Abstract
People with epilepsy (PwE) are at a greater risk of comorbid anxiety, which is often related to the fear of having another seizure for safety or social reasons. While virtual reality (VR) exposure therapy (ET) has been successfully used to treat several anxiety disorders, no studies to date have investigated its use in this population. This paper discusses Phase 1 of the three-phase AnxEpiVR pilot study. In Phase 1, we aimed to explore and validate scenarios that provoke epilepsy/seizure-specific (ES) interictal anxiety and provide recommendations that lay the foundation for designing VR-ET scenarios to treat this condition in PwE.
An anonymous online questionnaire (including open- and closed-ended questions) that targeted PwE and those affected by it (e.g., through a family member, friend, or as a healthcare professional) was promoted by a major epilepsy foundation in Toronto, Canada. Responses from n = 18 participants were analyzed using grounded theory and the constant comparison method. Participants described anxiety-provoking scenes, which were categorized under the following themes: location, social setting, situational, activity, physiological, and previous seizure. While scenes tied to previous seizures were typically highly personalized and idiosyncratic, public settings and social situations were commonly reported fears. Factors consistently found to increase ES-interictal anxiety included the potential for danger (physical injury or inability to get help), social factors (increased number of unfamiliar people, social pressures), and specific triggers (stress, sensory, physiological, and medication-related).
We make recommendations for incorporating different combinations of anxiety-related factors to achieve a customizable selection of graded exposure scenarios suitable for VR-ET. Subsequent phases of this study will include creating a set of VR-ET hierarchies (Phase 2) and rigorously evaluating their feasibility and effectiveness (Phase 3).
Keywords: Epilepsy, Anxiety, Virtual reality, Exposure therapy, Cognitive behavioural therapy (CBT), Non-pharmacological intervention
Introduction
Background
The consequences of living with epilepsy often extend beyond the seizures themselves. For example, many PwE experience seizure-related injuries, stigma, cognitive deficits, and troublesome side effects from anti-seizure medications [1]. Psychiatric comorbidities, such as depression and anxiety, affect 33 % of PwE and are linked with decreased quality of life [2]. Peri-ictal (pre-ictal, ictal, and postictal) anxiety has a temporal relationship to the seizures themselves. Conversely, interictal anxiety has no temporal relationship and is associated with exaggerated fears of the social and physical consequences of having a seizure, often resulting in avoidance behaviours that impact quality of life [3].
Hingray et al. (2019) suggested that epilepsy/seizure-specific (ES) interictal anxiety should be characterized as a set of distinct disorders, specifically: 1) anticipatory anxiety of epileptic seizures, 2) seizure phobia, 3) epileptic social phobia, and 4) epileptic panic disorder (Table 1) [4]). ES-interictal anxiety has drastic consequences for the sufferer and requires special attention that is distinct from peri-ictal anxiety or other classical disorders seen in PwE [4]. Nevertheless, very limited research is currently available on the content of specific epilepsy/seizure-related worries and on effective methods to treat these fears [5]. Namely, the details of anxiety-provoking situational factors that would be necessary to design a targeted exposure therapy program to treat ES-interictal fear remain poorly described.
Table 1.
Major Categories of Anxieties and Classic Disorders in PwE.1
| SPECIFIC TO EPILEPSY | CLASSIC DSM-52 DIAGNOSES | |
|---|---|---|
| PERI-ICTAL | INTERICTAL | |
| Pre-Ictal Ictal Post-Ictal |
Anticipatory anxiety of seizures (AAS) Seizure phobia Epileptic social phobia Epileptic panic disorder |
Generalized anxiety disorder Panic disorder Agoraphobia Social phobia |
Adapted from [6].
DSM-5:Diagnostic and Statistical Manual of Mental Disorders, fifth Edition.
Exposure therapy (ET) is a widely used and evidence-based anxiety treatment that involves exposing people to their fears [7]. Its utility in treating ES-interictal anxiety has been investigated in a limited number of studies with promising results demonstrating safety and efficacy [7], [8]. Exposures are typically administered in a hierarchical manner where the individual is repeatedly exposed to situations that first provoke the least amount of anxiety, moving gradually to situations that provoke the greatest amount of anxiety. The goals of ET are for individuals to habituate to the anxiety and/or learn that they can handle anxious feelings without needing to implement unnecessary safety-seeking behaviours [9].
Virtual reality (VR) has successfully been used for delivering ET (VR-ET) to treat several anxiety disorders [10], [11], [12], [13] as well as other neurological conditions [14] with generally comparable [15], [16] or in some cases superior [17] effectiveness to in vivo therapy exposure. Arguably, as VR is a useful tool for delivering ET and allows the therapist to customize exposures to the individual’s needs [18], it has potential to treat the unique fears experienced by PwE. Considering that many PwE have suspended driver’s licenses, VR-ET may hold particular benefit for this population by reducing the need to travel to in-person treatment [15]. The ability to perform ET remotely similarly increases accessibility for those who do not live in urban centers and those who have been advised to limit in-person interactions, such as for immunocompromised individuals during a pandemic.
The AnxEpiVR study
This paper reports on the results of Phase 1 of the three-phase “AnxEpiVR” pilot study; to our knowledge this study will be the first to use VR to deliver ET to PwE. The study is aimed at assessing the feasibility and efficacy of a pilot VR-ET intervention targeted at decreasing ES-interictal anxiety in PwE (see [19] for the full protocol). Phase 1 involved engaging individuals affected by epilepsy, either directly or through someone they know, to learn more about the scenarios and triggers that cause anxiety related to epilepsy/seizures.
Phase 2 of the study will involve filming 360° videos of exposure scenes (with varying intensity levels) that were most commonly reported by participants as producing ES-interictal anxiety in Phase 1.
Phase 3 will involve exposing PwE with ES-interictal anxiety to these 360° films using a VR head-mounted display in order to evaluate the feasibility of the intervention and refine the study protocol for a subsequent larger clinical trial (ClinicalTrials.gov ID: NCT05296057).
Objectives
This paper details the results from Phase 1 of the AnxEpiVR pilot study, which aimed to gather information on ES-interictal anxiety for the purpose of designing the VR-ET scenarios. Specifically, we sought to:
-
1.
Identify scenarios (situations, locations, or environments) that are most strongly associated with ES-interictal anxiety.
-
2.
Describe factors within these scenarios that contribute to increasing ES-interictal anxiety.
-
3.
Validate existing assumptions regarding ES-interictal anxiety as they relate to designing exposure scenarios and graded levels of exposure hierarchies that can be readily created and would suit a variety of individuals.
Methods
Data was collected through an anonymous online questionnaire delivered through a secure York University Qualtrics account (see Appendix B). Both PwE and people affected by PwE (through someone they know) were invited to participate. This study received Research Ethics Board approval by the York University Human Participants Review Committee (certificate number: 2022–105) on May 31, 2022.
Questionnaire design
The questionnaire included open- and closed-ended questions which were informed by the diagnostic protocol described by Hingray et al., (2019) [4] and other reports of ES-interictal anxiety (e.g., [7]). Questions were intentionally created to collect information useful for informing the design of VR-ET scenarios for PwE (i.e., anxiety-provoking locations and elements that might be readily filmed). Demographic questions were kept minimal to maintain participant privacy. Participants were directed to alternate versions of the questionnaire depending on whether they identified as a PwE or as someone affected by PwE.
Open-Ended questions
Participants were asked to list up to five scenes that would cause them anxiety related to their epilepsy/seizures and rate their avoidance behaviour for each scene using a four-point Likert-scale. Subsequently, participants were invited to describe what they see/hear/feel in that situation, factors about that scene that could increase or decrease their anxiety, and what specifically about the scene made them feel anxious.
Closed-Ended questions
We sought to confirm how the following elements might affect the level of anxiety experienced by PwE:
-
1)
Level of familiarity with the people in the scene
-
2)
Number of people in the scene
-
3)
Potential for danger
-
4)
Scenes with combinations of these factors
Participants were provided with a matrix of 14 scenes based on the above elements and asked to rate their agreement with respect to the scenes provoking ES-interictal anxiety (Appendix B).
Participants
Recruitment & consent
We aimed to target a sample of n = 15 individuals meeting the following inclusion criteria:
-
1)
Identify as having epilepsy or being affected by PwE (e.g., through a family member, friend, as a personal caregiver, as a health professional, etc.)
-
2)
Be 18 years of age or over
-
3)
Be willing to share details of ES-interictal anxiety for the PwE
Participants were recruited through Epilepsy Toronto, a non-profit community-centered organization, that promoted the questionnaire in their monthly newsletter and social media accounts (see Appendix A). Digital informed consent was obtained before proceeding with the survey. A snowball strategy was used wherein participants were prompted upon completion to share the questionnaire link with others in their network who may be interested in participating. Participants who took part in the questionnaire were eligible to receive a $5.00 e-gift card.
Response validation process
The Phase 1 questionnaire was open online for seven weeks (from June 19th to August 7th, 2022) and a total of 55 responses were collected over this period. All responses underwent a rigorous validation process to determine whether they would be included in the study, resulting in a final sample of n = 18 (see Fig. 1 and Appendix D). Accordingly, for this study, “participants” or “respondents” will refer to the 18 individuals whose responses were accepted and analyzed.
Fig. 1.
Phase 1 Survey Response Collection.
Analysis
Responses to open- and closed-ended questions were analyzed separately. Grounded theory [20] and the constant comparison method [21] were used to analyze the open-ended responses. Quantitative data from closed-ended questions were analyzed using descriptive statistics and then compared with emerging themes from the qualitative analysis to corroborate the findings.
Open-Ended questions
All open-ended responses (n = 18 participants) underwent thematic analysis. Two authors (DT and SL) manually coded the data using Excel spreadsheets, Word documents, and paper-and-pen methods. The coding process was performed separately by the two authors over multiple iterations, with the authors meeting to discuss connections between the codes and agree on emerging themes at each stage. Ambiguities and discrepancies were discussed by the two raters and compared to supporting context within the dataset (i.e., avoidance ratings, seizure type, and descriptions of thoughts, feelings, perceptions, PwE vs person affected by PwE) until agreement was reached.
The feared scenes listed by participants were first categorized using open coding, and then analyzed again with a revised scheme based on the remaining open-ended descriptions. An axial and selective coding process was then used to derive meaning with respect to developing VR exposure scenario hierarchies.
Closed-Ended questions
Responses from n = 16 participants (n = 12 PwE; n = 4 people affected by PwE) were analyzed using descriptive statistics (2/18 were excluded as they contained no closed-ended responses). A weighted point system was created to rank the 14 matrix scenes from most to least feared (Table 4). Responses from PwE and from people affected by PwE were analyzed separately using different weighting systems to allow for comparison between the two groups.
Table 4.
Validation Scenes Ranked by Points.
| RANKING BY PWE (n = 12) | PTS1 | %2 | RANKING BY INDIVIDUALS AFFECTED BY PWE (n = 4) | PTS3 | %4 |
|---|---|---|---|---|---|
| 7. Completely alone | 18 | 83.3 % | 1. On a subway platform | 4 | 100 % |
| 12. Surrounded by complete strangers in a public setting | 17 | 91.7 % | 2. On a subway train | 4 | 100 % |
| 6. At a shopping centre | 15 | 91.7 % | 10. At a large social gathering or party where I only know a few people | 4 | 100 % |
| 10. At a large social gathering or party where I only know a few people | 15 | 83.3 % | 11. At a large social gathering or party where I know some/all people | 4 | 100 % |
| 8. With a few people that I know (but not well) | 14 | 91.7 % | 12. Surrounded by complete strangers in a public setting | 4 | 100 % |
| 14. Exercising with gym equipment | 13 | 91.7 % | 4. On stairs or elevated platforms | 3 | 75 % |
| 3. On a bus | 12 | 66.7 % | 6. At a shopping centre | 3 | 75 % |
| 4. On stairs or elevated platforms | 11 | 75.0 % | 8. With a few people that I know (but not well) | 3 | 75 % |
| 13. Going for a walk outside | 11 | 75.0 % | 13. Going for a walk outside | 3 | 75 % |
| 1. On a subway platform | 11 | 66.7 % | 3. On a bus | 2 | 50 % |
| 2. On a subway train | 11 | 66.7 % | 5. In a washroom or other place with hard surfaces | 2 | 50 % |
| 11. At a large social gathering or party where I know some/all people | 11 | 66.7 % | 7. Completely alone | 2 | 50 % |
| 5. In a washroom or other place with hard surfaces | 9 | 66.7 % | 14. Exercising with gym equipment | 2 | 50 % |
| 9. With a few people that I have a close relationship with | 6 | 50.0 % | 9. With a few people that I have a close relationship with | 1 | 25 % |
Scoring: Each “Strongly Agree” earned 2 points (pts); each “Somewhat Agree” earned 1 point.
% refers to percentage of PwE who selected “Somewhat Agree” or “Strongly Agree” (n = 12).
Scoring: Each “Agree” earned 1pt.
% refers to percentage of individuals affected by PwE who selected “Agree” (n = 4).
Results
Demographics
A final sample of n = 18 accepted responses was obtained (n = 14 PwE and n = 4 people affected by PwE) (Table 2). The people affected by PwE included professionals (one psychologist, one epileptologist) and family members (one mother, one brother). The average age of PwE was 34.9 years with 57.1 % female. Table C.1 (Appendix C) summarizes reported epilepsy and seizure symptoms. Over half of participants (11/18, or 61.1 %) reported losing muscle control and half (9/18, or 50.0 %) reported losing consciousness during seizures.
Table 2.
Demographics.
| TOTAL PWE | 77.8 % (n = 14) |
|---|---|
| SEX AT BIRTH | |
| Female | 57.1 % (n = 8) |
| Male | 42.9 % (n = 6) |
| AGE (YEARS) | AVG = 34.9 YEARS |
| 18–20 | 21.4 % (n = 3) |
| 21–30 | 28.6 % (n = 4) |
| 31–40 | 14.3 % (n = 2) |
| 41–50 | 14.3 % (n = 2) |
| 51–60 | 14.3 % (n = 2) |
| 60+ | 7.1 % (n = 1) |
| TOTAL AFFECTED BY PWE | 22.2 % (n = 4) |
| TOTAL PARTICIPANTS | n = 18 |
Open-Ended questions
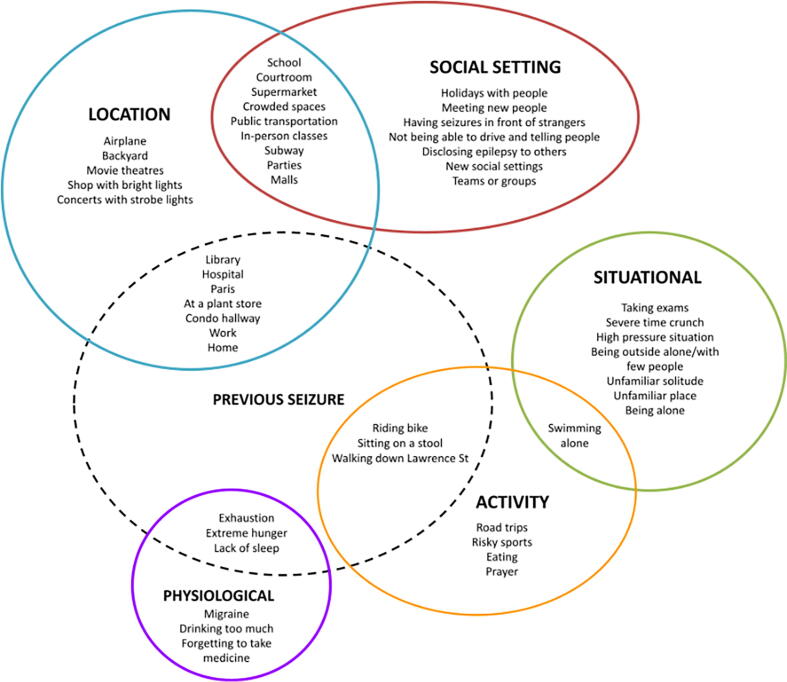
The feared scenes listed by participants were found to fall broadly under six main categories: location, social setting, activity, situational, physiological, and previous seizure. Fig. 2 provides a visual representation of scenes listed by participants based on these categories.
Fig. 2.
Categories of Scenes Identified by Participants.
Reports of feared scenes tied to a previous seizure emerged as separate from scenes that were situational or linked to social settings. Following further thematic analysis, themes from the open-ended responses were synthesized with respect to 1) main categories of exposure scenarios based on location and 2) elements of scenes that increase anxiety related to epilepsy. These themes are summarized in Table 3 and are described in detail below.
Table 3.
Summary of Themes: Exposure Scenario Categories and Factors That Increase Anxiety.
| 1) Main Types of Exposure Location | |
|---|---|
| a) Associated With Past Seizure |
|
| b) Other Locations |
Public Settings
|
| 2) Factors (Fear Elements) that Increase Anxiety | |
| a) Potential for Danger |
i) Unable to get help
|
ii) Physical danger
| |
| b) Social Factors |
i) Number of People
|
ii) Low Familiarity of People
| |
iii) Social Pressures
| |
| c) Presence of Triggers |
i) Stress
|
ii) Sensory/Space
| |
iii) Physiological
| |
iv) Medication
| |
Main categories of exposure location
-
a)
Locations associated with past seizure
Feared locations tied to previous seizures were variable and unique to the individual (e.g., a specific street “Lawrence St.” or store “Petsmart”, or “at home”). Anxiety associated with these locations centered around the fear of having another seizure or specific memories of a previous seizure. For example, one respondent reported that their sister “…will mostly get anxious about her epilepsy when in an environment where she has had a previous seizure. She will actively avoid these select locations when it is reasonable for her to do so.” Another respondent described their ES-interictal anxiety as being strongest when entering their condo hallway to leave their home: “Approximately 80 % of my seizures happen leaving or coming back home to my condo […] I fear leaving my condo and going outside into the public.”
-
b)
Public & social settings
The locations of feared scenes not tied to a previous seizure largely fell into two categories: 1) public settings and 2) social settings. For public settings, respondents reported worry of having a seizure in front of unfamiliar people, as well as a general fear of being out in public. Specific sensory triggers related to certain public spaces (e.g., bright lights/sun, noise) were sometimes specified. Conversely, descriptions of anxiety related to social settings were typically social in nature (e.g., feeling pressured to socialize, be around others, meet new people, or disclose having epilepsy to others), or related to situational stress (e.g., at work or school).
Factors that increase anxiety
-
a)
Scenes with potential for danger consistently related to: 1) activities with a risk for physical danger should a seizure occur, and/or 2) being completely alone or unable to get help. Fears of physical injury were sometimes related to a previous seizure, (e.g., fear of riding a bike or sitting on stools), but not always (e.g., fear of falling on subway rails). For those who reported fear of being unable to get help, some reported anxiety when alone in familiar locations including their own home, backyard, or street. Others reported feeling particularly helpless when there were people around but no one whom they trusted, particularly if they were in an unfamiliar location. One participant explained, “I would be even more anxious if there is no one around that I know because if something were to happen I am not sure who can or would help me.” Another described their feared scene as, “Since I'm in such an unfamiliar place, if I were to have a seizure or start to have an aura, I won't be able to properly give a location to ask/call for help […] I'll be completely vulnerable due to not knowing where I am + loss of consciousness.”
-
b)
Social factors
For public and social settings, anxiety related to social factors centered around the presence of 1) many people or crowds, 2) unfamiliar people, and 3) social pressures. While many respondents reported feeling unsafe without others present, many also described large crowds of people as most anxiety-provoking. Generally, the presence of only strangers or acquaintances was associated with increased anxiety for safety reasons as described above, or due to fear of embarrassment or judgement. For example, one parent explained, “Feeling embarrassed […] continues to be his strongest trigger for anxiety […] he'd “wake up” [after an absence seizure] to scolding by the teacher and laughter from fellow students.” Some respondents also described worrying about upsetting others (e.g., "What if they call an ambulance […] people will get scared.”). Other socially driven fears related to situations that would require the individual to socialize with, or disclose that they have epilepsy to, new people or acquaintances (e.g., “Disclosing my epilepsy to professors or supervisors”, “Others finding out that I have epilepsy”). It is worth mentioning here that although the presence of trusted and familiar people was reported as helpful by some respondents, others reported feelings of guilt about their condition as contributing to their anxiety. For example, one respondent’s feared scene described their child’s hospitalization for mental health reasons. They described anxiety about the impact of their epilepsy on their child: “[My child] has claimed that feeling guilty about my seizures and witnessing them, as well as related conflicts in family relationships, have had traumatic effects on [their] life.”
-
c)
Presence of triggers
Respondents described specific triggers for their ES-interictal anxiety, which fell broadly under the categories of 1) stressful situations, 2) sensory/space related, 3) physiological, and 4) medication-related fears. In each case, the source of anxiety was described as fear of having another seizure after recognizing a known seizure trigger. For one individual, the presence of specific triggers caused more fear than any specific location: “The physical context and location can vary but high-pressure deadlines or details to remember, lack of sleep or hunger, high humidity and unfamiliar routines, big changes, all seem to be triggers.”
Examples of stressful situations included school or work, or were interpersonal in nature, such as dealing with disagreements and family conflict. In some cases, the anxiety described by participants was first related to the specific stressor itself (e.g., fear of flying, fear of failure) and second, centered around effectively managing the stressor to prevent a seizure under stress (e.g., “Should I have a seizure […] I would have to stop studying to relax and sleep as I would lose time where I could be [studying].”).
Sensory/space-related triggers included bright lights or sun, flashing lights (e.g., at concerts), small, crowded or cluttered spaces, and noise. Physiological triggers included extreme hunger/fatigue, headaches, migraines, and drinking too much alcohol. Some participants also described a fear of forgetting to take medication (e.g., “Time freezes and I get nervous. I lose control of my breathing and I can only think about the earliest time I will be able to take my medicine.”).
Closed-Ended questions
Table 4 presents the 14 validation scenes ranked in order from highest to lowest points (column 1), followed by the percentage of respondents who agreed that the situation would provoke ES-interictal anxiety (column 2). PwE ranked having few or no familiar people nearby as highest for provoking anxiety, whether alone or in a public/social setting. Consistent with qualitative findings above, over 50 % of participants agreed that each scene in the matrix would cause ES-interictal anxiety with the exception of the lowest-ranking scenario for both groups: ‘[Being] with a few people that I have a close relationship with’.
Discussion
Through a combination of open- and closed-ended questions we were able to identify a number of anxiety-provoking scenes and commonly feared elements that may be used to inform the design of a VR-ET for PwE. In our sample, feared locations and situations associated with past seizures were varied, highly personalized, and idiosyncratic. Conversely, anxiety-provoking scenes not tied to a past seizure often occurred in public or social settings. Consistency across responses was observed with respect to factors reported to increase or decrease anxiety. These findings broadly support our original assumptions that the following factors increase ES-interictal anxiety: 1) the number of people and 2) level of familiarity with people in a scene, as well as 3) the potential for physical danger and 4) combinations of these factors. We also found that specific triggers (stress, sensory/space-related, and physiological) are elements that may also be built into VR-ET environments to create graded exposure hierarchies.
Our findings indicate that increasing the number of strangers in the environment can lead to increased ES-interictal anxiety due to a fear of embarrassment and/or lack of trust that someone will seek help. General social anxiety (e.g., feeling pressured to interact with unfamiliar people at a party) was also commonly described. On the other hand, having a small number of trusted people nearby, and being in a familiar location were helpful for reducing anxiety, possibly due in part to the anxiety-reducing effect of familiar stimuli [22]. Still, some described their anxiety as related to guilt associated with the emotional distress caused by loved ones witnessing a seizure (e.g., “The fear and concern of my wife made me feel bad.”). Similar feelings of guilt have been described by other people living with chronic conditions [23].
Respondents commonly indicated feeling anxious and often avoiding scenarios that could be dangerous (e.g., exercising with gym equipment, riding a bike, swimming/walking alone). Comparably, elements of the physical environment that pose a greater risk of injury, such as hard or slippery surfaces, have been found to augment fear of falling and avoidance behaviours in people with Parkinson’s disease, in particular when among strangers who may overreact when trying to help [24]. It is important to note that avoiding high-risk activities (e.g., driving, certain sports) may be medically recommended for certain PwE and that avoidance would be considered reasonable in this case [4].
Overall, examples in the data support the assumption that scenes with a combination of factors were more highly anxiety-provoking (e.g., navigating a crowded mall alone with excessive environmental stimuli such as noise and bright lights, with a time pressure). Nevertheless, exactly which combinations of feared elements are most likely to increase anxiety may depend on the specific epilepsy-related anxiety disorder diagnosis. For example, we might hypothesize that for individuals who present primarily with epileptic social phobia, elements related to social fears (e.g., presence of crowds, social interactions with strangers) would affect their level of anxiety more than factors related to physical danger. This notion is supported by our analysis where social situations emerged as more independent from other types of feared scenes. Although additional research will be required to confirm whether this is the case, one study using VR-ET to train coping mechanisms to counter alcohol cravings reported a similar finding where people responded to different factors (i.e., visual alcohol cues vs social pressures) within the scene depending on the type of relationship they had with alcohol (e.g., alcohol dependent vs social drinker) [25].
In designing a VR-ET program, it is necessary to consider which scenarios can be effectively reproduced in a virtual environment, as well as suit a variety of individuals. Although highly personalized exposure scenarios (e.g., based on a previous seizure experience) could prove to be more effective for treating anxiety for a given individual, extensive scene customization can be costly in terms of both time and resources [26], [27]. 360° video is a cost-effective and photo-realistic medium for designing VR-ET scenarios with potential to induce a strong sense of presence within a scene [28], [29], [30], [31]. Based on our results, we predict that tailoring of a VR-ET program for PwE that uses 360° video may be achieved by designing several exposure sets, each addressing different aspects/types of ES-interictal anxiety. Thus, a program may be designed for individuals to select the exposure set and specific scenes that best resonate with their anxiety. To address anxiety resulting from previous seizures without filming highly individualized scenes, exposure sets may include scene variations filmed to simulate the perspective of someone who has just experienced a seizure (i.e., through low camera height and varied reactions of surrounding people).
Based on the results of Phase 1, along with considering which locations could be readily filmable in 360° video and may be common/significant for daily life or social functioning, we propose the following example exposure sets:
SET A: Social Setting (Dinner Party)
Exposure scenes in this set may focus predominantly on incorporating varied social fear elements (e.g., number of people, familiarity of people, social pressures) including social interaction with actors within the scenes.
SET B: Public Setting 1 (Subway)
Scenes in this set may focus on varying elements that can affect a person’s sense of risk of physical harm should a seizure occur. Environmental factors might include noise, lighting, crowds of people, and proximity to subway tracks. Additionally, scenes may involve few or no other people, since some respondents feared being alone and unable to get help in an emergency situation.
SET C: Public Setting 2 (Shopping Centre)
Another exposure set may consider a second common public setting such as a shopping centre, where we alter different elements of the physical environment (e.g., noise, lighting, crowds of people). Some scenes within this scenario may include a task-oriented component requiring social interaction.
It is important to highlight that the proposed VR-ET program is not meant to be a standalone treatment for ES-interictal anxiety. Instead, VR-ET should supplement therapy delivered by a trained clinician for maximum benefit [18]. Cognitive behavioural therapy (CBT) is considered to be the primary treatment for anxiety disorders in PwE [5]. Additionally, we recommend that the design of exposure scenarios include consultation with specialists (e.g., epileptologists, psychologists) to ensure that the program is safe for PwE.
Limitations
The novelty of this research, methodology, and small sample size presents limitations that impact the generalizability of the findings. First, the study included a relatively small sample of participants (n = 18). Many scenes did not include detailed descriptions, and without greater context, it was not possible to know the specific underlying cause for the individual’s anxiety. Likewise, some scenes were clearly described as linked to previous seizures (e.g., a condo hallway) as opposed to other fears, but other cases were unclear. Responses to open-ended questions were not mandatory, and skipped questions further reduced the number of useful responses available for analysis. A further limitation of our dataset is that we were not able to describe whether any differences may exist based on epilepsy/seizure type, (i.e., in individuals who lose consciousness during a seizure vs in those who do not) or any other key demographics. As knowledge of such differences may be relevant to designing effective exposure scenarios, follow-up studies with larger and more diverse samples will be required.
Additionally, the questionnaire was designed to be anonymous, collected limited personal information, and was distributed through social media links. Consequently, it was necessary for the researchers to determine “true” respondents to the questionnaire by examining the data. It is possible that some legitimate questionnaires were excluded, however a rigorous process of sorting the responses (see Appendix D) was followed by two coders to reduce this risk. We must also acknowledge the limitation that voluntary online surveys can introduce a sampling bias due to selective non-response.
Finally, little prior work has been done in this area and evidence on ES-interictal anxiety is overall scarce. As such, we are not able to directly compare to other literature in terms of how the fears described by respondents may be used to create virtual scenes. Further qualitative research will be needed to gather information from a larger sample size, and to collect more in-depth responses from individuals (e.g., such as through interviews). We plan to interview participants when piloting scenes in Phase 3 to collect their feedback on how effectively these virtual scenes recreated the feared scenarios and presented a graded exposure hierarchy.
Conclusion
This paper describes the results from Phase 1 of the AnxEpiVR pilot, which to our knowledge, is the first study to design and evaluate a VR-ET to treat ES-interictal anxiety in PwE. Given the relative paucity of literature describing how ES-interictal anxiety is experienced, our findings add to the body of knowledge on treating anxiety more generally in this population. We identified a number of common themes across scenes feared by PwE and discussed implications for designing VR exposure hierarchies to capture these elements. These findings provide a foundation for designing exposure scenarios that include public locations and social settings in combination with varying levels of factors that increase ES-interictal anxiety.
Funding
This work was conducted with financial support obtained through a Junior Faculty Fund and Minor Research Grant from York University.
Ethics
This study received Research Ethics Board approval by the York University Human Participants Review Committee (certificate number: 2022-105) on May 31, 2022.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgements
The authors wish to thank Dr. David Gold (Toronto Western Hospital) for providing consultation during the development of the study protocol. We would also like to thank Epilepsy Toronto for their support with recruiting Phase 1 participants.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.ebr.2023.100588.
Appendix A. Supplementary data
The following are the Supplementary data to this article:
References
- 1.Kerr M.P. The impact of epilepsy on patients’ lives. Acta Neurol Scand. 2012;126(s194):1–9. doi: 10.1111/ane.12014. [DOI] [PubMed] [Google Scholar]
- 2.Mula M., Kanner A.M., Jetté N., Sander J.W. Psychiatric Comorbidities in People With Epilepsy. Neurol Clin Pract. 2021;11(2):e112–e120. doi: 10.1212/CPJ.0000000000000874. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Ertan D., Hubert-Jacquot C., Maillard L., Sanchez S., Jansen C., Fracomme L., et al. Anticipatory anxiety of epileptic seizures: An overlooked dimension linked to trauma history. Seizure - Eur J Epilepsy. 2021;1(85):64–69. doi: 10.1016/j.seizure.2020.12.006. [DOI] [PubMed] [Google Scholar]
- 4.Hingray C., McGonigal A., Kotwas I., Micoulaud-Franchi J.A. The Relationship Between Epilepsy and Anxiety Disorders. Curr Psychiatry Rep. 2019;21(6):40. doi: 10.1007/s11920-019-1029-9. [DOI] [PubMed] [Google Scholar]
- 5.Mula M. Treatment of anxiety disorders in epilepsy: An evidence-based approach. Epilepsia. 2013;54(s1):13–18. doi: 10.1111/epi.12101. [DOI] [PubMed] [Google Scholar]
- 6.Munger Clary H.M. Epilepsy-Specific Anxiety: A Potential Clue to the Seizure Onset Zone. Epilepsy Curr. 2022;22(5):285–287. doi: 10.1177/15357597221109345. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Newsom-Davis I., Goldstein L.H., Fitzpatrick D. Fear of seizures: an investigation and treatment. Seizure. 1998;7(2):101–106. [PubMed] [Google Scholar]
- 8.Blocher J.B., Fujikawa M., Sung C., Jackson D.C., Jones J.E. Computer-assisted cognitive behavioral therapy for children with epilepsy and anxiety: A pilot study. Epilepsy Behav. 2013;27(1):70–76. doi: 10.1016/j.yebeh.2012.12.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Abramowitz J.S. The Practice of Exposure Therapy: Relevance of Cognitive-Behavioral Theory and Extinction Theory. Behav Ther. 2013;44(4):548–558. doi: 10.1016/j.beth.2013.03.003. [DOI] [PubMed] [Google Scholar]
- 10.Carl E., Stein A.T., Levihn-Coon A., Pogue J.R., Rothbaum B., Emmelkamp P., et al. Virtual reality exposure therapy for anxiety and related disorders: A meta-analysis of randomized controlled trials. J Anxiety Disord. 2019;61:27–36. doi: 10.1016/j.janxdis.2018.08.003. [DOI] [PubMed] [Google Scholar]
- 11.Powers M.B., Emmelkamp P.M.G. Virtual reality exposure therapy for anxiety disorders: A meta-analysis. J Anxiety Disord. 2008;22(3):561–569. doi: 10.1016/j.janxdis.2007.04.006. [DOI] [PubMed] [Google Scholar]
- 12.Wiebe A., Kannen K., Selaskowski B., Mehren A., Thöne A.K., Pramme L., et al. Virtual reality in the diagnostic and therapy for mental disorders: A systematic review. Clin Psychol Rev. 2022;98 doi: 10.1016/j.cpr.2022.102213. [DOI] [PubMed] [Google Scholar]
- 13.Shin B., Oh J., Kim B.H., Kim H.E., Kim H., Kim S., et al. Effectiveness of Self-Guided Virtual Reality-Based Cognitive Behavioral Therapy for Panic Disorder: Randomized Controlled Trial. JMIR Ment Health. 2021;8(11):e30590. doi: 10.2196/30590. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Freitas L., de Araújo V.S., Magalhães F., Marinho V., Ayres C., Teixeira S., et al. Virtual reality exposure therapy for neuro-psychomotor recovery in adults: a systematic review. Disabil Rehabil Assist Technol. 2021;16(6):646–652. doi: 10.1080/17483107.2019.1688400. [DOI] [PubMed] [Google Scholar]
- 15.Deng W., Hu D., Xu S., Liu X., Zhao J., Chen Q., et al. The efficacy of virtual reality exposure therapy for PTSD symptoms: A systematic review and meta-analysis. J Affect Disord. 2019;1(257):698–709. doi: 10.1016/j.jad.2019.07.086. [DOI] [PubMed] [Google Scholar]
- 16.Wechsler TF, Kümpers F, Mühlberger A. Inferiority or Even Superiority of Virtual Reality Exposure Therapy in Phobias?—A Systematic Review and Quantitative Meta-Analysis on Randomized Controlled Trials Specifically Comparing the Efficacy of Virtual Reality Exposure to Gold Standard in vivo Exposure in Agoraphobia, Specific Phobia, and Social Phobia. Front Psychol [Internet]. 2019 [cited 2022 Dec 6];10. Available from: https://www.frontiersin.org/articles/10.3389/fpsyg.2019.01758. [DOI] [PMC free article] [PubMed]
- 17.Bouchard S., Dumoulin S., Robillard G., Guitard T., Klinger É., Forget H., et al. Virtual reality compared with in vivo exposure in the treatment of social anxiety disorder: a three-arm randomised controlled trial. Br J Psychiatry J Ment Sci. 2017;210(4):276–283. doi: 10.1192/bjp.bp.116.184234. [DOI] [PubMed] [Google Scholar]
- 18.Boeldt D., McMahon E., McFaul M., Greenleaf W. Using Virtual Reality Exposure Therapy to Enhance Treatment of Anxiety Disorders: Identifying Areas of Clinical Adoption and Potential Obstacles. Front Psychiatry. 2019;25(10):773. doi: 10.3389/fpsyt.2019.00773. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Gray H.G., Tchao D., Lewis S., Pardini S., Harris L., Appel L. Virtual Reality Therapy for People With Epilepsy and Related Anxiety (AnxEpiVR): Protocol for a Three-Phase Pilot Clinical Trial [Internet] JMIR Preprints. 2022 https://www.researchprotocols.org/2023/1/e41523 [cited 2022 Dec 6]. Available from: [Google Scholar]
- 20.Glaser B, Strauss A. The Discovery of Grounded Theory: Strategies for Qualitative Research. Aldine Transaction; 1967. 282 p.
- 21.Hallberg L.R.M. The “core category” of grounded theory: Making constant comparisons. Int J Qual Stud Health Well-Being. 2006;1:141–148. [Google Scholar]
- 22.Orive R., Gerard H.B. The familiar stimulus as a reducer of anxiety: An experimental study. J Soc Clin Psychol. 1987;5:330–338. [Google Scholar]
- 23.Fusi-Schmidhauser T., Froggatt K., Preston N. Living with Advanced Chronic Obstructive Pulmonary Disease: A Qualitative Interview Study with Patients and Informal Carers. COPD. 2020;17(4):410–418. doi: 10.1080/15412555.2020.1782867. [DOI] [PubMed] [Google Scholar]
- 24.Jonasson S.B., Nilsson M.H., Lexell J., Carlsson G. Experiences of fear of falling in persons with Parkinson’s disease – a qualitative study. BMC Geriatr. 2018;18(1):44. doi: 10.1186/s12877-018-0735-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Lee J.S., Namkoong K., Ku J., Cho S., Park J.Y., Choi Y.K., et al. Social pressure-induced craving in patients with alcohol dependence: application of virtual reality to coping skill training. Psychiatry Investig. 2008;5(4):239–243. doi: 10.4306/pi.2008.5.4.239. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Pardini S., Gabrielli S., Dianti M., Novara C., Zucco G.M., Mich O., et al. The Role of Personalization in the User Experience, Preferences and Engagement with Virtual Reality Environments for Relaxation. Int J Environ Res Public Health. 2022;19(12):7237. doi: 10.3390/ijerph19127237. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Pizzoli SFM, Mazzocco K, Triberti S, Monzani D, Alcañiz Raya ML, Pravettoni G. User-Centered Virtual Reality for Promoting Relaxation: An Innovative Approach. Front Psychol [Internet]. 2019 [cited 2022 Dec 6];10. Available from: https://www.frontiersin.org/articles/10.3389/fpsyg.2019.00479. [DOI] [PMC free article] [PubMed]
- 28.Ionescu A., Van Daele T., Rizzo A., Blair C., Best P. 360° Videos for Immersive Mental Health Interventions: a Systematic Review. J Technol Behav Sci. 2021;6(4):631–651. [Google Scholar]
- 29.Reeves R., Elliott A., Curran D., Dyer K., Hanna D. 360° Video virtual reality exposure therapy for public speaking anxiety: A randomized controlled trial. J Anxiety Disord. 2021;1(83) doi: 10.1016/j.janxdis.2021.102451. [DOI] [PubMed] [Google Scholar]
- 30.Lundin J., Lundström A., Gulliksen J., Blendulf J., Ejeby K., Nyman H., et al. Using 360-degree videos for virtual reality exposure in CBT for panic disorder with agoraphobia: a feasibility study. Behav Cogn Psychother. 2022;50(2):158–170. doi: 10.1017/S1352465821000473. [DOI] [PubMed] [Google Scholar]
- 31.Holmberg T.T., Eriksen T.L., Petersen R., Frederiksen N.N., Damgaard-Sørensen U., Lichtenstein M.B. Social Anxiety Can Be Triggered by 360-Degree Videos in Virtual Reality: A Pilot Study Exploring Fear of Shopping. Cyberpsychology Behav Soc Netw. 2020;23(7):495–499. doi: 10.1089/cyber.2019.0295. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.