (68.8%) | 119 (58.9%) | 20 (58.8%) | |||
| Number of children | 1.36 (1.28) | 1.47 (1.24) | 1.22 (1.29) | 1.41 (1.46) | 2.00 | 0.137 | .009 |
| Work schedule+ | 10.58 | 0.005 | .153 | ||||
| Day shift only | 292 (64.3%) | 140 (62.5%) | 138 (68.3%)a | 14 (41.2%)a | |||
| Night or rotating | 162 (35.7%) | 82 (36.6%) | 60 (29.7%)b | 20 (58.8%)b |
Note. +For these measures, n = 457, n = 454 due to missing data.
*Due to small cell sizes, statistical comparison for race was collapsed to white vs. other.
abNonmatching letter pairs within columns indicate significantly different observed value than expected for post hoc comparisons (adjusted standardized residuals).
Measures
Development of the Nightmare Disorder Index (NDI)
The NDI is a 5-item self-report screening measure intended to evaluate symptoms of nightmare disorder according to DSM-5 diagnostic criteria (see Appendix 1) [13]. In brief, the DSM-5 criteria for nightmare disorder includes: (1) repeated occurrences of extended, extremely Supplementary Materials dysphoric, and well-remembered dreams, (2) on awakening from the dysphoric dreams, the individual rapidly becomes oriented and alert, (3) the sleep disturbance causes clinically significant distress or impairment in social, occupational, or other areas of functioning, (4) the nightmare symptoms are not attributable to the physiological effects of a substance, and (5) coexisting medical and mental disorders do not adequately explain the predominant complaint of dysphoric dreams [13]. The DSM-5 does not specify a frequency of nightmares required for diagnosis, though a generally accepted threshold is a minimum of one nightmare episode per month.
NDI questions assess nightmare frequency, characteristics, distress, and impairment, and duration that nightmares have been experienced with individual ratings ranging from 0 to 4. The NDI can be summed to obtain a total score ranging from 0 to 20, with higher scores indicating greater nightmare severity, or alternately used dichotomously to determine whether it is likely that an individual meets DSM-5 criteria for nightmare disorder (i.e. endorses all criteria above threshold). Individuals were considered to meet DSM-5 criteria for probable nightmare disorder if they endorsed nightmares more than zero times per week (on a 5-point scale ranging from 0 nights per week to nightly [seven nights per week]) and reported a frequency of “sometimes” or greater for questions regarding alertness after a nightmare, distress, and impairment (indicated by gray shading on the NDI; Appendix 1). In the current study, subthreshold nightmare disorder status was defined as endorsing any nightmares (i.e. frequency of Supplementary Materials nightmares more than zero times per week) but less than “sometimes” on one or more of the questions regarding alertness after a nightmare, distress, and impairment. The NDI was developed by our team of experts based on the content of the DSM-5 diagnostic criteria in a format similar to the Sleep Condition Indicator [24].
Convergent measures
PTSD checklist for DSM-5 (PCL-5); nightmare item
The current study included one question from the PCL-5 (described below) regarding nightmares as a convergent measure: “In the past month, how much were you bothered by repeated, disturbing dreams of the stressful experience?” This item was chosen because it is frequently used as the basis for assessing nightmares in the current literature. However, this item does not assess whether the disturbing dream causes an awakening or assess nightmares unrelated to the identified traumatic event.
Sleep diary nightmare items
Two items of nightmares were added to the CSD (described below), which participants reported on after waking each day of the study. The two items were included as convergent measures: “How many nightmares did you have that woke you up?” (participants could enter any number) and “How would you rate the overall severity of your nightmares?” (response options ranged from 0 = not at all to 4 = extremely). The generalizability coefficients for within person variations averaged over time (time nested within people) were 0.98 and 0.97, respectively, indicating high reliability. Responses to these items over 14 days were averaged to facilitate comparison to the NDI.
Pittsburgh Sleep Quality Indicator (PSQI); nightmare item
The PSQI is a 19-item self-rated questionnaire that is used as a broad measure of sleep quality. The PSQI has demonstrated excellent reliability and validity in samples of health controls, patients with sleep disorders, and depressed patients [25]. The current study only included the PSQI question regarding nightmares: “During the past month, how often have you had trouble sleeping because you have bad dreams?” This item is also commonly used to assess nightmares in the current literature.
Discriminant measures
Actigraphy-derived total sleep time (TST)
The current study included the measure of actigraphy-assessed total sleep time (TST) as a discriminant measure as it is unexpected that objective total sleep time would be significantly related to the presence or frequency of nightmares. Two prior studies have demonstrated that average objective (PSG) total sleep time does not differ for individuals with and without frequent nightmares [26, 27]. Rather, differences are more pronounced regarding the subjective experience of sleep. Although PSG and actigraphy are not entirely overlapping methods, we were also guided by research which has shown a discrepancy between sleep diary and actigraphy estimates of sleep among individuals with PTSD [28]. Further, DSM-5 criteria do not specify that nightmares must cause trouble falling back to sleep (a symptom of insomnia), only that they cause nighttime awakenings. Therefore, an individual could have frequent nightmares and awakenings, but still have adequate objective sleep duration (if they are able to return to sleep, extend time in bed to account for awakenings, or if nightmares happen early in the morning after a full night of sleep). Regardless, prior research has shown even insomnia (e.g. “trouble falling back to sleep”) as measured by the Insomnia Severity Index is not related to actigraphy-assessed TST [29].
Daily diary survey; mean alcoholic drinks
The current study included the data from the Quick Drinking Screen (described below), collected in a daily diary format across the 14 days of the study, to assess self-reported daily mean alcoholic drinks as a discriminant measure. The generalizability coefficient for within person variations averaged over time (time nested within people) was 0.99, indicating high reliability.
Composite Scale of Morningness – Reduced (rCSM)
The rCSM [30] is a 7-item version of the Composite Scale of Morningness [31]. The rCSM is a self-report measure intended to capture an individual’s chronotype, or circadian preference. Scores range from 7–30, with scores 7–15 indicating evening chronotype, scores 16–20 indicating intermediate chronotype, and scores 20–30 indicating morning chronotype. The rCSM has demonstrated excellent psychometric properties, correlating with self-reported sleep–wake rhythm, sleep midpoint, and other previously validated measures of chronotype [30]. In the current study, the rCSM demonstrated good internal consistency (α = 0.83).
Patient Health Questionnaire-9 (PHQ-9)
[32]. The PHQ-9 is a 9-item self-report measure used widely to assess the severity of depressive symptoms. It assesses both affective and somatic symptoms related to depression and depressive disorders and corresponds to the diagnostic criteria for DSM-5 Major Depressive Disorder [13]. The PHQ-9 is summed to obtain a total score ranging from 0 to 27, with greater scores indicating greater depressive symptomatology. A score ≥10 indicated clinically significant depression (i.e. moderate to severe depression symptoms) [33]. The PHQ-9 has been well-validated and demonstrated good sensitivity and specificity (88% for both) compared to a structured clinical interview [32]. In the current study, the PHQ-9 had good internal consistency (α = 0.87).
Generalized Anxiety Disorder Screener (GAD-7)
[34]. The GAD-7 is a 7-item self-report measure used widely to screen for generalized anxiety disorder and assess the severity of anxiety symptoms. The GAD-7 is summed to obtain a total score ranging from 0 to 21, with greater scores indicating greater anxiety symptoms. A score ≥10 indicated clinically significant anxiety (i.e. moderate to severe anxiety symptoms). The GAD-7 has been well-validated and demonstrated good sensitivity (89%) and specificity (82%) compared to a structured clinical interview [34]. In the current study, the GAD-7 demonstrated good internal consistency (α = 0.89).
PTSD checklist for DSM-5 (PCL-5)
[35]. The PCL-5 is a 20-item self-report measure used widely to assess the symptoms of PTSD identified by the DSM-5. The measure is summed to obtain a total score ranging from 0 to 80, with greater scores indicating greater PTSD symptom severity. A score ≥33 indicates clinically significant PTSD (i.e. moderate to severe PTSD symptoms) [36]. In a previous study, the PCL-5 demonstrated good internal consistency, test-retest reliability, and convergent and discriminant validity [35]. In the current study, the PCL-5 demonstrated good internal consistency (α = 0.94). In discriminant validity analyses, we used a calculation of the PCL-5 without the nightmare item. For all other analyses, we included the full measure.
Perceived Stress Scale (PSS)
[37]. The PSS is a 10-item self-report questionnaire used widely to assess the stress domains of unpredictability, lack of control, burden overload, and stressful life circumstances. The measure is summed to obtain a total score ranging from 0 to 40, with greater scores indicating greater perceived stress. A score ≥27 indicates clinically significant stress (i.e. severe stress symptoms) [38]. The PSS has previously demonstrated good internal consistency, factor reliability, and hypothesis validity [39]. In the current study, the PSS demonstrated good internal consistency (α = 0.85).
Additional sleep, psychosocial, and personality measures
Consensus Sleep Diary (CSD)
[40]. The Consensus Sleep Diary is a self-report, prospective assessment of subjective sleep patterns (e.g. duration, efficacy, circadian midpoint). Participants completed a daily sleep diary for 14 days via REDCap on their smartphone device upon waking. Sleep diaries are significantly correlated with polysomnography (PSG) on sleep onset latency, wake time after sleep onset, total sleep time, and sleep efficiency (r = 0.23–0.56) [41, 42] in several populations and are preferable to single-point retrospective estimates of sleep. The sleep diary included two items to assess nightmare frequency (i.e. how many nightmares the individual had that night) and severity (i.e. the perceived intensity of or disturbance produced by the nightmare episode; further described below in the Convergent Measures section).
Actigraphy
Actigraphy is a prospective measure of sleep and activity patterns used concurrently with sleep diaries to assess inferred sleep parameters (e.g. duration, efficiency, midpoint). Actigraphy was recorded for 14 days with Actiwatch Spectrum devices (Phillips Respironics, Andover, MA), which are compact, wrist-worn, battery-operated activity monitors that look similar to a small wristwatch with an event marker button participants can press to indicate in and out of bed times [43]. Scoring was performed according to guidelines developed by an expert task force of the Society of Behavioral Sleep Medicine including one of the authors of the current study (DJT) [44]. Two trained research assistants independently set sleep intervals for each actigraphy record using an internally developed scoring hierarchy [45] that relies on an iterative process of examining, in order of priority, event markers, sleep diary data, activity, and light levels. Naps were not included in analyses. Discrepancies between the double-scored data were resolved by a third individual. Once intervals were set, data were analyzed using the default algorithm and exported using the following settings: 10 immobile minutes for sleep onset and offset, and medium wake threshold (40 activity counts).
Quick Drinking Screen
[46]. The QDS is a 4-item self-report screening measure intended to identify people with hazardous or harmful patterns of alcohol consumption. The four items of the QDS assess the frequency and amount of alcohol use across the past 2 weeks. The QDS has previously been validated against the Timeline Followback daily estimation measure of alcohol use, and it shows good psychometric properties [46, 47]. In the current study, the PSS demonstrated acceptable internal consistency (α = 0.70).
Big Five Inventory (BFI-2)
[48]. The BFI-2 is a 60-item self-report questionnaire assessing big five personality traits (i.e. extraversion, agreeableness, conscientiousness, negative emotionality, and open-mindedness). In the current sample, the Cronbach’s alpha for the BFI-2 extraversion subscale was 0.85, 0.73 for the agreeableness subscale, 0.87 for the neuroticism subscale, 0.84 for the conscientiousness subscale, and 0.84 for the openness to experience subscale.
Analyses
Prior to analyses, all data were screened for missingness, outliers, and violation of assumptions (e.g. excessive skew). Convergent validity (i.e. the degree of concordance between the NDI and another measure of sleep) was assessed by calculating Pearson or Spearman correlation coefficients (as appropriate) between the NDI and the measures listed above under “convergent measures.” Discriminant validity (i.e. the degree of concordance between the NDI and measures not assessing nightmares) was assessed by calculating Pearson or Spearman correlation coefficients (as appropriate) between the NDI and the measures listed above under “discriminant measures.” Exploratory factor analysis was conducted to examine the latent factor structure of the NDI (only including those who endorsed any nightmares on the NDI). Principal axis factoring was used and multiple factor extraction methods were examined per recommendations of Henson and Roberts [49], including Kaiser method [50], scree plot examination [51], parallel analysis [52], and minimum average partial [52].
Comparisons between nurses with no nightmares, subthreshold nightmare complaints, and probable nightmare disorder were conducted using one-way ANOVAs or χ2 (as appropriate). Holm–Bonferroni [53] sequential corrections were applied to p-values to adjust for multiple comparisons within group (i.e. within psychosocial measures group, within sleep parameters group) [54].
Results
Psychometrics of Nightmare Disorder Index
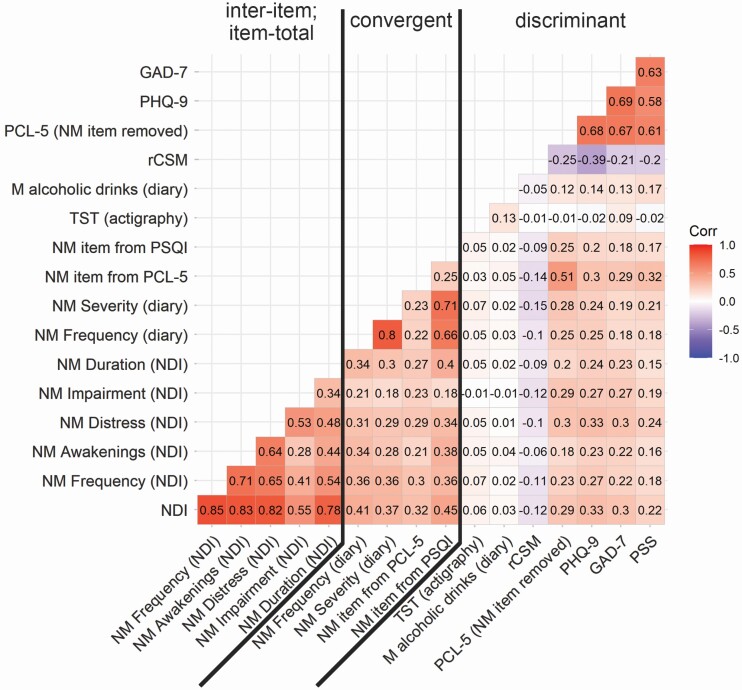
The NDI total score mean was 4.14 (SD = 2.41) for those with subthreshold nightmare disorder symptoms and 9.24 (SD = 2.62) for those who met full criteria for nightmare disorder based on the NDI. The mean was not calculated for individuals who endorsed no nightmares, as their total score is zero. In the current study, the NDI had good internal consistency (α = 0.80). Inter-item and item-total correlations are shown in Figure 1. Inter-item correlations ranged from r = 0.28 to 0.71, with an average inter-item correlation of r = 0.50. The item-total correlation with the total NDI was highest for the nightmare frequency question (r = 0.85) and lowest for the nightmare impairment question (r = 0.55).
Figure 1.
Inter-item, item-total, convergent, and discriminant correlations between Nightmare Disorder Index facets and other nightmare and non-nightmare measures. Note: TST, total sleep time; NM, nightmare; NDI, Nightmare Disorder Index; PCL-5, Posttraumatic Stress Disorder Checklist; PSQI, Pittsburgh Sleep Quality Index; rCSM, reduced Composite Scale of Morningness.
Correlations to establish convergent validity are shown in Figure 1. In general, the NDI total score had medium to large correlations with averaged 14-day diary (r = 0.37–0.41) and single-item (r = 0.32–0.45) measures of nightmares, demonstrating acceptable convergent validity. The highest correlation for the total NDI score was between the NDI total score and the nightmare item from the PSQI, and the lowest correlation was with the nightmare item from the PCL-5. The correlation between the NDI frequency component and average nightmare frequency on the sleep diary was moderate, as was the correlation between the NDI distress component and nightmare severity on the diary. Correlations to establish discriminant validity are shown in Figure 1. In general, the NDI had small correlations (all rs < ±0.15) with measures of constructs which were not expected to be related to nightmare disorder (i.e. actigraphy-derived total sleep time, mean alcoholic drinks, and chronotype), demonstrating good discriminant validity. The NDI had moderate correlations (rs = 0.22–0.33) with constructs which were expected to be somewhat related with nightmare disorder yet not entirely overlapping (i.e. posttraumatic stress, depression, anxiety, perceived stress).
Results from the principal axis factoring analysis provided evidence for a unitary factor structure after examining each of the factor retention methods listed above. The single factor which was retained, which we named “NDI,” had an eigenvalue of 2.31 and reproduced 33.72% of the variance in the items. Pattern coefficients for all items were in the moderate to high range indicating all items were strongly associated with the extracted factor. See Table 3 for factor structure of the NDI.
Table 3.
Pattern/structure coefficients and extracted communalities for the Nightmare Disorder Index
| Item | Factor 1: NDI | h 2 |
|---|---|---|
| 1. Frequency | 0.62 | 0.38 |
| 2. Awakenings | 0.42 | 0.18 |
| 3. Distress | 0.75 | 0.57 |
| 4. Impairment | 0.53 | 0.28 |
| 5. Duration | 0.53 | 0.28 |
Nightmare disorder associations with psychosocial and sleep factors
As shown in Table 2, 48.7% (n = 224) of nurses reported no nightmares in the past month on the NDI, whereas 43.9% (n = 202) met partial/subthreshold criteria and 7.4% (n = 34) met full criteria for probable nightmare disorder. Of the subsample who additionally completed sleep diary and actigraphy measures (n = 400), rates on the NDI were comparable (47.5%, 44.5%, 8.0%, respectively). Demographics did not differ by nightmare disorder status. Night-/rotating-shift workers were more likely to have subthreshold nightmares or probable nightmare disorder compared to day-shift workers. Psychosocial characteristics by nightmare disorder status are shown in Table 4. Significant differences between nightmare status groups were found for depression, anxiety, perceived stress, PTSD symptoms, and the negative emotionality dimension of personality. The pattern was consistent across these constructs, where participants with no nightmare symptoms reported the lowest mean values, followed by those with subthreshold nightmare symptoms, followed by those with probable nightmare disorder. The result remained the same for PTSD symptoms when the nightmare item was removed from the scale, F(2, 456) = 17.97, p < 0.001. Rates of clinically significant PTSD symptoms on the PCL-5 differed significantly between those with no nightmares and with subthreshold nightmare symptoms (both 9.4%) compared to those with probable nightmare disorder (32.4%), χ2(2) = 16.78, p < 0.001. There were no significant differences found between nightmare groups for alcoholic drinks per week, chronotype, or the other four personality traits (i.e. openness, conscientiousness, extraversion, agreeableness).
Table 4.
Psychosocial characteristics by nightmare status on the Nightmare Disorder Index
| Total sample (N = 460) | No nightmares (N = 224) | Subthreshold nightmare symptoms (N = 202) | Probable nightmare disorder (N = 34) | p* | Part. η2 | |
|---|---|---|---|---|---|---|
| M (SD) | M (SD) | M (SD) | M (SD) | |||
| Depression (PHQ-9) | 3.68 (4.03) | 2.87 (3.51)a | 3.86 (3.86)b | 8.03 (5.21)c | <0.001 | 0.107 |
| Anxiety (GAD-7) | 2.83 (3.56) | 2.13 (3.20)a | 3.12 (3.45)b | 5.76 (4.72)c | <0.001 | 0.072 |
| Perceived Stress (PSS) | 12.33 (6.35) | 11.32 (6.25)a | 12.75 (6.19)b | 16.47 (6.17)c | <0.001 | 0.046 |
| PTSD Symptoms (PCL-5)+ | 19.12 (10.75) | 17.00 (8.99)a | 19.86 (11.20)b | 28.57 (13.06)c | <0.001 | 0.078 |
| Alcoholic Drinks per Week (QDS)+ | 2.50 (3.91) | 2.63 (3.28) | 3.19 (4.28) | 3.59 (5.18) | 0.414 | 0.007 |
| Chronotype (rCSM) | 19.23 (4.49) | 19.82 (4.54) | 18.73 (4.26) | 18.26 (4.99) | 0.090 | 0.017 |
| Personality Dimensions (BFI-2) | ||||||
| Openness | 3.73 (0.60) | 3.75 (0.62) | 3.71 (0.59) | 3.75 (0.60) | 0.838 | 0.001 |
| Conscientiousness | 4.22 (0.60) | 4.28 (0.59) | 4.20 (0.62) | 4.03 (0.54) | 0.171 | 0.012 |
| Extraversion | 3.62 (0.72) | 3.69 (0.73) | 3.59 (0.69) | 3.37 (0.69) | 0.116 | 0.015 |
| Agreeableness | 4.25 (0.49) | 4.28 (0.49) | 4.25 (0.45) | 4.01 (0.59) | 0.078 | 0.019 |
| Negative emotionality | 2.31 (0.74) | 2.17 (0.75)a | 2.38 (0.69)b | 2.86 (0.75)c | <0.001 | 0.062 |
Note. PHQ-9, Patient Health Questionnaire-9; GAD-7, General Anxiety Disorder-7; PSS, Perceived Stress Scale; PTSD, posttraumatic stress disorder; PCL-5, PTSD Checklist-5; QDS, Quick Drinking Screen; rCSM, reduced Composite Scale of Morningness; BFI-2, Big Five Inventory-2.
+For these measures, n = 459 due to missing data.
*p-values adjusted for multiple comparisons using Holm–Bonferroni correction.
abcNonmatching letter pairs indicate significant difference for Tukey post-hoc comparisons across rows.
Sleep characteristics by nightmare disorder status are shown in Table 5. Significant differences were found for sleep quality and insomnia symptoms. The pattern was consistent across these constructs, where participants with no nightmare symptoms reported the lowest mean values, followed by those with subthreshold nightmare symptoms, followed by those with probable nightmare disorder. Among sleep diary variables, participants with any nightmares had more awakenings per night and worse nightly sleep quality compared to participants with no nightmares as assessed by the NDI, but participants with subthreshold versus probable nightmare disorder did not differ significantly. On the sleep diary, participants with probable nightmare disorder had more frequent nightmares than those with subthreshold nightmares, who in turn had more frequent nightmares than those with no nightmares. On nights in which nightmares were reported, individuals with subthreshold nightmares (n = 101) reported more severe nightmares than those with no nightmares on the NDI (n = 70). Individuals with probable nightmare disorder (n = 25) did not differ from either group in terms of nightmare severity. There were no significant differences between groups on actigraphy-derived sleep parameters.
Table 5.
Sleep characteristics by nightmare status on the Nightmare Disorder Index
| Total subsample (N = 400) | No nightmares (N = 190) | Subthreshold nightmare symptoms (N = 178) | Probable nightmare disorder (N = 32) | ||||
|---|---|---|---|---|---|---|---|
| M (SD) | M (SD) | M (SD) | M (SD) | F | p* | Part. η2 | |
| Questionnaires | |||||||
| Sleep Quality (PSQI)+ | 5.27 (2.38) | 4.71 (2.11)a | 5.54 (2.42)b | 7.33 (2.57)c | 17.68 | <0.001 | 0.085 |
| Insomnia Symptoms (ISI)+ | 5.77 (4.5) | 4.65 (3.99)a | 6.40 (4.62)b | 9.00 (4.67)c | 15.96 | <0.001 | 0.076 |
| Sleep Diary | |||||||
| SOL (min) | 17.98 (15.36) | 17.47 (16.21) | 17.91 (14.58) | 21.43 (14.41) | 0.91 | 1.0 | 0.005 |
| NWAK (num) | 1.70 (1.00) | 1.46 (0.90)a | 1.86 (1.04)b | 2.28 (1.03)b | 13.76 | <0.001 | 0.065 |
| WASO (min) | 11.28 (11.25) | 10.60 (11.24) | 11.32 (10.99) | 15.05 (12.37) | 2.15 | 1.0 | 0.011 |
| TWAK (min) | 13.31 (10.88) | 13.26 (11.83) | 13.15 (10.05) | 14.44 (9.64) | 0.19 | 1.0 | 0.001 |
| TST (min) | 431.95 (49.86) | 429.07 (47.95) | 437.51 (50.70) | 418.07 (53.54) | 2.69 | 0.690 | 0.013 |
| SE (%) | 90.96 (5.16) | 91.10 (5.27) | 91.19 (4.92) | 88.83 (5.53) | 2.99 | 0.676 | 0.015 |
| SM (time) | 4.19 (2.66) | 4.18 (2.58) | 4.06 (2.67) | 5.00 (3.04) | 1.66 | 1.0 | 0.008 |
| Quality (0–4) | 2.57 (0.56) | 2.68 (0.57)a | 2.50 (0.54)b | 2.30 (0.47)b | 8.73 | <0.001 | 0.042 |
| Nightmare Frequency (sum) | 1.36 (2.25) | 0.67 (0.09)a | 1.75 (0.19)b | 3.31 (0.61)c | 26.68 | <0.001 | 0.118 |
| Nightmare Severity | 1.31 (0.70) | 1.12 (0.09)a | 1.43 (0.07)b | 1.37 (0.09) | 4.34 | 0.014 | 0.043 |
| Actigraphy | |||||||
| SOL+ (min) | 12.72 (10.71) | 12.45 (10.39) | 13.13 (11.33) | 12.09 (9.04) | 0.24 | 1.0 | 0.001 |
| NWAK+ (num) | 30.48 (8.49) | 29.72 (8.30) | 31.59 (8.57) | 28.76 (8.66) | 2.93 | 0.676 | 0.015 |
| WASO+ (min) | 33.30 (13.58) | 31.61 (12.73) | 34.73 (13.73) | 35.41 (16.74) | 2.83 | 0.676 | 0.014 |
| TWAK+ (min) | 13.70 (8.70) | 13.66 (9.45) | 13.71 (8.14) | 13.79 (7.18) | 0.00 | 1.0 | 0.000 |
| TST+ (min) | 402.01 (50.89) | 398.13 (51.91) | 407.04 (49.52) | 396.76 (51.40) | 1.58 | 1.0 | 0.008 |
| SE+ (%) | 86.95 (4.88) | 87.15 (5.08) | 86.84 (4.66) | 86.38 (4.99) | .412 | 1.0 | 0.002 |
| SM+ (time) | 4.24 (2.72) | 4.15 (2.53) | 4.18 (2.79) | 5.14 (3.27) | 1.85 | 1.0 | 0.009 |
Note. PSQI, Pittsburgh Sleep Quality Index; ISI, Insomnia Severity Index; SOL, sleep onset latency; NWAK, number of awakenings; WASO, wake after sleep onset; TWAK, terminal wakefulness; TST, total sleep time; SE, sleep efficiency; SM, sleep midpoint.
+For these measures, ns range from 387 to 396 due to missing data.
abcNonmatching letter pairs indicate significant difference for Tukey post-hoc comparisons across rows.
*p-values adjusted for multiple comparisons using Holm–Bonferroni correction.
Discussion
These findings provide preliminary evidence that the NDI is a brief, reliable, and valid assessment of nightmare disorder, particularly among nurses. The rate of nightmare disorder (7.4%) in the current sample was higher than previous studies of the general population (2%–5%) [1, 2], and much lower than rates previously reported by psychiatric outpatients (30%) [3]. The frequency of nightmare disorders in nurses is expected to be a little higher than the general population, given their stressful working environment, but much lower than an outpatient psychiatric population, given psychiatric symptoms were not a requirement for inclusion in the study. The current study found rates of subclinical or higher nightmare symptoms (51.3%) to be greater than the 35% previously reported by nurses who completed a single-item self-report measure that is likely less sensitive than the NDI [21]. Single item measures, which are common in the nightmare literature, risk misrepresenting the severity and prevalence of nightmare disorder. Additionally, these single items each examine only a single dimension of the nightmare experience (e.g. frequency or distress), which could in part explain why correlations with the NDI, which assesses each of the DSM-5 criterion (i.e. frequency, intensity, chronicity, recall, sleep disruption, daytime impact) for nightmare disorder, were lower than anticipated. In contrast to existing single item measures, the NDI is likely more sensitive and specific for specifically assessing nightmare disorder symptoms, though this will need to be confirmed in follow up studies. The supply of trained nurses is scarce, so a reliable, valid, sensitive and specific nightmare screening measure should be helpful in identifying nurses who might benefit from a brief nightmare specific treatment [55], which in turn might reduce psychotherapy stigma, high turnover, and burnout.
Nightmares (subclinical and probable diagnosis) were associated with significant psychosocial burden across nurses and occurred at a greater frequency in nurses working rotating or night shifts. The severity of nightmare symptoms was related to the severity of the psychosocial burden, such that nurses who had probable nightmare disorder based on the NDI had significantly greater symptoms of depression, anxiety, perceived stress, and PTSD symptoms compared to nurses with subthreshold or no nightmares. Further, a similar pattern was shown for the negative emotionality dimension of personality which may be a contributing factor to this finding. The rate of nightmares and associated psychosocial factors of this population is particularly troublesome given the integral role nurses play in the health care system and warrants further exploration and treatment of nightmares in this population.
Despite a general paucity of research on nightmare disorder in nurse populations, these findings replicate previous research investigating the heightened risk of other mental health symptoms in various domains of functioning for nurses. A sample of pediatric intensive care nurses displayed heightened rates of PTSD (21%), nightmares (49%), anxiety symptoms (16%), depression symptoms (10%), and overall burnout (68%), with approximately 82% of the nurses reporting at least one significantly distressing psychological symptom [22]. Similarly, nurses in acute or critical care experienced elevated rates of PTSD (24%) [20]. One previous study demonstrated approximately 14% of general practice nurses displayed significant PTSD symptoms [20], which is similar to the rate of 11% found in the current study. Although clinically significant PTSD symptoms were significantly higher among those with probable nightmare disorder compared to those with subthreshold or no nightmares, PTSD does not appear to be the sole driver of nightmare disorder reporting in this sample; only a third of those with probable nightmare disorder reported significant PTSD symptoms. The results of this study are consistent with previous research which demonstrates nurses carry a significant psychosocial burden. Given the finding that these psychosocial symptoms increase with the severity of nightmare disorder symptoms, this indicates a need for further research on the detection and treatment of nightmares, particularly for nurses.
Additionally, this study indicated nurses who engage in overnight or rotating shift work experience more severe nightmare symptoms than do those who only work the day shift. This finding is also consistent with previous research that suggests shift workers experience higher rates of parasomnias including nightmares [56]. One hypothesis to explain this relationship between shift work and nightmares is the significant increase in REM sleep during the daytime sleep for shift workers [57]. It is possible that the increase in REM sleep pressure and frequency of interruptions in REM sleep for nurses engaging in regular shift work in turn increases the propensity to experience nightmares [58]. Although examining sleep architecture was outside the scope of the current study, this is an important future direction when considering the mechanisms of increased parasomnias among nurses.
Probable nightmare disorder, and to a lesser extent subthreshold nightmares, were associated with greater subjective number of awakenings and poorer self-reported sleep quality across the 14 days of sleep diary. These results are overall consistent with self-report of nightmare experiences, in which the dreams cause awakenings often paired with heightened physiological arousal (e.g. racing heart, shallow breathing, sweating). Individuals who report difficulty returning to sleep are more likely to form a memory of the awakening and thus individuals who report nightmares may experience their sleep as more fragmented and less restorative. Although groups differed on number of awakenings, they did not significantly differ on wake after sleep onset on the sleep diary. There are several potential explanations for this. First, the WASO was based on two full weeks of sleep diaries. WASO on nights without nightmares might be low or 0, which could lower the mean WASO overall even if WASO is longer on nights with nightmares. Second, examining individual means across the groups reveals about the amount of WASO one would expect given the number of awakenings. By dividing WASO/number of awakenings (NWAK), we see the average length of awakening for the probable nightmare disorder group is 6.6 min, versus 6.1 min for the subthreshold nightmares group and 7.3 min for the no nightmares group. The differences in WASO are small, thus not statistically significantly different, but the magnitude of differences is unsurprising in the context of the relatively small group differences in NWAK. Third, WASO and NWAK are not necessarily highly related. Individuals with nightmares could wake frequently, but briefly, which would demonstrate high NWAK but low WASO. Alternatively, individuals with insomnia could wake only once or twice in the night but be awake for a longer period of time, which would demonstrate NWAK but higher WASO. It appears that individuals with nightmares in this sample fell more into the former category rather than the latter.
There were no significant differences between groups (i.e. no nightmares, subthreshold nightmare symptoms, probable nightmare disorder) for any actigraphy-derived sleep parameters. Actigraphy tends to have low specificity to detect wakefulness among sleep-disordered populations [59], but it is surprising that differences did not arise given the nature of nightmare awakenings is likely to induce significant movement. It is possible that 14 days of actigraphy was not long enough to detect differences between groups given that someone may experience nightmares once a week or once a month and still qualify for a diagnosis of nightmare disorder. Previous studies similarly have shown that individuals with frequent nightmares report poorer subjective sleep quality, more waking problems, and more severe insomnia symptoms, but no differences in overall PSG sleep architecture [26]. The current study reveals nightmares and probable nightmare disorder primarily impact number of awakenings and perceived quality of sleep. More research is needed using a comprehensive measurement strategy to better understand the impact of nightmares on sleep.
The current study presents with a variety of strengths and fills an important gap in the understanding of nightmare disorder. To date, we are unaware of any studies that estimate the rate of DSM-5 criteria nightmare disorders in nurses. Given the well documented deleterious implications of nightmare disorder (e.g. increased symptoms of depression, anxiety, burnout), this knowledge of nightmare disorder prevalence is important to the mental health of nurses as well as their job satisfaction and performance. Given the integral role nurses play in the health care system, this is beneficial to not only nurses themselves but also to society. Additionally, this study provides the first brief assessment for DSM-5 defined nightmare disorder. As indicated in Table 1, although various nightmare questions exist, they often do not assess important domains of the nightmares (e.g. recall, sleep/wake impact) or are possibly burdensome for the participant/patient to complete (e.g. 30 items). The NDI fills this gap in sleep disorder assessment by providing a psychometrically sound, 5-item assessment for DSM-5 nightmare disorder that can be used as both a continuous measure of nightmare severity and a categorical measure of nightmare disorder.
While the current study demonstrated many strengths, it is also important to address its shortcomings. One limitation of the current study was the lack of a full-length nightmare measure and a structured clinical interview to compare with the NDI. However, given the participant burden in the parent study, it was not possible to add measures above and beyond those reported here. That said, this is one of the few studies to compare the frequency and severity of nightmares with 14 daily sleep diaries. An additional limitation was that, in the parent study, the NDI was not given to assess the same time period as the 14-day sleep diary completed by participants. Due to this, it is possible the correlations between the NDI and sleep diary outcomes were slightly attenuated, as nightmares do not necessarily present consistently across weeks. It is possible that our relatively small samples size and limited recruitment sites (i.e. two hospitals) provided limited power to detect differences in some measures such as actigraphy outcomes. However, as shown in Table 1, ours is among the largest validity studies of a nightmare assessment tool to date.
Finally, it is important to point out the limitations of the NDI itself as a brief screening measure. Per the DSM-5, nightmare disorder which occurs solely in the context of PTSD does not necessitate an independent diagnosis; thus, the NDI should be used with caution in populations with high risk of PTSD. Beyond this consideration, the NDI is a brief screening measure and should not be used to assign a definitive diagnosis of nightmare disorder. Rather, it should be used to indicate probable nightmare disorder which could be confirmed by clinical interview. This is made especially salient by the overlap (i.e. small to medium correlations) between the NDI and other measures of psychiatric symptoms, particularly depression It is also important to note that the DSM-5 does not indicate the minimum frequency of nightmares necessary in order to assign a nightmare disorder diagnosis in the criteria (although DSM-5 does specify that severity can be classified as mild [less than one episode per week on average], moderate [one or more episodes per week but less than nightly], or severe [episodes nightly]). In the current study, we used a minimum cutoff of 1×/month in order to maximize detection of potential nightmare disorder with this brief screening measure. If researchers prefer to use a higher minimum frequency (e.g. 1×/week) the measure can be used in that manner, although the validation results presented here may not translate. However, given all of the limitations mentioned above, the NDI does appear to be a more valid and reliable measure of probable nightmare disorder than the previous penchant for using single items from other questionnaires, and we hope future epidemiological and treatment studies will transition to the more precise NDI.
To address these limitations, further investigation is warranted. Primarily, additional validation of the NDI in a variety of populations and contexts would continue to strengthen the evidence for its utility in screening nightmare disorder. A study comparing participant responses on the NDI to a clinical interview would provide important information on the validity of this measure and its ability to reliably identify nightmare disorder. Additionally, given that the NDI has only been preliminarily examined in nurses, it is important that future research explore its utility in a variety of populations (e.g. primary care, military, undergraduate students) and in a variety of settings (e.g. outpatient, online) to determine the generalizability of the assessment.
As previously indicated by Nadorff et al. [11], the experience of nightmares is often underreported and seen by patients as untreatable. Their study indicates approximately 62.2% of adults and 88.9% of undergraduate students with clinically significant nightmares reported they have not discussed these nightmares with a healthcare provider. This severe lack in reporting clinically significant symptoms is further exacerbated by a lack of screening for nightmares by healthcare providers. All these factors taken together leads to an underutilization of evidence-based nightmare treatments. Provided the psychosocial consequences of nightmare disorder, this low rate of detection and treatment is both individually and societally significant. Overall, this study continues to emphasize a need for further assessment and treatment of nightmare disorder, particularly in nurses.
Preliminary results indicate the NDI is an efficient and clinically useful screener for nightmare disorder as defined by the DSM-5. Given this, the NDI provides a brief assessment tool for both researchers and clinicians to screen for clinically significant nightmare disorder in their participants and patients. Hopefully, through increased assessment for nightmare disorder, a parallel increase in the utilization of evidence-based treatment for nightmares [55] (e.g. imagery rehearsal therapy or exposure, relaxation, and rescription therapy) will be observed.
Supplementary Material
Acknowledgments
This research supported by National Institute of Allergy and Infectious Diseases grant 1R01AI128359-01. We would like to thank the nurse PIs, the participants, and the research assistants for their help facilitating this study.
Disclosure Statement
Financial disclosure: This research was supported by National Institute of Allergy and Infectious Diseases (grant 1R01AI128359-01).
Non-financial disclosure: None.
References
- 1. American Academy of Sleep Medicine. International Classification of Sleep Disorders, Third Edition (ICSD-3). 3rd ed. Chicago, IL: American Academy of Sleep Medicine; 2014. [Google Scholar]
- 2. Schredl M. Nightmare frequency and nightmare topics in a representative German sample. Eur Arch Psychiatry Clin Neurosci. 2010;260(8):565–570. [DOI] [PubMed] [Google Scholar]
- 3. Swart ML, et al. . Prevalence of nightmare disorder in psychiatric outpatients. Psychother Psychosom. 2013;82(4):267–268. [DOI] [PubMed] [Google Scholar]
- 4. Krakow B. Nightmare complaints in treatment-seeking patients in clinical sleep medicine settings: diagnostic and treatment implications. Sleep. 2006;29(10):1313–1319. [DOI] [PubMed] [Google Scholar]
- 5. Blagrove M, et al. . The relationship of nightmare frequency and nightmare distress to well-being. J Sleep Res. 2004;13(2):129–136. [DOI] [PubMed] [Google Scholar]
- 6. Levin R, et al. . Nightmare prevalence, nightmare distress, and self-reported psychological disturbance. Sleep. 2002;25(2):205–212. [PubMed] [Google Scholar]
- 7. Nadorff MR, et al. . Insomnia symptoms, nightmares, and suicidal ideation in a college student sample. Sleep. 2011;34(1):93–98. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Sandman N, et al. . Nightmares as predictors of suicide: an extension study including war veterans. Sci Rep. 2017;7:44756. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Pigeon WR, et al. . Meta-analysis of sleep disturbance and suicidal thoughts and behaviors. J Clin Psychiatry. 2012;73(9):e1160–7. [DOI] [PubMed] [Google Scholar]
- 10. Gieselmann A, et al. . Aetiology and treatment of nightmare disorder: state of the art and future perspectives. J Sleep Res. 2019;28(4):e12820. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Nadorff MR, et al. . Nightmares: under-reported, undetected, and therefore untreated. J Clin Sleep Med. 2015;11(7):747–750. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Creamer JL, et al. . Nightmares in United States military personnel with sleep disturbances. J Clin Sleep Med. 2018;14(3):419–426. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders (DSM-5®). Washington, DC: American Psychiatric Association; 2013. [Google Scholar]
- 14. Taylor DJ, et al. ; STRONG STAR Consortium. Reliability of the structured clinical interview for DSM-5 sleep disorders module. J Clin Sleep Med. 2018;14(3):459–464. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Zak RS, et al.. Best practice guide for the treatment of nightmare disorder in adults. J Clin Sleep Med. 2010;6(04):389–401. [PMC free article] [PubMed] [Google Scholar]
- 16. Lancee J, et al. . Cognitive-behavioral self-help treatment for nightmares: a randomized controlled trial. Psychother Psychosom. 2010;79(6):371–377. [DOI] [PubMed] [Google Scholar]
- 17. Blagrove M, et al. . Evaluating the awakening criterion in the definition of nightmares: how certain are people in judging whether a nightmare woke them up? J Sleep Res. 2006;15(2):117–124. [DOI] [PubMed] [Google Scholar]
- 18. Acker KH. Do critical care nurses face burnout, PTSD, or is it something else?: getting help for the helpers. AACN Clin Issues Crit Care Nurs. 1993;4(3):558–565. [PubMed] [Google Scholar]
- 19. Campbell RL, et al. . Nightmares and posttraumatic stress disorder (PTSD). Curr Sleep Med Rep. 2016;2(2):74–80. [Google Scholar]
- 20. Mealer ML, et al. . Increased prevalence of post-traumatic stress disorder symptoms in critical care nurses. Am J Respir Crit Care Med. 2007;175(7):693–697. [DOI] [PubMed] [Google Scholar]
- 21. Mealer M, et al. . The prevalence and impact of post traumatic stress disorder and burnout syndrome in nurses. Depress Anxiety. 2009;26(12):1118–1126. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Czaja AS, et al. . Symptoms of posttraumatic stress disorder among pediatric acute care nurses. J Pediatr Nurs. 2012;27(4):357–365. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Pruiksma KE, et al. . Residual sleep disturbances following PTSD treatment in active duty military personnel. Psychol Trauma. 2016;8(6):697–701. [DOI] [PubMed] [Google Scholar]
- 24. Espie CA, et al. . The Sleep Condition Indicator: a clinical screening tool to evaluate insomnia disorder. BMJ Open. 2014;4(3):e004183. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Buysse DJ, et al. . The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213. [DOI] [PubMed] [Google Scholar]
- 26. Paul F, et al. . Nightmares affect the experience of sleep quality but not sleep architecture: an ambulatory polysomnographic study. Borderline Personal Disord Emot Dysregul. 2015;2:3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Woodward SH, et al. . Laboratory sleep correlates of nightmare complaint in PTSD inpatients. Biol Psychiatry. 2000;48(11):1081–1087. [DOI] [PubMed] [Google Scholar]
- 28. Stout JW, et al. . Sleep disturbances among combat military veterans: a comparative study using subjective and objective sleep assessments. Military Psychol. 2017;29(3):189–201. [Google Scholar]
- 29. Wong ML, et al. . Psychometric properties of the Sleep Condition Indicator and Insomnia Severity Index in the evaluation of insomnia disorder. Sleep Med. 2017;33:76–81. [DOI] [PubMed] [Google Scholar]
- 30. Randler C. Validation of the full and reduced Composite Scale of Morningness. Biol Rhythm Res. 2009;40(5):413–423. [Google Scholar]
- 31. Smith CS, et al. . Evaluation of three circadian rhythm questionnaires with suggestions for an improved measure of morningness. J Appl Psychol. 1989;74(5):728–738. [DOI] [PubMed] [Google Scholar]
- 32. Kroenke K, et al. . The PHQ‐9. J Gen Intern Med. 2001;16(9):606–613. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Manea L, et al. . A diagnostic meta-analysis of the Patient Health Questionnaire-9 (PHQ-9) algorithm scoring method as a screen for depression. Gen Hosp Psychiatry. 2015;37(1):67–75. [DOI] [PubMed] [Google Scholar]
- 34. Spitzer RL, et al. . A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006;166(10):1092–1097. [DOI] [PubMed] [Google Scholar]
- 35. Blevins CA, et al. . The posttraumatic stress disorder checklist for DSM-5 (PCL-5): development and initial psychometric evaluation. J Trauma Stress. 2015;28(6):489–498. [DOI] [PubMed] [Google Scholar]
- 36. Weathers F, et al. . The PTSD checklist for DSM-5 (PCL-5). Scale available from the National Center for PTSD www.ptsd.va.gov. 2013. [Google Scholar]
- 37. Cohen S, et al. . A global measure of perceived stress. J Health Soc Behav. 1983;24(4):385–396. [PubMed] [Google Scholar]
- 38. Bhat R, et al. . Analysis of the perceived stress score (PSS) and blood pressure (BP) during examinations in medical students. J Clin Diagn Res 2012;5(7):1331–1335. [Google Scholar]
- 39. Lee EH. Review of the psychometric evidence of the perceived stress scale. Asian Nurs Res (Korean Soc Nurs Sci). 2012;6(4):121–127. [DOI] [PubMed] [Google Scholar]
- 40. Coursey RD, et al. . A comparison of relaxation techniques with electrosleep therapy for chronic, sleep-onset insomnia a sleep-EEG study. Biofeedback Self Regul. 1980;5(1):57–73. [DOI] [PubMed] [Google Scholar]
- 41. McCall C, et al. . Comparison of actigraphy with polysomnography and sleep logs in depressed insomniacs. J Sleep Res. 2012;21(1):122–127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42. Matthews KA, et al. . Similarities and differences in estimates of sleep duration by polysomnography, actigraphy, diary, and self-reported habitual sleep in a community sample. Sleep Health. 2018;4(1):96–103. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43. Respironics. Actiwatch Instruction Manual: Software Version 5.0. Bend, OR: Respironics, Inc.; 2005. [Google Scholar]
- 44. Ancoli-Israel S, et al. . The SBSM guide to actigraphy monitoring: clinical and research applications. Behav Sleep Med. 2015;13(Suppl 1):S4–S38. [DOI] [PubMed] [Google Scholar]
- 45. Rijsketic J, et al. . Actigraphy (Actiware) Scoring Hierarchy Manual. Available at www.insomnia.arizona.edu/actigraphy
- 46. Sobell LC, et al. . Comparison of a quick drinking screen with the timeline followback for individuals with alcohol problems. J Stud Alcohol. 2003;64(6):858–861. [DOI] [PubMed] [Google Scholar]
- 47. Roy M, et al.. Comparison of the Quick Drinking Screen and the Alcohol Timeline Followback with Outpatient Alcohol Abusers. Substance Use Misuse. 2008;43(14):2116–2123. [DOI] [PubMed] [Google Scholar]
- 48. Soto CJ, et al. . The next Big Five Inventory (BFI-2): developing and assessing a hierarchical model with 15 facets to enhance bandwidth, fidelity, and predictive power. J Pers Soc Psychol. 2017;113(1):117–143. [DOI] [PubMed] [Google Scholar]
- 49. Henson RK, et al. . Use of exploratory factor analysis in published research: common errors and some comment on improved practice. Educ Psychol Meas. 2006;66(3):393–416. [Google Scholar]
- 50. Kaiser HF. The application of electronic computers to factor analysis. Educ Psychol Meas. 1960;20(1):141–151. [Google Scholar]
- 51. Cattell RB. The Scree Test for the number of factors. Multivariate Behav Res. 1966;1(2):245–276. [DOI] [PubMed] [Google Scholar]
- 52. O’Connor BP. SPSS and SAS programs for determining the number of components using parallel analysis and Velicer’s MAP test. Behav Res Methods Instrum Comput. 2000;32(3):396–402. [DOI] [PubMed] [Google Scholar]
- 53. Holm S. A simple sequentially rejective multiple test procedure. Scand J Stat. 1979;6(2):65–70. [Google Scholar]
- 54. Gaetano J. Holm-Bonferroni sequential correction: an EXCEL calculator (1.1) [Microsoft Excel workbook].2013. Available at https://bit.ly/2VQOqcn
- 55. Morgenthaler TI, et al. . Position paper for the treatment of nightmare disorder in adults: an American Academy of Sleep Medicine position paper. J Clin Sleep Med. 2018;14(6):1041–1055. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56. Bjorvatn B, et al. . Parasomnias are more frequent in shift workers than in day workers. Chronobiol Int. 2015;32(10):1352–1358. [DOI] [PubMed] [Google Scholar]
- 57. Goldbart A, et al. . Narcolepsy and predictors of positive MSLTs in the Wisconsin Sleep Cohort. Sleep. 2014;37(6):1043–1051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58. Miller KE, et al. . REM sleep: what is it good for? Curr Biol. 2019;29(16):R806–R807. [DOI] [PubMed] [Google Scholar]
- 59. Marino M, et al. . Measuring sleep: accuracy, sensitivity, and specificity of wrist actigraphy compared to polysomnography. Sleep. 2013;36(11):1747–1755. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.