Abstract
Purpose:
The aim of the study was to examine the association between cognitive impairment and low physical function over a 20-year follow-up period among older Mexican Americans.
Methods:
The final sample included 1,545 community-dwelling Mexican Americans age ≥ 65 years from the Hispanic Established Population for the Epidemiological Study of the Elderly, who scored moderate-high on Short Physical Performance Battery (SPPB) and were non-disabled at baseline (1993/94). Cognitive impairment was defined at each observation wave as ≤21 points on the Mini Mental State Examination. General Estimating Equation was used to estimate the odds ratio of having low physical function (SPPB <7 Page 2 points) over time as a function of cognitive impairment, adjusting for socio-demographics, self-reported medical conditions, body mass index, and depressive symptoms. All variables were time-varying, except sex and education.
Results:
Participants with cognitive impairment had increased odds ratio of low physical function over time compared to those without cognitive impairment (Odds Ratio = 1.89; 95% Confidence Interval = 1.59–2.26, p<.0001), after controlling for all covariates.
Conclusion:
Despite having moderate to high physical function and being non-disabled at baseline, participants with cognitive impairment were more likely to decline in physical function over 20-years of follow-up.
Keywords: Cognition, Physical Functional Performance, Mexican Americans, Aging, Longitudinal Studies
Introduction
Due to the increased life expectancy of adults, the trend in the number of older adults living with cognitive impairment has increased in recent decades. Between 1998 and 2014, approximately two out of three older Americans experienced cognitive impairment with an average age of cognitive impairment onset at 70 years.1,2 From 2015–2017, 11.7% of older Americans self-reported cognitive decline (i.e. memory loss or confusion) over the past 12 months.3 Cognitive impairment and cognitive decline are early signs of dementia in older adults, and the number of Americans with dementia is projected to be 13.8 million by 2050.4
In addition to the high prevalence of cognitive impairment, approximately 15% of older Americans live with at least one physical function limitation, such as difficulty walking or climbing stairs.5 Age increases the risk of developing physical function limitations, and adults aged at least 85 years are three times more likely to have a mobility limitation compared to adults 65 to 75 years.5 Having a limitation in physical function can increase the risk of developing a functional disability (e.g. mobility or independent living) and contribute to high healthcare cost associated with disability.6
Physical function has been identified as a predictor of cognitive function in older adults, but it has been suggested that cognitive impairment precedes the decline in physical function.7 The strength of the association between cognitive and physical function may not remain the same over time, and this dynamic process may partially explain why studies of different durations have dissimilar findings regarding the relationship between cognitive function and physical function. Grande et al. (2019) recently reported older adults free of dementia with cognitive impairment and low physical function may experience a steeper decline towards functional disability compared to older adults without cognitive impairment and high physical function.8
Current studies on cognitive and physical function are not representative of the Hispanic population and are often limited to self-reported function or short follow-up periods. Self-reported physical function assessments may not be appropriate for older adults who are experiencing cognitive decline or do not speak the same language as the interviewer. Also, studying participants with good physical function or free of disability at baseline will help better understand the relationship between cognitive and physical function later in life, but this exclusion is not always possible for studies.
Hispanics may be at greater risk of having low function and disability than other racial and ethnic groups due to longer life-expectancy that is often accompanied with chronic illnesses, suggesting years spent later in life do not equate to higher wellbeing as an older adult.9,10 Cognitive function has been found to predict low physical function among high-functioning older adults from Latin America at baseline only compared to Canadian participants.11 Hispanics of Mexican-origin residing in the United States have been shown to have increased risk of cognitive impairment and physical function decline later in life, which may be attributed to several factors, such as having type 2 diabetes, depression, and high number of chronic conditions.15,16 Compared to non-Hispanic White Americans, socio-economic risk factors, such as low income and low education increase the likelihood of having cognitive impairment or physical function limitations among Mexican Americans.17 Conversely, higher global cognitive function may decrease the risk of having decline in physical function over time among older Mexican Americans.15 Analyzing the relationship between cognitive function and physical function over long follow-up periods using repeated measures and objective measures of physical function will allow the change in both cognitive and physical function over time while accounting for well-known time-varying predictors of physical function decline later in life.
It is also important to consider the heterogeneity of the United States Hispanic population when studying the relationship between cognitive and physical functioning among Hispanic older adults. It has been suggested cognitive function may differ by Hispanic subgroups.12 For example, a study found Hispanics of Cuban- or Mexican- origin with diabetes may have worse certain cognitive domains than those without diabetes, but a significant relationship between diabetes and cognitive function was not found among other Hispanic populations (e.g., Dominican, Central American, Puerto Rican, South American).13 However, a longitudinal study on Latinos living in the United States found that the relationship between poor cognitive function and self-reported functional impairments was consistent across Latino subgroups.14
We seek to address the gaps in the literature described above by examining the effect of cognitive impairment on low physical function over a 20-year follow-up period among older Mexican Americans who had moderate to high physical function and were non-disabled at baseline. We hypothesized that older Mexican Americans with cognitive impairment will be more likely to experience low physical function over time than those without cognitive impairment.
Methodology
Data source and sample
The data used are from the Hispanic Established Population for the Epidemiological Study of the Elderly (H-EPESE), which is an on-going longitudinal study of older, community-dwelling Mexican Americans from five Southwestern states (Texas, California, Arizona, New Mexico, and Colorado).18 As previously described,19–21 a multistate area probability sample was used to select counties in the Southwestern United States that had >30% Hispanics in the population. The original H-EPESE sample consisted of 3,050 participants ≥ 65 years interviewed in-home in either English or Spanish in 1993/94 and followed every 2–3 years. The present study used data from Wave 1 (1993–1994) to Wave 8 (2012–2013), for a total follow-up of approximately 20 years. Information and data for the H-EPESE are available at the National Archive of Computerized Data on Aging.22
For this study, 1,505 participants were excluded at baseline based on the following criteria: reported needing assistance or were unable to perform one of seven activities of daily living (ADLs): walking, bathing, grooming, dressing, eating, transferring, or toileting (n=430), scored less than 7 points on the Short Physical Performance Battery (SPPB) (n=984), and had incomplete data for baseline covariates (n=91). The final analytical sample included 1,545 participants (Fig. S1). Excluded participants had greater mean age, completed fewer years of education, and were more likely to not be married, have lower score in the SPPB, experience depressive symptoms, have cognitive impairment, and to report more chronic conditions than included participants (Table S1). At the end of follow-up (2012/13), 305 participants were re-interviewed, 189 were lost to follow-up/refused to be re-interviewed, and 1,051 were confirmed dead through the National Death Index and report from relatives. The average follow-up time was 9.37 ± 6.54 years.
Physical Function
To assess physical function, the SPPB was performed. The SPPB is often used to objectively assess lower body physical function and physical performance in older adults.23 The SPPB has been deemed a reliable and valid functional assessment for community-dwelling older adults and is suitable for clinical and community practice.23 The SPPB assessment includes three components—a balance, gait, and chair-to-stand test. The balance test included a series of timed tests (i.e., standing side-by-side with feet together, standing semi-tandem with a flat side-by-side heel-to-toe touch, and full-tandem with a flat one foot in front of the other heel-to-toe touch). The gait test measures the amount of time taken to complete a 2.4-meter walk with or without assistive devices. The timed chair-to-stand test requires participants to stand up and sit back down on a chair five times without stopping or using upper extremities. Each task scores were based on a scale of 0–4, with 0 being unable to perform and 4 being the highest achievable score. These scores summed together to create a total SPPB score of 0–12. Higher scores indicated better physical performance. As previously described, an SPPB score 0–7 is considered low physical performance, whereas an SPPB score of 7–10 and ≥10 are considered moderate or high physical performance.24
Cognitive impairment
Cognitive impairment was assessed using the Mini-Mental State Examination (MMSE), which is the most commonly used cognitive screening tool in aging research.25 The MMSE has been previously used in either English or Spanish for Hispanic populations, adapted from Diagnostic Interview Scale, to assess global cognitive function.26 The MMSE score ranges from 0–30 with a higher score indicating better global cognitive function. For this study, MMSE score was dichotomized as cognitive impairment (MMSE<21) versus no cognitive impairment (MMSE ≥21) to better capture participants with lower educational attainment.27
Covariates
Measures previously found to increase the risk of low physical function in older Mexican Americans were included—socio-demographic variables (age, sex, education, and marital status), body mass index (BMI), and self-reported, well-known chronic conditions (i.e. type 2 diabetes, hypertension, stroke, heart attack, cancer, and hip fracture).18 Depressive symptoms were measured using the Center for Epidemiologic Studies Depression Scale (CES-D), where a score ≥16 was considered as experiencing high depressive symptoms.28
Statistical Analysis
Baseline characteristics were described using means ± standard deviations for continuous variables and frequencies for categorical variables. A chi-square test and t-test were used to examine group differences in baseline characteristics by SPPB score. A generalized estimating equation model analysis using the GENMOD procedure in SAS was performed to estimate the odds ratio of having low physical performance (SPPB < 7) over 20-years as a function of cognitive impairment. The models used a logit link binomial distribution and an autoregressive order covariance matrix. All variables including cognitive impairment were analyzed as time varying (with the potential to change as time progressed), except for sex and education. Additional analysis was performed using the general linear mixed models MIXED procedure with an unstructured covariance matrix in SAS to estimate the average population change in SPPB over time as a continuous score as a function of cognitive impairment. These methods were chosen to account for missing or incomplete observations, as well as the modeling of time-dependent change between the variables and the modeling effects of time on the outcome. A p-value of <0.05 was set for statistical significance. SAS System for Windows (version 10; SAS Institute, Cary, NC) was used to perform all analyses.
Results
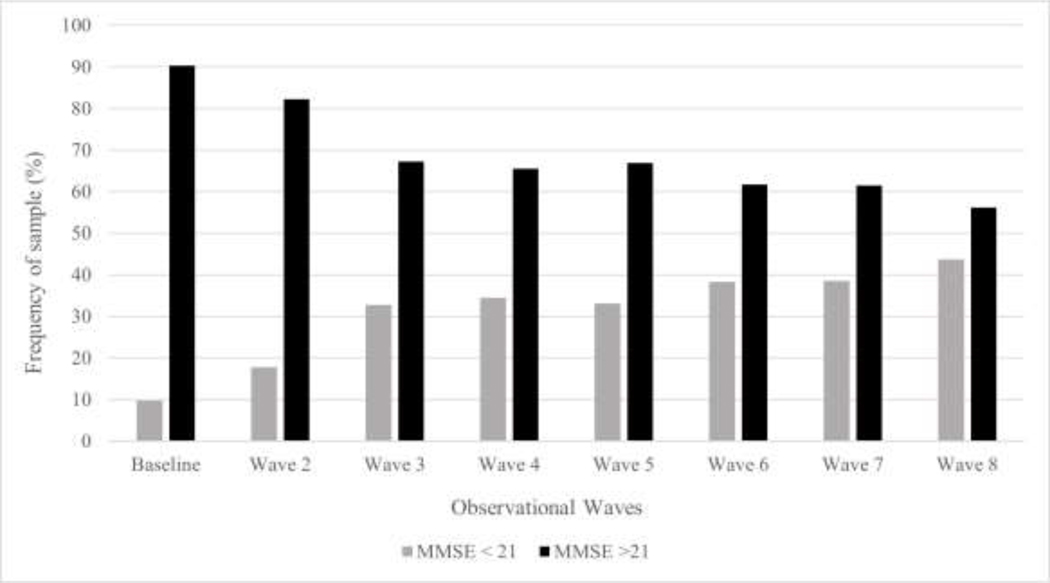
Table 1 presents the overall descriptive characteristics of the baseline sample and by physical function (SPPB 7–10 vs SPPB ≥10). On average, participants were 71.98 ± 5.51 years, overweight (BMI = 27.73 ± 4.96 kg/m2) and had 5.18 ± 4.11 total years of education. Approximately 55% of the participants were female and 61% were married at baseline. The average SPPB score was 9.01 ± 1.42 and 9.71% had cognitive impairment (MMSE <21). The most reported chronic conditions were type 2 diabetes (23.43%), hypertension (39.74%), and depressive symptoms (15.92%). At baseline, participants with moderate physical function (SPPB 7–10) compared to participants with high physical function (SPPB ≥10) were more likely to be female (60.5% vs 44.74%, p<.0001), not married (57.95% vs 65.79%, p=0.002), have higher BMI (27.79 ± 5.17 vs 27.64 ± 4.58, p<.0001), have fewer years of educational attainment (4.88 ± 3.95 vs 5.67 ± 4.33, p<.0001), have type 2 diabetes (25.74% vs 19.47%, p=0.005), and have depressive symptoms (18.97% vs 10.70%, p<.0001). Figure 1 shows the percent of cognitive impairment steadily increased over time ranging from 9.71% at baseline to 43.77% in Wave 8.
Table 1.
Baseline descriptive characteristics of participants at baseline by physical function (N=1545)
| Independent Variables | Overall N (%) | Moderate Physical Function N (%) | High Physical Function N (%) | p-value |
|---|---|---|---|---|
|
| ||||
| Total | 1545 | 975 | 570 | |
| Age (years), mean ± SD | 71.98 ± 5.51 | 72.31 ± 5.78 | 71.42 ± 4.96 | |
| Sex | <.0001 | |||
| Male | 700 (45.31) | 385 (39.49) | 315 (55.26) | |
| Female | 845 (54.69) | 590 (60.51) | 255 (44.74) | |
| Marital status (married) | 940 (60.84) | 565 (57.95) | 375 (65.79) | 0.002 |
| BMI, mean ± SD | 27.73 ± 4.96 | 27.79 ± 5.17 | 27.64 ± 4.58 | <.0001 |
| Education (years), mean ± SD | 5.18 ± 4.11 | 4.88 ± 3.95 | 5.67 ± 4.33 | <.0001 |
| MMSE (<21) | 150 (9.71) | 95 (9.74) | 55 (9.65) | 0.952 |
| SPPB score, mean ± SD | 9.01 ± 1.42 | 8.09 ± 0.80 | 10.58 ± 0.69 | <.0001 |
| Type 2 Diabetes | 362 (23.43) | 251 (25.74) | 111 (19.47) | 0.005 |
| Hypertension | 614 (39.74) | 401 (41.13) | 213 (37.37) | 0.145 |
| Stroke | 47 (3.04) | 34 (3.49) | 13 (2.28) | 0.183 |
| Heart Attack | 119 (7.70) | 75 (7.69) | 44 (7.72) | 0.985 |
| Cancer | 68 (4.40) | 48 (4.92) | 20 (3.51) | 0.191 |
| Hip Fracture | 28 (1.81) | 16 (1.64) | 12 (2.11) | 0.509 |
| Depressive symptoms | 246 (15.92) | 185 (18.97) | 61 (10.70) | <.0001 |
Note. Moderate physical function=SPPB <10; High physical function=SPPB ≥10; SD=standard deviation; BMI=body mass index (kg/m2), MMSE=Mini-Mental State Examination (0–30 range); SPPB=Short Physical Performance Battery (0–12 range); Depressive symptoms measured by Center for Epidemiologic Studies Depression Scale (CES-D >16)
Figure 1.
Percent of cognitive impairment versus no cognitive impairment over observational waves.
Table 2 shows the results of the generalized estimating equation analysis for low physical function (SPPB<7) in participants who were non-disabled and scored moderate to high physical function at baseline. Participants with cognitive impairment had an increased odds ratio (OR) for low physical function (SPPB < 7) over time (OR=1.89, 95% Confidence Interval [CI], 1.59–2.26) compared to participants without cognitive impairment after controlling for all covariates. Older age (OR=1.07, 95% CI: 1.05–1.09), being female (OR=1.54, 95% CI: 1.27–1.87), higher BMI (OR=1.02, 95% CI: 1.01–1.04), having type 2 diabetes (OR=1.37, 95% CI: 1.14–1.65), previous hip fracture (OR=2.51, 95% CI: 1.59–3.97) and higher depressive symptoms (OR=1.67, 95% CI: 1.39–2.00) increased the odds of low physical function over time.
Table 2.
Generalized estimating equation model for low physical function (SPPB < 7) as a function of cognitive impairment over a 20-year period (N=1,545)
| Predictor variables | Odds Ratio Estimate | 95% CI | p-value |
|---|---|---|---|
|
| |||
| Time (years) | 1.13 | (1.11, 1.15) | <.0001 |
| Cognition (MMSE < 21) | 1.89 | (1.59, 2.26) | <.0001 |
| Age (years) | 1.07 | (1.05, 1.09) | <.0001 |
| Sex (female) | 1.54 | (1.27, 1.87) | <.0001 |
| Marital status (married) | 1.05 | (0.88, 1.24) | 0.58 |
| BMI | 1.02 | (1.01, 1.04) | 0.005 |
| Education (years) | 0.97 | (0.95, 0.99) | 0.012 |
| Type 2 Diabetes | 1.37 | (1.14, 1.65) | 0.001 |
| Hypertension | 0.95 | (0.81, 1.24) | 0.575 |
| Stroke | 1.02 | (0.71, 1.46) | 0.908 |
| Heart Attack | 1.28 | (0.93, 1.76) | 0.132 |
| Cancer | 1.06 | (0.79, 1.43) | 0.682 |
| Hip Fracture | 2.51 | (1.59, 3.97) | <.0001 |
| Depressive symptoms | 1.67 | (1.39, 2.00) | <.0001 |
Note. SE=standard error; BMI=body mass index (kg/m2), MMSE = Mini-Mental State Examination (0–30 range); SPPB=Short Physical Performance Battery (0–12 range); Depressive symptoms measured by Center for Epidemiologic Studies Depression Scale (CES-D ≥16)
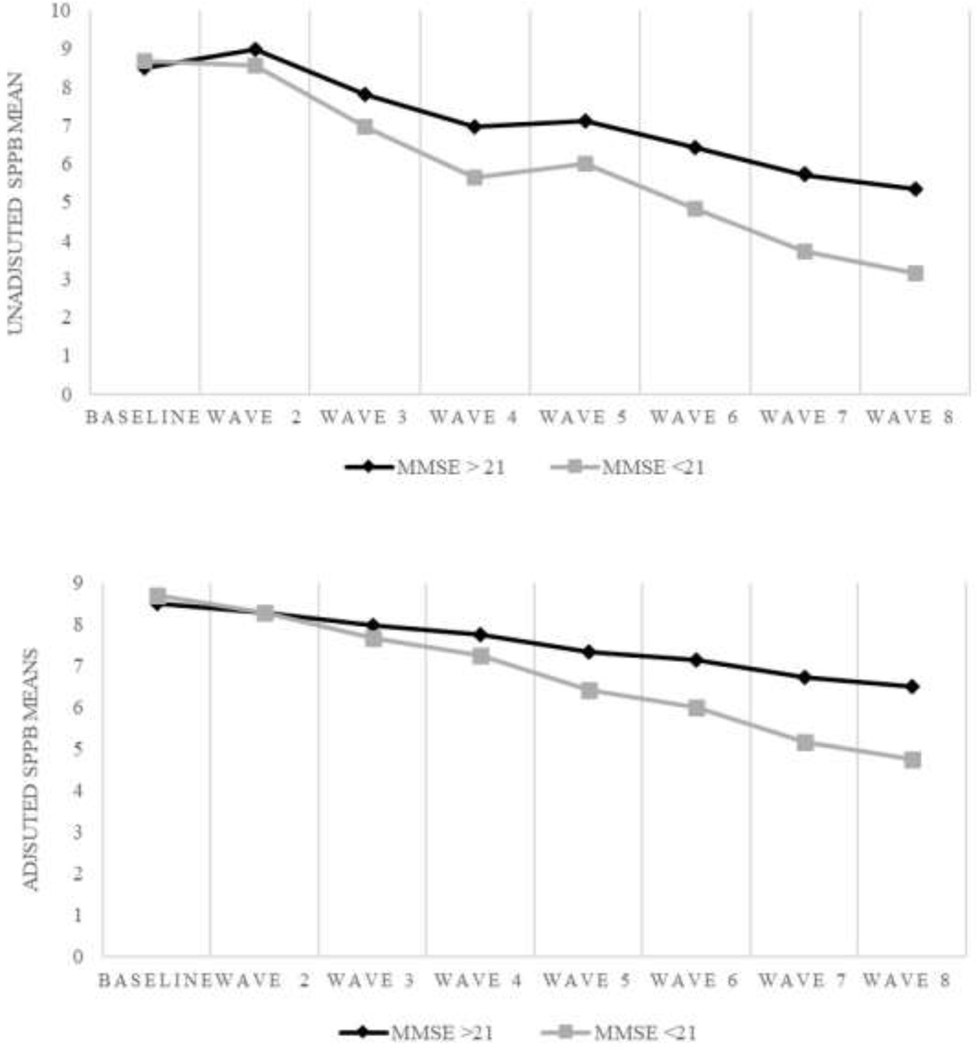
When SPPB was analyzed as a continuous score, we found that those with cognitive impairment on average experienced greater decline in the SPPB (estimate= −0.26, Standard Error = 0.08, p-value = 0.001) than those without cognitive impairment, after controlling for all covariates (Table 3). Figure 2a-b shows the estimated unadjusted and adjusted means for SPPB score as a function of cognition (MMSE < 21 and MMSE ≥ 21) over a 20-year follow-up period.
Table 3.
Mixed models estimate for SPPB score over a 20-year period as a function of cognitive impairment (N=1,545)
| Predictor variables | β(SE) | p-value |
|---|---|---|
|
| ||
| Intercept | 12.93 (0.47) | <.0001 |
| Time (years) | −0.19 (0.01) | <.0001 |
| Cognition (MMSE < 21) | −0.26 (0.08) | 0.001 |
| Age (years) | −0.05 (0.01) | <.0001 |
| Sex (female) | −0.55 (0.07) | <.0001 |
| BMI | −0.00 (0.01) | 0.353 |
| Education (years) | 0.03 (0.01) | <.0001 |
| Marital status (married) | 0.05 (0.07) | 0.448 |
| Type 2 Diabetes | −0.30 (0.07) | <.0001 |
| Hypertension | −0.06 (0.06) | 0.064 |
| Stroke | −0.35 (0.15) | 0.017 |
| Heart Attack | −0.33 (0.11) | 0.003 |
| Cancer | −0.05 (0.13) | 0.683 |
| Hip Fracture | −0.60 (0.20) | <.0001 |
| Depressive symptoms | −0.65 (0.08) | <.0001 |
Note. SPPB=Short Physical Performance Battery (0–12 range); SE=standard error; BMI=body mass index (kg/m2), MMSE=Mini-Mental State Examination (0–30 range); Depressive symptoms measured by Center for Epidemiologic Studies Depression Scale (CES-D≥16)
Figure 2.
a) Unadjusted mean for Short Physical Performance Battery (SPPB) score as a function of cognition (MMSE<21 and MMSE ≥ 21) over a 20-year follow-up period. B) Adjusted means for SPPB score and adjusted means for all covariates as a function of cognitive impairment over a 20-year follow-up period. MMSE: Mini-Mental State Examination.
Discussion
This longitudinal study demonstrates that older Mexican Americans with cognitive impairment—who performed moderate to high on the SPPB and were free of ADL disability at baseline—were 1.89 times more likely to present decline in physical function over 20 years of follow-up.
On average, there was a greater decline in the SPPB of 0.26 points among those with cognitive impairment compared to those without cognitive impairment, after controlling for all covariates. Although the SPPB is widely used in clinical and community settings due to its feasibility and simple calculations, guidelines with normative values have not been established. However, a change in SPPB of 0.3–0.8 points may have slight clinical meaningfulness, whereas a change in SPPB of 0.4–1.5 points may be considered a substantial change.29 The change in SPPB found in the current study may be more meaningful in everyday activities and can be easily translated at an individual level.29 Interestingly, at baseline, participants with cognitive impairment scored higher on the SPPB than participants without cognitive impairment, but participants with cognitive impairment had a steeper decline in the SPPB score and performed worse throughout the 20-year follow-up compared to participants without cognitive impairment (Figure 2). A potential explanation for this finding is that the longitudinal analyses allow for change in all variables rather than cognitive status alone, such as physical function. Previous research has shown that a joint effect of cognitive and physical function decline may accelerate the rate of functional decline among older Mexican Americans, and factors such as older age or having type 2 diabetes might interact with this joint effect and accelerate further functional decline.30
Theoretically, the strong relationship between cognitive impairment and low physical function may be related to the biology of aging. For example, the prefrontal cortex is associated with executive function, and assessments related to executive function predict physical function more than verbal and memory assessments.31 Also, brain magnetic resonance imaging have identified an association between microvascular abnormalities and gait performance in participants free of dementia.32 Furthermore, greater gait variability were associated with increased prevalence of brain abnormalities.32 Although the present study assessed global cognitive function and physical function among older Mexican Americans, previous research can further support the strong relationship between cognitive and physical function domains. In a 5–12-year observational study using the Longitudinal Aging Study Amsterdam and the Leiden 85-plus Study, a temporal relationship across all cognitive and physical function domains were reported in participants aged 85 to 90 years compared to participants 55 to 84 years of age.33 Specifically, executive function predicted a decline in gait speed for all ages groups (55 to 90 years), gait speed and grip strength predicted a 1-point and 2-point steeper decline in the global cognitive function (i.e. MMSE) in adults aged 65 to74 years and 75 to 85 years.33 For participants 85 to 90 years of age, global cognitive function predicted a steeper decline in gait speed of 0.01 meters/second and decline in hand grip strength of 0.2 kilogram.33 Further, Handing and colleagues (2021) recently used an integrative data analysis from the Wake Forest Older American Independence Center and found an association between cognitive and physical function was moderated by race.34 Global cognitive function (Montreal Cognitive Assessment) and 4-m gait speed were harmonized from raw data sets then the association between cognitive and physical function was estimated while accounting for demographic characteristics.34 The pattern of association between the cognitive and physical function differed across age categories for African Americans compared to White participants.34 Several studies on the relationship between cognitive and physical function has been predominately studied among non-Hispanic populations. The findings from the present study and related literature underscores the need to use repeated measures over long follow-up periods to gain a better understanding of the driving forces beneath the impact and change of cognitive and physical function in older Mexican Americans.
Similar to previous studies, older age, being female, having type 2 diabetes, previous hip fracture, higher depressive symptoms, and higher BMI also increased odds of declining in physical function over time. Higher depressive symptoms increased the odds of declining in physical function 1.67 times than those with lower depressive symptoms.35 This is aligned with previous research that show having depressive symptoms are highly predictive of low physical function over time among older Mexican Americans.35,36 Raji et al. (2002) examined the moderation effect of cognitive function and depressive symptoms on physical function over a 2-year follow-up.35 After controlling for all covariates, participants with low cognitive function and higher depressive symptoms were more likely to decline in physical function compared to participants with high cognitive function and higher depressive symptoms.35 Not presented here, our study did not find a significant interaction effect between cognitive function and having depressive symptoms at baseline predicting physical function over 20 years. This discordance may be attributed to the different study durations and statistical procedures (i.e., repeated measures allowing for change). Depressive symptoms should be monitored during regular screening regardless of cognitive status to prevent adverse outcomes due to change in depression over time.36–38 Also, having had a hip fracture exceeded the likelihood of declining in physical function 2.51 times than participants without previous hip fracture over time, which may have contributed to overall decline in physical health given the increased risk of hip fracture and hip fracture reoccurrence among older Mexican Americans.39 In our baseline sample, approximately 23% of participants self-reported having type 2 diabetes and the sample on average had a high BMI. Our results show having type 2 diabetes and high BMI predicted the decline in physical function over time, which are known predictors of disability.40 Elfassy et al. (2019) found that Hispanics of Mexican-origin with type 2 diabetes had worse processing speeds and those with prediabetes or diabetes had worse delayed recall compared to those with normal glucose levels.13 This raises the concern that participants who have worse health and chronic conditions may be at greater risk of transitioning to disability state after experiencing physical function decline, which warrants more research. Despite controlling for strong, well-known predictors of decline in physical function over a 20-year follow-up period, cognitive impairment predicted decline in physical function among non-disabled older Mexican Americans.
The present study has some limitations. First, the health conditions were self-reported, which may not provide precise information about the relationship between health conditions and physical function. Self-reported limitations with ADLs were used to exclude participants with functional disability, but a participants’ perceived limitation in physical capabilities might not be in agreement with actual requirements for physical assistance;41 however, participants in this study were excluded based on their objective measures in physical function (SPPB<7) at baseline. Second, the generalizability of this study is limited to older Mexican Americans from Southwestern states and may not be representative of Mexican Americans in other regions or other Hispanic subpopulations in the United States. Third, participants excluded from the study were less healthy compared to those included, which might have resulted in underestimating the relationship between cognitive impairment and change in physical function. Fourth, the MMSE may underestimate cognitive impairment and should not be used to diagnose dementia; however, scores have been adjusted to capture those with low educational attainment. Fifth, there is potential reverse causality bias. For example, Okely and Deary (2020) found declines in cognitive function (i.e. visuospatial function and processing speed) predicted physical function decline (i.e. walking speed and grip strength), and the decline in physical function predicted declines in verbal memory among older adults over 9-years.42 However, participants were excluded if they required any assistance with ADLs or had an SPPB score <7 at baseline.
Despite these limitations, this study has some strengths. First, the H-EPESE is a large, longitudinal cohort study of community-dwelling older Mexican Americans, an underserved population that are aging rapidly. Second, this study used objective measures of physical function as opposed to self-reported perception of physical function, which is more appropriate for groups with lower cognitive function.41 Third, the present study used a follow-up period of 20 years, which is longer than that of previous research.
This study found that older Mexican Americans with cognitive impairment are at greater risk of experiencing low physical function compared to participants without cognitive impairment over a 20-year follow-up period, despite being non-disabled and having moderate to high SPPB at baseline and controlling for well-known predictors of physical function decline. Future studies should identify predictors of cognitive impairment among moderate to high functioning older Mexican Americans to prevent cognitive impairment and attenuate the risk of physical function decline and subsequent disabilities.
Supplementary Material
Acknowledgments
AG was involved in the study design, interpretation of results, and writing of the manuscript. ;BD was involved in revising of the manuscript. ; LC was involved in the interpretation of results.; SAS was involved in the study design, interpretation of results, and revising the manuscript.
Funding
This work was supported in part by the National Institute on Aging, the National Institute on Minority Health and Health Disparities, and Texas Resource Center on Minority Aging Research (R01 AG10939, R01 AG017638, RF1AG068988, 1P30 AG059301-01, R01 MD010355, and K01 AG058789). Mrs. Givan is supported by the training grant #T32HS02613303 from the Agency for Healthcare Research and Quality.
List of Abbreviations and Acronyms
- ADL
Activities of daily living
- BMI
Body mass index
- CES-D
Center for Epidemiologic Studies Depression Scale
- CI
Confidence interval
- H-EPESE
Hispanic Established Population for the Epidemiological Study of the Elderly
- MMSE
Mini-Mental State Examination
- OR
Odds ratio
- SD
Standard deviation
- SE
Standard error
- SPPB
Short Physical Performance Battery
Footnotes
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Supplemental Information
Table S1. Descriptive characteristics of excluded and included participants at baseline
Fig. S1. Flow chart of exclusion criteria for baseline sample.
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
References
- 1.Hale JM, Schneider DC, Mehta NK, Myrskylä M. Cognitive impairment in the U.S.: Lifetime risk, age at onset, and years impaired. SSM - Popul Heal. 2020;11. doi: 10.1016/j.ssmph.2020.100577 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Hale JM, Schneider DC, Gampe J, Mehta NK, Myrskylä M. Trends in the risk of cognitive impairment in the United States, 1996–2014. Epidemiology. 2020;31(5):745–754. doi: 10.1097/EDE.0000000000001219 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Centers of Disease Control and Prevention. Subjective Cognitive Decline — A Public Health Issue. U.S. Department of Health and Human Services. Published 2018. https://www.cdc.gov/aging/data/subjective-cognitive-decline-brief.html [Google Scholar]
- 4.Herbert LE, Weuve J, Scherr PA, Evans DA. Alzheimer disease in the United States (2010–2050) estimated using the 2010 census. Am Acad Neurol. 2013;80(19):17781783. doi: 10.1002/jcu.1870130614 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Roberts AW, Ogunwole SU, Blakeslee L, Rabe MA. The population 65 years and older in the United States: 2016. Am Community Surv Reports. Published online 2018:ACS-38. files/2125/Roberts et al. - 2018 - The population 65 years and older in the United St.pdf
- 6.Centers of Disease Control and Prevention. Disability and Health Healthcare Cost Data. Published 2020. Accessed January 22, 2021. https://www.cdc.gov/ncbddd/disabilityandhealth/data-highlights.html
- 7.Tolea MI, Morris JC, Galvin JE. Longitudinal associations between physical and cognitive performance among community-dwelling older adults. PLoS One. 2015;10(4):1–12. doi: 10.1371/journal.pone.0122878 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Grande G, Vetrano DL, Fratiglioni L, et al. Disability trajectories and mortality in older adults with different cognitive and physical profiles. Aging Clin Exp Res. 2020;32(6):1007–1016. doi: 10.1007/s40520-019-01297-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Melvin J, Hummer R, Elo I, Mehta N. Age patterns of racial/ethnic/nativity differences in disability and physical functioning in the United States. Demogr Res. 2014;31:497–510. doi: 10.4054/DemRes.2014.31.17.Age [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Angel RJ, Angel JL, Hill TD. Longer lives, sicker lives? Increased longevity and extended disability among Mexican-origin elders. Journals Gerontol - Ser B Psychol Sci Soc Sci. 2015;70(4):639–649. doi: 10.1093/geronb/gbu158 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Dansereau A, Hunter SW, Gomez F, Guralnik JM, DePaul VG, Auais M. Global cognition predicts the incidence of poor physical performance among older adults: A cross-national study. Published online 2020. doi: 10.1111/ggi.13864 [DOI] [PubMed]
- 12.González HM, Tarraf W, Gouskova N, et al. Neurocognitive function among middle-aged and older hispanic/latinos: Results from the hispanic community health study/study of latinos. Arch Clin Neuropsychol. 2015;30(1):68–77. doi: 10.1093/arclin/acu066 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Elfassy T, Aiello AE, Schneiderman N, et al. Relation of Diabetes to Cognitive Function in Hispanics/Latinos of Diverse Backgrounds in the United States. J Aging Health. 2019;31(7):1155–1171. doi: 10.1177/0898264318759379 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Stickel AM, Tarraf W, Wu B, et al. Cognition and daily functioning: results from the Hispanic Community Health Study/Study of Latinos (SOL) and Study of Latinos - Investigation of Neurocognitive Aging (SOL-INCA). J Alzheimers Dis. 2020;77(3):1267–1278. doi: 10.3233/JAD-200502. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Mutambudzi M, Chen NW, Howrey B, Garcia MA, Markides KS. Physical Performance Trajectories and Mortality among Older Mexican Americans. Journals Gerontol - Ser A Biol Sci Med Sci. 2019;74(2):233–239. doi: 10.1093/gerona/gly013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.KS M, K. G. Immigration, Aging, and Health in the United States. (Settersten R, Angel J, eds.). Springer; 2011. doi: 10.1007/978-1-4419-7374-0_7 [DOI] [Google Scholar]
- 17.Louie GH, Ward MM. Socioeconomic and ethnic differences in disease burden and disparities in physical function in older adults. Am J Public Health. 2011;101(7):1322–1329. doi: 10.2105/AJPH.2010.199455 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Markides KS, Stroup-Benham CA, Goodwin JS, Perkowski LC, Lichtenstein M, Ray LA. The effect of medical conditions on the functional limitations of MexicanAmerican elderly. Ann Epidemiol. 1996;6(5):386–391. doi: 10.1016/S10472797(96)00061-0 [DOI] [PubMed] [Google Scholar]
- 19.Markides K Hispanic established populations for the epidemiologic studies of the elderly, 1993–1994: (Arizona, California, Colorado, New Mexico, and Texas). In: Inter-University Consortium for Political and Social Research. ; 2009. doi: 10.3886/ICPSR02851.v2. [DOI] [Google Scholar]
- 20.Markides K, Ray L, R A. Hispanic Established Populations for the Epidemiologic Study of the Elderly (HEPESE) Wave 5, 2004–2005 (Arizona, California, Colorado, New Mexico, and Texas). In: Interuniversity Consortium for Political and Social Research. ; 2009. doi: 10.3886/ICPSR25041.v1. [DOI] [Google Scholar]
- 21.Eschbach K, Ostir GV., Patel KV, Markides KS, Goodwin JS Neighborhood context and mortality among older Mexican Americans: Is there a barrio advantage? Am J Public Health. 2004;94(10):1807–1812. doi: 10.2105/AJPH.94.10.1807 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Markides KS, N-W C, Angel R, Palmer R Hispanic Established Populations for the Epidemiologic Study of the Elderly (HEPESE) Wave 8, 2012–2013 [Arizona, California, Colorado, New Mexico, and Texas].; 2016. doi: 10.3886/ICPSR36537.v2 [DOI]
- 23.Freiberger E, De vreede P, Schoene D, et al. Performance-based physical function in older community-dwelling persons: A systematic review of instruments. Age Ageing. 2012;41(6):712–721. doi: 10.1093/ageing/afs099 [DOI] [PubMed] [Google Scholar]
- 24.Pavasini R, Guralnik J, Brown JC, et al. Short Physical Performance Battery and allcause mortality: Systematic review and meta-analysis. BMC Med. 2016;14(1):1–9. doi: 10.1186/s12916-016-0763-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Folstein Marshal F., Folstein Susan E., and McHugh PR Mini-Mental State: A practical method for grading the cognitive state of patients for the clinician. Published online 1975:189–198. [DOI] [PubMed]
- 26.Bird HR, Canino G, Stipec MR, Shrout P. Use of the mini-mental state examination in a probability sample of a hispanic population. J Nerv Ment Dis. 1987;175(12):731–737. doi: 10.1097/00005053-198712000-00005 [DOI] [PubMed] [Google Scholar]
- 27.Crum RM, Anthony JC, Bassett SS, Folstein MF. Population-Based Norms for the Mini-Mental State Examination by Age and Educational Level. JAMA J Am Med Assoc. 1993;269(18):2386–2391. doi: 10.1001/jama.1993.03500180078038 [DOI] [PubMed] [Google Scholar]
- 28.Radloff LS. The CES-D Scale: a self reported depression scale for research in the general population. Appl Psychol Meas. 1977;1(3):385–401. doi: 10.1177/014662167700100306 [DOI] [Google Scholar]
- 29.Guralnik J, Bandeen-Roche K, Bhasin SAR, et al. Clinically Meaningful Change for Physical Performance: Perspectives of the ICFSR Task Force. J frailty aging. 2020;9(1):9–13. doi: 10.14283/jfa.2019.33 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Gonzales MM, Wang CP, Quiben M, et al. Joint trajectories of cognition and gait speed in Mexican American and European American older adults: The San Antonio longitudinal study of aging. Int J Geriatr Psychiatry. 2020;35(8):897–906. doi: 10.1002/gps.5310 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Holtzer R, Wang C, Verghese J. The relationship between attention and gait in aging: Facts and fallacies. Motor Control. 2012;16(1):64–80. doi: 10.1123/mcj.16.1.64 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Rosano C, Brach J, Studenski S, Longstreth WT, Newman AB. Gait variability is associated with subclinical brain vascular abnormalities in high-functioning older adults. Neuroepidemiology. 2008;29(3–4):193–200. doi: 10.1159/000111582 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Stijntjes M, Aartsen MJ, Taekema DG, et al. Temporal relationship between cognitive and physical performance in middle-aged to oldest old people. Journals Gerontol - Ser A Biol Sci Med Sci. 2017;72(5):662–668. doi: 10.1093/gerona/glw133 [DOI] [PubMed] [Google Scholar]
- 34.Handing EP, Rapp SR, Chen S-H, et al. Heterogeneity in Association Between Cognitive Function and Gait Speed Among Older Adults: An Integrative Data Analysis Study. Journals Gerontol Ser A. 2020;76(4):710–715. doi: 10.1093/gerona/glaa211 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Raji MA, Ostir GV., Markides KS, Goodwin JS The interaction of cognitive and emotional status on subsequent physical functioning in older Mexican Americans: Findings from the hispanic established population for the epidemiologic study of the elderly. Journals Gerontol - Ser A Biol Sci Med Sci. 2002;57(10):678–682. doi: 10.1093/gerona/57.10.M678 [DOI] [PubMed] [Google Scholar]
- 36.Patino J, Rodriguez MA, Al Snih S. Depressive symptoms predict low physical performance among older Mexican Americans. Aging Clin Exp Res. 2021;33(9):2549–2555. doi: 10.1007/s40520-020-01781-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Schousboe JT, Vo TN, Kats AM, et al. Depressive Symptoms and Total Healthcare Costs: Roles of Functional Limitations and Multimorbidity. J Am Geriatr Soc. 2019;67(8):1596–1603. doi: 10.1111/jgs.15881 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Monserud M, Markides KS. Changes in depressive symptoms during widowhood among older Mexican Americans: The role of financial strain, social support, and church attendance. Aging Ment Heal. 2017;21(6):586–594. doi: 10.1080/13607863.2015.1132676 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Ojo F, Al Snih S, Ray LA, Raji MA, Markides KS. History of fractures as predictor of subsequent hip and nonhip fractures among older Mexican Americans. J Natl Med Assoc. 2007;99(4):412–418. [PMC free article] [PubMed] [Google Scholar]
- 40.Al Snih S, Fisher MN, Raji MA, Markides KS, Ostir GV., Goodwin JS. Diabetes mellitus and incidence of lower body disability among older Mexican Americans. Journals Gerontol - Ser A Biol Sci Med Sci. 2005;60(9):1152–1156. doi: 10.1093/gerona/60.9.1152 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Cress ME, Schechtman KB, Mulrow CD, Fiatarone MA, Gerety MB, Buchner DM. Relationship Between Physical Performance and Self- Perceived Physical Function. J Am Geriatr Soc. 1995;43(2):93–101. doi: 10.1111/j.1532-5415.1995.tb06372.x [DOI] [PubMed] [Google Scholar]
- 42.Okely JA, Deary IJ. Associations between declining physical and cognitive functions in the Lothian Birth Cohort 1936. Journals Gerontol - Ser A Biol Sci Med Sci. 2020;75(7):1393–1402. doi: 10.1093/gerona/glaa023 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.